NHMRC Glaucoma Guidelines - ANZGIG
NHMRC Glaucoma Guidelines - ANZGIG
NHMRC Glaucoma Guidelines - ANZGIG
You also want an ePaper? Increase the reach of your titles
YUMPU automatically turns print PDFs into web optimized ePapers that Google loves.
<strong>NHMRC</strong> GUIDELINES FOR THE SCREENING, PROGNOSIS, DIAGNOSIS, MANAGEMENT AND PREVENTION OF GLAUCOMA<br />
Chapter 7 – Diagnosis of glaucoma<br />
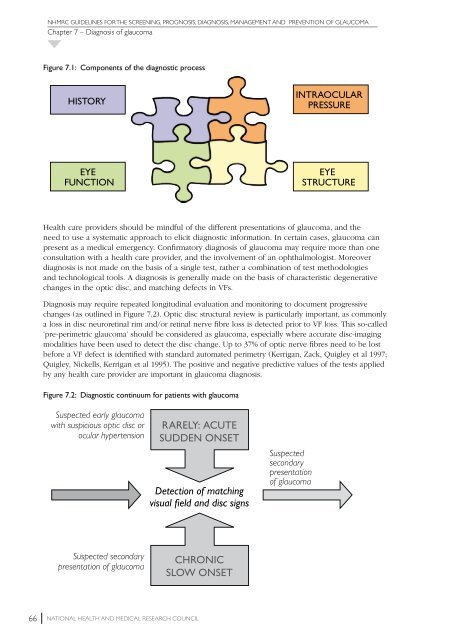
Figure 7.1: Components of the diagnostic process<br />
HISTORY<br />
INTRAOCULAR<br />
PRESSURE<br />
EYE<br />
FUNCTION<br />
EYE<br />
STRUCTURE<br />
Health care providers should be mindful of the different presentations of glaucoma, and the<br />
need to use a systematic approach to elicit diagnostic information. In certain cases, glaucoma can<br />
present as a medical emergency. Confirmatory diagnosis of glaucoma may require more than one<br />
consultation with a health care provider, and the involvement of an ophthalmologist. Moreover<br />
diagnosis is not made on the basis of a single test, rather a combination of test methodologies<br />
and technological tools. A diagnosis is generally made on the basis of characteristic degenerative<br />
changes in the optic disc, and matching defects in VFs.<br />
Diagnosis may require repeated longitudinal evaluation and monitoring to document progressive<br />
changes (as outlined in Figure 7.2). Optic disc structural review is particularly important, as commonly<br />
a loss in disc neuroretinal rim and/or retinal nerve fibre loss is detected prior to VF loss. This so-called<br />
‘pre-perimetric glaucoma’ should be considered as glaucoma, especially where accurate disc-imaging<br />
modalities have been used to detect the disc change. Up to 37% of optic nerve fibres need to be lost<br />
before a VF defect is identified with standard automated perimetry (Kerrigan, Zack, Quigley et al 1997;<br />
Quigley, Nickells, Kerrigan et al 1995). The positive and negative predictive values of the tests applied<br />
by any health care provider are important in glaucoma diagnosis.<br />
Figure 7.2: Diagnostic continuum for patients with glaucoma<br />
Suspected early glaucoma<br />
with suspicious optic disc or<br />
ocular hypertension<br />
Rarely: Acute<br />
sudden onset<br />
Detection of matching<br />
visual field and disc signs<br />
Suspected<br />
secondary<br />
presentation<br />
of glaucoma<br />
Suspected secondary<br />
presentation of glaucoma<br />
chronic<br />
slow onset<br />
66 National Health and Medical Research Council