programma & abstracts - Nederlandse Vereniging voor Radiologie
programma & abstracts - Nederlandse Vereniging voor Radiologie
programma & abstracts - Nederlandse Vereniging voor Radiologie
You also want an ePaper? Increase the reach of your titles
YUMPU automatically turns print PDFs into web optimized ePapers that Google loves.
16<br />
29 en 30 september 2011<br />
radio<br />
logen<br />
dagen<br />
m e c c , m a a s t r i c h t<br />
<strong>Nederlandse</strong> <strong>Vereniging</strong> <strong>voor</strong> <strong>Radiologie</strong><br />
Radiological Society of the Netherlands<br />
<strong>programma</strong> & <strong>abstracts</strong>
<strong>programma</strong> <strong>voor</strong>woord & <strong>abstracts</strong><br />
Kwaliteit<br />
Dames en heren, geachte leden van de <strong>Nederlandse</strong> <strong>Vereniging</strong> <strong>voor</strong> <strong>Radiologie</strong>,<br />
Welkom in Maastricht op de Radiologendagen 2011! Het thema dit lustrumjaar is Kwaliteit.<br />
Kwaliteitseisen in de gezondheidszorg worden steeds meer opgelegd en zijn belangrijk <strong>voor</strong> een goede praktijkvoering. Dit<br />
geldt uiteraard ook <strong>voor</strong> de radiologie, dan bij <strong>voor</strong>keur door ons als vereniging zelf de eisen opgesteld en in goede samenwerking<br />
met onze klinische collega’s.<br />
Voor de hand liggend is het om kwalitatief beter te worden door te leren van eigen fouten. Het <strong>programma</strong> begint donderdagochtend<br />
daarom met ‘Deze misser maak je maar 1 keer’.<br />
In de tweede plenaire sessie op donderdag ‘Setting standards in healthcare – many ways, no return’ zal het onderwerp<br />
kwaliteit belicht worden door gastsprekers Dr. M-J Vrancken Peeters (chirurg, NKI-AvL) en Prof. Dr. D. Rubin (radioloog,<br />
Stanford University, USA).<br />
Op vrijdag zal er door een drietal pro-con koppels worden gedebatteerd over het hanteren van kwaliteitsnormen: ‘Pro-con:<br />
setting standards in healthcare – which way to go?’.<br />
Nieuw onderwerp bij de parallelsessies is de Educatieve Voordracht. Dit is bedoeld om onderwerpen welke direct toepasbaar<br />
zijn in uw praktijk, maar (nog) niet zijn verworden tot een wetenschappelijk artikel.<br />
Bij alle wetenschappelijke abstract sessies zijn hierbij passende keynote lectures gezocht.<br />
De ‘Research Corner’ uit 2009 is gestoken in een nieuw jasje. Acht UMC’s presenteren niet alleen hun spraakmakende<br />
wetenschappelijke onderzoeken, maar steken ook de hand naar elkaar uit, om samen beter te worden.<br />
De Refresher Courses op beide dagen worden deels verzorgd door toonaangevende gastsprekers uit het buitenland. Aan de<br />
hand van de verstrekte leerdoelen kunt u beter schatten of een onderwerp uw belangstelling heeft.<br />
Wij zijn buitengewoon verheugd een aantal van u ook een workshop te kunnen aanbieden. De geluksvogels onder u gaan<br />
statistisch gezien herboren naar huis en met bouwstenen <strong>voor</strong> een robuuste teachingfile (millennium proof). Lees <strong>voor</strong> details<br />
het volledige <strong>programma</strong>.<br />
Dit jaar is er een andere formule gekozen <strong>voor</strong> de verschillende prijzen. Naast de bekende Philipsprijs en Radiologendagen<br />
prijs zal er een toelichting op en uitreiking van de NVvR Travel Grant plaatsvinden.<br />
Bent u dit jaar niet in de prijzen gevallen dan bent u niet minder welkom in feestelijke kleding op het Diner & Galafeest met<br />
als thema ‘Dress to impress’. Op een prachtige locatie in Maastricht wordt u op zuidelijke wijze verwend.<br />
De radiologendagen kunnen mede mogelijk worden gemaakt door sponsoring van de industrie, u wordt dan ook van harte<br />
uitgenodigd om met de industrie in contact te komen op de expositie.<br />
Onze dank gaat uit naar de inzet van velen, zichtbaar in het <strong>programma</strong> boekje. Namen noemen is ontoereikend, enthousiaste<br />
deelnemers is uw verdienste.<br />
Veel plezier op de radiologendagen 2011!<br />
Bert-Jan de Bondt, <strong>voor</strong>zitter<br />
Vincent Cappendijk<br />
Marion Smits<br />
Bart Wiarda<br />
Henk-Jan van der Woude
16 E RADIOLOGENDAGEN 2011<br />
Organisatie<br />
Organisatie Comité<br />
Bert-Jan de Bondt, <strong>voor</strong>zitter<br />
Vincent Cappendijk<br />
Marion Smits<br />
Bart Wiarda<br />
Henk-Jan van der Woude<br />
WETENSCHAPPELIJK COMITÉ<br />
Henk Jan Baarslag<br />
Ludo Beenen<br />
Marc Engelbrecht<br />
Nanko de Graaf<br />
Jan-Cees de Groot<br />
Ieneke Hartmann<br />
Mechli Imhof-Tas<br />
Simone Jap-a-Joe<br />
Viola Koen<br />
Martin Kraai<br />
Krijn van Lienden<br />
Ruud Pijnappel<br />
Stefan Steens<br />
Joachim Wilberger<br />
CONGRESSECRETARIAAT<br />
Postbus 2428<br />
5202 CK ‘s-Hertogenbosch<br />
Tel 073 700 3500<br />
Fax 073 700 3505<br />
info@congresscompany.com<br />
www.congresscompany.com<br />
1 6 E R A D I O L O G E N D A G E N - 2 9 e n 3 0 S E P T E M B E R 2 0 1 1 1
<strong>programma</strong> & <strong>abstracts</strong><br />
<strong>programma</strong><br />
Donderdag 29 september 2011<br />
Tijdstip<br />
Onderwerp<br />
TRAJECTUM<br />
10.00 - 10.40 Ontvangst & registratie<br />
AUDITORIUM 2<br />
10.40 - 10.45 Opening door <strong>voor</strong>zitter<br />
Dr. R.B.J. de Bondt, Isala klinieken, Zwolle<br />
AUDITORIUM 2<br />
10.45 - 12.00 Plenaire sessie: Deze misser maak je maar één keer<br />
Voorzitter: Mw. Drs. V.H. Koen, Kennemer Gasthuis, Haarlem<br />
Dr. K.P. van Lienden, AMC, Amsterdam<br />
Mw. Dr. C.S.P. van Rijswijk, LUMC, Leiden<br />
Dr. M.W. de Haan, MUMC, Maastricht<br />
EXPOFOYER<br />
12.00 - 13.00 Lunch<br />
EXPOFOYER<br />
12.15 - 12.45 Postersessie<br />
AUDITORIUM 2<br />
13.00 - 14.00 Plenaire sessie: Setting standards in healthcare - many ways, no return<br />
Kwaliteitseisen opgelegd door de zorgverzekeraar, maar ook die van de heelkundige beroepsvereniging<br />
zijn opmerkelijk in het nieuws geweest. Onvermijdelijk dat de radiologie hiermee te maken krijgt. Van<br />
buitenaf opgelegd dan wel zelf opgesteld. In deze sessie schetst dr. M-J. Vrancken Peeters, chirurg en<br />
woordvoerster van de NVvH, de aanloop tot -en achtergrond van de recent gepubliceerde kwaliteitseisen<br />
<strong>voor</strong> oncologische chirurgie. Vervolgens stelt dr. D. Rubin een ambitieuze maar praktische manier<br />
<strong>voor</strong> om de kwaliteit van het radiologisch werk te verbeteren.<br />
Inleiding door: Prof. dr. J.S. Laméris, AMC, Amsterdam<br />
Gastsprekers:<br />
Dr. M-J. Vrancken Peeters, chirurg, NKI-AvL, Amsterdam<br />
Prof. D. Rubin, Stanford University, USA<br />
14.05 - 15.35 Parallelsessies vrije <strong>voor</strong>drachten<br />
Voorafgaand aan de wetenschappelijke <strong>voor</strong>drachten zal iedere sessie aanvangen met een keynote lecture.<br />
ZAAL 2.1 COLORADO<br />
Sessie 1: Abdominale radiologie 1<br />
Voorzitters: Dr. R.F.A. Vliegen, Atrium MC, Heerlen & Drs. J.E. van den Bergh, AMC, Amsterdam<br />
PET-MRI: tool or toy<br />
Dr. J. Buscombe, Addenbrooke’s Hospital, Cambridge, UK<br />
Learning objectives:<br />
Understand technical issues of PET/MR<br />
Look at possible indications for PET/MR<br />
Understand some of the issues for nuclear medicine staff<br />
The first PET/MR machines are now on the market for €2 million. However there are significant<br />
technical issues including just trying to acquire images. What compromises are made in terms of image<br />
quality for both PET and MR. How can attenuation correction be applied? Once these technical issues<br />
have been resolved is PET/MR just a technique looking for an indication?<br />
ZAAL 0.8 ROME<br />
Sessie 2: Abdominale radiologie / Acute radiologie / Diversen<br />
Voorzitters: Mw. M.A. Stam, Medisch Centrum Alkmaar & L.F.M. Beenen, AMC, Amsterdam<br />
Alternatieve diagnoses bij MRI appendicitis<br />
Mw. M.A. Stam, Medisch Centrum Alkmaar, Alkmaar<br />
ZAAL 0.5 PARIS<br />
Sessie 3: Cardiovasculaire radiologie<br />
Voorzitters: Dr. H.J. Lamb, LUMC, Leiden & H.C.M. van den Bosch, Catharina Ziekenhuis, Eindhoven<br />
MRI bij diabetes en metabool syndroom<br />
Dr. H.J. Lamb, LUMC, Leiden<br />
ZAAL 0.9 ATHENS<br />
Sessie 4: Mammadiagnostiek 1<br />
Voorzitters: Dr. M.J.C.M. Rutten, Jeroen Bosch Ziekenhuis & Mw. K.M. Duvivier, UMC Utrecht, Utrecht<br />
3D echografie van de mamma; een poor mans MRI?<br />
Dr. M.J.C.M. Rutten, Jeroen Bosch Ziekenhuis, ‘s-Hertogenbosch<br />
ZAAL 0.4 BRUSSELS<br />
Sessie 5: Interventieradiologie / Cardiovasculaire radiologie<br />
Voorzitters: Dr. M.W. de Haan, MUMC, Maastricht & L.W. Kaufmann, Spaarne Ziekenhuis, Hoofddorp<br />
Update abdominale endoprothesen<br />
Dr. M.W. de Haan, MUMC, Maastricht<br />
AUDITORIUM 2<br />
Research Corner<br />
Voorzitters: Mw. Prof. dr. R.G.H. Beets-Tan, MUMC, Maastricht & Prof. dr. J.S. Laméris, AMC, Amsterdam<br />
Tijdens deze parallelsessie zullen de 8 UMC’s de gelegenheid hebben een presentatie te geven van een<br />
hoogstaand en origineel onderzoeksproject. Van het project wordt een kort overzicht gegeven. Duidelijk<br />
zal worden wat de positie van het onderzoek is ten opzichte van andere groepen in Nederland en daarbuiten,<br />
en wat het perspectief van het onderzoek is in 5 a 10 jaar van nu. Tot slot wordt aangegeven<br />
met welke additionele (externe?) kennis, men dit perspectief verwacht eerder te kunnen halen.<br />
2<br />
k i j k o o k o p w w w . c o n g r e s s c o m p a n y . c o m<br />
o f w w w . r a d i o l o g e n . n l
Tijdstip<br />
Onderwerp<br />
16 E RADIOLOGENDAGEN 2011<br />
EXPOFOYER<br />
15.35 - 16.00 Theepauze<br />
LUMC: Toepassingen van ultrahoogveld MRI bij patientenpopulaties<br />
Prof. dr. M.A. van Buchem<br />
Erasmus MC: Population Imaging<br />
Prof. dr. A. van der Lugt<br />
UMC Groningen: Screening for Coronary Artery Disease by Non-invasive Imaging in Patients with<br />
known Extra-cardiac Atherosclerotic Disease: the GROUND-2 study<br />
Mw. Dr. R. Vliegenthart<br />
VUMC: Pseudo-continuous arterial spin-labeling at 3T in Alzheimer’s disease<br />
Drs. M.A.A. Binnewijzend<br />
UMC St Radboud: MR gestuurde prostaat interventies; klaar <strong>voor</strong> de praktijk?<br />
Dr. J.J. Fütterer<br />
MUMC: Wait and See in rectal cancer patients: selection by imaging and outcome<br />
Mw. Drs. M. Maas & Mw. Prof. dr. R.G.H. Beets-Tan<br />
AMC: Neurotransmitters in de MRI<br />
Mw. Dr. L. Reneman, neuroradioloog<br />
UMC Utrecht: MRI-guided High Intensity Focused Ultrasound: The future of tumor ablation?<br />
Dr. M.A.A.J. van den Bosch<br />
16.00 - 17.15 Refresher courses<br />
ZAAL 0.4 BRUSSELS<br />
Chronische thrombo-embolische pulmonale hypertensie<br />
Voorzitter: Dr. H.W. van Es, St. Antonius Ziekenhuis, Nieuwegein<br />
Het klinisch gezichtspunt<br />
L. van den Toorn, Erasmus MC, Rotterdam<br />
Leerdoelen:<br />
* De patient met pulmonale hypertensie bestaat (niet)?<br />
* Work-up van patiënten met (vermoeden) pulmonale hypertensie<br />
* Wat zijn de verschillende behandelingen (medicamenteus en chirurgisch).<br />
CT beeldvorming<br />
Mw. Dr. W. van Lankeren, Erasmus MC, Rotterdam<br />
Leerdoelen:<br />
* Welk protocol bij analyse pulmonale hypertensie?<br />
* Wat zijn de direct en indirecte kenmerken CTEPH op CT?<br />
* Wat zijn de pitfalls?<br />
MRI beeldvorming<br />
Prof. dr. A. Vonk-Noordegraaf, VUMC, Amsterdam<br />
Leerdoelen:<br />
* Welk protocol bij analyse pulmonale hypertensie?<br />
* Wat zijn de direct en indirecte kenmerken CTEPH op CT?<br />
* Toegevoegde waarde van functionele informatie?<br />
Chirurgie<br />
Dr. W.J. Morshuis, St. Antonius Ziekenhuis, Nieuwegein<br />
Leerdoelen:<br />
* Wat zijn de operatie-indicaties<br />
* Wat houdt CTEPH chirurgie in?<br />
* Post-operatief beloop: succes gegarandeerd?<br />
Paneldiscussie<br />
Leerdoel:<br />
Kunnen MRI en CT angiografie vervangen?<br />
ZAAL 0.8 ROME<br />
Beeldvorming bij groei- en puberteitsstoornissen<br />
Voorzitter: Drs. N. de Graaf, Erasmus MC, Rotterdam<br />
Beeldvorming<br />
Mw. A.M.J.B. Smets, AMC, Amsterdam<br />
What the clinician wants to know!<br />
Drs. N. Zwaveling-Soonawala, kinderarts-endocrinoloog, EKZ-AMC, Amsterdam<br />
Leerdoelen:<br />
Beeldvorming bij groei- en puberteitsstoornissen<br />
Beeldvorming is een essentieel onderdeel in de work-up van een slecht of juist te snel groeiend kind,<br />
van een puberteit die te lang op zich laat wachten of juist te vroeg begint.<br />
Beeldvormers beschikken over een palet aan technieken om de kinderarts te ondersteunen in<br />
de diagnostiek van deze problemen. Na deze refresher course, weet u meer over de achtergrond van<br />
groei- en puberteitsstoornissen, beheerst u welke radiologische onderzoeken sleutels kunnen zijn in<br />
het oplossen van een endocrinologisch probleem bij kinderen en hoe u deze modaliteiten optimaal kunt<br />
inzetten.<br />
ZAAL 2.1 COLORADO<br />
What is the best imaging modality for ‘aseptic/low grade infection/infectious<br />
loosening of joint prostheses?’<br />
Chairman: Dr. A. Ginai, AMC, Amsterdam & Erasmus MC, Rotterdam<br />
Imaging of Total Hip Replacement and Complications<br />
Dr. A. Ginai, AMC, Amsterdam & Erasmus MC, Rotterdam<br />
Learning objectives:<br />
* Various types of hip prostheses and their radiological appearances.<br />
* Recognition of postoperative complications.<br />
* Role of imaging in diagnosis of prosthetic loosening.<br />
* Recommendations and an algorithm for imaging in ‘a patient with painful total hip arthroplasty or THP’<br />
1 6 E R A D I O L O G E N D A G E N - 2 9 e n 3 0 S E P T E M B E R 2 0 1 1 3
<strong>programma</strong> & <strong>abstracts</strong><br />
Tijdstip<br />
Onderwerp<br />
Radionuclide imaging of the problematical prosthetic hip<br />
Dr. J. Buscombe, Addenbrooke’s Hospital, Cambridge, UK<br />
Learning objectives:<br />
Understand the role of multiphase scintigraphy in the painful hip prosthesis<br />
Understand advantages and problems of labelled leucocyte imaging in the painful hip prosthesis<br />
Understand the interaction of nuclear medicine and other investigations.<br />
Whilst many areas of clinical practice has been lost to nuclear medicine the assessment of the painful<br />
hip prosthesis remains a common indication. The incidence of infected hip prosthesis is less than that<br />
for the knee (1% vs4%) but hip replacements remain more common. In many cases pain in a hip<br />
prosthesis is not due to infection or loosening but the advantage of nuclear medicine techniques is their<br />
high negative predictive value. However care must be taken when using various scintigraphic<br />
techniques to ensure an accurate final diagnosis is established.<br />
AUDITORIUM 2<br />
Respons monitoring made sexy<br />
Chairman: Dr. B. Brans, nucleair geneeskundige, MUMC, Maastricht<br />
Accurate respons monitoring is crucial for the patient<br />
Prof. dr. H.C. Schouten, hemato-oncologist, MUMC, Maastricht<br />
Learning objectives:<br />
Refresh knowledge about respons workhorses RECIST and HOVON<br />
Advantages and disadvantages of these workhorses<br />
What does the oncologist do with the (standardized) radiology report?<br />
Learn about the impact of respons monitoring on survival, management, and complications<br />
Respons monitoring, State of the art<br />
Prof. Dr. V. Vandecaveye, UZ Leuven, Belgium<br />
Learning objectives:<br />
Overview of methods of respons monitoring of the near future (automatic volume measurements, DWI,<br />
dynamic postcontrast imaging, PETCT/PETMRI, other?)<br />
Work out of 1 or 2 of these techniques; how do I, interpretation, reporting (with emphasize on daily<br />
practice)<br />
Information technology solutions for practical implementation of these new techniques<br />
Prof. D. Rubin, Stanford University, USA<br />
Learning objectives:<br />
* Learn about IT developments which can accelerate introduction of new techniques in daily practice<br />
* Learn about IT developments which can accelerate introduction of quantitative imaging in daily practice<br />
* Learn about basic IT concepts to achieve your optimal workflow -learn about who can do this for you<br />
ZAAL 0.5 PARIS<br />
Neuroanatomie <strong>voor</strong> dummies<br />
Voorzitter: Prof. dr. F.A. Barkhof, VUMC, Amsterdam<br />
Oppervlakte en diepte anatomie - chirurgische landmarks<br />
Prof. dr. F.A. Barkhof, VUMC, Amsterdam<br />
Functionele anatomie - toepassingen fMRI en tractografie<br />
Prof. dr. S. Sunaert, UZ Leuven, België<br />
Vasculaire anatomie - arteriële en veneuze territoirs<br />
Dr. G.J. Lycklama à Nijeholt, MCH Westeinde, Den Haag<br />
Leerdoelen:<br />
Kennis van anatomie vormt de basis van elke radiologische interpretatie. Gezien de complexiteit van de<br />
hersenanatomie geldt dat zeker ook <strong>voor</strong> de Neuroradiologie. Toenemende scankwaliteit en geavanceerde<br />
beeldvormingstechnieken zoals fMRI en DTI maken het mogelijk steeds meer descriptieve en<br />
functionele anatomie af te beelden van zowel cortex als subcorticale structuren. Kennis hiervan is van<br />
belang <strong>voor</strong> goede diagnostiek en planning van therapie. Deze ‘refresher course’ behandelt aan de hand<br />
van state-of-the-art MRI beelden de descriptieve en functionele anatomie van de cortex, diepe kernen,<br />
vezelbanen en vasculaire territoria en reikt praktische tips aan <strong>voor</strong> een klinisch relevante beschrijving<br />
van afwijkingen van deze structuren. Het volgen van deze cursus zal hopelijk leiden tot een verbetering<br />
van uw neuroradiologische verslagen. Verder kan de verworven kennis uw inzicht in ziekteprocessen<br />
vergroten, en zullen uw diagnostisch arsenaal en didactische vaardigheden toenemen.<br />
ZAAL 0.2 BERLIN<br />
Workshop “Interpretatie van radiologisch wetenschappelijk onderzoek”<br />
Mw. Dr. S. Spronk, klinisch epidemioloog, Erasmus MC, Rotterdam<br />
Leerdoelen:<br />
* Het toepassen van risicomaten zoals incidentiecijfer en cumulatieve incidentie, en de effectmaten<br />
zoals relatief risico, (populatie-)attributief risico<br />
* Het beoordelen van een studie op validiteit en precisie en daarbij de volgende begrippen leren<br />
gebruiken: selectiebias, informatiebias, confounding bias, effectmodificatie, verification bias,<br />
regressie naar het gemiddelde<br />
* Berekenen van sensitiviteit en specificiteit op basis van onderzoeksgegevens en werken met de regel<br />
van Bayes<br />
* Onderzoeksdesign kunnen herkennen: follow-up onderzoek (retrospectief, prospectief); patientcontrole<br />
onderzoek; experimenteel onderzoek; non-expirimentele evaluatie van therapie; meta-analyse.<br />
ZAAL 0.3 COPENHAGEN<br />
Emeritus <strong>programma</strong> (parallel aan het algemene <strong>programma</strong>)<br />
Voorzitters: Prof. dr. G. Rosenbusch en J.F.M. Panhuysen<br />
11.20 - 12.00 Een bijzondere tentoonstelling in 1929: Invloed van de Russische kunst op de kinderboek<br />
illustratie in het westen vóór de 2e wereldoorlog<br />
Dr. A. Lemmens<br />
4<br />
k i j k o o k o p w w w . c o n g r e s s c o m p a n y . c o m<br />
o f w w w . r a d i o l o g e n . n l
16 E RADIOLOGENDAGEN 2011<br />
Tijdstip<br />
Onderwerp<br />
14.05 - 14.35 Opwekking van röntgenstraling m.b.v. het teruggevonden toestel van Hoffmans uit januari<br />
1896 te Maastricht<br />
Prof. dr. J. van Engelshoven en Dr. G. Kemerink<br />
14.35 - 15.15 De eerste Wereldoorlog in België, <strong>Radiologie</strong> in ‘Trench Coat’<br />
Dr. R. van Tiggelen<br />
16.00 - 16.35 “Koorts en Honger” ofwel geneeskunde op het platteland in de afgelopen eeuwen<br />
J.A.C. van den Broek<br />
16.35 - 17.15 De gang van J.S. Bach naar Nederland<br />
Prof. dr. M. Oudkerk, UMC Groningen, Groningen<br />
AUDITORIUM 2<br />
17.15 - 18.45 Uitreiking prestigieuze WSS penning aan Prof. dr. J.O. Barentsz met aansluitend de ALV NVvR<br />
& Juniorsectie<br />
EXPOFOYER<br />
18.15 Industrieborrel: exclusief aangeboden door<br />
Vrijdag 30 september 2011<br />
Tijdstip<br />
Onderwerp<br />
8.30 - 9.00 Ontvangst & registratie<br />
9.00 - 10.15 Refresher courses<br />
ZAAL 0.4 BRUSSELS<br />
Buiktrauma, waar gaat het nou eigenlijk om<br />
Voorzitter: L.F.M. Beenen, AMC, Amsterdam<br />
Classificaties van orgaanletsels, lever en milt<br />
L.F.M. Beenen, AMC, Amsterdam<br />
Classificaties van orgaanletsels, overige organen<br />
Mw. D.R. Kool, Jeroen Bosch Ziekenhuis, ‘s-Hertogenbosch<br />
Interventieradiologie bij buiktrauma<br />
Dr. O.M. van Delden, AMC, Amsterdam<br />
Leerdoelen:<br />
* Inzicht in wat wel en wat niet van belang is bij buiktrauma’s<br />
* Inzicht achter de ratio van de verschillende chirurgische en radiologische classificaties<br />
* Rol van de interventieradiologie in de behandeling van buiktrauma’s<br />
ZAAL 0.5 PARIS<br />
Acute pijn op de borst: Stand van zaken<br />
Voorzitter: Prof. dr. M. Oudkerk, UMC Groningen, Groningen<br />
Acute Chest Pain: The clinical perspective<br />
Dr. S.C.A.M. Bekkers, MUMC, Maastricht<br />
* To understand the challenges for the clinical assessment of pulmonary embolism, acute aortic<br />
pathologies and coronary artery disease<br />
* To define the in- and exclusion criteria for imaging in patients with acute chest pain<br />
Acute Chest Pain: The imaging perspective<br />
Prof. dr. J.E. Wildberger, MUMC, Maastricht<br />
* To summarize the technical prerequisites for advanced cross-sectional imaging<br />
* To define the role of CT and MR in the assessment of pulmonary embolism, acute aortic pathologies<br />
and coronary artery disease<br />
* To understand the potential clinical impact of imaging in the emergency setting, also in the<br />
perspective of logistics and cost-effectiveness<br />
Acute Chest Pain: Statement of the European Society of Cardiac Radiology<br />
Prof. dr. M. Oudkerk, UMC Groningen, Groningen<br />
* To summarize current clinical concepts and guidelines for acute chest pain<br />
* To learn about the specific role of different imaging modalities (CT, MR, Ultrasound, QCA) in this context<br />
Differentiated examination protocols even for the emergency setting have become technically feasible<br />
due to ongoing advances especially in non-invasive imaging techniques. The aim of this refresher<br />
course is to provide an overview on the rationale, the opportunities and current concepts for the<br />
work-up in patients with acute chest pain.<br />
ZAAL 0.8 ROME<br />
De knie: Niet standaard MRI bevindingen en de postoperatieve knie<br />
Voorzitter: Mw. Dr. M.P. Terra, AMC, Amsterdam<br />
De postoperatieve knie (MRI)<br />
Dr. P. Van Dyck, UZ Antwerpen, België<br />
De postoperatieve knie<br />
Mw. Dr. G.A. Meins, orthopedisch chirurg, ZGT, Almelo-Hengelo / clubarts FC Twente<br />
Niet standaard MRI bevindingen in en rond de knie<br />
Dr. P. Van Dyck, UZ Antwerpen, België<br />
ZAAL 0.9 ATHENS<br />
Opleiden anno 2011<br />
Voorzitter: Dr. H.J. Baarslag, Meander MC, Amersfoort<br />
AIOS als “active learner”<br />
Mw. Drs. J.A. Baane, AMC, Amsterdam<br />
1 6 E R A D I O L O G E N D A G E N - 2 9 e n 3 0 S E P T E M B E R 2 0 1 1 5
<strong>programma</strong> & <strong>abstracts</strong><br />
Tijdstip<br />
Onderwerp<br />
EXPOFOYER<br />
10.15 - 10.45 Koffiepauze<br />
Intervisie <strong>voor</strong> opleiders<br />
Prof. dr. O.R.C. Busch, chirurg, AMC, Amsterdam<br />
Optimalisatie radiologie bespreking<br />
Dr. M. Maas, AMC, Amsterdam & Drs. B.M. Wiarda, MCA, Alkmaar<br />
Leerdoelen:<br />
De HORA heeft veel veranderd en verbeterd in opleidingsland. Maar daarmee zijn we er nog niet. Met<br />
betrekking tot het opleiden anno 2011 is een nog actievere instelling mogelijk, die zowel de AIOS, de<br />
opleider als ook de gehele opleidingsstaf stimuleert. Alle 3 genoemde groepen komen zowel individueel<br />
als interactief aan bod bij deze refreshercourse onderwijs.<br />
ZAAL 2.1 COLORADO<br />
Veneuze interventies<br />
Voorzitters: Dr. K.P. van Lienden, AMC, Amsterdam & Mw. Dr. C.S.P. van Rijswijk, LUMC, Leiden<br />
Pelvic congestion syndroom<br />
Dr. J.H.B. Boomsma<br />
Behandeling veneuze trombose<br />
Dr. J.A. Vos, St. Antonius Ziekenhuis, Nieuwegein<br />
Rol van cava filters<br />
Prof. dr. J.A. Reekers, AMC, Amsterdam<br />
Veneuze toegang; PICCs, Dialyse catheters en andere CVCs<br />
Dr. H. van Overhagen, HagaZiekenhuis, Den Haag<br />
ZAAL 0.1 LONDON<br />
Workshop / hands-on: To make Radlex more familiar.<br />
Using IHE TCE for export of PACS data to an MIRC teaching file<br />
E. Sanders, Amphia Ziekenhuis, Breda<br />
P. van Ooijen, UMC Groningen, Groningen<br />
10.45 - 12.15 Parallelsessies vrije <strong>voor</strong>drachten<br />
Voorafgaand aan de wetenschappelijke <strong>voor</strong>drachten zal iedere sessie aanvangen met een keynote lecture.<br />
ZAAL 0.4 BRUSSELS<br />
Sessie 6: Abdominale radiologie 2<br />
Voorzitters: Prof. dr. A.A.M. Masclee, MUMC, Maastricht & Dr. R.E. van Gelder, AMC, Amsterdam<br />
Endoscopie vs CTC<br />
Prof. dr. A.A.M. Masclee, MUMC, Maastricht<br />
ZAAL 0.8 ROME<br />
Sessie 7: Kinderradiologie / Diversen<br />
Voorzitters: Dr. R.A.J. Nievelstein, UMC Utrecht, Utrecht & N. de Graaf, Erasmus MC, Rotterdam<br />
Huidige status en toekomstperspectief<br />
Dr. R.A.J. Nievelstein, UMC Utrecht, Utrecht<br />
ZAAL 0.5 PARIS<br />
Sessie 8: Mammadiagnostiek 2 & Uitreiking Jan Hendriksprijs<br />
Voorzitters: Drs. R.D.M. Mus, UMC St Radboud, Nijmegen & Mw. M.W. Imhof-Tas, UMC St Radboud, Nijmegen<br />
MRI van de mamma in 2 minuten?<br />
Drs. R.D.M. Mus, UMC St Radboud, Nijmegen<br />
ZAAL 2.1 COLORADO<br />
Sessie 9: Neuro-Hoofdhals radiologie<br />
Voorzitters: Dr. J.C. de Groot, UMC Groningen, Groningen & Dr. S.C.A. Steens, UMC St Radboud,<br />
Nijmegen<br />
Vasculaire evaluatie van het brein in stroomversnelling<br />
Dr. J.C. de Groot, UMC Groningen, Groningen<br />
ZAAL 0.9 ATHENS<br />
Sessie 10: MSK / Thorax / Diversen<br />
Voorzitters: Mw. Dr. M. Reijnierse, LUMC, Leiden & Dr. P.J.W. Wensing, ZGT Almelo/Hengelo<br />
Postop infection around metals: CT/Mri techniques<br />
Mw. Dr. M. Reijnierse, LUMC, Leiden<br />
AUDITORIUM 2<br />
De educatieve <strong>voor</strong>dracht<br />
Voorzitters: Dr. C.J. van Rooden, HagaZiekenhuis & Dr. R. Ouwendijk, Erasmus MC, Rotterdam<br />
In deze gloednieuwe sessie tijdens de Radiologendagen komt een groot scala aan klinisch georiënteerde<br />
onderwerpen <strong>voor</strong>bij, van echogeleide bijnierpunctie tot beeldvorming van atherosclerose. Voor het<br />
eerst konden dit jaar, naast wetenschappelijke, ook educatieve <strong>abstracts</strong> ingestuurd worden.<br />
De kwaliteit van de inzendingen was hoog, dus deze primeur belooft een erg interessante, gevarieerde<br />
en <strong>voor</strong>al ook leuke sessie te worden, <strong>voor</strong>gezeten door twee top-radiologen!<br />
Future clinical applications of high resolution anatomical imaging of the brain at 7.0 Tesla MRI<br />
A.G. van der Kolk, UMC Utrecht, Utrecht<br />
Is beeldvorming van atherosclerose klaar <strong>voor</strong> de dagelijkse praktijk?<br />
Mw. S. Gerretsen, MUMC, Maastricht<br />
Lung perfusion defects on dual-energy Computed Tomography (DECT): review of morphology<br />
and differential diagnosis<br />
Mw. Dr. A.E. Odink, Erasmus MC, Rotterdam<br />
Value of computed tomography coronary angiography in failed conventional coronary angiography<br />
A.S. Thijssen, Erasmus MC, Rotterdam<br />
Pseudotumoren bij metaal op metaal totale heup artroplastiek<br />
M.F. Boomsma, Isala klinieken, Zwolle<br />
6<br />
k i j k o o k o p w w w . c o n g r e s s c o m p a n y . c o m<br />
o f w w w . r a d i o l o g e n . n l
Tijdstip<br />
Onderwerp<br />
16 E RADIOLOGENDAGEN 2011<br />
EXPOFOYER<br />
12.15 - 13.15 Lunch<br />
EXPOFOYER<br />
12.30 - 13.00 Postersessie<br />
De vergrote bijnier: Endosonografische FNA van de linker-bijnier<br />
R. de Ridder, MDL-arts, MUMC, Maastricht<br />
Long-term follow-up features on rectal MRI during a wait-and-see approach after a clinical<br />
complete response in rectal cancer patients treated with chemoradiotherapy<br />
D.M.J. Lambregts, MUMC, Maastricht<br />
Implementatie van virtuele colonoscopie in de dagelijkse radiologische praktijk<br />
M.T. de Witte, VieCuri Medisch Centrum, Venlo / UMC St Radboud, Nijmegen<br />
Mw. Dr. P.C.G. Simons, VieCuri Medisch Centrum, Venlo<br />
ZAAL 0.2 BERLIN<br />
Workshop “Interpretatie van radiologisch wetenschappelijk onderzoek”<br />
Mw. Dr. S. Spronk, klinisch epidemioloog, Erasmus MC, Rotterdam<br />
Leerdoelen:<br />
* Het toepassen van risicomaten zoals incidentiecijfer en cumulatieve incidentie, en de effectmaten<br />
zoals relatief risico, (populatie-)attributief risico<br />
* Het beoordelen van een studie op validiteit en precisie en daarbij de volgende begrippen leren<br />
gebruiken: selectiebias, informatiebias, confounding bias, effectmodificatie, verification bias,<br />
regressie naar het gemiddelde<br />
* Berekenen van sensitiviteit en specificiteit op basis van onderzoeksgegevens en werken met de regel<br />
van Bayes<br />
* Onderzoeksdesign kunnen herkennen: follow-up onderzoek (retrospectief, prospectief); patient-controle<br />
onderzoek; experimenteel onderzoek; non-expirimentele evaluatie van therapie; meta-analyse.<br />
AUDITORIUM 2<br />
13.15 - 13.30 Wetenschappelijk beleid NvvR <strong>voor</strong> academische -en niet academische centra<br />
Mw. Prof. dr. R.G.H. Beets-Tan, MUMC, Maastricht<br />
AUDITORIUM 2<br />
Plenaire sessie<br />
13.30 - 14.30 Pro-con: Setting standards in healthcare - Which way to go?<br />
Ook <strong>voor</strong> de radiologie zullen kwaliteitsnormen steeds belangrijker worden. Wat vinden de debaters,<br />
maar ook: Wat vindt U! Drie onderwerpen zullen U raken. Drie pro-con koppels testen uw dekking.<br />
Fair play is de regel, maar neem uw bokshandschoenen mee.<br />
Voorzitter: Dr. J.A. Vos, St. Antonius Ziekenhuis, Nieuwegein<br />
De kwaliteitseisen <strong>voor</strong> de radiologie zijn autonoom op te stellen<br />
Pro: Dr. C. Holt, Isala klinieken, Zwolle<br />
Con: J.W.A.P. van Hoogstraten, Deventer Ziekenhuis, Deventer<br />
Hoog complex, (laag volume) diagnostiek moet alleen door experts worden uitgevoerd<br />
Pro: Prof. dr. J. Stoker, AMC, Amsterdam<br />
Con: Mw. L.F.I.J. Oudenhoven, ZGT Almelo, Almelo<br />
Information technology in radiology - Yes, it helps!<br />
Pro: Prof. D. Rubin, Stanford University, USA<br />
Con: R.H.M. Smithuis, Rijnland Ziekenhuis, Leiderdorp<br />
14.30 - 15.15 Richtlijnen sessie<br />
Voorzitter: Drs. B.M. Wiarda, Medisch Centrum Alkmaar, Alkmaar<br />
Licht traumatisch hoofd/hersenletsel<br />
Mw. D.R. Kool, Jeroen Bosch Ziekenhuis, ‘s-Hertogenbosch<br />
Distale Radius Fracturen<br />
Mw. S. Kolkman, AMC, Amsterdam<br />
Acuut lateraal enkelletsel en Interne indicatoren Acuut lateraal enkelbandletsel<br />
J.W.A.P. van Hoogstraten, Deventer Ziekenhuis, Deventer<br />
Oesofaguscarcinoom<br />
Prof. dr. E.J. van der Jagt, UMC Groningen, Groningen<br />
EXPOFOYER<br />
15.15 - 15.45 Theepauze<br />
AUDITORIUM 2<br />
15.45 - 16.25 Uitreiking Philipsprijs, gevolgd door bekendmaking en presentatie van achtereenvolgens de<br />
Posterprijs, Radiologendagen prijs, NVvR Travel Grant en Fellowshipdiploma’s<br />
AUDITORIUM 2<br />
16.25 - 17.15 Quiz<br />
Door de maatschap radiologie van het Albert Schweitzer ziekenhuis<br />
AUDITORIUM 2<br />
17.15 - 17.20 Afsluiting door <strong>voor</strong>zitter<br />
Dr. R.B.J. de Bondt, Isala klinieken, Zwolle<br />
Vanaf 20.00<br />
Diner & Galafeest<br />
Amrâth Grand Hotel De L’Empereur Maastricht<br />
1 6 E R A D I O L O G E N D A G E N - 2 9 e n 3 0 S E P T E M B E R 2 0 1 1 7
<strong>programma</strong> genomineerden & <strong>abstracts</strong><br />
Genomineerde <strong>abstracts</strong> <strong>voor</strong><br />
de Radiologendagenprijs 2011<br />
O1.7 ASSESSMENT OF A COMPLETE RESPONSE OF RECTAL CANCER TO<br />
PREOPERATIVE CHEMORADIATION THERAPY: A COMPARISON<br />
BETWEEN MR VOLUMETRY AND DIFFUSION-WEIGHTED MRI<br />
D.M.J. Lambregts 1 , L. Curvo-Semedo 2 , M. Maas 1 , T. Thywissen 1 , G. Lammering 1 , G.L. Beets 1 ,<br />
F. Caseiro-Alves 2 , R.G.H. Beets-Tan 1<br />
1<br />
Maastricht Universitair Medisch Centrum, Maastricht<br />
2<br />
Radiology University Clinic, Coimbra University Hospital, Coimbra, Portugal<br />
O4.3 LESION DETECTION AND BI-RADS CLASSIFICATION IN 3D-US AUTO-<br />
MATED BREAST VOLUME SCANS (ABVS): CORRELATION WITH BREAST MRI<br />
T.A. Fassaert, I.J.M. Dubelaar, M.D.F. de Jong, M.C.J.M. Rutten<br />
Jeroen Bosch Ziekenhuis, Den Bosch<br />
O5.8 1 JAAR NA EVAR BESTAAT NOG ONGEVEER EENDERDE DEEL VAn de<br />
ANEURYSMAZAK UIT ONGEORGANISEERDE THROMBUS BIJ PATIENTEN<br />
MET EN ZONDER AANTOONBAAR ENDOLEAK<br />
S.A.P. Cornelissen 1 , E.P.A. Vonken 1 , H.J. Verhagen 2 , F.L. Moll 1 , L.W. Bartels 3<br />
1<br />
Universitair Medisch Centrum Utrecht, Utrecht<br />
2<br />
Erasmus Medisch Centrum, Rotterdam<br />
3<br />
Image Sciences Institute, Universitair Medisch Centrum Utrecht, Utrecht<br />
O9.1 ARTERIAL CALCIFICATION IN RELATION TO COGNITION AND<br />
STRUCTURAL BRAIN CHANGES<br />
D. Bos, M.W. Vernooij, S.E. Elias-Smale, G.P. Krestin, A. Hofman, W.J. Niessen, J.C.M. Witteman,<br />
A. van der Lugt, M.A. Ikram<br />
Erasmus Medisch Centrum, Rotterdam<br />
O10.5 IMPACT ON DIAGNOSTIC PERFORMANCE AND READING TIME OF A<br />
COMPUTER AIDED DETECTION ALGORITHM FOR THE DETECTION OF<br />
ACUTE PE: SECOND READING VERSUS CONCURRENT READING<br />
R. Wittenberg 1 , J.F. Peters 2 , I.A.H. Van den Berk 3 , N.J.M. Freling 3 , R.J. Lely 4 , B. de Hoop 5 , K. Horsthuis 3 ,<br />
C.J. Ravesloot 5 , M. Prokop 6 , C.M. Schaefer-Prokop 7<br />
1<br />
Universitair Medisch Centrum Utrecht, Utrecht<br />
2<br />
Philips Healthcare, Best<br />
3<br />
Academisch Medisch Centrum, Amsterdam<br />
4<br />
VU Medisch Centrum, Amsterdam<br />
5<br />
Universitair Medisch Centrum Utrecht, Utrecht<br />
6<br />
Universitair Medisch Centrum St Radboud, Nijmegen<br />
7<br />
Meander Medisch Centrum, Amersfoort<br />
8<br />
k i j k o o k o p w w w . c o n g r e s s c o m p a n y . c o m<br />
o f w w w . r a d i o l o g e n . n l
16 E RADIOLOGENDAGEN 2011<br />
Genomineerde <strong>abstracts</strong> <strong>voor</strong><br />
de NVvR Travel Grant 2011<br />
O2.3 MRI FEATURES ASSOCIATED WITH ACUTE APPENDICITIS<br />
M.M.N. Leeuwenburgh 1 , B.M. Wiarda 2 , A. Spilt 3 , P.M.M. Bossuyt 1 , M.A. Boermeester 1 ,<br />
J. Stoker 1 , OPTIMAP Studiegroep<br />
1<br />
Academisch Medisch Centrum, Amsterdam<br />
2<br />
Medisch Centrum Alkmaar, Alkmaar<br />
3<br />
Kennemer Gasthuis, Haarlem<br />
O2.4 OPTIMAL STRATEGY IN PATIENTS WITH SUSPECTED ACUTE APPENDICITIS,<br />
CAN MRI REPLACE CT?<br />
M.M.N. Leeuwenburgh 1 , H.W. van Es 2 , J.W.C. Gratama 3 , P.M.M. Bossuyt 1 , M.A. Boermeester 1 ,<br />
J. Stoker 1 , OPTIMAP Studiegroep<br />
1<br />
Academisch Medisch Centrum, Amsterdam<br />
2<br />
St. Antonius Ziekenhuis, Nieuwegein<br />
3<br />
Gelre ziekenhuizen, Apeldoorn<br />
O2.7 MR EVALUATION OF URETHRAL DIVERTICULA AND DIFFERENTIAL<br />
DIAGNOSIS IN SYMPTOMATIC FEMALE PATIENTS<br />
S.I. Verschuuren, R.S. Dwarkasing, W. Dinkelaar, W.C.J. Hop, G.R. Dohle, G.P. Krestin<br />
Erasmus Medisch Centrum, Rotterdam<br />
O5.7 CAROTID ATHEROSCLEROTIC PLAQUE PROGRESSION AND CHANGE<br />
IN PLAQUE COMPOSITION OVER TIME; A PROSPECTIVE IN VIVO SERIAL CT<br />
ANGIOGRAPHY STUDY<br />
M.J. van Gils, D. Vukadinovic, D.W.J. Dippel, W.J. Niessen, A. van der Lugt<br />
Erasmus Medisch Centrum, Rotterdam<br />
O6.4 PERCEIVED BURDEN OF SCREENING BY COLONOSCOPY OR<br />
CT-COLONOGRAPHY IN THE DETECTION OF ADVANCED NEOPLASIA:<br />
A RANDOMIZED CONTROLLED TRIAL<br />
M.C. de Haan 1 , T.R. de Wijkerslooth 1 , E. Stoop 2 , P.M. Bossuyt 1 , M. Thomeer 2 ,<br />
M.L. Essink-Bot 1 , M.E. van Leerdam 2 , P. Fockens 1 , E.J. Kuipers 2 , E. Dekker 1 , J. Stoker 1<br />
1<br />
Academisch Medisch Centrum, Amsterdam<br />
2<br />
Erasmus Medisch Centrum, Rotterdam<br />
O7.2 MINIMALLY INVASIVE MRI BY OMITTING INTRAVENOUS CONTRAST<br />
INJECTION; DOES IT CHANGE THE RADIOLOGIC ASSESSMENT OF KNEE<br />
JOINT PATHOLOGIES IN JIA?<br />
R. Hemke, M.A.J. van Rossum, M. van Veenendaal, T.W. Kuijpers, M. Maas<br />
Academisch Medisch Centrum, Amsterdam<br />
1 6 E R A D I O L O G E N D A G E N - 2 9 e n 3 0 S E P T E M B E R 2 0 1 1 9
<strong>programma</strong> genomineerden & <strong>abstracts</strong><br />
Vervolg<br />
O7.3 ULTRASOUND TO PREDICT SIGNIFICANT HEPATIC STEATOSIS IN OBESE<br />
ADOLESCENTS: POOR POST-TEST PROBABILITY DESPITE ACCEPTABLE<br />
SENSITIVITY AND SPECIFICITY<br />
A.E. Bohte 1 , B.G. Koot 1 , A.J. Nederveen 1 , O.H. van der Baan-Slootweg 2 , S. Bipat 1 , T.H. Pels Rijcken 3 ,<br />
P.L.M. Jansen 1 , M.A. Benninga 1 , J. Stoker 1<br />
1<br />
Academisch Medisch Centrum, Amsterdam<br />
2<br />
Heideheuvel Kliniek, Hilversum<br />
3<br />
Tergooiziekenhuizen, Hilversum<br />
O9.1 ARTERIAL CALCIFICATION IN RELATION TO COGNITION AND STRUCTURAL<br />
BRAIN CHANGES<br />
D. Bos, M.W. Vernooij, S.E. Elias-Smale, G.P. Krestin, A. Hofman, W.J. Niessen,<br />
J.C.M. Witteman, A. van der Lugt, M.A. Ikram<br />
Erasmus Medisch Centrum, Rotterdam<br />
O9.2 TIA AND STROKE PATIENTS WITH CAROTID STENOSIS: PRESENCE<br />
OF COMPLICATED PLAQUE FEATURES AT MRI IS ASSOCIATED WITH<br />
RECURRENT EVENTS<br />
R.M. Kwee 1 , R.J. van Oostenbrugge 1 , W.H. Mess 1 , M.H. Prins 1 , R.J. van der Geest 2 , J.W.M. ter Berg 3 ,<br />
C.L. Franke 4 , A.G.G.C. Korten 5 , B.J. Meems 6 , J.M.A. van Engelshoven 1 , J.E. Wildberger 1 , M.E. Kooi 1<br />
1<br />
Maastricht Universitair Medisch Centrum, Maastricht<br />
2<br />
Leids Universitair Medisch Centrum, Leiden<br />
3<br />
Orbis Medisch Centrum, Sittard<br />
4<br />
Atrium Medisch Centrum Parkstad, Heerlen<br />
5<br />
Laurentius Ziekenhuis, Roermond<br />
6<br />
VieCuri Medisch Centrum, Venlo<br />
O10.6 DEVELOPMENT AND VALIDATION OF A DIAGNOSTIC MODEL FOR<br />
AIRFLOW LIMITATION IN HEAVY SMOKERS BY USING QUANTITATIVE<br />
COMPUTED TOMOGRAPHY<br />
O.M. Mets 1 , C.M.F. Buckens 1 , P. Zanen 1 , I. Isgum 1 , M. Prokop 2 , P.A. de Jong 1<br />
1<br />
Universitair Medisch Centrum Utrecht, Utrecht<br />
2<br />
Universitair Medisch Centrum St Radboud, Nijmegen<br />
P02<br />
AUTOMATED BREAST VOLUME SCANNER: 3D-ULTRASOUND<br />
OF BREAST LESIONS<br />
T.A. Fassaert, M.D.F. de Jong, I.J.M. Dubelaar, M.C.J.M. Rutten<br />
Jeroen Bosch Ziekenhuis, ‘s-Hertogenbosch<br />
10<br />
k i j k o o k o p w w w . c o n g r e s s c o m p a n y . c o m<br />
o f w w w . r a d i o l o g e n . n l
Auteursindex<br />
16 E RADIOLOGENDAGEN 2011<br />
AUTEUR<br />
abstract<br />
Aalten, S.M. van O6.7<br />
Adam, J. O1.8<br />
Adams, A. O8.7<br />
Adriaanse, S.M. O9.6<br />
Akkerman, E.M. O1.8<br />
Amstel, J.D. van O8.10<br />
Aquarius, R. O5.2<br />
Baan-Slootweg, O.H. van der O7.3<br />
Backes, W.H. O1.3<br />
Backx, F.J.G. O3.7<br />
Bakers, F.C.H. E02, O1.3<br />
Bakker, C.J. O5.4<br />
Ballegooijen, M. van O6.3<br />
Barkhof, F.A. O9.5, O9.6<br />
Bartels, L.W. O3.2, O5.8<br />
Bechan, M.A.H.<br />
P03<br />
Beek, F.J.A. O1.8, O7.4<br />
Beek, H. van O10.8<br />
Beenen, L.F.M. O2.5<br />
Beerman, H. O10.8<br />
Beets, G.L. E02, O1.1, O1.2, O1.3,<br />
O1.6, O1.7, P14<br />
Beets-Tan, R.G.H. E02, O1.1, O1.2,<br />
O1.3, O1.6, O1.7, O2.2,<br />
O4.1, O6.8, P14<br />
Benedictus, M.R. O9.5<br />
Benninga, M.A. O7.3<br />
Bentohami, A. O7.5<br />
Berckel, B.N.M. van O9.6<br />
Berg, A.S. van den O5.1<br />
Berg, R. van den O9.5, P09, P12, P13<br />
Berk, I.A.H. van den O10.5<br />
Berkhof, M. O1.1<br />
Bernsen, M.R. O7.7, O7.8<br />
Beumer, D. O9.5<br />
Beute, G.N. O9.8<br />
Bierings, M.B. O1.8<br />
Biermann, K. O6.3<br />
Biessels, G.J. O3.8<br />
Bijlsma, T.S. O7.5<br />
Binnewijzend, M.A.A. O9.6<br />
Bipat, S. O2.1, O5.3, O5.5, O6.1,<br />
O6.5, O7.1, O7.3<br />
Bisschops, R.H.C. O8.6<br />
Bluekens, A.M.J. O8.4<br />
Boelens, J.J. O7.4<br />
Boellaard, T.N. O6.2, O6.5<br />
Boer, E. de O6.6<br />
Boer, R. de O9.4<br />
Boermeester, M.A. O2.3, O2.4<br />
Boersma, E.H. O3.1<br />
Boetes, C. † O4.1<br />
Bohté, A.E. O7.3<br />
Boiten, J. O5.6, O9.5<br />
Bokkers, R.P.H.<br />
P05, P06<br />
Bonenkamp, J.<br />
P04<br />
Booij, R.<br />
E06<br />
Boomsma, M.F.<br />
E08<br />
Borst, G.J. de<br />
P05<br />
Bos, D. O9.1<br />
Bosch, M.A.A.J. van den O4.4,<br />
O5.4, O8.5, O8.10<br />
Bosker, B.H.<br />
E08<br />
Bosker, R.J.I. O1.4<br />
Bosscha, K.<br />
P10<br />
Bossuyt, P.M.M. O2.3, O2.4, O6.1,<br />
O6.2, O6.3, O6.4<br />
Bot, J. O9.5<br />
Bouwhuijsen, Q.J.A. van den O9.3<br />
Breest Smallenburg, V. van O4.3<br />
Brink, R.B.A. van den O3.6<br />
Broeder, A.A. den O10.4<br />
Broeders, M.J.M. O8.4<br />
Bron, E. O10.1<br />
Bruijnes, V. O4.5<br />
Brundel, M. O3.8<br />
Buckens, C.M.F. O10.6<br />
Budde, R.P.J. O3.2, O3.4, O3.5, O3.6<br />
Buijsen, J. O1.2<br />
Caan, M.W.A. O2.1, O7.1<br />
Cappendijk, V.C. E01, E02, E05,<br />
O1.3, O2.2<br />
Carli, D.F.M. O9.8<br />
Caseiro-Alves, F. O1.7<br />
Chamuleau, S.A.J. O3.6<br />
Cleutjens, J. O4.1<br />
Cornelissen, S.A.P. O5.8<br />
Cramer, M.J.M. O3.7<br />
Cremers, P.T.J. O1.5<br />
Cremers, S.E.H. O1.5<br />
Curvo-Semedo, L. O1.7<br />
Dalen, T. van O4.4<br />
Damoiseaux, J.S. O9.6<br />
Das, M.<br />
E05<br />
Dekker, E. O6.3, O6.4<br />
Dekker, H.M. O2.6<br />
Dharampal, A.S. O3.1, O3.3<br />
Diepstraten, S.C.E. O4.4<br />
Diest, P.J. van O4.4, O8.10<br />
Dijk, R.A.J.M. van O1.4, O4.6, O8.3<br />
Dijkman, B.A. van O7.5<br />
Dinkelaar, W. O2.7<br />
Dippel, D.W.J. O5.7, O9.5, P08<br />
Doeswijk, G. O7.7, O7.8<br />
Dohle, G.R. O2.7<br />
Doorn, M.M.A.C. van O2.5, O9.5<br />
Douwes, D.C.E. O2.2<br />
Dubelaar, I.J.M. O4.2, O8.1, P02<br />
P04, P07<br />
Duijm, L.E.M. O4.3, O8.2, 08.9<br />
Duvivier, K.M. O4.4<br />
Dwarkasing, R.S. O2.7, O6.1, O6.7<br />
Eddes, E.H. O1.4<br />
Eeftinck Schattenkerk, M. O1.4<br />
Elias, S.G. O8.7<br />
Elias-Smale, S.E. O9.1<br />
Elschot, M. O5.4<br />
Engelen, S.M.E. O1.2<br />
Engelshoven, J.M.A. van E05, O9.2<br />
Ernst, M.<br />
P10<br />
Es, H.W. van O2.4<br />
Essink-Bot, M.L. O6.4<br />
Ettema, H.B.<br />
E08<br />
Fassaert, T.A. O4.2, O8.1, P02<br />
Fernandez-Gallardo, M.A. O4.4<br />
Feyter, P.J. de O3.1, O3.3<br />
Fijnheer, R. O1.8<br />
Flier, W.M. van der O9.5, O9.6<br />
Flucke, U.<br />
P04<br />
Fockens, P. O6.3, O6.4<br />
Folbert, E.C. O10.3<br />
Franke, C.L. O9.2<br />
Frans, F.A. O5.3, O5.5<br />
Fransen, P.S. O9.5<br />
Freling, N.J.M. O10.5<br />
Frotscher, C. O4.1<br />
Geelen, L.M.H. O9.7<br />
Geerdes, M. O5.2<br />
Geest, R.J. van der O9.2<br />
Gerretsen, S.C.<br />
E05<br />
Gilhuijs, K.G.A. O4.5<br />
Gillissen, F. O1.2<br />
Gils, M.J. van<br />
O5.7, P08<br />
Gorp, T. van O6.8<br />
Goslings, J.C. O7.5<br />
Gratama, J.W.C. O2.4<br />
Gryspeerdt, S. O1.5<br />
Guenoun, J. O7.7, O7.8<br />
1 6 E R A D I O L O G E N D A G E N - 2 9 e n 3 0 S E P T E M B E R 2 0 1 1 11
<strong>programma</strong> index & <strong>abstracts</strong><br />
Haan, M.C. de O6.1, O6.3, O6.4<br />
Habets, J. O3.4, O3.5, O3.6<br />
Hartkamp, N.S.<br />
P05, P06<br />
Hartmann, I.J.C. E06, O10.7<br />
Hauptmann, M. O7.6<br />
Havinga, M.E. O5.2<br />
Heer, L.M. de O3.2<br />
Heeten, G.J. den O8.4<br />
Hegeman, J.H. O10.3<br />
Heijde, D.M.F.M. van der O10.4,<br />
P12, P13<br />
Helle, M.<br />
P06<br />
Hellemondt, F.J. van O3.7<br />
Hemke, R. O7.2<br />
Hendrikse, J.<br />
E04, O3.8,<br />
P05, P06<br />
Hendriks-Roelofs, F. O10.4<br />
Hensen, J.J. O8.8, O10.8<br />
Herk, M. van O7.6<br />
Herwerden, L.A. van O3.2<br />
Hobbelink, M. O8.10<br />
Hoeberigs, M.C. O9.7<br />
Hofman, A. O9.1<br />
Hofman, P.A.M. O9.7<br />
Holland, R. O8.4<br />
Homburg, P.J.<br />
P08<br />
Hoop, B. de O10.5<br />
Hop, W.C.J. O2.7<br />
Horsthuis, K. O10.5<br />
Houterman, S. O1.5<br />
Huizinga, T.W.J.<br />
P12, P13<br />
Hummel, T.Z. O7.1<br />
IJzermans, J.N.M. O6.7<br />
Ikram, M.A. O9.1, O9.3, O9.4<br />
Imholz, A.L.T. O4.6, O8.3<br />
Isgum, I. O10.6<br />
Jager, G.J.<br />
O8.1, P10<br />
Jansen, F.H. O4.3, 08.9<br />
Jansen, P.L.M. O7.3<br />
Jansen, R.J. O6.1<br />
Jasperse, B. O9.4<br />
Jens, S. O5.5<br />
Jeukens, C.R.L.P.N O1.6<br />
Jong, H.W. de O5.4<br />
Jong, M.D.F. de O4.3, O8.1,<br />
P02, P10<br />
Jong, P.A. de O7.4, O10.6<br />
Kallen, B.F.W. van der O5.6, O9.5<br />
Karssemeijer, N. O8.4<br />
Kate, F.J.W. ten O6.6<br />
Kauffman, D. O6.1<br />
Kersten, M.J. O1.8<br />
Kessel, C.S. van O6.6<br />
Keymeulen, K. O4.1<br />
Kindermann, A. O7.1<br />
Klein, S. O10.1<br />
Klein, W.M.<br />
P01<br />
Klerk, J.M.H. de O1.8<br />
Klieverik, S.J.<br />
P14<br />
Klomp, D.W. O8.5<br />
Kluin, J. O3.2<br />
Kluza, E.<br />
O1.6, P14<br />
Koek, M. O9.4<br />
Koelemay, M.J.W. O5.3, O5.5<br />
Kolk, A.G. van der E04, O3.8<br />
Kollen, B.J.<br />
E08<br />
Koning, G.A. O7.7, O7.8<br />
Kooi, M.E. E05, O9.2<br />
Koot, B.G. O7.3<br />
Korten, A.G.G.C. O9.2<br />
Korteweg, M.A. O8.5, O8.10<br />
Koster, K. O1.4<br />
Kotek, G. O10.1<br />
Kraai, M. O10.3<br />
Kraal, K.J. O8.8<br />
Kreb, D.<br />
P10<br />
Krestin, G.P. E07, O2.7, O3.1, O3.3<br />
O7.7, O7.8, O9.1, O9.3<br />
O10.1, O10.2<br />
Kruitwagen, R. O6.8<br />
Kruse, A. O6.8<br />
Kuijer, J.P.A. O9.5<br />
Kuijpers, T.W. O7.2<br />
Kuipers, E.J. O6.3, O6.4<br />
Kwee, R.M. E05, O9.2<br />
Kwee, T.C. O1.8<br />
Lahaye, J. O1.2, O4.1<br />
Lalisang, R. O6.8<br />
Lalji, U.C. O2.8<br />
Lam, M.G.E.H. O5.4<br />
Lambregts, D.<br />
E02, O1.1,<br />
O1.2, O1.3, O1.6,<br />
O1.7, O6.8, P14<br />
Laméris, J.S. O7.6<br />
Lammering, G. E02, O1.7<br />
Lavini, C. O2.1, O7.1<br />
Ledeboer, M. O1.4<br />
Leerdam, M.E. van O6.3, O6.4<br />
Leeuwen, M.S. van O1.8, O6.6<br />
Leeuwenburgh, M.M.N. O2.3, O2.4<br />
Lefere, P. O1.5<br />
Legemate, D.A. O5.3<br />
Leij, C. van der O6.1<br />
Leiner, T. E05, O3.4<br />
Lely, R.J. O10.5<br />
Liedenbaum, M.H. O6.1<br />
Lijn, F. van der O9.4<br />
Lijster, M.S. de O6.1<br />
Lima Passos, V. O4.1<br />
Linden, H. van der<br />
P10<br />
Linden, E. van der O5.6<br />
Lobbes, M.B.I. E05, O4.1<br />
Loeffen, D.V. O2.2<br />
Loo, C. O4.5<br />
Looij, B.G.<br />
P10<br />
Ludwig, I. O1.8<br />
Lugt, A. van der O5.7, O9.1, O9.3,<br />
O9.4, O9.5, P08<br />
Luijkx, T. O3.7<br />
Luijten, P.R. E04, O3.8, O8.5<br />
Lute, C.C. O6.1<br />
Lutgens, L. O6.8<br />
Lycklama à Nijeholt, G.J. O5.6, O9.5<br />
Maas, M.<br />
E02, O1.1, O1.2,<br />
O1.3, O1.6, O1.7, P14<br />
Maas, M. E08, O7.2, O7.5<br />
Maat, G.H. van de O5.4<br />
Majoie, C.B.L.M. O9.5, P09<br />
Mali, W.P.Th.M. O3.2, O3.4, O3.6,<br />
O3.7, O4.4,<br />
O8.5, O8.7, O8.10<br />
Man, R.A. de O6.7<br />
Marcelis, C.<br />
P01<br />
Meems, B.J. O9.2<br />
Meijer, F.A.<br />
P07<br />
Mendez, C.P.<br />
P03<br />
Mess, W.H. O9.2<br />
Met, R. O5.3<br />
Mets, O.M. O10.6<br />
Mol, B.A.J.M. de O3.4, O3.5<br />
Moll, F.L. O5.8<br />
Mollet, N.R.A. E07, O3.1, O3.3<br />
Mongula, J.E. O6.8<br />
Mourik, J.E.M. O8.7<br />
Nederend, J. O8.9<br />
Nederkoorn, P.J. O9.5<br />
Nederveen, A.J. O2.1, O6.5, O7.1, O7.3<br />
Neefjes, L. O3.1, O3.3<br />
Nieman, K. O3.1, O3.3<br />
Niessen, W.J. O5.7, O9.1, O9.3, O9.4<br />
Nievelstein, R.A.J. O1.8, O7.6<br />
Niezen, R.A. O8.8, O10.8<br />
Nijman, J. O8.8<br />
12<br />
k i j k o o k o p w w w . c o n g r e s s c o m p a n y . c o m<br />
o f w w w . r a d i o l o g e n . n l
16 E RADIOLOGENDAGEN 2011<br />
Nijsen, J.F.W. O5.4<br />
Nio, C.Y. O6.2, O6.3<br />
Nunspeet, L. van O1.4<br />
Odink, A.E. E06, O10.7<br />
Odink, H. O5.1<br />
Oei, E.H.G. O10.1, O10.2<br />
Oostenbrugge, R.J. van O9.2, O9.5<br />
Osch, M.J.P. van<br />
P06<br />
Paardt, M.P. van der O6.1, O6.5<br />
Pels Rijcken, T.H. O7.3<br />
Pengel, K. O4.5<br />
Pennings, J.P. O8.6<br />
Peters, J.F. O10.5<br />
Plas, G.J.J.<br />
P08<br />
Ponsioen, C.Y. O2.1<br />
Prakken, N.H.J. O3.7<br />
Prehn, J. van O3.2<br />
Prins, M.H. O9.2<br />
Prokop, M. O3.5, O10.5, O10.6, P04<br />
Quarles van Ufford, H.M.E. O1.8<br />
Ravesloot, C.J. O10.5<br />
Reekers, J.A. O5.3, O5.5<br />
Reijnierse, M. O10.4, P12, P13<br />
Riedl, R.G. O1.3<br />
Ridder, R. de<br />
E01<br />
Ronckers, C.M. O7.6<br />
Rooij, W.J.J. van O9.8<br />
Roos, Y.B. O9.5<br />
Rooy, J.W.J. de<br />
P04<br />
Rooy, T.D. de O5.6<br />
Rossi, A. O3.1, O3.3<br />
Rossius, M. E06, O10.7<br />
Rossum, M.A.J. van O7.2<br />
Rozendaal, R. O8.6<br />
Ruggiero, A.R. O7.8<br />
Rutten, I.J.G. O1.3<br />
Rutten, M.J.C.M. O4.2, O8.1<br />
P02, P10<br />
Sandt-Koenderman, W.M.E. van de<br />
P03<br />
Sanz-Arigita, E. O9.6<br />
Schaefer-Prokop, C.M. E06, O10.5,<br />
O10.7<br />
Scheltens, P. O9.5, O9.6<br />
Schep, N.W.L O7.5<br />
Schepers-Bok, R. O5.2<br />
Schip, A.D. van het O5.4<br />
Schoonheim, M.M. O9.6<br />
Seevinck, P.R. O5.4<br />
Senden, P.J. O3.7<br />
Setz-Pels, W. O4.3, O8.2<br />
Siebelt, M. O10.2<br />
Sijbrandij, L.<br />
E08<br />
Sikkenk, A.C. O8.8<br />
Simons, P.C.G.<br />
E03<br />
Slaar, A. O7.5<br />
Slangen, B.F. O6.8<br />
Slooter, G. O1.5<br />
Sluzewski, M.S. O9.8<br />
Smets, A.M. O7.1, O7.6<br />
Smit, H. O10.1<br />
Smit, R.S. O10.3<br />
Smits, M.<br />
O9.4, P03<br />
Smits, M.L.J. O5.4<br />
Spijkerboer, A.M. O2.1, O3.6<br />
Spilt, A. O2.3<br />
Sprengers, M.E. O9.5<br />
Stehouwer, B.L. O8.5, O8.10<br />
Stoker, J. O1.8, O2.1, O2.3, O2.4<br />
O6.1, O6.2, O6.3, O6.4<br />
O6.5, O7.1, O7.3<br />
Stokkers, P. O2.1<br />
Stoop, E. O6.3, O6.4<br />
Storm, R. O8.6<br />
Straten, M. van O10.2<br />
Symersky, P. O3.4, O3.5<br />
Tanghe, H.L.J.<br />
P08<br />
Ter Berg, J.W.M. O9.2<br />
Terkivatan, T. O6.7<br />
Thijssen, A.S.<br />
E07<br />
Thomeer, M.G.J. O6.1, O6.3,<br />
O6.4, O6.7<br />
Thywissen, T. O1.7<br />
Tiel, J. van O10.1, O10.2<br />
Tilborg, G.F.A.J.B. van<br />
E07<br />
Tolboom, N. O9.6<br />
Tran, V.H.P. O8.3<br />
Uijlings, R. O3.6<br />
Uiterwaal, C.S.P. O1.8<br />
Vandenbussche, F.<br />
P01<br />
Veenendaal, M. van O7.2<br />
Velde, D. van der O10.3<br />
Veldhuis, W.B. O8.5, O8.10<br />
Velthuis, B.K. O3.7<br />
Vente, M.A.D. O5.4<br />
Verhagen, H.J. O5.8<br />
Verheij, J. O6.7<br />
Verhulst, M.L. O1.5<br />
Verkooijen, H.M. O4.4<br />
Vermeule, W. O10.7<br />
Vermoolen, M.A. O1.8<br />
Vernooij, M.W. O9.1, O9.3, O9.4<br />
Verreyen, C.C.C.M.<br />
E08<br />
Verschuuren, S.I. O2.7<br />
Versluys, A.B. O7.4<br />
Vijver, M.J. van de O6.3<br />
Vincken, K.L. O3.2<br />
Visch-Brink, E.G.<br />
P03<br />
Visser, R.N. de<br />
E07<br />
Visser, F. E04, O3.8<br />
Visser, P.J. O9.5<br />
Vliegen, R. O6.8<br />
Vlies, M. van der<br />
P09<br />
Volmerink, M.H.M. O4.6, O8.3<br />
Vonken, E.P.A. O5.8<br />
Voogd, A.C. O8.2<br />
Voort, M. van der O8.7<br />
Vossen, M.H.E. O10.4, P12, P13<br />
Vroegindeweij, D. O8.8, O10.8<br />
Vrooman, H.A. O9.4<br />
Vukadinovic, D. O5.7<br />
Waarsing, J.H. O10.2<br />
Walenkamp, M.W. O7.5<br />
Wattjes, M.P. O9.5<br />
Weerink, L.B.M. O10.3<br />
Weinans, H. O10.1, O10.2<br />
Wensing, P.J.W. dr. O5.2<br />
Weustink, A.C. E07, O3.1, O3.3<br />
Wiarda, B.M. O2.3<br />
Wielopolski, P.A. O7.7<br />
Wiersma, H.W. O1.4<br />
Wijkerslooth, T.R. de O6.3, O6.4<br />
Wildberger, J.E. E05, O4.1, O9.2<br />
Wilde, J.C.H. O7.5<br />
Wink, A.M. O9.6<br />
Winkens, B. O5.1<br />
Witkamp, A.J. O4.4, O8.10<br />
Witte, M.T. de<br />
E03<br />
Witteman, J.C.M. O9.1, O9.3<br />
Wittenberg, R. O10.5<br />
Worp, H.B. van der<br />
P05<br />
Ypma, Y.F.R. O10.8<br />
Zagers, M.B. O5.5<br />
Zanen, P. O10.6<br />
Ziech, M.L.W. O2.1, O7.1<br />
Zijlstra, I.J.A. O6.1<br />
Zijta, F.M. O6.5<br />
Zonnenberg, B.A. O5.4<br />
Zsiros, J. O1.8<br />
Zwam, W. van O9.5<br />
Zwanenburg, J.J.M. E04, O3.8<br />
1 6 E R A D I O L O G E N D A G E N - 2 9 e n 3 0 S E P T E M B E R 2 0 1 1 13
RC<strong>programma</strong> <strong>abstracts</strong><br />
& <strong>abstracts</strong><br />
Samenvattingen<br />
‘Research Corner’<br />
Donderdag 29 september, 14.05 - 15.35 uur<br />
LUMC<br />
TOEPASSINGEN VAN ULTRAHOOGVELD<br />
MRI BIJ PATIENTENPOPULATIES<br />
M.A. van Buchem<br />
Enkele jaren geleden zijn MRI-systemen ontwikkeld met een<br />
zeer hoge veldsterkte die geschikt zijn <strong>voor</strong> onderzoek bij<br />
mensen. Recent zijn twee van zulke systemen, functionerend<br />
bij een veldsterkte van het magnetisch veld van 7Tesla, in<br />
Nederland geplaatst, respectievelijk in het LUMC en het<br />
UMCU. Inmiddels zijn een groot aantal patiënten op deze<br />
systemen onderzocht. In deze presentatie zal een indruk<br />
geschetst worden van de eerste ervaringen die daarbij<br />
opgedaan zijn.<br />
Erasmus MC<br />
POPULATION IMAGING<br />
A. van der Lugt, M. Vernooij, M. Smits, W. Niessen,<br />
G.P. Krestin<br />
Introductie: Beeldvormende technieken worden in toenemende<br />
mate gebruikt in epidemiologische studies.<br />
Het gaat hier niet meer alleen om de relatief goedkopere<br />
technieken zoals conventionele Röntgenonderzoeken of<br />
echografie, maar ook om state-of-the-art CT en MRI. In<br />
grote populatiestudies met langdurige follow-up wordt<br />
onderzoek gedaan naar 1) determinanten van ziekten,<br />
gericht op 1a) inzicht in de pathofysiologie van ziekte en 1b)<br />
de mogelijkheid tot preventie door middel van interventie;<br />
2) vroegtijdige detectie van ziekte; 3) vaststellen van hoog<br />
risico groepen.<br />
Gezien het jarenlange subklinische beloop van ziekten<br />
zoals aderverkalking en neurodegeneratieve afwijkingen<br />
(dementie) waarvan de afwijkingen (mogelijk) al vroeg in<br />
het ziekte proces zichtbaar te maken zijn, kan beeldvorming<br />
een belangrijke rol spelen in deze onderzoeks<strong>programma</strong>’s.<br />
Beeldvorming en met name seriële beeldvorming kan surrogaat<br />
eindpunten leveren <strong>voor</strong> ziekte waardoor het onderzoek<br />
naar determinanten kan verbeteren en meer inzicht<br />
kan worden verkregen in de pathofysiologie van ziekte.<br />
Beeldvorming kan bijdrage aan vroege detectie van ziekte<br />
waardoor een tijdige interventie ook binnen handbereik<br />
komt.<br />
Project: De afdeling <strong>Radiologie</strong> van het Erasmus MC<br />
is partner in twee grote lopende populatie studies: de<br />
Rotterdam Studie en Generation R. In beide studies wordt<br />
(seriële) MRI verricht bij alle deelnemers in de studie<br />
(>1000). Het onderzoek richt zich op hersenen, bloedvaten,<br />
hart en skelet. In de presentatie wordt aangegeven wat<br />
de meerwaarde is van de radiologische bijdrage in het<br />
beantwoorden van de studie vraagstellingen. Tevens wordt<br />
ingegaan op de specifieke radiologische problemen zoals<br />
kwaliteitscontrole, dataopslag, data analyse en toevalsbevindingen.<br />
Bijzonder: Beeldvorming in populatie studies heeft een<br />
andere oogpunt dan de klinische radiologie waarbij men<br />
gericht is op het oplossen van een specifiek klinisch probleem<br />
en de radioloog met een differentiaal diagnose een<br />
bijdrage levert aan de zorg van de individuele patiënt. In<br />
populaties studies gaat het om grote aantallen deelnemers<br />
waarbij <strong>voor</strong>namelijk wordt gekeken naar “normale afwijkingen”<br />
die geleidelijk optreden bij veroudering en waarbij<br />
afwijking van de norm relevant is. Grote datasets zijn<br />
nodig <strong>voor</strong> het vaststellen van determinanten (waaronder<br />
genetische variaties) en het <strong>voor</strong>spellen van ziekte. (Semi)-<br />
automatische kwantitatieve evaluatie van afwijkingen is<br />
noodzakelijk gezien de omvang van de datasets en de subtiliteit<br />
van de afwijkingen.<br />
Perspectief: Door de inbreng van de radiologie worden de<br />
nieuwste technieken direct toegepast in wetenschappelijk<br />
onderzoek. Andersom kan de klinische radiologie leren van<br />
de manier waarop consistente data acquisitie plaats vindt,<br />
wat het belang is van standaardisatie en kwantificatie<br />
van data. Ontwikkelde kwantificatiesoftware kan gebruikt<br />
worden in de kliniek. Tot slot verschaffen deze studies normaal<br />
waarden waartegen klinische pathologie kan worden<br />
uitgezet.<br />
14<br />
k i j k o o k o p w w w . c o n g r e s s c o m p a n y . c o m<br />
o f w w w . r a d i o l o g e n . n l
RC<br />
research naam corner sessie 1<br />
UMC Groningen<br />
SCREENING FOR CORONARY ARTERY<br />
DISEASE BY NON-INVASIVE IMAGING<br />
IN PATIENTS WITH KNOWN EXTRA-<br />
CARDIAC ATHEROSCLEROTIC DISEASE: THE<br />
GROUND-2 STUDY<br />
R. Vliegenthart 1 , M. Oudkerk 1 , M.A.M. Dekker 1 ,<br />
J.J.A.M. van den Dungen 2 , R.A. Tio 3 , W.P.Th.M. Mali 4 ,<br />
M.M.J.J.R. Jaspers 5<br />
1<br />
Center for Medical Imaging – North East Netherlands<br />
(CMINEN), Dept of Radiology, University Medical Center<br />
Groningen/University of Groningen, Groningen<br />
2<br />
Dept of Surgery, University Medical Center Groningen/<br />
University of Groningen, Groningen<br />
3<br />
Dept of Cardiology, University Medical Center Groningen/<br />
University of Groningen, Groningen<br />
4<br />
Dept of Radiology, University Medical Center Utrecht,<br />
Utrecht<br />
5<br />
Dept of Radiology, Deventer Hospital, Deventer<br />
Patients with extra-cardiac atherosclerosis, like claudication,<br />
carotid stenosis or aortic aneurysm, have an increased risk<br />
of coronary heart disease. The purpose of the GROUND-2<br />
study is to non-invasively evaluate the presence of asymptomatic<br />
coronary artery disease (CAD) by CT calcium scoring,<br />
coronary CT angiography (CTA) and adenosine perfusion cardiac<br />
magnetic resonance imaging (APMR) in case of known<br />
extra-cardiac atherosclerosis.<br />
This study is designed as a prospective multicenter study.<br />
Patients aged 50 and over, diagnosed with extra-coronary<br />
atherosclerosis, either stenotic or aneurysmatic, are eligible<br />
to participate. Exclusion criteria are a history of symptomatic<br />
cardiac disease, severe arterial hypertension and contraindications<br />
to the used imaging modalities. All patients will<br />
non-contrast CT scanning to evaluate the coronary calcium<br />
score. In case of a zero calcium score, patients will be followed.<br />
In all other cases, CTA will be performed to evaluate<br />
the coronary arteries for significant stenoses. In case of a<br />
calcium score above 1000, the CTA is bypassed.<br />
Next, APMR will be used to assess perfusion defects of the<br />
myocardium. If there is a left main stenosis or equivalent on<br />
CTA or a perfusion defect on APMR, the patient will be referred<br />
to a cardiologist for further evaluation and treatment.<br />
All patients will be followed for 5 years for the occurrence<br />
of events.<br />
In this multicenter study, at least 1030 patients will be<br />
included. Inclusion has started in December 2009. This study<br />
will provide insight into the prevalence of silent severe<br />
CAD, detected by non-invasive cardiac imaging, in patients<br />
with known extra-cardiac atherosclerosis. Radiological<br />
screening for asymptomatic CAD may improve survival in<br />
these patients. Preliminary results indicate that significant<br />
coronary atherosclerosis is prevalent in patient with known<br />
extracoronary atherosclerosis.<br />
VUMC<br />
PSEUDO-CONTINUOUS ARTERIAL SPIN<br />
LABELING AT 3T IN ALZHEIMER’S DISEASE -<br />
INITIAL EXPERIENCE IN A MEMORY CLINIC<br />
M.A.A. Binnewijzend, J.P.A. Kuijer, M.R. Benedictus,<br />
P.J. Visser, W.M. van der Flier, M.P. Wattjes, P. Scheltens,<br />
F.A. Barkhof<br />
3D pseudo-continuous arterial spin labeling (PCASL) is a<br />
non-invasive scan technique that measures cerebral blood<br />
flow (CBF). We aimed to compare CBF of subjects with<br />
Alzheimer’s disease (AD), mild cognitive impairment (MCI)<br />
and subjective memory complaints (SMC).<br />
MRI scans, including MPRAGE and 3D-PCASL (post-label<br />
delay 2.0s, 3D-FSE, TR=4.8s, TE=4.7ms, spiral readout 8<br />
arms x 512 samples; 36x5.0mm axial slices; total scan time<br />
4min) were acquired on a 3T GE HDxt scanner in 76 consecutive<br />
subjects (33 AD, 15 MCI, 28 SMC) that visited our<br />
memory clinic. Partial volume estimates were obtained from<br />
MPRAGE images (using the FAST algorithm, part of FSL) to<br />
create CBF maps corrected for partial volume effects. Gray<br />
matter (GM) CBF-values were compared using analyses-ofvariance.<br />
Correlations with cognition (MMSE-scores) and<br />
vascular white matter lesions (WML) were investigated<br />
using linear regression analyses, correcting for age and<br />
gender.<br />
Four subjects (1 AD, 2 MCI, 1 SMC) were excluded from<br />
further analyses because of poor scan quality. Compared<br />
to SMC subjects, GM-CBF was decreased in both MCI<br />
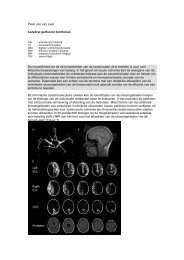
(43±7 vs. 50±8 ml/100g/min; p
RC<br />
<strong>programma</strong> <strong>abstracts</strong> & <strong>abstracts</strong><br />
Figure 1: Whole brain CBF map.<br />
Figure 2: Partial volume corrected gray matter CBF map.<br />
Figure 3: Boxplot of gray matter CBF in SMC, MCI and AD.<br />
UMC St Radboud<br />
MR GESTUURDE PROSTAAT INTERVENTIES;<br />
KLAAR VOOR DE PRAKTIJK?<br />
J.J. Fütterer<br />
Next to digital rectal examination and PSA level, biopsy of<br />
the prostate is an essential procedure for determining optimal<br />
treatment. Systematic TRUSBx is the gold standard, but<br />
it fails to detect numerous tumors. This systematic approach<br />
is characterized by low sensitivity (39–52%) and high specificity<br />
(81–82%).<br />
Using diagnostic MRimages during an MR-directed biopsy<br />
procedure improves quality of the biopsy. In open MR scanners,<br />
the prebiopsy MR images often must be registered to<br />
the real-time biopsy images because open MR scanners do<br />
not provide optimal tissue contrast; thus, the patient must<br />
first be examined in a closed MR scanner and then biopsied<br />
in an open scanner. The advantage of open MR over closed<br />
MR is that the physician has easy patient access. Closed<br />
MR scanners can be used for the prebiopsy scan as well as<br />
for the biopsy procedure. Because operating room is limited<br />
within the closed MR scanner, manipulators are used to perform<br />
the biopsy. The MR detection rates after one negative<br />
biopsy round using MR-guided biopsy ranges between 38%<br />
and 55.5%.<br />
The clinical value of MR-guided prostate biopsy lies in<br />
the fact that a high percentage of prostate cancers can be<br />
depicted using an targeted biopsy technique, eliminating<br />
unnecessary systematic prostate biopsies for patients with<br />
elevated PSA levels and repeated tumor-negative TRUSBx.<br />
Extensive clinical studies are still essential to review the<br />
value of MR-guided biopsy. One of the largest challenges<br />
in taking biopsiesof the prostate is the correction for movements<br />
of the prostate tissue during the biopsy procedure.<br />
In conclusion the combination of a diagnostic MR examination<br />
and MR-guided biopsy is a promising tool and may be<br />
used in patients with previous negative TRUSBx.<br />
MUMC<br />
WAIT AND SEE IN RECTAL CANCER<br />
PATIENTS: SELECTION BY IMAGING AND<br />
OUTCOME<br />
M. Maas, R.G.H. Beets-Tan<br />
Locally advanced rectal cancer is treated with neoadjuvant<br />
chemoradiation. In approximately 20% of the patients the<br />
tumor and the involved lymph nodes disappear or become<br />
sterilized due to this chemoradiation: a complete response.<br />
With a combination of T2-weighted MRI, diffusion-weighted<br />
MRI, gadofosveset-enhanced MRI and endoscopy these<br />
patients can be selected for a ‘wait-and-see policy’, in which<br />
surgery is omitted and patients undergo intensive follow-up.<br />
Maastricht University Medical Centre is the only Dutch<br />
centre that currently performs a study to evaluate this waitand-see<br />
policy with MRI-based selection and follow-up. The<br />
preliminary results are very encouraging and for the future<br />
we expect to be able to offer this wait-and-see policy safely<br />
to complete responders after neoadjuvant chemoradiation.<br />
16<br />
k i j k o o k o p w w w . c o n g r e s s c o m p a n y . c o m<br />
o f w w w . r a d i o l o g e n . n l
esearch naam corner sessie<br />
RC<br />
AMC<br />
NEUROTRANSMITTERS IN DE MRI<br />
L. Reneman<br />
Kinderen krijgen steeds vaker medicijnen <strong>voor</strong>geschreven,<br />
terwijl niet duidelijk is òf en hoe dit hun hersenontwikkeling<br />
beïnvloedt. Onderzoek is er nauwelijks. Niet naar de<br />
bijwerkingen en zelfs niet naar de effectiviteit. Toch stijgt het<br />
gebruik fors, want ze kunnen er baat bij hebben. Er is weinig<br />
bekend over bijwerkingen bij kinderen omdat deze medicijnen<br />
altijd zijn getest in volwassen dieren en mensen. Het meerendeel<br />
van de medicijnen dat wordt <strong>voor</strong>geschreven is zelfs<br />
niet geregistreerd <strong>voor</strong> gebruik in kinderen. Ze worden off<br />
label en off license <strong>voor</strong>geschreven. Uit proefdieronderzoek<br />
weten we dat medicijnen de ontwikkeling van het brein langdurig<br />
kunnen beïnvloeden en daardoor een tegenovergesteld<br />
effect kunnen hebben van wat je zou verwachten. Onderzoek<br />
naar eventuele bijwerkingen van medicijnen bij kinderen is<br />
<strong>voor</strong>al belangrijk <strong>voor</strong> geneesmiddelen die hun invloed uitoefenen<br />
op de hersenen, zoals middelen tegen depressie en<br />
ADHD. Want niet alleen wijkt de stofwisseling van kinderen<br />
af van dan die van volwassenen, hun brein is nog in ontwikkeling<br />
tot aan de jong volwassenheid. Medicijnen zouden die<br />
ontwikkeling kunnen verstoren. In Nederland hebben 8.500<br />
kinderen in de leeftijd van 0 t/m 20 jaar in de eerste helft van<br />
2008 een antidepressivum via de apotheek gekregen. Echter,<br />
de sterkste stijging de afgelopen tien jaar zijn medicijnen<br />
<strong>voor</strong> attention deficit hyperactivity disorder (ADHD). Werden<br />
in 2008 ongeveer 500.00 recepten uitgeschreven, was dit<br />
in 1999 nog maar 132.000 keer. De oorzaak van de forse<br />
stijging zijn de verbeterde diagnostiek en de steeds sterkere<br />
behoefte van ouders en artsen aan verlichting van klachten.<br />
De afdeling <strong>Radiologie</strong> van het AMC heeft door de jaren<br />
heen een sterke reputatie opgebouwd in het bestuderen<br />
van effecten van middelen (misbruik) op de hersenen. Zowel<br />
nationaal als internationaal vervult het AMC hierin een<br />
pioniersfunctie en wordt baanbrekend onderzoek verricht.<br />
In een groot multidisciplinair project onderzoeken we nu de<br />
zogeheten neurologische imprinting van geneesmiddelen.<br />
Bij<strong>voor</strong>beeld, rond 2004 kwamen aanwijzingen dat bij<br />
jongvolwassenen het percentage zelfmoordgevallen juist<br />
toenam onder invloed van serotonine heropname remmers<br />
(SSRIs), waardoor dit medicijn een tijdje gecontraindiceerd<br />
is geweest in deze populatie. Wij onderzoeken hoe dat komt<br />
en wat de werking is van andere geneesmiddelen op de<br />
hersenontwikkeling. Kleven er risico’s aan het gebruik op<br />
jonge leeftijd, of misschien juist onverwachte <strong>voor</strong>delen?<br />
We visualiseren de veranderingen die medicijnen kunnen<br />
aanbrengen in de hersenontwikkeling met behulp van farmacologsiche<br />
magnetic resonance imaging (phMRI). Hierbij<br />
kijken we <strong>voor</strong>al naar hersensystemen die werken op basis<br />
van de neurotransmitters serotonine - waarop medicijnen<br />
tegen depressie aangrijpen - en dopamine - <strong>voor</strong> medicijnen<br />
tegen ADHD. Ook kijken we naar het functioneren van de<br />
hersenen met behulp van neuropsychologisch onderzoek.<br />
Wij denken dat hoe jonger kinderen medicijnen krijgen, hoe<br />
meer ze ingrijpen op de normale uitrijping van de hersenen.<br />
Alle artsen willen het beste <strong>voor</strong> kinderen, maar dan moet<br />
wel duidelijk zijn of je meer goed dan kwaad doet. Ons<br />
onderzoek stelt artsen en ouders in staat de eventuele<br />
risico’s van bijwerkingen af te wegen tegen de <strong>voor</strong>delen<br />
van een medicamenteuze behandeling.<br />
UMC Utrecht<br />
MRI-GUIDED HIGH INTENSITY FOCUSED<br />
ULTRASOUND: THE FUTURE OF TUMOR<br />
ABLATION?<br />
M.A.A.J. van den Bosch<br />
MR-HIFU is an innovative, noninvasive tumor ablation technique.<br />
MR-imaging and focused ultrasound is combined allowing<br />
real-time anatomic guidance and temperature mapping<br />
during treatment. Recently, the volumetric ablation approach<br />
has been introduced in order to reduce treatment length and<br />
more homogenous tumor ablation.<br />
A MR-HIFU system has been installed at the department of<br />
Radiology UMC Utrecht in 2009. From the beginning a successful<br />
program for MR-HIFU treatment of uterine fibroids<br />
has been started. Currently one patient a week is treated in<br />
clinical practice, and a phase2 efficacy study is running.<br />
The first step for treatment of malignant tumors with<br />
MR-HIFU has been made in patients with painful bone<br />
metastases. Palliative treatment of painful bone metastases<br />
is applied in clinical practice since the beginning of this<br />
year. It is expected that besides bone, the first breast cancer<br />
patients will be treated in the beginning of 2012.<br />
Several issues need to be further investigated for successful<br />
cancer treatment with MR-HIFU, including patient selection<br />
criteria, definition of treatment margins and optimal<br />
transducer technology. For this we have a multidisciplinary<br />
MR-HIFU team in UMC Utrecht consisting of interventional<br />
radiologists, radiotherapists, physicists, postdocs and PhDstudents.<br />
1 6 E R A D I O L O G E N D A G E N - 2 9 e n 3 0 S E P T E M B E R 2 0 1 1<br />
17
1 <strong>programma</strong> Abstracts & <strong>abstracts</strong><br />
Sessie 1<br />
Abdominale radiologie 1<br />
Donderdag 29 september, 14.05 - 15.35 uur<br />
O1.1<br />
RESTAGING NODAL STATUS AFTER CHEMO-<br />
RADIATION FOR LOCALLY ADVANCED<br />
RECTAL CANCER: PREDICTIVE FACTORS<br />
M. Maas, D.M.J. Lambregts, M. Berkhof, G.L. Beets,<br />
R.G.H. Beets-Tan<br />
Maastricht Universitair Medisch Centrum, Maastricht<br />
Purpose: Restaging N-stage after CRT for rectal cancer is<br />
more accurate than N-stage prediction at primary staging<br />
of rectal cancer. The aim was to identify predictive factors<br />
which can help a radiologist in predicting the yN-stage.<br />
Methods: 39 patients with locally advanced rectal cancer<br />
underwent MRI before and after CRT. All visible nodes in<br />
the mesorectum were measured and recorded before and<br />
after CRT on a 3DT1W GRE-sequence with 1mm3 voxels.<br />
Baseline characteristics were collected and compared between<br />
patients with and without nodal involvement at pathology<br />
with t-tests and χ2. With regression analyses predictive<br />
factors for nodal involvement after CRT were identified.<br />
Based on the regression analyses a predictive model for yNstage<br />
was constructed and ROC curves were constructed for<br />
this predictive model.<br />
Results: 895 nodes were identified, of which 392 (44%)<br />
disappeared after CRT. Patients with ypN+ had larger nodes<br />
than ypN0-patients: mean 6.3 vs 3.6mm before CRT and 4.5<br />
vs 2.3mm after CRT, respectively (both p
Abdominale radiologie 1 1<br />
MRI is used for EMR identification and thus for identification<br />
of patients who need CRT on the obturator areas, patients<br />
can be spared an extensive resection with associated morbidity.<br />
O1.3<br />
GADOFOSVESET-ENHANCED MRI FOR<br />
NODAL STAGING IN RECTAL CANCER:<br />
PREDICTIVE CRITERIA<br />
D.M.J. Lambregts, M. Maas, I.J.G. Rutten, W.H. Backes,<br />
R.G. Riedl, F.C.H. Bakers, V.C. Cappendijk, G.L. Beets,<br />
R.G.H. Beets-Tan<br />
Maastricht Universitair Medisch Centrum, Maastricht<br />
Purpose: Recently, we showed that MRI using a new<br />
lymph-node contrast (gadofosveset) can significantly<br />
improve accuracy for staging of rectal cancer nodes. Aim<br />
of the present study was to determine the most accurate<br />
predictive imaging criteria for lymph node assessment using<br />
gadofosveset-MRI.<br />
On gadofosveset-MRI, SI was significantly higher in the<br />
benign nodes (p
1<br />
<strong>programma</strong> Abstracts & <strong>abstracts</strong><br />
in 10 en respectievelijk 8 tumoren. Op MRI 3 tumoren op<br />
niveau omslagplooi: peroperatief 2 rectumtumoren en 1<br />
sigmoïdtumor.<br />
De PS-lijn heeft geen onderscheidend vermogen tussen rectum-<br />
en sigmoïdtumor. Ondanks de matige zichtbaarheid van<br />
de omslagplooi correleert MRI in 18 van de 23 tumoren met<br />
peroperatieve bevindingen. De afstand omslagplooi tot anus<br />
(MRI) benadert het 15cm-criterium (endoscopie).<br />
O1.5<br />
CHRONIC DIVERTICULITIS VERSUS<br />
COLORECTAL CANCER: FINDINGS ON CT<br />
COLONOGRAPHY<br />
S.E.H. Cremers 1 , S. Gryspeerdt 2 , P. Lefere 2 , S. Houterman 3 ,<br />
G. Slooter 3 , M.L. Verhulst 3 , P.T.J. Cremers 3<br />
1<br />
Albert Schweitzer ziekenhuis, Dordrecht<br />
2<br />
Virtual Colonoscopy Teaching Centre (VCTC), Hooglede<br />
3<br />
Máxima Medisch Centrum, Veldhoven<br />
Purpose: In CT colonography chronic diverticulitis (CD) can<br />
mimic colorectal cancer (CRC) masses. In order to distinguish<br />
these two entities several findings were analysed.<br />
Methods: 525 symptomatic patients consecutively underwent<br />
CT colonography between June 2008 and February<br />
2011. All patients with pathologic confirmation of CD (13)<br />
and CRC (30) on surgical specimens were included. The<br />
images were analysed in retrospect by a consensus of<br />
two reviewers. Length of the mass, diverticula included in<br />
the mass, growth pattern, luminal narrowing, presence of<br />
perilesional lymph nodes and mesenteric fat stranding were<br />
evaluated. Statistical analysis was performed using Mann-<br />
Whitney and Chi-Square tests.<br />
Results: There was a significant difference in median<br />
length of the mass between CD and CRC, 100 and 49 mm<br />
respectively ( p
Abdominale radiologie 1 1<br />
Figure 1: A) T1-weighted images (T1W) acquired before, 30 s and 60 s after contrast agent (CA) administration, obtained for a patient with<br />
rectal cancer during primary staging. Red line indicates the tumor boundaries. White arrows indicate different tissue components of the rectum.<br />
T2W tumor image is shown as an image inset (upper left). B) Average signal enhancement-time curves obtained for the tumor (black line), rectal<br />
muscle (red line), mucosa (green line) and mesorectal fat (blue line) in three patients. In patient 3, the delineation of ROIs in rectal muscle and<br />
mucosa was not possible.<br />
O1.7<br />
ASSESSMENT OF A COMPLETE RESPONSE<br />
OF RECTAL CANCER TO PREOPERATIVE<br />
CHEMORADIATION THERAPY: A<br />
COMPARISON BETWEEN MR VOLUMETRY<br />
AND DIFFUSION-WEIGHTED MRI<br />
D.M.J. Lambregts 1 , L. Curvo-Semedo 2 , M. Maas 1 ,<br />
T. Thywissen 1 , G. Lammering 1 , G.L. Beets 1 , F. Caseiro-Alves 2 ,<br />
R.G.H. Beets-Tan 1<br />
1<br />
Maastricht Universitair Medisch Centrum, Maastricht<br />
2<br />
Radiology University Clinic, Coimbra University Hospital,<br />
Coimbra, Portugal<br />
Purpose: To determine the performance of diffusion-weighted<br />
MRI (DWI) in assessing a complete tumor response (CR) after<br />
chemoradiation (CRT) in patients with locally advanced rectal<br />
cancer (LARC) by means of [1] volumetric signal intensity and<br />
[2] apparent diffusion coefficient (ADC) measurements, and to<br />
compare its performance with volumetry on T2W-MRI.<br />
Methods: Fifty LARC patients underwent standard T2W-FSE<br />
and DWI (b0,500,1000) pre- and post-CRT. Two independent<br />
readers retrospectively placed free-hand ROIs in each tumorslice<br />
on both datasets to determine pre-CRT and post-CRT<br />
tumor volumes and the tumor volume reduction (∆volume).<br />
ROIs were copied to an ADC-map to calculate mean tumor<br />
ADCs. Histology (ypT0) was the standard reference. ROCcurves<br />
were generated to compare the performance of T2Wvolumetry,<br />
DWI-volumetry and ADC in assessing a CR. The<br />
intraclass correlation coefficient (ICC) was used to evaluate<br />
interobserver variability and the correlation between T2Wvolumetry<br />
and DWI-volumetry.<br />
Results: Areas under the ROC-curve (AUC) for identification<br />
of a CR based on pre-volume / post-volume / ∆volume were<br />
0.57 / 0.70 / 0.84 for T2W-volumetry versus 0.63 / 0.93 / 0.92<br />
for DWI-volumetry (p=0.15 / 0.02 / 0.42). For ADC, AUCs were<br />
0.55, 0.54 and 0.51. Interobserver agreement was excellent for<br />
all pre-CRT measurements (ICC 0.91-0.96) versus good (0.61-<br />
0.79) post-CRT. The ICC between T2W- and DWI-volumetry<br />
was excellent (0.97) pre-CRT versus fair (0.25) post-CRT.<br />
Conclusion: Post-CRT DWI-volumetry provided a high diagnostic<br />
performance is assessing a CR and was significantly<br />
more accurate than T2W-volumetry. Post-CRT DWI was<br />
equally accurate as ∆volume of both T2W-MRI and DWI. Pretreatment<br />
volumetry and ADC were not reliable.<br />
1 6 E R A D I O L O G E N D A G E N - 2 9 e n 3 0 S E P T E M B E R 2 0 1 1 21
1<br />
<strong>programma</strong> Abstracts & <strong>abstracts</strong><br />
Figure 1: ROC-curves for assessment of a CR.<br />
O1.8<br />
WHOLE-BODY MRI, INCLUDING DIFFUSION-<br />
WEIGHTED IMAGING, FOR STAGING NEWLY<br />
DIAGNOSED LYMPHOMA: COMPARISON<br />
TO COMPUTED TOMOGRAPHY IN 101<br />
PATIENTS<br />
T.C. Kwee 1 , M.A. Vermoolen 1 , E.M. Akkerman 2 ,<br />
M.J. Kersten 2 , R. Fijnheer 3 , I. Ludwig 1 , F.J. Beek 1 ,<br />
M.S. van Leeuwen 1 , M.B. Bierings 1 , J. Zsiros 2 ,<br />
H.M.E. Quarles van Ufford 1 , J.M.H. de Klerk 3 , J. Adam 2 ,<br />
J. Stoker 2 , C.S.P. Uiterwaal 1 , R.A.J. Nievelstein 1<br />
1<br />
Universitair Medisch Centrum Utrecht, Utrecht<br />
2<br />
Academisch Medisch Centrum, Amsterdam<br />
3<br />
Meander Medisch Centrum, Amersfoort<br />
Purpose: To compare whole-body magnetic resonance<br />
imaging (MRI), including diffusion-weighted imaging (DWI),<br />
to computed tomography (CT) for staging newly diagnosed<br />
lymphoma.<br />
30.7% (31/101), and lower in 4.0% (4/101) of patients, with<br />
correct/incorrect/unresolved overstaging and incorrect/<br />
unresolved understaging relative to CT in 13/12/6 and 3/1<br />
patient(s), respectively. Staging results of whole-body MRI<br />
with DWI were equal to those of CT in 62.5% (60/96),<br />
higher in 32.3% (31/96), and lower in 5.2% (5/96) of<br />
patients, with correct/incorrect/unresolved overstaging and<br />
incorrect/unresolved understaging relative to CT in 18/10/3<br />
and 4/1 patient(s), respectively.<br />
Conclusion: Staging of newly diagnosed lymphoma using<br />
whole-body MRI (without and with DWI) equals staging<br />
using CT in the majority of patients. Disagreements between<br />
whole-body MRI and CT are mostly caused by overstaging of<br />
the former relative to the latter, with the number of correctly<br />
and incorrectly overstaged cases being approximately equal.<br />
The potential advantage of DWI is still unproven.<br />
Materials and methods: One hundred and one consecutive<br />
patients with newly diagnosed lymphoma prospectively<br />
underwent whole-body MRI (T1-weighted and T2-weighted<br />
short inversion time inversion recovery [n=101], and DWI<br />
[n=96]) and CT. Ann Arbor stages were assigned according<br />
to whole-body MRI and CT findings. Disagreements in<br />
staging between whole-body MRI (without and with DWI)<br />
and CT were resolved using bone marrow biopsy, 18F-fluoro-<br />
2-deoxyglucose positron emission tomography (FDG-PET),<br />
and follow-up FDG-PET, CT, and whole-body MRI studies as<br />
reference standard.<br />
Results: Staging results of whole-body MRI without DWI<br />
were equal to those of CT in 65.4% (66/101), higher in<br />
22<br />
k i j k o o k o p w w w . c o n g r e s s c o m p a n y . c o m<br />
o f w w w . r a d i o l o g e n . n l
Sessie 2<br />
Abdominale radiologie/<br />
Acute radiologie/Diversen<br />
2<br />
Abdominale radiologie/<br />
Acute radiologie/Diversen<br />
Donderdag 29 september, 14.05 - 15.35 uur<br />
O2.1<br />
DYNAMIC CONTRAST ENHANCED MRI FOR<br />
THE EVALUATION OF PERIANAL FISTULAS<br />
IN PATIENTS WITH CROHN’S DISEASE<br />
M.L.W. Ziech, C. Lavini, C.Y. Ponsioen, M.W.A. Caan,<br />
S. Bipat, A.M. Spijkerboer, P. Stokkers, A.J. Nederveen,<br />
J. Stoker<br />
Academisch Medisch Centrum, Amsterdam<br />
Purpose: To determine if dynamic contrast enhanced MRI<br />
(DCE-MRI) can evaluate disease activity in patients with<br />
perianal fistulizing Crohn’s disease.<br />
Methods and materials: Patients with perianal fistulizing<br />
Crohn’s disease, underwent DCE-MRI. The van Assche<br />
MRI-based score and perianal disease activity index (PDAI)<br />
were determined. Transversal DCE-MRI was performed at 3T<br />
during intravenous contrast injection (TE 2.3, TR 5.1, FA 30,<br />
15 slices, total duration of dynamic scan 5.05 min, 70 scans<br />
per slice, temporal resolution 4.2 sec per volume).<br />
The qualitative parameters Maximum Enhancement (ME),<br />
slope of the enhancement curve (SoE) and curve shape type<br />
(as by Lavini et al), as well as the quantitative parameters<br />
Ktrans, Vep, Kep as in the Tofts model were calculated<br />
(using a measured arterial input function) on a pixel by pixel<br />
basis, and then averaged of over an ROI drawn around the<br />
fistula. Spearman correlations between DCE-MRI parameters<br />
and PDAI and MRI-based score were calculated.<br />
Results: Sixteen patients (7 males) were included, mean<br />
age 37 (range 18-63). PDAI correlated with ME (r=0.669,<br />
p=0.005), SoE (r=0.582, p=0.018), ROI volume (r=0.786,<br />
p
2<br />
<strong>programma</strong> <strong>abstracts</strong> & <strong>abstracts</strong><br />
Figure 1<br />
Figure 2<br />
O2.3<br />
MRI FEATURES ASSOCIATED WITH ACUTE<br />
APPENDICITIS<br />
M.M.N. Leeuwenburgh 1 , B.M. Wiarda 2 , A. Spilt 3 ,<br />
P.M.M. Bossuyt 1 , M.A. Boermeester 1 , J. Stoker 1 , OPTIMAP<br />
Studiegroep<br />
1<br />
Academisch Medisch Centrum, Amsterdam<br />
2<br />
Medisch Centrum Alkmaar, Alkmaar<br />
3<br />
Kennemer Gasthuis, Haarlem<br />
Purpose: To identify MRI features associated with appendicitis.<br />
Methods: Signs expected to be associated with appendicitis<br />
were recorded by two expert radiologists in 223 abdominal<br />
MRI scans of patients with suspected appendicitis<br />
(HASTE, HASTE SPAIR, DWI). The investigated features<br />
were:<br />
(1) Diameter >6mm;<br />
(2) Appendicolith;<br />
(3) Peri-appendiceal fat infiltration;<br />
(4) Peri-appendiceal fluid;<br />
(5) Absence of gas in the appendix;<br />
(6) Destruction of the appendiceal wall structure;<br />
(7) Restricted diffusion of the appendiceal wall;<br />
(8) Restricted diffusion of the appendiceal lumen;<br />
(9) Restricted diffusion of focal fluid collections<br />
An expert panel assigned acute appendicitis as final diagnosis<br />
in 117 of 223 patients based on histopathology and<br />
follow-up after 3 months. Associations between imaging<br />
features and appendicitis were evaluated with multivariable<br />
logistic regression analysis.<br />
Results: In 210 of 223 scans the appendix could be visualised.<br />
All 9 investigated MRI features were significantly<br />
associated with appendicitis in univariate analysis. Presence<br />
of two of these features had a probability of appendicitis<br />
between 85%(95%CI: 78-91%) and 100%(95%CI: 86-100%).<br />
If no features were identified in the MRI appendicitis was<br />
present in 0%(95%CI: 0%-8%) of patients. In multivariable<br />
Table 1<br />
24<br />
k i j k o o k o p w w w . c o n g r e s s c o m p a n y . c o m<br />
o f w w w . r a d i o l o g e n . n l
Abdominale radiologie/<br />
Acute radiologie/Diversen<br />
2<br />
analysis only peri-appendiceal fat infiltration and restricted<br />
diffusion of the appendiceal wall had a significant association<br />
with appendicitis. The probability of appendicitis was<br />
96%(95%CI: 90-98%) in presence of both features, and<br />
5%(95%CI: 2-11%) in their absence.<br />
Conclusion: In MRI, peri-appendiceal fat infiltration and<br />
restricted diffusion of the appendiceal wall are strongly<br />
associated with appendicitis. Presence of both features in a<br />
MRI examination leads to a high probability of appendicitis,<br />
whereas their absence almost rules appendicitis out.<br />
O2.4<br />
OPTIMAL STRATEGY IN PATIENTS WITH<br />
SUSPECTED ACUTE APPENDICITIS, CAN MRI<br />
REPLACE CT?<br />
M.M.N. Leeuwenburgh 1 , H.W. van Es 2 , J.W.C. Gratama 3 ,<br />
P.M.M. Bossuyt 1 , M.A. Boermeester 1 , J. Stoker 1 , OPTIMAP<br />
Studiegroep<br />
1<br />
Academisch Medisch Centrum, Amsterdam<br />
2<br />
St. Antonius Ziekenhuis, Nieuwegein<br />
3<br />
Gelre ziekenhuizen, Apeldoorn<br />
Purpose: To identify the optimal imaging strategy in adult<br />
patients with suspected appendicitis.<br />
Methods: We included consecutive patients with suspected<br />
appendicitis in six hospitals. Patients underwent initial<br />
US, followed by CT in case of non-diagnostic US results.<br />
Additionally, all patients underwent MRI (HASTE, HASTE<br />
SPAIR, DWI), with the MRI reader blinded for the results of<br />
the other imaging methods. An expert panel assigned a final<br />
diagnosis based on histopathology and clinical follow up<br />
after 3 months. We evaluated the sensitivity and specificity<br />
of the following scenarios: (1) US only;(2) US in all patients<br />
followed by CT after a non-diagnostic US;(3) US followed by<br />
MRI after a non-diagnostic US;(4) MRI only.<br />
Results: We performed 229 US, 126 CT and 223 MRI examinations<br />
in 230 patients (mean age 38 years, 41% male).<br />
Acute appendicitis was assigned as final diagnosis in 118<br />
patients (51%). Sensitivity of US only was 0.76(95%CI:<br />
0.68-0.83); specificity 0.94(95%CI: 0.88-0.97). Conditional<br />
imaging strategies with CT or MR after a non-diagnostic US<br />
resulted in a significantly increased sensitivity (p
2<br />
<strong>programma</strong> <strong>abstracts</strong> & <strong>abstracts</strong><br />
O2.5<br />
IS TRAUMA SIMULATIE NUTTIG BIJ<br />
TRAINING VAN RADIOLOGEN IN<br />
OPLEIDING?<br />
M.M.A.C. van Doorn, L.F.M. Beenen<br />
Academisch Medisch Centrum, Amsterdam<br />
Doelstelling: Evalueren van het effect van simulatie van<br />
polytrauma Total Body CT scans.<br />
Achtergrond: In grote traumacentra kan het <strong>voor</strong>komen dat<br />
er meerdere traumata tegelijk moeten worden opgevangen.<br />
Van al deze patiënten wordt beeldvorming verricht, waarbij<br />
er steeds vaker een Total Body CT scan (TBCT) wordt uitgevoerd.<br />
Dit genereert een grote druk bij arts-assistenten,<br />
die in korte tijd uit >1000 beelden per patiënt, allereerst de<br />
klinisch meest relevante afwijkingen moeten vaststellen.<br />
Beschrijving: In een prospectieve setting zijn 3 simulaties<br />
uitgevoerd. Per simulatie werd een groot ongeval aangekondigd<br />
met betrokkenheid van 5 slachtoffers, waarbij om de<br />
10 minuten een TBCT scan werd vervaardigd. Elke arts-assistent<br />
kreeg de uitdrukkelijke opdracht binnen 10 minuten de<br />
levensbedreigende letsels op te sporen. De dataset betrof<br />
alleen axiale coupes, reconstructies konden naar eigen<br />
inzicht worden uitgevoerd op het PACS-station. De simulatie<br />
is 3 maal herhaald, met enkele maanden tussenpoos.<br />
Bij de eerste simulatie werd een blanco invulformulier<br />
gebruikt, bij de tweede en derde simulatie een checklist.<br />
Een Likert-scale van 5 werd gebruikt als confidence-score.<br />
Een webbased-enquête werd opgesteld om achteraf de<br />
ervaringen te evalueren.<br />
Resultaten: 19 van de 31 arts-assistenten hebben minimaal<br />
2 simulaties meegedaan.<br />
Het merendeel van de arts-assistenten vindt de simulatie<br />
reëel met betrekking tot tijdsdruk (20/23) en pathologie<br />
(23/23), en goede <strong>voor</strong>bereiding op een ramp(21/22). Bij<br />
8/19 van de arts-assistenten is er een toename van de<br />
confidence-score.<br />
Conclusie: Simulatie is een eenvoudige methode, die het<br />
vertrouwen van arts-assistenten zowel objectief als subjectief<br />
vergroot.<br />
Met behulp van een checklist verloopt de beoordeling meer<br />
gestructureerd.<br />
O2.6<br />
SIMULTANE INTRODUCTIE VAN EEN<br />
NIEUWE PREVENTIE RICHTLIJN VOOR<br />
CONTRASTNEFROPATHIE IN COMBINATIE<br />
MET EEN AANGEPAST RADIOLOGISCH<br />
AANVRAAGFORMULIER: 1 JAAR ERVARING<br />
H.M. Dekker<br />
Universitair Medisch Centrum St Radboud, Nijmegen<br />
Doel: De evaluatie van de toepassing van een aangepast<br />
radiologisch aanvraagformulier.<br />
Methoden: Ziekenhuisbreed is een nieuwe richtlijn<br />
geïntroduceerd om contrastnefropathie(CN) te <strong>voor</strong>komen.<br />
Deze richtlijn adviseert om bij alle patiënten de<br />
serumcreatinineconcentratie te bepalen en de eGFR te<br />
schatten met de MDRD formule en om patiënten met hoog<br />
risico te identificeren en <strong>voor</strong>zorgsmaatregelen te nemen.<br />
Hoog-risicopatiënten zijn gedefinieerd als eGFR1 risicofactor (risicofactoren: hartfalen, perifeer<br />
vaatlijden, dehydratie, >75 jaar, anemie, symptomatische<br />
hypotensie, >150 ml contrastmiddel, nefrotoxische<br />
medicatie) of ziekte van Kahler/Waldenström met lichte<br />
ketens in de urine. Op het aangepaste aanvraagformulier<br />
dienen de MDRD en risicofactoren verplicht te worden aangegeven.<br />
Hoog-risicopatiënten werden verwezen naar een<br />
CN-polikliniek. Gedurende 1 jaar werden gegevens<br />
verzameld van alle poliklinisch geplande urologische patiënten<br />
van ≥18 jaar, gepland <strong>voor</strong> CT met iv contrast.<br />
Resultaten: Er waren 622 patiënten, met een gemiddelde<br />
leeftijd van 56 jaar. Bij 99% was een serumcreatinineconcentratie<br />
bekend. In 23% was de eGFR
Abdominale radiologie/<br />
Acute radiologie/Diversen<br />
2<br />
O2.7<br />
MR EVALUATION OF URETHRAL<br />
DIVERTICULA AND DIFFERENTIAL<br />
DIAGNOSIS IN SYMPTOMATIC FEMALE<br />
PATIENTS<br />
S.I. Verschuuren, R.S. Dwarkasing, W. Dinkelaar, W.C.J. Hop,<br />
G.R. Dohle, G.P. Krestin<br />
Erasmus Medisch Centrum, Rotterdam<br />
Objective: The purpose of this study was to evaluate the<br />
role of MRI in the diagnosis and differential diagnosis of<br />
urethral diverticula (UD) in symptomatic female patients.<br />
Materials and methods: Female patients referred for MRI<br />
at a single institution with suspicion of UD were included<br />
retrospectively. All MRI examinations were independently<br />
evaluated by two radiologists and compared with patients’<br />
follow-up data. Sensitivity and specificity of MRI for UD was<br />
calculated using surgery and clinical confirmation as the<br />
reference standard. Image quality of the urethra and<br />
periurethral region performed with the endoluminal coil was<br />
compared with the pelvic phased array coil.<br />
Results: From a study group of 60 patients (mean age, 44<br />
years), 20 patients (33 %) had UD, 28 (47 %) had an alternative<br />
diagnosis, of which 13 (46 %) were demonstrated with<br />
MRI. In the remaining 12 patients (20 %) no abnormalities<br />
were found. For UD, MRI had a sensitivity and specificity of<br />
both 100 %. Twenty patients had a total of 27 diverticula;<br />
these were mostly locally round (n=12) with sharp margins<br />
(n=25) and high (n=19), homogeneous (n=16) signal intensity<br />
on T2- weighted sequences. The ostium of UD was identified<br />
in 23 (85 %) diverticula by both readers. Agreement was<br />
93 % with a kappa value of 0.72. Endoluminal coil in the<br />
vagina demonstrated the best image quality of the urethra<br />
and periurethral region.<br />
Conclusion: Dedicated MRI is an excellent imaging<br />
modality for UD, furthermore, MRI will show the alternative<br />
diagnosis in almost half of the remaining patients.<br />
O2.8<br />
WAARDE VAN METOCLOPRAMIDE BIJ MRI<br />
ENTEROGRAFIE<br />
U.C. Lalji<br />
Maastricht Universitair Medisch Centrum, Maastricht<br />
Vraagstelling: Is metoclopramide nuttig bij MR-enterografie <strong>voor</strong><br />
het diagnostiseren van Crohn met betrekking tot darmdistentie.<br />
maag of beoordeelbaarheid van het onderzoek.<br />
Metoclopramide interfereerde niet met de acquisitie van de beelden<br />
na toediening van buscopan.<br />
Discussie: Metoclopramide lijkt geen toegevoegde waarde te<br />
hebben bij MR-enterografie.<br />
Methode: In de periode van 1 mei 2010 tot 30 juni 2010<br />
werden 24 patienten geincludeerd met de vraagstelling Crohn.<br />
Hier<strong>voor</strong> ondergingen ze een MRI van de dunne darm volgens<br />
ons MR-enterografie protocol waarbij er 1 liter water met hierin<br />
opgelost metamucil 1 uur <strong>voor</strong> het onderzoek moest worden<br />
gedronken. Van deze 24 patienten kregen 10 patiënten 3 uur <strong>voor</strong><br />
aanvang van het onderzoek 10 mg metoclopramide per os. Ook<br />
moesten zij een vragenlijst invullen m.b.t. bijwerkingen en vragen<br />
over het onderzoek zelf.<br />
De overige 14 patiënten kregen geen metoclopramide maar volgden<br />
wel de rest van het protocol.<br />
2 abdominale radiologen scoorden de onderzoeken op de volgende<br />
punten:<br />
Distentie proximale dunne darm, distentie distale dunne darm,<br />
distensie terminale ilium, maagresidu en beoordeelbaarheid<br />
onderzoek.<br />
De radiologen waren hierbij niet op de hoogte welke patiënten<br />
metoclopramide hadden gekregen.<br />
Resultaten: De onderzoeken waren over het algemeen goed te<br />
beoordelen. Vergeleken met de groep zonder metoclopramide liet<br />
de groep met metoclopramide geen significante verschillen zien in<br />
mate van distentie van de delen van de dunne darm, residu in de<br />
1 6 E R A D I O L O G E N D A G E N - 2 9 e n 3 0 S E P T E M B E R 2 0 1 1<br />
27
3 <strong>programma</strong> <strong>abstracts</strong> & <strong>abstracts</strong><br />
Sessie 3<br />
Cardiovasculaire radiologie<br />
Donderdag 29 september, 14.05 - 15.35 uur<br />
O3.1<br />
DIAGNOSTIC ACCURACY OF COMPUTED<br />
TOMOGRAPHY CORONARY ANGIOGRAPHY<br />
(CTCA) IN WOMEN WITH LOW,<br />
INTERMEDIATE AND HIGH RISK FOR<br />
CORONARY ARTERY DISEASE (CAD)<br />
A.S. Dharampal, A. Rossi, A.C. Weustink, L. Neefjes,<br />
K. Nieman, N.R.A. Mollet, E.H. Boersma, G.P. Krestin,<br />
P.J. de Feyter<br />
Erasmus Medisch Centrum, Rotterdam<br />
Purpose: To determine the diagnostic accuracy of CTCA<br />
in women with low, intermediate and high risk of having<br />
significant CAD.<br />
Materials and methods: Retrospective study including<br />
symptomatic women without prior history of coronary<br />
revascularization who underwent both CTCA and invasive<br />
coronary angiography between 2004 and 2009. The pre-test<br />
probability for significant CAD was estimated using the<br />
Duke Clinical Score and were grouped in low (≤20%), intermediate<br />
(21-80%), and high risk (≥81% probability) groups.<br />
The diagnostic accuracy of CTCA to detect significant CAD<br />
(≥50% lumen diameter narrowing) was assessed in the dif<br />
ferent risk groups on a per patient level.<br />
Results: Two-hundred-and-seventy-five women were included<br />
and stratified in low (n=50), intermediate (n=183) and<br />
high (n=42) risk group. The pre-test probability in the low,<br />
intermediate and high risk groups were 12%, 49% and 89%<br />
with a prevalence of 38%, 66%, and 83%, respectively.<br />
In the low risk group the sensitivity, specificity, PPV and NPV<br />
were 100%(95%CI: 83-100%), 74%(57-86%), 70%(52-84%)<br />
and 100%(85-100%).<br />
In the intermediate risk group the sensitivity, specificity, PPV<br />
and NPV were 98%(94-100%), 78%(66-86%), 89%(83-94%)<br />
and 96%(87-99%).<br />
In the high risk group the sensitivity, specificity, PPV and<br />
NPV were 100%(90-100%), 57%(25-84%), 92%(81-97%)<br />
and 100%(51-100%).<br />
Conclusion: The prevalence of CAD in women is underestimated<br />
in low and intermediate risk groups.<br />
CTCA can accurately rule out significant CAD in women with<br />
all risk groups.<br />
The post-test probability for detecting significant CAD is not<br />
depended on the pre-test probability of disease.<br />
O3.2<br />
ANALYSIS OF AORTIC VALVE ANNULUS<br />
PULSATILE DISTENSION IN PATIENTS<br />
WITHOUT AORTIC VALVE DISEASE BY<br />
ECG-GATED MULTISLICE COMPUTED<br />
TOMOGRAPHY (MSCT)<br />
L.M. de Heer, L.W. Bartels, L.A. van Herwerden,<br />
W.P.Th.M. Mali, K.L. Vincken, J. van Prehn, J. Kluin,<br />
R.P.J. Budde<br />
Universitair Medisch Centrum Utrecht, Utrecht<br />
Objective: A key element of successful transcatheter<br />
aortic valve (AV) implantation is adequate prosthesis sizing.<br />
Cardiac output and aortic compliance result in aortic shape<br />
changes throughout the cardiac cycle. This may result in<br />
inadequate prosthesis sizing. To understand the dynamic<br />
changes in stenotic AV, the healthy aorta has to be studied<br />
first. We assessed the dynamic changes of the AV annulus<br />
using ECG-gated MSCT.<br />
Methods: Fifteen patients without AV disease who had<br />
undergone cardiac MSCT were identified. 3D datasets were<br />
reconstructed at each 10% of the ECG-interval. Per phase a<br />
cross-section in-plane with the AV annulus was reconstructed.<br />
The annulus area was segmented and analysed using<br />
in-home developed software (Dynamix, ISI) (figure). Radius<br />
changes were measured over 360 degrees from the center<br />
of mass per phase and plotted. The complete annulus shape<br />
change in all directions was depicted by fitting an ellipse<br />
over the data obtained in 360 degrees and described by<br />
radius changes over the major and minor axis. The asymmetry<br />
ratio was calculated by dividing the major by the minor<br />
axis. In addition area change was determined.<br />
28<br />
k i j k o o k o p w w w . c o n g r e s s c o m p a n y . c o m<br />
o f w w w . r a d i o l o g e n . n l
Cardiovasculaire radiologie 3<br />
Results: In all patients distension of the AV annulus was<br />
asymmetric (ratio 1.3±0.2). Diameter and area changes<br />
were significant in all patients. Mean diameter change was<br />
20±4%. Mean area change was 28±7%.<br />
Conclusions: The healthy AV annulus diameter and area<br />
show over 20% change during the cardiac cycle and these<br />
changes are asymmetrical. Quantification of dynamic morphological<br />
changes may aid prosthesis sizing and it may<br />
have implications for ultimate clinical success.<br />
Figure 1: Aortic segmentation (pink) by thresholding<br />
O3.3<br />
DIAGNOSTIC PERFORMANCE OF 128-<br />
SLICE DUAL SOURCE CT CORONARY<br />
ANGIOGRAPHY IN PATIENTS WITH<br />
VARIOUS HEART RATES USING 3 DIFFERENT<br />
SCAN PROTOCOLS: A RANDOMIZED STUDY<br />
L.A. Neefjes, A. Rossi, A.S. Dharampal, K. Nieman,<br />
A.C. Weustink, P.J. de Feyter, G.P. Krestin, N.R. Mollet<br />
Erasmus Medisch Centrum, Rotterdam<br />
Purpose: To compare radiation dose and diagnostic performance<br />
of 3 CT coronary angiography (CTCA) protocols using<br />
a 128-slice Dual Source CT scanner (Siemens): a prospective<br />
high pitch spiral (HPS), a prospective step-and-shoot (SAS),<br />
and a retrospective (RS) scan protocol.<br />
Materials and methods: We prospectively included 459<br />
symptomatic patients with a regular heart rate (HR). Patients<br />
with a pre-scan HR
3<br />
<strong>programma</strong> <strong>abstracts</strong> & <strong>abstracts</strong><br />
on a 64 detector-row scanner. Diastolic and systolic images<br />
were reconstructed with FBP (high and low-dose) and the<br />
IR algorithm (low-dose only). Hypo- and hyperdense artifact<br />
volumes were determined using two threshold filters (≤-50<br />
HU and ≥175 HU, respectively). Image noise was measured.<br />
Results: Mean image noise was 16.3±1.6 HU (high-dose<br />
FBP), 23.2±2.3 HU (low-dose FBP) and 16.5±1.7 (low-dose<br />
IR). Low-dose IR reconstructions had similar image noise<br />
compared to high-dose FBP (16.5±1.7 vs. 16.3±1.6, mean<br />
± SD). Mean hypo- and hyperdense artifact volumes (mm 3 )<br />
were 1235/5346 (high-dose FBP); 2405/6877 (low-dose FBP)<br />
and 1218/5333 (low-dose IR). For all PHV types, hypodense<br />
and hyperdense artifact volumes were similar for the highdose<br />
scans reconstructed with FBP when compared to lowdose<br />
scans reconstructed with IR.<br />
Conclusion: Iterative reconstruction allows ECG-gated PHV<br />
imaging with similar image noise and PHV artifacts at 50%<br />
less dose compared to FBP in an in vitro pulsatile model.<br />
Figure 1<br />
O3.5<br />
RADIATION DOSE AND ARTIFACTS<br />
ARE REDUCED BY PROSPECTIVE ECG-<br />
TRIGGERING RELATIVE TO RETROSPECTIVE<br />
ECG-GATING FOR IMAGING OF PROSTHETIC<br />
HEART VALVES WITH 256-SLICE CTS<br />
P. Symersky 1 , J. Habets 2 , B.A.J.M. de Mol 1 , M. Prokop 3 ,<br />
R.P.J. Budde 2<br />
1<br />
Academisch Medisch Centrum, Amsterdam<br />
2<br />
Universitair Medisch Centrum, Utrecht<br />
3<br />
Radboud University Nijmegen Medical Center, Nijmegen<br />
Introduction: Multislice CT imaging has complementary<br />
diagnostic value in the evaluation of prosthetic heart valve<br />
(PHV) dysfunction. For PHV imaging, modified coronary protocols<br />
with retrospective ECG-gating have been used at<br />
considerable radiation exposure. We compared image noise,<br />
radiation dose and artifacts with prospective triggering to<br />
retrospective gating for PHV evaluation.<br />
Methods: Two mechanical PHVs (St Jude bileaflet and<br />
Medtronic Hall tilting disc) were scanned using a pulsatile<br />
in vitro model. Image acquisition was performed with a<br />
256-slice scanner with either a retrospectively gated helical<br />
scan (120kV, 600mAs, CTDI vol<br />
39.8mGy) or a prospectively<br />
triggered axial scan (120kV, 200mAs, CTDI vol<br />
13.3mGy), rotation<br />
time 0.27sec. Hypo- and hyperdense artifact volumes<br />
were quantified using thresholds of -45 and 175HU. Image<br />
noise and artifacts were compared between protocols.<br />
Additionally, mean image noise and radiation dose were<br />
compared between 6 patients with mechanical PHVs<br />
scanned with a prospectively triggered protocol and 20<br />
30<br />
k i j k o o k o p w w w . c o n g r e s s c o m p a n y . c o m<br />
o f w w w . r a d i o l o g e n . n l
Cardiovasculaire radiologie 3<br />
patients scanned with retrospective gating.<br />
Results: In vitro, prospective triggering reduced valve-induced<br />
hypo- and hyperdense artifacts by 35 and 26%, respectively<br />
(p
3<br />
<strong>programma</strong> <strong>abstracts</strong> & <strong>abstracts</strong><br />
aortic (n=59), mitral (n=17), pulmonary (n=1) and tricuspid<br />
(n=1) position. In addition, seven annuloplasty rings were<br />
present. PHV artifacts prohibiting assessment of at least one<br />
coronary segment were present in 12/70 patients (17%).<br />
Artifacts were located in the RCA, LCX and LAD: in 9/70<br />
patients (13%) (mainly from PHVs in the aortic position), in<br />
7/70 patients (10%) and in 3/70 patients (4%) (both mainly<br />
from PHVs in mitral position), respectively, and never in the<br />
left main coronary artery. Biological PHVs (0/17), annuloplasty<br />
rings (0/7), Carbomedics bileaflet (0/20), ON-X bileaflet<br />
(0/7) and Medtronic Hall tilting disc (1/11) PHVs caused no<br />
artifacts precluding coronary artery assessment. However,<br />
coronary artery assessment was hampered by PHV artifacts<br />
in the Bileaflet Saint Jude (3/11) and Duromedics (1/1) PHVs<br />
as well as Sorin (5/7) and Björk Shiley (4/4) tilting disc PHVs.<br />
Conclusions: MSCT imaging is a suitable technique to<br />
assess coronary artery segments in most patients with<br />
PHVs. Björk-Shiley and Sorin tilting disc PHVs prohibit diagnostic<br />
assessment due to PHV artifacts.<br />
Figure 1: PHV artifact in the RCA.<br />
O3.7<br />
MORE NON-COMPACTED MYOCARDIUM IN<br />
BLACK FOOTBALLERS ON CARDIAC MRI<br />
T. Luijkx 1 , B.K. Velthuis 1 , F.J. van Hellemondt 2 , P.J. Senden 2 ,<br />
N.H.J. Prakken 1 , F.J.G. Backx 1 , W.P.T.M. Mali 1 ,<br />
M.J.M. Cramer 1<br />
1<br />
Universitair Medisch Centrum Utrecht, Utrecht<br />
2<br />
Meander Medisch Centrum, Amersfoort<br />
Purpose: Electro- and echocardiographic (e.g. septal wall<br />
thickness, SWT) characteristics are known to differ between<br />
athletes of black and white ethnic descent. We used cardiac<br />
MRI (CMR) to study differences between elite black and<br />
white football (soccer) players.<br />
Methods: 38 healthy elite male football players aged 19-34<br />
years (mean age 23±4 years) underwent CMR: 28 of white<br />
and 10 of black ethnic descent. Blinded observers used a<br />
reproducible contour tracing protocol to assess ventricular<br />
volumes, function and wall mass. Maximum SWT and the<br />
ratio of non-compacted to compacted (NC/C ratio) myocardium<br />
was determined on a standardized apical-to-mid-ventricular<br />
CMR short axis slice at six positions recommended<br />
by the American Heart Association.<br />
Results: Black athletes showed slightly lower end-diastolic<br />
volumes and higher end-systolic volumes in both ventricles,<br />
resulting in lower ejection fractions. SWT was larger in<br />
black athletes. Myocardial NC was more widely present and<br />
more pronounced in black athletes with both a higher peak<br />
(white/black mean 1.81/2.30, range 1.13-2.42/1.14-3.66) and<br />
average (white/black mean 1.02/1.40, range 0.42-1.66/0.69-<br />
2.08) NC/C ratio.<br />
Conclusions: In this small sample footballers of black ethnicity<br />
show decreased ventricular systolic function at rest,<br />
which may be related to more pronounced myocardial noncompaction.<br />
The NC/C ratio frequently exceeds the clinically<br />
used CMR cut-off value of 2.3.<br />
Table 1<br />
32<br />
k i j k o o k o p w w w . c o n g r e s s c o m p a n y . c o m<br />
o f w w w . r a d i o l o g e n . n l
Cardiovasculaire radiologie 3<br />
O3.8<br />
INTRACRANIAL VESSEL WALL IMAGING AT<br />
7.0 TESLA MRI IN ISCHEMIC STROKE AND<br />
TIA PATIENTS<br />
A.G. van der Kolk, J.J.M. Zwanenburg, M. Brundel,<br />
G.J. Biessels, F. Visser, P.R. Luijten, J. Hendrikse<br />
Universitair Medisch Centrum Utrecht, Utrecht<br />
Background & purpose: Conventional imaging methods<br />
cannot depict the vessel wall of intracranial arteries at<br />
sufficient resolution. This hampers the evaluation of intracranial<br />
arterial disease. The aim of the present study was to<br />
develop a high-resolution MRI method to image intracranial<br />
vessel wall.<br />
Methods: We developed a volumetric (3D) turbo spin<br />
echo (TSE) sequence for intracranial vessel wall imaging<br />
at 7.0 Tesla MRI. Inversion Recovery (IR) was used to null<br />
cerebrospinal fluid to increase contrast with the vessel wall.<br />
Magnetization preparation (MP) was applied prior to inversion<br />
to improve signal-to-noise ratio (SNR). 35 patients<br />
with ischemic stroke or TIA (Transient Ischemic Attack) of<br />
various causes were imaged to test the MPIR-TSE sequence.<br />
Gadolinium-based contrast agent (Gadobutrol, 0.1mL/kg)<br />
was administered to assess possible lesion enhancement in<br />
the patients.<br />
Results: The walls of intracranial arterial vessels could be<br />
visualized in all volunteers and patients with good contrast<br />
between wall, blood and cerebrospinal fluid. The quality of<br />
the vessel wall depiction was independent of the vessel<br />
orientation relative to the plane of acquisition. In 21 of the<br />
35 patients a total number of 52 intracranial vessel wall<br />
lesions were identified. Eleven of the 52 lesions showed<br />
enhancement after contrast administration. Only 14 of the<br />
52 lesions resulted in a stenosis of the arterial lumen.<br />
Conclusions: Intracranial vessel wall and its pathology can<br />
be depicted with the MPIR-TSE sequence at 7.0 Tesla. The<br />
MPIR-TSE sequence will make it possible to study the role<br />
of intracranial arterial wall pathology in ischemic stroke.<br />
Figure 1: Example of wall lesion on 7T MPIR-TSE & TOF-MRA<br />
1 6 E R A D I O L O G E N D A G E N - 2 9 e n 3 0 S E P T E M B E R 2 0 1 1<br />
33
4 <strong>programma</strong> <strong>abstracts</strong> & <strong>abstracts</strong><br />
Sessie 4<br />
Mammadiagnostiek 1<br />
Donderdag 29 september, 14.05 - 15.35 uur<br />
O4.1<br />
VISUELE VERSUS SEMI-AUTOMATISCHE<br />
BEOORDELING VAN MAMMADENSITEIT<br />
IN STANDAARD MAMMOGRAFISCH<br />
ONDERZOEK<br />
M.B.I. Lobbes 1 , J. Cleutjens 1 , V. Lima Passos 2 ,<br />
K. Keymeulen 1 , R.G. Beets-Tan 1 , C. Frotscher 1 , M.J. Lahaye 1 ,<br />
J. Wildberger 1 , C. Boetes †<br />
1<br />
Maastricht Universitair Medisch Centrum, Maastricht<br />
2<br />
Universiteit Maastricht, Maastricht<br />
Doel: BI-RADS richtlijnen adviseren analyse van de klierweefseldensiteit<br />
op mammografisch onderzoek als deel van<br />
de mammografische evaluatie. Over het algemeen wordt<br />
visuele inspectie gebruikt om de densiteit van het klierweefsel<br />
in te schatten. Vergelijking tussen visuele en semi-automatische<br />
beoordeling van de klierdensiteit nog niet eerder<br />
onderzocht met een zogenaamde ‘threshold techniek’.<br />
Methoden: Klierdensiteit werd beoordeeld door een<br />
ervaren en onervaren radioloog in 200 mammografieën.<br />
Klierdensiteit werd ook gemeten met een software<strong>programma</strong><br />
dat gebruik maakt van een zogenaamde ‘threshold<br />
technique’ (figuur 1). Klierdensiteit werd gescoord volgens de<br />
richtlijnen van het BI-RADS classificatiesysteem. De correlatie<br />
tussen klierdensiteit van beide radiologen, alsook de correlatie<br />
tussen hun beoordeling versus de semi-automatische<br />
methode, werd uitgedrukt in de gewogen Kappa-waarde.<br />
Resultaten: Klierdensiteitmetingen van beide mammae en<br />
in beide projectierichtingen waren uitstekend en hoog significant<br />
(intraclass correlation coefficients >0.9, alle p
Mammadiagnostiek 1 4<br />
tly be visualized for evaluation in most patients.<br />
To date, 50 patients are evaluated: 3D-US evaluation of the<br />
breast shows a sensitivity of 88% and specificity of 97%,<br />
compared to MR imaging findings (and histology). In coming<br />
months all 201 patients will be evaluated.<br />
Conclusion: In our study so far, 3D-US shows high sensitivity<br />
and specificity in the detection of suspicious lesions compared<br />
to MRI. Automated breast volume scanning seems a promising<br />
new ultrasound technique in breast evaluation.<br />
O4.3<br />
MEDICOLEGAL CLAIMS FOLLOWING<br />
SCREENING MAMMOGRAPHY IN THE<br />
NETHERLANDS<br />
V. van Breest Smallenburg, W. Setz-Pels, F.H. Jansen,<br />
L.E.M. Duijm<br />
Catharina Ziekenhuis, Eindhoven<br />
Purpose: To determine the type and frequency of medicolegal<br />
claims at a Dutch breast cancer screening programme.<br />
Materials and methods: The study population consisted of<br />
all 80019 women who underwent screening mammography<br />
at a southern breast screening region of the Netherlands<br />
between January 1997 and July 2007 (301139 screens). We<br />
included all medicolegal claims that had been recorded at the<br />
central screening department within 3 years following screening<br />
mammography. During 2-year follow-up, we collected the<br />
biopsy results and surgery reports of all referred women. Two<br />
screening radiologists reviewed the screening mammograms<br />
of all screen detected cancers (SDC) and interval cancers (IC)<br />
and determined whether the cancer had been missed at the<br />
previous screen (in case of SDC) or latest screen (in case of<br />
IC). The radiologists were blinded to each others review; discrepant<br />
readings were followed by consensus reading.<br />
Results: Just 3 medicolegal claims had been reported,<br />
all of them related to financial compensation following a<br />
diagnosis of IC. The verdicts of these cases still have to be<br />
finalized. Excisional biopsy had been performed in 10.7%<br />
(234/2183) of false positive referrals. Review showed that<br />
20.8% (261/1254) of SDC had been missed at the previous<br />
screen and 23.6% (139/588) of IC should have been detected<br />
at the latest screen.<br />
Conclusions: Medicolegal claims were very rare, although<br />
a substantial proportion of false positive referred women<br />
had been confronted with excision biopsy and over 20% of<br />
cancers had been missed at the previous screen or latest<br />
screen, respectively.<br />
O4.4<br />
RADIOFREQUENCY-ASSISTED INTACT<br />
SPECIMEN BIOPSY OF BREAST TUMORS:<br />
AN EVALUATION ACCORDING TO THE<br />
IDEAL GUIDELINES<br />
S.C.E. Diepstraten 1 , H.M. Verkooijen 1 , P.J. van Diest 1 ,<br />
M.A. Fernandez-Gallardo 1 , K.M. Duvivier 1 , A.J. Witkamp 1 ,<br />
T. van Dalen 2 , W.P.Th.M. Mali 1 , M.A.A.J. van den Bosch 1<br />
1<br />
Universitair Medisch Centrum Utrecht, Utrecht<br />
2<br />
Diakonessenhuis, Utrecht<br />
Purpose: Radiofrequency-assisted intact specimen biopsy<br />
(RFIB) has been introduced for percutaneous biopsy or<br />
removal of breast tumors. Using radiofrequency cutting,<br />
the system enables the interventional radiologist to obtain<br />
an intact sample of the target lesion. According to IDEAL<br />
guidelines, we performed a critical evaluation of our initial<br />
experience with RFIB.<br />
Methods: Between June and November of 2010, X-ray guided<br />
RFIB was performed in 19 female patients. All patients<br />
presented with suspicious microcalcifications (BI-RADS<br />
III-V) on mammography. Biopsy specimen integrity, thermal<br />
damage and histological diagnosis were assessed by an<br />
expert breast pathologist. Data on technical success,<br />
diagnostic and therapeutic accuracy and peri-procedural<br />
complications were collected and analyzed according to the<br />
IDEAL guidelines.<br />
Results: Median age was 59 years. Median lesion diameter<br />
on mammography was 8 mm (range 2-76 mm). The procedure<br />
was successful in 17/19 (89%) patients and unsuccessful<br />
in 2/19 (11%) patients (1 nonrepresentative sample,<br />
1 sample with extensive thermal damage). Histological<br />
analysis of the RFIB specimen revealed 12/19 (63%) benign<br />
lesions and 7/19 (37%) malignancies (4 DCIS lesions and 3<br />
invasive ductal carcinomas). In 1 patient a DCIS lesion was<br />
completely removed with RFIB. Overall, 3 peri-procedural<br />
complications occurred (1 wound leakage, 1 arterial hemorrhage<br />
and 1 infection requiring oral antibiotics).<br />
Conclusion: Tissue sampling of suspicious breast lesions<br />
can be performed successfully with RFIB. In 1 patient DCIS<br />
was radically excised with RFIB, which illustrates its potential<br />
as a minimally invasive therapeutic procedure for removal<br />
of small breast tumors. This is an interesting focus for<br />
further research when larger probe sizes become available.<br />
1 6 E R A D I O L O G E N D A G E N - 2 9 e n 3 0 S E P T E M B E R 2 0 1 1<br />
35
4<br />
<strong>programma</strong> <strong>abstracts</strong> & <strong>abstracts</strong><br />
O4.5<br />
CAN COMPUTER-AIDED ANALYSIS OF<br />
BREAST MRI PREDICT THE NOTTINGHAM<br />
PROGNOSTIC INDEX OF PATIENT SURVIVAL?<br />
K.G.A. Gilhuijs 1 , K. Pengel 2 , V. Bruijnes 2 , C. Loo 2<br />
1<br />
Universitair Medisch Centrum Utrecht, Utrecht<br />
2<br />
NKI-AvL, Amsterdam<br />
Purpose: The aim of this study is to identify imaging biomarkers<br />
from contrast-enhanced breast MRI that predict the<br />
Nottingham prognostic index (NPI) prior to surgery.<br />
Methods: Patients with invasive breast cancer and eligible<br />
for breast-conserving therapy on the basis of conventional<br />
breast imaging and clinical examination received additional<br />
preoperative breast MRI in a prospective study. Temporal and<br />
morphological features of contrast uptake were automatically<br />
analyzed by a custom-build workstation. The size and grade<br />
of the tumor as well as the number of positive lymph nodes<br />
were assessed at histopathology. From their combination, the<br />
NPI was calculated. Based on NPI, patients were stratified in<br />
subgroups with expected 5-year survival rates larger or equal<br />
to 93% and subgroups with lower survival rates. Multivariate<br />
analyses were performed to identify correlations between<br />
computer-extracted MRI features and NPI. Bonferroni correction<br />
and receiver-operating characteristics were employed.<br />
Results: Five-hundred-and-forty-nine patients were included<br />
between 2000 and 2007. The mean patient age was 57<br />
years, the mean tumor size was 1.6 cm. A total of 224/549<br />
patients had one or more positive lymph nodes. The mean<br />
NPI was 3.1 (range 1.2 - 36.2), 304 patients were at or<br />
above the expected 93% 5-year survival threshold, 245 were<br />
below. From 20 computer-extracted features, the largest<br />
diameter of the washout in the enhancing lesion was most<br />
predictive to discriminate between the two groups, yielding<br />
an area under the curve of 0.74.<br />
Discussion and conclusion: Computer-aided analysis<br />
of breast MRI shows potential to estimate the NPI prior to<br />
surgery, and may thus ultimately provide complementary<br />
information to select neoadjuvant or minimally invasive<br />
treatment strategies.<br />
O4.6<br />
MRI RESPONSE MONITORING IN<br />
NEOADJUVANTLY TREATED<br />
MAMMACARCINOMA: ADVANTAGE OF<br />
TWO- AND THREE-DIMENSIONAL OVER<br />
ONE DIMENSIONAL MEASUREMENTS?<br />
M.H.M. Volmerink, A.L.T. Imholz, R.A.J.M. van Dijk<br />
Deventer Ziekenhuis, Deventer<br />
Aim: to investigate the associations of (changes in) MRI<br />
tumoursize in one, two and three dimensions with specimen<br />
pathology of neoadjuvantly treated mammacarcinoma.<br />
Methods: In this retrospective study, in 35 patients dynamic<br />
contrast-enhanced MRI was performed before, during and<br />
after chemotherapy. Tumoursize was measured by RECIST,<br />
cross-section area (2D), volume (3D; all at early (70s) and<br />
late (450s) enhancement) and by RECIST washout<br />
. Change in<br />
tumoursize from MRI 1 to 2, and tumoursize at MRI3 were<br />
correlated with pathology by logistic regression.<br />
Results: decrease in tumoursize measured by 2D late<br />
(ß=4,1<br />
p=0,03), RECIST early<br />
(ß=2,5 p=0,01) and RECIST washout<br />
(ß=3,4<br />
p
Interventieradiologie/<br />
Cardiovasculaire radiologie<br />
Sessie 5<br />
5<br />
Interventieradiologie/<br />
Cardiovasculaire radiologie<br />
Donderdag 29 september, 14.05 - 15.35 uur<br />
O5.1<br />
CRURAL PTA FOR CRITICAL LIMB ISCHEMIA;<br />
TECHNICAL AND CLINICAL LONG-TERM<br />
RESULTS<br />
A.S. van den Berg 1 , H. Odink 1 , B. Winkens 2<br />
1<br />
Atrium Medisch Centrum, Heerlen<br />
2<br />
Universiteit Maastricht, Maastricht<br />
Purpose: To evaluate the technical and clinical long-term<br />
effectiveness of angioplasty of the crural arteries to preserve<br />
the leg.<br />
Materials and methods: In a 5½ year period a retrospective<br />
study was performed with 109 crural PTA’s of consecutive<br />
patients (47 men and 62 women; median age 79 years; SD<br />
= 9) with critical limb ischemia. Analysis of the clinical longterm<br />
effectiveness of angioplasty of the lower leg arteries<br />
in time (limb salvage rate = LSR), was performed using the<br />
Kaplan-Meier life-table analysis.<br />
Results: PTA included 29 stenoses (mean grade of stenosis<br />
= 90%; SD = 6%, mean length = 5 cm; SD = 12 cm) and 80<br />
occlusions (mean length = 15 cm; SD = 10 cm). Total technical<br />
failures were 16 (TF = 15%) and 93 procedures were<br />
successful (TS = 85%). The procedure-related mortality rate<br />
was 4%.<br />
Of 109 limbs 90 procedures were a PTA of a de novo lesion<br />
(83%). In the group of de novo lesions the LSR after 3 years<br />
was 78% (SD = 4.8). For the 80 technically successful procedures<br />
only the LSR after 3 years was 87% (SD = 4.1).<br />
Conclusion: PTA of the crural arteries appears to be an<br />
effective treatment for patients suffering from critical limb<br />
ischemia.<br />
Figure 1: Kaplan-Meier survival curves of PTA .<br />
1 6 E R A D I O L O G E N D A G E N - 2 9 e n 3 0 S E P T E M B E R 2 0 1 1<br />
37
5<br />
<strong>programma</strong> <strong>abstracts</strong> & <strong>abstracts</strong><br />
O5.2<br />
CLINICAL PERFORMANCE OF A NOVEL<br />
BIOACTIVE COMPOSITE IN THE TREATMENT<br />
OF VERTEBRAL COMPRESSION FRACTURES<br />
R. Schepers-Bok 1 , M. Geerdes 1 , M.E. Havinga 1 , R. Aquarius 2 ,<br />
P.J.W. Wensing 1<br />
1<br />
Ziekenhuisgroep Twente, Hengelo<br />
2<br />
Radboud University Nijmegen Medical Centre, Nijmegen<br />
Objective: To analyse the outcome of percutaneous vertebroplasty<br />
with CortossTM in patients with vertebral compression<br />
fractures.<br />
Methods: Between 2005 and 2010, 221 vertebral compression<br />
fractures were treated with percutaneous vertebroplasty<br />
in 132 patients. Inclusion criteria were: compression fractures<br />
due to osteoporosis, trauma or malignancy, invalidating<br />
back pain due to compression fracture, no improvement<br />
to standard conservative therapy for minimal 6 weeks,<br />
Numerical Rating Scale (NRS) score of at least 7 and bone<br />
marrow edema on MRI scan.<br />
NRS score was obtained before, and two and six weeks<br />
after vertebroplasty. Primary outcome was pain reduction<br />
measured by NRS score. Clinically significant pain relief<br />
was defined as a decrease in NRS score of at least 3 points.<br />
Secondary outcome were new vertebral fractures, injected<br />
volume and complications.<br />
Results: Two weeks after vertebroplasty, 84,7% of the<br />
patients showed a decrease of at least three points on NRS<br />
score. This increased to 86,8% after six weeks. 34 new fractures<br />
occurred in 22 patients (17,4%).No embolisms occurred.<br />
Mean injected volume of Cortoss was 1,54 mL.<br />
Conclusion: In a group of patients with vertebral compression<br />
fractures percutaneous vertebroplasty with Cortoss is<br />
an effective and safe treatment option. PVP leads to a significant,<br />
rapid decrease in pain. Our results are comparable<br />
to results of other studies which used PMMA. These good<br />
clinical results, together with advantages of Cortoss, such<br />
as the low cement volume needed, and the mix-on-demand<br />
delivery system, make it a strong candidate to be a standard<br />
material in vertebral augmentation.<br />
Figure 1: Distribution of Cortoss: trabecular pattern.<br />
Table 1: Patient characteristics.<br />
38<br />
k i j k o o k o p w w w . c o n g r e s s c o m p a n y . c o m<br />
o f w w w . r a d i o l o g e n . n l
Interventieradiologie/<br />
Cardiovasculaire radiologie<br />
5<br />
Table 2: Mean NRS before and after vertebroplasty.<br />
O5.3<br />
INTERVENTIES BIJ PATIËNTEN MET KRITIEKE<br />
ISCHEMIE EN KWALITEIT VAN LEVEN<br />
F.A. Frans, R. Met, S. Bipat, M.J.W. Koelemay,<br />
D.A. Legemate, J.A. Reekers<br />
Academisch Medisch Centrum, Amsterdam<br />
De keuze van de behandeling bij patiënten met kritieke<br />
ischemie (CLI) van het onderbeen is maatwerk. Behoud van<br />
het been en Kwaliteit van Leven (Qol) zijn belangrijke uitkomstmaten<br />
bij de behandeling. Doel van dit onderzoek was<br />
het inventariseren van de behandelingen en het vervolgen<br />
van de Qol bij patiënten met CLI.<br />
In deze prospectieve cohort studie werden alle opeenvolgende<br />
patiënten met CLI die zich presenteerden in ons<br />
ziekenhuis geïncludeerd. De ziektespecifieke VascuQol<br />
vragenlijst werd ingevuld bij presentatie (baseline) en na<br />
6 maanden. Verschillen in scores werden getoetst met de<br />
Wilcoxon-Signed Ranks test.<br />
Van mei 2007 t/m mei 2010 presenteerden zich 218 patiënten<br />
met CLI. Hiervan konden 150 patiënten worden geïncludeerd<br />
in de studie. De uiteindelijke studiepopulatie bestond na 6<br />
maanden uit 127 patiënten. Primaire behandeling was een<br />
PTA (79;62%), chirurgisch (32;25%), conservatief (12;10%) of<br />
een amputatie (4;3%). Bij 43 patiënten (34%) was binnen 6<br />
maanden opnieuw een interventie nodig. De hele groep liet<br />
een toename zien in Qol na 6 maanden in de somscore en op<br />
alle individuele domeinen van de VascuQol (p
5<br />
<strong>programma</strong> <strong>abstracts</strong> & <strong>abstracts</strong><br />
Methods: five patients with liver metastases were treated<br />
with 166 Ho-radioembolization. In order to assess microsphere<br />
biodistribution, pre and post treatment multi-gradient echo<br />
T 2<br />
*-weighted MR images and post treatment SPECT images<br />
were acquired. R 2<br />
* (R 2<br />
*=1/ T 2<br />
*) maps were constructed,<br />
since increases in R 2<br />
* are known to linearly relate to the<br />
166<br />
Ho-MS concentration. R 2<br />
*-maps were compared with<br />
SPECT images. Couinaud’s liver segments and up to 5 index<br />
lesions per patient were selected in volumes of interest<br />
(VOI) using anatomical MR images. VOIs were projected<br />
over the SPECT images and R 2<br />
*-maps and the intensity per<br />
VOI was expressed in percentage of total liver intensity.<br />
From the 5 patients a total of 61 VOIs from R 2<br />
*-maps and<br />
SPECT were compared.<br />
Results: Presence of 166 Ho-MS in the human liver was clearly<br />
visible with both modalities. In certain cases, the higher<br />
resolution of MR-acquired R2*-maps provided additional<br />
information to the SPECT images with regard to the microsphere<br />
biodistribution within a tumor. Biodistribution measurements<br />
showed a high correlation between SPECT and MRI<br />
for liver segments (r 2 0.92) and index lesions (r 2 0.83).<br />
Conclusion: The intrahepatic biodistribution of 166 Ho-<br />
MS can be clearly visualized with both SPECT and MRI.<br />
Biodistribution measurements based on MRI and based on<br />
SPECT show a very good correlation.<br />
Figure 2: Percentage of total liver intensity in each VOI.<br />
Figure 1: 166Ho microspheres visualised on<br />
R2*-map and SPECT.<br />
O5.5<br />
COMPARISON OF SELF REPORTED WALKING<br />
DISTANCE, TREADMILL TEST PERFORMANCE<br />
AND WALKING ABILITY IN PATIENTS WITH<br />
INTERMITTENT CLAUDICATION<br />
M.B. Zagers, F.A. Frans, S. Bipat, J.A. Reekers, S. Jens,<br />
M.J.W. Koelemay<br />
Academisch Medisch Centrum, Amsterdam<br />
Objectives: Decisions regarding treatment of patients with<br />
intermittent claudication (IC) are guided by the patient’s perceived<br />
disability due to limited pain free (PWD) and<br />
maximum walking distance (MWD), and objective assessment<br />
of PWD and MWD on a treadmill. There are few data<br />
on the relationship between treadmill test, daily life and<br />
patient reporting regarding the outcomes, PWD and MWD.<br />
Our objective was to determine correlations between these<br />
assessments.<br />
Methods: All consecutive outpatients with IC who gave<br />
informed consent were included in this prospective study.<br />
Assessments included PWD and MWD during a standardized<br />
treadmill test (3,0 km/h, 8% incline), and on a walking<br />
track on the corridor at the patient’s own pace. All patients<br />
40<br />
k i j k o o k o p w w w . c o n g r e s s c o m p a n y . c o m<br />
o f w w w . r a d i o l o g e n . n l
Interventieradiologie/<br />
Cardiovasculaire radiologie<br />
5<br />
also estimated their Subjective (S)PWD and (S)MWD.<br />
Differences and correlations between the assessments<br />
were determined with the Wilcoxon-Signed Ranks test and<br />
Spearman’s rank test, respectively.<br />
Results: 35 patients (71% men, mean age 64 years) were<br />
included. Mean PWD and MWD at corridor were significantly<br />
higher (115 and 265 meters) compared to the distances<br />
on the treadmill (62 and 128 meters) (P
5<br />
<strong>programma</strong> <strong>abstracts</strong> & <strong>abstracts</strong><br />
Figure 2: Opname na thrombectomie (C) zonder thrombolytica.<br />
O5.7<br />
CAROTID ATHEROSCLEROTIC PLAQUE<br />
PROGRESSION AND CHANGE IN PLAQUE<br />
COMPOSITION OVER TIME; A PROSPECTIVE<br />
IN VIVO SERIAL CT ANGIOGRAPHY STUDY<br />
M.J. van Gils, D. Vukadinovic, D.W.J. Dippel, W.J. Niessen,<br />
A. van der Lugt<br />
Erasmus Medisch Centrum, Rotterdam<br />
Purpose: Serial in vivo imaging would improve our understanding<br />
of atherosclerotic plaque progression and would be<br />
useful in assessing cardiovascular risk and monitoring treatment<br />
efficacy. Purpose of this prospective study is to quantify<br />
changes in atherosclerotic carotid plaque volume and<br />
plaque composition over time with CT angiography (CTA).<br />
Results: Thirty out of 222 arteries were excluded (local<br />
treatment, occlusion or poor image quality). Mean follow-up<br />
was 63±8 months. Intra-observer reproducibility of all volume<br />
measurements was good (ICC=0.90-1.00), except for lipid<br />
(ICC=0.79). Wall volume decreased in 30% and increased<br />
in 70% of vessels (range -6.8-10.9%/year). Baseline lumen<br />
volume was 1479±632 mm 3 , wall volume was 1089±461<br />
mm 3 . On average, volumes of vessel, lumen and wall increased<br />
0.6%, 0.5% and 1.2% per year (p≤0.001, oneway<br />
t-test). Plaque composition changed significantly from<br />
baseline (fibrous 66.3%, lipid 29.0%, calcifications 4.7%):<br />
fibrous tissue decreased with 1.1% (p
Interventieradiologie/<br />
Cardiovasculaire radiologie<br />
5<br />
O5.8<br />
1 JAAR NA EVAR BESTAAT NOG ONGEVEER<br />
EENDERDE DEEL VAN DE ANEURYSMAZAK<br />
UIT ONGEORGANISEERDE THROMBUS<br />
BIJ PATIENTEN MET EN ZONDER<br />
AANTOONBAAR ENDOLEAK<br />
S.A.P. Cornelissen 1 , E.P.A. Vonken 1 , H.J. Verhagen 2 ,<br />
F.L. Moll 1 , L.W. Bartels 3<br />
1<br />
Universitair Medisch Centrum Utrecht, Utrecht<br />
2<br />
Erasmus Medisch Centrum, Rotterdam<br />
3<br />
Image Sciences Institute, Universitair Medisch Centrum<br />
Utrecht, Utrecht<br />
Doel: Doel van dit onderzoek was om de veranderende<br />
organisatiegraad van de aneurysmazak gedurende het eerste<br />
jaar na EVAR af te beelden met MRI.<br />
Methoden: In deze METC-goedgekeurde studie ondergingen<br />
30 patiënten MRI-onderzoeken pre-operatief, < 6 weken<br />
postoperatief, 6 maanden en 1 jaar na EVAR. Er werden<br />
pre-contrast T1- en T2- en postcontrast T1-gewogen beelden<br />
gemaakt. De aneurysmazak werd met speciaal hier<strong>voor</strong> ontwikkelde<br />
software door een ervaren radioloog uitgesplitst<br />
in gebieden met endoleak, ongeorganiseerde en georganiseerde<br />
thrombus aan de hand van de signaalintensiteit op<br />
de verschillende beelden.<br />
Resultaten: Het gemiddelde ongeorganiseerde thrombusvolume<br />
pre-operatief was 23 ml(95%CI 16-30ml), postoperatief<br />
51 ml(95%CI 41-61 ml), na 6 maanden 39 ml(95%CI<br />
29-48ml), na 1 jaar 32 ml(23-41ml), zie figuur 1. Er was een<br />
significante toename in ongeorganiseerde thrombusvolume<br />
postoperatief t.o.v. pre-operatief (gepaarde t-test, p
6<br />
<strong>programma</strong> <strong>abstracts</strong> & <strong>abstracts</strong><br />
Sessie 6<br />
Abdominale radiologie 2<br />
Vrijdag 30 september, 10.45 - 12.15 uur<br />
O6.1<br />
EVALUATION OF A STANDARDIZED CT<br />
COLONOGRAPHY TRAINING PROGRAM IN<br />
NOVICE READER<br />
M.H. Liedenbaum 1 , S. Bipat 1 , P.M.M. Bossuyt 1 ,<br />
R.S. Dwarkasing 2 , M.C. de Haan 1 , R.J. Jansen 1 ,<br />
D. Kauffman 1 , C. van der Leij 1 , M.S. de Lijster 1 , C.C. Lute 1 ,<br />
M.P. van der Paardt 1 , M.G. Thomeer 2 , I.J.A. Zijlstra 1 ,<br />
J. Stoker 1<br />
1<br />
Academisch Medisch Centrum, Amsterdam<br />
2<br />
Erasmus Medisch Centrum, Rotterdam<br />
Purpose: To determine how many CT colonography (CTC) training<br />
examinations have to be evaluated by novice readers to<br />
obtain an adequate level of competence in polyp detection.<br />
Methods: Informed consent was obtained from all participants.<br />
Six physicians (one radiologist, three radiology<br />
residents, two researchers) and three technicians completed<br />
a CTC training program. 200 CTC’s with colonoscopic verification<br />
were selected from a research database, with 100<br />
CTC’s with at least one polyp ≥6mm. After a lecture session<br />
and an individual hands-on training, CTC reading was done<br />
individually with immediate feedback of the colonoscopy<br />
outcome. The increase in per-polyp sensitivity was calculated<br />
for four sets of 50 CTC’s for lesions ≥6mm. Using logistic<br />
regression analyses, the number of CTC’s to reach 90%<br />
sensitivity for lesions ≥6mm was estimated. Reading times<br />
were registered.<br />
Results: The average per-polyp sensitivity for lesions<br />
≥6mm was 76% (207/270) in the first set of 50 CTC’s,<br />
77% (262/342) in the second set (p=0.96 vs. first set), 80%<br />
(310/387) in the third set (p=0.67 vs. first set) and 91%<br />
(261/288) in the fourth set (p=0.018). The estimated number<br />
of CTC’s to be evaluated to reach a sufficient sensitivity for<br />
lesions ≥6mm was 164. Six of the nine readers reached<br />
this level of competence within 175 CTC’s. Reading times<br />
decreased significantly from the first 50 CTC’s to the second<br />
50 CTC’s for 6 readers.<br />
Conclusions: Novice CT colonography readers obtained a<br />
sensitivity equal to that of experienced readers after practicing<br />
on average 164 CTC studies.<br />
O6.2<br />
THE FEASIBILITY OF TRAINING<br />
RADIOLOGIC TECHNOLOGISTS IN<br />
TRIAGING CT-COLONOGRAPHY FOR<br />
EXTRACOLONIC FINDINGS<br />
T.N. Boellaard, C.Y. Nio, P.M. Bossuyt, J. Stoker<br />
Academisch Medisch Centrum, Amsterdam<br />
Purpose: Cost-effectiveness is important for the implementation<br />
of CT-colonography as a screening tool for colorectal<br />
cancer. Radiologists’ reading time contributes substantially<br />
to CT-colonography costs. Therefore we evaluate the<br />
feasibility of radiologic technologists in triaging screening<br />
CT-colonography for extracolonic findings.<br />
Method and materials: Eight technologists participated in<br />
a training program and subsequently reported extracolonic<br />
findings in 280 CT-colonography exams. The dataset<br />
contained 86 possibly (E3) and 30 probably important (E4)<br />
findings (C-RADS). The first and last 40 cases were identical<br />
examination cases. Feedback was given after each case<br />
from reference standard (the consensus read by two radiologists),<br />
except for the examination cases. Technologists<br />
reported lesion location and characteristics, C-RADS classification,<br />
need for a radiologist’s read and reading time.<br />
We constructed learning curves for correct scan and lesion<br />
triaging using a moving average technique.<br />
Results: For the final exam 70% of scans with E3 or E4<br />
findings were correctly triaged, while 30.5% of scans<br />
without E3 or E4 findings were incorrectly triaged. For the<br />
final exam technologists correctly identified and classified<br />
64.4%(67/104) of E3 and 67.5%(27/40) of E4 findings.<br />
This is an improvement, compared to the first exam, of<br />
33.6%(p0.05). The learning curve for<br />
E3 and E4 findings combined did not reach a plateau after<br />
280 cases. The technologists’ average reading time decreased<br />
from 11:51 to 4:13 minutes(p
Abdominale radiologie 2<br />
6<br />
Conclusion: A training program for radiologic technologists<br />
leads to an increased capability of triaging extracolonic findings<br />
at CT-colonography. The number of cases was too low<br />
to reach a sufficient competence.<br />
O6.3<br />
A RANDOMIZED CONTROLLED TRIAL<br />
COMPARING PARTICIPATION AND<br />
DIAGNOSTIC YIELD IN COLONOSCOPY AND<br />
CT-COLONOGRAPHY FOR POPULATION<br />
BASED COLORECTAL CANCER SCREENING<br />
(COCOS TRIAL)<br />
M.C. de Haan 1 , E. Stoop 2 , T.R. de Wijkerslooth 1 , P.M. Bossuyt 1 ,<br />
M. van Ballegooijen 2 , Y. Nio 1 , M.J. van de Vijver 1 , K. Biermann 2 ,<br />
M. Thomeer 2 , M.E. van Leerdam 2 , P. Fockens 1 , J. Stoker 1 ,<br />
E.J. Kuipers 2 , E. Dekker 1<br />
1<br />
Academisch Medisch Centrum, Amsterdam<br />
2<br />
Erasmus Medisch Centrum, Rotterdam<br />
Purpose: To compare participation rate and diagnostic yield<br />
of colonoscopy and CT-colonography screening in a RCT trial.<br />
Methods: A random selection of the Dutch population, aged<br />
50-75 years, was 2:1 randomized to colonoscopy or CTC<br />
for primary CRC screening. Participation rate was defined<br />
as number of invitees undergoing the examination divided<br />
by the total number of invitees. Colonoscopy was positive<br />
when advanced neoplasia (adenomas with a diameter ≥10<br />
mm, a ≥25% villous component, or high grade dysplasia or<br />
CRC) was detected; CTC when a lesion >5mm was found.<br />
Individuals with ≥1 lesions 6-9mm at CTC were offered<br />
surveillance CTC and colonoscopy was offered for lesions<br />
≥10mm. Diagnostic yield was calculated as number of<br />
advanced neoplasia per 100 invitees.<br />
Results: 1,276 of 5,923 colonoscopy invitees participated<br />
(22%) compared to 982 of 2,919 CTC invitees (34%)<br />
(p
6<br />
<strong>programma</strong> <strong>abstracts</strong> & <strong>abstracts</strong><br />
O6.5<br />
MR-COLONOGRAPHY WITH IODINE-<br />
TAGGED LIMITED BOWEL PREPARATION<br />
AND AUTOMATED CARBON DIOXIDE<br />
INSUFFLATION FOR COLONIC DISTENSION<br />
M.P. van der Paardt, F.M. Zijta, T.N. Boellaard, S. Bipat,<br />
A.J. Nederveen, J. Stoker<br />
Academisch Medisch Centrum, Amsterdam<br />
Introduction: To prospectively evaluate image quality and<br />
diagnostic accuracy of 3.0Tesla MR-colonography using<br />
iodine-tagged preparation and CO2 for bowel distension.<br />
Methods: 40 patients at increased risk for colorectal carcinoma<br />
underwent 3.0Tesla MR-colonography using iodinetagged<br />
bowel preparation and automated CO2 insufflation.<br />
Coronal FS 3D-T1-weighted SPGR were acquired in supine<br />
and prone position, 2D-T2-weighted SSFSE in supine<br />
position. Five parameters (Table) were assessed by two<br />
observers for 6 colon segments (240 segments/observer,<br />
480 segments/sequence). Wilcoxon-signed-rank test was<br />
used for comparison. MR-colonography results were compared<br />
with colonoscopy and sensitivity/specificity were<br />
assessed.<br />
Results: The amount of fecal residue was rated ‘0-25%<br />
of lumen filled’ in 66.9%(321/480) of the images. Overall,<br />
the consistency of the residue was scored ‘liquid’;<br />
93.3%(448/480).<br />
Supine distension was ‘adequate’ to ‘optimal’ in<br />
89.2%(428/480) segments on T1-weighted images<br />
and 90.4%(427/472; 8 missing values) on T2-weighted<br />
series. In the T1-weighted series distension was better in<br />
supine compared to prone position: 89.2%(428/480) versus<br />
74.1%(347/468; 12 missing values), p
Abdominale radiologie 2 6<br />
cases, Gd-EOB-DTPA (Primovist®) can be used, which is<br />
taken up by hepatocytes, if they are connected to biliary<br />
ducts, leading to hyperintensity in the hepatobiliary phase.<br />
However, thus far specific enhancement patterns of FNH<br />
have not been reported.<br />
Material and Methods: Retrospective evaluation was<br />
performed of 29 FNH lesions, imaged with MRI precontrast<br />
and after Gd-EOB-DTPA. MR examination consisted<br />
of precontrast T1 sequences, in and out of phase T1<br />
sequences, T1-weighted dynamic sequences after<br />
Gd-EOB-DTPA injection, T2-weighted sequences, Diffusion<br />
weighted imaging and T1 hepatobiliary phase after 10<br />
and 20 minutes.<br />
Results: Evaluation of 29 FNH lesions during the hepatobiliary<br />
phase yielded four types of enhancement: homogenous<br />
hyperintense 12/29 (41,4%), heterogeneous 3/29 (10,3%),<br />
hypointense with peripheral rim enhancement 5/29 (17,3%)<br />
and isointens to liver parenchyma 9/29 (31,0%). In all cases,<br />
enhancement patterns observed at 5 minutes persisted<br />
during 10 and 20 minutes post injection. Pathological examination<br />
demonstrated correlation of observed enhancement<br />
patterns with specific vascular and biliary duct distribution.<br />
Conclusion: In the hepatobiliary phase of the Gd-EOB-DTPA<br />
four different enhancement patterns were recognized in<br />
FNH. Pathological correlation suggests specific subtypes of<br />
FNH lesions.<br />
Figure 1: Four different enhancement patterns FNH.<br />
1 6 E R A D I O L O G E N D A G E N - 2 9 e n 3 0 S E P T E M B E R 2 0 1 1<br />
47
6<br />
<strong>programma</strong> <strong>abstracts</strong> & <strong>abstracts</strong><br />
O6.7<br />
MAGNETIC RESONANCE IMAGING<br />
FINDINGS CORRELATES WITH<br />
PATHOLOGICAL SUBTYPE CLASSIFICATION<br />
OF HEPATOCELLULAR ADENOMAS<br />
S.M. van Aalten, M.G.J. Thomeer, T. Terkivatan,<br />
R.S. Dwarkasing, J. Verheij, R.A. de Man, J.N.M. IJzermans<br />
Erasmus Medisch Centrum, Rotterdam<br />
Purpose: To investigate the correlation between magnetic<br />
resonance imaging (MRI) findings and pathological subtype<br />
classification of hepatocellular adenoma (HCA) and to propose<br />
guidelines for follow-up and management.<br />
Methods: This retrospective study was approved by the<br />
institutional review board and the requirement for informed<br />
consent was waived. Seventy-one resected tumours previously<br />
diagnosed as HCA were classified based on pathological<br />
findings and immunohistochemical analysis: liver-fatty<br />
acid binding protein (L-FABP) negative HCA, inflammatory<br />
HCA, β-catenin positive HCA and unclassified HCA. The<br />
available MRI scans of 61 lesions (48 patients, median age<br />
36 years) were independently reviewed by two radiologists,<br />
thereafter consensus was obtained. Chi-square and Fishers’<br />
exact tests were performed for statistical analysis.<br />
Results: MRI signs of diffuse intratumoral fat deposition<br />
were present in 7 of 9 L-FABP-negative HCA compared to<br />
5 of 29 inflammatory HCA (P = 0.001). Steatosis within the<br />
non-tumoral liver was present in 11 of 29 inflammatory<br />
HCA compared to none L-FABP-negative HCA (P = 0.038). A<br />
characteristic ‘atoll’ sign was only seen in the inflammatory<br />
group (P = 0.027). Presence of a typical vaguely defined type<br />
of scar was seen in 5 of 7 β-catenin positive HCA<br />
(P = 0.003). No specific MRI features were identified for the<br />
unclassified cases.<br />
Conclusions: L-FABP-negative HCA, inflammatory HCA and<br />
β-catenin positive HCA were related to MRI signs of diffuse<br />
intratumoral fat deposition, an ‘atoll’ sign, and a typical<br />
vagely defined scar, respectively. Since β-catenin positive<br />
HCA are considered premalignant, closer follow-up with<br />
MRI or resection may be preferred.<br />
O6.8<br />
MAGNETIC RESONACE IMAGING FOR<br />
PREDICTING RESIDUAL DISEASE AFTER<br />
RADIOTHERAPY IN LOCALLY ADVANCED<br />
CERVICAL CANCER<br />
J.E. Mongula 1 , D. Lambregts 1 , R. Kruitwagen 2 , T. van Gorp 2 ,<br />
A .Kruse 2 , L. Lutgens 3 , R. Lalisang 2 , R. Vliegen 4 ,<br />
B.F. Slangen 2 , R. Beets-Tan 1<br />
1<br />
Maastricht Universitair Medisch Centrum, Maastricht<br />
2<br />
GROW, School for Oncology and Developmental Biology,<br />
Maastricht<br />
3<br />
Maastro clinic, Maastricht<br />
4<br />
Atrium Medisch Centrum, Heerlen<br />
Objective: To assess whether MRI is valuable for evaluating<br />
the presence of residual tumor after RT and which<br />
imaging criteria are the best predictors of response.<br />
Methods: 40 patients with histologically proven primary<br />
cervical cancer FIGO ≥1b were retrospective included, to<br />
date 20 out of 40 have been analyzed. Patients underwent<br />
MRI (standard T2-weighted FSE in 3 planes at 1.5T) before<br />
and 2-3 months after RT. An experienced gynaecologic radiologist<br />
scored the likelihood of residual tumor on post-RT MRI<br />
using a 5-point confidence level score based on assessment<br />
of isointens residual mass, hypointens fibrotic mass, border<br />
irregularity and nodular shape. The standard reference<br />
consisted of gynecological examination with biopsy and/or<br />
clinical follow-up. ROC curve analyses were performed to<br />
determine the performance for assessing residual tumor. The<br />
value of each imaging criterion was assessed.<br />
Results: 3/20 patients had residual disease. AUC for identification<br />
of residual tumor based on visual interpretation<br />
was 0,94; sensitivity 100%, specificity 88%. The individual<br />
imaging criteria resulted in AUCs of 0,94 (isointense mass),<br />
0,50 (hypointense mass), 0,67 (irregular border) and 0,70<br />
(nodular shape). The combination of an isointens nodular<br />
mass resulted in a AUC of 0,98, sensitivity 100%, specificity<br />
88%. Adding an irregular border in AUC of 1,00, sensitivity<br />
100%, specificity 100%<br />
Discussion: MRI can provide high accuracy for the assessment<br />
of residual tumor after RT in patients with locally<br />
advanced cervical carcinoma. The best imaging criteria to<br />
predict residual disease are the presence of an isointense<br />
residual mass with nodular shape and irregular borders.<br />
Use of these criteria could benefit the MR assessment of<br />
residual disease in daily clinical practice.<br />
48<br />
k i j k o o k o p w w w . c o n g r e s s c o m p a n y . c o m<br />
o f w w w . r a d i o l o g e n . n l
Sessie 7<br />
Kinderradiologie/Diversen 7<br />
Kinderradiologie/Diversen<br />
Vrijdag 30 september, 10.45 - 12.15 uur<br />
O7.1<br />
THE ROLE OF DYNAMIC CONTRAST<br />
ENHANCED MR ENTEROGRAPHY AS<br />
COMPARED TO ABDOMINAL ULTRASOUND<br />
IN DIAGNOSING INFLAMMATORY BOWEL<br />
DISEASE IN CHILDREN<br />
M.L.W. Ziech, T.Z. Hummel, A.M. Smets, C. Lavini,<br />
A. Kindermann, S. Bipat, A.J. Nederveen, M.W.A. Caan,<br />
J. Stoker<br />
Academisch Medisch Centrum, Amsterdam<br />
Purpose: Our purpose was to assess if dynamic contrast<br />
enhanced magnetic resonance imaging is useful as compared<br />
to ultrasound in diagnosing inflammatory bowel disease<br />
(IBD) in children.<br />
Method and materials: Consecutive consenting pediatric<br />
patients with suspected IBD were included. All patients<br />
underwent diagnostic work-up including ileo-colonoscopy<br />
and esophagogastroduodenoscopy under general anesthesia,<br />
MR enterography (800 ml sorbitol ingested in 3 hours<br />
as an small bowel and colonic intraluminal contrast agent,<br />
3T coronal dynamic contrast enhanced 3D T1-weighted<br />
sequence, temporal resolution 0.8 seconds) and<br />
abdominal ultrasound (including Doppler measurements of<br />
the superior and inferior mesenteric artery). At MRI maximum<br />
enhancement (ME) was calculated in a region of interest<br />
representing the terminal ileum, ascending, transverse<br />
and descending colon. Statistical analysis was performed<br />
with the Kruskall-Wallis test.<br />
Results: Eighteen paediatric patients were included (9<br />
males, 50%; mean age 14, range 10-18 years). Seven were<br />
diagnosed with ulcerative colitis (39%) and eight with<br />
Crohn’s disease (44%). Three patients had no IBD (17%).<br />
Fifteen patients underwent all modalities, three did not<br />
undergo ultrasound. Patients with Crohn’s disease had significantly<br />
larger wall thickness of the terminal ileum (p=0.037)<br />
measured with abdominal ultrasound. There were no differences<br />
between groups for all other segments and flow<br />
velocities. Mean ME at DCE-MRI did not differ significantly<br />
between the three groups (p=0.202).<br />
Conclusion: Wall thickness of the terminal ileum on abdominal<br />
ultrasound can be used for the diagnosing Crohn’s<br />
disease, but not for ulcerative colitis. There seems to be no<br />
role for DCE-MRI in children with suspected IBD.<br />
O7.2<br />
MINIMALLY INVASIVE MRI BY OMITTING<br />
INTRAVENOUS CONTRAST INJECTION;<br />
DOES IT CHANGE THE RADIOLOGIC<br />
ASSESSMENT OF KNEE JOINT PATHOLOGIES<br />
IN JIA?<br />
R. Hemke, M.A.J. van Rossum, M. van Veenendaal,<br />
T.W. Kuijpers, M. Maas<br />
Academisch Medisch Centrum, Amsterdam<br />
Purpose: MRI is the most preferred imaging modality in<br />
detecting joint pathologies in Juvenile Idiopathic Arthritis<br />
(JIA), despite practical limitations. Gadolinium (Gd) contrast<br />
use prolongs examination time, increases invasiveness and<br />
patient discomfort, and thereby reduces feasibility of MRI<br />
in JIA patients. Therefore, our objective is to evaluate if JIA<br />
joint pathologies can be reliably assessed by MRI<br />
without Gd injection compared with Gd-enhanced MRI as<br />
the reference.<br />
Methods: Data-sets (open-bore, 1.0T) of 46 JIA patients<br />
(mean age 12 years [range 4-18]) were prospectively scored<br />
twice by two experienced readers for the presence of knee<br />
joint pathologies. MRI features were evaluated using a<br />
literature-based assessment score, comprising synovial<br />
hypertrophy, bone marrow edema (BME), cartilage lesions<br />
and bone erosions. The first reading included unenhanced<br />
images (-Gd), whereas complete image sets were available<br />
for the second reading (+Gd).<br />
Results: Using +Gd MRI as the reference, sensitivity and<br />
specificity of -Gd MRI in the detection of BME (89%, 99%),<br />
cartilage lesions (73%, 100%) and erosions (100%, 99%)<br />
were high. Good -Gd and +Gd interreader agreements (ICC)<br />
1 6 E R A D I O L O G E N D A G E N - 2 9 e n 3 0 S E P T E M B E R 2 0 1 1<br />
49
7<br />
<strong>programma</strong> <strong>abstracts</strong> & <strong>abstracts</strong><br />
were found regarding BME (0.87, 0.88), cartilage lesion<br />
(1.00, 0.97) and bone erosion scores (0.90, 0.93). Regarding<br />
synovial hypertrophy scores, the specificity of -Gd MRI was<br />
98%, though the sensitivity was 60%. ICC for +Gd MRI was<br />
0.88, however omitting post-Gd acquisitions increased interreader<br />
variation (ICC=0.76).<br />
Conclusion: Omitting intravenous contrast is unimportant<br />
in the assessment of bone marrow edema, cartilage lesion<br />
and bone erosion scores in knees of JIA patients, but decreases<br />
the reliability of synovial hypertrophy scores.<br />
O7.3<br />
ULTRASOUND TO PREDICT SIGNIFICANT<br />
HEPATIC STEATOSIS IN OBESE<br />
ADOLESCENTS: POOR POST-TEST<br />
PROBABILITY DESPITE ACCEPTABLE<br />
SENSITIVITY AND SPECIFICITY<br />
A.E. Bohté 1 , B.G. Koot 1 , A.J. Nederveen 1 ,<br />
O.H. van der Baan-Slootweg 2 , S. Bipat 1 , T.H. Pels Rijcken 3 ,<br />
P.L.M. Jansen 1 , M.A. Benninga 1 , J. Stoker 1<br />
1<br />
Academisch Medisch Centrum, Amsterdam<br />
2<br />
Heideheuvel Kliniek, Hilversum<br />
3<br />
Tergooiziekenhuizen, Hilversum<br />
Purpose: to evaluate the post-test probability of ultrasound<br />
(US) for the prediction of hepatic steatosis (HS) in a severely<br />
obese adolescent population with 1 H-MRS as reference<br />
standard.<br />
Methods: HS was prospectively evaluated in 113 obese<br />
adolescents with US and 1 H-MRS. For US, HS was<br />
graded semi-quantitatively as 0:none, 1:mild, 2:moderate,<br />
3:severe). 1 H-MR spectra were acquired with a PRESS<br />
sequence in a voxel of 8cm3 at 3T. The fat fraction (FF) was<br />
calculated as: total fat peak area/reference water peak area.<br />
HS was defined as a FF>1.8% and US score ≥1. Moderate/<br />
severe HS as a FF>7.7% and US score ≥2. Sensitivity and<br />
specificity for both thresholds were calculated. Based on<br />
these values the negative and positive post-test probabilities<br />
were determined and plotted against the prevalence of HS.<br />
Results: Mean age was 14.1y; mean BMI was 38.3 kg/m2.<br />
The overall prevalence of HS was 0.45 (95%CI:0.36-0.54)<br />
with a sensitivity of 0.84 (0.78-0.91) and a specificity of 0.55<br />
(0.46-0.64) for US grade ≥1. The prevalence of moderate/<br />
severe HS was 0.14 (0.08-0.21) with a sensitivity of 0.75<br />
(0.67-0.83) and a specificity of 0.87(0.80-0.93) for US grade<br />
≥2. The positive and negative post-test probabilities are<br />
plotted in fig.1 for both threshold values. The positive posttest<br />
probabilities were low: 0.61 for US grade ≥1 and 0.48<br />
for grade ≥2. Negative post-test probabilities (1-NPV) were<br />
adequate: 0.19 and 0.05 respectively.<br />
Discussion: The positive post-test probability of US for HS<br />
was poor. This implies that the applicability of US to predict<br />
HS in the individual obese adolescent is limited.<br />
Figure 1<br />
50<br />
k i j k o o k o p w w w . c o n g r e s s c o m p a n y . c o m<br />
o f w w w . r a d i o l o g e n . n l
Kinderradiologie/Diversen 7<br />
O7.4<br />
RESPIRATORY DISEASE IN PAEDIATRIC<br />
ALLOGENEIC HEMATOPOIETIC STEM<br />
CELL TRANSPLANT (HSCT) RECIPIENTS:<br />
COULD A HIGH-RESOLUTION COMPUTED<br />
TOMOGRAPHY (HRCT) SCORE AID IN<br />
DIAGNOSIS?<br />
P.A. de Jong, A.B. Versluys, J.J. Boelens, F.J.A. Beek<br />
Universitair Medisch Centrum Utrecht, Utrecht<br />
Background: HSCT can be complicated by a variety of<br />
live-threatening infectious and non-infectious pulmonary<br />
complications, but much overlap appears to be present in<br />
HRCT features of these complications.<br />
Aims: To assess observer agreement of a HRCT-score for<br />
typical post-HSCT abnormalities and to determine whether<br />
this HRCT-score can differentiate between infectious and<br />
non-infectious diseases.<br />
Methods: Following protocol paediatric HSCT-recipients<br />
undergo HRCT when respiratory symptoms occur or when<br />
infection is suspected for which chest radiography demonstrates<br />
no obvious cause. Forty-five consecutive disease<br />
episodes in 45 children were studied. HRCT were scored for<br />
severity per lobe (maximum score 18) by two blinded independent<br />
radiologists for various airway and parenchyma/<br />
interstitial abnormalities. Clinical diagnosis was established<br />
by an expert HSCT-physician based on all available information<br />
including follow-up. Possible diagnoses were; pulmonary<br />
infection, early alloimmune lung disease (0.80)<br />
for consolidation and composite<br />
HRCT-score and moderate (intraclass-correlation 0.60-0.79)<br />
for bronchiectasis, tree-in-bud, nodules, ground glass and<br />
expiratory air trapping. The prevalence of abnormalities<br />
largely overlapped between infectious and non-infectious<br />
complications, but alloimmune lung disease was associated<br />
with significantly higher composite HRCT-score (both early<br />
and late), ground glass HRCT-score (early) and air trapping<br />
HRCT-score (late, Figure 1) when compared to infectious<br />
disease.<br />
Conclusion: Our data suggest that the severity of certain<br />
HRCT abnormalities aids in the differentiation between<br />
infectious and non-infectious complications in pediatric<br />
HSCT recipients. The role of the HRCT-score in HSCTrecipients<br />
needs confirmation in an independent study.<br />
Figure 1: Two patients with alloimmune lung disease.<br />
O7.5<br />
OVERCONSUMPTIE VAN RÖNTGEN-<br />
DIAGNOSTIEK BIJ KINDEREN NA<br />
POLSTRAUMA; DE NOODZAAK VAN EEN<br />
KLINISCHE BESLISREGEL<br />
A. Slaar 1 , A. Bentohami 1 , M.W. Walenkamp 1 ,<br />
B.A. van Dijkman 2 , T.S. Bijlsma 3 , M. Maas 1 , J.C.H. Wilde 1 ,<br />
N.W.L. Schep 1 , J.C. Goslings 1<br />
1<br />
Academisch Medisch Centrum, Amsterdam<br />
2<br />
Flevoziekenhuis, Almere<br />
3<br />
Spaarne Ziekenhuis, Hoofddorp<br />
Acuut polsletsel bij kinderen is een van de meest <strong>voor</strong>komende<br />
redenen van een bezoek aan de spoedeisende hulp.<br />
In de meeste ziekenhuizen wordt routinematig een<br />
Röntgenfoto gemaakt van de pols. Echter, een groot aantal<br />
van de Röntgenfoto’s laat geen afwijkingen zien.<br />
Doel: onderzoeken welk percentage van de aangevraagde<br />
röntgenfoto’s met de vraagstelling fractuur ook daadwerkelijk<br />
een fractuur liet zien bij kinderen met polsletsel.<br />
Gegevens van de kinderen (3 tot en met 16 jaar oud) die zich<br />
van 1 september 2009 tot 1 september 2010 presenteerden<br />
op de spoedeisende hulp van een ziekenhuis, waarvan een<br />
röntgenfoto van de pols werd gemaakt met de vraagstelling<br />
polsfractuur, werden geanalyseerd. Van deze patiënten werden<br />
de demografische gegevens, het traumamechanisme,<br />
aanwezigheid van een fractuur en fractuurtype verzameld.<br />
309 patiënten konden worden geanalyseerd. De gemiddelde<br />
leeftijd bedroeg 11.20 (SD=3.1); 153 waren jongens. 77%<br />
1 6 E R A D I O L O G E N D A G E N - 2 9 e n 3 0 S E P T E M B E R 2 0 1 1<br />
51
7<br />
<strong>programma</strong> <strong>abstracts</strong> & <strong>abstracts</strong><br />
van de patiënten was gevallen, 33% van de kinderen waren<br />
gevallen tijdens spelen.<br />
Slechts 50 % van de röntgenfoto’s liet een polsfractuur zien.<br />
Bij 34% van deze patiënten bedroeg het een torus fractuur,<br />
17% een radius fractuur, 13% een greenstick fractuur, 15%<br />
een antebrachii fractuur, bij 19% een Salter Harris type 2<br />
fractuur, resterende fracturen 2%.<br />
Conclusie: De helft van de röntgenfoto’s van kinderen na<br />
een polstrauma liet geen fractuur gezien. Deze overconsumptie<br />
van röntgendiagnostiek leidt tot onnodige wachttijden,<br />
onnodige stralenbelasting bij kinderen, en onnodige<br />
kosten.<br />
Derhalve is er behoefte aan een klinische beslisregel analoog<br />
aan de Ottowa Ankle rules. Deze Amsterdam Wrist<br />
Rules zijn op dit moment in ontwikkeling.<br />
O7.6<br />
STRALING DOOR CT SCANS BIJ KINDEREN<br />
EN HET RISICO OP KANKER: EEN<br />
EPIDEMIOLOGISCHE STUDIE<br />
M. Hauptmann 1 , A.M. Smets 2 , M. van Herk 1 ,<br />
R.A.J. Nievelstein 3 , J.S. Laméris 2 , C.M. Ronckers 2,4<br />
1<br />
Nederlands Kanker Instituut, Amsterdam<br />
2<br />
Academisch Medisch Centrum, Amsterdam<br />
3<br />
Universitair Medisch Centrum Utrecht, Utrecht<br />
4<br />
Stichting Kinderoncologie Nederland, Den Haag<br />
Computer tomografie (CT) scans gaan gepaard met hogere<br />
stralingsdoses dan conventionele beeldvormende technieken.<br />
Omdat het gebruik van CT gestaag stijgt is het van<br />
belang ongewenste neveneffecten goed in kaart te brengen,<br />
in het bijzonder het ontstaan van kanker. Kinderen vormen<br />
een extra kwetsbare groep omdat zij gevoeliger zijn dan<br />
volwassenen <strong>voor</strong> de schadelijke gevolgen van ioniserende<br />
straling en omdat zij een lange levensverwachting hebben<br />
waardoor er een grotere kans is dat negatieve bijwerkingen<br />
tot uiting kunnen komen. Er is op dit moment echter geen<br />
direct empirisch bewijs <strong>voor</strong> een verband tussen CT scans<br />
en kanker.<br />
Wij beschrijven de opzet van een Nederlands retrospectief<br />
cohortonderzoek als onderdeel van een groot multinationaal<br />
samenwerkingsverband. Het onderzoek heeft als doel om<br />
(1) het gebruik van CT scans bij kinderen in Nederland te<br />
beschrijven en (2) het verband tussen CTgerelateerde stralingsdosis<br />
en het risico op kanker (<strong>voor</strong>namelijk leukemie) te<br />
kwantificeren. De methoden van dataverzameling zijn getest<br />
in een pilot-studie en geoptimaliseerd. De beoogde studie<br />
betreft circa 100.000 mensen die in de periode 1999-2010<br />
op kinderleeftijd (0-17 jaar) één of meerdere CT scans hebben<br />
gehad in Nederland. De cohortleden worden geïdentificeerd<br />
en de dosis zal worden geschat op basis van elektronische<br />
archieven (RIS, PACS) van de afdelingen (kinder)<br />
radiologie van deelnemende ziekenhuizen. Follow-up <strong>voor</strong><br />
incidente gevallen van kanker zal via de <strong>Nederlandse</strong> Kanker<br />
Registratie (NKR) gaan. Voorbereidingen <strong>voor</strong> de dataverzameling<br />
zijn dit <strong>voor</strong>jaar van start gegaan, in nauwe samenwerking<br />
met de <strong>Nederlandse</strong> <strong>Vereniging</strong> <strong>voor</strong> <strong>Radiologie</strong> en<br />
de radiologie afdelingen van <strong>Nederlandse</strong> ziekenhuizen.<br />
O7.7<br />
LONGITUDINAL IN VIVO IMAGING OF<br />
GD-LABELED MSCS AND OPTIMIZATION OF<br />
LABELING STRATEGY<br />
J. Guenoun, G.A. Koning, P.A. Wielopolski, G. Doeswijk,<br />
G.P. Krestin, M.R. Bernsen<br />
Erasmus Medisch Centrum, Rotterdam<br />
Purpose: Optimizing the labeling of mesenchymal stem<br />
cells with Gd-liposomes for sensitive, longitudinal cell tracking<br />
in vivo.<br />
Materials and methods: Gd-DTPA was incorporated<br />
in liposomes. Rat mesenchymal stem cells were labeled<br />
with liposomes containing various Gd-dosages, for various<br />
labeling times. Cellular Gd load, cellular toxicity, cell proliferation<br />
rate and cell differentiation were then determined<br />
for the different conditions. Intracellular retention of Gd<br />
was assessed (20d). Intracellular fate of Gd-liposomes was<br />
imaged with confocal microscopy, using intraliposomal fluorescent<br />
dyes. MRI of MSCs was performed on a 1.5T<br />
and 3.0T clinical scanner. Cells were transplanted in rat<br />
skeletal muscle and imaged for 3 weeks in vivo. At several<br />
time-points histology was performed to correlate to MRI<br />
findings. Statistical tests: one-way ANOVA, with Bonferroni<br />
post-hoc test.<br />
Results: Labeling for 4h with 125 µM lipid is most<br />
preferred, combining time-efficiency with sufficient cellular<br />
Gd uptake (30±2.5 pg Gd cell-1), lacking significant<br />
effects on cell viability, proliferation and differentiation.<br />
Gd-liposomes were well retained intracellularly in endosomes.<br />
Gd-liposome labeled MSCs were visualized at 1.5T and<br />
3.0T both in vitro and in vivo. At least 10.000 Gd-MSCs were<br />
detected. Histology showed cellular incorporated liposomes<br />
at the site of injection. Prolonged in vivo imaging of 500,000<br />
Gd-labeled cells was possible for at least two weeks (3.0T).<br />
Conclusion: Gd-loaded liposomes are suitable for cell<br />
labeling, without detrimental effects on cell viability, proliferation<br />
and differentiation allowing sensitive and longitudinal<br />
visualization by MRI.<br />
52<br />
k i j k o o k o p w w w . c o n g r e s s c o m p a n y . c o m<br />
o f w w w . r a d i o l o g e n . n l
Kinderradiologie/Diversen 7<br />
Figure 1<br />
O7.8<br />
CELLULAR IMAGING: IN VIVO ASSESSMENT<br />
OF GD- OR SPIO-LABELED CELL GRAFT<br />
VIABILITY, COMBINING MRI AND<br />
BIOLUMINESCENCE IMAGING<br />
J. Guenoun, A.R. Ruggiero, G. Doeswijk, G.A. Koning,<br />
G.P. Krestin, M.R. Bernsen<br />
Erasmus Medisch Centrum, Rotterdam<br />
Purpose: Using MRI mapping techniques to determine<br />
possible differences in R1, R2 or R2* relaxation rate of<br />
viable and non-viable transplanted rMSCs, labeled with Gd<br />
or SPIO .<br />
Using bioluminescence imaging to link changes in R1, R2 or<br />
R2* to cell viability.<br />
Materials and methods: Study type: experimental longitudinal<br />
follow up.<br />
Gd-DTPA was intraliposomal incorporated. Rat mesenchymal<br />
stem cells (rMSCs), expressing firefly luciferase, were labeled<br />
with SPIO or Gd-liposomes. Cells were divided in a viable<br />
and non-viable fraction (non-viable cells were acquired<br />
by repeated freeze-thawing). For in vivo studies, 5x105<br />
viable or non viable rMSCs were injected intramuscular and<br />
imaged with MRI and BLI at days 2, 5, 10, 15. T1, T2 and<br />
T2* mapping was performed on 3T. At end-point animals<br />
were sacrificed for immunofluorescent staining.<br />
Results: Irrelevant MRI signal from non-viable Gd-MSCs<br />
disappeared quickly (
7<br />
<strong>programma</strong> <strong>abstracts</strong> & <strong>abstracts</strong><br />
Figure 1<br />
54<br />
k i j k o o k o p w w w . c o n g r e s s c o m p a n y . c o m<br />
o f w w w . r a d i o l o g e n . n l
Sessie 8<br />
Mammadiagnostiek 2 8<br />
Mammadiagnostiek 2<br />
Vrijdag 30 september, 10.45 - 12.15 uur<br />
O8.1<br />
EVALUATIE IN TIJD EN ACCURATESSE<br />
VAN CORONALE BEOORDELING VERSUS<br />
CORONALE, SAGITTALE EN AXIALE<br />
VLAKKEN BIJ AUTOMATED BREAST<br />
VOLUME SCANNING<br />
M.D.F. de Jong, G.J. Jager, I.J.M. Dubelaar, T.A. Fassaert,<br />
M.J.C.M. Rutten<br />
Jeroen Bosch Ziekenhuis, ‘s-Hertogenbosch<br />
Doel: Borstkankerscreening middels mammografie is een<br />
effectieve manier van screenen om de sterfte aan boorstkanker<br />
te verlagen. Echter de sensitiviteit wordt lager naarmate<br />
densiteit van het borstweefsel toeneemt. Automated breast<br />
volume scanning (ABVS) kan worden ingezet als toegevoegde<br />
screeningsmodaliteit. Voorafgaand hieraan zullen de testeigenschappen<br />
(hoge sensitiviteit en laag aantal fout negatieven)<br />
geëvalueerd moeten worden. Voordat implementatie in<br />
een screenings<strong>programma</strong> mogelijk is, zal ook het gebruiksgemak<br />
en beoordelingstijd geëvalueerd moeten worden.<br />
Materiaal & methode: Van 50 ABVS scans werden eerst<br />
de coronale reconstructies beoordeeld volgens de BI-RADS<br />
criteria. Ieder onderzoek betrof 3 a 5 scans per borst. Aantal<br />
en locatie van elke laesie en beoordelingstijd werd genoteerd.<br />
Daarna werden de drie richting scans beoordeeld en<br />
vergeleken met de coronale.<br />
Resultaten: Als proof of principal werden 9 patiënten<br />
beoordeeld tot nu, resulterend in 59 scans van 17 borsten.<br />
Er was geen verschil in BI-RADS classificatie en de<br />
drie vlakken beoordeling detecteerde vier extra cysten.<br />
Beoordelingstijd bedroeg bij de coronale evaluatie 28,1<br />
seconden in vergelijking met 96,0 seconden met drie vlakken,<br />
hetgeen een factor 3,4 bedraagt.<br />
Conclusie: Voorlopige resultaten tonen een goede overeenkomst<br />
tussen de twee manieren van beoordelen, waarbij er<br />
aanzienlijke tijdwinst te behalen valt met de coronale scan<br />
beoordeling. Dit kan belangrijk zijn als ABVS als screeningsmodaliteit<br />
ingezet gaat worden.<br />
O8.2<br />
OPBRENGST VAN HERHAALDE VERWIJZING<br />
NA EEN EERDERE FOUT POSITIEVE<br />
SCREENINGSMAMMOGRAFIE<br />
W. Setz-Pels 1 , L.E. Duijm 1 , A.C. Voogd 2<br />
1<br />
Catharina Ziekenhuis, Eindhoven<br />
2<br />
Universiteit Maastricht, Maastricht<br />
Doel: Bepaling van de screeningsuitkomsten van vrouwen<br />
die opnieuw zijn verwezen <strong>voor</strong> een laesie welke na een<br />
eerdere verwijzing als fout positief is afgegeven.<br />
Methoden: We includeerden alle 424703 screeningsonderzoeken,<br />
welke van 1995 t/m 2009 bij 2 screeningseenheden<br />
waren gemaakt. Van alle 5676 verwijzingen werd na 1 jaar,<br />
middels de verslagen van radiologische, chirurgische en<br />
PA-bevindingen in het natraject, vastgesteld of er al dan niet<br />
sprake was van borstkanker. Bij 61 van de 147 vrouwen, die<br />
na een eerdere fout-positieve verwijzing <strong>voor</strong> een tweede<br />
keer waren verwezen, werd middels de screeningsfoto’s<br />
en notities van de screeningsradiologen vastgesteld dat de<br />
reden <strong>voor</strong> herhaalde verwijzing dezelfde laesie betrof.<br />
Resultaten: Bij 2180 verwezen vrouwen was sprake van<br />
borstkanker (5,1 borstkankers per 1000 screens, positief<br />
<strong>voor</strong>spellende waarde van verwijzing (PVW): 38,4%, 95%<br />
betrouwbaarheids-interval 37,1%-39,7%). Bij 22 van de<br />
61 vrouwen, opnieuw verwezen <strong>voor</strong> dezelfde laesie<br />
na een eerdere fout positieve screen, werd borstkanker<br />
vastgesteld (PVW 36,1%, 95% betrouwbaarheids-interval<br />
23,7%-48,5%). Bij 4 van deze 22 borstkankers betrof het<br />
een advanced cancer (invasief carcinoom >20 mm en/of<br />
lymfkliermetastasen). De vertraging in borstkanker diagnose<br />
varieerde van 21 tot 92 maanden (gemiddeld 42,5 maanden)<br />
en 9 vrouwen (40.9%) waren tenminste 1 keer gescreend<br />
(en niet verwezen) tussen de eerste, ten onrechte fout positieve<br />
verwijzing, en de tweede verwijzing.<br />
Discussie: Bij een belangrijk percentage vrouwen die<br />
opnieuw wordt verwezen <strong>voor</strong> dezelfde laesie, is sprake<br />
van borstkanker. Verder onderzoek is vereist om te bepalen<br />
welke factoren in het natraject en in de screening leiden tot<br />
een vertraging in de diagnose borstkanker.<br />
1 6 E R A D I O L O G E N D A G E N - 2 9 e n 3 0 S E P T E M B E R 2 0 1 1<br />
55
8<br />
<strong>programma</strong> <strong>abstracts</strong> & <strong>abstracts</strong><br />
O8.3<br />
RESPONSE EVALUATION OF NEOADJUVANT<br />
CHEMOTHERAPY IN MAMMACARCINOMA:<br />
ASSOCIATION OF CHANGES IN MRI<br />
DYNAMIC GADOLINEUM ENHANCEMENT<br />
AND DIFFUSION WEIGHTED IMAGING (DWI)<br />
V.H.P. Tran, M.H.M. Volmerink, A.L.T. Imholz,<br />
R.A.J.M. van Dijk<br />
Deventer Ziekenhuis, Deventer<br />
Background: Monitoring tumour response in neoadjuvant<br />
chemotherapy in mammacarcinoma is based on MRI dynamic<br />
gadolineum enhancement. However, the role of DWI in<br />
tumour response monitoring remains to be established.<br />
Methods: In this retrospective study, (changes in) apparent<br />
diffusion coefficient (ADC) after three cycles of neoadjuvant<br />
chemotherapy in 29 consecutive patients treated in our hospital<br />
between 2006 and 2010 were compared to changes<br />
in tumour size measured by RECIST, cross sectional area of<br />
tumour (both early enhancement), and diameter of gadolineum<br />
washout.<br />
Results: Following chemotherapy, ADC increased from<br />
1,44*10 -3 mm 2 /sec (SD0,37*10 -3 ) to 1,69*10 -3 mm 2 /sec<br />
(SD0,40*10 -3 ; Student’s t-test p
Mammadiagnostiek 2 8<br />
MRI was performed on a 7T whole-body scanner (Philips<br />
Health Care, Cleveland, USA) using a two-channel doubletuned<br />
unilateral RF breast coil. The protocol included a dynamic<br />
series consisting of 7 consecutive 3D T1-weighted Turbo<br />
Field Echo scans with fat suppression by means of selective<br />
water excitation [TR/TE 5.0/2.0ms, binominal FA 20˚, FOV<br />
160x160x160mm 3 , acquired resolution<br />
1mm isotropic, temporal resolution of 63seconds]; and a<br />
high resolution T1-weighted 3D Fast Field Echo Spectral<br />
Selection Attenuated Inversion Recovery sequence [acquired<br />
resolution 0.45x0.57x0.45mm 3 ]. After the 1st dynamic scan<br />
0.1mmol/kg Gadobutrol was injected.<br />
Lesions were assessed according to ACR BI-RADS-MRI criteria.<br />
Results were compared to histopathology.<br />
Results: The exams were technically successful. Lipid suppressed<br />
sequences showed good lesion-and-fibroglandulartissue<br />
to fat contrast. All lesions were masses of irregular<br />
shape. Margins were spiculated in 4 and irregular in 1.<br />
Enhancement was heterogeneous in 3, homogeneous in<br />
1 and rim type in 1. In 4 lesions the kinetic curve showed<br />
rapid-rise, followed by wash-out: type-3 curve. 1 lesion showed<br />
rapid-rise followed by a plateau-phase: type-2 curve.<br />
All lesions were categorized BI-RADS V. Histopathology<br />
showed 3 ductulolobular and 2 ductal carcinomas.<br />
Conclusion: CE Breast MRI at 7T is technically feasible.<br />
The exams were amenable to BI-RADS-MRI conform analysis,<br />
allowing for future intra-individual comparison between<br />
7T and 3T.<br />
Figure 1: X-ray mammography and 7T CE-MRI results<br />
obtained from a 62 year old patient.<br />
a) X-ray mammography (Cranio-Caudal view, rotated to correspond<br />
to the MRI orientation), showed a BI-RADS V lesion (circle).<br />
b) Pre-contract T1 weighted MRI (voxel size 1x1x2mm3) showed a<br />
irregular mass.<br />
c) After administration of contrast agent the mass showed heterogeneous<br />
enhancement (T1w imaging, voxel size 1x1x2mm3)<br />
d) High resolution T1w SPAIR (voxel size 0.45x0.45x0.57mm3) showed<br />
good fat suppression and fine morphological details.<br />
e) The most malignant curve (squares) shoed a rapid initial rise, followed<br />
by a plateau in the delayed phase. The average curve showed<br />
a similar “tpe-2” pattern (triangles).<br />
O8.6<br />
DE INVLOED VAN MRI OP HET BELEID EN<br />
DE UITKOMST VAN PATIËNTEN MET EEN<br />
INVASIEF LOBULAIR MAMMACARCINOOM<br />
J.P. Pennings, R. Storm, R. Rozendaal, R.H.C. Bisschops<br />
Albert Schweitzer ziekenhuis, Dordrecht<br />
Doel: Preoperatieve MRI is een onderdeel van de<br />
EU-richtlijnen bij het beleid van het invasieve lobulaire carcinoom<br />
(ILC), vanwege de permeatieve groei, frequent gerapporteerd<br />
multifocaal en multicentrisch <strong>voor</strong>komen (32%) en<br />
contralaterale laesies (7%). In deze retrospectieve studie<br />
is gekeken of er verschil is in de chirurgische behandeling<br />
sinds het invoeren van een preoperatieve MRI.<br />
Methode: Tussen januari 2007 en maart 2011 werden 117<br />
patiënten met een histologisch bewezen ILC geïncludeerd.<br />
49 (42%) patiënten onderging sinds het invoeren van de<br />
richtlijn in 2008 een MRI, van wie 5 postoperatief. Alle<br />
patiënten werden behandeld conform de geldende richtlijnen.<br />
De volgende primaire uitkomstmaten werden vergeleken:<br />
contralaterale bevindingen, chirurgische behandeling,<br />
irradicaliteit en heroperaties.<br />
Resultaten: Tussen de patiënten met (n= 49) en zonder<br />
(n=68) een MR mammografie zijn geen significant verschillen<br />
in patiëntkarakteristieken, bevindingen op X-mammagram<br />
of echografie. In beide groepen werd één contralaterale<br />
tumor gevonden, echter geen ILC maar een ductaal adeno-<br />
1 6 E R A D I O L O G E N D A G E N - 2 9 e n 3 0 S E P T E M B E R 2 0 1 1<br />
57
8<br />
<strong>programma</strong> <strong>abstracts</strong> & <strong>abstracts</strong><br />
carcinoom. In de MRI groep toonde 14 (28%) patiënten een<br />
multifocale of een multicentrische laesie. Bij acht patiënten<br />
werd een additionele benigne contralaterale laesie gevonden<br />
met de MRI. Er is geen significant verschil in chirurgische<br />
behandeling tussen de twee groepen, 19 (39%) patiënten<br />
met MRI en 18 (27%) patiënten zonder MRI ondergingen<br />
een lumpectomie. Er zijn ook geen significante verschillen<br />
tussen de MRI groep en de niet-MRI groep in irradicaliteit<br />
(18% vs. 12%) en het aantal heroperaties (14% vs. 4%).<br />
Discussie: Er werd geen contralaterale ILC gevonden.<br />
Preoperatieve MRI liet geen significant verschil zien in chirurgische<br />
behandeling in de door ons onderzochte populatie.<br />
O8.7<br />
MOLECULAR OPTICAL IMAGING USING<br />
AN ORGANIC FLUOROPHORE AND A<br />
CLINICAL FLUORESCENCE DIFFUSE OPTICAL<br />
TOMOGRAPHY SYSTEM - EXTENSIVE<br />
PHANTOM EXPERIMENTS<br />
A. Adams 1 , J.E.M. Mourik 2 , M. van der Voort 3 ,<br />
W.P.Th.M. Mali 1 , S.G. Elias 1<br />
1<br />
Universitair Medisch Centrum Utrecht, Utrecht<br />
2<br />
Leids Universitair Medisch Centrum, Leiden<br />
3<br />
Philips Research, Eindhoven<br />
Purpose: Fluorescence Diffuse Optical Tomography (FDOT)<br />
is an emerging clinical breast imaging modality. To estimate<br />
Limits of Detection (LOD) of a clinical FDOT breast system<br />
(Philips, The Netherlands), phantoms filled with the clinical<br />
grade available near-infrared organic fluorophore IRDye800CW<br />
(Licor, Lincoln, NE) were scanned in various situations.<br />
Methods: Phantoms (0.9cm 3 , 2.1cm 3 ) were filled with<br />
IRDye800CW and suspended in optical matching fluid (with<br />
optical properties of average breast tissue) at a center and<br />
an edge position in a medium sized breast cup (±500cm 3 ).<br />
Relative (1-120:0, 1-6:1) and absolute (2-20nM) phantom-tobackground<br />
concentration differences were assessed. Threedimensional<br />
fluorescence images (excitation: 730nm; filters:<br />
>750nm) were obtained twice on different days. Average<br />
signal intensities were determined on reconstructed images<br />
for volumes matching the sizes and locations of the phantoms.<br />
Regression lines were fitted and LOD were estimated<br />
(LOD=(s B<br />
/β)*k n<br />
; s B<br />
: standard deviation of measurements of<br />
blanks; β: slope of regression line; kn: coverage factor (3.13<br />
for duplicate measurements and five measurements of<br />
blanks to reach a type-1 error of 1%)). Pearson’s correlationcoefficients<br />
and between-day reproducibility were calculated.<br />
Results: The LOD ranged from 0.1nM to 2.3nM for the different<br />
situations. The fluorescent signal was very well linearly<br />
correlated with concentration differences (R 2 : 0.95-1.00); between-day<br />
reproducibility was excellent (intraclass-correlation:<br />
0.93-0.99). Differences in regression line slopes were observed<br />
for the two phantoms and locations but did not affect the LOD.<br />
Conclusion: Limits of Detection of the Fluorescence Diffuse<br />
Optical Tomography system for IRDye800CW are in the lownanomolar<br />
range for relevant situations. Upcoming clinical<br />
studies with this system and this fluorophore are feasible.<br />
This research was supported by the Center for Translational<br />
Molecular Medicine (MAMMOTH).<br />
Figure 1: The clinical Fluorescence Diffuse Optical Tomography<br />
(FDOT) breast imaging system. (Philips, The Netherlands)<br />
Table 1<br />
58<br />
k i j k o o k o p w w w . c o n g r e s s c o m p a n y . c o m<br />
o f w w w . r a d i o l o g e n . n l
Mammadiagnostiek 2 8<br />
Figure 2<br />
O8.8<br />
CORRELATIE VAN GEBIOPTEERDE<br />
MICROCALCIFICATIES IN DE MAMMAE MET<br />
DE INITIËLE BI-RADS CODERING; ANALYSE<br />
EN HERBEOORDELING VAN BI-RADS 3<br />
CALCIFICATIES<br />
K.J. Kraal, J.J. Hensen, A.C. Sikkenk, J. Nijman, R.A. Niezen,<br />
D. Vroegindeweij<br />
Maasstad Ziekenhuis, Rotterdam<br />
Doel: evaluatie en justificatie van stereotactisch gebiopteerde<br />
microcalcificaties in de mammae en vergelijking van<br />
de initiële en gereviseerde BI-RADS codering.<br />
Methode: retrospectieve analyse van de in de periode<br />
2007-2009 stereotactisch gebiopteerde microcalcificaties.<br />
Per mammabiopt werd de oorspronkelijke BI-RADS codering<br />
vergeleken met de PA-uitslag.<br />
De BI-RADS 3 groep (42 biopten) werd <strong>voor</strong> herbeoordeling<br />
<strong>voor</strong>gelegd aan een ervaren mammaradioloog (A) en een<br />
ouderejaars assistent (B), zonder kennis van de oorspronkelijke<br />
codering maar met kennis van de oorspronkelijke klinische<br />
informatie en ondergane stereotaxie. Maligne werd<br />
gedefinieerd als BIRADS 4 en 5.<br />
Bij herevaluatie van de oorspronkelijke BI-RADS 3 codering,<br />
ivm te hoog percentage maligniteit, ontstond een spreiding<br />
naar andere coderingen waarbij 44% een BI-RADS code 2<br />
of 3 en 56% code 4 of 5 kregen. Beoordelaar A en B bereikten<br />
een sensitiviteit van 86%, resp. 57 % en een positief<br />
<strong>voor</strong>spellende waarde van 25%, resp. 17 % <strong>voor</strong> de maligne<br />
microcalcificaties.<br />
Conclusie: van de stereotactische biopten in verband met<br />
microcalcificaties bleek 26% maligne. De oorspronkelijke<br />
codering laat een te hoog percentage maligne microcalcificaties<br />
met oorspronkelijke BI-RADS 3 codering zien.<br />
Bij herbeoordeling ontstaat een significante verschuiving van<br />
code 3 naar een hogere codering en een betere correlatie<br />
met de PA.<br />
De meest ervaren beoordelaar haalt bij herbeoordeling de<br />
hoogste sensitiviteit en PVW <strong>voor</strong> maligne microcalcificaties.<br />
Resultaten: van 236 biopten bleek 74% benigne en 26%<br />
maligne. Respectievelijk 0% van de BI-RADS 2-, 16% van de<br />
BI-RADS 3-, 26% van de BI-RADS 4- en 88% van de BIRADS<br />
5 gecodeerde microcalcificaties waren maligne.<br />
1 6 E R A D I O L O G E N D A G E N - 2 9 e n 3 0 S E P T E M B E R 2 0 1 1<br />
59
8<br />
<strong>programma</strong> <strong>abstracts</strong> & <strong>abstracts</strong><br />
O8.9<br />
TRENDS IN INCIDENCE AND DETECTION<br />
OF ADVANCED BREAST CANCERS AT<br />
BIENNIAL SCREENING MAMMOGRAPHY:<br />
A POPULATION BASED COHORT STUDY<br />
J. Nederend, F.H. Jansen, L.E.M. Duijm<br />
Catharina Ziekenhuis, Eindhoven<br />
Purpose: To determine trends in incidence of advanced<br />
breast cancer (ABC) at screening mammography and determine<br />
the potential of reducing ABC at screening.<br />
Methods and Materials: We included all 351,009 biennial<br />
screening mammograms obtained in a Dutch breast<br />
cancer screening region between 1997-2009. Two screening<br />
radiologists reviewed screening mammograms of all advanced<br />
screen detected cancers (SDCs) and advanced interval<br />
cancers (ICs) and determined whether the ABC (defined as<br />
>T2-tumour and/or axillary lymph node positive tumour) had<br />
been visible at the previous screen (SDC) or latest screen<br />
(IC). Outcome measures were the proportions of ABCs<br />
among SDCs and ICs through the years and the potential of<br />
detecting SDCs and ICs at an earlier stage.<br />
Results: The incidence of ABC did not decline through the<br />
years and fluctuated annually from 28.7% to 35.4% (mean<br />
32.2%, 571/1773 among SDCs and from 52.0% to 68.1<br />
% (mean 63.4%, 424/669) among ICs. Of the 571 screen<br />
detected ABCs, 106 (18.6%) were detected at the initial<br />
screen, respectively 266 (46.6%) and 88 (15.4%) were either<br />
not visible or showed a minimal sign at the previous screen<br />
and 111 (19.4%) had been missed at the previous screen.<br />
Advanced ICs were either not visible at the latest screen or<br />
showed a minimal sign in respectively 50.9% (216/424) and<br />
24.3% (103/424) of cases, whereas 25.1% (105/394) had<br />
been missed at screening.<br />
Conclusions: No decline in ABC was observed during 12<br />
years of biennial screening mammography. A majority of<br />
ABCs cannot be prevented through earlier breast cancer<br />
detection at screening.<br />
O8.10<br />
THE VALUE OF BLUE DYE FOR DETECTING<br />
THE SENTINEL LYMPH NODE IN BREAST<br />
CANCER PATIENTS IN ADDITION TO<br />
LYMPHOSCINTIGRAPHY<br />
M.A. Korteweg, J.D. van Amstel, M. Hobbelink,<br />
B.L. Stehouwer, M.A.A.J. van den Bosch, A.J. Witkamp,<br />
P.J. van Diest, W.P.Th.M. Mali, W.B. Veldhuis<br />
Universitair Medisch Centrum Utrecht, Utrecht<br />
Background: Sentinel lymph node biopsy (SLNB) is<br />
performed for axillary staging of breast cancer patients by<br />
blue dye injection, lymphoscintigraphy or combining both<br />
techniques. This study assesses the added value of blue dye<br />
for sentinel lymph node (SLN) detection in comparison to<br />
lymphoscintigraphy.<br />
Materials & methods: Patients with invasive breast<br />
cancer who underwent a SLNB following both lymphoscintigraphy<br />
(figure1) and blue dye injection between January<br />
2007 and August 2010, were included. The outcome was<br />
recorded. Sensitivity, specificity, positive and negative predictive<br />
value (PPV, NPV) were determined.<br />
Results: 256 SLNs were harvested of 151 patients who<br />
received 153 SLNB procedures. 68 (26%) nodes contained<br />
metastases. Lymphoscintigraphy was unsuccessful in 5 procedures<br />
(3%), of which in 1 case (1/5; 20%) blue dye detected<br />
the SLN (table1). The added overall value of blue dye is<br />
0.7% (1/153). Blue dye was unsuccessful in 55 procedures<br />
(36%), of which lymphoscintigraphy was successful in<br />
51 procedures (51/55; 93%). Of the 4 procedures both techniques<br />
failed, an axillary nodal dissection was performed<br />
in 3 cases and in 1 case the SLN was found by palpability.<br />
Sensitivity, specificity, PPV and NPV for blue dye and for<br />
lymphoscintigraphy were respectively 68%, 50%, 33%,<br />
81% and 97%, 12%, 40%, 92%. Combining both techniques<br />
resulted in values of 99%, 5%, 27% and 90%.<br />
Conclusion: Blue dye injection, as adjunct to lymphoscintigraphy<br />
resulted in 0.7% additional SLN detection. Blue<br />
dye detected the SLN in 20% of failed lymphoscintigraphy<br />
procedures. This implies that blue dye should only be used<br />
when lymphoscintigraphy is unsuccessful.<br />
60<br />
k i j k o o k o p w w w . c o n g r e s s c o m p a n y . c o m<br />
o f w w w . r a d i o l o g e n . n l
Mammadiagnostiek 2 8<br />
Figure 1: Anterior(A) and lateral(B) scintigraphic imaging in a 59-year old female patient with breast cancer, two hours after injection of technetium-99<br />
nanocolloid. The largest spot is the injection site of technetium-99-nanocolloid. The nannocolloid was injected peri-tumorally in the<br />
breast. The lateral image also depicts two axillary lymph nodes (arrows) which have taken up the nanocolloid. These nodes are sentinel lymph<br />
nodes as they are assumed to also be the first nodes to accumulate metastases.<br />
# Age Breast Cancer Type Metastatic Node Blue Node<br />
1 69 Ductal None No<br />
2 83 Lobular None No<br />
3 64 Mixed ductal-lobular Macro No<br />
4 73 Mixed ductal-lobular Macro No<br />
5 79 Ductal Macro Yes<br />
Table 1: Patient characteristics of the patients with an unsuccessful lymphoscintigraphy procedure: Patients 1-3 received an axillary lymph node<br />
dissection. Patient number 4 and 5 received a sentinel lymph node biopsy as in patient 4 the node was palpable and in patient 5 the sentinel node<br />
dyed blue.<br />
1 6 E R A D I O L O G E N D A G E N - 2 9 e n 3 0 S E P T E M B E R 2 0 1 1<br />
61
9 <strong>programma</strong> <strong>abstracts</strong> & <strong>abstracts</strong><br />
Sessie 9<br />
Neuro- en Hoofdhals radiologie<br />
Vrijdag 30 september, 10.45 - 12.15 uur<br />
O9.1<br />
ARTERIAL CALCIFICATION IN RELATION<br />
TO COGNITION AND STRUCTURAL BRAIN<br />
CHANGES<br />
D. Bos, M.W. Vernooij, S.E. Elias-Smale, G.P. Krestin,<br />
A. Hofman, W.J. Niessen, J.C.M. Witteman, A. van der Lugt,<br />
M.A. Ikram<br />
Erasmus Medisch Centrum, Rotterdam<br />
Purpose: Atherosclerosis plays an important role in the<br />
pathogenesis of cognitive decline and dementia. Calcified<br />
plaque measured with CT is a marker of atherosclerosis.<br />
This study investigates associations between CT-measured<br />
arterial calcifications measured at four locations, with cognition<br />
and macro- and microstructural brain changes.<br />
Method and materials: From the general population, 2437<br />
participants underwent CT of the coronary arteries, aortic<br />
arch, extracranial and intracranial carotid arteries to quantify<br />
calcification volume. Cognitive function was assessed in the<br />
following domains: memory, executive function, information<br />
processing speed and motor speed. In a random subgroup of<br />
844 participants brain MRI was performed to obtain measures<br />
of brain atrophy. Automated quantification of brain MRI<br />
scans yielded tissue-specific brain volumes. Furthermore,<br />
microstructural integrity of white matter was quantified<br />
using diffusion tensor imaging (DTI). Associations between<br />
arterial calcification and cognition, brain tissue volumes and<br />
DTI-measures were assessed with linear regression, adjusted<br />
for relevant confounders.<br />
Results: Larger calcification load was associated with<br />
worse cognitive scores in all domains. Calcification in all<br />
vessel beds was also associated with smaller total brain<br />
volume. Specifically, coronary calcification was associated<br />
with smaller grey matter volume, whilst both extra- and<br />
intracranial carotid artery calcification was associated with<br />
smaller white matter volume. Calcification in all vessel beds<br />
was associated with worse microstructural integrity of white<br />
matter.<br />
Conclusion: Arterial calcification load is associated with<br />
worse cognitive performance. Moreover, larger calcification<br />
load is associated with smaller brain tissue volumes and<br />
with worse white matter microstructural quality, elucidating<br />
possible mechanisms through which atherosclerosis leads to<br />
poorer cognition.<br />
O9.2<br />
TIA AND STROKE PATIENTS WITH CAROTID<br />
STENOSIS: PRESENCE OF COMPLICATED<br />
PLAQUE FEATURES AT MRI IS ASSOCIATED<br />
WITH RECURRENT EVENTS<br />
R.M. Kwee 1 , R.J. van Oostenbrugge 1 , W.H. Mess 1 ,<br />
M.H. Prins 1 , R.J. van der Geest 2 , J.W.M. ter Berg 3 ,<br />
C.L. Franke 4 , A.G.G.C. Korten 5 , B.J. Meems 6 ,<br />
J.M.A. van Engelshoven 1 , J.E. Wildberger 1 , M.E. Kooi 1<br />
1<br />
Maastricht Universitair Medisch Centrum, Maastricht<br />
2<br />
Leids Universitair Medisch Centrum, Leiden<br />
3<br />
Orbis Medisch Centrum, Sittard<br />
4<br />
Atrium Medisch Centrum Parkstad, Heerlen<br />
5<br />
Laurentius Ziekenhuis, Roermond<br />
6<br />
VieCuri Medisch Centrum, Venlo<br />
Purpose: There is a need for improved risk stratification of<br />
TIA and stroke patients with carotid atherosclerosis. The<br />
purpose of the present study was to prospectively investigate<br />
whether certain MRI-based carotid plaque characteristics<br />
are associated with recurrent ischemic events.<br />
Materials and Methods: One hundred TIA/stroke patients<br />
with ipsilateral 30-69% carotid stenosis underwent multisequence<br />
MRI, including contrast-enhanced images, of the<br />
carotid plaque within 32.7±19.9 days after the initial event.<br />
For each plaque, vessel wall volume and volumes of lipidrich<br />
necrotic core (LRNC), calcifications, and fibrous tissue<br />
were assessed. Maximum vessel wall thickness, minimum<br />
lumen area, fibrous cap status, and intraplaque hemorrhage<br />
(IPH) were also assessed. Patients were followed by structured<br />
interviews and chart review to determine the recurrence<br />
of ipsilateral TIA and/or ischemic stroke within one year.<br />
62<br />
k i j k o o k o p w w w . c o n g r e s s c o m p a n y . c o m<br />
o f w w w . r a d i o l o g e n . n l
Neuro- en Hoofdhals radiologie 9<br />
Results: Ten of hundred included patients suffered from<br />
recurrent ipsilateral clinical ischemic events (9 TIAs and 1<br />
ischemic stroke). The presence of IPH was associated with<br />
recurrence (Pearson Chi-Square= 7.373, P=0.007). Patients<br />
with recurrent events also had plaques with larger LRNC<br />
volume and larger maximum vessel wall thickness, although<br />
these findings were borderline significant (P=0.032 and<br />
P=0.055, respectively). Other MRI-based parameters were<br />
not related to recurrent ischemic events.<br />
Conclusion: The results of this study indicate that the<br />
presence of IPH, larger LRNC volume, and larger maximum<br />
vessel wall thickness of carotid plaques are associated with<br />
recurrent TIA and ischemic stroke. Assessment of carotid<br />
plaque characteristics by MRI may help identifying high-risk<br />
patients, which could improve patient selection for carotid<br />
endarterectomy or stenting.<br />
O9.3<br />
CAROTID PLAQUE MORPHOLOGY AND<br />
ISCHEMIC VASCULAR BRAIN DISEASE ON<br />
MRI<br />
Q.J.A. van den Bouwhuijsen, M.W. Vernooij, W.J. Niessen,<br />
G.P. Krestin, M.A. Ikram, J.C.M. Witteman, A. van der Lugt<br />
Erasmus Medisch Centrum, Rotterdam<br />
Purpose: Vulnerable plaque components in carotid arteries<br />
can be detected non-invasively with magnetic resonance<br />
imaging (MRI). In asymptomatic persons, the relation between<br />
carotid plaque composition and vascular brain disease<br />
is not well studied. We studied the association between<br />
carotid atherosclerotic plaque characteristics and ischemic<br />
brain disease on MRI.<br />
Methods: From the population-based Rotterdam Study, 952<br />
participants with carotid wall thickening on ultrasound >2.5<br />
mm underwent both carotid MRI and brain MRI. Maximum<br />
carotid wall thickening, degree of stenosis and presence of<br />
intraplaque hemorrhage, lipid core and calcification were<br />
assessed in both carotid arteries. Associations between<br />
plaque characteristics and white matter lesions (WMLs),<br />
lacunar and cortical infarcts were investigated per<br />
participant and additionally per carotid artery. Analysis were<br />
adjusted for cardiovascular risk factors.<br />
Results: Carotid stenosis (OR per 10% stenosis increase<br />
1.2 95% confidence interval (1.0-1.4), maximum carotid<br />
wall thickness (per mm increase 1.3,1.1-1.6) en presence of<br />
intraplaque hemorrhage (1.9,1.1-3.3), were all found to be<br />
significantly associated with presence of cortical infarcts,<br />
both in the participant based analysis and in the carotid<br />
artery based analysis. There were no associations between<br />
any plaque characteristics and presence of lacunar infarcts.<br />
In the subject based analysis maximum plaque thickness,<br />
presence of intraplaque hemorrhage and calcification were<br />
associated with WML-volume. In the artery based analysis<br />
only the association for calcifications remained.<br />
Conclusion: Presence of carotid intraplaque hemorrhage<br />
and measures of carotid plaque size are independently associated<br />
with cortical infarcts, but not with lacunar infarcts.<br />
Plaque calcification, but not vulnerable plaque components,<br />
is related to WML volume.<br />
Clinical relevance: This MRI study gives insight into the<br />
importance of atherosclerotic plaque composition, also in<br />
small plaques, for development of ischemic brain disease.<br />
O9.4<br />
A COMPUTER BASED DIAGNOSTIC<br />
SYSTEM TO FACILITATE THE EARLY AND<br />
DIFFERENTIAL DIAGNOSIS OF DEMENTIA<br />
B. Jasperse, H.A. Vrooman, M. Koek, M.W. Vernooij,<br />
R. de Boer, F. van der Lijn, M.A. Ikram, M. Smits,<br />
W. Niessen, A. van der Lugt<br />
Erasmus Medisch Centrum, Rotterdam<br />
Purpose: Patterns of brain atrophy, hippocampal atrophy and<br />
vascular changes, as visualized on brain-MRI, play an important<br />
role in determining the underlying cause of dementia<br />
syndromes. The visual interpretation of these pathological<br />
changes can be very challenging due to intercurrent agerelated<br />
brain changes.To facilitate the distinction between<br />
abnormal and ‘normal age-related’ brain changes, we<br />
developed an automated system that provides individualspecific<br />
lobar brain volumes, hippocampal volumes and white<br />
matter lesion volume taking into account age- and sex-specific<br />
reference data from a ‘healthy’ aging population.<br />
Methods and Materials: Automated brain tissue segmentation<br />
and atlas-based registration is performed on T1, T2<br />
and FLAIR MR-images, generating lobar brain volumes, hippocampal<br />
volumes and white matter lesion volume. For each<br />
resulting volume, reference curves are used to generate<br />
age- and sex-specific percentile values. The results are then<br />
presented in an on-line viewer to interpret the quality of tissue<br />
and structure segmentation and the quantitative results.<br />
Reference curves are generated from 867 healthy aging<br />
individuals (age-range (years): 61-91, Male/female-ratio (N):<br />
425/422).<br />
1 6 E R A D I O L O G E N D A G E N - 2 9 e n 3 0 S E P T E M B E R 2 0 1 1<br />
63
9<br />
<strong>programma</strong> <strong>abstracts</strong> & <strong>abstracts</strong><br />
Results/conclusion: An example of segmentation results<br />
and percentile plots (colored lines represent percentile-lines)<br />
for a 69 year old male patient with suspected dementia<br />
is provided in figure 1. Visual inspection suggests parietal<br />
atrophy, which might be attributed to global cortical atrophy.<br />
The automated analysis results show that overall brain<br />
volume is appropriate for age (75th to 95th percentile), with<br />
a strikingly low parietal lobe volume (37th percentile), confirming<br />
the initially suspected parietal lobe atrophy.<br />
A system prototype is currently under evaluation at our<br />
radiology department. Future work aims to incorporate<br />
automated analysis of microbleeds, shape of individual<br />
brain structures and microstructural integrity using diffusionweighted<br />
MRI sequences.<br />
Figure 1: Results for a patient with suspected dementia.<br />
O9.5<br />
MECHANICAL THROMBECTOMY WITH<br />
THE TREVO STENT DEVICE IN PROXIMAL<br />
INTRACRANIAL ARTERIAL OCCLUSIONS<br />
M.M.A.C. van Doorn 1 , R. van den Berg 1 , B. van der Kallen 2 ,<br />
G.J. Lycklama à Nijeholt 2 , W. van Zwam 3 , Y.B. Roos 1 , P.J.<br />
Nederkoorn 1 , M.E. Sprengers 1 , J. Bot 1 , J. Boiten 3 , R. van<br />
Oostenbrugge 3 , A. van der Lugt 4 , D. Beumer 4 , P.S. Fransen 4 ,<br />
D.W.J. Dippel 4 , C.B.L.M. Majoie 1<br />
1<br />
Academisch Medisch Centrum, Amsterdam<br />
2<br />
Medisch Centrum Haaglanden, Den Haag<br />
3<br />
Maastricht Universitair Medisch Centrum, Maastricht<br />
4<br />
Erasmus Medisch Centrum, Rotterdam<br />
Background and Purpose: To evaluate the safety and<br />
effectiveness of a self-expanding and fully retrievable stent<br />
(Trevo; Concentric Medical Inc, Mountain View, CA, USA) in<br />
revascularization of patients with acute ischemic stroke.<br />
Methods: Prospective multicenter case series of 22 patients<br />
with an acute ischemic stroke caused by a proximal intracranial<br />
arterial occlusion treated with a fully retrievable stent<br />
within the first 8 hours from symptom onset (median NIHSS<br />
21 [range 13-28]). Thrombectomy was used as rescue therapy<br />
in patients who were refractory to, had contraindications<br />
for or were to late for IV rtPA. The occlusion site was the<br />
middle cerebral artery in 7, terminus internal carotid artery<br />
in 2, cervical internal carotid artery/middle cerebral artery in<br />
4 and basilar artery in 9 patients. Complications related to<br />
the procedure and outcome at 3-6 months were assessed.<br />
Results: Stent placement was feasible in all procedures<br />
and successful recanalization defined as thrombosis in cerebral<br />
ischemia (TICI) grade 2b or 3 was achieved in 18 of 22<br />
treated vessels (82%). The mean number of passes for maximal<br />
recanalization was 2 (range 1-5). The median time from<br />
groin puncture to recanalization was 110 minutes (range<br />
26 – 199). One significant procedural event occurred (carotid<br />
artery occlusion after stent removal). 33% of all patients had<br />
a good outcome (mRS 0-2), 0% moderate outcome (mRS 3),<br />
67% poor outcome (mRS 4-6).<br />
Conclusions: These results suggest that with the Trevo<br />
device, clots can be safely and effectively removed from<br />
intracranial large vessel occlusions in acute ischemic stroke.<br />
64<br />
k i j k o o k o p w w w . c o n g r e s s c o m p a n y . c o m<br />
o f w w w . r a d i o l o g e n . n l
Neuro- en Hoofdhals radiologie 9<br />
O9.6<br />
RESTING-STATE FUNCTIONAL MRI CHANGES<br />
IN ALZHEIMER’S DISEASE AND MILD<br />
COGNITIVE IMPAIRMENT<br />
M.A.A. Binnewijzend 1 , M.M. Schoonheim 1 , E. Sanz-Arigita 2 ,<br />
A.M. Wink 1 , W.M. van der Flier 1 , N. Tolboom 1 ,<br />
J.S. Damoiseaux 3 , S.M. Adriaanse 1 , P. Scheltens 1 ,<br />
B.N.M. van Berckel 1 , F.A. Barkhof 1<br />
1<br />
VU medisch centrum, Amsterdam<br />
2<br />
Foundation CITA-AD, San Sebastian, Spain<br />
3<br />
Stanford University School of Medicine, Palo Alto, Cal, USA<br />
Alzheimer’s disease (AD) features distinct structural and functional<br />
brain changes. With the prospect of disease-modifying<br />
therapies it is desirable to detect signs of neurodegeneration<br />
before it is detectable on structural MRI as atrophy. In this<br />
study we used resting-state functional MRI (rs-fMRI) to<br />
compare regional functional connectivity of patients with AD,<br />
mild cognitive impairment (MCI) and healthy elderly controls<br />
(HC). MRI scans and neuropsychological assessments were<br />
acquired of 39 AD patients, 23 MCI patients and 43 HC. After<br />
a mean follow-up of 2.8±1.9 years seven MCI patients<br />
converted to AD, while 14 patients remained cognitively stable.<br />
Rs-fMRI scans were non-linearly registered to standard<br />
space and analyzed using independent component analysis<br />
(ICA), followed by a “dual-regression”technique to create<br />
and compare subject-specific maps of each spatio-temporal<br />
independent component, correcting for age, gender and additionally<br />
for gray matter atrophy. AD patients displayed decreased<br />
functional connectivity within the default-mode network<br />
(DMN) in the precuneus and posterior cingulate cortex compared<br />
to HC, which survived correction for gray matter atrophy.<br />
Within these regions, decreased functional connectivity was<br />
found in converting MCI as well, while no differences were<br />
found between stable MCI patients and HC. Correlation with<br />
cognitive dysfunctions demonstrated the clinical relevance of<br />
functional connectivity changes within the DMN. In conclusion,<br />
a clinically relevant decrease in functional connectivity<br />
was observed within the DMN in AD, independent of cortical<br />
atrophy. Similar decreases were present in MCI patients<br />
before conversion to AD. Rs-fMRI is a promising technique<br />
that can identify functional impairment in early AD.<br />
Figure 1: Differences in DMN FC between HC and AD patients.<br />
1 6 E R A D I O L O G E N D A G E N - 2 9 e n 3 0 S E P T E M B E R 2 0 1 1<br />
65
9 <strong>programma</strong> <strong>abstracts</strong> & <strong>abstracts</strong><br />
Figure 2: Boxplots of regional FC mean z-values.<br />
O9.7<br />
COMPUTER-AIDED DIAGNOSIS OF<br />
CORTICAL LESIONS IN EPILEPSY PATIENTS<br />
M.C. Hoeberigs 1 , L.M.H. Geelen 1 , P.A.M. Hofman 2<br />
1<br />
Maastricht Universitair Medisch Centrum, Maastricht<br />
2<br />
Kempenhaeghe Epilepsiecentrum, Heeze<br />
About 30% of epilepsy patients with partial seizures have<br />
intractable epilepsy. MRI detection of an epileptogenic lesion<br />
is of clinical importance because focal resection may be the<br />
only viable therapeutic option. In up to 74% of patients with<br />
partial seizures, MRI shows no abnormalities, although it is<br />
assumed that the majority of these patients have a small cortical<br />
dysplasia. In some of these cases the lesion is visible on<br />
the MRI study, but not detected by the neuroradiologist.<br />
We investigated the additional value of a computer-aided<br />
diagnostic technique, by retrospectively analyzing all scans<br />
from patients with partial seizures acquired between<br />
December 2008 and December 2009. The scan protocol on<br />
a 3T scanner included a 3D-T1 weighted scan, which was<br />
used for the post-processing. The other sequences were<br />
axial TSE-T2, FFE-T2 and FLAIR, coronal FLAIR and IR.<br />
MRI post-processing was a fully-automated voxel-based 3D<br />
MRI analysis within SPM5 (normalization, segmentation,<br />
results compared to normal database): feature maps of cortical<br />
thickness, gray-white junction and gray matter extension<br />
were generated. These maps were visually evaluated and<br />
correlated with the full exam. Only when the detected<br />
cortical lesion was also visible on the original scans it was<br />
considered a true cortical lesion.<br />
A total of 289 MRIs were evaluated. Based on visual<br />
assessment, a cortical lesion was described in 45/289. In<br />
28/45 positive scans and in 5 out of the initially negative<br />
244 patients a cortical lesion was detected by computeraided<br />
technique.<br />
Computer-aided postprocessing can increase the diagnostic<br />
yield, but not replace visual assessment.<br />
66<br />
k i j k o o k o p w w w . c o n g r e s s c o m p a n y . c o m<br />
o f w w w . r a d i o l o g e n . n l
Neuro- en Hoofdhals radiologie 9<br />
O9.8<br />
COMPLICATIONS OF PARTICLE<br />
EMBOLIZATION OF MENINGIOMAS:<br />
FREQUENCY, RISK FACTORS, AND<br />
OUTCOME<br />
D.F.M. Carli, M.S. Sluzewski, G.N. Beute, W.J.J. van Rooij<br />
St. Elisabeth Ziekenhuis, Tilburg<br />
Purpose: We assessed the frequency and outcome of<br />
complications of embolization of meningiomas and tried to<br />
identify risk factors.<br />
Methods: Between 1994 and 2009, a total of 198 patients<br />
with 201 meningiomas underwent embolization. Indication<br />
for embolization was preoperative in 165 meningiomas<br />
and adjunctive to radiosurgery in 8. In the remaining 28<br />
meningiomas, embolization was initially offered as a sole<br />
therapy. There were 128 women and 70 men with a mean<br />
age of 54.4 years (median age, 54 years; range, 15-90<br />
years). Complications were defined as any neurologic deficit<br />
or death that occurred during or after embolization. Logistic<br />
regression was used to identify the following possible risk<br />
factors: age above median, female sex, tumor size above<br />
median, meningioma location in 5 categories, use of small<br />
particle size (45-150 microm), the presence of major peritumoral<br />
edema, and arterial supply in 3 categories.<br />
Results: Complications occurred in 11 patients (5.6%; 95%<br />
confidence interval [CI], 3.0%-9.8%). Ten complications<br />
were hemorrhagic, and 1 was ischemic. Six of 10 patients<br />
with hemorrhagic complications underwent emergency<br />
surgery with removal of the hematoma and meningioma.<br />
Complications of embolization resulted in death in 2 and<br />
dependency in 5 patients (7/198, 3.5%; 95% CI, 1.6%-2.0%).<br />
The use of small particles (45-150 mum) was the only risk<br />
factor for complications (odds ratio [OR], 10.21; CI, 1.3-80.7;<br />
P = .028).<br />
Conclusions: In this series, particle embolization of meningiomas<br />
had a complication rate of 5.6%. We believe that<br />
the use of small polyvinyl alcohol (PVA) particles (45-150<br />
microm) should be discouraged.<br />
1 6 E R A D I O L O G E N D A G E N - 2 9 e n 3 0 S E P T E M B E R 2 0 1 1<br />
67
10<br />
<strong>programma</strong> <strong>abstracts</strong> & <strong>abstracts</strong><br />
Sessie 10<br />
MSK/Thorax/Diversen<br />
Vrijdag 30 september, 10.45 - 12.15 uur<br />
O10.1<br />
REPRODUCIBILITY OF 3D DELAYED<br />
GADOLINIUM ENHANCED MRI OF<br />
CARTILAGE OF THE KNEE AT 3.0 TESLA<br />
IN PATIENTS WITH EARLY-STAGE<br />
OSTEOARTHRITIS<br />
J. van Tiel, G. Kotek, H. Smit, E. Bron, S. Klein, G.P. Krestin,<br />
H. Weinans, E.H.G. Oei<br />
Erasmus Medisch Centrum, Rotterdam<br />
Purpose: To assess the reproducibility of 3D delayed<br />
Gadolinium Enhanced MRI of Cartilage (dGEMRIC) of the<br />
knee at 3.0Tesla in patients with early-stage osteoarthritis<br />
(OA).<br />
Methods: In three early-stage knee OA patients (Kellgren<br />
and Lawrence grade I or II) dGEMRIC was performed twice<br />
with an interval of seven days using a 3.0Tesla MRI-scanner<br />
and a custom-made open design knee coil. This coil was<br />
specifically developed to enable imaging of OA patients who<br />
would not fit in the commercially available knee coil. The<br />
new coil has a higher signal-to-noise ratio in the weightbearing<br />
cartilage compared to the regular knee<br />
coil. The dGEMRIC consisted of an Inversion Recovery Fast<br />
Spoiled Gradient Echo sequence with five different inversion<br />
times. Using Matlab, three regions of interest (ROIs) in the<br />
medial and lateral cartilage (weight-bearing condyle and<br />
plateau and non weight-bearing condyle) were drawn on<br />
three consecutive slices. Mean T1GD relaxation time per<br />
ROI per slice was calculated and compared between the<br />
two dGEMRIC scans using a paired t-test and an intraclass<br />
correlation coefficient (ICC) to assess reproducibility of the<br />
measurements.<br />
Results: In all ROIs of all slices mean T1GD relaxation<br />
time was not significantly different between the two<br />
examinations (p=0.1-0.5). The ICCs of mean T1GD relaxation<br />
times of all ROIs were good to excellent (ICC:0.64-<br />
0.99;p=0.004-0.0001).<br />
Conclusions: These preliminary results suggest that 3D<br />
dGEMRIC of the knee at 3.0Tesla is a reproducible measure<br />
of cartilage quality in early-stage OA patients. Therefore,<br />
it is a valuable tool to assess cartilage quality over time in<br />
longitudinal studies.<br />
Figure 1<br />
68<br />
k i j k o o k o p w w w . c o n g r e s s c o m p a n y . c o m<br />
o f w w w . r a d i o l o g e n . n l
MSK/Thorax/Diversen 10<br />
O10.2<br />
CT-ARTHROGRAPHY TO MEASURE<br />
CARTILAGE QUALITY: INFLUENCE OF<br />
SULPHATED GLYCOSAMINOGLYCAN<br />
CONTENT AND STRUCTURAL<br />
COMPOSITION OF EXTRACELLULAR<br />
MATRIX ON CONTRAST AGENT DIFFUSION<br />
INTO CARTILAGE<br />
J. van Tiel, M. Siebelt, J.H. Waarsing, M. van Straten,<br />
G.P. Krestin, H. Weinans, E.H.G. Oei<br />
Erasmus Medisch Centrum, Rotterdam<br />
Purpose: To assess the potential of CT-arthrography to<br />
evaluate cartilage quality in terms of sulphated glycosaminoglycan<br />
content (sGAG) and structural composition of the<br />
extra-cellular matrix (ECM).<br />
Methods: Eleven human cadaveric knee joints were<br />
scanned on a second generation dual source spiral CT scanner<br />
before and after intra-articular injection of a negatively<br />
charged contrast agent. Mean X-ray attenuation values of<br />
both scans were calculated in seven regions of interest<br />
(ROIs) of the cartilage (weight-bearing condyles and plateaus,<br />
non weight-bearing condyles and patella). Next, all<br />
ROIs were rescanned with contrast-enhanced<br />
micro-CT (μCT), which served as reference standard because<br />
it accurately measures sGAG content and hence quality<br />
of cartilage. Correlation between mean X-ray attenuation<br />
values of CT-arthrography and μCT was analyzed with linear<br />
regression. Additionally, residual values from the linear fit<br />
between unenhanced CT and μCT were used as a covariate<br />
measure to identify the influence of structural composition<br />
of cartilage ECM, i.e. without influence of sGAG, on contrast<br />
diffusion into cartilage.<br />
Results: Mean X-ray attenuation of cartilage was<br />
significantly higher for CT-arthrography compared to<br />
unenhanced CT in all ROIs. Furthermore, CT-arthrography<br />
attenuation values correlated excellently with reference<br />
μCT values representing sGAG content of cartilage<br />
(R=0.86;R2=0.73;p
10<strong>programma</strong> <strong>abstracts</strong> & <strong>abstracts</strong><br />
O10.3<br />
FRACTUREN VAN DE THORACALE EN<br />
LUMBALE WERVELKOLOM IN HET CENTRUM<br />
VOOR GERIATRISCHE TRAUMATOLOGIE:<br />
VASTSTELLEN VAN SCHADE AAN DE MIDDEL-<br />
STE PIJLER NIET VAN BELANG VOOR BELEID<br />
L.B.M. Weerink, M. Kraai, E.C. Folbert, R.S. Smit,<br />
J.H Hegeman, D. van der Velde<br />
Ziekenhuisgroep Twente, Almelo<br />
Over de behandeling van ouderen met een wervelfractuur<br />
door de middelste pijler is geen consensus. De relevantie<br />
van de CT-scan in de diagnostiek staat hiermee ook ter<br />
discussie. Doel van dit onderzoek is de meerwaarde van de<br />
CT-scan bij ouderen met een wervelfractuur te bepalen.<br />
Voor dit onderzoek werden 106 patiënten in het Centrum<br />
<strong>voor</strong> Geriatrische Traumatologie met een fractuur ter hoogte<br />
van de thocacolumbale wervelkolom geïncludeerd. Er werden<br />
retrospectief gegevens verzameld over radiologische<br />
parameters zoals betrokkenheid van de middelste pijler en<br />
diameter van het spinale kanaal. Algemene patiëntengegevens<br />
en gegevens over het functioneren na 6 weken en<br />
3 maanden werden geregistreerd.<br />
In onze populatie is er geen relatie is tussen betrokkenheid<br />
van de middelste pijler, compressie van het spinale kanaal<br />
en andere radiologische parameters met het functioneel<br />
eindresultaat.<br />
In tegenstelling tot de literatuur werd bij patiënten met een<br />
fractuur door <strong>voor</strong>ste en middelste pijler het beleid in 83,3%<br />
(45 patiënten) gewijzigd naar snelle mobilisatie. Het functioneel<br />
eindresultaat in beide groepen is vergelijkbaar.<br />
Conclusie: In onze studie hebben radiologische kenmerken<br />
van een wervelfractuur geen relatie met het functioneringsniveau<br />
na 6 weken en 3 maanden. De toepassing van snelle<br />
mobilisatie in plaats van strikte bedrust bij een fractuur met<br />
betrokkenheid van de middelste pijler is een veilige optie.<br />
Het vaststellen van de betrokkenheid van de middelste pijler<br />
door middel van een CT-scan lijkt met deze conclusies minder<br />
relevant <strong>voor</strong> het te volgen beleid. De rol van de CT-scan<br />
bij de diagnostiek van ouderen met een wervelfractuur staat<br />
hiermee ter discussie.<br />
O10.4<br />
IMPROVING DEPLOYMENT OF MR-SI IN<br />
PATIENTS SUSPECTED FOR SPONDYLO-<br />
ARTHRITIS IN A LARGE CLINICAL PRACTICE,<br />
USING A TARGETED INTERVENTION<br />
M.H.E. Vossen 1 , A.A. den Broeder 2 , F. Hendriks-Roelofs 2 ,<br />
D.M.F.M. van der Heijde 1 , M. Reijnierse 1<br />
1<br />
Leiden Universitair Medisch Centrum, Leiden<br />
2<br />
Sint Maartenskliniek, Nijmegen<br />
Background: Diagnosing axial spondyloarthritis (SpA) can<br />
be difficult: sacroiliac (SI) joint radiographs are often normal.<br />
Magnetic Resonance (MR) exam of SI joints (MR-SI) may<br />
reduce diagnostic uncertainty. Optimal deployment requires<br />
pretest chance of approximately 50%. Otherwise, increased<br />
numbers of MR-SI requests, false positives, excessive<br />
patient burden and costs will result.<br />
Objective: To examine characteristics of deployment of<br />
MR-SI in patients with suspected SpA before and after<br />
targeted intervention.<br />
An introduction on effect of pretest chance on predictive<br />
value, patient burden, costs was given. Alternative behavioral<br />
strategy was offered through a simple diagnostic<br />
algorithm.<br />
Results: 198 MR-SI (148 females / 50 males; mean age 36<br />
± 9.8yrs) were performed between April 1st, 2004 and April<br />
17th, 2007. 166 MR-SI (84%) were normal, 5 (2.5%) suspicious<br />
and 27 (13.5%) positive.<br />
After intervention, MR-SI number dropped to 58 (41 females<br />
/ 17 males; mean age 35. ± 9.8 years). Corrected for total<br />
number of patients seen (mean increase 12%), this is<br />
decrease of 79% with almost doubling of positive MR-SI: 44<br />
normal (76%), 0 suspicious and 14 (24%) positive.<br />
Conclusion: A simple, three stage feedback intervention<br />
resulted in 79% reduction of MR-SI requests with increase<br />
in number of positive MR-SI. This approach may benefit<br />
future research in areas with diagnostic uncertainty.<br />
Methods: MR-SI from April 1st, 2004 to December 31st,<br />
2010 were retrospectively collected. Inclusion criteria: MR-SI<br />
ordered by rheumatologist, suspicion of axial SpA, complete<br />
patient data. MR-SI reports were graded ‘normal’, ‘suspected<br />
sacroiliitis’ and ‘sacroiliitis’. Descriptive statistics were<br />
mean ± standard deviation (SD) or median (25-p75). In April<br />
2007, an intervention was done to improve deployment.<br />
Review data on requesting behavior, patient characteristics,<br />
outcomes were presented to rheumatologists.<br />
70<br />
k i j k o o k o p w w w . c o n g r e s s c o m p a n y . c o m<br />
o f w w w . r a d i o l o g e n . n l
MSK/Thorax/Diversen 10<br />
Figure 1: Diagnostic algorithm by Rudwaleit, M. et al.<br />
O10.5<br />
IMPACT ON DIAGNOSTIC PERFORMANCE<br />
AND READING TIME OF A COMPUTER<br />
AIDED DETECTION ALGORITHM FOR<br />
THE DETECTION OF ACUTE PE: SECOND<br />
READING VERSUS CONCURRENT READING<br />
R. Wittenberg 1 , J.F. Peters 2 , I.A.H. Van den Berk 3 ,<br />
N.J.M. Freling 3 , R.J. Lely 4 , B. de Hoop 5 , K. Horsthuis 3 ,<br />
C.J. Ravesloot 5 , M. Prokop 6 , C.M. Schaefer-Prokop 7<br />
1<br />
Universitair Medisch Centrum Utrecht, Utrecht<br />
2<br />
Philips Healthcare, Best<br />
3<br />
Academisch Medisch Centrum, Amsterdam<br />
4<br />
VU Medisch Centrum, Amsterdam<br />
5<br />
Universitair Medisch Centrum Utrecht, Utrecht<br />
6<br />
Universitair Medisch Centrum St Radboud, Nijmegen<br />
7<br />
Meander Medisch Centrum, Amersfoort<br />
Purpose: Evaluation of a CTPA study for the detection of<br />
pulmonary embolism (PE) represents a time consuming and<br />
tiring reading process. Computer-aided detection (CAD),<br />
when used as second reader, was found to improve reader<br />
performance for the detection of small emboli but inevitably<br />
at the expense of a substantial increase of reading time. We<br />
hypothesised that CAD may be used more advantageously<br />
when used as concurrent reading tool.<br />
Methods and materials: In this retrospective study, six<br />
observers of varying experience evaluated 157 negative and<br />
39 positive 64-slice consecutively acquired CTPA. With a<br />
time interval of 6 weeks, all cases were read twice in different<br />
order using CAD as second and as concurrent reader,<br />
respectively. Per patient, observers were asked to determine<br />
the presence of PE using a 5 point confidence scale and<br />
to document their reading time with and without CAD.<br />
Sensitivity and specificity were calculated by comparing the<br />
reader data with an independent consensus standard.<br />
Results: Baseline performance without CAD was high with<br />
a mean sensitivity of 91 % and increased further to 95 %<br />
with CAD as second reader and 94 % with CAD as concurrent<br />
reader. Mean specificity decreased with CAD as second<br />
reader (96%, 94 % and 96 %, respectively). The mean<br />
reading time with CAD as concurrent reader significantly<br />
decreased (108 s, 136 s and 91s, respectively).<br />
Conclusions: CAD used as concurrent reader has the<br />
potential to achieve the same high sensitivities without<br />
loss of specificity at the advantage of a significantly shorter<br />
reading time.<br />
1 6 E R A D I O L O G E N D A G E N - 2 9 e n 3 0 S E P T E M B E R 2 0 1 1<br />
71
10<strong>programma</strong> <strong>abstracts</strong> & <strong>abstracts</strong><br />
O10.6<br />
DEVELOPMENT AND VALIDATION OF<br />
A DIAGNOSTIC MODEL FOR AIRFLOW<br />
LIMITATION IN HEAVY SMOKERS BY USING<br />
QUANTITATIVE COMPUTED TOMOGRAPHY<br />
O.M. Mets 1 , C.M.F. Buckens 1 , P. Zanen 1 , I. Isgum 1 ,<br />
M. Prokop 2 , P.A. de Jong 1<br />
1<br />
Universitair Medisch Centrum Utrecht, Utrecht<br />
2<br />
Universitair Medisch Centrum St Radboud, Nijmegen<br />
Purpose: To develop a CT based diagnostic model for the<br />
presence of airflow limitation in smokers participating in a<br />
lung cancer screening study.<br />
Materials and methods: In 1173 screening participants,<br />
we analyzed inspiratory and expiratory chest computed<br />
tomography (CT) scans, patient characteristics, smoking history<br />
and prebronchodilator spirometry obtained at the same<br />
day as the CT scan. Scan parameters were: 120kVp (≤80kg)<br />
or 140kVp (>80kg) at 30mAs for inspiratory scans, and 90kVp<br />
(≤80kg) or 120kVp (>80kg) at 20mAs for expiratory scans.<br />
Axial slices of 1mm at 0.7mm increment were reconstructed.<br />
CT emphysema was defined as percentage of voxels
MSK/Thorax/Diversen 10<br />
O10.8<br />
ANALYSE RESULTATEN CYTOLOGISCH EN<br />
HISTOLOGISCHE PUNCTIES;CORRELATIE<br />
AAN PA-DIAGNOSE EN UITVOERDER<br />
Y.F.R. Ypma, J.J. Hensen, D. Vroegindeweij, H. van Beek,<br />
R.A Niezen, H. Beerman<br />
Maasstad Ziekenhuis, Rotterdam<br />
Doel: Evaluatie hoe frequent een CT, echografisch of stereotactisch<br />
geleide cytologische en histologische punctie<br />
resulteerde in een PA diagnose. Tevens werd het verschil<br />
in materiaal opbrengst tussen radioloog en arts-assistent<br />
geanalyseerd.<br />
Methode: Retrospectief werden alle cytologische en histologische<br />
puncties van 2009 en 2010 geincludeerd geanalyseerd.<br />
Het verschil tussen cytologische en histologische<br />
punctie werd geanalyseerd alsmede de methode hoe het PA<br />
materiaal werd verkregen en door wie de punctie werd verricht<br />
(radioloog versus assistent).<br />
Daarnaast werden alle puncties gecorreleerd aan de PA<br />
diagnose.<br />
Resultaten: In 2009 en 2010 werden 814 histologische<br />
biopten en 1260 cytologische puncties verricht.<br />
Radiologen verrichtten in deze periode 1056 puncties,<br />
waarvan 407 histologisch en 649 cytologisch. Assistenten<br />
verrichtten 1018 puncties, waarvan 407 histologisch en 611<br />
cytologisch.<br />
Van alle puncties (cytologisch en histologisch) waren er 67<br />
CT geleid, 1820 echogeleid en 175 stereotactisch.<br />
Cytologische puncties gaven in 88,5% (1116/1260) een<br />
PA diagnose en histologie in 95,3% (776/814). Van deze<br />
histologische biopten resulteerde het stereotactische biopt<br />
in de hoogste opbrengst, 96% (168/175), gevolgd door het<br />
echogeleide biopt, 95% (554/581). De laagste opbrengst gaf<br />
het CT geleide biopt, 93 % (62/67).<br />
Radiologen verkregen in 91,1% (962/1056) van de puncties<br />
representatief materiaal, assistenten in 91,3% (930/1018).<br />
Conclusie: Het stereotactisch geleide histologische biopt<br />
resulteerde in de hoogste PA score. Zowel cytologische<br />
puncties als histologische biopten resulteerden in vrijwel<br />
alle gevallen in een juiste PA diagnose. Er was geen significant<br />
verschil tussen de verschillende uitvoerders van de<br />
puncties.<br />
1 6 E R A D I O L O G E N D A G E N - 2 9 e n 3 0 S E P T E M B E R 2 0 1 1<br />
73
E <strong>programma</strong> <strong>abstracts</strong> & <strong>abstracts</strong><br />
Samenvattingen<br />
‘De educatieve <strong>voor</strong>dracht’<br />
Vrijdag 30 september, 10.45 - 12.15 uur<br />
E01<br />
DE VERGROTE BIJNIER:<br />
ENDOSONOGRAFISCHE FNA VAN DE<br />
INKER BIJNIER<br />
R.J.J. de Ridder 1 , V.C. Cappendijk 2<br />
1<br />
Maag-, darm-, leverziekten, Maastricht Universitair<br />
Medisch Centrum, Maastricht<br />
2<br />
<strong>Radiologie</strong>, Maastricht Universitair Medisch Centrum,<br />
Maastricht<br />
Incidentalomen van de bijnier worden door toenemend<br />
gebruik van beeldvormende technieken vaker gevonden.<br />
Driekwart van deze afwijkingen wordt gevonden bij personen<br />
welke beeldvorming ondergaan <strong>voor</strong> de stadiering van een<br />
maligniteit. Vaak kan door beeldvorming, eventueel aangevuld<br />
met endocrinologisch onderzoek, vastgesteld worden dat het<br />
om een (niet-functioneel) bijnieradenoom gaat. Bij twijfel over<br />
een primaire dan wel secundaire maligniteit, en indien relevant<br />
in de klinische context, is nader onderzoek aangewezen.<br />
Percutane CT- of echo geleide FNA van de bijnier heeft een<br />
sensitiviteit <strong>voor</strong> het aantonen van een maligniteit van 93%. In<br />
studies bedraagt het aantal niet diagnostische puncties echter<br />
19-24% [1,2] Belangrijke complicaties ontstaan in 3-8% van<br />
de patiënten aansluitend aan een percutane punctie.[3,4] De<br />
belangrijkste complicaties zijn pneumothorax, bloeding, hematoom<br />
en het risico op entmetastase.<br />
Referenties:<br />
1. Harisinghani MG, Maher MM, Pinkney PF et al. Predictive value<br />
of benign percutaneous adrenal biopsies in oncology patients.<br />
Clin Radiol 2002;57: 898-901<br />
2. Gilliams A, Roberts CM, Shaw P. et al. The value of CT scanning<br />
and percutaneous fine needle aspiration of adrenal masses in<br />
biopsy-proven lung cancer. Clin Radiol 1992;46: 18-22<br />
3. Mody MK, Kazerooni EA, Korobkin M et al. Pecutaneous CT-guided<br />
biopsy of adrenal masses: immediate and delayed complications.<br />
J Comput Assist Tomogr 1995;19:434-439<br />
4. Welch TJ, Sheedy PF, Stephens DH et al. Pecutaneous adrenal<br />
biopsy: review of 10-year experience. Radiology 1994;193:341-4<br />
5. Dietrich CF, WehrmannT, Hoffmann C et al, Detection of the<br />
adrenal gland by endoscopic or transabdominal ultrasound.<br />
Endoscopy 1997;29:859-864<br />
6. Schuurbiers OCJ, Tournoy KG, Schoppers et al. EUS-FNA for the<br />
detection of left adrenal metastasis in patients with lung cancer;<br />
Lung Cancer, in press<br />
7. DeWitt J, Alsatie M, LeBlanc J et al, Endoscopic ultrasoundguided<br />
fine-needle aspiration of left adrenal gland masses,<br />
Endoscopy 2007;39:65-71<br />
Transgastrische endosonografie (onder sedatie middels midazolam)<br />
is een beproefde methode <strong>voor</strong> afbeelding van met name<br />
de linker bijnier. De linker bijnier kan in 98% van de patiënten<br />
middels EUS in beeld worden gebracht, de rechter in 30% van<br />
de gevallen. Transabdomiale echo kan in 69% van de gevallen<br />
de linker bijnier visualiseren.[5]<br />
De sensitiviteit <strong>voor</strong> het aantonen van een maligniteit middels<br />
EUS met FNA bedraagt 86%. Niet diagnostische puncties<br />
variëren sterk tussen studies van 5.9-24%.[6,7] In de literatuur<br />
is slechts een casus van een post-procudurele bloeding<br />
beschreven na EUS-FNA.<br />
De procedure wordt door patiënten goed getolereerd en duurt<br />
ca. 10 minuten.<br />
EUS-FNA is een veilige en weinig belastende procedure <strong>voor</strong><br />
het verkrijgen van een weefsel diagnose indien er bij een vergrote<br />
linkerbijnier de verdenking bestaat op een maligniteit.<br />
74<br />
k i j k o o k o p w w w . c o n g r e s s c o m p a n y . c o m<br />
o f w w w . r a d i o l o g e n . n l
Educatieve <strong>abstracts</strong><br />
E<br />
E02<br />
LONG-TERM FOLLOW-UP FEATURES ON<br />
RECTAL MRI DURING A WAIT-AND-SEE<br />
APPROACH AFTER A CLINICAL COMPLETE<br />
RESPONSE IN RECTAL CANCER PATIENTS<br />
TREATED WITH CHEMORADIOTHERAPY<br />
D.M.J. Lambregts, M. Maas, F.C.H. Bakers, V.C. Cappendijk,<br />
G. Lammering, G.L. Beets, R.G.H. Beets-Tan<br />
Maastricht Universitair Medisch Centrum, Maastricht<br />
Background: Surgical resection is the standard treatment<br />
for patients with locally advanced rectal cancer who have<br />
undergone preoperative chemoradiation (CRT). There is now,<br />
however, a trend towards a conservative wait-and-see policy<br />
for patients with a complete tumor regression. It is not clear<br />
how patients should be monitored once they are managed<br />
non-operatively and whether follow-up by MRI has any role.<br />
As part of an observational study, a series of 19 carefully<br />
selected patients with a clinical complete response was<br />
managed with a wait-and-see policy and followed regularly<br />
by rectal MRI.<br />
Purpose: To study the short-term and long-term morphological<br />
MRI-features of rectal cancer patients with a complete<br />
tumor response undergoing a wait-and-see policy with regular<br />
MR follow-up after CRT.<br />
MR-imaging features: Shortly (6-8 weeks) after CRT,<br />
patients with a complete tumor response showed either<br />
a normalised rectal wall (26%) or a hypointense fibrotic<br />
remnant (74%). Three patterns of fibrosis could be classified,<br />
the aspects of which were dependent on the initial tumor<br />
morphology at primary MR staging (figure 1). The aspect of<br />
the normalised wall or fibrosis remained entirely consistent<br />
during long-term follow-up (median 20, range 9-57 months).<br />
During the first months after CRT, varying degrees of postradiation<br />
edema were observed in 26% of patients, which<br />
gradually disappeared during longer follow-up (figure 2).<br />
Conclusion: The morphological MR patterns observed in<br />
these patients may be used as a reference for the follow-up<br />
of rectal cancer patients with a complete tumor response<br />
after CRT, managed with a ‘wait and see policy’.<br />
Figure 1: Patterns of post-CRT fibrosis (d-f) and the corresponding types of primary tumors (a-c). Small polypoid tumors (a) typically resulted in<br />
a minimal fibrotic residue (d). Larger, bulky tumors (b) mostly resulted in a ’full thickness’ fibrosis (e). Spicular tumors (c) resulted in a similarly<br />
spicular fibrosis.<br />
Figure 2: Small primary tumor (a). Six weeks after CRT there is an edematous wall thickening (b), visible as a three layered rectal wall consisting<br />
of an inner mucosa (arrowhead), a hyperintense submucosa (*) and a hypointense outer muscular wall (arrow). During long-term follow-up<br />
the edema gradually decreases untill a normalised two-layered rectal wall (d) becomes visible.<br />
1 6 E R A D I O L O G E N D A G E N - 2 9 e n 3 0 S E P T E M B E R 2 0 1 1 75
e<br />
<strong>programma</strong> <strong>abstracts</strong> & <strong>abstracts</strong><br />
E03<br />
IMPLEMENTATIE VAN VIRTUELE<br />
COLONOSCOPIE IN DE DAGELIJKSE<br />
RADIOLOGISCHE PRAKTIJK<br />
M.T. de Witte 1,2 , P.C.G. Simons 1<br />
1<br />
VieCuri Medisch Centrum, Venlo<br />
2<br />
UMC St Radboud, Nijmegen<br />
Colorectaal carcinoom is 2 e kankergerelateerde doodsoorzaak<br />
in Nederland en de Westerse landen. De incidentie zal naar<br />
verwachting nog stijgen. De adenomateuze poliep wordt<br />
gezien als <strong>voor</strong>loper van het CRC, de zogenaamde “adenomacarcinoma<br />
sequence”. Het vroegtijdig opsporen en verwijderen<br />
van deze benige <strong>voor</strong>loper <strong>voor</strong>komt het uitgroeien tot CRC(1).<br />
Virtuele colonoscopie werd <strong>voor</strong> het eerst beschreven door<br />
David Vining in 1994 (2). Initieel gestart als 2D techniek,<br />
werd al snel ook de 3D “virtuele endoscopie” ontwikkeld.<br />
De segmentatie van darmsegmenten moest aanvankelijk<br />
handmatig gebeuren, een tijdrovende en arbeidsintensieve<br />
procedure. Inmiddels is Virtuele Colonoscopie volgroeid tot<br />
een volautomatische software tool met snelle segmentatie<br />
van darmsegmenten, panoramische weergave, automatische<br />
poliepdetectie (CAD), en elektronische cleansing.<br />
Officieel geaccepteerde indicaties <strong>voor</strong> Virtuele Colonoscopie<br />
zijn onvolledige optische coloscopie <strong>voor</strong> beoordeling van het<br />
proximale colon, verhoogd complicatie risico door hoge leeftijd<br />
en / of comorbiditeit en patientenweigering (3).<br />
In onze ervaring is deze techniek echter breder toepasbaar.<br />
Uit initieel onderzoek blijkt dat bij goede patientenselectie<br />
optische coloscopie in ruim 85% van de gevallen kan<br />
worden <strong>voor</strong>komen (4). Een recente en interessante ontwikkeling<br />
is korte termijn VC follow-up bij 1-2 kleine poliepen.<br />
Door de zeer accurate anatomische lokalisatie van afwijkingen<br />
middels VC blijkt deze techniek bij uitstek geschikt<br />
<strong>voor</strong> follow up van deze poliepen(5). Dit lijkt een geschikt<br />
alternatief <strong>voor</strong> de huidige richtlijnen waarbij excisie van<br />
poliepen ongeacht de grootte wordt geadviseerd (6). Nu<br />
besloten is om in Nederland vanaf 2012 een landelijk screenings<strong>programma</strong><br />
naar CRC middels i-FOBT op te starten, zal<br />
het aantal coloscopieen en dus ook het aantal onvolledige<br />
procedures toenemen. Hierdoor zal de vraag naar VC zeker<br />
toenemen. VC is een betrouwbare en robuuste techniek<br />
met een grote toekomst. Deze techniek dient dan ook geimplemeteerd<br />
te worden op elke radiologische afdeling.<br />
Referenties:<br />
1. J. Stoker. CT colografie en bevolkingsonderzoek <strong>voor</strong> colorectaal<br />
carcinoom. Memorad 13 (4), 2008; 13-18. <br />
2. DJ Vining, DW Gelfand, RE Bechtold et al. Technical feasibility of<br />
colon imaging with helical CT and virtual reality. AJR Am J Roentgenol<br />
1994; 162:Suppl: 104 abstract.<br />
3. EG MacFarland, JG Fletcher, PJ Pickhardt et al. ACR Colon Cancer<br />
Committee White Paper: Status of CT Colonography 2009. J Am<br />
Coll Radiol. 2009; 6: 756-772. <br />
4. CT-colografie als eerstelijnsdiagnosticum bij patienten met darmklachten.<br />
JS Peulen. MT de Witte, P Friederich et. al. Ned Tijdschr<br />
Geneeskd 2010; 154: A1681. <br />
5. The natural history of small polyps at CT colonography. PJ Pickhardt,<br />
DH kim et al. Annual meeting for the Soceity of Gastrointestinal<br />
Radiologsts 2008; Rancho Mirage, CA. <br />
6. Coloncarcinoom. Landelijke richtlijn versie 2.0, 09-01-08, Landelijke<br />
Werkgroep Gastro Intestinale Tumoren.<br />
E04<br />
FUTURE CLINICAL APPLICATIONS OF HIGH<br />
RESOLUTION ANATOMICAL IMAGING OF<br />
THE BRAIN AT 7.0 TESLA MRI<br />
A.G. van der Kolk, J.J.M. Zwanenburg, F. Visser, P.R. Luijten,<br />
J. Hendrikse<br />
Universitair Medisch Centrum Utrecht, Utrecht<br />
Purpose: To show the clinical potential of anatomically highly<br />
detailed images of the brain obtained with 7.0 Tesla MRI.<br />
Background: Although not widely used clinically, an<br />
increasing number of sites worldwide have the availability<br />
of an MRI scanner with a field strength of 7.0 Tesla. There is<br />
active debate if and when it may become the field strength<br />
of choice for certain clinical applications. Specifically,<br />
high resolution anatomical brain imaging at 7.0 Tesla with<br />
sequences such as FLAIR, T1- and T2*-weighted imaging<br />
and MR angiography may be the potential area where 7.0<br />
Tesla MRI provides additional diagnostic information not<br />
found on lower field strengths.<br />
Materials & Methods: Apart from a review of the current<br />
literature regarding anatomical brain MRI at 7.0 Tesla, the<br />
focus will be on clinical patient examples where 7.0 Tesla<br />
MRI gives additional diagnostic information or a better delineation<br />
of pathology than lower field strengths. Also, normal<br />
findings and anatomical variants not seen on 1.5 or 3.0 Tesla<br />
will be shown. When possible, comparison with 3.0 Tesla or<br />
1.5 Tesla MR images will be given (figure 1) to further illustrate<br />
the additional information which can be gained with<br />
7.0 Tesla scanning compared to lower field strength.<br />
Conclusion: High resolution anatomical brain imaging at<br />
7.0 Tesla MRI can give additional information about pathology<br />
and normal anatomical variations and will be able to<br />
contribute to faster and more accurate diagnosing.<br />
76<br />
k i j k o o k o p w w w . c o n g r e s s c o m p a n y . c o m<br />
o f w w w . r a d i o l o g e n . n l
Educatieve <strong>abstracts</strong><br />
e<br />
Figuur 1: White matter lesions at 1.5T as compared to 7.0T.<br />
E05<br />
IS BEELDVORMING VAN ATHEROSCLEROSE<br />
KLAAR VOOR DE DAGELIJKSE PRAKTIJK?<br />
S.C. Gerretsen 1 , V.C. Cappendijk 1 , R.M. Kwee 1 ,<br />
M.B.I. Lobbes 1 , M. Das 1 , T. Leiner 2 , J.M.A. van Engelshoven 1 ,<br />
M.E. Kooi 1 , J.E. Wildberger 1<br />
1<br />
Maastricht Universitair Medisch Centrum, Maastricht<br />
2<br />
Universitair Medisch Centrum Utrecht, Utrecht<br />
Doelstelling: Het bieden van een overzicht van de huidige<br />
mogelijkheden <strong>voor</strong> het detecteren en karakteriseren van<br />
atherosclerotische plaques.<br />
Beschrijving: In deze presentatie wordt een overzicht gegeven<br />
van de routine- en geavanceerde technieken die kunnen<br />
worden gebruikt <strong>voor</strong> beeldvorming van atherosclerose. Er<br />
wordt getoond hoe verschillende stadia van atherosclerose<br />
kunnen worden gedetecteerd, hoe stabiele atherosclerotische<br />
plaques van instabiele plaques onderscheiden kunnen worden<br />
en hoe plaques in symptomatische en asymptomatische<br />
patiënten kunnen verschillen. Tenslotte zal uitgelegd worden<br />
welke studies er nodig zijn om het afbeelden van een atherosclerotische<br />
plaques klinisch toepasbaar te maken.<br />
Conclusie: Niet-invasieve beeldvorming is geschikt <strong>voor</strong> de<br />
detectie en karakterisatie van atherosclerotische plaques.<br />
Deze presentatie beoogt de radioloog bewust te maken van<br />
het belang van detectie en rapportage van atherosclerose.<br />
Dit is een belangrijke stap om beeldvorming van atherosclerose<br />
klinisch toepasbaar te maken.<br />
Achtergrond: Atherosclerose is een chronische aandoening<br />
van de arteriële vaatwand die vaatvernauwingen en<br />
thrombo-emboliën kan veroorzaken hetgeen kan leiden tot<br />
een hersen- of hartinfarct. Ondanks <strong>voor</strong>uitgang in diagnostiek<br />
en behandeling blijft atherosclerose één van de belangrijkste<br />
doodsoorzaken in de westerse wereld. Geavanceerde<br />
technieken hebben aangetoond dat het mogelijk is om op<br />
niet-invasieve wijze de arteriële vaatwand af te beelden.<br />
Hierbij kunnen verschillende stadia van atherosclerose in<br />
beeld gebracht worden en zijn er verschillen waargenomen<br />
in plaques tussen symptomatische en asymptomatische personen.<br />
Echter ook op routine-onderzoeken is veel informatie<br />
over de aanwezigheid en mate van atherosclerose te verkrijgen.<br />
Gezien de mogelijke complicaties van atherosclerose is<br />
vroege detectie en rapportage van atherosclerose belangrijk.<br />
1 6 E R A D I O L O G E N D A G E N - 2 9 e n 3 0 S E P T E M B E R 2 0 1 1 77
e<br />
<strong>programma</strong> <strong>abstracts</strong> & <strong>abstracts</strong><br />
E06<br />
LUNG PERFUSION DEFECTS ON DUAL-<br />
ENERGY COMPUTED TOMOGRAPHY<br />
(DECT): REVIEW OF MORPHOLOGY AND<br />
DIFFERENTIAL DIAGNOSIS?<br />
A.E. Odink 1 , M. Rossius 1 , R. Booij 1 , C.M. Schaefer-Prokop 2 ,<br />
I.J.C. Hartmann 1<br />
1<br />
Erasmus Medisch Centrum, Rotterdam<br />
2<br />
Meander Medisch Centrum, Amersfoort<br />
Purpose: To present insight on the basic principles of DECT<br />
and provide a pictorial review of the range of morphology<br />
of lung perfusion with diagnostic clues for differentiating<br />
pulmonary embolism from other underlying diseases.<br />
Content organization: The classic presentation on a<br />
DECT perfusion map of acute pulmonary embolism (PE) is a<br />
peripheral, wedge shaped defect. However, other underlying<br />
parenchymal diseases such as emphysema, lung cysts, fibrosis<br />
or pneumonia also cause perfusion defects. Location,<br />
distribution and configuration of perfusion defects together<br />
with findings in lung window settings provide the necessary<br />
information for correct differential diagnosis. Also artifacts<br />
caused by beam hardening or pulsation cause perfusion<br />
inhomogeneities that occur in typical locations and are<br />
mostly easy to dismiss.<br />
The exhibit provides an overview of the spectrum of perfusion<br />
map findings to be encountered in a group of unselected<br />
patients undergoing evaluation for suspected PE and<br />
with known or unknown concomitant lung diseases. Typical<br />
and atypical perfusion defects caused by artifacts, focal or<br />
diffuse lung parenchymal diseases will be presented together<br />
with some guidelines for correct interpretation.<br />
Conclusion: Especially in an unselected group of patients<br />
with accompanying lung disease, knowledge of pitfalls and<br />
artifacts is important for correct interpretation of the spectrum<br />
of lung perfusion defects seen in DECT.<br />
E07<br />
VALUE OF COMPUTED TOMOGRAPHY<br />
CORONARY ANGIOGRAPHY IN<br />
FAILED CONVENTIONAL CORONARY<br />
ANGIOGRAPHY<br />
A.S. Thijssen 1 , R.N. de Visser 2 , G.F.A.J.B van Tilborg 2 ,<br />
A.C. Weustink 1 , G.P. Krestin 1 , N.R.A. Mollet 1<br />
1<br />
Erasmus Medisch Centrum, Rotterdam<br />
2<br />
St. Elisabeth Ziekenhuis, Tilburg<br />
Purpose/aim: If conventional X-ray coronary angiography<br />
(CCA) fails, computed tomography coronary angiography<br />
(CTCA) has the potential to provide the desired diagnostical<br />
information concerning coronary patency but may also<br />
demonstrate the cause of failing CCA exams.<br />
Content organization: CTCA has proved its usefulness in<br />
ruling out significant coronary artery stenosis in patients<br />
with an intermediate risk of having coronary artery disease.<br />
Although CCA is superior for this purpose, the exam cannot<br />
always be successfully completed.<br />
We will present a series of cases in which CCA could not be<br />
successfully completed and where CTCA revealed the cause<br />
of the failed exam. The presentation will feature several<br />
images from CTCA studies (multiplanar reformations and 3D<br />
renderings).<br />
Summary: Although CTCA is primarily reserved for patients<br />
with an intermediate risk of coronary artery disease, it can<br />
be employed to image the coronary tree in cases where CCA<br />
fails. In several instances, CTCA will reveal the cause of<br />
failed CCA. CTCA data may also provide useful information<br />
for planning interventional procedures or surgery in patients<br />
with a failed CCA exam.<br />
Figure 1 Figure 2 Figure 3<br />
78<br />
k i j k o o k o p w w w . c o n g r e s s c o m p a n y . c o m<br />
o f w w w . r a d i o l o g e n . n l
Educatieve <strong>abstracts</strong><br />
e<br />
E08<br />
PSEUDOTUMOREN BIJ METAAL OP METAAL<br />
TOTALE HEUP ARTROPLASTIEK<br />
M.F. Boomsma 1 , L. Sijbrandij 1 , B.H. Bosker 2 , H.B. Ettema 2 ,<br />
C.C.C.M. Verreyen 2 , B.J. Kollen 3 , M. Maas 4<br />
1<br />
<strong>Radiologie</strong>, Isala klieken, Zwolle<br />
2<br />
Orthopedie Isala klieken, Zwolle<br />
3<br />
Faculteit Medische wetenschappen, Universitair Medisch<br />
Centrum Groningen, Groningen<br />
4<br />
<strong>Radiologie</strong>, Academisch Medisch Centrum, Amsterdam<br />
Na het ondergaan van een totale heupartroplastiek is<br />
bekend dat er als complicatie pseudotumoren kunnen<br />
optreden. Recente vermoedens van verhoogde incidentie<br />
van klachten, gepaard gaande met pseudotumorvorming bij<br />
metaal op metaal totale heup artroplastiek (MoM THA), hebben<br />
geleid tot veel media-aandacht. Inmiddels zijn meerdere<br />
<strong>Nederlandse</strong> ziekenhuizen overgegaan tot het oproepen van<br />
patiënten die een MoM THA hebben ondergaan.<br />
In een recent uitgevoerd prospectief single center cohort<br />
studie is aangetoond dat de incidentie van pseudotumoren bij<br />
deze groep patiënten 36% is. Dit heeft inmiddels geleid tot<br />
revisie tot een polyethyleen acetabulum component van de<br />
MoM THA in 28% van de patiënten met een pseudotumor.[1]<br />
In deze presentatie zal de beeldvorming van de normale en<br />
postoperatieve heup in het kader van de THA worden besproken.<br />
Tevens wordt een overzicht gegeven van de verschillende<br />
uitingsvormen van pseudotumoren bij de MoM THA.<br />
Ervaringen van auteurs hebben geleid tot een “recall imaging”<br />
strategie, welke zal worden besproken. Een belangrijk<br />
item hieruit is het gebruik van CT bevindingen en de verhouding<br />
hiervan ten opzichte van een gangbare MR classificatie<br />
van pseudotumoren bij MoM THA patiënten.[2]<br />
Referenties:<br />
1. Risk assessment for pseudotumor after metal-on-metal largediameter<br />
femoral head total hip arthroplasty: a prospective cohort<br />
study. Bosker BH, Ettema HB, Boomsma MF, Kollen BJ, Wagemakers<br />
B and Verheyen CCPM. (Submitted)<br />
2. Grading the severity of soft tissue changes associated with metalon-metal<br />
hip replacements: reliability of an MR grading system.<br />
Anderson H, Toms AP Cahir JG, Goodwin RW, Wimhurst J and<br />
Nolan JF. Skeletal Radiol (2011) 40:303–307<br />
1 6 E R A D I O L O G E N D A G E N - 2 9 e n 3 0 S E P T E M B E R 2 0 1 1 79
P<br />
<strong>programma</strong> posterpresentaties & <strong>abstracts</strong><br />
Samenvattingen<br />
Posterpresentaties<br />
P01<br />
FOETALE POSTMORTEM<br />
RADIOLOGIE<br />
W.M. Klein, C. Marcelis, F. Vandenbussche<br />
Universitair Medisch Centrum St Radboud, Nijmegen<br />
Doel: verbetering radiologie congenitale afwijkingen bij<br />
overleden foetussen.<br />
Achtergrond: Met de komst van de 20-wekenecho neemt<br />
het aantal gevonden congenitale afwijkingen sterk toe, en<br />
hiermee ook het aantal zwangerschapsafbrekingen. Toch<br />
daalt het aantal autopsieen (gouden standaard). Postmortem<br />
MRI en CT kunnen, zonder het kind te beschadigen, aanvullende<br />
informatie geven.<br />
Discussie & conclusie: Postmortem foetale MRI en CT<br />
kunnen belangrijke bevestiging en additionele informatie.<br />
Dit is van grote waarde <strong>voor</strong> de verwerking door ouders en<br />
<strong>voor</strong> genetic counseling ten behoeve van volgende kinderen.<br />
Zeker bij een dalend aantal autopsieen is dit van groot<br />
belang.<br />
Een prospectieve studie in samenwerking met pathologie,<br />
radiologie, klinische genetica en gynaecologie zal de diagnostische<br />
waarde moeten aantonen.<br />
Techniek en casuistiek: Postmortem radiologische diagnostiek<br />
(
posterpresentaties<br />
P<br />
Figuur 2: Thanatofore dysplasie.<br />
Figuur 3: Tubureuze sclerose astrocytoom.<br />
P02<br />
AUTOMATED BREAST VOLUME SCANNER:<br />
3D-ULTRASOUND OF BREAST LESIONS<br />
T.A. Fassaert, M.D.F. de Jong, I.J.M. Dubelaar,<br />
M.C.J.M. Rutten<br />
Jeroen Bosch Ziekenhuis, ‘s-Hertogenbosch<br />
Purpose: Familiarize the reader with the imaging characteristics<br />
of benign and malignant findings in 3-dimensional<br />
breast ultrasound (3D-US) obtained with an automated<br />
breast volume scanner (ABVS). Emphasis is put on the<br />
added value of the new coronal plane (surgeon view) and<br />
the multiplanar correlation.<br />
Content: From a study of 200 consecutive patients, who<br />
underwent breast MRI and ABVS, we demonstrate 3D-US<br />
findings in a selection of illustrative cases with benign and<br />
malignant breast lesions. The illustrated cases are correlated<br />
with digital mammography, handheld 2D ultrasound,<br />
MRI and histopathological findings.<br />
Summary: ABVS provides high-resolution 3D-US images of<br />
breast lesions. The new coronal view and multiplanar correlation<br />
facilitate the sonographic assessment of benign and<br />
malignant breast lesions.<br />
Figuur 1: 3D-UScorrelation necrotic focus after RFA.<br />
1 6 E R A D I O L O G E N D A G E N - 2 9 e n 3 0 S E P T E M B E R 2 0 1 1<br />
81
P<br />
<strong>programma</strong> posterpresentaties & <strong>abstracts</strong><br />
Figuur 2: 3D-US correlation of lymph node & vascular bundle.<br />
Figuur 3: 3D-US correlation of a stellate lesion.<br />
82<br />
k i j k o o k o p w w w . c o n g r e s s c o m p a n y . c o m<br />
o f w w w . r a d i o l o g e n . n l
posterpresentaties<br />
P<br />
P03<br />
BRAIN PLASTICITY IN APHASIC PATIENTS<br />
AFTER MELODIC INTONATION THERAPY<br />
ASSESSED WITH FUNCTIONAL MAGNETIC<br />
RESONANCE IMAGING (FMRI)<br />
M.A.H. Bechan 1 , W.M.E. van de Sandt-Koenderman 2 ,<br />
C.P. Mendez 1 , E.G. Visch-Brink 1 , M. Smits 1<br />
1<br />
Erasmus Medisch Centrum, Rotterdam<br />
2<br />
Rijndam revalidatiecentrum, Rotterdam<br />
Purpose: Certain aphasic patients are treated with Melodic<br />
Intonation Therapy (MIT), which uses musical elements of<br />
speech to initiate language production. The purpose of this<br />
study is to visualize neuronal reorganizational processes in<br />
the brain in response to MIT using fMRI.<br />
Methods and materials: Four patients with chronic and<br />
two with acute aphasia (22-67 years; 4 males; 5 righthanded)<br />
were scanned at 3T before and after six weeks of<br />
MIT, which consisted of naming, repeating and spontaneous<br />
speech. To visualize language processing a block design<br />
task, consisting of listening to stories versus reverse speech,<br />
was used. Language performance was measured using the<br />
Sabadel story telling task. Imaging data were analyzed<br />
using Statistical Parametric Mapping 8 (London, UK). After<br />
preprocessing individual statistical t-contrast maps were<br />
calculated for pre- and post-therapy datasets. Lateralization<br />
indices (LI) were calculated using the number of significantly<br />
(p
P<br />
<strong>programma</strong> posterpresentaties & <strong>abstracts</strong><br />
P04<br />
DESMOID-TYPE FIBROMATOSIS:<br />
A COMPREHENSIVE REVIEW OF<br />
MULTIMODALITY IMAGING FINDINGS<br />
IN PRIMARY, RECURRENT AND<br />
DEDIFFERENTIATED DISEASE WITH<br />
HISTOPATHOLOGIC CORRELATION<br />
I.J.M. Dubelaar 1 , U. Flucke 2 , J. Bonenkamp 2 , M. Prokop 2 ,<br />
J.W.J. de Rooy 2<br />
1<br />
Jeroen Bosch Ziekenhuis, ‘s-Hertogenbosch<br />
2<br />
Universitair Medisch Centrum St Radboud, Nijmegen<br />
Summary: Desmoid-type fibromatoses are rare, locally<br />
aggressive, non-metastazing soft tissue tumors with high<br />
tendency towards local recurrence.<br />
This exhibition will review:<br />
1. the various types and the multimodality imaging features<br />
of primary, recurrent and dedifferentiated disease with<br />
histopathological correlation<br />
2. The role of imaging in the management of these types of<br />
soft tissue tumors<br />
3. Current treatment options<br />
Content organization:<br />
1. Desmoid-type fibromatosis review; - epidemiology, aetiology,<br />
localization and clinical features of different types<br />
- multimodality imaging features of primary, recurrent/<br />
dedifferentiated disease and post- therapy changes<br />
2. Histopathologic morphology and genetics<br />
3. Treatment options: - local excision - radiotherapy -<br />
systemic therapy<br />
P05<br />
REPEATED PHASE-CONTRAST MAGNETIC<br />
RESONANCE ANGIOGRAPHY TO ASSESS<br />
CEREBROVASCULAR REACTIVITY IN<br />
PATIENTS WITH CAROTID ARTERY STENOSIS<br />
N.S. Hartkamp, J. Hendrikse, H.B. van der Worp,<br />
G.J. de Borst, R.P.H. Bokkers<br />
Universitair Medisch Centrum Utrecht, Utrecht<br />
Purpose: To assess the cerebrovascular reactivity in<br />
patients with internal carotid artery (ICA) stenosis and<br />
identify the optimal timing for reactivity measurements with<br />
acetazolamide as vasodilatory challenge medication.<br />
Methods: Twenty-one patients with a symptomatic ICA<br />
stenosis and 18 healthy control subjects underwent twodimensional<br />
phase-contrast magnetic resonance angiography<br />
to repeatedly measure the blood flow (ml/min) in the<br />
ICAs at baseline and in 5 minute intervals for 30 minutes<br />
after intravenous administration of 12 gram acetazolamide<br />
per kilogram body weight.<br />
Results: The blood flow during the exam was significantly<br />
lower in the stenosed ICA of patients (figure 1, indicated<br />
with the star) than in the contralateral ICA (light gray)<br />
and than in the ICAs of healthy controls (white). The<br />
absolute increase of blood flow after 15 minutes was as<br />
well significantly lower in the stenosed ICA than in the<br />
contralateral ICA and than in the healthy ICAs (respectively<br />
74.6±12, 122±18, and 137±15 ml/min), whereas the relative<br />
increase was not (respectively 46.9±6.7%, 56.0±9.4%, and<br />
58.2±7.2%). The vasodilatory effect in the stenosed ICAs<br />
Figure 1: Blood flow after acetazolamide administration.<br />
Figure 2: Time to peak after acetazolamide<br />
administration.<br />
84<br />
k i j k o o k o p w w w . c o n g r e s s c o m p a n y . c o m<br />
o f w w w . r a d i o l o g e n . n l
posterpresentaties<br />
P<br />
was maximal after 15 minutes (figure 2, indicated with the<br />
star) and decreased after 20 minutes (figure 1), which was<br />
significantly later than in the contralateral ICA (light gray)<br />
and healthy ICAs (white).<br />
Conclusion: Patients with ICA stenosis have a reduced<br />
absolute increase in blood flow with preserved relative<br />
increase after a vasodilatory challenge with acetazolamide.<br />
The time to maximum vasodilatation was also longer in<br />
the stenosed ICA of patients. The optimal timing for single<br />
reactivity measurements using acetazolamide is between 15<br />
to 20 minutes after administration.<br />
P06<br />
MIXED CEREBRAL PERFUSION TERRITORIES<br />
IN THE POSTERIOR CIRCULATION<br />
INVESTIGATED USING SUPER-SELECTIVE<br />
ARTERIAL SPIN LABELING MRI<br />
N.S. Hartkamp 1 , M. Helle 2 , R.P.H. Bokkers 1 , J. Hendrikse 1 ,<br />
M.J.P. Van Osch 3<br />
1<br />
Universitair Medisch Centrum Utrecht, Utrecht<br />
2<br />
Institute of Neuroradiology, Christian-Albrechts-Universität,<br />
Kiel, Germany<br />
3<br />
Leiden Universitair Medisch Centrum, Leiden<br />
Purpose: The posterior circulation is supplied with blood by<br />
the vertebral arteries (VA) that fuse into the basilar artery<br />
(BA). We aim to investigate to which extent blood mixes in<br />
the BA before it arrives in cerebral hemispheres.<br />
Methods: Five healthy volunteers were investigated on a 3T<br />
MRI scanner with super-selective pseudo-continuous arterial<br />
spin labeling (ASL) perfusion imaging, which allows separate<br />
labeling of the VAs. The contribution to the perfusion<br />
of each individual VAs was calculated for the left and right<br />
hemisphere of the cerebellum and cerebrum.<br />
Results: The relative amount of ASL-signal from each VA<br />
to either hemisphere of the cerebellum and cerebrum are<br />
summarized in table 1. The posterior circulation of subject 1<br />
was almost exclusively supplied by one VA due to a variant<br />
anatomy. The perfusion images of both the left and right VA<br />
from subject 5 shown in figure 1. Examination of the perfusion<br />
images reveals areas in the cerebellum exclusively supplied<br />
by either the left or the right VA (also shown in figure<br />
1). The perfusion images show increasing overlap in the<br />
cerebrum. Both in the cerebellum and in the cerebrum most<br />
of the ASL-signal is observed ipsilateral from the labeled<br />
VA, although significant signal is also observed contralaterally,<br />
especially in the cerebrum.<br />
Conclusion: The results show that although most ASLsignal<br />
in the posterior flow territory originates from the<br />
ipsilateral VA, a considerable amount of ASL-signal stems<br />
from the contralateral VA, indicating mixing of blood or at<br />
least exchange of magnetization between blood streams in<br />
the BA. Mixing in the BA however does not produce a completely<br />
homogeneous blood supply to the cerebral posterior<br />
circulation in our subjects.<br />
Figure 1: Perfusion images of the left and right VA.<br />
Table 1: Relative contributions of the left and right VA.<br />
1 6 E R A D I O L O G E N D A G E N - 2 9 e n 3 0 S E P T E M B E R 2 0 1 1<br />
85
P<br />
<strong>programma</strong> posterpresentaties & <strong>abstracts</strong><br />
P07<br />
MALFORMATIE VAN DE VENE<br />
VAN GALENI<br />
I.J.M. Dubelaar 1 , F.A. Meijer 2<br />
1<br />
Jeroen Bosch Ziekenhuis, ‘s-Hertogenbosch<br />
2<br />
Universitair Medisch Centrum St Radboud, Nijmegen<br />
Purpose: To inform the reader of the rare congenital<br />
aneurysmal malformation of the vein of Galen. To illustrate<br />
the appearance, therapy options and various outcome in a<br />
pictorial review.<br />
Content organization: Aneurysmal malformation of the<br />
vein of Galen is a rare congenital vascular malformation,<br />
resulting in developmental delay, congestive heart failure,<br />
hydrocephalus, brain damage and/or death in childhood.<br />
In a pictorial review, we illustrate the best outcome<br />
(spontaneous thrombosis), the worst outcome (melting<br />
brain) and therapy options (endovascular embolization).<br />
Pathophysiology, clinical presentation and therapy options<br />
will be briefly discussed.<br />
Summary: Vein of Galen malformation and resulting<br />
aneurysm is a rare, often fatal congenital disorder. Various<br />
outcome is illustrated and therapy options discussed.<br />
P08<br />
SUBSEQUENT ISCHEMIC STROKE IN<br />
VASCULAR TERRITORIES AFFECTED BY<br />
INTRACRANIAL ARTERIAL STENOSIS IN<br />
PATIENTS WITH TRANSIENT ISCHEMIC<br />
ATTACK AND ISCHEMIC STROKE<br />
P.J. Homburg, M.J. van Gils, G.J.J. Plas, H.L.J. Tanghe,<br />
D.W.J. Dippel, A. van der Lugt<br />
Erasmus Medisch Centrum, Rotterdam<br />
Background and purpose: Compared to extracranial carotid<br />
artery atherosclerosis, intracranial arterial stenosis (ICAS)<br />
has received little attention as a cause of cortical ischemic<br />
stroke. We evaluated the stroke recurrence risk of ICAS per<br />
arterial territory in a large cohort of patients with a transient<br />
ischemic attack (TIA) or ischemic stroke.<br />
Methods: Consecutive patients (n=786) were prospectively<br />
evaluated for the presence and distribution of ICAS (≥30%<br />
stenosis) using CT angiography. Multivariable Cox<br />
proportional hazards models were used to identify risk<br />
factors associated with subsequent ischemic stroke and to<br />
analyze the stroke recurrence risk for ICAS per territory (left<br />
carotid territory, right carotid territory and posterior territory).<br />
Results: In 178/786 patients (23%), 288 ICAS were<br />
observed. Subsequent ischemic stroke occurred in 49<br />
patients (6%), of which 15/49 (31%) occurred in a territory<br />
affected by ICAS. After adjustment for age, sex, hypertension,<br />
diabetes mellitus and extracranial artery stenosis ≥50%,<br />
ischemic stroke risks in territories affected by ICAS were HR<br />
4.34 (95%CI 1.36-13.87) for the left carotid territory, HR 8.09<br />
(95%CI 2.53-25.92) for the right carotid territory and HR 6.94<br />
(95%CI 1.93-25.04) for the posterior territory.<br />
Conclusions: Ischemic stroke and TIA patients with ICAS<br />
have a particularly high risk of subsequent ischemic stroke<br />
in the affected arterial territory. This finding warrants more<br />
research in the pathophysiology of ICAS and modified treatment<br />
for patients with ICAS.<br />
P09<br />
PROSPECTIVE QUALITATIVE COMPARISON<br />
OF 4D RADIAL ACQUISITION CONTRAST-<br />
ENHANCED MR ANGIOGRAPHY VERSUS<br />
DIGITAL SUBTRACTION ANGIOGRAPHY<br />
IN CHARACTERIZING INTRACRANIAL<br />
ARTERIOVENOUS MALFORMATIONS<br />
M. van der Vlies 1, 2 , R. van den Berg 1 , C.B.L.M. Majoie 1<br />
1<br />
Academisch Medisch Centrum, Amsterdam<br />
2<br />
Onze Lieve Vrouwe Gasthuis, Amsterdam<br />
Introduction: Digital subtraction angiography (DSA) is<br />
the gold-standard procedure for diagnosis and follow-up<br />
of cerebral AVM because of its high temporal and spatial<br />
resolution. However, alternative time-resolved techniques<br />
such as TRICKS (GE Healthcare), TWIST (Siemens) and 4D<br />
TRAK (Philips Healthcare) are now widely available<br />
to allow dynamic MR imaging for the appreciation of<br />
contrast kinetics. We hypothesized that in agreement with<br />
other studies, 4D radial acquisition contrast enhanced<br />
MRA (4D rCE-MRA) compared to DSA, approximates<br />
vascular architecture and flow dynamics of AVMs, furthermore<br />
implying a reduction in risk exposure and in<br />
procedural risks.<br />
Methods: A total of 21 consecutive patients were assessed<br />
prospectively, 7 had AVM, 7 had AV-fistula and 2 had a DVA.<br />
4D rCE-MRA and DSA were performed. The 4D rCE-MRA<br />
images were assessed regarding vascular architecture and<br />
dynamic flow characteristics.<br />
Results: 4D rCE-MRA correctly depicted location, nidal<br />
size, venous drainage pattern and prominent arterial feeders<br />
in almost all cases of AVMs and AV-fistulas. There<br />
86<br />
k i j k o o k o p w w w . c o n g r e s s c o m p a n y . c o m<br />
o f w w w . r a d i o l o g e n . n l
posterpresentaties<br />
P<br />
was good agreement (approximately 90%) between DSA<br />
and 4D rCE-MRA images.<br />
Conclusion: 4D rCE-MRA is a good alternative imaging<br />
modality tool approximating the imaging gold standard of<br />
DSA and furthermore proving to be a reliable minimal invasive<br />
imaging tool that avoids the risks associated with DSA.<br />
Figure 1: 4D MRA arterial phase.<br />
Figure 2: 4D MRA venous phase.<br />
Figure 3: 4D MRA late venous phase, showing cerebellar AVM.<br />
P10<br />
RADIOFREQUENTE ABLATIE VAN OUDERE<br />
PATIENTEN MET T1 MAMMACARCINOOM<br />
DIE NIET IN AANMERKING KOMEN VOOR<br />
CHIRURGIE<br />
M.D.F. de Jong, M.J.C.M. Rutten, D. Kreb, B.G. Looij,<br />
K. Bosscha, M. Ernst, H. van der Linden, G.J. Jager<br />
Jeroen Bosch Ziekenhuis, ‘s-Hertogenbosch<br />
Doel: Radiofrequente ablatie (RFA) kan een alternatieve en<br />
effectieve behandeling vormen bij patiënten met T1 borstkanker,<br />
welke niet geschikt zijn <strong>voor</strong> chirurgisch ingrijpen.<br />
Doel is te bepalen of RFA technisch haalbaar en veilig is<br />
en of lokale tumorcontrole verkregen kan worden. Daarbij<br />
wordt geëvalueerd hoe de behandeling door patiënten wordt<br />
ervaren.<br />
Methode: Patiënten >70 jaar met een oestrogeen positief<br />
mammacarcinoom < 2 cm worden gevraagd deel te nemen<br />
aan deze studie. De respons na de aanvullende RFA therapie<br />
(naast hormonale therapie) zal geëvalueerd worden, middels<br />
mammografie, echografie en MRI na 1, 6 en 12 maanden.<br />
Tevens zal een echogeleid vacuümbiopt volgen van het<br />
RFA-gebied <strong>voor</strong> histologische analyse volgen na een jaar.<br />
1 6 E R A D I O L O G E N D A G E N - 2 9 e n 3 0 S E P T E M B E R 2 0 1 1<br />
87
P<br />
<strong>programma</strong> posterpresentaties & <strong>abstracts</strong><br />
Ervaringen van patiënten <strong>voor</strong>, tijdens en na de behandeling<br />
worden geëvalueerd.<br />
Resultaten: In totaal hebben vijf patiënten RFA ondergaan,<br />
waarbij er geen aanwijzingen waren op lokaal recidief<br />
of residu weefsel na een jaar follow-up. De geableerde<br />
gebieden vertoonden afname van grootte en ringaankleuring<br />
gedurende follow-up. Bij één patiënte is interval follow-up<br />
niet verricht in verband met een CVA. Patiënten vonden<br />
RFA-behandeling verdraagbaar en er was afname van één<br />
punt op een zeven puntsschaal ter analyse van de kwaliteit<br />
van leven.<br />
Conclusie: RFA kan technisch veilig worden uitgevoerd bij<br />
inoperabele, oudere patiënten met een solitaire borsttumor,<br />
met minimale afname op de kwaliteit van leven.<br />
Figuur 1: bewezen maligne laesie linker mamma.<br />
Figuur 2: controle na 1 maand toont ringaankleuring.<br />
Figuur 3: na 1 jaar afname aankleuring, geen recidief.<br />
88<br />
k i j k o o k o p w w w . c o n g r e s s c o m p a n y . c o m<br />
o f w w w . r a d i o l o g e n . n l
posterpresentaties<br />
P<br />
P12<br />
PROPOSAL FOR AN ADAPTATION OF THE<br />
BERLIN ALGORITHM FOR DIAGNOSING<br />
SPA: RESULTS OF THE SPONDYLOARTHRITIS<br />
CAUGHT EARLY (SPACE)-COHORT<br />
R. van den Berg, M.H.E. Vossen, M. Reijnierse,<br />
T.W.J. Huizinga, D.M.F.M. van der Heijde<br />
Leids Universitair Medisch Centrum, Leiden<br />
Background: The Berlin algorithm assists clinicians in diagnosing<br />
early axial SpA.<br />
Objectives: Validate the Berlin algorithm in the<br />
SPondyloArthritis Caught Early (SPACE)-cohort.<br />
Methods: The SPACE-cohort is set-up in our hospital to<br />
early diagnose and treat (axial) spondyloarthritis (SpA)-<br />
patients. Patients with back pain (>3 months, < 2 years;<br />
onset 80% probability. In patients<br />
(n=65) not diagnosed with axial SpA, 14 (21.5%) patients<br />
fulfilled ASAS axial SpA criteria and 7 (10.8%) had >80%<br />
probability; the majority did not have IBP.<br />
The modified Berlin algorithm, with IBP as additional SpAfeature,<br />
resulted in three entry groups; requirement of ≥4,<br />
2-3, and 0-1 SpA-features. According to this modified algorithm,<br />
57 patients (50%) has axial SpA; 45 (78.9%) fulfilled<br />
ASAS axial SpA criteria and 55 (96.5%) had >80% probability.<br />
Of the 57 patients not diagnosed as SpA, six (10.5%)<br />
fulfilled ASAS axial SpA criteria. 15 additional patients<br />
could now be diagnosed as axial SpA by the modified Berlin<br />
algorithm and no single patient with a probability >80% was<br />
excluded.<br />
Conclusions: We propose a slightly modified Berlin algorithm<br />
excluding IBP as entry criterion that is better in accordance<br />
with the new ASAS axial SpA criteria.<br />
Results: In 4/114 patients no MRI was made and were analyzed<br />
as MRI-. According to the Berlin algorithm 49 patients<br />
Figure 1: The Berlin algorithm.<br />
1 6 E R A D I O L O G E N D A G E N - 2 9 e n 3 0 S E P T E M B E R 2 0 1 1<br />
89
P<br />
<strong>programma</strong> posterpresentaties & <strong>abstracts</strong><br />
Figure 2: The modified Berlin algorithm.<br />
P13<br />
DIFFERENCE IN CLINICAL PRESENTATION OF<br />
PATIENTS WITH SPONDYLOARTHRITIS WITH<br />
A POSITIVE MRI OF THE SI JOINTS AND/OR<br />
HLA-B27 POSITIVITY<br />
R. van den Berg, M.H.E. Vossen, M. Reijnierse,<br />
T.W.J. Huizinga, D.M.F.M. van der Heijde<br />
Leids Universitair Medisch Centrum, Leiden<br />
Background: The SPondyloArthritis Caught Early (SPACE)-<br />
cohort is set-up in our hospital to early diagnose and treat<br />
(axial) spondyloarthritis (SpA)-patients. The new ASAS axial<br />
and peripheral SpA criteria rely on the presence of active<br />
sacroiliitis on MRI and on HLA-B27 positivity.<br />
Objective: Investigate the difference in presentation of<br />
patients with sacroiliitis vs. non-sacroiliitis on MRI and presence<br />
vs. absence of HLA-B27.<br />
Methods: Patients with back pain (>3 months, < 2 years;<br />
onset
posterpresentaties<br />
P<br />
Table 1: Presence and distribution of SpA-features.<br />
P14<br />
FEASIBILITY OF FUNCTIONAL IMAGING,<br />
INCLUDING DYNAMIC CONSTRAST-<br />
ENHANCED MRI AND PERFUSION CT,<br />
FOR POST-CHEMORADIOTHERAPEUTIC<br />
RESTAGING IN RECTAL CANCER PATIENTS<br />
S.J. Klieverik, E. Kluza, M. Maas, R.G.H. Beets-Tan, G. Beets,<br />
D.M.J. Lambregts<br />
Maastricht Universitair Medisch Centrum, Maastricht<br />
Aim: The aim of this study was to perform a review of the<br />
literature to determine whether 1) the current literature<br />
reports correlations between functional imaging and clinicopathological<br />
markers in rectal cancer patients and 2) if<br />
functional imaging is sensitive to chemoradiotherapy (CRT)-<br />
induced changes in rectal cancer.<br />
Methods: The literature of interest was searched using<br />
Pubmed. Studies were included when correlations between<br />
functional and clinicopathological markers and differences<br />
in functional parameters between pre- and post-CRT were<br />
reported.<br />
Results: Five studies used dynamic constrast-enhanced MRI<br />
(DCE-MRI) and two studies used perfusion CT (p-CT) to<br />
investigate the correlation between functional and clinicopathological<br />
markers. Two studies compared functional parameters<br />
from DCE-MRI in CRT responders vs. non-responders.<br />
Studies correlating DCE-MRI parameters with clinicopathological<br />
markers showed that higher endothelial transfer<br />
coefficient (Ktrans) and perfusion index (PI; a measure of<br />
both perfusion and cappilary permeability surface product)<br />
were significantly correlated with more advanced cancer<br />
stages (e.g. TNM stage) and that these functional parameters<br />
were significantly higher before treatment in patients<br />
with a good response to CRT than in non-responders. Two<br />
studies evaluated the correlation between p-CT parameters<br />
and clinicopathological parameters. Results showed that<br />
significantly higher blood volume, blood flow and mean<br />
transit time were found in groups with poor prognosis (e.g.<br />
high MVD, existence of lympathic metastasis). There were<br />
no studies comparing p-CT parameter in a pre vs. post-CRT<br />
setting.<br />
Conclusion: The reviewed literature shows that functional<br />
imaging parameters, especially Ktrans in DCE-MRI and<br />
BV and BF in p-CT, correlate with clinical and pathological<br />
markers. Therefore, both DCE-MRI and p-CT are of great<br />
potentional as non-invasive therapy-monitoring or therapypredicting<br />
methods in rectal cancer.<br />
1 6 E R A D I O L O G E N D A G E N - 2 9 e n 3 0 S E P T E M B E R 2 0 1 1<br />
91
<strong>programma</strong> aantekeningen & <strong>abstracts</strong><br />
92<br />
k i j k o o k o p w w w . c o n g r e s s c o m p a n y . c o m<br />
o f w w w . r a d i o l o g e n . n l
16 E RADIOLOGENDAGEN 2011<br />
1 6 E R A D I O L O G E N D A G E N - 2 9 e n 3 0 S E P T E M B E R 2 0 1 1<br />
93
<strong>programma</strong> PLATTEGRONDEn & <strong>abstracts</strong><br />
0-niveau<br />
0.4 0.5<br />
Brussels<br />
Paris<br />
Naar Expo Foyer<br />
Copenhagen<br />
0.3<br />
Lobby<br />
0.6<br />
0.7<br />
0.2<br />
0.9 0.8<br />
Berlin<br />
Athens<br />
Rome<br />
0.1<br />
London<br />
Naar hotel<br />
K1<br />
K2<br />
K3<br />
0.14 0.12<br />
0.13<br />
0.11<br />
94<br />
k i j k o o k o p w w w . c o n g r e s s c o m p a n y . c o m<br />
o f w w w . r a d i o l o g e n . n l
16 E RADIOLOGENDAGEN 2011<br />
1-niveau<br />
Forum Passage<br />
Registratiebalie<br />
Trajectum<br />
Entree<br />
Naar hotel<br />
Expo Foyer<br />
Auditorium 1<br />
Slide preview ><br />
1.3<br />
1.2<br />
Podium<br />
Auditorium 2<br />
1 6 E R A D I O L O G E N D A G E N - 2 9 e n 3 0 S E P T E M B E R 2 0 1 1<br />
95
<strong>programma</strong> PLATTEGRONDen En <strong>programma</strong> & <strong>abstracts</strong><br />
2-niveau<br />
2.7 2.8 2.9 2.10<br />
Promenade<br />
2.11<br />
2.12<br />
2.13<br />
2.6<br />
2.5<br />
Auditorium 1<br />
2.14<br />
2.4<br />
2.3<br />
Podium<br />
2.1<br />
Colorado<br />
Auditorium 2<br />
96<br />
k i j k o o k o p w w w . c o n g r e s s c o m p a n y . c o m<br />
o f w w w . r a d i o l o g e n . n l
Donderdag 29 september 2011<br />
Expofoyer Auditorium 2 Zaal 0.2 Berlin Zaal 0.3 Copenhagen Zaal 0.4 Brussels Zaal 0.5 Paris Zaal 0.8 Rome Zaal 0.9 Athens Zaal 2.1 Colorado<br />
10.00 - 10.45 Ontvangst<br />
10.45 - 12.00 Plenaire sessie: Emeritus <strong>programma</strong><br />
Deze misser maak je (start vanaf 11.20 uur)<br />
maar één keer<br />
12.00 - 13.00 Lunch<br />
12.15 - 12.45 Postersessie<br />
13.00 - 14.00 Plenaire sessie:<br />
Setting standards in<br />
healthcare -<br />
many ways, no return<br />
14.05 - 15.35 Research corner Vervolg Parallelsessie: Parallelsessie: Parallelsessie: Parallelsessie: Parallelsessie:<br />
Emeritus <strong>programma</strong> Interventieradiologie / Cardiovasculaire Abdominale radiologie / Mammadiagnostiek 1 Abdominale<br />
Cardiovasculaire radiologie radiologie Acute radiologie / Diversen radiologie 1<br />
15.35 - 16.00 Theepauze<br />
16.00 - 17.15 Refresher course: Workshop: Vervolg Refresher course: refresher course: Refresher course: refresher course:<br />
Respons monitoring “Interpretatie van radiologisch Emeritus <strong>programma</strong> Chronische thrombo- Neuranatomie Beeldvorming bij groei- What is the best imaging<br />
made sexy wetenschappelijk onderzoek” embolische pulmonale <strong>voor</strong> dummies en puberteitsstoornissen modality for “aseptic/low<br />
hypertensie grade infection/infectious<br />
loosening of joint prostheses?”<br />
17.15 - 17.30 Uitreiking WSS penning<br />
17.30 - 18.45 ALV NVvR & Juniorsectie<br />
18.15 Industrieborrel:<br />
excl. aangeboden door<br />
Vrijdag 30 september 2011<br />
Expofoyer Auditorium 2 Zaal 0.1 London Zaal 0.2 Berlin Zaal 0.4 Brussels Zaal 0.5 Paris Zaal 0.8 Rome Zaal 0.9 Athens Zaal 2.1 Colorado<br />
08.30 - 09.00 Ontvangst<br />
09.00 - 10.15 Workshop/hands-on: Workshop: refresher course: refresher course: Refresher course: refresher course: refresher course:<br />
To make Radlex more familiar. “Interpretatie van Buiktrauma, waar gaat Acute pijn op de borst: De knie: Niet standaard Opleiden anno 2011 Veneuze<br />
Using IHE TCE for radiologisch het nou eigenlijk om Stand van zaken MRI bevindingen en interventies<br />
export of PACS data to wetenschappelijk de postoperatieve knie<br />
an MIRC teaching file onderzoek”<br />
10.15 - 10.45 Koffiepauze<br />
10.45 - 12.15 Parallelsessie: Parallelsessie: Parallelsessie: Parallelsessie: Parallelsessie: Parallelsessie:<br />
De educatieve Abdominale Mammadiagnostiek 2 Kinderradiologie / MSK / Thorax / Neuro-Hoofdhals<br />
<strong>voor</strong>dracht radiologie 2 & Uitreiking Diversen Diversen radiologie<br />
Jan Hendriksprijs<br />
12.15 - 13.15 Lunch<br />
12.30 - 13.00 Postersessie<br />
13.15 - 13.30 Wetenschappelijk beleid<br />
NVvR <strong>voor</strong> academischeen<br />
niet academische centra<br />
13.30 - 14.30 Plenaire sessie:<br />
Pro-con: Setting standards in<br />
healthcare - which way to go?<br />
14.30 - 15.15 Richtlijnen sessie<br />
15.15 - 15.45 Theepauze<br />
15.45 - 16.25 Prijsuitreiking:<br />
Philipsprijs, Posterprijs,<br />
Radiologendagenprijs,<br />
NVvR Travel Grant en<br />
Fellowshipdiploma’s<br />
16.25 - 17.15 Quiz<br />
Vanaf 20.00 Diner & galafeest in Amrâth Grand Hotel De L’Empereur, Maastricht<br />
Het uitgebreide <strong>programma</strong> en de leerdoelen vindt<br />
u <strong>voor</strong>aan in dit <strong>programma</strong>- en abstractboek:<br />
Donderdag 29 september 2011: bladzijde 2 t/m 5<br />
Vrijdag 30 september 2011: bladzijde 5 t/m 7
Hoofdsponsoren radiologendagen 2011<br />
sponsoren en exposanten<br />
Agfa HealthCare<br />
Alliance Medical<br />
Bard Benelux<br />
Bayer Schering Pharma<br />
Biomedic<br />
Bracco Imaging Europe<br />
Covidien Nederland<br />
Esaote Pie Medical<br />
GE Healthcare<br />
Guerbet Nederland<br />
Haga Medical<br />
Helsebemanning<br />
Medtronic Nederland<br />
Melius Pro<br />
Oldelft Benelux<br />
Radiomatix<br />
Toshiba Medical Systems Nederland<br />
Tromp Medical<br />
Vrest Medical