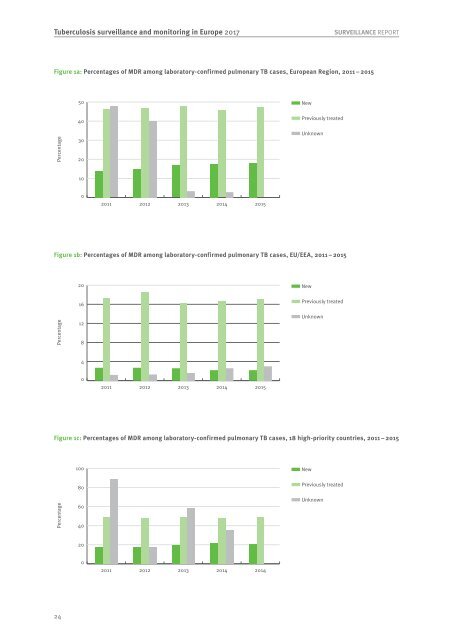
Tuberculosis surveillance and monitoring in Europe 2017 SURVEILLANCE REPORT Figure 1a: Percentages of MDR among laboratory-confirmed pulmonary TB cases, European Region, 2011 – 2015 50 New Percentage 40 30 20 Previously treated Unknown 10 0 2011 2012 2013 2014 2015 Figure 1b: Percentages of MDR among laboratory-confirmed pulmonary TB cases, EU/EEA, 2011 – 2015 20 New Percentage 16 12 8 Previously treated Unknown 4 0 2011 2012 2013 2014 2015 Figure 1c: Percentages of MDR among laboratory-confirmed pulmonary TB cases, 18 high-priority countries, 2011 – 2015 100 New Percentage 80 60 40 Previously treated Unknown 20 0 2011 2012 2013 2014 2014 24
SURVEILLANCE REPORT Tuberculosis surveillance and monitoring in Europe 2017 1b). In the non-EU/EEA area, three countries had an MDR TB prevalence ranging from 10–19% among new cases tested for first-line DST: Armenia (14.6%), Azerbaijan (15.9%) and Georgia (11.6%). Five countries had 20–29% MDR TB among new cases: Kazakhstan (24.0%), Kyrgyzstan (25.0%), Russia (26.7%), Tajikistan (24.2%) and Ukraine (20.9%). In Belarus, Moldova and Uzbekistan the percentage of confirmed MDR TB cases was 35.8%, 31.1% and 44.6% respectively, however the quality of data reported from Uzbekistan limits interpretation, due to selective DST as a result of capacity limitations. The percentage of confirmed MDR TB cases among 32 652 previously-treated TB cases whose isolates were tested for first-line DST was 47.4 %, which is comparable to the 2014 rate (46.2%) (Fig 1a). Fifteen countries had between 15% and 49% MDR TB among previously-treated TB cases tested for first line DST. In eight countries this rate was even higher: Armenia (87.0%), Moldova (71.9%), Belarus (68.4%), Albania (66.7%), Russia (59.1%), Kyrgyzstan (56.3%), Uzbekistan (56.2%) and Estonia (51.4%) (Table 12). However, it should be noted that in Albania this involved only four cases in absolute numbers. In 2015, the per capita rate of MDR TB notification among new TB cases at Regional level was 2.0 per 100 000. This represents an average annual increase of 11% between 2011 and 2015 (Table V). Trends in the MDR percentage among new TB cases and trends in the per capita notification rate of MDR TB among new cases have differed significantly by country in recent years (Table V). The proportion of MDR among new pulmonary TB cases tested for drug resistance decreased slightly in the EU/EEA sub-region over the last five years, from 2.7 to 2.2%, and the per capita rate of notified MDR TB cases remained stable at around 0.1 case per 100 000 population. Meanwhile, in the non-EU/EEA countries the MDR percentages among new cases increased from 18.3% in 2011 to 22.9% in 2015. At the same time, despite an impressive decline in incident TB cases per capita, the notification rate for MDR TB increased from 3.0 to 3.9 per 100 000 population, suggesting that the replacement of susceptible TB strains with resistant strains is becoming more common in the Region. The Regional trend is influenced by an increase in the MDR notification rate experienced by Azerbaijan, Belarus, Moldova, Russia, Tajikistan, Ukraine and Uzbekistan. In a few settings (Armenia, Georgia, Lithuania) the MDR rate has levelled off, while Estonia and Latvia serve as clear examples of countries that have reversed the trend in rising epidemics of MDR TB. In central Asian countries the prevalence and rate of MDR TB fluctuates widely from year to year, indicating weakness in routine drug-resistance surveillance. In 2015, a total of 43 countries reported on second-line DST data, however all 43 together only accounted for 33% of notified MDR TB cases (Table 14). Of the 9 165 MDR TB cases subjected to second-line DST, 2 149 (23.4%) were XDR TB, which represents an increase of five percentage points on the previous year. This rapid change at Regional level is related to the fact that Ukraine began reporting SLD data to the global TB database for the first time, together with a sharp increase in the XDR TB notification rate in Belarus from 29.3% in 2014 to 35.5% in 2015. In EU/EEA countries, where 76.7% of MDR TB cases were tested for second-line drugs, the prevalence of XDR among MDR cases was 19.7%, which is comparable to the result for 2014. Among the countries reporting at least 30 MDR cases with secondline DST results, or at least 70% of SLD testing coverage, seven countries reported over 20% XDR prevalence among MDR TB cases: Belarus (35.5%), Latvia (25.4%), Ukraine (24.9%), Lithuania (24.5%), Estonia (24.3%), Romania (22.6%) and United Kingdom (22.2%). Of the 42 826 MDR TB patients notified, 41 188 (96.2%) were enrolled into MDR TB treatment programmes. Six high-priority countries reported a gap of over 5% between the number of patients enrolled and the number diagnosed: Azerbaijan (70.6%), Turkey (75.7%), Ukraine (89.1%), Moldova (90.7%), Estonia (92.1%), and Tajikistan (93.0%) (Table 15). Compared to the previous year, access to XDR TB treatment had increased significantly among the reporting countries, with an overall XDR TB treatment coverage of 98.6% at Regional level, compared to 66.0% in 2014. TB/HIV co-infection A total of 39 countries provided surveillance data on TB/HIV co-infection (Table 16). In the reporting countries, of the 206 096 new and relapse TB patients notified 181 995 were screened for HIV (88.3%). Ten high-priority countries achieved a testing level above 90%: Armenia, Azerbaijan, Belarus, Estonia, Kazakhstan, Kyrgyzstan, Moldova, Russia, Tajikistan and Ukraine. A total of 16 380 TB cases were detected with HIV-positive status and 9.0 % of those tested. This is higher than the 8.2% with HIV-positive status recorded in 2014, indicating that the absolute number of TB/HIV cases continues to increase in the Region, as it has done annually at an average of 13.1% since 2011. The Regional trend is influenced by a sharp increase in TB/HIV co-infection in the countries of eastern Europe, Russia and central Asia, although in EU/EEA countries the TB/HIV co-infection rate is decreasing. Among those countries reporting representative HIV testing (above 50% HIV testing coverage), five documented a significant overlap of the HIV and TB epidemics by exceeding 10% HIV prevalence among new and re-treatment TB cases (Table 16): Ukraine (22.3%), Latvia (16.5%), Malta (15.4%), Portugal (14.3%) and Estonia (11.6%). Ten countries had 5–10% HIV prevalence among TB patients: Russia (9.8%), Armenia (9.1%), Moldova (8.7%), the Netherlands (7.4%), Belgium (7.2), and Greece (7.1%), Uzbekistan and Spain (6.4% each), Belarus (5.5%) and Israel (5.0%). In 2015, 22 countries in the Region provided information on anti-retroviral therapy (ART) enrolment among TB cases with HIV-positive status. Of 9 320 HIV-positive tuberculosis cases, 5 818 (62.4%) had received ART. This is somewhat higher than in 2014 (59.1%), but far below the WHO target of universal ART coverage. Among the high-priority countries there were only eight that achieved coverage of over 75%: Armenia, Azerbaijan, Belarus, Estonia, Georgia, Kyrgyzstan, Romania and Turkey. 25