Emerson Hospital
1U3T81d
1U3T81d
Create successful ePaper yourself
Turn your PDF publications into a flip-book with our unique Google optimized e-Paper software.
he recalls. “He answered every one of them<br />
and didn’t rush me. I like Dr. Schloss very<br />
much; he is very friendly and has a sincere,<br />
caring manner.”<br />
When it comes to prostate cancer, there is<br />
plenty to cover. “The side effects of treatment,<br />
such as imperfect urinary control and<br />
erectile dysfunction, are a big part of the<br />
discussion,” says Dr. Schloss. “Most men<br />
need reassurance.”<br />
Treatment designed to prevent a<br />
recurrence<br />
Dr. Schloss performed Mr. Walsh’s surgery<br />
the following week, after which he spent<br />
three days at <strong>Emerson</strong>. “The nurses were<br />
outstanding,” he says. “I wrote a letter describing<br />
how impressed I was.” Although<br />
he was weak and couldn’t lift anything, he<br />
slowly returned to the legal work that was<br />
waiting for him.<br />
Six weeks after his surgery, Mr. Walsh had<br />
a repeat PSA test and saw Dr. Schloss for a<br />
follow-up appointment. “I expected to hear<br />
that everything was fine, and I was done<br />
with treatment,” he says. “Instead, Dr.<br />
Schloss told me that my PSA was still high,<br />
and I needed to have radiation.”<br />
director of radiation oncology, and the staff<br />
are committed to delivering treatment with a<br />
high degree of precision. “When we treat<br />
prostate cancer, we regularly perform imaging<br />
to assure that everything is aligned,” Dr.<br />
McGrath explains. “For example, even the<br />
presence of fluid in the bladder will affect<br />
the precision of where we aim the radiation.<br />
We make regular adjustments in order to<br />
treat the patient with the utmost precision.”<br />
Mr. Walsh’s physicians conferred regularly<br />
on his treatment plan. Midway through his<br />
radiation therapy, Dr. Schloss and Dr.<br />
McGrath decided that adding a testosteronelowering<br />
medication would be prudent.<br />
“We don’t want Jim to develop a recurrence<br />
of prostate cancer,” notes Dr. Schloss.<br />
With Dr. Schloss, Dr. McGrath and Jon<br />
DuBois, MD, medical director of the Mass<br />
General Cancer Center at <strong>Emerson</strong> <strong>Hospital</strong>-<br />
Bethke, collaborating on his care, Mr. Walsh<br />
knew he was in good hands. He will continue<br />
to see all three physicians periodically.<br />
Dr. DuBois attends the urologic oncology<br />
conferences at Mass General, where patients<br />
are discussed. “The conference allows me<br />
to build relationships with urologists and<br />
radiation oncologists at MGH, which makes<br />
consultations and referrals with our<br />
<strong>Emerson</strong> patients more streamlined and<br />
rewarding,” says Dr. DuBois.<br />
Much progress has occurred in the treatment<br />
of prostate cancer: during the past 30 years,<br />
five-year survival has increased from 73<br />
percent to 99 percent. “With respect to<br />
advanced or metastatic cancer, the last few<br />
years have seen the FDA approval of more<br />
treatments than ever,” says Dr. DuBois.<br />
“They include molecular therapies and<br />
vaccine technology.”<br />
Dr. DuBois also helps lead the twicemonthly<br />
multidisciplinary oncology conference<br />
at <strong>Emerson</strong> with Dr. McGrath, Dr.<br />
Schloss and other specialists in attendance.<br />
They review newly diagnosed patients together<br />
and determine the best course of<br />
management.<br />
By November 2014, with treatment well<br />
behind him, Mr. Walsh’s PSA was down to<br />
normal. He is grateful—for the expertise<br />
that was available nearby and the outstanding,<br />
personalized care he received. “When<br />
I look back, it was a better experience than I<br />
could have imagined,” he says. “I wouldn’t<br />
have gone anywhere else.”<br />
Dr. Schloss says he considered all the<br />
factors. “The pathology report after Jim’s<br />
surgery showed that the tumor was locally<br />
advanced, meaning that the surgery did not<br />
remove every cancer cell. His high PSA<br />
level convinced me that having a course of<br />
radiation was necessary.”<br />
“I’m not a ‘woe is me’ guy,” Mr. Walsh says.<br />
“But I got emotional when I heard that I<br />
needed more treatment.” He managed to<br />
schedule himself for the first treatment of<br />
the day and began the six weeks of radiation<br />
at <strong>Emerson</strong>.<br />
Mr. Walsh quickly became attached to the<br />
radiation oncology staff, who made him feel<br />
comfortable and cared for. “They’re my<br />
friends now, including Dr. McGrath,” he<br />
says. “They’re wonderful people, and<br />
they are doing God’s work. I still stop in<br />
to visit them.”<br />
In addition to providing personalized care<br />
and attention, John McGrath, MD, medical<br />
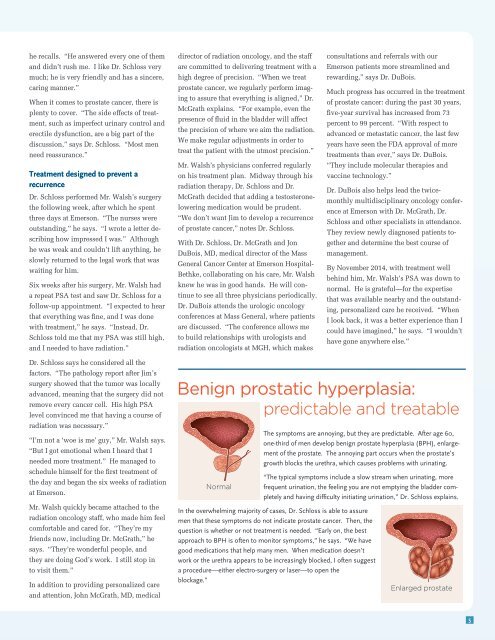
Benign prostatic hyperplasia:<br />
predictable and treatable<br />
Normal<br />
The symptoms are annoying, but they are predictable. After age 60,<br />
one-third of men develop benign prostate hyperplasia (BPH), enlargement<br />
of the prostate. The annoying part occurs when the prostate’s<br />
growth blocks the urethra, which causes problems with urinating.<br />
“The typical symptoms include a slow stream when urinating, more<br />
frequent urination, the feeling you are not emptying the bladder completely<br />
and having difficulty initiating urination,” Dr. Schloss explains.<br />
In the overwhelming majority of cases, Dr. Schloss is able to assure<br />
men that these symptoms do not indicate prostate cancer. Then, the<br />
question is whether or not treatment is needed. “Early on, the best<br />
approach to BPH is often to monitor symptoms,” he says. “We have<br />
good medications that help many men. When medication doesn’t<br />
work or the urethra appears to be increasingly blocked, I often suggest<br />
a procedure—either electro-surgery or laser—to open the<br />
blockage.”<br />
Enlarged prostate<br />
5