Development of a Disposable Spray Canister for Talc Pleurodesis*
Development of a Disposable Spray Canister for Talc Pleurodesis*
Development of a Disposable Spray Canister for Talc Pleurodesis*
You also want an ePaper? Increase the reach of your titles
YUMPU automatically turns print PDFs into web optimized ePapers that Google loves.
<strong>Development</strong> <strong>of</strong> a <strong>Disposable</strong> <strong>Spray</strong><br />
<strong>Canister</strong> <strong>for</strong> <strong>Talc</strong> <strong>Pleurodesis*</strong><br />
A Preliminary Report<br />
Henri G. Colt, MD, FCCP; and Jean-Francois Dumon, MD, FCCP<br />
<strong>Talc</strong> pleurodesis has been used <strong>for</strong> more than 50 years<br />
in both the United States and in Europe, and it has<br />
proven to be safe and effective in patients with malignant<br />
pleural effusions as well as recurrent pneumothorax.<br />
In this preliminary report, we describe a disposable,<br />
single-use spray canister that allows intrapleural administration<br />
<strong>of</strong> sterile, asbestos-free Luzenac talc, thus<br />
facilitating thoracoscopic talc insufflation <strong>for</strong> pleurodesis,<br />
particularly in patients with recurrent malignant<br />
effusions. The talc is delivered ready to use, administered<br />
via a hollow plastic delivery catheter that can be<br />
pleurodesis is usually recommended when patients<br />
with persistent or recurrent pleural effusions have<br />
failed multiple drainage procedures. The vast majority<br />
<strong>of</strong> these patients have malignant pleural effusions<br />
(MPE), <strong>of</strong>ten with pleural metastases, and are<br />
no longer responsive to systemic therapy. Others have<br />
paramalignant effusions or effusions related to massive<br />
ascites or peritoneal carcinomatosis.1 During the<br />
last 100 years, surgeons and chest physicians have<br />
searched <strong>for</strong> an effective means <strong>of</strong> pleurodesis, and<br />
many chemical, as well as other agents have been<br />
employed with varying degrees <strong>of</strong> success.2 Although<br />
never approved <strong>for</strong> intrapleural use by the Food and<br />
Drug Administration, tetracycline has been most<br />
frequently used in the recent past, but is no longer<br />
available.3 Bleomycin, a cytotoxic agent ropprtedly<br />
successful in up to 70% <strong>of</strong> instances, is costly and has<br />
systemic adverse effects.4 With the recent resurgence<br />
<strong>of</strong> thoracoscopy, talc pleurodesis, once quite popular,<br />
is increasingly used, and several investigators have<br />
shown that talc is superior to other agents in both<br />
clinical and experimental settings.5-7<br />
DESCRIPTION OF SPRAY CANISTER<br />
The purpose <strong>of</strong> this report is to describe a spray<br />
canister that allows intrapleural administration <strong>of</strong><br />
sterile, asbestos-free talc powder (developed in collaboration<br />
with Luzenac Europe [Toulouse, France]<br />
*From the Pulmonary and Critical Care Medicine Division,<br />
University <strong>of</strong> Cali<strong>for</strong>nia, San Diego Medical Center, San Diego<br />
(Dr. Colt); and the Centre Laser du CHU Sud, St. Marguerite<br />
Hospital, Marseille, France (Dr. Dumon).<br />
Manuscript received January 24, 1994; revision accepted April 19,<br />
1994.<br />
Reprint requests: Dr. Colt, Pulmonary Special Procedures UCSD<br />
Medical Center, 200 W. Arbor Drive, San Diego, CA 92103<br />
1 776<br />
Downloaded From: http://chestioumal.chestpubs.org/ on 02/22/2013<br />
inserted through the pleural trocars used during thoracoscopy.<br />
Use <strong>of</strong> this spray canister allows practitioners<br />
to avoid complex handling and sterilization procedures<br />
required <strong>for</strong> bulk talc powder. (Chest 1994; 106:1776-80)<br />
MPE=malignant pleural effusions<br />
Key words: canister; pleurodesis; talc; thoracoscopy<br />
and Axion [Aubagne, France] and distributed by<br />
Bryan Corp. [Woburn, Mass.] as aerosolized talc). The<br />
talc is from Luzenac, a small town located in the area<br />
<strong>of</strong> Ariege, France, the site <strong>of</strong> one <strong>of</strong> the largest<br />
open-air talc mines in the world. Luzenac talc is<br />
known <strong>for</strong> its relative purity: the canister contains 4<br />
g <strong>of</strong> Luzenac PR 7841 white talc powder (talc and<br />
chlorite concentration greater than or equal to 95%)<br />
with a pH <strong>of</strong> 9, a real density <strong>of</strong> 2.58 to 2.83, and a<br />
solubility in water less than 0.1%. Associated minerals<br />
include dolomite (less than 3%), calcite (trace<br />
elements only), and quartz (less than 3%). No amphiboles<br />
have ever been detected (x-ray diffraction as<br />
described in the Cosmetic, Toiletry, and Fragrance<br />
Association J4-1 norms <strong>of</strong> the American cosmetic industry).<br />
Products have been systematically controlled<br />
since 1978 (in<strong>for</strong>mation supplied by the manufacturer).<br />
Additional elements include soluble calcium<br />
(0.17%), soluble magnesium (0.09%) soluble iron (60<br />
ppm), chloride (> 140 ppm), and insoluble calcium<br />
(
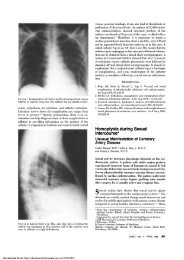
FIGURE 1. <strong>Disposable</strong> talc spray canister with nozzle and 15-cm<br />
delivery catheter. Also shown is a standard pneumatic talc atomizer<br />
with bellows applicator (Richard Wolf Co.), 2.5 g <strong>of</strong> talc in<br />
sterile test tube, and atraumatic lOF silicone catheter.<br />
by gamma radiation and marketed in a sterile peel<br />
pack in which are also enclosed 15- and 25-cm hollow<br />
plastic delivery catheters. The propellant is<br />
dichlorodifluoromethane.<br />
Prior to pleurodesis, the sterile talc canister and<br />
nozzles should be removed from the sterile packaging,<br />
after which the protective cap on the canister<br />
may be removed and the canister shaken. The nozzle<br />
and delivery catheter are then securely attached<br />
to the canister. Usage <strong>of</strong> the shorter 15-cm catheter<br />
is recommended <strong>for</strong> application through pleural<br />
trocars or at the thoracotomy site. The distal extremity<br />
should not be in close proximity to lung parenchyma.<br />
It is somewhat sharp and may cause parenchymal<br />
damage. In addition, the talc is delivered<br />
under pressure. Although no pressure-related damage<br />
has yet been seen, it is a potential danger <strong>of</strong><br />
pressurized talc spray administration. While firmly<br />
holding the nozzle and delivery catheter together in<br />
one hand, pressure is applied to the nozzle on the<br />
canister. The distal extremity <strong>of</strong> the delivery catheter<br />
should be pointed in several different directions<br />
to ensure equal and extensive delivery over all pleural<br />
surfaces. The talc canister is kept vertical to<br />
maximize distribution. In case <strong>of</strong> limited talc pleurodesis,<br />
talc is applied only to the area <strong>of</strong> interest.<br />
During talc delivery, the canister becomes cold, signaling<br />
near total talc evacuation. If talc is delivered<br />
through a pleural trocar during thoracoscopy, care<br />
should be taken to keep the distal extremity <strong>of</strong> the<br />
delivery catheter about 0.5 cm beyond the tip <strong>of</strong> the<br />
pleural cannula. Otherwise, talc will adhere to the<br />
sides <strong>of</strong> the cannula, and intrapleural distributions<br />
will be unsatisfactory. After application, the talc<br />
canister and delivery catheters should be discarded.<br />
Downloaded From: http://chestioumal.chestpubs.org/ on 02/22/2013<br />
Preliminary Clinical Experience<br />
We have used this device in 12 patients with MPE<br />
and in 9 patients with spontaneous pneumothoraxes<br />
(in addition to bleb or bulla resection). Pleurodesis<br />
was successful at 90 d (defined as absence <strong>of</strong> symptoms<br />
attributable to effusions, clinically insignificant<br />
increase <strong>of</strong> pleural effusion evidenced on chest x-ray<br />
film compared with baseline films, and requiring no<br />
further thoracentesis) in 11 <strong>of</strong> 12 patients and in all<br />
patients with pneumothorax (the follow-up was 1<br />
year). No complications <strong>of</strong> talc administration occurred,<br />
although about 30% <strong>of</strong> patients had lowgrade<br />
temperatures after thoracoscopy. A prospective<br />
study comparing talc pleurodesis using this device<br />
and routine talc powder administration using a<br />
standard pneumatic atomizer (Richard Wolf Co.) is<br />
underway.<br />
Possible Benefits and Pitfalls<br />
Overall, this disposable canister is effective and<br />
practical. Complex in-hospital sterilization and handling<br />
procedures <strong>of</strong> bulk talc powder are avoided,<br />
and talc administration is simple, rapid, and clean.<br />
The canister is expensive, however, when compared<br />
with other talc preparations. For example, at University<br />
<strong>of</strong> Cali<strong>for</strong>nia, San Diego, Medical Center,<br />
routine talc preparation, including purchase, sterilization,<br />
packaging, and handling, costs only $4.00.<br />
Another drawback <strong>of</strong> the canister is the inability to<br />
quantify talc administration. For example, we use the<br />
entire contents <strong>of</strong> a canister <strong>for</strong> patients with MPE<br />
and extensive neoplastic parietal pleura involvement,<br />
but we use only a few spray applications <strong>for</strong> limited<br />
pleurodesis in patients with benign disease or pneumothorax.<br />
Un<strong>for</strong>tunately, there is no way <strong>of</strong> quantifying<br />
the amount <strong>of</strong> talc delivered is less than the<br />
entire contents is used. This is quite different from the<br />
way standard talc powder is packaged in our institutions<br />
(in sterile plastic test tubes containing either<br />
1.2 or 2.5 g <strong>of</strong> sterile talc powder).<br />
Some minor pitfalls relate to the delivery catheters.<br />
Their tips are too sharp and could tear lung parenchyma.<br />
We have easily done this in experimental<br />
animal models. Also, talc tends to clump if the<br />
delivery catheter is held too close to the lung or to the<br />
chest wall parietal pleura. We believe that thoracoscopic<br />
administration <strong>of</strong> talc with the canister through<br />
a single point <strong>of</strong> entry is more difficult than through<br />
two points <strong>of</strong> entry, where the delivery catheter's<br />
position can be easily verified thoracoscopically. The<br />
delivery catheter also may detach from the nozzle as<br />
pressure is applied. For this reason, the canister,<br />
nozzle, and catheter should be held firmly during<br />
application. In regard to previous suggestions <strong>of</strong><br />
aerosolized talc delivery through an indwelling chest<br />
tube, we find this totally unsatisfactory. <strong>Talc</strong> clumps<br />
CHEST / 106 / 6 / DECEMBER, 1994 1777
up inside the chest tube, even when the longer 25-cm<br />
delivery catheter is used. There<strong>for</strong>e, we do not<br />
believe that aerosolized talc delivery through an indwelling<br />
chest tube can replace talc slurry administration.<br />
DISCUSSION<br />
<strong>Talc</strong> pleurodesis was first suggested in 1935 by<br />
Bethune,8 a Canadian surgeon who investigated<br />
methods <strong>of</strong> achieving adherence <strong>of</strong> lung parenchyma<br />
to the chest wall prior to per<strong>for</strong>ming lobectomy. In<br />
this study, Bethune actually credits a deceased Canadian<br />
physician, R. U. Harwood, <strong>for</strong> suggesting the<br />
use <strong>of</strong> commercial talc <strong>for</strong> this technique because <strong>of</strong><br />
the known fibrogenic properties <strong>of</strong> silicate powders.<br />
Bethune also describes the first thoracoscopic administration<br />
<strong>of</strong> talc powder using a specially designed<br />
"return-air" blower made by the Pilling Company.<br />
Subsequently, thoracoscopic talc poudrage (poudrage,<br />
which is French <strong>for</strong> powdering, consists <strong>of</strong><br />
spraying sterile talc powder over the visceral and<br />
parietal pleura surfaces) was used <strong>for</strong> pleurodesis<br />
in patients with tuberculosis as well as in<br />
patients with spontaneous pneumothorax,9,10 although<br />
several surgeons later preferred talc administration<br />
via thoracotomy, even in patients with malignant<br />
pleural effusions.11"'5 In 1958, Chambers,'6 a<br />
thoracic surgeon from San Diego, revived the technique<br />
<strong>of</strong> talc slurry pleurodesis (by talc slurry, one<br />
usually means that sterile talc powder is diluted in 50<br />
to 200 mL <strong>of</strong> normal saline solution and instilled via<br />
pleural trocar or chest tube), reporting an 85% success<br />
rate after instillation through an indwelling chest<br />
tube. Similar results were reported in 1967 by Jones17<br />
using thoracoscopic application <strong>of</strong> talc slurry, and in<br />
1976 by Adler and Sayek.18 This thoracic surgeon<br />
from New York also described a novel talc powder<br />
aerosol delivery system developed in cooperation<br />
with the Union Carbide Corporation in 1967.19 Microcel<br />
B, an amorphous calcium silicate used to fluidify<br />
talc and avoid clumping, was added in small<br />
amounts to US Pharmacopoeia-approved talc inside<br />
a metal container. A small Teflon delivery catheter<br />
was employed <strong>for</strong> administration into the body cavity<br />
during thoracotomy. Although successful, this<br />
product was not commercialized owing to lack <strong>of</strong><br />
interest by the company (verbal communication, R.<br />
Adler, MD, December 1993).<br />
Although talc was repeatedly used <strong>for</strong> pleurodesis<br />
in patients with MPE in both Europe and the United<br />
States throughout the 1960s,20-24 it was largely abandoned<br />
in the 1970s, especially in the United States.<br />
Indeed, there had been suggestions that proportional<br />
mortality from carcinoma <strong>of</strong> the lung and pleura<br />
among talc workers was four times that <strong>of</strong> a control<br />
population.25 In addition, tetracycline was becoming<br />
1 778<br />
Downloaded From: http://chestioumal.chestpubs.org/ on 02/22/2013<br />
a most popular agent since the first report <strong>of</strong> its successful<br />
use <strong>for</strong> pleurodesis by Rubinson and Bolooki<br />
in 1972.26<br />
A potential problem <strong>of</strong> intrapleural talc administration,<br />
there<strong>for</strong>e, is the carcinogenicity <strong>of</strong> the talc.<br />
The issue surrounding talc use is particularly confusing<br />
because many mineral talcs, especially those<br />
previously mined from New York, were heavily<br />
contaminated with tremolite or anthrophyllite.27'28<br />
<strong>Talc</strong> asbestosis, produced by inhalation <strong>of</strong> talc with<br />
asbestos fibers, is a well recognized medical illness.29<br />
<strong>Talc</strong> is, after all, a hydrous magnesium silicate<br />
(Mg6Si8020[OH]4), sometimes containing a small<br />
amount <strong>of</strong> aluminum silicate. Its <strong>for</strong>mula is similar to<br />
that <strong>of</strong> asbestos. The <strong>for</strong>mula <strong>for</strong> chrysotile asbestos,<br />
<strong>for</strong> example, is Mg6Si4010(0H)8, and contamination<br />
<strong>of</strong> talc with asbestos, especially tremolite, has<br />
been reported.3032 Other minerals such as dolomite<br />
(calcium magnesium carbonate) may also "contaminate"<br />
talc.33 The results <strong>of</strong> experimental studies <strong>of</strong><br />
Wagner et a134 and Rubinoet et al,35 as well as those<br />
<strong>of</strong> retrospective studies per<strong>for</strong>med by the Research<br />
Committee <strong>of</strong> the British Thoracic Association36 in<br />
England and by Leophonte et a137 in France show<br />
that pure talc (containing no asbestos) is not carcinogenic.<br />
Both the European and American Pharmacopoeia,<br />
there<strong>for</strong>e, have instituted strict guidelines <strong>for</strong><br />
medical-grade and cosmetic-grade talc composition,38-40<br />
not only addressing requirements <strong>for</strong> asbestos-free<br />
talc, but also limiting its contamination with<br />
bacteria or other minerals. Although further research<br />
is required in this area, current evidence suggests that<br />
fears <strong>of</strong> asbesto-free, pure talc-induced neoplasms are<br />
unfounded. To our knowledge, no cases <strong>of</strong> neoplasm<br />
caused by intrapleural administration <strong>of</strong> sterile,<br />
asbestos-free talc have been reported.<br />
Many studies have demonstrated that talc pleurodesis<br />
is a safe and effective means <strong>of</strong> achieving apposition<br />
<strong>of</strong> the pleural surfaces in patients with MPE.<br />
Success rates are reportedly greater than 85%.6,22,4147<br />
In animal experiments as early as in 1941, Lelourd41<br />
showed that pleurodesis was achieved by the 7th day<br />
after talc administration. In a recent canine study,<br />
Bresticker et a17 reported that pleural symphysis from<br />
talc was comparable to that obtained by mechanical<br />
abrasion. Mathlouti et a149 showed that talc caused an<br />
inflammatory reaction confined to the pleural surfaces,<br />
confirming previous work done by Frankel et<br />
al.50 Controversy subsists, however, regarding the<br />
ideal method <strong>of</strong> administration, and it is unclear<br />
whether poudrage has any advantages over slurry.<br />
Boutin et al5l, <strong>for</strong> example, has repeatedly advocated<br />
thoracoscopic talc poudrage. Additional support <strong>for</strong><br />
this procedure, which may be safely per<strong>for</strong>med with<br />
the patient under local or general anesthesia, is provided<br />
by several studies. Ohri et a143 reported 95.5%<br />
<strong>Development</strong> <strong>of</strong> a <strong>Disposable</strong> <strong>Spray</strong> <strong>Canister</strong> <strong>for</strong> <strong>Talc</strong> Pleurodesis (Colt, Dumon)
success in 42 patients, and Aelony et al44 showed<br />
success in 23 <strong>of</strong> 28 (82%) patients. Hartman et a16<br />
compared the use <strong>of</strong> insufflation <strong>of</strong> talc under thoracoscopic<br />
guidance with control populations who had<br />
received either tetracycline or bleomycin pleurodesis,<br />
reporting a 95% success rate <strong>of</strong> talc at 90 days<br />
compared with 70%o <strong>for</strong> bleomycin and 47% <strong>for</strong> tetracycline.<br />
Poudrage may be more effective than<br />
simple administration <strong>of</strong> talc slurry through a previously<br />
placed chest tube because adhesions and loculated<br />
fluid collections seen during thoracoscopy can<br />
be removed prior to pleurodesis. Additional, prospective,<br />
multi-armed randomized protocols and animate<br />
laboratory research are necessary, however, to further<br />
define indications <strong>for</strong> the selected techniques <strong>of</strong><br />
talc administration.<br />
In contrast to many favorable clinical reports <strong>of</strong><br />
talc pleurodesis, there are reports <strong>of</strong> immediate adverse<br />
effects <strong>of</strong> intrapleural talc administration and<br />
those suggesting potential restrictive ventilatory impairment<br />
years after talc pleurodesis <strong>for</strong> recurrent<br />
pneumothorax.52 Roujeau and Rose53 linked talc use<br />
to pulmonary talcoma. <strong>Talc</strong> pachypleuritis (pleural<br />
inflammation and thickenning), although not constant<br />
radiographically,51 has been described.17'49<br />
Acute pneumonitis54'55 and acute respiratory distress<br />
syndrome56 also have occurred shortly after intrapleural<br />
talc administration, although definite causal<br />
relationships between respiratory insufficiency and<br />
talc, however, have not been established. Whether<br />
adverse effects <strong>of</strong> talc are related to dose or mode <strong>of</strong><br />
administration requires investigation. In regard to<br />
potential long-term restrictive lung disease after<br />
intrapleural talc administration in patients with<br />
pneumothorax, Lange et a157 per<strong>for</strong>med pulmonary<br />
function tests on 114 patients during a 22- to 35-year<br />
follow-up study. Only mild, statistically insignificant<br />
differences in ventilatory function were discovered.<br />
In the experimental setting, McCahren et a158 showed<br />
that talc pleurodesis did not affect dynamic or static<br />
lung compliance in growing swine. It appears, there<strong>for</strong>e,<br />
that fears <strong>of</strong> decreased lung function due to talc<br />
pleurodesis probably are unfounded.<br />
In summary, if talc is to be recognized by medical<br />
and surgical communities as an effective and safe<br />
method <strong>of</strong> pleurodesis, clinical and laboratory studies<br />
need to be per<strong>for</strong>med to answer specific questions<br />
regarding mode <strong>of</strong> administration, talc composition,<br />
and effects <strong>of</strong> talc pleurodesis compared with other<br />
methods <strong>of</strong> pleural symphysis. Practical problems<br />
also must be addressed. Intrapleural talc administration<br />
has not been <strong>for</strong>mally recognized by the US Food<br />
and Drug Administration, and lack <strong>of</strong> standardization<br />
regarding dose, mode <strong>of</strong> administration, packaging,<br />
and handling persists. Many practitioners,f or<br />
example, use European or US Pharmacopoeia-<br />
Downloaded From: http://chestioumal.chestpubs.org/ on 02/22/2013<br />
approved talc in its "pure" <strong>for</strong>m. It is unclear<br />
whether the composition <strong>of</strong> talc obtained from<br />
different sources can alter its fibrogenicity. Others<br />
combine talc with thymol iodide, as originally described<br />
by Bethune.8'46 Advantages <strong>of</strong> this mixture<br />
over pure asbestos-free talc are undefined. It is noteworthy<br />
that several different talc sterilization techniques<br />
are available. For example, talc may be gamma-radiated<br />
and placed into sterile peel packs,59<br />
whereas, at the University <strong>of</strong> Cali<strong>for</strong>nia, San Diego,<br />
Medical Center, medical-grade asbestos-free US<br />
Pharmacopoeia-approved talc powder is purchased<br />
in bulk <strong>for</strong>m, packaged in unit doses, and sterilized<br />
using a combination <strong>of</strong> ethylene oxide and dry heat.<br />
While some hospitals willingly share their handling<br />
guidelines, others refuse to do so categorically. The<br />
availability <strong>of</strong> a sterile, asbestos-free talc spray canister<br />
could facilitate talc acquisition and provide an<br />
alternative to institutionally prepared talc <strong>for</strong> pleurodesis.<br />
REFERENCES<br />
1 Hausheer PH, Yarbro JW. Diagnosis and treatment <strong>of</strong> malignant<br />
pleural effusion. Semin Oncol 1985; 12:54-75<br />
2 Keller SM. Current and future therapy <strong>for</strong> malignant pleural<br />
effusion. Chest 1993; 103:63S-7S<br />
3 Vaughn LM, Walker PB, Sahn SA. Alternatives to tetracycline<br />
pleurodesis. Ann Pharmacol 1992; 26:562<br />
4 Ostrowski MJ. Intracavitary therapy with bleomycin <strong>for</strong> the<br />
treatment <strong>of</strong> malignant pleural effusions. J Surg Oncol Suppl<br />
1989; 1:7-13<br />
5 Fentiman IS, Rubens RD, Hayward JL. A comparison <strong>of</strong> intracavitary<br />
talc and tetracycline <strong>for</strong> the control <strong>of</strong> pleural effusions<br />
secondary to breast cancer. Curr J Cancer Clin Oncol<br />
1986; 22:1079-81<br />
6 Hartman DL, Gaither JM, Kesler KA, Mylet DM, Brown JW,<br />
Mathur PN. Comparison <strong>of</strong> insufflated talc under thoracoscopic<br />
guidance with standard tetracycline and bleomycin pleurodesis<br />
<strong>for</strong> control <strong>of</strong> malignant pleural effusions. J Thorac Cardiovasc<br />
Surg 1993; 105:743-48<br />
7 Bresticker MA, Oba J, LoCicero J, Greene R. Optimal pleurodesis:<br />
a comparison study. Ann Thorac Surg 1993; 55:364-67<br />
8 Bethune N. Pleural poudrage. J Thorac Cardiovasc Surg 1935;<br />
4:251-61<br />
9 Despeigne H, Fraisse P. Justification technique et indications<br />
dans la chirurgie de la tuberculose: les methodes derives du<br />
poudrage de Bethune. Le Poumon 1948; 4:97-107<br />
10 Bernard E, Meyer A, Nico JP, Depierre M. Sur le traitment du<br />
pneumothorax spontane severe du a la rupture de bulles<br />
emphysemateuses (symphyse provoquee par talcage intrapleural).<br />
J Fr Med Chir Thor 1949; 3:536-40<br />
11 Medici FA. Results <strong>of</strong> pleurodesis by Bethune method in benign<br />
spontaneous pneumothorax. Ann Cat Pat Clin Tuberc 1944;<br />
6: 106-115<br />
12 Meade RH, Blades BB. Surgical treatment <strong>of</strong> recurrent and<br />
chronic spontaneous pneumothorax. Am Rev Tuberc 1949;<br />
60:683-98<br />
13 Shedbalker AR, Head JM, Head LR, Murphy DJ, Mason JH.<br />
Evaluation <strong>of</strong> talc symphysis in management <strong>of</strong> malignant<br />
pleural effusion. J Thorac Cardiovasc Surg 1971; 61:492-97<br />
14 Camishion RC, Gibbon JH, Nealon TF. <strong>Talc</strong> poudrage in the<br />
treatment <strong>of</strong> pleural effusion due to cancer. S Clin North Am<br />
1962; 42:1521-26<br />
CHEST / 106 / 6 / DECEMBER, 1994 1779
15 Prorok J, Nealon TF. Pleural symphysis by talc poudrage in the<br />
treatment <strong>of</strong> malignant pleural effusion. Bull Soc Intern Chir<br />
1968; 6:630-36<br />
16 Chambers JS. Palliative treatment <strong>of</strong> neoplastic pleural effusions<br />
with intercostal intubation and talc instillation. West J<br />
Surg 1958; 66:26-28<br />
17 Jones GR. Treatment <strong>of</strong> recurrent malignant pleural effusion by<br />
iodized talc pleurodesis. Thorax 1969; 24:69-73<br />
18 Adler RH, Sayek I. Treatment <strong>of</strong> malignant pleural effusion: a<br />
method using tube thoracostomy and talc. Ann Thorac Surg<br />
1976; 22:8-15<br />
19 Adler RH, Rappole BW. Recurrent malignant pleural effusions<br />
and talc powder aerosol treatment. Surgery 1967; 62:1000-06<br />
20 Roche G, Delanoe Y, Moayer N. <strong>Talc</strong>age de la plevre sous<br />
pleuroscopie: resultats, indications, techniques (a propos de 14<br />
observations). J Fr Med Chir Thor 1963; 17:677-92<br />
21 Scarbonchi J, Razzouk H. Traitment palliatif des epanchements<br />
pleuraux neoplasiques: talcage des plevres sous pleuroscopie<br />
avec un melange de virgimycine. Marseille Med 1967; 104:<br />
939-47<br />
22 Haupt GJ, Camishion RC, Templeton JY, Gibbon JH. Treatment<br />
<strong>of</strong> malignant pleural effusions by talc poudrage. JAMA<br />
1960; 172:918-21<br />
23 Pearson FG, MacGregor DC. <strong>Talc</strong> poudrage <strong>for</strong> malignant<br />
pleural effusions. J Thorac Cardiovasc Surg 1966; 51:732-38<br />
24 Bloomberg AE. Thoracoscopy in diagnosis <strong>of</strong> pleural effusion.<br />
NY State J Med 1970; 70:1974-77<br />
25 Kleinfeld M, Messite J, Kooyman 0, Zaki MH. Mortality among<br />
talc miners and millers in New York state. Arch Environ Health<br />
1967; 14:663-67<br />
26 Rubinson RM, Bolooki H. Intrapleural tetracycline control <strong>of</strong><br />
malignant pleural effusion: a preliminary report. South Med J<br />
1972; 65:847-49<br />
27 Merliss RR. <strong>Talc</strong> treated rice and Japanese stomach cancer.<br />
Science 1971; 143:1141-43<br />
28 Gamble JF, Fellner W, Dimeo MJ. An epidemiologic study <strong>of</strong><br />
a group <strong>of</strong> talc workers. Am Rev Respir Dis 1979; 19:741-53<br />
29 Feigin DS. Misconceptions regarding the pathogenicity <strong>of</strong> silica<br />
and silicates. J Thorac Imag 1989; 4:68-80<br />
30 Cralley LJ, Key MM, Groth DH, Lainhart WS, Ligo RM. Fibrous<br />
and mineral content <strong>of</strong> cosmetic talcum products. Am<br />
Industr Hyg Assoc J 1968; 29:350-54<br />
31 Rose HA. Detection and determination <strong>of</strong> crysotile in talc USP.<br />
J Pharm Sci 1974; 63:268-69<br />
32 Miller A, Tierstein AS, Bader ME, Bader RA, Selik<strong>of</strong>f IJ. <strong>Talc</strong><br />
pneumonoconiosis: significance <strong>of</strong> sublight microscopic mineral<br />
particles. Am J Med 1971; 50:395-402<br />
33 Schulz RZ, Williams CR. Commercial talc: animal and mineralogical<br />
studies. J Ind Hyg Toxicol 1942; 24:75-9<br />
34 Wagner JC, Berry G, Cooke TJ, Hill RJ, Pooley FD, Skidemore<br />
JW. Animal experiments with talc. In: Walton WH, ed.<br />
Proceedings <strong>of</strong> the Fourth International Symposium on Inhaled<br />
Particles. Edinburgh, Scotland: Pergamon Press, 1977; 647-54<br />
35 Rubino GF, Scansetti G, Piolatto G, Romano CA. Mortality<br />
study <strong>of</strong> talc minors and millers. J Occup Med 1976; 18:186-93<br />
36 Chappell AG, Johnson A, Wagner CJC, Seal RME, Berry G,<br />
Nicholson D. A survey <strong>of</strong> the long-term effects <strong>of</strong> talc and kaolin<br />
pleurodesis: Research Committee <strong>of</strong> the British Thoracic<br />
Association. Br J Dis Chest 1979; 73:285-88<br />
37 Leophonte P, Basset MF, Pincemin J, Louis A, Pernet P,<br />
1780<br />
Downloaded From: http://chestioumal.chestpubs.org/ on 02/22/2013<br />
Delaude A. Mortalitie des travailleurs du talc en France. Rev<br />
Fr Mal Resp 1983; 11:489-90<br />
38 Specification No. 12: Cosmetic talc. London, England: Cosmetic,<br />
Toiletry, Perfumery Assoc Ltd; 1977<br />
39 Specification: <strong>Talc</strong> cosmetic, issue 10-7. Cosmetic, Toiletry, and<br />
Fragrance Association, 1976<br />
40 British Pharmaceutical Codex. London, England: The Pharmaceutical<br />
Press, 1973;492<br />
41 Austin EH, Flye MW. The treatment <strong>of</strong> recurrent malignant<br />
pleural effusion. Ann Thorac Surg 1979; 28:190-203<br />
42 Daniel TM, Tribble CG, Rodgers BM. Thoracoscopy and talc<br />
poudrage <strong>for</strong> pneumothoraces and effusions. Ann Thorac Surg<br />
1990; 50:186-89<br />
43 Ohri SK, Shashi KO, Townsend ER, Fountain SW. Early and<br />
late outcome after diagnostic thoracoscopy and talc pleurodesis.<br />
Ann Thorac Surg 1992; 53:1038-41<br />
44 Aelony Y, King R, Boutin C. Thoracoscopic talc poudrage<br />
pleurodesis <strong>for</strong> chronic pleural effusions. Ann Intern Med 1991;<br />
115:778-82<br />
45 van de Brekel JA, Duurkens VAM, Vanderschueren RGJRA.<br />
Pneumothorax: results <strong>of</strong> thoracoscopy and pleurodesis with<br />
talc poudrage and thoracotomy. Chest 1993; 103:345-47<br />
46 Webb WR, Ozmen V, Moulder PV, Shabahang B, Breaux J.<br />
Iodized talc pleurodesis <strong>for</strong> the treatment <strong>of</strong> pleural effusions.<br />
J Thorac Cardiovasc Surg 1992; 103:881-86<br />
47 Boniface E, Guerin JC. Interet du talcage par thoracoscopie<br />
dans le traitement symptomatique des pleuresies recidivantes.<br />
Rev Mal Resp 1989; 6:133-39<br />
48 LeLourd H. Symphyse pleural provoquee par le poudrage<br />
pleuroscopique de Bethune. J Med Bordeaux 1941; 11:448-53<br />
49 Mathlouti A, Chabchoub A, Labbene N, Amara A, Ghorbel A,<br />
Kacem S, et al. Etude anatamopathologique experimentale du<br />
talcage pleural. Rev Mal Resp 1992; 9:617-21<br />
50 Frankel A, Krasna I, Baron<strong>of</strong>sky ID. An experimental study <strong>of</strong><br />
pleural symphysis. J Thorac Cardiovasc Surg 1961; 42:65-7<br />
51 Boutin C, Astoul Ph, Seitz B. The role <strong>of</strong> thoracoscopy in the<br />
evaluation and management <strong>of</strong> pleural effusions. Lung 1990;<br />
168(suppl): 1113-21<br />
52 Gaensler EA. Parietal pleurectomy <strong>for</strong> recurrent spontaneous<br />
pneumothorax. Surg Gynec Obstet 1956; 102:293-308<br />
53 Roujeau J, Rose Y. Sur certains talcomes pulmonaires. J Fr Med<br />
Chir Thor 1958; 12:330-36<br />
54 Bouchama A, Chastre J, Gaudichet A, Soler P, Gibert C. Acute<br />
pneumonitis with bilateral pleural effusion after talc pleurodesis.<br />
Chest 1984; 86:795-97<br />
55 Factor SM. Granulomatous pneumonitis: a result <strong>of</strong> intrapleural<br />
instillation <strong>of</strong> quinacrine and talcum powder. Arch Pathol<br />
1975; 99:499-502<br />
56 Rinaldo JE, Owens GR, Rogers RM. Adult respiratory distress<br />
syndrome following intrapleural instillation <strong>of</strong> talc. J Thorac<br />
Cardiovasc Surg 1983; 85:523-26<br />
57 Lange P, Mortensen J, Groth S. Lung function 22-35 years after<br />
treatment <strong>of</strong> idiopathic spontaneous pneumothorax with<br />
talc poudrage or simple drainage. Thorax 1988; 43:559-61<br />
58 McCahren ED, Teague WG, Flanagan T, White B, Rodgers<br />
BM. The effects <strong>of</strong> talc pleurodesis on growing swine. J Ped Surg<br />
1990; 25:1147-51<br />
59 Bubik JS. Preparation <strong>of</strong> sterile talc <strong>for</strong> treatment <strong>of</strong> pleural<br />
effusion [letter]. Am J Hosp Pharm 1992; 49:562-63<br />
<strong>Development</strong> <strong>of</strong> a <strong>Disposable</strong> <strong>Spray</strong> <strong>Canister</strong> <strong>for</strong> <strong>Talc</strong> Pleurodesis (Colt, Dumon)