Guidelines for the Rational Use of Benzodiazepines
Guidelines for the Rational Use of Benzodiazepines
Guidelines for the Rational Use of Benzodiazepines
Create successful ePaper yourself
Turn your PDF publications into a flip-book with our unique Google optimized e-Paper software.
<strong>Guidelines</strong> <strong>for</strong> <strong>the</strong> <strong>Rational</strong><br />
<strong>Use</strong> <strong>of</strong> <strong>Benzodiazepines</strong><br />
When and What to <strong>Use</strong><br />
Pr<strong>of</strong>essor C Hea<strong>the</strong>r Ashton, DM, FRCP<br />
Clinical Psychopharmacology Unit,<br />
Department <strong>of</strong> Psychiatry<br />
The Royal Victoria Infirmary<br />
Queen Victoria Road<br />
Newcastle upon Tyne NE1 4LP<br />
The Ashton Manual · Pr<strong>of</strong>essor Ashton's Main Page<br />
Review Article from: Drugs 48 (1):25-40. 1994<br />
Contents<br />
Summary<br />
1. Differences Between <strong>Benzodiazepines</strong><br />
2. <strong>Rational</strong> <strong>Use</strong> <strong>of</strong> <strong>Benzodiazepines</strong> <strong>for</strong> Insomnia<br />
2.1 Prevalence <strong>of</strong> Insomnia<br />
2.2 Causes and Types <strong>of</strong> Insomnia<br />
2.3 General Indications <strong>for</strong> Drug Treatment <strong>of</strong> Insomnia<br />
2.4 Effects <strong>of</strong> <strong>Benzodiazepines</strong> on Sleep<br />
2.5 Disadvantages <strong>of</strong> Benzodiazepine Hypnotics<br />
2.5.1 Tolerance<br />
2.5.2 Rebound Insomnia<br />
2.5.3 Hangover Effects<br />
2.5.4 Dependence<br />
2.5.5 Respiratory Depression<br />
2.6 Choice <strong>of</strong> Benzodiazepine Hypnotic<br />
2.6.1 The Elderly<br />
2.6.2 The Young<br />
2.6.3 Pregnancy and Lactation<br />
2.6.4 Disease States<br />
2.6.5 Withdrawal <strong>of</strong> Benzodiazepine Hypnotics<br />
2.6.6 Alternatives to <strong>Benzodiazepines</strong><br />
3. <strong>Rational</strong> <strong>Use</strong> <strong>of</strong> <strong>Benzodiazepines</strong> <strong>for</strong> Anxiety<br />
3.1 Prevalence <strong>of</strong> Anxiety<br />
3.2 Classification <strong>of</strong> Anxiety<br />
3.3 Effects <strong>of</strong> <strong>Benzodiazepines</strong> on Anxiety<br />
3.4 Disadvantages <strong>of</strong> Benzodiazepine Anxiolytics<br />
3.4.1 Tolerance<br />
3.4.2 Psychomotor impairment<br />
3.4.3 Disinhibition, Paradoxical Effects<br />
3.4.4 Affective Reactions<br />
3.4.5 Dependence<br />
3.5 Choice and <strong>Use</strong> <strong>of</strong> <strong>Benzodiazepines</strong> in Anxiety
Summary<br />
3.5.1 Panic Disorder and Phobias<br />
3.5.2 Withdrawal <strong>of</strong> <strong>Benzodiazepines</strong><br />
3.5.3 Prevention <strong>of</strong> Benzodiazepine Dependence<br />
4. <strong>Benzodiazepines</strong> as Anticonvulsants<br />
4.1 Status Epilepticus<br />
4.2 Prophylaxis in Epilepsy<br />
4.3 Adverse Effects<br />
5. O<strong>the</strong>r <strong>Use</strong>s <strong>of</strong> <strong>Benzodiazepines</strong><br />
5.1 Anaes<strong>the</strong>sia<br />
5.2 Motor Disorders<br />
5.3 Acute Psychoses<br />
6. The Future<br />
References<br />
Table I<br />
Table II<br />
Table III<br />
Table IV<br />
The main actions <strong>of</strong> benzodiazepines (hypnotic, anxiolytic, anticonvulsant, myorelaxant<br />
and amnesic) confer a <strong>the</strong>rapeutic value in a wide range <strong>of</strong> conditions. <strong>Rational</strong> use<br />
requires consideration <strong>of</strong> <strong>the</strong> large differences in potency and elimination rates between<br />
different benzodiazepines, as well as <strong>the</strong> requirements <strong>of</strong> individual patients.<br />
As hypnotics, benzodiazepines are mainly indicated <strong>for</strong> transient or short term insomnia,<br />
<strong>for</strong> which prescriptions should if possible be limited to a few days, occasional or<br />
intermittent use, or courses not exceeding 2 weeks. Temazepam, loprazolam and<br />
lormetazepam, which have a medium duration <strong>of</strong> action are suitable. Diazepam is also<br />
effective in single or intermittent dosage. Potent, short-acting benzodiazepines such as<br />
triazolam appear to carry greater risks <strong>of</strong> adverse effects.<br />
As anxiolytics, benzodiazepines should generally be used in conjunction with o<strong>the</strong>r<br />
measures (psychological treatments, antidepressants, o<strong>the</strong>r drugs) although such<br />
measures have a slower onset <strong>of</strong> action. Indications <strong>for</strong> benzodiazepines include acute<br />
stress reactions, episodic anxiety, fluctuations in generalised anxiety and as initial<br />
treatment <strong>for</strong> severe panic and agoraphobia. Diazepam is usually <strong>the</strong> drug <strong>of</strong> choice,<br />
Given in single doses, very short (1 to 7 days) or short (2 to 4 weeks) courses, and only<br />
rarely <strong>for</strong> longer term treatment. Alprazolam has been widely used, particularly in <strong>the</strong><br />
US, but is not recommended in <strong>the</strong> UK, especially <strong>for</strong> long term use.<br />
<strong>Benzodiazepines</strong> also have uses in epilepsy (diazepam, clonazepam, clobazam),<br />
anaes<strong>the</strong>sia (midazolam), some motor disorders and occasionally in acute psychoses.<br />
The major clinical advantages <strong>of</strong> benzodiazepines are high efficacy, rapid onset <strong>of</strong> action<br />
and low toxicity. Adverse effects include psychomotor impairment, especially in <strong>the</strong><br />
elderly, and occasionally paradoxical excitement. With long term use, tolerance,<br />
dependence and withdrawal effects can become major disadvantages. Unwanted effects<br />
can largely be prevented by keeping dosages minimal and courses short (ideally 4 weeks<br />
maximum, and by careful patient selection. Long term prescription is occasionally<br />
required <strong>for</strong> certain patients.<br />
All benzodiazepines exert, in slightly varying degrees, 5 major actions: hypnotic,<br />
anxiolytic, anticonvulsant, muscular relaxant and amnesic. Their main advantages are<br />
<strong>the</strong>ir high efficacy, rapid onset <strong>of</strong> action and low toxicity. Few, if any, o<strong>the</strong>r drugs can<br />
compete with <strong>the</strong>m in all <strong>the</strong>se respects.
In short term use, benzodiazepines can be valuable, and sometimes lifesaving, across a<br />
wide range <strong>of</strong> clinical conditions. Nearly all <strong>the</strong> disadvantages <strong>of</strong> benzodiazepines result<br />
from long term use, and it is such use, involving some millions <strong>of</strong> people worldwide,<br />
which has earned <strong>the</strong>m a poor reputation, particularly as drugs <strong>of</strong> dependence. This<br />
article suggests how benzodiazepines can best be used rationally, to maximise <strong>the</strong>ir<br />
advantages and minimise <strong>the</strong>ir disadvantages. As with all <strong>the</strong>rapies, <strong>the</strong> balance<br />
between benefits and risks may vary between individual patients.<br />
1. Differences Between <strong>Benzodiazepines</strong><br />
Some properties <strong>of</strong> benzodiazepines are shown in Table I. There are large differences in<br />
potency between different benzodiazepines, so that equivalent doses vary as much as<br />
20-fold. This factor must be taken into account when changing a patient from one<br />
benzodiazepine to ano<strong>the</strong>r, and special care must be taken in prescribing minimal<br />
effective doses <strong>of</strong> potent benzodiazepines such as alprazolam, triazolam and lorazepam.<br />
There are slight differences in <strong>the</strong> potency <strong>of</strong> separate effects, possibly due to<br />
differences in affinity <strong>for</strong> various receptor subtypes. Thus, some benzodiazepines are<br />
more effective than o<strong>the</strong>rs as anticonvulsants and some may differ in <strong>the</strong> ratio between<br />
anxiolytic and hypnotic actions, although <strong>the</strong> marketing <strong>of</strong> different benzodiazepines as<br />
hypnotics or anxiolytics is governed more by commercial than by pharmacological<br />
factors. Rates <strong>of</strong> penetration into <strong>the</strong> brain also differ: oxazepam penetrates relatively<br />
slowly and <strong>the</strong>re<strong>for</strong>e has a slower onset <strong>of</strong> action than, <strong>for</strong> example. diazepam.<br />
Oxazepam is, thus, less suitable as an hypnotic, but also has a lower abuse potential.<br />
<strong>Benzodiazepines</strong> also differ markedly in <strong>the</strong>ir rates <strong>of</strong> elimination (elimination half-lives<br />
vary from 2 to 100 hours) and some have pharmacologically active metabolites. The<br />
possibility <strong>of</strong> residual effects after single doses and cumulative effects with multiple-dose<br />
administration must be kept in mind, especially in elderly patients. Potent<br />
benzodiazepines with relatively short elimination half-lives (triazolam, alprazolam,<br />
lorazepam) appear to carry <strong>the</strong> highest risk <strong>of</strong> causing problems with dependence.[1]<br />
Indications <strong>for</strong> benzodiazepines and <strong>the</strong> optimal choice <strong>of</strong> different benzodiazepines are<br />
discussed below in order <strong>of</strong> <strong>the</strong> conditions <strong>for</strong> which <strong>the</strong>y are most commonly prescribed.<br />
2. <strong>Rational</strong> <strong>Use</strong> <strong>of</strong> <strong>Benzodiazepines</strong> <strong>for</strong> Insomnia<br />
The UK Committee on Safety <strong>of</strong> Medicines[2] and <strong>the</strong> Royal College <strong>of</strong> Psychiatrists[3]<br />
both recommended that benzodiazepines be prescribed <strong>for</strong> insomnia 'only when it is<br />
severe, disabling, or subjecting <strong>the</strong> individual to extreme distress'. The Drug and<br />
Therapeutics Bulletin[4] was scarcely less stringent in its view that <strong>the</strong>y 'should only be<br />
used when sleep disturbance markedly affects <strong>the</strong> life <strong>of</strong> an individual or his family, and<br />
when o<strong>the</strong>r approaches have failed'. Yet nearly 14 million prescriptions <strong>for</strong><br />
benzodiazepine hypnotics are dispensed annually in <strong>the</strong> UK. Prescribing levels have<br />
remained steady despite a decline in <strong>the</strong> prescription <strong>of</strong> benzodiazepine anxiolytics.[5]<br />
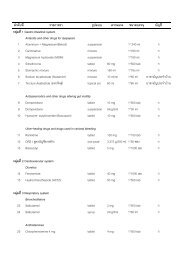
TABLE I. Indications and characteristics <strong>of</strong> benzodiazepines<br />
Drug<br />
t1/2 (h)<br />
[metabolite] [c]<br />
Approximately<br />
equivalent<br />
oral dosages (mg)
Hypnotics<br />
Loprazolam 6-12 1<br />
Lormetazepam 10-12 1<br />
Nitrazepam 15-38 10<br />
Temazepam 8-15 20<br />
Triazolam [a] 2-5 0.5<br />
Anxiolytics<br />
Alprazolam 6-12 0.5<br />
Chlordiazepoxide 5-30 [36-200] 25<br />
Diazepam [b] 20-100 [36-200] 10<br />
Lorazepam 10-18 1<br />
Oxazepam 4-15 10<br />
Anticonvulsants<br />
Clobazam 12-60 20<br />
Clonazepam 24-48 1<br />
Premedication, anaes<strong>the</strong>sia induction; sedation in intensive care<br />
Midazolam[d] 2<br />
Not available <strong>for</strong><br />
oral administration.<br />
Usual dosage range<br />
IV or IM 2-7.5mg<br />
a Withdrawn from <strong>the</strong> UK market in 1991.<br />
b Although classed as an anxiolytic, diazepam is a useful<br />
hypnotic in single or intermittent dosage and is used im as<br />
an anticonvulsant (see table IV).<br />
c Half-life <strong>of</strong> pharmacologically active metabolite.<br />
d Oral dosage not available.<br />
Abbreviations: IM = intramuscular; IV = intravenous;<br />
t1/2 = elimination half-life.<br />
Such widespread prescribing may be considered casual,[6] but <strong>the</strong>re is no doubt that in<br />
short term use benzodiazepines are effective sleep inducers and sleep promotors. Their<br />
use be<strong>for</strong>e an individual has reached a state <strong>of</strong> 'extreme distress' may sometimes be<br />
appropriate. Although <strong>the</strong> drugs provide only symptomatic relief and do not affect <strong>the</strong><br />
underlying cause, <strong>the</strong>y can, if prescribed judiciously, improve <strong>the</strong> quality <strong>of</strong> life <strong>for</strong> many<br />
patients with insomnia.<br />
2.1 Prevalence <strong>of</strong> Insomnia
Insomnia is common, particularly in <strong>the</strong> elderly and especially in women. Thus, up to<br />
40% <strong>of</strong> individuals over 65 years <strong>of</strong> age complain <strong>of</strong> disturbed sleep[7] and '<strong>the</strong> five<br />
million British women over 65 probably consume around 40% <strong>of</strong> all benzodiazepine<br />
hypnotics supplied by <strong>the</strong> FPS'[5] (FPS = Family Practitioner Service, i.e. general<br />
practitioners). However, insomnia is by no means confined to <strong>the</strong> elderly[6] and rational<br />
use <strong>of</strong> benzodiazepines or o<strong>the</strong>r hypnotics <strong>for</strong> this symptom requires consideration <strong>of</strong> <strong>the</strong><br />
causes and types <strong>of</strong> insomnia, <strong>the</strong> pharmacological effects <strong>of</strong> <strong>the</strong> drugs, and <strong>the</strong> needs <strong>of</strong><br />
<strong>the</strong> individual patient.<br />
2.2 Causes and Types <strong>of</strong> Insomnia<br />
The many causes <strong>of</strong> insomnia can be broadly categorised as physical, physiological,<br />
psychological, psychiatric and pharmacological - <strong>the</strong> '5P's'.[8] The sleep disturbance<br />
itself may consist mainly <strong>of</strong> difficulty in falling asleep, frequent nocturnal arousals, early<br />
morning wakening or a general dissatisfaction with <strong>the</strong> quality <strong>of</strong> sleep that is perceived<br />
as unrefreshing. The insomnia may be transient, short term or chronic. Pharmacological<br />
treatment is not always, or perhaps rarely, indicated. Explanation <strong>of</strong> sleep requirements,<br />
instruction in sleep hygiene, reduction in alcohol (ethanol) and [7,9] need to be<br />
considered be<strong>for</strong>e <strong>the</strong> decision is made to prescribe hypnotics.<br />
2.3 General Indications <strong>for</strong> Drug Treatment <strong>of</strong> Insomnia<br />
An international conference (National Institute <strong>of</strong> Mental Health Consensus Conference)<br />
on drugs and insomnia[10] made reasonable general recommendations <strong>for</strong> appropriate<br />
use <strong>of</strong> hypnotic drugs, based on <strong>the</strong> cause and duration <strong>of</strong> insomnia. For transient<br />
insomnia caused by disruption <strong>of</strong> circadian rhythms such as in overnight travel, rapid<br />
transit over time zones, alteration <strong>of</strong> shift work or temporary admission to hospital, an<br />
hypnotic drug with a short or moderate duration <strong>of</strong> action and few residual effects would<br />
be appropriate to use on 1 or 2 occasions. For short term insomnia resulting from<br />
temporary environmental stress, hypnotics may occasionally be indicated, but should be<br />
prescribed in low dosages <strong>for</strong> 1 or 2 weeks only, or intermittently. Chronic insomnia,<br />
which is usually secondary to o<strong>the</strong>r conditions (physical, psychiatric or psychological),<br />
presents a much greater problem. In selected cases an hypnotic may be helpful, but it<br />
should be used in minimal effective dosage, intermittently, or in short courses.<br />
2.4 Effects <strong>of</strong> <strong>Benzodiazepines</strong> on Sleep<br />
<strong>Benzodiazepines</strong> and related drugs are probably <strong>the</strong> best (as well as <strong>the</strong> most widely<br />
used) hypnotics at present available. However, in prescribing <strong>the</strong>m it is necessary to<br />
bear in mind that <strong>the</strong> sleep <strong>the</strong>y induce differs from natural sleep.<br />
<strong>Benzodiazepines</strong> in general hasten sleep onset, decrease nocturnal awakenings, increase<br />
total sleeping time and <strong>of</strong>ten impart a sense <strong>of</strong> deep, refreshing sleep. However, <strong>the</strong>y<br />
alter <strong>the</strong> normal sleep pattern: Stage 2 (light sleep) is prolonged and mainly accounts<br />
<strong>for</strong> <strong>the</strong> increased sleeping time, while <strong>the</strong> duration <strong>of</strong> slow wave sleep (SWS) and rapid<br />
eye movement sleep (REMS) may be considerably reduced. The onset <strong>of</strong> <strong>the</strong> first REMS<br />
episode is delayed and dreaming is diminished. These effects <strong>of</strong> benzodiazepines have<br />
been well studied.[11-13] The abnormal sleep pr<strong>of</strong>ile probably results from unselective<br />
depression <strong>of</strong> both arousal and sleep mechanisms in <strong>the</strong> brainstem. The suppression <strong>of</strong><br />
REMS may initially be helpful in decreasing nightmares, but may also be an important<br />
factor in determining rebound insomnia in drug withdrawal (see section 2.5.2).<br />
The typical changes in sleep stages occur with most benzodiazepines in most patients,<br />
but individual variations in response are considerable and are influenced by dosage,<br />
duration <strong>of</strong> treatment, type <strong>of</strong> benzodiazepine, age and clinical state. The increase in<br />
total sleeping time appears to be greatest in patients who complain <strong>of</strong> insomnia and in
those with short baseline sleep duration. However, patients with insomnia tend to<br />
overestimate both <strong>the</strong>ir baseline degree <strong>of</strong> sleep disturbance and <strong>the</strong> efficacy <strong>of</strong> hypnotic<br />
drugs.[14]<br />
2.5 Disadvantages <strong>of</strong> Benzodiazepine Hypnotics<br />
2.5.1 Tolerance<br />
<strong>Benzodiazepines</strong> are initially very, efficacious in inducing and prolonging sleep. However,<br />
tolerance to <strong>the</strong> hypnotic effects develops rapidly, sometimes after only a few days <strong>of</strong><br />
regular use.[15,16] Sleep latency, Stage 2 sleep, SWS, REMS and intrasleep awakenings<br />
all tend to return to pretreatment levels after a few weeks.[11,12,16-18] Never<strong>the</strong>less,<br />
poor sleepers may report continued efficacy without escalation <strong>of</strong> dosage[19] and <strong>the</strong><br />
drugs are <strong>of</strong>ten used long term, possibly because <strong>of</strong> difficulties in withdrawal.<br />
Tolerance to o<strong>the</strong>r effects <strong>of</strong> benzodiazepines does not necessarily develop at <strong>the</strong> same<br />
rate as to <strong>the</strong> hypnotic actions. Thus, tolerance to <strong>the</strong> anxiolytic effects appears to<br />
develop more slowly (see section 3.4.1), while complete tolerance to some psychomotor<br />
and cognitive functions may never develop. [20,21]<br />
2.5.2 Rebound Insomnia<br />
Rebound insomnia, in which sleep is poorer than be<strong>for</strong>e drug treatment, is common on<br />
withdrawal <strong>of</strong> benzodiazepines. It is most marked when <strong>the</strong> drugs have been taken<br />
regularly <strong>for</strong> long periods, but can occur after only 1 week <strong>of</strong> low dose<br />
administration.[l6,l8,22,23] Sleep latency is prolonged, intrasleep wakenings become<br />
more frequent, REMS duration and intensity is increased with vivid dreams or<br />
nightmares that may add to frequent awakenings.<br />
Rebound insomnia is conspicuous with moderately rapidly eliminated benzodiazepines<br />
(lorazepam, temazepam) and may last <strong>for</strong> weeks in some patients.[24] With rapidly<br />
eliminated benzodiazepines (triazolam), rebound effects may occur in <strong>the</strong> latter part <strong>of</strong><br />
<strong>the</strong> night and cause early morning waking and daytime anxiety.[25] With slowly<br />
eliminated benzodiazepines (nitrazepam, diazepam), SWS and REMS may remain<br />
depressed <strong>for</strong> some weeks and <strong>the</strong>n slowly return to baseline, sometimes without a<br />
rebound. Rebound effects, when <strong>the</strong>y occur, encourage continued hypnotic usage and<br />
contribute to <strong>the</strong> development <strong>of</strong> hypnotic dependence.<br />
2.5.3 Hangover Effects<br />
Benzodiazepine hypnotics <strong>of</strong>ten give rise to subjective hangover. After most <strong>of</strong> <strong>the</strong>m,<br />
even those that are rapidly eliminated (eg triazolam), psychomotor per<strong>for</strong>mance and<br />
memory may be impaired <strong>the</strong> next day.[26] However, <strong>the</strong>re is considerable<br />
interindividual variation.[27] The effects also differ between different benzodiazepines,<br />
and with dosage and duration <strong>of</strong> administration.[28]<br />
Residual effects are most likely to occur with slowly eliminated benzodiazepines,<br />
especially if used long term, and are most marked in <strong>the</strong> elderly. Thus, nitrazepam<br />
commonly produces a subjective feeling <strong>of</strong> hangover and impairs per<strong>for</strong>mance <strong>the</strong> next<br />
day in single or repeated doses[28,29] although subjective effects may decrease as<br />
tolerance develops. Diazepam (5 and 10mg) was shown to produce few residual effects<br />
when used in single doses or intermittently,[27] although long term use impairs daytime<br />
per<strong>for</strong>mance.
It is probably an individual matter whe<strong>the</strong>r per<strong>for</strong>mance <strong>the</strong> next morning is likely to be<br />
more impaired by lack <strong>of</strong> sleep or by an hypnotic agent. For transient or short term<br />
insomnia. many patients prefer to use an hypnotic ra<strong>the</strong>r than to have a sleepless night.<br />
Daytime sleepiness resulting from chronic insomnia can itself have adverse effects,[30]<br />
but regular hypnotic use does not usually provide a satisfactory long term solution.<br />
Treatment is better directed, where possible, towards its underlying cause.<br />
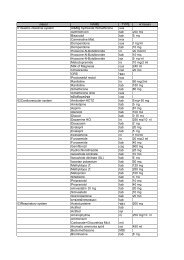
Table II. <strong>Rational</strong> use <strong>of</strong> benzodiazepines in insomnia. Recommended drugs include<br />
temazepam, lormetazepam, loprazolam and diazepam (occasionally in single doses). It is<br />
important to warn patients <strong>of</strong> possible residual effects, risks associated with driving,<br />
interactions with alcohol (ethanol) and o<strong>the</strong>r depressants, danger <strong>of</strong> dependence with<br />
regular use and possible withdrawal effects.<br />
Type <strong>of</strong> insomnia<br />
Dosage and administration<br />
General cases<br />
Transient insomnia (e.g. disruption <strong>of</strong><br />
circadian rhythm)<br />
Short term insomnia (e.g. temporary<br />
environmental stress)<br />
Chronic insomnia (e.g. secondary to<br />
physical, psychological or psychiatric<br />
causes)<br />
1-2 nights only. Minimal dosage (usually not more than diazepam 2-5mg or<br />
equivalent)<br />
Not <strong>for</strong> more than 2 weeks. Intermittent if possible (1 night in 2 or 3 nights).<br />
Minimal effective dosage (start with small dose; increase if needed, usually not<br />
more than diazepam 10mg or equivalent.<br />
Treat primary cause first. Intermittent treatment if possible. Not more than 2<br />
weeks (course may be repeated after an interval). Minimal effective dosage (as<br />
above).<br />
Special cases<br />
Elderly patients[a]<br />
Children<br />
Pregnancy and lactation<br />
Disease states<br />
Benzodiazepine dependent patients[a]<br />
<strong>Use</strong> half adult doses<br />
Generally contraindicated, but single dose may be effective.<br />
Avoid regular use in pregnancy, occasional use safe during lactation.<br />
Avoid in chronic respiratory disease. May occasionally be indicated in o<strong>the</strong>r<br />
disease states is if insomnia distressing.<br />
Gradual withdrawal possible and may improve sleep but withdrawal should not be<br />
<strong>for</strong>ced.<br />
2.5.4 Dependence<br />
[a] Continued long term use may sometimes be necessary.<br />
Dependence on benzodiazepine hypnotics can develop if <strong>the</strong> drugs are taken regularly<br />
<strong>for</strong> several weeks.[4] Many long term users are reluctant to withdraw <strong>the</strong> drugs because<br />
<strong>of</strong> rebound insomnia. Withdrawal from benzodiazepine hypnotics in dependent users may<br />
also give rise to anxiety and o<strong>the</strong>r typical withdrawal symptoms.[31-35]<br />
2.5.5 Respiratory Depression
<strong>Benzodiazepines</strong> can cause respiratory depression and decrease <strong>the</strong> ventilatory response<br />
to hypercapnia[34] and increase hypopnoeic episodes during; sleep.[35] Like o<strong>the</strong>r<br />
drugs which depress respiration <strong>the</strong>y should be avoided in patients with severe chronic<br />
obstructive airways disease.<br />
2.6 Choice <strong>of</strong> Benzodiazepine Hypnotic<br />
For an hypnotic drug, a rapid onset combined with a medium duration <strong>of</strong> action is usually<br />
desirable. Temazepam, loprazolam and lormetazepam meet <strong>the</strong>se criteria (Table II).<br />
Temazepam tablets act as rapidly as when <strong>the</strong> drug is administered in s<strong>of</strong>t gelatine<br />
capsules. The tablets also have less abuse potential and can be cut in half to minimise<br />
dosage.<br />
Rapidly eliminated benzodiazepines, such as triazolam, can impair memory <strong>the</strong> next<br />
day,[26,28] give rise to daytime anxiety,[25] and probably carry a greater dependence<br />
risk.[1] Oxazepam is not recommended as it has a relatively slow onset <strong>of</strong> action.<br />
Nitrazepam is only slowly eliminated. Diazepam acts rapidly and, although slowly<br />
eliminated, does not have a prolonged action when used in single doses.<br />
Doses should be minimised to avoid residual effects (especially important <strong>for</strong> drivers,<br />
airline pilots, and machinery operators) and <strong>the</strong> patient should be warned about additive<br />
effects with alcohol and o<strong>the</strong>r depressants. Recommended dosage schedules are shown<br />
in Table II.<br />
2.6.1 The Elderly<br />
The elderly are especially vulnerable to adverse effects <strong>of</strong> hypnotic drugs. Rates <strong>of</strong><br />
metabolism <strong>of</strong> benzodiazepines that are oxidised (diazepam, nitrazepam) decline with<br />
age.[35,36] Elderly patients are also more susceptible to CNS depression and may<br />
develop confusional states and ataxia, leading to falls and fractures.[37] They are<br />
sensitive to respiratory depression and prone to sleep apnoea and o<strong>the</strong>r sleep<br />
disorders.[38]<br />
However, insomnia is particularly common in this age group and regular hypnotics may<br />
sometimes be indicated if sleep disturbance is distressing. Temazepam, lormetazepam<br />
and loprazolam (which do not have pharmacologically active metabolites) remain<br />
suitable choices. but dosage should be adjusted, usually to half <strong>the</strong> recommended adult<br />
dose.<br />
2.6.2 The Young<br />
Hypnotics are generally contraindicated <strong>for</strong> children. Sedative antihistamines are<br />
commonly used if sedation is required, but a single dose <strong>of</strong> a benzodiazepine, with<br />
suitable dosage reduction, may be more effective.<br />
2.6.3 Pregnancy and Lactation<br />
Regular use <strong>of</strong> hypnotics in pregnancy is contraindicated as <strong>the</strong> drugs readily traverse<br />
<strong>the</strong> placenta. Intermittent doses <strong>of</strong> relatively rapidly eliminated benzodiazepines have<br />
been shown to be safe during breastfeeding.<br />
2.6.4 Disease States<br />
<strong>Benzodiazepines</strong> are rarely helpful in insomnia due to organic disease and may depress<br />
respiration in chronic pulmonary disease. However, in terminal conditions, <strong>the</strong> possibility
<strong>of</strong> drug dependence becomes less important and regular use <strong>of</strong> hypnotics should not be<br />
denied if <strong>the</strong>y provide symptomatic relief.<br />
2.6.5 Withdrawal <strong>of</strong> Benzodiazepine Hypnotics<br />
Many patients who have taken benzodiazepine hypnotics nightly <strong>for</strong> years can have <strong>the</strong><br />
drugs withdrawn successfully (see section 3.5.2). Often <strong>the</strong>re is surprisingly little sleep<br />
disturbance if withdrawal is carried out sufficiently slowly. Many patients find <strong>the</strong>y<br />
actually sleep better without <strong>the</strong> drugs. The use <strong>of</strong> liquid preparations <strong>of</strong> temazepam,<br />
nitrazepam or diazepam facilitates small dosage reductions. However, unmotivated<br />
patients (<strong>of</strong>ten elderly patients who have taken hypnotics <strong>for</strong> years) should not be <strong>for</strong>ced<br />
to withdraw <strong>the</strong>se agents against <strong>the</strong>ir will simply because <strong>the</strong>y are dependent. Long<br />
term prescriptions (in minimal dosage) are sometimes necessary.<br />
2.6.6 Alternatives to <strong>Benzodiazepines</strong><br />
<strong>Benzodiazepines</strong> compare favourably with o<strong>the</strong>r hypnotics in efficacy and safety. They<br />
have fewer adverse effects than chlormethiazole and chloral derivatives and are more<br />
efficacious than sedative antihistamines.[4] Zopiclone, which has a similar mechanism <strong>of</strong><br />
action, is expensive and is not free <strong>of</strong> dependence liability and o<strong>the</strong>r adverse<br />
effects.[39,40] Although antidepressants and antipsychotics may improve sleep in<br />
patients with depression or psychosis, <strong>the</strong>y are more toxic than benzodiazepines and<br />
should not be used as general hypnotics, but reserved <strong>for</strong> patients with disorders <strong>for</strong><br />
which <strong>the</strong>se drugs are specifically indicated.<br />
3. <strong>Rational</strong> <strong>Use</strong> <strong>of</strong> <strong>Benzodiazepines</strong> <strong>for</strong> Anxiety<br />
Official recommendations on <strong>the</strong> use <strong>of</strong> benzodiazepines in anxiety are similar to those<br />
<strong>for</strong> insomnia. The UK Committee on Safety <strong>of</strong> Medicines[2] advised that <strong>the</strong>y 'are<br />
indicated <strong>for</strong> <strong>the</strong> short term relief (2-4 weeks only) <strong>of</strong> anxiety that is severe, disabling or<br />
causing unacceptable distress'. To a considerable extent this advice appears to have<br />
been heeded and yearly prescriptions <strong>for</strong> benzodiazepine anxiolytics have decreased in<br />
<strong>the</strong> UK from a peak <strong>of</strong> 18 million in 1978 to less than 10 million at present. There is no<br />
doubt that benzodiazepines can be highly efficacious in anxiety. The indications <strong>for</strong> <strong>the</strong>ir<br />
rational use in different types <strong>of</strong> anxiety disorders have become clearer in recent years.<br />
[41,42]<br />
3.1 Prevalence <strong>of</strong> Anxiety<br />
Anxiety symptoms are common in <strong>the</strong> general population. Uhlenuth et al.[43] estimated<br />
<strong>the</strong> prevalence <strong>of</strong> generalised anxiety disorder among US adults to be 6.4%, while<br />
ano<strong>the</strong>r 3.5% experienced panic, agoraphobia and o<strong>the</strong>r phobias. Prevalence (<strong>of</strong>ten<br />
elderly patients who have taken hypnotics <strong>for</strong> years) should not be <strong>for</strong>ced to withdraw<br />
<strong>the</strong>se agents against <strong>the</strong>ir will simply because <strong>the</strong>y are dependent. Long term<br />
prescriptions (in minimal dosage) are sometimes necessary.<br />
3.2 Classification <strong>of</strong> Anxiety<br />
There is still some controversy about how anxiety states should be classified. Anxiety<br />
disorders recognised on <strong>the</strong> DSM-III-R criteria [45] include generalised anxiety disorder,<br />
panic disorder, agoraphobic disorder, social phobia, simple phobia and post-traumatic<br />
stress disorder. Generalised anxiety is <strong>the</strong> most common <strong>of</strong> <strong>the</strong> disorders, but Tyrer<br />
[46,47] stresses <strong>the</strong> considerable overlap <strong>of</strong> symptoms between different anxiety<br />
disorders, as well as <strong>the</strong> co-occurrence <strong>of</strong> depressive symptoms. He argues <strong>for</strong> a simple<br />
descriptive term, <strong>the</strong> generalised neurotic syndrome, to encompass most categories.
Acute stress reactions and post-traumatic stress disorder, which may persist as<br />
adjustment disorders, are clearly precipitated by major life events, but <strong>the</strong> reasons <strong>for</strong><br />
anxiety in generalised anxiety disorder, panic and phobias is usually not known.[47]<br />
Vulnerability to stress may be linked with genetic factors[48] and environmental<br />
influences. Most patients with anxiety symptoms have a long history <strong>of</strong> high anxiety<br />
levels going back to childhood.<br />
Management <strong>of</strong> anxiety conditions, however classified or caused, usually calls <strong>for</strong><br />
nondrug measures that may range from simple counselling to specific psychological<br />
techniques. The latter may include anxiety management training, behaviour or cognitive<br />
<strong>the</strong>rapy. Drug treatment may also be indicated and <strong>the</strong> range <strong>of</strong> effective drugs includes<br />
benzodiazepines, antidepressants, antipsychotics and (฿-blockers, each with its own<br />
advantages, disadvantages and specific indications.[47] Possible alternatives include<br />
buspirone and some newer anxiolytics likely to be introduced soon (alpidem, suriclone<br />
and o<strong>the</strong>rs).[49,50]<br />
3.3 Effects <strong>of</strong> <strong>Benzodiazepines</strong> on Anxiety<br />
<strong>Benzodiazepines</strong> are potent anxiolytic agents and are effective both in o<strong>the</strong>rwise-healthy<br />
patients undergoing stress and in anxious patients. Anxiolytic effects are exerted in<br />
doses that cause minimal sedation, although <strong>the</strong> hypnotic, muscular relaxant and<br />
perhaps amnesic actions may all contribute to relief <strong>of</strong> associated tension and insomnia.<br />
The relatively selective effect on anxiety is probably related to <strong>the</strong> fact that<br />
benzodiazepines suppress activity in many limbic and o<strong>the</strong>r brain areas involved in<br />
anxiogenesis, including <strong>the</strong> septal area, amygdala, hippocampus, hypothalamus, locus<br />
coeruleus and raph◌้ nuclei. They also decrease <strong>the</strong> turnover <strong>of</strong> acetylcholine,<br />
norepinephrine (noradrenaline), serotonin (5-hydroxy-tryptamine, 5-HT) and dopamine<br />
in <strong>the</strong>se areas.[51] Suppression <strong>of</strong> noradrenergic and/or serotonergic pathways appears<br />
to be <strong>of</strong> particular importance in relation to anxiolytic effects.<br />
The major clinical advantage <strong>of</strong> benzodiazepines as anxiolytics is <strong>the</strong> rapid onset <strong>of</strong><br />
action, usually apparent after a single dose. This immediate effect contrasts with <strong>the</strong><br />
delayed anxiolytic effects <strong>of</strong> antidepressants, buspirone and psychological treatments. In<br />
addition, benzodiazepines are relatively non-toxic and safer than most <strong>of</strong> <strong>the</strong> alternative<br />
drugs. Their immediate efficacy and safety combine to make benzodiazepines <strong>the</strong> drugs<br />
<strong>of</strong> first choice <strong>for</strong> rapid relief <strong>of</strong> anxiety that is unacceptably distressing, whatever <strong>the</strong><br />
cause.<br />
As in insomnia, benzodiazepines provide only symptomatic treatment <strong>for</strong> anxiety; <strong>the</strong>y<br />
do not cure <strong>the</strong> underlying disorder. Never<strong>the</strong>less <strong>the</strong>y can provide valuable short term<br />
cover, allowing time <strong>for</strong> more specific treatments to take effect, and can alleviate<br />
exacerbations <strong>of</strong> anxiety which are <strong>of</strong>ten self-limiting.<br />
3.4 Disadvantages <strong>of</strong> Benzodiazepine Anxiolytics<br />
3.4.1 Tolerance<br />
Tolerance to <strong>the</strong> anxiolytic effects <strong>of</strong> benzodiazepines seems to develop more slowly and<br />
less completely than to <strong>the</strong> hypnotic effects. There is, however, little evidence that <strong>the</strong>y<br />
retain <strong>the</strong>ir effectiveness after 4 months <strong>of</strong> regular treatment.[52,53] While some<br />
studies indicate that anxiolytic effects are maintained <strong>for</strong> at least 22 weeks in chronic<br />
anxiety states,[54] clinical observations <strong>of</strong> long term recipients <strong>of</strong> <strong>the</strong>se agents suggest<br />
that <strong>the</strong> prolonged benzodiazepine use over years does little to control and may even<br />
aggravate anxiety states.[55]
The question remains controversial.[44,56] but <strong>the</strong>re is general agreement that<br />
benzodiazepine use in most anxiety states should be limited where possible to short<br />
term (ideally not more than 4 weeks) or intermittent courses.[2,41,42,47]<br />
3.4.2 Psychomotor Impairment<br />
Subjective oversedation is not usually a problem with anxious patients, but <strong>the</strong> drugs<br />
can impair psychomotor per<strong>for</strong>mance, increasing <strong>the</strong> risk <strong>of</strong> traffic and o<strong>the</strong>r accidents,<br />
especially when combined with alcohol. Memory lapses may lead to uncharacteristic<br />
behaviours such as shoplifting.[57,58] <strong>Benzodiazepines</strong>, by inhibiting learning, may<br />
decrease <strong>the</strong> effectiveness <strong>of</strong> psychological <strong>the</strong>rapies.[59] Although judicious short term<br />
administration <strong>of</strong> benzodiazepines can improve psychomotor per<strong>for</strong>mance by<br />
counteracting <strong>the</strong> disruptive effects <strong>of</strong> anxiety, long term users <strong>of</strong> normal <strong>the</strong>rapeutic<br />
dosages show cognitive deficits, especially in visuospatial and learning ability.[21]<br />
3.4.3 Disinhibition, Paradoxical Effects<br />
Occasionally benzodiazepines produce paradoxical stimulation. This effect is most<br />
marked in anxious patients[60] and in children. Symptoms may include excitement,<br />
increased anxiety, irritability, hostility and outbursts <strong>of</strong> rage, sometimes leading to<br />
violent behaviour. Although this phenomenon appears to be rare,[61] it is not always<br />
clinically recognised and its true incidence may be underreported. [62]<br />
3.4.4 Affective Reactions<br />
Long term use <strong>of</strong> benzodiazepines can cause or aggravate depression, a possible risk in<br />
patients with mixed anxiety/depression, and suicidal tendencies may be increased.[60]<br />
Some patients complain <strong>of</strong> 'emotional anaes<strong>the</strong>sia', while some obtain a degree <strong>of</strong><br />
euphoria. A minority <strong>of</strong> anxious patients escalate <strong>the</strong>ir dosage to <strong>the</strong> point <strong>of</strong> abuse, and<br />
benzodiazepines have become popular among illicit drug abusers who take <strong>the</strong>m in<br />
addition to <strong>the</strong>ir o<strong>the</strong>r drugs <strong>of</strong> abuse.<br />
3.4.5 Dependence<br />
Long term use <strong>of</strong> benzodiazepines carries an undisputed risk <strong>of</strong> inducing dependence.<br />
Approximately 35% <strong>of</strong> patients taking benzodiazepines <strong>for</strong> more than 4 weeks develop<br />
dependence as evidenced by <strong>the</strong> appearance <strong>of</strong> withdrawal symptoms if dosage is<br />
reduced or <strong>the</strong> drugs are stopped.[63] Factors increasing <strong>the</strong> risk <strong>of</strong> dependence include<br />
high dosage, regular continuous use, dependent personality characteristics and previous<br />
drug dependence. [1,53,64]<br />
3.5 Choice and <strong>Use</strong> <strong>of</strong> <strong>Benzodiazepines</strong> in Anxiety<br />
Despite <strong>the</strong> drawbacks <strong>of</strong> long term use, benzodiazepines remain valuable in <strong>the</strong> short<br />
term management <strong>of</strong> anxiety, especially where immediate action is required. In most<br />
cases, diazepam is <strong>the</strong> drug <strong>of</strong> choice, since onset <strong>of</strong> action is rapid, while slow<br />
elimination protects against major fluctuations in blood concentration. Potent<br />
benzodiazepines such as lorazepam and alprazolam have been widely used <strong>for</strong> anxiety,<br />
but are probably inappropriate. These drugs are relatively quickly eliminated and<br />
interdose anxiety frequently occurs.[65] Lack <strong>of</strong> recognition <strong>of</strong> <strong>the</strong> high potency <strong>of</strong> <strong>the</strong>se<br />
drugs relative to diazepam (Table 1) has <strong>of</strong>ten led to excessive dosages, increasing <strong>the</strong><br />
risk <strong>of</strong> adverse effects, dependence and problems in withdrawal.<br />
<strong>Guidelines</strong> <strong>for</strong> benzodiazepine use in various types <strong>of</strong> anxiety are provided by Tyrer,[47]<br />
Consensus Conference,[41] and Russell and Lader[42] among o<strong>the</strong>rs. Single doses may
e appropriate as prophylaxis against acute stress reactions in predictably stressful<br />
situations (e.g. air travel, dental appointments in phobic patients), although<br />
psychological <strong>the</strong>rapies are preferable in <strong>the</strong> long run.<br />
Similarly. very short term treatment (1 to 7 days) may be indicated in stress reactions<br />
after catastrophic events (natural disasters, accidents), which have a high rate <strong>of</strong><br />
spontaneous resolution. <strong>Benzodiazepines</strong> are not usually recommended after<br />
bereavement as <strong>the</strong>y may impair <strong>the</strong> adjustment to grief, but a few days' use may<br />
sometimes be justified. The drugs are probably not suitable <strong>for</strong> adjustment disorders and<br />
post-traumatic stress disorders that can persist <strong>for</strong> many months; psychological<br />
treatments are preferable in <strong>the</strong>se cases.<br />
Intermittent treatment in courses <strong>of</strong> 2 to 4 weeks can be <strong>of</strong> value in episodic anxiety<br />
<strong>of</strong>ten associated with fluctuations in chronic generalised anxiety. Similarly a short course<br />
(2 to 4 weeks) <strong>of</strong> benzodiazepines may be indicated <strong>for</strong> <strong>the</strong> immediate relief <strong>of</strong> anxiety in<br />
generalised anxiety disorder, but <strong>the</strong> longer <strong>the</strong> duration <strong>of</strong> <strong>the</strong>rapy <strong>the</strong> less <strong>the</strong> benefit<br />
and <strong>the</strong> greater <strong>the</strong> disadvantages. In <strong>the</strong>se cases benzodiazepines are best combined<br />
with longer term treatments such as antidepressant drugs and/or psychological<br />
<strong>the</strong>rapies.<br />
Long term treatment over months or years has been much used in <strong>the</strong> past <strong>for</strong> chronic<br />
generalised anxiety disorder. However, Rickels et al.[54] found that most patients with<br />
chronic anxiety remained symptom-free <strong>for</strong> at least several months after a course <strong>of</strong><br />
diazepam lasting 22 weeks, and in 37% <strong>the</strong>re was no recrudescence <strong>of</strong> anxiety within a<br />
year. Similar sustained improvement was noted after a shorter 6-week course <strong>of</strong><br />
diazepam. The authors concluded that intermittent ra<strong>the</strong>r than long term benzodiazepine<br />
<strong>the</strong>rapy is preferable in most cases.<br />
A course <strong>of</strong> 2 to 4 weeks' medication followed by tapering over 1 to 2 weeks, and<br />
temporary restitution <strong>of</strong> treatment only if anxiety symptoms recur, is probably rational.<br />
Nondrug <strong>the</strong>rapies should be <strong>of</strong>fered. However, <strong>the</strong>re remains a small core <strong>of</strong> patients<br />
who fail to benefit from psychological and o<strong>the</strong>r <strong>the</strong>rapies and, <strong>for</strong> <strong>the</strong>se patients,<br />
prolonged treatment, combined with general support, may be <strong>the</strong> only practical option.<br />
3.5.1 Panic Disorder and Phobias<br />
There is a divergence <strong>of</strong> opinion over <strong>the</strong> use <strong>of</strong> benzodiazepines in panic disorder,<br />
agoraphobia and o<strong>the</strong>r phobias. Alprazolam, lorazepam, diazepam and clonazepam have<br />
been widely used <strong>for</strong> <strong>the</strong>se disorders.[66-72] Some <strong>of</strong> <strong>the</strong>se studies and o<strong>the</strong>rs reviewed<br />
by Marks and O'Sullivan[73] and Tyrer[47] have compared <strong>the</strong> efficacy <strong>of</strong><br />
benzodiazepines with that <strong>of</strong> antidepressants and o<strong>the</strong>r treatments.<br />
Most investigations have shown that high doses <strong>of</strong> benzodiazepines (e.g. as much as 6<br />
to 10mg alprazolam daily) can be effective. They have a rapid onset <strong>of</strong> action and<br />
improvement with benzodiazepines, compared with antidepressants, is greater in <strong>the</strong><br />
first 4 to 5 weeks <strong>of</strong> treatment, but is not superior after 5 to 6 weeks. Tyrer [47]<br />
concludes from <strong>the</strong> available evidence that 'monoamine oxidase inhibitors, tricyclic<br />
antidepressants, and benzodiazepines are all effective in <strong>the</strong> treatment <strong>of</strong> panic with a<br />
hierarchy <strong>of</strong> efficacy headed by MAOIs with benzodiazepines as <strong>the</strong> least effective'.<br />
Since cessation <strong>of</strong> pharmacological treatment in panic disorders and agoraphobia is<br />
followed by relapse in over 80% <strong>of</strong> cases, [66] <strong>the</strong>re is a tendency to use <strong>the</strong> drugs long<br />
term. However, long term use <strong>of</strong> benzodiazepines, especially in high dosages, carries <strong>the</strong><br />
disadvantages <strong>of</strong> inducing dependence, tolerance withdrawal reactions if <strong>the</strong> drugs are<br />
stopped,[1] increased anger/hostility,[74] cognitive impairment[21] and o<strong>the</strong>r adverse<br />
effects mentioned in section 3.4. There is evidence that psychological treatments, such
as exposure <strong>the</strong>rapy (supervised. gradually increasing exposure to <strong>the</strong> specific anxiety or<br />
panic-provoking situations), can decrease relapses and improve <strong>the</strong> long term outcome,<br />
but benzodiazepines appear to interfere with such treatments.[59,73]<br />
For <strong>the</strong>se reasons <strong>the</strong> consensus <strong>of</strong> current opinion in much <strong>of</strong> Europe and Australasia is<br />
that antidepressant drugs combined with psychological <strong>the</strong>rapies are in <strong>the</strong> long run<br />
superior to benzodiazepines <strong>for</strong> panic disorder, agoraphobia and o<strong>the</strong>r<br />
phobias.[47,53,73,75] In North America, <strong>the</strong>re may be less concern about long term<br />
benzodiazepine use <strong>for</strong> <strong>the</strong>se conditions. Never<strong>the</strong>less, it would seem more logical to<br />
reserve benzodiazepines <strong>for</strong> short term initial cover if panic is severe and disabling, while<br />
awaiting <strong>the</strong> delayed effects <strong>of</strong> o<strong>the</strong>r treatments.<br />
Fur<strong>the</strong>rmore, panic and agoraphobia may coexist with generalised anxiety as part <strong>of</strong> <strong>the</strong><br />
general neurotic syndrome. In <strong>the</strong>se cases, intermittent use <strong>of</strong> benzodiazepines may be<br />
combined with antidepressants and psychological <strong>the</strong>rapies.[47] The observation that<br />
low dose intranasal midazolam taken at <strong>the</strong> first sign <strong>of</strong> panic may abort <strong>the</strong> attack[76]<br />
may <strong>of</strong>fer a fur<strong>the</strong>r use <strong>of</strong> benzodiazepines in panic disorder, but confirmation <strong>of</strong> <strong>the</strong><br />
efficacy and safety <strong>of</strong> this treatment is needed.<br />
<strong>Benzodiazepines</strong> are not suitable <strong>for</strong> obsessive-compulsive disorder and should be<br />
avoided where possible in depression, or in <strong>the</strong> presence <strong>of</strong> significant depressive<br />
symptoms. Alprazolam is claimed to have antidepressant properties[77]and is effective<br />
in secondary depression associated with anxiety[78] but carries a high risk <strong>of</strong><br />
dependence and o<strong>the</strong>r adverse effects, especially when used long term.<br />
3.5.2 Withdrawal <strong>of</strong> <strong>Benzodiazepines</strong><br />
There remains a large population <strong>of</strong> patients, numbering over a million in <strong>the</strong> UK[5,79]<br />
who have taken benzodiazepines <strong>for</strong> many months or years. Many <strong>of</strong> <strong>the</strong>se suffer from<br />
symptoms included in <strong>the</strong> general neurotic syndrome (chronic anxiety, panic attacks,<br />
agoraphobia, depression). Slow withdrawal <strong>of</strong> benzodiazepines is a practical option <strong>for</strong><br />
motivated patients. Withdrawal symptoms, when <strong>the</strong>y occur, are mainly those <strong>of</strong><br />
increased anxiety, although some perceptual and motor disturbances may be especially<br />
prominent.[1]<br />
The management <strong>of</strong> benzodiazepine withdrawal consists <strong>of</strong> gradual dosage reduction<br />
combined with appropriate psychological support. The rate <strong>of</strong> dosage tapering should be<br />
tailored to individual needs, and best results are usually obtained in an outpatient setting<br />
with <strong>the</strong> patient in control <strong>of</strong> <strong>the</strong> rate <strong>of</strong> withdrawal and proceeding at whatever pace is<br />
found to be tolerable. The process may take 2 to 3 months in some patients or up to a<br />
year in o<strong>the</strong>rs.<br />
Typical dosage reductions <strong>for</strong> a patient taking 20mg diazepam (or equivalent) daily<br />
would be 1mg every 1 to 2 weeks initially, followed by decrements <strong>of</strong> 0.5mg every 1 to 2<br />
weeks when a dosage <strong>of</strong> 4 to 5mg has been reached. Initial dosage reductions <strong>of</strong> 2mg<br />
every 1 to 2 weeks may be more appropriate <strong>for</strong> patients taking over 20mg diazepam<br />
equivalent daily. No adjuvant drugs have been found to be generally helpful in alleviating<br />
withdrawal symptoms, but antidepressants may be indicated <strong>for</strong> depression and ฿-<br />
blockers are useful <strong>for</strong> some patients with prominent somatic symptoms.<br />
The degree <strong>of</strong> psychological support required is also an individual matter and may range<br />
from simple encouragement to <strong>for</strong>mal anxiety management or cognitive and behavioural<br />
<strong>the</strong>rapy. Support should be available not only during dosage reduction, but also <strong>for</strong> a<br />
prolonged period afterwards. Frequent contact with <strong>the</strong> physician or o<strong>the</strong>r <strong>the</strong>rapist or<br />
counsellor is <strong>of</strong>ten desirable throughout withdrawal and post-withdrawal phases.
In <strong>the</strong> majority <strong>of</strong> cases, symptoms gradually improve after withdrawal [55,80] although<br />
some patients may need fur<strong>the</strong>r temporary courses <strong>of</strong> benzodiazepines.[81] For those<br />
unwilling to withdraw or who find withdrawal symptoms intolerable, and <strong>for</strong> those in<br />
whom withdrawal is likely to incur more serious problems, such as alcohol<br />
dependence,[1] continued prescribing in minimal doses may be necessary.<br />
Table III. <strong>Rational</strong> use <strong>of</strong> benzodiazepines in anxiety. Recommended agent is diazepam<br />
in most cases. Minimal effective dosage may vary from 5 to 30mg daily; usually best<br />
given divided twice daily. Start with a small dose and increase if necessary. It is<br />
important to warn patients <strong>of</strong> sedative effects, risks associated with driving, interactions<br />
with alcohol and o<strong>the</strong>r depressants, danger <strong>of</strong> dependence with regular use and possible<br />
withdrawal effects<br />
Anxiety state Duration <strong>of</strong> treatment O<strong>the</strong>r treatments<br />
Mild anxiety<br />
Acute stress reaction prophylaxis (e.g.<br />
dental appointments, aeroplane travel in<br />
patients with phobias)<br />
<strong>Benzodiazepines</strong> not recommended<br />
Single dose be<strong>for</strong>e event<br />
Counselling,<br />
psychological treatment<br />
Psychological treatment<br />
Acute stress reaction<br />
(accidents/disasters)<br />
1-7 days Counselling<br />
Acute stress reaction (bereavement)<br />
Adjustment disorders; post-traumatic<br />
stress<br />
Episodic anxiety<br />
Chronic generalised anxiety[a]<br />
General neurotic syndrome[a]<br />
Panic disorder[a]<br />
Agoraphobia[a]<br />
O<strong>the</strong>r phobias<br />
Benzodiazepine-dependent patients[a]<br />
Single doses or a few days only if distress is severe<br />
Single doses or a few days only initially - not suitable <strong>for</strong> long term<br />
management<br />
Single or intermittent courses (2-4 weeks followed by 1-2 weeks in<br />
tapering doses). <strong>Use</strong> in conjunction with o<strong>the</strong>r treatments<br />
Initial course 2-4 weeks (if symptoms severe) followed by 1-2 weeks<br />
tapering. <strong>Use</strong> in conjunction with o<strong>the</strong>r treatments as above<br />
(alprazolam not recommended in UK, especially high dose, long<br />
term, though widely used in US)<br />
Gradual withdrawal is possible and may improve anxiety symptoms,<br />
but should not be <strong>for</strong>ced. Longer term prescriptions may sometimes<br />
be necessary<br />
General support,<br />
counselling,<br />
psychological treatment<br />
Psycho<strong>the</strong>rapy<br />
Antidepressants, ฿-<br />
blockers, psychological<br />
treatment<br />
Antidepressants, ฿-<br />
blockers, psychological<br />
treatment<br />
Psychological support,<br />
antidepressants<br />
[a] Occasionally, longer term prescriptions are required <strong>for</strong><br />
patients who do not respond to o<strong>the</strong>r measures.<br />
3.5.3 Prevention <strong>of</strong> Benzodiazepine Dependence<br />
Prevention <strong>of</strong> dependence in new patients depends partly on patient selection, avoiding<br />
prescriptions where possible in patients with dependent-avoidant personalities, identified<br />
clinically as 'timid worriers'.[64] Minimal effective dosage should be used and courses<br />
kept short (4 weeks maximum whenever possible).
The risk <strong>of</strong> dependence is probably greater with potent, short-acting benzodiazepines<br />
such as lorazepam and alprazolam.[1,64,82] Monitoring <strong>of</strong> patients be<strong>for</strong>e issuing a<br />
repeat prescription is important to ensure that short term treatment does not insidiously<br />
become long term. Practitioners should also be aware that prescriptions (especially <strong>of</strong><br />
temazepam capsules) are sometimes diverted to illicit use.<br />
Recommended schedules <strong>for</strong> benzodiazepine treatment in anxiety are shown in Table III.<br />
4. <strong>Benzodiazepines</strong> as Anticonvulsants<br />
4.1 Status Epilepticus<br />
<strong>Benzodiazepines</strong> are drugs <strong>of</strong> first choice <strong>for</strong> status epilepticus and convulsions due to<br />
drug poisoning, and are effective in 80% <strong>of</strong> cases. [83] Diazepam is given intravenously<br />
or as a rectal solution. Clonazepam and lorazepam can also be given intravenously.<br />
4.2 Prophylaxis in Epilepsy<br />
Clonazepam (a 1,4-benzodiazepine) and clobazam (a 1,5-benzodiazepine) are available<br />
as oral anticonvulsant drugs. Clonazepam is effective in myoclonic and generalised<br />
absence seizures but less effective in generalised tonic-clonic seizures.[84] Clobazam is<br />
also effective in <strong>the</strong>se <strong>for</strong>ms <strong>of</strong> seizures, but is usually reserved as adjunctive <strong>the</strong>rapy in<br />
refractory epilepsy. It can also be valuable when used intermittently in epilepsy related<br />
to menstruation or in patients who have regular clusters <strong>of</strong> generalised tonic-clonic or<br />
partial seizures,[85] and as cover during changes <strong>of</strong> anticonvulsant medication. Most<br />
o<strong>the</strong>r benzodiazepines have anticonvulsant actions in varying degrees[84] and are useful<br />
in individual cases. Diazepam and chlordiazepoxide are used briefly in alcohol<br />
detoxification to prevent withdrawal seizures, fits and anxiety symptoms (but care is<br />
needed to ensure that alcohol dependence is not followed, after relapse, by alcohol plus<br />
benzodiazepine dependence).<br />
4.3 Adverse Effects<br />
<strong>Benzodiazepines</strong> are not generally suitable <strong>for</strong> <strong>the</strong> long term treatment <strong>of</strong> epilepsy<br />
because <strong>of</strong> <strong>the</strong> development <strong>of</strong> tolerance in a high proportion <strong>of</strong> patients[85] However,<br />
tolerance may be partial and some patients may continue to show a reduction in seizure<br />
frequency and/or severity.[86] Both clonazepam and clobazam may cause sedation and<br />
psychomotor impairment, although this is less marked with clobazam. These agents may<br />
also result in irritability, depression, and behaviour disturbance with aggression and<br />
hyperkinesis in children. Exacerbation <strong>of</strong> seizures may occur on withdrawal which, as<br />
with any anticonvulsant, should always be carried out slowly.[86] Indications and dosage<br />
schedules are shown in Table IV.<br />
5. O<strong>the</strong>r <strong>Use</strong>s <strong>of</strong> <strong>Benzodiazepines</strong><br />
5.1 Anaes<strong>the</strong>sia<br />
<strong>Benzodiazepines</strong> are valuable in anaes<strong>the</strong>tic practice <strong>for</strong> <strong>the</strong>ir sedative and amnesic<br />
actions.[87] Oral lorazepam and temazepam, or intramuscular midazolam are suitable<br />
<strong>for</strong> premedication and <strong>for</strong> brief procedures such as cardioversion. Midazolam can be<br />
combined with a local anaes<strong>the</strong>tic <strong>for</strong> surgical procedures, can be used intravenously <strong>for</strong><br />
induction <strong>of</strong> anaes<strong>the</strong>sia and as an infusion <strong>for</strong> patients under mechanical ventilation.<br />
Patients who have undergone benzodiazepine withdrawal can be reassured that <strong>the</strong> use<br />
<strong>of</strong> a benzodiazepine <strong>for</strong> anaes<strong>the</strong>sia will not re-establish dependence.
5.2 Motor Disorders<br />
The muscular relaxant effects <strong>of</strong> benzodiazepines can sometimes be used in a variety <strong>of</strong><br />
motor disorders.[88] These include a range <strong>of</strong> dystonias and involuntary movements,<br />
myoclonus, aki<strong>the</strong>sia, restless legs syndrome and muscle spasm associated with pain.<br />
However, tolerance develops with long term use and <strong>the</strong> drugs are not always effective<br />
and may give rise to withdrawal problems. More esoteric uses are to control muscle<br />
spasms in tetanus and rabies.<br />
Table IV. <strong>Use</strong> <strong>of</strong> benzodiazepines as anticonvulsants<br />
Indication Drug Dosage<br />
Acute treatment<br />
Status epilepticus Diazepam IV 10-20mg (5 mg/min), repeated if necessary<br />
Convulsions due to poisoning<br />
Prolonged or recurrent febrile convulsions<br />
(children)<br />
Seizure prophylaxis<br />
Myoclonic seizures<br />
Generalised absence seizures<br />
Tonic-clonic seizures<br />
Refractory epilepsy<br />
Cluster or catamenial exacerbations<br />
Detoxification from alcohol (ethanol) and<br />
o<strong>the</strong>r CNS depressants<br />
Diazepam Alternatives:<br />
clonazepam or lorazepam<br />
Diazepam<br />
Clonazepam (short term or as<br />
adjunctive <strong>the</strong>rapy)<br />
Clonazepam (short term or as<br />
adjunctive <strong>the</strong>rapy)<br />
Clonazepam (short term or as<br />
adjunctive <strong>the</strong>rapy)<br />
Clonazepam (short term or as<br />
adjunctive <strong>the</strong>rapy)<br />
Clonazepam (short term or as<br />
adjunctive <strong>the</strong>rapy)<br />
Diazepam<br />
IV infusion (max 3 mg/kg/day) PR 10mg (adult), IV<br />
PR 500 ตg/kg (repeated if necessary)<br />
PO 2-8mg<br />
PO 2-8mg<br />
PO 2-8mg<br />
PO 10-40mg<br />
PO 10-40mg<br />
PO - not more than 7 days in declining doses (also<br />
alleviates anxiety symptoms)<br />
Abbreviations: IV = intravenous; PO = oral; PR = rectal.<br />
5.3 Acute Psychoses<br />
In acute psychoses with hyperexcitability and aggressiveness (drug-induced, mania,<br />
schizophrenia), benzodiazepines in single doses or as short term <strong>the</strong>rapy may be an<br />
effective addition to antipsychotic drugs. Their value as adjunctive treatment in chronic<br />
psychosis has not been established.[89]<br />
6. The Future
With rational prescribing, benzodiazepines are likely to remain valuable drugs <strong>for</strong> many<br />
years. Total numbers <strong>of</strong> prescriptions should continue to decline as <strong>the</strong> number <strong>of</strong> long<br />
term users decreases and fewer new patients become dependent. The development <strong>of</strong><br />
partial benzodiazepine agonists/antagonists and <strong>of</strong> o<strong>the</strong>r drugs that act more selectively<br />
on different subtypes <strong>of</strong> benzodiazepine receptors may overcome some <strong>of</strong> <strong>the</strong><br />
disadvantages <strong>of</strong> <strong>the</strong>se agents.[90] However, <strong>the</strong> degree to which such drugs, if<br />
effective, are free <strong>of</strong> <strong>the</strong> problems <strong>of</strong> tolerance and dependence in long term use remains<br />
to be established.<br />
References<br />
1. Marriott S, Tyrer P. Benzodiazepine dependence: avoidance and<br />
withdrawal. Drug Saf 1993: 9: 93-103.<br />
2. Committee on Safety <strong>of</strong> Medicines. <strong>Benzodiazepines</strong>, dependence and<br />
withdrawal symptoms. Curr Probl 1988; 21.<br />
3. Royal College <strong>of</strong> Psychiatrists. Benzodiazepine, and dependence: a college<br />
statement. Bull Royal College Psychiatrists 1988; 12:107-8.<br />
4. The treatment <strong>of</strong> insomnia. [editorial). Drug Ther Bull 1990; 28: 97-9.<br />
5. Taylor D. Current usage <strong>of</strong> benzodiazepines in Britain. In: Freeman H, Rue<br />
Y, editors. The benzodiazepines in current clinical practice. London: Royal<br />
Society <strong>of</strong> Medicine Services, 1987; 13-8.<br />
6. Swift CG. Shapiro CM. Sleep and sleep problems in elderly people. BMJ<br />
1993; 306: 1468-71.<br />
7. Crook TH, Kupfer DJ, Hoch CC, et al. Treatment <strong>of</strong> sleep disorders in <strong>the</strong><br />
elderly. In: Meltzer HY, editor. Psychopharmacology: <strong>the</strong> third generation<br />
<strong>of</strong> progress. New York: Raven Press. 1987;1159-65.<br />
8. Beaumont G. The use <strong>of</strong> benzodiazepines in general practice. In:<br />
Hindmarch I, Beaumont G, Brandon S. Leonard BE. editors.<br />
<strong>Benzodiazepines</strong>: current concepts. Chichester: John Wiley & Sons, 1990;<br />
141-152.<br />
9. Espie CA. Practical management <strong>of</strong> insomnia: behavioural and cognitive<br />
techniques. BMJ 1993; 306: 509-11.<br />
10. Marks J, Nicholson AN. Drugs and insomnia. BMJ 1984; 288: 261.<br />
11. Hartman E. Long term administration <strong>of</strong> psychotropic drugs: Effects on<br />
human sleep. In: Williams RI, Karacan I, editors. Pharmacology <strong>of</strong> sleep.<br />
New York: John Wiley & Sons Inc.1976; 211-4.<br />
12. Kay DC, Blackburn .AB, Buckingham JA. Karacan I. Human pharmacology<br />
<strong>of</strong> sleep. In: Williams RL. Karacan I, editors. Pharmacology <strong>of</strong> sleep, New<br />
York: John Wiley & Sons Inc. 1976; 83-210.<br />
13. Wheatley D. Effects <strong>of</strong> drugs on sleep. In: Wheatley D, editor.<br />
Psychopharmacology <strong>of</strong> sleep. New York: Raven Press.1981; 153-76.<br />
14. Schneider-Helmert D. Overestimations <strong>of</strong> hypnotic drug effects by<br />
insomniacs - a hypo<strong>the</strong>sis. Psychopharmacology 1985; 87: 107-10.<br />
15. Petursson H, Lader MH. Benzodiazepine dependence. Br J Addict 1984; 76:<br />
133-45.<br />
16. Kales A, Scharf MB, Kales JD. Rebound insomnia: a new clinical syndrome.<br />
Science 1978; 201:1039-41.<br />
17. Adam K, Adamson L. Brezinova V, et al. Nitrazepam: Lastingly effective<br />
but trouble on withdrawal. BMJ 1976; 1: 1558-62 .<br />
18. Kales A, Soldatos CR, Bixler EO, et al. Diazepam: effects on sleep and<br />
withdrawal phenomena. J Clin Psychopharmacol 1988; 8: 340-6.<br />
19. Oswald I, French C, Adam K, et al. Benzodiazepine hypnotics remain<br />
effective <strong>for</strong> 24 weeks. BMJ 1982; 2: 860-3.<br />
20. Lucki I, Rickels K, Geller AM. Chronic use <strong>of</strong> benzodiazepines and<br />
psychomotor and cognitive test per<strong>for</strong>mance. Psychopharmacology 1986;<br />
88: 426-33.
21. Lader M. Long-term benzodiazepine use and psychological functioning. In:<br />
Freeman H, Rue Y, editors. The benzodiazepines in current clinical<br />
practice. International Congress and Symposium Series, Royal Society <strong>of</strong><br />
Medicine Services. London and New York, 1987; 55-69.<br />
22. Nicholson AN. Hypnotics: rebound insomnia and residual sequelae. Br J<br />
Clin Pharmacol 1980; 9: 223-5.<br />
23. Nicholson AN. The use <strong>of</strong> short and long-acting hypnotics in clinical<br />
medicine. Br J Clin Pharmacol 1980; 11 Suppl. 1: 61-9.<br />
24. Tyrer P. Withdrawal from hypnotic drugs;. BMJ 1993; 306: 706-8.<br />
25. Morgan K, Oswald I. Anxiety caused by a short-life hypnotic. BMJ 1982;<br />
284: 942.<br />
26. Bixler EO, Kales A. Manfredi RL, et al. Next day memory impairment with<br />
triazolam use. Lancet 1991; 337: 827-31.<br />
27. Bond A, Lader M. After-effects <strong>of</strong> sleeping drugs. In: Wheatley D, editor.<br />
Psychopharmacology <strong>of</strong> sleep. New York: Raven Press. 1981; 177-97.<br />
28. Hindmarch I. Human psychopharmacological differences between<br />
benzodiazepines. In: Hindmarch I, Beaumont G. Brandon S. Leonard BE,<br />
editors. <strong>Benzodiazepines</strong>: current concepts. Chichester: John Wiley &<br />
Sons, l990; 73-92.<br />
29. Castleden CH, George GF, Marcer D, et al. Increased sensitivity to<br />
nitrazepam in old age. BMJ 1977; 1: 10-2.<br />
30. Dement WC, Mitler MM. It's time to wake up to <strong>the</strong> importance <strong>of</strong> sleep<br />
disorders. JAMA 1993; 269: 1548-50.<br />
31. Hallström C, Lader M. Benzodiazepine withdrawal phenomena. Int<br />
Pharmacopsychiat 1981; 16: 235-44.<br />
32. Owen RT, Tyrer P. Benzodiazepine dependence: a review <strong>of</strong> <strong>the</strong> evidence.<br />
Drugs 1983; 25: 385-98.<br />
33. Ashton H. Benzodiazepine withdrawal: an unfinished story. BMJ 1984;<br />
288: 1135-40.<br />
34. Cohn MA. Hypnotics and <strong>the</strong> control <strong>of</strong> breathing: a review. Br J Clin<br />
Pharmacol 1983; 16: 245S-50S.<br />
35. Morgan K. Hypnotics in <strong>the</strong> elderly: what cause <strong>for</strong> concern Drugs 1990;<br />
40: 688-96.<br />
36. Greenblatt DJ, Divoll M, Abernethy DR, et al. Clinical pharmacokinetics <strong>of</strong><br />
<strong>the</strong> newer benzodiazepines. Clin Pharmacokinet 1983; 8: 233-52.<br />
37. Lader M. Avoiding long-term use <strong>of</strong> benzodiazepine drugs;. Prescriber<br />
March 1991; 79-83.<br />
38. Mendelson WB. Medications in <strong>the</strong> treatment <strong>of</strong> sleep disorders. In:<br />
Meltzer HY, editor. Psychopharmacology: <strong>the</strong> third generation <strong>of</strong> progress.<br />
New York: Raven Press. 1987: 1305-11.<br />
39. Dorian P, Sellers EM, Kaplan H, et al. Evaluation <strong>of</strong> zopiclone physical<br />
dependence liability in normal volunteers. Pharmacology 1983; 27 Suppl.<br />
2: P228-34.<br />
40. Committee on Safety <strong>of</strong> Medicines. Current problems. 1990; 30.<br />
41. Consensus Conference. <strong>Guidelines</strong> <strong>for</strong> <strong>the</strong> management <strong>of</strong> patients with<br />
generalised anxiety. Psychiatric Bull 1992; 16: 560-5.<br />
42. Russell J, Lader M. editors. <strong>Guidelines</strong> <strong>for</strong> <strong>the</strong> prevention and treatment <strong>of</strong><br />
benzodiazepine dependence. London: Mental Health Foundation. 1993.<br />
43. Uhlenuth EH, Balter MB, Mellinger GD, et al. Symptom check-list<br />
syndromes in <strong>the</strong> general population. Arch Gen Psychiatry 1983; 40:<br />
1167-73<br />
44. Hallström C. Coping with anxiety: <strong>the</strong> patient's predicament. In: Wheatley<br />
D, editor. The anxiolytic jungle: where next Chichester: John Wiley &<br />
Sons Ltd., 1990; 99-111.<br />
45. American Psychiatric Association. Diagnostic and statistical manual <strong>of</strong><br />
mental disorders 3rd. rev., ed. Washington DC: American Psychiatric<br />
Association. 1987; 297-313.
46. Tyrer P. Neurosis divisible. Lancet 1985; 1: 685-8.<br />
47. Tyrer P. Choices <strong>of</strong> treatment in anxiety. In: Tyrer P. editor.<br />
Psychopharmacology <strong>of</strong> anxiety. Ox<strong>for</strong>d: Ox<strong>for</strong>d Medical Publications.<br />
1989; 255-82.<br />
48. Cloninger CR. Recent advances in <strong>the</strong> genetics <strong>of</strong> anxiety and somato<strong>for</strong>m<br />
disorders. In: Meltzer HY, editor. Psychopharmacology: <strong>the</strong> third<br />
generation <strong>of</strong> progress. New York: Raven Press, 1987; 995-65.<br />
49. Nutt DJ. Anxiety and its <strong>the</strong>rapy: today and tomorrow. In: Briley M, File<br />
SE, editors. New Concepts in Anxiety. Basingstoke: Macmillan Press Ltd,<br />
1990; 2-11.<br />
50. Wheatley D. The new alternatives. In: Wheatley D, editor. The anxiolytic<br />
jungle: where next Chichester: John Wiley & Sons. 1990; 163-84.<br />
51. Haeftely W, Pieri L, Pole P, et al. General pharmacology and<br />
neuropharmacology <strong>of</strong> benzodiazepine derivatives. In: H<strong>of</strong>fmeister H,<br />
Stille G. editors. Handbook <strong>of</strong> experimental pharmacology (Vol. 55, II)<br />
Berlin: Springer Verlag. 1081:113-62.<br />
52. Committee on Review <strong>of</strong> Medicines. Systematic review <strong>of</strong> <strong>the</strong><br />
benzodiazepines. BMJ 1980; 1: 910-2.<br />
53. Tyrer P. Benefits and risks <strong>of</strong> benzodiazepines. In: Freeman H, Rue Y,<br />
editors. The benzodiazepines in current clinical practice. London: Royal<br />
Society <strong>of</strong> Medicine Services, 1987; 3-12.<br />
54. Rickels K, Case WG, Downing RW, et al. Indications and contraindications<br />
<strong>for</strong> chronic anxiolytic treatment: is <strong>the</strong>re tolerance to <strong>the</strong> anxiolytic effect<br />
In: Kemali D, Racagni G, editors. Chronic treatments in neuropsychiatry.<br />
New York: Raven Press. 1985; 193-204.<br />
55. Ashton H. Benzodiazepine withdrawal: outcome in 50 patients. Br J Addict<br />
1987; 82: 665-71.<br />
56. Kraupl Taylor F. The damnation <strong>of</strong> benzodiazepines. Br J Psychiatry 1989;<br />
154: 697-704.<br />
57. Lader M. Benzos and memory loss: More than just 'old age'. Prescriber<br />
1992; 3: 13.<br />
58. McClelland HA. The <strong>for</strong>ensic implications <strong>of</strong> benzodiazepine usage. In:<br />
Hindmarch I, Beaumont G, Brandon S, Leonard BE, editors.<br />
<strong>Benzodiazepines</strong>: current concepts. Chichester: John Wiley & Sons, 1990;<br />
227-50.<br />
59. Gray JA. The neuropsychology <strong>of</strong> emotion and personality. In: Stahl SM,<br />
Iversen SD, Goodman ED, editors. Cognitive neurochemistry. Ox<strong>for</strong>d:<br />
Ox<strong>for</strong>d University Press, 1987; 171-90.<br />
60. Lader MH, Petursson H. Benzodiazepine derivatives - side effects and<br />
dangers. Biol Psychiatry 1981; 16: 1195-212.<br />
61. Dietch JT, Jennings RK. Aggressive dyscontrol in patients treated with<br />
benzodiazepines. J Clin Psychiatry 1998; 49: 184-8.<br />
62. Van Der Bijl P, Roel<strong>of</strong>se JA. Disinhibitory reactions to benzodiazepines: a<br />
review. J Oral Maxill<strong>of</strong>ac Sur 1991; 49: 519-23.<br />
63. Murphy SB, Tyrer P. The essence <strong>of</strong> benzodiazepine dependence. In: Lader<br />
M, editor. The psychopharmacology and addiction. Ox<strong>for</strong>d: Ox<strong>for</strong>d<br />
University Press. 1988; 157-67.<br />
64. Tyrer P. Risks <strong>of</strong> dependence on benzodiazepine drugs: <strong>the</strong> importance <strong>of</strong><br />
patient selection. BMJ 1989; 298; 102-5.<br />
65. Herman JB. Brotman AW. Rosenbaum JF. Rebound anxiety in panic<br />
disorder patients treated with shorter-acting benzodiazepines. J Clin<br />
Psychiatry 1987; 48 Suppl. 10: 22-6.<br />
66. Sheehan DV, Coleman JH, Greenblatt DJ, et al. Some biochemical<br />
correlates <strong>of</strong> panic attacks with agoraphobia and <strong>the</strong>ir response to a new<br />
treatment. J Clin Psychopharmacol 1984; 4: 66-75.<br />
67. Sheehan DV. <strong>Benzodiazepines</strong> in panic disorder and agoraphobia. J Affect<br />
Disord 1987; 13: 169-81.
68. Ballenger JC, Burrows GD, DuPont RL, et al. .Alprazolam in panic disorder<br />
and agoraphobia: from a multicenter trial. Arch Gen Psychiatry 1988; 45:<br />
413-22.<br />
69. Noyes R, DuPont RL. Pecknold JC. et al. Alprazolam in panic disorder and<br />
agoraphobia: results from a multicenter trial: II. Patient acceptance. side<br />
effects and safety. Arch Gen Psychiatry 1988; 45: 423-8.<br />
70. Tesar GE. High-potency benzodiazepines <strong>for</strong> short-term management <strong>of</strong><br />
panic disorder: <strong>the</strong> CIS experience. J Clin Psychiatry 1990; 51: 4-10.<br />
71. Pecknold JC. Swinson RP. Kuch K, et al. Alprazolam in panic disorder and<br />
agoraphobia: results from a multicenter trial. III. Discontinuation effects.<br />
Arch Gen Psychiatry 1988; 45: 429- 36.<br />
72. Pollack MH. Long-term management <strong>of</strong> panic disorder. J Clin Psychiatry<br />
1990; 51: 11-3.<br />
73. Marks IM, O'Sullivan G. Anti-anxiety drug and psychological treatment<br />
effects in agoraphobia/panic and obsessive-compulsive disorders. In:<br />
Tyrer P, editor. Psychopharmacology <strong>of</strong> anxiety. Ox<strong>for</strong>d: Ox<strong>for</strong>d University<br />
Press, 1989; 196-242.<br />
74. Rizley R, Kahn RJ, McNair DM, et al. A comparison <strong>of</strong> alprazolam and<br />
imipratnine in <strong>the</strong> treatment <strong>of</strong> agoraphobia and panic disorder.<br />
Psychopharmacol Bull 1986; 22: 167-72.<br />
75. Nutt DJ, Glue P. Clinical pharmacology <strong>of</strong> anxiolytics and antidepressants:<br />
a psychopharmacological perspective. Pharmacol Ther 1989; 44: 309-34.<br />
76. Schweizer E, Clary C, Dever AI, et al. The use <strong>of</strong> low-dose intranasal<br />
midazolam to treat panic disorder: a pilot study. J Clin Psychiatry 1992;<br />
53: 19-22.<br />
77. Feighner JP. <strong>Benzodiazepines</strong> as antidepressants. In: Ban TA, editor.<br />
Modern problems <strong>of</strong> pharmacopsychiatry. Basel: S Karger. 1982; 196-212.<br />
78. Lesser IM, Rubin RT, Pecknold JC, et al. Secondary' depression in panic<br />
disorder and agoraphobia. I. frequency. severity, and response to<br />
treatment. Arch Gen Psychiatry 1988; 44: 437-43.<br />
79. Ashton H, Golding JF. Tranquillisers: prevalence. predictors and possible<br />
consequences. Data from a large United Kingdom survey. Br J Addict<br />
1989; 84: 541-6.<br />
80. Ashton H. Protracted withdrawal syndromes from benzodiazepines. J Subst<br />
Abuse Treat 1991; 8:19-28.<br />
81. Holton A, Tyrer P. Five year outcome in patients withdrawn from long term<br />
treatment with diazepam. BMJ 1990; 300: 1241-2.<br />
82. Rickels K, Schweizer E, Case WG. Withdrawal problems with anti-anxiety<br />
drugs: nature and management. In: Tyrer P. editor. Psychopharmacology<br />
<strong>of</strong> anxiety. Ox<strong>for</strong>d: Ox<strong>for</strong>d University Press. 1989; 283-94.<br />
83. Brodie MJ. Status epilepticus in adults. BMJ 1990; 336: 551-2.<br />
84. Trimble MR. <strong>Benzodiazepines</strong> in clinical practice. In: Wheatley D, editor.<br />
The anxiolytic jungle: where next Chichester: John Wiley & Sons, 1990;<br />
336: 350-4.<br />
85. Brodie MJ. Established anticonvulsants and treatment <strong>of</strong> refractory<br />
epilepsy. BMJ 1990; 336: 350-4.<br />
86. Feely M. Clonazepam and clobazam. Prescribers J 1989; 29: 111-5.<br />
87. Dundee JW. The application <strong>of</strong> <strong>the</strong> benzodiazepines in anaes<strong>the</strong>sia. In:<br />
Hindmarch I, Beaumont G, Brandon, S, Leonard BE, editors.<br />
<strong>Benzodiazepines</strong>: Current Concepts. Chichester: John Wiley & Sons Ltd,<br />
1990; 153-68.<br />
88. Herrington RN. The uses <strong>of</strong> benzodiazepines in neuropsychiatry. In:<br />
Hindmarch I Beaumont G, Brandon S, Leonard BE, editors.<br />
<strong>Benzodiazepines</strong>: Current Concepts. Chichester: John Wiley & Sons Ltd,<br />
1990; 95-110.
89. Wolkowitz OM, Pickar D. <strong>Benzodiazepines</strong> in <strong>the</strong> treatment <strong>of</strong><br />
schizophrenia: a review and reappraisal. Am J Psychiatry 1991; 148: 714-<br />
26.<br />
90. Potokar J, Nutt DJ. Anxiolytic potential <strong>of</strong> benzodiazepine receptor partial<br />
agonists. CNS Drugs 1994; 1: 305-15.<br />
Correspondence: Pr<strong>of</strong>essor Hea<strong>the</strong>r Ashton, Clinical Psychopharmacology Unit,<br />
Department <strong>of</strong> Psychiatry, Royal Victoria Infirmary, Newcastle upon Tyne, NE1 1LP,<br />
England