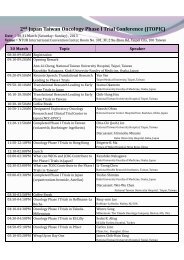
H. T. Liu et al./JCRP 28(2012) 94-98 97 A B Figure 4. (A) Series <strong>of</strong> chest films show initial response to a course <strong>of</strong> chemo<strong>the</strong>rapy with paclitaxel and cisplatin, and (B) progressive disease two months later express CDX2, which was previously thought to be a specific marker for tumors with intestinal differentiation. Due to <strong>the</strong> introduction <strong>of</strong> <strong>the</strong> new classification system and rare disease incidence rate, <strong>the</strong>re were lim-
98 H. T. Liu et al./JCRP 28(2012) 94-98 ited studies that had mentioned <strong>the</strong> treatment <strong>of</strong> invasive mucinous adenocarcinoma. According to WHO 2004 classification, research has shown that surgery for resectable disease remains <strong>the</strong> mainstay treatment <strong>of</strong> BAC [4]. However, for invasive mucinous adenocarcinoma, <strong>the</strong>re was no study which demonstrated an optimum treatment response. Some reports showed a good treatment response to tyrosine kinase inhibitor (TKI) in MIA patients harboring <strong>the</strong> EGFR mutation [5,6]. However, <strong>the</strong> EGFR mutation represents a relatively low percentage <strong>of</strong> total cases in comparison with o<strong>the</strong>r types <strong>of</strong> adenocarcinoma. For this patient, comprehensive studies had been done to exclude various metastatic origins. Ultimately, she was diagnosed with stage IV primary lung cancer. Because <strong>of</strong> <strong>the</strong> wild type EGFR sequencing, we chose paclitaxel (175 mg/m 2 ) plus cisplatin (50 mg/m 2 ) (TC) as first line chemo<strong>the</strong>rapy. Although <strong>the</strong> patient’s initial response to this course <strong>of</strong> treatment was good, her disease progressed after three cycles <strong>of</strong> TC regimen (Figure 4). The clinical course implied that <strong>the</strong> disease had aggressive behavior, which <strong>of</strong>ten leads to a poor prognosis as occurred in this case. The valuable information we obtained from this case was that invasive mucinous adenocarcinoma can have unusual presentation and distinct pathological features, highlighting <strong>the</strong> importance <strong>of</strong> multidisciplinary cooperation for accurate diagnosis and treatment. Although we have found no strong evidence <strong>of</strong> a particularly efficacious, long-term treatment, we suggest paclitaxel plus cisplatin as an option for <strong>the</strong> first line chemo<strong>the</strong>rapy. REFERENCES 1. Travis WD, Brambilla E, Noguchi M, et al. International association for <strong>the</strong> study <strong>of</strong> lung cancer/american thoracic society/european respiratory society international multidisciplinary classification <strong>of</strong> lung adenocarcinoma. J Thorac Oncol 6: 244-285, 2011. 2. Morency E, Rodriguez Urrego PA, Szporn AH, et al. The “drunken honeycomb” feature <strong>of</strong> pulmonary mucinous adenocarcinoma: a diagnostic pitfall <strong>of</strong> bronchial brushing cytology. Diagn Cytopathol: n/a–n/a, 2011. 3. Mazziotta RM, Borczuk AC, Powell CA, et al. CDX2 immunostaining as a gastrointestinal marker: expression in lung carcinomas is a potential pitfall. Appl Immunohistochem Mol Morphol 13: 55-60, 2005. 4. Whitson BA, Groth SS, Andrade RS, et al. <strong>Invasive</strong> adenocarcinoma with bronchoalveolar features: a population-based evaluation <strong>of</strong> <strong>the</strong> extent <strong>of</strong> resection in bronchoalveolar cell carcinoma. J Thorac Cardiovasc Surg 143(3):591-600,2012 . 5. Kitazaki T, Fukuda M, Kohno S, et al. Novel effects <strong>of</strong> gefitinib on mucin production in bronchioloalvelar carcinoma; two case reports. <strong>Lung</strong> Cancer 49(1):125-8, 2005. 6. Popat N, Raghavan N, McIvor RA. Severe bronchorrhea in a patient with bronchioloalveolar carcinoma. CHEST 141(2): 513-514, 2012.