Lower GI referral form - Barts Health NHS Trust
Lower GI referral form - Barts Health NHS Trust
Lower GI referral form - Barts Health NHS Trust
You also want an ePaper? Increase the reach of your titles
YUMPU automatically turns print PDFs into web optimized ePapers that Google loves.
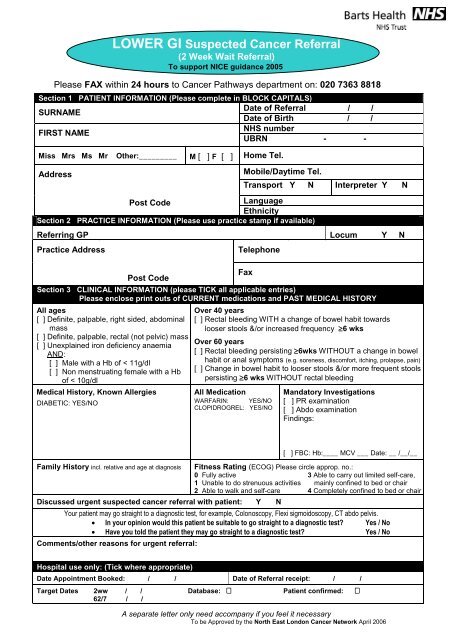
LOWER <strong>GI</strong> Suspected Cancer Referral<br />
(2 Week Wait Referral)<br />
Please FAX within 24 hours to Cancer Pathways department on: 020 7363 8818<br />
Section 1 PATIENT INFORMATION (Please complete in BLOCK CAPITALS)<br />
SURNAME<br />
Date of Referral / /<br />
Date of Birth / /<br />
FIRST NAME<br />
<strong>NHS</strong> number<br />
UBRN - -<br />
Miss Mrs Ms Mr Other:_________ M [ ] F [ ] Home Tel.<br />
Address<br />
Mobile/Daytime Tel.<br />
Post Code<br />
Language<br />
Ethnicity<br />
Section 2 PRACTICE INFORMATION (Please use practice stamp if available)<br />
Transport Y N Interpreter Y N<br />
Referring GP Locum Y N<br />
Practice Address<br />
Post Code<br />
Telephone<br />
Section 3 CLINICAL INFORMATION (please TICK all applicable entries)<br />
Please enclose print outs of CURRENT medications and PAST MEDICAL HISTORY<br />
All ages<br />
[ ] Definite, palpable, right sided, abdominal<br />
mass<br />
[ ] Definite, palpable, rectal (not pelvic) mass<br />
[ ] Unexplained iron deficiency anaemia<br />
AND:<br />
[ ] Male with a Hb of < 11g/dl<br />
[ ] Non menstruating female with a Hb<br />
of < 10g/dl<br />
Medical History, Known Allergies<br />
DIABETIC: YES/NO<br />
To support NICE guidance 2005<br />
Fax<br />
Over 40 years<br />
[ ] Rectal bleeding WITH a change of bowel habit towards<br />
looser stools &/or increased frequency 6 wks<br />
Over 60 years<br />
[ ] Rectal bleeding persisting 6wks WITHOUT a change in bowel<br />
habit or anal symptoms (e.g. soreness, discomfort, itching, prolapse, pain)<br />
[ ] Change in bowel habit to looser stools &/or more frequent stools<br />
persisting 6 wks WITHOUT rectal bleeding<br />
All Medication<br />
WARFARIN: YES/NO<br />
CLOPIDROGREL: YES/NO<br />
Mandatory Investigations<br />
[ ] PR examination<br />
[ ] Abdo examination<br />
Findings:<br />
Family History incl. relative and age at diagnosis<br />
Discussed urgent suspected cancer <strong>referral</strong> with patient: Y N<br />
[ ] FBC: Hb:____ MCV ___ Date: __ /__/__<br />
Fitness Rating (ECOG) Please circle approp. no.:<br />
0 Fully active 3 Able to carry out limited self-care,<br />
1 Unable to do strenuous activities mainly confined to bed or chair<br />
2 Able to walk and self-care 4 Completely confined to bed or chair<br />
Your patient may go straight to a diagnostic test, for example, Colonoscopy, Flexi sigmoidoscopy, CT abdo pelvis.<br />
In your opinion would this patient be suitable to go straight to a diagnostic test? Yes / No<br />
Have you told the patient they may go straight to a diagnostic test? Yes / No<br />
Comments/other reasons for urgent <strong>referral</strong>:<br />
Hospital use only: (Tick where appropriate)<br />
Date Appointment Booked: / / Date of Referral receipt: / /<br />
Target Dates 2ww / / Database: Patient confirmed: <br />
62/7 / /<br />
A separate letter only need accompany if you feel it necessary<br />
To be Approved by the North East London Cancer Network April 2006
LOCAL CONTACT DETAILS<br />
If you wish to discuss any clinical issues concerning this <strong>referral</strong> please contact:<br />
Mr Roger Le Fur Consultant Colorectal Surgeon 020 7363 8037<br />
Anne Smart <strong>Lower</strong> <strong>GI</strong> Nurse Specialist 020 7363 4000 Bleep 287<br />
If you wish to discuss any other aspect of this <strong>referral</strong>, please contact the Cancer<br />
Pathways Office on 020 7363 8817 / 9275 / 3399<br />
CRITERIA FOR URGENT SUSPECTED CANCER REFERRAL 1<br />
Please FAX the <strong>referral</strong> <strong>form</strong> within 24 hours<br />
Refer a patient who presents with symptoms suggestive of colorectal or anal cancer to<br />
a team specialising in the management of lower gastrointestinal cancer, depending on<br />
local arrangements.<br />
Investigations<br />
<br />
<br />
<br />
<br />
Always carry out a digital rectal examination in patients with unexplained<br />
symptoms related to the lower gastrointestinal tract.<br />
Where symptoms are equivocal a full blood count may help in identifying the<br />
possibility of colorectal cancer by demonstrating iron deficiency anaemia, which<br />
should then determine if a <strong>referral</strong> should be made and its urgency.<br />
When referring, a full blood count will assist specialist assessment in the<br />
outpatient clinic.<br />
When referring, no examinations or investigations other than abdominal and<br />
rectal examination and FBC are recommended as this may delay <strong>referral</strong>
Risk factors<br />
Offer patients with ulcerative colitis or a history of ulcerative colitis a follow-up plan<br />
agreed with a specialist in an effort to detect colorectal cancer in this high-risk group.<br />
Low Risk Criteria<br />
Patients of all ages with the following symptoms and no abdominal or rectal mass<br />
are at very low risk of colorectal cancer and should therefore not be referred under<br />
the two-week system:<br />
• Rectal bleeding WITH anal symptoms, e.g. soreness, discomfort, itching,<br />
lumps, prolapse and pain<br />
• Rectal bleeding with an obvious external cause for bleeding on simple<br />
examination of the perineum, e.g. anal fissure, thrombosed or prolapsed pile<br />
and rectal prolapse<br />
• Transient changes in bowel habit, particularly to harder stools and/or<br />
decreased frequency of defecation<br />
• Abdominal pain as a single symptom WITHOUT other higher risk<br />
age/symptom/sign profiles, an abdominal mass, an iron deficiency anaemia or<br />
intestinal obstruction<br />
If your patient fits these “low risk” criteria, please do not use this <strong>form</strong><br />
Refer the patient by means of a routine <strong>referral</strong> letter<br />
Fitness rating or ECOG<br />
The ECOG (Eastern Cooperative Oncology Group) per<strong>form</strong>ance score:<br />
0 = fully active, the same as before suspicion of cancer<br />
1 = unable to do strenuous activities but still able to do tasks such as light<br />
housework or office work<br />
2 = able to walk and carry out self-care (e.g. eating, dressing), but not able to work<br />
3 = only able to carry out limited self-care, mainly confined to bed or chair<br />
4 = completely confined to bed or chair and not able to carry out self-care<br />
1 Based on Referral Guidelines for Suspected Cancer (NICE, 2005) Notes in grey refer to the evidence<br />
grading used in the NICE guidelines, for more in<strong>form</strong>ation see www.nice.org.uk/cg027NICEguideline)<br />
2 In this guideline, unexplained is defined as ‘a symptom(s) and/or sign(s) that has not led to a diagnosis<br />
being made by the primary care professional after initial assessment of the history, examination and<br />
primary care investigations (if any)’. In the context of this recommendation, unexplained means a<br />
patient whose anaemia is considered on the basis of a history and examination in primary care not to<br />
be related to other sources of blood loss (for example, ingestion of NSAIDs) or blood dyscrasia.