Craniofacial Anomalies, Part 2 - Plastic Surgery Internal
Craniofacial Anomalies, Part 2 - Plastic Surgery Internal
Craniofacial Anomalies, Part 2 - Plastic Surgery Internal
Create successful ePaper yourself
Turn your PDF publications into a flip-book with our unique Google optimized e-Paper software.
TABLE 7<br />
Brain Growth During the First 20 Years of Life<br />
(Data from Blinkov SM, Glezer II: The Human Brain in Figures<br />
and Tables: A Quantitative Handbook. New York, Plenum<br />
Press, 1968. Reprinted with permission from Marchac D, Renier<br />
D: <strong>Craniofacial</strong> <strong>Surgery</strong> for Craniosynostosis. Boston, Little<br />
Brown, 1982, p 36.)<br />
metrical deformities to lessen the need for major<br />
revisions at a later date. 404<br />
Certainly unilateral cases can be expected to<br />
achieve better results than bilateral cases. McCarthy<br />
demonstrated good to excellent results in 86% of<br />
patients undergoing unilateral procedures and in 49–<br />
70% of bilateral procedures. 418,419<br />
SURGERY FOR COMBINED CRANIOSYNOSTOSIS AND<br />
HYPOPLASIA OF THE MIDFACE<br />
There have been few changes in the treatment of<br />
Crouzon disease since Tessier first described his classic<br />
facial osteotomy technique. 275,288,367,420,421 Modifications<br />
have progressed from the Tessier I—a<br />
subcranial Le Fort III—in 1958, through the more<br />
radical Tessier VIII of 1976, which split and bent a<br />
frontofacial monobloc segment, derotated the orbits,<br />
and brought the maxilla forward. In Tessier’s hands<br />
this extensive procedure yielded nearly normal results.<br />
In 1976 and again in 1979, Van der Meulen 422,423<br />
described a similar operation that involves simultaneous<br />
total osteotomy of the two halves of the face<br />
and correction of the orbitofrontal and maxillary<br />
deformities. The coronal approach to osteotomy of<br />
SRPS Volume 10, Number 17, <strong>Part</strong> 2<br />
the pterygomaxillary fissure obviates intraoral surgery<br />
with its potential contamination.<br />
Ortiz Monasterio and associates 402 first advocated<br />
monobloc advancement of the entire forehead and<br />
face (Fig 23) in 1977. Anderl and coworkers 424 proposed<br />
a modification of the frontoorbital bar with<br />
preservation of an intact anterior cranial base to separate<br />
the cranial and nasal spaces when indicated for<br />
relief of respiratory or orbital distress accompanying<br />
severe craniosynostosis. Although many surgeons<br />
believe that monobloc advancements are hazardous<br />
because of the high number of associated infectious<br />
sequelae, the authors feel their technique is safe even<br />
at a young age.<br />
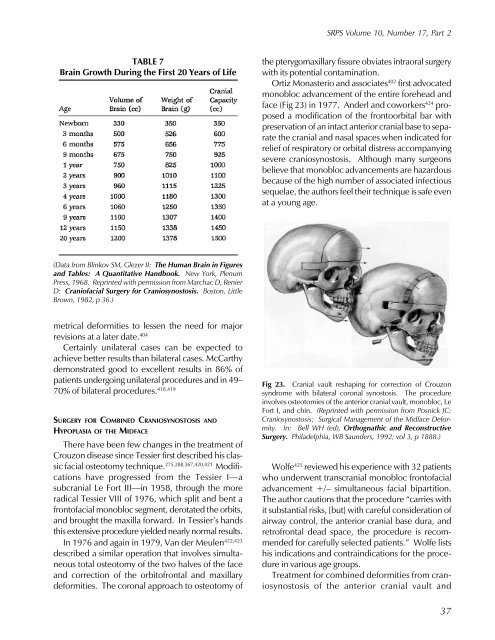
Fig 23. Cranial vault reshaping for correction of Crouzon<br />
syndrome with bilateral coronal synostosis. The procedure<br />
involves osteotomies of the anterior cranial vault, monobloc, Le<br />
Fort I, and chin. (Reprinted with permission from Posnick JC:<br />
Craniosynostosis: Surgical Management of the Midface Deformity.<br />
In: Bell WH (ed), Orthognathic and Reconstructive<br />
<strong>Surgery</strong>. Philadelphia, WB Saunders, 1992; vol 3, p 1888.)<br />
Wolfe 425 reviewed his experience with 32 patients<br />
who underwent transcranial monobloc frontofacial<br />
advancement +/– simultaneous facial bipartition.<br />
The author cautions that the procedure “carries with<br />
it substantial risks, [but] with careful consideration of<br />
airway control, the anterior cranial base dura, and<br />
retrofrontal dead space, the procedure is recommended<br />
for carefully selected patients.” Wolfe lists<br />
his indications and contraindications for the procedure<br />
in various age groups.<br />
Treatment for combined deformities from craniosynostosis<br />
of the anterior cranial vault and<br />
37