Craniofacial Anomalies, Part 2 - Plastic Surgery Internal
Craniofacial Anomalies, Part 2 - Plastic Surgery Internal
Craniofacial Anomalies, Part 2 - Plastic Surgery Internal
Create successful ePaper yourself
Turn your PDF publications into a flip-book with our unique Google optimized e-Paper software.
Le Fort II Osteotomy<br />
The Le Fort II osteotomy was popularized by<br />
Henderson and Jackson447 in cleft patients with associated<br />
paranasal and nasal shortening. Several variations<br />
have been described, including the tripartite<br />
osteotomy of Converse. 448<br />
Le Fort III Osteotomy<br />
The mainstay of total maxillary advancement is<br />
the Le Fort III osteotomy. 421 The procedure can be<br />
combined with other osteotomies, specifically a Le<br />
Fort I, for definitive treatment of severe midfacial<br />
retrusion. 288 Interpositional bone grafts and a<br />
maxillomandibular fixation appliance373–377 are useful<br />
adjuncts. If decreasing the interorbital distance or<br />
widening of the palate is necessary, a facial bipartition<br />
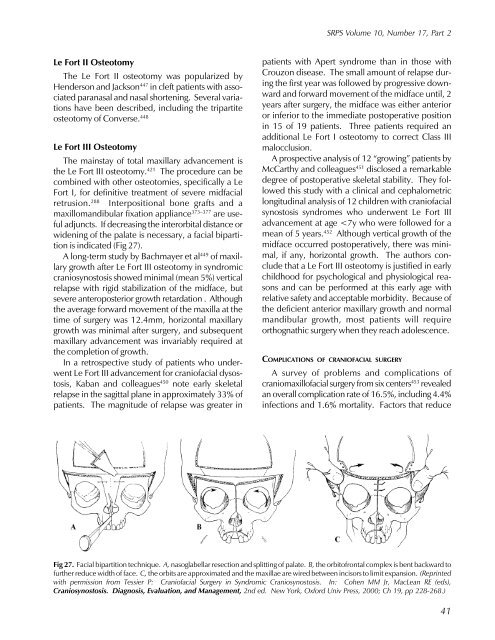
is indicated (Fig 27).<br />
A long-term study by Bachmayer et al449 of maxillary<br />
growth after Le Fort III osteotomy in syndromic<br />
craniosynostosis showed minimal (mean 5%) vertical<br />
relapse with rigid stabilization of the midface, but<br />
severe anteroposterior growth retardation . Although<br />
the average forward movement of the maxilla at the<br />
time of surgery was 12.4mm, horizontal maxillary<br />
growth was minimal after surgery, and subsequent<br />
maxillary advancement was invariably required at<br />
the completion of growth.<br />
In a retrospective study of patients who underwent<br />
Le Fort III advancement for craniofacial dysostosis,<br />
Kaban and colleagues450 note early skeletal<br />
relapse in the sagittal plane in approximately 33% of<br />
patients. The magnitude of relapse was greater in<br />
SRPS Volume 10, Number 17, <strong>Part</strong> 2<br />
patients with Apert syndrome than in those with<br />
Crouzon disease. The small amount of relapse during<br />
the first year was followed by progressive downward<br />
and forward movement of the midface until, 2<br />
years after surgery, the midface was either anterior<br />
or inferior to the immediate postoperative position<br />
in 15 of 19 patients. Three patients required an<br />
additional Le Fort I osteotomy to correct Class III<br />
malocclusion.<br />
A prospective analysis of 12 “growing” patients by<br />
McCarthy and colleagues 451 disclosed a remarkable<br />
degree of postoperative skeletal stability. They followed<br />
this study with a clinical and cephalometric<br />
longitudinal analysis of 12 children with craniofacial<br />
synostosis syndromes who underwent Le Fort III<br />
advancement at age