Antiretroviral Therapy in Resource-Poor Settings - GiveWell
Antiretroviral Therapy in Resource-Poor Settings - GiveWell
Antiretroviral Therapy in Resource-Poor Settings - GiveWell
You also want an ePaper? Increase the reach of your titles
YUMPU automatically turns print PDFs into web optimized ePapers that Google loves.
Mukherjee et al J Acquir Immune Defic Syndr Volume 43, Supplement 1, December 1, 2006<br />
barriers. First, all services and medications are provided free of<br />
charge to the patient. It has been documented by several<br />
projects that user fees are a significant barrier to seek<strong>in</strong>g HIV<br />
test<strong>in</strong>g, obta<strong>in</strong><strong>in</strong>g laboratory evaluations, and attend<strong>in</strong>g<br />
follow-up appo<strong>in</strong>tments. 10 Such cost shar<strong>in</strong>g is detrimental<br />
to long-term adherence, as data from Senegal 11 and Botswana 9<br />
<strong>in</strong>dicate. In the HEI, user fees for services (visits and<br />
monitor<strong>in</strong>g) and all medications are waived entirely. All<br />
treatment is given free of charge (<strong>in</strong>clud<strong>in</strong>g not only ART but<br />
drugs for opportunistic <strong>in</strong>fections, family plann<strong>in</strong>g, and<br />
medications for other conditions such as hypertension).<br />
Second, HIV test<strong>in</strong>g, treatment, and care are provided <strong>in</strong><br />
the context of primary care services. This is particularly<br />
important and primary care cl<strong>in</strong>ics were revitalized by<br />
provid<strong>in</strong>g essential medic<strong>in</strong>es and pay<strong>in</strong>g stipends to MSPP<br />
staff <strong>in</strong> rural areas where patients rout<strong>in</strong>ely walk 4 or more<br />
hours to seek care. Most of the people attend<strong>in</strong>g the<br />
PIH/MSPP cl<strong>in</strong>ics come only when they are ill rather than<br />
to seek test<strong>in</strong>g for HIV per se. In the context of primary health<br />
care, ill patients are screened for tuberculosis, treatable causes<br />
of diarrheal disease, sexually transmitted diseases, and other<br />
conditions that may be associated with HIV. As part of the<br />
evaluation of the ill patient, HIV test<strong>in</strong>g may be offered by the<br />
cl<strong>in</strong>ician, if <strong>in</strong>dicated. This strategy, sometimes called ‘‘opt<br />
out’’ or ‘‘rout<strong>in</strong>e offer’’ HIV test<strong>in</strong>g, has been found to be<br />
acceptable <strong>in</strong> many sett<strong>in</strong>gs, particularly when ART is<br />
available. 12,13<br />
The third aspect of the program to <strong>in</strong>crease access and<br />
adherence to HIV treatment is an attempt to m<strong>in</strong>imize the<br />
significant out-of-pocket expenses. Studies from several<br />
sett<strong>in</strong>gs have shown that costs such as payment for transportation<br />
to and from a cl<strong>in</strong>ic serve as a deterrent to ART<br />
adherence. Patients attend<strong>in</strong>g PIH/MSPP cl<strong>in</strong>ic receive<br />
a monthly transportation stipend to attend follow-up appo<strong>in</strong>tments.<br />
Transportation for emergency visits is also covered by<br />
the program. 14 Similarly, a lack of food has been associated with<br />
poor adherence to ART, and provision of food and micronutrients<br />
has been shown to improve outcomes 15–17 Many<br />
families throughout the develop<strong>in</strong>g world spend more than 50%<br />
of their household <strong>in</strong>come on food, and food production and<br />
wage earn<strong>in</strong>g are adversely affected when an adult has<br />
AIDS. 18,19 Therefore, the PIH/MSPP program provides food<br />
or cash transfers for food to the most vulnerable patients.<br />
The fourth aspect of the HEI program to support adherence<br />
and m<strong>in</strong>imize barriers to access is the use of community<br />
health workers. Community health workers perform active<br />
case f<strong>in</strong>d<strong>in</strong>g for HIV and tuberculosis and provide a l<strong>in</strong>k<br />
between the patient, family, community, and cl<strong>in</strong>ic. Their daily<br />
role is to give psychologic support and directly observed<br />
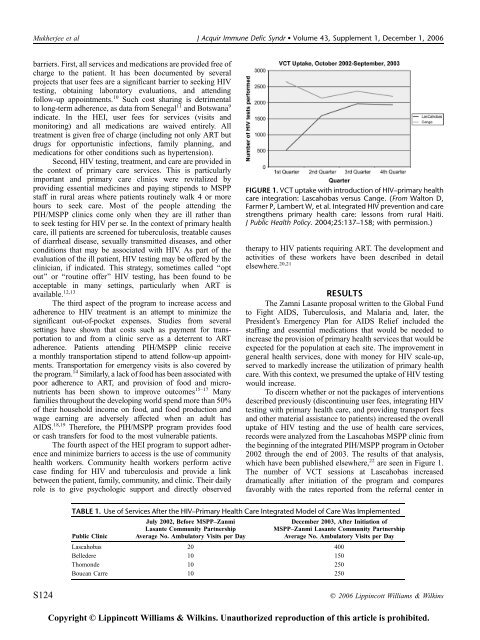
FIGURE 1. VCT uptake with <strong>in</strong>troduction of HIV–primary health<br />
care <strong>in</strong>tegration: Lascahobas versus Cange. (From Walton D,<br />
Farmer P, Lambert W, et al. Integrated HIV prevention and care<br />
strengthens primary health care: lessons from rural Haiti.<br />
J Public Health Policy. 2004;25:137–158; with permission.)<br />
therapy to HIV patients requir<strong>in</strong>g ART. The development and<br />
activities of these workers have been described <strong>in</strong> detail<br />
elsewhere. 20,21<br />
RESULTS<br />
The Zamni Lasante proposal written to the Global Fund<br />
to Fight AIDS, Tuberculosis, and Malaria and, later, the<br />
President’s Emergency Plan for AIDS Relief <strong>in</strong>cluded the<br />
staff<strong>in</strong>g and essential medications that would be needed to<br />
<strong>in</strong>crease the provision of primary health services that would be<br />
expected for the population at each site. The improvement <strong>in</strong><br />
general health services, done with money for HIV scale-up,<br />
served to markedly <strong>in</strong>crease the utilization of primary health<br />
care. With this context, we presumed the uptake of HIV test<strong>in</strong>g<br />
would <strong>in</strong>crease.<br />
To discern whether or not the packages of <strong>in</strong>terventions<br />
described previously (discont<strong>in</strong>u<strong>in</strong>g user fees, <strong>in</strong>tegrat<strong>in</strong>g HIV<br />
test<strong>in</strong>g with primary health care, and provid<strong>in</strong>g transport fees<br />
and other material assistance to patients) <strong>in</strong>creased the overall<br />
uptake of HIV test<strong>in</strong>g and the use of health care services,<br />
records were analyzed from the Lascahobas MSPP cl<strong>in</strong>ic from<br />
the beg<strong>in</strong>n<strong>in</strong>g of the <strong>in</strong>tegrated PIH/MSPP program <strong>in</strong> October<br />
2002 through the end of 2003. The results of that analysis,<br />
which have been published elsewhere, 22 are seen <strong>in</strong> Figure 1.<br />
The number of VCT sessions at Lascahobas <strong>in</strong>creased<br />
dramatically after <strong>in</strong>itiation of the program and compares<br />
favorably with the rates reported from the referral center <strong>in</strong><br />
TABLE 1. Use of Services After the HIV–Primary Health Care Integrated Model of Care Was Implemented<br />
Public Cl<strong>in</strong>ic<br />
July 2002, Before MSPP–Zanmi<br />
Lasante Community Partnership<br />
Average No. Ambulatory Visits per Day<br />
December 2003, After Initiation of<br />
MSPP–Zanmi Lasante Community Partnership<br />
Average No. Ambulatory Visits per Day<br />
Lascahobas 20 400<br />
Belledere 10 150<br />
Thomonde 10 250<br />
Boucan Carre 10 250<br />
S124<br />
q 2006 Lipp<strong>in</strong>cott Williams & Wilk<strong>in</strong>s<br />
Copyright © Lipp<strong>in</strong>cott Williams & Wilk<strong>in</strong>s. Unauthorized reproduction of this article is prohibited.