MRSA policy - Hampshire Hospitals NHS Foundation Trust
MRSA policy - Hampshire Hospitals NHS Foundation Trust
MRSA policy - Hampshire Hospitals NHS Foundation Trust
Create successful ePaper yourself
Turn your PDF publications into a flip-book with our unique Google optimized e-Paper software.
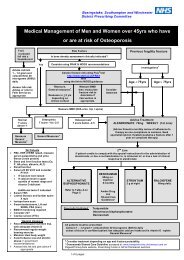
Methicillin Resistant Staphylococcus Aureus Policy<br />
<strong>MRSA</strong><br />
Authorities<br />
Document Control Information<br />
Author:<br />
Sue Dailly, Lead Nurse<br />
Infection Control<br />
Type:<br />
Policy<br />
Sponsor:<br />
Paula Shobbrook, Director<br />
of Infection Prevention and<br />
Control<br />
Reviewer(s): Members of the Infection<br />
Control Committee and<br />
Nursing and Midwifery<br />
Policy Group<br />
Approval<br />
body:<br />
Infection Control<br />
Committee<br />
and Policy Advisory Group<br />
Scope:<br />
Major<br />
<strong>Trust</strong> Reference CP055<br />
Number:<br />
Issue Number: 4<br />
Status:<br />
Published<br />
Effective Date: April 2010<br />
Review Date: April 2013<br />
Disposal Date: April 2035<br />
Document Authorisation Control<br />
Prepared By:<br />
Sue Dailly<br />
Lead Nurse Infection Control<br />
Signature:<br />
Authorised Officer<br />
Martin Wakeley<br />
Chief Executive<br />
Signature:<br />
Authorities<br />
Document Control Information<br />
Author: Sue Dailly Lead Nurse IC Type: Policy<br />
Sponsor: Director of Infection Prevention and Scope:<br />
Major<br />
Control<br />
Reference:<br />
CP055<br />
Issue Number: 4<br />
Date April 2010 Status: Published<br />
Page 1 of 55
DOCUMENT CONTROL<br />
Document Amendments<br />
Winchester & Eastleigh Healthcare <strong>NHS</strong> <strong>Trust</strong><br />
<strong>MRSA</strong> POLICY<br />
Number Details By Whom Date<br />
1.0 Original document<br />
2.0 Amended to match <strong>Trust</strong> Policy for the<br />
Management of Controlled Documents<br />
and <strong>NHS</strong>LA Standard and new national<br />
guidance on <strong>MRSA</strong> screening<br />
3.0 Amended to include new <strong>MRSA</strong><br />
screening guidance<br />
3.4 Document format alignment to <strong>NHS</strong>LA<br />
Standards<br />
4.0 Document format changed to match PCT<br />
wide <strong>MRSA</strong> screening and treatment<br />
regime<br />
Sue Dailly ICN 3/02/08<br />
Sue Dailly ICN 02/2009<br />
Steven Jennings<br />
Divisional<br />
Governance<br />
Head<br />
Sue Dailly<br />
12/03/09<br />
January<br />
2010<br />
Review Timetable<br />
Date Reason By Whom Date Completed<br />
February<br />
2013<br />
Three yearly review cycle for<br />
<strong>policy</strong> document. If national<br />
guidance changes the <strong>policy</strong> will<br />
be reviewed sooner<br />
Infection<br />
Control<br />
Team<br />
Distribution List<br />
No<br />
Title<br />
1 Infection Control Team<br />
2 Members of the Infection Control Committee<br />
3 <strong>Trust</strong> Intranet<br />
4 Winchester & Eastleigh Healthcare <strong>NHS</strong> <strong>Trust</strong> Website<br />
5 Holders of Infection Control Manual<br />
Authorities<br />
Document Control Information<br />
Author: Sue Dailly Lead Nurse IC Type: Policy<br />
Sponsor: Director of Infection Prevention and Control Scope: Major<br />
Reference: CP055<br />
Issue Number: 4<br />
Date April 2010 Status: Published<br />
Page 2 of 55
Winchester & Eastleigh Healthcare <strong>NHS</strong> <strong>Trust</strong><br />
<strong>MRSA</strong> POLICY<br />
RELATED TRUST POLICIES<br />
LTP09 Methicillin Resistant Staphylococcus aureus Patients in Theatre Policy<br />
CP07 Single Use Devices Policy<br />
CP03 Disinfection, Decontamination and Cleaning Policy<br />
CP008 Incident Management & Reporting Policy Including the Management of<br />
Serious Untoward Incidents<br />
CP014 Antibiotic Policy for adults<br />
CP030 Overarching Decontamination Policy<br />
OP052 Waste Disposal Policy<br />
CP061 Policy for the Intraward Transfer of Patients with Infection Control<br />
Issues<br />
CP070 Deceased Infected Patient Policy<br />
CP072 Training Policy for Employees of WEHCT in Infection Control<br />
CP073 Hand hygiene <strong>policy</strong><br />
CP079 <strong>Trust</strong> <strong>policy</strong> for uniform and clothing worn whilst delivering direct<br />
clinical care<br />
CP080 Theatre Uniforms<br />
OP010 <strong>Trust</strong> Induction Policy<br />
OP006 Risk Management & Patient Safety Policy<br />
OP036 Risk Register Policy<br />
PG011 Antimicrobial Prescribing Guidelines (Adults)<br />
CPr049 Theatres <strong>MRSA</strong> Policy<br />
Authorities<br />
Document Control Information<br />
Author: Sue Dailly Lead Nurse IC Type: Policy<br />
Sponsor: Director of Infection Prevention and Control Scope: Major<br />
Reference: CP055<br />
Issue Number: 4<br />
Date April 2010 Status: Published<br />
Page 3 of 55
Winchester & Eastleigh Healthcare <strong>NHS</strong> <strong>Trust</strong><br />
<strong>MRSA</strong> POLICY<br />
Contents<br />
Section Title Page<br />
1.0 PURPOSE 6<br />
2.0 SCOPE 6<br />
3.0 ROLES AND RESPONSIBILITIES 6<br />
4.0 INTRODUCTION 7<br />
5.0 ANTIBIOTICS 8<br />
6.0 <strong>MRSA</strong> SCREENING 8<br />
7.0 DECOLONISATION AND TREATMENT 11<br />
8.0 WARD STAFF RESPONSIBILITY 12<br />
9.0 POST TREATMENT 12<br />
10.0 CONTACT SCREENING 13<br />
11.0 ISOLATION OPTIONS 13<br />
12.0 HIGH RISK AREAS 13<br />
13.0 MEDIUM RISK AREAS 14<br />
14.0 LOW RISK AREAS 14<br />
15.0 COHORT BAY OF PATIENTS WITH <strong>MRSA</strong> 14<br />
16.0 SURVEILLANCE 15<br />
17.0 IF A SINGLE CASE IS FOUND ON A WARD 15<br />
18.0 IF 2 OR MORE CASES ARE FOUND IN A WARD 16<br />
THIS MAY CONSITUTE AN OUTBREAK<br />
19.0 BANK AND AGENCY STAFF 17<br />
20.0 STAFF SCREENING 17<br />
21.0 VISITS BY <strong>MRSA</strong> POSITIVE PATIENTS TO OTHER 18<br />
DEPARTMENTS<br />
22.0 PATIENTS WITH <strong>MRSA</strong> HAVING A SURGICAL 18<br />
PROCEDURE<br />
23.0 TRANSFER OF PATIENT TO ANOTHER HOSPITAL 19<br />
24.0 TELLING PATIENTS AND RELATIVES 20<br />
25.0 INFORMATION FOR HEALTHCARE STAFF 20<br />
VISITING THE WARD<br />
26.0 VISITORS – FRIENDS AND RELATIVES 21<br />
27.0 PATIENT DISCHARGE 21<br />
28.0 PATIENT EQUIPMENT 21<br />
29.0 CLEANING, WASTE AND LINEN 22<br />
30.0 DECEASED PATIENTS 22<br />
31.0 TRAINING IMPLICATIONS 22<br />
32.0 MONITORING COMPLIANCE WITH AND 23<br />
EFFECTIVENESS OF THE POLICY<br />
33.0 DEFINITIONS 23<br />
34.0 REFERENCES 24<br />
Authorities<br />
Document Control Information<br />
Author: Sue Dailly Lead Nurse IC Type: Policy<br />
Sponsor: Director of Infection Prevention and Control Scope: Major<br />
Reference: CP055<br />
Issue Number: 4<br />
Date April 2010 Status: Published<br />
Page 4 of 55
Winchester & Eastleigh Healthcare <strong>NHS</strong> <strong>Trust</strong><br />
<strong>MRSA</strong> POLICY<br />
Appendix 1 Admission Screening 27<br />
Appendix 2 Decolonisation 32<br />
Appendix 3 Isolation procedures 35<br />
Appendix 4 Kingfisher ward 36<br />
Appendix 5 <strong>MRSA</strong> cohorts 37<br />
Appendix 6 Patient visits to other departments 38<br />
Appendix 7 Patients going to theatre 40<br />
Appendix 8 Transfer of patients to another hospital 41<br />
Appendix 9 Cleaning, waste and linen 42<br />
Appendix 10 Control of VISA and VRSA 44<br />
Appendix 11 <strong>MRSA</strong> staff screening regime 46<br />
Appendix 12 Criteria for elective screening exemptions 53<br />
Appendix 13 Equality Impact Assessment Tool 54<br />
Appendix 15 Communication log 55<br />
Authorities<br />
Document Control Information<br />
Author: Sue Dailly Lead Nurse IC Type: Policy<br />
Sponsor: Director of Infection Prevention and Control Scope: Major<br />
Reference: CP055<br />
Issue Number: 4<br />
Date April 2010 Status: Published<br />
Page 5 of 55
Winchester & Eastleigh Healthcare <strong>NHS</strong> <strong>Trust</strong><br />
<strong>MRSA</strong> POLICY<br />
1.0 PURPOSE<br />
1.1 Specific guidelines for the control and prevention of spread are justified<br />
because <strong>MRSA</strong> can cause serious illness and results in significant additional<br />
healthcare costs. Approximately a third of those colonized with <strong>MRSA</strong> will<br />
develop an infection, including invasive infection which may result in<br />
death (Joint Working Party 2006).<br />
1.2 The <strong>Trust</strong>’s objective is to reduce the spread of <strong>MRSA</strong> and minimize the impact<br />
in high risk patients and key clinical areas. Controls have a substantial impact<br />
on both the reservoir of <strong>MRSA</strong> patients and the attack rate of <strong>MRSA</strong><br />
bacteraemia. <strong>MRSA</strong> control measures as part of an infection control<br />
programme can also reduce the impact of other multi-resistant bacteria in ill<br />
patients<br />
2.0 SCOPE<br />
2.1 This <strong>policy</strong> extends to cover all Winchester and Eastleigh Healthcare <strong>NHS</strong><br />
<strong>Trust</strong>. This <strong>policy</strong> will also apply to honorary contract holders and staff<br />
employed by other organizations, who work with the Winchester and Eastleigh<br />
Healthcare <strong>NHS</strong> <strong>Trust</strong> patients and for the <strong>Trust</strong>’s other staff.<br />
2.2 This <strong>policy</strong> complements professional and ethical guidelines and the NMC Code<br />
of Professional Conduct (NMC 2008).<br />
2.3 Infection control is the responsibility of ALL staff associated with patient care. A<br />
high standard of infection control is required on ALL wards and units,<br />
although the level of risk may vary. It is an important part of total patient care.<br />
2.4 It is essential that infection control is seen as an organizational<br />
responsibility and priority, that adequate facilities and resources are<br />
provided, and that appropriate infection control staff and support services are<br />
available.<br />
3.0 DUTIES, ROLES AND RESPONSIBILITIES<br />
3.1 Chief Executive Officer(CEO)<br />
The CEO has overall responsibility for ensuring the <strong>Trust</strong> has appropriate<br />
strategies, policies and procedures in place to ensure the <strong>Trust</strong> continues to<br />
work to best practice and complies with all legislation. The CEO has overall<br />
responsibility for the provision of adequate isolation facilities to enable national<br />
guidance on the control of <strong>MRSA</strong> to be implemented. There is a mandatory<br />
requirement for the CEO to report all cases of <strong>MRSA</strong> bacteraemia to the Health<br />
Protection Agency.<br />
Authorities<br />
Document Control Information<br />
Author: Helen Williams Type: Policy<br />
Sponsor: Chief Executive Scope: Major<br />
Reference:<br />
OP001<br />
Issue Number: 3.4<br />
Date April 2010 Status: Published<br />
Page 6 of 55
Winchester & Eastleigh Healthcare <strong>NHS</strong> <strong>Trust</strong><br />
<strong>MRSA</strong> POLICY<br />
3.2 Line managers<br />
Are responsible for ensuring this <strong>policy</strong> is accessible for all staff and that they<br />
have read and understood the content. Line managers are responsible for<br />
ensuring any changes in practice are implemented, and any further training<br />
needs identified and addressed. Line managers assist with the root cause<br />
analysis (RCA) which will be carried out on all cases of <strong>MRSA</strong> bacteraemia.<br />
3.3 All staff<br />
All staff must ensure that their practice follows the current policies. Information<br />
regarding the failure to comply with the <strong>policy</strong> (e.g. lack of training, inadequate<br />
equipment) must be reported to the line manager and the incident reporting<br />
system used where appropriate.<br />
3.4 Infection Control Team(ICT)<br />
The Infection Control Team reports cases of <strong>MRSA</strong> bacteraemia on behalf of<br />
the <strong>Trust</strong>, to the Health Protection Agency (HPA) via the national reporting<br />
system and within the <strong>Trust</strong>. Advice is provided to healthcare staff on treatment<br />
and isolation requirements of patients with <strong>MRSA</strong>. Data are collated and shared<br />
within the <strong>Trust</strong> for patient management, RCA performance, <strong>NHS</strong> <strong>Hampshire</strong><br />
and South Central SHA reporting. Formal review is via the Infection Control<br />
Committee, Patient Safety Committee and learning is also shared with the<br />
Infection Control divisional Leads.<br />
4.0 INTRODUCTION<br />
4.1 Methicillin Sensitive Staphylococcus aureus (MSSA) is a common bacterium<br />
which is carried naturally in the nose of many (about 1 in 3) healthy people and<br />
may not cause any problems. Alternatively, it may be the cause of wound or<br />
skin infections.<br />
4.2 When this bacterium becomes resistant to certain antibiotics it is referred to as<br />
<strong>MRSA</strong> – Methicillin Resistant Staphylococcus aureus. <strong>MRSA</strong> was first reported<br />
in 1961. There are many different strains of <strong>MRSA</strong> and some spread more<br />
easily than others.<br />
4.3 Data available to date strongly implicate <strong>MRSA</strong> as a significant cause of<br />
hospital acquired infection resulting in additional mortality and morbidity as well<br />
as contributing to healthcare costs.<br />
4.4 Patients and the public are increasingly seeing <strong>MRSA</strong> and rates of <strong>MRSA</strong><br />
infections as indicators of the quality of patient care. They require assurance<br />
that all healthcare professionals are taking reasonable and sensible precautions<br />
to minimize spread.<br />
Authorities<br />
Document Control Information<br />
Author: Sue Dailly Lead Nurse IC Type: Policy<br />
Sponsor: Director of Infection Prevention and Control Scope: Major<br />
Reference: CP055<br />
Issue Number: 4<br />
Date April 2010 Status: Published<br />
Page 7 of 55
Winchester & Eastleigh Healthcare <strong>NHS</strong> <strong>Trust</strong><br />
<strong>MRSA</strong> POLICY<br />
4.5 Control measures have been shown to be effective, resulting in reduced<br />
mortality as well as helping to contain healthcare costs. Consequently the<br />
national <strong>MRSA</strong> Working Party is of the strong opinion that an active <strong>MRSA</strong><br />
control programme, as part of an overall infection control strategy within a<br />
hospital, continues to be the recommended approach.<br />
4.6 Good infection control practice should be placed at the centre of clinical<br />
practice and requires explicit support of the organisational executive to<br />
ensure that it is seen as having an appropriate position within the<br />
organisation and can be enforced as a matter of clinical governance.<br />
5.0 ANTIBIOTICS<br />
5.1 Excessive use of antibiotics promotes the spread of existing strains of<br />
<strong>MRSA</strong> through reduction in colonization resistance in patients and by<br />
giving resistant strains a survival advantage in a hospital setting.<br />
5.2 Antibiotic usage should be guided by the following:<br />
Authorities<br />
1 Ensuring that antibiotics are given at the correct dosage and for an<br />
appropriate duration because inappropriate antibiotic use promotes the<br />
emergence and spread of antibiotic resistance<br />
2 Avoidance of inappropriate or excessive antibiotic therapy and prophylaxis in<br />
all healthcare settings.<br />
3 Limiting the use of glycopeptide antibiotics to situations where their use has<br />
been shown to be appropriate. If possible prolonged courses should be<br />
avoided.<br />
4 Reduce the use of broad spectrum antibiotics, particularly third generation<br />
cephalosporins and fluoroquinolones, to what is clinically appropriate,<br />
because exposure to these are independent risk factors for <strong>MRSA</strong><br />
colonization and infection.<br />
5.3 Instituting antibiotic stewardship programmes to include surveillance of<br />
antibiotic resistance and antibiotic consumption, and prescriber education will<br />
help to manage <strong>MRSA</strong> within a <strong>Trust</strong>. See CP014 Antibiotic Policy for<br />
adults for further details<br />
6.0 <strong>MRSA</strong> SCREENING<br />
6.1.1 Patients sometimes bring <strong>MRSA</strong> into our hospitals without their or our<br />
knowledge, sometimes from other hospitals in Britain or abroad where they<br />
have received treatment or from the community. Patients from residential and<br />
Document Control Information<br />
Author: Sue Dailly Lead Nurse IC Type: Policy<br />
Sponsor: Director of Infection Prevention and Control Scope: Major<br />
Reference: CP055<br />
Issue Number: 4<br />
Date April 2010 Status: Published<br />
Page 8 of 55
Winchester & Eastleigh Healthcare <strong>NHS</strong> <strong>Trust</strong><br />
<strong>MRSA</strong> POLICY<br />
nursing homes may also bring <strong>MRSA</strong> into our hospitals. Occasionally other<br />
patients from the community who may have no known risk factors are identified.<br />
For these reasons all elective and emergency patients will now be screened for<br />
<strong>MRSA</strong>, either pre-admission or on admission, except those excluded by DH<br />
guidance ( see page 19 for details)<br />
6.1.2 The aim of screening is to identify all positive patients before or on admission to<br />
the hospital, to allow decolonisation treatment to reduce their risk of infection.<br />
This also enables the <strong>Trust</strong> to target the use of isolation and cohort facilities in<br />
order to minimize the risk of onward transmission to other patients.<br />
6.1.3 In most cases <strong>MRSA</strong> will not actually be causing an infection but is merely<br />
present (colonising) for example the nose or groin. <strong>MRSA</strong> colonisation does<br />
make the person a potential source of spread to others. Colonized and infected<br />
patients are the primary reservoir of <strong>MRSA</strong> for others, and their identification by<br />
active screening allows focusing of effective but limited infection control<br />
resources (Farr 2002).<br />
6.1.4 Since February 2008 all emergency medical admissions have been screened<br />
for <strong>MRSA</strong>. Screening of all elective surgical patients commenced in February<br />
2009 and the programme was rolled out by April 2009, with monitoring<br />
throughout 2009. Screening all other emergency patients commenced in<br />
December 2009 and will roll out in advance of the December 2010 DH deadline.<br />
The SHA have requested all emergency patients are screened for <strong>MRSA</strong> by<br />
March 2010. The aim is universal <strong>MRSA</strong> screening of ALL appropriate elective<br />
and emergency patients from 2010 onwards.<br />
• See Table 1 for details of admission screening regime for each ward<br />
6.2 What <strong>MRSA</strong> screening swabs to take and when<br />
6.2.1 Wounds include sites of intravenous cannula (IV), central vascular access<br />
device (CVAD) and other line insertion sites, all skin lesions, leg ulcers,<br />
pressure sores, surgical and trauma wounds, cuts and grazes.<br />
6.2.2 <strong>MRSA</strong> may also be found on other specimens submitted for clinical reasons,<br />
such as sputum. In such cases follow up specimens from the same site should<br />
be included as part of the screening set.<br />
6.2.3 Patients who are persistently colonised will require a throat swab to be taken.<br />
6.2.4 Screening table: definitions<br />
High risk patients - Admissions from Nursing Homes, Residential homes, other health<br />
or social care institutions, anyone admitted within last 12 months. Hospital transfers or<br />
Authorities<br />
Document Control Information<br />
Author: Sue Dailly Lead Nurse IC Type: Policy<br />
Sponsor: Director of Infection Prevention and Control Scope: Major<br />
Reference: CP055<br />
Issue Number: 4<br />
Date April 2010 Status: Published<br />
Page 9 of 55
Winchester & Eastleigh Healthcare <strong>NHS</strong> <strong>Trust</strong><br />
<strong>MRSA</strong> POLICY<br />
transfers from any health care institution abroad, IV drug users. Those who play<br />
contact sports (e.g. rugby, football, martial arts)<br />
CSU – take sample if catheter present on admission<br />
Table 1<br />
NOSE<br />
SKIN<br />
BREAKS<br />
GROIN<br />
[Only if<br />
no skin<br />
break]<br />
CSU* [Only sample<br />
if catheter in place on<br />
admission]<br />
MEDICAL DIVISION<br />
All emergency Admissions √ √ √ √<br />
All elective admissions √ √ √ √<br />
All previous <strong>MRSA</strong> +ve or high risk<br />
√<br />
patients √ √ must do<br />
√<br />
SURGICAL WARDS<br />
Emergency Admissions √ √ √ √<br />
All elective admissions √ √ √ √<br />
All previous <strong>MRSA</strong> +ve or high risk<br />
√<br />
patients √ √ must do<br />
√<br />
ITU/HDU admissions √ √ √ √<br />
ORTHOPAEDIC WARDS<br />
All emergency Admissions √ √ √ √<br />
All elective admissions √ √ √ √<br />
All previous <strong>MRSA</strong> +ve or high risk<br />
√<br />
patients √ √ must do<br />
√<br />
MATERNITY<br />
All elective caesarean sections √ √ √ √<br />
All previous <strong>MRSA</strong> +ve or high risk<br />
patients √ √<br />
√<br />
must do<br />
√<br />
<strong>MRSA</strong> contacts (Ante-natal) √ √<br />
√<br />
must do<br />
√<br />
Works in health care environment<br />
(48 hours after last working day √ √<br />
√<br />
must do<br />
√<br />
GYNAE WARD<br />
Emergency Admissions √ √ √ √<br />
All elective admissions √ √ √ √<br />
All previous <strong>MRSA</strong> +ve or high risk<br />
patients √ √ √ √<br />
NORTHBROOK<br />
Emergency & Elective High Risk<br />
Patients* √ √<br />
√<br />
must do<br />
√<br />
All previous <strong>MRSA</strong> +ve or high risk<br />
patients √ √ √ √<br />
ALL DIVISIONS/WARDS<br />
Inpatient <strong>MRSA</strong> contacts √ √ √ √<br />
NEO-NATAL UNIT<br />
Post natal admissions √ √ Umbilicus/Ear<br />
Hospital Transfers & Andover Birth √ √ Umbilicus/Ear<br />
Authorities<br />
Document Control Information<br />
Author: Sue Dailly Lead Nurse IC Type: Policy<br />
Sponsor: Director of Infection Prevention and Control Scope: Major<br />
Reference: CP055<br />
Issue Number: 4<br />
Date April 2010 Status: Published<br />
Page 10 of 55
Centre<br />
Winchester & Eastleigh Healthcare <strong>NHS</strong> <strong>Trust</strong><br />
<strong>MRSA</strong> POLICY<br />
Emergency admissions/from home √ √ Umbilicus/Ear<br />
6.3 Emergency Re-admission of previously <strong>MRSA</strong> positive patients<br />
6.3.1 Patients who have had <strong>MRSA</strong> in the past must have a full screen on admission,<br />
and be isolated in a single room until the <strong>MRSA</strong> screening result is known.<br />
They should not be cohort nursed with other <strong>MRSA</strong> patients until proven<br />
positive on this admission and found to be suitable to be cohort nursed with<br />
others. Please inform Infection Control via phone or email when a patient who<br />
has had <strong>MRSA</strong> in the past is admitted. Please check the patient’s medical<br />
notes for <strong>MRSA</strong> stickers and specific details on the patients electronic CRS<br />
(Care Records Service) clinical records for electronic alerts and yellow stars.<br />
6.3.2 Patients admitted from areas where <strong>MRSA</strong> is known to be present, or have<br />
had <strong>MRSA</strong> in the past, should be isolated until <strong>MRSA</strong> carriage has been<br />
excluded.<br />
6.3.3 <strong>MRSA</strong> positive patients should not be admitted to the Treatment Centre.<br />
6.4 Routine screening<br />
6.4.1 Regular (weekly/monthly) screening of all patients on high risk units may be<br />
requested due to an outbreak or unusual event. At present, there is regular<br />
weekly screening of all patients in ITU / NNU. Regular screening is not carried<br />
out on any other wards.<br />
7.0 DECOLONISATION AND TREATMENT<br />
7.1 Complete eradication is not always possible but a decrease of <strong>MRSA</strong><br />
carriage can reduce the risk of transmission in healthcare settings.<br />
7.2 Decolonisation will also reduce the risk of infection eg via inoculation in the<br />
patient’s own surgical wound during an operation. See Appendix 7 for details of<br />
prophylaxis and care of patients having a surgical procedure. Theatre staff to<br />
refer to the LTP09 <strong>MRSA</strong> Theatre Policy for further specific information.<br />
7.3 The efficacy of any decolonisation regimen will depend on the presence of<br />
wounds, skin lesions and foreign bodies such as urinary catheters, nasogastric<br />
tubes and haemodialysis lines. It also requires the thorough application of<br />
topical treatments.<br />
Authorities<br />
Document Control Information<br />
Author: Sue Dailly Lead Nurse IC Type: Policy<br />
Sponsor: Director of Infection Prevention and Control Scope: Major<br />
Reference: CP055<br />
Issue Number: 4<br />
Date April 2010 Status: Published<br />
Page 11 of 55
Winchester & Eastleigh Healthcare <strong>NHS</strong> <strong>Trust</strong><br />
<strong>MRSA</strong> POLICY<br />
7.4 Higher success rates are reported for eradicating <strong>MRSA</strong> from hospitalized<br />
patients using a protocol that includes mupirocin® nasal ointment, daily<br />
chlorhexidine i.e. Hibiscrub baths, systemic therapy and removal and<br />
replacement of all foreign bodies (e.g. catheters) and routine cleaning of the<br />
environment. Using a combination of interventions together gives a better<br />
success rate of decolonization.<br />
7.5 Each patient’s <strong>MRSA</strong> infection must be assessed individually.<br />
Treatment whether oral or IV should follow CP014 Antibiotic Policy for<br />
adults (available on the intranet). Consultant Microbiologists are available<br />
for advice.<br />
• See Appendix 2 for details of decolonisation options and treatment.<br />
8.0 WARD STAFF RESPONSIBILITY<br />
8.1 It is the responsibility of the ward staff, nurses and doctors, to be aware of each<br />
patient’s <strong>MRSA</strong> status and at what stage of treatment they are. Delays in<br />
screening patients means they remain isolated in side rooms for unnecessary<br />
periods of time. The detrimental psychological effect of being isolated in a<br />
single room is well documented, so staff should make every effort to ensure<br />
that complete sets of screening samples are taken on time and the progress of<br />
results and treatment is documented. An <strong>MRSA</strong> care plan should be used to<br />
record and monitor a patient’s progress (template found on the Intranet under<br />
Infection Control documents).<br />
8.2 Starting sometime in 2010 patients newly identified as having <strong>MRSA</strong> will be<br />
provided with an <strong>MRSA</strong> Hand Held records book. The Infection Control nurses<br />
will supply the inpatients on the wards with these books. Pre-Assessment clinics<br />
will supply these books to their patients, and GPs will give them to patients<br />
identified via samples taken in the community. Each time a patient visits the<br />
<strong>Trust</strong>, for any reason, these records should be checked and up-dated so that<br />
recent information on screening and treatment are logged. Other <strong>Trust</strong>s within<br />
the area will also be providing these hand held records to their newly identified<br />
<strong>MRSA</strong> patients.<br />
8.3 Treatment at discharge<br />
8.4 Patients discharged during a course of treatment should complete their topical<br />
treatment and course of antibiotics if prescribed. There is no requirement for<br />
patients colonized with <strong>MRSA</strong> to continue extended eradication protocols after<br />
discharge. Treatment may continue if there is an anticipated re-admission to<br />
hospital, especially for a planned invasive procedure.<br />
Authorities<br />
Document Control Information<br />
Author: Sue Dailly Lead Nurse IC Type: Policy<br />
Sponsor: Director of Infection Prevention and Control Scope: Major<br />
Reference: CP055<br />
Issue Number: 4<br />
Date April 2010 Status: Published<br />
Page 12 of 55
Winchester & Eastleigh Healthcare <strong>NHS</strong> <strong>Trust</strong><br />
<strong>MRSA</strong> POLICY<br />
8.5 The general practitioner (GP) and others involved in the patient’s community<br />
care should be informed of the patient’s individual <strong>MRSA</strong> status at discharge via<br />
the discharge letter and the patient’s hand held records.<br />
8.6 If a patient is discharged to a residential care facility the medical and/or nursing<br />
staff should be informed in advance.<br />
8.7 Colonisation or infection with <strong>MRSA</strong> is not a contra-indication to the transfer of a<br />
patient to a nursing or convalescent home. The carriage of <strong>MRSA</strong> is not a valid<br />
reason for exclusion from residential care homes.<br />
9 POST TREATMENT<br />
9.1 A full screen must be taken on day 3 after antibiotic and topical treatment has<br />
finished.<br />
9.2 Full screen to include, nose, groin, skin breaks, any wounds and CSU if<br />
catheter present. Other samples may be required if the patient had <strong>MRSA</strong> at<br />
other sites e.g. sputum/throat.<br />
9.3 If the patient is still <strong>MRSA</strong> positive, topical treatment will be re-commenced.<br />
After two episodes of treatment the individual will be reviewed. A course of<br />
Mupirocin® treatment should not be given more than twice, within a short period<br />
of time, without consulting the Infection Control Team. (ICT)<br />
9.4 There is no evidence that once colonised any group of patients remain<br />
permanently <strong>MRSA</strong> free after a decolonisation regime. It should be assumed<br />
that previously positive patients are always potentially carrying <strong>MRSA</strong>.<br />
10 CONTACT SCREENING<br />
10.1 <strong>MRSA</strong> contacts should be screened once the patient with <strong>MRSA</strong> has been<br />
moved from the ward bay. Nose, skin breaks /wound swabs or groins and<br />
CSUs must be taken.<br />
11.0 ISOLATION OPTIONS<br />
11.1 The provision of <strong>MRSA</strong> isolation precautions must take into consideration:<br />
1 Ward speciality<br />
2 Whether affected patients are likely to be heavy skin shedders<br />
3 Whether patients are at high risk of developing invasive infection e.g.<br />
patients with multiple trauma, major life saving surgery, patients on<br />
immuno-suppressive therapy<br />
4 Design of ward<br />
Authorities<br />
Document Control Information<br />
Author: Sue Dailly Lead Nurse IC Type: Policy<br />
Sponsor: Director of Infection Prevention and Control Scope: Major<br />
Reference: CP055<br />
Issue Number: 4<br />
Date April 2010 Status: Published<br />
Page 13 of 55
Winchester & Eastleigh Healthcare <strong>NHS</strong> <strong>Trust</strong><br />
<strong>MRSA</strong> POLICY<br />
5 Provision of side rooms<br />
6 Resistance pattern, virulence and potential transmissibility of the<br />
organism<br />
See Appendix 10 for advice regarding Vancomycin Resistant Staphylococcus<br />
aureus and Vancomycin Intermediate Staphylococcus aureus<br />
• Patient’s medical and psychological welfare should not be<br />
compromised by unnecessarily restrictive infection control practices<br />
12 High Risk Areas<br />
12.1 High risk areas include wards or units where the consequence of uncontrolled<br />
<strong>MRSA</strong> is serious because of the risk of invasive infection and difficulties in<br />
treatment e.g. ITU, neonatal intensive care, orthopaedic, trauma and<br />
vascular wards and those where patients are having implants.<br />
12.2 No patient with <strong>MRSA</strong> will be admitted to an elective orthopaedic ward.<br />
12.3 On all the other high risk wards patients must be isolated in a single room<br />
unless their clinical condition would be compromised by being isolated. The<br />
patient’s condition must be reviewed daily and infection control precautions<br />
taken within the bay. When the patient can be safely isolated provision should<br />
be made promptly to move the patient into a side room or cohort bay. All<br />
patient contacts must then be screened.<br />
13 Medium risk areas<br />
13.1 Medium risk areas include admission wards, general surgery, paediatric,<br />
general medicine and elderly medicine.<br />
13.2 Ideally these patients should be isolated in single rooms. Cohorting patients in<br />
a defined area of the ward and using designated staff may be a necessary<br />
alternative to using single rooms where there are more cases of <strong>MRSA</strong> than<br />
side rooms available. Such areas should be capable of physical separation<br />
from other ward areas.<br />
13.3 <strong>MRSA</strong> positive patients should not be admitted to the Treatment Centre.<br />
14 Low risk areas<br />
14.1 These are areas where patients are at a low risk of invasive infection but the<br />
patients are at a high risk of colonisation e.g. nursing homes, psycho-geriatric<br />
and long term care facilities. Hence, consideration must be given to a<br />
balance between risk of infection and need for rehabilitation and social contact.<br />
Authorities<br />
Document Control Information<br />
Author: Sue Dailly Lead Nurse IC Type: Policy<br />
Sponsor: Director of Infection Prevention and Control Scope: Major<br />
Reference: CP055<br />
Issue Number: 4<br />
Date April 2010 Status: Published<br />
Page 14 of 55
Winchester & Eastleigh Healthcare <strong>NHS</strong> <strong>Trust</strong><br />
<strong>MRSA</strong> POLICY<br />
14.2 In these area patients at high risk of transmission of <strong>MRSA</strong> should be<br />
isolated e.g. skin shedders and those with throat colonisation and a<br />
productive cough.<br />
Authorities<br />
• See Appendix 3 for details on how to barrier nurse a patient with <strong>MRSA</strong><br />
• See Appendix 4 for protocol for Kingfisher ward<br />
15 COHORT BAY OF PATIENTS WITH <strong>MRSA</strong><br />
15.1 The site co-ordinator and the IC team will allocate patients to the <strong>MRSA</strong> bay in<br />
consultation with ward staff. It is important to check at which sites the <strong>MRSA</strong><br />
patient is positive, whether he/she is on treatment and that the patient is<br />
suitable to be placed in the bay (Cooper 2003).<br />
15.2 Patients admitted to an <strong>MRSA</strong> bay must have <strong>MRSA</strong> positive<br />
microbiology results from this admission or within the last 14 days. These could<br />
include results from a specimens sent by a GP or from a recent previous<br />
admission (within the last 2 weeks).<br />
15.3 Patients who have been identified as being <strong>MRSA</strong> positive more than 14 days<br />
ago, or have a history of being <strong>MRSA</strong> positive, cannot be admitted into the<br />
<strong>MRSA</strong> bay until they are proven to be still <strong>MRSA</strong> positive. These patients<br />
should be admitted into a side room and screened. They can be transferred<br />
into an <strong>MRSA</strong> bay if they are found to be positive, AND are compatible with the<br />
other patients in the bay i.e. same antibiotic pattern and similar sites positive.<br />
15.4 Not all patients with <strong>MRSA</strong> are suitable for nursing in a bay with other<br />
<strong>MRSA</strong> patients. The ICT will assess the individual patient’s suitability.<br />
• See Appendix 5 for details on how to set up and run a cohort bay of <strong>MRSA</strong><br />
patients<br />
16 SURVEILLANCE<br />
16.1 Surveillance is carried out as part of the hospital’s infection control programme<br />
and is an element of clinical governance.<br />
16.2 Surveillance data are collected on :<br />
• Number of new cases of <strong>MRSA</strong><br />
• Ward<br />
• Source of their <strong>MRSA</strong> e.g. hospital or community acquired<br />
• Colonisation or infection<br />
Document Control Information<br />
Author: Sue Dailly Lead Nurse IC Type: Policy<br />
Sponsor: Director of Infection Prevention and Control Scope: Major<br />
Reference: CP055<br />
Issue Number: 4<br />
Date April 2010 Status: Published<br />
Page 15 of 55
Winchester & Eastleigh Healthcare <strong>NHS</strong> <strong>Trust</strong><br />
<strong>MRSA</strong> POLICY<br />
• Mandatory bacteraemia data<br />
16.3 Surveillance data are fed back to staff on a quarterly basis and are discussed at<br />
the Infection Control Committee. These data are used to target infection control<br />
resources e.g. increased education. RCA findings on bacteraemias are fed<br />
back contemporaneously to relevant staff and more widely when appropriate for<br />
learning.<br />
17 IF A SINGLE CASE IS FOUND ON A WARD<br />
If a single case of <strong>MRSA</strong> is found on a ward (index case):<br />
17.1 The <strong>MRSA</strong> positive patient should be discharged from hospital if the clinical<br />
condition allows, or isolated in a single room and barrier nursed if discharge is<br />
not possible.<br />
17.2 Patients in the same bay should have one set of screening swabs taken from<br />
their nose, skin breaks / wounds, groins and CSU if a catheter is present.<br />
17.3 Patients should not be transferred from the contact bay to other ward until<br />
discussed with the Infection Control Team (in an emergency please inform the<br />
receiving ward that a side room is required).<br />
17.4 Once the bed, fittings and furniture have been cleaned and the curtains in the<br />
bed space changed, the empty bed in the bay can be used.<br />
18 IF 2 OR MORE CASES ARE FOUND IN A WARD THIS MAY CONSITUTE AN<br />
OUTBREAK<br />
18.1 If the contacts of the index case are found to be <strong>MRSA</strong> positive the<br />
following action MAY BE requested by the Infection Control Team.<br />
Each incident will be considered on an individual basis as the risk for<br />
patients varies with different specialities.<br />
1 Close affected bay to admissions and transfers<br />
2 Close ward to admissions and transfers<br />
3 Contact screen all patients on the ward<br />
4 Screening of staff<br />
18.2 Factors influencing consideration of ward closure to admissions<br />
include:<br />
1 Risk status of patients to be admitted<br />
2 Number of cases of <strong>MRSA</strong> present on the ward<br />
3 <strong>MRSA</strong> strain e.g. virulence, resistance<br />
Authorities<br />
Document Control Information<br />
Author: Sue Dailly Lead Nurse IC Type: Policy<br />
Sponsor: Director of Infection Prevention and Control Scope: Major<br />
Reference: CP055<br />
Issue Number: 4<br />
Date April 2010 Status: Published<br />
Page 16 of 55
Winchester & Eastleigh Healthcare <strong>NHS</strong> <strong>Trust</strong><br />
<strong>MRSA</strong> POLICY<br />
4 Ward/unit staffing levels<br />
5 Ability to isolate/cohort colonised patients and contacts during<br />
quarantine.<br />
18.3 Wards will only be closed on infection control grounds, following<br />
recommendation from the Consultant Microbiologist, and after discussion with<br />
the ward manager, Consultants, Management and the Infection Control Team.<br />
18.4 Patients maybe discharged home or to a nursing or residential home, other<br />
wards or other hospitals ONLY after discussion with the Infection Control Team.<br />
18.5 Before re-opening to new admissions the ward/unit must have a terminal clean,<br />
including the changing of curtains.<br />
18.6 Ward closure to new admissions may need to be considered in certain<br />
circumstances on the basis of risk assessment. The Consultant<br />
Microbiologist will make the decision when to close and re-open a ward.<br />
18.7 Any ward closure has to be reported on PRISM and as a SUI (serious untoward<br />
incident). Details must be sent to the Director of Infection Prevention and<br />
Control (DIPC) and the Head of Patient Safety and Healthcare Governance.<br />
18.8 Discharge screening from the affected area may be instituted by the Consultant<br />
Microbiologist.<br />
18.9 If an outbreak is declared, an outbreak control meeting will be convened by the<br />
DIPC (see Ward Closure Policy). In the event of a major outbreak, the Major<br />
Outbreak Plan should be followed (available in the Infection Control Manual or<br />
on the <strong>Trust</strong> intranet).<br />
19 BANK AND AGENCY STAFF<br />
19.1 Where possible ward staff should avoid using bank and agency staff to care for<br />
patients known to be <strong>MRSA</strong> positive or are being barrier nursed. This is<br />
because these staff move around the wards and increase the potential of<br />
spreading <strong>MRSA</strong>. BUT the needs and care of the patient must take priority and<br />
where it is necessary bank and agency staff can care for patients known to<br />
have <strong>MRSA</strong>. Ward staff must check the competence of bank and agency staff<br />
to carry out isolation nursing safely. Good hand hygiene is critical to the<br />
prevention of spread of <strong>MRSA</strong>.<br />
20 STAFF SCREENING<br />
20.1 Screening of staff is not recommended routinely. Staff screening is indicated if:<br />
Authorities<br />
Document Control Information<br />
Author: Sue Dailly Lead Nurse IC Type: Policy<br />
Sponsor: Director of Infection Prevention and Control Scope: Major<br />
Reference: CP055<br />
Issue Number: 4<br />
Date April 2010 Status: Published<br />
Page 17 of 55
Winchester & Eastleigh Healthcare <strong>NHS</strong> <strong>Trust</strong><br />
<strong>MRSA</strong> POLICY<br />
1 New carriers are found among the patients<br />
2 Transmission continues on a unit despite active control measures<br />
3 If epidemiological aspects of an outbreak are unusual<br />
4 Or if they suggest persistent <strong>MRSA</strong> carriage by staff<br />
20.2 New staff should be screened for <strong>MRSA</strong> if they have ever been <strong>MRSA</strong> positive.<br />
A full screen must be taken. If they are clinical staff and will be working in the<br />
surgical or orthopaedic unit/ ITU / NNU. A nasal swab should be taken and<br />
swabs from any skin breaks/wounds if present. Staff can begin work before the<br />
results are known.<br />
20.3 <strong>MRSA</strong> screening of new staff will be co-ordinated by the Occupational<br />
Health and Safety Department (OH&S). <strong>MRSA</strong> screening due to an outbreak<br />
will be coordinated by the Infection Control team. Coordination of treatment and<br />
follow up screening will be carried out by the Occupational Health & Safety<br />
Department.<br />
20.4 Care is needed to distinguish between transient carriage (i.e. carriage<br />
which is lost within a day or so of removal from contact with <strong>MRSA</strong> positive<br />
patients which carries little risk of onward transmission) and prolonged carriage<br />
(especially associated with throat colonization and skin lesions).<br />
20.5 This is best achieved by screening staff as they come on duty at the<br />
beginning of their shift, and not as they leave.<br />
20.6 Nurses, doctors, physiotherapists, other allied health professionals and nonclinical<br />
support staff should be considered for screening. Locum and agency<br />
staff may need to be screened if the Infection Control Team deems it<br />
necessary.<br />
20.7 Please see Appendix 11 for advice on staff screening and the OH&S<br />
Department data sheets (also available from OH&S department) on swabbing,<br />
treatment and working restrictions for staff.<br />
21 VISITS BY <strong>MRSA</strong> POSITIVE PATIENTS TO OTHER DEPARTMENTS<br />
21.1 Visits by <strong>MRSA</strong> positive patients to other departments should be kept to a<br />
minimum. If it is necessary either for investigation, treatment or to visit<br />
another member of the family, prior arrangements should be made with the<br />
staff of the receiving department, so that control of infection measures can be<br />
implemented.<br />
• See Appendix 6 for details of safe movement of patients around the<br />
hospital and visits to other departments. See also CP061 Policy for the Intra<br />
ward transfer of patients with Infection Control issues.<br />
Authorities<br />
Document Control Information<br />
Author: Sue Dailly Lead Nurse IC Type: Policy<br />
Sponsor: Director of Infection Prevention and Control Scope: Major<br />
Reference: CP055<br />
Issue Number: 4<br />
Date April 2010 Status: Published<br />
Page 18 of 55
Winchester & Eastleigh Healthcare <strong>NHS</strong> <strong>Trust</strong><br />
<strong>MRSA</strong> POLICY<br />
22 PATIENTS WITH <strong>MRSA</strong> UNDERGOING A SURGICAL PROCEDURE<br />
22.1 Following the circulation of the Department of Health Operating Framework for<br />
2008/9 all elective patients must be screened for <strong>MRSA</strong>. This includes<br />
medicine, surgery, family services and orthopaedics.<br />
22.2 <strong>MRSA</strong> operational guidance issued in 2008 clarified the criteria for elective<br />
screening exemptions:<br />
• Day case ophthalmology<br />
• Day case dental<br />
• Day case endoscopy<br />
• Minor dermatology procedures<br />
• Paediatrics – unless high risk<br />
• Maternity except elective caesarean sections and high risk cases<br />
If these patients have previously had <strong>MRSA</strong> they should be screened prior to<br />
admission, like any other elective <strong>MRSA</strong> positive patient. See Appendix 12 for<br />
updated information regarding inclusion or exclusion criteria for elective <strong>MRSA</strong><br />
screening. Any changes will be communicated directly to staff involved in<br />
elective screening of patients and updated on the trust intranet and Infection<br />
Control intranet site.<br />
22.3 Elective patients who are found to be <strong>MRSA</strong> positive following screening will be<br />
divided into 2 different patient pathways.<br />
22.4 High Risk Patients<br />
• Orthopaedics – especially prosthetic<br />
• Vascular grafts<br />
• Breast implants and complex surgery<br />
• Cardio thoracic<br />
• Diabetic patients<br />
• Any other individual patient the admitting Consultant diagnoses as high<br />
risk on a case by case basis.<br />
These patients will complete a course of decolonisation treatment provided by<br />
the <strong>Trust</strong>, or GP, and have 2 sets of negative swabs prior to admission. When<br />
admitted he/she will be isolated in a single room and re-commence a course of<br />
topical treatment prior to surgery. <strong>MRSA</strong> appropriate prophylactic antibiotics will<br />
also be given for the surgical procedure.<br />
If the patient remains <strong>MRSA</strong> positive he/she will be admitted immediately after a<br />
course of treatment with all the precautions listed above. Antibiotic prophylaxis<br />
appropriate for <strong>MRSA</strong> must be given in all such cases.<br />
Authorities<br />
Document Control Information<br />
Author: Sue Dailly Lead Nurse IC Type: Policy<br />
Sponsor: Director of Infection Prevention and Control Scope: Major<br />
Reference: CP055<br />
Issue Number: 4<br />
Date April 2010 Status: Published<br />
Page 19 of 55
Winchester & Eastleigh Healthcare <strong>NHS</strong> <strong>Trust</strong><br />
<strong>MRSA</strong> POLICY<br />
All other patients<br />
All other patients will commence topical treatment 6 days prior to their day of<br />
admission. The aim is to minimise the risk of infection by carrying out surgery<br />
immediately after a course of topical treatment. On the morning of surgery they<br />
will have mupirocin® nasal ointment applied and a chlorhexidine wash i.e.<br />
Hibiscrub. They will be admitted into a single room and barrier nursed. <strong>MRSA</strong><br />
appropriate prophylactic antibiotics will also be given. No post treatment<br />
screening swabs will be taken unless clinically required.<br />
Previously <strong>MRSA</strong> positive patients and those who are high risk of having <strong>MRSA</strong>, e.g.<br />
those living in nursing homes who are admitted as an emergency and require surgery<br />
before their <strong>MRSA</strong> status is known must commence decolonisation prior to surgery<br />
and continue post surgery. Prophylactic antibiotics must cover <strong>MRSA</strong>.<br />
22.5 No <strong>MRSA</strong> positive patient should be admitted to the Treatment Centre.<br />
• See Appendix 7 for details, also see CPr049 Theatres <strong>MRSA</strong> Policy<br />
23 TRANSFER OF PATIENT TO ANOTHER HOSPITAL<br />
23.1 Refusal to accept transfer of a patient is not justifiable on the basis of the risk<br />
posed to other patients by an individual’s carriage of, or infection with, <strong>MRSA</strong>.<br />
All units should have procedures in place and adequate facilities for<br />
containment of <strong>MRSA</strong>.<br />
23.2 Identification of infected or colonised patients is the responsibility of the<br />
transferring hospital. Before transfer a member of the clinical team for the<br />
patient, at the transferring hospital, must inform the ward staff at the receiving<br />
hospital of the patient’s status.<br />
23.3 Patients with <strong>MRSA</strong> do not need to wear a mask when travelling in the<br />
ambulance.<br />
See Appendix 8 for details of how to transport patients with <strong>MRSA</strong><br />
24 TELLING PATIENTS AND RELATIVES<br />
24.1 The implications of <strong>MRSA</strong> colonization, infection and treatment should be<br />
explained to the patient and if appropriate close relatives, at the time of<br />
diagnosis and ideally prior to transfer into a single room, isolation facility or<br />
designated cohort area.<br />
Authorities<br />
Document Control Information<br />
Author: Sue Dailly Lead Nurse IC Type: Policy<br />
Sponsor: Director of Infection Prevention and Control Scope: Major<br />
Reference: CP055<br />
Issue Number: 4<br />
Date April 2010 Status: Published<br />
Page 20 of 55
Winchester & Eastleigh Healthcare <strong>NHS</strong> <strong>Trust</strong><br />
<strong>MRSA</strong> POLICY<br />
24.2 All visitors entering an isolation room must wear gloves and apron. Thorough<br />
hand hygiene should be carried out once the gloves and apron are removed.<br />
Parents caring for their children should wear an apron but do not need to wear<br />
gloves. Parents and relatives who are staying at the hospital and using<br />
communal facilities must be careful with hand hygiene and use the alcohol gel<br />
each time they leave the isolation room.<br />
24.3 Information leaflets should be available giving general information on<br />
<strong>MRSA</strong> to the recipient ( on intranet or contact Infection Control Department for<br />
copies). Patients should be informed that there are minimal risks to healthy<br />
relatives and contacts outside the hospital, and their normal social interaction<br />
should not be compromised.<br />
24.4 Patients should be informed that if they are hospitalized in the future, they<br />
should advise admitting staff that they have been identified as carriers of <strong>MRSA</strong><br />
in the past, to ensure that they are managed appropriately. They should take<br />
their <strong>MRSA</strong> hand held records book with them when seeing healthcare staff<br />
whether at the hospital or in the community eg GP surgery.<br />
25 INFORMATION FOR HEALTHCARE STAFF VISITING THE WARD<br />
e.g. doctors, phlebotomists, physiotherapists, pharmacists (Boyce 2002)<br />
1 Staff must be bare below the elbow. Wash or gel hands and put on gloves<br />
and apron before entering the room. Minimal numbers of staff for the<br />
interaction planned should enter the isolation room or cohort bay.<br />
2 Take into the room the minimum items of equipment required. Do not place<br />
these items on the bed.<br />
3 Do not sit on the patient’s bed when you are in the room.<br />
4 When you have completed the procedure and are ready to leave, place the<br />
items near the door.<br />
5 Remove gloves and apron and place in orange waste bag.<br />
6 Wash hands thoroughly.<br />
7 Collect your equipment and leave the room.<br />
8 Use the alcohol hand gel after you have left the room.<br />
9 All items removed from the room must be cleaned before use on another<br />
patient.<br />
Authorities<br />
Document Control Information<br />
Author: Sue Dailly Lead Nurse IC Type: Policy<br />
Sponsor: Director of Infection Prevention and Control Scope: Major<br />
Reference: CP055<br />
Issue Number: 4<br />
Date April 2010 Status: Published<br />
Page 21 of 55
Winchester & Eastleigh Healthcare <strong>NHS</strong> <strong>Trust</strong><br />
<strong>MRSA</strong> POLICY<br />
26 VISITORS – FRIENDS AND RELATIVES<br />
26.1 It is safe for pregnant women and children to visit patients with <strong>MRSA</strong>. If there<br />
are specific concerns please contact the Infection Control Team for advice.<br />
Patients’ social contact such as hugging, kissing and holding hands<br />
should continue.<br />
26.2 If visiting other people in the hospital, to see these first and visit the person in<br />
isolation last.<br />
26.3 Relatives and visitors should wear gloves and apron when entering the room.<br />
They should remove their PPE, wash their hands with soap and water and use<br />
the alcohol hand gel before they leave the ward.<br />
27 PATIENT DISCHARGE<br />
27.1 There is no requirement for patients colonized with <strong>MRSA</strong> to continue extended<br />
eradication protocols after discharge, unless there is anticipated re-admission to<br />
hospital, especially for a planned invasive procedure. They should complete the<br />
course of treatment already commenced whether topical or systemic.<br />
27.2 The GP and others involved in the patients community care should be informed<br />
of the patient’s individual <strong>MRSA</strong> status at discharge in the discharge letter. The<br />
<strong>MRSA</strong> hand held record should also be updated.<br />
27.3 If a patient is discharged to a residential care facility the medical and/or<br />
nursing staff should be informed in advance.<br />
27.4 Colonisation or infection with <strong>MRSA</strong> is not a contra-indication to the<br />
transfer of a patient to a nursing or convalescent home. The carriage of <strong>MRSA</strong><br />
is not a valid reason for exclusion from residential care homes.<br />
28 PATIENT EQUIPMENT<br />
28.1 All equipment on the ward must be single use, single patient use or able to be<br />
decontaminated prior to use by another patient.<br />
28.2 Single use items or single patient use items must be disposed of in an orange<br />
waste bag after use or after the patient is discharged /transferred. Please refer<br />
to 07 Single Use Devices Policy<br />
24.3 For the cleaning of non-disposable items please refer to the CP03<br />
Disinfection, Decontamination and Cleaning Policy.<br />
Authorities<br />
Document Control Information<br />
Author: Sue Dailly Lead Nurse IC Type: Policy<br />
Sponsor: Director of Infection Prevention and Control Scope: Major<br />
Reference: CP055<br />
Issue Number: 4<br />
Date April 2010 Status: Published<br />
Page 22 of 55
Winchester & Eastleigh Healthcare <strong>NHS</strong> <strong>Trust</strong><br />
<strong>MRSA</strong> POLICY<br />
29 CLEANING, WASTE AND LINEN<br />
29.1 Management of the environment and equipment should be considered as<br />
central to decrease the spread of <strong>MRSA</strong>. General principles should be adopted<br />
to minimize the bacterial burden. The ability of <strong>MRSA</strong> to survive in dust<br />
demonstrates the need for dust minimization, the removal of bacteria from<br />
surfaces, and the appropriate disposal of contaminated waste and linen<br />
(Duckworth 1990). There should be planned, periodic and thorough cleaning of<br />
the whole ward, including bedding and curtains (French 2004).<br />
• See Appendix 9 for further details<br />
30 DECEASED PATIENTS<br />
30.1 The infection control precautions for handling deceased patients are the same<br />
as those used in life, but the mortuary should be informed if the patient has<br />
<strong>MRSA</strong> or any other infection or colonization with a resistant organism.<br />
30.2 Use a body bag the same as for other patients without <strong>MRSA</strong> – unless there are<br />
circumstances which deem a more robust body bag necessary e.g.<br />
haemorrhage.<br />
30.3 There is negligible risk to mortuary staff or undertakers provided that<br />
standard precautions are followed. For more details please see CP070 -<br />
Deceased Infected Patient Policy.<br />
31 TRAINING IMPLICATIONS<br />
• Infection control training on basic principles is part of the <strong>Trust</strong> wide mandatory<br />
training scheme for all staff and is monitored via attendance records, as per<br />
CP072 - Training Policy for Employees of WEHCT in Infection Control.<br />
• Training is offered to all staff at induction , as per OP010 - <strong>Trust</strong> Induction<br />
Policy<br />
• Training is offered to all staff at annual update<br />
• Antibiotic and infection control audits and updates are made quarterly to the<br />
Infection Control Committee and sent to every clinical team and ward<br />
• Specialty based training is offered via divisional meetings on an ongoing basis.<br />
• The link nurses /practitioners participate in a specialist programme of on going<br />
training.<br />
• It is the responsibility of individuals and their line managers to ensure<br />
attendance at training. The Training Department feedback non attendance to<br />
line managers and it is their responsibility to follow up non attenders and ensure<br />
their subsequent attendance.<br />
Authorities<br />
Document Control Information<br />
Author: Sue Dailly Lead Nurse IC Type: Policy<br />
Sponsor: Director of Infection Prevention and Control Scope: Major<br />
Reference: CP055<br />
Issue Number: 4<br />
Date April 2010 Status: Published<br />
Page 23 of 55
Winchester & Eastleigh Healthcare <strong>NHS</strong> <strong>Trust</strong><br />
<strong>MRSA</strong> POLICY<br />
• E learning for infection control is acceptable on alternate years once face to<br />
face induction is completed. E learning is accompanied by certification which<br />
can be used in evidence at appraisal.<br />
• The workbook approach is acceptable in alternate years<br />
32 MONITORING COMPLIANCE WITH AND EFFECTIVENESS OF THE POLICY<br />
• There is a regular programme of audits, led by the DIPC and co-ordinated by<br />
the Infection Control Team, which are reported to the Infection Control<br />
Committee e.g. Hand Hygiene, use of Isolation facilities, infection control <strong>policy</strong><br />
compliance, High Impact Interventions.<br />
• Divisional audits are reported via the divisions to the Infection Control<br />
committee<br />
• <strong>MRSA</strong> surveillance and trends are reported to the Infection Control Committee<br />
(ICC)<br />
• Mandatory <strong>MRSA</strong> and <strong>MRSA</strong> bacteraemia surveillance is reported to the ICC,<br />
divisions and <strong>Trust</strong> Board.<br />
• Serious Untoward Incidents (Infection) are discussed at ICC and reported to the<br />
Patient Safety Committee Protection Agency and Strategic Health Authority, as<br />
per CP008 - Incident Management & Reporting Policy Including the<br />
Management of Serious Untoward Incidents, OP006 – Risk Management &<br />
Patient Safety Policy and OP036 - Risk Register Policy<br />
• Antibiotic usage is monitored and audited by the Antibiotic Pharmacist and<br />
reported to the ICC and Drugs and Therapeutics Committee , as per PG011 -<br />
Antimicrobial Prescribing Guidelines (Adults)<br />
• Monthly reports on infection control and surveillance are taken by the DIPC to<br />
the <strong>Trust</strong> Board.<br />
• Training attendance reports are presented to the ICC<br />
• Training and education attendance is monitored by the Education Centre and<br />
reported to individual managers and collectively to the Integrated Governance<br />
Committee<br />
33 DEFINITIONS<br />
MSSA<br />
<strong>MRSA</strong><br />
Methicillin Sensitive Staphylococcus aureus is a common<br />
bacterium which is carried naturally in the nose of healthy people<br />
and may not cause any problems. Alternatively, it may be the<br />
cause of wound or skin infections.<br />
When MSSA becomes resistant to certain antibiotics it is referred<br />
to as <strong>MRSA</strong> – Methicillin Resistant Staphylococcus aureus. <strong>MRSA</strong><br />
was first reported in 1961. There are many different strains of<br />
<strong>MRSA</strong> and some spread more easily than others.<br />
Authorities<br />
Document Control Information<br />
Author: Sue Dailly Lead Nurse IC Type: Policy<br />
Sponsor: Director of Infection Prevention and Control Scope: Major<br />
Reference: CP055<br />
Issue Number: 4<br />
Date April 2010 Status: Published<br />
Page 24 of 55
Winchester & Eastleigh Healthcare <strong>NHS</strong> <strong>Trust</strong><br />
<strong>MRSA</strong> POLICY<br />
CSU<br />
Cohort<br />
Isolation<br />
Catheter urine sample. Abbreviation used to identify a sample of<br />
urine taken from a urinary catheter.<br />
a well-defined group of patients who have had a common<br />
experience or exposure i.e. have <strong>MRSA</strong> and are cared for<br />
together in a bay.<br />
nursing the patient in a single room with barrier nursing<br />
precautions (the wearing of gloves and apron/gown for hands on<br />
contact).<br />
<strong>MRSA</strong> contact - a person who has been nursed in the same room as a person<br />
with <strong>MRSA</strong> or a member of staff who has been in contact with a person with<br />
<strong>MRSA</strong>.<br />
34 REFERENCES<br />
1 Ambulance Association (2008) National guidance and procedures for<br />
infection prevention and control.<br />
2 Boyce,J.Pittet,D. (2002) Guidelines for hand hygiene in healthcare settings:<br />
recommendations of the Healthcare Infection Control Practices Advisory<br />
Committee and the Hand hygiene task force. Journal of Hospital<br />
epidemiology 23(sple) S3-41<br />
3 Cooper,B. Stone,S. et al (2003) Systematic review of isolation policies in<br />
the hospital management of methicillin resistant Staphylococcus aureus: a<br />
review of the literature with epidemiological and economic modelling.<br />
Health Technical Assess 7 1-94<br />
4 Duckworth, G. Jordan,J.(1990) Adherence and survival properties of an<br />
epidemic methicillin resistant Staphylococcus aureus compared with those<br />
of methicillin sensitive strains. Journal of Medical Microbiology 32 195-200<br />
5 Farr,B, Jarvis,J.(2002) Would active surveillance cultures help control<br />
healthcare related methicillin resistant Staphylococcus aureus. Infection<br />
Control Hospital Epidemiology 23 65-8<br />
6 French, G. et al (2004) Tackling contamination of hospital environment by<br />
methicillin resistant Staphylococcus aureus (<strong>MRSA</strong>): a comparison between<br />
conventional terminal clean and hydrogen peroxide decontamination.<br />
Journal of Hospital Infection 57 31-7<br />
Authorities<br />
Document Control Information<br />
Author: Sue Dailly Lead Nurse IC Type: Policy<br />
Sponsor: Director of Infection Prevention and Control Scope: Major<br />
Reference: CP055<br />
Issue Number: 4<br />
Date April 2010 Status: Published<br />
Page 25 of 55
Winchester & Eastleigh Healthcare <strong>NHS</strong> <strong>Trust</strong><br />
<strong>MRSA</strong> POLICY<br />
7 Joint Working Party (2006) Guidelines for the control and prevention of<br />
methicillin resistant Staphylococcus aureus in healthcare facilities. Journal<br />
of Hospital Infection 635, S1-55<br />
8 Nursing and Midwifery Council (2008) Code of Professional Conduct.<br />
9 Department of Health (2008) Screening for <strong>MRSA</strong> colonisation – a strategy<br />
for <strong>NHS</strong> <strong>Trust</strong>s: a summary of best practice.<br />
10 Department of Health (2008) <strong>MRSA</strong> screening – operational guidance.<br />
11 DH guidance on elective screening implementation 2009<br />
12 HNS <strong>Hampshire</strong> Health Economy Wide <strong>MRSA</strong> Screening Guidance<br />
2009<br />
Authorities<br />
Document Control Information<br />
Author: Sue Dailly Lead Nurse IC Type: Policy<br />
Sponsor: Director of Infection Prevention and Control Scope: Major<br />
Reference: CP055<br />
Issue Number: 4<br />
Date April 2010 Status: Published<br />
Page 26 of 55
Appendix 1<br />
1.1 Admission Screening<br />
Winchester & Eastleigh Healthcare <strong>NHS</strong> <strong>Trust</strong><br />
<strong>MRSA</strong> POLICY<br />
1.2 Following the circulation of the Department of Health Operating Framework for<br />
2008/9 all elective patients must be screened for <strong>MRSA</strong>. This includes<br />
medicine, surgery, family services and orthopaedics.<br />
• <strong>MRSA</strong> operational guidance issued in 2008 clarified the criteria for elective<br />
screening exemptions: See appendix 12 for further details<br />
• Day case ophthalmology<br />
• Day case dental<br />
• Day case endoscopy<br />
• Minor dermatology procedures<br />
• Paediatrics – except high risk<br />
• Maternity except elective caesarean sections and high risk cases<br />
If these patients have previously had <strong>MRSA</strong> they should be screened prior to<br />
admission, like any other elective <strong>MRSA</strong> positive patient.<br />
1.3 Who to screen<br />
A - Elective surgery – Pre Admission screening<br />
1.3.1 Patients awaiting elective admission should be screened before admission<br />
either in the pre-assessment clinics or Out Patient Department.<br />
34.1 Elective patients who are found to be <strong>MRSA</strong> positive following screening will be<br />
divided into 2 different patient pathways.<br />
34.2 High Risk Patients<br />
• Orthopaedics – especially prosthetic<br />
• Vascular grafts<br />
• Breast implants and complex surgery<br />
• Cardio thoracic<br />
• Diabetic patients<br />
• Any other patient the consultant feels is at high risk<br />
These patients will complete a course of decolonisation treatment provided by<br />
the <strong>Trust</strong>, or GP, and have 2 sets of negative swabs prior to admission. When<br />
admitted they will be isolated in a single room and re-commence a course of<br />
topical treatment prior to surgery. <strong>MRSA</strong> appropriate prophylactic antibiotics will<br />
also be given.<br />
Authorities<br />
Document Control Information<br />
Author: Sue Dailly Lead Nurse IC Type: Policy<br />
Sponsor: Director of Infection Prevention and Control Scope: Major<br />
Reference: CP055<br />
Issue Number: 4<br />
Date April 2010 Status: Published<br />
Page 27 of 55
Winchester & Eastleigh Healthcare <strong>NHS</strong> <strong>Trust</strong><br />
<strong>MRSA</strong> POLICY<br />
1.3.2 For High Risk procedures if after 2 courses of decolonisation treatment the<br />
patient is still <strong>MRSA</strong> positive the decision must be made between the<br />
consultant and consultant microbiologist how best to reduce the risk of <strong>MRSA</strong><br />
infection whilst going ahead with the procedure.<br />
1.3.3 A side room will need to be arranged on the trauma orthopaedic or emergency<br />
surgical wards as patients with <strong>MRSA</strong> must not be admitted to the elective<br />
orthopaedic ward or the Treatment Centre. The patient should be admitted<br />
immediately after a course of treatment, isolate in a single room, recommence<br />
topical treatment and antibiotic prophylaxis appropriate for <strong>MRSA</strong> must be<br />
given in all such cases<br />
1.3.4 All other patients<br />
All other patients will commence topical treatment 6 days prior to their day of<br />
admission. The aim is to minimise the risk of infection by carrying out surgery<br />
after a course of topical treatment. On the morning of surgery they will have<br />
mupirocin® nasal ointment applied and a chlorhexidine wash. They will be<br />
admitted into a single room and barrier nursed. <strong>MRSA</strong> appropriate prophylactic<br />
antibiotics will also be given. No post treatment screening swabs will be taken<br />
unless clinically required.<br />
1.3.5 Previously <strong>MRSA</strong> positive patients and those who are high risk of having <strong>MRSA</strong>,<br />
e.g. those living in nursing homes who are admitted as an emergency and require<br />
surgery before their <strong>MRSA</strong> status is known must commence decolonisation prior to<br />
surgery and continue post surgery. Prophylactic antibiotics must cover <strong>MRSA</strong>.<br />
1.3.6 The date of admission need not be delayed but the patient should be admitted<br />
to a single room and be placed on the end of the list. Prophylactic antibiotics<br />
which cover <strong>MRSA</strong> should be prescribed to cover the procedure – see CP014<br />
Antimicrobial Policy and current guidelines.<br />
1.3.7 Patients for the Treatment Centre who are <strong>MRSA</strong> positive during preassessment<br />
will be admitted to another ward for their surgical procedure. No<br />
cases of <strong>MRSA</strong> are to be admitted to the Treatment Centre. They will receive<br />
decolonisation treatment immediately prior to admission. On admission, the<br />
patient will be placed in a single cubicle, be last on the theatre list and receive<br />
antibiotic prophylaxis to cover <strong>MRSA</strong> – please refer to current <strong>Trust</strong> CP014<br />
Antimicrobial Policy.<br />
1.3.5 Patients who are at a continuing high risk of acquiring <strong>MRSA</strong> between the time<br />
of pre-admission screening and that of admission, (e.g. resident in a nursing<br />
home) must be re-screened on admission and should be isolated until the<br />
results of the screening swabs are known.<br />
Authorities<br />
Document Control Information<br />
Author: Sue Dailly Lead Nurse IC Type: Policy<br />
Sponsor: Director of Infection Prevention and Control Scope: Major<br />
Reference: CP055<br />
Issue Number: 4<br />
Date April 2010 Status: Published<br />
Page 28 of 55
Winchester & Eastleigh Healthcare <strong>NHS</strong> <strong>Trust</strong><br />
<strong>MRSA</strong> POLICY<br />
B - All surgical emergency patients must be screened on admission<br />
1.2.1 Swabs to be taken within 24 hours of admission. Some patients are at greater<br />
risk of having <strong>MRSA</strong> these patients include:<br />
• Frequent re-admissions to any healthcare facility<br />
• Direct inter hospital transfers<br />
• Recent in-patient in hospitals abroad or in the UK<br />
• Residents of residential care facilities – rest homes or nursing homes<br />
• Injecting drug users<br />
• Those with immuno-compromised<br />
• Members of contact sports teams<br />
• Individuals with eczema, psoriasis, dermatitis<br />
1.2.2 These patients should have nasal swabs, skin breaks/wounds or groin swabs<br />
and CSUs taken.<br />
1.2.3 Ideally these patients should be isolated until the results of their screen are<br />
known. Priority should be given to isolating patients from residential and<br />
nursing homes and patients transferred from another hospital.<br />
C – Surgical patients known to have been infected or colonised with <strong>MRSA</strong> in<br />
the past<br />
1.3.1 Patients who have had <strong>MRSA</strong> in the past should have a yellow and black<br />
sticker on the front of their notes, or inside the front cover of new sets of notes<br />
and details in their computerised CRS notes. An alert and yellow star should<br />
be present or entered on the <strong>Trust</strong> electronic patient records.<br />
1.3.2 Patients with a history of being <strong>MRSA</strong> positive within the last 12 months must<br />
commence topical treatment pre-operatively, after screening, but prior to the<br />
results being known. If they are found negative the treatment should be<br />
discontinued.<br />
1.3.3 These patients require a full screen: nose, groin, skin breaks / wounds and a<br />
CSU if a catheter is present on admission. These patients should be admitted<br />
to a side room and barrier nursed until their screening swabs are <strong>MRSA</strong><br />
negative. If a complete set of swabs/samples is negative these patients can<br />
be moved into a bay with other non-<strong>MRSA</strong> positive patients<br />
D - Medical Elective Admissions<br />
1.4.1 All elective medical patients must be screened prior to admission for <strong>MRSA</strong>. If<br />
found <strong>MRSA</strong> positive, decolonisation treatment should take place immediately<br />
prior to admission, or on admission if the admission date precludes treatment in<br />
Authorities<br />
Document Control Information<br />
Author: Sue Dailly Lead Nurse IC Type: Policy<br />
Sponsor: Director of Infection Prevention and Control Scope: Major<br />
Reference: CP055<br />
Issue Number: 4<br />
Date April 2010 Status: Published<br />
Page 29 of 55
Winchester & Eastleigh Healthcare <strong>NHS</strong> <strong>Trust</strong><br />
<strong>MRSA</strong> POLICY<br />
advance. On admission to be placed in a side room and barrier nursed and<br />
decolonisation to continue or be commenced.<br />
1.4.2 Elective medical patients who are frequent attendees e.g. chemotherapy or<br />
haematology patients must be screened once on presentation and then no<br />
more frequently than 6 monthly.<br />
E - Medical emergency admissions<br />
1.5.1 Patients admitted as a medical emergency will be screened on admission with<br />
nose and skin breaks/wound or groin swabs. If previously <strong>MRSA</strong> positive to<br />
have a full screen taken.<br />
G - ITU<br />
1.6.1 All admissions/transfers to ITU will be screened within 24 hours of admission.<br />
Take a full screen: nose, groin, skin breaks/wounds and CSU if catheter<br />
present. Patients on the elective orthopaedic ward, who are <strong>MRSA</strong> negative,<br />
can return to the elective orthopaedic ward without waiting for screening results,<br />
if they have been on the unit for less than 48 hours and not in close contact to a<br />
patient with <strong>MRSA</strong>. Weekly <strong>MRSA</strong> screening will be carried out. Swabs will be<br />
taken from the nose and wounds or groins.<br />
H – NNU<br />
1.7.1 All admissions from labour ward/theatre will have nose, groin, umbilicus and ear<br />
swabs taken. One set of swabs will suffice for both Group B Streptococcus and<br />
<strong>MRSA</strong> investigations.<br />
1.7.2 Any inter hospital transfer, including babies from the Andover Birth Centre, will<br />
have nose, groin, umbilicus and ear swabs taken.<br />
1.7.3 Any emergency admission from home will have nose, groin, umbilicus and ear<br />
swabs.<br />
1.7.4 Weekly <strong>MRSA</strong> screens will be carried out. Swabs to be taken from nose and<br />
wounds or groins.<br />
I - Elective Orthopaedic ward<br />
1.8.1 All patients for elective orthopaedic surgery involving an implant must be<br />
screened at pre-assessment clinic. Nose, skin breaks/wounds or groins and<br />
CSU are required. If the patient has had <strong>MRSA</strong> in the past they must have a<br />
full screen: nose, groins and skin breaks / wounds and CSU if catheter present.<br />
Authorities<br />
Document Control Information<br />
Author: Sue Dailly Lead Nurse IC Type: Policy<br />
Sponsor: Director of Infection Prevention and Control Scope: Major<br />
Reference: CP055<br />
Issue Number: 4<br />
Date April 2010 Status: Published<br />
Page 30 of 55
Winchester & Eastleigh Healthcare <strong>NHS</strong> <strong>Trust</strong><br />
<strong>MRSA</strong> POLICY<br />
1.8.2 No medical patients are to be admitted or transferred to the elective orthopaedic<br />
ward. Surgical and orthopaedic patients who have been screened <strong>MRSA</strong><br />
negative within the last 10 days can be transferred to the elective orthopaedic<br />
ward. They must be screened again within 24 hours of transfer. If they are<br />
positive they will be moved off the elective orthopaedic ward and their contacts<br />
screened.<br />
J - Trauma orthopaedic ward<br />
1.9.1 All patients will be screened on admission or transfer to the ward. Those who<br />
have been positive in the past must be admitted into a side room and barrier<br />
nursed until found to be <strong>MRSA</strong> negative on this admission. All <strong>MRSA</strong> positive<br />
patients must be isolated and barrier nursed. If the number exceeds single<br />
room capacity then an <strong>MRSA</strong> bay must be established and managed so as to<br />
minimise the risk of spread (see Appendix 5). Patients who are at risk of being<br />
<strong>MRSA</strong> positive should ideally be isolated until found negative.<br />
1.9.2 All emergency orthopaedic patients must be screened for <strong>MRSA</strong> on admission<br />
so they can be transferred to the elective or trauma orthopaedic ward when a<br />
bed becomes available.<br />
1.9.3 Patients with a history of being <strong>MRSA</strong> positive within the last 12 months must<br />
commence topical treatment pre-operatively, after screening, prior to the results<br />
being known. If they are found negative the treatment should be discontinued.<br />
Authorities<br />
Document Control Information<br />
Author: Sue Dailly Lead Nurse IC Type: Policy<br />
Sponsor: Director of Infection Prevention and Control Scope: Major<br />
Reference: CP055<br />
Issue Number: 4<br />
Date April 2010 Status: Published<br />
Page 31 of 55
Winchester & Eastleigh Healthcare <strong>NHS</strong> <strong>Trust</strong><br />
<strong>MRSA</strong> POLICY<br />
Appendix 2<br />
Decolonisation<br />
2.0 Nasal decolonisation<br />
2.0.1 The Infection Control Team will advise staff which topical treatment is required<br />
by each patient.<br />
2.0.2 Mupirocin 2% (Bactroban®) is a paraffin based antibiotic applied to the inner<br />
surface of each nostril 3 times a day for 5 days. The patient should be able to<br />
taste Mupirocin at the back of the throat after the application. Mupirocin should<br />
not be used for more than 5 days or used repeatedly, (no more than two<br />
courses consecutively) as resistance will be encouraged. Mupirocin is not<br />
specifically licensed for pregnant women, and its usage on pregnant women<br />
should be discussed with the Consultant Obstetrician or Microbiologist. .<br />
2.0.3 Naseptin® ointment qds for 10 days should be used for those patients whose<br />
strain of <strong>MRSA</strong> is resistant to mupirocin at a high level. (In low level mupirocin<br />
resistance it is still possible to use mupirocin. The laboratory report will indicate<br />
if the strain is mupirocin resistant.<br />
2.0.4 Polyfax ointment tds for 10 days maybe used as an alternative.<br />
2.0.5 Tea tree topical treatment may very occasionally be recommended for some<br />
patients particularly if there is mupirocin resistance or for those where<br />
decolonisation with the above has been unsuccessful, or where carriage is<br />
persistent.<br />
2.1 Unbroken SKIN decolonisation<br />
2.1.1 4% Chlorhexidine gluconate aqueous solution (Hibiscrub®) body wash/<br />
shampoo (or Octennisan® if skin is fragile or for those aged under 8 years of<br />
age) are useful in eradicating or suppressing skin colonisation. In particular use<br />
pre-operatively to reduce the risk of surgical site infections.<br />
2.1.2 Patients should bathe/wash daily for 5 days. The skin should be moistened<br />
and antiseptic detergent applied thoroughly to all areas before rinsing, in a<br />
shower or bath. Special attention should be given to skin creases, axilla, groin<br />
and perineal areas.<br />
2.1.3 If possible hair should be washed with antiseptic detergent (Hibiscrub®) or<br />
Octennisan® twice during the 5 day regime.<br />
Authorities<br />
Document Control Information<br />
Author: Sue Dailly Lead Nurse IC Type: Policy<br />
Sponsor: Director of Infection Prevention and Control Scope: Major<br />
Reference: CP055<br />
Issue Number: 4<br />
Date April 2010 Status: Published<br />
Page 32 of 55
Winchester & Eastleigh Healthcare <strong>NHS</strong> <strong>Trust</strong><br />
<strong>MRSA</strong> POLICY<br />
2.1.4 After each bath/shower/wash, clean clothing/nightwear, bedding and towels<br />
should be provided.<br />
2.1.5 For patients with eczema, dermatitis or other skin conditions:<br />
2.2 Throat<br />
First attempt to treat underlying condition.<br />
Secondly try Dermol 500® for skin and hair wash.<br />
2.2.1 Corsodyl® mouth wash/gargle will be prescribed for any patient on topical<br />
treatment for <strong>MRSA</strong>. This is not suitable for paediatrics or neonates.<br />
2.2.2 Systemic treatment of throat carriage should only be considered in exceptional<br />
circumstances e.g. where there is evidence that there is transmission from a<br />
throat carrier in a continuing outbreak or when the patient carrying <strong>MRSA</strong> in the<br />
throat has experienced episodes of invasive infection.<br />
2.2.3 Systemic treatment should only be prescribed on the advice of the<br />
microbiologist and with appropriate monitoring. If treatment is required it should<br />
be restricted to one course of treatment. Possible side effects must be<br />
explained to the patient. Systemic treatment should be given in conjunction<br />
with nasal mupirocin and skin decolonisation.<br />
2.2.4 Throat carriage may be associated with the presence of foreign bodies<br />
e.g. nasal gastric tube or dentures. An ENT opinion may be useful if<br />
structural/physiological abnormalities are suspected.<br />
2.2.5 Gargling is rarely effective at eradicating <strong>MRSA</strong> colonisation unless the<br />
person is able to gargle for 2 minutes 3 times a day.<br />
2.3 <strong>MRSA</strong> in urine<br />
2.3.1 A patient clinically diagnosed as having a urinary tract infection should receive<br />
antibiotics to which it is susceptible. If in doubt contact the consultant<br />
microbiologist. If the urine is only colonised, systemic treatment may not be<br />
indicated.<br />
2.4 <strong>MRSA</strong> in Catheter urine<br />
2.4.1 Catheter urines routinely colonize with organisms. However, if the patient has<br />
an infection then systemic treatment maybe required. The catheter must be<br />
changed whilst the patient is on the course of antibiotics.<br />
Authorities<br />
Document Control Information<br />
Author: Sue Dailly Lead Nurse IC Type: Policy<br />
Sponsor: Director of Infection Prevention and Control Scope: Major<br />
Reference: CP055<br />
Issue Number: 4<br />
Date April 2010 Status: Published<br />
Page 33 of 55
Winchester & Eastleigh Healthcare <strong>NHS</strong> <strong>Trust</strong><br />
<strong>MRSA</strong> POLICY<br />
2.4.2 If the catheter urine is colonized, no systemic treatment is recommended.<br />
Antibiotic cover is required for a change of catheter. Please see CP014<br />
Antibiotic Policy for information or, in complex cases, contact Consultant<br />
Microbiologists for advice.<br />
2.5 Colonised Skin lesions/ wounds<br />
2.5.1 Small clean wounds can be treated using Bactroban® tds for 5 days.<br />
This is useful for small wounds (
Winchester & Eastleigh Healthcare <strong>NHS</strong> <strong>Trust</strong><br />
<strong>MRSA</strong> POLICY<br />
Appendix 3<br />
Isolation procedures – single rooms<br />
3.1 Single rooms with en-suite facilities are the preferred standard of<br />
accommodation. However a designated toilet and bathroom should be allocated.<br />
3.2 A yellow barrier nursing sign detailing isolation precautions must be displayed<br />
prominently on the side room door or at the entrance to the bay or isolation ward.<br />
These are available from the Infection Control Nurses.<br />
3.3 The room door should be kept closed to minimize spread to adjacent areas. If<br />
this compromises patient treatment the door must be kept shut during procedures<br />
that may generate staphylococcal aerosols such as chest physiotherapy and bed<br />
making.<br />
3.4 High standards of hand decontamination are required to minimise the risk of<br />
cross infection. Hands must be thoroughly decontaminated with chlorhexidine<br />
(Hibiscrub®) and water before and after patient contact, and alcohol gel used on<br />
leaving an isolation facility/side room.<br />
3.5 Yellow disposable aprons and gloves must be worn by all staff handling the<br />
patient or having contact with their immediate environment. Staff may need to<br />
wear surgical masks, along with eye protection, during sputum inducing<br />
procedures like suctioning and chest physiotherapy.<br />
3.6 Staff from other wards and departments e.g. physiotherapy, phlebotomy, other<br />
medical teams, social worker should only enter after permission and instruction<br />
from the nurse in charge. This also applies to visitors who assist with the<br />
patient’s bodily care. All visitors should put on a yellow apron and gloves before<br />
entering the room, wash their hands before leaving the room, and use alcohol gel<br />
after exiting.<br />
Outside the isolation room<br />
Non-sterile gloves<br />
Yellow Aprons<br />
Alcohol gel<br />
Linen bag (when required)<br />
Patients observation and drug charts<br />
Inside the isolation room<br />
Orange waste bag<br />
Chlorhexidine (Hibiscrub®)<br />
Alginate bag for linen(when required)<br />
Minimal equipment necessary<br />
Authorities<br />
Document Control Information<br />
Author: Sue Dailly Lead Nurse IC Type: Policy<br />
Sponsor: Director of Infection Prevention and Control Scope: Major<br />
Reference: CP055<br />
Issue Number: 4<br />
Date April 2010 Status: Published<br />
Page 35 of 55
Winchester & Eastleigh Healthcare <strong>NHS</strong> <strong>Trust</strong><br />
<strong>MRSA</strong> POLICY<br />
Appendix 4<br />
Kingfisher ward isolation and decolonisation regime.<br />
4.1 Background<br />
4.2 Rehabilitation wards are considered low risk in the 2006 national guidance.<br />
4.3 Screening on transfer<br />
4.4 On transfer (including RHCH) or admission from the community, please screen<br />
nose, skin breaks/wounds or groins and catheter urine if catheter in situ.<br />
Previously positive patients admitted from the community must have a full screen<br />
on admission. Those already on <strong>MRSA</strong> treatment regimes should be screened<br />
according to their treatment care plan.<br />
4.5 Isolation<br />
4.6 Ideally isolate all patients with <strong>MRSA</strong> but if side rooms are limited, priority should<br />
be given to those who are skin shedders or throat/sputum positive and have a<br />
productive cough. All other patients can be nursed in a bay.<br />
4.7 All <strong>MRSA</strong> positive patients will be treated, in-line with our present regime, if and<br />
when they are identified.<br />
4.8 Protection<br />
4.9 Good quality hand hygiene is essential, as per CP073 - Hand hygiene <strong>policy</strong><br />
4.10 All staff and patients must have their wounds covered. An ‘<strong>MRSA</strong> free’ bay may<br />
need to be allocated if Kingfisher ward begin receiving patients with sutures or<br />
clips still in situ post operation. Surgical wounds must remain covered until<br />
completely healed.<br />
4.11 Gloves and aprons must be changed between patients and worn for intimate<br />
care. Yellow aprons will be used when caring for patients with <strong>MRSA</strong> or who are<br />
being barrier nursed for another reason.<br />
4.12 Ward must have high quality cleaning by housekeeping staff and nursing staff.<br />
Must be carefully monitored by ward sisters and infection control link nurse and<br />
immediate remedial action taken if the quality or frequency of cleaning<br />
deteriorates.<br />
4.13 Curtains should be changed on a planned programme every 3 months.<br />
4.14 Screening of patients for <strong>MRSA</strong> should take place at RHCH if a patient is<br />
readmitted.<br />
Authorities<br />
Document Control Information<br />
Author: Sue Dailly Lead Nurse IC Type: Policy<br />
Sponsor: Director of Infection Prevention and Control Scope: Major<br />
Reference: CP055<br />
Issue Number: 4<br />
Date April 2010 Status: Published<br />
Page 36 of 55
Winchester & Eastleigh Healthcare <strong>NHS</strong> <strong>Trust</strong><br />
<strong>MRSA</strong> POLICY<br />
Appendix 5<br />
How to cohort nurse patients with <strong>MRSA</strong><br />
5.1 Patients suitable to be nursed in an <strong>MRSA</strong> bay<br />
<strong>MRSA</strong> nose only<br />
<strong>MRSA</strong> nose and wound only (providing wound is covered)<br />
<strong>MRSA</strong> in CSU only<br />
<strong>MRSA</strong> in CSU and nose only<br />
Patients with <strong>MRSA</strong> in other sites who are on treatment<br />
5.2 Patients not suitable to be nursed in an <strong>MRSA</strong> bay<br />
<strong>MRSA</strong> in throat and coughing<br />
<strong>MRSA</strong> in sputum and coughing<br />
<strong>MRSA</strong> positive wound which cannot be occluded<br />
<strong>MRSA</strong> nose, and groin and not on any treatment, or is a treatment failure.<br />
Surgical patients who are wound negative or have a prosthetic implant/internal<br />
fixation<br />
<strong>MRSA</strong> positive patients with an exfoliating skin condition e.g. eczema<br />
Patients with a resistant strain of <strong>MRSA</strong> e.g. mupirocin resistance<br />
5.3 Patients with <strong>MRSA</strong> in a bay of patients who are <strong>MRSA</strong> negative<br />
5.3.1 Patients who are found to be <strong>MRSA</strong> positive on this admission will only be<br />
nursed in a bay with patients who are <strong>MRSA</strong> negative under exceptional<br />
circumstances i.e. if they would be clinically, mentally or physically at risk if<br />
nursed in a single room, or if nursed on a different speciality ward. The<br />
patient’s doctor and senior ward nurse will make the decision whether the<br />
patient is safe to be nursed in a single room or on another speciality ward. If<br />
the patient remains in the bay the Infection Control Team must be informed if<br />
this situation occurs so that specific infection control measures can be carried<br />
out. The patient must be reviewed at least daily, and when able to, moved into<br />
a single room. The Infection Control team will assist in co-ordinating the<br />
contact screening.<br />
5.3.2 Only under exceptional circumstances should the above advice be over ruled.<br />
When the number of single rooms becomes inadequate, the Infection Control<br />
team should be contacted to review current side room allocation, and when and<br />
where an <strong>MRSA</strong> bay could be made. Outside of hours the site co-ordinator, in<br />
consultation with consultant microbiologist if advice is necessary, will allocate<br />
patients to an <strong>MRSA</strong> bay.<br />
Authorities<br />
Document Control Information<br />
Author: Sue Dailly Lead Nurse IC Type: Policy<br />
Sponsor: Director of Infection Prevention and Control Scope: Major<br />
Reference: CP055<br />
Issue Number: 4<br />
Date April 2010 Status: Published<br />
Page 37 of 55
Winchester & Eastleigh Healthcare <strong>NHS</strong> <strong>Trust</strong><br />
<strong>MRSA</strong> POLICY<br />
5.4 Elderly care / rehabilitation wards<br />
5.4.1 Patients, who are <strong>MRSA</strong> positive only in wounds which can be occluded, can<br />
be nursed in a bay with patients who are <strong>MRSA</strong> negative.<br />
5.5 General surgical wards<br />
5.5.1 Patients with <strong>MRSA</strong> at any site will be nursed in a side room or in a bay with<br />
other <strong>MRSA</strong> positive patients. The only exception is if it is clinically necessary<br />
for the patient to be nursed in an observation bay and not in a side room. The<br />
patient’s doctor and senior ward nurse will make the decision. The Infection<br />
Control team must be informed if the situation occurs so that specific infection<br />
control measures can be carried out and contact screening can be organised.<br />
5.6 Orthopaedic wards<br />
5.6.1 Patients with <strong>MRSA</strong> will be moved off the elective orthopaedic ward. Elective<br />
orthopaedic patients with <strong>MRSA</strong> will be accommodated in side rooms on the<br />
trauma orthopaedic ward.<br />
Authorities<br />
Document Control Information<br />
Author: Sue Dailly Lead Nurse IC Type: Policy<br />
Sponsor: Director of Infection Prevention and Control Scope: Major<br />
Reference: CP055<br />
Issue Number: 4<br />
Date April 2010 Status: Published<br />
Page 38 of 55
Winchester & Eastleigh Healthcare <strong>NHS</strong> <strong>Trust</strong><br />
<strong>MRSA</strong> POLICY<br />
Appendix 6 Patient visits to other departments<br />
6.1.1 Visits by <strong>MRSA</strong> positive patients to other departments should be kept to a<br />
minimum. If it is necessary either for investigation or treatment, prior<br />
arrangements should be made with the staff of the receiving department, so<br />
that infection control measures can be implemented.<br />
These include:<br />
1 See these Patients at the end of the working session if possible.<br />
2 The patient should spend the minimum time in the dept, and should not<br />
be left in communal waiting areas with other patients.<br />
3 Staff coming into close or physical contact with the patient should wear<br />
disposable aprons and gloves.<br />
4 Equipment and the number of staff attending should be kept to a<br />
minimum.<br />
5 Surfaces with which the patient has had direct contact should be<br />
decontaminated with 1000ppm hypochlorite – Actichlor Plus®. .<br />
6 Linen should be treated as infected.<br />
7 Staff should decontaminate their hands after contact with the patient.<br />
8 For theatres please refer to LTP08 Methicillin Resistant patients in<br />
Theatre Policy.<br />
6.2 Intra hospital patient transfer<br />
6.2.1 Movement of patients with <strong>MRSA</strong> within a hospital should be kept to a minimum<br />
to reduce the risk of cross-infection, but this should not compromise other<br />
aspects of care, such as rehabilitation. The receiving ward should be notified of<br />
the patient’s <strong>MRSA</strong> status in advance of the transfer to minimise their contact<br />
with other patients. Transport of the infected/colonised patient should be<br />
undertaken carefully. Transfer letter to be completed.<br />
7 Infection control precautions<br />
1 Lesions of staff should be occluded with an impermeable dressing.<br />
2 Porters who have physical contact with the patient should wear<br />
disposable yellow plastic aprons to protect their clothing whilst in contact<br />
with the patient.<br />
3 Aprons should be removed when contact with the patient has finished<br />
and disposed of as clinical waste. Apron and gloves do not need to be<br />
worn whilst wheeling the patient down the corridor.<br />
4 Gloves need only be worn if staff transporting the patient has skin<br />
abrasions, or hands in contact with the patient.<br />
5 The trolley or chair should be decontaminated after use.<br />
6 All linen disposed of as infected.<br />
7 Staff should decontaminate their hands thoroughly after dealing with<br />
the patient and cleaning the trolley or chair.<br />
Authorities<br />
Document Control Information<br />
Author: Sue Dailly Lead Nurse IC Type: Policy<br />
Sponsor: Director of Infection Prevention and Control Scope: Major<br />
Reference: CP055<br />
Issue Number: 4<br />
Date April 2010 Status: Published<br />
Page 39 of 55
Winchester & Eastleigh Healthcare <strong>NHS</strong> <strong>Trust</strong><br />
<strong>MRSA</strong> POLICY<br />
Appendix 7 Patients going to theatre<br />
7.1.1 Prior to any planned invasive procedure, efforts should be made to minimize<br />
the risk of infection through topical and sometimes systemic decolonization,<br />
and prophylactic antimicrobial therapy.<br />
7.1.2 For high risk patients – decolonisation will take place at least 2 weeks prior to<br />
admission allowing time for patients to have two sets of negative swabs prior to<br />
admission. For all other patients, topical decolonisation should commence preoperatively<br />
and continue for a total of five days, with surgery taking place on<br />
day 6 for maximum effect. For patients who remain positive, decolonisation will<br />
commence pre-op and continue post op.<br />
7.2 As part of pre-op preparation<br />
1 Bath/shower the patient with an antiseptic detergent e.g. Hibiscrub®, applied<br />
direct to skin as soap and rinsed off.<br />
2 Cover affected lesions with an impermeable dressing.<br />
3 Change all the bed linen and place patient in a clean gown.<br />
4 Apply Mupirocin to the nose before the operation if the organism is sensitive<br />
- preferably commencing 24 hours pre-op.<br />
5 Consider appropriate prophylactic antibiotic cover for surgical procedures in<br />
colonised or infected patients (see CP014 Antibiotic Policy on the<br />
intranet). Complex cases can be discussed with consultant microbiologists.<br />
6 Consideration should be given to placing patients at the end of the operating<br />
session but with effective ventilation systems there should be an adequate<br />
number of air exchanges to provide a safe environment within 15 minutes of<br />
removal of the <strong>MRSA</strong> patient from the operating theatre. Time is still<br />
needed for thorough cleaning and drying (see below) so procedures at the<br />
end of the list may still be most practical.<br />
7.3 Within the theatre<br />
1 After the procedure all the theatre surfaces in close contact or near the<br />
patient, such as the operating table or instrument trolley should be<br />
decontaminated with 1,000ppm hypochlorite – Actichlor Plus®.<br />
2 Low risk patients can go to the main recovery room, high risk patients e.g.<br />
those who are skin shedders should be recovered in the theatre.<br />
3 Patients may be allowed recovery after surgery in the operating theatre or<br />
an area not occupied by other patients to avoid possible contamination of<br />
the usual recovery area. The patients should be segregated as far as<br />
possible within the recovery area, and nursed by staff dedicated to their<br />
care, employing standard precautions of gloves, aprons and thorough hand<br />
hygiene.<br />
Please see the LTP09 Methicillin Resistant Patients Theatre Policy for further<br />
information<br />
Authorities<br />
Document Control Information<br />
Author: Sue Dailly Lead Nurse IC Type: Policy<br />
Sponsor: Director of Infection Prevention and Control Scope: Major<br />
Reference: CP055<br />
Issue Number: 4<br />
Date April 2010 Status: Published<br />
Page 40 of 55
Winchester & Eastleigh Healthcare <strong>NHS</strong> <strong>Trust</strong><br />
<strong>MRSA</strong> POLICY<br />
Appendix 8<br />
8.1 Transfer of patients to another hospital<br />
8.1.1 Refusal to accept transfer of a patient is not justifiable on the basis of the risk<br />
posed to other patients by an individual’s carriage of, or infection with, <strong>MRSA</strong>.<br />
All units should have procedures in place and adequate facilities for<br />
containment of <strong>MRSA</strong>.<br />
8.1.2 Identification of infected or colonised patients is the responsibility of the<br />
transferring hospital. Before transfer a member of the clinical team for the<br />
patient, at the transferring hospital, must inform the ward staff at the receiving<br />
hospital of the patient’s status.<br />
8.2 Ambulances/hospital vehicles<br />
8.2.1 The risk of cross infection from an <strong>MRSA</strong> colonised or infected patient to other<br />
patients in an ambulance is minimal. Good infection control practices and<br />
routine cleaning should suffice to prevent cross-infection. Ambulance staff<br />
should be informed in advance if a patient has <strong>MRSA</strong>.<br />
8.2.2 Most <strong>MRSA</strong> carriers maybe transported with other patients in the same<br />
ambulance without any special precautions. High risk categories of patients<br />
e.g. immuno-compromised should not be transported in the same ambulance<br />
as a known <strong>MRSA</strong> positive patient or those with an infection e.g. chest<br />
infection.<br />
8.3 Infection control precautions<br />
1 Skin lesions should be covered (patients and ambulance crew).<br />
2 Ambulance staff should use an antibacterial hand gel after contact with<br />
all patients.<br />
3 Linen must be changed.<br />
4 Surfaces wiped with detergent and water.<br />
5 The patient does not need to wear a mask when travelling in the<br />
ambulance.<br />
.<br />
Reference: ‘National guidance and procedures for infection prevention and control’ by<br />
the Ambulance Association (2008).<br />
Authorities<br />
Document Control Information<br />
Author: Sue Dailly Lead Nurse IC Type: Policy<br />
Sponsor: Director of Infection Prevention and Control Scope: Major<br />
Reference: CP055<br />
Issue Number: 4<br />
Date April 2010 Status: Published<br />
Page 41 of 55
Winchester & Eastleigh Healthcare <strong>NHS</strong> <strong>Trust</strong><br />
<strong>MRSA</strong> POLICY<br />
Appendix 9 Cleaning, waste and linen<br />
Cleaning<br />
9.1 Management of the environment and equipment should be considered as<br />
critical to decrease the spread of <strong>MRSA</strong>. General principles should be<br />
adopted to minimize the bacterial burden. The ability of <strong>MRSA</strong> to survive in<br />
dust demonstrates the need for dust minimization, the removal of bacteria<br />
from surfaces, and the appropriate disposal of contaminated waste and<br />
linen.<br />
9.2 An enhanced level of cleaning requires additional time to enable the daily<br />
removal of organic material, undertaken wearing gloves and apron. Yellow colour<br />
coded bucket and cleaning equipment must be used. Mop head must be changed<br />
and sent for laundering after use in each isolation area.<br />
9.3 There must also be adequate removal of all of the dust particularly from areas<br />
like ventilator ducts, radiators and equipment like fans.<br />
9.4 There should be planned, quarterly, thorough cleaning of the whole ward<br />
including bedding and the laundering or steam cleaning of curtains.<br />
9.5 The quality of the cleaning of isolation rooms and equipment will be audited<br />
regularly by housekeeping, Matrons, Execs and the Infection Control Team.<br />
9.6 Cleaning regime after discharge/transfer of patient<br />
9.6.1 <strong>MRSA</strong> contaminated patient areas should be cleaned thoroughly after<br />
each patient’s discharge with 1,000ppm hypochlorite – Actichlor Plus®.<br />
This includes locker, table, bed frame, chair, floor and all patient contact<br />
surfaces. Sinks, toilets, baths and showers are to be cleaned as usual<br />
and again after the patient has been discharged.<br />
9.6.2 Curtains should be removed and laundered or steam cleaned if not<br />
single use disposable curtains.<br />
9.6.3 Pillows and mattresses should be checked for damage and cleaned.<br />
9.6.4 All disposable items should be disposed of as clinical waste. If in doubt<br />
ask a member of ward based nursing staff first.<br />
9.6.5 If possible room should be decontaminated using the Bioquell method..<br />
Authorities<br />
Document Control Information<br />
Author: Sue Dailly Lead Nurse IC Type: Policy<br />
Sponsor: Director of Infection Prevention and Control Scope: Major<br />
Reference: CP055<br />
Issue Number: 4<br />
Date April 2010 Status: Published<br />
Page 42 of 55
Winchester & Eastleigh Healthcare <strong>NHS</strong> <strong>Trust</strong><br />
<strong>MRSA</strong> POLICY<br />
9.7 Waste<br />
9.7.1 All disposable items, e.g. aprons and gloves must be disposed of as<br />
clinical waste in an orange plastic bag in the room. Needles, syringes<br />
and other sharps must be placed in a sharps container.<br />
9.8 Linen<br />
9.8.1 All linen from patients infected or colonised with <strong>MRSA</strong> should be<br />
considered to be contaminated. All linen must be placed inside an<br />
alginate bag and tied whilst in the patient’s room then placed inside a red<br />
plastic bag outside the room. Curtains should be removed and<br />
laundered or steam cleaned after the patient is discharged or transferred.<br />
The room maybe decontaminated using Bioquell after the patient has left<br />
the room.<br />
9.9 Patients clothing<br />
9.9.1 Patients’ clothing should normally be laundered by their relatives. Soiled<br />
personal clothing should be placed in a plastic bag. Advise relatives to<br />
wash the clothing separately at home. Ward staff on wards where<br />
patients’ clothes that are laundered on site (Clifton and RDU) should<br />
place the items of clothing in an alginate bag, and a clear plastic bag.<br />
This clothing will be hot washed and there is a risk delicate fabrics will be<br />
damaged.<br />
Authorities<br />
Document Control Information<br />
Author: Sue Dailly Lead Nurse IC Type: Policy<br />
Sponsor: Director of Infection Prevention and Control Scope: Major<br />
Reference: CP055<br />
Issue Number: 4<br />
Date April 2010 Status: Published<br />
Page 43 of 55
Winchester & Eastleigh Healthcare <strong>NHS</strong> <strong>Trust</strong><br />
<strong>MRSA</strong> POLICY<br />
Appendix 10<br />
10 Control of vancomycin intermediate and resistant Staphylococcus aureus<br />
(VISA and VRSA)<br />
10.2.1 Antibiotic resistance flourishes when antimicrobial drugs are overused,<br />
misused and dispensed at levels lower than treatment guidelines dictate.<br />
Virtually all strains of S.aureus with reduced sensitivity to glycopeptide<br />
antibiotics, so far, are thought to have arisen from pre- existing<br />
reservoirs of <strong>MRSA</strong>, usually in patients with chronic and underlying<br />
disease who have received multiple and/or prolonged courses of<br />
glycopeptide treatment.<br />
10.3 Action to be taken on identification of a VISA or a GISA<br />
(glycopeptide-intermediate S.aureus).<br />
10.3.1 Laboratory staff to immediately inform Consultant Microbiologist and<br />
infection control team who will contact the clinician and ward staff.<br />
Infection Control Team will ascertain patient’s movements and identify all<br />
contacts.<br />
Health Protection Agency will be notified by the Consultant Microbiologist or<br />
appropriate delegate.<br />
10.4 If patient is still an inpatient<br />
a. Isolate patient in single room with en suite toilet facilities and a hand wash<br />
sink.<br />
b. Strict barrier nursing must be carried out with the door closed.<br />
c. The number of healthcare staff having contact with the patient should be<br />
reduced.<br />
d. Healthcare staff with chronic skin conditions should not be involved in direct<br />
care of the patient.<br />
e. Ward will be closed to admissions whilst screening of all patients on the<br />
ward takes place. Patients may be discharged home but cannot be<br />
transferred to another ward, hospital or institution until their screening<br />
results is known.<br />
f. No fans to be placed in the patient’s room.<br />
10.5 Infection Control procedures<br />
10.5.1 Uniforms should not be taken home to launder, staff to wear theatre<br />
scrub suits under their gowns/aprons and to change on site before going<br />
home. Disposable masks and eye protection should be worn for<br />
procedures likely to generate aerosol/splashing. (As per CP079 <strong>Trust</strong><br />
Authorities<br />
Document Control Information<br />
Author: Sue Dailly Lead Nurse IC Type: Policy<br />
Sponsor: Director of Infection Prevention and Control Scope: Major<br />
Reference: CP055<br />
Issue Number: 4<br />
Date April 2010 Status: Published<br />
Page 44 of 55
Winchester & Eastleigh Healthcare <strong>NHS</strong> <strong>Trust</strong><br />
<strong>MRSA</strong> POLICY<br />
<strong>policy</strong> for uniform and clothing worn whilst delivering direct<br />
clinical care and CP080 Theatre Uniforms)<br />
10.5.2 Hand hygiene with an antibacterial preparation must be used before and<br />
after any patient contact. Visibly soiled hands should be washed with<br />
chlorhexidine first prior to alcohol gel, as per CP073 - Hand hygiene<br />
<strong>policy</strong>.<br />
10.5.3 Non-disposable items which cannot easily be cleaned should be<br />
dedicated for use only by infected/colonised patient as per CP030 -<br />
Overarching Decontamination Policy.<br />
10.5.4 Linen should be treated as infected, as per CP030 Overarching<br />
Decontamination Policy.<br />
10.5.5 All waste discarded into clinical waste bins, as per OP052 - Waste<br />
Disposal Policy.<br />
10.5.6 Transfers between institutions should be avoided unless essential and<br />
the receiving institute made aware of the patients colonization/infection<br />
status prior to transfer, as per CP061 Policy for the Intraward<br />
Transfer of Patients with Infection Control Issues.<br />
10.5.7 After discharge, the room must be thoroughly cleaned with<br />
1,000ppm hypochlorite Actichlor Plus® paying special attention to<br />
horizontal surfaces. Curtains must be changed, as per CP030<br />
Overarching Decontamination Policy.<br />
10.6 Screening of patient and ALL contacts since admission<br />
10.6.1 Patients<br />
10.6.2 Nose, groins, skin breaks/wounds and manipulated sites (eg IV cannula<br />
sites) of the index case and all other patients on the ward/unit should be<br />
screened for carriage of VISA/GISA or VRSA. Screening may need to<br />
be extended to other areas the index case has had contact with.<br />
10.7 ALL Staff caring for VISA patient<br />
10.7.1 Nose, and groins of healthcare workers and others with close physical<br />
contact with the case should be screened. Staff who maintain contact<br />
with the patient will require weekly screening until patient is discharged.<br />
Authorities<br />
Document Control Information<br />
Author: Sue Dailly Lead Nurse IC Type: Policy<br />
Sponsor: Director of Infection Prevention and Control Scope: Major<br />
Reference: CP055<br />
Issue Number: 4<br />
Date April 2010 Status: Published<br />
Page 45 of 55
Winchester & Eastleigh Healthcare <strong>NHS</strong> <strong>Trust</strong><br />
<strong>MRSA</strong> POLICY<br />
10.7.2 Feedback of results, maintenance of confidence and support are<br />
required. Treatment will be prescribed. Colonized staff should be<br />
excluded from work until eradication has been achieved.<br />
Appendix 11<br />
11 <strong>MRSA</strong> staff screening regime<br />
11.2 Which sites to swab from staff<br />
11.3 Nose and areas of abnormal or broken skin.<br />
11.4 All positive results will be phoned to the member of staff by the<br />
Occupational Health & Safety Dept in the working week. Topical treatment will<br />
be provided by the <strong>Trust</strong>. Follow up screening will be co-ordinated by the<br />
Occupational Health & Safety Dept. Out of hours treatment packs are held in<br />
A&E and occasionally staff will be contacted by their duty manager out of hours<br />
if positive results are identified over a weekend or bank holiday.<br />
11.5 A minimum of 2 screens at weekly intervals (while not receiving<br />
antimicrobial therapy) should be performed before a previously positive staff<br />
member can be considered to be clear of <strong>MRSA</strong>. Consider the individual’s risk<br />
of transmission to patients when agreeing their continuation or return to work. It<br />
is recommended only staff with colonised or infected hand lesions should be off<br />
work whilst receiving courses of clearance therapy.<br />
11.6 Staff colonised or infected with Vancomycin Intermediate<br />
Staphylococcus aureus (VISA) or Vancomycin Resistant Staphylococcus<br />
aureus (VRSA) must be excluded from work until they have had 3 negative<br />
samples.<br />
11.7 Staff with persistent carriage at a site other than the nose should be<br />
considered for appropriate specialist opinion – e.g. dermatologist, ENT surgeon.<br />
Authorities<br />
Document Control Information<br />
Author: Sue Dailly Lead Nurse IC Type: Policy<br />
Sponsor: Director of Infection Prevention and Control Scope: Major<br />
Reference: CP055<br />
Issue Number: 4<br />
Date April 2010 Status: Published<br />
Page 46 of 55
Winchester & Eastleigh Healthcare <strong>NHS</strong> <strong>Trust</strong><br />
<strong>MRSA</strong> POLICY<br />
Employee Safety & Occupational Health Department<br />
INSTRUCTIONS FOR STAFF WHO HAVE A POSITIVE <strong>MRSA</strong> RESULT<br />
NAME<br />
WARD<br />
Your recent initial nasal swab has been reported to be positive to <strong>MRSA</strong><br />
therefore as a healthcare worker you must comply with the treatment and follow<br />
up screening detailed below.<br />
Because of possible restrictions on working, you MUST inform the senior nurse/line<br />
manager on duty so that staffing levels can be adjusted if necessary.<br />
STANDARD TREATMENT – PACK A<br />
STAGE 1<br />
Date Treatment<br />
to Commence:<br />
………………..<br />
STAGE 2<br />
PRIOR TO COMMENCING TREATMENT<br />
1. Swab nose, groins and any skin breaks/ wounds.<br />
(One swab should be used for both nostrils, another for<br />
both groins and another for both groins).<br />
3. Now commence treatment below.<br />
TREATMENT<br />
All 3 Treatment products to be used as detailed<br />
below. Please notify OH or Infection Control if you<br />
have any hypersensitivity to the products below<br />
Day 1<br />
day<br />
Day 2<br />
day<br />
Day 3<br />
day<br />
Day 4<br />
day<br />
Day 5<br />
day<br />
<br />
<br />
<br />
<br />
<br />
1. Apply Bactroban® nasal cream - 3 times a day for 5<br />
Days<br />
2. Gargle with Corsodyl® for 2 minutes (minimum) - 3<br />
times a day for 5 days – Leave an interval of 30<br />
minutes between using the mouth wash and toothpaste<br />
if possible.<br />
3. Wash with Hibiscrub® – 2 times a day for 5 days<br />
paying particular attention to axillae, groin and skin<br />
creases. Not for use on the face.<br />
N.B In the event of a resistant strain being reported<br />
you will be contacted again and treatment may vary<br />
Authorities<br />
Document Control Information<br />
Author: Sue Dailly Lead Nurse IC Type: Policy<br />
Sponsor: Director of Infection Prevention and Control Scope: Major<br />
Reference: CP055<br />
Issue Number: 4<br />
Date April 2010 Status: Published<br />
Page 47 of 55
Winchester & Eastleigh Healthcare <strong>NHS</strong> <strong>Trust</strong><br />
<strong>MRSA</strong> POLICY<br />
STAGE 3<br />
Day 8 <br />
day<br />
Date:<br />
Day 13 <br />
day<br />
Date:<br />
Please Note:<br />
AFTER TREATMENT<br />
Re-swab all sites as above after 2 clear days following<br />
treatment<br />
(before attending shift / work that day).<br />
Re-swab all sites as above after a further 5 days (before<br />
attending shift / work that day) unless you are informed<br />
that the swab results on ‘Day 8’ remain positive in which<br />
case you will be advised on further treatment.<br />
1. It is important that you continue the treatment for the full 5 days.<br />
2. If any of the re-swab results are <strong>MRSA</strong> positive the Occupational Health<br />
Adviser will contact you again and a further 5 day treatment schedule is likely to<br />
be recommended.<br />
3. After the second treatment you will be informed of the results. If any of the reswab<br />
results remain <strong>MRSA</strong> positive the Consultant Microbiologist will be<br />
contacted by the Occupational Health Adviser who will in turn contact you<br />
regarding any treatment and work.<br />
IF YOU HAVE ANY FURTHER WORRIES OR CONCERNS PLEASE CONTACT<br />
INFECTION CONTROL 5170 OR THE OCCUPATIONAL HEALTH DEPARTMENT<br />
4326<br />
WORKING ARRANGEMENTS - High Risk Areas (ICU, HDU, elective orthopaedics<br />
or NNU)<br />
Treatment Day 1 Day 2 Day 3 Day 4<br />
Day 5<br />
Do not work on Day 1 and Day 2<br />
unless you can work with no<br />
patient contact i.e. if you can carry<br />
out an administrative role.<br />
Return to work from day 3 without<br />
restriction on work activities<br />
WORKING ARRANGEMENTS - Theatre Staff<br />
Authorities<br />
Document Control Information<br />
Author: Sue Dailly Lead Nurse IC Type: Policy<br />
Sponsor: Director of Infection Prevention and Control Scope: Major<br />
Reference: CP055<br />
Issue Number: 4<br />
Date April 2010 Status: Published<br />
Page 48 of 55
Winchester & Eastleigh Healthcare <strong>NHS</strong> <strong>Trust</strong><br />
<strong>MRSA</strong> POLICY<br />
Treatment Day 1 Day 2 Day 3 Day 4<br />
Day 5<br />
Continue working from Day 1.<br />
You must not undertake or assist<br />
in invasive procedures i.e. work as<br />
a surgeon, ‘scrub nurse’, insert<br />
central lines or cannulate for the<br />
first 2 days but may work in other<br />
areas<br />
Anaethetist?<br />
May resume normal work activities<br />
from day 3<br />
WORKING ARRANGEMENTS - Lower risk areas (All other Clinical areas not<br />
indicated above)<br />
Treatment Day 1 Day 2 Day 3 Day 4<br />
Day 5<br />
Continue working from Day 1.<br />
You must not carry out aseptic<br />
techniques or invasive procedures<br />
for day 1 and 2.<br />
May resume normal work activities<br />
from day 3<br />
This includes IV drugs and Stoma<br />
Care<br />
IF YOU OR YOUR MANAGER HAS ANY CONCERNS PLEASE CONTACT<br />
INFECTION CONTROL 5170 OR THE OCCUPATIONAL HEALTH DEPARTMENT<br />
4326<br />
Authorities<br />
Document Control Information<br />
Author: Sue Dailly Lead Nurse IC Type: Policy<br />
Sponsor: Director of Infection Prevention and Control Scope: Major<br />
Reference: CP055<br />
Issue Number: 4<br />
Date April 2010 Status: Published<br />
Page 49 of 55
Winchester & Eastleigh Healthcare <strong>NHS</strong> <strong>Trust</strong><br />
<strong>MRSA</strong> POLICY<br />
Employee Safety & Occupational Health Department<br />
INSTRUCTIONS FOR STAFF WHO HAVE A POSITIVE <strong>MRSA</strong> RESULT<br />
NAME<br />
WARD<br />
Your recent swab has been reported to be positive to <strong>MRSA</strong> and resistant to the<br />
standard treatment therefore as a healthcare worker you must ensure that you<br />
fully comply with the treatment and follow up screening detailed below.<br />
Because of possible restrictions on working, you MUST inform the senior nurse/your<br />
manager on duty so that staffing levels can be adjusted.<br />
STAGE 1<br />
Date<br />
Treatment<br />
to Commence:<br />
……………..<br />
………... day<br />
STAGE 2<br />
Day 1<br />
day<br />
Day 2<br />
day<br />
Day 3<br />
day<br />
Day 4<br />
day<br />
Day 5<br />
day<br />
Day 6<br />
day<br />
Day 7<br />
day<br />
<br />
<br />
<br />
<br />
<br />
<br />
<br />
RESISTANT TREATMENT – PACK B<br />
PRIOR TO COMMENCING TREATMENT<br />
1. Swab nose, groins and any skin breaks/wounds.<br />
(One swab should be used for both nostrils, another for<br />
both grains and another for both groins).<br />
3. Now commence treatment below.<br />
TREATMENT<br />
All 3 Treatment products to be used as detailed below.<br />
Please notify OH or Infection Control if you have any<br />
hypersensitivity to the products below<br />
2.<br />
3. 1. Apply Naseptin® nasal cream - 4 times a day for 10<br />
days.<br />
4.<br />
2. Gargle with Corsodyl® for 2 minutes (minimum) - 4<br />
times a day for 10 days – Leave an interval of 30<br />
minutes between using the mouth wash and toothpaste<br />
if possible.<br />
3. Wash with Hibiscrub® – 2 times a day for 10 days<br />
paying particular attention to axillae, groin and skin<br />
creases. Not for use on the face.<br />
N.B It is important that you continue the treatment for<br />
the full 10 days.<br />
Day 8 <br />
day<br />
Day 9 <br />
day<br />
Authorities<br />
Document Control Information<br />
Author: Sue Dailly Lead Nurse IC Type: Policy<br />
Sponsor: Director of Infection Prevention and Control Scope: Major<br />
Reference: CP055<br />
Issue Number: 4<br />
Date April 2010 Status: Published<br />
Page 50 of 55
Winchester & Eastleigh Healthcare <strong>NHS</strong> <strong>Trust</strong><br />
<strong>MRSA</strong> POLICY<br />
Day 10 <br />
day<br />
STAGE 3<br />
Day 13 <br />
day<br />
Date:<br />
Day 18 <br />
day<br />
Date:<br />
Please Note:<br />
AFTER TREATMENT<br />
Re-swab all sites as above after 2 clear days following<br />
treatment (before attending shift / work that day).<br />
Re-swab all sites as above after a further 5 days (before<br />
attending shift / work that day) unless you are informed that<br />
the swab results on ‘Day 13’ remain positive in which case<br />
you will be advised on further treatment.<br />
1. It is important that you continue the treatment for the full 10 days.<br />
2. If any of the re-swab results are <strong>MRSA</strong> positive the Occupational Health<br />
Adviser will contact you again and a further treatment schedule is likely to be<br />
recommended.<br />
3. After the second treatment you will be informed of the results, if any of the reswab<br />
results remain <strong>MRSA</strong> positive the Consultant Microbiologist will be<br />
contacted by the Occupational Health Adviser who will in turn contact you<br />
regarding any treatment and work.<br />
IF YOU HAVE ANY FURTHER WORRIES OR CONCERNS PLEASE CONTACT<br />
INFECTION CONTROL 5170 OR THE OCCUPATIONAL HEALTH DEPARTMENT<br />
4326<br />
WORKING ARRANGEMENTS - High Risk Areas (ICU, HDU, elective orthopaedic<br />
ward and NNU)<br />
Treatment Day 1 Day 2 Day 3 Day 4<br />
Day 5<br />
Do not work on Day 1 and Day 2<br />
unless you can work with no<br />
patient contact i.e. if you can carry<br />
out an administrative role.<br />
Return to work from day 3 without<br />
restriction on work activities<br />
WORKING ARRANGEMENTS - Theatre Staff<br />
Authorities<br />
Document Control Information<br />
Author: Sue Dailly Lead Nurse IC Type: Policy<br />
Sponsor: Director of Infection Prevention and Control Scope: Major<br />
Reference: CP055<br />
Issue Number: 4<br />
Date April 2010 Status: Published<br />
Page 51 of 55
Winchester & Eastleigh Healthcare <strong>NHS</strong> <strong>Trust</strong><br />
<strong>MRSA</strong> POLICY<br />
Treatment Day 1 Day 2 Day 3 Day 4<br />
Day 5<br />
Continue working from Day 1.<br />
You must not undertake or assist<br />
in invasive procedures i.e. work as<br />
a ‘scrub nurse’, central lines or<br />
cannulate for the first 2 days but<br />
may work in other areas<br />
Change as before to include staff<br />
who are not nurses<br />
May resume normal work activities<br />
from day 3<br />
WORKING ARRANGEMENTS - Lower risk areas (All other Clinical areas not<br />
indicated above)<br />
Treatment Day 1 Day 2 Day 3 Day 4<br />
Day 5<br />
Continue working from Day 1.<br />
You must not carry out aseptic<br />
techniques or invasive procedures<br />
for day 1 and 2.<br />
May resume normal work activities<br />
from day 3<br />
This includes IV drugs and Stoma<br />
Care<br />
IF YOU OR YOUR MANAGER HAS ANY CONCERNS PLEASE CONTACT<br />
INFECTION CONTROL 5170 OR THE OCCUPATIONAL HEALTH DEPARTMENT<br />
4326<br />
Authorities<br />
Document Control Information<br />
Author: Sue Dailly Lead Nurse IC Type: Policy<br />
Sponsor: Director of Infection Prevention and Control Scope: Major<br />
Reference: CP055<br />
Issue Number: 4<br />
Date April 2010 Status: Published<br />
Page 52 of 55
Winchester & Eastleigh Healthcare <strong>NHS</strong> <strong>Trust</strong><br />
<strong>MRSA</strong> POLICY<br />
Appendix 12 – Criteria for elective screening exemptions<br />
Following the circulation of the Department of Health Operating Framework for 2008/9<br />
all elective patients must be screened for <strong>MRSA</strong>. This includes medicine, surgery,<br />
family services and orthopaedics. If the criteria of patients for exclusion of <strong>MRSA</strong><br />
screening changes this appendix will be amended and circulated by the Infection<br />
Control Team to staff involved in elective <strong>MRSA</strong> screening.<br />
• <strong>MRSA</strong> operational guidance issued in 2008 clarified the criteria for elective<br />
screening exemptions:<br />
• Day case ophthalmology<br />
• Day case dental<br />
• Day case endoscopy<br />
• Minor dermatology procedures<br />
• Paediatrics – except high risk<br />
• Maternity except elective caesarean sections and high risk cases<br />
If these patients have previously had <strong>MRSA</strong> they should be screened prior to<br />
admission, like any other elective <strong>MRSA</strong> positive patient.<br />
Authorities<br />
Document Control Information<br />
Author: Sue Dailly Lead Nurse IC Type: Policy<br />
Sponsor: Director of Infection Prevention and Control Scope: Major<br />
Reference: CP055<br />
Issue Number: 4<br />
Date April 2010 Status: Published<br />
Page 53 of 55
Winchester & Eastleigh Healthcare <strong>NHS</strong> <strong>Trust</strong><br />
<strong>MRSA</strong> POLICY<br />
Appendix 12 - Equality Impact Assessment Tool<br />
To be completed and attached to any controlled document when submitted to the appropriate<br />
committee for consideration and approval.<br />
Yes/No<br />
Comments<br />
1. Does the <strong>policy</strong>/guidance affect one group<br />
less or more favourably than another on the<br />
basis of:<br />
• Race<br />
• Ethnic origins (including gypsies and<br />
travellers)<br />
• Nationality<br />
• Gender<br />
• Culture<br />
• Religion or belief<br />
• Sexual orientation including lesbian, gay<br />
and bisexual people<br />
• Age<br />
• Disability - learning disabilities, physical<br />
disability, sensory impairment and mental<br />
health problems<br />
No<br />
No<br />
No<br />
No<br />
No<br />
No<br />
No<br />
No<br />
No<br />
No<br />
2. Is there any evidence that some groups are<br />
affected differently?<br />
3. If you have identified potential<br />
discrimination, are any exceptions valid,<br />
legal and/or justifiable?<br />
4. Is the impact of the <strong>policy</strong>/guidance likely to<br />
be negative?<br />
5. If so can the impact be avoided? No<br />
No<br />
No<br />
No<br />
6. What alternatives are there to achieving the<br />
<strong>policy</strong>/guidance without the impact?<br />
7. Can we reduce the impact by taking<br />
different action?<br />
No<br />
No<br />
If you have identified a potential discriminatory impact of this procedural document, please refer it to the<br />
Head of Corporate Services, together with any suggestions as to the action required to avoid/reduce<br />
this impact. For advice in respect of answering the above questions, please contact:<br />
Board Secretary Tel No: 01962 825903<br />
Authorities<br />
Document Control Information<br />
Author: Sue Dailly Lead Nurse IC Type: Policy<br />
Sponsor: Director of Infection Prevention and Control Scope: Major<br />
Reference: CP055<br />
Issue Number: 4<br />
Date April 2010 Status: Published<br />
Page 54 of 55
Winchester & Eastleigh Healthcare <strong>NHS</strong> <strong>Trust</strong><br />
<strong>MRSA</strong> POLICY<br />
Appendix 13 – Communications Log<br />
Ref Policy Date of<br />
Issue<br />
To Whom<br />
OP999 An example 09/09/1999 A Member of Staff<br />
Signed as read<br />
and<br />
Understood<br />
Authorities<br />
Document Control Information<br />
Author: Sue Dailly Lead Nurse IC Type: Policy<br />
Sponsor: Director of Infection Prevention and Control Scope: Major<br />
Reference: CP055<br />
Issue Number: 4<br />
Date April 2010 Status: Published<br />
Page 55 of 55