Cladribine combined with cyclophosphamide and ... - Hem-aids.ru
Cladribine combined with cyclophosphamide and ... - Hem-aids.ru
Cladribine combined with cyclophosphamide and ... - Hem-aids.ru
You also want an ePaper? Increase the reach of your titles
YUMPU automatically turns print PDFs into web optimized ePapers that Google loves.
Patients <strong>and</strong> methods<br />
Patients<br />
Between August 1998 <strong>and</strong> December 2000, 62 previously<br />
untreated patients <strong>with</strong> progressive or symptomatic CLL were<br />
treated <strong>with</strong> a <strong>combined</strong> chemotherapy consistingof 2-CdA,<br />
<strong>cyclophosphamide</strong> <strong>and</strong> mitoxantrone. The characteristics of<br />
the patients are shown in Table 1. All of the patients fulfilled<br />
the National Cancer Institute-Sponsored WorkingGroup criteria<br />
for CLL. 22 Pretreatment evaluation included examination<br />
of medical history, physical examination, complete blood cell<br />
count, differential count of WBC, chemical survey, bone marrow<br />
examination <strong>and</strong> se<strong>ru</strong>m immunoglobulin level quantitation.<br />
Cytogenetic analysis was not routinely performed. The<br />
patients had peripheral lymphocytosis greater than 10 × 10 9 /l<br />
<strong>and</strong> more than 30% lymphocytes in normal or hypercellular<br />
bone marrow. The differences between mean values in both<br />
groups of patients were not significant. Cell marker studies<br />
were performed to confirm B cell origin <strong>and</strong> monoclonal proliferation.<br />
All patients were CD5, CD19, CD20 <strong>and</strong> CD23<br />
positive <strong>and</strong> showed monoclonality for light chain immunoglobulin<br />
membrane surface receptors.<br />
The clinical stage of disease was determined at the time of<br />
initiation of the treatment accordingto Rai’s classification. 23<br />
The distribution is shown in Table 1. Patients in stage 0, I <strong>and</strong><br />
II were eligible if they had evidence of active disease, including<br />
progressive lymphocytosis, massive splenomegaly or<br />
bulky lymphadenopathy, recurrent disease-related infections,<br />
weight loss 10% over a 6 month period, temperature of<br />
38°C related to disease or extreme fatigue. Patients <strong>with</strong> poor<br />
performance status (WHO scale 4), active infection, abnormal<br />
liver or renal function <strong>and</strong> Richter’s syndrome were excluded<br />
from the study. The study was approved by Local Ethical Committees<br />
<strong>and</strong> the patients had signed the informed consent<br />
form.<br />
Treatment modality<br />
The doses <strong>and</strong> schedule of the treatment agents were based<br />
on previous studies in cases of CLL relapse, refractory CLL or<br />
low-grade lymphoma. 7,19–21<br />
CMC in untreated CLL<br />
T Robak et al<br />
In the first part of the study, CMC protocol consisted of 2-<br />
CdA administered at a dose 0.12 mg/kg in 2-h i.v. infusion for<br />
5 (CMC5) days, mitoxantrone 10 mg/m 2 i.v. on day 1 <strong>and</strong><br />
<strong>cyclophosphamide</strong> 650 mg/m 2 i.v. on day 1. In the second<br />
part of the study, 2-CdA administration was shortened to 3<br />
days (CMC3) because of excessive hematological toxicity of<br />
CMC5 protocol. The doses of mitoxantrone <strong>and</strong> <strong>cyclophosphamide</strong><br />
were the same as in the CMC5 protocol. 2-CdA<br />
(Biodrybin) was synthesized accordingto the method of Kazimierczuk<br />
et al 24 <strong>and</strong> was commercially available from the<br />
Institute of Biotechnology <strong>and</strong> Antibiotics- Bioton (Warsaw,<br />
Pol<strong>and</strong>).<br />
The cycles were repeated over 28 days for three courses. If<br />
hematological complications (thrombocytopenia 50 × 10 9 /l,<br />
granulocytopenia 0.5 × 10 9 /l) or severe infections developed<br />
the d<strong>ru</strong>gs were re-administered at time intervals longer than<br />
28 days, ranging from 2 to 4 months, until the increase of<br />
hematological parameters or recovery from infections was<br />
noted. If a response had been documented, patients were<br />
treated until maximal response or prohibitive toxicity. If no<br />
response or progression of the disease was observed after<br />
three cycles, the treatment was discontinued. Packed red cells<br />
were transfused for symptomatic anemia or prophylactically<br />
if the hemoglobin level was lower than 7.0 g/dl. Platelets were<br />
administered prophylactically if the platelet count was less<br />
than 15.0 × 10 9 /l. Blood products were irradiated. In order to<br />
prevent hype<strong>ru</strong>ricemia, allopurinol (300 mg/daily) was administered.<br />
No patients received antibiotics or antiviral agents<br />
prophylactically. No patients received hematopoietic growth<br />
factors prophylactically but G-CSF or GM-CSF were administered<br />
if the absolute granulocyte count was less than 1.0 ×<br />
10 9 /l <strong>and</strong> active infection was present.<br />
Response criteria<br />
Treatment effect was monitored by physical examination,<br />
blood count evaluation <strong>and</strong> bone marrow examination before<br />
<strong>and</strong> after every course of chemotherapy. Guidelines for<br />
response were those developed by the NCI-Sponsored WorkingGroup.<br />
22,25 Complete response (CR) required the absence<br />
of symptoms <strong>and</strong> organomegaly, normal complete blood cell<br />
count (absolute neutrophil count 1.0 × 10 9 /l, hemoglobin<br />
1511<br />
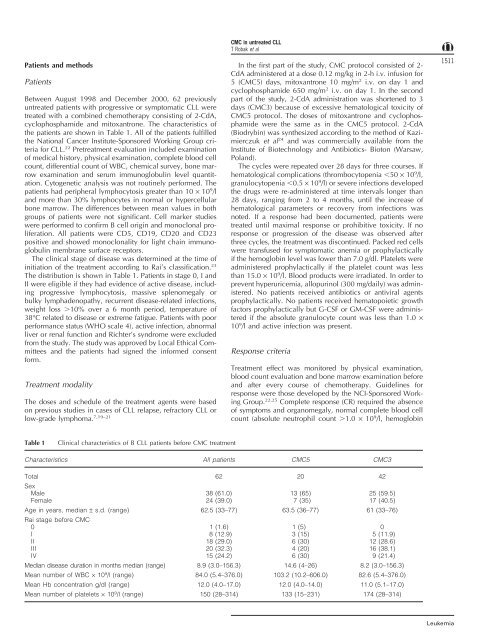
Table 1<br />
Clinical characteristics of B CLL patients before CMC treatment<br />
Characteristics All patients CMC5 CMC3<br />
Total 62 20 42<br />
Sex<br />
Male 38 (61.0) 13 (65) 25 (59.5)<br />
Female 24 (39.0) 7 (35) 17 (40.5)<br />
Age in years, median ± s.d. (range) 62.5 (33–77) 63.5 (36–77) 61 (33–76)<br />
Rai stage before CMC<br />
0 1 (1.6) 1 (5) 0<br />
I 8 (12.9) 3 (15) 5 (11.9)<br />
II 18 (29.0) 6 (30) 12 (28.6)<br />
III 20 (32.3) 4 (20) 16 (38.1)<br />
IV 15 (24.2) 6 (30) 9 (21.4)<br />
Median disease duration in months median (range) 8.9 (3.0–156.3) 14.6 (4–26) 8.2 (3.0–156.3)<br />
Mean number of WBC × 10 9 /l (range) 84.0 (5.4–376.0) 103.2 (10.2–606.0) 82.6 (5.4–376.0)<br />
Mean Hb concentration g/dl (range) 12.0 (4.0–17.0) 12.0 (4.0–14.0) 11.0 (5.1–17.0)<br />
Mean number of platelets × 10 9 /l (range) 150 (28–314) 133 (15–231) 174 (28–314)<br />
Leukemia