Mary Fitzpatrick, BSN, MPH, ANP
Mary Fitzpatrick, BSN, MPH, ANP
Mary Fitzpatrick, BSN, MPH, ANP
Create successful ePaper yourself
Turn your PDF publications into a flip-book with our unique Google optimized e-Paper software.
<strong>Mary</strong> <strong>Fitzpatrick</strong>, <strong>ANP</strong>, MSCN<br />
Michelle Cameron, MD, PT
This continuing education activity is managed<br />
and accredited by Professional Education<br />
Service Group. The material presented in this<br />
activity represents the opinion of the faculty.<br />
Neither PESG, nor any accrediting<br />
organization endorses any commercial<br />
products displayed in conjunction with this<br />
activity.<br />
Commercial Support was not received for this<br />
activity.
Michelle Cameron, MD, PT has received<br />
research support from Acorda Therapeutics<br />
<strong>Mary</strong> <strong>Fitzpatrick</strong>, <strong>ANP</strong>, has attended and been<br />
compensated for a Biogen-Idec nurse<br />
advisory meeting<br />
CME Staff Disclosures<br />
◦ Professional Education Services Group staff have no<br />
financial interest or relationships to disclose
At the conclusion of this activity, the<br />
participant will be able to:<br />
◦ Describe the nature of gait and balance<br />
impairments common in Veterans with MS<br />
◦ Recognize Veterans with MS with gait and balance<br />
impairments<br />
◦ Recommend interventions to improve walking and<br />
reduce fall risk in Veterans with MS
Background<br />
Walking impairment in MS<br />
◦ Nature of walking impairments in MS<br />
◦ Treatment of slowed walking in Veterans with MS –<br />
A VA experience with dalfampridine<br />
Falls and Imbalance in MS<br />
◦ Prevalence and incidence of falls in MS<br />
◦ Falls in Veterans with MS<br />
◦ Management of imbalance and falls in MS
CNS disorder (brain, spinal cord, optic nerves)<br />
Symptoms separated in time and space<br />
Complex immune-mediated disorder
Very varied but… @ initial presentation<br />
◦ Reduced sensation (33%*)<br />
◦ Visual changes – vision loss (16%), diplopia (7%)<br />
◦ Weakness (13%)<br />
◦ Unsteadiness when walking (5%)<br />
◦ Poor balance (3%)<br />
◦ Multiple symptoms (15%)<br />
Also<br />
◦ Spasticity<br />
◦ Incontinence<br />
◦ Cognitive changes<br />
All of these can affect walking and balance
Compared with health controls, people with<br />
MS:<br />
◦ Walk more slowly<br />
◦ Have reduced gait endurance<br />
◦ Have reduced community mobility<br />
◦ Take shorter steps<br />
◦ Step more slowly<br />
◦ Have less joint movement during gait<br />
◦ Have more variability in most gait parameters<br />
◦ Slow down more when performing a cognitive task
Sensory changes – particularly proprioception<br />
Lower extremity weakness<br />
Lower extremity spasticity<br />
Cerebellar ataxia
Timed measures<br />
◦ Timed 25-Foot Walk Test (for speed)<br />
◦ 6-minute/2-minute walk test (for endurance)<br />
◦ Timed Up and Go (for functional speed)<br />
Patient Reported Outcomes<br />
◦ Multiple Sclerosis Walking Scale-12<br />
• a patient-based measure of the impact of MS on<br />
walking<br />
Observational Gait Analysis<br />
◦ Watch them walk
Instrumented walkway<br />
Gait lab<br />
Gyroscopes and accelerometers
Objectives:<br />
For a 12 month cohort of patients with MS<br />
prescribed dalfampridine at a VA Medical Center, to<br />
determine tolerability and effects of dalfampridine<br />
on:<br />
◦ walking speed, (Timed 25 foot walk)<br />
◦ self-perceived impact of multiple sclerosis (MS) on walking,<br />
(MSWS-12)<br />
◦ walking endurance, (2 minute timed walk)<br />
◦ community participation, (Community Integration<br />
Questionnaire)
01/22/2010 the FDA approved dalfampridine to<br />
improve walking in patients with MS<br />
Based on research demonstrating improved<br />
◦ walking speed on the timed 25-foot walk test (T25FWT)<br />
◦ self-perceived walking using the Multiple Sclerosis Walking<br />
Scale-12 (MSWS-12).<br />
Since dalfampridine became clinically available, no<br />
analyses of its real-world tolerability or<br />
effectiveness have been published.
All patients prescribed dalfampridine at the Portland VA<br />
Medical Center from 10/01/10-09/30/11<br />
◦ T25FTW,<br />
◦ MSWS-12,<br />
◦ two minute timed walk (2MTW)<br />
◦ Community Integration Questionnaire (CIQ)<br />
Baseline assessment prior to taking dalfampridine.<br />
Individuals reporting a favorable response to<br />
dalfampridine at 3-4 weeks continued to take the drug<br />
All measures repeated at 1-4 months and at follow-up<br />
MS clinic visits.<br />
Measures were compared with baseline using paired t-<br />
tests.
Time (seconds)<br />
25 Foot Timed Walk<br />
50<br />
45<br />
Mean: 13.86 ± 9.55<br />
N = 23<br />
Mean: 10.55 ± 6.18<br />
N = 22, P = 0.002<br />
Mean: 9.40 ± 2.75<br />
N = 16, P = 0.071<br />
40<br />
35<br />
30<br />
25<br />
20<br />
15<br />
10<br />
5<br />
0<br />
Baseline 1-4 months 5-10 months
Score<br />
MS Walking Scale - 12<br />
60<br />
50<br />
40<br />
30<br />
20<br />
Mean: 53.09 5.66<br />
N=22<br />
Mean: 41.82 ± 11.66<br />
N = 22, P = 0.000<br />
Mean: 48.00 ± 9.53<br />
N = 6, P = 0.064<br />
10<br />
Baseline 1-4 months 5-10 months
Distance (feet)<br />
Two Minute Timed Walk<br />
620<br />
520<br />
Mean: 196.75 ± 58.92<br />
N=20<br />
Mean: 266.16 ± 99.94, N = 16, P = 0.008 Mean: 207.86 ± 72.62<br />
N = 7, P = 0.967<br />
420<br />
320<br />
220<br />
120<br />
20<br />
Baseline 1-4 months 5-10 months
Score<br />
Community Integration Questionnaire<br />
25<br />
23<br />
21<br />
Mean: 13.26 ± 3.58<br />
N=21<br />
Mean: 14.40 ± 3.72, N = 20, P = 0.094 Mean: 13.75 ± 3.86<br />
N = 4, P = 0.391<br />
19<br />
17<br />
15<br />
13<br />
11<br />
9<br />
7<br />
5<br />
Baseline 1-4 months 5-10 months
1. 39 individuals were prescribed dalfampridine during<br />
the 12 month period analyzed.<br />
2. 23 individuals (58%) continued beyond the initial 3-4<br />
week trial.<br />
3. 16 individuals (42%) stopped within 3-4 weeks due to<br />
intolerance and/or perceived lack of efficacy. There<br />
were no serious AEs.<br />
4. Walking speed, endurance and self-perceived walking<br />
improved significantly at 1-4 month follow-up.<br />
5. There was a trend towards improvement in walking<br />
speed and self-perceived walking at 5-10 month<br />
follow-up.
‣ Walking speed, endurance, and self-perceived<br />
walking were improved at 1-4 months with<br />
dalfampridine.<br />
‣ Community participation was not significantly<br />
improved at 1-4 month follow-up.<br />
‣ More complete follow-up of the sample is needed<br />
to reliably and validly assess longer term impacts
75% complain of balance abnormalities<br />
>50% fall in 3 months<br />
12% had an injurious fall in 6 months<br />
50% with an injurious fall ever<br />
Balance abnormalities occur in those with<br />
minimal or undetectable impairments, as well<br />
as in those with significant impairments
Balance – control of center of mass over base<br />
of support<br />
Postural control - Control of the body’s<br />
position in space, when stationary or moving<br />
Fall – unintentional change in position<br />
resulting in coming to rest on the ground or<br />
at a lower level
% Falls in 12 months<br />
How many people with MS fall?<br />
489 Neurology inpatients<br />
34% had fallen in the last year<br />
32% of those with MS had fallen in the last year<br />
70<br />
60<br />
50<br />
40<br />
30<br />
20<br />
10<br />
0<br />
PD Sync PNP EPIL SD MND MS PSY Stroke Pain<br />
Neurological Diagnosis<br />
PD Parkinson’s disease<br />
Sync Syncope<br />
PNP Polyneuropathy<br />
SD Spinal disorders<br />
EPIL Epilepsy<br />
MND Motor neuron disease<br />
MS Multiple sclerosis<br />
PSY Psychogenic<br />
Falls in Frequent Neurological Diseases, Stolze et al J Neurology, 251:79-84, 2004
Risk of Falls in Subjects with MS<br />
Cattaneo D, DeNuzzo C, Fascia T, et al. Risks of falls in subjects<br />
with multiple sclerosis. Arch Phys Med Rehabil.<br />
2002;83(6):864-7.<br />
50 people with MS in Italy<br />
◦ 54% (27/50) reported 1 or more falls in the<br />
previous 2 months<br />
◦ 32% (17/50)reported 2 or more falls in the<br />
previous 2 months
Falling in People with MS Aged 45-90<br />
years<br />
Finlayson, ML, Peterson EW. Arch Phys Med Rehabil.<br />
2006;87:1274-9<br />
1,089 people with MS in the Midwest US<br />
◦ 52% reported falling at least once in the prior<br />
6 months<br />
Nilsagard, 48/76 (63%) people with MS in<br />
Sweden recorded 270 falls in 3 months
– 58 people with MS in Portand<br />
falls in 2 mo - # who fell – 30/58 (52%)<br />
# w/ ≥ 2 falls - 16/58 (28%)<br />
falls in 12 mo # who fell – 43/58 (74%)<br />
# w/ ≥ 2 falls - 36/58 (62%)<br />
# w/ > 10 falls - 5/58 (9%)
Falls in Veterans with MS in VISN20<br />
◦ 195,417 Veterans in VISN20 (NW USA), 721 with MS<br />
◦ Unadjusted odds of an injurious fall was 1.9 times<br />
higher in veterans with MS than in veterans without<br />
MS<br />
◦ For females: Odds were 3 times higher for veterans<br />
with MS than for veterans without MS (OR 3.0, 95%<br />
CI 1.6-5.5)<br />
◦ For males: Odds were 1.2 times higher for veterans<br />
with MS than for veterans without MS (OR 1.2, 95%<br />
CI 0.8-2.1)
Fear of falling<br />
Injuries and death<br />
Impaired balance<br />
Impaired walking<br />
Use of a walking aide<br />
Disturbed proprioception<br />
Spasticity<br />
More severe MS<br />
Lower income<br />
Leg weakness
Divided attention<br />
Reduced muscular endurance<br />
Fatigue<br />
Heat sensitivity
Have you fallen in the last year?<br />
Questionnaires<br />
◦ Activities-specific Balance Confidence (ABC)<br />
◦ Falls Efficacy Scale (FES)<br />
◦ Dizziness Handicap Inventory (DHI)<br />
Fall diaries<br />
Romberg<br />
Clinical Tests<br />
◦ Berg Balance Scale<br />
◦ Functional Reach<br />
◦ Balance Evaluation Systems Test (BESTest)
Based on<br />
◦ General common pathophysiology<br />
• Somatosensory dysfunction<br />
• Impaired central integration<br />
◦ Individual examination and assessment
Gait assistive devices<br />
Exercise/balance training<br />
Safety strategies<br />
Home modifications
Enhance input<br />
◦ TENS, strap or brace on leg<br />
◦ Light touch cane<br />
◦ Auditory input<br />
◦ Tongue stimulation<br />
◦ Practice<br />
Substitution<br />
◦ Increase reliance on vision and vestibular<br />
Avoidance<br />
◦ Avoid low light<br />
◦ Avoid uneven surfaces
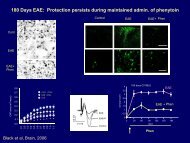
A cane or hiking poles to provide proprioceptive<br />
information more than support
Light touch – increases proprioceptive<br />
input<br />
No Touch Light Touch Heavy Touch<br />
A-P<br />
M-L<br />
Center of Pressure<br />
M-L<br />
M-L<br />
Dickstein and Horak<br />
Gait and Posture,<br />
2000
Practice<br />
◦ Dual task<br />
Avoid<br />
◦ Dual/multiple task
Walking and talking<br />
Walking and head turns<br />
Walking and visual distraction<br />
Walking and auditory distraction
Foot wear<br />
Home hazards<br />
◦ Lights<br />
◦ Trips
Many Veterans with MS have impaired walking<br />
and poor balance and fall frequently<br />
There are many ways to assess gait and<br />
imbalance in Veterans with MS<br />
Interventions to improve gait and imbalance<br />
in Veterans with MS include:<br />
◦ Medications<br />
◦ Devices<br />
◦ Exercise<br />
◦ Environmental modifications
If you would like to receive continuing<br />
education credit for this activity, please visit:<br />
http://pva.cds.pesgce.com/