Spring 2013 - Tufts University School of Dental Medicine
Spring 2013 - Tufts University School of Dental Medicine
Spring 2013 - Tufts University School of Dental Medicine
Create successful ePaper yourself
Turn your PDF publications into a flip-book with our unique Google optimized e-Paper software.
“WHAT’SREALLYSPECIALABOUTTHEEPIGENOMEISTHAT<br />
ITGIVESCELLSTHEABILITYTOREGULATEWHICHGENESARE<br />
EXPRESSED,WITHOUTALTERINGINFORMATIONSTOREDIN<br />
THEDNAITSELF.”—Jonathan Garlick<br />
in on recipes relevant to liver<br />
cells, and a healthy nerve cell<br />
will focus only on recipes that<br />
make nerve cells.<br />
This selective reading <strong>of</strong><br />
DNA is made possible by a<br />
biochemical control system<br />
called the epigenome.<br />
Like a set <strong>of</strong> bookmarks, it<br />
highlights certain sections<br />
<strong>of</strong> DNA, allowing specific<br />
genes to “turn on” as a cell<br />
develops. The epigenome can<br />
also “mask” parts <strong>of</strong> DNA,<br />
effectively turning those genes<br />
<strong>of</strong>f. By selecting which genes<br />
can be activated at a given<br />
time, the system guides cells<br />
to develop into specific types.<br />
“What’s really special about<br />
the epigenome is that it gives<br />
cells the ability to regulate<br />
which genes are expressed,<br />
without altering information<br />
stored in the DNA itself,” says<br />
Garlick.<br />
The epigenome is also key<br />
to creating iPS cells. The four<br />
genes that Garlick’s lab add to<br />
skin cells can rearrange these<br />
DNA “bookmarks,” making<br />
only specific parts <strong>of</strong> the DNA<br />
cookbook (the parts needed<br />
to make an embryoniclike<br />
cell) available for browsing.<br />
As a result, the cell is reprogrammed<br />
back to its original<br />
embryonic state.<br />
Understanding the epigenome<br />
has big implications for<br />
understanding disease, Garlick<br />
notes. A patient may have flawless<br />
DNA, but if his or her cells<br />
are reading it wrong, well, there<br />
are going to be problems. He<br />
thinks these epigenetic glitches<br />
might cause some nonhealing<br />
disorders—and that iPS cells<br />
could <strong>of</strong>fer a tantalizing cure.<br />
“If we can understand the<br />
epigenome in iPS, we can think<br />
about using cells derived from<br />
them to treat a chronic wound<br />
or periodontal gum defect that<br />
doesn’t heal, and potentially<br />
reverse those defects,” he says.<br />
Although iPS cell therapy is<br />
promising, it’s not yet a magic<br />
bullet. Clinical trials, slated to<br />
begin in Japan by March 2014,<br />
haven’t yet been approved in<br />
the United States. The field<br />
is so new, Garlick notes, it’s<br />
unclear whether iPS cells can<br />
be used in humans without<br />
complications. “We have to<br />
be 100 percent sure that any<br />
cell derived from an iPS won’t<br />
give rise to a tumor,” he says.<br />
“That’s going to be a big challenge<br />
to the field.”<br />
In the meantime, he and his<br />
team are using tissues grown<br />
from iPS cells to study diabetic<br />
foot ulcers in the lab. “By using<br />
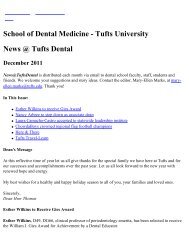
A colony <strong>of</strong> human-induced pluripotent stem cells. Each <strong>of</strong> the cells in this<br />
cluster has the potential to remain a stem cell or can be stimulated to<br />
become a more specialized cell type with therapeutic potential.<br />
iPS-derived cells to engineer<br />
skinlike tissues, it’s possible<br />
to examine the behavior and<br />
biology <strong>of</strong> diseases in ways we<br />
couldn’t do in humans,” he<br />
says. “Essentially, we have a<br />
surrogate for a human right on<br />
our lab bench.”<br />
In a dish filled with orange<br />
fluid, he points out a translucent,<br />
dime-sized puck. It’s<br />
human skin tissue grown<br />
from iPS cells. Garlick’s team<br />
is using it to examine how<br />
the cells might behave once<br />
transplanted into a patient. Up<br />
close, it looks like an insignificant<br />
blurry mass, yet what it<br />
represents is something much<br />
bigger. By using tissues like<br />
these to gain a deeper understanding<br />
<strong>of</strong> what makes new<br />
iPS-derived cells tick, Garlick<br />
says it may one day be possible<br />
to create a sort <strong>of</strong> biological<br />
“repair kit” to treat nonhealing<br />
diseases in the mouth and<br />
throughout the body.<br />
“<strong>Dental</strong> research like this<br />
contributes to an understanding<br />
<strong>of</strong> basic disease processes<br />
that are broadly relevant to the<br />
entire body,” he says. “After all,<br />
our mission as dentist-scientists<br />
is to advance both oral and<br />
systemic health—to reduce<br />
the burden <strong>of</strong> disease, and to<br />
improve quality <strong>of</strong> life.”<br />
David Levin is a freelance<br />
science writer based in Boston.<br />
IMAGES: IPSC CORE LAB/SCHOOL OF DENTAL MEDICINE<br />
spring <strong>2013</strong> tufts dental medicine 9