Scientific <strong>Poster</strong>s – <strong>Poster</strong> <strong>Session</strong> 2Physics, Fondazione IRCCS Istituto Nazionale Dei Tumori,Milano, Italy; 5 Department of Pathology and MolecularBiology, Fondazione IRCCS Istituto Nazionale Dei Tumori,Milano, ItalyObjective: Radical surgery is the gold standard of chordomas,but often it is unfeasible due to the tumor anatomicallocation. Definitive high-dose radiation therapy (RT) isan alternative, as reported for proton-beam RT. IntensityModulated RT (IMRT) allows to deliver high-dose RT withphotons (X-RT). We report on a series of locally advancedchordoma patients treated at our institution with exclusivehigh-dose X-RT alone or in combination with imatinib.Methods: We retrospectively reviewed all consecutivechordoma patients affected by a primary, localized disease,who were referred to the RT Department of our Institutionfrom 2004 to 2012, focusing on those treated with high-doseexclusive X-RT (e.g. ≥70Gy). Among 41 screened patients,19 (M/F = 15/4; median age/range = 66.3/32-86 yrs; site= 89% sacrum, 11% lumbar spine; previous debulkingsurgery: 6) received exclusive high-dose X-RT and areconsidered in the present analysis. 3 more patients are ontreatment, 3 underwent high-dose proton-beam RT, 3 receivedpalliative RT, 13 received complete surgery followedby adjuvant RT, and are not considered in this analysis. In 9cases, RT was administered with concomitant imatinib, 400mg/day. Toxicity, radiological response (tumor shrinkageand signal changes on MRI) and symptomatic improvementwere reviewed. Local progression-free survival (PFS)was calculated from the end of the treatment. Patients deadfor any reason were considered as failed to treatment. Median(range) follow-up was 23 (2-55) months.Results: The averaged delivered dose to the gross tumorvolume (GTV) was 73 Gy (range: 70-78). Overall, therapywas well tolerated (no G3-4 toxicities), without neurologicalside effects, even in the subgroup receiving concomitantimatinib. 5/19 patients had a local recurrence (26%) with amedian local PFS of 41 months (range 14-55). The medianlocal PFS was 24 months (range 2-50). All relapsed patientshad a sacral chordoma, and received 70-72Gy administeredby using a 3DCRT technique.Conclusion: Our series provides preliminary evidence thathigh-dose X-RT in extra-cranial chordoma is feasible, evenin combination with imatinib. Pts who received >73Gywith IMRT/Arc therapy had a better prognosis than thosetreated with 3DCRT at a dose
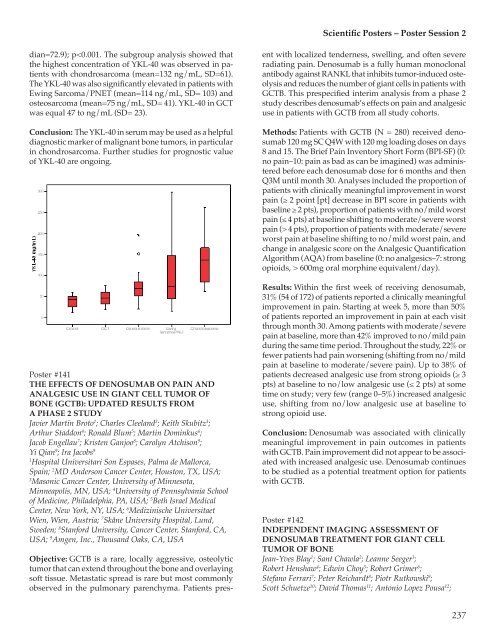
Scientific <strong>Poster</strong>s – <strong>Poster</strong> <strong>Session</strong> 2dian=72.9); p 4 pts), proportion of patients with moderate/severeworst pain at baseline shifting to no/mild worst pain, andchange in analgesic score on the Analgesic QuantificationAlgorithm (AQA) from baseline (0: no analgesics–7: strongopioids, > 600mg oral morphine equivalent/day).Results: Within the first week of receiving denosumab,31% (54 of 172) of patients reported a clinically meaningfulimprovement in pain. Starting at week 5, more than 50%of patients reported an improvement in pain at each visitthrough month 30. Among patients with moderate/severepain at baseline, more than 42% improved to no/mild painduring the same time period. Throughout the study, 22% orfewer patients had pain worsening (shifting from no/mildpain at baseline to moderate/severe pain). Up to 38% ofpatients decreased analgesic use from strong opioids (≥ 3pts) at baseline to no/low analgesic use (≤ 2 pts) at sometime on study; very few (range 0–5%) increased analgesicuse, shifting from no/low analgesic use at baseline tostrong opioid use.Conclusion: Denosumab was associated with clinicallymeaningful improvement in pain outcomes in patientswith GCTB. Pain improvement did not appear to be associatedwith increased analgesic use. Denosumab continuesto be studied as a potential treatment option for patientswith GCTB.<strong>Poster</strong> #142INDEPENDENT IMAGING ASSESSMENT OFDENOSUMAB TREATMENT FOR GIANT CELLTUMOR OF BONEJean-Yves Blay 1 ; Sant Chawla 2 ; Leanne Seeger 3 ;Robert Henshaw 4 ; Edwin Choy 5 ; Robert Grimer 6 ;Stefano Ferrari 7 ; Peter Reichardt 8 ; Piotr Rutkowski 9 ;Scott Schuetze 10 ; David Thomas 11 ; Antonio Lopez Pousa 12 ;237