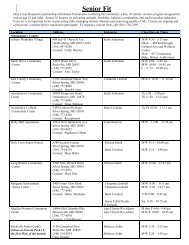
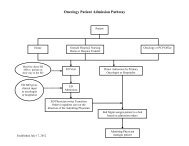
Go,baby, go!Born needinglife-saving care,Zadie is ahealthy and feisty2-year-old todayWhen Zadie Brown was born 12 weeksearly, she weighed only 2 pounds,2 ounces.“I worried that every breath wouldbe her last,” says Zadie’s mom, MeghanChapple-Brown, with tears in her eyes.Because of serious pregnancy complications,Zadie was born at only28 weeks. She spent 46 days in <strong>Holy</strong> <strong>Cross</strong><strong>Hospital</strong>’s Neonatal Intensive Care Unit(NICU), the largest NICU in the state.“The medical and emotional supportfrom the NICU staff and love of familyand friends is what got us through,” saysthe 36-year-old mother.SPECIAL MOMENTS: Ty Brown bondswith his newborn daughter, Zadie, in<strong>Holy</strong> <strong>Cross</strong> <strong>Hospital</strong>’s NICU.highest-quality care While all prematurebabies are at risk for health problems,those born before 32 weeks are atgreater risk for serious complications.The biggest challenge for Zadie wasa significant breathing problem calledrespiratory distress syndrome (RDS).Babies with RDS lack a protein calledsurfactant, which keeps small air sacsin the lungs from collapsing. Zadiewas treated with replacement surfactantto coat her lungs and to allow foreasier breathing, and a small plastictube placed in her nose continuously8 <strong>Holy</strong> <strong>Cross</strong> Health
delivered pressurized air to her lungs.“We offer the highest degree of qualitycare for critically ill newborns,” saysSharon Kiernan, MD, medical director,Neonatology Services. “Our Level IIIBNICU features state-of-the-art technologyto treat babies who are born earlyor have medical complications thatrequire constant observation or specializedcare.”Because of her underdeveloped centralnervous system, Zadie sometimesstopped breathing, a condition calledapnea. Babies in the NICU are constantlymonitored for apnea. When externalstimulation does not remind the baby tostart breathing, a nurse quickly coversthe baby’s face with a mask to pumpoxygen into the lungs.“Zadie had to be resuscitated twice,and it was terrifying,” Meghan says. “Thenurses were very calm and very professional.They and the doctors were alwaysreassuring us while keeping us in touchwith the realities that Zadie faced.”Another common problem foundin premature babies is a heart defectcalled patent ductus arteriosus (PDA).Before birth a large artery lets bloodbypass the lungs, because the fetus getsits oxygen through the placenta. Thisartery normally closes soon after birth sothat blood can travel to the lungs to getoxygen. When the artery does not closeproperly, it can lead to heart failure.A specialized form of ultrasound,called echocardiography, helped physiciansdiagnose Zadie with PDA, andmedication helped close the artery.PREPARED FOR COMPLICATIONS TheNICU team—including neonatologists(physicians who specialize in newborncare), registered nurses, neonatal nursepractitioners, physical therapists, respiratorytherapists, social workers, case managersand lactation consultants—alsocarefully monitored Zadie for commonmedical complications faced by prematurebabies, including the inabilityto maintain body temperature, braindamage, vision loss, jaundice and reflux.Coordinating patient care in the NICUis a nurse navigator, who works witheach family to answer questions and toensure that each baby has everythinghe or she needs to thrive. For familiesinterested in spiritual support, chaplainsare available to patients and families ofall faiths and beliefs.“We couldn’t have asked for bettercare and attention from <strong>Holy</strong> <strong>Cross</strong><strong>Hospital</strong>’s doctors and nurses,” Meghansays. “We were there for two months,and they became our family. I have theutmost confidence in their care and trustin their staff.”<strong>Holy</strong> <strong>Cross</strong> <strong>Hospital</strong> delivers morebabies than any other hospital in Marylandor the District of Columbia.“And if pregnancycomplications occur, weoffer a unique on-callservice through whichobstetricians can consultwith a maternalfetalmedicine specialistand admit high-riskpatients to <strong>Holy</strong> <strong>Cross</strong><strong>Hospital</strong> under the specialist’scare,” says AnnB. Burke, MD, medicaldirector, Obstetrics andGynecology.ONGOING SUPPORTR e m i n i s c i n g a b o u tZadie’s discharge fromthe NICU, Meghan says,“Taking Zadie home forthe first time was anamazing and wonderfulday.”But leaving the NICUand going home alsocan be scary becauseSIMPLy THE BEST:“We couldn’t haveasked for better careand attention from<strong>Holy</strong> <strong>Cross</strong> <strong>Hospital</strong>’sdoctors and nurses,”says MeghanChapple-Brown,mother of ZadieBrown.physicians and nurses are no longerproviding around-the-clock care. To easethe transition, a <strong>Holy</strong> <strong>Cross</strong> Home Carenurse visited the Brown family the verynext day. The home care nurse did afull assessment of Zadie and during thenext three visits helped the family withbreathing and feeding difficulties.“Today, there are no lingering medicalissues, and she has caught up toher peers,” Meghan says. All her NICUworries are behind her.“Zadie loves to dance,” Meghansays. “You should see her salsa. It’shysterical!”Learn more about <strong>Holy</strong> <strong>Cross</strong><strong>Hospital</strong>’s Maternity Services atour free baby fair on Sunday, Nov. 15,from 1 to 4 p.m. For more information,see page 15, call 301-754-8800 or visitwww.holycrosshealth.org.www.holycrosshealth.org9