<strong>M<strong>in</strong>eral</strong> <strong>Homeostasis</strong> <strong>in</strong> <strong>CKD</strong> - <strong>M<strong>in</strong>eral</strong> <strong>and</strong> <strong>Bone</strong> <strong>Disorder</strong>: Evolv<strong>in</strong>g Concepts <strong>in</strong> Prevention <strong>and</strong> Treatment CME/CEDr. Block: You br<strong>in</strong>g up a great po<strong>in</strong>t. David <strong>and</strong> I have done some of that work, <strong>and</strong> I agree with you -- some of the researchpo<strong>in</strong>ts <strong>in</strong> one direction <strong>and</strong> some po<strong>in</strong>ts <strong>in</strong> the other direction, <strong>and</strong> so there is uncerta<strong>in</strong>ty. One of the th<strong>in</strong>gs that you brought upwith calcium vs noncalcium agents is whether serum calcium values should be the marker by which we evaluate their safety. Arethese drugs safe because they do, or do not, <strong>in</strong>crease serum calcium? I th<strong>in</strong>k all of you have done some work with regard to howmuch calcium actually gets <strong>in</strong>to us. What is the calcium balance? As you said, Munro, the physiology we try to ma<strong>in</strong>ta<strong>in</strong> is a neutralbalance as you reach a steady state -- the “<strong>in</strong>” equals the “out.” But when we provide this elemental calcium load <strong>in</strong> the form of calciumb<strong>in</strong>ders, we run <strong>in</strong>to some potential problems. One of the excit<strong>in</strong>g th<strong>in</strong>gs at this year’s meet<strong>in</strong>g are the abstracts that both ofyou have submitted with regard to calcium balance. We have had very little calcium balance data or phosphorus balance data <strong>in</strong>the past 20 years. Katie, maybe you can share with us a little bit about your work with Dr. Peacock on this <strong>and</strong> how you approachthis balance issue.Dr. Hill: What I will show you with our data is that you can have very high positive calcium balance but serum calcium rema<strong>in</strong>scompletely normal -- you have not affected it. At the ASN [American Society of Nephrology] meet<strong>in</strong>g this year, we are report<strong>in</strong>gour results from a study <strong>in</strong> patients with stage 3 <strong>and</strong> 4 <strong>CKD</strong>, where we measured calcium balance <strong>and</strong> phosphate balance while thepatients were on a controlled calcium <strong>and</strong> phosphate diet. We previously reported our calcium balance data <strong>in</strong> these patients atthe American Society of <strong>Bone</strong> <strong>and</strong> <strong>M<strong>in</strong>eral</strong> Research <strong>in</strong> September 2011. What we found is that, as expected, when patients aregiven 1500 mg per day of elemental calcium <strong>in</strong> the form of a calcium carbonate phosphate b<strong>in</strong>der, fecal calcium <strong>in</strong>creases from884 mg per day to just over 2000 mg per day. Ur<strong>in</strong>ary calcium, however, is unaffected. Patients are absorb<strong>in</strong>g a lot more netcalcium, but they are not excret<strong>in</strong>g any more <strong>in</strong> their ur<strong>in</strong>e. This is a problem that results <strong>in</strong> a positive calcium balance. We can seethat, on placebo, when the patients were on a basal diet of around 1000 mg of calcium per day, they essentially were <strong>in</strong> neutralcalcium balance, but given the 1500 mg of calcium from the phosphate b<strong>in</strong>der, they went up to around 400 mg positive calciumbalance. This was a significant difference, be<strong>in</strong>g able to produce a pretty substantial positive calcium balance by giv<strong>in</strong>g thisphosphate b<strong>in</strong>der. We did not see any differences <strong>in</strong> serum calcium, so we were not produc<strong>in</strong>g hypercalcemia <strong>in</strong> these patients.Dr. Block: That is fundamentally important for how we treat these patients, particularly if we are go<strong>in</strong>g to start treat<strong>in</strong>g them early.Given the FGF data, the temptation is to start us<strong>in</strong>g phosphate b<strong>in</strong>ders very early <strong>in</strong> the course of <strong>CKD</strong>-MBD. I th<strong>in</strong>k we have toshow a little restra<strong>in</strong>t, because we do not have the cl<strong>in</strong>ical studies to demonstrate whether or not us<strong>in</strong>g cl<strong>in</strong>ical doses of a b<strong>in</strong>derto produce nearly 400 mg per day of positive calcium balance will turn out to be beneficial.Dr. Peacock: This is of concern to the population with osteoporosis <strong>and</strong> the elderly. Many of these patients are <strong>in</strong> early renalfailure, <strong>and</strong> one of the st<strong>and</strong>ard therapies is calcium supplementation. We hope the calcium is go<strong>in</strong>g <strong>in</strong>to the bone, but of coursethere is no way of know<strong>in</strong>g that it is not go<strong>in</strong>g <strong>in</strong>to the soft tissues.Pg.14
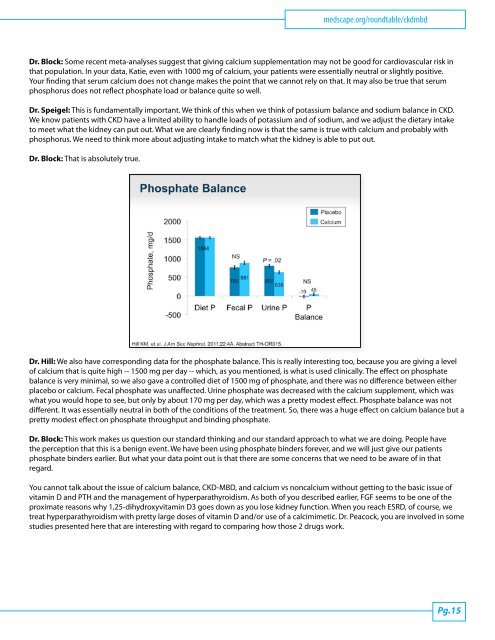
medscape.org/roundtable/ckdmbdDr. Block: Some recent meta-analyses suggest that giv<strong>in</strong>g calcium supplementation may not be good for cardiovascular risk <strong>in</strong>that population. In your data, Katie, even with 1000 mg of calcium, your patients were essentially neutral or slightly positive.Your f<strong>in</strong>d<strong>in</strong>g that serum calcium does not change makes the po<strong>in</strong>t that we cannot rely on that. It may also be true that serumphosphorus does not reflect phosphate load or balance quite so well.Dr. Speigel: This is fundamentally important. We th<strong>in</strong>k of this when we th<strong>in</strong>k of potassium balance <strong>and</strong> sodium balance <strong>in</strong> <strong>CKD</strong>.We know patients with <strong>CKD</strong> have a limited ability to h<strong>and</strong>le loads of potassium <strong>and</strong> of sodium, <strong>and</strong> we adjust the dietary <strong>in</strong>taketo meet what the kidney can put out. What we are clearly f<strong>in</strong>d<strong>in</strong>g now is that the same is true with calcium <strong>and</strong> probably withphosphorus. We need to th<strong>in</strong>k more about adjust<strong>in</strong>g <strong>in</strong>take to match what the kidney is able to put out.Dr. Block: That is absolutely true.Dr. Hill: We also have correspond<strong>in</strong>g data for the phosphate balance. This is really <strong>in</strong>terest<strong>in</strong>g too, because you are giv<strong>in</strong>g a levelof calcium that is quite high -- 1500 mg per day -- which, as you mentioned, is what is used cl<strong>in</strong>ically. The effect on phosphatebalance is very m<strong>in</strong>imal, so we also gave a controlled diet of 1500 mg of phosphate, <strong>and</strong> there was no difference between eitherplacebo or calcium. Fecal phosphate was unaffected. Ur<strong>in</strong>e phosphate was decreased with the calcium supplement, which waswhat you would hope to see, but only by about 170 mg per day, which was a pretty modest effect. Phosphate balance was notdifferent. It was essentially neutral <strong>in</strong> both of the conditions of the treatment. So, there was a huge effect on calcium balance but apretty modest effect on phosphate throughput <strong>and</strong> b<strong>in</strong>d<strong>in</strong>g phosphate.Dr. Block: This work makes us question our st<strong>and</strong>ard th<strong>in</strong>k<strong>in</strong>g <strong>and</strong> our st<strong>and</strong>ard approach to what we are do<strong>in</strong>g. People havethe perception that this is a benign event. We have been us<strong>in</strong>g phosphate b<strong>in</strong>ders forever, <strong>and</strong> we will just give our patientsphosphate b<strong>in</strong>ders earlier. But what your data po<strong>in</strong>t out is that there are some concerns that we need to be aware of <strong>in</strong> thatregard.You cannot talk about the issue of calcium balance, <strong>CKD</strong>-MBD, <strong>and</strong> calcium vs noncalcium without gett<strong>in</strong>g to the basic issue ofvitam<strong>in</strong> D <strong>and</strong> PTH <strong>and</strong> the management of hyperparathyroidism. As both of you described earlier, FGF seems to be one of theproximate reasons why 1,25-dihydroxyvitam<strong>in</strong> D3 goes down as you lose kidney function. When you reach ESRD, of course, wetreat hyperparathyroidism with pretty large doses of vitam<strong>in</strong> D <strong>and</strong>/or use of a calcimimetic. Dr. Peacock, you are <strong>in</strong>volved <strong>in</strong> somestudies presented here that are <strong>in</strong>terest<strong>in</strong>g with regard to compar<strong>in</strong>g how those 2 drugs work.Pg.15










![NIH STROKE SCALE Interval: 1[ ] Baseline 2[ ] 2 hours ... - Medscape](https://img.yumpu.com/43645244/1/190x245/nih-stroke-scale-interval-1-baseline-2-2-hours-medscape.jpg?quality=85)