extensive subgaleal abscess and epidural empyema in
extensive subgaleal abscess and epidural empyema in
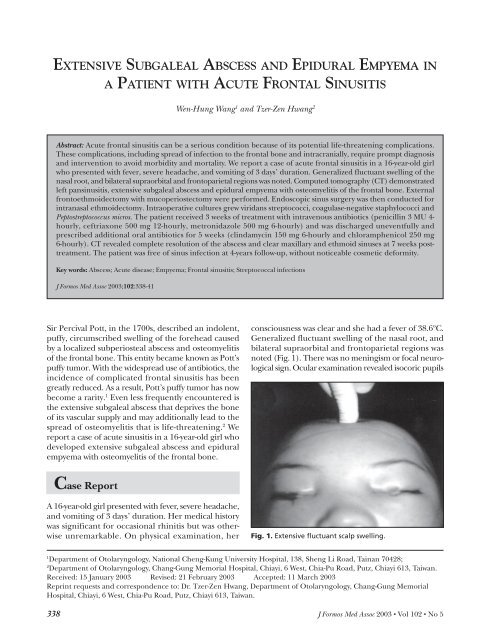
extensive subgaleal abscess and epidural empyema in
Create successful ePaper yourself
Turn your PDF publications into a flip-book with our unique Google optimized e-Paper software.
Pott’s Puffy TumorA) B)Fig. 2. A) Pretreatment axial computed tomogram show<strong>in</strong>g left maxillary opacification. B) Pretreatment coronal computedtomogram show<strong>in</strong>g left ethmoid opacification.A) B)Fig. 3. A) Coronal computed tomogram show<strong>in</strong>g air-fluid level <strong>in</strong> the left frontal s<strong>in</strong>us <strong>and</strong> <strong>extensive</strong> <strong>subgaleal</strong> <strong>abscess</strong> <strong>in</strong>the bilateral parietal regions. Note: this section was taken <strong>in</strong> the sup<strong>in</strong>e position, show<strong>in</strong>g fluid above air. B) Axial computedtomogram show<strong>in</strong>g <strong>subgaleal</strong> <strong>abscess</strong> <strong>and</strong> <strong>epidural</strong> <strong>empyema</strong>.with prompt light reflex, unimpaired visual acuity<strong>and</strong> unlimited extraocular muscle movement. Nasalexam<strong>in</strong>ation revealed purulent discharge <strong>in</strong> the leftmiddle meatus. Laboratory <strong>in</strong>vestigations showedleukocytosis with a left shift; C-reactive prote<strong>in</strong> was20.4 mg/dL (normal range, 0 to 5 mg/dL).Computed tomography (CT) demonstrated leftpans<strong>in</strong>usitis (Fig. 2A <strong>and</strong> 2B), <strong>extensive</strong> <strong>subgaleal</strong><strong>abscess</strong> <strong>in</strong> the bilateral frontoparietal regions <strong>and</strong><strong>epidural</strong> <strong>empyema</strong> of the frontal lobe (Fig. 3A <strong>and</strong>3B). Bony destruction of the frontal s<strong>in</strong>us was noted,<strong>in</strong>dicat<strong>in</strong>g osteomyelitis of the frontal bone (Fig. 4).A preoperative diagnosis of acute s<strong>in</strong>usitis complicatedby <strong>subgaleal</strong> <strong>abscess</strong> <strong>and</strong> <strong>epidural</strong> <strong>empyema</strong> was made,<strong>and</strong> the patient was taken to surgery.An eyebrow <strong>in</strong>cision was performed <strong>in</strong> the gullw<strong>in</strong>g fashion. As the scalp was <strong>in</strong>cised, a significantamount of pus gushed from the <strong>in</strong>cision. The scalphad been spontaneously dissected <strong>subgaleal</strong>ly by<strong>abscess</strong> formation. The outer table of the left frontals<strong>in</strong>us was centrally eroded with a bony defect, activelydischarg<strong>in</strong>g pus. The defect was widened <strong>and</strong> bone withabnormal appearance was removed us<strong>in</strong>g an air drill.Mucoperiostectomy was performed. A bony defect ofthe <strong>in</strong>ner table was found <strong>and</strong> a burr hole was drilled todra<strong>in</strong> the purulent, <strong>epidural</strong> accumulation. The <strong>in</strong>feriorwall was removed with preservation of the supraorbitalridge. Endoscopic s<strong>in</strong>us surgery was then conductedfor <strong>in</strong>tranasal ethmoidectomy, particularly focus<strong>in</strong>gon unroof<strong>in</strong>g the frontal recess. Middle meatal antrostomywas also performed for the concomitant maxillarys<strong>in</strong>usitis. The scalp wound was vigorously irrigated <strong>and</strong>closed <strong>in</strong> layers. Catheters were placed <strong>subgaleal</strong>ly fordra<strong>in</strong>age <strong>and</strong> removed 9 days after surgery.Intraoperative cultures grew viridans streptococci,coagulase-negative staphylococci <strong>and</strong> Peptostreptococcusmicros. The patient received 3 weeks of treatment with<strong>in</strong>travenous antibiotics (penicill<strong>in</strong> 3 MU 4-hourly,J Formos Med Assoc 2003 • Vol 102 • No 5 339
Pott’s Puffy Tumorcomplications. 7,8 Pla<strong>in</strong> films may not demonstratemucosal thicken<strong>in</strong>g, bone erosion, or soft tissue changesseen with <strong>abscess</strong>es.Aggressive surgical dra<strong>in</strong>age <strong>and</strong> debridement ofthe osteomyelitic bone rema<strong>in</strong> the ma<strong>in</strong>stay of therapy.Pott’s puffy tumor is best treated by treph<strong>in</strong>ationthrough the medial aspect of the floor of the frontals<strong>in</strong>us to decompress the <strong>in</strong>fected s<strong>in</strong>us. Material may,thus, be obta<strong>in</strong>ed for culture <strong>and</strong> sensitivity tests. 6Recent advances <strong>in</strong> endoscopic s<strong>in</strong>us surgery haveprovided alternative access to the frontal recess todecompress the frontal s<strong>in</strong>us. Accurate assessment <strong>and</strong>thorough dra<strong>in</strong>age of the <strong>abscess</strong> <strong>and</strong> removal ofosteomyelitic bone up to the marg<strong>in</strong>s of normal boneis essential to treat an <strong>extensive</strong> <strong>subgaleal</strong> <strong>abscess</strong><strong>and</strong> spread<strong>in</strong>g osteomyelitis. Close cooperation withthe neurosurgeon is necessary to deal with <strong>in</strong>tracranialcomplications. S<strong>in</strong>ce patients who present withcomplications of acute frontal s<strong>in</strong>usitis frequently havemultis<strong>in</strong>us disease, dra<strong>in</strong>age of the other diseased s<strong>in</strong>usmay prevent future episodes of s<strong>in</strong>usitis.The cultures from frontal s<strong>in</strong>usitis with complicationsfrequently reveal polymicrobial <strong>in</strong>volvement.Streptococci, staphylococci <strong>and</strong> anaerobic bacteria arethe predom<strong>in</strong>ant pathogens. 9,10 Patients should bestarted on broad-spectrum <strong>in</strong>travenous antibioticsbefore availability of surgical culture results. A frequentlychosen comb<strong>in</strong>ation is: 1) a third-generationcephalospor<strong>in</strong>; 2) metronidazole; <strong>and</strong> 3) a penicill<strong>in</strong>or vancomyc<strong>in</strong>. Although penicill<strong>in</strong> is active aga<strong>in</strong>stmost anaerobes, most stra<strong>in</strong>s of Bacteroides fragilis areresistant. It has been suggested, therefore, that unlessanaerobes can be excluded, all paranasal s<strong>in</strong>us<strong>in</strong>fections fail<strong>in</strong>g to respond promptly or develop<strong>in</strong>gcomplications should be treated with metronidazole<strong>in</strong> addition to the normal therapeutic regimen. 11,12Thus, we chose comb<strong>in</strong>ation therapy with penicill<strong>in</strong>,ceftriaxone, <strong>and</strong> metronidazole to treat this patient.Microbiological identification of the pathogens isimportant for adm<strong>in</strong>istration of the most appropriateantimicrobial therapy. The duration of antimicrobialtherapy should be about 6 to 8 weeks. 1,11Extensive <strong>subgaleal</strong> <strong>abscess</strong> <strong>and</strong> <strong>epidural</strong> <strong>empyema</strong>are rare complications of s<strong>in</strong>usitis <strong>in</strong> this postantibioticera. Nonetheless, the cl<strong>in</strong>ical course is fulm<strong>in</strong>at<strong>in</strong>g <strong>and</strong>potentially life-threaten<strong>in</strong>g. There must be a high<strong>in</strong>dex of suspicion for prompt identification of s<strong>in</strong>usitiscomplications <strong>and</strong> prompt management <strong>in</strong> order toavoid further progression <strong>and</strong> debilitat<strong>in</strong>g sequelae.References1. Babu RP, Todor R, Kasoff SS: Pott’s puff tumor: the forgotten entity.Case report. J Neurosurg 1996;84:110-2.2. Thomas JN, Nel JR: Acute spread<strong>in</strong>g osteomyelitis of the skullcomplicat<strong>in</strong>g frontal s<strong>in</strong>usitis. J Laryngol Otol 1977;91:55-62.3. Montgomery WW, Cheney ML, Jacobs EE: Osteomyelitis of thefrontal bone. Ann Otol Rh<strong>in</strong>ol Laryngol 1989;98:848-53.4. Morgan PR, Morrison WV: Complications of frontal <strong>and</strong> ethmoids<strong>in</strong>usitis. Laryngoscope 1980;90:661-6.5. Fairbanks DNF, Milmoe GJ: The diagnosis <strong>and</strong> management ofs<strong>in</strong>usitis <strong>in</strong> children. Complications <strong>and</strong> sequelae: an otolaryngologist’sperspective. Pediatr Infect 1985;4(Suppl):S75-8.6. Altman KW, Aust<strong>in</strong> MB, Tom LWC, et al: Complications of frontals<strong>in</strong>usitis <strong>in</strong> adolescents: case presentations <strong>and</strong> treatmentoptions. Int J Pediatr Otorh<strong>in</strong>olaryngol 1997;41:9-20.7. S<strong>in</strong>gh B, Van Dellen J, Ramjettan S, et al: S<strong>in</strong>ogenic <strong>in</strong>tracranialcomplications. J Laryngol Otol 1995;109:945-50.8. Wells RG, Sty JR, L<strong>and</strong>ers D: Radiological evaluation of Pott puffytumor. JAMA 1986;255:1331-3.9. Verbon A, Husni RN, Gordon SM, et al: Pott’s puffy tumor dueto Haemophilus <strong>in</strong>fluenzae: case report <strong>and</strong> review. Cl<strong>in</strong> InfectDis 1996;23:1305-7.10. Feder HM Jr, Cates KL, Cement<strong>in</strong>a AM: Pott puffy tumor: aserious occult <strong>in</strong>fection. Pediatrics 1987;79:625-9.11. Giannoni CM, Stewart MG, Alford EL: Intracranial complicationsof s<strong>in</strong>usitis. Laryngoscope 1997;107:863-7.12. Daya S, To SS: A ‘silent’ <strong>in</strong>tracranial complication of frontals<strong>in</strong>usitis. J Laryngol Otol 1990;104:645-7.J Formos Med Assoc 2003 • Vol 102 • No 5 341