23 Lower Eyelid Blepharoplasty - Facial plastic surgeon in San Diego
23 Lower Eyelid Blepharoplasty - Facial plastic surgeon in San Diego
23 Lower Eyelid Blepharoplasty - Facial plastic surgeon in San Diego
Create successful ePaper yourself
Turn your PDF publications into a flip-book with our unique Google optimized e-Paper software.
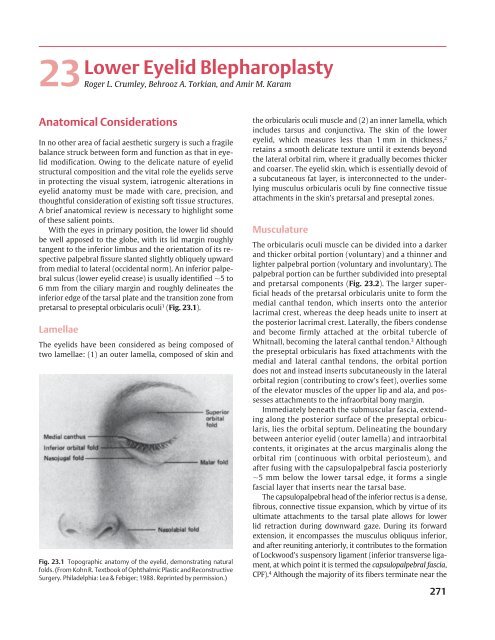
<strong>Lower</strong> <strong>Eyelid</strong> <strong>Blepharoplasty</strong><strong>23</strong>Roger L. Crumley, Behrooz A. Torkian, and Amir M. KaramAnatomical ConsiderationsIn no other area of facial aesthetic surgery is such a fragilebalance struck between form and function as that <strong>in</strong> eyelidmodification. Ow<strong>in</strong>g to the delicate nature of eyelidstructural composition and the vital role the eyelids serve<strong>in</strong> protect<strong>in</strong>g the visual system, iatrogenic alterations <strong>in</strong>eyelid anatomy must be made with care, precision, andthoughtful consideration of exist<strong>in</strong>g soft tissue structures.A brief anatomical review is necessary to highlight someof these salient po<strong>in</strong>ts.With the eyes <strong>in</strong> primary position, the lower lid shouldbe well apposed to the globe, with its lid marg<strong>in</strong> roughlytangent to the <strong>in</strong>ferior limbus and the orientation of its respectivepalpebral fissure slanted slightly obliquely upwardfrom medial to lateral (occidental norm). An <strong>in</strong>ferior palpebralsulcus (lower eyelid crease) is usually identified 5 to6 mm from the ciliary marg<strong>in</strong> and roughly del<strong>in</strong>eates the<strong>in</strong>ferior edge of the tarsal plate and the transition zone frompretarsal to preseptal orbicularis oculi 1 (Fig. <strong>23</strong>.1).LamellaeThe eyelids have been considered as be<strong>in</strong>g composed oftwo lamellae: (1) an outer lamella, composed of sk<strong>in</strong> andFig. <strong>23</strong>.1 Topographic anatomy of the eyelid, demonstrat<strong>in</strong>g naturalfolds. (From Kohn R. Textbook of Ophthalmic Plastic and ReconstructiveSurgery. Philadelphia: Lea & Febiger; 1988. Repr<strong>in</strong>ted by permission.)the orbicularis oculi muscle and (2) an <strong>in</strong>ner lamella, which<strong>in</strong>cludes tarsus and conjunctiva. The sk<strong>in</strong> of the lowereyelid, which measures less than 1 mm <strong>in</strong> thickness, 2reta<strong>in</strong>s a smooth delicate texture until it extends beyondthe lateral orbital rim, where it gradually becomes thickerand coarser. The eyelid sk<strong>in</strong>, which is essentially devoid ofa subcutaneous fat layer, is <strong>in</strong>terconnected to the underly<strong>in</strong>gmusculus orbicularis oculi by f<strong>in</strong>e connective tissueattachments <strong>in</strong> the sk<strong>in</strong>’s pretarsal and preseptal zones.MusculatureThe orbicularis oculi muscle can be divided <strong>in</strong>to a darkerand thicker orbital portion (voluntary) and a th<strong>in</strong>ner andlighter palpebral portion (voluntary and <strong>in</strong>voluntary). Thepalpebral portion can be further subdivided <strong>in</strong>to preseptaland pretarsal components (Fig. <strong>23</strong>.2). The larger superficialheads of the pretarsal orbicularis unite to form themedial canthal tendon, which <strong>in</strong>serts onto the anteriorlacrimal crest, whereas the deep heads unite to <strong>in</strong>sert atthe posterior lacrimal crest. Laterally, the fibers condenseand become firmly attached at the orbital tubercle ofWhitnall, becom<strong>in</strong>g the lateral canthal tendon. 3 Althoughthe preseptal orbicularis has fixed attachments with themedial and lateral canthal tendons, the orbital portiondoes not and <strong>in</strong>stead <strong>in</strong>serts subcutaneously <strong>in</strong> the lateralorbital region (contribut<strong>in</strong>g to crow’s feet), overlies someof the elevator muscles of the upper lip and ala, and possessesattachments to the <strong>in</strong>fraorbital bony marg<strong>in</strong>.Immediately beneath the submuscular fascia, extend<strong>in</strong>galong the posterior surface of the preseptal orbicularis,lies the orbital septum. Del<strong>in</strong>eat<strong>in</strong>g the boundarybetween anterior eyelid (outer lamella) and <strong>in</strong>traorbitalcontents, it orig<strong>in</strong>ates at the arcus marg<strong>in</strong>alis along theorbital rim (cont<strong>in</strong>uous with orbital periosteum), andafter fus<strong>in</strong>g with the capsulopalpebral fascia posteriorly5 mm below the lower tarsal edge, it forms a s<strong>in</strong>glefascial layer that <strong>in</strong>serts near the tarsal base.The capsulopalpebral head of the <strong>in</strong>ferior rectus is a dense,fibrous, connective tissue expansion, which by virtue of itsultimate attachments to the tarsal plate allows for lowerlid retraction dur<strong>in</strong>g downward gaze. Dur<strong>in</strong>g its forwardextension, it encompasses the musculus obliquus <strong>in</strong>ferior,and after reunit<strong>in</strong>g anteriorly, it contributes to the formationof Lockwood’s suspensory ligament (<strong>in</strong>ferior transverse ligament,at which po<strong>in</strong>t it is termed the capsulopalpebral fascia,CPF). 4 Although the majority of its fibers term<strong>in</strong>ate near the271
272 II Aesthetic <strong>Facial</strong> SurgeryFig. <strong>23</strong>.2 Major divisions of the m. orbicularisoculi <strong>in</strong>to pretarsal, preseptal, and orbital components.<strong>in</strong>ferior tarsal border, some extend through orbital fat contribut<strong>in</strong>gto compartmentalization, some penetrate the preseptalorbicularis to <strong>in</strong>sert subcutaneously about the lowereyelid crease, and others extend from the <strong>in</strong>ferior fornix superiorlyto contribute to Tenon’s capsule (Fig. <strong>23</strong>.3).Orbital FatConta<strong>in</strong>ed beh<strong>in</strong>d the orbital septum and with<strong>in</strong> theorbital cavity, the orbital fat has been classically segmented<strong>in</strong>to discrete pockets (lateral, central, and medial), although<strong>in</strong>terconnections truly exist. 5 The lateral fat pad is smallerand more superiorly situated, and the larger nasal pad isdivided by the <strong>in</strong>ferior oblique muscle <strong>in</strong>to a larger centralfat compartment and an <strong>in</strong>termediate medial compartment.(Dur<strong>in</strong>g surgery, care must be taken to avoid <strong>in</strong>jury tothe <strong>in</strong>ferior oblique.) The medial pad has characteristicdifferences from its other counterparts, <strong>in</strong>clud<strong>in</strong>g a lightercolor, a more fibrous and compact lobular pattern, and afrequent association with a sizable blood vessel near itsmedial aspect. The orbital fat can be considered an adynamicstructure because its volume is not related to bodyhabitus, and once removed it is not thought to regenerate.InnervationSensory <strong>in</strong>nervation to the lower lid derives ma<strong>in</strong>ly fromthe <strong>in</strong>fraorbital nerve with m<strong>in</strong>or contributions from the<strong>in</strong>fratrochlear and zygomaticofacial nerve branches. Theblood supply is obta<strong>in</strong>ed from the angular, <strong>in</strong>fraorbital,and transverse facial arteries. Situated 2 mm below theciliary marg<strong>in</strong>, between the orbicularis oculi and the tarsus,is the marg<strong>in</strong>al arcade, which should be avoided if asubciliary <strong>in</strong>cision is used.Fig. <strong>23</strong>.3 Cross-sectional diagram of the lower eyeliddemonstrat<strong>in</strong>g connective tissue expansion of <strong>in</strong>feriorrectus <strong>in</strong>to its term<strong>in</strong>al <strong>in</strong>sertions.
<strong>23</strong> <strong>Lower</strong> <strong>Eyelid</strong> <strong>Blepharoplasty</strong> 273Term<strong>in</strong>ologySeveral descriptive terms are used pervasively <strong>in</strong> the literatureof eyelid analysis and should be understood bythose <strong>in</strong>volved <strong>in</strong> surgical management of this area.Blepharochalasis is a commonly misused term. It is anuncommon disorder of the upper eyelids, of unknowncause, which affects ma<strong>in</strong>ly young and middle-agedfemales. Blepharochalasis is characterized by recurrentattacks of pa<strong>in</strong>less unilateral or bilateral lid edema, caus<strong>in</strong>ga loss of sk<strong>in</strong> elasticity and atrophic changes.Dermatochalasis is an acquired condition of <strong>in</strong>creased,abnormal laxity of the eyelid sk<strong>in</strong> <strong>in</strong>terrelated withgenetic predisposition, natural ag<strong>in</strong>g phenomenon, andenvironmental <strong>in</strong>fluences. It is frequently associated withprolapsed orbital fat.Steatoblepharon is a condition of true herniation orpseudoherniation of orbital fat beh<strong>in</strong>d a weakened orbitalseptum, caus<strong>in</strong>g areas of discrete or diffuse fullness <strong>in</strong> theeyelids. This condition and dermatochalasis are the twomost common reasons why a patient presents to discusseyelid surgery.Festoons are s<strong>in</strong>gle or multiple folds of orbicularis oculi<strong>in</strong> the lower lid that drape over onto themselves, creat<strong>in</strong>gan external, hammock-like bag. Depend<strong>in</strong>g on location,this bag may be preseptal, orbital, or jugal (cheek). It mayconta<strong>in</strong> fat.Malar bags are areas of soft tissue fullness on the lateraledge of the <strong>in</strong>fraorbital ridge and zygomatic prom<strong>in</strong>encejust superior to the palpebromalar sulcus. Theyare believed to be a result of recurrent dependent tissueedema and secondary fibrosis.Preoperative EvaluationA systematic and thorough preoperative assessment ofblepharoplasty candidates is essential to m<strong>in</strong>imize potentialpostoperative complications. Thus, patient analysis isdirected to determ<strong>in</strong><strong>in</strong>g how much eyelid sk<strong>in</strong>, orbicularisoculi, and orbital fat needs to be resected to optimizefunctional and aesthetic results, and whether the ocularand adnexal structures will tolerate such a surgical manipulationwithout undesirable sequelae.Risk Factors for PostoperativeDry Eye SyndromeRealiz<strong>in</strong>g that the protective physiological functions ofbl<strong>in</strong>k<strong>in</strong>g and eyelid closure are temporarily impairedfollow<strong>in</strong>g blepharoplasty, an appropriate ocular historyshould elicit <strong>in</strong>formation that might put the patient atgreater risk for postoperative dry eye syndrome. Excessivetear<strong>in</strong>g, a burn<strong>in</strong>g or gritty sensation, ocular discomfort,foreign bodies, mucus production, eyelid crust<strong>in</strong>g, anda frequent need to bl<strong>in</strong>k are all symptoms suggestive ofborderl<strong>in</strong>e or <strong>in</strong>adequate tear production. A possibleatopic cause has to be ruled out.Certa<strong>in</strong> systemic diseases, particularly the collagenvascular diseases (i.e., systemic lupus erythematosus,scleroderma, periarteritis nodosa), Sjögren syndrome,Wegener granulomatosis, ocular pemphigoid, and Stevens–Johnson syndrome, can <strong>in</strong>terfere with the glandular lubricat<strong>in</strong>gfunction and should be identified. 6,7 The <strong>in</strong>filtrativeophthalmopathy of Graves’ disease can result <strong>in</strong> verticaleyelid retraction and <strong>in</strong>adequate corneal protection aftersurgery and should be managed with medical treatmentpreoperatively and surgical conservatism dur<strong>in</strong>g surgery.Thyroid hypofunction associated with a myxedematousstate may mimic the baggy eyelids of dermatochalasisand should be ruled out. Incomplete recovery of a previousfacial nerve <strong>in</strong>sult may <strong>in</strong>terfere with eyelid closureand predispose a patient to dry eye syndrome.Risk Factors for Postoperative Bl<strong>in</strong>dnessPostoperative bl<strong>in</strong>dness, the most catastrophic complicationof blepharoplasty, is associated with retrobulbarhemorrhage. 8,9 Factors that <strong>in</strong>fluence bleed<strong>in</strong>g tendenciesshould therefore be identified and controlled beforesurgery. 10 Ingestion of aspir<strong>in</strong>, nonsteroidal anti<strong>in</strong>flammatorydrugs (NSAIDS), antiarthritics, cortisone preparations,and vitam<strong>in</strong> E should be withheld for at least14 days before surgery because of qualitative effects onplatelet function. Over-the-counter medications shouldbe discont<strong>in</strong>ued as well because g<strong>in</strong>gko biloba, for example,has been implicated <strong>in</strong> excessive bleed<strong>in</strong>g. Similarly,St. John’s wort is known to have hypertensive effectsthrough a monoam<strong>in</strong>e oxidase <strong>in</strong>hibitor mechanism.Warfar<strong>in</strong> compounds, if medically feasible, should bewithheld to normalize the prothromb<strong>in</strong> time and may bere<strong>in</strong>stituted 48 to 72 hours after surgery.Any history of abnormal or easy bruis<strong>in</strong>g, prolongedclott<strong>in</strong>g time, or family members with bleed<strong>in</strong>g dyscrasiashould be noted with appropriate coagulation profiles.Hypertensive patients should be medically stabilized atleast 2 weeks before surgery to ensure a nonfluctuat<strong>in</strong>gnormotensive state. Women have a greater bleed<strong>in</strong>g tendencydur<strong>in</strong>g their menstrual period than at other cycletimes, and this should be considered <strong>in</strong> plann<strong>in</strong>g surgery.Other important factors <strong>in</strong>clude dr<strong>in</strong>k<strong>in</strong>g and smok<strong>in</strong>ghistory, as the former (<strong>in</strong> large amounts) may <strong>in</strong>fluenceplatelet function, and the latter has been associated withdelayed wound heal<strong>in</strong>g and dim<strong>in</strong>ished flap viability.F<strong>in</strong>ally, any patient with a documented or suspected historyof glaucoma must be evaluated and managed by an
274 II Aesthetic <strong>Facial</strong> Surgeryophthalmologist to normalize <strong>in</strong>traocular pressures andguard aga<strong>in</strong>st a potential acute closed-angle attack priorto any eyelid surgery. Some facial <strong>plastic</strong> <strong>surgeon</strong>s recommenda rout<strong>in</strong>e ophthalmologic exam for all of theirpatients preoperatively.Ocular AssessmentExam<strong>in</strong>ation of the eyes should beg<strong>in</strong> with an overall<strong>in</strong>spection. The eyelid should be assessed for symmetry(by not<strong>in</strong>g palpebral fissure height and length),position of the lower eyelid marg<strong>in</strong> with respect tothe <strong>in</strong>ferior limbus, scleral show, and the presence ofectropion/entropion or exophthalmos/enophthalmos.Scars or sk<strong>in</strong> lesions should be noted because it may bepossible to <strong>in</strong>clude these <strong>in</strong> the resection. Areas of sk<strong>in</strong>discoloration or abnormal pigmentation should also benoted.Other basel<strong>in</strong>e features of the periorbital area should bepo<strong>in</strong>ted out to the patient, particularly <strong>in</strong> lieu of the <strong>in</strong>abilityof blepharoplasty to correct them. 11 The f<strong>in</strong>e wr<strong>in</strong>kl<strong>in</strong>gand "crepe paper" appearance of the eyelid sk<strong>in</strong> is notamenable to correction by blepharoplasty alone. Areasof abnormal pigmentation or discoloration (e.g., fromvenous stasis) will not be changed if outside the area ofsurgery and <strong>in</strong> fact may be more noticeable after surgery(because of light-refractile changes associated with conversionof a convex surface to a concave or flattened one).One of the greatest sources of dissatisfaction after lowerblepharoplasty is the persistence of malar bags. The patientshould realize that the upward tension necessary to attenuatesuch a soft tissue prom<strong>in</strong>ence would not be toleratedby the support<strong>in</strong>g structures of the lower lid and couldlead to ectropion. F<strong>in</strong>ally, lateral smile l<strong>in</strong>es (crow’s feet),despite the amount of lateral extension and underm<strong>in</strong><strong>in</strong>g,are also not amenable to correction by standard blepharoplastytechnique. All of these factors need to be discussedwith the patient.As a m<strong>in</strong>imum, basel<strong>in</strong>e ocular assessment shoulddocument visual acuity (i.e., best corrected vision if glassesor contact lenses are worn), extraocular movements, grossvisual fields by confrontation, corneal reflexes, the presenceof Bell’s phenomenon and lagophthalmos. If thereis any question of dry eye syndrome, the patient shouldbe evaluated with Schirmer test<strong>in</strong>g (to quantitate tearoutput) and tear film break-up times (to assess stabilityof precorneal tear film). 12 Patients who demonstrateabnormalities <strong>in</strong> either or both of these tests or who havepast or anatomical evidence that would predispose themto dry eye complications should be thoroughly evaluatedby an ophthalmologist preoperatively. Also, a conservativesk<strong>in</strong>–muscle excision (if not staged resection of upper andlower lids) would seem prudent.Assessment of Fat PocketsEvaluation of the adnexal structures should <strong>in</strong>cludeassessment of the fat pockets. Palpation of the <strong>in</strong>fraorbitalrim is an essential component of this exam<strong>in</strong>ation.A <strong>surgeon</strong> must recognize that a prom<strong>in</strong>ent rim limits theamount of orbital fat that can be removed without creat<strong>in</strong>gdisparities <strong>in</strong> confluence between the lower eyelid andthe anterior cheek. What appears to be an appropriatefat resection may contribute to a sunken-eye appearanceif the patient has a very prom<strong>in</strong>ent rim. Assessmentof the fat pockets may be facilitated by direct<strong>in</strong>g thepatient’s gaze <strong>in</strong> certa<strong>in</strong> directions; a superior gazeaccentuates the medial and central pockets, whereaslook<strong>in</strong>g upward and to the contralateral side accentuatesthe lateral pocket. Further confirmation of fatty prom<strong>in</strong>encemay be obta<strong>in</strong>ed by gentle retropulsion of theglobe with the eyelid closed and observation of theoutward movements of the respective fat pads.Assessment of Lid-Support<strong>in</strong>g StructuresBecause the most common cause of lower lid ectropionafter blepharoplasty is failure to recognize a lax lowerlid before surgery, it is essential to properly assess thelid-support<strong>in</strong>g structures. Two simple cl<strong>in</strong>ical tests aid <strong>in</strong>this evaluation. A lid distraction test (snap test) 13 is performedby gently grasp<strong>in</strong>g the midportion of the lowereyelid between the thumb and <strong>in</strong>dex f<strong>in</strong>gers and outwardlydisplac<strong>in</strong>g the eyelid from the globe (Fig. <strong>23</strong>.4).Movement of the lid marg<strong>in</strong> greater than 10 mm <strong>in</strong>dicatesan abnormally lax support<strong>in</strong>g lid structure and suggeststhe need for a lid-shorten<strong>in</strong>g procedure. The lid retractiontest 11 is used to assess lid tone as well as medial and lateralFig. <strong>23</strong>.4 Lid distraction test used to assess laxity of tarsoligamentoussl<strong>in</strong>g. (From Tenzel RR. Complications of blepharoplasty: orbital hematoma,ectropion, and scleral show. Cl<strong>in</strong> Plast Surg 1981;8:799.)
<strong>23</strong> <strong>Lower</strong> <strong>Eyelid</strong> <strong>Blepharoplasty</strong> 275Fig. <strong>23</strong>.5 Lid retraction test used to assess lower eyelid tone and stabilityof medial and lateral canthal tendon attachments. (From Tenzel RR.Complications of blepharoplasty: orbital hematoma, ectropion, andscleral show. Cl<strong>in</strong> Plast Surg 1981;8:800.)canthal tendon stability (Fig. <strong>23</strong>.5). By us<strong>in</strong>g the <strong>in</strong>dexf<strong>in</strong>ger to <strong>in</strong>feriorly displace the lower lid toward the orbitalrim, observations are made <strong>in</strong> terms of punctal or lateralcanthal malposition (movement of puncta greater than3 mm from the medial canthus <strong>in</strong>dicates an abnormallylax canthal tendon and suggests the need for tendoplication).Releas<strong>in</strong>g the eyelid, the pattern and rate of returnof the lid to rest<strong>in</strong>g position should be observed. A slowreturn, or one that requires multiple bl<strong>in</strong>ks, <strong>in</strong>dicates poorlid tone and eyelid support. Aga<strong>in</strong>, a conservative sk<strong>in</strong>–muscle resection and lower lid–shorten<strong>in</strong>g procedurewould be warranted.Surgical TechniqueThree basic surgical approaches have been described <strong>in</strong>lower lid blepharoplasty: (1) transconjunctival, (2) sk<strong>in</strong>–muscle flap, and (3) sk<strong>in</strong> flap.Transconjunctival ApproachThe transconjunctival approach to lower eyelid blepharoplastywas first described <strong>in</strong> 1924 by Bourquet. 14Although it is not a new procedure, over the past 10 yearsthere has been a surge of <strong>in</strong>terest and a growth of proponentsfor this approach. The transconjunctival lower lidblepharoplasty respects the <strong>in</strong>tegrity of the orbicularisoculi, an active support structure of the lower eyelid. Thism<strong>in</strong>imizes the <strong>in</strong>cidence of ectropion. Also, an externalscar can be avoided.Proper patient selection for the transconjunctivalapproach is required. Ideal candidates <strong>in</strong>clude olderpatients with pseudoherniation of orbital fat and a limitedamount of sk<strong>in</strong> excess, young patients with familial hereditarypseudoherniation of orbital fat and no excess sk<strong>in</strong>, allrevision blepharoplasty patients, patients who do not wantan external scar, patients with a history of keloids, anddark-sk<strong>in</strong>ned <strong>in</strong>dividuals who have a small possibility ofhypopigmentation of the external scar. 15,16 Because severalauthors have reported a significant reduction <strong>in</strong> short- andlong-term complications with the transconjunctivalapproach to lower eyelid blepharoplasty compared with thesk<strong>in</strong>–muscle method, the <strong>in</strong>dications for the technique havebeen gradually expand<strong>in</strong>g. 15,17 The presence of excess lowerlid sk<strong>in</strong> does not preclude use of the transconjunctivalapproach. In the senior author’s practice, the most commonlyperformed lower lid procedure consists of transconjunctivalfat excision, p<strong>in</strong>ch excision of sk<strong>in</strong>, and 35% trichloroaceticacid (TCA) peel<strong>in</strong>g (described later). 15,18–20 The sk<strong>in</strong> excisionis needed to recontour the lower eyelid once the fathas been removed. There frequently is less excess than one<strong>in</strong>itially estimates before the fat excision is performed. 17,21PreparationWhile sitt<strong>in</strong>g upright, the patient is asked to look upward.This helps to refresh the <strong>surgeon</strong>’s memory as to which fatpads are the most prom<strong>in</strong>ent, and these are marked. Thepatient is then placed sup<strong>in</strong>e. Two drops of ophthalmictetraca<strong>in</strong>e hydrochloride 0.5% are then <strong>in</strong>stilled <strong>in</strong>to each<strong>in</strong>ferior fornix. Prior to the local <strong>in</strong>jections, our patientstypically receive some <strong>in</strong>travenous sedation composedof midazolam (Versed) and meperid<strong>in</strong>e hydrochloride(Demerol). Ten milligrams of <strong>in</strong>travenous dexamethasone(Decadron) is also given to help m<strong>in</strong>imize postoperativeedema. A local anesthetic mixture, consist<strong>in</strong>gof equal parts of 0.25% bupivaca<strong>in</strong>e (Marca<strong>in</strong>e) and1% lidoca<strong>in</strong>e (Xyloca<strong>in</strong>e) with 1:100,000 ep<strong>in</strong>ephr<strong>in</strong>e towhich is added a 1:10 dilution of sodium bicarbonate,is then <strong>in</strong>jected <strong>in</strong>to the lower lid conjunctiva us<strong>in</strong>g a30 gauge needle. Experience has demonstrated that thismixture affords prolonged analgesic effect while m<strong>in</strong>imiz<strong>in</strong>gthe st<strong>in</strong>g of <strong>in</strong>itial <strong>in</strong>filtration through alkal<strong>in</strong>izationof the local agent. The needle is advanced through theconjunctiva until the bony orbital rim is palpated. The localis slowly <strong>in</strong>jected as the needle is withdrawn. This is performedmedially, centrally, and laterally. Several <strong>surgeon</strong>salso like to <strong>in</strong>ject transcutaneously, although we have
276 II Aesthetic <strong>Facial</strong> SurgeryFig. <strong>23</strong>.6 Transconjunctival approach to lower eyelid fat pockets.Simultaneous eversion of the lower eyelid and ballottement of theglobe produces a bulge of orbital fat that helps to guide the dissection.(From Baylis HI, Long JA, Groth MJ. Transconjunctival lowereyelid blepharoplasty: technique and complications. Ophthalmology1989;96:1027.)found that this is usually not necessary and may lead tounnecessary bruis<strong>in</strong>g.The upper lid is placed over the globe to protect it. Either aguarded needle-tip bovie on a low sett<strong>in</strong>g or a no. 15 bladeis used (others prefer a laser) to make the transconjunctival<strong>in</strong>cision 2 mm below the <strong>in</strong>ferior edge of the <strong>in</strong>ferior tarsalplate. This <strong>in</strong>ferior tarsal edge appears gray through theconjunctiva. The medial aspect of the <strong>in</strong>cision is <strong>in</strong> l<strong>in</strong>e withthe <strong>in</strong>ferior punctum. The <strong>in</strong>cision is carried just 4 to 5 mmshy of the lateral canthus.Immediately after the transconjunctival <strong>in</strong>cision ismade, a s<strong>in</strong>gle 5–0 nylon suture is placed <strong>in</strong> the conjunctivaclosest to the fornix and used to retract the posteriorlamella over the entire cornea (Fig. <strong>23</strong>.8). Mosquitossnapped onto the patient’s headwrap are used to hold thesutures under tension. The conjunctiva acts as a naturalcorneal protector and the superior retraction allows foreasier plane dissection. The two sk<strong>in</strong> hooks are then carefullyremoved and a Desmarres retractor is now used toevert the free edge of the lower lid (Fig. <strong>23</strong>.9).The distance of the transconjunctival <strong>in</strong>cision fromthe <strong>in</strong>ferior edge of the <strong>in</strong>ferior tarsal plate determ<strong>in</strong>eswhether one will approach the orbital fat preseptallyor postseptally. 16 We usually utilize the preseptal approach;therefore, our <strong>in</strong>cisions are always 2 mm below the tarsus.The preseptal plane is an avascular plane between theorbicularis oculi and the orbital septum. 22 Because the orbitalseptum is still <strong>in</strong>tact while the preseptal plane is be<strong>in</strong>gdeveloped, orbital fat does not bulge <strong>in</strong>to one’s view. Thevisualization obta<strong>in</strong>ed is closely similar to the orientationone is used to hav<strong>in</strong>g when perform<strong>in</strong>g a sk<strong>in</strong>–muscleQ1IncisionAfter wait<strong>in</strong>g a full 10 m<strong>in</strong>utes for vasoconstriction tooccur, the lower lid is gently retracted by an assistant us<strong>in</strong>gtwo small, double-pronged sk<strong>in</strong> hooks (Figs. <strong>23</strong>.6 and <strong>23</strong>.7).Fig. <strong>23</strong>.7 The needle-tip bovie is poised to <strong>in</strong>itiate the <strong>in</strong>cision. (A cornealprotector, or upper lid sk<strong>in</strong>, is used for protection when the actual <strong>in</strong>cisionis made.)Fig. <strong>23</strong>.8 Retraction suture <strong>in</strong> place; cotton-tipped applicator spreads<strong>in</strong>cision site.
<strong>23</strong> <strong>Lower</strong> <strong>Eyelid</strong> <strong>Blepharoplasty</strong> 277Fig. <strong>23</strong>.9 Desmarres retractor exposes orbital septum.flap blepharoplasty. The orbital septum will still have tobe opened to access the orbital fat below (Fig. <strong>23</strong>.10).Others prefer the postseptal approach to the orbitalfat. 19 To directly access the fat pads the conjunctiva is<strong>in</strong>cised 4 mm below the <strong>in</strong>ferior border of the <strong>in</strong>feriortarsal plate and directly toward the anterior edge of the<strong>in</strong>ferior orbital rim. The big advantage of this method is thatthe orbital septum is kept completely <strong>in</strong>tact. Proponentsfor this technique state that the <strong>in</strong>tact orbital septumadds to the support of the lower eyelid. One disadvantageis that the orbital fat immediately bulges <strong>in</strong>to one's view.Care must be taken not to <strong>in</strong>cise close to the conjunctivalcul-de-sac to avoid the risk of synechiae. 16 Also, the viewfrom the direct approach is one to which most facial <strong>plastic</strong><strong>surgeon</strong>s are less accustomed.After the 5–0 suture retraction and Desmarres retractorare <strong>in</strong> place, the preseptal plane is developed with a comb<strong>in</strong>ationof blunt dissection with a cotton swab and sharpdissection with scissors. It is mandatory to ma<strong>in</strong>ta<strong>in</strong> a drysurgical field. Therefore, a bipolar cautery, “hot loop,” ormonopolar cautery is used to cauterize any bleeders.The medial, central, and lateral fat pads are each <strong>in</strong>dividuallyidentified through the septum with the help ofsome gentle digital pressure on the conjunctiva cover<strong>in</strong>gthe globe. The orbital septum is then opened with scissors.Us<strong>in</strong>g forceps and a cotton-tipped applicator, the excess fatis carefully teased above the orbital rim and septum. Caremust be taken to remove only the excessive and herniatedfat because the eyes may take on a hollowed-out appearancefollow<strong>in</strong>g excessive fat excision. The ultimate goalis to achieve a lower eyelid contour that forms a smooth,gentle concave transition between it and cheek sk<strong>in</strong>.A 30 gauge needle is then used to <strong>in</strong>ject a small amountof local anesthetic <strong>in</strong>to the excess fat (Fig. <strong>23</strong>.11). The bipolarcautery is used to cauterize across the fat stalk. Whenone is sure the entire stalk has been cauterized, scissors areused to cut across the cauterized area. Others, notably Cook,reduce fat volume with electrocautery, m<strong>in</strong>imiz<strong>in</strong>g surgicalexcision. Many <strong>surgeon</strong>s feel that the lateral fat pocketshould be explored <strong>in</strong>itially because its volume contributionbecomes more difficult to assess after removal of its adjacentand <strong>in</strong>terconnected central fat pad. 11,<strong>23</strong> After excessfat has been removed from each compartment, the field isexam<strong>in</strong>ed to make sure there is no bleed<strong>in</strong>g. Although CO 2laser fat excision has been advocated based on the advantagesof hemostatic efficiency, precision, and reduced tissuetrauma, the <strong>in</strong>creased costs, requirements for highly tra<strong>in</strong>edpersonnel, and additional laser precautions have led us andothers to abandon laser <strong>in</strong>cisions for lower lid surgery. 24,25Fig. <strong>23</strong>.10 Fat appear<strong>in</strong>g through orbital septum.Fig. <strong>23</strong>.11 Fat of medial compartment, partially excised.
278 II Aesthetic <strong>Facial</strong> SurgeryThe Desmarres retractor should be removed periodicallyand the lower eyelid redraped over the fat thatrema<strong>in</strong>s <strong>in</strong> place to facilitate exam<strong>in</strong>ation of the contourof the eyelid. The fat that is removed is reta<strong>in</strong>ed on agauze on the surgical field <strong>in</strong> order from lateral to medial,allow<strong>in</strong>g for comparison with the fat removed from theopposite side. For example, if preoperatively the <strong>surgeon</strong>felt that the right lateral fat pad was much larger than allothers, then <strong>in</strong>traoperatively that compartment wouldhave the most fat removed.The medial and central fat compartments are separatedby the <strong>in</strong>ferior oblique muscle. This muscle mustbe clearly identified prior to the excision of excess fatfrom these compartments to prevent muscle <strong>in</strong>jury. Themedial fat pad is whiter than the central and lateral fatpads. This helps <strong>in</strong> its identification. The lateral compartmentis usually isolated from the central one by a fascialband off the <strong>in</strong>ferior oblique muscle. This fascial band canbe cut safely.After each successive fat compartment is treated, theentire field must aga<strong>in</strong> be exam<strong>in</strong>ed for bleed<strong>in</strong>g. Afterall of the bleed<strong>in</strong>g has been cauterized with the bipolar,the Desmarres and the retraction sutures are removed.The lower lid is gently elevated upward and outward andthen allowed to snap back <strong>in</strong>to its proper position. Thisallows for proper realignment of the edges of the transconjunctival<strong>in</strong>cision. No suture is required, althoughsome <strong>surgeon</strong>s feel more comfortable clos<strong>in</strong>g the <strong>in</strong>cisionwith one, buried 6–0 fast-absorb<strong>in</strong>g gut stitch. Both eyesshould then be irrigated with sodium chloride (ophthalmicBbalanced salt solution).In an older patient with sk<strong>in</strong> excess, a lower lid sk<strong>in</strong>p<strong>in</strong>ch or chemical peel may now be performed. Us<strong>in</strong>g fixationforceps or Brown–Adson forceps, a 2 to 3 mm raisedfold of redundant sk<strong>in</strong> is raised just below the ciliary marg<strong>in</strong>(Fig. <strong>23</strong>.12). The sk<strong>in</strong> fold is excised with sharp scissors,Fig. <strong>23</strong>.13 P<strong>in</strong>ch excision progression.with care taken not to cut the lower eyelashes (Fig. <strong>23</strong>.13).The edges of the sk<strong>in</strong> p<strong>in</strong>ch are then brought together with<strong>in</strong>terrupted 6–0 fast-absorb<strong>in</strong>g gut stitches. Several authorshave closed this <strong>in</strong>cision with cyanoacrylate (Histoacryl) orfibr<strong>in</strong> glue. 15,26Patients with crepey or f<strong>in</strong>e lower eyelid rhytids arethen treated with a 25 to 35% TCA peel. The TCA is appliedimmediately below the sk<strong>in</strong> p<strong>in</strong>ch <strong>in</strong>cision. A typical “frost”is generated (Fig. <strong>23</strong>.14). Phenol is not used for lowerlids <strong>in</strong> our hands because the erythema and <strong>in</strong>flammationphase is much longer than the TCA peel.Postoperative CareImmediately after surgery, the patient is kept quiet withhead elevated at least 45 degrees. Cold compresses areplaced on both eyes and changed every 20 m<strong>in</strong>utes. TheFig. <strong>23</strong>.12 Fixation forceps used to create ridge or mound for p<strong>in</strong>chexcision.Fig. <strong>23</strong>.14 Thirty percent trichloroacetic acid (TCA) lower lid peelfrost. (Different patient <strong>in</strong> whom no p<strong>in</strong>ch excision was done.) Whenthe p<strong>in</strong>ch technique is used, the TCA must not be applied any closerthan 1 mm below the suture l<strong>in</strong>e.
<strong>23</strong> <strong>Lower</strong> <strong>Eyelid</strong> <strong>Blepharoplasty</strong> 279patient is observed closely for at least an hour for anysigns of bleed<strong>in</strong>g complications. The patient is given strict<strong>in</strong>structions to limit physical activity for the next week.The patient who is diligent about the cold compressesand head elevation dur<strong>in</strong>g the first 48 hours will experiencesubstantially less swell<strong>in</strong>g. Some physicians placetheir patients on sulfacetamide ophthalmic drops dur<strong>in</strong>gthe first 5 postoperative days to help prevent an <strong>in</strong>fectionwhile the transconjunctival <strong>in</strong>cision is heal<strong>in</strong>g.Sk<strong>in</strong>–Muscle Flap ApproachThe sk<strong>in</strong>–muscle flap approach was perhaps the mostcommonly used method <strong>in</strong> the 1970s and early 1980s. Inpatients with a large amount of excess sk<strong>in</strong> and orbicularisoculi as well as fat pseudoherniation, this is an excellentprocedure. The advantages of this approach are related tothe safety and facility of dissect<strong>in</strong>g <strong>in</strong> the relatively avascularsubmuscular plane and the ability to remove redundantlower eyelid sk<strong>in</strong>. One must realize that even withthe sk<strong>in</strong>–muscle flap one is limited by how much sk<strong>in</strong>can safely be removed without risk<strong>in</strong>g scleral show andeven an ectropion. Persistent rhytids often rema<strong>in</strong> despiteattempts to safely resect redundant eyelid sk<strong>in</strong>.prepp<strong>in</strong>g and sterile drap<strong>in</strong>g, the <strong>in</strong>cision l<strong>in</strong>e (beg<strong>in</strong>n<strong>in</strong>glaterally) and entire lower lid down to the <strong>in</strong>fraorbitalrim are <strong>in</strong>filtrated (superficial to orbital septum) with ouranesthetic mixture previously described.IncisionThe <strong>in</strong>cision, which is begun medially with a no. 15 scalpelblade, is only through sk<strong>in</strong> to the level of the lateral canthus,but through sk<strong>in</strong> and musculus orbicularis oculi lateral tothis po<strong>in</strong>t. Us<strong>in</strong>g a blunt-tipped, straight-dissection scissors,the <strong>in</strong>cision is underm<strong>in</strong>ed <strong>in</strong> a submuscular plane fromlateral to medial and is then cut sharply by orientation ofthe blades <strong>in</strong> a caudal direction (optimiz<strong>in</strong>g the <strong>in</strong>tegrity ofthe pretarsal muscle sl<strong>in</strong>g). A Frost-type retention suture,us<strong>in</strong>g 5–0 nylon, is then placed through the tissue edge abovethe <strong>in</strong>cision to aid <strong>in</strong> counterretraction. Us<strong>in</strong>g blunt dissection(with scissors and cotton-tipped applicators), a sk<strong>in</strong>–muscle flap is developed down to, but not below, the<strong>in</strong>fraorbital rim to avoid disruption of important lymphaticchannels. 27 Any bleed<strong>in</strong>g po<strong>in</strong>ts up to this po<strong>in</strong>t shouldbe meticulously controlled with the handheld cautery orbipolar cautery, 28 with conservatism exercised <strong>in</strong> thesuperior marg<strong>in</strong> of the <strong>in</strong>cision to avert potential thermaltrauma to the eyelash follicles.PreparationPreparation for this method is similar to that for thetransconjunctival approach, except that tetraca<strong>in</strong>e dropsare not necessary. A subciliary <strong>in</strong>cision is planned 2 to3 mm beneath the eyelid marg<strong>in</strong> and is marked with amark<strong>in</strong>g pen or methylene blue with the patient <strong>in</strong> thesitt<strong>in</strong>g position. Any prom<strong>in</strong>ent fat pads are also marked.The importance of mark<strong>in</strong>g the patient <strong>in</strong> the uprightposition before <strong>in</strong>jection relates to the changes <strong>in</strong> softtissue relationships that occur as a result of dependencyand <strong>in</strong>filtration. The medial extent of the <strong>in</strong>cision is marked1 mm lateral to the <strong>in</strong>ferior punctum to avoid potentialdamage to the <strong>in</strong>ferior canaliculus, whereas the subciliaryextension is carried to a po<strong>in</strong>t 8 to 10 mm lateralto the lateral canthus (to m<strong>in</strong>imize potential for round<strong>in</strong>gof the canthal angle and lateral scleral show). At thispo<strong>in</strong>t, the lateral-most portion of the <strong>in</strong>cision achieves amore horizontal orientation and is planned to lie with<strong>in</strong>a crow’s-foot crease l<strong>in</strong>e. Care should be exercised <strong>in</strong>plann<strong>in</strong>g the lateral extension of this <strong>in</strong>cision to allow atleast 5 mm, and preferably 10 mm, between it and thelateral extension of the upper blepharoplasty <strong>in</strong>cision toobviate prolonged lymphedema.Our patients typically receive <strong>in</strong>travenous sedationcomposed of midazolam and meperid<strong>in</strong>e hydrochlorideafter the preoperative mark<strong>in</strong>g has been accomplishedand <strong>in</strong>travenous dexamethasone is <strong>in</strong>. Before surgicalFat RemovalIf preoperative assessment suggests the need for fat-padmanagement, selective open<strong>in</strong>gs are made through theorbital septum over the areas of pseudoherniation andare guided by gentle digital pressure of the closed eyelidaga<strong>in</strong>st the globe. Although alternatives aimed at electrocauteriz<strong>in</strong>ga weakened orbital septum exist 29 that mayobviate violation of this important barrier, we are comfortablewith the long-term results and predictability of ourtechnique of direct fat-pocket management.After open<strong>in</strong>g the septum (usually 5 to 6 mm above theorbital rim), the fat lobules are gently teased above theorbital rim and septum us<strong>in</strong>g forceps and a cotton-tippedapplicator. The fat resection technique is very much asdescribed <strong>in</strong> the transconjunctival technique and is notrepeated.Access to the medial compartment may be limited <strong>in</strong>part by the medial aspect of the subciliary <strong>in</strong>cision. This<strong>in</strong>cision should not be extended; <strong>in</strong>stead, the fat shouldbe gently teased <strong>in</strong>to the <strong>in</strong>cision, tak<strong>in</strong>g care to avoidthe <strong>in</strong>ferior oblique muscle. The medial fat pad is dist<strong>in</strong>guishedfrom the central pad by its lighter color.ClosureIn preparation for sk<strong>in</strong> excision and closure the patientis asked to open the jaw widely and gaze <strong>in</strong> a superior
280 II Aesthetic <strong>Facial</strong> Surgerydirection. This maneuver creates a maximal voluntaryseparation of the wound edges and assists the <strong>surgeon</strong><strong>in</strong> perform<strong>in</strong>g accurate resection of the sk<strong>in</strong>–muscle flap.With the patient ma<strong>in</strong>ta<strong>in</strong><strong>in</strong>g this position, the <strong>in</strong>feriorflap is redraped over the subciliary <strong>in</strong>cision <strong>in</strong> a superotemporaldirection. At the level of the lateral canthus,the extent of sk<strong>in</strong> muscle overlap is marked and <strong>in</strong>cisedvertically. A tack<strong>in</strong>g stitch of 5–0 fast absorb<strong>in</strong>g gut isthen placed to ma<strong>in</strong>ta<strong>in</strong> the position of the flap. Us<strong>in</strong>gstraight scissors, the areas of overlap are conservativelyresected (medial and lateral to the retention suture)so that edge-to-edge apposition can be ma<strong>in</strong>ta<strong>in</strong>ed withoutthe need for re<strong>in</strong>forcement. It is important to bevelthe blades caudally to allow for a 1 to 2 mm strip resectionof orbicularis oculi on the lower flap edge to avoida prom<strong>in</strong>ent ridge at the time of closure. Some <strong>surgeon</strong>srefrigerate the resected sk<strong>in</strong> (viable for at least48 hours) <strong>in</strong> sterile sal<strong>in</strong>e <strong>in</strong> case replacement tissuegraft is needed after an overzealous resection eventuat<strong>in</strong>g<strong>in</strong> ectropion. It is far better to prevent such complicationsby perform<strong>in</strong>g a conservative resection.After fat removal from the second eyelid, simple <strong>in</strong>terrupted6–0 fast-absorb<strong>in</strong>g gut sutures are placed to closethe <strong>in</strong>cision on the <strong>in</strong>itial eyelid. Attention can then beredirected back to redrap<strong>in</strong>g, trimm<strong>in</strong>g, and sutur<strong>in</strong>g the secondeyelid. F<strong>in</strong>ally, <strong>in</strong>ch-long sterile strips are placed to aid<strong>in</strong> temporal support, and a light application of antibiotico<strong>in</strong>tment is applied to the sutured <strong>in</strong>cision after irrigat<strong>in</strong>gthe eyes with sodium chloride (balanced salt solution).Postoperative CarePostoperative care after the sk<strong>in</strong>–muscle approach isessentially identical to the aftercare used <strong>in</strong> the transconjunctivalapproach. Bacitrac<strong>in</strong> ophthalmic o<strong>in</strong>tmentis given to the patient for the subciliary <strong>in</strong>cision. Icedsal<strong>in</strong>e compresses, head elevation, and limited activityare stressed to all patients.Sk<strong>in</strong> Flap ApproachThe sk<strong>in</strong> flap approach is perhaps the oldest and the leastfrequently used. This method allows <strong>in</strong>dependent resectionand redrap<strong>in</strong>g of lower eyelid sk<strong>in</strong> and underly<strong>in</strong>g orbicularisoculi and is effective <strong>in</strong> reposition<strong>in</strong>g and redrap<strong>in</strong>gexcessively wr<strong>in</strong>kled, redundant, or deeply creased sk<strong>in</strong>. 30In cases <strong>in</strong>volv<strong>in</strong>g hypertrophy or festoon<strong>in</strong>g of the orbicularisoculi, direct access is provided for management, whichallows for a greater and safer resection than wouldotherwise be tolerated if the flap were raised as a conjo<strong>in</strong>edmusculocutaneous unit. Disadvantages of this approach<strong>in</strong>clude a more tedious dissection that is associated withgreater sk<strong>in</strong> trauma (manifested by <strong>in</strong>creased bleed<strong>in</strong>gand eyelid <strong>in</strong>duration), an <strong>in</strong>creased risk of vertical eyelidretraction, and a higher demand placed on preoperativeassessment of the fat pockets because of obscured subseptalobservation by the overly<strong>in</strong>g orbicularis oculi. 31,32The <strong>in</strong>itial <strong>in</strong>cision through sk<strong>in</strong> is made only throughthe lateral extension of the subciliary mark<strong>in</strong>g to facilitateunderm<strong>in</strong><strong>in</strong>g. With an assistant ma<strong>in</strong>ta<strong>in</strong><strong>in</strong>g downwardtraction on the lower eyelid sk<strong>in</strong> (by plac<strong>in</strong>g a handnear the orbital rim), the lateral sk<strong>in</strong> edge is grasped andpulled superiorly while sharp-scissors dissection carefullyunderm<strong>in</strong>es the sk<strong>in</strong> flap to a po<strong>in</strong>t just below the orbitalrim. With the underm<strong>in</strong><strong>in</strong>g accomplished, the subciliary<strong>in</strong>cision is completed with the scissors. All bleed<strong>in</strong>g po<strong>in</strong>tsare precisely cauterized.If the problem is sk<strong>in</strong> redundancy or excessive wr<strong>in</strong>kl<strong>in</strong>gonly, the sk<strong>in</strong> flap is simply redraped <strong>in</strong> the mannerdescribed for sk<strong>in</strong>–muscle flap. If access to the orbital fatcompartments is required, these are approached by <strong>in</strong>cis<strong>in</strong>gthe orbicularis oculi 3 to 4 mm <strong>in</strong>ferior to the <strong>in</strong>itialsk<strong>in</strong> <strong>in</strong>cision or via the transconjunctival approach. However,when orbicularis hypertrophy or festoon<strong>in</strong>g is present,optimal management is achieved by development of<strong>in</strong>dependent sk<strong>in</strong> and muscle flaps. In this case, the muscleis <strong>in</strong>cised (bevel<strong>in</strong>g caudally) across the extent of the <strong>in</strong>cision,beg<strong>in</strong>n<strong>in</strong>g 2 mm below the sk<strong>in</strong> <strong>in</strong>cision to preservethe pretarsal muscle sl<strong>in</strong>g. Underm<strong>in</strong><strong>in</strong>g of the muscle flapis carried to just below the most dependent muscle roll(with festoon<strong>in</strong>g) or to a po<strong>in</strong>t that will allow effacementof a prom<strong>in</strong>ent muscle bulge (with hypertrophy) aftermuscle resection. After fat-pad management, the muscleflap is re<strong>in</strong>forced by sutur<strong>in</strong>g of its lateral end to orbitalperiosteum with 5–0 Vicryl (Ethicon, Inc., Somerville, NJ)and reapproximation of its pretarsal muscle edges with afew <strong>in</strong>terrupted 5–0 chromic sutures. Aga<strong>in</strong>, sk<strong>in</strong> closurefollows the pattern previously described.ComplicationsComplications after blepharoplasty are usually the result ofoverzealous sk<strong>in</strong> or fat resection, lack of hemostasis, or an<strong>in</strong>adequate preoperative assessment. 33,34 Less commonly,an <strong>in</strong>dividual’s physiological response to wound repairmay lead to undesirable sequelae despite execution of theproper technique. The goal <strong>in</strong> m<strong>in</strong>imiz<strong>in</strong>g complicationsconsequent to blepharoplasty must therefore focus on preventionby identify<strong>in</strong>g and manag<strong>in</strong>g known risk factors.EctropionOne of the most common complications after lower lidblepharoplasty is eyelid malposition, which may range<strong>in</strong> presentation from a mild scleral show or round<strong>in</strong>g of
<strong>23</strong> <strong>Lower</strong> <strong>Eyelid</strong> <strong>Blepharoplasty</strong> 281the lateral canthal angle, to a frank ectropion with actualeyelid eversion. In most cases result<strong>in</strong>g <strong>in</strong> permanentectropion, a failure to address excessive lower lid laxityis the etiologic culprit. Other causes <strong>in</strong>clude excessivesk<strong>in</strong> or sk<strong>in</strong>–muscle excisions, <strong>in</strong>ferior contracturealong the plane of the lower lid retractors and orbital septum(greater <strong>in</strong> sk<strong>in</strong> flap technique), <strong>in</strong>flammation of thefat pockets, and, rarely, destabilization of the lower lidretractors (a potential yet uncommon complication of thetransconjunctival approach). Temporary ectropion hasbeen associated with lid load<strong>in</strong>g from reactionary edemaor hematoma and muscle hypotonicity.A conservative approach to management may <strong>in</strong>cludethe follow<strong>in</strong>g: (1) a short course of perioperative steroidswith cold compresses and head elevation to manageedema; (2) warm and cool compresses alternated tohasten resolution of m<strong>in</strong>or established hematomas andimprove circulatory status; (3) repeated squ<strong>in</strong>t<strong>in</strong>g exercisesto improve muscle tonus; (4) gentle massage <strong>in</strong> anupward direction; and (5) supportive tap<strong>in</strong>g of the lowerlid (upward and outward) to assist <strong>in</strong> corneal protectionand tear collection.When sk<strong>in</strong> excisions are recognized to be excessivewith<strong>in</strong> the first 48 hours, the banked eyelid sk<strong>in</strong> shouldbe used as a replacement graft. If recognition is delayed,conservative measures to protect the eye should be usedto allow the scar to mature and a full-thickness graft (preferablyupper eyelid sk<strong>in</strong> or, alternatively, postauricularsk<strong>in</strong>, or foresk<strong>in</strong> <strong>in</strong> males) used to replace the deficit. Inmany cases, a lid-shorten<strong>in</strong>g procedure is comb<strong>in</strong>ed withthe tissue graft<strong>in</strong>g and is the ma<strong>in</strong>stay of treatment whenan atonic lid is present. Management of persistent <strong>in</strong>durations,result<strong>in</strong>g from hematoma formation or <strong>in</strong>flammatoryresponses of the fat pockets, generally <strong>in</strong>volves directdepot <strong>in</strong>jections of corticosteroid.HematomasCollections of blood beneath the sk<strong>in</strong> surface can usuallybe m<strong>in</strong>imized before surgery by optimiz<strong>in</strong>g coagulationprofiles and normotensive status dur<strong>in</strong>g surgery throughdelicate tissue handl<strong>in</strong>g and meticulous hemostasis andafter surgery through head elevation, cold compress<strong>in</strong>g, acontrolled level of activity, and appropriate analgesic support.Should a hematoma develop, its extent and time ofpresentation will guide management.Small, superficial hematomas are relatively commonand are typically self-limit<strong>in</strong>g. If organization occurs withthe development of an <strong>in</strong>durated mass and resolution isslow or nonprogressive, conservative steroid <strong>in</strong>jectionsmay be used to hasten the heal<strong>in</strong>g process. Moderate orlarge hematomas recognized after several days are bestmanaged by allow<strong>in</strong>g the clot to liquify (7 to 10 days) andthen evacuat<strong>in</strong>g the hematoma through large-bore needleaspiration or by creat<strong>in</strong>g a small stab wound over it with ano. 11 blade. Hematomas that are large and present early,that are expand<strong>in</strong>g, or that represent symptomatic retrobulbarextension (decrease <strong>in</strong> visual acuity, proptosis, ocularpa<strong>in</strong>, ophthalmoplegia, progressive chemosis) demandimmediate exploration and hemostatic control. In thecase of the latter, urgent ophthalmologic consultation andorbital decompression are the ma<strong>in</strong>stays of treatment.Bl<strong>in</strong>dnessBl<strong>in</strong>dness, though rare, is the most feared potential complicationof blepharoplasty. It occurs with an <strong>in</strong>cidence of0.04%, 35 typically presents itself with<strong>in</strong> the first 24 hoursafter surgery, and is associated with orbital fat removal andthe development of a retrobulbar hematoma (medial fatpocket most commonly <strong>in</strong>volved). Commonly implicatedcauses of retrobulbar hemorrhage <strong>in</strong>clude the follow<strong>in</strong>g:(1) excessive traction on orbital fat result<strong>in</strong>g <strong>in</strong> disruptionof small arterioles or venules <strong>in</strong> the posterior orbit; (2)retraction of an open vessel beneath the septum after fatrelease; (3) failure to recognize an open vessel because ofvasospasm or ep<strong>in</strong>ephr<strong>in</strong>e effect; (4) direct vessel traumaresult<strong>in</strong>g from <strong>in</strong>jections done bl<strong>in</strong>dly beneath the orbitalseptum; and (5) rebleed<strong>in</strong>g after closure result<strong>in</strong>g from anymaneuver or event that leads to an <strong>in</strong>creased ophthalmicarteriovenous pressure head.Early recognition of a develop<strong>in</strong>g orbital hematoma canbe facilitated by delay<strong>in</strong>g <strong>in</strong>traoperative closure (first side),avoid<strong>in</strong>g occlusive-pressure eye dress<strong>in</strong>gs, and extend<strong>in</strong>gthe postoperative observational period. Although manymethods of management have been described to managethreatened vision result<strong>in</strong>g from elevated <strong>in</strong>traocular pressures(reopen<strong>in</strong>g the wound, lateral canthotomy, steroids,diuretics, anterior chamber paracentesis), the most effectivedef<strong>in</strong>itive treatment is immediate orbital decompression,which is usually accomplished through medial walland orbital floor resections. 8,36 Certa<strong>in</strong>ly, ophthalmologicconsultation is advisable.EpiphoraAssum<strong>in</strong>g dry eye syndrome was ruled out before surgeryor managed appropriately <strong>in</strong>traoperatively (conservativeand staged resections), a dysfunctional lacrimal collect<strong>in</strong>gsystem rather than a high glandular output state istypically responsible for postoperative epiphora (althoughreflex hypersection may be a contribut<strong>in</strong>g factor becauseof coexistent lagophthalmos or vertical retraction ofthe lower lid). This response is common <strong>in</strong> the early postoperativeperiod and is usually self-limited. Causes <strong>in</strong>clude thefollow<strong>in</strong>g: (1) punctal eversion and canalicular distortionsecondary to wound retraction and edema; (2) impairment
282 II Aesthetic <strong>Facial</strong> Surgeryof the lacrimal pump result<strong>in</strong>g from atony, edema,hematoma, or partial resection of the orbicularis oculi sl<strong>in</strong>g;and (3) a temporary ectropion result<strong>in</strong>g from lid load<strong>in</strong>g.Outflow obstructions, secondary to a lacerated <strong>in</strong>feriorcanaliculus, are preventable by keep<strong>in</strong>g the lower lid <strong>in</strong>cisionlateral to the punctum. Should laceration <strong>in</strong>jury occur,primary repair over a Silastic stent (Crawford tube; DowCorn<strong>in</strong>g, Midland, MI) is recommended. Persistent punctaleversion can be managed by cauterization or diamond excisionof the conjunctival surface below the canaliculus.Suture L<strong>in</strong>e ComplicationsMilia or <strong>in</strong>clusion cysts are common lesions seen alongthe <strong>in</strong>cisional l<strong>in</strong>e result<strong>in</strong>g from trapped epithelial debrisbeneath a healed sk<strong>in</strong> surface or possibly from the occlusionof a glandular duct. They are typically associated withsimple or runn<strong>in</strong>g cuticular stitches. Their formation ism<strong>in</strong>imized by subcuticular closure. If they develop, def<strong>in</strong>itivetherapy is aimed at uncapp<strong>in</strong>g the cyst (no. 11 bladeor epilation needle) and teas<strong>in</strong>g out the sac. Granulomasmay develop as nodular thicken<strong>in</strong>gs with<strong>in</strong> or beneaththe suture l<strong>in</strong>e and are typically treated by steroid <strong>in</strong>jectionsif small and by direct excision if large. Suture tunnelsdevelop as a result of prolonged suture retention and epithelialsurface migration along the suture tract. Preventivetreatment <strong>in</strong>cludes early suture removal (3 to 5 days), anddef<strong>in</strong>itive treatment <strong>in</strong>volves unroof<strong>in</strong>g the tunnel. Suturemarks are also related to prolonged suture retention andtheir formation can usually be avoided by us<strong>in</strong>g a rapidlyabsorb<strong>in</strong>g suture (fast-absorb<strong>in</strong>g gut or mild chromic), byremov<strong>in</strong>g a monofilament suture early, or by employ<strong>in</strong>g asubcuticular closure.Wound Heal<strong>in</strong>g ComplicationsAlthough rare, hypertrophic or prom<strong>in</strong>ent lower eyelidscars may develop because of improper placement ofthe lower lid <strong>in</strong>cision. If extended too far medially <strong>in</strong> theepicanthal region, bow-str<strong>in</strong>g or web formation mayoccur (conditions usually amenable to correction byZ-plasty technique). A lateral canthal extension (whichnormally overlies a bony prom<strong>in</strong>ence) that is orientedtoo obliquely downward or is closed under excessivetension predisposes an <strong>in</strong>cision to hypertrophic scarr<strong>in</strong>g,and dur<strong>in</strong>g heal<strong>in</strong>g the vertical contraction vectors act onthe lateral lid to favor scleral show or eversion. If the lowerlid <strong>in</strong>cision is oriented too far superiorly or too close tothe lateral aspect of the upper lid <strong>in</strong>cision, the forces ofcontraction (now favor<strong>in</strong>g a downward pull) provideconditions that predispose the patient to lateral canthalhood<strong>in</strong>g. Aga<strong>in</strong>, proper treatment should be aimed atreorient<strong>in</strong>g the direction of contract<strong>in</strong>g vectors.Wound dehiscence may develop as a result of closureunder excessive tension, early removal of sutures, extensionof an <strong>in</strong>fectious process (unusual), or hematoma(more commonly). Sk<strong>in</strong> separation is seen most often <strong>in</strong>the lateral aspect of the <strong>in</strong>cision with the sk<strong>in</strong>–muscle andsk<strong>in</strong> techniques, and treatment is directed to supportivetap<strong>in</strong>g or resutur<strong>in</strong>g. If tension is too great for conservativemanagement, then a lid suspension technique and lateralgraft<strong>in</strong>g should be considered. Sk<strong>in</strong> slough may developas a result of devascularization of the sk<strong>in</strong> segment. It isalmost exclusively seen <strong>in</strong> the sk<strong>in</strong>-only technique andtypically occurs <strong>in</strong> the lateral portion of the lower eyelidafter wide underm<strong>in</strong><strong>in</strong>g and subsequent hematoma formation.Treatment consists of local wound care, evacuation ofany hematomas, establishment of a l<strong>in</strong>e of demarcation,and early sk<strong>in</strong> replacement to obviate scar contracture ofthe lower lid.Sk<strong>in</strong> DiscolorationAreas of sk<strong>in</strong> underm<strong>in</strong><strong>in</strong>g are frequently evident ashyperpigmentation <strong>in</strong> the early recovery period secondaryto bleed<strong>in</strong>g beneath the sk<strong>in</strong> surface with subsequenthemosider<strong>in</strong> formation. This process is usually self-limit<strong>in</strong>gand often takes longer to resolve <strong>in</strong> darkly pigmented<strong>in</strong>dividuals. It is imperative dur<strong>in</strong>g the heal<strong>in</strong>g process, andparticularly <strong>in</strong> this patient population, to avoid direct sunlightbecause this may lead to permanent pigment changes.Refractory cases (after 6 to 8 weeks) may be considered forcamouflage, periorbital peel<strong>in</strong>g, or depigmentation therapy(e.g., hydroxyqu<strong>in</strong>one, kojic acid). Telangiectasias maydevelop after sk<strong>in</strong> underm<strong>in</strong><strong>in</strong>g, particularly <strong>in</strong> areasbeneath or near the <strong>in</strong>cision, and most commonly occur<strong>in</strong> patients with preexist<strong>in</strong>g telangiectasias. Treatmentoptions may <strong>in</strong>clude chemical peel<strong>in</strong>g or dye laser ablation.Ocular InjuryCorneal abrasions or ulcerations may result from <strong>in</strong>advertentrubb<strong>in</strong>g of the corneal surface with a gauze sponge orcotton applicator, <strong>in</strong>strument or suture mishandl<strong>in</strong>g,or desiccation develop<strong>in</strong>g as a result of lagophthalmos,ectropion, or preexistent dry eye syndrome. Symptomssuggestive of corneal <strong>in</strong>jury, which <strong>in</strong>clude pa<strong>in</strong>, eyeirritation, and blurred vision, should be confirmed by fluoresce<strong>in</strong>sta<strong>in</strong><strong>in</strong>g and slitlamp exam<strong>in</strong>ation by an ophthalmologist.Therapy for mechanical <strong>in</strong>jury typically <strong>in</strong>volvesuse of an antibiotic ophthalmic drop with lid closureuntil epithelialization is complete (usually 24 to 48 hours).Treatment for dry eye syndrome <strong>in</strong>cludes the addition ofocular lubricants, such as Liquitears and Lacri-lube.Extraocular muscle imbalance, manifested by gazediplopia, may be seen and is often transitory, presumably
<strong>23</strong> <strong>Lower</strong> <strong>Eyelid</strong> <strong>Blepharoplasty</strong> 283reflect<strong>in</strong>g resolution of an edematous process. However,permanent muscle <strong>in</strong>jury may result from bl<strong>in</strong>d clamp<strong>in</strong>g,deep penetration of the fat pockets dur<strong>in</strong>g section<strong>in</strong>g ofthe pedicle, thermal <strong>in</strong>jury result<strong>in</strong>g from electrocauterization,suture <strong>in</strong>corporation dur<strong>in</strong>g closure, or ischemiccontracture of the Volkman type. Patients with evidenceof refractory and <strong>in</strong>complete recovery of muscle functionshould be referred to an ophthalmologist for evaluationand def<strong>in</strong>itive treatment.Contour IrregularitiesContour irregularities are generally caused by technicalomissions. Overzealous fat resection, particularly <strong>in</strong> apatient with a prom<strong>in</strong>ent <strong>in</strong>fraorbital rim, results <strong>in</strong>a lower lid concavity and contributes to a sunken-eyeappearance. Failure to remove enough fat (common <strong>in</strong>lateral pocket) leads to surface irregularities and persistentbulges. A ridge that persists beneath the <strong>in</strong>cision l<strong>in</strong>eis usually the result of <strong>in</strong>adequate resection of a strip oforbicularis oculi before redrap<strong>in</strong>g. Areas of <strong>in</strong>durationor lump<strong>in</strong>ess below the suture l<strong>in</strong>e usually can beattributed to unresolved or organized hematoma, tissuereaction or fibrosis secondary to electrocauterization orthermal <strong>in</strong>jury, or soft tissue response to fat necrosis.Treatment <strong>in</strong> each case is directed at the specific cause.Persistent fat bulges are managed by resection, whereasareas of lid depression can be managed by slid<strong>in</strong>g fatpadgrafts, free-fat or dermal fat grafts, 37 or orbicularisoculi flap reposition<strong>in</strong>g. Some patients with such bulgesor prom<strong>in</strong>ences respond to direct <strong>in</strong>jections of triamc<strong>in</strong>ol<strong>in</strong>e(40 mg/cm 3 ). In selected cases, <strong>in</strong>fraorbital rimreductions distract noticeability from a hollow-eyeappearance and may be used as an adjunctive technique.Unresolved hematomas and areas of heightened <strong>in</strong>flammatoryresponse may be managed with conservative<strong>in</strong>jections of steroids.References1. Zide BM. Anatomy of the eyelids. Cl<strong>in</strong> Plast Surg 1981;8:6<strong>23</strong>2. Aguilar GL, Nelson C. <strong>Eyelid</strong> and anterior orbital anatomy. In: HornblassA, ed. Oculo<strong>plastic</strong>, Orbital and Reconstructive Surgery. Vol. 1: <strong>Eyelid</strong>s.Baltimore: Williams & Wilk<strong>in</strong>s; 19883. Jones LT. New concepts of orbital anatomy. In: Tessier P, Callahan A,Mustarde JC, et al, eds. Symposium on Plastic Surgery <strong>in</strong> the OrbitalRegion. St Louis: CV Mosby; 19764. Doxanas MT. <strong>Blepharoplasty</strong>: key anatomical concepts. <strong>Facial</strong> PlastSurg 1984;1:2595. Nesi F, Lisman R, Lev<strong>in</strong>e M. Smith’s Ophthalmic Plastic and ReconstructiveSurgery. 2nd ed. St. Louis: CV Mosby; 1998:1–786. Rees TD, Jelks GW. <strong>Blepharoplasty</strong> and the dry eye syndrome: guidel<strong>in</strong>esfor surgery? Plast Reconstr Surg 1981;68:2497. Jelks GW, McCord CD. Dry eye syndrome and other tear film abnormalities.Cl<strong>in</strong> Plast Surg 1981;8:8038. Sacks SH, Lawson W, Edelste<strong>in</strong> D, et al. Surgical treatment of bl<strong>in</strong>dnesssecondary to <strong>in</strong>traorbital hemorrhage. Arch Otolaryngol Head NeckSurg 1988;114:8019. Mahaffey PJ, Wallace AF. Bl<strong>in</strong>dness follow<strong>in</strong>g cosmetic blepharoplasty:a review. Br J Plast Surg 1986;39:21310. Callahan MA. Prevention of bl<strong>in</strong>dness after blepharoplasty. Ophthalmology1983;90:1047–105111. Beekhuis GJ. <strong>Blepharoplasty</strong>. Otolaryngol Cl<strong>in</strong> North Am 1982;15:17912. McK<strong>in</strong>ney P, Zukowski ML. The value of tear film breakup and schirmer’stests <strong>in</strong> preoperative blepharoplasty evaluation. Plast ReconstrSurg 1989;84:57213. Holt JE, Holt GR. <strong>Blepharoplasty</strong>: <strong>in</strong>dications and preoperative assessment.Arch Otolaryngol 1985;111:39414. Bourquet J. Les hernies graisseuses de l’orbite: notre traitment chirurgical.Bull Acad Natl Med 1924;92:1270–127215. Perk<strong>in</strong>s SW, Dyer WD II, Simo F. Transconjunctival approach to lowereyelid blepharoplasty. Arch Otolaryngol Head Neck Surg 1994;120:172–17716. Mahe E. <strong>Lower</strong> lid blepharoplasty: the transconjunctival approach:extended <strong>in</strong>dications. Aesthetic Plast Surg 1998;22:1–817. Zarem HA, Resnick JI. M<strong>in</strong>imiz<strong>in</strong>g deformity <strong>in</strong> lower blepharopasty:the transconjuctival approach. Plast Reconstr Surg 1991;88:21518. McK<strong>in</strong>ney P, Zukowshi ML, Mossie R. The 4th option: a novelapproach to lower lid blepharoplasty. Aesthetic Plast Surg 1991;15:293–29619. Baylis HI, Long JA, Groth MJ. Transconjunctival lower eyelid blepharoplasty.Ophthalmology 1989;96:102720. Cheney ML. <strong>Facial</strong> Surgery: Plastic and Reconstructive. Baltimore:Williams & Wilk<strong>in</strong>s; 1987:895–90421. Netscher DT, Patr<strong>in</strong>ely JR, Peltier M, et al. Transconjunctival versustranscutaneous lower eyelid blepharoplasty: a prospective study. PlastReconstr Surg 1995;96:1053–105922. Tessier P. The conjunctival approach to the orbital floor and maxilla <strong>in</strong>congenital malformation and trauma. J Maxillofac Surg 1973;1:3–8<strong>23</strong>. Spira M. <strong>Blepharoplasty</strong>. Cl<strong>in</strong> Plast Surg 1978;5:12124. David LM. The laser approach to blepharoplasty. J Dermatol SurgOncol 1988;14:74125. Mele JA III, Kulick MI, Lee D. Laser blepharoplasty: is it safe? AestheticPlast Surg 1998;22:9–1126. Mommaerts MY, Beirne JC, Jacobs WI, Abeloos JSV. Use of fibr<strong>in</strong> glue <strong>in</strong>lower blepharoplasties. J Craniomaxillofac Surg 1996;24:78–8227. Holt JE, Holt GR, Cortez EA. <strong>Blepharoplasty</strong>. Ear Nose Throat J1981;60:4228. Rob<strong>in</strong>son L, Crumley RL. Electrocoagulation <strong>in</strong> blepharoplasty: experimentaldata <strong>in</strong> the rabbit, 1990; unpublished.29. Cook TA, Dereberry J, Harrah ER. Reconsideration of fat pad management<strong>in</strong> lower lid blepharoplasty surgery. Arch Otolaryngol1984;110:52130. Klatsky SA, Manson PN. Separate sk<strong>in</strong> and muscle flaps <strong>in</strong> lower lidblepharoplasty. Plast Reconstr Surg 1981;67:15131. Wolfey DE. <strong>Blepharoplasty</strong>: the ophthalmologist’s view. OtolaryngolCl<strong>in</strong> North Am 1980;13:<strong>23</strong>732. McCollough EG, English JL. <strong>Blepharoplasty</strong>: avoid<strong>in</strong>g <strong>plastic</strong> eyelids.Arch Otolaryngol Head Neck Surg 1988;114:64533. Adams BJS, Feurste<strong>in</strong> SS. Complications of blepharoplasty. Ear NoseThroat J 1986;65(1):11–2834. Castanares S. Complications <strong>in</strong> blepharoplasty. Cl<strong>in</strong> Plast Surg1978;5:14935. Moser MH, DiPirro E, MaCoy FJ. Sudden bl<strong>in</strong>dness follow<strong>in</strong>g blepharoplasty:report of seven cases. Plast Reconstr Surg 1973;51:36336. Anderson RL, Edwards JJ. Bilateral visual loss after blepharoplasty.Ann Plast Surg 1980;5:28837. Loeb R. Fat pad slid<strong>in</strong>g and fat graft<strong>in</strong>g for level<strong>in</strong>g lid depressions. Cl<strong>in</strong>Plast Surg 1981;8:757Q2
Author QueryQ1: AU: Mosquito clips? unclear.Q2: AU: Ref 28: unpublished material can not be listed <strong>in</strong> the references. It must be cited <strong>in</strong> text <strong>in</strong> parens, such as: (Rob<strong>in</strong>sonL, Crumley RL, unpublished data, 1990). Please move citation to text. Can you provide a substitute reference for Ref28? If no, delete ref number from text and list and re-number go<strong>in</strong>g forward <strong>in</strong> text and <strong>in</strong> ref list.