082098 Staphylococcus aureus Infections - Goodsamim.com
082098 Staphylococcus aureus Infections - Goodsamim.com
082098 Staphylococcus aureus Infections - Goodsamim.com
You also want an ePaper? Increase the reach of your titles
YUMPU automatically turns print PDFs into web optimized ePapers that Google loves.
MEDICAL PROGRESS<br />
No. of <strong>Infections</strong><br />
3000<br />
2000<br />
1000<br />
0<br />
1987<br />
No. of infections<br />
Percent of infections resistant to methicillin<br />
Percent of methicillin-resistant infections<br />
sensitive only to van<strong>com</strong>ycin<br />
1988<br />
1989<br />
1990<br />
1991<br />
1992<br />
Year<br />
1993<br />
1994<br />
1995<br />
1996<br />
1997<br />
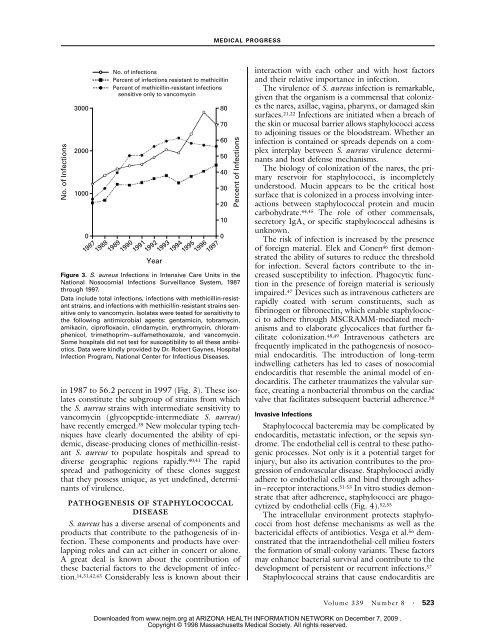
Figure 3. S. <strong>aureus</strong> <strong>Infections</strong> in Intensive Care Units in the<br />
National Noso<strong>com</strong>ial <strong>Infections</strong> Surveillance System, 1987<br />
through 1997.<br />
Data include total infections, infections with methicillin-resistant<br />
strains, and infections with methicillin-resistant strains sensitive<br />
only to van<strong>com</strong>ycin. Isolates were tested for sensitivity to<br />
the following antimicrobial agents: gentamicin, tobramycin,<br />
amikacin, ciprofloxacin, clindamycin, erythromycin, chloramphenicol,<br />
trimethoprim–sulfamethoxazole, and van<strong>com</strong>ycin.<br />
Some hospitals did not test for susceptibility to all these antibiotics.<br />
Data were kindly provided by Dr. Robert Gaynes, Hospital<br />
Infection Program, National Center for Infectious Diseases.<br />
in 1987 to 56.2 percent in 1997 (Fig. 3). These isolates<br />
constitute the subgroup of strains from which<br />
the S. <strong>aureus</strong> strains with intermediate sensitivity to<br />
van<strong>com</strong>ycin (glycopeptide-intermediate S. <strong>aureus</strong>)<br />
have recently emerged. 39 New molecular typing techniques<br />
have clearly documented the ability of epidemic,<br />
disease-producing clones of methicillin-resistant<br />
S. <strong>aureus</strong> to populate hospitals and spread to<br />
diverse geographic regions rapidly. 40,41 The rapid<br />
spread and pathogenicity of these clones suggest<br />
that they possess unique, as yet undefined, determinants<br />
of virulence.<br />
PATHOGENESIS OF STAPHYLOCOCCAL<br />
DISEASE<br />
S. <strong>aureus</strong> has a diverse arsenal of <strong>com</strong>ponents and<br />
products that contribute to the pathogenesis of infection.<br />
These <strong>com</strong>ponents and products have overlapping<br />
roles and can act either in concert or alone.<br />
A great deal is known about the contribution of<br />
these bacterial factors to the development of infection.<br />
14,31,42,43 Considerably less is known about their<br />
80<br />
70<br />
60<br />
50<br />
40<br />
30<br />
20<br />
10<br />
0<br />
Percent of <strong>Infections</strong><br />
interaction with each other and with host factors<br />
and their relative importance in infection.<br />
The virulence of S. <strong>aureus</strong> infection is remarkable,<br />
given that the organism is a <strong>com</strong>mensal that colonizes<br />
the nares, axillae, vagina, pharynx, or damaged skin<br />
surfaces. 21,22 <strong>Infections</strong> are initiated when a breach of<br />
the skin or mucosal barrier allows staphylococci access<br />
to adjoining tissues or the bloodstream. Whether an<br />
infection is contained or spreads depends on a <strong>com</strong>plex<br />
interplay between S. <strong>aureus</strong> virulence determinants<br />
and host defense mechanisms.<br />
The biology of colonization of the nares, the primary<br />
reservoir for staphylococci, is in<strong>com</strong>pletely<br />
understood. Mucin appears to be the critical host<br />
surface that is colonized in a process involving interactions<br />
between staphylococcal protein and mucin<br />
carbohydrate. 44,45 The role of other <strong>com</strong>mensals,<br />
secretory IgA, or specific staphylococcal adhesins is<br />
unknown.<br />
The risk of infection is increased by the presence<br />
of foreign material. Elek and Conen 46 first demonstrated<br />
the ability of sutures to reduce the threshold<br />
for infection. Several factors contribute to the increased<br />
susceptibility to infection. Phagocytic function<br />
in the presence of foreign material is seriously<br />
impaired. 47 Devices such as intravenous catheters are<br />
rapidly coated with serum constituents, such as<br />
fibrinogen or fibronectin, which enable staphylococci<br />
to adhere through MSCRAMM-mediated mechanisms<br />
and to elaborate glycocalices that further facilitate<br />
colonization. 48,49 Intravenous catheters are<br />
frequently implicated in the pathogenesis of noso<strong>com</strong>ial<br />
endocarditis. The introduction of long-term<br />
indwelling catheters has led to cases of noso<strong>com</strong>ial<br />
endocarditis that resemble the animal model of endocarditis.<br />
The catheter traumatizes the valvular surface,<br />
creating a nonbacterial thrombus on the cardiac<br />
valve that facilitates subsequent bacterial adherence. 50<br />
Invasive <strong>Infections</strong><br />
Staphylococcal bacteremia may be <strong>com</strong>plicated by<br />
endocarditis, metastatic infection, or the sepsis syndrome.<br />
The endothelial cell is central to these pathogenic<br />
processes. Not only is it a potential target for<br />
injury, but also its activation contributes to the progression<br />
of endovascular disease. Staphylococci avidly<br />
adhere to endothelial cells and bind through adhesin–receptor<br />
interactions. 51-53 In vitro studies demonstrate<br />
that after adherence, staphylococci are phagocytized<br />
by endothelial cells (Fig. 4). 52,55<br />
The intracellular environment protects staphylococci<br />
from host defense mechanisms as well as the<br />
bactericidal effects of antibiotics. Vesga et al. 56 demonstrated<br />
that the intraendothelial-cell milieu fosters<br />
the formation of small-colony variants. These factors<br />
may enhance bacterial survival and contribute to the<br />
development of persistent or recurrent infections. 57<br />
Staphylococcal strains that cause endocarditis are<br />
Volume 339 Number 8 · 523<br />
Downloaded from www.nejm.org at ARIZONA HEALTH INFORMATION NETWORK on December 7, 2009 .<br />
Copyright © 1998 Massachusetts Medical Society. All rights reserved.