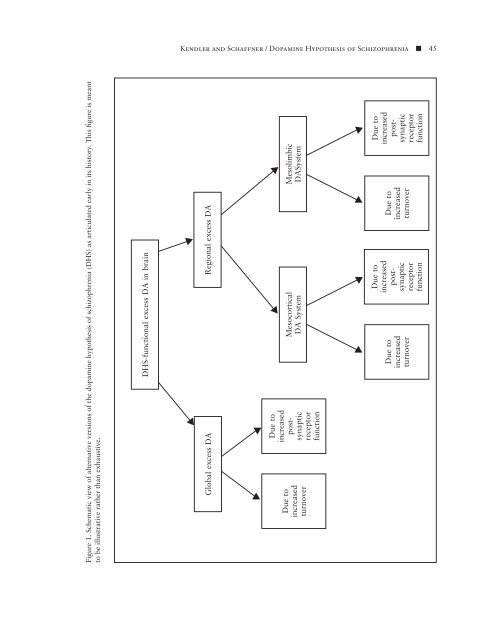
Kendler <strong>and</strong> Schaffner / <strong>Dopamine</strong> <strong>Hypothesis</strong> <strong>of</strong> <strong>Schizophrenia</strong> ■ 45 Figure 1. Schematic view <strong>of</strong> alternative versions <strong>of</strong> the dopamine hypothesis <strong>of</strong> schizophrenia (DHS) as articulated early in its history. This figure is meant to be illustrative rather than exhaustive. DHS-functional excess DA in brain Regional excess DA Global excess DA Mesolimbic DASystem Mesocortical DA System Due to increased postsynaptic receptor function Due to increased turnover Due to increased postsynaptic receptor function Due to increased turnover Due to increased postsynaptic receptor function Due to increased turnover
46 ■ PPP / Vol. 18, No. 1 / March 2011 perspective. <strong>The</strong> last two areas are, by contrast, quite active foci <strong>of</strong> on-going research <strong>and</strong> therefore cannot be definitively summarized at this time. CSF Studies <strong>The</strong> first empirical method widely used to test the DHS was an examination <strong>of</strong> the key DA metabolite in humans—homovanillic acid (HVA)—in the CSF <strong>of</strong> schizophrenic versus control patients. If, as predicted by the DHS, DA systems in the brains <strong>of</strong> schizophrenic individuals are overactive, this overactivity should be reflected in increased levels <strong>of</strong> HVA in CSF. This expectation <strong>of</strong> an effect on the CSF is a subsidiary hypothesis <strong>of</strong> this variant <strong>of</strong> the general DHS. By 1976, Meltzer <strong>and</strong> Stahl reviewed a number <strong>of</strong> studies inconsistent with this prediction. Indeed, they showed, if anything, a tendency toward reduced DA metabolites in the CSF <strong>of</strong> schizophrenic patients. A later meta-analysis reached the same conclusion as the earlier Meltzer <strong>and</strong> Stahl review (Tuckwell <strong>and</strong> Kosiol 1993). <strong>The</strong>se negative results raise two important points about the DHS. First, it could be understood as predicting global changes in brain DA function or only changes in specific DA systems. In this article, we refer to these two subforms <strong>of</strong> the DHS as global <strong>and</strong> regional, respectively. Second, functional excess <strong>of</strong> DA function could arise in two broad ways: IT or increased post-synaptic receptor function (IRF for increased receptor function) that could in turn result from changes in the number or sensitivity <strong>of</strong> receptors. Only the IT subform <strong>of</strong> the DHS predicts that individuals with schizophrenia would have excess CSF levels <strong>of</strong> HVA. (Indeed, some version <strong>of</strong> the IRF form <strong>of</strong> the DHS would predict decreased levels <strong>of</strong> CSF HVA.) <strong>The</strong> non-confirmation <strong>of</strong> the predictions <strong>of</strong> the DHS by the CSF findings had little impact on enthusiasm for the DHS. As noted by Meltzer <strong>and</strong> Stahl: this result should not be used to reject the hypothesis <strong>of</strong> increased DA turnover in schizophrenia since the functional activity <strong>of</strong> DA relevant to schizophrenia may not be measured by the method. (1976, 52) In humans, much <strong>of</strong> the HVA in CSF comes from the caudate nucleus (Sourkes 1973), the endpoint <strong>of</strong> the nigrostriatal DA system. We interpret Meltzer <strong>and</strong> Stahl’s comment as suggesting that these results argue against a global DHS—in which excess DA activity is seen in all brain DA systems—but does not disprove a more restricted DHS in which excess DA activity is limited to certain regional DA systems not reflected in CSF, particularly those outside the striatum. This point was elaborated upon by Carlsson in a 1978 review, which enumerated a total <strong>of</strong> five possible subforms <strong>of</strong> the DHS including IT, IRF, <strong>and</strong> other possibilities we do not examine in detail in this review, including “deficient inactivation <strong>of</strong> DA” <strong>and</strong> alterations in presynaptic DA systems. Hormonal Systems Because two pituitary hormones—growth hormone (GH) <strong>and</strong> prolactin—are significantly influenced by brain DA systems, early attempts were made to validate the DHS by determining whether expected abnormalities in these hormonal systems were seen in patients with schizophrenia. GH is phasically stimulated by DA in the arcuate nucleus <strong>of</strong> the hypothalamus. If schizophrenia were due to widespread IT in DA neurons or to IRF <strong>of</strong> the relevant DA receptors, then excess GH stimulation should be seen in schizophrenia. As reviewed by Marx <strong>and</strong> Lieberman (1998), studies <strong>of</strong> basal GH secretion in schizophrenic <strong>and</strong> control subjects have been inconsistent with a few finding increased levels <strong>of</strong> GH in schizophrenic subjects, but with most finding no difference. <strong>The</strong> IRF form <strong>of</strong> the DHS could be specifically tested by examining whether schizophrenia is associated with greater GH stimulation in response to DA agonist drugs. A modest number <strong>of</strong> studies have examined this question <strong>and</strong> results were quite variable. In aggregate, Marx <strong>and</strong> Lieberman conclude that “schizophrenic <strong>and</strong> control subjects do not appear to differ significantly in GH response to dopamine agonists” (1998, 415). <strong>The</strong> sensitivity <strong>of</strong> the GH system can also be tested by the administration <strong>of</strong> GH-releasing hormone. In a review <strong>of</strong> three such studies, compared with controls, schizophrenic patients had a similar GH response to GH releasing hormone in two studies <strong>and</strong> a diminished response in a third (Skare et al. 1994). Prolactin is inhibited by DA secreted into the portal vein <strong>of</strong> the pituitary. Increased DA turnover
- Page 1 and 2: The Dopamine Hypothesis of Schizoph
- Page 3 and 4: 42 ■ PPP / Vol. 18, No. 1 / March
- Page 5: 44 ■ PPP / Vol. 18, No. 1 / March
- Page 9 and 10: 48 ■ PPP / Vol. 18, No. 1 / March
- Page 11 and 12: 50 ■ PPP / Vol. 18, No. 1 / March
- Page 13 and 14: 52 ■ PPP / Vol. 18, No. 1 / March
- Page 15 and 16: 54 ■ PPP / Vol. 18, No. 1 / March
- Page 17 and 18: 56 ■ PPP / Vol. 18, No. 1 / March
- Page 19 and 20: 58 ■ PPP / Vol. 18, No. 1 / March
- Page 21 and 22: 60 ■ PPP / Vol. 18, No. 1 / March
- Page 23 and 24: 62 ■ PPP / Vol. 18, No. 1 / March