Full Clinical Guidelines - Community First Health Plans.
Full Clinical Guidelines - Community First Health Plans.
Full Clinical Guidelines - Community First Health Plans.
Create successful ePaper yourself
Turn your PDF publications into a flip-book with our unique Google optimized e-Paper software.
<strong>Community</strong> <strong>First</strong> <strong>Health</strong> <strong>Plans</strong><br />
Quality Improvement <strong>Guidelines</strong><br />
www.cfhp.com<br />
Member Services: 1-800-434-2347<br />
Servicios de Miembros: 1-800-434-2347<br />
Serving Atascosa, Bandera, Bexar, Comal, Guadalupe, Kendall, Medina & Wilson counties.<br />
Sirviendo los condados de Atascosa, Bandera, Bexar, Comal, Guadalupe, Kendall, Medina y Wilson.
Table of Contents<br />
Table of Contents..................................................................................................................................................... 2<br />
1.1 Quality Improvement <strong>Guidelines</strong>........................................................................................................................ 4<br />
2.1 Access and Availability Standards...................................................................................................................... 9<br />
3.1 Preventive Services for Adults........................................................................................................................... 11<br />
3.2 Recommended Adult Immunization Schedule................................................................................................ 13<br />
4.1 Asthma Disease Management........................................................................................................................... 17<br />
Asthma Flow Sheet.................................................................................................................................................. 19<br />
4.3 Classifying Asthma Severity and Initiating Therapy In Children ...................................................................... 20<br />
4.4 Assessing Asthma Control and Adjusting Therapy in Children........................................................................ 21<br />
4.5 Stepwise Approach for Managing Asthma Long Term in Children.................................................................. 22<br />
4.6 Classifying Asthma Severity and Initiating Treatment in Youths & Adults...................................................... 23<br />
4.7 Assessing Asthma Control and Adjusting Therapy in Youths and Adults........................................................ 24<br />
4.8 Stepwise Approach for Managing Asthma in Youth and Adults..................................................................... 25<br />
4.9 Estimated Comparative Daily Dosages for Inhaled Corticosteroids................................................................ 26<br />
4.10 Classifying Severity of Asthma Exacerbation in the Urgent or EC Setting.................................................... 27<br />
5.1 Attention-Deficit Hyperactivity Disorder <strong>Clinical</strong> Practice <strong>Guidelines</strong>.............................................................. 28<br />
6.1 Behavioral <strong>Health</strong> Documentation <strong>Guidelines</strong>.................................................................................................. 31<br />
6.2 Behavioral <strong>Health</strong> Medical Record Review Tool............................................................................................... 34<br />
7.1 Management of Common Breast Problems...................................................................................................... 35<br />
8.1 Child Abuse and Neglect.................................................................................................................................... 37<br />
8.2 AAP Policy Recommendations.......................................................................................................................... 39<br />
9.1 Diabetes <strong>Guidelines</strong>............................................................................................................................................ 42<br />
9.2 Glycemic Control Algorithm Type 2 DM in Children and Adults....................................................................... 44<br />
9.3 Insulin Algorithm Type 1 DM in Children and Adults......................................................................................... 46<br />
9.4 Insulin Algorithm Type 2 DM in Children and Adults ....................................................................................... 47<br />
9.5 Exercise Algorithm Type 2 Diabetes Prevention and Therapy......................................................................... 53<br />
9.6 Hypertension Algorithm for DM in Adults........................................................................................................ 55<br />
9.7 Lipid Treatment Algorithm Type 1 and Type 2 DM in Adults............................................................................ 57<br />
9.8 Diabetes Medical Nutrion Therapy and Prevention Algorithm....................................................................... 60<br />
9.9 Weight Loss Algorithm Overweight and Obese Adults................................................................................... 61<br />
9.10 Prevention and Delay Type 2 Diabetes in Children and Adults...................................................................... 63<br />
9.11 Diabetic Foot Screen, Exam, Care and Referral............................................................................................... 65<br />
9.12 Weight Management Algorithm Overweight Children & Adolescents.......................................................... 69<br />
9.13 IV Insulin Infusion Protocol Critically IU Adult Patients.................................................................................. 73<br />
9.14 ICU Insulin Orders............................................................................................................................................. 76<br />
9.15 Screening & Management of Hyperglycemia in the Geriatric Population..................................................... 78<br />
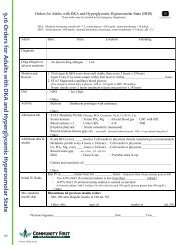
9.16 Orders for Adults with DKA and Hyperglycemic Hyperosmolar State.......................................................... 80<br />
9.17 Transition Algorithm From IV to SQ Insulin for Patients with Diabetes or Hyperglycemia........................... 83<br />
9.18 Recommendations for Treatment of Painful Peripheral Diabetic Neuropathy in Adults............................. 84<br />
10.1 Management of High Blood Cholesterol in Adults.......................................................................................... 85<br />
10.2 National Cholesterol Education <strong>Guidelines</strong>..................................................................................................... 86<br />
10.3 Progression of Therapy to Achieve LDL-C Goals............................................................................................. 87<br />
10.4 Drugs Affecting Lipoprotein Metabolism........................................................................................................ 88<br />
2 H EALTH PLANS<br />
www.cfhp.com
10.5 ATP III Classification of Cholesterol................................................................................................................. 89<br />
10.6 <strong>Clinical</strong> Identification of the Metabolic Syndrome.......................................................................................... 90<br />
10.7 ATP III Classification of Serum Triglycerides.................................................................................................... 91<br />
11.1 Management of High Blood Pressure............................................................................................................... 92<br />
11.2 Classification of Blood Pressure........................................................................................................................ 93<br />
11.3 Treatment of Hypertension............................................................................................................................... 95<br />
12.1 Depression Management & Antidepressant Treatment................................................................................. 96<br />
12.2 Depression Outpatient Treatment................................................................................................................... 98<br />
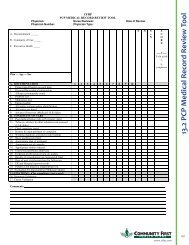
13.1 PCP Medical Record Documentation <strong>Guidelines</strong>............................................................................................. 99<br />
13.2 PCP Medical Record Review Tool..................................................................................................................... 101<br />
13.3 Specialist Medical Record Documentation <strong>Guidelines</strong>.................................................................................... 105<br />
13.4 Specialist Medical Record Review Tool........................................................................................................... 107<br />
14.1 Management of Osteoporosis.......................................................................................................................... 108<br />
14.2 Recommendations from National Osteoporosis Foundation........................................................................ 109<br />
15.1 Management of Overweight and Obesity in Adults........................................................................................ 111<br />
15.2 Classification of Overweight and Obesity by BMI........................................................................................... 112<br />
15.3 Treatment of Overweight and Obesity in Adults............................................................................................. 114<br />
16.1.1 Preventive Pediatric <strong>Health</strong> Care <strong>Guidelines</strong>................................................................................................. 115<br />
16.1.2 Texas <strong>Health</strong> Steps Periodicity Schedule....................................................................................................... 116<br />
16.1.3 Texas <strong>Health</strong> Steps Mental <strong>Health</strong> Interview Tool........................................................................................ 119<br />
16.1.4 Texas <strong>Health</strong> Steps Mental <strong>Health</strong> Questionnaire........................................................................................ 124<br />
16.2.1 Immunization Schedule 0-6 years ................................................................................................................. 140<br />
16.2.2 Immunization Schedule 7-18 years................................................................................................................ 141<br />
16.2.3 Immunization Catch-up Schedule ................................................................................................................ 142<br />
17.1 Prenatal Care <strong>Guidelines</strong>................................................................................................................................... 143<br />
17.2 Cesarean Section <strong>Guidelines</strong>............................................................................................................................. 145<br />
17.3 OB/GYN Medical Record Documentation <strong>Guidelines</strong>...................................................................................... 146<br />
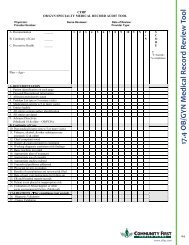
17.4 OB/GYN Medical Record Review Tool.............................................................................................................. 149<br />
18.1 RSV Prophylaxis................................................................................................................................................. 152<br />
19.1 Pediatric and Adolescent Overweight and Obesity......................................................................................... 153<br />
19.2 Assessment, Prevention and Treatment of Pediatric Obesity........................................................................ 154<br />
19.3 Weight Management Algorithm for Overweight Children & Adolescents.................................................... 158<br />
19.4 CDC BMI for Age Percentiles........................................................................................................................... 159<br />
Asthma Disease Management ................................................................................................................................ 161<br />
Diabetes in Control................................................................................................................................................... 162<br />
Prenatal Assessment and Education Program....................................................................................................... 163<br />
*The most current version of guidelines can be found at http://www.cfhp.com/providers/clinicalguidelines<br />
H EALTH PLANS<br />
www.cfhp.com<br />
3
1.1 Quality Improvement <strong>Guidelines</strong><br />
An Introduction to <strong>Community</strong> <strong>First</strong> <strong>Health</strong> <strong>Plans</strong><br />
<strong>Community</strong> <strong>First</strong> <strong>Health</strong> <strong>Plans</strong> (CFHP) evolved from a desire to provide superior health care to our community. Locally owned<br />
and managed, our non-profit HMO strives to make this goal an affordable reality for our members, while at the same time,<br />
supporting the local economic base.<br />
Dedicated to the ideal of good health for the good of the whole community, our goal is to make preventive health services<br />
more accessible to our members. Choices of physicians, hospitals and other providers are spread throughout the area, and the<br />
benefits are easy to understand.<br />
Our plan’s design emphasizes regular, preventive care for the whole family. We encourage all network physicians and other<br />
medical professionals to help our members learn about and develop better habits for a healthier lifestyle. We want to partner<br />
with you and your patients for disease prevention, early detection of illness and more effective treatment management.<br />
Committed. Responsive. Innovative. Now is the time to discover the advantages of a locally owned health care plan that<br />
reinvests in its members, its physicians and its community. At <strong>Community</strong> <strong>First</strong> <strong>Health</strong> <strong>Plans</strong>, helping our members maintain<br />
their health is our first concern.<br />
Quality <strong>Health</strong> Care<br />
Under our plan, members have access to a large group of physicians offering primary care, behavioral health and other specialty<br />
care, as well as access to related health care professionals. With the help of their chosen primary care physician, members<br />
take control of their health care needs, using preventive measures that help minimize the risk of future illness. Instead of just<br />
reacting to problems, our <strong>Health</strong> Plan aims to be progressive with annual check-ups, immunizations, health education, preferred<br />
drug listing (Open Pharmacy Benefit), preventive health programs, clinical care coordination programs and easy referrals to<br />
specialists.<br />
Access<br />
Members can freely choose their primary care physicians from the excellent group of professionals that have contracted with<br />
<strong>Community</strong> <strong>First</strong> <strong>Health</strong> <strong>Plans</strong>. In addition, family members may decide to use the same or a different physician, depending on<br />
individual preferences. By developing a close relationship with the primary care physician, our members enjoy ready access to<br />
quality care and proper coordination of referrals. <strong>Community</strong> <strong>First</strong> <strong>Health</strong> <strong>Plans</strong> allows open access for OB/Gyn services and for<br />
behavioral health initial consults. Behavioral health providers are required to notify the member’s PCP when behavioral health<br />
services are rendered. Our members are allowed to use any participating OB/Gyn physician without obtaining a referral for the<br />
following services:<br />
• annual well woman check-up;<br />
• care related to a pregnancy;<br />
• care for all gynecological conditions; and<br />
• care for any disease or treatment within the scope of the doctor’s license including diseases of the breast.<br />
The Only Plan of its Kind: Local Economic Benefits<br />
<strong>Community</strong> <strong>First</strong> is the only plan of its kind with roots firmly based in San Antonio. This strengthens our local economic base<br />
and allows us to continue improving our plan as we become successful. Our values are:<br />
• commitment to quality health care and service at an affordable price;<br />
• loyalty to our customers;<br />
• integrity in all business interactions;<br />
• accountability to our community; and<br />
• mutual accountability for performance.<br />
Confidentiality<br />
At <strong>Community</strong> <strong>First</strong> <strong>Health</strong> <strong>Plans</strong>, we rigorously protect the confidentiality of personal and proprietary information. This holds<br />
true for all of our members, providers and employees.<br />
Member information is kept strictly confidential. This includes information regarding medical conditions, history, medication,<br />
family illnesses, and personal and financial data.<br />
4 H EALTH PLANS<br />
www.cfhp.com
Such information is released only to those authorized to receive it, either by law or by the member’s written consent. When<br />
such information is released, it is done so only to the extent to which it is necessary.<br />
Commitment<br />
We continually seek new ways to offer the most affordable and innovative coverage to employers and their employees. We<br />
strive to provide timely information to physicians regarding information that will assist in keeping our members healthy. At<br />
<strong>Community</strong> <strong>First</strong> <strong>Health</strong> <strong>Plans</strong>, our name is our commitment.<br />
Communication<br />
Effective communication is essential to providing clinical care coordination for our <strong>Community</strong> <strong>First</strong> members. We are dedicated<br />
to interacting closely with physicians, ancillary health care professionals and patients with a carefully designed support system<br />
to improve clinical outcomes and patient satisfaction. Our clinical guidelines are recommendations developed by national<br />
specialty societies and adapted and approved by local community physicians. They are NOT intended to be a cookbook set of<br />
rules to substitute for good clinical judgment.<br />
Quality Management Program & Structure<br />
Our Quality Management Program is an integrated, comprehensive program that incorporates review and evaluation of all<br />
aspects of the health care delivery system. Components of this program include problem-focused studies, peer review, risk<br />
management, credentialing, compliance with external regulatory agencies, utilization review, medical records review, ongoing<br />
monitoring of key indicators (e.g., mortality review and Cesarean section rates), and health care services evaluation.<br />
The purpose of our Quality Management Program is to improve the health of our members. <strong>Community</strong> <strong>First</strong> continues to<br />
focus our attention on ensuring that health care quality and appropriateness are consistent with accepted practice and meet<br />
or exceed regulatory standards. The scope of the program is comprehensive and includes health care services provided in<br />
institutional or non-institutional settings<br />
The Quality Management program is under the direct supervision of our Vice President of <strong>Health</strong> Care Services, the Medical<br />
Director and our Quality Improvement Committee.<br />
Quality Improvement Committee (QIC)<br />
<strong>Community</strong> <strong>First</strong>’s Quality Improvement Committee (QIC) develops, implements, evaluates and revises the Quality Management<br />
and Improvement Program as delegated by the CEO and the Board of Directors. The QIC performs the following functions:<br />
• Recommends and approves all health care plans (i.e., Quality Management and Improvement, Utilization Management,<br />
<strong>Health</strong> Promotion and Wellness, etc.) and policies that govern the execution of <strong>Community</strong> <strong>First</strong> activities that<br />
significantly impact the health status of <strong>Community</strong> <strong>First</strong> membership;<br />
• Critically analyzes trends and other population-based data specific to the health care needs of <strong>Community</strong> <strong>First</strong> members;<br />
• Evaluates summary information from quality reports; reviews identified quality of care problems;<br />
• Assists with the development of protocols, standards, guidelines and indicators for clinical practice that support quality<br />
of care monitoring activities;<br />
• Oversees the actions of the P& T and Credentialing Committees;<br />
• Reviews and approves all physician-related Corrective Action <strong>Plans</strong> and re-evaluates the effectiveness of those plans; and<br />
• Actively contributes to the development of study topics and special reports.<br />
A <strong>Community</strong> <strong>First</strong> participating health care physician serves as Chair of the QIC. The entire QIC membership, as well as<br />
any ad hoc committees that may be appointed by the QIC, consists of <strong>Community</strong> <strong>First</strong>’s Medical Director and at least eight<br />
primary care and specialty providers. <strong>Health</strong> care providers reflective of the health care needs of <strong>Community</strong> <strong>First</strong> members<br />
including behavioral health participating health care providers are involved in the review of <strong>Community</strong> <strong>First</strong>’s utilization and<br />
management program as well as in the development of Practice <strong>Guidelines</strong>. Any practicing physician who is interested in<br />
participating in our QIC process should feel free to contact our Medical Director at (210) 358-6101.<br />
The current members of the QIC are:<br />
• Chair<br />
• Ernesto Parra, MD<br />
H EALTH PLANS<br />
www.cfhp.com<br />
5
• Averell Sutton, MD<br />
• Robert Parker, MD<br />
• Priti Mody-Bailey, MD, MA<br />
• Mary Garcia-Holguin, MD, Associate Medical Director, Behavioral <strong>Health</strong><br />
• Greg Gieseman, President/CEO<br />
• Mark Funk, MD<br />
• Fred C. Campbell, Jr., MD<br />
• B.D. Tiner, MD<br />
• Sheila Owens-Collins, MD, Vice President and Senior Medical Director<br />
• Medical Director<br />
• Ruben Guerrero, Member Representative<br />
Pharmacy & Therapeutics Committee (P&T)<br />
A Pharmacy & Therapeutics Committee (P&T) has been formed by <strong>Community</strong> <strong>First</strong>. Launched in January of 1998, the<br />
Committee is devoted to improving the effectiveness of prescription drug therapies and usage. The P&T advises network<br />
physicians and participates in Quality Improvement activities related to the administration of prescription medications. It also<br />
reviews pharmacy quality assurance results.<br />
The goal of the Committee is to improve the overall quality and effectiveness of patient drug usage by developing standards<br />
and procedures to ensure the propriety, safety, and effectiveness of drug therapies. The P&T’s recommendations – which<br />
are presented to the Quality Improvement Committee – are based on an extensive review of drug utilization reports. To<br />
complement these measures, the P&T is also implementing educational programs and exploring innovative ways to correct<br />
drug usage deficiencies and provide cost-effective drug therapy.<br />
The current members of our P&T Committee are:<br />
• George Crawford, MD, Chair<br />
• Mary Garcia-Holguin, MD, Associate Medical Director, Behavioral <strong>Health</strong><br />
• Sheila Owens-Collins, MD, Vice President and Senior Medical Director<br />
• Ramie Ramirez, D. Ph, R. Ph, MBA, Manager <strong>Clinical</strong> Pharmacy Services<br />
• Currently assigned <strong>Clinical</strong> Program Manager<br />
• Medical Director<br />
• Michael Johnson, MD<br />
• Krista Bowers, MD<br />
• David Van Buskirk, RPh<br />
Credentialing Committee<br />
<strong>Community</strong> <strong>First</strong>’s Credentialing Committee is responsible for reviewing and evaluating provider credentials, delegated<br />
credentialing and the credentialing policies and procedures of both the <strong>Health</strong> Plan and each delegate. As designated by the<br />
Quality Improvement Committee and the Board of Directors, the Credentialing Committee performs the following functions:<br />
• Oversees verification of providers participating within <strong>Community</strong> <strong>First</strong>’s network;<br />
• Reviews and approves the credentials of all providers submitting applications to <strong>Community</strong> <strong>First</strong> <strong>Health</strong> <strong>Plans</strong> using the<br />
criteria established by NCQA, TDI, and <strong>Community</strong> <strong>First</strong> policies and procedures;<br />
• Assists with the development and improvement of the credentialing policies and procedures; and<br />
• Reviews and approves summary and audit information supplied by each entity providing delegated credentialing.<br />
The current members of our Credentialing Committee, which is chaired by <strong>Community</strong> <strong>First</strong>’s Medical Director(s), are:<br />
Voting<br />
• Bakthavathsalam Athreya, MD<br />
• Nancy Amodei, PhD<br />
• William Elizondo, OD<br />
• James Hadnott, MD<br />
• Freeman Jardan, MD<br />
• Leopoldo Tecaunhey, MD<br />
• Donald Dudley, MD<br />
• Mary Garcia-Holguin, MD, Associate Medical Director, Behavioral <strong>Health</strong><br />
• Medical Director<br />
6 H EALTH PLANS<br />
www.cfhp.com
Non Voting<br />
• Martin Jimenez, Director Network Management<br />
• Director Quality Management<br />
• Paul Maldonado, Credentialing Manager<br />
<strong>Health</strong> Services Management (HSM)<br />
The members of the <strong>Health</strong> Services Management staff are:<br />
Sheila Owens-Collins, MD, MPH, MBA, Vice President and Senior Medical Director<br />
Dr. Owens-Collins is the Senior Medical Director for <strong>Community</strong> <strong>First</strong> <strong>Health</strong> <strong>Plans</strong>. She is a Neonatologist with a Master of<br />
Science Degree in Public <strong>Health</strong> and Business Administration. Prior to becoming the Senior Medical Director, she served as a<br />
Consultant and Associate Medical Director for <strong>Community</strong> <strong>First</strong> <strong>Health</strong> <strong>Plans</strong> for 5 years, during which time she was primarily<br />
involved with utilization and case management of complex newborns. Her managed care experience began with a five year<br />
tenure at <strong>Community</strong> <strong>Health</strong> Choice, Inc. in Houston, Texas, where she was the Vice President of Medical Affairs. In addition to<br />
her experience in managed care, Dr. Owens-Collins has several years experience as a practicing neonatologist.<br />
Ramie Ramirez, D.Ph., R.Ph., MBA, Manager of <strong>Clinical</strong> Pharmacy Services<br />
Dr. Ramirez has an extensive career in managed care pharmacy having been involved in many segments of Managed Care<br />
since 1983. His expertise includes Commercial, Medicare, and Medicaid pharmacy benefit design, PBM contracting, Pharmacy<br />
Network Contracting, and Pharmaceutical Manufacturer contracting. Dr. Ramirez came to CFHP as Manager of <strong>Clinical</strong><br />
Pharmacy Services. He began work at CFHP in 2008. Most recently he was Pharmacy Program Manager with Aetna where<br />
he was responsible for the Pre-Cert edits for Prior Authorization. His experience includes serving as Director of Pharmacy<br />
<strong>Clinical</strong> Services for AmeriChoice, a United<strong>Health</strong> Group where he was responsible for the prior authorization unit for 13 State<br />
Medicaid <strong>Plans</strong>. Before United<strong>Health</strong> he was Pharmacy Services Manager for Blue Cross Blue Shield of Louisiana where he was<br />
responsible for the pharmacy benefit for BCBSLA. He received his BS in Pharmacy form the University Of Houston College Of<br />
Pharmacy, his Doctor of Pharmacy from the State of Louisiana, and his Masters in Business Administration from the University<br />
of Phoenix.<br />
Carol Hoppes, RN, Director, Case Management<br />
Carol has traditional and managed care experience in a health insurance plan. Prior to joining <strong>Community</strong> <strong>First</strong> <strong>Health</strong> <strong>Plans</strong>,<br />
Carol worked with a health insurance plan in both the traditional insurance plan and managed care. In addition, she has<br />
experience as a <strong>Clinical</strong> Consultant conducting change management and process improvements in hospital care, Perioperative<br />
materials management, staff development, leadership training and computer programming. Carol received her Bachelor of<br />
Science in Nursing from the University of Nebraska Medical Center, Omaha, NE. She completed the MBA at the University of<br />
Nebraska, Omaha, NE. She received a Certificate in Mainframe Programming from the Creighton Institute, Omaha, NE.<br />
Denise Kain, RN, Director, Utilization Management<br />
Denise holds a Masters in Human Services Administration from Springfield College, Springfield, Massachusetts, a Bachelors<br />
in Business Administration from Westfield State College, Westfield, Massachusetts and Associates in Nursing from Holyoke<br />
<strong>Community</strong> College, Holyoke, Massachusetts. She has over 34 years of varied Registered Nursing experience including 25 years<br />
of managerial experience and 16 years of Managed Care Experience. Her insurance experience includes HMO, PPO, Medicare<br />
and Military Managed Care. Denise joined <strong>Community</strong> <strong>First</strong> <strong>Health</strong> Plan in February of 2006. She received her certification in<br />
Case Management in April of 2006 and is a member of the Case Management Society of America.<br />
Christine Hollis, Director, Preventive <strong>Health</strong> & Disease Management<br />
Christine joined <strong>Community</strong> <strong>First</strong> in 1996 as a <strong>Health</strong> Educator, in 2003 she was promoted to Manager of the <strong>Health</strong> Promotion<br />
and Wellness Department and in 2007 was promoted to Director of the department. Christine has more than 20 years of<br />
experience working with the community through the public, private, and managed care arenas of healthcare. She earned a<br />
Bachelor’s degree in Sociology with a minor in psychology and has completed some course work on her Master’s in Pubic<br />
Administration with a concentration in Public <strong>Health</strong> at the University of Texas at San Antonio.<br />
H EALTH PLANS<br />
www.cfhp.com<br />
7
Mary Garcia-Holguin, MD, Associate Medical Director<br />
Dr. Garcia-Holguin, a San Antonio native, is board certified in adult psychiatry. She obtained her medical degree from the<br />
University of Texas Medical School in Houston. She completed her general psychiatric residency at Duke University Medical<br />
Center in Durham, North Carolina. She received and completed a fellowship in child and adolescent psychiatry at the University<br />
of Texas <strong>Health</strong> Science Center in San Antonio. In her private practice she specializes in working with children, adolescents and<br />
adults who have emotional difficulties such as depression, panic and anxiety disorders, attention deficit/hyperactivity disorder,<br />
behavioral disorders and substance abuse. She has been the Associate Medical Director with CFHP since December 1998. Dr.<br />
Garcia-Holguin is enthusiastic about continuing to assure quality psychiatric services to her native San Antonio.<br />
Dianna M. Burns, MD, Associate Medical Director<br />
Dr. Burns is board certified in Pediatrics and has been in private practice in East San Antonio since 1986. She obtained her<br />
medical degree from the University of Louisville and completed her pediatrics residency at the University of Louisville Children’s<br />
Hospital. She has served on the Board of Directors of the Bexar County Medical Society and chairs the Department of Pediatrics<br />
at Baptist Medical Center. Dr. Burns recently received her Masters Degree in <strong>Health</strong> Care Administration from Trinity University.<br />
8 H EALTH PLANS<br />
www.cfhp.com
The purpose of these guidelines is to ensure that health services are available and accessible to CFHP members. Because CFHP<br />
contracts with a closed panel of practitioners, it is essential that we have a sufficient number of practitioners in our network<br />
who are conveniently located to serve our enrollees. By monitoring compliance with these guidelines, CFHP can identify<br />
opportunities to improve our performance, and to develop and implement intervention strategies to effect any necessary<br />
improvement.<br />
CFHP has Primary Care Physicians (PCPs) available throughout the service area to ensure that no member must travel more than<br />
30 miles, or 45 minutes, whichever is less, to access the PCP.<br />
CFHP Providers shall be available to members by telephone twenty-four (24) hours a day, seven (7) days a week for consultation<br />
and/or management of medical concerns.<br />
TYPE OF APPOINTMENT<br />
Emergency Care, including Behavioral <strong>Health</strong><br />
Urgent Care (PCP)<br />
(Specialist)<br />
(Behavioral <strong>Health</strong>)<br />
Routine Care (PCP)<br />
(Specialist)<br />
(Behavioral <strong>Health</strong>)<br />
Routine/scheduled inpatient/outpatient care<br />
Behavioral <strong>Health</strong> Discharge Planning/Aftercare<br />
Initial Outpatient Behavioral <strong>Health</strong> Visits<br />
Routine Specialty Care Referrals<br />
Physical Examinations<br />
Prenatal Care (Initial)<br />
High-risk Pregnancies or New Members in the Third Trimester<br />
Well-Child Care<br />
Well Adolescent Care<br />
Texas <strong>Health</strong> Steps Medical Checkups<br />
Migrant Farm Worker Children<br />
Newborn Care (in a hospital)<br />
Newborn Care (after discharge from a hospital)<br />
APPOINTMENT AVAILABILITY<br />
24 hours a day, 7 days a week, upon Member presentation<br />
at the delivery site, including non-network and out-of-area<br />
facilities<br />
Within 24 hours of request<br />
Within 24 hours of request<br />
Within 24 hours of request<br />
Within 14 days of request<br />
Within 14 days of request<br />
Within 14 days of request<br />
Members discharged from an impatient setting must have a<br />
scheduled follow-up outpatient appointment within 7 days<br />
after discharge. Members should be strongly encouraged to<br />
attend and participate in aftercare appointments.<br />
Within 14 days of request.<br />
Within 30 days of request.<br />
56 days or less (4 - 8 weeks)<br />
14 calendar days or less or by the 12th week of gestation.<br />
Members who express concern about termination will be<br />
addressed as Urgent Care.<br />
Within 5 days or immediately if an emergency exists.<br />
Routine Well-Child Care: In accordance with Academy of<br />
Pediatrics periodicity schedule<br />
Routine Well Adolescent Care: In accordance with American<br />
Academy of Pediatrics periodicity schedule and CFHP’s<br />
Quality Improvement <strong>Guidelines</strong>, as amended from time to<br />
time.<br />
Within 14 days of enrollment and no later than 60 days<br />
of enrollment for other eligible child members and in<br />
accordance with HHSC published periodicity schedule for<br />
Texas <strong>Health</strong> Steps.<br />
Staff must ensure prompt delivery of services to children of<br />
migrant farm workers and other migrant populations who<br />
may transition into or out of HMO program more rapidly and/<br />
or unpredictably than the general population.<br />
Newborns must receive an initial newborn checkup before<br />
discharge from the hospital to include all required tests and<br />
immunizations.<br />
Within 3 to 5 days after birth and then within 14 days of<br />
hospital discharge.<br />
2.1 Access and Availability Standards<br />
H EALTH PLANS<br />
www.cfhp.com<br />
9
TYPE OF APPOINTMENT<br />
Preventive <strong>Health</strong> Services for Children and Adolescents<br />
Preventive <strong>Health</strong> Services for Adults<br />
Physical Therapy<br />
Radiology<br />
Home <strong>Health</strong>/DME/Supplies (OT, PT, ST SNV, etc)<br />
Provider Office Waiting TIme<br />
Requests for Feedback from Pharmacy Related to<br />
Prescriptions<br />
APPOINTMENT AVAILABILITY<br />
Within 60 days of request in accordance with American<br />
Academy of Pediatrics periodicity schedule.<br />
Within 90 days of request in accordance with US Preventive<br />
Service Task Force recommendations.<br />
Within 24 hours (urgent)<br />
3 days or less (routine)<br />
14 days or less (follow-up)<br />
Within 24 hours (urgent)<br />
7 days or less (MRI/CT Scan)<br />
10 days or less (IVP/UGI)<br />
21 days or less (Mammogram)<br />
Within 2 hours for IV therapy or oxygen therapy.<br />
Within 24 hours for standard nursing care and delivery of nonurgent<br />
equipment.<br />
Significant changes in health status of the patient are to<br />
be relayed to the attending physician within 4 hours of<br />
detection.<br />
Within 30 minutes of scheduled appointment time.<br />
Within 24 business hours.<br />
10 H EALTH PLANS<br />
www.cfhp.com
Table 1. Adult Preventive Services That Providers and Care Systems Must Assess the Need for and Offer to Each Patient. These<br />
Have the Highest Priority Value (Level I)<br />
SERVICE 21 to 39 Years 40 to 64 Years 65 Years and Older<br />
Alcohol abuse; hazardous and<br />
harmful drinking screening<br />
and brief counseling<br />
Aspirin chemoprophylaxis<br />
counseling<br />
Breast cancer screening<br />
Cervical cancer screening No screening before age 21<br />
regardless of age of onset<br />
of sexual activity. Screening<br />
every 2 years between ages<br />
21-29 and every 3 years after<br />
age 30 after 3 consecutive<br />
normal Pap tests.<br />
Chlamydia screening<br />
Colorectal cancer screening<br />
Hypertension screening<br />
Influenza immunization<br />
Lipid screening<br />
Pneumococcal immunization<br />
Tobacco use screening and<br />
brief intervention<br />
Identify those with risky or hazardous drinking, as well as those who have carried that<br />
behavior to the point of meeting criteria for dependence, and then provide brief intervention.<br />
Encourage for men age 45-79 years when the potential<br />
benefit of a reduction in myocardial infarctions outweighs the<br />
potential harm of an increase in gastrointestinal hemorrhage.<br />
Encourage for women age 55-79 years when the potential<br />
benefit of a reduction in ischemic strokes outweighs the<br />
potential harm of an increase in gastrointestinal hemorrhage.<br />
Mammogram every 1 to 2 years for women age 50 to 75 years.<br />
(See Annotation #2 for evidence and recommendations for<br />
other ages.)<br />
Every 3 years after 3<br />
consecutive normal Pap tests.<br />
Stop screening between ages<br />
65-70 if no abnormal Pap<br />
tests in 10 years.<br />
All sexually active women aged 25 years and younger, and older women at increased risk for<br />
infection.<br />
Age 50 years and older or age 45 years and older for African<br />
Americans and American Indians at appropriate intervals as<br />
determined by whichever screening method is chosen.<br />
Blood pressure every 2 years if less than 120/80; every year if 120 to 139/80 to 89 mm Hg.<br />
Annually during entire flu season for individuals age 50 and older, those at high risk, and<br />
others.<br />
Fasting fractionated lipid<br />
screening for men over age<br />
34 every 5 years.<br />
Immunize high-risk groups once. Re-immunize those at risk of<br />
losing immunity once after 5 years.<br />
Fasting fractionated lipid screening for men over age 34 and<br />
women over age 44 every five years.<br />
Immunize at age 65 if<br />
not done previously. Reimmunize<br />
once if first<br />
received more than 5 years<br />
ago and before age 65, or<br />
an immunocompromising<br />
condition is present.<br />
Establish tobacco use status for all patients and reassess at every opportunity. Provide brief<br />
intervention.<br />
3.1 Preventive Services for Adults<br />
H EALTH PLANS<br />
www.cfhp.com<br />
11
Table 2. Adult Preventive Services That Providers and Care Systems Should Assess the Need for and Offer to Each Patient. These<br />
Have Value But Less Than Those in Level I (Level II)<br />
SERVICE 21 to 39 Years 40 to 64 Years 65 Years and Older<br />
Abdominal aortic aneurysm<br />
screening<br />
Depression screening<br />
Folic acid chemoprophylaxis<br />
counseling<br />
Hearing screening<br />
Hepatitis B immunization<br />
Herpes zoster/shingles<br />
immunization<br />
Men ages 65 to 75 who<br />
have smoked more than 100<br />
cigarettes in lifetime.<br />
Routine screening if there are systems in place to ensure accurate diagnosis, effective<br />
treatment, and careful follow-up.<br />
Counsel women of reproductive age to consume 400 to<br />
800 micrograms of folic acid per day from food sources or<br />
supplements.<br />
Universal routine<br />
immunization for young<br />
adults less than 40 years of<br />
age.<br />
Human papillomavirus Catch up through age 26.<br />
(HPV) immunization<br />
Inactivated polio vaccine<br />
(IPV) immunization<br />
Measles, mumps, rubella<br />
(MMR) immunization<br />
Obesity screening<br />
Osteoporosis screening<br />
Tetanus-diphtheria (Td)<br />
immunization<br />
Varicella immunization<br />
Vision screening<br />
Subjective hearing screen (by questionnaire) followed by<br />
counseling on hearing aid devices and making referrals as<br />
appropriate for older adults.<br />
Vaccination should occur for adults not previously immunized against polio.<br />
Persons born during or after<br />
1957 should have one dose<br />
of measles vaccine; a second<br />
dose may be required in<br />
special circumstances.<br />
Record height, weight and calculate BMI at least annually.<br />
Immunize at age 60 or<br />
older patients who have no<br />
contraindications.<br />
Women age 65 and older<br />
should be screened for<br />
osteoporosis.<br />
All adults should have completed a primary Td series. For all adults, immunize with a booster<br />
dose of Td every 10 years thereafter.<br />
For all adults without evidence of immunity, a dose of varicella vaccine should be given<br />
followed by a second dose at an interval of at least 28 days. A catch-up second dose of<br />
varicella vaccine should be given to all children, adolescents, and adults who received only<br />
one dose previously.<br />
Objective vision testing for<br />
adults age 65 and older.<br />
<strong>Guidelines</strong> taken from: Institute for <strong>Clinical</strong> Systems Improvement (ICSI). Preventive services for adults. Bloomington (MN):<br />
Institute for <strong>Clinical</strong> Systems Improvement (ICSI); 2010 Sep. 79 p. [167 references]<br />
12 H EALTH PLANS<br />
www.cfhp.com
Recommended Adult Immunization Schedule—United States - 2012<br />
Note: These recommendations must be read with the footnotes that follow<br />
containing number of doses, intervals between doses, and other important information.<br />
Figure 1. Recommended adult immunization schedule, by vaccine and age group 1<br />
VACCINE ▼ AGE GROUP ► 19-21 years 22-26 years 27-49 years 50-59 years 60-64 years ≥ 65 years<br />
Influenza 2<br />
1 dose annually<br />
Tetanus, diphtheria, pertussis (Td/Tdap) 3, *<br />
Substitute 1-time dose of Tdap for Td booster; then boost with Td every 10 yrs<br />
Td/Tdap 3<br />
Varicella 4, *<br />
2 Doses<br />
Human papillomavirus (HPV) Female 5, *<br />
3 doses<br />
Human papillomavirus (HPV) Male 5, *<br />
3 doses<br />
Zoster 6<br />
1 dose<br />
Measles, mumps, rubella (MMR) 7, *<br />
1 or 2 doses<br />
1 dose<br />
Pneumococcal (polysaccharide) 8,9<br />
1 or 2 doses<br />
1 dose<br />
Meningococcal 10, *<br />
1 or more doses<br />
Hepatitis A 11, *<br />
2 doses<br />
Hepatitis B 12, *<br />
3 doses<br />
*Covered by the Vaccine Injury Compensation Program<br />
For all persons in this category who<br />
meet the age requirements and who<br />
lack documentation of vaccination<br />
or have no evidence of previous<br />
infection<br />
Recommended if some other risk<br />
factor is present (e.g., on the basis<br />
of medical, occupational, lifestyle, or<br />
other indications)<br />
Tdap recommended for ≥65 if contact<br />
with
Figure 2. Vaccines that might be indicated for adults based on medical and other indications 1<br />
VACCINE ▼ INDICATION ► Pregnancy<br />
Immunocompromising<br />
conditions<br />
(excluding human<br />
immunodeficiency<br />
virus<br />
infection 4,7,13,14<br />
CD4+ T lymphocyte<br />
count<br />
HIV<br />
200<br />
cells/μL<br />
Men who<br />
have<br />
sex with men<br />
(MSM)<br />
Heart disease,<br />
chronic<br />
lung disease,<br />
chronic<br />
alcoholism<br />
Asplenia 13<br />
(including<br />
elective<br />
splenectomy<br />
and persistent<br />
complement<br />
component<br />
deficiencies)<br />
Chronic<br />
liver<br />
disease<br />
Diabetes,<br />
kidney failure,<br />
end-stage<br />
renal<br />
disease,<br />
receipt of<br />
hemodialysis<br />
<strong>Health</strong>-care<br />
personnel<br />
Influenza 2<br />
1 dose TIV annually<br />
1 dose TIV or<br />
LAIV annually 1 dose TIV annually<br />
1 dose TIV or<br />
LAIV annually<br />
Tetanus, diphtheria, pertussis (Td/Tdap) 3, *<br />
Substitute 1-time dose of Tdap for Td booster; then boost with Td every 10 yrs<br />
Varicella 4, *<br />
Contraindicated<br />
2 doses<br />
Human papillomavirus (HPV) Female 5, *<br />
3 doses through age 26 yrs<br />
3 doses through age 26 yrs<br />
Human papillomavirus (HPV) Male 5, *<br />
3 doses through age 26 yrs 3 doses through age 21 yrs<br />
Zoster 6 Contraindicated<br />
1 dose 1 dose<br />
Measles, mumps, rubella (MMR) 7, *<br />
Contraindicated<br />
1 or 2 doses<br />
Pneumococcal (polysaccharide) 8,9<br />
1 dose 1 or TIV 2 doses annually<br />
Meningococcal 10, *<br />
1 or more doses<br />
Hepatitis A 11, *<br />
2 doses<br />
Hepatitis B 12, *<br />
3 doses<br />
*Covered by the Vaccine Injury Compensation Program<br />
The recommendations in this<br />
schedule were approved by the<br />
Centers for Disease Control and<br />
Prevention’s (CDC) Advisory<br />
Committee on Immunization<br />
Practices (ACIP), the American<br />
Academy of Family Physicians<br />
(AAFP), the American College of<br />
Physicians (ACP), American College<br />
of Obstetricians and Gynecologists<br />
(ACOG) and American College of<br />
Nurse-Midwives (ACNM).<br />
For all persons in this category who<br />
meet the age requirements and who<br />
lack documentation of vaccination<br />
or have no evidence of previous<br />
infection<br />
Recommended if some other risk<br />
factor is present (e.g., on the basis<br />
of medical, occupational, lifestyle,<br />
or other indications)<br />
Contraindicated No recommendation<br />
These schedules indicate the recommended age groups and medical indications for which administration of currently licensed vaccines is commonly<br />
indicated for adults ages 19 years and older, as of January 1, 2012. For all vaccines being recommended on the Adult Immunization Schedule: a vaccine<br />
series does not need to be restarted, regardless of the time that has elapsed between doses. Licensed combination vaccines may be used whenever<br />
any components of the combination are indicated and when the vaccine’s other components are not contraindicated. For detailed recommendations on<br />
all vaccines, including those used primarily for travelers or that are issued during the year, consult the manufacturers’ package inserts and the complete<br />
statements from the Advisory Committee on Immunization Practices (www.cdc.gov/vaccines/pubs/acip-list.htm). Use of trade names and commercial sources<br />
is for identification only and does not imply endorsement by the U.S. Department of <strong>Health</strong> and Human Services.<br />
U.S. Department of <strong>Health</strong> and Human Services<br />
Centers for Disease Control and Prevention<br />
14 H EALTH PLANS<br />
www.cfhp.com
Footnotes — Recommended Adult Immunization Schedule—United States - 2012<br />
7. Measles, mumps, rubella (MMR) vaccination (cont’d)<br />
Rubella component:<br />
• For women of childbearing age, regardless of birth year, rubella immunity should be<br />
determined. If there is no evidence of immunity, women who are not pregnant should be<br />
vaccinated. Pregnant women who do not have evidence of immunity should receive MMR<br />
vaccine upon completion or termination of pregnancy and before discharge from the healthcare<br />
facility.<br />
<strong>Health</strong>-care personnel born before 1957:<br />
• For unvaccinated health-care personnel born before 1957 who lack laboratory evidence of<br />
measles, mumps, and/or rubella immunity or laboratory confirmation of disease, health-care<br />
facilities should consider routinely vaccinating personnel with 2 doses of MMR vaccine at the<br />
appropriate interval for measles and mumps or 1 dose of MMR vaccine for rubella.<br />
8. Pneumococcal polysaccharide (PPSV) vaccination<br />
• Vaccinate all persons with the following indications:<br />
— age 65 years and older without a history of PPSV vaccination;<br />
— adults younger than 65 years with chronic lung disease (including chronic obstructive<br />
pulmonary disease, emphysema, and asthma); chronic cardiovascular diseases; diabetes<br />
mellitus; chronic liver disease (including cirrhosis); alcoholism; cochlear implants;<br />
cerebrospinal fluid leaks; immunocompromising conditions; and functional or anatomic<br />
asplenia (e.g., sickle cell disease and other hemoglobinopathies, congenital or acquired<br />
asplenia, splenic dysfunction, or splenectomy [if elective splenectomy is planned, vaccinate<br />
at least 2 weeks before surgery]);<br />
— residents of nursing homes or long-term care facilities; and<br />
— adults who smoke cigarettes.<br />
• Persons with asymptomatic or symptomatic HIV infection should be vaccinated as soon as<br />
possible after their diagnosis.<br />
• When cancer chemotherapy or other immunosuppressive therapy is being considered, the<br />
interval between vaccination and initiation of immunosuppressive therapy should be at least 2<br />
weeks. Vaccination during chemotherapy or radiation therapy should be avoided.<br />
• Routine use of PPSV is not recommended for American Indians/Alaska Natives or other<br />
persons younger than 65 years of age unless they have underlying medical conditions that<br />
are PPSV indications. However, public health authorities may consider recommending PPSV<br />
for American Indians/Alaska Natives who are living in areas where the risk for invasive<br />
pneumococcal disease is increased.<br />
9. Revaccination with PPSV<br />
• One-time revaccination 5 years after the first dose is recommended for persons 19 through<br />
64 years of age with chronic renal failure or nephrotic syndrome; functional or anatomic<br />
asplenia (e.g., sickle cell disease or splenectomy); and for persons with immunocompromising<br />
conditions.<br />
• Persons who received PPSV before age 65 years for any indication should receive another<br />
dose of the vaccine at age 65 years or later if at least 5 years have passed since their previous<br />
dose.<br />
• No further doses are needed for persons vaccinated with PPSV at or after age 65 years.<br />
10. Meningococcal vaccination<br />
• Administer 2 doses of meningococcal conjugate vaccine quadrivalent (MCV4) at least<br />
2 months apart to adults with functional asplenia or persistent complement component<br />
deficiencies.<br />
• HIV-infected persons who are vaccinated should also receive 2 doses.<br />
• Administer a single dose of meningococcal vaccine to microbiologists routinely exposed<br />
to isolates of Neisseria meningitidis, military recruits, and persons who travel to or live in<br />
countries in which meningococcal disease is hyperendemic or epidemic.<br />
• <strong>First</strong>-year college students up through age 21 years who are living in residence halls should be<br />
vaccinated if they have not received a dose on or after their 16th birthday.<br />
• MCV4 is preferred for adults with any of the preceding indications who are 55 years old and<br />
younger; meningococcal polysaccharide vaccine (MPSV4) is preferred for adults 56 years and<br />
older.<br />
• Revaccination with MCV4 every 5 years is recommended for adults previously vaccinated<br />
with MCV4 or MPSV4 who remain at increased risk for infection (e.g., adults with anatomic or<br />
functional asplenia or persistent complement component deficiencies).<br />
11. Hepatitis A vaccination<br />
• Vaccinate any person seeking protection from hepatitis A virus (HAV) infection and persons<br />
with any of the following indications:<br />
— men who have sex with men and persons who use injection drugs;<br />
1. Additional information<br />
• Advisory Committee on Immunization Practices (ACIP) vaccine recommendations and<br />
additional information are available at: http://www.cdc.gov/vaccines/pubs/acip-list.htm.<br />
• Information on travel vaccine requirements and recommendations (e.g., for hepatitis A<br />
and B, meningococcal, and other vaccines) available at http://wwwnc.cdc.gov/travel/page/<br />
vaccinations.htm.<br />
2. Influenza vaccination<br />
• Annual vaccination against influenza is recommended for all persons 6 months of age and<br />
older.<br />
• Persons 6 months of age and older, including pregnant women, can receive the trivalent<br />
inactivated vaccine (TIV).<br />
• <strong>Health</strong>y, nonpregnant adults younger than age 50 years without high-risk medical conditions<br />
can receive either intranasally administered live, attenuated influenza vaccine (LAIV) (FluMist),<br />
or TIV. <strong>Health</strong>-care personnel who care for severely immunocompromised persons (i.e., those<br />
who require care in a protected environment) should receive TIV rather than LAIV. Other<br />
persons should receive TIV.<br />
• The intramuscular or intradermal administered TIV are options for adults aged 18–64 years.<br />
• Adults aged 65 years and older can receive the standard dose TIV or the high-dose TIV<br />
(Fluzone High-Dose).<br />
3. Tetanus, diphtheria, and acellular pertussis (Td/Tdap) vaccination<br />
• Administer a one-time dose of Tdap to adults younger than age 65 years who have not<br />
received Tdap previously or for whom vaccine status is unknown to replace one of the 10-year<br />
Td boosters.<br />
• Tdap is specifically recommended for the following persons:<br />
— pregnant women more than 20 weeks’ gestation,<br />
— adults, regardless of age, who are close contacts of infants younger than age 12 months<br />
(e.g., parents, grandparents, or child care providers), and<br />
— health-care personnel.<br />
• Tdap can be administered regardless of interval since the most recent tetanus or diphtheriacontaining<br />
vaccine.<br />
• Pregnant women not vaccinated during pregnancy should receive Tdap immediately<br />
postpartum.<br />
• Adults 65 years and older may receive Tdap.<br />
• Adults with unknown or incomplete history of completing a 3-dose primary vaccination series<br />
with Td-containing vaccines should begin or complete a primary vaccination series. Tdap<br />
should be substituted for a single dose of Td in the vaccination series with Tdap preferred as<br />
the first dose.<br />
• For unvaccinated adults, administer the first 2 doses at least 4 weeks apart and the third dose<br />
6–12 months after the second.<br />
• If incompletely vaccinated (i.e., less than 3 doses), administer remaining doses.<br />
Refer to the ACIP statement for recommendations for administering Td/Tdap as prophylaxis in<br />
wound management (See footnote 1).<br />
4. Varicella vaccination<br />
• All adults without evidence of immunity to varicella (as defined below) should receive 2 doses<br />
of single-antigen varicella vaccine or a second dose if they have received only 1 dose.<br />
• Special consideration for vaccination should be given to those who<br />
— have close contact with persons at high risk for severe disease (e.g., health-care personnel<br />
and family contacts of persons with immunocompromising conditions) or<br />
— are at high risk for exposure or transmission (e.g., teachers; child care employees;<br />
residents and staff members of institutional settings, including correctional institutions;<br />
college students; military personnel; adolescents and adults living in households with<br />
children; nonpregnant women of childbearing age; and international travelers).<br />
• Pregnant women should be assessed for evidence of varicella immunity. Women who do not<br />
have evidence of immunity should receive the first dose of varicella vaccine upon completion or<br />
termination of pregnancy and before discharge from the health-care facility. The second dose<br />
should be administered 4–8 weeks after the first dose.<br />
• Evidence of immunity to varicella in adults includes any of the following:<br />
— documentation of 2 doses of varicella vaccine at least 4 weeks apart;<br />
— U.S.-born before 1980 (although for health-care personnel and pregnant women, birth<br />
before 1980 should not be considered evidence of immunity);<br />
— history of varicella based on diagnosis or verification of varicella by a health-care provider<br />
(for a patient reporting a history of or having an atypical case, a mild case, or both, healthcare<br />
providers should seek either an epidemiologic link to a typical varicella case or to a<br />
H EALTH PLANS<br />
www.cfhp.com<br />
15
laboratory-confirmed case or evidence of laboratory confirmation, if it was performed at the<br />
time of acute disease);<br />
— history of herpes zoster based on diagnosis or verification of herpes zoster by a health-care<br />
provider; or<br />
— laboratory evidence of immunity or laboratory confirmation of disease.<br />
5. Human papillomavirus (HPV) vaccination<br />
• Two vaccines are licensed for use in females, bivalent HPV vaccine (HPV2) and quadrivalent<br />
HPV vaccine (HPV4), and one HPV vaccine for use in males (HPV4).<br />
• For females, either HPV4 or HPV2 is recommended in a 3-dose series for routine vaccination<br />
at 11 or 12 years of age, and for those 13 through 26 years of age, if not previously vaccinated.<br />
• For males, HPV4 is recommended in a 3-dose series for routine vaccination at 11 or 12 years<br />
of age, and for those 13 through 21 years of age, if not previously vaccinated. Males 22<br />
through 26 years of age may be vaccinated.<br />
• HPV vaccines are not live vaccines and can be administered to persons who are<br />
immunocompromised as a result of infection (including HIV infection), disease, or medications.<br />
Vaccine is recommended for immunocompromised persons through age 26 years who did<br />
not get any or all doses when they were younger. The immune response and vaccine efficacy<br />
might be less than that in immunocompetent persons.<br />
• Men who have sex with men (MSM) might especially benefit from vaccination to prevent<br />
condyloma and anal cancer. HPV4 is recommended for MSM through age 26 years who did<br />
not get any or all doses when they were younger.<br />
• Ideally, vaccine should be administered before potential exposure to HPV through sexual<br />
activity; however, persons who are sexually active should still be vaccinated consistent with<br />
age-based recommendations. HPV vaccine can be administered to persons with a history of<br />
genital warts, abnormal Papanicolaou test, or positive HPV DNA test.<br />
• A complete series for either HPV4 or HPV2 consists of 3 doses. The second dose should be<br />
administered 1–2 months after the first dose; the third dose should be administered 6 months<br />
after the first dose (at least 24 weeks after the first dose).<br />
• Although HPV vaccination is not specifically recommended for health-care personnel<br />
(HCP) based on their occupation, HCP should receive the HPV vaccine if they are in the<br />
recommended age group.<br />
6. Zoster vaccination<br />
• A single dose of zoster vaccine is recommended for adults 60 years of age and older<br />
regardless of whether they report a prior episode of herpes zoster. Although the vaccine is<br />
licensed by the Food and Drug Administration (FDA) for use among and can be administered to<br />
persons 50 years and older, ACIP recommends that vaccination begins at 60 years of age.<br />
• Persons with chronic medical conditions may be vaccinated unless their condition constitutes a<br />
contraindication, such as pregnancy or severe immunodeficiency.<br />
• Although zoster vaccination is not specifically recommended for health-care personnel (HCP),<br />
HCP should receive the vaccine if they are in the recommended age group.<br />
7. Measles, mumps, rubella (MMR) vaccination<br />
• Adults born before 1957 generally are considered immune to measles and mumps. All adults<br />
born in 1957 or later should have documentation of 1 or more doses of MMR vaccine unless<br />
they have a medical contraindication to the vaccine, laboratory evidence of immunity to each of<br />
the three diseases, or documentation of provider-diagnosed measles or mumps disease. For<br />
rubella, documentation of provider-diagnosed disease is not considered acceptable evidence of<br />
immunity.<br />
Measles component:<br />
• A routine second dose of MMR vaccine, administered a minimum of 28 days after the first<br />
dose, is recommended for adults who<br />
— are students in postsecondary educational institutions;<br />
— work in a health-care facility; or<br />
— plan to travel internationally.<br />
• Persons who received inactivated (killed) measles vaccine or measles vaccine of unknown<br />
type from 1963 to 1967 should be revaccinated with 2 doses of MMR vaccine.<br />
Mumps component:<br />
• A routine second dose of MMR vaccine, administered a minimum of 28 days after the first<br />
dose, is recommended for adults who<br />
— are students in postsecondary educational institutions;<br />
— work in a health-care facility; or<br />
— plan to travel internationally.<br />
• Persons vaccinated before 1979 with either killed mumps vaccine or mumps vaccine of<br />
unknown type who are at high risk for mumps infection (e.g., persons who are working in a<br />
health-care facility) should be considered for revaccination with 2 doses of MMR vaccine.<br />
— persons working with HAV-infected primates or with HAV in a research laboratory setting;<br />
— persons with chronic liver disease and persons who receive clotting factor concentrates;<br />
— persons traveling to or working in countries that have high or intermediate endemicity of<br />
hepatitis A; and<br />
— unvaccinated persons who anticipate close personal contact (e.g., household or regular<br />
babysitting) with an international adoptee during the first 60 days after arrival in the United<br />
States from a country with high or intermediate endemicity. (See footnote 1 for more<br />
information on travel recommendations). The first dose of the 2-dose hepatitis A vaccine<br />
series should be administered as soon as adoption is planned, ideally 2 or more weeks<br />
before the arrival of the adoptee.<br />
• Single-antigen vaccine formulations should be administered in a 2-dose schedule at either<br />
0 and 6–12 months (Havrix), or 0 and 6–18 months (Vaqta). If the combined hepatitis A and<br />
hepatitis B vaccine (Twinrix) is used, administer 3 doses at 0, 1, and 6 months; alternatively,<br />
a 4-dose schedule may be used, administered on days 0, 7, and 21–30 followed by a booster<br />
dose at month 12.<br />
12. Hepatitis B vaccination<br />
• Vaccinate persons with any of the following indications and any person seeking protection<br />
from hepatitis B virus (HBV) infection:<br />
— sexually active persons who are not in a long-term, mutually monogamous relationship<br />
(e.g., persons with more than one sex partner during the previous 6 months); persons<br />
seeking evaluation or treatment for a sexually transmitted disease (STD); current or recent<br />
injection-drug users; and men who have sex with men;<br />
— health-care personnel and public-safety workers who are exposed to blood or other<br />
potentially infectious body fluids;<br />
— persons with diabetes younger than 60 years as soon as feasible after diagnosis; persons<br />
with diabetes who are 60 years or older at the discretion of the treating clinician based on<br />
increased need for assisted blood glucose monitoring in long-term care facilities, likelihood<br />
of acquiring hepatitis B infection, its complications or chronic sequelae, and likelihood of<br />
immune response to vaccination;<br />
— persons with end-stage renal disease, including patients receiving hemodialysis; persons<br />
with HIV infection; and persons with chronic liver disease;<br />
— household contacts and sex partners of persons with chronic HBV infection; clients and<br />
staff members of institutions for persons with developmental disabilities; and international<br />
travelers to countries with high or intermediate prevalence of chronic HBV infection; and<br />
— all adults in the following settings: STD treatment facilities; HIV testing and treatment<br />
facilities; facilities providing drug-abuse treatment and prevention services; healthcare<br />
settings targeting services to injection-drug users or men who have sex with<br />
men; correctional facilities; end-stage renal disease programs and facilities for chronic<br />
hemodialysis patients; and institutions and nonresidential daycare facilities for persons with<br />
developmental disabilities.<br />
• Administer missing doses to complete a 3-dose series of hepatitis B vaccine to those persons<br />
not vaccinated or not completely vaccinated. The second dose should be administered 1<br />
month after the first dose; the third dose should be given at least 2 months after the second<br />
dose (and at least 4 months after the first dose). If the combined hepatitis A and hepatitis B<br />
vaccine (Twinrix) is used, give 3 doses at 0, 1, and 6 months; alternatively, a 4-dose Twinrix<br />
schedule, administered on days 0, 7, and 21–30 followed by a booster dose at month 12 may<br />
be used.<br />
• Adult patients receiving hemodialysis or with other immunocompromising conditions should<br />
receive 1 dose of 40 μg/mL (Recombivax HB) administered on a 3-dose schedule or 2 doses<br />
of 20 μg/mL (Engerix-B) administered simultaneously on a 4-dose schedule at 0, 1, 2, and 6<br />
months.<br />
13. Selected conditions for which Haemophilus influenzae type b (Hib) vaccine may be used<br />
• 1 dose of Hib vaccine should be considered for persons who have sickle cell disease,<br />
leukemia, or HIV infection, or who have anatomic or functional asplenia if they have not<br />
previously received Hib vaccine.<br />
14. Immunocompromising conditions<br />
• Inactivated vaccines generally are acceptable (e.g., pneumococcal, meningococcal, and<br />
influenza [inactivated influenza vaccine]), and live vaccines generally are avoided in persons<br />
with immune deficiencies or immunocompromising conditions. Information on specific<br />
conditions is available at http://www.cdc.gov/vaccines/pubs/acip-list.htm.<br />
16 H EALTH PLANS<br />
www.cfhp.com
CFHP has adopted the National Asthma Education and Prevention Program Expert Panel Report 3: guidelines for the diagnosis<br />
and management of asthma -2007. This guideline updates a previous version: Expert Panel Report 2: guidelines for the diagnosis<br />
and management of asthma and its update on selected topics in 2002. Bethesda (MD): U.S. Department of <strong>Health</strong> and Human<br />
Services, Public <strong>Health</strong> Service, National Institutes of <strong>Health</strong>, National Heart, Lung and Blood Institute; 1997 JulCopies of the<br />
complete NAEPP guidelines are available at their web site http://www.nhlbi.nih.gov/guidelines/asthma/index.htm or from CFHP.<br />
The 2007 NAEPP Expert Panel identified questions about asthma management in four main catergories: Assesing and<br />
Monitoring Asthma Severity and Asthma Control, Education for a Partnership in Care, Control of Environmental Factors and<br />
Comorbid Conditions that Affect Asthma, and Medications. The <strong>Guidelines</strong> updated guidelines also focused on Stepwise<br />
Approach for Manageing Asthma and Managing Exacerbations. Some key topics in each category include:<br />
• Assessing and Monitoring Asthma Severity and Astma Control<br />
• Utilizes multiple measures of the patient’s level of current impairment and future risks.<br />
• Stress to look for those at high risk for frequent exacerbations even though appear to have low day-to-day effects<br />
of asthma.<br />
• Education for a Partnership in Care<br />
• Patient skills to self-monitor and manage asthma<br />
• Use of a written asthma action plan.<br />
• Recommendations on educational opportunities in a variety of settings<br />
• Clinician education programs to improve patient-provider communication.<br />
• Control of Environmental Factors and Comorbid Conditions that Affect Asthma<br />
• Allergans and Irritants<br />
• Comorbid conditions<br />
• Medications<br />
• General Mechanisms and Role in Therapy<br />
• Delivery Devices for Inhaled Medications<br />
• Safety Issues for Inhaled Cortisosteroids and Long-Acting Beta2–Agonists<br />
• Stepwise Approach for Managing Asthma<br />
• Stepwise Treatment Recommendations for Differnet Ages<br />
1. Steps for Children 0-4 Years of Age<br />
2. Steps for Children 5-11 Years of Age<br />
3. Steps for Youths > 12 Years of Age and Adults<br />
• Manging Special Situations<br />
1. Exercise-Induced Bronchospasm<br />
2. Pregnancy<br />
3. Surgery<br />
4. Disparities<br />
• Managing Exacerbations<br />
• Classifying Severity<br />
• Home Management<br />
• Management in the Urgent or Emergency Care and Hospital Settings<br />
4.1 Asthma Disease Management<br />
The foundation of care for asthma can be summarized in nine key points.<br />
1. Conduct a detailed medical history, physical examination and pulmonary function tests (PFT).<br />
2. Tailor asthma treatment plan to the needs of the individual patient.<br />
3. Provide written self-management plan and tools for self-management.<br />
4. Gain control as quickly as possible; then decrease medication to the least necessary.<br />
5. Provide asthma education to patient and caregivers.<br />
6. Teach proper inhaler technique.<br />
7. Control environmental and other factors contributing to asthma severity.<br />
8. Review treatment every 1 – 6 months, depending on severity. If control is sustained for at least 3 months, consider gradual<br />
reduction in treatment. If control is not achieved, consider step-up in treatment after reviewing patient compliance,<br />
medication use technique and control of allergens/trigger factors.<br />
9. Consultation with an asthma specialist is recommended for unstable or complex patients.<br />
ACAAI Asthma Disease Management Resource Manual, October 1997.<br />
H EALTH PLANS<br />
www.cfhp.com<br />
17
History may include cough, wheezing, chest tightness, shortness of breath and/or exercise intolerance. Children may report<br />
chest pain or nighttime coughing as their presenting symptoms. Asthma may be suspected by observing wheezing or<br />
auscultating prolonged expirations.<br />
Asymptomatic patients may give history of prior episodes of cough, wheezing, or exercise intolerance. These patients may not<br />
have physical exam findings of asthma. Some patients may deny active asthma and have wheezing or prolonged expirations on<br />
exam.<br />
Most patients suspected of asthma should have pulmonary function testing (PFT). This may not be obtainable on children<br />
under 5 years of age. PFT done before and after inhaled bronchodilators will often support the diagnosis of asthma, however,<br />
the lack of response does not rule out asthma. Other maneuvers may demonstrate reversibility, such as 5 – 10 day course<br />
of oral steroids followed by repeat PFT (specialty consultation is recommended). For patients with normal or near-normal<br />
PFT, provocative testing (i.e. methacholine challenge) may be indicated. Alternatively, home peak flow monitoring may<br />
demonstrate intraday variations consistent with asthma.<br />
When patients present with history, physical exam or lab findings of asthma, a chest X-Ray (CXR) within the past year<br />
is indicated for adults. Preview of a previous normal CXR may be adequate for children. When an asthma diagnosis is<br />
substantiated, patients should be categorized according to the NHI guidelines as intermittent, mild persistent, moderate<br />
persistent, or severe persistent.<br />
Home Peak Flow Monitoring: Home peak flow monitoring may demonstrate intraday variability consistent with a diagnosis<br />
of asthma. During a period of 2 –3 weeks, peak expiratory flow (PEF) should be recorded at least twice a day. If patient uses<br />
a bronchodilator, PEF should be recorded before and after treatment. The personal best is the highest PEF achieved. If the<br />
personal best is less than 80% of predicted or daily variability is more than 15% after adequate bronchodilator, more aggressive<br />
therapy and continued daily monitoring are indicated.<br />
Day-to-day variability of PEF provides a reasonable index of asthma stability and/or severity. This can be calculated from at least<br />
two values (AM and PM) before and after bronchodilators (if patient is on bronchodilators):<br />
Average Daily Variability = (highest PEF – lowest PEF) x 100 / Highest PEF.<br />
Variability greater than 15% supports a diagnosis of asthma.<br />
18 H EALTH PLANS<br />
www.cfhp.com
Patient Name ________________________________________________________________________<br />
Chart No. ____________________________________________ DOB _________________________<br />
Asthma Symptoms<br />
Current exacerbation? YES NO YES NO YES NO YES NO<br />
Hosp for Asthma since last visit? YES NO YES NO YES NO YES NO<br />
ER for Asthma since last visit? YES NO YES NO YES NO YES NO<br />
Wheeze, cough, SOB, chest tightness (days/wk) YES NO YES NO YES NO YES NO<br />
Night cough, wheeze, SOB, chest tightness YES NO YES NO YES NO YES NO<br />
(night/wk)<br />
Cough / wheeze w/exercise YES NO YES NO YES NO YES NO<br />
Freq of β – agonist use? (days/wk) YES NO YES NO YES NO YES NO<br />
Peak flow (best / predicted) YES NO YES NO YES NO YES NO<br />
Physical Exam<br />
Asthma Flow Sheet<br />
HEENT<br />
Chest<br />
Current Symptoms<br />
Severity of Asthma M. Int M. Pers<br />
Moderate<br />
Severe<br />
M. Int M. Pers<br />
Moderate<br />
Severe<br />
M. Int M. Pers<br />
Moderate<br />
Severe<br />
M. Int M. Pers<br />
Moderate<br />
Severe<br />
Medications<br />
Albuterol (type/dose/freq)<br />
Long acting β – agonist<br />
Inhaled corticosteroid<br />
Combination drugs<br />
Cromolyn / Nedocromil<br />
Leukotriene modifer<br />
Systemic steroid<br />
Astihistamine<br />
Nasal steroid<br />
Other<br />
Flu shot YES NO YES NO YES NO YES NO<br />
Referral (specialist) YES NO YES NO YES NO YES NO<br />
Education<br />
Plan given/reviewed YES NO YES NO YES NO YES NO<br />
Allergen control YES NO YES NO YES NO YES NO<br />
How to use MDI YES NO YES NO YES NO YES NO<br />
How to use spacer YES NO YES NO YES NO YES NO<br />
How to use PFMeter YES NO YES NO YES NO YES NO<br />
How to use nebulizer YES NO YES NO YES NO YES NO<br />
Signature _________________________________________________________________ Initials _______<br />
H EALTH PLANS<br />
www.cfhp.com<br />
19
40 <strong>Guidelines</strong> for the Diagnosis and Management of Asthma<br />
FIGURE 11. CLASSIFYING ASTHMA SEVERITY AND INITIATING THERAPY IN CHILDREN<br />
Key: FEV 1 ,forced expiratory volume<br />
in 1 second; FVC, forced vital capacity;<br />
ICS, inhaled corticosteroids; ICU,<br />
intensive care unit; N/A, not applicable<br />
Notes:<br />
■ Level of severity is determined by<br />
both impairment and risk. Assess<br />
impairment domain by caregiver’s<br />
recall of previous 2–4 weeks.<br />
Assign severity to the most severe<br />
category in which any feature<br />
occurs.<br />
■ Frequency and severity of exacerbations<br />
may fluctuate over time for<br />
patients in any severity category.<br />
At present, there are inadequate<br />
data to correspond frequencies<br />
of exacerbations with different<br />
levels of asthma severity. In general,<br />
more frequent and severe exacerbations<br />
(e.g., requiring urgent,<br />
unscheduled care, hospitalization,<br />
or ICU admission) indicate greater<br />
underlying disease severity. For<br />
treatment purposes, patients with ≥2<br />
exacerbations described above may<br />
be considered the same as patients<br />
who have persistent asthma, even in<br />
the absence of impairment levels<br />
consistent with persistent asthma.<br />
4.3 Classifying Asthma Severity and Initiating Therapy In Children<br />
20 H EALTH PLANS<br />
www.cfhp.com
Managing Asthma Long Term<br />
41<br />
FIGURE 12. ASSESSING ASTHMA CONTROL AND ADJUSTING THERAPY IN CHILDREN<br />
Key: EIB, exercise-induced bronchospasm,<br />
FEV 1 ,forced expiratory<br />
volume in 1 second; FVC, forced vital<br />
capacity; ICU, intensive care unit;<br />
N/A, not applicable<br />
Notes:<br />
■ The level of control is based on the<br />
most severe impairment or risk<br />
category. Assess impairment<br />
domain by patient’s or caregiver’s<br />
recall of previous 2–4 weeks.<br />
Symptom assessment for longer<br />
periods should reflect a global<br />
assessment, such as whether<br />
the patient’s asthma is better or<br />
worse since the last visit.<br />
■ At present, there are inadequate<br />
data to correspond frequencies of<br />
exacerbations with different levels of<br />
asthma control. In general, more<br />
frequent and intense exacerbations<br />
(e.g., requiring urgent, unscheduled<br />
care, hospitalization, or ICU<br />
admission) indicate poorer<br />
disease control.<br />
4.4 Assessing Asthma Contraol and Adjusting Therapy in Children<br />
H EALTH PLANS<br />
www.cfhp.com<br />
21
4.5 Stepwise Approach for Managing Asthma Long Term in Children<br />
FIGURE 13. STEPWISE APPROACH FOR MANAGING ASTHMA LONG TERM IN CHILDREN, 0–4 YEARS OF AGE AND 5–11 YEARS OF AGE<br />
42 <strong>Guidelines</strong> for the Diagnosis and Management of Asthma<br />
22 H EALTH PLANS<br />
www.cfhp.com
FIGURE 14. CLASSIFYING ASTHMA SEVERITY AND INITIATING TREATMENT IN YOUTHS 12 YEARS OF AGE AND ADULTS<br />
Assessing severity and initiating treatment for patients who are not currently taking<br />
long-term control medications<br />
Key: EIB, exercise-induced bronchospasm,<br />
FEV1, forced expiratory<br />
volume in 1 second; FVC, forced vital<br />
capacity; ICU, intensive care unit<br />
Notes:<br />
• The stepwise approach is meant to<br />
assist, not replace, the clinical<br />
decisionmaking required to meet<br />
individual patient needs.<br />
• Level of severity is determined by<br />
assessment of both impairment and<br />
risk. Assess impairment domain by<br />
patient’s/caregiver’s recall of<br />
previous 2–4 weeks and spirometry.<br />
Assign severity to the most severe<br />
category in which any feature<br />
occurs.<br />
• At present, there are inadequate<br />
data to correspond frequencies of<br />
exacerbations with different levels<br />
of asthma severity. In general, more<br />
frequent and intense exacerbations<br />
(e.g., requiring urgent, unscheduled<br />
care, hospitalization, or ICU<br />
admission) indicate greater<br />
underlying disease severity. For<br />
treatment purposes, patients who<br />
had ≥2 exacerbations requiring oral<br />
systemic corticosteroids in the past<br />
year may be considered the same<br />
as patients who have persistent<br />
asthma, even in the absence of<br />
impairment levels consistent with<br />
persistent asthma.<br />
4.6 Classifying Asthma Severity and Initiating Treatment in Youths & Adults<br />
Managing Asthma Long H EALTH Term PLANS43<br />
www.cfhp.com<br />
23
<strong>Guidelines</strong> for the Diagnosis and Management of Asthma<br />
FIGURE 15. ASSESSING ASTHMA CONTROL AND ADJUSTING THERAPY IN YOUTHS ≥12 YEARS OF AGE AND ADULTS<br />
*ACQ values of 0.76–1.4 are indeterminate regarding<br />
well-controlled asthma.<br />
Key: EIB, exercise-induced bronchospasm; ICU, intensive care<br />
unit<br />
Notes:<br />
• The stepwise approach is meant to assist, not replace,<br />
the clinical decisionmaking required to meet individual<br />
patient needs.<br />
• The level of control is based on the most severe impairment<br />
or risk category. Assess impairment domain by<br />
patient’s recall of previous 2–4 weeks and by<br />
spirometry/or peak flow measures. Symptom assessment<br />
for longer periods should reflect a global assessment, such<br />
as inquiring whether the patient’s asthma is better or<br />
worse since the last visit.<br />
• At present, there are inadequate data to correspond frequencies<br />
of exacerbations with different levels of asthma<br />
control. In general, more frequent and intense<br />
exacerbations (e.g., requiring urgent, unscheduled care,<br />
hospitalization, or ICU admission) indicate poorer disease<br />
control. For treatment purposes, patients who had ≥2<br />
exacerbations requiring oral systemic corticosteroids in the<br />
past year may be considered the same as patients who<br />
have not-well-controlled asthma, even in the absence of<br />
impairment levels consistent with not-well-controlled asthma.<br />
ATAQ = Asthma Therapy Assessment Questionnaire ©<br />
ACQ = Asthma Control Questionnaire ©<br />
ACT = Asthma Control Test<br />
Minimal Important<br />
Difference: 1.0 for the ATAQ; 0.5 for the ACQ; not<br />
determined for the ACT.<br />
Before step up in therapy:<br />
— Review adherence to medication, inhaler technique,<br />
environmental control, and comorbid conditions.<br />
— If an alternative treatment option was used in a step,<br />
discontinue and use the preferred treatment for that step.<br />
4.7 Assessing Asthma Control and Adjusting Therapy in Youths and Adults<br />
24 H EALTH PLANS<br />
www.cfhp.com
FIGURE 16. STEPWISE APPROACH FOR MANAGING ASTHMA IN YOUTHS ≥12 YEARS OF AGE AND ADULTS<br />
Key: Alphabetical order is used when more than one<br />
treatment option is listed within either preferred or<br />
alternative therapy. ICS, inhaled corticosteroid; LABA, longacting<br />
inhaled beta 2 -agonist; LTRA, leukotriene receptor<br />
antagonist; SABA, inhaled short-acting beta 2 -agonist<br />
Notes:<br />
• The stepwise approach is meant to assist, not replace, the<br />
clinical decisionmaking required to meet individual patient<br />
needs.<br />
• If alternative treatment is used and response is inadequate,<br />
discontinue it and use the preferred treatment before<br />
stepping up.<br />
• Zileuton is a less desirable alternative due to limited<br />
studies as adjunctive therapy and the need to monitor<br />
liver function. Theophylline requires monitoring of serum<br />
concentration levels.<br />
• In step 6, before oral corticosteroids are introduced, a trial<br />
of high-dose ICS + LABA + either LTRA, theophylline, or<br />
zileuton may be considered, although this approach has<br />
not been studied in clinical trials.<br />
• Step 1, 2, and 3 preferred therapies are based on Evidence<br />
A; step 3 alternative therapy is based on Evidence A for<br />
LTRA, Evidence B for theophylline, and Evidence D for<br />
zileuton. Step 4 preferred therapy is based on Evidence B,<br />
and alternative therapy is based on Evidence B for LTRA<br />
and theophylline and Evidence D zileuton. Step 5<br />
preferred therapy is based on Evidence B. Step 6 preferred<br />
therapy is based on (EPR—2 1997) and Evidence B for<br />
omalizumab.<br />
• Immunotherapy for steps 2–4 is based on Evidence B for<br />
house-dust mites, animal danders, and pollens; evidence is<br />
weak or lacking for molds and cockroaches. Evidence is<br />
strongest for immunotherapy with single allergens. The role<br />
of allergy in asthma is greater in children than in adults.<br />
• Clinicians who administer immunotherapy or omalizumab<br />
should be prepared and equipped to identify and treat<br />
anaphylaxis that may occur.<br />
Managing Asthma Long Term<br />
45<br />
4.8 Stepwise Approach for Managing Asthma in Youth and Adults<br />
H EALTH PLANS<br />
www.cfhp.com<br />
25
4.9 Estimated Comparative Daily Dosages for Inhaled Corticosteroids<br />
FIGURE 18. ESTIMATED COMPARATIVE DAILY DOSAGES FOR INHALED CORTICOSTEROIDS<br />
Drug<br />
Beclomethasone HFA<br />
40 or 80 mcg/puff<br />
Budesonide DPI<br />
90, 180, or 200<br />
mcg/inhalation<br />
Budesonide Inhaled<br />
Inhalation suspension<br />
for nebulization<br />
Flunisolide<br />
250 mcg/puff<br />
Flunisolide HFA<br />
80 mcg/puff<br />
Fluticasone<br />
HFA/MDI: 44, 110, or<br />
220 mcg/puff<br />
DPI: 50, 100, or<br />
250 mcg/inhalation<br />
Mometasone DPI<br />
200 mcg/inhalation<br />
Triamcinolone<br />
acetonide<br />
75 mcg/puff<br />
NA<br />
NA<br />
0.25–0.5 mg<br />
NA<br />
NA<br />
176 mcg<br />
NA<br />
NA<br />
NA<br />
80–160 mcg<br />
180–400 mcg<br />
0.5 mg<br />
500–750 mcg<br />
160 mcg<br />
88–176 mcg<br />
100–200 mcg<br />
NA<br />
300–600 mcg<br />
80–240 mcg<br />
180–600 mcg<br />
NA<br />
500–1,000 mcg<br />
320 mcg<br />
88–264 mcg<br />
100–300 mcg<br />
200 mcg<br />
300–750 mcg<br />
NA<br />
NA<br />
>0.5–1.0 mg<br />
NA<br />
NA<br />
>176–352 mcg<br />
NA<br />
NA<br />
NA<br />
Key: DPI, dry power inhaler; HFA, hydrofluoroalkane; MDI, metered-dose inhaler; NA, not available (either not approved, no data available, or safety and efficacy not established for this age group)<br />
Therapeutic Issues:<br />
Child 0–4<br />
Years of Age<br />
>160–320 mcg<br />
>400–800 mcg<br />
1.0 mg<br />
1,000–<br />
1,250 mcg<br />
320 mcg<br />
>176–352 mcg<br />
>200–400 mcg<br />
NA<br />
>600–900 mcg<br />
>240–480 mcg<br />
>600–<br />
1,200 mcg<br />
NA<br />
>1,000–<br />
2,000 mcg<br />
>320–640 mcg<br />
>264–440 mcg<br />
>300–500 mcg<br />
400 mcg<br />
>750–<br />
1,500 mcg<br />
NA<br />
NA<br />
>1.0 mg<br />
NA<br />
NA<br />
>352 mcg<br />
NA<br />
NA<br />
NA<br />
>320 mcg<br />
>800 mcg<br />
2.0 mg<br />
>1,250 mcg<br />
≥640 mcg<br />
>352 mcg<br />
>400 mcg<br />
NA<br />
>900 mcg<br />
>480 mcg<br />
>1,200 mcg<br />
NA<br />
>2,000 mcg<br />
>640 mcg<br />
>440 mcg<br />
>500 mcg<br />
>400 mcg<br />
>1,500 mcg<br />
■ The most important determinant of appropriate dosing is the clinician’s judgment of the patient’s response to therapy. The clinician must monitor the patient’s response on several<br />
clinical parameters and adjust the dose accordingly. Once control of asthma is achieved, the dose should be carefully titrated to the minimum dose required to maintain control.<br />
■ Preparations are not interchangeable on a mcg or per puff basis. This figure presents estimated comparable daily doses. See EPR—3 <strong>Full</strong> Report 2007 for full discussion.<br />
■ Some doses may be outside package labeling, especially in the high-dose range. Budesonide nebulizer suspension is the only inhaled corticosteroid (ICS) with FDA-approved<br />
labeling for children
FIGURE 20. CLASSIFYING SEVERITY OF ASTHMA EXACERBATIONS IN THE URGENT OR EMERGENCY CARE SETTING<br />
Note: Patients are instructed to use quick-relief medications if symptoms occur or if PEF drops below 80 percent predicted or personal best. If<br />
PEF is 50–79 percent, the patient should monitor response to quick-relief medication carefully and consider contacting a clinician. If PEF is below<br />
50 percent, immediate medical care is usually required. In the urgent or emergency care setting, the following parameters describe the severity<br />
and likely clinical course of an exacerbation.<br />
Mild<br />
Moderate<br />
Severe<br />
Subset: Life<br />
threatening<br />
Symptoms and Signs<br />
Dyspnea only with<br />
activity (assess<br />
tachypnea in young<br />
children)<br />
Dyspnea interferes with<br />
or limits usual activity<br />
Dyspnea at rest;<br />
interferes with<br />
conversation<br />
Too dyspneic to speak;<br />
perspiring<br />
Initial PEF (or FEV1)<br />
PEF ≥ 70 percent<br />
predicted or personal best<br />
<strong>Clinical</strong> Course<br />
■<br />
■<br />
■<br />
■<br />
■<br />
■<br />
■<br />
■<br />
■<br />
■<br />
■<br />
■<br />
■<br />
■<br />
Usually cared for at home<br />
Prompt relief with inhaled SABA<br />
Possible short course of oral<br />
systemic corticosteroids<br />
Usually requires office or ED visit<br />
Relief from frequent inhaled SABA<br />
Oral systemic corticosteroids;<br />
some symptoms last for<br />
1–2 days after treatment is begun<br />
Usually requires ED visit and<br />
likely hospitalization<br />
Partial relief from frequent<br />
inhaled SABA<br />
Oral systemic corticosteroids;<br />
some symptoms last for<br />
>3 days after treatment is begun<br />
Adjunctive therapies are helpful<br />
Requires ED/hospitalization;<br />
possible ICU<br />
Minimal or no relief from<br />
frequent inhaled SABA<br />
Intravenous corticosteroids<br />
Adjunctive therapies are helpful<br />
Key: ED, emergency department; FEV 1 , forced expiratory volume in 1 second; ICU, intensive care unit; PEF, peak expiratory flow;<br />
SABA, short-acting beta 2 -agonist<br />
Management in the Urgent or Emergency Care and<br />
Hospital Settings<br />
Emergency medical services providers should have<br />
prehospital protovols that allow administration of<br />
SABA, supplemental oxygen, and (with appropriate<br />
medical oversight) anticholinergics and oral systemic<br />
corticosteriods to patients who have signs or symptoms<br />
of an asthma exacerbation.<br />
Treatment strategies for managing moderate or severe<br />
exacerbations in the urgent or emergency care setting<br />
are described below. Also see figure 21 for a detailed<br />
sequence of recommended actions for monitoring<br />
and treatment and figure 22 for dosages of drugs for<br />
asthma exacerbations.<br />
PEF 40–69 percent<br />
predictedor personal<br />
best<br />
PEF
5.1 Attention-Deficit Hyperactivity Disorder <strong>Clinical</strong> Practice <strong>Guidelines</strong><br />
Introduction: In our ongoing effort to improve consumer/patient and provider satisfaction, quality of care, and access to the<br />
most appropriate level and intensity of treatment, <strong>Community</strong> <strong>First</strong> has adopted the following clinical practice guidelines for<br />
Attention-Deficit/Hyperactivity Disorder. <strong>Community</strong> <strong>First</strong>’s guidelines are based upon scientific evidence and knowledge<br />
from the following resources: DSM-IV-TM, Diagnostic and Statistical Manual for Mental Disorders, Fourth Edition, American<br />
Psychiatric Association, 2000; “ Practice Parameters for the Assessment and Treatment of Children, Adolescents and Adults<br />
with Attention-Deficit/Hyperactivity Disorder”, Journal of the American Academy of Child and Adolescent Psychiatry,<br />
Washington DC, October 1997; and InterQual Behavioral <strong>Health</strong> Psychiatry Level of Care Criteria 2006.<br />
Attention-Deficit/Hyperactivity Disorder, Combined Type<br />
• Criteria for both inattention and hyperactivity/impulsivity are met for the past 6 months.<br />
Attention-Deficit/Hyperactivity Disorder, Predominantly Inattentive Type<br />
• Criteria for only inattention are met for the past 6 months.<br />
Attention-Deficit/Hyperactivity Disorder, Predominantly Hyperactive-Impulsive Type<br />
• Criteria for hyperactivity impulsivity are met for the past 6 months.<br />
Attention-Deficit/Hyperactivity Disorder, Not Otherwise Specified<br />
• This category is for disorders with prominent symptoms of inattention or hyperactivity/impulsivity that do not meet<br />
criteria for Attention-Deficit/Hyperactivity Disorder.<br />
For individuals, especially adolescents and adults, who currently have symptoms that no longer meet full criteria, “In Partial<br />
Remission” should be specified.<br />
Diagnostic Criteria:<br />
I. Either A or B:<br />
A. Six (or more) of the following symptoms of inattention have persisted for at least 6 months to a degree that is maladaptive<br />
and inconsistent with developmental level:<br />
Inattention:<br />
1. often fails to give close attention to details or makes careless mistakes in schoolwork, work, or other activities<br />
2. often has difficulty sustaining attention in tasks or play activities<br />
3. often does not seem to listen when spoken to directly<br />
4. often does not follow through on instructions and fails to finish schoolwork, chores, or duties in the workplace (not due<br />
to oppositional behavior or failure to understand instructions)<br />
5. often has difficulty organizing tasks and activities<br />
6. often avoids, dislikes or is reluctant to engage in tasks that require sustained mental effort (such as schoolwork or<br />
homework)<br />
7. often loses things necessary for tasks or activities (eg., toys, school assignments, pencils, books, or tools)<br />
8. is often easily distracted by extraneous stimuli<br />
9. is often forgetful in daily activities<br />
B. Six (or more) of the following symptoms of hyperactivity-impulsivity have persisted for at least 6 months to a degree that is<br />
maladaptive and inconsistent with developmental level:<br />
Hyperactivity:<br />
1. often fidgets with hands or feet or squirms in seat<br />
2. often leaves seat in classroom or in other situations in which remaining seated is expected<br />
3. often runs about or climbs excessively in situations in which it is inappropriate (in adolescents or adults, may be limited<br />
to subjective feeling of restlessness)<br />
4. often has difficulty playing or engaging in leisure activities quietly<br />
5. is often “on the go” or often acts as if “driven by a motor”<br />
6. often talks excessively<br />
Impulsivity:<br />
1. often blurts out answers before questions have been completed<br />
2. often has difficulty awaiting turn<br />
3. often interrupts or intrudes on others (eg., butts into conversations or games)<br />
28 H EALTH PLANS<br />
www.cfhp.com
II.<br />
Some hyperactive-impulsive or inattentive symptoms that caused impairment were present before age 7 years. However,<br />
at times inattentiveness specifically may not be noticed prior to age 7.<br />
III. Some impairment from the symptoms is present in two or more settings (eg., at school or work and at home).<br />
IV. There must be clear evidence of clinically significant impairment in social, academic, or occupational functioning.<br />
V. The symptoms do not occur exclusively during the course of a Pervasive Developmental Disorder, Schizophrenia, or other<br />
Psychotic Disorder and are not better accounted for by another mental disorder (eg., Mood Disorder, Anxiety Disorder,<br />
Dissociative Disorder, or a Personality Disorder).<br />
There are no known specific laboratory or other diagnostic tests that establish, confirm or rule out Attention-Deficit/<br />
Hyperactivity Disorder.<br />
The most accepted and effective ways of diagnosing ADHD are through:<br />
1. Reports from guardian; parents, grandparents, caretakers, spouses, other significant individuals.<br />
2. Reports from individuals from the school, day care, work place, and other physicians.<br />
3. <strong>Clinical</strong> interview<br />
4. Legal system; probation officer, court<br />
5. Physical examination to rule out physical causes for the symptoms<br />
The optimal approach/treatment for Attention-Deficit/Hyperactivity Disorder is a multiple-modality approach that combines<br />
psychosocial interventions and medical interventions.<br />
1. Psychosocial Interventions<br />
• Family-Focused Interventions<br />
• Parent education<br />
• Parent management training<br />
• Parent support groups ie. CHADD<br />
• Family Counseling<br />
• Child-Focused Intervention<br />
• Individual counseling<br />
• Social Skills training<br />
• School focused interventions (consultation with school personnel)<br />
2. Medications<br />
• Stimulants: Ritalin (LA), Adderall (XR), Dexedrine, Metadate (CD/ER), Focalin, Concerta,<br />
• Antidepressants: Imipramine, Wellbutrin, Effexor<br />
• Alpha 2 Agonist: Tenex, Clonidine<br />
• Selective norepinephrine reuptake inhibitor: Strattera<br />
When Attention-Deficit/Hyperactivity Disorder is Comorbid with other Disorders:<br />
1. Oppositional Defiant Disorder<br />
2. Conduct Disorder<br />
3. Depressive Disorders<br />
4. Bipolar Disorder<br />
5. Anxiety Disorders<br />
6. Learning Disorders<br />
7. Substance Abuse Disorders<br />
It is optimal to inform guardians that medication for ADHD does not usually impact those behaviors resulting from the above<br />
listed disorders. Treatment should include those listed for ADHD but may include more intense interventions.<br />
Psychological Testing is not utilized to diagnose ADHD, however, it may be indicated for ruling out other psychiatric disorders.<br />
Educational Testing is not indicated to diagnose ADHD, however, school resources should be utilized if educational testing is<br />
indicated for school placement.<br />
H EALTH PLANS<br />
www.cfhp.com<br />
29
Treatment Intensity:<br />
1. Outpatient<br />
a. If the patient is being seen by a non-psychiatrist behavioral health provider and continues to have ADHD symptoms,<br />
the patient may have a comorbid condition and should be referred to a psychiatrist for a psychiatric evaluation.<br />
b. If the patient is being seen by a non-psychiatrist physician and is on stimulants, tricyclic antidepressants, or other<br />
medications used to treat ADHD and not showing a response the patient may have a comorbid condition and should<br />
be referred to a psychiatrist for a psychiatric evaluation.<br />
2. Inpatient<br />
In general, patients with an Axis I diagnosis of ADHD do not require hospitalization, however, if a comorbid Axis I<br />
diagnosis is identified psychiatric hospitalization may be warranted.<br />
Inpatient intensity of treatment is warranted when a patient meets the <strong>Community</strong> <strong>First</strong> Utilization Review Criteria for<br />
admission to an acute inpatient facility including:<br />
• Presence of a DSM IV Axis I diagnosis; and<br />
• GAF
COMMUNITY FIRST HEALTH PLANS<br />
BEHAVIORAL HEALTH MEDICAL RECORD DOCUMENTATION GUIDELINES<br />
<strong>Community</strong> <strong>First</strong> has established guidelines for medical record documentation. Individual medical records for each<br />
family member are to be maintained. The medical records must be handled and maintained in a confidential manner and<br />
must be organized in such a manner that all progress notes, diagnostic tests, reports, letters, discharge summaries and<br />
other pertinent medical information are readily accessible. In addition, each office should have a written policy in place to<br />
ensure that medical records are safeguarded against loss, destruction, or unauthorized use.<br />
Criteria<br />
Requirements<br />
1. Patient Identification Each page of the medical record must include a unique identifier, which may include<br />
patient ID number, medical record number, first and last name.<br />
2. Personal Data Personal/biographical data including the age, sex, address, employer, home and work<br />
telephone numbers, marital status of the patient, and emergency contacts must be included<br />
in the medical record.<br />
3. Allergies (P) Medication allergies and adverse reactions should be prominently noted in the record. If<br />
the patient has no known allergies or history of adverse reactions, this should be<br />
appropriately noted in the record.<br />
4. Problem List For patients seen three (3) or more times, a separate list of all the patient’s<br />
chronic/significant problems must be maintained. A chronic problem is defined as one<br />
that is of long duration, shows little change or is of slow progression.<br />
5. Medication List (P) For patients seen three (3) or more times, maintenance/ongoing medications should be<br />
listed on a medication sheet and updated as necessary with dosage changes and the date<br />
the change was made. A separate medication sheet is recommended but if a physician<br />
chooses to write out all current medications at each visit, this is acceptable. The<br />
medication list should include information/instruction to the member.<br />
6. Chart Legible Medical records must be legible to someone other than the author. A record that is<br />
deemed illegible by the reviewer should be evaluated by a second person.<br />
7. Author Signature All entries in the medical record must be signed by the author/performing provider.<br />
8. Dated entries Each and every entry must be accompanied by a date (month, day and year).<br />
9. Presenting Problems Problems/Symptoms identified by the patient and/or others that are presently occurring<br />
must be documented. This should be completed for each visit.<br />
10. Past Psychiatric<br />
History<br />
11. Tobacco, alcohol, &<br />
other substance use<br />
12. Significant<br />
Medical/Physical<br />
History<br />
13. Significant<br />
Developmental<br />
History<br />
14. Significant Family<br />
Psychiatric History<br />
During the initial visit, the past psychiatric history must be easily identified and include<br />
serious psychiatric incidents (to include hospitalizations, etc). For children and<br />
adolescents (18 years and younger), past psychiatric history may include special<br />
education.<br />
For patients 12 years and older, assessment of tobacco, alcohol, and other substance use<br />
should be documented in the medical record.<br />
During the initial visit, a history of significant medical history/information must be<br />
documented. For patients seen 3 or more times, past medical history should be easily<br />
identified including serious accidents, operations and illnesses. For children, past medical<br />
history relates to prenatal care and birth.<br />
For all patients at the initial visit, a history of the developmental history must be<br />
documented.<br />
The psychiatric history of family members should be documented as it may relate to the<br />
patient’s presenting problems to include both appropriate subjective and objective<br />
information.<br />
(P) Required by Psychiatrists ONLY. (Not within scope of practice for other types of Behavioral <strong>Health</strong> Providers)<br />
6.1 Behavioral <strong>Health</strong> Documentation <strong>Guidelines</strong><br />
P: Quality Management\Medical Record Review\SFY2012\Documentation <strong>Guidelines</strong> Revised 1/10, 8/11<br />
H EALTH PLANS<br />
www.cfhp.com<br />
31
Criteria<br />
Requirements<br />
15. Support Systems Admission and initial assessments must include current support system or lack thereof.<br />
16. Risk Factors Factors that may put the patient at risk must be documented; examples include current<br />
abuse, current living situation, no family support, history of mental illness, danger to self<br />
or others, perceptual disorders, etc.<br />
17. Mental Status At each visit the patient’s current mental status is documented.<br />
18. Diagnosis The diagnosis identified during each visit should be documented and should be consistent<br />
with findings. ICD-9 code(s) may be used but must include the written description of the<br />
diagnosis.<br />
19. Treatment<br />
Based on the chief complaint, exam findings and diagnosis, the treatment plan is clearly<br />
Plan/Goals<br />
documented.<br />
20. Appropriate Use of If a patient problem occurs which is outside the physician’s scope of practice, there must<br />
Consultants<br />
21. Appropriate<br />
Studies<br />
Ordered<br />
be a referral to an appropriate specialist.<br />
The laboratory and other studies ordered should be consistent with the treatment plan as<br />
related to the working diagnosis and should be documented at the time of the visit.<br />
Abnormal findings must have an explicit notation of follow-up plans.<br />
22. Review of Studies There must be evidence that the physician has reviewed the results of diagnostic studies.<br />
Methods can vary, but often the physician will initial the lab report or mention it in the<br />
progress notes.<br />
23. Medication<br />
Management (P)<br />
24. Medication<br />
Education (P)<br />
25. Hospital/ER Records<br />
(appropriate to<br />
behavioral health)<br />
26. Results of<br />
Consultation/<br />
Referrals<br />
27. Teaching Regarding<br />
BH Issues<br />
28. Change in<br />
Behaviors/Symptoms<br />
29. Coordination with<br />
PCP<br />
30. If Child – Involvement<br />
Of Family<br />
31. Follow-up if missed<br />
appointment<br />
Documentation should reflect that the psychiatrist provides continuous evaluation of the<br />
medication(s) prescribed to the patient as well as review of other medications prescribed<br />
by the PCP or other specialist.<br />
Documentation will include information about the effects of a prescribed medication to<br />
include adverse effects. Information should include whether handouts on the medication<br />
were given to the patient and/or parent/guardian.<br />
Pertinent inpatient records must be maintained in the office medical record.<br />
When the patient is referred to another physician/practitioner for consultation, there must<br />
be a copy of the consult report and any associated diagnostic work up in the medical<br />
record. The BH physician/practitioner’s review of the consultation must be documented.<br />
Often the physician/practitioner initials the consult report.<br />
The member is provided basic teaching/instructions regarding behavioral health<br />
conditions.<br />
At each subsequent visit, changes in the patient’s behavioral health symptoms/behaviors<br />
are documented.<br />
Evidence (at least quarterly, or more often if clinically indicated) that the patient’s PCP is<br />
notified that his/her patient is receiving behavioral health services. This can be<br />
demonstrated through use of the CFHP form or a summary report of the patient’s<br />
status/progress from the Behavior <strong>Health</strong> provider to the PCP. A copy of the report<br />
should be maintained in the record.<br />
If the patient is a minor, involvement of his/her parent/guardian is documented. If the<br />
minor is receiving services that allow for no involvement of the parent/guardian, this is<br />
also documented.<br />
If the patient misses a scheduled appointment, documentation will reflect that follow-up<br />
contact was made. This can be done by letter or phone. If there is no response, this also<br />
should be documented.<br />
32. Date of Next Visit Encounter forms or notes should have a notation, when indicated, regarding follow-up<br />
care, calls, or visits. Specific time of return should be noted in weeks, months, or as<br />
needed.<br />
(P) Required by Psychiatrists ONLY. (Not within scope of practice for other types of Behavioral <strong>Health</strong> Providers)<br />
P: Quality Management\Medical Record Review\SFY2012\Documentation <strong>Guidelines</strong> Revised 1/10, 8/11<br />
32 H EALTH PLANS<br />
www.cfhp.com
Criteria<br />
Requirements<br />
33. Release of<br />
A signed release of information is obtained as indicated, which will permit specific<br />
Information<br />
information sharing between providers.<br />
34. Care Coordination The medical record should reflect evidence that all professionals are included in primary and<br />
for Members with specialty care service team for CCSHCN members who may have co-occurring Behavioral<br />
Disabilities or <strong>Health</strong> disorders.<br />
Chronic/Complex<br />
Special <strong>Health</strong> Care<br />
Needs (CCSHCN)<br />
35. Evaluation for abuse The medical record should reflect evidence that the provider evaluates for signs / symptoms or<br />
/ neglect or other behaviors associated with abuse / neglect or other significant socioenvironmental factors.<br />
socioenvironmental<br />
factors<br />
36. Diagnosis Validation The record should reflect that the billing diagnosis is consistent with that of the chief<br />
complaint.<br />
37. Claims Validation The record should reflect the documented encounter is appropriate for the level of E/M<br />
services billed.<br />
(P) Required by Psychiatrists ONLY. (Not within scope of practice for other types of Behavioral <strong>Health</strong> Providers)<br />
P: Quality Management\Medical Record Review\SFY2012\Documentation <strong>Guidelines</strong> Revised 1/10, 8/11<br />
H EALTH PLANS<br />
www.cfhp.com<br />
33
6.2 Behavioral <strong>Health</strong> Medical Record Review Tool<br />
34 H EALTH PLANS<br />
www.cfhp.com
The evaluation of breast disease is based on risk factors and age and is determined by history, physical examination, imaging<br />
studies, cytologic examination, and biopsy. The clinician should be able to:<br />
• Obtain a history related to breast disorders including:<br />
• Duration, onset, and cyclicity of signs and symptoms<br />
• Menstrual and reproductive history<br />
• Hormone use<br />
• Dietary habits<br />
• Breast implants<br />
• Perform a thorough physical examination of the breasts<br />
• Educate patients on technique of breast self-examination<br />
• Counsel patients on the appropriate screening and diagnostic modalities for life-threatening breast disease, such as<br />
mammography and sonography, including timing and follow-up<br />
• Diagnose and manage (consistent with training and experience) or refer for management, patients with:<br />
• A solid or cystic breast mass<br />
• A mammographic abnormality<br />
• Breast pain<br />
• Physiologic and pathologic nipple discharge<br />
• Mastitis<br />
• Fibrocystic conditions<br />
• Counsel patients on familial risk and behavioral factors related to breast disease<br />
Thorough communication with patients about all management options, their risks, and all test results, as well as written<br />
documentation of these discussions, is of the utmost importance to the provision of quality care.<br />
Palpable Mass<br />
Cyst<br />
• Ultrasound or cyst aspiration useful to differentiate between solid and cystic mass.<br />
• With aspiration, if mass does not disappear or fluid is bloody, send for cytology and refer to surgeon. Fluid can otherwise<br />
by discarded. Re-examine breast in six weeks for recurrence. If cyst recurs refer to surgeon. Otherwise, follow routinely.<br />
Solid<br />
• Refer patient to surgeon for solid, dominant, persistent mass as biopsy is almost always indicated.<br />
• A normal mammogram does not eliminate need for further evaluation of a clinically suspicious mass. However, if mass<br />
is clinically benign on breast exam, and this is confirmed by cytologic exam and mammography, patient may be followed<br />
by a surgeon every three months until biopsy or resolution of problem.<br />
• Women
analgesic, and recommend use of a well-supporting brassiere.<br />
• If conservative measures do not relieve pain symptoms, referral to surgeon is indicated.<br />
Skin/Nipple Change and Nipple Discharge<br />
• Women with skin breakdown on the nipple or areola should be referred to a surgeon.<br />
• Patient with palpable mass and any nipple discharge should be referred to a surgeon.<br />
• If discharge suspicious for neoplasm (spontaneous; unilateral; confined to single duct; occurring in older patient; clear,<br />
bloody, serous, or serosanguinous) send patient for mammography and surgical consult.<br />
• Nipple discharge (particularly if bilateral or multiductal, or milky) is not suspicious for cancer and needs no referral. If<br />
milky discharge is profuse, medical workup for galactorrhea may be indicated.<br />
The Worried Patient with a Negative Workup<br />
• Refer patient to a surgeon for a second opinion.<br />
Difficult Breast Examinations<br />
• May refer woman to surgeon if she has had reduction or augmentation mammoplasty; if breasts very large or<br />
multinodular; if multiple biopsies severely scar breasts.<br />
• All women who are pregnant or lactating and have a breast mass or area of patient concern should be referred to a<br />
surgeon.<br />
High Risk Patients<br />
• Consult breast cancer specialist for a woman with prior history of breast cancer, strong first-degree family history, or<br />
previous history of atypia or multiple biopsies. Such a woman may need a special followup regimen.<br />
Taken from the <strong>Guidelines</strong> for Women’s <strong>Health</strong> Care, Second Edition, The American College of Obstetrics and Gynecologist,s, p.<br />
270, 2002<br />
PREPARED BY THE SOCIETY OF SURGICAL ONCOLOGY AND THE COMMISSION ON CANCER OF THE AMERICAN<br />
COLLEGE OF SURGEONS<br />
36 H EALTH PLANS<br />
www.cfhp.com
Prevent Child Texas, a non-profit organization working to prevent child abuse and neglect in Texas, reports that:<br />
• In the United States, 4 children die from child abuse every day;<br />
• 13,700 children are abused and neglected every day in the United States;<br />
• Every 11 seconds a child is reported abused or neglected;<br />
• 184 children died from abuse and neglect in Texas in 2003.<br />
The legal definitions of child abuse and neglect are defined in the Texas Family Code §261.001 / Texas Penal Code<br />
§21.11,21.011,22.021,43.01, 43.25 / Texas <strong>Health</strong> and Safety Code Ch. 481.<br />
Child abuse includes the following acts or omissions by any person:<br />
A. mental or emotional injury to a child that results in an observable and material impairment in the child’s growth,<br />
development, or psychological functioning;<br />
B. causing or permitting the child to be in a situation in which the child sustains a mental or emotional injury that results in an<br />
observable and material impairment in the child’s growth, development, or psychological functioning;<br />
C. Physical injury that results in substantial harm to the child, or the genuine threat of substantial harm from physical injury<br />
to the child, including an injury that is at variance with the history or explanation given and excluding an accident or<br />
reasonable discipline by a parent, guardian, or managing or possessory conservator that does not expose the child to a<br />
substantial risk of harm;<br />
D. failure to make a reasonable effort to prevent an action by another person that results in physical injury that results in<br />
substantial harm to the child;<br />
E. sexual conduct harmful to a child’s mental, emotional, or physical welfare, including conduct that constitutes the offense of<br />
indecency with a child under Section 21.11, Penal Code, sexual assault under Section 22.011, Penal Code, or aggravated sexual<br />
assault under Section 22.021, Penal Code;<br />
F. failure to make a reasonable effort to prevent sexual conduct harmful to a child;<br />
G. compelling or encouraging a child to engage in sexual conduct as defined by Section 43.01, Penal Code;<br />
H. causing, permitting, encouraging, engaging in, or allowing the photographing, filming, or depicting of the child if the person<br />
knew or should have known that the resulting photograph, film, or depiction of the child is obscene (as defined by the<br />
Penal Code) or pornographic;<br />
I. the current use by a person of a controlled substance as defined by chapter 481, <strong>Health</strong> and Safety Code, in a manner to the<br />
extent that the use results in physical, mental, or emotional injury to a child, or<br />
J. causing, expressly permitting, or encouraging a child to use a controlled substance as defined by Chapter 481, <strong>Health</strong> and<br />
Safety Code.<br />
K. causing, permitting, encouraging, engaging in, or allowing a sexual performance by a child as defined by Section 43.25,<br />
Penal Code.<br />
8.1 Child Abuse and Neglect<br />
Neglect includes the following acts or omissions:<br />
• the leaving of a child in a situation where the child would be exposed to a substantial risk of physical or mental harm,<br />
without arranging for necessary care for the child, and a demonstration of an intent not to return by a parent, guardian,<br />
or managing or possessory conservator of the child; or<br />
• placing the child in or failing to remove the child from a situation that a reasonable person would realize requires<br />
judgment or actions beyond the child’s level of maturity, physical condition, or mental abilities and that results in bodily<br />
injury or a substantial risk of immediate harm to the child;<br />
• the failure to seek, obtain, or follow through with medical care for the child, with the failure resulting in or presenting<br />
a substantial risk of death, disfigurement, or bodily injury or with the failure resulting in an observable and material<br />
impairment to the growth, development, or functioning of the child;<br />
• the failure to provide the child with food, clothing, or shelter necessary to sustain the life or health of the child, excluding<br />
failure caused primarily by financial inability unless relief services had been offered and refused;<br />
• placing the child in or failing to remove the child from a situation in which the child would be exposed to a substantial risk<br />
of sexual conduct harmful to the child; or<br />
• the failure by the person responsible for a child’s care, custody, or welfare to permit the child to return to the child’s<br />
home without arranging for the necessary care for the child after the child has been absent from the home for any<br />
reason, including having been in residential care or having run away.<br />
H EALTH PLANS<br />
www.cfhp.com<br />
37
CFHP has adopted the American Academy of Pediatrics guidelines for When Inflicted Skin Injuries Constitute Child Abuse;<br />
Assessment of Maltreatment of Children With Disabilities; Investigation and Review of Unexpected Infant and Child Deaths;<br />
Shaken Baby Syndrome: Rotational Cranial Injuries and Failure to Thrive as a Manifestation of Child Neglect. Copies of the<br />
complete guidelines can be found on http://aappolicy.aappublications.org/.<br />
To report an emergency, call 911. To report child abuse or neglect, call 1-800-252-5400 or use our secure website:<br />
https://www.txabusehotline.org<br />
38 H EALTH PLANS<br />
www.cfhp.com
AMERICAN ACADEMY OF PEDIATRICS:<br />
Failure to Thrive as a Manifestation of Child Neglect<br />
Robert W. Block, MD, Nancy F. Krebs, MD and the Committee on Child Abuse and Neglect and the Committee on Nutrition<br />
PEDIATRICS Vol. 116 No. 5 November 2005, pp. 1234-1237 (doi:10.1542/peds.2005-2032)<br />
Recognition of Failure to Thrive (FTT) Secondary To Neglect or Abuse<br />
The risk factors that should alert the pediatrician to the possibility of neglect as the cause of FTT include:<br />
• parental depression, stress, marital strife, divorce;<br />
• parental history of abuse as a child;<br />
• mental retardation and psychological abnormalities in the parent(s);<br />
• young and single mothers without social supports;<br />
• domestic violence;<br />
• alcohol or other substance abuse;<br />
• previous child abuse in the family;<br />
• social isolation and/or poverty;<br />
• parents with inadequate adaptive and social skills;<br />
• parents who are overly focused on career and/or activities away from home;<br />
• failure to adhere to medical regimens;<br />
• lack of knowledge of normal growth and development; and/or<br />
• infant with low birth weight or prolonged hospitalization.<br />
Guidance for the Pediatrician<br />
1. Pediatricians are encouraged to recognize that child neglect is among the many causes of FTT.<br />
2. Pediatricians are strongly encouraged to consider child abuse and neglect and to report cases of FTT that do not resolve<br />
with appropriate interventions.<br />
AMERICAN ACADEMY OF PEDIATRICS:<br />
Investigation and Review of Unexpected Infant and Child Deaths<br />
Committee on Child Abuse and Neglect and Committee on <strong>Community</strong> <strong>Health</strong> Services<br />
PEDIATRICS Vol. 104 No. 5 November 1999, pp. 1158-1160<br />
The American Academy of Pediatrics recommends that:<br />
1. Pediatricians advocate for proper death certification for children. Such certification is not possible in sudden unexpected<br />
deaths in the absence of a comprehensive death investigation, including scene investigation, autopsy, and review of<br />
previous medical records.<br />
2. Individual pediatricians and those working through AAP chapters support state legislation that requires autopsies of<br />
all deaths of children younger than 18 years that result from trauma; that are unexpected, including SIDS; and that are<br />
suspicious, obscure, or otherwise unexplained. These same guidelines about unexplained deaths should apply to all<br />
children, even those with chronic diseases.<br />
3. Individual pediatricians and those working through AAP chapters advocate for and support state legislation and other<br />
efforts that establish comprehensive child death investigation and review systems at the local and state levels.<br />
4. Pediatricians accept the responsibility to be involved with the death review process, including serving as a member of a<br />
review team, providing information from case files to the medical examiner or other agency investigating the death of a<br />
child who was a patient, or by serving as a consultant to the child fatality team on medical issues that need clarification.<br />
5. Pediatricians assist local public health, medical society, and other interested groups to become involved with the child<br />
death review process.<br />
6. Pediatricians become involved in the training of death scene investigators so that appropriate knowledge of issues such as<br />
SIDS, child abuse, child development, and pediatric disease is used in the determination of the cause of death.<br />
7. Public policy initiatives directed at preventing childhood deaths, based on information acquired at the local and state levels<br />
from adequate death investigations, accurate death certifications, and systematic death reviews, be supported at the<br />
national and chapter level.<br />
8. The following recommendations pertaining to the investigation and review of child deaths, published by the US Advisory<br />
Board on Child Abuse and Neglect should be supported.<br />
• “The supply of professionals qualified to identify and investigate child abuse and neglect fatalities should be increased.”<br />
• “There must be a major enhancement of joint training by government agencies and professional organizations on the<br />
identification and investigation of serious and fatal child abuse and neglect.”<br />
• “States, military branches, and Indian Nations should implement joint criminal investigation teams in cases of fatal child<br />
abuse and neglect.”<br />
8.2 AAP Policy Recommendations<br />
H EALTH PLANS<br />
www.cfhp.com<br />
39
• “The Secretary of <strong>Health</strong> and Human Services and the United States Attorney General should work together to assure<br />
there is an ongoing national focus on fatal child abuse and neglect and to oversee an ongoing process to support the<br />
national system of local, state, and federal child abuse and neglect fatality review efforts.”<br />
• “Child death review teams should be established at the local or regional level within states.”<br />
AMERICAN ACADEMY OF PEDIATRICS:<br />
Maltreatment of Children With Disabilities<br />
Roberta A. Hibbard, MD, Larry W. Desch, MD, and the Committee on Child Abuse and Neglect and Council on Children With<br />
Disabilities<br />
PEDIATRICS Vol. 119 No. 5 May 2007, pp. 1018-1025<br />
1. Be capable of recognizing signs and symptoms of child maltreatment in all children and adolescents, including those<br />
with disabilities.<br />
2. Be familiar with disabling conditions that can mimic abuse or pose an increased risk of accidental injury that can be<br />
confused with abuse.<br />
3. Because children with disabilities are at increased risk of maltreatment, remain vigilant not only in assessment for<br />
indications of abuse but also in offerings of emotional support and provision of equipment and resources to meet the<br />
needs of children and families.<br />
4. Ensure that any child in whom maltreatment has been identified is evaluated thoroughly for disabilities.<br />
5. Advocate for all children, especially those who have disabilities or special health care needs, to have a medical home. If a<br />
child is hospitalized and does not have a medical home, the inpatient attending physician can help the family secure one<br />
before discharge, preferably as early as possible in the hospital course.<br />
6. Be actively involved with treatment plans developed for children with disabilities and participate in collaborative team<br />
approaches.<br />
7. Use health supervision visits as a time to assess a family’s strengths and need for resources to counterbalance family<br />
stressors and parenting demands.<br />
8. Advocate for changes in state and local policies in which system failures seem to occur regarding the identification,<br />
treatment, and prevention of maltreatment of children with disabilities.<br />
9. Advocate for the implementation of positive behavioral supports and elimination of aversive techniques and<br />
unnecessary physical restraints in homes, schools, and other educational and therapeutic programs (both public and<br />
private), institutions, and settings for children who have disabilities.<br />
10. Advocate for better health care coverage by both private insurers and governmental funding.<br />
AMERICAN ACADEMY OF PEDIATRICS:<br />
Shaken Baby Syndrome: Rotational Cranial Injuries<br />
Committee on Child Abuse and Neglect<br />
PEDIATRICS Vol. 108 No. 1 July 2001, pp. 206-210<br />
The American Academy of Pediatrics recommends that pediatricians:<br />
1. Become educated about the recognition, diagnosis, treatment, and outcome of shaken baby and abusive head-impact<br />
injuries in infants and children;<br />
2. Be aware of and exercise their responsibility to report these injuries to appropriate authorities;<br />
3. Provide pertinent medical information to other members of multidisciplinary teams investigating these injuries;<br />
4. Support home visitation programs and any other child abuse prevention efforts that prove efficacious; and<br />
5. Provide or have appropriate referrals to resources to educate parents about healthy coping strategies when dealing<br />
with their child.<br />
AMERICAN ACADEMY OF PEDIATRICS:<br />
Evaluation of Suspected Child Physical Abuse<br />
Nancy D. Kellogg, MD and the Committee on Child Abuse and Neglect<br />
PEDIATRICS Vol. 119 No. 6 June 2007, pp. 1232-1241<br />
The interview of parents or caregivers of infants or children who present with serious injuries may be conducted in an<br />
outpatient or inpatient setting. If the child presents to a clinic with a serious injury that requires further medical care in a<br />
specialty (eg, orthopedics) or hospital setting, the clinician may opt to gather the minimum information to establish a need<br />
for reporting to child protective services. Any statements made by the caregiver regarding the injury should be documented<br />
accurately and completely. Once the clinician has assessed all the injuries, including approximate ages of injuries (when<br />
40 H EALTH PLANS<br />
www.cfhp.com
possible), a careful, complete, and detailed history should be obtained from the caregivers.<br />
Explanations that are concerning for intentional trauma include:<br />
1. no explanation or vague explanation for a significant injury;<br />
2. an important detail of the explanation changes dramatically;<br />
3. an explanation that is inconsistent with the pattern, age, or severity of the injury or injuries;<br />
4. an explanation that is inconsistent with the child’s physical and/or developmental capabilities; and<br />
5. different witnesses provide markedly different explanations for the injury or injuries.<br />
Information regarding the child’s behavior before, during, and after the injury occurred, including feeding times and levels<br />
of responsiveness, should be gathered. Victims of significant trauma usually have observable changes in behavior. Access to<br />
caregivers and caregiver activities before, during, and after the injury occurred are also important to document. Frequently,<br />
infants and children present to medical settings with a history of a fall. Recent studies have indicated that short falls may result<br />
in bruising; however, more significant types of head trauma, including skull fractures, are exceedingly uncommon but possible.<br />
Information should be gathered in a non-accusatory but detailed manner. Other information that may be useful in the medical<br />
assessment of suspected physical abuse includes:<br />
1. past medical history (trauma, hospitalizations, congenital conditions, chronic illnesses);<br />
2. family history (especially of bleeding, bone disorders, and metabolic or genetic disorders);<br />
3. pregnancy history (wanted/unwanted, planned/unplanned, prenatal care, postnatal complications, postpartum<br />
depression, delivery in non-hospital settings);<br />
4. familial patterns of discipline;<br />
5. child temperament (easy to care for or fussy child);<br />
6. history of past abuse to child, siblings, or parents;<br />
7. developmental history of child (language, gross motor, fine motor, psychosocial milestones);<br />
8. substance abuse by any caregivers or people living in the home;<br />
9. social and financial stressors and resources; and<br />
10. violent interactions among other family members.<br />
AMERICAN ACADEMY OF PEDIATRICS:<br />
The Evaluation of Sexual Abuse in Children<br />
Nancy Kellogg, MD and the Committee on Child Abuse and Neglect<br />
PEDIATRICS Vol. 116 No. 2 August 2005, pp. 506-512<br />
Physicians should be aware that child sexual abuse often occurs in the context of other family problems, including physical<br />
abuse, emotional maltreatment, substance abuse, and family violence. If these problems are suspected, referral for a more<br />
comprehensive evaluation is imperative and may involve other professionals with expertise needed for evaluation and<br />
treatment. In difficult cases, pediatricians may find consultation with a regional child abuse specialist or assessment center<br />
helpful.<br />
<strong>Guidelines</strong> for Making the Decision to Report Sexual Abuse of Children<br />
History<br />
Behavioral<br />
Symptoms<br />
Data Available<br />
Physical<br />
Examination<br />
Clear Statement Present or Absent Normal or<br />
abnormal<br />
None or vague Present or Absent Normal or<br />
nonspecific<br />
None or vague Present or Absent Concerning or<br />
diagnostic findings<br />
Vague, or history<br />
by parent only<br />
Present or Absent<br />
Normal or<br />
nonspecific<br />
Diagnotic Tests<br />
Positive or<br />
negative<br />
Positive test for<br />
C trachomatis,<br />
gonorrhea, T<br />
vaginalis, HIV,<br />
syphilis, or herpes*<br />
Negative or<br />
positive<br />
Level of Concern<br />
About Sexual<br />
Abuse<br />
High<br />
High<br />
High 1<br />
Response<br />
Report Decision<br />
Report<br />
Report<br />
Report<br />
Negative Indeterminate Refer when<br />
possible<br />
None Present Normal or<br />
nonspecific<br />
Negative Intermediate Possible report + ,<br />
refer, or follow<br />
*: If nonsexual transmission is unlikely or excluded.<br />
1: Confirmed with various examination techniques and/or peer review with expert consultant.<br />
+: If behaviors are rare/unusual in normal children<br />
H EALTH PLANS<br />
www.cfhp.com<br />
41
9.1 Diabetes <strong>Guidelines</strong><br />
MANAGEMENT OF DIABETES MELLITUS IN ADULTS AND CHILDREN<br />
CFHP has adopted the Minimum Standards for Diabetic Care that were developed by the Texas Diabetes Council, as the<br />
standard physician protocol for the preventive care of members who have been diagnosed with diabetes mellitus. The Texas<br />
Diabetes Council was created in 1983 by the 68th legislature as the recommendation of the Special Committee on Diabetes<br />
Services in Texas. The Council’s mission is to assist in the planning and coordination of diabetes control activities and to develop<br />
and carry out a state plan for diabetes control. Diabetes can cause blindness, kidney failure, amputations, heart disease, birth<br />
defects, strokes, and premature death and disability. Early interventions can prevent many of the complications associated with<br />
diabetes.<br />
The Texas Diabetes Council reports:<br />
• Prevalence of Diagnosed 1 Diabetes in Persons 18 and Older<br />
• An estimated 1.7 million persons aged eighteen years and older in Texas (9.7% of this age group) have been<br />
diagnosed with diabetes. Nationwide, 19.8 million persons eighteen years of age and older have been diagnosed<br />
with diabetes (8.3% of this age group).<br />
• Prevalence of Undiagnosed 2 Diabetes in Persons 18 and Older<br />
• Another estimated 425,157 persons aged eighteen years and older in Texas are believed to have undiagnosed<br />
diabetes (based on 2003-2006 NHANES age-adjusted prevalence estimate of 2.5% of persons twenty years of age<br />
and older). The total for both diagnosed and undiagnosed diabetes is 2.1 million.<br />
• Diabetes Mortality 3 Rate (Per 100,000) by Race/Ethnicity, Texas, 2006<br />
• The 2006 diabetes mortality rate for Texas was 27 deaths per 100,000 persons. Mortality rates for each race/<br />
ethnicity were applied to the 2006 population by race/ethnicity:<br />
• 20 per 100,000 whites (non-Hispanic)<br />
• 42 per 100,000 Hispanics<br />
• 49 per 100,000 blacks (non-Hispanic)<br />
• 21 per 100,000 persons who fall in the “Other” category<br />
The 2006 mortality rates (per 100,000) for blacks (non-Hispanic) and Hispanics were more than double that of whites<br />
(non-Hispanic).<br />
The purpose of the guidelines is to ensure that all adults with diabetes who are enrolled with <strong>Community</strong> <strong>First</strong> receive accepted<br />
standards of care. These guidelines will promote consistency in clinical practice and improve the quality and outcome of care<br />
for our members.<br />
Complete history & physical<br />
Diabetes Education*<br />
Medical Nutrition Therapy<br />
Exercise Counseling<br />
Psychosocial Counseling<br />
Diabetes Minimum Practice Recommendations<br />
(Established by the Texas Diabetes Council Revised 7-27-06)<br />
Examination/Test<br />
Lifestyle / Behavior Changes Counseling<br />
Weight / Height / BMI<br />
Adult Overweight = BMI 25-29.9<br />
Adult Obesity = BMI ≥30<br />
Blood Pressure<br />
Target:
Examination/Test<br />
Oral / Dental Inspection<br />
Refer for dental care annually or as needed<br />
Growth and Development (including height) in Children<br />
Aspirin / Antiplatelet Prophylaxis (if no contra-indications)<br />
Type 1 or 2 ≥ age 30<br />
A1c<br />
Target: A1c≤6.5%<br />
Kidney Evaluation<br />
Estimate GFR (eGFR) & microalbumin determination (≥30mg<br />
= abnormal). Consider nephro/endocrine evaluation at Stage<br />
3 CKD (eGFR
Glycemic Control Algorithm For Type 2 Diabetes Mellitus In Children And Adults<br />
Goals<br />
A1C≤6.0% 1<br />
Fasting SMBG ≤100 mg/dL<br />
2-hr PP SMBG ≤140 mg/dL<br />
Avoid hypoglycemia; i.e.<br />
glucose
GLYCEMIC CONTROL BIBLIOGRAPHY<br />
• Recent Review Articles<br />
Inzucchi SE. Oral antihyperglycemic therapy for type 2 diabetes: scientific<br />
review. JAMA. 2002;287(3):360-72.<br />
Riddle, MC. Glycemic management of type 2 diabetes: An emerging<br />
strategy with oral agents, insulins and combinations. Endocrinol Metab<br />
Clin N Am. 2005;34(1):77-98.<br />
• Metformin or Sulfonylurea + Acarbose<br />
Chiasson JL, Josse RG, Hunt JA, et al. The efficacy of acarbose in the<br />
treatment of patients with non-insulin-dependent diabetes mellitus. A<br />
multicenter controlled clinical trial. Ann Intern Med. 1994;121(12):928-35.<br />
• Metformin + Thiazolidinedione<br />
Pioglitazone:<br />
Einhorn D, Rendell M, Rosenzweig J, et al. Pioglitazone hydrochloride in<br />
combination with metformin in the treatment of type 2 diabetes mellitus: a<br />
randomized, placebo-controlled study. The Pioglitazone 027 Study Group.<br />
Clin Ther. 2000;22(12):1395-409.<br />
Rosiglitazone:<br />
Fonseca V, Rosenstock J, Patwardhan R, et al. Effect of metformin and<br />
rosiglitazone combination therapy in patients with type 2 diabetes mellitus:<br />
a randomized controlled trial. JAMA. 2000;283(13):1695-702. Erratum in:<br />
JAMA 2000;284(11):1384.<br />
• Sulfonylurea + Thiazolidinedione<br />
Pioglitazone:<br />
Kipnes MS, Krosnick A, Rendell MS, et al. Pioglitazone hydrochloride in<br />
combination with sulfonylurea therapy improves glycemic control in<br />
patients with type 2 diabetes mellitus: a randomized, placebo-controlled<br />
study. Am J Med. 2001;111(1):10-7.<br />
Rosiglitazone:<br />
Wolffenbuttel BH, Gomis R, Squatrito S, et al. Addition of low-dose<br />
rosiglitazone to sulphonylurea therapy improves glycaemic control in Type<br />
2 diabetic patients. Diabet Med. 2000;17(1):40-7.<br />
• Metformin or Sulfonylurea + Exenatide<br />
Buse JB, Henry RR, Han J,et.al. Effects of exenatide (exendin-4) on<br />
glycemic control over 30 weeks in sulfonylurea-treated patients with type 2<br />
diabetes. Diabetes Care. 2004;27(11):2628-35.<br />
DeFronzo RA, Ratner RE, Han J, et.al. Effects of exenatide (exendin-4) on<br />
glycemic control and weight over 30 weeks in metformin-treated patients<br />
with type 2 diabetes. Diabetes Care. 2005;28(5):1092-100.<br />
• Nateglinide or Repaglinide + Metformin<br />
Raskin P, Klaff L, McGill J, et al Efficacy and safety of combination<br />
therapy: repaglinide plus metformin versus nateglinide plus metformin.<br />
Diabetes Care. 2003;26(7):2063-8. Erratum in: Diabetes Care.<br />
2003;26(9):2708.<br />
Repaglinide:<br />
Moses R, Slobodniuk R, Boyages S, et al. Effect of repaglinide addition to<br />
metformin monotherapy on glycemic control in patients with type 2<br />
diabetes. Diabetes Care. 1999;22(1):119-24.<br />
Nateglinide:<br />
Horton ES, Clinkingbeard C, Gatlin M, et al. Nateglinide alone and in<br />
combination with metformin improves glycemic control by reducing<br />
mealtime glucose levels in type 2 diabetes. Diabetes Care.<br />
2000;23(11):1660-5.<br />
• Nateglinide or Repaglinide + Thiazolidinedione<br />
Nateglinide:<br />
Rosenstock J, Shen SG, Gatlin MR, et al. Combination therapy with<br />
nateglinide and a thiazolidinedione improves glycemic control in type 2<br />
diabetes. Diabetes Care. 2002;25(9):1529-33.<br />
Repaglinide:<br />
Fonseca V, Grunberger G, Gupta S, et al. Addition of nateglinide to<br />
rosiglitazone monotherapy suppresses mealtime hyperglycemia and<br />
improves overall glycemic control. Diabetes Care. 2003;26(6):1685-90.<br />
Raskin P, Jovanovic L, Berger S, et al. Repaglinide/troglitazone<br />
combination therapy: improved glycemic control in type 2 diabetes.<br />
Diabetes Care. 2000;23(7):979-83.<br />
• Triple Therapy<br />
Sulfonylurea + Metformin + Alpha glucosidase inhibitors:<br />
Lam KS, Tiu SC, Tsang MW, et al. Acarbose in NIDDM patients with poor<br />
control on conventional oral agents. A 24-week placebo-controlled study.<br />
Diabetes Care. 1998;21(7):1154-8.<br />
Standl E, Schernthaner G, Rybka J, et al. Improved glycaemic control with<br />
miglitol in inadequately-controlled type 2 diabetics. Diabetes Res Clin<br />
Pract. 2001;51(3):205-13.<br />
Sulfonylurea + Metformin + Thiazolidinedione:<br />
Dailey GE 3rd, Noor MA, Park JS, et al. Glycemic control with glyburide/<br />
metformin tablets in combination with rosiglitazone in patients with type 2<br />
diabetes: a randomized, double-blind trial. Am J Med. 2004;116(4):223-9.<br />
Aljabri K, Kozak SE, Thompson DM. Addition of pioglitazone or bedtime<br />
insulin to maximal doses of sulfonylurea and metformin in type 2 diabetes<br />
patients with poor glucose control: a prospective, randomized trial. Am J<br />
Med. 2004;116(4):230-5.<br />
Sulfonylurea + Metformin + Exenatide<br />
Kendall DM, Riddle MC, Rosenstock J, et.al. Effects of exenatide (exendin-<br />
4) on glycemic control over 30 weeks in patients with type 2 diabetes<br />
treated with metformin and a sulfonylurea. Diabetes Care.<br />
2005;28(5):1083-91.<br />
Heine RJ, Van Gaal LF, Johns D, et al. Exenatide versus insulin<br />
glargine in patients with suboptimally controlled type 2 diabetes: a<br />
randomized study. Ann Intern Med. 2005; 143(8):559-69.<br />
H EALTH PLANS<br />
www.cfhp.com<br />
45
INSULIN ALGORITHM FOR TYPE 1 DIABETES MELLITUS 1<br />
IN CHILDREN AND ADULTS<br />
ABBREVIATIONS:<br />
BASAL: Glargine or Detemir<br />
BOLUS (Prandial):<br />
Reg: Regular Insulin (peak action 3-4 hrs)<br />
RAI: Rapid Acting Insulin = Aspart, Glulisine, or<br />
Lispro (peak action 1-1 ½ hrs)<br />
PPG: Post-Prandial Glucose<br />
SMBG: Self-monitored blood glucose 2<br />
TDI: Total daily insulin dosage in units<br />
Targets<br />
A1c < 6.5%<br />
Fasting SMBG 2
Publication # 45-11647<br />
Targets*<br />
A1 C<br />
8.5%<br />
0.5 units/kg/day,<br />
take 80% of total NPH dosage as<br />
glargine [basal]; bolus dose=80% of<br />
glargine dose divided tid)<br />
Multi-dose Insulin Therapy (MDI) 10<br />
-2 shots<br />
Split mix NPH + Short-acting insulin (SAI) (vial)<br />
(2:1 ratio AM, 1:1 ratio PM; or SAI sliding<br />
scale 7 )<br />
or premix 70/30; 75/25 or 50/50 (pen/vial)<br />
-3 shots (especially if nocturnal hypoglycemia)<br />
SAI: ACB and ACS sliding scale 7 (pen/vial)<br />
+<br />
NPH: ACB and HS (pen/vial) or LAI: q daily (pen/vial)<br />
Starting dose 8 : 0.3–0.5 units/kg/day (or if<br />
current dose >0.5 units/kg/day, take 80% of<br />
QDI dosage) divided 2/3 as NPH/LAI; 1/3 as<br />
SAI; titrate to achieve glycemic targets<br />
Follow A1 C<br />
every 3–6 months and Adjust Regimen<br />
to Maintain Glycemic Targets<br />
(Insulin Requirement May Decrease as A1 C<br />
improves)<br />
ACS: Before supper<br />
FPG: Fasting plasma glucose<br />
HS: Bedtime<br />
LAI: Long-acting insulin = Glargine<br />
PCP: Primary care provider<br />
PPG: Postprandial plasma glucose<br />
SAI: Short-acting insulin = Regular<br />
(peak action 3-4 hrs); Lispro or<br />
Aspart (peak action 1 ½ hr)<br />
SMBG: Self-monitored blood glucose<br />
SQ: Subcutaneous<br />
TDI: Total daily insulin in units<br />
Pramlintide 10,12<br />
Consider as<br />
adjunct<br />
therapy to<br />
insulin in<br />
patients<br />
unable to<br />
stabilize<br />
postprandial<br />
glucose.<br />
Footnotes<br />
1 See Glycemic Control Algorithm<br />
for Type 2 Diabetes Mellitus in<br />
Children and Adults<br />
2 Consider simultaneous<br />
combination oral agent therapy<br />
3 Combining metformin with insulin therapy has been<br />
shown to result in less weight gain and better glycemic<br />
control with lower insulin requirements<br />
4 Continue combination oral agent therapy + sulfonylurea<br />
5 Continue metformin (+ 3<br />
rd<br />
oral agent); probably<br />
discontinue sulfonylurea<br />
6 PCP may decide to “ease” patient with poor beta-cell<br />
reserve into insulin therapy initially with QDI<br />
See web site (http://www.texasdiabetescouncil.org) for latest version and disclaimer.<br />
See reverse side for more information. (Page 1 of 6)<br />
7 ~1-2 units for every 50 mg/dL above target SMBG; Regular insulin to be given 30-60 minutes AC meal<br />
8 Dosages may differ in children and adolescents; consider referral to pediatric<br />
endocrinologist/comprehensive diabetes specialty team<br />
9 Go lower and slower for thin/elderly/complicated patients<br />
10 Consider referral to pediatric/adult endocrinologist/diabetes specialty team (option—<br />
insulin pump, Pramlintide)<br />
11 Typical “carb” bolus = 1 unit SAI covers 500/TDI x g carbohydrates from meal (~ 10-15 g);<br />
strongly recommend referral to Registered/Licensed Dietitian or Certified Diabetes<br />
Educator with experience in diabetes nutrition counseling (see Worksheet D.)<br />
(Page 1 of 6)<br />
9.4 Insulin Algorithm Type 2 DM in Children and Adults<br />
H EALTH PLANS<br />
www.cfhp.com<br />
47
INITIATION OF INSULIN THERAPY<br />
FOR TYPE 2 DIABETES MELLITUS IN CHILDREN AND ADULTS 1 :<br />
A SIMPLIFIED APPROACH<br />
Targets<br />
A1 C<br />
WORKSHEET<br />
Revised 10-20-05<br />
Advancing to Intensive/Physiologic Basal: Bolus Insulin Therapy<br />
Note: “Analog” = Rapid Acting (Bolus) Analog insulin throughout this document.<br />
A. Conversion from once-daily insulin to intensive/physiologic insulin replacement:<br />
Oral therapy failure: Once-daily glargine was added to the oral regimen and titrated to 30 units per day. How do you add analog insulin if the patient reports the<br />
following SMBG values?<br />
2-hr pp 2-hr pp 2-hr pp<br />
FPG Brkft Lunch Dinner<br />
Case 1 105 140 140 240<br />
Case 2 105 140 190 240<br />
Case 3 105 190 240 240<br />
Case 1<br />
a. Continue the oral agents (+ sulfonylurea) and 30 units glargine (or NPH)<br />
b. There are 2 approaches for adding analog 10 minutes before a meal:<br />
#1 Arbitrary start: 5 units<br />
Titrate: Add 2 units every 2 days to reach 2-hr pp goal<br />
#2 Carb-counting 1 unit/50 mg/dL over 2-hr pp goal<br />
PLUS<br />
1 unit/15 grams carbohydrate<br />
Titrate: Add 1 unit/50 mg/dL >2-hr pp goal every 2 days<br />
Cases 2 and 3<br />
As above, but add and titrate analog before each meal where the postprandial glucose is above goal. Also, see part D, below, for more information on<br />
how to optimize the use of analog insulin. Re-evaluate each week to be certain that about half of the total daily dose is basal and half is bolus insulin.<br />
B. Conversion from once-daily premix to intensive/physiologic insulin replacement:<br />
Oral therapy failure: Once-daily 70/30 premixed insulin was added and titrated to 30 units per day. The fasting glucose is at goal, but daytime control is poor.<br />
How do you convert to physiologic insulin therapy?<br />
a. Basal insulin dose: The first step in the conversion is based on the total dose of intermediate-acting insulin. In this case, the person is taking 21 units<br />
of NPH or aspart-protamine insulin (70% x 30 units=21 units). So, give 21 units basal glargine (use “unit-for-unit” conversion for once-daily<br />
intermediate regimens.) Remember, do not stop oral agents (+ sulfonylurea) at this time.<br />
b. Bolus insulin dose: There are several ways to start the analog.<br />
i. See Case 1, page 2 (Arbitrary start or Carb-counting)<br />
ii. Begin with the previous dose of fast-acting insulin, divide it before meals and titrate every 2 days. In this case, the person was using 30 units of<br />
70/30 or about 9 units of fast-acting insulin (30% x 30 units=9 units). So give 3 units of analog before each meal and titrate every 2 days as per Case 1.<br />
(Page 3 of 6)<br />
H EALTH PLANS<br />
www.cfhp.com<br />
49
Note: “Analog” = Rapid Acting (Bolus) Analog insulin throughout this document.<br />
WORKSHEET<br />
Advancing to Intensive/Physiologic Basal: Bolus Insulin Therapy<br />
Revised 10-20-05<br />
A. Conversion from once-daily insulin to intensive/physiologic insulin replacement:<br />
Oral therapy failure: Once-daily glargine was added to the oral regimen and titrated to 30 units per day. How do you add analog insulin if the patient reports the<br />
following SMBG values?<br />
2-hr pp 2-hr pp 2-hr pp<br />
FPG Brkft Lunch Dinner<br />
Case 1 105 140 140 240<br />
Case 2 105 140 190 240<br />
Case 3 105 190 240 240<br />
Case 1<br />
a. Continue the oral agents (+ sulfonylurea) and 30 units glargine (or NPH)<br />
b. There are 2 approaches for adding analog 10 minutes before a meal:<br />
#1 Arbitrary start: 5 units<br />
Titrate: Add 2 units every 2 days to reach 2-hr pp goal<br />
#2 Carb-counting 1 unit/50 mg/dL over 2-hr pp goal<br />
PLUS<br />
1 unit/15 grams carbohydrate<br />
Titrate: Add 1 unit/50 mg/dL >2-hr pp goal every 2 days<br />
Cases 2 and 3<br />
As above, but add and titrate analog before each meal where the postprandial glucose is above goal. Also, see part D, below, for more information on<br />
how to optimize the use of analog insulin. Re-evaluate each week to be certain that about half of the total daily dose is basal and half is bolus insulin.<br />
B. Conversion from once-daily premix to intensive/physiologic insulin replacement:<br />
Oral therapy failure: Once-daily 70/30 premixed insulin was added and titrated to 30 units per day. The fasting glucose is at goal, but daytime control is poor.<br />
How do you convert to physiologic insulin therapy?<br />
a. Basal insulin dose: The first step in the conversion is based on the total dose of intermediate-acting insulin. In this case, the person is taking 21 units<br />
of NPH or aspart-protamine insulin (70% x 30 units=21 units). So, give 21 units basal glargine (use “unit-for-unit” conversion for once-daily<br />
intermediate regimens.) Remember, do not stop oral agents (+ sulfonylurea) at this time.<br />
b. Bolus insulin dose: There are several ways to start the analog.<br />
i. See Case 1, page 2 (Arbitrary start or Carb-counting)<br />
ii. Begin with the previous dose of fast-acting insulin, divide it before meals and titrate every 2 days. In this case, the person was using 30 units of<br />
70/30 or about 9 units of fast-acting insulin (30% x 30 units=9 units). So give 3 units of analog before each meal and titrate every 2 days as per Case 1.<br />
(Page 3 of 6)<br />
50 H EALTH PLANS<br />
www.cfhp.com
D. Optimizing analog insulin use<br />
Revised 10-20-05<br />
Tight control of blood glucose requires that the patient participates in the management of their diabetes. This includes monitoring their blood glucose and<br />
learning to count carbohydrates or “carb count.” The following material explains how to calculate the dose of analog required to cover a meal and how to add<br />
extra analog to correct a hyperglycemic event.<br />
a. Determining the dose of analog insulin to use before a meal<br />
The “Rule of 500” is used to determine how many grams of carbohydrate 1 unit of analog insulin will cover. When this number is known, then the<br />
person can easily give the correct dose of analog by simply counting the grams of carbohydrate they intend to eat at the meal.<br />
Specifically, 500 divided by the total daily insulin dose (500/TDI) yields the number of grams of carbohydrate that 1 unit of analog will cover. For<br />
example, if a person has established that they require about 50 units of insulin per day, then it follows that 1 unit of analog will cover 10 grams of<br />
carbohydrate (500/50 = 10). If the person carb counts 140 grams in the dinner meal, then the dose of analog will be 14 units given 10 minutes before eating.<br />
b. Correcting for hyperglycemia<br />
The “Rule of 1800” is used to determine how much insulin to use to bring a high glucose reading back to goal. Even with tight control, hyperglycemia<br />
occurs and people need to be able to correct this situation.<br />
Specifically, 1800 divided by the total daily insulin dose yields a value indicating how much 1 unit of analog insulin will lower the blood glucose.<br />
Thus, if a person uses 90 units of insulin per day, then 1 unit of analog will reduce the blood glucose by 20 mg/dL (1800/90 = 20). This augment dose<br />
of insulin can be used by itself to correct hyperglycemia, or added to the bolus dose if glucose is high before a meal.<br />
1. Riddle MC, Rosenstock J, Gerich, J. Diabetes Care, 2003; 26:3080-3086.<br />
2. Spellman CW, Renda SM, Davis SN. Realizing the Potential of Insulin Therapy in Type 2 Diabetes: A Case Presentation-Based Monograph, presented<br />
at the American College of Osteopathic Internists 64 th Annual Convention; Chicago, IL (September 30, 2004).<br />
3. www.texasdiabetescouncil.org<br />
(Page 5 of 6)<br />
H EALTH PLANS<br />
www.cfhp.com<br />
51
Reviews/Important Articles:<br />
Abraira C, Colwell J, Nuttall F, et al. Cardiovascular events and correlates in the<br />
Veterans Affairs Diabetes Feasibility Trial. Veterans Affairs Cooperative Study on<br />
Glycemic Control and Complications in Type II Diabetes. Arch Intern Med.<br />
1997;157(2):181-8.<br />
Anonymous. Intensive blood-glucose control with sulphonylureas or insulin<br />
compared with conventional treatment and risk of complications in patients with<br />
type 2 diabetes (UKPDS 33). UK Prospective Diabetes Study (UKPDS) Group.<br />
Lancet. 1998;352(9131):837-53.<br />
DeWitt DE, Dugdale DC. Using new insulin strategies in the outpatient treatment<br />
of diabetes: clinical applications. JAMA. 2003;289(17):2265-9.<br />
DeWitt DE, Hirsch IB. Outpatient insulin therapy in type 1 and type 2 diabetes<br />
mellitus: scientific review. JAMA. 2003;289(17):2254-64.<br />
Implementation Conference for ACE Outpatient Diabetes Mellitus Consensus<br />
Conference Recommendations: Position Statement, February 2, 2005. Available<br />
online at http://www.aace.com/pub/odimplementation/PositionStatement.pdf.<br />
Accessed on May 2, 2005.<br />
Hirsch IB. Insulin analogues. N Engl J Med. 2005;352(2):174-83.<br />
ONCE DAILY INSULIN<br />
Morning vs. Bedtime NPH<br />
Groop LC, Widen E, Ekstrand A, et al. Morning or bedtime NPH insulin<br />
combined with sulfonylurea in treatment of NIDDM. Diabetes Care.<br />
1992;15(7):831-4.<br />
Morning vs. Bedtime Glargine<br />
Fritsche A, Schweitzer MA, Haring HU. Glimepiride combined with morning<br />
insulin glargine, bedtime neutral protamine hagedorn insulin, or bedtime insulin<br />
glargine in patients with type 2 diabetes. A randomized, controlled trial. Ann Intern<br />
Med. 2003;138(12):952-9.<br />
NPH vs. Glargine<br />
Riddle MC, Rosenstock J, Gerich J. The treat-to-target trial: randomized<br />
addition of glargine or human NPH insulin to oral therapy of type 2 diabetic<br />
patients. Diabetes Care. 2003;26(11):3080-6.<br />
ONCE DAILY vs. TWICE DAILY REGIMEN<br />
Raskin P, Allen E, Hollander P, et al. Initiating insulin therapy in type 2 Diabetes: a<br />
comparison of biphasic and basal insulin analogs. Diabetes Care. 2005;28(2):260-5.<br />
MULTIPLE DOSE INSULIN REGIMENS<br />
2-shot regimens<br />
NPH/Regular vs. NPH/ short acting analogue therapy<br />
Vignati L, Anderson JH Jr, Iversen PW. Efficacy of insulin lispro in combination<br />
with NPH human insulin twice per day in patients with insulin-dependent or noninsulin-dependent<br />
diabetes mellitus. Multicenter Insulin LisproStudy Group.<br />
Clin Ther. 1997;19(6):1408-21.<br />
Revised 10-20-05<br />
2-shot regimens (continued)<br />
70% NPH/ 30% Regular vs. Humalog Mix 75/25 TM or Novolog Mix 70/30 TM<br />
Roach P, Yue L, Arora V. Improved postprandial glycemic control during<br />
treatment with Humalog Mix25, a novel protamine-based insulin lispro<br />
formulation. Humalog Mix25 Study Group. Diabetes Care. 1999;22(8):1258-61.<br />
Boehm BO, Home PD, Behrend C, et al. Premixed insulin aspart 30 vs.<br />
premixed human insulin 30/70 twice daily: a randomized trial in Type 1 and<br />
Type 2 diabetic patients. Diabet Med. 2002;19(5):393-9.<br />
3-shot Regimens<br />
Ohkubo Y, Kishikawa H, Araki E, et al. Intensive insulin therapy prevents the<br />
progression of diabetic microvascular complications in Japanese patients with<br />
non-insulin-dependent diabetes mellitus: a randomized prospective 6-year study.<br />
Diabetes Res Clin Pract. 1995;28(2):103-17.<br />
Intensive Insulin Therapy<br />
Ohkubo Y, Kishikawa H, Araki E, et al. Intensive insulin therapy prevents the<br />
progression of diabetic microvascular complications in Japanese patients with<br />
non-insulin-dependent diabetes mellitus: a randomized prospective 6-year study.<br />
Diabetes Res Clin Pract. 1995;28(2):103-17.<br />
Saudek CD, Duckworth WC, Giobbie-Hurder A, et al. Implantable insulin pump<br />
vs multiple-dose insulin for non-insulin-dependent diabetes mellitus: a<br />
randomized clinical trial. Department of Veterans Affairs Implantable Insulin<br />
Pump Study Group. JAMA. 1996;276(16):1322-7.<br />
Raskin P, Bode BW, Marks JB, et al. Continuous subcutaneous insulin infusion<br />
and multiple daily injection therapy are equally effective in type 2 diabetes: a<br />
randomized, parallel-group, 24-week study. Diabetes Care. 2003;26(9):2598-603.<br />
Bretzel RG, Arnolds S, Medding J, et al. A direct efficacy and safety comparison<br />
of insulin aspart, human soluble insulin, and human premix insulin (70/30) in<br />
patients with type 2 diabetes. Diabetes Care. 2004;27(5):1023-7.<br />
(Page 6 of 6)<br />
52 H EALTH PLANS<br />
www.cfhp.com
Publication # 45-11266<br />
Age 126 mg/dL<br />
Consider ETT 1<br />
Prior to Prescription<br />
Low intensity/Low impact<br />
activity 2<br />
Low intensity/Low impact<br />
activity 2, 3<br />
Low intensity/Low impact<br />
activity 2<br />
ETT is recommended prior<br />
to moderate or vigorous<br />
activity 1<br />
If your patients are “apparently healthy” and have<br />
fewer than two major risk factors for cardiovascular<br />
disease (CVD), then they are categorized by age.<br />
• For men and women under 35 yrs. of age, there<br />
are no limitations. They can safely begin or<br />
continue a program of moderate or vigorous activity.<br />
• If they exceed the age limit (≥35 yrs.), it is safe to<br />
limit your recommendations to moderate activity<br />
(55% to 70% maximum heart rate) for both genders.<br />
Patients in this group who wish to participate in<br />
vigorous or competitive activities should be<br />
considered for an ETT screening.<br />
If your patients have one or more major risk factors<br />
for cardiovascular disease, they should undergo an<br />
ETT before beginning a moderate exercise program.<br />
It is important to underscore the fact that the<br />
majority of your patients, regardless of risk<br />
factors, can and should be encouraged to start or<br />
continue a program of regular moderate physical<br />
activity.<br />
Revised 01-22-04<br />
9.5 Exercise Algorithm Type 2 Diabetes Prevention and Therapy<br />
H EALTH PLANS<br />
www.cfhp.com<br />
53
Considerations for Prescribing Physical Activity for<br />
Type 2 Diabetes Prevention and Treatment<br />
Significant health benefits can be obtained by including an accumulated 30 minutes of<br />
moderate physical activity on most, if not all, days of the week.<br />
Regular physical activity lowers the risk of developing Type 2 diabetes.<br />
1996 Surgeon General’s Report on<br />
Physical Activity and <strong>Health</strong><br />
“Regular physical activity” includes all movements in everyday life, including work,<br />
recreation, exercise, and sporting activities.<br />
Low Intensity/Low Impact Activity - includes activities like walking,<br />
housework, light gardening, light yard work, and social dancing<br />
Moderate Intensity Activity - includes activities like brisk walking,<br />
vigorous gardening, slow cycling, aerobic dancing, doubles tennis,<br />
or hard work around the house.<br />
.<br />
Precautions for Exercise Prescription<br />
Retinopathy<br />
Patients with proliferative diabetic retinopathy have abnormal hemodynamic responses of the cerebral and<br />
ophthalmic circulation both at rest and with exercise. Vigorous physical activity, especially isometric contractions,<br />
produces significant increases in blood pressure and can accelerate proliferative diabetic retinopathy with<br />
significant risk of retinal and vitreal hemorrhage and detachment. Low impact/low intensity physical activity<br />
recommended.<br />
Orthopedic Problems<br />
Neuropathy and peripheral vascular disease can predict unnoticed foot injury. Footwear that relieves forefoot<br />
plantar pressure by up to 50% has been shown to be effective in preventing the recurrence of foot ulcers when worn for more<br />
than 60% of the day (Peirce, N. 1999. British Journal of Sports Medicine)<br />
<strong>Guidelines</strong> for Exercise Prescription<br />
1. Appropriate attire for physical activity, i.e., footwear - socks, shoes, insoles/orthotics.<br />
2. Do not exercise at peak hypoglycemic times.<br />
3. Monitor blood glucose before and during exercise if symptoms of hypoglycemia occur with exercise.<br />
4. Wear a form of personal identification or medical alert.<br />
5. Carry fast acting carbohydrate, i.e., sucrose and glucose products.<br />
6. Examine feet after exercise.<br />
7. Maintain adequate hydration.<br />
54 H EALTH PLANS<br />
www.cfhp.com
Hypertension Algorithm for Diabetes Mellitus in Adults<br />
Assess Blood<br />
Pressure 1 (BP)<br />
Follow-up BP each visit<br />
If microalbuminuria or<br />
nephropathy present (Table 1)<br />
BP 130/80 mmHg<br />
Start ACE inhibitor (ACEi) therapy 2-5<br />
If microalbuminuria or nephropathy present (Table 1)<br />
If African-American- Start ACEi in combination with diuretic or CCB<br />
If SBP >145mmHg and/or DBP>90mmHg 6<br />
Start with combination antihypertensive therapy<br />
Reassess therapy in 4-8 weeks-Titrate to at least ½ max dose<br />
Encourage self-monitoring of blood pressure 1<br />
(on average > 3 medications will be needed<br />
to achieve blood pressure goals)<br />
Revised 1-26-06<br />
Table1<br />
Microalbuminuria/Proteinuria 3<br />
• In Type 2 patients, an ACEi<br />
or angiotensin receptor<br />
blocker (ARB) may be used<br />
first line.<br />
• In Type 1 patients, an ACEi<br />
is recommended to reduce<br />
protein excretion<br />
• Consider the use of<br />
verapamil or diltiazem in<br />
patients with proteinuria<br />
unable to tolerate ACEi or<br />
ARBs.<br />
BP130/80 mmHg<br />
Continue Therapy<br />
BP Check Every Visit<br />
Add 6 Diuretic OR Calcium Channel Blocker (CCB) OR Beta Blocker<br />
If Diuretic Chosen: (Preferred if no other compelling indications)<br />
Creatinine 130/80 mmHg despite above agents or if<br />
intolerance/contraindications exist:<br />
Refer to Specialist (Endocrinologist or Nephrologist)<br />
OR<br />
ADD: α blocker, hydralazine, clonidine (caution with β blocker)<br />
9.6 Hypertension Algorithm for DM in Adults<br />
H EALTH PLANS<br />
www.cfhp.com<br />
55
Proper blood pressure assessment<br />
National Committee on Detection,<br />
Evaluation and Treatment of High Blood<br />
Pressure: The Seventh Report of the Joint<br />
National Committee on Detection,<br />
Evaluation and Treatment of High Blood<br />
Pressure (JNC 7). National Institutes of<br />
<strong>Health</strong>, National Heart, Lung and Blood<br />
Institute, 2003<br />
http://www.nhlbi.nih.gov/guidelines/<br />
hypertension/<br />
ACE inhibitor as 1 st line therapy in Diabetes<br />
Mellitus<br />
National Committee on Detection,<br />
Evaluation and Treatment of High Blood<br />
Pressure: The Seventh Report of the Joint<br />
National Committee on Detection,<br />
Evaluation and Treatment of High Blood<br />
Pressure (JNC 7). National Institutes of<br />
<strong>Health</strong>, National Heart, Lung and Blood<br />
Institute, 2003<br />
http://www.nhlbi.nih.gov/guidelines/<br />
hypertension/<br />
Kasiske BL, Kalil RS, Ma JZ, et al.:<br />
Effect of antihypertensive therapy on the<br />
kidney in patients with diabetes: a metaregression<br />
analysis. Ann Intern Med<br />
118:129–38, 1993<br />
UK Prospective Diabetes Study<br />
Group: Efficacy of atenolol and captopril<br />
in reducing the risk of macrovascular<br />
complications in type 2 diabetes (UKPDS<br />
39) BMJ 317:713–20, 1998<br />
The Heart Outcomes Prevention<br />
Evaluation Study. Effects of an ACE<br />
inhibitor, ramipril, on cardiovascular events<br />
in high risk patients. N Engl J Med<br />
342:145–53, 2000<br />
Pahor M, Psaty BM, Alderman MH, et<br />
al. Therapeutic benefits of ACE inhibitors<br />
and other antihypertensive drugs in<br />
patients with type 2 diabetes. Diabetes<br />
Care 23:888–92, 2000<br />
Wing LMH, Reid CM, Ryan P, et al. A<br />
comparison of outcomes with angiotensinconverting-enzyme<br />
inhibitors and diuretics<br />
for hypertension in the elderly (ANBP2). N<br />
Engl J Med 348:583-92, 2003<br />
Hypertension Algorithm for Diabetes Mellitus in Adults<br />
Diuretic as second line<br />
National Committee on Detection,<br />
Evaluation and Treatment of High<br />
Blood Pressure: The Seventh Report<br />
of the Joint National Committee on<br />
Detection, Evaluation and Treatment<br />
of High Blood Pressure (JNC 7).<br />
National Institutes of <strong>Health</strong>, National<br />
Heart, Lung and Blood Institute, 2003<br />
http://www.nhlbi.nih.gov/guidelines/<br />
hypertension/<br />
Antihypertensive & Lipid<br />
Lowering Treatment to Prevent Heart<br />
Attack (ALLHAT) JAMA 288:2981-97,<br />
2002<br />
Beta-Blocker as second line<br />
National Committee on Detection,<br />
Evaluation and Treatment of High<br />
Blood Pressure: The Seventh Report<br />
of the Joint National Committee on<br />
Detection, Evaluation and Treatment<br />
of High Blood Pressure (JNC 7).<br />
National Institutes of <strong>Health</strong>, National<br />
Heart, Lung and Blood Institute, 2003<br />
http://www.nhlbi.nih.gov/guidelines/<br />
hypertension/<br />
UK Prospective Diabetes Study<br />
Group: Efficacy of atenolol and captopril<br />
in reducing the risk of macrovascular<br />
complications in type 2 diabetes<br />
(UKPDS 39) BMJ 317:713–20, 1998<br />
Hansson L, Lindholm LH,<br />
Niskanen L, et al. Effect of angiotensin<br />
converting-enzyme inhibition compared<br />
with conventional therapy on<br />
cardiovascular morbidity and mortality<br />
in hypertension: the Captopril Prevention<br />
Project (CAPPP) randomised trial.<br />
Lancet 353: 611–16, 1999<br />
Verapamil or Diltiazem<br />
Hansson L, Hedner T, Lund-<br />
Johansen P, et al. Randomized trial of<br />
effects of calcium antagonists<br />
compared with diuretics and betablockers<br />
on cardiovascular morbidity<br />
and mortality in hypertension.<br />
NORDIL. Lancet 356:359–65, 2000<br />
Bakris GL, Copley JB, Vicknair N,<br />
et al. Calcium channel blockers versus<br />
other antihypertensive therapies on<br />
progression of NIDDM associated<br />
nephropathy. Kidney Int 50:1641–50,<br />
1996<br />
Dihydropyridine calcium channel<br />
blockers<br />
Tuomilehto J, Rastenyte D,<br />
Birkenhager WH, et al. Effect of<br />
calcium channel blockage in older<br />
patients with diabetes and systolic<br />
hypertension. N Engl J Med 340:<br />
677–84, 1999<br />
Dahlof B, Sever P, Poulter N, et al.<br />
Prevention of cardiovascular events<br />
with an antihypertensive regimen of<br />
amlodipine adding perindopril as<br />
required versus atenolol adding<br />
bendroflumethiazide as required, in<br />
the Anglo-Scandinavian Cardiac<br />
Outcomes Trial-Blood Pressure<br />
Lowering Arm (ASCOT-BPLA): a<br />
multicentre randomised controlled<br />
trial. Lancet 366: 895-906, 2005<br />
Estacio RO, Jeffers BW, Hiatt WR,<br />
et al. The effect of nisoldipine as<br />
compared with enalapril on<br />
cardiovascular outcomes in patients<br />
with non-insulin-dependent diabetes<br />
and hypertension. N Engl J Med<br />
338:645–52, 1998<br />
Alpha-Blockers<br />
Major cardiovascular events in<br />
hypertensive patients randomized to<br />
doxazosin vs chlorthalidone.<br />
(ALLHAT Data) JAMA<br />
283:1967–75, 2000<br />
Blood Pressure Goal 1 gram/24<br />
hour BP goal
Lipid Algorithm For Type 1 and Type 2 Diabetes Mellitus in Adults<br />
Revised 1-24-08<br />
FLP Goals:<br />
LDL-C
Lipid Algorithm For Type 1 and Type 2 Diabetes Mellitus in Adults<br />
Revised 1-24-08<br />
HMG Co-A Reductase Inhibitors LDL-C Equivalency in Patients with Hypercholesterolemia*<br />
Fluvastatin<br />
Pravastatin<br />
Lovastatin<br />
Simvastatin<br />
Atorvastatin<br />
Rosuvastatin<br />
Ezetimibe/<br />
Simvastatin<br />
Approximate<br />
%LDL↓<br />
20 mg 10 mg 10 mg<br />
-----<br />
-----<br />
-----<br />
-----<br />
15-20<br />
40 mg 20 mg 20 mg 5-10 mg -----<br />
-----<br />
-----<br />
21-29<br />
80-XL 40-80 mg 40 mg 20 mg 10 mg<br />
-----<br />
-----<br />
30-38<br />
-----<br />
-----<br />
80 mg 40 mg 20 mg 5-10 mg 10/10 mg 39-47<br />
-----<br />
-----<br />
-----<br />
80 mg 40 mg<br />
20 mg 10/20 mg 48-54<br />
-----<br />
-----<br />
-----<br />
-----<br />
80 mg<br />
40 mg 10/40 mg 55-59<br />
-----<br />
-----<br />
-----<br />
-----<br />
-----<br />
----- 10/80 mg >59<br />
Footnote: *this information is not based on head to head comparison<br />
(Page 2 of 3)<br />
58 H EALTH PLANS<br />
www.cfhp.com
References:<br />
Revised 1-24-08<br />
• Collins R, Armitage J, Parish S, Sleigh P, Peto R; Heart Protection Study Collaborative Group. MRC/BHF Heart Protection Study<br />
of cholesterol-lowering with simvastatin in 5963 people with diabetes: a randomised placebo-controlled trial. Lancet. 2003 Jun<br />
14;361(9374):2005-16.<br />
• Heart Protection Study Collaborative Group. MRC/BHF Heart Protection Study of cholesterol lowering with simvastatin in 20,536<br />
high-risk individuals: a randomised placebo-controlled trial. Lancet. 2002 Jul 6;360(9326):7-22.<br />
• Colhoun HM, Betteridge DJ, Durrington PN, Hitman GA, Neil HA, Livingstone SJ, Thomason MJ, Mackness MI, Charlton-Menys<br />
V, <strong>Full</strong>er JH; CARDS investigators. Primary prevention of cardiovascular disease with atorvastatin in type 2 diabetes in the<br />
Collaborative Atorvastatin Diabetes Study (CARDS): multicentre randomised placebo-controlled trial.Lancet. 2004 Aug 21-<br />
27;364(9435):685-96.<br />
• Grundy SM, Cleeman JI, Merz CN, Brewer HB Jr, Clark LT, Hunninghake DB, Pasternak RC, Smith SC Jr, Stone NJ; National<br />
Heart, Lung, and Blood Institute; American College of Cardiology Foundation; American Heart Association.Implications of recent<br />
clinical trials for the National Cholesterol Education Program Adult Treatment Panel III guidelines. Circulation. 2004 Jul 13;<br />
110(2):227-39.<br />
• Jones P, Kafonek S, Laurora I, Hunninghake D.Comparative dose efficacy study of atorvastatin versus simvastatin, pravastatin,<br />
lovastatin, and fluvastatin in patients with hypercholesterolemia (the CURVES study) Am J Cardiol. 1998 Mar 1;81(5):582-7.<br />
• Jones PH, Davidson MH. Reporting rate of rhabdomyolysis with fenofibrate + statin versus gemfibrozil + any statin.Am J Cardiol.<br />
2005 Jan 1;95(1):120-2.<br />
• Maeda K, Noguchi Y, Fukui T.The effects of cessation from cigarette smoking on the lipid and lipoprotein profiles: a metaanalysis.<br />
Prev Med. 2003 Oct;37(4):283-90.<br />
• Keech A, Simes RJ, Barter P, Best J, Scott R, Taskinen MR, Forder P, Pillai A, Davis T, Glasziou P, Drury P, Kesäniemi YA,<br />
Sullivan D, Hunt D, Colman P, d'Emden M, Whiting M, Ehnholm C, Laakso M; FIELD study investigators. Effects of long-term<br />
fenofibrate therapy on cardiovascular events in 9795 people with type 2 diabetes mellitus (the FIELD study): randomised<br />
controlled trial. Lancet. 2005 Nov 26;366(9500):1849-61.<br />
• Rubins HB, Robins SJ, Collins D, Fye CL, Anderson JW, Elam MB, Faas FH, Linares E, Schaefer EJ, Schectman G, Wilt TJ,<br />
Wittes J.Gemfibrozil for the secondary prevention of coronary heart disease in men with low levels of high-density lipoprotein<br />
cholesterol. Veterans Affairs High-Density Lipoprotein Cholesterol Intervention Trial Study Group. N Engl J Med. 1999 Aug 5;<br />
341(6):410-8.<br />
• Cholesterol Treatment Trialists' (CTT) Collaborators, Kearney PM, Blackwell L, Collins R, Keech A, Simes J, Peto R, Armitage J,<br />
Baigent C.Efficacy of cholesterol-lowering therapy in 18,686 people with diabetes in 14 randomised trials of statins: a metaanalysis.Lancet.<br />
2008 Jan 12;371(9607):117-25.<br />
(Page 3 of 3)<br />
H EALTH PLANS<br />
www.cfhp.com<br />
59
9.8 Diabetes Medical Nutrion Therapy and Prevention Algorithm<br />
Publication # 45-10778<br />
Fasting glucose<br />
>110 mg/dL;<br />
2-hr PP >140–180<br />
mg/dL<br />
Refer to<br />
Glycemic Control<br />
Algorithm<br />
Diabetes Medical Nutrition Therapy<br />
and Prevention Algorithm<br />
Diabetes Mellitus<br />
Fasting glucose >126 mg/dL;<br />
2 hr. PP >200 mg/dL<br />
Revised 04-27-06<br />
A1 C<br />
—Glycosylated<br />
Hemoglobin A1 C IGT—Impaired Glucose Tolerance<br />
BMI—Body Mass Index LDL-C—Low Density<br />
BP—Blood Pressure Lipoprotein Cholesterol<br />
CHO—Carbohydrates PCP—Primary Care Provider<br />
IFG—Impaired Fasting PP—Postprandial<br />
Glucose<br />
TG—Triglycerides<br />
Medical Nutrition Therapy<br />
by Registered/Licensed Dietitian or Certified Diabetes Educator with Experience in Diabetes Nutrition Counseling<br />
Individual Nutrition Assessment<br />
BMI, Waist Circumference, Medical History, Lab Values, Diet History, Lifestyle, Physical Activity, Readiness to Change<br />
Overweight/Obesity 2<br />
BMI >25<br />
Set weight loss goals<br />
5–7% weight loss<br />
minimum<br />
Evaluate total calories from fat and CHO<br />
If excessive, ↓ Kcal from CHO and/or fat,<br />
(especially from saturated fat) by 500-1000<br />
Kcal below usual daily intake<br />
TG 3<br />
>150 mg/dL<br />
Decrease total CHO intake<br />
↑ monounsaturated fats<br />
↑ Omega-3 fatty acids<br />
PCP to follow Lipid<br />
Algorithm<br />
If TG >500 mg/dL,<br />
↓ fat calories<br />
to 100 mg/dL 3<br />
Saturated fat 130/80 mmHg 4<br />
If proteinuric >125/75 mmHg<br />
restrict protein to 0.8–1g/kg<br />
Sodium Restriction<br />
< 2.3 g/day,<br />
If > age 50, < 1.5 g/day 5<br />
Monitor glucose (SMBG), A1 C<br />
, weight, lipids, and blood pressure. Adjust food portions and distribution with medication and activity to achieve metabolic goals.<br />
Footnotes<br />
IFG: Fasting glucose 100–125 mg/dL;<br />
IGT: Post challenge glucose >140–199 mg/dL<br />
Interventions<br />
• Self-monitored blood glucose<br />
• Increase physical activity (Refer to Exercise Algorithm)<br />
• Meal plan 1<br />
Distribute food throughout the day to avoid large concentrations of calories or carbohydrates<br />
that cause postprandial glucose elevations.<br />
Recommended: 45-65% of Kcal from CHO Not Recommended:
WEIGHT LOSS ALGORITHM FOR OVERWEIGHT AND OBESE ADULTS 1<br />
Publication #45-11694<br />
Normal<br />
BMI 18.5–24.9<br />
Obtain Accurate Height (Ht) and Weight (Wt);<br />
Calculate Body Mass Index (BMI) (See Table on Page 2)<br />
BMI = Wt in kg<br />
(Ht in m) 2<br />
Revised 01-27-05<br />
Reinforce <strong>Health</strong>y Lifestyle, Diet,<br />
and Exercise<br />
Overweight<br />
BMI 25–29.9<br />
Obesity 2<br />
BMI >30<br />
Class 3 Obesity 2<br />
BMI >40<br />
= Wt in lb x 703<br />
(Ht in inches) 2<br />
Assess Comorbidities and Risk Factors 3<br />
Metabolic 3 or Insulin Resistance 4 Syndromes; Waist Circumference (Men >40 inches; Women >35 inches);<br />
Dyslipidemia 3 (Elevated LDL-C and/or TG; Low HDL-C); HTN 5 ;<br />
Impaired Fasting Glucose (FPG 100-125 mg/dL); Impaired Glucose Tolerance (Post-challenge PG<br />
140–199mg/dL); Diabetes Mellitus 6 (FPG >126 mg/dL; Post-challenge PG >200 mg/dL);<br />
Coronary Heart or Other Vascular Disease (CVD); Sleep Apnea; DJD; GERD; Gallstones; NAFLD/NASH;<br />
Polycystic Ovary Syndrome; Urinary Incontinence<br />
Consider Contributing Factors<br />
Drugs 7<br />
Hypothyroidism<br />
Cushing Syndrome<br />
Male Hypogonadism<br />
Adult GH Deficiency<br />
Wt LossTargets<br />
2-3 unit Reduction in BMI<br />
>5–10% Reduction in Wt<br />
(>15% Wt Loss for Class 3 Obese Pts)<br />
+<br />
Significant Improvement in Comorbidities<br />
Consider Obesity Pharmacotherapy<br />
For Maintenance of Wt Loss<br />
(See Pharmacotherapy Box)<br />
Maintain <strong>Health</strong>y Lifestyle,<br />
Diet and Exercise<br />
and Monitor Wt Weekly for Life<br />
with Periodic Follow-up by HCP<br />
Consider Referral for Bariatric<br />
Surgery 14 as Adjunct to Lifestyle<br />
Changes if BMI >35 with<br />
Comorbidities or if BMI >40<br />
Targets Not<br />
Maintained<br />
Offer Medically-Supervised<br />
Wt Loss Intervention 8<br />
Pt Motivated<br />
Education;<br />
Lifestyle Change—<br />
Hypocaloric Diet (Deficit 250–1000<br />
Kcal/d 9 + Meal Replacements);<br />
Exercise (>30–60 Minutes/day);<br />
Behavior Modification;<br />
Nutrition/Family Counseling<br />
See web site (http://www.texasdiabetescouncil.org) for latest version and disclaimer.<br />
Pt Not<br />
Motivated<br />
3–6 months<br />
6 months<br />
Wt Loss<br />
Targets<br />
Maintenance<br />
Met<br />
Targets Maintained<br />
If Unsuccessful in 4–12 Weeks<br />
(with Motivated/Adherent Pt), Targets<br />
Consider Switching Drug Class or Not Met<br />
Using Combination Therapy 13<br />
Targets<br />
Not Met<br />
Educate; Manage Risk Factors<br />
Aggressively, and Reassess<br />
Readiness to Change Periodically<br />
Pt Not Motivated<br />
Targets Not Met<br />
Pt Motivated and Adherent<br />
Consider Obesity Pharmacologic Monotherapy<br />
as Adjunct to Lifestyle Changes if: BMI >27 with<br />
Comorbidities or if BMI >30<br />
Appetite Suppressants Lipase Inhibitor<br />
Phentermine 10<br />
11, 12<br />
Contraindicated in:<br />
Orlistat<br />
Uncontrolled HTN; CVD; Supported by<br />
Arrhythmia; Stroke; CHF; Hx; Evidence in Type 2<br />
Substance Abuse; Diabetes Mellitus;<br />
Glaucoma (Narrow-angle); Contraindicated in:<br />
Chronic<br />
Concurrent MAOI Rx<br />
Sibutramine 11<br />
Contraindicated in:<br />
Uncontrolled HTN;<br />
Glaucoma (Narrow-angle);<br />
Arrhythmia; Stroke; CVD;<br />
CHF; Concurrent SSRI &<br />
MAOI Therapy<br />
Malabsorption;<br />
Cholestasis; Orlistat<br />
Hypersensitivity;<br />
Concurrent<br />
Cyclosporin Therapy<br />
See reverse side for more information.<br />
9.9 Weight Loss Algorithm Overweight and Obese Adults<br />
H EALTH PLANS<br />
www.cfhp.com<br />
61
1 Adapted from NIH/NHLBI/NAASO;1998; NIH<br />
Publication No. 98-4083 (Obes Res<br />
1998;6[Suppl 2]:51S-210S)<br />
2 Consider starting obesity pharmacotherapy<br />
concurrent with other treatment modalities at<br />
presentation in motivated/adherent pts if BMI >35<br />
with comorbidities or >40 with no comorbidities<br />
3 National Cholesterol Education Program-Adult<br />
Treatment Panel III. JAMA 2001;285:2466-97<br />
4 American Association of <strong>Clinical</strong><br />
Endocrinologists Consensus Conference on the<br />
Insulin Resistance Syndrome, Washington, DC;<br />
August 2002 (Diabetes Care 2003;26:1297-<br />
1303)<br />
5 The 7th Report of the Joint National Committee<br />
on Detection, Evaluation and Treatment of High<br />
Blood Pressure (JNC 7). JAMA 2003;289:2560-72<br />
6 See Glycemic Control Algorithm in Type 2<br />
Diabetes Mellitus in Children and Adults; Diabetes<br />
medications may need to be adjusted to avoid<br />
hypoglycemia in pts who lose wt<br />
8 Assuming BMI >25 and/or waist<br />
circumference >40 inches in men; >35 inches in<br />
women and 1 or more major comorbidity<br />
9 Calorie deficit of 250 Kcal/day will result in ~1/2<br />
lb/week wt loss (1000 Kcal/day ~2 lb/week wt loss)<br />
10FDA-approved for adjunctive short-term use
Publication #45-11825<br />
Screening 1 :<br />
1. General population; BMI >25<br />
Individuals >45 years<br />
Baseline and q 3 years<br />
2. High risk population >18 years; BMI >25<br />
Baseline and yearly<br />
3. Children and youth at risk<br />
Baseline at age 10 and q 2 years<br />
• Overweight BMI (>85th %’ile for age and gender<br />
and > two risk factors)<br />
Risk Factors:<br />
• 1st degree (and/or 2nd degree in children) relative<br />
with diabetes<br />
• Hx of gestational diabetes or delivery of a baby<br />
weighing >9 lbs<br />
• High-risk ethnic group<br />
• Hypertension<br />
• Dyslipidemia<br />
• Polycystic Ovary Syndrome<br />
• Metabolic 2 and/or Insulin Resistance 3 Syndromes<br />
• Vascular disease<br />
• Acanthosis nigricans<br />
TESTING 1,4,5 : FPG Recommended: (if abnormal<br />
confirm X 1); however 2-hr OGTT acceptable in adults<br />
and should be used for diagnosis in children 6 (routine<br />
measurement of insulin levels is not recommended) a<br />
Diagnosis:<br />
IFG<br />
FPG >100 and 140 and 126 mg/dL and/or<br />
2-hr OGTT >200 mg/dL—<br />
Refer to Texas Diabetes<br />
Council Algorithms<br />
BMI—Body mass index (kg/m 2 )<br />
FPG—Fasting plasma glucose<br />
OGTT—1.75g/kg to max 75g Oral glucose tolerance test<br />
PCP—Primary care provider<br />
NORMAL<br />
FPG
Footnotes<br />
1. American Diabetes Association: <strong>Clinical</strong> Practice <strong>Guidelines</strong> 2004. Screening for type 2 diabetes. Diabetes Care. 2004;27(suppl<br />
1):S11-4; Diabetes Care. 2005;28(suppl 1):S4-S36.<br />
2. National Cholesterol Education Program Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults<br />
(Adult Treatment Panel III). JAMA. 2001;285(19):2486–97.<br />
3. American College of Endocrinology position statement on the insulin resistance syndrome. Endocr Pract. 2003;9(3):237-52.<br />
4. American Diabetes Association: <strong>Clinical</strong> Practice <strong>Guidelines</strong> 2004. The prevention or delay of type 2 diabetes. Diabetes Care.<br />
2004;27(suppl 1):S47-54; Diabetes Care. 2005;28(suppl 1):S4-S36.<br />
5. Edelstein SL, Knowler WC, Bain RP, et al. Predictors of progression from impaired glucose tolerance to NIDDM: an analysis of six<br />
prospective studies. Diabetes. 1997;46(4):701-10.<br />
6. Sinha R, Fisch G, Teague B, et al. Prevalence of impaired glucose tolerance among children and adolescents with marked obesity.<br />
N Engl J Med. 2002;346(11):802-10. Erratum in: N Engl J Med. 2002;346(22):1756. Correction of dosage error in abstract.<br />
7. See Texas Diabetes Council algorithms for treatment of exercise, weight loss, and nutrition.<br />
8. Knowler WC, Barrett-Connor E, Fowler SE, et al. Diabetes Prevention Program Research Group. Reduction in the incidence of type<br />
2 diabetes with lifestyle intervention or metformin. N Engl J Med. 2002;346(6):393-403 (dose of metformin 850 mg twice daily).<br />
9. No medication is currently FDA-approved for prevention of type 2 diabetes in adults, but a number of studies provide evidence for<br />
drug treatment.<br />
10. Metformin is as effective as lifestyle intervention in individuals 35; metformin is nearly ineffective in<br />
individuals >age 60 or those with BMI
Publication #45-12000<br />
DIABETIC FOOT SCREEN*<br />
* performed every primary care visit (for complete foot exam details, see page 2)<br />
Acute swelling and/or Acute deformity ……………….<br />
Skin breakdown (ulcer):……………………………..<br />
Callus – with deeper color changes …………………<br />
Digital Deformity ……………………………..….….….<br />
or chronic midfoot/rearfoot prominence<br />
History of amputation and/or ulceration ………....…….<br />
Dystrophic Nails &/or Dry Skin …………………….<br />
Neuropathy: using 10-gram nylon monofilament<br />
performed yearly<br />
4 out of 10 sites imperceptible = “yes”<br />
Foot Pulses :<br />
Right : Dorsalis Pedis ……………………..…<br />
Left :<br />
Posterior Tibialis..…………..…… …<br />
Dorsalis Pedis …………….………<br />
Posterior Tibialis..…….……….…<br />
Palpable<br />
NO<br />
YES<br />
Assign Risk Category:<br />
No Present Risk.<br />
_____ 0 No loss of protective sensation, no deformity.<br />
Impending Risk.<br />
_____ 1 No loss of protective sensation. Deformity present.<br />
High Risk.<br />
_____ 2 Loss of Protective sensation with or without<br />
weakness, deformity, callus, pre-ulcer or<br />
history of ulceration.<br />
Adapted from the National Foot Treatment Center<br />
LEAP Program<br />
NONpalpable<br />
Approved<br />
04-23-04<br />
Page 4-A<br />
Page 4-C<br />
Page 4-B<br />
Page 3-C<br />
Page 3<br />
Page 3-D<br />
Page 3-B<br />
Ankle<br />
Brachial<br />
Index<br />
(ABI)—<br />
Page 3-A<br />
9.11 Diabetic Foot Screen, Exam, Care and Referral<br />
Resources & References:<br />
1. International Consensus on the Diabetic Foot, 2003. International Working Group on the Diabetic Foot<br />
(consultative section of the International Diabetes Federation)<br />
2. University of Texas <strong>Health</strong> Science Center-San Antonio Texas-Department of Orthopedics-Division of<br />
Podiatry<br />
3. Scott & White Clinic / Texas A&M University System <strong>Health</strong> Science Center-Department of Surgery,<br />
Division of Podiatry<br />
4. American Diabetes Association: <strong>Clinical</strong> Practice Recommendations. Diabetes Care. 2004; 27[S1]:63-64.<br />
See web site (http://www.texasdiabetescouncil.org) for latest version and disclaimer.<br />
Page 1<br />
H EALTH PLANS<br />
www.cfhp.com<br />
65
DIABETIC FOOT EXAM**<br />
**Performed Initially at Diagnosis, Annually In Primary Care<br />
FOOT<br />
HISTORY<br />
1. Ulcers: location, time to heal, wound care necessary for healing<br />
2. Infections: type, bacteria involved, medical treatment necessary<br />
3. Amputations: type, time to heal, modalities used in healing process<br />
4. Surgeries/Injuries: type, location<br />
FOOT EXAM<br />
Vascular<br />
(Vasc)<br />
Neurologic<br />
(Neuro)<br />
1. Palpate DP, PT pulses (present or absent)<br />
2. Temperature gradient: from ankle to toes, focal “hot spots”<br />
3. General Color: pink, palor, rubor on dependency<br />
4. Digital Capillary refill time: in seconds<br />
5. ABI: for both DP & PT arteries (abnl if 10 secs) OR Biothesiometer<br />
(>25 volts)—tested at hallux<br />
3. Tactile sensation (light touch): via cotton wool (dorsum of foot)<br />
4. Reflexes: Achilles tendon<br />
Dermatologic<br />
(Derm)<br />
1. General skin turgor/texture<br />
2. Focal lesions: calluses (debride to fully assess), cracks, pigmentation<br />
3. Interdigital: calluses, maceration<br />
4. Nails: incurvated, nail plate thickness, coloration, inappropriate self-care<br />
Musculoskeletal<br />
(Msk)<br />
1. General Range of Motion: ankle, subtalar, midtarsal, metarsophalangeal<br />
2. Foot type: rectus, pes planus, pes cavus, Charcot foot<br />
3. Digits: hammertoes, claw toes, mallet toes, bunion/hallux abductovalgus<br />
4. Bony prominences<br />
Footwear<br />
1. Type<br />
2. Wear pattern: outsole and upper counter distortion<br />
3. Insole inspection: foreign bodies, staining, excessive wear<br />
4. Socks: foreign bodies, staining, excessive wear<br />
Social<br />
1. Tobacco/alcohol/drug use<br />
2. Work environment/foot demands/footwear requirements<br />
3. Physical activities: footwear used<br />
4. Family support: marital status, spouse/family involvement in health<br />
5. Education: diabetes self-management<br />
Page 2<br />
66 H EALTH PLANS<br />
www.cfhp.com
DIABETIC FOOT CARE/REFERRAL ALGORITHM<br />
Complete Diabetic Foot Exam** (see page 2)<br />
NORMAL (NL) EXAM<br />
NL vasc<br />
NL neuro<br />
NL msk<br />
NL derm<br />
MD/DO/DPM<br />
(or physician extender)<br />
DM FOOT EDUCATION<br />
-patient/family (Diabetes Self-<br />
Management Education)<br />
-verbal/written<br />
-websites<br />
-clinic phone #s<br />
ABBREVIATIONS:<br />
MD = medical doctor<br />
DO = doctor of osteopathy<br />
DPM = doctor of podiatric medicine (Podiatrist)<br />
NL = normal<br />
ABNL = abnormal<br />
ABI = ankle/brachial index<br />
TCPO2 = transcutaneous oxygen pressure<br />
NCV = nerve conduction velocities<br />
PSSD = pressure specified sensory device<br />
REPEAT Diabetic Foot Screen*<br />
-per MD, DO, physician extender visits<br />
or DPM exam<br />
REPEAT EVERY VISIT<br />
ABNORMAL (ABNL)<br />
EXAMS<br />
NORMAL testing-repeat per change in exam<br />
or onset symptoms<br />
A<br />
ABNL VASC<br />
NL neuro<br />
NL msk<br />
NL derm<br />
VASCULAR<br />
CONSULT/TESTING<br />
Consider : PVR, Seg.pres., ABI, TCPO2<br />
-peripheral arteriogram as indicated<br />
-intervention as indicated to re-establish<br />
blood flow<br />
Documentation<br />
of vascular<br />
disease OR<br />
Post intervention<br />
with<br />
improvement<br />
-EDUCATION: signs/symptoms<br />
-HIGH RISK foot status<br />
-Foot screen every MD/DO/DPM,<br />
or physician extender visit<br />
B<br />
NL vasc<br />
ABNL NEURO<br />
NL msk<br />
NL derm<br />
NEURO or PM&R CONSULT<br />
Consider: NCV, PSSD<br />
-other causes: consider and rule out as indicated<br />
-if painful consider<br />
pharmaceutical vs. surgical treatment<br />
-EDUCATION: signs/symptoms<br />
-HIGH RISK foot status<br />
-Foot screen every MD/DO/DPM,<br />
or physician extender visit, PRN<br />
C<br />
NL vasc<br />
NL neuro<br />
ABNL MSK<br />
NL derm<br />
COMPLETE BIOMECHANICAL EXAM<br />
(Podiatrist, Orthopedist)<br />
-discuss clinical significance<br />
-Treatment options: surgical, non-surgical<br />
-EDUCATION: signs/symptoms<br />
-Intervention: surgery→healed = low risk<br />
-Biomech: shoes, orthoses, phys.medicine<br />
-Follow up DPM per modality needed<br />
-Foot screen: every MD/DO/physician<br />
extender visit<br />
D<br />
NL vasc<br />
NL neuro<br />
NL msk<br />
ABNL DERM<br />
Dystrophic (thick,<br />
discolored) toenails<br />
-Debride/reduce<br />
-Culture as needed<br />
-Educate on condition management<br />
-Referral as needed (podiatrist,<br />
dermatologist)<br />
Dry skin, fissures<br />
-Diagnostic tests as indicated, e.g. for fungus<br />
-Topicals as indicated<br />
-referral as indicated<br />
Ingrown toenail<br />
-Instruct on proper nail care<br />
-Matrixectomy if NL vasc exam<br />
Page 3<br />
H EALTH PLANS<br />
www.cfhp.com<br />
67
A<br />
Peripheral Sensory<br />
NEUROPATHY<br />
&<br />
UNILATERAL<br />
SWELLING /calor<br />
-x-ray exam<br />
-r/o infection<br />
Deep venous<br />
thrombosis (DVT)<br />
B<br />
C<br />
HYPERKERATOSIS<br />
With underlying<br />
sub-epidermal<br />
hemorrhage<br />
(no ulceration)<br />
ULCER<br />
-assess/document<br />
HIGH RISK SCENARIO AND ULCER MANAGEMENT<br />
NO SKIN BREAKDOWN<br />
or LESION, no erythema<br />
SKIN<br />
BREAKDOWN<br />
Treat as ULCER<br />
4-C (below)<br />
EXTREMELY HIGH<br />
PROBABILITY OF CHARCOT<br />
ARTHROPATHY<br />
CAUTION<br />
Follow pathways for associated abnl VASC, NEURO as indicated<br />
1. DEBRIDE callus<br />
2. Re-examine MSK exam for<br />
underlying cause – follow 3-C<br />
1. OFF-LOAD as needed<br />
(change insole, offloading devices as<br />
indicated)<br />
2. Assess FOOTWEAR & INSOLES<br />
for causes, prevention<br />
Once healed = patient remains extremely HIGH RISK—frequent foot exams/education<br />
Treat as such until proven otherwise<br />
COMPLETE OFF-LOADING OF<br />
EXTREMITY to prevent severe<br />
foot/ankle deformity<br />
Consider Double ETIOLOGY,<br />
OFF-LOAD to prevent<br />
severe foot/ankle deformity<br />
1. Re-examine/debride q 3–7 days until skin<br />
normalized<br />
2. Progress back to normal activities/footwear<br />
based on etiology & risk factors<br />
IMMEDIATE<br />
DEBRIDEMENT &<br />
Wound Care<br />
1.Local wound care, dressings per etiology<br />
and clinical course<br />
2.Surgical (OR) treatment if indicated<br />
1. Frequent re-assessment & re-debridements as indicated<br />
2. Continued changes in dressings/wound care<br />
3. Advanced wound care if needed<br />
GRADE ULCER<br />
1. Assess size<br />
depth, tissue<br />
levels<br />
2. X-ray exam<br />
GRADE 1 GRADE 2 GRADE 3<br />
Superficial full thickness<br />
- not penetrating deeper<br />
than dermis<br />
Deep ulcer (below dermis)<br />
-subcutaneous structures (fascia,<br />
muscle, tendon)<br />
All subsequent layers involved<br />
-including bone &/or joint<br />
-assess probing to bone/soft tissue tracts<br />
TYPE of ulcer<br />
-underlying<br />
etiology<br />
1- NEUROPATHIC<br />
2- ISCHEMIC<br />
3 -NEURO-ISCHEMIC<br />
Assess/manage causal<br />
pathway(s) 3–A, B, C<br />
OFF-LOAD (relieve pressure)<br />
-non-weightbearing essential<br />
-crutches, walkers, modified<br />
shoes/insoles, total contact cast, etc.<br />
INFECTION<br />
Assess: fever, WBC,<br />
ESR, erythema, calor,<br />
drainage, necrosis,<br />
foreign material<br />
1. Inflammatory response may be mitigated by diabetic complications<br />
2. Outpatient vs. inpatient based on severity of infection & co-morbidity management<br />
Culture & Sensitivity via<br />
-tissue at wound base<br />
-aspirating pus<br />
-swab base of wound AFTER debridement<br />
-bone culture if suspect osteomyelitis<br />
-blood if systemic toxicity suspected<br />
ETIOLOGIC AGENTS<br />
-Aerobic gram positive cocci most frequent<br />
(staphylococcus)<br />
-Gram negative & anaerobes usually part of<br />
polymicrobial, chronic necrotic ulcers<br />
ANTIBIOTICS—consider<br />
-local institutional and<br />
community susceptibility<br />
data when prescribing<br />
-published efficacy data<br />
Page 4<br />
68 H EALTH PLANS<br />
www.cfhp.com
Publication # 45-12083<br />
WEIGHT MANAGEMENT ALGORITHM<br />
FOR OVERWEIGHT CHILDREN AND ADOLESCENTS 1<br />
Normal 2<br />
95 th %ile BMI for Age & Gender<br />
Age & Gender; Rapid Wt Gain 2<br />
Assess for Comorbidities 3<br />
Sleep Apnea; Pseudotumor Cerebri; Dyslipidemia (Elevated LDL-C and/or TG; Low HDL-C); HTN;<br />
NAFLD; GERD; Wt-bearing Joint Pain; PCOS /Hyperandrogenism; AN; Psychological Adjustment Disorders; T2DM (FPG>126 mg/dL;<br />
Post Challenge PG >200 mg/dL)<br />
Assess for Risk Factors and/or Contributing Factors<br />
Medications 4 ; Hypothyroidism; Cushing Syndrome; Prader-Willi Syndrome; SGA; Low Birth Wt; Post Malignancy Treatment<br />
Initial Wt Loss Targets 5 (1 st 6 Months)<br />
• >95 th %ile BMI for Age & Gender<br />
• >85 th %ile BMI with Comorbidities<br />
Pubertal: =10% Body Wt Loss<br />
Pre-pubertal: >age 7 = 1–2 lbs per Month Wt Loss<br />
6 months<br />
>6 months<br />
Motivated & Targets Not Met<br />
Pt/Family Not Motivated Educate Patient and Family; Manage<br />
Comorbidities and Risk Factors;<br />
Reassess Readiness Periodically<br />
Pt/Family Motivated<br />
>6 months<br />
Pt/Family Not Motivated<br />
Targets Not Met<br />
Pt/Family Motivated<br />
Consider Obesity Pharmacologic Monotherapy as Adjunct to Lifestyle<br />
Changes if BMI >27 with Comorbidities or if BMI >30<br />
Appetite Suppressant Lipase Inhibitor<br />
Sibutramine 6 Orlistat 7<br />
Contraindicated in: Contraindicated in:<br />
Uncontrolled HTN; Chronic Malabsorption<br />
Glaucoma (Narrow-angle) Cholestasis; Orlistat<br />
Arrhythmia; CVA; CVD; Hypersensitivity;<br />
CHF; Concurrent SSRI; Concurrent Cyclosporin Therapy;<br />
MAOI Therapy; Pregnancy; Pregnancy<br />
Bulimia/Anorexia Nervosa Hx<br />
See web site (http://www.texasdiabetescouncil.org) for latest version and disclaimer. See reverse side for more information.<br />
9.12 Weight Management Algorithm Overweight Children & Adolcents<br />
H EALTH PLANS<br />
www.cfhp.com<br />
69
ABBREVIATIONS<br />
AN: Acanthosis Nigricans<br />
CHF: Congestive Heart Failure<br />
CVA: Cerebrovascular Accident<br />
CVD: Cardiovascular Disease<br />
FPG: Fasting Plasma Glucose<br />
GERD: Gastro-esophageal Reflux Disease<br />
HCP: <strong>Health</strong> Care Professional<br />
HDL-C: High-density Lipoprotein Cholesterol<br />
HTN: Hypertension (>95 th %ile Blood Pressure for Age & Gender & Ht)<br />
LDL-C: Low-density Lipoprotein Cholesterol<br />
MAOI: Monoamine Oxidase Inhibitors<br />
NAFLD: Non-alcoholic Fatty Liver Disease<br />
PCOS: Polycystic Ovary Syndrome<br />
SGA: Small for Gestational Age<br />
SSRI: Selective Serotonin Reuptake Inhibitors<br />
T2DM: Type 2 Diabetes Mellitus<br />
TG: Triglycerides<br />
Criteria for Bariatric Surgery 8<br />
Adolescents being considered for bariatric surgery should:<br />
• Have failed 6 months of organized attempts at wt management, as<br />
determined by their primary care provider<br />
• Have attained or nearly attained physiologic maturity<br />
• Be severely obese (BMI >40) with serious obesity-related<br />
comorbidities or BMI >50 with less severe comorbidities<br />
• Demonstrate commitment to comprehensive medical and psychologic<br />
evaluations both before and after surgery<br />
• Agree to avoid pregnancy for at least 1 yr postoperatively<br />
• Be capable of and willing to adhere to nutritional guidelines<br />
postoperatively<br />
• Provide informed consent to surgical treatment<br />
• Demonstrate decisional capacity<br />
• Have a supportive family environment<br />
FOOTNOTES<br />
1. Adapted from the Texas Diabetes Council’s Weight Loss Algorithm for Overweight<br />
and Obese Adults<br />
2. Barlow SE, Dietz WH. Obesity evaluation and treatment: Expert Committee<br />
recommendations. The Maternal and Child <strong>Health</strong> Bureau, <strong>Health</strong> Resources and<br />
Services Administration and the Department of <strong>Health</strong> and Human Services.<br />
Pediatrics. 1998;102(3):E29<br />
3. Barlow SE, Dietz WH. Obesity evaluation and treatment: Expert Committee<br />
recommendations. The Maternal and Child <strong>Health</strong> Bureau, <strong>Health</strong> Resources and<br />
Services Administration and the Department of <strong>Health</strong> and Human Services.<br />
Pediatrics. 1998;102(3):E29; and American Diabetes Association. Type 2 diabetes<br />
in children and adolescents. Pediatrics. 2000;105(3 Pt 1):671-80; Refer to<br />
appropriate Texas Diabetes Council algorithms<br />
4. Medications that affect insulin sensitivity:<br />
Inhaled steroids:<br />
1000 mcg/day fluticasone<br />
(Flovent)<br />
2000 mcg/day of all others<br />
Oral Steroids:<br />
20 days in previous year, or<br />
any within 60 days of screening<br />
L- asparaginase<br />
FK506 (Tacrolimus)<br />
Cyclosporine (Neoral/<br />
Sandimmune)<br />
Niacin<br />
Medications known to cause wt gain:<br />
Risperidone (Risperdal)<br />
Olanzapine (Zyprexa)<br />
Clozapine (Clozaril)<br />
Quetiapine (Seroquel)<br />
Ziprasidone (Geodon)<br />
Carbamazepine (Tegretol)<br />
Valproic acid (Depakote/Depakene/Depacon)<br />
Tricyclic Antidepressants<br />
Lithium<br />
Insulin/Insulin Analogs<br />
Sulfonylureas<br />
Cyproheptadine<br />
Estrogens/Progestins<br />
5. No evidence-based outcomes data are yet available for weight loss targets<br />
6. Berkowitz RI, Wadden TA, Tershakovec AM, et al. Behavior therapy and<br />
sibutramine for the treatment of adolescent obesity: a randomized controlled trial.<br />
JAMA. 2003;289(14):1805-12; sibutramine is FDA-approved for ages >16 yr<br />
7. McDuffie JR, Calis KA, Uwaifo GI, et al. Efficacy of orlistat as an adjunct to<br />
behavioral treatment in overweight African American and Caucasian adolescents<br />
with obesity-related co-morbid conditions. J Pediatr Endocrinol Metab.<br />
2004;17(3):307-19; orlistat is FDA-approved for ages >12 yr<br />
8. Inge TH, Krebs NF, Garcia VF, et al. Bariatric surgery for severely overweight<br />
adolescents: concerns and recommendations. Pediatrics. 2004;114(1):217-23<br />
9. Rosner B, Prineas R, Loggie J, et al. Percentiles for body mass index in U.S.<br />
children 5 to 17 years of age. J Pediatr. 1998;132(2):211-22.<br />
Additional References<br />
Bobo N, Evert A, Gallivan J, et al. An update on type 2 diabetes in youth from the<br />
National Diabetes Education Program. Pediatrics. 2004;114(1):259-63<br />
Garcia VF, Langford L, Inge TH. Application of laparoscopy for bariatric surgery in<br />
adolescents. Curr Opin Pediatr. 2003;15(3):248-55<br />
Krebs NF, Jacobson MS; American Academy of Pediatrics Committee on Nutrition.<br />
Prevention of pediatric overweight and obesity. Pediatrics. 2003;112(2):424-30<br />
70 H EALTH PLANS<br />
www.cfhp.com
9<br />
H EALTH PLANS<br />
www.cfhp.com<br />
71
2 to 20 years: Girls<br />
Body mass index-for-age percentiles<br />
NAME<br />
RECORD #<br />
Date Age Weight Stature BMI* Comments<br />
95<br />
BMI<br />
27<br />
90<br />
26<br />
85<br />
25<br />
24<br />
75<br />
23<br />
22<br />
21<br />
50<br />
28<br />
20<br />
25<br />
19<br />
10<br />
18<br />
5<br />
17<br />
kg/m 2<br />
16<br />
15<br />
14<br />
13<br />
12<br />
AGE (YEARS)<br />
2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20<br />
Published May 30, 2000 (modified 10/16/00).<br />
SOURCE: Developed b y the National Center for <strong>Health</strong> Statistics in collaboration with<br />
the National Center for Chronic Disease Prevention and <strong>Health</strong> Promotion (2000).<br />
http://www.cdc.gov/growthcharts<br />
BMI<br />
35<br />
34<br />
33<br />
32<br />
31<br />
30<br />
29<br />
27<br />
26<br />
25<br />
24<br />
23<br />
22<br />
21<br />
20<br />
19<br />
18<br />
17<br />
16<br />
15<br />
14<br />
13<br />
12<br />
kg/m 2<br />
2 to 20 years: Boys<br />
Body mass index-for-age percentiles<br />
NAME<br />
RECORD #<br />
Date Age Weight Stature BMI* Comments<br />
95<br />
BMI<br />
27<br />
90<br />
26<br />
85<br />
25<br />
24<br />
75<br />
23<br />
22<br />
50<br />
28<br />
21<br />
25<br />
20<br />
10<br />
19<br />
5<br />
18<br />
kg/m 2<br />
17<br />
16<br />
15<br />
14<br />
13<br />
12<br />
AGE (YEARS)<br />
2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20<br />
Published May 30, 2000 (modified 10/16/00).<br />
SOURCE: Developed b y the National Center for <strong>Health</strong> Statistics in collaboration with<br />
the National Center for Chronic Disease Prevention and <strong>Health</strong> Promotion (2000).<br />
http://www.cdc.gov/growthcharts<br />
BMI<br />
35<br />
34<br />
33<br />
32<br />
31<br />
30<br />
29<br />
27<br />
26<br />
25<br />
24<br />
23<br />
22<br />
21<br />
20<br />
19<br />
18<br />
17<br />
16<br />
15<br />
14<br />
13<br />
12<br />
kg/m 2<br />
72 H EALTH PLANS<br />
www.cfhp.com
Revised 10-25-07<br />
IV INSULIN INFUSION PROTOCOL FOR CRITICALLY-ILL ADULT PATIENTS<br />
IN THE ICU SETTING<br />
This algorithm is not intended to be used for those individuals with Type 1 diabetes,<br />
diabetic ketoacidosis or hyperglycemic hyperosmolar states.<br />
Target Range for Glycemic Control: 80-140 mg/dL (Generally 110 mg/dL)<br />
1. Standard drip 100 units/100 mL 0.9% NaCl .<br />
Approved IV insulins include Regular, aspart and glulisine<br />
Publication #: 45-12063<br />
2. Start IV insulin therapy when glucose is above target range. Insulin infusions should be<br />
discontinued when<br />
a. Patient has no history of diabetes and is receiving 80 units/day of insulin as an outpatient.<br />
• Algorithm 3: For patients not controlled on Algorithm 2. NO PATIENT<br />
STARTS HERE without authorization from the endocrine service.<br />
• Algorithm 4: For patients not controlled on Algorithm 3. NO PATIENT<br />
STARTS HERE<br />
Algorithm 1<br />
Algorithm 2<br />
Algorithm 3<br />
Algorithm 4<br />
Glucose units/h Glucose units/h Glucose units/h Glucose units/h<br />
Revised 10-25-07 Publication #: 45-12063<br />
6. Moving from Algorithm to Algorithm<br />
• Moving Up: When glucose remains outside the target range after titrating insulin<br />
• Moving Down: When glucose is 60 mg/dl in 1 hour<br />
7. Patient Monitoring<br />
• Hourly venous (lab) determinations until glucose
Revised 10-25-07 Publication #: 45-12063<br />
REFERENCES:<br />
1. Garber AJ, Moghissi ES, Bransome ED Jr., et al; American College of Endocrinology Task Force<br />
on Inpatient Diabetes Metabolic Control. American College of Endocrinology position statement on<br />
inpatient diabetes and metabolic control. Endocr Pract. 2004;10 (Suppl 2):4–9.<br />
2. Bode BW, Braithwaite SS, Steed RD, et al. Intravenous insulin infusion therapy:<br />
indications, methods, and transition to subcutaneous insulin therapy. Endocr Pract.<br />
2004;10 (Suppl 2):71–80.<br />
3. Goldberg PA, Siegel MD, Sherwin RS, et al. Implementation of a safe and effective insulin<br />
infusion protocol in a medical intensive care unit. Diabetes Care. 2004;27(2):461–7.<br />
4. Vora AC, Saleem TM, Polomano RC, et al. Improved perioperative glycemic control by<br />
continuous insulin infusion under supervision of an endocrinologist does not increase costs<br />
in patients with diabetes. Endocr Pract. 2004;10(2):112–8.<br />
5. Chaudhuri A, Janicke D, Wilson MF, et al. Anti-inflammatory and profibrinolytic effect of insulin<br />
in acute ST-segment-elevation myocardial infarction. Circulation.<br />
2004;109(7):849–54.<br />
6. Trence DL, Kelly JL, Hirsch IB. The rationale and management of hyperglycemia for inpatients<br />
with cardiovascular disease: time for change. J Clin Endocrinol Metab.<br />
2003;88(6):2430–7.<br />
7. Lien L, Spratt S, Woods Z, et al. A new intravenous insulin nomogram in intensive care<br />
units improves management of persistent hyperglycemia (Abstract). Diabetes. 2003;52 (Suppl<br />
1):A125.<br />
8. Preiser JC, Devos P, Van den Berghe G. Tight control of glycaemia in critically ill<br />
patients. Curr Opin Clin Nutr Metab Care. 2002;5(5):533–7.<br />
9. Markovitz LJ, Wiechmann RJ, Harris N, et al. Description and evaluation of a glycemic<br />
management protocol for patients with diabetes undergoing heart surgery. Endocr Pract.<br />
2002;8(1):10–8.<br />
10. Van den Berghe G, Wouters P, Weekers F, et al. Intensive insulin therapy in the critically ill<br />
patients. N Engl J Med. 2001;345(19):1359–67.<br />
11. Hirsch IB. Insulin therapy for diabetes: is the future now? Clin Diabetes. 2001;19:146–7.<br />
12. Furnary AP, Zerr KJ, Grunkemeier GL, et al. Continuous intravenous insulin infusion<br />
reduces the incidence of deep sternal wound infection in diabetic patients after cardiac<br />
surgical procedures. Ann Thorac Surg. 1999;67(2):352–60.<br />
13. Malmberg K, Ryden L, Efendic S, et al. Randomized trial of insulin-glucose infusion<br />
followed by subcutaneous insulin treatment in diabetic patients with acute myocardial<br />
infarction (DIGAMI study): effects on mortality at 1 year. J Am Coll Cardiol.<br />
1995;26(1):57–65.<br />
14. Woo J, Lam CW, Kay R, et al. The influence of hyperglycemia and diabetes mellitus on<br />
immediate and 3-month morbidity and mortality after acute stroke. Arch Neurol. 1990;<br />
47(11):1174–77.<br />
15. Watts NB, Gebhart SS, Clark RV, et al. Postoperative management of diabetes mellitus:<br />
steady-state glucose control with bedside algorithm for insulin adjustment. Diabetes Care.<br />
1987;10(6):772–8.<br />
16. Pittas AG, Siegel RD, Lau J. Insulin therapy for critically ill hospitalized patients: a metaanalysis<br />
of randomized controlled trials. Arch Intern Med. 2004;164(18):2005-11.<br />
17. Desantis AJ, Schmeltz LR, Schmidt K et.al. Inpatient management of hyperglycemia: The<br />
northwestern experience. Endocrine Practice. 2006;12(5):491-505.<br />
18. Donaldson S, Villanuueva G, Rondinelli L, Baldwin D. Rush university guidelines and<br />
protocols for the management of hyperglycemia in hospitalized patients. Elimination of the<br />
sliding scale and improvement of glycemic control throughout the hospital. The Diabetes<br />
Educator. 2006;32(6):954-962.<br />
19. Hirsch IB. An endocrinologist’s view on the practical use of insulin. Insulin. 2006;1(Suppl<br />
A):S18-23.<br />
20. Novo Nordisk detemir monograft, 2005. Studies 1337,1530, NNTTT, 1373.<br />
3<br />
H EALTH PLANS<br />
www.cfhp.com<br />
75
9.14 ICU Insulin Orders<br />
Revised 2-21-08<br />
Publication #E45-12614<br />
ICU INSULIN ORDERS<br />
IV INSULIN INFUSION PROTOCOL<br />
(Not intended for use in patients with type 1 diabetes, DKA or hyperglycemic hyperosmolar states)<br />
1) Start IV Insulin Flow Sheet and keep record at bedside<br />
2) Start IV: ___ D5W at 100ml/h<br />
___ D5W½NS at __________ ml/h<br />
___ Other:_______________________________________________<br />
3) Mix standard insulin drip:<br />
• 100 units Regular, aspart or glulisine insulin in 100 cc NS (1 unit insulin /cc) (Circle one)<br />
4) Give initial insulin bolus:<br />
• Bolus units of I.V. insulin = Glucose ÷ 100 (e.g. if glucose = 240 mg/dL, give 2.5 units)<br />
5) Start insulin infusion:<br />
• Initial infusion rate of insulin units/h = Glucose ÷ 100 ( e.g. if glucose=240, begin 2.5 units/h)<br />
6) Target range for glucose:<br />
• Low Target (circle one) High Target (circle one)<br />
70 100 or ________ mg/dL 110 120 140 or _______ mg/dL<br />
7) Monitor capillary (finger stick) glucose every hour:<br />
• Obtain lab glucose if finger stick BG is 400 mg/dL<br />
• Change frequency of glucose monitoring to:___________________________________<br />
8) Adjust insulin infusion rate each hour after initial insulin bolus and infusion<br />
Start on Algorithm 1 (No patient begins on Algorithm 3 or 4 without endocrine service authorization)<br />
Start on Algorithm 2 (s/p CABG, transplant, glucocorticoids or >80 units/d insulin outpatient)<br />
• Move up or down on the same algorithm each hour if glucose remains outside the target range<br />
• Advance to the next algorithm (i.e. 1→2 etc.) if outside target range at highest infusion rate<br />
• Treat for hypoglycemia is glucose 60 mg/dL in 1 hour<br />
Algorithm 1 Algorithm 2 Algorithm 3 Algorithm 4<br />
BG units/h BG units/h BG units/h BG units/h<br />
Revised 2-21-08<br />
Publication #: E45-12614<br />
ICU INSULIN ORDERS, CONTINUED<br />
IV INSULIN INFUSION PROTOCOL<br />
(Not intended for use in patients with type 1 diabetes, DKA or hyperglycemic hyperosmolar states)<br />
9) Treat for hypoglycemia if glucose
Screening and Management of Hyperglycemia in the Geriatric Population<br />
Geriatric is defined as age 65+ years 1<br />
Diabetes Management<br />
Screening Recommendations for IFG, IGT & DM<br />
FPG Annually 2 : if above 100 mg/dL confirm with<br />
consider checking postload glucose 2<br />
repeat fasting glucose. Avoid OGTT if possible 2<br />
if below 100 and high risk based on<br />
multiple risk factors and/or metabolic syndrome<br />
Diabetes Management<br />
Goals of Therapy: consider comorbidities<br />
before setting targets 1 :<br />
A1c < 7% if attainable without significant<br />
hypoglycemia 3<br />
BP
Abbreviations<br />
AGI Alpha-Glucosidase Inhibitors<br />
ACE inhibitor Angiotensin Converting Enzyme Inhibitor<br />
ARB Angiotensin Receptor Blocker<br />
BAR Bile Acid Resin (colesevelam)<br />
CAD Coronary Artery Disease<br />
DPP-4 Dipeptidyl peptidase-4 Inhibitor<br />
FPG Fasting Plasma Glucose<br />
IFG Impaired Fasting Glucose<br />
IGT Impaired Glucose Tolerance<br />
GAD* Glutamic Acid Decarboxylase<br />
ICA* Islet Cell Antibodies<br />
OGTT Oral Glucose Tolerance Test<br />
SU Sulfonylurea<br />
TZD Thiazolidinedione<br />
*note: ICA and GAD antibodies usually take 1-2 weeks to be reported. If result is positive then<br />
patient has autoimmune mediated diabetes and insulin needs to be considered and oral agents<br />
may need to be discontinued<br />
Hypoglycemia: Autonomic hypoglycemic warning<br />
signs may not be recognized in older adults due to<br />
changes in counter regulatory hormone response.<br />
Symptoms of hypoglycemia are often mistaken for<br />
co-existing medical conditions including postural<br />
hypotension, Parkinson’s, dementia, traumatic brain<br />
injury or CVA. Patients that cannot communicate<br />
verbally with caregivers are at greater risk.<br />
References<br />
1. Sinclair A, Finucane P, eds. Diabetes in Old Age. 2nd ed. Chichester, UK: John Wiley & Sons, Ltd; 2001.<br />
2. Madden KM, Tedder G, Lockhart C. The oral glucose tolerance test induces myocardial ischemia in healthy older adults. <strong>Clinical</strong> and Investigative<br />
Medicine 2007;30(3):E118-26.<br />
3. Chang AM, Smith MJ, Bloem CJ, Galecki AT, Halter JB. Effect of lowering postprandial hyperglycemia on insulin secretion in older people with impaired<br />
glucose tolerance. Am J Physiol Endocrinol Metab 2004;287(5):E906-11.<br />
4. Meneilly GS, Cheung E, Tuokko H. Altered responses to hypoglycemia of healthy elderly people. J Clin Endocrinol Metab 1994;78(6):1341-8.<br />
5. Munshi M, Grande L, Hayes M, et al. Cognitive dysfunction is associated with poor diabetes control in older adults. Diabetes Care 2006;29(8):1794-9.<br />
6. Care California <strong>Health</strong>care Foundation/American Geriatrics Society Panel in Improving Care for Elders with D. <strong>Guidelines</strong> for Improving the Care of the<br />
Older Person with Diabetes Mellitus. J Am Geriatr Soc 2003;51(5s):265-80.<br />
7. Katakura M, Naka M, Kondo T, et al. Prospective analysis of mortality, morbidity, and risk factors in elderly diabetic subjects: Nagano study. Diabetes<br />
Care 2003;26(3):638-44.<br />
8. Lipscombe LL, Gomes T, Levesque LE, Hux JE, Juurlink DN, Alter DA. Thiazolidinediones and cardiovascular outcomes in older patients with diabetes.<br />
JAMA 2007;298(22):2634-43.<br />
9. Durso SC. Using clinical guidelines designed for older adults with diabetes mellitus and complex health status. JAMA 2006;295(16):1935-40.<br />
10. Kuo HK, Jones RN, Milberg WP, et al. Effect of blood pressure and diabetes mellitus on cognitive and physical functions in older adults: a longitudinal<br />
analysis of the advanced cognitive training for independent and vital elderly cohort. J Am Geriatr Soc 2005;53(7):1154-61.<br />
11. McBean AM, Huang Z, Virnig BA, Lurie N, Musgrave D. Racial variation in the control of diabetes among elderly medicare managed care beneficiaries.<br />
Diabetes Care 2003;26(12):3250-6.<br />
12. Holt RM, Schwartz FL, Shubrook JH. Diabetes care in extended-care facilities: appropriate intensity of care? Diabetes Care 2007;30(6):1454-8.<br />
13. Bertoni AG, Hundley WG, Massing MW, Bonds DE, Burke GL, Goff DC, Jr. Heart failure prevalence, incidence, and mortality in the elderly with diabetes.<br />
Diabetes Care 2004;27(3):699-703.<br />
14. Okereke OI, Kang JH, Cook NR, et al. Type 2 diabetes mellitus and cognitive decline in two large cohorts of community-dwelling older adults. J Am<br />
Geriatr Soc 2008;56(6):1028-36.<br />
15. The ADVANCE Collaborative Group. Intensive Blood Glucose Control and Vascular Outcomes in Patients with Type 2 Diabetes. N Engl J Med<br />
2008;358(24):2560-72.<br />
16. The Action to Control Cardiovascular Risk in Diabetes Study G. Effects of Intensive Glucose Lowering in Type 2 Diabetes. N Engl J Med<br />
2008;358(24):2545-59.<br />
17. European Diabetes Working Group for Older People. <strong>Clinical</strong> <strong>Guidelines</strong> for Type 2 Diabetes: European Union Geriatrics Medicine Society; 2004.<br />
H EALTH PLANS<br />
www.cfhp.com<br />
79
9.16 Orders for Adults with DKA and Hyperglycemic Hyperosmolar State<br />
Orders for Adults with DKA and Hyperglycemic Hyperosmolar State (HHS)<br />
These orders may be initiated in the Emergency Department<br />
DKA: Moderate ketonemia, arterial pH 250 mg/dL, serum bicarbonate 600 mg/dL, minimal ketonemia or ketonuria, serum bicarbonate >15 mEq/L, pH ≥7.3<br />
Admit Date: Time: Location: Attending<br />
Diagnosis<br />
Drug allergies or<br />
adverse reactions<br />
Monitor and<br />
Record<br />
No known drug allergies List:<br />
1. Vital signs & I&O every hour until stable, then every 2 hours x 24 hours<br />
Insert Foley if no urine output within first hour or within_________________________ hours<br />
2. STAT fingerstick (capillary) blood glucose<br />
(Use venous or arterial draw if glucose >450 or
Orders for Adults with DKA and Hyperglycemic Hyperosmolar State (HHS)<br />
These orders may be initiated in the Emergency Department<br />
Give initial IV<br />
insulin bolus<br />
Start insulin<br />
infusion<br />
Target range for<br />
glucose<br />
Monitor glucose<br />
every hour<br />
Adjust insulin<br />
infusion rate<br />
Treat<br />
hypoglycemia<br />
Maintenance<br />
IV fluids<br />
Bolus___________ units Regular insulin IV (recommend 10-15 units Regular insulin IV)<br />
Other: Bolus units of insulin in mL NS<br />
Start insulin infusion at ______________________________ units per hour<br />
Recommend infusion rate is calculated as: Glucose mg/dL ÷ 100 (Ex: Glucose=350 → Start 3.5 units/h)<br />
Rate of glucose reduction not to exceed 100 mg/dL per hour<br />
DKA: 100 to 130 mg/dL<br />
Other _________________________________<br />
HHS: Low target:<br />
High target:<br />
Obtain lab glucose if fingerstick blood glucose is >450 or
Orders for Adults with DKA and Hyperglycemic Hyperosmolar State (HHS)<br />
These orders may be initiated in the Emergency Department<br />
Potassium<br />
replacement<br />
Phosphorus<br />
replacement<br />
Sodium<br />
bicarbonate<br />
(DKA)<br />
Alert parameters<br />
for notifying<br />
physician<br />
Call physician if K is 6 mEq/L (Note: Urine output should be >30 mL/hour before starting K + replacement)<br />
Add KCl to IV fluids:<br />
♦ If K is 5.2 mEq/L, hold KCl<br />
♦ Consider KPO 4 instead of KCl if serum PO 4 is low<br />
Other:<br />
Consider if evidence of alcohol abuse, malnutrition, etc.<br />
Give 10 mEq/L KPO 4 in one liter of IV fluid x 1<br />
Other:___________________________________________________________________<br />
Give sodium bicarbonate<br />
If pH 1 hour with no other source of insulin<br />
♦ TPN stopped, interrupted or any change in formulation<br />
♦ Deterioration in mental status<br />
♦ Patient does not respond to above orders for glycemic control<br />
Other_________________________________________________________________<br />
Transition to<br />
SQ insulin<br />
Other orders<br />
Other _________________________________________________________________<br />
Proceed to Texas Diabetes Council Transition Algorithm From I.V. to S.Q. Insulin<br />
Other:<br />
1. ________________________________________________________________________________<br />
2. ________________________________________________________________________________<br />
3.________________________________________________________________________________<br />
4. ________________________________________________________________________________<br />
References:<br />
1. American Diabetes Association. Standards of medical care in diabetes-2008. Diabetes Care. 2008;31(Suppl 1):<br />
S12-S54.<br />
2. Kitabchi AE, Umpierrez GE, Murphy MB, et al. Hyperglycemic crises in adult patients with diabetes. A consensus<br />
statement from the American Diabetes Association. Diabetes Care. 2006;29(12):2739-2748.<br />
3. American Diabetes Association. Hyperglycemic crises in patients with diabetes mellitus (Position Statement).<br />
Diabetes Care. 2004;27 (Suppl 1):S94-S102.<br />
4. Clement S, Braithwaite S, Magee M, et al. Management of diabetes and hyperglycemia in hospitals<br />
(technical review). Diabetes Care. 2004;27:533-591.<br />
5. Lee P, Greenfield JR, Campbell LV. “Mind the gap” when managing ketoacidosis in type 1 diabetes. Diabetes Care.<br />
2008;31(7):e58.<br />
Physician Signature__________________________________________Date_________________Time___<br />
Approved: July 31, 2008<br />
3 of 3<br />
82 H EALTH PLANS<br />
www.cfhp.com
D i a b e t e s t r e a t m e n t a l g o r i t h m s<br />
Transition Algorithm from I.v. to S.Q. Insulin for<br />
Patients with Diabetes or Hyperglycemia<br />
Approved 7/31/08<br />
GOALS: NPO or PO<br />
FpG 100-130 mg/dl<br />
2h pp
D i a b e t e s t r e a t m e n t a l g o r i t h m s<br />
Recommendations for Treatment of Painful<br />
Peripheral Diabetic Neuropathy in Adults<br />
publication #45-12613<br />
Approved 04/26/07<br />
No treatment has been shown to result in superior<br />
pain control compared to another agent<br />
Choice of agent should be based on:<br />
u side effects<br />
u comorbidities<br />
u cost<br />
u concomitant Medications<br />
u realistic expectations: Goal pain relief /partial relief<br />
Evaluate for and treat secondary causes of peripheral neuropathy:<br />
u Glucose control<br />
u Macrocytic anemia, b12, Folic acid or vitamin d deficiency<br />
u lifestyle changes-alcohol & smoking cessation<br />
u radiculopathy<br />
u electrophysiology assessment recommended if glucose control does not improve pain due to<br />
other potential etiologies<br />
Glycemic control<br />
goals should be met,<br />
if possible, prior<br />
to the start of pain<br />
medications<br />
select any of the<br />
agents to initiate at<br />
low dose and titrate<br />
to minimal effective<br />
At least<br />
2 months<br />
change to a different<br />
agent if initial therapy<br />
at minimum is not effective<br />
dose 1 effective dose<br />
or<br />
u refer to specialist<br />
u consider low dose combination therapy if partial pain relief with<br />
any agent<br />
u consider other therapeutic agents with reported efficacy<br />
u consider surgical intervention/referral if other modalities fail<br />
Medications Listed Alphabetically<br />
Pros:<br />
Duloxetine 1<br />
u May also treat depression<br />
Cons:<br />
u May cause nausea, dizzy/drowsy<br />
u use with caution with other<br />
antidepression medication<br />
Pros:<br />
u Generic<br />
Cons:<br />
Gabapentin 1<br />
u saturable absorption gives lower<br />
absorption with increasing doses<br />
u example: absorption at 900mg/day:<br />
60%<br />
3600mg/day: 33%<br />
u some risk of dizzy/drowsiness/<br />
weight gain<br />
u renal adjustment of dose may be<br />
needed<br />
Pros:<br />
Pregabalin 1<br />
u no saturable absorption issues as<br />
with gabapentin<br />
Cons:<br />
u similar mechanism of action to<br />
gabapentin<br />
u some risk of dizzy/drowsiness/<br />
weight gain<br />
u renal adjustment of dose may be<br />
needed<br />
Pros:<br />
u Generic<br />
Cons:<br />
u nausea<br />
u dizziness<br />
Cautions<br />
Tramadol 1<br />
u contraindicated in known seizure<br />
disorder or with MAo inhibitors<br />
u caution with use with other<br />
serotonergic agents<br />
u Avoid abrupt withdrawal<br />
Pros:<br />
Tricyclic antidepressants 1<br />
(TCA’s)<br />
u Generic<br />
Cons:<br />
u Anticholinergic side effects<br />
Cautions<br />
u caution with use with other<br />
antidepressants<br />
u dose-related Qtc prolongation<br />
u caution with other medications that<br />
inhibit cYp450 significantly<br />
Minimum Effective Dose<br />
60 mg daily<br />
Minimum Effective Dose<br />
100-600 mg tid<br />
Minimum Effective Dose<br />
50 mg tid or 150 mg hs<br />
Minimum Effective Dose<br />
50 mg bid<br />
Minimum Effective Dose<br />
12.5-50 mg at bedtime<br />
Other therapeutic agents with reported efficacy:<br />
topical capsaicin, topical lidocaine, venlafaxine, bupropion, opioid<br />
derivatives, alpha-lipoic acid, Mire therapy (Anodyne);<br />
Consider surgical intervention if other modalities fail.<br />
1<br />
refer to prescribing information for titration recommendations Argoff ce et al. Mayo clin. proc. 2006 Apr; 81(4 suppl): s12-25.<br />
1 of 1 – recommendations for treatment of painful peripheral diabetic neuropathy in Adults – Approved 4/26/07 See disclaimer at www.tdctoolkit.org/algorithms_and_guidelines.asp<br />
9.18 Recommendations for Treatment of Painful Peripheral Diabetic Neuropathy in Adults<br />
84 H EALTH PLANS<br />
www.cfhp.com
CFHP has adopted the National Institutes of <strong>Health</strong> (NIH) <strong>Guidelines</strong> on Cholesterol Management in Adults. Based on these<br />
guidelines, the National Heart, Lung, and Blood Institute (NHLBI) developed the Third Report of the Expert Panel on Detection,<br />
Evaluation, and Treatment of High Blood Cholesterol in Adults (Adult Treatment Panel III). A complete copy of the Third Report<br />
are available at their web site (www.nhlbi.nih.gov/guidelines/cholesterol).<br />
The areas addressed in the Report consist of the classification of lipids and lipoproteins, risk assessment for coronary heart<br />
disease (CHD), major lifestyle risk factors, and treatment. Recommendations for special populations such as patients with CHD,<br />
patients at high risk for developing CHD, patients with diabetes, women, older Americans, young adults, and racial and ethnic<br />
groups are provided.<br />
The number one killer of Americans is heart disease. More than one million men and women in the United States have a heart<br />
attack each year and about a half a million die from heart disease. <strong>Community</strong> <strong>First</strong> has chosen to use these guidelines to<br />
promote healthy lifestyles, improve patient outcomes and to help reduce risk for heart disease.<br />
The update of the Adult Treatment Panel III is in development.<br />
10.1 Management of High Blood Cholesterol in Adults<br />
H EALTH PLANS<br />
www.cfhp.com<br />
85
10.2 National Cholesterol Education <strong>Guidelines</strong><br />
NATIONAL CHOLESTEROL EDUCATION PROGRAM (NCEP) GUIDELINES FOR LDL-C 1<br />
TLC Cut Points and LDL-C Goals by Risk Category<br />
Risk Category LDL-C Goal Initiate TLC Consider Drug Therapy<br />
High risk: CHD 1 or CHD<br />
risk equivalents 2 (10-year<br />
risk>20%)<br />
Moderately high risk: 2+ risk<br />
factors 3 (10-year risk 10% to<br />
20%)<br />
< 100 mg/dL (optional goal: ≥ 100 mg/dL 8 > 100 mg/dL 10 (
No CHD; 0 to 1, or 2+ Risk Factors<br />
Initiate TLC diet and exercise<br />
6 wks<br />
If LDL-C goal is not achieved, initiate LDL-C<br />
- lowering drug therapy<br />
6 wks 6 wks<br />
If LDL-C goal is not achieved, intensify therapy with higher dose<br />
or add-on therapy<br />
6 wks<br />
If LDL-C goal is not achieved, intensify therapy or refer<br />
to a lipid specialist<br />
Every 4 to 6 months<br />
Periodically monitor response and adherence to therapy<br />
CHD or CHD Risk Equivalents<br />
(Baseline LDL-C ≥ 130 mg/dL)<br />
Initiate TLC diet and exercise. Simultaneously<br />
initiate LDL-C lowering drug therapy (if LDL-C<br />
< 130 md/dL, simultaneous drug treatment<br />
may be considered)<br />
10.3 Progression of Therapy to Achieve LDL-C Goals<br />
H EALTH PLANS<br />
www.cfhp.com<br />
87
10.4 Drugs Affecting Lipoprotein Metabolism<br />
• Consider drug simultaneously with TLC for CHD and CHD equivalents<br />
• Consider adding drug to TLC after 3 months for other risk categories<br />
Drug Class<br />
HMG CoA<br />
reductase<br />
inhibitors<br />
(statins)<br />
Bile acid<br />
sequestrants<br />
Nicotinic acid<br />
Fibric acids<br />
Agents and Daily Doses<br />
Lovastatin (20-80 mg)<br />
Pravastatin (20-40 mg)<br />
Simvastatin (20-80 mg)<br />
Fluvstatin (20-80 mg)<br />
Atorvastatin (10-80 mg)<br />
Cerivastatin (0.4-0.8 mg)<br />
Cholestyramine (4-16 gm)<br />
Colestipol (5-20 gm)<br />
Colessevelam (2.6-3.8 gm)<br />
Immediate release<br />
(crystalline) nicotinic<br />
acid (1.5-3 gm), extended<br />
release nicotinic acid<br />
(Niaspan®)(1-2 gm),<br />
sustained release nicotinic<br />
acid (1-2 gm)<br />
Gemfibrozil (600 mg BID)<br />
Fenofibrate (200 mg)<br />
Clofibrate (1000 mg BID)<br />
Lipid/Lipoprotein<br />
Effects<br />
LDL ↓18-55%<br />
HDL ↑ 5-15%<br />
TG ↓ 7-30%<br />
LDL ↓15-30%<br />
HDL ↑ 3-5%<br />
TG No change or<br />
increase<br />
LDL ↓5-25%<br />
HDL ↑ 15-35%<br />
TG ↓20-50%<br />
LDL ↓5-20%<br />
(may be increased in<br />
patients with high TG)<br />
HDL ↑ 10-20%<br />
TG ↓20-50%<br />
Side Effects<br />
Myopathy<br />
Increased liver<br />
enzymes<br />
Gastrointestinal<br />
distress<br />
Constipation<br />
Decreased absorption<br />
of other drugs<br />
Flushing<br />
Hyperglycemia<br />
Hyperglycemia (or<br />
gout)<br />
Upper GI distress<br />
Hepatotoxicity<br />
Dyspepsia<br />
Gallstones<br />
Myopathy<br />
Contraindications<br />
Absolute:<br />
• Active or chronic liver<br />
disease<br />
Relative:<br />
• Concomitant use of<br />
certain drugs*<br />
Absolute:<br />
• dysbetalipoproteinemia<br />
• TG > 400 mg/dL<br />
Relative:<br />
• TG > 200 mg/dL<br />
Absolute:<br />
• Chronic liver disease<br />
• Severe gout<br />
Relative:<br />
• Diabetes<br />
• Hyperuricemia<br />
• Peptic ulcer disease<br />
Absolute:<br />
• Severe renal disease<br />
• Severe hepatic disease<br />
Cyclosporine, macrolide antibiotics, various anti-fungal agents, and cytochrome P-450 inhibitors (fibrates and niacin should be used<br />
with appropriate caution).<br />
Taken from NCEP Expert Panel. Executive Summary of the Third Report of the National Cholesterol Education Program(NCEP) Expert<br />
Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults (Adult Treatment Panel III ). Bethesda, Md: National<br />
Heart, Lung, and Blood Institute, National Institutes of <strong>Health</strong>; 2001. NIH publication 01-3670.<br />
88 H EALTH PLANS<br />
www.cfhp.com
NATIONAL CHOLESTEROL EDUCATION PROGRAM (NCEP) GUIDELINES FOR LDL-C 1<br />
ATP III CLASSIFICATION OF LDL, TOTAL, AND HDL CHOLESTEROL (mg/dL)<br />
LDL Cholesterol – Primary Target of Therapy<br />
< 100 Optimal<br />
100 – 129 Near optimal / above optimal<br />
130 – 159 Borderline high<br />
160 – 189 High<br />
≥ 190<br />
Very high<br />
Total Cholesterol<br />
< 200 Desirable<br />
200 – 239 Borderline high<br />
≥ 240<br />
High<br />
HDL Cholesterol<br />
< 40 Low<br />
≥ 60<br />
High<br />
Therapeutic Lifestyle Changes (TLC) if LDL is Above Goal<br />
• TLC Diet:<br />
• Saturated fat < 7% of calories, cholesterol < 200 mg/day<br />
• Consider increased viscous (soluble) fiber (10 – 25 g/day) and plant stanols / sterols<br />
• (2 g/day) as therapeutic options to enhance LDL lowering<br />
• Weight management<br />
• Increased physical activity<br />
1.<br />
Taken from NCEP Expert Panel. Executive Summary of the Third Report of the National Cholesterol Education Program(NCEP) Expert Panel on Detection,<br />
Evaluation, and Treatment of High Blood Cholesterol in Adults (Adult Treatment Panel III ). Bethesda, Md: National Heart, Lung, and Blood Institute, National<br />
Institutes of <strong>Health</strong>; 2001. Final Report 2004 Update<br />
10.5 ATP III Classification of Cholesterol<br />
H EALTH PLANS<br />
www.cfhp.com<br />
89
10.6 <strong>Clinical</strong> Identification of teh Metabolic Syndrome<br />
NATIONAL CHOLESTEROL EDUCATION PROGRAM (NCEP) GUIDELINES FOR LDL-C 1<br />
CLINICAL IDENTIFICATION OF THE METABOLIC SYNDROME**<br />
ANY 3 OF THE FOLLOWING:<br />
RISK FACTOR<br />
DEFINING LEVEL<br />
Abdominal Obesity * Waist circumference †<br />
Men<br />
> 102 cm (> 40 in)<br />
Women<br />
> 88 cm (>35 in)<br />
Trigylcerides<br />
HDL Cholesterol<br />
Men<br />
Women<br />
Blood Pressure<br />
Fasting glucose<br />
≥ 150 mg/dL<br />
< 40 mg/dL<br />
< 50 mg/dL<br />
≥ 130 / ≥ 85 mmHg<br />
≥ 110 mg/dL<br />
* Overweight and obesity are associated with insulin resistance and the metabolic syndrome. However, the presence of abdominal<br />
obesity is more highly correlated with the metabolic risk factors than is an elevated body mass index (BMI). Therefore, the simple<br />
measure of waist circumference is recommended to identify the body weight component of the metabolic syndrome.<br />
† Some male patients can develop multiple metabolic risk factors when the waist circumference is only marginally increased, e.g. 94-<br />
102 cm (37 – 39 in). Such patients may have a strong genetic contribution to insulin resistance. They should benefit from changes in<br />
life habits, similarly to men with categorical increases in waist circumference.<br />
** The ATP III panel did not find adequate evidence to recommend routine measurement of insulin resistance (e.g., plasma insulin),<br />
proinflammatory state (e.g., high-sensitivity C-reactive protein), or prothrombotic state (e.g., fibrinogen or PAI-1) in the diagnosis of<br />
the metabolic syndrome<br />
TREATMENT OF THE METABOLIC SYNDROME<br />
• Treat underlying causes (overweight / obesity and physical inactivity):<br />
• Intensify weight management<br />
• Increase physical activity<br />
• Treat lipid and non-lipid risk factors if they persist despite these lifestyle therapies:<br />
• Treat hypertension<br />
• Use aspirin for CHD patients to reduce prothrombotic state<br />
• Treat elevated triglycerides and/or low HDL<br />
1. Taken from NCEP Expert Panel. Executive Summary of the Third Report of the National Cholesterol Education Program(NCEP)<br />
Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults (Adult Treatment Panel III ).<br />
Bethesda, Md: National Heart, Lung, and Blood Institute, National Institutes of <strong>Health</strong>; 2001. Final Report 2004 Update<br />
90 H EALTH PLANS<br />
www.cfhp.com
NATIONAL CHOLESTEROL EDUCATION PROGRAM (NCEP) GUIDELINES FOR LDL-C 1<br />
ATP III Classification of Serum Triglycerides (mg/dL)<br />
< 150 Normal<br />
150 – 199 Borderline high<br />
200 – 499 High<br />
≥ 500<br />
Very High<br />
Treatment of Elevated Triglycerides (≥ 150 mg/dL)<br />
• Primary aim of therapy is to reach LDL goal<br />
• Intensify weight management<br />
• Increase physical activity<br />
• If triglycerides are ≥ 200 mg/dL after LDL goal is reached, set secondary goal for non-HDL cholesterol (total – HDL) 30 mg/<br />
dL higher than LDL goal<br />
Comparison of LDL Cholesterol and Non-HDL Cholesterol Goals for Three Risk Categories<br />
Risk Category LDL Goal (mg/dL) Non-HDL Goal (mg/dL)<br />
CHD and CHD Risk Equivalent (10-year<br />
risk for CHD >20%)<br />
Multiple (2+) Risk Factors and 10-year<br />
risk ≤ 20%<br />
< 100 < 130<br />
< 130 < 160<br />
0 – 1 Risk Factor < 160 < 190<br />
If triglycerides 200 – 499 mg/dL after LDL goal is reached, consider adding drug if needed to reach non-HDL goal:<br />
• Intensify therapy with LDL-lowering drug, or<br />
• Add nicotinic acid or fibrate to further lower VLDL<br />
If triglycerides ≥ 500 mg/dL, first lower triglycerides to prevent pancreatitis:<br />
• Very low-fat diet (
11.1 Management of High Blood Pressure<br />
Hypertension is a growing problem in the United States. The American Heart Association: Heart Disease and Stroke<br />
Statistics-2010 Update reports:<br />
• Hypertension killed 56,561 people in the United States in 2006;<br />
• Nearly one in three adults has high blood pressure<br />
• Of those people with hypertension ages 20 and older: 77.6% were aware of their condition; 67.9% were under current<br />
treatment; 44.1% had it under control, and 55.9% did not have it controlled.<br />
• The cause of 90–95% of the cases of high blood pressure isn’t known; however, high blood pressure is easily detected and<br />
usually controllable.<br />
• From 1996 to 2006, the death rate from high blood pressure increased 19.5%, and the actual number of deaths rose 48.1%.<br />
• Non-Hispanic blacks are more likely to suffer from high blood pressure than are non-Hispanic whites.<br />
• Within the African-American community, those with the highest rates of hypertension, are more likely to be middle aged<br />
or older, less educated, overweight or obese, physically inactive, and to have diabetes<br />
• In 2006, the death rates per 100,000 population from high blood pressure were 15.6 for white males, 51.1 for black males,<br />
14.3 for white females and 37.7 for black females.<br />
CFHP has adopted the National Institutes of <strong>Health</strong> (NHI) <strong>Guidelines</strong> on High Blood Pressure. Based on these guidelines, the<br />
National Institutes of <strong>Health</strong> and National Heart, Lung, and Blood Institute developed the Seventh Report of the Joint National<br />
Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure (JNC7). A complete copy of the JNC7<br />
Report is available at their web site http://www.nhlbi.nih.gov.<br />
The areas addressed in the report include the classification of blood pressure, diagnostic workup of hypertension, major<br />
cardiovascular risk factors, identifiable causes of hypertension, principles of hypertension treatment, blood pressure<br />
measurement techniques, causes of resistant hypertension, indications for individual drug classes, and principles of lifestyle<br />
modification and recommendations.<br />
The update of the JNC7 is in development.<br />
92 H EALTH PLANS<br />
www.cfhp.com
Identification, Evaluation, and Treatment of High Blood Pressure 1<br />
Classification of Blood Pressure (BP)<br />
Category SBP mmHg DBP mmHg<br />
Normal < 120 And < 80<br />
Prehypertension 120 – 139 Or 80 – 89<br />
Hypertension, Stage 1 140 – 159 Or 90 – 99<br />
Hypertension, Stage 2 ≥ 160 Or ≥ 100<br />
Key: SBP = systolic blood pressure<br />
Diagnostic Workup of Hypertension<br />
• Assess risk factors and comorbidities<br />
• Reveal identifiable causes of hypertension<br />
• Assess presence of target organ damage<br />
• Conduct history and physical examination<br />
DBP = diastolic blood pressure<br />
• Obtain laboratory tests: urinalysis, blood glucose, hematocrit, and lipid panel, serum potassium, creatinine, and calcium.<br />
Optional: urinary albumin / creatinine ratio<br />
• Obtain electrocardiogram<br />
Assess for Major Cardiovascular Disease (CVD) Risk Factors<br />
• Hypertension<br />
• Physical inactivity<br />
• Obesity (body mass index ≥ 30kg/m 2<br />
• Microalbuminuria, estimated glomerular filtration rate 55 for men, >65 for women)<br />
• Diabetes mellitus<br />
• Family history of premature CVD (
Causes of Resistant Hypertension<br />
• Improper BP measurement<br />
• Excess sodium intake<br />
• Inadequate diuretic therapy<br />
• Medication<br />
• Inadequate doses<br />
• Drug actions and interactions (e.g. nonsteroidal anti-inflammatory drugs (NSAIDs), illicit drugs, sympathomimetrics,<br />
oral contraceptives)<br />
• Over-the-counter (OTC) drugs and herbal supplements<br />
• Excess alcohol intake<br />
• Identifiable causes of hypertension<br />
Compelling Indications for Individual Drug Classes<br />
Compelling Indication<br />
• Heart failure<br />
• Post myocardial infarction<br />
• High CVD risk<br />
• Diabetes<br />
• Chronic kidney disease<br />
• Recurrent stroke prevention<br />
Initial Therapy Options<br />
THIAZ, BB, ACEI, ARB, ALDO ANT<br />
BB, ACEI, ALDO ANT<br />
THIAZ, BB, ACEI, CCB<br />
THIAZ, BB, ACEI, ARB, CCB<br />
ACEI, ARB<br />
THIAZ, ACEI<br />
Key: THIAZ = thiazide diuretic, ACEI = angiotensin converting enzyme inhibitor, ARB = angiotensin receptor blocker<br />
BB = beta blocker, CCB = calcium channel blocker, ALDO ANT = aldosterone antagonist<br />
Strategies for Improving Adherence to Therapy<br />
• Clinician empathy increases patient trust, motivation, and adherence to therapy<br />
• Physicians should consider their patients’ cultural believes and individual attitudes in formulating therapy<br />
Principles of Lifestyle Modification<br />
• Encourage healthy lifestyles for all individuals<br />
• Prescribe lifestyle modifications for all patients with prehypertension and hypertension<br />
• Components of lifestyle modifications include weight reduction, DASH eating plan, dietary sodium reduction, aerobic<br />
physical activity, and moderation of alcohol consumption<br />
Lifestyle Modification Recommendations<br />
Weight reduction<br />
DASH eating plan<br />
Dietary sodium reduction<br />
Aerobic physical activity<br />
Modification Recommendation Avg SBP Reduction †<br />
Maintain normal body weight (body<br />
mass index 18.5 – 24.9 kg/m 2 )<br />
Adopt a diet rich in fruits, vegetables,<br />
and low fat dairy products with reduced<br />
content of saturated and total fat<br />
Reduce dietary sodium intake to ≤<br />
100 mmol per day (2.4 g sodium or 6 g<br />
sodium chloride)<br />
Regular aerobic physical activity (e.g.,<br />
brisk walking) at least 30 minutes per<br />
day, most days of week<br />
Moderation of alcohol consumption Men: limit to ≤ 2 drinks* per day<br />
Women and lighter weight persons:<br />
limit to ≤ 1 drink* per day<br />
* 1 drink = ½ oz or 15 mL ethanol (e.g., 12 oz beer, 5 oz wine, 1.5 oz 80-proof whiskey<br />
† Effects are dose and time dependant<br />
5 – 20 mmHg/10 kg<br />
8 – 14 mmHg<br />
2 – 8 mmHg<br />
4 – 9 mmHg<br />
2 -4 mmHg<br />
1<br />
Taken from National Institutes of <strong>Health</strong> (NHI) <strong>Guidelines</strong> on High Blood Pressure. National Institutes of <strong>Health</strong> and National Heart, Lung, and Blood Institute<br />
developed the Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure (JNC7) , NIH<br />
Publication No. 03 - 5231, May 2003<br />
94 H EALTH PLANS<br />
www.cfhp.com
11.3 Treatment of Hypertension<br />
H EALTH PLANS<br />
www.cfhp.com<br />
95
12.1 Depression Mangement & Antidepressant Treatment<br />
<strong>Clinical</strong> Practice Guideline for Depression Management & Antidepressant Treatment<br />
This guideline is designed to assist practitioners by providing an analytical framework for the evaluation and treatment of<br />
patients, and is not intended to replace a practitioner’s judgement.<br />
Depression is a common health problem seen frequently in primary care and psychiatric settings. Depression is more common<br />
in young adults and adolescents, persons with a family history or personal history of depression, those with chronic illnesses,<br />
those who perceive or have experienced a recent loss, those with sleep disorders, chronic pain, or multiple unexplained somatic<br />
complaints. Screening of patients should occur yearly or as office visits and history indicate.<br />
Major Depression Screening Tool<br />
Must have a total of five or more symptoms for at least two weeks. One of the symptoms must be a depressed mood or loss of<br />
interest.<br />
1. Depressed mood.<br />
2. Markedly diminished interest or pleasure in all or almost all activities.<br />
3. Significant (>5% body weight) weight loss or gain, or decrease or increase in appetitie.<br />
4. Insomnia or hypersomnia.<br />
5. Psychomotor agitation or retardation.<br />
6. Fatigue or loss of energy.<br />
7. Feeling of worthlessness or inappropriate guilt.<br />
8. Diminished concentration or indecisiveness.<br />
9. Recurrent thoughts of death or suicide.<br />
10. Presence of psychotic symptoms.<br />
Patients with some depressive symptoms who do not fully meet the criteria for major depression often respond positively to<br />
antidepressant medication.<br />
Patients with indications of depression should be treated as deemed appropriate by the physician and may include a referral to<br />
a mental health provider.<br />
References<br />
Guide to <strong>Clinical</strong> Preventive Services – Second Edition, US Department of <strong>Health</strong> and Human Services, April 1989.<br />
Institute for <strong>Clinical</strong> Systems Integration, January 1997.<br />
Psychiatric Algorithms For Primary Care, Part 1, Primary Psychiatry, February, 2000.<br />
96 H EALTH PLANS<br />
www.cfhp.com
ALGORITHM FOR TREATMENT OF MAJOR DEPRESSION WITH SELECTIVE SEROTONIN REUPTAKE INHIBITORS (SSRIs)<br />
Major Depressive Disorder<br />
Acute Treatment Goal: Decrease symptoms at least 50%<br />
Suggested Initial Dose of SSRI’s, Include<br />
(May need to be adjusted lower in geriatrics, debilitated, etc.)<br />
Fluvoxamine maleate 25mg po bid OR<br />
Citalopram hydrobromide 20 mg po q d OR<br />
Paroxetine hydrochloride 20 mg po q d OR<br />
Fluoxetine hydrochloride 20 mg q am OR<br />
Sertraline hydrochloride 50 mg po q am<br />
Escitalopram oxalate 10 mg q am<br />
**Practitioner should check current formulary guidelines for appropriate SSRI choices.<br />
Response After 6 weeks No Response<br />
Continuation<br />
Goal: Complete remission<br />
Duration for first episode:<br />
6-9 months before taper<br />
and D/C<br />
Maintenance<br />
(Consider use of half tablets in Fluvoxamine<br />
maleate, Paroxetine hydrochloride, Escitalopram<br />
oxalate, Citalopram hydrobromide, Fluoxetine<br />
hydrochloride or QOD in Fluoxetine hydrochloride,<br />
if appropriate)<br />
Partial Response<br />
Increase Dose<br />
Citalopram hydrobromide 20 – 40 mg po q d OR<br />
Fluvoxamine maleate 50 – 100 mg po bid OR<br />
Paroxetine hydrochloride 20 – 40 mg po q d OR<br />
Fluoxetine hydrochloride 20 – 40 mg po q d OR<br />
Sertraline hydrochloride 50 – 100 mg po q am OR<br />
Escitalopram oxalate- 20mg q am<br />
Change<br />
antidepressant or<br />
referral<br />
After 6 weeks<br />
Partial Response<br />
Change antidepressant or referral<br />
H EALTH PLANS<br />
www.cfhp.com<br />
97
12.2 Depression Outpatient Treatment<br />
Is the patient depressed?<br />
Psychiatric consultation<br />
Psychotherapy<br />
Guideline For Outpatient Depression Treatment<br />
Yes<br />
Consider referral to Therapist<br />
Yes<br />
Maintain medication at current dosage<br />
for 9 months (for first episode) or<br />
indefinitely for third episode.<br />
Is the patient suicidal or<br />
displaying psychotic<br />
symptoms?<br />
No<br />
Yes<br />
Yes<br />
No<br />
Does the patient have lingering<br />
unexplained somatic symptoms?<br />
Has thorough medical eval been<br />
completed?<br />
Do medical eval.<br />
Yes<br />
No<br />
Are four other vegetative signs of<br />
depression present for at least 2 weeks?<br />
Yes<br />
• Prescribe an SSRI or other appropriate anti -<br />
depressant and advance to reasonable dosage within<br />
2 weeks.<br />
• Follow-up appointment in 2 to 6 weeks.<br />
• Follow-up every 2 to 6 weeks until responding.<br />
Is the patient improving?<br />
No<br />
• Switch to another antidepressant drug<br />
• Follow-up every 2 to 6 weeks<br />
Is the patient improving?<br />
No<br />
Maintain med at current dosage for 9<br />
months (for first episode) or indefinitely<br />
for third episode.<br />
Yes<br />
Yes<br />
Is the patient well, in remission after 3 months?<br />
No<br />
Psychiatric Consultation<br />
Augment with another drug<br />
Switch to another drug<br />
Refer for Psychotherapy<br />
Electro Convulsive Therapy<br />
98 H EALTH PLANS<br />
www.cfhp.com
CFHP has established guidelines for medical record documentation. Individual medical records for each family member are to be<br />
maintained. The medical records must be handled and maintained in a confidential manner and must be organized in such a manner<br />
that all progress notes, diagnostic tests, reports, letters, discharge summaries and other pertinent medical information are readily<br />
accessible. In addition, each office should have a written policy in place to ensure that medical records are safeguarded against loss,<br />
destruction, or unauthorized use.<br />
CRITERIA<br />
REQUIREMENTS<br />
1. Patient Identification Each page of the medical record must include a unique identifier, which may include patient<br />
identification number, medical record number, first and last name.<br />
2. Personal Data Personal/biographical data including the age, sex, address, employer, home and work telephone<br />
numbers, marital status of the patient, and emergency contacts must be included in the medical<br />
record.<br />
3. Allergies Medication allergies and adverse reactions (including immunization reactions) should be prominently<br />
noted in the record. If the patient has no known allergies or history of adverse reactions, this should<br />
be appropriately noted in the record.<br />
4. Problem List For patients seen three (3) or more times, a separate list of all the patient’s chronic/significant<br />
problems must be maintained. A chronic problem is defined as one that is of long duration, shows<br />
little change or is of slow progression.<br />
5. Medication List For patients seen three (3) or more times, maintenance/ongoing medications should be listed on<br />
a medication sheet and updated as necessary with dosage changes and the date the change was<br />
made. A separate medication sheet is recommended but if a physician chooses to write out all current<br />
medications at each visit, this is acceptable. The medication list should include information/instruction<br />
to the member.<br />
6. Chart Legible Medical records must be legible to someone other than the author. A record that is deemed illegible<br />
by the reviewer should be evaluated by a second person.<br />
7. Author Signature All entries in the medical record must be signed by the author/performing provider.<br />
8. Dated Entries Each and every entry must be accompanied by a date (month, day and year).<br />
9. Advance Directive For medical records of Medicaid adults, 18 years and older, the medical record must document<br />
whether or not the individual has executed an advance directive. An advanced directive is a written<br />
instruction such as a living will or durable power of attorney for health care relating to the provision of<br />
health care when the individual is incapacitated.<br />
10. Past Medical History For patients seen three (3) or more times, a past medical history should be easily identified and<br />
should include serious accidents, operations, and illnesses. For children and adolescents (18 years<br />
and younger), past medical history should relate to prenatal care, birth, operations, and childhood<br />
illnesses.<br />
11. Tobacco, alcohol, &<br />
other substance use<br />
For patients 12 years and older, assessment of tobacco, alcohol, and other substance use should be<br />
documented in the medical record.<br />
12. Chief Complaint Every visit should have a notation identifying the current problem (significant illnesses, medical and<br />
behavioral health conditions and health maintenance concerns).<br />
13. History And Physical<br />
Relevant To Chief<br />
Complaint<br />
14. Diagnosis/<br />
Impression For Chief<br />
Complaint<br />
15. Basic Teaching<br />
Provided<br />
16. Appropriate Plan Of<br />
Treatment<br />
17. Appropriate Use Of<br />
Consultants<br />
18. Appropriate Studies<br />
Ordered<br />
The history and physical records should reflect appropriate subjective and objective information<br />
pertinent to the patient’s presenting complaints.<br />
The diagnosis identified during each visit should be documented and should be consistent with<br />
findings. ICD-9 code(s) may be used but must include the written description of the diagnosis.<br />
The medical record should reflect that the member is provided with basic teaching/instructions<br />
regarding their physical and/or behavioral health condition.<br />
Based on the chief complaint, physical exam findings and diagnosis, the treatment plan should be<br />
clearly documented.<br />
If a patient problem occurs which is outside the physician’s scope of practice, there must be a referral<br />
to an appropriate specialist.<br />
The laboratory and other studies ordered should be consistent with the treatment plan as related<br />
to the documented working diagnosis and should be documented at the time of the visit. Abnormal<br />
findings must have an explicit notation of follow-up plans.<br />
13.1 PCP Medical Record Documentation <strong>Guidelines</strong><br />
H EALTH PLANS<br />
www.cfhp.com<br />
99
CRITERIA<br />
19. Unresolved Problems<br />
From Previous Visits<br />
Addressed<br />
20. MD Review Of<br />
Studies<br />
REQUIREMENTS<br />
Documentation should reflect that the physician provides continuous evaluation of problems noted in<br />
previous visits.<br />
There must be evidence that the physician has reviewed the results of diagnostic studies. Methods<br />
can vary, but often the physician will initial the lab report or mention it in the progress notes.<br />
21. Results Of<br />
Consultations<br />
When the patient is referred to another physician for consultation, there must be a copy of the results<br />
of the consult report and any associated diagnostic work-up in the medical record. Primary physician<br />
review of the consultation must be documented. Often the physician initials the consult report.<br />
22. Date Of Next Visit Encounter forms or notes should have a notation, when indicated, regarding follow-up care, calls, or<br />
visits. Specific time of return should be noted in weeks, months, or as needed.<br />
23. ER And Hospital<br />
Records<br />
24. Evidence That<br />
Patient Was Not Placed<br />
At Risk<br />
25. Evaluation for<br />
abuse / neglect or other<br />
socioenvironmental<br />
factors (Medicaid only)<br />
Pertinent inpatient records must be maintained in the office medical record. These records may<br />
include but are not limited to the following: H&P, surgical procedure reports, authorizations, ER<br />
reports and hospital discharge summaries. For pediatric patients seen since birth, the labor and<br />
delivery records, including the newborn assessment, should be in the medical record.<br />
The record should reflect that the patient has not been placed at inappropriate risk by a diagnostic or<br />
therapeutic problem.<br />
Medical records of Medicaid adults should reflect evidence that the provider evaluates for signs/<br />
symptoms or behaviors associated with abuse / neglect or other significant socioenvironmental<br />
factors.<br />
26. Diagnosis Validation The record should reflect that the billing diagnosis is consistent with that of the chief complaint.<br />
27. Claims Validation The record should reflect the documented encounter is appropriate for the level of E/M services<br />
billed.<br />
100 H EALTH PLANS<br />
www.cfhp.com
A. Documentation ______<br />
B. Continuity of Care _____<br />
C. Preventive <strong>Health</strong> _____<br />
Plan --- Age --- Sex<br />
CFHP<br />
PCP MEDICAL RECORD REVIEW TOOL<br />
Physician: Nurse Reviewer: Date of Review:<br />
Physician Number:<br />
Physician Type:<br />
A. DOCUMENTATION 1 2 3 4 5 6 7 8 9 10<br />
1. Patient identification on each page<br />
2. Personal/Biographical information<br />
3. Allergies prominently noted<br />
4. Problem List<br />
5. Medication List<br />
6. Entries legible<br />
7. All entries contain author identification<br />
8. All entries are dated<br />
9. Advance Directives (Medicaid 18 & older)<br />
B. CONTINUITY OF CARE<br />
10. Past medical history (pts w/3 or more visits)<br />
11. Tobacco, alcohol, & other substance use assessed<br />
(12 & older)<br />
12. Chief complaint noted<br />
13. History & exam pertinent to complaint<br />
14. Working diagnosis consistent with findings<br />
15. Basic teaching provided<br />
16. Appropriate plan of treatment<br />
17. Appropriate use of consults<br />
18. Appropriate studies ordered<br />
19. Unresolved problems addressed<br />
20. Evidence of physician review on studies<br />
21. Results of consultations are reviewed & filed<br />
22. Date of next visit/instructions for follow-up<br />
23. ER and Hospital reports/records<br />
24. Patient is not placed at inappropriate risk<br />
25. Evaluation for abuse/neglect (Medicaid Adults)<br />
VALIDATIONS - √ for compliance (not scored)<br />
26. Diagnosis Validation<br />
27. Claims Validation<br />
Y N Y<br />
+<br />
N<br />
S<br />
C<br />
O<br />
R<br />
E<br />
___Y___<br />
Y+N x100<br />
=<br />
%<br />
compliance<br />
13.2 PCP Medical Record Review Tool<br />
Comments:________________________________________________________________________________________________<br />
__________________________________________________________________________________________________________<br />
__________________________________________________________________________________________________________<br />
__________________________________________________________________________________________________________<br />
__________________________________________________________________________________________________________<br />
__________________________________________________________________________________________________________<br />
__________________________________________________________________________________________________________<br />
__________________________________________________________________________________________________________<br />
__________________________________________________________________________________________________________<br />
P: Quality Management\Medical Record Review\SFY 2012\Audit Tools Revised 12/04, 1/06, 7/07, 03/08, 5/09, 11/09, 8/11<br />
H EALTH PLANS<br />
www.cfhp.com<br />
101
PREVENTIVE CARE<br />
CFHP<br />
PCP MEDICAL RECORD REVIEW TOOL<br />
Physician: Nurse Reviewer: Date of Review:<br />
Physician Number:<br />
Physician Type:<br />
Name:<br />
Member ID:<br />
Y N Y<br />
+<br />
N<br />
S<br />
C<br />
O<br />
R<br />
E<br />
Plan --- Age --- Sex<br />
ADULT SCREENING 1 2 3 4 5 6 7 8 9 10<br />
1. Routine check-up<br />
2. Blood Pressure measurement<br />
3. Obesity Screening/BMI Measurement<br />
Latest Date BMI Documented – Not Scored<br />
*BMI Value – Not Scored<br />
4. Cholesterol profile<br />
(Every 5 yrs for men 35 & older and women 45 & older)<br />
5. STD screening (At risk only)<br />
6. Colorectal Exam to include 1 of the following:<br />
• Stool for occult blood,<br />
• Flexible Sigmoidoscopy, or<br />
• Colonoscopy<br />
7. Fasting Plasma Glucose / Oral GTT (At risk only)<br />
8. Tuberculosis screening (PPD) (At risk only)<br />
9. Depression Screening<br />
10. General counseling<br />
WOMEN<br />
11. Mammogram<br />
(Every 1-2yrs for women 50 & older)<br />
12. Cervical Cancer Screening<br />
13. Osteoporosis Screening (Women 65 & older)<br />
MEN<br />
14. Abdominal Aortic Aneurysm Screening<br />
(Men 65-75 who have hx of smoking)<br />
IMMUNIZATIONS<br />
15. Tetanus, Diphtheria, Pertussis (Td/Tdap)<br />
16. HPV (Women
CFHP<br />
PCP MEDICAL RECORD REVIEW TOOL<br />
Physician: Nurse Reviewer: Date of Review:<br />
Physician Number:<br />
PREVENTIVE CARE<br />
Name:<br />
Member ID:<br />
Physician Type:<br />
Y N Y<br />
+<br />
N<br />
S<br />
C<br />
O<br />
R<br />
E<br />
Plan --- Age --- Sex<br />
PEDIATRIC SCREENING 1 2 3 4 5 6 7 8 9 10<br />
1. Family history<br />
1. Neonatal history<br />
3. Physical, mental health & developmental history<br />
4. Physical examination<br />
5. Height/Weight<br />
6. Obesity Screening/BMI Measurement (2 & older)<br />
Latest Date BMI Documented – Not Scored<br />
*BMI Value – Not Scored<br />
BMI Percentile for Children Under 16 Years<br />
7. Head circumference<br />
8. Blood Pressure measurement<br />
9. Nutrition screening (Medicaid/THSteps only)<br />
10. Developmental/Autism screening<br />
11. Mental health screening<br />
12. Vision screening<br />
13. Hearing screening<br />
14. Tuberculosis screening (PPD)<br />
15. Newborn hereditary/metabolic testing<br />
16. Hemoglobin or Hematocrit<br />
17. Lead screening<br />
18. Hemoglobin type (Medicaid/THSteps only)<br />
19. Cervical Cancer Screening (11 & older AAP only)<br />
19. STD screening (11 & older)<br />
20. HIV screening (Medicaid/THSteps 11 & older)<br />
21. Cholesterol profile<br />
22. Diabetes screening (Medicaid/THSteps only)<br />
23. Dental referral<br />
24. Anticipatory guidance<br />
IMMUNIZATIONS<br />
25. Hepatitis B<br />
26. Rotavirus<br />
27. DTP/DTaP/Tdap<br />
28. Hib<br />
29. Pneumococcal (PCV)<br />
30. IPV<br />
31. Influenza<br />
32. MMR<br />
33. Varicella<br />
34. Hepatitis A<br />
35. Meningococcal<br />
36. HPV<br />
X = Patient qualifies for screening but timeframe has not yet expired<br />
N/A<br />
N/A<br />
N/A<br />
Comments:__________________________________________________________________________________________________<br />
____________________________________________________________________________________________________________<br />
____________________________________________________________________________________________________________<br />
P: Quality Management\Medical Record Review\SFY 2012\Audit Tools Revised 12/04, 1/06, 7/07, 03/08, 5/09, 11/09, 8/11<br />
H EALTH PLANS<br />
www.cfhp.com<br />
103
CFHP<br />
PCP MEDICAL RECORD REVIEW TOOL<br />
Physician: Nurse Reviewer: Date of Review:<br />
Physician Number:<br />
Physician Type:<br />
Medical Record Review Comments:<br />
____________________________________________________________________________________________________________<br />
____________________________________________________________________________________________________________<br />
____________________________________________________________________________________________________________<br />
____________________________________________________________________________________________________________<br />
____________________________________________________________________________________________________________<br />
____________________________________________________________________________________________________________<br />
____________________________________________________________________________________________________________<br />
____________________________________________________________________________________________________________<br />
____________________________________________________________________________________________________________<br />
____________________________________________________________________________________________________________<br />
____________________________________________________________________________________________________________<br />
____________________________________________________________________________________________________________<br />
____________________________________________________________________________________________________________<br />
____________________________________________________________________________________________________________<br />
____________________________________________________________________________________________________________<br />
____________________________________________________________________________________________________________<br />
____________________________________________________________________________________________________________<br />
____________________________________________________________________________________________________________<br />
____________________________________________________________________________________________________________<br />
____________________________________________________________________________________________________________<br />
____________________________________________________________________________________________________________<br />
____________________________________________________________________________________________________________<br />
____________________________________________________________________________________________________________<br />
____________________________________________________________________________________________________________<br />
____________________________________________________________________________________________________________<br />
____________________________________________________________________________________________________________<br />
____________________________________________________________________________________________________________<br />
____________________________________________________________________________________________________________<br />
____________________________________________________________________________________________________________<br />
____________________________________________________________________________________________________________<br />
____________________________________________________________________________________________________________<br />
____________________________________________________________________________________________________________<br />
____________________________________________________________________________________________________________<br />
____________________________________________________________________________________________________________<br />
Reviewed with ______________________________________________________________________________________________<br />
Comments _________________________________________________________________________________________________<br />
____________________________________________________________________________________________________________<br />
____________________________________________________________________________________________________________<br />
____________________________________________________________________________________________________________<br />
____________________________________________________________________________________________________________<br />
___________________________________________________________________________________________________________<br />
____________________________________________________________________________________________________________<br />
____________________________________________________________________________________________________________<br />
____________________________________________________________________________________________________________<br />
____________________________________________________________________________________________________________<br />
____________________________________________________________________________________________________________<br />
____________________________________________________________________________________________________________<br />
____________________________________________________________________________________________________________<br />
____________________________________________________________________________________________________________<br />
____________________________________________________________________________________________________________<br />
____________________________________________________________________________________________________________<br />
____________________________________________________________________________________________________________<br />
____________________________________________________________________________________________________________<br />
____________________________________________________________________________________________________________<br />
____________________________________________________________________________________________________________<br />
P: Quality Management\Medical Record Review\SFY 2012\Audit Tools Revised 12/04, 1/06, 7/07, 03/08, 5/09, 11/09, 8/11<br />
104 H EALTH PLANS<br />
www.cfhp.com
13.3 Specialist Medical Record Documentation <strong>Guidelines</strong><br />
H EALTH PLANS<br />
www.cfhp.com<br />
105
106 H EALTH PLANS<br />
www.cfhp.com
13.4 Specialist Medical Record Review Tool<br />
H EALTH PLANS<br />
www.cfhp.com<br />
107
14.1 Management of Osteoporosis<br />
Traditionally, osteoporosis is a disease associated with menopause. It is thought to affect only women but men are also at risk<br />
for osteoporosis.<br />
The National Institutes of <strong>Health</strong> Osteoporosis and Related Bone Disease National Resource Center reports that:<br />
• Osteoporosis is a major public health threat for 44 million Americans, 68% of whom are women;<br />
• In the U.S. today, 10 million individuals already have osteoporosis and 34 million more have low bone mass, placing them<br />
at increased risk for this disease;<br />
• One out of every two women and one in four men over 50 will have an osteoporosis-related fracture in their lifetime;<br />
• More than 2 million American men suffer from osteoporosis, and millions more are at risk. Each year, 80,000 men suffer a<br />
hip fracture and one-third of these men die within a year;<br />
• Osteoporosis can strike at any age;<br />
• Estimated national direct expenditures (hospitals and nursing homes) for osteoporosis and related fractures are $14<br />
billion each year.<br />
CFHP has adopted the Recommendations and the Guide to Prevention and Treatment from the National Osteoporosis<br />
Foundation. Osteoporosis is a preventable disease and with adherence to these recommendations, patients can reduce their<br />
risk for this disease and for those who already are affected by it, their outcomes can be improved.<br />
108 H EALTH PLANS<br />
www.cfhp.com
Risk Factors for Osteoporosis Fractures<br />
www.nof.org<br />
Non-modifiable:<br />
• Personal history of fracture as an adult<br />
• History of fracture in first-degree relative<br />
• Caucasian/Asian race<br />
• Advanced age<br />
• Female sex<br />
• Dementia<br />
• Poor health/frailty<br />
Potentially Modifiable:<br />
• Current cigarette smoking<br />
• Low body weight (1 year)<br />
• Low calcium intake (lifelong)<br />
• Alcoholism<br />
• Impaired eyesight despite correction<br />
• Recurrent falls<br />
• Inadequate physical activity<br />
• Poor health/frailty<br />
• Use of corticosteroid therapy for >3 months<br />
The four items in boldface type are key factors in determining risk of hip fracture independent of BMD.<br />
Who should be tested?<br />
Your healthcare provider may recommend a bone mineral density (BMD) test if you are:<br />
• A postmenopausal woman under age 65 with one or more risk factors for osteoporosis<br />
• A man age 50-70 with one or more risk factors for osteoporosis<br />
• A woman age 65 or older, even without any risk factors<br />
• A man age 70 or older, even without any risk factors<br />
• A woman or man after age 50 who has broken a bone<br />
• A woman going through menopause with certain risk factors<br />
• A postmenopausal woman who has stopped taking estrogen therapy (ET) or hormone therapy (HT)<br />
Some other reasons your healthcare provider may recommend a BMD test:<br />
• Long-term use of certain medications including steroids (for example, prednisone and cortisone), some anti-seizure<br />
medications, Depo-Provera® and aromatase inhibitors (for example, anastrozole, brand name Arimidex®)<br />
• A man receiving certain treatments for prostate cancer<br />
• A woman receiving certain treatments for breast cancer<br />
• Overactive thyroid gland (hyperthyroidism) or taking high doses of thyroid hormone medication<br />
• Overactive parathyroid gland (hyperparathyroidism)<br />
• X-ray of the spine showing a fracture or bone loss<br />
• Back pain with a possible fracture<br />
• Significant loss of height<br />
• Loss of sex hormones at an early age, including early menopause<br />
• Having a disease or condition that can cause bone loss (such as rheumatoid arthritis or anorexia nervosa)<br />
National Osteoporosis Foundation. Physician’s guide to prevention and treatment of osteoporosis. Washington (DC): National Osteoporosis Foundation; 2008,<br />
p.13<br />
Who should be treated?<br />
Postmenopausal women and men age 50 and older presenting with the following should be considered for treatment:<br />
• A hip or vertebral (clinical or morphometric) fracture<br />
• T-score ≤ -2.5 at the femoral neck or spine after appropriate evaluation to exclude secondary causes<br />
• Low bone mass (T-score between -1.0 and -2.5 at the femoral neck or spine) and a 10-year probability of a hip fracture ≥ 3%<br />
or a 10-year probability of a major osteoporosis-related fracture ≥ 20% based on the US-adapted WHO algorithm<br />
14.2 Recommendations from National Osteoporosis Foundation<br />
H EALTH PLANS<br />
www.cfhp.com<br />
109
Examples<br />
1.0<br />
0.5<br />
0<br />
-0.5<br />
-1.0<br />
-1.5<br />
-2.0<br />
-2.5<br />
-3.0<br />
-3.5<br />
-4.0<br />
World <strong>Health</strong> Organization Definitions of Osteoporosis Based on Bone Density<br />
T-Scores<br />
Range<br />
BMD Category<br />
-1 and above Normal BMD<br />
Between -1 and -2.5<br />
Low BMD (Osteopenia)<br />
-2.5 and below Osteoporosis<br />
National Osteoporosis Foundation. Physician’s guide to prevention and treatment of osteoporosis. Washington (DC): National Osteoporosis Foundation; 2008, p.19<br />
110 H EALTH PLANS<br />
www.cfhp.com
It is well documented that obesity is a risk factor for many chronic conditions, such as diabetes and cardiovascular disease.<br />
Depression and self-esteem issues can also result from obesity.<br />
Results from the 2005-2006 National <strong>Health</strong> and Nutrition Examination Survey (NHANES), using measured heights and weights,<br />
indicate that an estimated 32.7 percent of U.S. adults 20 years and older are overweight, 34.3 percent are obese and 5.9 percent<br />
are extremely obese. One of the national health objectives for 2010 is to reduce the prevalence of obesity among adults to less<br />
than 15 percent.<br />
CFHP has adopted the National Institutes of <strong>Health</strong> (NHI) <strong>Guidelines</strong> on Overweight and Obesity in Adults. Based on these<br />
guidelines, the National Institutes of <strong>Health</strong> and National Heart, Lung, and Blood Institute developed the <strong>Clinical</strong> <strong>Guidelines</strong> on<br />
the Identification, Evaluation, and Treatment of Overweight and Obesity in Adults.<br />
A complete copy of the report is available at their web site http://www.nhlbi.nih.gov/guidelines/obesity/.<br />
The areas addressed in the report include the classification of overweight and obesity by BMI; risk status; BMI categorized by<br />
inches; classification by BMI, waist circumference and associated disease risk; advantages of weight loss; goals for weight loss;<br />
how to achieve weight loss; and goals for weight loss maintenance.<br />
The update of the <strong>Guidelines</strong> on Overweight and Obesity in Adults is in development.<br />
15.1 Management of Overweight and Obesity in Adults<br />
H EALTH PLANS<br />
www.cfhp.com<br />
111
15.2 Classification of Overweight and Obesity by BMI<br />
<strong>Clinical</strong> <strong>Guidelines</strong> on the Identification, Evaluation, and Treatment of Overweight and Obesity in Adults 1<br />
CLASSIFICATION OF OVERWEIGHT AND OBESITY BY BMI<br />
OBESITY CLASS BMI (kg/m 2 )<br />
Underweight < 18.5<br />
Normal 18.5 – 24.9<br />
Overweight 25.0 – 29.9<br />
Obesity I 30.0 – 34.9<br />
II 35.0 – 39.9<br />
Extreme Obesity III ≥ 40<br />
HIGH RISK<br />
Men<br />
Women<br />
> 102 cm (> 40 in)<br />
> 88 cm (35 in)<br />
SELECTED BMI UNITS CATEGORIZED BY INCHES (cm) AND POUNDS (kg)<br />
Height in inches (cm) BMI 25 kg/m 2 BMI 27 kg/m 2<br />
Body Weight in pounds (kg)<br />
BMI 30 kg/m 2<br />
58 (147.32) 119 (53.98) 129 (58.51) 143 (64.86)<br />
59 (149.86) 124 (56.25) 133 (60.33) 148 (67.13)<br />
60 (152.40) 128 (58.06) 138 (62.60) 153 (69.40)<br />
61 (154.94) 132 (59.87) 143 (64.86) 158 (71.67)<br />
62 (157.48) 136 (61.69) 147 (66.68) 164 (74.39)<br />
63 (160.02) 141 (63.96) 152 (68.95) 169 (76.66)<br />
64 (162.56) 145 (65.77) 157 (71.22) 174 (78.93)<br />
65 (165.10) 150 (68.04) 162 (73.48) 180 (81.65)<br />
66 (167.64) 155 (70.31) 167 (75.75) 186 (84.37)<br />
67 (170.18) 159 (72.12) 172 (78.02) 191 (86.64)<br />
68 (172.72) 164 (74.39) 177 (80.29) 197 (89.36)<br />
69 (175.26) 169 (76.66) 182 (82.56) 203 (92.08)<br />
70 (177.80) 174 (78.93) 188 (85.28) 207 (93.90)<br />
71 (180.34) 179 (81.19) 193 (87.54) 215 (97.52)<br />
72 (182.88) 184 (83.46) 199 (90.27) 221 (100.25)<br />
73 (185.42) 189 (85.73) 204 (92.53) 227 (102.97)<br />
74 (187.96) 194 (88.00) 210 (95.26) 233 (105.69)<br />
75 (190.50) 200 (90.72) 216 (97.98) 240 (108.86)<br />
76 (193.04) 205 (92.99) 221 (100.25) 246 (111.59)<br />
Metric conversion formula = weight (kg) / height (m) 2<br />
Example of BMI calculation: A person who weighs 78.93<br />
kilograms and is 177 centimeters tall has a BMI of 25:<br />
Weight (78.93 kg) / height (1.77 m) 2 = 25<br />
Non-metric conversion formula =<br />
[weight (pounds) / height (inches) 2 ] x 703<br />
Example of BMI calculation:<br />
A person who weighs 164 pounds and is 68 inches (or 5’8”) tall<br />
has a BMI of 25:<br />
[weight (164 pounds) / height (68 inches) 2 ] x 703= 25<br />
112 H EALTH PLANS<br />
www.cfhp.com
CLASSIFICATION OF OVERWEIGHT AND OBESITY BY BMI, WAIST CIRCUMFERENCE AND ASSOCIATED DISEASE RISKS<br />
BMI (kg/m 2 )<br />
Obesity Class<br />
Disease Risk* Relative to Normal Weight and Waist<br />
Circumference<br />
Men ≤ 102 cm (≤ 40 in)<br />
Women ≤ 88 cm (≤35 in)<br />
> 102 cm (> 40 in)<br />
> 88 cm (35 in)<br />
Underweight < 18.5 ---- ----<br />
Normal † 18.5 – 24.9 ---- ----<br />
Overweight 25.0 – 29.9 Increased High<br />
Obesity 30.0 – 34.9 I High Very High<br />
35.0 – 39.9 II Very High Very High<br />
Extreme Obesity ≥ 40 III Extremely High Extremely High<br />
* Disease risk for type 2 diabetes, hypertension, and CVD<br />
† Increased waist circumference can also be a marker for increased risk even in persons of normal weight.<br />
1<br />
Taken from <strong>Clinical</strong> <strong>Guidelines</strong> on the Identification, Evaluation, and Treatment of Overweight and Obesity in Adults. National<br />
Institutes of <strong>Health</strong> (NHI) <strong>Guidelines</strong> on Overweight and Obesity in Adults.<br />
H EALTH PLANS<br />
www.cfhp.com<br />
113
15.3 Treatment of Overweight and Obesity in Adults<br />
114 H EALTH PLANS<br />
www.cfhp.com
16.1.1 Preventive Pediatric <strong>Health</strong> Care <strong>Guidelines</strong><br />
H EALTH PLANS<br />
www.cfhp.com<br />
115
THSteps Medical Checkups Periodicity Schedule for Infants. Children, and Adolescents (Birth Through 20 Years of Age)<br />
The columns across the top of the schedule indicate the age a client is periodically eligible for a medical checkup. The first column on the left of the chart identifies each procedure that must be performed at each appropriate age.<br />
(See Key at bottom of page and Footnotes on the following page.)<br />
History<br />
Weeks Months Years<br />
Age 1 Inpatient 3-5 Days 2 2 4 6 9 12 15 18 24 30 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20<br />
Family • • • <br />
Neonatal • • • <br />
Physical, Mental <strong>Health</strong>, and<br />
Developmental<br />
• • • • • • • • • • • • • • • • • • • • • • • • • • • • • •<br />
Unclothed Physical<br />
Examination 2 • • • • • • • • • • • • • • • • • • • • • • • • • • • • • •<br />
Measurements<br />
Length/Height, Weight • • • • • • • • • • • • • • • • • • • • • • • • • • • • • •<br />
Body Mass Index (BMI) • • • • • • • • • • • • • • • • • • • •<br />
Fronto-Occipital<br />
Circumference<br />
• • • • • • • • • • •<br />
Blood Pressure • • • • • • • • • • • • • • • • • •<br />
Nutrition Screening • • • • • • • • • • • • • • • • • • • • • • • • • • • • • •<br />
Developmental/Autism<br />
Screening 3 • • • • • S • S S S S • •<br />
Mental <strong>Health</strong> Screening • • • • • • • • • • • • • • • • • • • • • • • • • • • • •<br />
Sensory Screening 4<br />
Vision Screening 4a • • • • • • • • • • • • S S S S • S • S • S • • S • • S • •<br />
Hearing Screening 4b • • • • • • • • • • • • • S S S • S • S • • • • • • • • • •<br />
Tuberculosis Screening 5 • • • • • • • • • • • • • • • • • • • • • • •<br />
Laboratory Tests 6<br />
Newborn Hereditary/<br />
Metabolic Testing 7 • • <br />
Hgb or Hct 8 • • • • • • <br />
Lead Screening 9 + + • • <br />
Hemoglobin Type 10 • • <br />
STD Screening 11 + + + + + + + + + +<br />
HIV Screening 12 + + + + + + + + + +<br />
Cervical Cancer Screening 13 + + + + + + + + + +<br />
Hyperlipidemia 14 + + + + + + + + + + + + + + + + + + + +<br />
Type II Diabetes 15 + + + + + + + + + + + + + + + + + + + +<br />
Immunizations 16 • • • • • • • • • • <br />
Dental Referral 17 • • • • • • • • • • • • • • • • • • • • • • •<br />
Anticipatory Guidance 18 • • • • • • • • • • • • • • • • • • • • • • • • • • • • • •<br />
Key<br />
•<br />
<br />
Required, unless medically contraindicated or because of parent’s reasons of conscience including a religious belief or the dated results obtained within the previous month<br />
documented on the health record.<br />
Required as above, unless already provided on a previous checkup at the required age, or the dated results obtained within the previous month, and documented on the health<br />
record with the date of service.<br />
+ If answers on risk assessment questionnaires or other screening show a risk factor, further screening is required. Refer to Footnotes for more information about marked items.<br />
S Standardized screening tool must be used at these ages.<br />
16.1.2 Texas <strong>Health</strong> Steps Periodocity Schedule<br />
116 H EALTH PLANS<br />
www.cfhp.com
H EALTH PLANS<br />
www.cfhp.com<br />
117
118 H EALTH PLANS<br />
www.cfhp.com
TEXAS MEDICAID PROVIDER PROCEDURES MANUAL: VOL. 2<br />
CH.46<br />
Mental <strong>Health</strong> Interview Tool/Referral Form (Ages 0–2 Years)<br />
Mental <strong>Health</strong> Interview Tool/Referral Form (Ages 0–2 Years)<br />
Mental <strong>Health</strong> Interview Tool/Referral Form<br />
Ages 0 to 2<br />
Child’s Name: ____________________________<br />
Birth Date: _______________________________<br />
Date: ____________________________________<br />
For this age group you will obtain information from the parent/caregiver and from your own observations of the child.<br />
Circle items of concern. * The presence of any of these symptoms or behaviors may signal that the child is in crisis, and<br />
efforts should be made to secure prompt evaluation.<br />
Feelings: Does your child display feelings that<br />
concern you or seem out of the ordinary?<br />
Behavior: Does your child display behavior that<br />
concerns you or seems out of the ordinary for his/<br />
her age?<br />
Social Interaction: Do you have concerns about<br />
how your child gets along with you? Other family<br />
members or adults? Siblings?<br />
Thinking: Do you think your child’s development is<br />
normal for age?<br />
Physical Problems: Do you have any concerns<br />
about your child’s physical health? If physical<br />
problems exist, have they been medically<br />
evaluated?<br />
Other:<br />
Comments:<br />
Infants<br />
1 to 2 Years<br />
❏ Anxious ❏ Irritable ❏ Sullen<br />
❏ Cries excessively ❏ Angry ❏ Anxious<br />
❏ Cries too little ❏ Sad ❏ Cries excessively<br />
❏ Fearful ❏ Cries too little<br />
Infants<br />
1 to 2 Years<br />
❏ Overactive ❏ Overactive<br />
❏ Listlessness ❏ Listlessness<br />
❏ Harms others<br />
❏ Frequent temper tantrums<br />
Infants<br />
1 to 2 Years<br />
❏ No eye contact or smile ❏ * No eye contact or smile<br />
❏ Stiffens and arches ❏ Clings excessively<br />
❏ Not responsive ❏ Not responsive<br />
❏ Language delay<br />
Infants (> 8 months)<br />
❏ No communication skills<br />
(pointing to request an<br />
object) or efforts to<br />
make words<br />
Infants to 2 Years<br />
❏ Low weight or weight loss<br />
❏ Frequent vomiting<br />
❏ Eating problem (poor appetite, eats nonfoods)<br />
❏ Sleeping problem (frequent night waking)<br />
❏ Lethargic<br />
1 to 2 Year<br />
❏ Mistrustful<br />
❏ Problems concentrating or paying attention<br />
Are there any situations which are causing your family particular stress at this time?<br />
Has this child or his/her parents been subject to neglect, physical, sexual, or emotional abuse?<br />
If yes, what form, when, treatment initiated, etc.?<br />
Did the mother of this child use drugs or drink alcohol during the pregnancy?<br />
Signature/Title: _______________________________________________________________________________________<br />
16.1.3 Texas <strong>Health</strong> Steps Mental <strong>Health</strong> Interview Tool<br />
CH-314<br />
CPT ONLY - COPYRIGHT 2010 AMERICAN MEDICAL ASSOCIATION. ALL RIGHTS RESERVED.<br />
H EALTH PLANS<br />
www.cfhp.com<br />
119
CHILDREN’S SERVICES HANDBOOK<br />
CH.47<br />
Mental <strong>Health</strong> Interview Tool/Referral Form (Ages 3–9 Years)<br />
Mental <strong>Health</strong> Interview Tool/Referral Form (Ages 3–9 Years)<br />
Mental <strong>Health</strong> Interview Tool/Referral Form<br />
Ages 3 to 9<br />
Child’s Name: ____________________________<br />
Birth Date: _______________________________<br />
Date: _____________________________________<br />
For this age group you will obtain information from the parent/caregiver and from your own observations of the child’s behavior. If possible,<br />
interview the parent alone when asking questions about sexual or physical abuse. Circle items of concern. * The presence of any of these<br />
symptoms or behaviors may signal that the child is in crisis, and efforts should be made to secure prompt evaluation.<br />
Feelings:<br />
Behavior:<br />
Does your child display feelings that concern you or seem out of<br />
the ordinary for age?<br />
Does your child frequently display behavior that seems out of the<br />
ordinary for age?<br />
❏ Restless ❏ Problems in school<br />
❏ Sad or cries easily ❏ * Harms other children or animals<br />
❏ Excessively guilty ❏ Lacks interest in things s/he used to enjoy<br />
❏ Lack of remorse ❏ Engages in sexual play with others, toys, animals<br />
❏ Irritable, angers or temper tantrums easily ❏ * Destroys possessions or other property<br />
❏ Sullen ❏ Steals<br />
❏ Fearful or anxious ❏ Refuses to talk<br />
❏ * Sets fires<br />
❏ Overactive<br />
❏ * Self-destructive<br />
❏ * Has been in trouble with the police (older child)<br />
Social Interaction:<br />
Thinking:<br />
Do you have concerns about how child gets along with you, other Have you noticed any of the following to be a problem for your child?<br />
family members, playmates, other adults?<br />
❏ Withdraws including no eye contact ❏ * Frequently confused<br />
❏ Clings excessively ❏ Daydreams excessively<br />
❏ Difficulty making and keeping friends ❏ Distracted, doesn’t pay attention<br />
❏ Defiant, a discipline problem ❏ * Bizarre thoughts<br />
❏ Severe or frequent tantrums ❏ Mistrustful<br />
❏ Aggressive ❏ * Sees or hears things that are not there (excluding<br />
imaginary friends in younger children)<br />
❏ Argues excessively ❏ Blames others for his/her misdeeds or thoughts<br />
❏ Refuses to go to school ❏ * Talks about death<br />
❏ Prefers to be alone ❏ * Frequent memory loss<br />
❏ Schoolwork is slipping (grades going down)<br />
Physical Problems:<br />
Do you have any concerns about the following physical signs?<br />
Has this been evaluated?<br />
❏ Daytime wetting<br />
❏ Soils pants<br />
❏ Refusal to eat<br />
❏ Headaches<br />
❏ Excessive weight loss or gain<br />
❏ Sleep problems, nightmares, sleep-walking, early<br />
waking<br />
❏ Vomits frequently<br />
❏ Frequent stomachaches<br />
❏ Lacks energy<br />
Comments:<br />
Other:<br />
Is this child accident-prone?<br />
Are there any situations that are causing your family particular<br />
stress?<br />
Has this child or his/her parents been subject to neglect, physical,<br />
sexual or emotional abuse? If yes, what type, when, treatment, etc.<br />
* Is this child at risk for out-of-home placement because of behavior<br />
problems?<br />
Signature/Title: _____________________________________________________________________________<br />
120 H EALTH PLANS<br />
www.cfhp.com<br />
CH-315<br />
CPT ONLY - COPYRIGHT 2010 AMERICAN MEDICAL ASSOCIATION. ALL RIGHTS RESERVED.
TEXAS MEDICAID PROVIDER PROCEDURES MANUAL: VOL. 2<br />
CH.48<br />
Mental <strong>Health</strong> Interview Tool/Referral Form (Ages 10–12 Years)<br />
Mental <strong>Health</strong> Interview Tool/Referral Form (Ages 10–12 Years)<br />
Mental <strong>Health</strong> Interview Tool/Referral Form<br />
Child’s Name: ____________________________<br />
Ages 10 to 12<br />
Birth Date: _______________________________<br />
Date: _____________________________________<br />
Both child and parent will be able to provide information, and it is important to incorporate the child into the interview process. In each section,<br />
a sample question is directed toward the parent. To the extent possible, elicit the child’s perception of the parent’s response with a<br />
question such as “Do you agree with what your Mom is saying?” It may be useful to allow time for discussion with the caregiver alone. The<br />
child should be interviewed alone when asking questions about sexual or physical abuse and about substance abuse. Circle items of concern.<br />
* The presence of any of these symptoms or behaviors may signal that the child is in crisis, and efforts should be made to secure prompt<br />
evaluation..<br />
Feelings:<br />
Behavior:<br />
Does your child (do you) have feelings that concern you or seem<br />
out of the ordinary for age?<br />
Does your child (do you) behave in ways that seems out of the<br />
ordinary for age?<br />
❏ Restless ❏ Problems in school<br />
❏ Sad or cries easily ❏ * Threatens or harms other children or animals<br />
❏ Guilty ❏ Lacks interest in things s/he used to enjoy<br />
❏ Irritable or angers easily ❏ Engages in sexual play with others, toys, animals<br />
❏ Sullen ❏ * Destroys possessions or other property<br />
❏ Fearful or anxious ❏ Steals<br />
❏ Bored ❏ Refuses to talk<br />
❏ * Sets fires<br />
❏ Overactive<br />
❏ * Has been in trouble with the police<br />
❏ * Self-destructive<br />
Social Interaction:<br />
Thinking:<br />
Do you have concerns about how your child (you) gets along with<br />
family members, other adults or children?<br />
Have you noticed any of the following to be a problem for your child<br />
(you)?<br />
❏ Prefers to be alone ❏ * Frequently confused<br />
❏ Difficulty making and keeping friends ❏ Daydreams excessively<br />
❏ Defiant, a discipline problem ❏ Distracted, doesn’t pay attention<br />
❏ Aggressive ❏ Mistrustful<br />
❏ Argues excessively ❏ * Sees or hears things that are not there<br />
❏ Refuses to go to school ❏ Blames others for his/her misdeeds or thoughts<br />
❏ * Talks about death or suicide<br />
❏ * Frequent memory loss<br />
❏ * Bizarre thoughts<br />
❏ Schoolwork is slipping (grades going down)<br />
Physical Problems:<br />
Other:<br />
Do you have any concerns about the following physical signs? Is this child (are you) accident-prone?<br />
Has this been evaluated?<br />
Are there any situations that are causing your family particular<br />
stress?<br />
❏ Lacks energy<br />
Has this child or his/her parents been subject to neglect, physical,<br />
❏ Uses laxatives<br />
sexual or emotional abuse? If yes, what type, when, treatment, etc.<br />
❏ Vomits frequently ❏ * Is this child at risk for out-of-home placement<br />
❏ Food refusal, secretive eating<br />
because of behavior problems?<br />
❏ Frequent stomachaches ❏ Has the child (have you) been treated for mental health<br />
❏ Headaches<br />
problems or substance abuse?<br />
❏ Excessive weight loss or gain Substance Abuse Questions:<br />
❏ Sleep problems, nightmares, sleep-walking, early<br />
waking, frequent night waking<br />
(May want to use screens such as the TACE, CAGE, MAST to obtain<br />
information concerning substance abuse.)<br />
❏ Has been identified as a problem<br />
Comments:<br />
Signature/Title: _____________________________________________________________________________<br />
CH-316<br />
CPT ONLY - COPYRIGHT 2010 AMERICAN MEDICAL ASSOCIATION. ALL RIGHTS RESERVED.<br />
H EALTH PLANS<br />
www.cfhp.com<br />
121
CHILDREN’S SERVICES HANDBOOK<br />
CH.49<br />
Mental <strong>Health</strong> Interview Tool/Referral Form (Ages 13–20 Years)<br />
Mental <strong>Health</strong> Interview Tool/Referral Form (Ages 13–20 Years)<br />
Mental <strong>Health</strong> Interview Tool/Referral Form<br />
Child’s Name: ____________________________<br />
Ages 13 to 20<br />
Birth Date: _______________________________<br />
Date: _____________________________________<br />
You may begin with a joint interview or begin with separate interviews with the parent/caregiver and adolescent. It is<br />
preferable to interview the adolescent first. Circle items of concern. * The presence of any of these symptoms or behaviors<br />
may signal that the child is in crisis, and efforts should be made to secure prompt evaluation.<br />
Feelings:<br />
Behavior:<br />
Do you (does your teen) have feelings that concern you or seem<br />
out of the ordinary for (their) age?<br />
Do you (does your child) behave in ways that seems out of the<br />
ordinary for your (their) age?<br />
❏ Restless ❏ Problems at school or work<br />
❏ Sad or cries easily ❏ * Threatens or harms other children or animals<br />
❏ Guilty ❏ Lacks interest in things s/he used to enjoy<br />
❏ Irritable or angers easily ❏ Engages in sexual play with others, toys, animals<br />
❏ Sullen ❏ * Destroys possessions or other property<br />
❏ Fearful or anxious ❏ Steals<br />
❏ Bored ❏ Refuses to talk<br />
❏ * Sets fires<br />
❏ Overactive<br />
❏ * Has been in trouble with the police<br />
❏ * Self-destructive<br />
Social Interaction:<br />
Thinking:<br />
Do you have concerns about how (you) your child gets along with<br />
family members, other adults, or peers?<br />
Have you noticed any of the following to be a problem for you (your<br />
child)?<br />
❏ Prefers to be alone ❏ * Frequently confused<br />
❏ Difficulty making and keeping friends ❏ Daydreams excessively<br />
❏ Defiant, a discipline problem ❏ Distracted, doesn’t pay attention<br />
❏ Aggressive ❏ Mistrustful<br />
❏ Argues excessively ❏ * Sees or hears things that are not there<br />
❏ Refuses to go to school ❏ Blames others for his/her misdeeds or thoughts<br />
❏ * Talks about death or suicide<br />
❏ * Frequent memory loss<br />
❏ * Bizarre thoughts<br />
❏ Schoolwork is slipping (grades going down)<br />
Physical Problems:<br />
Other:<br />
Do you have any concerns about the following physical signs? Are you (is this child) accident-prone?<br />
Has this been evaluated?<br />
Are there any situations that are causing your family particular<br />
stress?<br />
❏ Lacks energy<br />
Have you (has this child) or your (his/her) parents been subject to<br />
❏ Uses laxatives<br />
neglect, physical, sexual or emotional abuse? If yes, what type, when,<br />
treatment, etc.<br />
❏ Vomits frequently ❏ * Are you (is this child) at risk for out-of-home<br />
❏ Food refusal, secretive eating<br />
placement because of behavior problems?<br />
❏ Frequent stomachaches ❏ Have you (has this child) been treated for mental health<br />
❏ Headaches<br />
problems or substance abuse?<br />
❏ Excessive weight loss or gain Substance Abuse Questions:<br />
❏ Sleep problems, nightmares, sleep-walking, early<br />
waking, frequent night waking<br />
(May want to use screens such as the TACE, CAGE, MAST to obtain<br />
information concerning substance abuse.)<br />
❏ Has been identified as a problem<br />
Comments:<br />
Signature/Title: ____________________________________________________________________________<br />
122 H EALTH PLANS<br />
CH-317<br />
www.cfhp.com<br />
CPT ONLY - COPYRIGHT 2010 AMERICAN MEDICAL ASSOCIATION. ALL RIGHTS RESERVED.
TEXAS MEDICAID PROVIDER PROCEDURES MANUAL: VOL. 2<br />
CH.48<br />
Mental <strong>Health</strong> Interview Tool/Referral Form (Ages 10–12 Years)<br />
Mental <strong>Health</strong> Interview Tool/Referral Form (Ages 10–12 Years)<br />
Mental <strong>Health</strong> Interview Tool/Referral Form<br />
Child’s Name: ____________________________<br />
Ages 10 to 12<br />
Birth Date: _______________________________<br />
Date: _____________________________________<br />
Both child and parent will be able to provide information, and it is important to incorporate the child into the interview process. In each section,<br />
a sample question is directed toward the parent. To the extent possible, elicit the child’s perception of the parent’s response with a<br />
question such as “Do you agree with what your Mom is saying?” It may be useful to allow time for discussion with the caregiver alone. The<br />
child should be interviewed alone when asking questions about sexual or physical abuse and about substance abuse. Circle items of concern.<br />
* The presence of any of these symptoms or behaviors may signal that the child is in crisis, and efforts should be made to secure prompt<br />
evaluation..<br />
Feelings:<br />
Behavior:<br />
Does your child (do you) have feelings that concern you or seem<br />
out of the ordinary for age?<br />
Does your child (do you) behave in ways that seems out of the<br />
ordinary for age?<br />
❏ Restless ❏ Problems in school<br />
❏ Sad or cries easily ❏ * Threatens or harms other children or animals<br />
❏ Guilty ❏ Lacks interest in things s/he used to enjoy<br />
❏ Irritable or angers easily ❏ Engages in sexual play with others, toys, animals<br />
❏ Sullen ❏ * Destroys possessions or other property<br />
❏ Fearful or anxious ❏ Steals<br />
❏ Bored ❏ Refuses to talk<br />
❏ * Sets fires<br />
❏ Overactive<br />
❏ * Has been in trouble with the police<br />
❏ * Self-destructive<br />
Social Interaction:<br />
Thinking:<br />
Do you have concerns about how your child (you) gets along with<br />
family members, other adults or children?<br />
Have you noticed any of the following to be a problem for your child<br />
(you)?<br />
❏ Prefers to be alone ❏ * Frequently confused<br />
❏ Difficulty making and keeping friends ❏ Daydreams excessively<br />
❏ Defiant, a discipline problem ❏ Distracted, doesn’t pay attention<br />
❏ Aggressive ❏ Mistrustful<br />
❏ Argues excessively ❏ * Sees or hears things that are not there<br />
❏ Refuses to go to school ❏ Blames others for his/her misdeeds or thoughts<br />
❏ * Talks about death or suicide<br />
❏ * Frequent memory loss<br />
❏ * Bizarre thoughts<br />
❏ Schoolwork is slipping (grades going down)<br />
Physical Problems:<br />
Other:<br />
Do you have any concerns about the following physical signs? Is this child (are you) accident-prone?<br />
Has this been evaluated?<br />
Are there any situations that are causing your family particular<br />
stress?<br />
❏ Lacks energy<br />
Has this child or his/her parents been subject to neglect, physical,<br />
❏ Uses laxatives<br />
sexual or emotional abuse? If yes, what type, when, treatment, etc.<br />
❏ Vomits frequently ❏ * Is this child at risk for out-of-home placement<br />
❏ Food refusal, secretive eating<br />
because of behavior problems?<br />
❏ Frequent stomachaches ❏ Has the child (have you) been treated for mental health<br />
❏ Headaches<br />
problems or substance abuse?<br />
❏ Excessive weight loss or gain Substance Abuse Questions:<br />
❏ Sleep problems, nightmares, sleep-walking, early<br />
waking, frequent night waking<br />
(May want to use screens such as the TACE, CAGE, MAST to obtain<br />
information concerning substance abuse.)<br />
❏ Has been identified as a problem<br />
Comments:<br />
Signature/Title: _____________________________________________________________________________<br />
CH-316<br />
CPT ONLY - COPYRIGHT 2010 AMERICAN MEDICAL ASSOCIATION. ALL RIGHTS RESERVED.<br />
H EALTH PLANS<br />
www.cfhp.com<br />
123
16.1.4 Texas <strong>Health</strong> Steps Menatl <strong>Health</strong> Questionnaire<br />
TEXAS MEDICAID PROVIDER PROCEDURES MANUAL: VOL. 2<br />
CH.50<br />
Mental <strong>Health</strong> Parent Questionnaire (Ages Birth–2 Years) (2 Pages)<br />
Mental <strong>Health</strong> Parent Questionnaire (Ages Birth–2 Years) (2 Pages)<br />
Mental <strong>Health</strong> Parent Questionnaire<br />
Ages Birth to 2 Years<br />
Child’s Name: ____________________________<br />
Birth Date: _______________________________<br />
Today’s Date: ____________________________<br />
To the Parent: If you will assist us by filling out this form, we can help you find your child’s strengths and any problem<br />
areas, too. Your answers will help us to know if we need to talk with you and find out more about your child. Please<br />
check all items below that are true for your child. Some of the behaviors noted may be normal but if you are concerned<br />
please let us know.<br />
F<br />
e<br />
e<br />
l<br />
i<br />
n<br />
g<br />
s<br />
B<br />
e<br />
h<br />
a<br />
v<br />
i<br />
o<br />
r<br />
S<br />
o<br />
c<br />
i<br />
a<br />
l<br />
T<br />
h<br />
i<br />
n<br />
k<br />
i<br />
n<br />
g<br />
Does your child show feelings that concern you or seem strange for their age? ❑ Yes ❑ No<br />
Infants<br />
❑ Fearful<br />
❑ Cries too much<br />
❑ Cries too little<br />
1 to 2 Years<br />
❑ Is irritable<br />
❑ Is angry<br />
❑ Is sad<br />
❑ Is sullen<br />
❑ Fearful<br />
❑ Cries too little<br />
❑ Cries too much<br />
Does your child do things that concern you or seem strange for their age? ❑ Yes ❑ No<br />
Infants<br />
❑ Is overactive<br />
❑ Is listless (has little energy)<br />
I<br />
n<br />
t<br />
e<br />
r<br />
a<br />
c<br />
t<br />
i<br />
o<br />
n<br />
1 to 2 Years<br />
❑ Is overactive<br />
❑ Is listless (has little energy)<br />
Do you have any concerns about how your child gets along with you? ❑ Yes ❑ No<br />
With other family members or adults? ❑ Yes ❑ No<br />
With brothers and sisters? ❑ Yes ❑ No<br />
Infants<br />
❑ Does not make eye contact or smile<br />
❑ Stiffens and arches back<br />
❑ Does not respond to you<br />
1 to 2 Years<br />
❑ Does not make eye contact<br />
or smile<br />
❑ Clings to you too much<br />
Do you think your child is as bright and thinks as clearly as others their age? ❑ Yes ❑ No<br />
Infants<br />
❑ (>8 months) Does not point to or ask<br />
for things or try to make words<br />
1 to 2 Years<br />
❑ Does not trust others<br />
❑ Has problems concentrating or paying attention<br />
❑ Harms others<br />
❑ Has temper tantrums often<br />
❑ Does not respond to you<br />
❑ Does not say any words yet<br />
124 H EALTH PLANS<br />
CH-318<br />
CPT ONLY - COPYRIGHT 2010 AMERICAN MEDICAL ASSOCIATION. ALL RIGHTS RESERVED.<br />
www.cfhp.com
CHILDREN’S SERVICES HANDBOOK<br />
P<br />
h<br />
y<br />
s<br />
i<br />
c<br />
a<br />
l<br />
O<br />
t<br />
h<br />
e<br />
r<br />
P<br />
r<br />
o<br />
b<br />
l<br />
e<br />
m<br />
s<br />
Do you have any concerns about these things? ❑ Yes ❑ No<br />
If you think your child may have a health problem, has he/she seen a doctor<br />
or nurse about the problem? ❑ Yes ❑ No<br />
Infants to 2 Years<br />
❑ Is low weight or has a lot of weight<br />
❑ Vomits (throws up) often<br />
❑ Has eating problems<br />
(poor appetite, eats non-foods)<br />
Is anything causing your family stress right now? ❑ Yes ❑ No<br />
Has this child or his/her parents been subject to neglect, physical, sexual, or<br />
emotional abuse? If yes, what from? _____________________ When? ________ ❑ Yes ❑ No<br />
Treatment initiated? ❑ Yes ❑ No<br />
Did the mother of this child use drugs or alcohol during the pregnancy? ❑ Yes ❑ No<br />
Comments: (Please write anything else you want us to know about in this space.)<br />
❑ Has sleeping problems (wakes a lot at night)<br />
❑ Has little energy<br />
Date: ____________<br />
Signature: ______________________________________________________<br />
Relation to patient: _______________________________________________<br />
CH-319<br />
CPT ONLY - COPYRIGHT 2010 AMERICAN MEDICAL ASSOCIATION. ALL RIGHTS RESERVED.<br />
H EALTH PLANS<br />
www.cfhp.com<br />
125
TEXAS MEDICAID PROVIDER PROCEDURES MANUAL: VOL. 2<br />
CH.51<br />
Mental <strong>Health</strong> Questionnaire (Ages Birth–2 Years) (2 Pages) (Spanish)<br />
Mental <strong>Health</strong> Questionnaire (Ages Birth–2 Years) (2 Pages) (Spanish)<br />
Cuestionario de la Salud Mental<br />
para los Padres<br />
De Recién Nacido a 2 Años de Edad<br />
Nombre del Niño:________________________________<br />
Fecha de Nacimiento: ___________________________<br />
Fecha: _________________________________________<br />
Para los Padres: Si nos ayuda llenando este formulario, le podremos ayudar a encontrar las áreas fuertes y también cualquier área problématica<br />
que tenga su bebé. Sus respuestas nos ayudarán a saber si necesitamos hablar con usted y saber más sobre su bebé. Favor de marcar<br />
todas las características abajo que son ciertas para su bebé. Algunos de los comportamientos en las listas tal vez sean normales, pero si<br />
usted está preocupado, favor de informarnos.<br />
S<br />
E<br />
N<br />
T<br />
I<br />
M<br />
I<br />
E<br />
N<br />
T<br />
O<br />
S<br />
C<br />
O<br />
M<br />
P<br />
O<br />
R<br />
T<br />
A<br />
M<br />
I<br />
E<br />
N<br />
T<br />
O<br />
¿Tiene su bebé sentimientos que le preocupan o tal vez parezcan extraños para su edad? ❏ Sí ❏ No<br />
Bebés<br />
De 1 a 2 Años<br />
❏ Siente miedo ❏ Es de mal carácter ❏ Siente miedo<br />
❏ Llora mucho ❏ Es enojón ❏ Llora muy poco<br />
❏ Llora muy poco ❏ Es triste ❏ Llora mucho<br />
❏ Es malhumorado<br />
¿Hace su bebé cosas que le preocupan o que parezcan extrañas para su edad? ❏ Sí ❏ No<br />
Bebés<br />
De 1 a 2 Años<br />
❏ Es demasiado activo ❏ Es demasiado activo<br />
❏ Es indiferente (tiene poca energía) ❏ Es indiferente (tiene poca energía)<br />
❏ Lastima a otros<br />
❏ Hace berrinches frecuentemente<br />
I<br />
N<br />
T<br />
E<br />
R<br />
A<br />
C<br />
C<br />
I<br />
O<br />
N<br />
E<br />
S<br />
S<br />
O<br />
C<br />
I<br />
A<br />
L<br />
E<br />
S<br />
¿Se preocupa sobre cómo se lleva su bebé con usted? ❏ Sí ❏ No<br />
¿Con otros miembros de la familia o adultos? ❏ Sí ❏ No<br />
¿Con sus hermanos o hermanas? ❏ Sí ❏ No<br />
Bebés<br />
De 1 a 2 Años<br />
❏ No ve a los ojos ni sonríe ❏ No ve a los ojos ni sonríe<br />
❏ Se pone tieso y se dobla arqueando la espalda ❏ La mayoría del tiempo no se le despega<br />
❏ No le responde ❏ No le responde<br />
❏ Todavía no dice ninguna palabra<br />
P<br />
E<br />
N<br />
S<br />
A<br />
M<br />
I<br />
E<br />
N<br />
T<br />
O<br />
S<br />
¿Piensa usted que su nino es tan inteligente y que piensa tan claramente como otros niños de su edad?<br />
Bebés<br />
De 1 a 2 Años<br />
❏ (>8 meses) No pide ni senala a las cosas o trata ❏ No le tiene confianza a otros<br />
de decir palabras ❏ Tiene problemas para concentrarse y poner atención<br />
❏ Sí<br />
❏ No<br />
CH-320<br />
126 H EALTH PLANS CPT ONLY - COPYRIGHT 2010 AMERICAN MEDICAL ASSOCIATION. ALL RIGHTS RESERVED.<br />
www.cfhp.com
CHILDREN’S SERVICES HANDBOOK<br />
P<br />
R<br />
O<br />
B<br />
L<br />
E<br />
M<br />
A<br />
S<br />
F<br />
I<br />
S<br />
I<br />
C<br />
O<br />
S<br />
¿Se preocupa usted sobre los siguientes problemas físicos? ❏ Sí ❏ No<br />
Si usted piensa que su niño tiene un problema de salud, ¿Lo ha llevado a consultar con<br />
un médico o una enfermera debido a ese problema? ❏ Sí ❏ No<br />
De recién nacidos a 2 Años<br />
❏ Es de peso bajo o ha perdido mucho peso ❏ Tiene problemas para dormir<br />
❏ Se vomita frecuentemente (se despierta mucho durante la noche)<br />
❏ Tiene problemas para comer (muy poco<br />
apetito, come alimentos que no son saludables)<br />
❏ Tiene muy poca energía<br />
¿Hay algo que le esté causando tensión a su familia ahora? ❏ Sí ❏ No<br />
O<br />
T<br />
R<br />
O<br />
S<br />
¿Ha estado este niño o sus padres sujetos a la negligencia o al abuso físicos, sexual o emocional? Si sí,<br />
¿en qué forma?_____________________ ¿Cuándo?_____________<br />
¿Empezó el tratamiento?<br />
¿Usó drogas o tomó bebidas alcohólicas durante su embarazo la mamá de este niño?<br />
❏ Sí ❏ No<br />
❏ Sí ❏ No<br />
❏ Sí ❏ No<br />
Comentarios: (Favor de escribir en este espacio cualquier comentario que quiera compartir con nosotros.)<br />
Fecha:_____________ Firma:________________________________________________________________<br />
Parentesco con el paciente:_____________________________________________<br />
CH-321<br />
CPT ONLY - COPYRIGHT 2010 AMERICAN MEDICAL ASSOCIATION. ALL RIGHTS RESERVED.<br />
H EALTH PLANS<br />
www.cfhp.com<br />
127
TEXAS MEDICAID PROVIDER PROCEDURES MANUAL: VOL. 2<br />
CH.52<br />
Mental <strong>Health</strong> Parent Questionnaire (Ages 3–9 Years) (2 Pages)<br />
Mental <strong>Health</strong> Parent Questionnaire (Ages 3–9 Years) (2 Pages)<br />
Mental <strong>Health</strong> Parent Questionnaire<br />
Child’s Name: ____________________________<br />
Birth Date: _______________________________<br />
Ages 3 to 9 Years<br />
Today’s Date: ____________________________<br />
To the Parent: If you will assist us by filling out this form, we can help you find your child’s strengths and any problem<br />
areas, too. Your answers will help us to know if we need to talk with you and find out more about your child. Please<br />
check all items below that are true for your child. Some of the behaviors noted may be normal but if you are concerned<br />
please let us know.<br />
F<br />
e<br />
e<br />
l<br />
i<br />
n<br />
g<br />
s<br />
Does your child show feelings that concern you or seem strange for their age? ❑ Yes ❑ No<br />
❑ Is restless<br />
❑ Is sad or cries easily<br />
❑ Is overly guilty<br />
❑ Lacks remorse<br />
❑ Is irritable, angers or temper tantrums easily<br />
❑ Is sullen<br />
❑ Fearful<br />
B<br />
e<br />
h<br />
a<br />
v<br />
i<br />
o<br />
r<br />
Does your child do things that seem strange for their age? ❑ Yes ❑ No<br />
❑ Has problems in school<br />
❑ Harms other children or animals<br />
❑ Lacks interest in things s/he used to enjoy<br />
❑ Plays sexual games with others, toys, animals<br />
❑ Destroys possessions or other property<br />
❑ Steals<br />
❑ Refuses to talk<br />
❑ Sets fires<br />
❑ Is over-active<br />
❑ Hurts himself or herself<br />
❑ Has been in trouble with the police<br />
S<br />
o<br />
c<br />
i<br />
a<br />
l<br />
I<br />
n<br />
t<br />
e<br />
r<br />
a<br />
c<br />
t<br />
i<br />
o<br />
n<br />
Do you have any concerns about how your child gets along with you? ❑ Yes ❑ No<br />
With other family members or adults? ❑ Yes ❑ No<br />
With playmates? ❑ Yes ❑ No<br />
❑ Withdraws and does not look into peoples’ eyes<br />
❑ Clings to you too much<br />
❑ Has a hard time making and keeping friends<br />
❑ Is defiant, has a disciplinary problem<br />
❑ Severe or frequent tantrums<br />
❑ Picks on others a lot or often gets into fights (hitting, etc.)<br />
❑ Argues too much<br />
❑ Will not go to school<br />
❑ Prefers to be alone<br />
T<br />
h<br />
i<br />
n<br />
k<br />
i<br />
n<br />
g<br />
Are any of these a problem for your child? ❑ Yes ❑ No<br />
❑ Is frequently confused (does not understand what is going<br />
on)<br />
❑ Daydreams a lot<br />
❑ Is distracted, doesn’t pay attention<br />
❑ Has very strange thoughts<br />
❑ Schoolwork is slipping (grades going down)<br />
❑ Does not trust others<br />
❑ Sees or hears things that are not there<br />
❑ Blames others for his/her misdeeds or thoughts<br />
❑ Talks about death a lot<br />
❑ Often cannot remember things<br />
128 H EALTH PLANS CH-322<br />
CPT ONLY - COPYRIGHT 2010 AMERICAN MEDICAL ASSOCIATION. ALL RIGHTS RESERVED.<br />
www.cfhp.com
CHILDREN’S SERVICES HANDBOOK<br />
P<br />
h<br />
y<br />
s<br />
i<br />
c<br />
a<br />
l<br />
O<br />
t<br />
h<br />
e<br />
r<br />
P<br />
r<br />
o<br />
b<br />
l<br />
e<br />
m<br />
s<br />
Do you have any concerns about these things? ❑ Yes ❑ No<br />
If you think your child may have a health problem, has he/she seen a doctor<br />
or nurse about the problem? ❑ Yes ❑ No<br />
❑ Has daytime wetting<br />
❑ Soils pants<br />
❑ Will not eat<br />
❑ Has headaches<br />
❑ Has lost or gained a lot of weight<br />
❑ Has sleeping problems, nightmares, sleep-walking, early waking<br />
❑ Vomits (throws up) often<br />
❑ Has stomach aches often<br />
❑ Lacks energy<br />
Is this child accident-prone? ❑ Yes ❑ No<br />
Is anything causing your family stress right now? ❑ Yes ❑ No<br />
Has this child or his/her parents been subject to neglect, physical, sexual, or emotional abuse? If yes, what from?<br />
_____________________ When? ________ ❑ Yes ❑ No<br />
Treatment initiated? ❑ Yes ❑ No<br />
Is this child at risk for out-of-home placement because of behavior problems? ❑ Yes ❑ No<br />
Comments: (Please write anything else you want us to know about in this space.)<br />
Date: ____________<br />
Signature: ______________________________________________________<br />
Relation to patient: _______________________________________________<br />
CH-323<br />
CPT ONLY - COPYRIGHT 2010 AMERICAN MEDICAL ASSOCIATION. ALL RIGHTS RESERVED.<br />
H EALTH PLANS<br />
www.cfhp.com<br />
129
TEXAS MEDICAID PROVIDER PROCEDURES MANUAL: VOL. 2<br />
CH.53<br />
Mental <strong>Health</strong> Parent Questionnaire (Ages 3–9 Years) (2 Pages) (Spanish)<br />
Mental <strong>Health</strong> Parent Questionnaire (Ages 3–9 Years) (2 Pages) (Spanish)<br />
Cuestionario de la Salud Mental<br />
para los Padres<br />
De 3 a 9 Años de Edad<br />
Nombre del Niño:________________________________<br />
Fecha de Nacimiento: ____________________________<br />
Fecha: _________________________________________<br />
Para los Padres: Si nos ayuda llenando este formulario, le podremos ayudar a encontrar las áreas fuertes y también cualquier área problématica<br />
que tenga su niño. Sus respuestas nos ayudarán a saber si necesitamos hablar con usted y saber más sobre su niño. Favor de marcar<br />
todas las características abajo que sean ciertas para su niño. Algunos de los comportamientos en las listas tal vez sean normales, pero si<br />
usted está preocupado, favor de informarnos.<br />
S<br />
E<br />
N<br />
T<br />
I<br />
M<br />
I<br />
E<br />
N<br />
T<br />
O<br />
S<br />
¿Tiene su niño sentimientos que le preocupan o tal vez parezcan extraños para su edad? ❏ Sí ❏ No<br />
❏ Es inquieto ❏ Es de mal carácter, enojón o hace berrinches<br />
❏ Es triste o llora fácilmente temperamentales fácilmente<br />
❏ Se siente muy culpable ❏ Es malhumorado<br />
❏ No tiene remordimiento ❏ Siente miedo<br />
C<br />
O<br />
M<br />
P<br />
O<br />
R<br />
T<br />
A<br />
M<br />
I<br />
E<br />
N<br />
T<br />
O<br />
¿Hace su niño cosas que le parezcan extrañas para su edad? ❏ Sí ❏ No<br />
❏ Tiene problemas en la escuela ❏ Se niega a hablar<br />
❏ Lastima a otros niños o a los animales ❏ Provoca incendios<br />
❏ No le interesan las cosas que antes le gustaban ❏ Es demasiado activo<br />
❏ Juega juegos sexuales con otros niños, ❏ Se lastima<br />
juguetes, o animales ❏ Ha tenido problemas con la policía<br />
❏ Destruye cosas personales u ajenas<br />
❏ Roba<br />
I<br />
N<br />
T<br />
E<br />
R<br />
A<br />
C<br />
C<br />
I<br />
O<br />
N<br />
E<br />
S<br />
S<br />
O<br />
C<br />
I<br />
A<br />
L<br />
E<br />
S<br />
¿Se preocupa sobre cómo se lleva su niño con usted? ❏ Sí ❏ No<br />
¿Con otros miembros de la familia o adultos? ❏ Sí ❏ No<br />
¿Con sus compañeros de juego? ❏ Sí ❏ No<br />
❏ Se aleja y no ve a nadie a los ojos ❏ Siempre molesta a otros o frecuentemente se<br />
❏ La mayoría del tiempo no se le despega pelea (pegando, etc.)<br />
❏ Se le dificulta hacer y mantener amistades ❏ Discute mucho<br />
❏ Es desafiante, tiene un problema de disciplina ❏ No quiere asistir a la escuela<br />
❏ Hace berrinches tempermentales fuertes o ❏ Prefiere estar solo<br />
frecuentemente<br />
P<br />
E<br />
N<br />
S<br />
A<br />
M<br />
I<br />
E<br />
N<br />
T<br />
O<br />
S<br />
¿Son algunas de estas características un problema para su niño? ❏ Sí ❏ No<br />
❏ Se confunde frecuentemente (no entiende ❏ No le tiene confianza a los demás<br />
lo que está pasando) ❏ Mira u oye cosas que no están allí<br />
❏ Sueña mucho despierto ❏ Culpa a otros por algo que hizo mal o por sus<br />
❏ Se distrae, no pone atención pensamientos<br />
❏ Tiene pensamientos muy extraños ❏ Habla mucho sobre la muerte<br />
❏ Se está atrasando en el trabajo de la escuela (sus<br />
grados están bajando)<br />
❏ Frecuentemente no se acuerda de cosas<br />
130 H EALTH PLANS<br />
www.cfhp.com<br />
CH-324
CHILDREN’S SERVICES HANDBOOK<br />
P<br />
R<br />
O<br />
B<br />
L<br />
E<br />
M<br />
A<br />
S<br />
F<br />
I<br />
S<br />
I<br />
C<br />
O<br />
S<br />
¿Se preocupa usted sobre los siguientes problemas físicos?<br />
❏ Sí ❏ No<br />
Si usted piensa que su niño tiene un problema de salud, ¿Lo ha llevado a consultar con<br />
un médico o una enfermera debido a ese problema? ❏ Sí ❏ No<br />
❏ Se orina durante el día ❏ Tiene problemas para dormir, pesadillas, se<br />
❏ Ensucia sus pantalones despierta temprano y sonámbulo<br />
❏ No quiere comer ❏ Se vomita frecuentemente<br />
❏ Tiene dolores de cabeza ❏ Tiene dolores de estómago frecuentemente<br />
❏ Ha perdido o aumentado mucho de peso ❏ No tiene energía<br />
O<br />
T<br />
R<br />
O<br />
S<br />
¿Es propenso este niño a tener accidentes? ❏ Sí ❏ No<br />
¿Hay algo que le está causando tensión a su familia ahora? ❏ Sí ❏ No<br />
¿Ha estado este niño o sus padres sujetos a la negligencia o al abuso físico, sexual o emocional?<br />
Si sí, ¿en qué forma?_________________ ❏ Sí ❏ No<br />
¿Cuándo? ___________ ¿Empezó el tratamiento? ❏ Sí ❏ No<br />
¿Corre el riesgo este niño de ser llevado a otro lugar fuera de su familia<br />
por problemas de comportamiento? ❏ Sí ❏ No<br />
Comentario: (Favor de escribir en este espacio cualquier comentario que quiera compartir con nosotros.)<br />
Fecha:_____________ Firma:________________________________________________________________<br />
Parentesco con el paciente:_____________________________________________<br />
CH-325<br />
H EALTH PLANS<br />
www.cfhp.com<br />
131
TEXAS MEDICAID PROVIDER PROCEDURES MANUAL: VOL. 2<br />
CH.54<br />
Mental <strong>Health</strong> Parent Questionnaire (Ages 10–12 Years) (2 Pages)<br />
Mental <strong>Health</strong> Parent Questionnaire (Ages 10–12 Years) (2 Pages)<br />
Mental <strong>Health</strong> Parent Questionnaire<br />
Child’s Name: _____________________________<br />
Birth Date: ________________________________<br />
Ages 10 to 12 Years<br />
Today’s Date: _____________________________<br />
To the Parent: If you will assist us by filling out this form, we can help you find your child’s strengths and any problem<br />
areas, too. Your answers will help us to know if we need to talk with you and find out more about your child. Please<br />
check all items below that are true for your child. Some of the behaviors noted may be normal but if you are concerned<br />
please let us know.<br />
F<br />
e<br />
e<br />
l<br />
i<br />
n<br />
g<br />
s<br />
Does your child (do you) show feelings that concern you or seem strange for their (your) age? ❑ Yes ❑ No<br />
❑ Is restless<br />
❑ Is sad or cries easily<br />
❑ Is guilty<br />
❑ Is irritable or angers easily<br />
❑ Is sullen<br />
❑ Is fearful<br />
❑ Is bored<br />
B<br />
e<br />
h<br />
a<br />
v<br />
i<br />
o<br />
r<br />
Does your child (do you) often do things that seem strange for their (your) age? ❑ Yes ❑ No<br />
❑ Has problems in school<br />
❑ Threatens or harms other children or animals<br />
❑ Lacks interest in things s/he used to enjoy<br />
❑ Is involved in sexual activity<br />
❑ Destroys possessions or other property<br />
❑ Steals<br />
❑ Refuses to talk<br />
❑ Sets fires<br />
❑ Is overactive<br />
❑ Hurts himself or herself<br />
❑ Has been in trouble with the police<br />
S<br />
o<br />
c<br />
i<br />
a<br />
l<br />
I<br />
n<br />
t<br />
e<br />
r<br />
a<br />
c<br />
t<br />
i<br />
o<br />
n<br />
Do you have any concerns about how your child (you) get(s) along with family members? ❑ Yes ❑ No<br />
With other adults? ❑ Yes<br />
❑ No<br />
With other children? ❑ Yes ❑ No<br />
❑ Prefers to be alone<br />
❑ Has a hard time making and keeping friends<br />
❑ Is defiant, a disciplinary problem<br />
❑ Picks on others a lot or often gets into fights (hitting, etc.)<br />
❑ Argues too much<br />
❑ Will not go to school<br />
T<br />
h<br />
i<br />
n<br />
k<br />
i<br />
n<br />
g<br />
Are any of these a problem for your child (you)? ❑ Yes ❑ No<br />
❑ Is frequently confused (does not understand what is<br />
going on)<br />
❑ Daydreams a lot<br />
❑ Is distracted, doesn’t pay attention<br />
❑ Has very strange thoughts<br />
❑ Schoolwork is slipping (grades going down)<br />
❑ Does not trust others<br />
❑ Sees or hears things that are not there<br />
❑ Blames others for his/her misdeeds or thoughts<br />
❑ Talks about death or suicide a lot<br />
❑ Often cannot remember things<br />
132 H EALTH PLANS<br />
www.cfhp.com<br />
CH-326<br />
CPT ONLY - COPYRIGHT 2010 AMERICAN MEDICAL ASSOCIATION. ALL RIGHTS RESERVED.
CHILDREN’S SERVICES HANDBOOK<br />
P<br />
h<br />
y<br />
s<br />
i<br />
c<br />
a<br />
l<br />
O<br />
t<br />
h<br />
e<br />
r<br />
P<br />
r<br />
o<br />
b<br />
l<br />
e<br />
m<br />
s<br />
Do you have any concerns about these things? ❑ Yes ❑ No<br />
If you think your child (you) may have a health problem, has he/she (have you) seen a doctor or nurse about the<br />
problem? ❑ Yes<br />
❑ No<br />
❑ Lacks energy<br />
❑ Uses laxatives<br />
❑ Vomits (throws up) often<br />
❑ Won’t eat in front of people, sneaks food<br />
later<br />
❑ Has stomach aches often<br />
❑ Has headaches<br />
❑ Has lost or gained a lot of weight<br />
❑ Has sleeping problems, nightmares, sleep-walking, early waking,<br />
frequent night waking<br />
Is your child (you) accident-prone? ❑ Yes ❑ No<br />
Is anything causing your family stress right now? ❑ Yes ❑ No<br />
Has this child or his/her parents been subject to neglect, physical, sexual, or emotional abuse? If yes, what from?<br />
_____________________ When? ________ ❑ Yes ❑ No<br />
Treatment initiated? ❑ Yes ❑ No<br />
Is this child (are you) at risk for out-of-home placement because of behavior problems? ❑ Yes ❑ No<br />
Does your child (do you) drink of use drugs (including street or over-the-counter)? ❑ Yes ❑ No<br />
Has this child (have you) been treated for mental health problems or substance abuse? ❑ Yes ❑ No<br />
Comments: (Please write anything else you want us to know about in this space.)<br />
Date: ____________<br />
Signature: ______________________________________________________<br />
Relation to patient: _______________________________________________<br />
CH-327<br />
CPT ONLY - COPYRIGHT 2010 AMERICAN MEDICAL ASSOCIATION. ALL RIGHTS RESERVED.<br />
H EALTH PLANS<br />
www.cfhp.com<br />
133
TEXAS MEDICAID PROVIDER PROCEDURES MANUAL: VOL. 2<br />
CH.55<br />
Mental <strong>Health</strong> Parent Questionnaire (Ages 10–12 Years) (2 Pages) (Spanish)<br />
Mental <strong>Health</strong> Parent Questionnaire (Ages 10–12 Years) (2 Pages) (Spanish)<br />
Cuestionario de la Salud Mental<br />
para los Padres<br />
De 10 a 12 Años de Edad<br />
Nombre del Niño:_________________________________<br />
Fecha de Nacimiento: ____________________________<br />
Fecha: _________________________________________<br />
Para los Padres: Si nos ayuda llenando este formulario, le podremos ayudar a encontrar las áreas fuertes y también cualquier área problématica<br />
que tenga su hijo. Sus respuestas nos ayudarán a saber si necesitamos hablar con usted y saber más sobre su niño. Favor de marcar<br />
todas las características abajo que son ciertas para su niño. Algunos de los comportamientos en las listas tal vez sean normales, pero si usted<br />
está preocupado, favor de informarnos.<br />
S<br />
E<br />
N<br />
T<br />
I<br />
M<br />
I<br />
E<br />
N<br />
T<br />
O<br />
S<br />
¿Tiene su niño sentimientos que le preocupan o tal vez parezcan extraños para su edad? ❏ Sí ❏ No<br />
❏ Es inquieto ❏ Es malhumorado<br />
❏ Es triste o llora fácilmente ❏ Siente miedo<br />
❏ Se siente culpable ❏ Se aburre<br />
❏ Es de mal carácter o se enoja fácilmente<br />
C<br />
O<br />
M<br />
P<br />
O<br />
R<br />
T<br />
A<br />
M<br />
I<br />
E<br />
N<br />
T<br />
O<br />
¿Hace su niño cosas que le parezcan extrañas para su edad? ❏ Sí ❏ No<br />
❏ Tiene problemas en la escuela ❏ Se niega a hablar<br />
❏ Amenaza o lastima a otros niños o a los ❏ Provoca incendios<br />
animales ❏ Es demasiado activo<br />
❏ No le interesan las cosas que antes le gustaban ❏ Se lastima<br />
❏ Participa en actividades sexuales ❏ Ha tenido problemas con la policía<br />
❏ Destruye cosas personales o ajenas<br />
❏ Roba<br />
I<br />
N<br />
T<br />
E<br />
R<br />
A<br />
C<br />
C<br />
I<br />
O<br />
N<br />
E<br />
S<br />
S<br />
O<br />
C<br />
I<br />
A<br />
L<br />
E<br />
S<br />
¿Se preocupa sobre cómo se lleva su niño con usted? ❏ Sí ❏ No<br />
¿Con otros adultos? ❏ Sí ❏ No<br />
¿Con otros niños? ❏ Sí ❏ No<br />
❏ Prefiere estar solo ❏ Siempre molesta a otros o frecuentemente se pelea<br />
(pegando, etc.)<br />
❏ Se le dificulta hacer y mantener amistades ❏ Discute mucho<br />
❏ Es desafiante, tiene un problema de disciplina ❏ No quiere asistir a la escuela<br />
P<br />
E<br />
N<br />
S<br />
A<br />
M<br />
I<br />
E<br />
N<br />
T<br />
O<br />
S<br />
¿Son algunas de estas características un problema para su ❏ Sí ❏ No<br />
niño?<br />
❏ Se confunde frecuentemente (no entiende lo que está<br />
pasando)<br />
❏ No le tiene confianza a los demás<br />
❏ Sueña mucho despierto ❏ Mira u oye cosas que no están allí<br />
❏ Se distrae, no pone atención ❏ Culpa a otros por algo que hizo mal o por sus<br />
pensamientos<br />
❏ Tiene pensamientos muy extraños ❏ Habla mucho sobre la muerte o del suicidio<br />
❏ Se está atrasando en el trabajo de la escuela (sus<br />
grados están bajando)<br />
❏ Frecuentemente no se acuerda de cosas<br />
134 H EALTH PLANS<br />
www.cfhp.com<br />
CH-328<br />
CPT ONLY - COPYRIGHT 2010 AMERICAN MEDICAL ASSOCIATION. ALL RIGHTS RESERVED.
CHILDREN’S SERVICES HANDBOOK<br />
P<br />
R<br />
O<br />
B<br />
L<br />
E<br />
M<br />
A<br />
S<br />
O<br />
T<br />
R<br />
O<br />
S<br />
F<br />
I<br />
S<br />
I<br />
C<br />
O<br />
S<br />
¿Se preocupa usted sobre los siguientes problemas físicos? ❏ Sí ❏ No<br />
Si piensa que su niño tiene un problema de salud, ¿ha ido a ❏ Sí ❏ No<br />
consultar con un médico o una enfermera debido a ese<br />
problema?<br />
❏ La falta energía ❏ Tiene dolores de cabeza<br />
❏ Usa laxantes ❏ Ha perdido o aumentado mucho peso<br />
❏ Se vomita frecuentemente ❏ Tiene problemas para dormir, pesadillas, sonambulismo,<br />
despierta temprano, despierta seguido por la noche<br />
❏ No come delante de la gente, come después a escondidas<br />
❏ Tiene dolores de estómago frecuentemente<br />
¿Es propenso a tener accidentes su niño? ❏ Sí ❏ No<br />
¿Hay algo que le está causando tensión a su familia ahora? ❏ Sí ❏ No<br />
¿Ha sido este niño o sus padres sujetos a la negligencia o al abuso físico, sexual o emocional?<br />
Si sí, ¿en qué forma?_________________ ¿Cuándo? ___________ ❏ Sí ❏ No<br />
¿Empezó el tratamiento? ❏ Sí ❏ No<br />
¿Corre este niño el riesgo de ser llevado a otro lugar fuera de su familia por problemas de comportamiento? ❏ Sí ❏ No<br />
¿Toma bebidas alcohólicas o usa drogas su niño (incluyendo las de la calle y las que se venden sin receta)? ❏ Sí ❏ No<br />
¿Ha recibido su niño tratamiento por problemas de la salud mental o por el abuso de sustancia como las ❏ Sí ❏ No<br />
drogas y bebidas alcohólicas?<br />
Comentario: (Favor de escribir en este espacio cualquier comentario que quiera compartir con nosotros.)<br />
Fecha:_____________ Firma:________________________________________________________________<br />
Parentesco con el paciente:_____________________________________________<br />
CH-329<br />
CPT ONLY - COPYRIGHT 2010 AMERICAN MEDICAL ASSOCIATION. ALL RIGHTS RESERVED.<br />
H EALTH PLANS<br />
www.cfhp.com<br />
135
TEXAS MEDICAID PROVIDER PROCEDURES MANUAL: VOL. 2<br />
CH.56<br />
Mental <strong>Health</strong> Parent Questionnaire (Ages 13–20 Years) (2 Pages)<br />
Mental <strong>Health</strong> Parent Questionnaire (Ages 13–20 Years) (2 Pages)<br />
Mental <strong>Health</strong> Parent Questionnaire<br />
Teen’s Name: ____________________________<br />
Ages 13 to 20 Years<br />
Birth Date: _______________________________<br />
Today’s Date: ____________________________<br />
To the Teen or Parent: If you will assist us by filling out this form, we can help you find your (your teen’s) strengths and<br />
any problem areas, too. Your answers will help us to know if we need to talk with you (your teen) and find out more about<br />
you (your teen). Please check all items below that are true for you (your teen). Some of the behaviors noted may be<br />
normal but if you are concerned please let us know.<br />
F<br />
e<br />
e<br />
l<br />
i<br />
n<br />
g<br />
s<br />
Do you (does your teen) show feelings that concern you or seem strange for your (their) age? ❑ Yes ❑ No<br />
❑Restless<br />
❑Sad or cry easily<br />
❑Guilty<br />
❑ Irritable or angered easily<br />
❑ Sullen<br />
❑ Fearful<br />
❑ Bored<br />
B<br />
e<br />
h<br />
a<br />
v<br />
i<br />
o<br />
r<br />
Do you (does your teen) often do things that seem strange for your (their) age? ❑ Yes ❑ No<br />
❑ Have problems in school or work<br />
❑ Threaten or harm other children or animals<br />
❑ Lack interest in things you used to enjoy<br />
❑ Is involved in sexual activity<br />
❑ Destroy possessions or other property<br />
❑ Steal<br />
❑ Refuse to talk<br />
❑ Set fires<br />
❑ Over-active<br />
❑ Hurt yourself<br />
❑ Have been in trouble with the police<br />
S<br />
o<br />
c<br />
i<br />
a<br />
l<br />
I<br />
n<br />
t<br />
e<br />
r<br />
a<br />
c<br />
t<br />
i<br />
o<br />
n<br />
Do you have any concerns about how you (your teen) get(s) along with family members? ❑ Yes ❑ No<br />
With other adults? ❑ Yes ❑ No<br />
With peers? ❑ Yes ❑ No<br />
❑ Prefer to be alone<br />
❑ Have a hard time making and keeping friends<br />
❑ Defiant, a disciplinary problem<br />
❑ Pick on others a lot or often get into fights (hitting, etc.)<br />
❑ Argue too much<br />
❑ Will not go to school<br />
T<br />
h<br />
i<br />
n<br />
k<br />
i<br />
n<br />
g<br />
Are any of these a problem for you (your teen)? ❑ Yes ❑ No<br />
❑ Frequently confused (does not understand what is going<br />
on)<br />
❑ Daydream a lot<br />
❑ Distracted, do not pay attention<br />
❑ Have very strange thoughts<br />
❑ Schoolwork is slipping (grades going down)<br />
❑ Do not trust others<br />
❑ See or hear things that are not there<br />
❑ Blame others for your misdeeds or thoughts<br />
❑ Talk about death or suicide a lot<br />
❑ Often cannot remember things<br />
136 H EALTH PLANS<br />
CH-330<br />
CPT ONLY - COPYRIGHT 2010 AMERICAN MEDICAL ASSOCIATION. ALL RIGHTS RESERVED.<br />
www.cfhp.com
CHILDREN’S SERVICES HANDBOOK<br />
P<br />
h<br />
y<br />
s<br />
i<br />
c<br />
a<br />
l<br />
O<br />
t<br />
h<br />
e<br />
r<br />
P<br />
r<br />
o<br />
b<br />
l<br />
e<br />
m<br />
s<br />
Do you have any concerns about these things? ❑ Yes ❑ No<br />
If you think you (your teen) may have a health problem, have you (has he/she) seen a doctor or nurse about the<br />
problem? ❑ Yes ❑ No<br />
❑ Lack energy<br />
❑ Use laxatives<br />
❑ Vomit (throw up) often<br />
❑ Won’t eat in front of people, sneak food<br />
later<br />
❑ Have stomachaches often<br />
❑ Have headaches<br />
❑ Have lost or gained a lot of weight<br />
❑ Have sleeping problems, nightmares, sleep-walking, early waking,<br />
frequent night waking<br />
Are you (is your teen) accident-prone? ❑ Yes ❑ No<br />
Is anything causing your family stress right now? ❑ Yes ❑ No<br />
Have you (has your teen) or your parents been subject to neglect, physical, sexual, or emotional abuse? If yes, what from?<br />
_____________________ When? ________ ❑ Yes ❑ No<br />
Treatment initiated? ❑ Yes ❑ No<br />
Are you (is this teen) at risk for out-of-home placement because of behavior problems? ❑ Yes ❑ No<br />
Do you (does your child) drink of use drugs (including street or over-the-counter)? ❑ Yes ❑ No<br />
Have you (has this teen) been treated for mental health problems or substance abuse? ❑ Yes ❑ No<br />
Comments: (Please write anything else you want us to know about in this space.)<br />
Date: ____________<br />
Signature: ______________________________________________________<br />
Relation to patient: _______________________________________________<br />
CH-331<br />
CPT ONLY - COPYRIGHT 2010 AMERICAN MEDICAL ASSOCIATION. ALL RIGHTS RESERVED.<br />
H EALTH PLANS<br />
www.cfhp.com<br />
137
TEXAS MEDICAID PROVIDER PROCEDURES MANUAL: VOL. 2<br />
CH.57<br />
Mental <strong>Health</strong> Parent Questionnaire (Ages 13–20 Years) (2 Pages) (Spanish)<br />
Mental <strong>Health</strong> Parent Questionnaire (Ages 13–20 Years) (2 Pages) (Spanish)<br />
Cuestionario de la Salud Mental<br />
para los Padres<br />
De 13 a 20 Años de Edad<br />
Nombre del Adolescente:__________________________<br />
Fecha de Nacimiento: ____________________________<br />
Fecha: _________________________________________<br />
Para los Padres: Si nos ayuda llenando este formulario, podremos ayudarle a encontrar las áreas fuertes que tenga su hijo y también cualquier<br />
área problématica. Sus respuestas nos ayudarán a saber si necesitamos hablar con su hijo y saber más sobre él. Favor de marcar todas las<br />
características abajo que son ciertas para su hijo. Algunos de los comportamientos en las listas tal vez sean normales, pero si usted está<br />
preocupado, favor de informarnos.<br />
S<br />
E<br />
N<br />
T<br />
I<br />
M<br />
I<br />
E<br />
N<br />
T<br />
O<br />
S<br />
C<br />
O<br />
M<br />
P<br />
O<br />
R<br />
T<br />
A<br />
M<br />
I<br />
E<br />
N<br />
T<br />
O<br />
¿Tiene su hijo sentimientos que le preocupan o tal vez ❏ Sí ❏ No<br />
parezcan extraños para su edad?<br />
❏ Es inquieto ❏ Es malhumorado<br />
❏ Es triste o llora fácilmente ❏ Siente miedo<br />
❏ Se siente culpable ❏ Se aburre<br />
❏ Es irrita o enoja fácilmente<br />
¿Hace su hijo cosas frecuentemente que le parezcan extrañas ❏ Sí ❏ No<br />
para su edad?<br />
❏ Tiene problemas en la escuela o en el trabajo ❏ Se niega a hablar<br />
❏ Amenaza o lastima a otros niños o a los animales ❏ Provoca incendios<br />
❏ No le interesan las cosas que antes le gustaban ❏ Es demasiado activo<br />
❏ Está envuelto en actividades sexuales ❏ Se lastima<br />
❏ Destruye cosas personales u otras cosas ajenas ❏ Ha tenido problemas con la policía<br />
❏ Roba<br />
I<br />
N<br />
T<br />
E<br />
R<br />
A<br />
C<br />
C<br />
I<br />
O<br />
N<br />
E<br />
S<br />
S<br />
O<br />
C<br />
I<br />
A<br />
L<br />
E<br />
S<br />
¿Le preocupa cómo se lleva su hijo con los miembros de la ❏ Sí ❏ No<br />
familia?<br />
¿Con otros adultos? ❏ Sí ❏ No<br />
¿Con su grupo social? ❏ Sí ❏ No<br />
❏ Prefiere estar solo ❏ Molesta mucho a otros o frecuentemente se pelea<br />
(pegando, etc.)<br />
❏ Se le dificulta hacer y mantener amistades ❏ Discute mucho<br />
❏ Es desafiante, tiene un problema de disciplina ❏ No quiere asistir a la escuela<br />
P<br />
E<br />
N<br />
S<br />
A<br />
M<br />
I<br />
E<br />
N<br />
T<br />
O<br />
S<br />
¿Son algunas de estas características un problema para su ❏ Sí ❏ No<br />
hijo?<br />
❏ Se confunde frecuentemente (no entiende lo que está<br />
pasando)<br />
❏ No le tiene confianza a los demás<br />
❏ Sueña mucho despierto ❏ Mira u oye cosas que no están allí<br />
❏ Se distrae, no pone atención ❏ Culpa a otros por algo que hizo mal o por sus<br />
pensamientos<br />
❏ Tiene pensamientos muy extraños ❏ Habla mucho sobre la muerte o el suicidio<br />
❏ Se está atrasando en el trabajo de la escuela (sus<br />
grados están bajando)<br />
❏ Frecuentemente no se acuerda de cosas<br />
138 H EALTH PLANS<br />
www.cfhp.com
H EALTH PLANS<br />
www.cfhp.com<br />
139
16.2.1 Immunization Schedule 0-6 years<br />
FIGURE 1: Recommended immunization schedule for persons aged 0 through 6 years—United States, 2012 (for those who fall behind or start late, see the catch-up<br />
schedule [Figure 3])<br />
Vaccine ▼ Age ► Birth<br />
1<br />
month<br />
2<br />
months<br />
4<br />
months<br />
6<br />
months<br />
Hepatitis B 1<br />
Hep B HepB<br />
Rotavirus 2 RV RV RV 2<br />
Diphtheria, tetanus, pertussis 3 DTaP DTaP DTaP<br />
Haemophilus influenzae type b 4 Hib Hib Hib 4<br />
Pneumococcal 5 PCV PCV PCV<br />
Inactivated poliovirus 6 IPV IPV<br />
Influenza 7<br />
Measles, mumps, rubella 8<br />
Varicella 9<br />
Hepatitis A 10<br />
Meningococcal 11<br />
9<br />
months<br />
12<br />
months<br />
HepB<br />
15<br />
months<br />
18<br />
months<br />
DTaP<br />
Hib<br />
PCV<br />
IPV<br />
Influenza (Yearly)<br />
19–23<br />
months<br />
2–3<br />
years<br />
4–6<br />
years<br />
PPSV<br />
IPV<br />
MCV4 — see footnote 11<br />
This schedule includes recommendations in effect as of December 23, 2011. Any dose not administered at the recommended age should be administered at a subsequent visit, when indicated<br />
and feasible. The use of a combination vaccine generally is preferred over separate injections of its equivalent component vaccines. Vaccination providers should consult the relevant Advisory<br />
Committee on Immunization Practices (ACIP) statement for detailed recommendations, available online at http://www.cdc.gov/vaccines/pubs/acip-list.htm. <strong>Clinical</strong>ly significant adverse events that<br />
follow vaccination should be reported to the Vaccine Adverse Event Reporting System (VAERS) online (http://www.vaers.hhs.gov) or by telephone (800-822-7967).<br />
1. Hepatitis B (HepB) vaccine. (Minimum age: birth)<br />
At birth:<br />
• Administer monovalent HepB vaccine to all newborns before hospital<br />
discharge.<br />
• For infants born to hepatitis B surface antigen (HBsAg)–positive mothers,<br />
administer HepB vaccine and 0.5 mL of hepatitis B immune globulin (HBIG)<br />
within 12 hours of birth. These infants should be tested for HBsAg and antibody<br />
to HBsAg (anti-HBs) 1 to 2 months after receiving the last dose of the series.<br />
• If mother’s HBsAg status is unknown, within 12 hours of birth administer<br />
HepB vaccine for infants weighing ≥2,000 grams, and HepB vaccine plus<br />
HBIG for infants weighing
FIGURE 2: Recommended immunization schedule for persons aged 7 through 18 years—United States, 2012 (for those who fall behind or start late, see the<br />
schedule below and the catch-up schedule [Figure 3])<br />
Vaccine ▼ Age ► 7–10 years 11–12 years 13–18 years<br />
Tetanus, diphtheria, pertussis 1<br />
Human papillomavirus 2<br />
Meningococcal 3<br />
Influenza 4<br />
Pneumococcal 5<br />
Hepatitis A 6<br />
Hepatitis B 7<br />
Inactivated poliovirus 8<br />
Measles, mumps, rubella 9<br />
Varicella 10<br />
This schedule includes recommendations in effect as of December 23, 2011. Any dose not administered at the recommended age should be administered at a subsequent<br />
visit, when indicated and feasible. The use of a combination vaccine generally is preferred over separate injections of its equivalent component vaccines. Vaccination providers<br />
should consult the relevant Advisory Committee on Immunization Practices (ACIP) statement for detailed recommendations, available online at http://www.cdc.gov/vaccines/<br />
pubs/acip-list.htm. <strong>Clinical</strong>ly significant adverse events that follow vaccination should be reported to the Vaccine Adverse Event Reporting System (VAERS) online (http://www.<br />
vaers.hhs.gov) or by telephone (800-822-7967).<br />
1. Tetanus and diphtheria toxoids and acellular pertussis (Tdap) vaccine.<br />
(Minimum age: 10 years for Boostrix and 11 years for Adacel)<br />
• Persons aged 11 through 18 years who have not received Tdap vaccine<br />
should receive a dose followed by tetanus and diphtheria toxoids (Td)<br />
booster doses every 10 years thereafter.<br />
• Tdap vaccine should be substituted for a single dose of Td in the catchup<br />
series for children aged 7 through 10 years. Refer to the catch-up<br />
schedule if additional doses of tetanus and diphtheria toxoid–containing<br />
vaccine are needed.<br />
• Tdap vaccine can be administered regardless of the interval since the last<br />
tetanus and diphtheria toxoid–containing vaccine.<br />
2. Human papillomavirus (HPV) vaccines (HPV4 [Gardasil] and HPV2<br />
[Cervarix]). (Minimum age: 9 years)<br />
• Either HPV4 or HPV2 is recommended in a 3-dose series for females<br />
aged 11 or 12 years. HPV4 is recommended in a 3-dose series for males<br />
aged 11 or 12 years.<br />
• The vaccine series can be started beginning at age 9 years.<br />
• Administer the second dose 1 to 2 months after the first dose and the<br />
third dose 6 months after the first dose (at least 24 weeks after the first<br />
dose).<br />
• See MMWR 2010;59:626–32, available at http://www.cdc.gov/mmwr/pdf/<br />
wk/mm5920.pdf.<br />
3. Meningococcal conjugate vaccines, quadrivalent (MCV4).<br />
• Administer MCV4 at age 11 through 12 years with a booster dose at age<br />
16 years.<br />
• Administer MCV4 at age 13 through 18 years if patient is not previously<br />
vaccinated.<br />
• If the first dose is administered at age 13 through 15 years, a booster<br />
dose should be administered at age 16 through 18 years with a minimum<br />
interval of at least 8 weeks after the preceding dose.<br />
• If the first dose is administered at age 16 years or older, a booster dose is<br />
not needed.<br />
• Administer 2 primary doses at least 8 weeks apart to previously<br />
unvaccinated persons with persistent complement component deficiency<br />
or anatomic/functional asplenia, and 1 dose every 5 years thereafter.<br />
• Adolescents aged 11 through 18 years with human immunodeficiency<br />
virus (HIV) infection should receive a 2-dose primary series of MCV4, at<br />
least 8 weeks apart.<br />
• See MMWR 2011;60:72–76, available at http://www.cdc.gov/mmwr/<br />
pdf/wk/mm6003.pdf, and Vaccines for Children Program resolution No.<br />
6/11-1, available at http://www.cdc.gov/vaccines/programs/vfc/downloads/<br />
resolutions/06-11mening-mcv.pdf, for further guidelines.<br />
4. Influenza vaccines (trivalent inactivated influenza vaccine [TIV] and<br />
live, attenuated influenza vaccine [LAIV]).<br />
• For most healthy, nonpregnant persons, either LAIV or TIV may be used,<br />
except LAIV should not be used for some persons, including those with<br />
asthma or any other underlying medical conditions that predispose them<br />
to influenza complications. For all other contraindications to use of LAIV,<br />
see MMWR 2010;59(No.RR-8), available at http://www.cdc.gov/mmwr/<br />
pdf/rr/rr5908.pdf.<br />
• Administer 1 dose to persons aged 9 years and older.<br />
1 dose (if indicated) 1 dose<br />
1 dose (if indicated)<br />
see footnote 2<br />
3 doses<br />
Complete 3-dose series<br />
See footnote 3<br />
Dose 1<br />
Booster at 16 years old<br />
Influenza (yearly)<br />
See footnote 5<br />
Complete 2-dose series<br />
Complete 3-dose series<br />
Complete 3-dose series<br />
Complete 2-Dose 2-dose series Series<br />
Complete 2-dose series<br />
Range of<br />
recommended<br />
ages for all<br />
children<br />
Range of<br />
recommended<br />
ages for<br />
catch-up<br />
immunization<br />
Range of<br />
recommended<br />
ages for certain<br />
high-risk<br />
groups<br />
• For children aged 6 months through 8 years:<br />
— For the 2011–12 season, administer 2 doses (separated by at least<br />
4 weeks) to those who did not receive at least 1 dose of the 2010–<br />
11 vaccine. Those who received at least 1 dose of the 2010–11<br />
vaccine require 1 dose for the 2011–12 season.<br />
— For the 2012–13 season, follow dosing guidelines in the 2012 ACIP<br />
influenza vaccine recommendations.<br />
5. Pneumococcal vaccines (pneumococcal conjugate vaccine [PCV] and<br />
pneumococcal polysaccharide vaccine [PPSV]).<br />
• A single dose of PCV may be administered to children aged 6 through<br />
18 years who have anatomic/functional asplenia, HIV infection or other<br />
immunocompromising condition, cochlear implant, or cerebral spinal fluid<br />
leak. See MMWR 2010:59(No. RR-11), available at http://www.cdc.gov/<br />
mmwr/pdf/rr/rr5911.pdf.<br />
• Administer PPSV at least 8 weeks after the last dose of PCV to children<br />
aged 2 years or older with certain underlying medical conditions,<br />
including a cochlear implant. A single revaccination should be<br />
administered after 5 years to children with anatomic/functional asplenia or<br />
an immunocompromising condition.<br />
6. Hepatitis A (HepA) vaccine.<br />
• HepA vaccine is recommended for children older than 23 months who<br />
live in areas where vaccination programs target older children, who are at<br />
increased risk for infection, or for whom immunity against hepatitis A virus<br />
infection is desired. See MMWR 2006;55(No. RR-7), available at http://<br />
www.cdc.gov/mmwr/pdf/rr/rr5507.pdf.<br />
• Administer 2 doses at least 6 months apart to unvaccinated persons.<br />
7. Hepatitis B (HepB) vaccine.<br />
• Administer the 3-dose series to those not previously vaccinated.<br />
• For those with incomplete vaccination, follow the catch-up<br />
recommendations (Figure 3).<br />
• A 2-dose series (doses separated by at least 4 months) of adult<br />
formulation Recombivax HB is licensed for use in children aged 11<br />
through 15 years.<br />
8. Inactivated poliovirus vaccine (IPV).<br />
• The final dose in the series should be administered at least 6 months<br />
after the previous dose.<br />
• If both OPV and IPV were administered as part of a series, a total of 4<br />
doses should be administered, regardless of the child’s current age.<br />
• IPV is not routinely recommended for U.S. residents aged18 years or<br />
older.<br />
9. Measles, mumps, and rubella (MMR) vaccine.<br />
• The minimum interval between the 2 doses of MMR vaccine is 4 weeks.<br />
10. Varicella (VAR) vaccine.<br />
• For persons without evidence of immunity (see MMWR 2007;56[No. RR-<br />
4], available at http://www.cdc.gov/mmwr/pdf/rr/rr5604.pdf), administer 2<br />
doses if not previously vaccinated or the second dose if only 1 dose has<br />
been administered.<br />
• For persons aged 7 through 12 years, the recommended minimum interval<br />
between doses is 3 months. However, if the second dose was administered<br />
at least 4 weeks after the first dose, it can be accepted as valid.<br />
• For persons aged 13 years and older, the minimum interval between<br />
doses is 4 weeks.<br />
16.2.2 Immunization Schedule 7-18 years<br />
This schedule is approved by the Advisory Committee on Immunization Practices (http://www.cdc.gov/vaccines/recs/acip),<br />
the American Academy of Pediatrics (http://www.aap.org), and the American Academy of Family Physicians (http://www.aafp.org).<br />
Department of <strong>Health</strong> and Human Services • Centers for Disease Control and Prevention<br />
H EALTH PLANS<br />
www.cfhp.com<br />
141
16.2.3 Immunization Catch-up Schedule<br />
FIGURE 3. Catch-up immunization schedule for persons aged 4 months through 18 years who start late or who are more than 1 month behind —United States • 2012<br />
The figure below provides catch-up schedules and minimum intervals between doses for children whose vaccinations have been delayed. A vaccine series<br />
does not need to be restarted, regardless of the time that has elapsed between doses. Use the section appropriate for the child’s age. Always use this table in<br />
conjunction with the accompanying childhood and adolescent immunization schedules (Figures 1 and 2) and their respective footnotes.<br />
Vaccine<br />
Minimum Age<br />
for Dose 1<br />
Hepatitis B Birth 4 weeks<br />
Persons aged 4 months through 6 years<br />
Minimum Interval Between Doses<br />
Dose 1 to dose 2 Dose 2 to dose 3 Dose 3 to dose 4 Dose 4 to dose 5<br />
8 weeks<br />
and at least 16 weeks after first dose; minimum age for<br />
the final dose is 24 weeks<br />
Rotavirus 1 6 weeks 4 weeks 4 weeks 1<br />
Diphtheria, tetanus, pertussis 2 6 weeks 4 weeks 4 weeks 6 months 6 months 2<br />
Haemophilus influenzae<br />
type b 3<br />
Pneumococcal 4<br />
6 weeks<br />
6 weeks<br />
4 weeks<br />
if first dose administered at younger than age 12 months<br />
8 weeks (as final dose)<br />
if first dose administered at age 12–14 months<br />
No further doses needed<br />
if first dose administered at age 15 months or older<br />
4 weeks<br />
if first dose administered at younger than age 12 months<br />
8 weeks (as final dose for healthy children)<br />
if first dose administered at age 12 months or older or current<br />
age 24 through 59 months<br />
No further doses needed<br />
for healthy children if first dose administered at<br />
age 24 months or older<br />
4 weeks 3<br />
if current age is younger than 12 months<br />
8 weeks (as final dose) 3<br />
if current age is 12 months or older and first dose<br />
administered at younger than age 12 months and second<br />
dose administered at younger than 15 months<br />
No further doses needed<br />
if previous dose administered at age 15 months or older<br />
4 weeks<br />
if current age is younger than 12 months<br />
8 weeks (as final dose for healthy children)<br />
if current age is 12 months or older<br />
No further doses needed<br />
for healthy children if previous dose administered at<br />
age 24 months or older<br />
Inactivated poliovirus 5 6 weeks 4 weeks 4 weeks<br />
Meningococcal 6 9 months 8 weeks 6<br />
Measles, mumps, rubella 7 12 months 4 weeks<br />
Varicella 8 12 months 3 months<br />
Hepatitis A 12 months 6 months<br />
Tetanus, diphtheria/ tetanus,<br />
diphtheria, pertussis 9 7 years 9 4 weeks<br />
Persons aged 7 through 18 years<br />
4 weeks<br />
if first dose administered at younger than age 12 months<br />
6 months<br />
if first dose administered at 12 months or older<br />
Human papillomavirus 10 9 years Routine dosing intervals are recommended 10<br />
Hepatitis A 12 months 6 months<br />
Hepatitis B Birth 4 weeks<br />
8 weeks<br />
(and at least 16 weeks after first dose)<br />
8 weeks (as final dose)<br />
This dose only necessary<br />
for children aged 12<br />
months through 59 months<br />
who received 3 doses<br />
before age 12 months<br />
8 weeks (as final dose)<br />
This dose only necessary<br />
for children aged 12<br />
months through 59 months<br />
who received 3 doses<br />
before age 12 months or<br />
for children at high risk<br />
who received 3 doses at<br />
any age<br />
6 months 5<br />
minimum age 4 years for<br />
final dose<br />
6 months<br />
if first dose administered at<br />
younger than<br />
age 12 months<br />
Inactivated poliovirus 5 6 weeks 4 weeks 4 weeks 5 6 months 5<br />
Meningococcal 6 9 months 8 weeks 6<br />
Measles, mumps, rubella 7 12 months 4 weeks<br />
Varicella 8<br />
12 months<br />
3 months<br />
if person is younger than age 13 years<br />
4 weeks<br />
if person is aged 13 years or older<br />
1. Rotavirus (RV) vaccines (RV-1 [Rotarix] and RV-5 [Rota Teq]).<br />
• The maximum age for the first dose in the series is 14 weeks, 6 days; and<br />
8 months, 0 days for the final dose in the series. Vaccination should not be<br />
initiated for infants aged 15 weeks, 0 days or older.<br />
• If RV-1 was administered for the first and second doses, a third dose is not<br />
indicated.<br />
2. Diphtheria and tetanus toxoids and acellular pertussis (DTaP) vaccine.<br />
• The fifth dose is not necessary if the fourth dose was administered at age 4<br />
years or older.<br />
3. Haemophilus influenzae type b (Hib) conjugate vaccine.<br />
• Hib vaccine should be considered for unvaccinated persons aged 5 years or<br />
older who have sickle cell disease, leukemia, human immunodeficiency virus<br />
(HIV) infection, or anatomic/functional asplenia.<br />
• If the first 2 doses were PRP-OMP (PedvaxHIB or Comvax) and were<br />
administered at age 11 months or younger, the third (and final) dose should<br />
be administered at age 12 through 15 months and at least 8 weeks after the<br />
second dose.<br />
• If the first dose was administered at age 7 through 11 months, administer<br />
the second dose at least 4 weeks later and a final dose at age 12 through 15<br />
months.<br />
4. Pneumococcal vaccines. (Minimum age: 6 weeks for pneumococcal conjugate<br />
vaccine [PCV]; 2 years for pneumococcal polysaccharide vaccine [PPSV])<br />
• For children aged 24 through 71 months with underlying medical conditions,<br />
administer 1 dose of PCV if 3 doses of PCV were received previously, or<br />
administer 2 doses of PCV at least 8 weeks apart if fewer than 3 doses of<br />
PCV were received previously.<br />
• A single dose of PCV may be administered to certain children aged 6 through 18<br />
years with underlying medical conditions. See age-specific schedules for details.<br />
• Administer PPSV to children aged 2 years or older with certain underlying<br />
medical conditions. See MMWR 2010:59(No. RR-11), available at http://<br />
www.cdc.gov/mmwr/pdf/rr/rr5911.pdf.<br />
5. Inactivated poliovirus vaccine (IPV).<br />
• A fourth dose is not necessary if the third dose was administered at age 4<br />
years or older and at least 6 months after the previous dose.<br />
• In the first 6 months of life, minimum age and minimum intervals are only<br />
recommended if the person is at risk for imminent exposure to circulating<br />
poliovirus (i.e., travel to a polio-endemic region or during an outbreak).<br />
• IPV is not routinely recommended for U.S. residents aged 18 years or older.<br />
6. Meningococcal conjugate vaccines, quadrivalent (MCV4). (Minimum age:<br />
9 months for Menactra [MCV4-D]; 2 years for Menveo [MCV4-CRM])<br />
• See Figure 1 (“Recommended immunization schedule for persons aged 0<br />
through 6 years”) and Figure 2 (“Recommended immunization schedule for<br />
persons aged 7 through 18 years”) for further guidance.<br />
7. Measles, mumps, and rubella (MMR) vaccine.<br />
• Administer the second dose routinely at age 4 through 6 years.<br />
8. Varicella (VAR) vaccine.<br />
• Administer the second dose routinely at age 4 through 6 years. If the<br />
second dose was administered at least 4 weeks after the first dose, it can be<br />
accepted as valid.<br />
9. Tetanus and diphtheria toxoids (Td) and tetanus and diphtheria toxoids<br />
and acellular pertussis (Tdap) vaccines.<br />
• For children aged 7 through 10 years who are not fully immunized with the<br />
childhood DTaP vaccine series, Tdap vaccine should be substituted for<br />
a single dose of Td vaccine in the catch-up series; if additional doses are<br />
needed, use Td vaccine. For these children, an adolescent Tdap vaccine<br />
dose should not be given.<br />
• An inadvertent dose of DTaP vaccine administered to children aged 7<br />
through 10 years can count as part of the catch-up series. This dose can<br />
count as the adolescent Tdap dose, or the child can later receive a Tdap<br />
booster dose at age 11–12 years.<br />
10. Human papillomavirus (HPV) vaccines (HPV4 [Gardasil] and HPV2 [Cervarix]).<br />
• Administer the vaccine series to females (either HPV2 or HPV4) and males<br />
(HPV4) at age 13 through 18 years if patient is not previously vaccinated.<br />
• Use recommended routine dosing intervals for vaccine series catch-up; see Figure<br />
2 (“Recommended immunization schedule for persons aged 7 through 18 years”).<br />
<strong>Clinical</strong>ly significant adverse events that follow vaccination should be reported to the Vaccine Adverse Event Reporting System (VAERS) online (http://www.vaers.hhs.gov) or by<br />
telephone (800-822-7967). Suspected cases of vaccine-preventable diseases should be reported to the state or local health department. Additional information, including precautions and<br />
contraindications for vaccination, is available from CDC online (http://www.cdc.gov/vaccines) or by telephone (800-CDC-INFO [800-232-4636]).<br />
142 H EALTH PLANS<br />
www.cfhp.com
Comprehensive antepartum care is vital for a successful pregnancy outcome. CFHP recommends a program that involves a<br />
coordinated approach to medical care and psychosocial support that optimally begins before conception and extends through<br />
the postpartum period. <strong>Health</strong> care professionals are encouraged to integrate the concept of family-centered care into the<br />
antepartum care. Preconception care includes identifying those conditions that could affect a future pregnancy but may<br />
be ameliorated by early interven¬tion, such as hypertension, diabetes mellitus, or other metabolic and inherited disorders.<br />
Women who receive early and regular prenatal care are more likely to have healthier babies. The early diagnosis of pregnancy is<br />
important in establishing a management plan.<br />
CFHP recommends routine screening for pregnancy in all women of childbearing age. The Preventive <strong>Health</strong> & Disease<br />
Management staff conducts routine assessments of new health plan female members to evaluate health status, including<br />
possible pregnancy. When a pregnancy is identified, a follow-up contact is made to further assess member health and<br />
education needs. High-risk gestational mothers are referred to the <strong>Health</strong> Services Management department for case<br />
management assessment. <strong>Health</strong> assessment and educational information is shared with the health care provider on an ongoing<br />
basis.<br />
Antepartum surveillance begins with the initial prenatal visit, at which time the physician establishes a baseline obstetric<br />
database. The frequency of follow-up visits is determined by the individual needs of the woman and an assessment her risks.<br />
The frequency of scheduled prenatal visits should be sufficient to enable providers to accomplish the following activities:<br />
• Provide education, recommended screenings and interventions, as needed<br />
• Reassure the mother and family members<br />
• Assess fetal and mother well-being<br />
• Detect medical and psychosocial complications and institute indi¬cated interventions<br />
Women with uncomplicated pregnancies are generally examined according to the following schedule:<br />
• Every 4 weeks for the first 28 weeks of pregnancy,<br />
• Every 2-3 weeks until 36 weeks of gestation,<br />
• Weekly after 36 weeks, and<br />
• 4-6 weeks post delivery.<br />
17.1 Prenatal Care Guideline<br />
Women with medi¬cal or obstetric problems and younger adolescents may require closer surveillance. Appropriate intervals<br />
between scheduled visits are determined by the nature and severity of identified risk factors and medical problems. The<br />
following table outlines the recommended examinations and testing schedule established for routine obstetrical care by the<br />
American College of Obstetricians and Gynecologist (ACOG).<br />
Prenatal Care <strong>Guidelines</strong><br />
Established by the American College of Obstetricians and Gynecologist for Routine Obstetrical Care<br />
EXAMINATION / TESTS<br />
1. Complete history and physical exam<br />
(inc. past pregnancies, medical history)<br />
2. Initial lab work<br />
Hematocrit or hemoglobin<br />
Urinalysis<br />
ABO / Rh typing & antibody screening<br />
Rubella screening<br />
VDRL, Gonorrhea*, Chlamydia Screening*<br />
Cervical Cytology (as needed)<br />
Hepatitis B Surface Antigen<br />
HIV<br />
3. Follow-up Visits<br />
Weight<br />
Vital signs inc. blood pressure<br />
Urine protein and glucose<br />
Fundal height<br />
Edema check<br />
Signs and symptoms of preterm labor; or other risk factors<br />
Fetal heart tones<br />
Fetal movement<br />
SCHEDULE<br />
Initial visit or as early in the pregnancy as possible<br />
As early in pregnancy as possible<br />
Every routine visit<br />
H EALTH PLANS<br />
www.cfhp.com<br />
143
EXAMINATION / TESTS<br />
4. Follow-up Lab<br />
Triple screen<br />
Glucose Challenge test/H & H/Ab screen<br />
H & H/VDRL/Group B Strep<br />
5. Postpartum Care<br />
Interim history and physical exam<br />
Evaluation of weight<br />
Vital signs<br />
Cervical cytology (as needed)<br />
Family planning / contraceptive practices<br />
STD prevention<br />
Assessment for postpartum depression<br />
At 8-20 weeks gestation<br />
At 24-28 weeks gestation<br />
At 35-37 weeks gestation<br />
4-6 weeks after delivery<br />
SCHEDULE<br />
*optional<br />
Management of pregnancy requires establishing an estimated date of delivery. Problems such as intrauterine growth<br />
restriction, preterm labor, and postterm pregnancy are managed most effectively when an accurate estimated date of delivery<br />
is known. In addition, accurate gestational dating is important for the application and interpretation of certain antepartum<br />
tests (ie, maternal serum alpha-fetoprotein or assessment of fetal maturity). If there is a size-date discrepancy or if menstrual<br />
dates are uncer¬tain, an ultrasound examination is indicated for the purpose of dating. Such an examination is most accurate<br />
when performed before 20 weeks of gestation. Ultrasound results are considered to be consistent with menstrual dates if<br />
there is gestational age agreement to within 3 days by crown-rump length (CRL) measurement obtained at 6-10 weeks of<br />
gestation, within 5 days by CRL measurement obtained at 10-14 weeks of gestation, or within 7 days by the average of multiple<br />
measurements obtained at 14-20 weeks of gestation.<br />
Identification of risk factors is critical in order to minimize maternal and neonatal morbidity and mortality. In some instances,<br />
obstetric problems require a multidis¬ciplinary approach to antepartum care. Some conditions may require the involvement<br />
of a maternal-fetal medicine (MFM) subspecialist, geneticist, pediatrician, neonatologist, anesthesiologist, or other medical<br />
special¬ist in the evaluation, counseling, and care of the patient. <strong>Community</strong> <strong>First</strong> <strong>Health</strong> <strong>Plans</strong> actively outreaches to all<br />
identified program members to assess risk status and to assist both member and provider with managing risk factors once<br />
identified. Much of our program is based on member education surrounding how to identify risk factors associated with<br />
pregnancy. If you have a member who would benefit from this program, please make a referral by contacting CFHP.<br />
Approximately 4 – 6 weeks after delivery, the mother should visit her physician for a postpartum review and examination. The<br />
follow-up appointment interval may be modified according to the needs of the patient. A visit within 7-14 days of delivery may<br />
be advisable after a cesarean delivery or a complicated gestation.<br />
144 H EALTH PLANS<br />
www.cfhp.com
The following variables should be examined when cesarean deliveries are performed:<br />
• When cervical dilation was less than 4 cm<br />
• In the presence of intact membranes<br />
• Without appropriate use of oxytocin<br />
• After the patient has received an epidural when cervical dilation was less than 4 cm<br />
• After the patient has undergone elective induction of labor at less than 41 completed weeks of gestation<br />
• Without trial of labor for suspected macrosomia in nondiabetic women<br />
• For failed induction of labor for suspected macrosomia in nondiabetic women<br />
• For the sole indication of twin gestation<br />
• For the indication of termed fetuses with breech presentations, without offering eternal cephalic version<br />
Taken from the Evaluation of Cesarean Delivery, American College of Obstetricians and Gynecologists, pages 34-35, 2000<br />
ELECTIVE REPEAT CESAREAN SECTION GUIDELINES<br />
Before elective repeat cesarean delivery, the maturity of the fetus should be established. For patients with an indication for an<br />
elective repeat cesarean delivery, fetal maturity may be assumed if one of the following criteria is met:<br />
• Fetal heart tones have been documented for 20 weeks by nonelectronic fetoscope or for 30 weeks by Doppler ultrasound.<br />
• Thirty-six weeks have elapsed since positive results were obtained from a serum or urine human chorionic gonadotropin<br />
pregnancy test performed by a reliable laboratory.<br />
• Ultrasound measurement of the crown-rump length obtained at 6-11 weeks of gestation supports a current gestational age<br />
of 39 weeks or more.<br />
• <strong>Clinical</strong> history and physical and ultrasound examinations performed at 12-20 weeks of gestation support a current<br />
gestational age of 39 weeks or more.<br />
These criteria are not intended to preclude the use of menstrual dating. If any one criterion confirms gestational age<br />
assessment in a patient who has normal menstrual cycles and no immediate antecedent use of oral contraceptives, it is<br />
appropriate to schedule delivery at 39 weeks of gestation or later on the basis of menstrual dates.<br />
Taken from guidelines for Perinatal Care, Sixth Edition, American Academy of Pediatrics and American College of Obstetricians and Gynecologists, page 160<br />
October 2007<br />
17.2 Cesarian Section <strong>Guidelines</strong><br />
VAGINAL BIRTH AFTER CESAREAN DELIVERY GUIDELINES<br />
Despite extensive data regarding the risks and success rates of vaginal birth after cesarean delivery (VBAC), there is relatively<br />
little information regarding how labor should be conducted:<br />
• External cephalic version for breech presentation may be as successful for VBAC candidates as for women who have not<br />
undergone previous cesarean delivery.<br />
• The use of prostaglandins for cervical ripening or labor induction in VBAC candidates is discouraged. If induction of labor<br />
is necessary for a clear and compelling clinical induction, the potential increased risk of uterine rupture with the use of<br />
prostaglandins should be discussed with the patient and documented in the medical record.<br />
• Oxytocin may be used for both labor induction and augmentation with close patient monitoring in VBAC candidates.<br />
• Once labor has begun, the patient should be evaluated promptly. Most authorities recommend continuos electronic<br />
monitoring of both fetal heart rate and uterine contractions. The most common sign of uterine rupture is a nonreassuring<br />
fetal heart rate pattern with variable decelerations that may evolve into late decelerations, bradycardia, and undetectable<br />
fetal heart rate. Personnel familiar with the potential complications of VBAC should be vigilant for nonreassuring fetal<br />
heart rate patterns and inadequate progress in labor. Because uterine rupture may be catastrophic and evolve rapidly,<br />
VBAC should be attempted in institutions equipped to respond to emergencies with physicians immediately available to<br />
provide emergency care.<br />
• Epidural analgesia and anesthesia may safely be used during a trial of labor and planned VBAC. Assurance of adequate pain<br />
relief during labor may encourage more women to choose a trial of labor. Success rates for VBAC are similar in women<br />
who do and those who do not receive epidural analgesia, as well as in those women who receive other types of pain<br />
relief. Epidural analgesia rarely masks the signs or symptoms of uterine rupture. The anesthesia service should be notified<br />
whenever there is a patient attempting VBAC in active labor on the labor floor.<br />
Taken from guidelines for Perinatal Care, Sixth Edition, American Academy of Pediatrics and American College of Obstetricians and Gynecologists, pages 156-157,<br />
October 2007<br />
H EALTH PLANS<br />
www.cfhp.com<br />
145
17.3 OB/GYN Medical Record Documentation <strong>Guidelines</strong><br />
CFHP has established guidelines for medical record documentation. Individual medical records for each family member are<br />
to be maintained. The medical records must be handled and maintained in a confidential manner and must be organized in<br />
such a manner that all progress notes, diagnostic tests, reports, letters, discharge summaries and other pertinent medical<br />
information are readily accessible. In addition, each office should have a written policy in place to ensure that medical records<br />
are safeguarded against loss, destruction, or unauthorized use.<br />
CRITERIA<br />
REQUIREMENTS<br />
1. Patient Identification Each page of the medical record must include a unique identifier, which may include patient<br />
identification number, medical record number, first and last name.<br />
2. Personal Data Personal/biographical data including the age, sex, address, employer, home and work<br />
telephone numbers, marital status of the patient, and emergency contacts must be<br />
included in the medical record.<br />
3. Allergies Medication allergies and adverse reactions (including immunization reactions) should be<br />
prominently noted in the record. If the patient has no known allergies or history of adverse<br />
reactions, this should be appropriately noted in the record.<br />
4. Problem List For patients seen (3) or more times, a separate list of all the patient’s chronic/significant<br />
problems must be maintained. A chronic problem is defined as one that is of long duration,<br />
shows little change or is of slow progression.<br />
5. Medication List For patients seen (3) or more times, maintenance/ongoing medications should be listed<br />
on a medication sheet and updated as necessary with dosage changes and the date the<br />
change was made. A separate medication sheet is recommended but if a physician chooses<br />
to write out all current medications, at each visit this is acceptable. The medication list<br />
should include information/instruction to the member.<br />
6. Chart Legible Medical records must be legible to someone other than the writer. A record that is<br />
deemed illegible by the reviewer should be evaluated by a second person.<br />
7. Author Signature All entries in the medical record must be signed by the author/performing provider.<br />
8. Dated Entries Each and every entry must be accompanied by a date (month, day and year).<br />
9. Advance Directive (OB/PCPs) For medical records of Medicaid adults, 18 years and older, the medical record must<br />
document whether or not the individual has executed an advance directive. An advanced<br />
directive is a written instruction such as a living will or durable power of attorney for health<br />
care relating to the provision of health care when the individual is incapacitated.<br />
10. Past Medical History For patients seen three (3) or more times, a past medical history should be easily identified<br />
and should include serious accidents, operations, illnesses and psychosocial/behavioral<br />
conditions. For children and adolescents (18 years and younger), past medical history<br />
should relate to prenatal care, birth, operations, and childhood illnesses.<br />
11. Tobacco, Alcohol, & Other<br />
Substance Use<br />
For patients 12 years and older, assessment of tobacco, alcohol, and other substance use<br />
should be documented in the medical record.<br />
12. Chief Complaint Every visit should have a notation identifying the current problem (significant illnesses,<br />
medical and behavioral health conditions and health maintenance concerns).<br />
13. History And Physical<br />
Relevant To Chief Complaint<br />
14. Diagnosis/ Impression For<br />
Chief Complaint<br />
The history and physical records should reflect appropriate subjective and objective<br />
information pertinent to the patient’s presenting complaints.<br />
The diagnosis identified during each visit should be documented and should be consistent<br />
with findings. ICD-9 code(s) may be used but must include the written description of the<br />
diagnosis.<br />
15. Basic Teaching Provided The medical record should reflect that member is provided with basic teaching/instructions<br />
regarding physical and/or behavioral health condition.<br />
16. Appropriate Plan Of<br />
Treatment<br />
17. Appropriate Use Of<br />
Consultants<br />
18. Appropriate Studies<br />
Ordered<br />
Based on the chief complaint, physical exam findings and diagnosis, the treatment plan<br />
should be clearly documented.<br />
If a patient problem occurs which is outside the physician’s scope of practice, there must be<br />
a referral to an appropriate specialist.<br />
The laboratory and other studies ordered should be consistent with the treatment plan as<br />
related to the documented working diagnosis and should be documented at the time of the<br />
visit. Abnormal findings must have an explicit notation of follow-up plans.<br />
146 H EALTH PLANS<br />
www.cfhp.com
CRITERIA<br />
19. Unresolved Problems From<br />
Previous Visits Addressed<br />
REQUIREMENTS<br />
Documentation should reflect that the physician provides continuous evaluation of<br />
problems noted in previous visits.<br />
20. MD Review Of Studies There must be evidence that the physician has reviewed the results of diagnostic studies.<br />
Methods can vary, but often the physician will initial the lab report or mention it in the<br />
progress notes.<br />
21. Results Of Consultations When the patient is referred to another physician for consultation, there must be a copy<br />
of the results of the consult report and any associated diagnostic work-up in the medical<br />
record. Primary physician review of the consultation must be documented. Often the<br />
physician initials the consult report.<br />
22. Date Of Next Visit Encounter forms or notes should have a notation, when indicated, regarding followup<br />
care, calls, or visits. Specific time of return should be noted in weeks, months, or as<br />
needed.<br />
23. ER And Hospital Records Pertinent inpatient records must be maintained in the office medical record. These<br />
records may include but are not limited to the following: H&P, surgical procedure reports,<br />
Authorizations, ER reports and hospital discharge summaries. For pediatric patients seen<br />
since birth the L&D records, including the newborn assessment, should be in the medical<br />
record.<br />
24. Evidence That Patient Was<br />
Not Placed At Risk<br />
25. Evaluation for abuse<br />
/ neglect or other socio<br />
environmental factors<br />
(Medicaid)<br />
The record should reflect that the patient has not been placed at inappropriate risk by a<br />
diagnostic or therapeutic problem.<br />
The medical reocord should reflect evidence that the provider evaluates for signs/<br />
symptoms or behaviors associated with abuse / neglect or other significant<br />
socioenvironmental factors.<br />
26. Diagnosis Validation The record should reflect that the billing diagnosis is consistent with that of the chief<br />
complaint.<br />
27. Claims Validation The record should reflect the documented encounter is appropriate for the level of E/M<br />
services billed.<br />
PRENATAL CARE<br />
1. Comprehensive History There must be evidence on the initial OB visit that the patient has been questioned<br />
regarding: family, genetic and obstetric history; dietary history; risk factors for intrauterine<br />
growth retardation and low birth weight; prior genital hepatic lesions; psychosocial history;<br />
and behavioral health conditions.<br />
2. Complete Physical Exam There must be evidence on the first examination that a patient has a complete OB physical<br />
examination including a pelvic examination. Particular attention should be paid to the<br />
thyroid, breasts, lungs, heart, extremities and abdomen.<br />
INITIAL LAB WORK<br />
3. Hematocrit or Hemoglobin Hemoglobin and hematocrit measures should be performed as early as possible in the<br />
pregnancy.<br />
4. Urinalysis A urinalysis for bacteriuria should be performed as early in the pregnancy as possible.<br />
5. ABO/RH Typing & Antibody<br />
Screening<br />
Determination of blood type and Rh factor should be performed as early as possible in the<br />
pregnancy.<br />
6. Rubella Screening A rubella antibody titer should be performed as early in the pregnancy as possible for<br />
women lacking evidence of immunity (proof of vaccination after the first birthday or<br />
laboratory evidence of immunity).<br />
7. VDRL, Gonorrhea* &<br />
Chlamydia* Testing (* optional)<br />
8. Cervical Cytology (as<br />
needed)<br />
A serological test for syphilis (VDRL) and cultures for gonorrhea* and chlamydia* should be<br />
performed as early as possible in the pregnancy.<br />
A Papanicolaou (Pap) smear /Cervical Cytology should be performed as needed.<br />
9. Hepatitis B Surface Antigen Initial screening for Hepatitis B should be performed as early in the<br />
pregnancy as possible.<br />
H EALTH PLANS<br />
www.cfhp.com<br />
147
CRITERIA<br />
REQUIREMENTS<br />
10. HIV Screening HIV Status should be determined on first prenatal visit for high risk patients.<br />
FOLLOW-UP VISITS<br />
11. Vital Signs and Weight Vial signs, including blood pressure and weight, to be obtained at each visit.<br />
12. Urine Checks for Protein<br />
and Glucose<br />
Testing for urinary protein, glucose, and ketones should be done at each prenatal visit.<br />
13. Fundal Height Fundal height should be measured and recorded at each visit.<br />
14. Edema Check The patient should be checked for edema of the hands, face and lower extremities at each<br />
visit.<br />
15. Signs & symptoms of<br />
preterm labor; or other<br />
risk factors<br />
Signs and symptoms of preterm labor or other risk factors are assessed and/or counseled<br />
with the patient.<br />
16. Fetal Heart Tones FHTs can usually be heard by 10-12 postmenstrual weeks using a hand-held Doppler device<br />
and should be documented at each visit.<br />
17. Fetal Movement The first fetal movement is usually appreciated at 17 weeks in the average multipara and at<br />
18 weeks in the average primipara. Documentation of fetal activity should be documented<br />
at each visit.<br />
FOLLOW-UP LABS<br />
18. Triple Screen Maternal serum alpha-fetoprotein (AFP) should be obtained between 8-20 weeks gestation.<br />
19. Glucose Challenge /H&H/<br />
AbScreen<br />
Routine screening consists of determining blood sugar 1 hour after a 50gram oral glucose<br />
load. If the plasma blood sugar level is over 135-140mg/dL, a 3 hour glucose tolerance titer<br />
should be performed. This screening should occur at 24-28 weeks gestation.<br />
20. GroupB Strep/H&H/VDRL Cultures of the lower vaginal tract for group B streptococcus should be obtained between<br />
35-37 weeks gestation.<br />
POST PARTUM CARE<br />
21. Interim History & Physical<br />
Exam<br />
The first post partum visit should include a nutritional assessment and history of activities<br />
post delivery. Physical examination should include a breast examination and a complete<br />
rectovaginal evaluation.<br />
22. Evaluation of weight The patient’s weight should be recorded.<br />
23. Vital Signs The patient’s vital signs including blood pressure should be recorded.<br />
24. Cervical Cytology (as<br />
needed)<br />
25. Family Planning /<br />
Contraceptive Practices<br />
The cervix should be inspected and a Papanicolaou (Pap) smear obtained during the post<br />
partum visit. (as needed)<br />
Contraceptive and family planning methods should be discussed and the patient advised of<br />
the relative risks of conception.<br />
26. STD Prevention STD prevention should be discussed in patient physician interview as indicated.<br />
27. Postpartum Depression Assessment for postpartum depression should be recorded.<br />
GYN PREVENTIVE CARE<br />
28. Pelvic & Pap Smear A pelvic examination and pap smear should be performed every 2 years between ages 21-29<br />
and every 3 years between ages 30-64 after 3 conscective normal pap tests. Stop screening<br />
between ages 65-70, if no abnormal pap tests in 10 years.<br />
29. Mammogram A mammogram should be obtained every 1-2yrs for women 50 & older<br />
30. Rubella Antibody Titer A rubella antibody titer should be performed for women lacking evidence of immunity<br />
(proof of vaccination after the first birthday or laboratory evidence of immunity).<br />
31. Family Planning /<br />
Contraceptive Practices<br />
Contraceptive and family planning methods should be discussed and patient<br />
advised of the relative risks of conception.<br />
32. STD Prevention STD prevention should be discussed in patient/physician interview as indicated.<br />
148 H EALTH PLANS<br />
www.cfhp.com
CFHP<br />
OB/GYN SPECIALTY MEDICAL RECORD AUDIT TOOL<br />
Physician: Nurse Reviewer: Date of Review:<br />
Provider Number:<br />
Provider Type:<br />
A. Documentation ______<br />
B. Continuity of Care ______<br />
C. Preventive <strong>Health</strong> ______<br />
_________________________________________<br />
Plan -- Age--<br />
A. DOCUMENTATION<br />
1. Patient identification on each page<br />
2. Personal/Biographical information<br />
3. Allergies prominently noted<br />
4. Problem List (pts w/3 or more visits)<br />
5. Medication List (pts w/3 or more visits)<br />
6. Entries legible<br />
7. All entries contain author identification<br />
8. All entries are dated<br />
9. Advance Directives<br />
(Medicaid 18 & older – OB/PCPs)<br />
B. Continuity of Care<br />
10. Past medical history (pts w/3 or more visits)<br />
11. Tobacco, alcohol, & other substances use<br />
assessed (12 & older)<br />
12. Chief complaint noted<br />
13. History & exam pertinent to complaint<br />
14. Working diagnosis consistent with findings<br />
15. Basic teaching provided<br />
16. Appropriate plan of treatment<br />
17. Appropriate use of consults<br />
18. Appropriate studies ordered<br />
19. Unresolved problems addressed<br />
20. Physician review on studies<br />
21. Results of consultations are reviewed & filed<br />
22. Date of next visit/instructions for follow-up<br />
23. ER and Hospital reports/records<br />
24. Patient is not placed at inappropriate risk<br />
25. Evaluation of Abuse/neglect or other<br />
socio environmental factors (Medicaid)<br />
VALIDATIONS - √ for compliance (not scored)<br />
26. Diagnosis Validation<br />
27. Claims Validation<br />
1 2 3 4 5 6 7 8 9 10 Y N Y<br />
+<br />
N<br />
S<br />
C<br />
O<br />
R<br />
E<br />
Y<br />
Y+Nx100=<br />
% compliance<br />
17.4 OB/GYN Medical Record Review Tool<br />
P: Quality Management\Medical Record Review\SFY2012\Audit Tools Revised 12/04, 7/07, 1/10, 8/11<br />
H EALTH PLANS<br />
www.cfhp.com<br />
149
CFHP<br />
OB/GYN SPECIALTY MEDICAL RECORD AUDIT TOOL<br />
Physician: Nurse Reviewer: Date of Review:<br />
Provider Number:<br />
Provider Type:<br />
A. Documentation ______<br />
B. Continuity of Care ______<br />
C. Preventive <strong>Health</strong> ______<br />
1 2 3 4 5 6 7 8 9 10 Y N Y<br />
+<br />
N<br />
S<br />
C<br />
O<br />
R<br />
E<br />
Y<br />
Y+Nx100=<br />
% compliance<br />
_________________________________________<br />
Plan -- Age--<br />
A. DOCUMENTATION<br />
1. Patient identification on each page<br />
2. Personal/Biographical information<br />
3. Allergies prominently noted<br />
4. Problem List (pts w/3 or more visits)<br />
5. Medication List (pts w/3 or more visits)<br />
6. Entries legible<br />
7. All entries contain author identification<br />
8. All entries are dated<br />
9. Advance Directives<br />
(Medicaid 18 & older – OB/PCPs)<br />
B. Continuity of Care<br />
10. Past medical history (pts w/3 or more visits)<br />
11. Tobacco, alcohol, & other substances use<br />
assessed (12 & older)<br />
12. Chief complaint noted<br />
13. History & exam pertinent to complaint<br />
14. Working diagnosis consistent with findings<br />
15. Basic teaching provided<br />
16. Appropriate plan of treatment<br />
17. Appropriate use of consults<br />
18. Appropriate studies ordered<br />
19. Unresolved problems addressed<br />
20. Physician review on studies<br />
21. Results of consultations are reviewed & filed<br />
22. Date of next visit/instructions for follow-up<br />
23. ER and Hospital reports/records<br />
24. Patient is not placed at inappropriate risk<br />
25. Evaluation of Abuse/neglect or other<br />
socio environmental factors (Medicaid)<br />
VALIDATIONS - √ for compliance (not scored)<br />
26. Diagnosis Validation<br />
27. Claims Validation<br />
P: Quality Management\Medical Record Review\SFY2012\Audit Tools Revised 12/04, 7/07, 1/10, 8/11<br />
150 H EALTH PLANS<br />
www.cfhp.com
CFHP<br />
OB/GYN SPECIALTY MEDICAL RECORD AUDIT TOOL<br />
Physician: Nurse Reviewer: Date of Review:<br />
Provider Number:<br />
Provider Type:<br />
PREVENTIVE CARE<br />
_________________________________________<br />
Plan-- Age<br />
1 2 3 4 5 6 7 8 9 10 Y N Y<br />
+<br />
N<br />
S<br />
C<br />
O<br />
R<br />
E<br />
Y<br />
Y+Nx100=<br />
% compliance<br />
PRENATAL CARE<br />
1. Comprehensive history documented<br />
2. Complete physical exam documented<br />
INITIAL LAB WORK<br />
3. Hematocrit or hemoglobin<br />
4. Urinalysis<br />
5. ABO/Rh typing & antibody screening<br />
6. Rubella screening<br />
7. VDRL, Gonorrhea* & Chlamydia* Screening<br />
(* = Optional)<br />
8. Cervical Cytology (as needed)<br />
9. Hepatitis B Surface Antigen<br />
10. HIV screening<br />
FOLLOW-UP OB VISITS<br />
11. Vital signs & weight<br />
12. Urine check for protein and glucose<br />
13. Fundal height measurement<br />
14. Edema check<br />
15. Signs & symptoms of preterm labor; or other<br />
risk factors<br />
16. Fetal heart tones noted<br />
17. Fetal movement noted<br />
FOLLOW-UP LABS<br />
18. Triple screen (8-20) weeks)<br />
19. Glucose challenge/H&H/Ab screen<br />
(24-28 weeks)<br />
20. Group B Strep/ H&H/ VDRL (35-37 weeks)<br />
POST PARTUM CARE<br />
21. Interim history & physical exam<br />
22. Evaluation of weight<br />
23. Vital signs<br />
24. Cervical Cytology (as needed)<br />
25. Family planning/contraceptive practices<br />
26. Education provided on STD prevention<br />
27. Assessment for postpartum depression<br />
GYN Preventive Care<br />
28. Pelvic & Pap Smear<br />
29. Mammogram (Every 1-2yrs for women 50 & older)<br />
30. Rubella Antibody Titer (High risk)<br />
31. Family planning/Contraceptive Practices<br />
32. Education provided on STD prevention<br />
X = Patient qualifies for screening but timeframe has not yet expires<br />
P: Quality Management\Medical Record Review\SFY2012\Audit Tools Revised 12/04, 7/07, 1/10, 8/11<br />
H EALTH PLANS<br />
www.cfhp.com<br />
151
18.1 RSV Prophylaxis<br />
RESPIRATORY SYNCYTIAL VIRUS (RSV) PROPHYLAXIS GUIDELINES<br />
Respiratory syncytial virus (RSV) is a virus that causes serious respiratory illness in preterm infants, especially those who<br />
develop perinatal respiratory problems. RSV prophylaxis drugs palivizumab (immune globulin intramuscular) (RSV-IgIM)) and<br />
(immune globulin intravenous (RSV-IGIV) are covered benefits which require authorization for <strong>Community</strong> <strong>First</strong> eligible children<br />
including members enrolled in HMO, Medicaid and CHIP plans. The immunity imparted by these immune globulins is effective<br />
for approximately 28 days.<br />
Palivizumab RSV immune globulin for intramuscular use (RSV-IgM or Synagis) and RSV immune globulin for intravenous use<br />
(RSV-IGIV or Respigam) are appropriate for at-risk children age 0 through 34 months of age according to the AAP guidelines<br />
below.<br />
The dose of palivizumab is 15 mg/kg and is supplied in 50 or 100 mg vials and is administered intramuscularly. RSV-IGIV is<br />
administered intravenously at a dosage of 750 mg/kg (15mL/Kg). RSV prophylaxis should be given monthly starting at the<br />
beginning of the RSV season and stopping at the end of the season (October through April in Texas). Once a child qualifies for<br />
initiation of prophylaxis at the start of the RSV season, administration should continue throughout the season regardless of the<br />
point where a child reaches 6 or 12 months of age. Hospitalized infants determined to be at risk of severe RSV disease should<br />
receive RSV-IGIV or palivizumab 48 to 72 hours before discharge home from the hospital during the RSV season and then every<br />
28-30 days until the end of the season.<br />
AMERICAN ACADEMY OF PEDIATRICS GUIDELINES:<br />
• Infants born at 28 weeks gestation or earlier during RSV season, whenever that occurs during the first 12 months of life<br />
• Infants born at 29–32 weeks gestation if they are younger than 6 months of age at the start of the RSV season<br />
• Infants born at 32–35 weeks gestation who are younger than 3 months of age at the start of the RSV season or who are<br />
born during RSV season if they have at least one of the following 2 risk factors: 1) infant attends child care; 2) infant has a<br />
sibling younger than 5 years of age<br />
• Infants and children younger than 2 years with cyanotic or complicated congenital heart disease<br />
• Infants and children younger than 2 years who have been treated for chronic lung disease within 6 months of the start of<br />
the RSV season.<br />
• Infants born before 35 weeks of gestation who have either congenital abnormalities of the airway or neuromuscular<br />
disease that compromises handling of respiratory secretions<br />
NOTE: Palivizumab does not interfere with routine childhood vaccine administration. See AAP guidelines for specific<br />
exceptions to vaccine administration when RSV-IGIV is used.<br />
152 H EALTH PLANS<br />
www.cfhp.com
According to the National Institute of Child <strong>Health</strong> and Human Development; the percentage of children and teens that are<br />
overweight has more than doubled in the past 30 years. Today, about 17 percent of American children ages 2-19 are overweight.<br />
For children, overweight also increases their health risks. Type 2 diabetes was once rare in children—but now it accounts for 8<br />
to 45 percent of newly diagnosed diabetes cases in American children and teens. And, overweight children are more likely to<br />
become overweight or obese as adults.<br />
BMI is used as a screening tool to identify possible weight problems for children. CDC and the American Academy of Pediatrics<br />
(AAP) recommend the use of BMI to screen for overweight and obesity in children beginning at 2 years old. A child’s weight<br />
status is determined based on an age- and sex-specific percentile for BMI rather than by the BMI categories used for adults.<br />
Classifications of overweight and obesity for children and adolescents are age- and sex-specific because children’s body<br />
composition varies as they age and varies between boys and girls<br />
BMI-for-age weight status categories and the corresponding percentiles<br />
Weight Status Category<br />
Underweight<br />
<strong>Health</strong>y weight<br />
Overweight<br />
Obese<br />
Percentile Range<br />
Less than the 5th percentile<br />
5th percentile to less than the 85th percentile<br />
85th to less than the 95th percentile<br />
Equal to or greater than the 95th percentile<br />
The CFHP web site includes a BMI calculator for children; the link is located in the provider section and found associated with<br />
each a product(Commercial, CHIP, or Star Medicaid). Link to CFHP: http://www.cfhp.com/<strong>Health</strong>wellness/BMI.asp<br />
The calculator is also available on the Centers for Disease Control web site: http://apps.nccd.cdc.gov/dnpabmi/Calculator.aspx<br />
CFHP adopted the following recommendations of an expert committee convened by AMA, HRSA and the CDC for the<br />
assessment, treatment and prevention of child and adolescent overweight and obesity which was published 1/25/2007.<br />
19.1 Pediatric and Adolescent Overweight and Obesity<br />
H EALTH PLANS<br />
www.cfhp.com<br />
153
19.2 Assessment, Prevention and Treatment of Pediatric Obesity<br />
Appendix: Expert Committee Recommendations on the Assessment, Prevention, and Treatment of Child and Adolescent<br />
Overweight and Obesity<br />
January 25, 2007<br />
Assessment Recommendations<br />
1. The Expert Committee recommends that physicians and allied healthcare providers perform, at a minimum, a yearly<br />
assessment of weight status in all children, and that this assessment include calculation of height, weight (measured<br />
appropriately), and body mass index (BMI) for age and plotting of those measures on standard growth charts.<br />
2. With regard to classification, the Expert Committee recommends that:<br />
a.<br />
Individuals from the ages of 2 to 18 years, with a BMI ≥ 95th percentile for age and sex, or BMI exceeding 30 (whichever<br />
a.<br />
is smaller), should be considered obese.<br />
Individuals with BMI ≥ 85th percentile, but < 95th percentile for age and sex, should be considered overweight, and this<br />
term replaces “at risk of overweight.”<br />
3. The Expert Committee recommends use of the 99th percentile of BMI for age cut-offs (indicate by using a table with<br />
cutpoints for the 99th percentile BMI by age and gender) to allow for improved accessibility of the data in the clinical<br />
setting and for additional study.<br />
4. The Expert Committee recommends against routine clinical use of skinfold thickness in the assessment of obesity in<br />
children.<br />
5. The Expert Committee was unable to recommend the use of waist circumference for routine clinical use at the present time<br />
because of incomplete information and lack of specific guidance for clinical application.<br />
6. The Expert Committee recommends that qualitative assessment of dietary patterns of all pediatric patients be conducted,<br />
at a minimum, at each well child visit for anticipatory guidance, and that assessment include the following areas:<br />
a.<br />
Self-efficacy and readiness to change:<br />
b.<br />
Identification of the following specific dietary practices, which may be targets for change<br />
i. Frequency of eating outside the home at restaurants or fast food establishments<br />
ii. Excessive consumption of sweetened beverages<br />
iii. Consumption of excessive portion sizes for age<br />
c.<br />
Additional practices to be considered for evaluation during the qualitative dietary assessment include:<br />
i. Excessive consumption of 100% fruit juiceii)<br />
ii. Breakfast consumption (frequency and quality)<br />
iii. Excessive consumption of foods that are high in energy density<br />
iv. Low consumption of fruits and vegetables<br />
v. Meal frequency and snacking patterns (including quality)<br />
7. The Expert Committee recommends that assessment of levels of physical activity and sedentary behaviors should be<br />
performed in all pediatric patients at a minimum, at each well child visit for anticipatory guidance, and should include these<br />
general areas:<br />
a.<br />
Self-efficacy and readiness to change<br />
b.<br />
Environment and social support and barriers to physical activity<br />
c.<br />
Whether the child is meeting recommendations of 60 minutes of at least moderate physical activity per day<br />
d.<br />
Level of sedentary behavior, which should include hours of behavior such as television and/or DVD watching, playing<br />
video games, and using the computer, and comparison to a baseline of
.<br />
aminotransferase (AST) and alanine aminotransferase (ALT), fasting glucose<br />
iii. greater than the 95th percentile, even in the absence of risk factors: all of the tests listed under ii., plus blood urea<br />
nitrogen (BUN) and creatinine<br />
<strong>Guidelines</strong> for laboratory assessment and testing are also provided for more detailed evaluation, typically performed and<br />
interpreted by subspecialists (see Assessment Report and Table 9 in that report)<br />
TREATMENT RECOMMENDATIONS<br />
1. The Expert Committee recommends that all physicians and healthcare providers should address weight management and<br />
lifestyle issues with all patients regardless of presenting weight, at a minimum, each year.<br />
2. The Expert Committee recommends that all children between 2 and 18 years of age with BMI between the 5th and 84th<br />
percentile should follow the recommendations for prevention as outlined in the Prevention Report.<br />
3. The Expert Committee recommends that the treatment of overweight children be approached in a staged method based<br />
upon the child’s age, BMI, any related comorbidities, weight status of parents, and progress in treatment, and that the<br />
child’s primary caregivers/families be involved in the process.<br />
4. The Expert Committee recommends the following staged approach for children between the ages of 2 and 19 years and<br />
whose BMI is above the 85th percentile:<br />
STAGE 1. PREVENTION PLUS PROTOCOL<br />
These recommendations can be implemented by the primary care physician or allied healthcare provider who has some training<br />
in pediatric weight management/behavioral counseling.<br />
Stage 1 recommendations include:<br />
I. Dietary habits and physical activity:<br />
1. Five or more servings of fruits and vegetables per day<br />
2. Two or fewer hours of screen time per day, and no television in the room where the child sleeps<br />
3. One hour or more of daily physical activity<br />
4. No sugar-sweetened beverages<br />
II. Patients and families of the patient be counseled to facilitate these eating behaviors:<br />
1. Eating a daily breakfast<br />
2. Limiting meals outside of the home<br />
3. Family meals should happen at least 5-6 times per week<br />
4. Allowing the child to self-regulate his or her meals and avoiding overly restrictive behaviors<br />
III. Within this category, the goal should be weight maintenance with growth that results in a decreasing BMI as age increases.<br />
Monthly follow-up.<br />
IV. After 3-6 months, if no improvement in BMI/weight status has been noted, advancement to Stage 2 is indicated and based<br />
on patient/family readiness to change.<br />
STAGE 2. STRUCTURED WEIGHT MANAGEMENT PROTOCOL<br />
These recommendations can be implemented by a primary care physician or allied healthcare provider highly trained in weight<br />
management. Stage 2 recommendations include:<br />
I. Dietary and physical activity behaviors;<br />
1. Development of a plan for utilization of a balanced macronutrient diet emphasizing low amounts of energy-dense foods<br />
2. Increased structured daily meals and snacks<br />
3. Supervised active play of at least 60 minutes per day<br />
4. Screen time of 1 hour or less per day<br />
II. Increased monitoring (eg, screen time, physical activity, dietary intake, restaurant logs) by provider, patient and/or family<br />
within this category, goal should be weight maintenance that results in a decreasing BMI as age and height increases;<br />
however, weight loss should not exceed 1 lb/month in children aged 2-11 years, or an average of 2 lb/wk in older overweight/<br />
obese children and adolescents.<br />
III. If no improvement in BMI/weight after 3-6 months, patient should be advanced to Stage 3<br />
STAGE 3. COMPREHENSIVE MULTIDISCIPLINARY PROTOCOL<br />
At this level of intervention, the patient should optimally be referred to a multidisciplinary obesity care team.<br />
I. Eating and activity goals are the same as in Stage 2<br />
II. Activities within this category should also include:<br />
1. Structured behavioral modification program, including food and activity monitoring and development of short-term diet<br />
and physical activity goals<br />
2. Involvement of primary caregivers/families for behavioral modification in children under age 12 years and training of<br />
primary caregivers/families for all children<br />
H EALTH PLANS<br />
www.cfhp.com<br />
155
III. Within this category, goal should be weight maintenance or gradual weight loss until BMI less than 85th percentile and<br />
should not exceed 1 lb/month in children aged 2-5 years, or 2 lbs/wk in older obese children and adolescents.<br />
The Expert Committee recommends the following for children with BMI > 95th percentile, with significant comorbidities and<br />
who have not been successful with Stages 1-3 or children > 99th percentile who have shown no improvement under Stage 3<br />
(Comprehensive Multidisciplinary Intervention):<br />
STAGE 4. TERTIARY CARE PROTOCOL.<br />
Referral to pediatric tertiary weight management center with access to a multidisciplinary team with expertise in childhood<br />
obesity and which operates under a designed protocol.<br />
1. This protocol should include continued diet and activity counseling and the consideration of such additions as meal<br />
replacement, very-low-calorie diet, medication, and surgery.<br />
The Expert Committee recommends that the following weight loss targets should be considered when implementing the<br />
staged treatment plan:<br />
Age 2-5 Years<br />
85th-94th BMI<br />
Weight maintenance until BMI< 85th percentile or slowing of weight gain as indicated by downward deflection in BMI curve.<br />
≥ 95th<br />
Weight maintenance until BMI < 85th percentile; however if weight loss occurs<br />
with a healthy and adequate caloric diet it should not exceed 1 lb/month. If greater loss is noted, monitor for causes of excessive<br />
weight loss.<br />
BMI (>21 or 22)<br />
(Rare, very high) Gradual weight loss, not to exceed 1 lb/mo. If greater loss occurs, monitor for causes of excessive weight loss.<br />
Age 6-11 Years<br />
85th -94th BMI<br />
Weight maintenance until BMI< 85th percentile or slowing of weight gain as indicated by downward deflection in BMI curve.<br />
95th -98th BMI<br />
Weight maintenance until BMI< 85th or gradual weight loss of approximately 1 lb/month. If greater loss is noted, monitor for<br />
causes of excessive weight loss.<br />
≥99th BMI<br />
Weight loss not to exceed an average of 2 lb/wk. If greater loss is noted, monitor for causes of excessive weight loss.<br />
Age 12-18 Years<br />
85th – 94th BMI<br />
Weight maintenance until BMI< 85th percentile, or slowing of weight gain as indicated by downward deflection in BMI curve.<br />
95th -98th BMI<br />
Weight loss until BMI < 85th percentile--no more than an average of 2 lbs/wk. If greater loss is noted, monitor for causes of<br />
excessive weight loss.<br />
≥99th BMI<br />
Weight loss not to exceed an average of 2lb/wk. If greater loss is noted, monitor for causes of excessive weight loss.<br />
The Expert Committee recommends that in children aged 12-18 years, with BMI greater than or equal to the 99th percentile,<br />
primary care physicians and other allied healthcare providers may begin treatment with stages 1, 2, or 3 as indicated based on<br />
patient/family readiness to change.<br />
156 H EALTH PLANS<br />
www.cfhp.com
PREVENTION RECOMMENDATIONS<br />
1. The Expert Committee recommends that physicians and allied healthcare providers counsel the following:<br />
a.<br />
For children aged 2-18 years whose BMI is at or above the 5th percentile and no greater than the 84th percentile:<br />
i. Dietary Intake:<br />
1. Limiting consumption of sugar-sweetened beverages and encouraging consumption of diets with recommended<br />
quantities of fruits and vegetables.<br />
ii. Physical Activity:<br />
1. Limiting television and other screen time to 1 or 2 hours per day in children starting as young as age 5 years, as<br />
advised by the American Academy of Pediatrics and removing television and computer screens from children’s<br />
primary sleeping area.<br />
iii. Eating Behaviors:<br />
1. Eating breakfast daily.<br />
2. Limiting eating out at restaurants, particularly fast food restaurants.<br />
3. Encouraging family meals in which parents and children eat together.<br />
4. Limiting portion size.<br />
2. The Expert Committee recommends that physicians, allied healthcare professionals, and professional organizations<br />
advocate for:<br />
a. The federal government to increase physical activity at school through intervention programs as early as grade<br />
1 through the end of high school and college, and through creating school environments that support physical<br />
activity in general.<br />
b. Supporting efforts to preserve and enhance parks as areas for physical activity, informing local development<br />
initiatives regarding the inclusion of walking and bicycle paths, and promoting families’ use of local physical activity<br />
options by making information and suggestions about physical activity alternatives available in doctors’ offices.<br />
3. The Expert Committee recommends using the following techniques to aid physicians and allied healthcare providers who<br />
may wish to support obesity prevention in clinical, school, and community settings:<br />
a. Actively engaging families with parental obesity or maternal diabetes, because these children are at increased risk<br />
for developing obesity even if they currently have normal BMI.<br />
b. Encouraging an authoritative * parenting style in support of increased physical activity and reduced sedentary<br />
behaviour, providing tangible and motivational support for children.<br />
c. Discouraging a restrictive † parenting style regarding child eating.<br />
d. Encouraging parents to model healthy diets and portion sizes, physical activity, and limited television time<br />
e. Promoting physical activity at school and in child care settings (including after school programs), by asking children<br />
and parents about activity in these settings during routine office visits.<br />
4. The Expert Committee suggests that children of healthy weight participate in 60 minutes of moderate to vigorous physical<br />
activity daily.<br />
i. The 60 minutes can be accumulated throughout the day, as opposed to only single or long bouts.<br />
ii. Ideally, such activity should be enjoyable to the child<br />
iii. Whereas some health and psychological benefits may be attained by achieving the 60 minute goal, greater duration<br />
should yield increased benefit<br />
5. The Expert Committee also suggests counselling patients and families to perform these behaviors:<br />
i. Dietary Intake:<br />
1. Eating a diet rich in calcium<br />
2. Eating a diet high in fiber<br />
3. Eating a diet with balanced macronutrients (calories from fat, carbohydrate, and protein in proportions for age<br />
recommended by Dietary Reference Intakes)<br />
4. Encouragement, support, and maintenance of breastfeeding<br />
ii. Eating Behaviors:<br />
1. Limiting consumption of energy-dense foods.<br />
* Authoritative parents are both demanding and responsive. “They monitor and impart clear standards for their children’s conduct. They are assertive, but not<br />
intrusive and restrictive. Their disciplinary methods are supportive, rather than punitive. They want their children to be assertive as well as socially responsible,<br />
and self-regulated as well as cooperative” (Baumrind, 1991, p. 62).<br />
† Restrictive parenting (heavy monitoring and controlling of a child’s behavior)<br />
H EALTH PLANS<br />
www.cfhp.com<br />
157
19.3 Weight Management Algorithm for Oveweight Children & Adolescents<br />
D i a b e t e s t r e a t m e n t a l g o r i t h m s<br />
Weight Management Algorithm for<br />
publication # 45-12083<br />
obtain Accurate Height (Ht) & Weight (Wt)<br />
2<br />
Calculate Body Mass Index (BMI-see page 3 of 4)<br />
th (refer to gender-specific bMi chart on page 4 of 4)<br />
BMI = Wt in kg<br />
2<br />
reinforce <strong>Health</strong>y lifestyle, diet, and exercise;<br />
2<br />
2<br />
2 2 >95th%ile bMi for Age & Gender<br />
3<br />
sleep Apnea; pseudotumor cerebri; dyslipidemia (elevated ldl-c and/or tG; low Hdl-c); Htn;<br />
nAFld; Gerd; Wt-bearing Joint pain; pcos /Hyperandrogenism; An; psychological Adjustment disorders; t2dM (FpG≥126 mg/dl;<br />
post challenge pG ≥200 mg/dl)<br />
Assess for Risk Factors and/or Contributing Factors<br />
4 birth Wt; post Malignancy pt/Family not Motivated<br />
5 Offer Medically Supervised Wt<br />
educate patient and Family; Manage<br />
Management Intervention<br />
comorbidities and risk Factors;<br />
u reassess readiness periodically<br />
u Pubertal: = 10% body Wt loss<br />
pt/Family Motivated<br />
pt/Family Motivated<br />
85th%ile bMi with comorbidities<br />
Pre-pubertal: ≥age 7 = 1–2 lbs per Month Wt loss<br />
Education; Lifestyle Changes 2 ; Nutrition;<br />
Overweight 2<br />
treatment<br />
(Ht in m) 2<br />
pt/Family Motivated<br />
degree of Wt loss will depend on the severity of<br />
the comorbidity<br />
Increased Physical Activity; Behavior<br />
Modification; Nutrition/Family Counseling.<br />
Approved 04/28/05<br />
= Wt in lb x 703<br />
(Ht in inches) 2<br />
pt/Family not Motivated<br />
≥6 months<br />
Consider Obesity Pharmacologic Monotherapy as Adjunct to<br />
lifestyle changes if bMi ≥27 with comorbidities or if bMi ≥30<br />
Maintain <strong>Health</strong>y lifestyle, diet and exercise;<br />
reinforce education; Monitor Wt Weekly for life with<br />
periodic Follow-up by Hcp<br />
Consider Bariatric Surgery 8 for adolescents<br />
who meet criteria. (See page 2)<br />
Wt Loss<br />
Maintenance<br />
targets Maintained<br />
Targets Met<br />
Motivated & targets not Met<br />
≥6 months<br />
Appetite Suppressant<br />
Sibutramine 6<br />
contraindicated in: uncontrolled<br />
Htn; Glaucoma (narrow-angle);<br />
Arrhythmia; cvA; cvd; cHF;<br />
concurrent ssri; MAoi therapy;<br />
pregnancy; bulimia/Anorexia<br />
nervosa Hx<br />
Lipase Inhibitor Orlistat 7<br />
contraindicated in:<br />
chronic Malabsorption;<br />
cholestasis; orlistat<br />
Hypersensitivity; concurrent<br />
cyclosporin therapy; pregnancy<br />
1 of 4 – Weight Management Algorithm for overweight children and Adolescents – Approved 04/28/05 See disclaimer at www.tdctoolkit.org/algorithms_and_guidelines.asp<br />
158 H EALTH PLANS<br />
www.cfhp.com
2 to 20 years: Boys<br />
Body mass index-for-age percentiles<br />
Date Age Weight Stature BMI* Comments<br />
NAME<br />
RECORD #<br />
BMI<br />
27<br />
26<br />
25<br />
24<br />
23<br />
22<br />
21<br />
20<br />
19<br />
18<br />
17<br />
16<br />
15<br />
14<br />
13<br />
12<br />
kg/m 2 AGE (YEARS)<br />
28<br />
27<br />
26<br />
25<br />
24<br />
23<br />
22<br />
21<br />
20<br />
19<br />
18<br />
17<br />
16<br />
15<br />
14<br />
13<br />
12<br />
kg/m 2<br />
90<br />
85<br />
75<br />
50<br />
25<br />
10<br />
5<br />
2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20<br />
95<br />
BMI<br />
35<br />
34<br />
33<br />
32<br />
31<br />
30<br />
29<br />
19.4 CDC BMI for Age Percentiles<br />
Published May 30, 2000 (modified 10/16/00).<br />
SOURCE: Developed by the National Center for <strong>Health</strong> Statistics in collaboration with<br />
the National Center for Chronic Disease Prevention and <strong>Health</strong> Promotion (2000).<br />
http://www.cdc.gov/growthcharts<br />
H EALTH PLANS<br />
www.cfhp.com<br />
159
2 to 20 years: Girls<br />
Stature-for-age and Weight-for-age percentiles<br />
NAME<br />
RECORD #<br />
S<br />
T<br />
A<br />
T<br />
U<br />
R<br />
E<br />
W<br />
E<br />
I<br />
G<br />
H<br />
T<br />
Mother’s Stature<br />
in<br />
62<br />
60<br />
58<br />
56<br />
54<br />
52<br />
50<br />
48<br />
46<br />
44<br />
42<br />
40<br />
38<br />
36<br />
34<br />
32<br />
30<br />
80<br />
70<br />
60<br />
50<br />
40<br />
30<br />
lb<br />
Date<br />
160<br />
155<br />
150<br />
145<br />
140<br />
135<br />
130<br />
125<br />
120<br />
115<br />
110<br />
105<br />
100<br />
95<br />
90<br />
85<br />
80<br />
35<br />
30<br />
25<br />
20<br />
15<br />
Father’s Stature<br />
Age Weight Stature BMI*<br />
cm 3 4 5 6 7 8 9 10 11<br />
Published May 30, 2000 (modified 11/21/00).<br />
SOURCE: Developed by the National Center for <strong>Health</strong> Statistics in collaboration with<br />
the National Center for Chronic Disease Prevention and <strong>Health</strong> Promotion (2000).<br />
http://www.cdc.gov/growthcharts<br />
12 13 14 15 16 17 18 19<br />
AGE (YEARS)<br />
kg<br />
10<br />
AGE (YEARS)<br />
2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19<br />
95<br />
90<br />
75<br />
50<br />
25<br />
10<br />
5<br />
95<br />
90<br />
75<br />
50<br />
25<br />
10<br />
5<br />
20<br />
cm<br />
190<br />
185<br />
180<br />
175<br />
170<br />
165<br />
160<br />
155<br />
150<br />
105<br />
100<br />
95<br />
90<br />
85<br />
80<br />
75<br />
70<br />
65<br />
60<br />
55<br />
50<br />
45<br />
40<br />
35<br />
30<br />
25<br />
20<br />
15<br />
kg 10<br />
20<br />
in<br />
76<br />
74<br />
72<br />
70<br />
68<br />
66<br />
64<br />
62<br />
60<br />
230<br />
220<br />
210<br />
200<br />
190<br />
180<br />
170<br />
160<br />
150<br />
140<br />
130<br />
120<br />
110<br />
100<br />
90<br />
80<br />
70<br />
60<br />
50<br />
40<br />
30<br />
lb<br />
S<br />
T<br />
A<br />
T<br />
U<br />
R<br />
E<br />
W<br />
E<br />
I<br />
G<br />
H<br />
T<br />
160 H EALTH PLANS<br />
www.cfhp.com
AsthmaMatters is an initiative developed by CFHP to improve the health, well-being and productivity of our members with<br />
asthma. Through ongoing review and oversight of this comprehensive disease management program, <strong>Community</strong> <strong>First</strong> works<br />
to provide quality health promotion and education services, in collaboration with our members, providers and community<br />
organizations. A key element of the program is to promote the development of a strong collaborative relationship between<br />
our members and their primary care providers and the use of nationally accepted care standards for asthma, to help members<br />
achieve long term control of their disease, which will result in the appropriate utilization of health care services.<br />
The AsthmaMatters program targets members identified to have asthma, via pharmacy management records, claim and<br />
encounter utilization data, and information received via the completion of member health surveys.<br />
Routinely, utilization patterns are assessed and targeted intervention is implemented to coordinate health care delivery and<br />
measures to improve members’ clinical, humanistic and economic status. <strong>Clinical</strong> outcomes may include a decrease in the<br />
use of beta-agonists, an increase in use of asthma controlling medications and an increase in the number of outpatient visits.<br />
Humanistic outcomes may include an improvement in quality of life factors (increased productivity and activity without asthma<br />
episodes, decreased absences from work or school, sleeping through the night without asthma episodes), increased knowledge<br />
about the disease, and overall asthma control with a decrease in acute asthma episodes. Economic outcome measures include<br />
decreased hospital admissions and emergency room events and/or unscheduled visits.<br />
Upon identification of prospective members, steps are taken to assess asthma severity levels and implement appropriate<br />
education and outreach services for each member. Prospective AsthmaMatters members are sent an asthma health risk<br />
appraisal form. Key areas assessed include current symptoms, treatment protocols and perception of quality of life. Upon<br />
receipt of the survey, members are stratified into one of three risk categories: minimal, mild to moderate, and higher risk. For<br />
each risk category, health promotion outreach activities include:<br />
Asthma Disease Management<br />
Minimal Risk<br />
Mild to Moderate Risk<br />
Higher Risk<br />
Send education literature quarterly<br />
Send education literature quarterly<br />
Provide peak flow meter and OptiChamber kit<br />
Follow-up call / Recommend asthma class<br />
Send education literature quarterly<br />
Refer to Case Management for further evaluation<br />
Possible health assessment and education<br />
Asthma education is coordinated with existing community education programs, to promote utilization of services currently<br />
available. Members who are categorized in the mild to moderate risk category are mailed a roster of up-to-date classes<br />
available in the community. Follow-up calls are conducted for members who continue to accrue inappropriate utilization of the<br />
emergency room and/or hospitalization, to assess for possible barriers to care and compliance.<br />
Members who require intensive assessment and education are referred to asthma disease management education. Education<br />
is provided on an individualized basis, over several visits, to promote member control and knowledge about their disease. The<br />
home environment is assessed and recommendations are given to decrease the risk of an acute asthma episode.<br />
Our goal is to provide programs, which encourage our members to actively participate in their asthma management, in<br />
collaboration with their physician. As part of the initiative, the primary care physician receives a copy of the members’ health<br />
assessment tool, with a summary of the assigned risk status and educational outreach CFHP has initiated for each member.<br />
Information regarding home assessment and education is also sent to the primary care provider, for inclusion in the medical<br />
record. Provider’s whose patients are stratified as high-risk through utilization data, receive utilization and pharmacy profiles<br />
for inclusion in member’s medical record.<br />
H EALTH PLANS<br />
www.cfhp.com<br />
161
Diabetes in Control<br />
According to prevalence studies conducted across the nation, diabetes affects over 17.9 million Americans, 7.8 percent of the<br />
population, and is the sixth leading cause of death in the United States. Most of the morbidity and mortality of diabetes is due<br />
to complications associated with the disease. Despite the existence of significant advancements in the treatment of diabetes,<br />
studies reveal that many secondary preventive care measures and tests are not applied in the outpatient setting.<br />
CFHP developed a diabetes disease management program, Diabetes In Control, which is accessible to our entire membership,<br />
to promote a collaborative approach to diabetes self management. The goals of the program include identification of members<br />
with diabetes, increase awareness and understanding of diabetes, increase risk reduction behaviors, improve access to quality<br />
diabetes education and health care services, and to promote diabetes standards of care, in coordination with the Texas<br />
Diabetes Council’s Minimum Standards for Diabetes Care in Texas.<br />
Members are identified via pharmacy management records, claims and encounter utilization data with a primary diagnosis<br />
of the disease state being managed, diabetes 250xx, physician referral, case management/utilization management /health<br />
promotion/member services, referrals and information gathered through self-reported member disclosure via health<br />
assessments. Case Managers screen members for possible referrals to the current Diabetes In Control programs by reviewing<br />
claims histories.<br />
Members enrolled in the Diabetes in Control program, receive ongoing information on: controlling blood sugar; tips for talking<br />
to the doctor; routine diabetes screening tests; the member’s role in preventing complications; blood sugar testing and<br />
supplies; and self-management during an illness. Members are eligible to attend community-based diabetes education classes.<br />
Higher risk members are referred to one-on-one intensive education, which provides education on the importance of regular<br />
checkups; checking blood sugars at home; exercising regularly; following a meal plan; taking necessary medication; maintaining<br />
recommended weight; taking care of skin and feet; and management of their diabetes in conjunction with other current acute<br />
or chronic conditions. Because depression is a well-documented component of this chronic condition, potential behavioral<br />
health needs are taken into consideration and incorporated into the plan of care.<br />
<strong>Clinical</strong>, humanistic, and financial outcomes are tracked, reported and evaluated on a regular basis, with a formal evaluation<br />
completed annually.<br />
162 H EALTH PLANS<br />
www.cfhp.com
According to the Centers for Disease Control, in 2006 more than 351,974 babies (8.3%) are low birth weight (defined as less than<br />
2500 grams or 5.5 pounds), while 59,000 (1.4%) are very low birth weight (defined as less than 1500 grams or 3.3 pounds). More<br />
than 13% are preterm births.<br />
The percentage of women seeking and obtaining prenatal care during the first trimester has increased over the years. Many<br />
high-risk women, however, continue to experience difficulty in accessing early prenatal care. The San Antonio Metropolitan<br />
<strong>Health</strong> District, reports that in 2006, 14% of pregnant women in Bexar County received late or no prenatal care. This is of particular<br />
concern for the pregnant teen, as 6% of all live births in Bexar County in 2003 were to young women under the age of 20.<br />
Access to early prenatal care is a hallmark of quality health care. CFHP Services Staff outreach to 100% of newly enrolled members.<br />
Successful contact has increased from 35% in August 2000 to 65% in August 2008. Barriers to contact across the state include<br />
inaccurate telephone numbers and addresses. <strong>Community</strong> <strong>First</strong> remains committed to continual improvement in outreach efforts<br />
to the prenatal population.<br />
The <strong>Health</strong> Services Staff collaborate with health plan providers to offer comprehensive perinatal services, as we believe<br />
education is an important factor in changing behaviors and improving the overall health of our members. Outreach to pregnant<br />
members includes:<br />
• completion of a prenatal health risk assessment;<br />
• referral to educational or community resources, as needed;<br />
• education regarding the importance of early prenatal care;<br />
• assignment of a pediatrician prior to birth and newborn check-ups; and<br />
• education regarding the importance of the 6 week postpartum visit.<br />
CFHP is committed to addressing these issues at large, through our <strong>Health</strong>y Expectations prenatal program, because of the<br />
opportunity for a “win-win” situation. <strong>Health</strong> outcomes can be improved, at the same time that the high costs of perinatal care<br />
can be reduced. The <strong>Health</strong>y Expectations program utilizes two phases to outreach and educate prenatal members.<br />
An assessment program for identified pregnant women provides an opportunity to identify risk factors. Social and behavioral<br />
health education and referral are typical outcome strategies at the initial assessment phase. When completed, the risk tool<br />
allows clinical staff time to outreach to those at increased risk for complications. Those at lower risk are sent educational<br />
materials by mail and encouraged to attend community sponsored prenatal education classes. Pregnant members are routinely<br />
reassessed at 20-24 weeks gestation, to evaluate for changes in prenatal health.<br />
Prenatal Assessment and Education Program<br />
A high-risk component to the prenatal program allows clinical staff an avenue for conducting ongoing education and outreach<br />
to women at a higher risk for adverse pregnancy outcomes. This component of the program was initiated in November 1999,<br />
and is intended to provide education and assistance to our members who are at risk for experiencing pregnancy complications,<br />
especially premature labor. Registered nurses, who have specialized and have clinical experience in obstetric care nursing,<br />
provide education and assistance in coordination of necessary services.<br />
The phases of the <strong>Health</strong>y Expectations prenatal program provide numerous opportunities to assess member health, pregnancy<br />
status, to promote compliance with appropriate perinatal guidelines, and provide member education. Programs such as our<br />
<strong>Health</strong>y Expectations have been recognized by the American Association of <strong>Health</strong> <strong>Plans</strong> as best practices in case management for<br />
prenatal care. Academic research and experience by other health plans have demonstrated a decrease in the costs of newborn<br />
care, mostly due to the prevention of premature births.<br />
H EALTH PLANS<br />
www.cfhp.com<br />
163
12238 Silicon Drive, Ste. 100 • San Antonio, Texas 78249<br />
www.cfhp.com<br />
Member Services: 1-800-434-2347<br />
Servicios de Miembros: 1-800-434-2347