Guidelines for the management of community ... - Brit Thoracic
Guidelines for the management of community ... - Brit Thoracic
Guidelines for the management of community ... - Brit Thoracic
Create successful ePaper yourself
Turn your PDF publications into a flip-book with our unique Google optimized e-Paper software.
BTS guidelines<br />
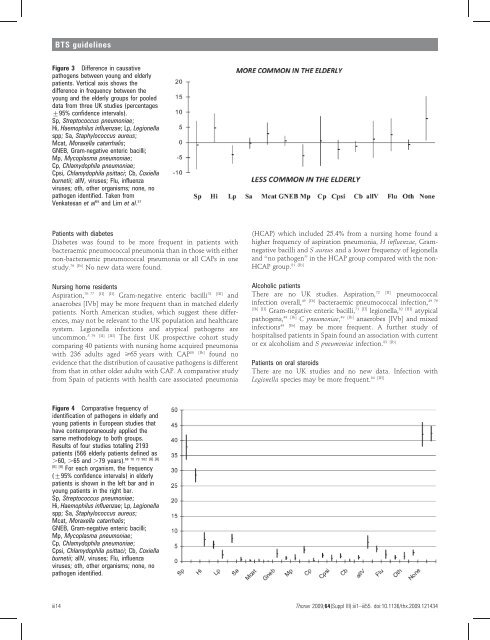
Figure 3 Difference in causative<br />
pathogens between young and elderly<br />
patients. Vertical axis shows <strong>the</strong><br />
difference in frequency between <strong>the</strong><br />
young and <strong>the</strong> elderly groups <strong>for</strong> pooled<br />
data from three UK studies (percentages<br />
¡95% confidence intervals).<br />
Sp, Streptococcus pneumoniae;<br />
Hi, Haemophilus influenzae; Lp, Legionella<br />
spp; Sa, Staphylococcus aureus;<br />
Mcat, Moraxella catarrhalis;<br />
GNEB, Gram-negative enteric bacilli;<br />
Mp, Mycoplasma pneumoniae;<br />
Cp, Chlamydophila pneumoniae;<br />
Cpsi, Chlamydophila psittaci; Cb, Coxiella<br />
burnetii; allV, viruses; Flu, influenza<br />
viruses; oth, o<strong>the</strong>r organisms; none, no<br />
pathogen identified. Taken from<br />
Venkatesan et al 69 and Lim et al. 37<br />
Patients with diabetes<br />
Diabetes was found to be more frequent in patients with<br />
bacteraemic pneumococcal pneumonia than in those with ei<strong>the</strong>r<br />
non-bacteraemic pneumococcal pneumonia or all CAPs in one<br />
study. 76 [Ib] No new data were found.<br />
Nursing home residents<br />
Aspiration, 76 77 [II] [II] Gram-negative enteric bacilli 78 [III] and<br />
anaerobes [IVb] may be more frequent than in matched elderly<br />
patients. North American studies, which suggest <strong>the</strong>se differences,<br />
may not be relevant to <strong>the</strong> UK population and healthcare<br />
system. Legionella infections and atypical pathogens are<br />
uncommon. 5 79 [II] [III] The first UK prospective cohort study<br />
comparing 40 patients with nursing home acquired pneumonia<br />
with 236 adults aged >65 years with CAP 80 [Ib] found no<br />
evidence that <strong>the</strong> distribution <strong>of</strong> causative pathogens is different<br />
from that in o<strong>the</strong>r older adults with CAP. A comparative study<br />
from Spain <strong>of</strong> patients with health care associated pneumonia<br />
(HCAP) which included 25.4% from a nursing home found a<br />
higher frequency <strong>of</strong> aspiration pneumonia, H influenzae, Gramnegative<br />
bacilli and S aureus and a lower frequency <strong>of</strong> legionella<br />
and ‘‘no pathogen’’ in <strong>the</strong> HCAP group compared with <strong>the</strong> non-<br />
81 [Ib]<br />
HCAP group.<br />
Alcoholic patients<br />
There are no UK studies. Aspiration, 72 [II] pneumococcal<br />
infection overall, 49 [Ib] 49 76<br />
bacteraemic pneumococcal infection,<br />
[Ib] [II]<br />
Gram-negative enteric bacilli, 71 [II] legionella, 82 [III] atypical<br />
pathogens, 49 [Ib] C pneumoniae, 49 [Ib] anaerobes [IVb] and mixed<br />
infections 49 [Ib] may be more frequent. A fur<strong>the</strong>r study <strong>of</strong><br />
hospitalised patients in Spain found an association with current<br />
83 [Ib]<br />
or ex alcoholism and S pneumoniae infection.<br />
Patients on oral steroids<br />
There are no UK studies and no new data. Infection with<br />
84 [III]<br />
Legionella species may be more frequent.<br />
Figure 4 Comparative frequency <strong>of</strong><br />
identification <strong>of</strong> pathogens in elderly and<br />
young patients in European studies that<br />
have contemporaneously applied <strong>the</strong><br />
same methodology to both groups.<br />
Results <strong>of</strong> four studies totalling 2193<br />
patients (566 elderly patients defined as<br />
69 70 73 502 [II] [II]<br />
.60, .65 and .79 years).<br />
[II] [II]<br />
For each organism, <strong>the</strong> frequency<br />
(¡95% confidence intervals) in elderly<br />
patients is shown in <strong>the</strong> left bar and in<br />
young patients in <strong>the</strong> right bar.<br />
Sp, Streptococcus pneumoniae;<br />
Hi, Haemophilus influenzae; Lp, Legionella<br />
spp; Sa, Staphylococcus aureus;<br />
Mcat, Moraxella catarrhalis;<br />
GNEB, Gram-negative enteric bacilli;<br />
Mp, Mycoplasma pneumoniae;<br />
Cp, Chlamydophila pneumoniae;<br />
Cpsi, Chlamydophila psittaci; Cb, Coxiella<br />
burnetii; allV, viruses; Flu, influenza<br />
viruses; oth, o<strong>the</strong>r organisms; none, no<br />
pathogen identified.<br />
iii14<br />
Thorax 2009;64(Suppl III):iii1–iii55. doi:10.1136/thx.2009.121434