Above elbow backslab - Living on the EDge
Above elbow backslab - Living on the EDge
Above elbow backslab - Living on the EDge
You also want an ePaper? Increase the reach of your titles
YUMPU automatically turns print PDFs into web optimized ePapers that Google loves.
Feature<br />
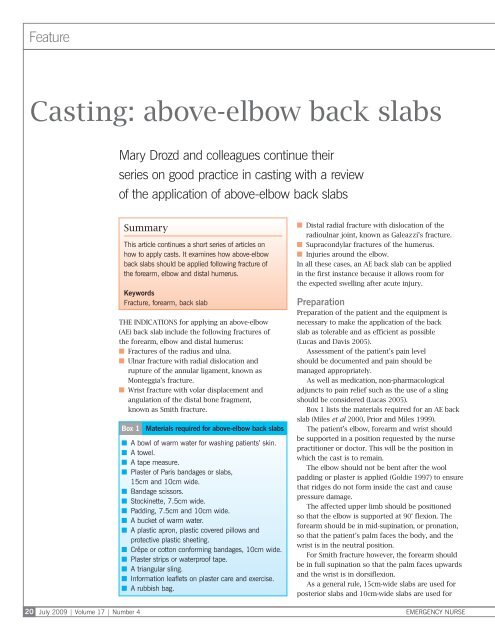
Casting: above-<str<strong>on</strong>g>elbow</str<strong>on</strong>g> back slabs<br />
Mary Drozd and colleagues c<strong>on</strong>tinue <strong>the</strong>ir<br />
series <strong>on</strong> good practice in casting with a review<br />
of <strong>the</strong> applicati<strong>on</strong> of above-<str<strong>on</strong>g>elbow</str<strong>on</strong>g> back slabs<br />
20<br />
July 2009 | Volume 17 | Number 4<br />
Summary<br />
This article c<strong>on</strong>tinues a short series of articles <strong>on</strong><br />
how to apply casts. It examines how above-<str<strong>on</strong>g>elbow</str<strong>on</strong>g><br />
back slabs should be applied following fracture of<br />
<strong>the</strong> forearm, <str<strong>on</strong>g>elbow</str<strong>on</strong>g> and distal humerus.<br />
Keywords<br />
Fracture, forearm, back slab<br />
The indicati<strong>on</strong>s for applying an above-<str<strong>on</strong>g>elbow</str<strong>on</strong>g><br />
(AE) back slab include <strong>the</strong> following fractures of<br />
<strong>the</strong> forearm, <str<strong>on</strong>g>elbow</str<strong>on</strong>g> and distal humerus:<br />
■■<br />
Fractures of <strong>the</strong> radius and ulna.<br />
■■<br />
Ulnar fracture with radial dislocati<strong>on</strong> and<br />
rupture of <strong>the</strong> annular ligament, known as<br />
M<strong>on</strong>teggia’s fracture.<br />
■■<br />
Wrist fracture with volar displacement and<br />
angulati<strong>on</strong> of <strong>the</strong> distal b<strong>on</strong>e fragment,<br />
known as Smith fracture.<br />
Box 1<br />
Materials required for above-<str<strong>on</strong>g>elbow</str<strong>on</strong>g> back slabs<br />
■■<br />
A bowl of warm water for washing patients’ skin.<br />
■■<br />
A towel.<br />
■■<br />
A tape measure.<br />
■■<br />
Plaster of Paris bandages or slabs,<br />
15cm and 10cm wide.<br />
■■<br />
Bandage scissors.<br />
■■<br />
Stockinette, 7.5cm wide.<br />
■■<br />
Padding, 7.5cm and 10cm wide.<br />
■■<br />
A bucket of warm water.<br />
■■<br />
A plastic apr<strong>on</strong>, plastic covered pillows and<br />
protective plastic sheeting.<br />
■■<br />
Crêpe or cott<strong>on</strong> c<strong>on</strong>forming bandages, 10cm wide.<br />
■■<br />
Plaster strips or waterproof tape.<br />
■■<br />
A triangular sling.<br />
■■<br />
Informati<strong>on</strong> leaflets <strong>on</strong> plaster care and exercise.<br />
■■<br />
A rubbish bag.<br />
■■<br />
Distal radial fracture with dislocati<strong>on</strong> of <strong>the</strong><br />
radioulnar joint, known as Galeazzi’s fracture.<br />
■■<br />
Suprac<strong>on</strong>dylar fractures of <strong>the</strong> humerus.<br />
■■<br />
Injuries around <strong>the</strong> <str<strong>on</strong>g>elbow</str<strong>on</strong>g>.<br />
In all <strong>the</strong>se cases, an AE back slab can be applied<br />
in <strong>the</strong> first instance because it allows room for<br />
<strong>the</strong> expected swelling after acute injury.<br />
Preparati<strong>on</strong><br />
Preparati<strong>on</strong> of <strong>the</strong> patient and <strong>the</strong> equipment is<br />
necessary to make <strong>the</strong> applicati<strong>on</strong> of <strong>the</strong> back<br />
slab as tolerable and as efficient as possible<br />
(Lucas and Davis 2005).<br />
Assessment of <strong>the</strong> patient’s pain level<br />
should be documented and pain should be<br />
managed appropriately.<br />
As well as medicati<strong>on</strong>, n<strong>on</strong>‐pharmacological<br />
adjuncts to pain relief such as <strong>the</strong> use of a sling<br />
should be c<strong>on</strong>sidered (Lucas 2005).<br />
Box 1 lists <strong>the</strong> materials required for an AE back<br />
slab (Miles et al 2000, Prior and Miles 1999).<br />
The patient’s <str<strong>on</strong>g>elbow</str<strong>on</strong>g>, forearm and wrist should<br />
be supported in a positi<strong>on</strong> requested by <strong>the</strong> nurse<br />
practiti<strong>on</strong>er or doctor. This will be <strong>the</strong> positi<strong>on</strong> in<br />
which <strong>the</strong> cast is to remain.<br />
The <str<strong>on</strong>g>elbow</str<strong>on</strong>g> should not be bent after <strong>the</strong> wool<br />
padding or plaster is applied (Goldie 1997) to ensure<br />
that ridges do not form inside <strong>the</strong> cast and cause<br />
pressure damage.<br />
The affected upper limb should be positi<strong>on</strong>ed<br />
so that <strong>the</strong> <str<strong>on</strong>g>elbow</str<strong>on</strong>g> is supported at 90° flexi<strong>on</strong>. The<br />
forearm should be in mid-supinati<strong>on</strong>, or pr<strong>on</strong>ati<strong>on</strong>,<br />
so that <strong>the</strong> patient’s palm faces <strong>the</strong> body, and <strong>the</strong><br />
wrist is in <strong>the</strong> neutral positi<strong>on</strong>.<br />
For Smith fracture however, <strong>the</strong> forearm should<br />
be in full supinati<strong>on</strong> so that <strong>the</strong> palm faces upwards<br />
and <strong>the</strong> wrist is in dorsiflexi<strong>on</strong>.<br />
As a general rule, 15cm-wide slabs are used for<br />
posterior slabs and 10cm-wide slabs are used for<br />
EMERGENCY NURSE
Feature<br />
medial and lateral slabs, although slab size depends<br />
<strong>on</strong> <strong>the</strong> size of <strong>the</strong> patient.<br />
Slabs should cover about two thirds of <strong>the</strong><br />
circumference of <strong>the</strong> patient’s forearm and should<br />
not meet <strong>on</strong> <strong>the</strong> anterior aspect.<br />
Method of applicati<strong>on</strong><br />
1. The length between <strong>the</strong> axilla and metacarpal<br />
heads is measured to assess <strong>the</strong> length of <strong>the</strong><br />
15cm-wide posterior slab (Figure 1).<br />
2. One 15cm-wide slab with about seven layers<br />
and two 10cm-wide, 25cm-l<strong>on</strong>g slabs, each with<br />
five layers, are prepared (Figure 2). Ei<strong>the</strong>r plaster<br />
slab or plaster bandages that are cut to size are<br />
used for all three slabs. The number of layers of<br />
<strong>the</strong> posterior slab depends <strong>on</strong> <strong>the</strong> patient. For<br />
example, a frail, older pers<strong>on</strong> needs fewer layers<br />
than a fit teenager, and would prefer <strong>the</strong> back<br />
slab to be as light as possible.<br />
3. Stockinette can be applied if <strong>the</strong> fracture is not<br />
being manipulated or if <strong>the</strong>re is no profound<br />
swelling. The stockinette must be <strong>the</strong> correct size<br />
and rolled gently <strong>on</strong>to <strong>the</strong> limb (Figure 3).<br />
4. Under-cast padding should be applied firmly<br />
and evenly in a single layer, but with extra layers<br />
applied around b<strong>on</strong>y prominences such as <strong>the</strong><br />
ulnar styloid, olecran<strong>on</strong> and medial epic<strong>on</strong>dyle.<br />
The use of padding allows for swelling and<br />
reduces fricti<strong>on</strong> between <strong>the</strong> cast and <strong>the</strong> skin<br />
(Lucas 2005). The padding should be placed 3cm<br />
bey<strong>on</strong>d <strong>the</strong> intended extent of <strong>the</strong> slab to protect<br />
<strong>the</strong> skin (Figure 4).<br />
5. The 15cm-wide plaster slab is folded and<br />
dipped into <strong>the</strong> bucket of water at a temperature<br />
of about 25°C. If <strong>the</strong> water is too cold, <strong>the</strong><br />
setting process is too slow; if it is too hot,<br />
<strong>the</strong> patient may be burned. After about four<br />
sec<strong>on</strong>ds, <strong>the</strong> slab is removed and excess water<br />
is squeezed out gently.<br />
6. The 15cm-wide plaster slab is applied to <strong>the</strong><br />
posterior aspect of <strong>the</strong> arm (Figure 5). A plastic<br />
apr<strong>on</strong>, plastic-covered pillows and protective<br />
plastic sheeting may be needed to ensure <strong>the</strong><br />
patient does not become wet.<br />
7. If <strong>the</strong> stockinette is being used, it should be<br />
folded over at each end of <strong>the</strong> posterior slab.<br />
8. The 10cm-wide slabs are soaked in a similar way<br />
to <strong>the</strong> 15cm-wide slab, and are applied al<strong>on</strong>g <strong>the</strong><br />
medial and lateral aspects of <strong>the</strong> <str<strong>on</strong>g>elbow</str<strong>on</strong>g> joint. The<br />
two slabs should not meet <strong>on</strong> <strong>the</strong> anterior aspect<br />
(Figure 6).<br />
9. Pre-soaked crêpe or cott<strong>on</strong> bandage is wrapped<br />
around <strong>the</strong> slabs and secured with plaster strips<br />
<strong>on</strong> <strong>the</strong> plaster slab <strong>on</strong>ly (Figure 7). Pre-soaking<br />
ensures <strong>the</strong> bandage does not shrink, stick <strong>on</strong>to<br />
<strong>the</strong> wet plaster and tighten around <strong>the</strong> limb.<br />
It can also ensure that <strong>the</strong> bandage is easy to<br />
remove <strong>on</strong> <strong>the</strong> patient’s return to clinic.<br />
Figure 1<br />
The length between <strong>the</strong> axilla and<br />
metacarpel heads is measured<br />
Figure 2<br />
One 15cm-wide slab and two 10cm-wide<br />
slabs are prepared<br />
Figure 3 Stockinette can be applied Figure 4 Under-cast padding is applied<br />
Neil O’C<strong>on</strong>nor<br />
EMERGENCY NURSE July 2009 | Volume 17 | Number 4 21
Feature<br />
Figure 5<br />
The 15cm-wide slab is applied to <strong>the</strong><br />
posterior aspect of <strong>the</strong> arm<br />
Figure 6<br />
The 10cm-wide slabs are applied al<strong>on</strong>g<br />
<strong>the</strong> medial and lateral aspects of <strong>the</strong> <str<strong>on</strong>g>elbow</str<strong>on</strong>g><br />
Figure 7<br />
Pre-soaked crepe or cott<strong>on</strong> bandage is<br />
applied and secured with plaster strips<br />
Figure 8<br />
A triangular sling is applied<br />
10. A triangular sling is applied (Figure 8).<br />
11. Patients are given verbal and written advice<br />
<strong>on</strong> plaster care, and <strong>on</strong> hand, shoulder and<br />
finger exercises that can prevent joints from<br />
stiffening and weakening. They are asked to<br />
sign for <strong>the</strong> written advice and to indicate<br />
that <strong>the</strong>y have received and understood <strong>the</strong><br />
verbal advice. The questi<strong>on</strong>ing of patients<br />
about this advice should elicit <strong>the</strong>ir levels<br />
of understanding.<br />
12. Unused plaster slab, padding or bandage is<br />
thrown away in <strong>the</strong> rubbish bag.<br />
Assessment and advice<br />
Signs of vascular or neurological damage should<br />
always be checked for, both before and after<br />
back slabs are applied, by observati<strong>on</strong> of <strong>the</strong><br />
colour, movement, sensati<strong>on</strong> and warmth of<br />
<strong>the</strong> limb distal to <strong>the</strong> injury (J<strong>on</strong>es 2003, Judge<br />
2007). This ensures that <strong>the</strong> applicati<strong>on</strong> has not<br />
compromised <strong>the</strong> limb.<br />
References<br />
Suprac<strong>on</strong>dylar fractures of <strong>the</strong> humerus, for<br />
example, can injure <strong>the</strong> brachial artery so radial<br />
pulse must be checked carefully. These serial<br />
assessments of vascular and neurovascular status<br />
must be documented in <strong>the</strong> patient’s notes (Be<strong>the</strong>l<br />
2008, Nursing and Midwifery Council 2002).<br />
Finally, a fracture clinic appointment should be<br />
arranged for follow-up treatment.<br />
Implicati<strong>on</strong>s for practice<br />
To undertake above-<str<strong>on</strong>g>elbow</str<strong>on</strong>g> back slab casting,<br />
practiti<strong>on</strong>ers must be trained, competent and<br />
possess <strong>the</strong> underpinning knowledge. They must<br />
understand <strong>the</strong> relevant anatomy, injuries and<br />
complicati<strong>on</strong>s that may follow applicati<strong>on</strong> of a cast.<br />
Fur<strong>the</strong>r reading<br />
In September’s Emergency Nurse, <strong>the</strong> authors will<br />
look at below-<str<strong>on</strong>g>elbow</str<strong>on</strong>g> back slab casting.<br />
Mary Drozd is a senior<br />
lecturer at <strong>the</strong> School<br />
of Health, University<br />
of Wolverhampt<strong>on</strong>,<br />
and an advanced nurse<br />
practiti<strong>on</strong>er in trauma<br />
and orthopaedics at<br />
<strong>the</strong> Dudley Group<br />
of Hospitals<br />
NHS Foundati<strong>on</strong> Trust<br />
Sue Miles is a nati<strong>on</strong>al<br />
casting training advisor<br />
at <strong>the</strong> British Orthopaedic<br />
Associati<strong>on</strong><br />
Jenny Davies is a<br />
senior sister in <strong>the</strong><br />
surgical and trauma and<br />
orthopaedic outpatient<br />
department and casting<br />
service at Russells Hall<br />
Hospital, <strong>the</strong> Dudley<br />
Group of Hospitals<br />
NHS Foundati<strong>on</strong> Trust<br />
Be<strong>the</strong>l J (2008) Paediatric Minor Emergencies.<br />
M&K Publishing, Keswick.<br />
Goldie BS (1997) Orthopaedic Diagnosis and<br />
Management: A guide to <strong>the</strong> care of orthopaedic<br />
patients. Sec<strong>on</strong>d editi<strong>on</strong>. Isis Medical<br />
Medic, L<strong>on</strong>d<strong>on</strong><br />
J<strong>on</strong>es G (2003) Emergency care of <strong>the</strong><br />
pers<strong>on</strong> with minor injury and minor<br />
illness. In J<strong>on</strong>es G, Endacott R, Crouch R<br />
(Eds) Emergency Nursing Care: Principles and<br />
practice. Greenwich Medical Media, L<strong>on</strong>d<strong>on</strong>.<br />
Judge NL (2007) Neurovascular assessment.<br />
Nursing Standard. 21, 45, 39-43.<br />
Lucas B (2005) Care of patients with upper<br />
limb injuries and c<strong>on</strong>diti<strong>on</strong>s. In Kneale J,<br />
Davis P (Eds) Orthopaedic and Trauma Nursing.<br />
Sec<strong>on</strong>d editi<strong>on</strong>. Churchill <str<strong>on</strong>g>Living</str<strong>on</strong>g>st<strong>on</strong>e, L<strong>on</strong>d<strong>on</strong>.<br />
Lucas B, Davis P (2005) Why restricting<br />
movement is important. In Kneale J, Davis P<br />
(Eds) Orthopaedic and Trauma Nursing.<br />
Sec<strong>on</strong>d editi<strong>on</strong>. Churchill <str<strong>on</strong>g>Living</str<strong>on</strong>g>st<strong>on</strong>e, L<strong>on</strong>d<strong>on</strong>.<br />
Miles S, Burden JW, Prior M et al (2000)<br />
A Practical to Casting. BSN Medical, Hull.<br />
Nursing and Midwifery Council (2002)<br />
Guidelines for Records and Record Keeping.<br />
NMC, L<strong>on</strong>d<strong>on</strong>.<br />
Prior M, Miles S (1999) Principles of casting.<br />
Journal of Orthopaedic Nursing. 3, 3, 162-170.<br />
22<br />
July 2009 | Volume 17 | Number 4<br />
EMERGENCY NURSE