Journal_1_2014_final_WEB
Journal_1_2014_final_WEB
Journal_1_2014_final_WEB
Create successful ePaper yourself
Turn your PDF publications into a flip-book with our unique Google optimized e-Paper software.
30<br />
25<br />
20<br />
15<br />
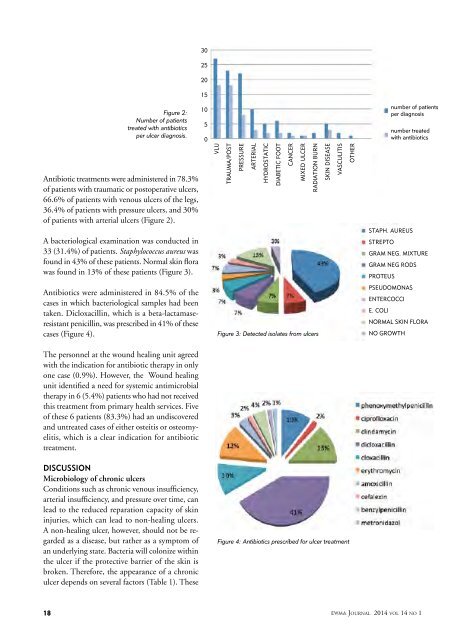
Figure 2:<br />
Number of patients<br />
treated with antibiotics<br />
per ulcer diagnosis.<br />
10<br />
5<br />
0<br />
number of patients<br />
per diagnosis<br />
number treated<br />
with antibiotics<br />
Antibiotic treatments were administered in 78.3%<br />
of patients with traumatic or postoperative ulcers,<br />
66.6% of patients with venous ulcers of the legs,<br />
36.4% of patients with pressure ulcers, and 30%<br />
of patients with arterial ulcers (Figure 2).<br />
A bacteriological examination was conducted in<br />
33 (31.4%) of patients. Staphylococcus aureus was<br />
found in 43% of these patients. Normal skin flora<br />
was found in 13% of these patients (Figure 3).<br />
VLU<br />
TRAUMA / POST<br />
PRESSURE<br />
ARTERIAL<br />
HYDROSTATIC<br />
DIABETIC FOOT<br />
CANCER<br />
MIXED ULCER<br />
RADIATION BURN<br />
SKIN DISEASE<br />
VASCULITIS<br />
OTHER<br />
STAPH. AUREUS<br />
STREPTO<br />
GRAM NEG. MIXTURE<br />
GRAM NEG RODS<br />
PROTEUS<br />
Antibiotics were administered in 84.5% of the<br />
cases in which bacteriological samples had been<br />
taken. Dicloxacillin, which is a beta-lactamaseresistant<br />
penicillin, was prescribed in 41% of these<br />
cases (Figure 4).<br />
Figure 3: Detected isolates from ulcers<br />
PSEUDOMONAS<br />
ENTERCOCCI<br />
E. COLI<br />
NORMAL SKIN FLORA<br />
NO GROWTH<br />
The personnel at the wound healing unit agreed<br />
with the indication for antibiotic therapy in only<br />
one case (0.9%). However, the Wound healing<br />
unit identified a need for systemic antimicrobial<br />
therapy in 6 (5.4%) patients who had not received<br />
this treatment from primary health services. Five<br />
of these 6 patients (83.3%) had an undiscovered<br />
and untreated cases of either osteitis or osteomyelitis,<br />
which is a clear indication for antibiotic<br />
treatment.<br />
Discussion<br />
Microbiology of chronic ulcers<br />
Conditions such as chronic venous insufficiency,<br />
arterial insufficiency, and pressure over time, can<br />
lead to the reduced reparation capacity of skin<br />
injuries, which can lead to non-healing ulcers.<br />
A non-healing ulcer, however, should not be regarded<br />
as a disease, but rather as a symptom of<br />
an underlying state. Bacteria will colonize within<br />
the ulcer if the protective barrier of the skin is<br />
broken. Therefore, the appearance of a chronic<br />
ulcer depends on several factors (Table 1). These<br />
Figure 4: Antibiotics prescribed for ulcer treatment<br />
18<br />
EWMA <strong>Journal</strong> <strong>2014</strong> vol 14 no 1