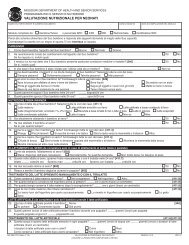
category 4 a - oasis data set forms - Missouri Department of Health ...
category 4 a - oasis data set forms - Missouri Department of Health ...
category 4 a - oasis data set forms - Missouri Department of Health ...
You also want an ePaper? Increase the reach of your titles
YUMPU automatically turns print PDFs into web optimized ePapers that Google loves.
Q118. [Q&A RETIRED 09/09; Duplicative <strong>of</strong> OASIS-C Guidance Manual]<br />
[Q&A ADDED 06/05; M number updated 09/09; Previously CMS OCCB 03/05 Q&A Q<br />
#5]<br />
Q119. M1610. A patient is determined to be incontinent <strong>of</strong> urine at SOC. After<br />
implementing clinical interventions (e.g., Kegel exercises, bi<strong>of</strong>eedback, and<br />
medication therapy) the episodes <strong>of</strong> incontinence stop. At the time <strong>of</strong> discharge,<br />
the patient has not experienced incontinence since the establishment <strong>of</strong> the<br />
incontinence program. At discharge, can the patient be considered continent <strong>of</strong><br />
urine for scoring <strong>of</strong> M1610, to reflect improvement in status?<br />
A119. Assuming that there has been ongoing assessment <strong>of</strong> the patient's response to<br />
the incontinence program (implied in the question), this patient would be assessed as<br />
continent <strong>of</strong> urine. Therefore Response 0, no incontinence or catheter, is an appropriate<br />
response to M1610.<br />
Timed-voiding was not specifically mentioned as an intervention utilized to defer<br />
incontinence. If, at discharge, the patient was dependent on a timed-voiding program to<br />
defer incontinence, the appropriate response to M1610 would be 1 (patient is<br />
incontinent), followed by response 0 to M1615 (timed-voiding defers incontinence).<br />
[Q&A ADDED 08/07; Previously CMS OCCB 05/07 Q&A #23]<br />
Q119.1. M1610. How long would a patient need to be continent <strong>of</strong> urine in order to<br />
qualify as being continent?<br />
A119.1. Utilize clinical judgment and current clinical guidelines and assessment findings<br />
to determine if the cause <strong>of</strong> the incontinence has been resolved, resulting in a patient no<br />
longer being incontinent <strong>of</strong> urine. There are no specific time frames that apply to all<br />
patients in all situations.<br />
[Q&A ADDED & EDITED 09/09; Previously CMS OCCB 04/08 Q&A #11]<br />
Q119.2. M1610. How should we answer M1610 for a patient with a nephrostomy<br />
tube? Can we interpret M1610 to mean if the urinary diversion is pouched with an<br />
ostomy appliance it is not a catheter but if it is accessed with a tube or catheter<br />
(external or otherwise) then the patient has a catheter? What about the patients<br />
with continent urinary diversions? They have a stoma but are accessing<br />
with intermittent catheterizations. Would they be reported as having a catheter on<br />
M1620?<br />
A119.2. When a patient has urinary diversion, with or without a stoma that is pouched for<br />
drainage the appropriate M1620 response would be "0-No incontinence or catheter".<br />
The appropriate response for a patient with urinary diversion, with or without a stoma,<br />
that has a catheter or "tube" for urinary drainage would be "2 -Patient requires a urinary<br />
catheter (i.e., external, indwelling, intermittent, suprapubic)." A patient that requires<br />
intermittent catheterization would be represented by Response 2, even if they have<br />
continent urinary diversions.<br />
[Q&A EDITED 09/09]<br />
Q120. M1615. How should I respond to M1615, When does Urinary Incontinence<br />
Occur, for the patient with an ureterostomy?<br />
Category 4 – OASIS Data Set – Forms and Items 09/09