2017 HCHB_digital
Create successful ePaper yourself
Turn your PDF publications into a flip-book with our unique Google optimized e-Paper software.
Fungal Nail Infections (Onychomycosis)<br />
Fungal nail infections (also known as onychomycosis or Tinea Unguium) account<br />
for 15%–40% of all nail diseases. Prevalence increases with age and the<br />
condition affects almost 20% of people older than 60 and over 50% of people<br />
in their seventies.<br />
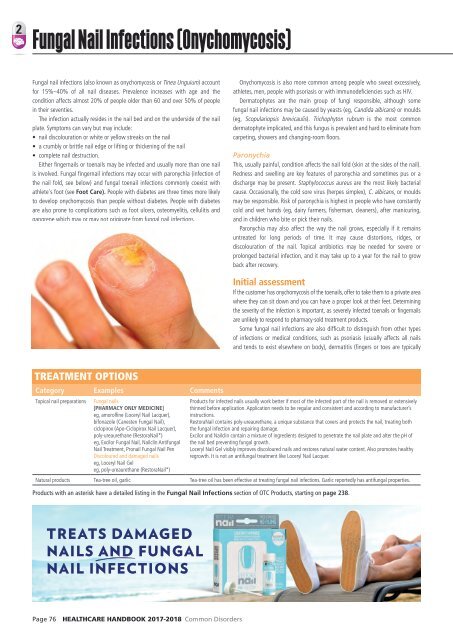
The infection actually resides in the nail bed and on the underside of the nail<br />
plate. Symptoms can vary but may include:<br />
• nail discolouration or white or yellow streaks on the nail<br />
• a crumbly or brittle nail edge or lifting or thickening of the nail<br />
• complete nail destruction.<br />
Either fingernails or toenails may be infected and usually more than one nail<br />
is involved. Fungal fingernail infections may occur with paronychia (infection of<br />
the nail fold, see below) and fungal toenail infections commonly coexist with<br />
athlete's foot (see Foot Care). People with diabetes are three times more likely<br />
to develop onychomycosis than people without diabetes. People with diabetes<br />
are also prone to complications such as foot ulcers, osteomyelitis, cellulitis and<br />
gangrene which may or may not originate from fungal nail infections.<br />
Onychomycosis is also more common among people who sweat excessively,<br />
athletes, men, people with psoriasis or with immunodeficiencies such as HIV.<br />
Dermatophytes are the main group of fungi responsible, although some<br />
fungal nail infections may be caused by yeasts (eg, Candida albicans) or moulds<br />
(eg, Scopulariopsis brevicaulis). Trichophyton rubrum is the most common<br />
dermatophyte implicated, and this fungus is prevalent and hard to eliminate from<br />
carpeting, showers and changing-room floors.<br />
Paronychia<br />
This, usually painful, condition affects the nail fold (skin at the sides of the nail).<br />
Redness and swelling are key features of paronychia and sometimes pus or a<br />
discharge may be present. Staphylococcus aureus are the most likely bacterial<br />
cause. Occasionally, the cold sore virus (herpes simplex), C. albicans, or moulds<br />
may be responsible. Risk of paronychia is highest in people who have constantly<br />
cold and wet hands (eg, dairy farmers, fisherman, cleaners), after manicuring,<br />
and in children who bite or pick their nails.<br />
Paronychia may also affect the way the nail grows, especially if it remains<br />
untreated for long periods of time. It may cause distortions, ridges, or<br />
discolouration of the nail. Topical antibiotics may be needed for severe or<br />
prolonged bacterial infection, and it may take up to a year for the nail to grow<br />
back after recovery.<br />
Initial assessment<br />
If the customer has onychomycosis of the toenails, offer to take them to a private area<br />
where they can sit down and you can have a proper look at their feet. Determining<br />
the severity of the infection is important, as severely infected toenails or fingernails<br />
are unlikely to respond to pharmacy-sold treatment products.<br />
Some fungal nail infections are also difficult to distinguish from other types<br />
of infections or medical conditions, such as psoriasis (usually affects all nails<br />
and tends to exist elsewhere on body), dermatitis (fingers or toes are typically<br />
TREATMENT OPTIONS<br />
Category Examples Comments<br />
Topical nail preparations<br />
Fungal nails<br />
[PHARMACY ONLY MEDICINE]<br />
eg, amorolfine (Loceryl Nail Lacquer),<br />
bifonazole (Canesten Fungal Nail),<br />
ciclopirox (Apo-Ciclopirox Nail Lacquer),<br />
poly-ureaurethane (RestoraNail*)<br />
eg, Excilor Fungal Nail, Nailclin Antifungal<br />
Nail Treatment, Pronail Fungal Nail Pen<br />
Discoloured and damaged nails<br />
eg, Loceryl Nail Gel<br />
eg, poly-ureaurethane (RestoraNail*)<br />
Products for infected nails usually work better if most of the infected part of the nail is removed or extensively<br />
thinned before application. Application needs to be regular and consistent and according to manufacturer’s<br />
instructions.<br />
RestoraNail contains poly-ureaurethane, a unique substance that covers and protects the nail, treating both<br />
the fungal infection and repairing damage.<br />
Excilor and Nailclin contain a mixture of ingredients designed to penetrate the nail plate and alter the pH of<br />
the nail bed preventing fungal growth.<br />
Loceryl Nail Gel visibly improves discoloured nails and restores natural water content. Also promotes healthy<br />
regrowth. It is not an antifungal treatment like Loceryl Nail Lacquer.<br />
Natural products Tea-tree oil, garlic Tea-tree oil has been effective at treating fungal nail infections. Garlic reportedly has antifungal properties.<br />
Products with an asterisk have a detailed listing in the Fungal Nail Infections section of OTC Products, starting on page 238.<br />
TREATS DAMAGED<br />
NAILS AND FUNGAL<br />
NAIL INFECTIONS<br />
Page 76 HEALTHCARE HANDBOOK <strong>2017</strong>-2018 Common Disorders