Canine Chronic Inflammatory Rhinitis
Canine Chronic Inflammatory Rhinitis
Canine Chronic Inflammatory Rhinitis
Create successful ePaper yourself
Turn your PDF publications into a flip-book with our unique Google optimized e-Paper software.
<strong>Canine</strong> <strong>Chronic</strong> <strong>Inflammatory</strong> <strong>Rhinitis</strong><br />
Rebecca C. Windsor, DVM*, and Lynelle R. Johnson, DVM, PhD, DACVIM †<br />
<strong>Chronic</strong> inflammatory rhinitis is commonly found in dogs with chronic nasal disease and is<br />
characterized by lymphoplasmacytic infiltrates in the nasal mucosa in the absence of an<br />
obvious etiologic process. The pathogenesis of lymphoplasmacytic rhinitis remains unknown.<br />
Animals respond poorly to antibiotics, oral glucocorticoids, and antihistamines,<br />
making primary infectious, immune-mediated, or allergic etiologies unlikely. Aberrant immune<br />
response to inhaled organisms or allergens may induce inflammation in some<br />
animals. Common clinical signs include nasal discharge, sneezing, coughing, epistaxis,<br />
and stertor. Diagnosis is made by performing a thorough history, physical examination,<br />
radiography or advanced imaging (via computed tomography or magnetic resonance imaging),<br />
rhinoscopy, and nasal mucosal biopsy to rule out primary etiologies of nasal<br />
discharge. Treatment strategies have included various antibiotics, antihistamines, oral and<br />
inhalant steroids, nonsteroidal antiinflammatories, and antifungal medications. Some dogs<br />
may respond partially to doxycycline or azithromycin, although it is unclear whether<br />
response is related to antimicrobial or antiinflammatory properties of these drugs. Hydration<br />
of the nasal cavity through nasal drops or aerosols may limit nasal discharge, and some<br />
animals may improve with inhalant (but rarely oral) glucocorticoids.<br />
Clin Tech Small Anim Pract 21:76-81 © 2006 Elsevier Inc. All rights reserved.<br />
Keywords rhinitis, nasal, canine, inflammatory, lymphoplasmacytic<br />
The most common causes of chronic nasal discharge in<br />
dogs include nasal neoplasia, fungal rhinitis, and lymphoplasmacytic<br />
rhinitis (LPR), also referred to as inflammatory<br />
rhinitis. Other causes of chronic nasal disease include<br />
nasal foreign body, rhinitis secondary to dental disease, parasitic<br />
rhinitis (Pneumonyssoides caninum), and primary ciliary<br />
dyskinesia. Idiopathic LPR is recognized with increasing frequency<br />
in the canine population and may be more common<br />
in certain geographic locations. Diagnosis is made via histopathologic<br />
identification of a lymphoplasmacytic infiltrate<br />
in the nasal mucosa with exclusion of specific causes of<br />
chronic inflammation. An effective therapeutic regimen for<br />
dogs with LPR has not been established, largely because the<br />
underlying pathogenesis is still unknown.<br />
Etiology<br />
The etiology of LPR has not been determined, although infectious,<br />
allergic, and immune-mediated mechanisms have<br />
*Department of Clinical Sciences at North Carolina State University, Raleigh,<br />
NC.<br />
†Diplomate of the American College of Veterinary Internal Medicine, Department<br />
of Medicine and Epidemiology at the University of California,<br />
Davis, CA.<br />
Supported in part by the Bailey Wrigley Fund and the American Kennel Club<br />
Grant 0389, and the Joseph and Mable Howe Research Scholarship.<br />
Address reprint requests to: Department of Clinical Sciences, North Carolina<br />
State University, 4700 Hillsborough Street, Raleigh, NC 27606.E-mail:<br />
rebecca_windsor@ncsu.edu.<br />
76 1096-2867/06/$-see front matter © 2006 Elsevier Inc. All rights reserved.<br />
doi:10.1053/j.ctsap.2005.12.014<br />
been suggested. LPR may have a multifactorial etiology in<br />
some dogs and/or different etiologies in different dogs, making<br />
it difficult to develop general treatment guidelines.<br />
Primary Infection<br />
Primary bacterial infection of the nasal cavity is rare, and no<br />
single infectious organism has been identified in dogs with<br />
LPR. However some dogs respond anecdotally to certain antibiotics<br />
including doxycycline and azithromycin, leading to<br />
the speculation that certain bacterial organisms such as<br />
Chlamydophila, Mycoplasma, orBartonella could be involved<br />
in the pathogenesis of LPR. Chlamydophila is a primary upper<br />
respiratory pathogen in humans, cats, and other species. Bartonella<br />
has been associated with nasal discharge, 1 granulomatous<br />
rhinitis, 2 and epistaxis2,3 in dogs. A recent study investigating<br />
the role of infectious organisms in LPR quantified<br />
DNA loads of Chlamydophila, Bartonella, <strong>Canine</strong>-adenovirus<br />
2 (CAV-2), and Parainfluenza virus 3 (PI-3) in biopsy samples<br />
from dogs with LPR by the use of quantitative PCR, and<br />
a role for these organisms could not be established. 4 In addition,<br />
endpoint PCR was used to examine nasal biopsy samples<br />
for evidence of Mycoplasma spp. and this also failed to<br />
identify a specific pathogen in DNA extracted from formalinfixed<br />
nasal biopsy samples. 4 The poor long-term response to<br />
multiple antibiotics in dogs with LPR suggests that a primary<br />
bacterial infectious etiology is unlikely, although ongoing<br />
studies investigating serologic evidence of Bartonella in dogs
<strong>Canine</strong> chronic inflammatory rhinitis 77<br />
with LPR may provide valuable information on the role of this<br />
organism in the syndrome.<br />
Table 1 Common Clinical Signs in 37 Dogs with Idiopathic<br />
<strong>Rhinitis</strong> 5<br />
Secondary Infection<br />
Secondary bacterial infection is common in dogs with<br />
chronic nasal disease, which may explain the transient response<br />
to antibiotics seen in some dogs with LPR. Nasal<br />
cultures from dogs with LPR yield mixed bacterial growth of<br />
normal nasal flora including Staphylococcus, Streptococcus,<br />
Escherichia coli, Proteus, Pasteurella, Corynebacterium, Bordetella,<br />
and Pseudomonas. 5-7 A recent study demonstrated no<br />
significant difference in bacterial DNA loads among dogs<br />
with LPR, fungal rhinitis, and nasal neoplasia; however, all<br />
three disease groups had significantly higher bacterial loads<br />
than did healthy control dogs. 4 Accumulation of bacterial<br />
organisms in dogs with chronic nasal disease could result<br />
from mucus trapping and decreased nasal mucosal defense<br />
mechanisms.<br />
Role of Fungal Organisms<br />
Aspergillus and Penicillium spp. are common inhabitants of<br />
the canine nasal cavity, 6 and a positive fungal culture can be<br />
found in the absence of primary fungal rhinitis. Candida,<br />
Trichosporum, and Cladosporidium have also been cultured<br />
from dogs with LPR. 5 In the study assessing molecular con -<br />
tent of paraffin-embedded nasal tissue from dogs, higher fungal<br />
DNA loads were reported in dogs with LPR than in<br />
healthy control dogs and dogs with nasal neoplasia. 4 Mucus<br />
trapping and decreased nasal defense mechanisms alone cannot<br />
explain this difference because dogs with nasal neoplasia<br />
would be expected to have similar mucosal compromise to<br />
dogs with LPR. Further research is required to determine the<br />
significance of increased fungal DNA in dogs with LPR. Fungal<br />
hypersensitivity characterized by an aberrant immune<br />
response has been identified in human chronic rhinosinusitis<br />
(CRS) patients. 8-14 Humans with CRS exhibit a humoral and<br />
cellular (Th1 and Th2) response to airborne fungi. 8 T-cell<br />
sensitization to fungus leads to production of T-helper 2<br />
cytokine release, namely Interleukin-5. 11 Fungal hypersensitivity<br />
in humans appears to be characterized by IgG3 rather<br />
than IgE production, suggesting that the hypersensitivity is<br />
not a true allergic response, 8,12 although humans with CRS<br />
do exhibit a predominantly eosinophilic infiltration. 13 In humans,<br />
the quantity of fungal DNA does not correlate with<br />
disease severity. 15 Further research is needed to assess the<br />
immune response of affected dogs to resident fungal organisms.<br />
Allergy<br />
There is some speculation that respiratory allergy may manifest<br />
with signs of chronic rhinitis as is seen in humans, although<br />
evidence of allergic rhinitis as a recognized disease<br />
entity in dogs has yet to be established. It is possible that dogs<br />
with LPR exhibit a heightened immune response to inhaled<br />
environmental allergens; however, no published studies to<br />
date have demonstrated an allergic inflammatory pattern in<br />
dogs with naturally occurring LPR. Experimentally, nasal<br />
congestion has been induced using ragweed pollen in Beagle<br />
colonies, 16-18 Th2 immune response was identified in the peripheral blood<br />
mononuclear cells of three dogs with rhinitis. 19 Nasal mucosal<br />
biopsies were not collected from dogs in these studies so it<br />
is not known whether lymphoplasmacytic infiltration characterized<br />
the disease. Dogs with LPR generally respond<br />
poorly to antihistamines and glucocorticoids, making an allergic<br />
etiology unlikely.<br />
Immune-Mediated<br />
The initial report describing LPR suggested that the disease<br />
was likely immune-mediated because three of five dogs in<br />
that study demonstrated a favorable response to glucocorticoids.<br />
and evidence of allergic response to house dustmite<br />
antigen characterized by increased IL-4 expression and<br />
20 Historically, in our experience, most dogs with LPR<br />
have exhibited a poor response to oral glucocorticoid treatment,<br />
suggesting that a primary immune-mediated etiology<br />
is unlikely. Cats with nasal inflammation exhibit a heightened<br />
Th1 immune response that is more pronounced as inflammation<br />
becomes more severe 21 Mucopurulent, mucoid, or serous<br />
35/37 (95%)<br />
nasal discharge<br />
Sneezing<br />
Coughing<br />
Epistaxis<br />
Reverse sneezing<br />
Stertor<br />
Ocular discharge<br />
Pawing at the muzzle<br />
19/37 (51%)<br />
15/37 (41%)<br />
15/37 (41%)<br />
6/37 (16%)<br />
5/37 (14%)<br />
4/37 (11%)<br />
2/37 (5%)<br />
; however, information is<br />
not available in dogs. Further studies evaluating the immunoregulatory<br />
patterns in the nasal mucosa of dogs with LPR<br />
are required to determine the role of immune dysregulation<br />
in disease.<br />
History<br />
Important historical features in dogs with chronic rhinitis<br />
include duration and progression of clinical signs, character<br />
and laterality of nasal discharge, and response to previous<br />
medical therapies. LPR can be seen in any breed but occurs<br />
most commonly in large-breed dogs. There is no apparent<br />
age or sex predilection. Duration of clinical signs may range<br />
from weeks to years at the time of diagnostic evaluation. The<br />
most common clinical signs include nasal discharge, sneezing,<br />
coughing (likely secondary to pharyngitis caused by<br />
swallowing irritant nasal secretions), and episodes of epistaxis<br />
(Table 1). Although signs related to LPR are often bilateral,<br />
many dogs with LPR have unilateral or lateralizing<br />
signs on presentation. Laterality of clinical signs based on<br />
history and physical examination correlates poorly with computed<br />
tomography, rhinoscopy, and biopsy findings. 5 Therefore,<br />
while unilateral nasal discharge is classically considered<br />
more typical of nasal neoplasia, fungal rhinitis, foreign body<br />
rhinitis, or an oronasal fistula, LPR remains a consideration,<br />
and all dogs with unilateral nasal discharge historically or on<br />
physical examination should be evaluated for bilateral nasal<br />
disease. Other clinical signs of LPR may include reverse<br />
sneezing, stertor, ocular discharge, and pawing/rubbing at<br />
the muzzle.
78 R.C. Windsor and L.R. Johnson<br />
Dogs with LPR typically have a history of poor or transient<br />
response to medical treatment. Many animals demonstrate<br />
little improvement with antibiotics, antihistamines, and glucocorticoids<br />
alone or in combination, while some demonstrate<br />
a transient response with return of clinical signs when<br />
medications are discontinued.<br />
Physical Examination<br />
The most common physical examination findings in dogs<br />
with LPR include fresh or dry nasal discharge or crusting<br />
around the nares. Most animals have mucoid or mucopurulent<br />
discharge, but hemorrhagic or serous discharge may be<br />
seen. Nasal airflow should be assessed using a microscope<br />
slide or cotton ball wisp. When assessing the patency of airflow,<br />
each nostril should be manually occluded to watch for<br />
a stress response, indicating occluded nasal airflow in the<br />
contralateral nostril. Nasal airflow is normally preserved in<br />
dogs with LPR, since obstruction would be more typical of a<br />
mass lesion.<br />
Facial palpation is often unremarkable in patients with<br />
LPR, which may be helpful in differentiating it from fungal<br />
rhinitis and nasal neoplasia, where facial pain is more common.<br />
Dogs with nasal neoplasia may also exhibit facial or<br />
skull deformity, which is not seen in dogs with LPR. Ocular<br />
retropulsion should be performed to detect retrobulbar<br />
masses or abscesses as a cause for nasal discharge. Nasal<br />
planar depigmentation may rarely be noted in dogs with<br />
severe and long-standing discharge associated with LPR but<br />
is more commonly exhibited in dogs with fungal rhinitis or<br />
immune-mediated dermatologic diseases such as discoid lupus<br />
erythematosus. Assessment of regional lymph nodes is<br />
important in animals with nasal discharge due to the tendency<br />
for neoplastic processes to metastasize locally. Lymph<br />
nodes are often enlarged in dogs with LPR or fungal rhinitis,<br />
but aspiration cytology reveals a reactive inflammatory process<br />
rather than neoplasia.<br />
Diagnostic Evaluation<br />
Laboratory Evaluation<br />
Complete blood count, chemistry panel, and urinalysis are often<br />
unremarkable in patients with chronic rhinitis. Dogs with epistaxis<br />
should be evaluated for clotting abnormalities by performing<br />
a platelet count OSPT, APTT, and BMBT to rule out coagulopathies,<br />
thrombocytopenias, and/or thrombocytopathias.<br />
Dogs presenting primarily for epistaxis should also have blood<br />
pressure measured for detection of systemic hypertension.<br />
Imaging Techniques<br />
Radiography has been used in some cases to help differentiate<br />
LPR from nasal neoplasia but has become less popular due to<br />
the availability of superior imaging techniques. Some dogs<br />
with LPR have radiographic evidence of lucent foci and multifocal<br />
lesions, which are not typically seen in dogs with nasal<br />
neoplasia. 22 Neoplastic lesions are more likely to invade - sur<br />
rounding bone22 ; however, neoplastic lesions without obvi -<br />
ous osteolysis may be difficult to differentiate from chronic<br />
rhinitis cases as both diseases cause soft-tissue opacification.<br />
Although one study identified the absence of frontal sinus<br />
Figure 1 Computed tomographic images through the rostral nasal<br />
cavity of two dogs with idiopathic LPR. In the panel on the left,<br />
soft-tissue or fluid opacity is noted between nasal turbinates and is<br />
worse on the right than on the left. In the panel on the right, more<br />
extensive soft-tissue or fluid opacity is noted bilaterally.<br />
involvement on radiographs as a positive predictive indicator<br />
for LPR compared with neoplasia, 22 a recent study showed<br />
that a high percentage of dogs with LPR have frontal sinus<br />
fluid accumulation. 5 LPR is difficult to differentiate from -fun<br />
gal rhinitis via radiography as both can cause turbinate destruction<br />
and frontal sinus accumulation.<br />
Recent studies have demonstrated that computed tomography<br />
(CT) is more sensitive and specific than radiography in<br />
differentiating LPR, nasal neoplasia, and fungal rhinitis. 23-25<br />
The most common CT findings in dogs with LPR include<br />
fluid accumulation within the nasal passages, soft-tissue<br />
opacification, turbinate destruction, frontal sinus accumulation,<br />
and gas pocketing 5 (Figs. 1 and and 2 Table 2) Imaging<br />
abnormalities noted on CT are often diffusely distributed<br />
throughout the nasal cavity, but rostral or caudal localization<br />
may be observed. Turbinate destruction tends to be less severe<br />
in dogs with LPR compared with dogs with nasal neoplasia<br />
or fungal rhinitis. 23 Dogs with nasal neoplasia com -<br />
monly exhibit a soft-tissue density with extensive turbinate<br />
destruction, while those with fungal rhinitis exhibit extensive<br />
turbinate destruction and hyperlucency of the nasal passages. 23<br />
Magnetic resonance imaging (MRI) is another excellent<br />
imaging modality for the nasal cavity, providing superior<br />
soft-tissue detail compared with CT. However no studies to<br />
date have compared the sensitivity and specificity of CT and<br />
MRI for differentiating causes of chronic nasal disease, and<br />
CT is currently the most popular imaging technique due to its<br />
lower cost compared with MRI.<br />
Rhinoscopy<br />
Rhinoscopic evaluation of patients with chronic nasal disease<br />
is essential. For complete assessment of the nasal mucosa and<br />
turbinates, a rigid or flexible endoscope is required. The most<br />
common rhinoscopic features in dogs with inflammatory rhinitis<br />
include mucoid or mucopurulent discharge, hyperemic,<br />
edematous, and/or friable nasal mucosa, and mild turbinate<br />
atrophy or destruction 5 (Fig. 3 and Table 3). Indistinct softtissue<br />
opacities noted on CT can be visualized rhinoscopically,<br />
allowing differentiation among nasal masses, nasal polyps,<br />
and mucus plugs. Fungal plaques or nasal mites may<br />
also be observed rhinoscopically, thus providing a primary<br />
etiology for nasal discharge. Representative biopsy specimens<br />
are best obtained by rhinoscopic identification of areas of
<strong>Canine</strong> chronic inflammatory rhinitis 79<br />
Figure 2 Sequential computed tomographic images through the<br />
frontal sinus of a dog with idiopathic LPR. The top panel shows<br />
soft-tissue or fluid opacification in the left frontal sinus. In the next<br />
7-mm slice, the frontal sinus has filled more completely and an<br />
air–fluid meniscus is present, suggesting that fluid is filling the<br />
frontal sinus.<br />
significant nasal mucosal pathology and visualization of the<br />
area sampled for histopathology.<br />
Other diagnostic techniques to perform after rhinoscopy<br />
are examination of the nasopharyngeal region using a<br />
dental mirror or retroflexed endoscope to look for nasopharyngeal<br />
polyps and dental probing to rule out oronasal<br />
fistula or dental disease as a cause for unilateral nasal<br />
discharge.<br />
Histopathology<br />
Nasal biopsy samples of dogs with chronic, idiopathic, inflammatory<br />
rhinitis are characterized by a primarily lymphoplasmacytic<br />
infiltrate, but concurrent neutrophilic or less<br />
commonly eosinophilic infiltrate may also be seen. Epithelial<br />
Table 2 Computed Tomography in 33 Dogs with Idiopathic<br />
<strong>Rhinitis</strong> 5<br />
Normal 4/33 (12%)<br />
Unilateral lesions 8/33 (24%)<br />
Bilateral lesions 21/33 (64%)<br />
Fluid accumulation 27/33 (82%)<br />
Soft-tissue opacification 25/33 (78%)<br />
Plaque-like lesions 24/33 (73%)<br />
Turbinate destruction 23/33 (70%)<br />
Gas pocketing 23/33 (70%)<br />
Frontal sinus opacification 14/33 (42%)<br />
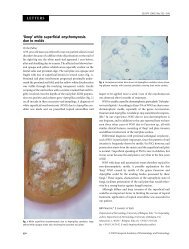
Figure 3 Rhinoscopic image of a dog with idiopathic LPR. Marked<br />
hyperemia and mucus accumulation are evident. (Color version of<br />
figure is available online.)<br />
changes are usually mild but may include epithelial hyperplasia<br />
and erosion. Turbinate remodeling or destruction can<br />
also be evident. The majority of dogs with unilateral clinical<br />
signs have bilateral nasal mucosal pathology, and severity of<br />
inflammation between the two sides of the nasal cavity often<br />
varies.<br />
Culture and Cytology<br />
Obtaining a positive culture of bacterial and/or fungal organisms<br />
in dogs with inflammatory rhinitis is not uncommon<br />
and likely reflects normal nasal mucosal flora or secondary<br />
infection rather than primary infectious rhinitis. Culture results<br />
from the rostral nasal cavity may differ from the caudal<br />
nasal cavity. 26 Similarly, brush or lavage samples from super -<br />
ficial epithelium may not adequately reflect bacterial and fungal<br />
infiltration into the nasal mucosa. When culture is desired,<br />
collection of a deep nasal lavage using a protected<br />
catheter brush or submission of a nasal biopsy sample for<br />
culture should be considered.<br />
Nasal mucosal cytology may be used to identify fungal or<br />
neoplastic lesions in some cases; however, cytology has poor<br />
sensitivity and specificity compared with histology in nasal<br />
mucosal samples27-29 and is often unreliable for detecting<br />
chronic changes. 29<br />
Table 3 Rhinoscopic Findings in 37 Dogs with Idiopathic <strong>Rhinitis</strong><br />
5<br />
Normal 1/37 (3%)<br />
Unilateral lesions 7/37 (19%)<br />
Bilateral lesions 21/37 (57%)<br />
Mucoid or mucopurulent discharge 29/37 (78%)<br />
Hyperemic, or inflamed mucosa 26/37 (70%)<br />
Mucosal edema 8/37 (22%)<br />
Turbinate atrophy, destruction, or loss 8/37 (22%)<br />
Hemorrhage or blood clots 5/37 (14%)<br />
Mucosal friability 4/37 (11%)
80 R.C. Windsor and L.R. Johnson<br />
Treatment<br />
No effective treatment regimen for LPR has been established;<br />
therefore, animals are commonly treated with a variety of<br />
medications including antibiotics, antiinflammatory drugs<br />
(glucocorticoids: oral or topical, or nonsteroidal antiinflammatory<br />
drugs), antihistamines, and antifungal medications.<br />
Antibiotics<br />
Dogs with mucopurulent nasal discharge likely have some<br />
degree of secondary bacterial contamination. Antibiotic treatment<br />
in these animals may help to reduce the severity of the<br />
nasal discharge and alter the character of discharge from<br />
mucopurulent to serous, but complete sustained resolution<br />
of nasal discharge is rarely achieved. Most nasal bacterial<br />
infections are susceptible to multiple antibiotics. Some dogs<br />
respond well to doxycycline (3 to 5 mg/kg PO twice per day),<br />
which may be attributed partially to its antiinflammatory<br />
effects. Macrolides such as azithromycin (5 mg/kg daily for 5<br />
days, then twice weekly) have also been effective in some<br />
dogs.<br />
Although the long-term response to antibiotics has not<br />
been reported, it is unlikely that such treatment results in<br />
cure of disease. Extended courses of suppressive antibiotic<br />
therapy or intermittent treatment with such drugs may be<br />
required for control of signs. If the severity of the nasal discharge<br />
worsens when antibiotics are discontinued, it is advisable<br />
to reinstitute therapy with the same antibiotic to avoid<br />
development of antibiotic resistance by use of multiple antibiotics.<br />
Anti-<strong>Inflammatory</strong> Agents<br />
Oral glucocorticoids have not proven effective in treating<br />
most dogs with LPR; therefore, long-term use of oral steroids<br />
should be avoided because of systemic side effects. Topical<br />
nasal steroid drops may be applied if the dog will tolerate<br />
administration. Topical glucocorticoid sprays such as fluticasone<br />
propionate have been used with variable success in human<br />
chronic rhinosinusitis patients 30-32 and have shown an -<br />
ecdotal promise in some dogs and cats with chronic nasal<br />
discharge. Although typically used to treat lower airway disease,<br />
metered dose inhalers (MDIs) containing fluticasone<br />
may also benefit animals with rhinitis as the drug must first<br />
pass through the nasal passages before reaching the lower<br />
respiratory tract. Aerosolized steroids can be administered<br />
using MDIs attached to a spacer and tightly fitting facemask.<br />
The MDI must be well-shaken before actuation into the<br />
spacer, and the animal must take 8 to 10 breaths without<br />
panting to carry the drug into the respiratory tract. A commercially<br />
available spacer with facemask designed for cats<br />
(Aerokat) works well in brachycephalic dogs. For larger,<br />
dolicocephalic dogs, human pediatric spacers must be obtained,<br />
and appropriate face masks must be acquired from a<br />
local pharmacy or anesthetic supply company.<br />
Nonsteroidal antiinflammatory drugs may be somewhat<br />
efficacious in reducing nasal inflammation in certain cases.<br />
These drugs are also sometimes used in feline nonspecific<br />
rhinitis, when it is unclear whether an infectious etiology<br />
might be present. The most commonly used drug is likely<br />
piroxicam. Like all nonsteroidal agents, this drug can be as-<br />
sociated with gastrointestinal effects associated with GI ulceration<br />
and with renal dysfunction. When used at 0.3 mg/kg<br />
PO daily in healthy animals, it is unlikely to have untoward<br />
side effects, although owners should be instructed to watch<br />
for anorexia, vomiting, or abdominal pain.<br />
Antihistamines<br />
Antihistamines are occasionally used in LPR dogs, although<br />
response is typically poor, and the sedative effects of some<br />
antihistamines may outweigh any therapeutic benefit. Also,<br />
antihistamines may have the undesirable side effect of drying<br />
nasal secretions and worsening mucus accumulation. However,<br />
if sneezing and nasal discharge worsen seasonally and<br />
an inhaled environmental allergen is suspected, an antihistamine<br />
trial may be employed.<br />
Antifungal Therapy<br />
A few dogs with LPR have been treated empirically with<br />
topical antifungal medications (clotrimazole, enilconazole)<br />
to treat a possible undiagnosed fungal rhinitis; however, improvement<br />
in clinical signs was not noted. 5 Response to oral<br />
antifungals has not been reported. Variable results have been<br />
reported in human chronic rhinusinusitis patients with suspected<br />
fungal hypersensitivity. Nasal amphotericin B resulted<br />
in deterioration of symptoms in one study, 33 while<br />
proving safe and effective in another. 34<br />
Other Therapies<br />
Some dogs with LPR may present with signs of reverse sneezing.<br />
Reverse sneezing occurs in response to irritation of the<br />
nasal mucosa, which may be caused by inhaled irritants or<br />
occasionally by the nasal mite, P. caninum. Dogs that exhibit<br />
reverse sneezing should be treated empirically with ivermectin<br />
(or milbemycin in Collie breeds) to rule out parasitic<br />
infestation as a cause of rhinitis before pursuing aggressive<br />
diagnostics.<br />
Increasing nasal hydration through the use of topical saline<br />
drops or with saline inhalation or nebulization can aid in<br />
evacuation of the nasal cavity. Dogs are variably tolerant of<br />
having saline nasal drops administered to the nasal cavity,<br />
but this is the least expensive alternative for liquefying nasal<br />
secretions and encouraging removal from the nasal cavity.<br />
Conclusion<br />
<strong>Inflammatory</strong> rhinitis is commonly found in dogs with<br />
chronic nasal disease. The etiology of this disorder remains<br />
unknown and may involve different pathogenic mechanisms<br />
in different dogs with chronic nasal disease. Some dogs may<br />
exhibit an aberrant immune response to commensal fungal<br />
organisms or other inhaled pathogens or irritants. The diagnosis<br />
of LPR requires a thorough history and physical examination,<br />
advanced imaging (CT or MRI), rhinoscopic evaluation,<br />
and biopsy. Culture and cytology may occasionally<br />
prove useful in differentiating LPR from other causes of rhinitis<br />
(ie, fungal rhinitis and neoplasia). The poor response to<br />
treatment with antibiotics, glucocorticoids, and antihistamines<br />
makes LPR a frustrating condition to treat. Current<br />
recommendations to be considered include the use of doxycycline<br />
or azithromycin for their antiinflammatory as well as
<strong>Canine</strong> chronic inflammatory rhinitis 81<br />
antibacterial effects, and trial therapy with piroxicam. Owners<br />
should be advised that antibiotics only treat secondary<br />
bacterial infections and nasal discharge will likely return<br />
once antibiotics are discontinued. Use of multiple antibiotics<br />
should be avoided. Oral corticosteroids have shown little<br />
therapeutic benefit and should be avoided due to unwanted<br />
systemic effects. However, inhalant corticosteroids may be<br />
effective in some patients. Further research is required to<br />
identify the pathogenesis of LPR with the aim of developing<br />
an effective treatment regimen.<br />
References<br />
1. Henn JB, Liu CH, Kasten RW, et al: Seroprevalence of antibodies<br />
against Bartonella species and evaluation of risk factors and clinical<br />
signs associated with seropositivity in dogs. Am J Vet Res 66(4):688-<br />
694, 2005<br />
2. Pappalardo BL, Brown T, Gookin JL, et al: Granulomatous disease<br />
associated with Bartonella infection in 2 dogs. J Vet Intern Med 14(1):<br />
37-42, 2000<br />
3. Breitschwerdt EB, Hegarty BC, Maggi R, et al: Bartonella species as a<br />
potential cause of epistaxis in dogs. J Clin Microbiol 43(5):2529-2533,<br />
2005<br />
4. Windsor RC, Johnson LR, Sykes JE, et al: Molecular detection of microbes<br />
in nasal biopsies of dogs with idiopathic lymphoplasmacytic<br />
rhinitis. J Vet Int Med (in press)<br />
5. Windsor RC, Johnson LR, Herrgesell EJ, et al: Idiopathic lymphoplasmacytic<br />
rhinitis in 37 dogs: 1997-2002. J Am Vet Med Assoc 224(12):<br />
1952-1957, 2004<br />
6. Norris AM, Laing EJ: Diseases of the nose and sinuses. Vet Clin North<br />
Am (Small Anim Pract) 15:865, 1985<br />
7. Greene CE: Bacterial infections of the upper respiratory system. In<br />
Greene CE (ed): Infectious Diseases of the Dog and Cat. Philadelphia,<br />
PA, WB Saunders, 1998, pp 583-584<br />
8. Shin SH, Ponikau JU, Sherris DA, et al: <strong>Chronic</strong> rhinosinusitis: an<br />
enhanced immune response to ubiquitous airborne fungi. J Allergy Clin<br />
Immunol 114(6):1369-1375, 2004<br />
9. Gosepath J, Brieger J, Vlachtsis K, et al: Fungal DNA is present in tissue<br />
specimens of patients with chronic rhinosinusitis. Am J Rhinol 18(1):<br />
9-13, 2004<br />
10. Gosepath J, Mann WJ: Role of fungus in eosinophilic sinusitis. Curr<br />
Opin Otolaryngol Head Neck Surg 13(1):9-13, 2005<br />
11. Hamilos DL, Lunf VJ: Etiology of chronic rhinosinusitis: the role of<br />
fungus. Ann Otol Rhinol Laryngol Suppl 193:27-31, 2004<br />
12. Pant H, Kette FE, Smith WB, et al: Fungal-specific humoral response in<br />
eosinophilic mucus chronic rhinosinusitis. Laryngoscope 115(4):601-<br />
606, 2005<br />
13. Sasama J, Sherris DA, Shin SH, et al: New paradigm for the roles of fungi<br />
and eosinophils in chronic rhinosinusitis. Curr Opin Otolaryngol Head<br />
Neck Surg 13(1):2-8, 2005<br />
14. Polzehl D, Weschta M, Podbielski A, et al: Fungus culture and PCR in<br />
nasal lavage samples of patients with chronic rhinosinusitis. J Med<br />
Microbiol 54:31-37, 2005<br />
15. Schueller MC, Murr AH, Goldberg AN, et al: Quantitative analysis of<br />
fungal DNA in chronic rhinosinusitis. Laryngoscope 114(3):467-471,<br />
2004<br />
16. Rudolph K, Bice DE, Hey JA, et al: A model of allergic nasal congestion<br />
in dogs sensitized to ragweed. Am J Rhinol 17(4):227-232, 2003<br />
17. Cardell LO, Agusti C, Nadel JA: Nasal secretion in ragweed-sensitized<br />
dogs: effect of leukotriene synthesis inhibition. Acta Otolaryngol<br />
120(6):757-760, 2000<br />
18. Tiniakov RL, Tiniakova OP, McLeod RL, et al: <strong>Canine</strong> model of nasal<br />
congestion and allergic rhinitis. J Appl Physiol 94(5):1921-1928, 2003<br />
19. Kurata K, Maeda S, Yasunaga S, et al: Immunological findings in 3 dogs<br />
clinically diagnosed with allergic rhinitis. J Vet Med Sci 66(1):25-29,<br />
2004<br />
20. Burgener DC, Slocombe RF, Zerbe CA: Lymphoplasmacytic rhinitis in<br />
five dogs. J Am Hosp Assoc 23:565-568, 1987<br />
21. Johnson LR, DeCock HE, Sykes HE, et al: Cytokine gene transcription<br />
in feline nasal tissue with histologic evidence of inflammation. Am J Vet<br />
Res 66(6):996-1001, 2005<br />
22. Russo M, Lamb CR, Jakovljevic S: Distinguishing rhinitis and nasal<br />
neoplasia by radiography. Vet Radiol Ultrasound 41(2):118-124, 2000<br />
23. Lefebvre J, Kuehn NF, Wortinger A: Computed tomography as an aid<br />
in the diagnosis of chronic nasal disease in dogs. J Small Anim Pract<br />
46(6):280-285, 2005<br />
24. Saunders JH, van Bree H, Gielen I, et al: Diagnostic value of computed<br />
tomography in dogs with chronic nasal disease. Vet Radiol Ultrasound<br />
44(4):409-413, 2003<br />
25. Codner EC, Lurus AG, Miller JB, et al: Comparison of CT with radiography<br />
as a noninvasive diagnostic technique for chronic nasal disease in<br />
dogs. J Am Vet Med Assoc 202(7):1106-1110, 1993<br />
26. Abramson AL, Isenberg HD, McDermott LM: Microbiology of the canine<br />
nasal cavities. Rhinology 18:143, 1980<br />
27. Cohen M, Bohling MW, Wright JC, et al: Evaluation of sensitivity and<br />
specificity of cytologic examination: 269 cases (1999-2000). J Am Vet<br />
Med Assoc 222(7):964-967, 2003<br />
28. Lin R, Nahal A, Lee M, et al: Cytologic distinctions between clinical<br />
groups using curette-probe compared to cytology brush. Ann Allergy<br />
Asthma Immunol 86:226-231, 2001<br />
29. Michiels L, Day MJ, Snaps F, et al: A retrospective study of non-specific<br />
rhinitis in 22 cats and the value of nasal cytology and histopathology. J<br />
Fel Med Surg 5:279-285, 2003<br />
30. Parikh A, Scadding GK, Darby Y, et al: Topical corticosteroids in<br />
chronic rhinosinusitis: a randomized double-blind, placebo-controlled<br />
trial using fluticasone proprionate aqueous nasal spray. Rhinology<br />
39(2):75-79, 2001<br />
31. Dolor RJ, Witsell DL, Hellkamp AS, et al: Comparison of cefuroxime<br />
with or without intranasal fluticasone for the treatment of rhinosinusitis.<br />
The CAFFS Trial: a randomized controlled trial. J Am Med Assoc<br />
286(24):3097-3105, 2001<br />
32. Dijkstra MD, Ebbens FA, Poublon RM, et al: Fluticasone propionate<br />
aqueous nasal spray does not influence the recurrence rate of chronic<br />
rhinosinusitis and nasal polyps 1 year after functional endoscopic sinus<br />
surgery. Clin Exp Allergy 34(9):1395-1400, 2004<br />
33. Weschta M, Rimek D, Formanek M, et al: Topical antifungal treatment<br />
of chronic rhinosinusitis with nasal polyps: a randomized, doubleblind<br />
clinical trial. J Allergy Clin Immunol 113(6):1122-1128, 2004<br />
34. Ponikau JU, Sherris DA, Kita H, et al: Intranasal antifungal treatment in<br />
51 patients with chronic rhinosinusitis. J Allergy Clin Immunol 111(5):<br />
1137-1138, 2003