Performance Evaluation of Contemporary Spirometers - Chest
Performance Evaluation of Contemporary Spirometers - Chest
Performance Evaluation of Contemporary Spirometers - Chest
You also want an ePaper? Increase the reach of your titles
YUMPU automatically turns print PDFs into web optimized ePapers that Google loves.
<strong>Performance</strong> <strong>Evaluation</strong> <strong>of</strong> <strong>Contemporary</strong><br />
<strong>Spirometers</strong>*<br />
Steven B. Nelson, M.S.; Reed M. Gardner, Ph.D.;<br />
Robert 0. Crapo, M.D., F.C.C.P; and Robert L. Jensen, Ph.D.<br />
A comprehensive evaluation <strong>of</strong> 62 spirometers from 37<br />
different sources was performed using a two-part protocol:<br />
calibrated syringe, and dynamic waveform testing. All<br />
testingwas done with ambient air. Calibrated syringe testing<br />
examined the ability <strong>of</strong> the spirometers to accurately<br />
measure the output <strong>of</strong> a 3 L calibrating syringe under<br />
varying conditions. The accuracy, FVC volume linearity,<br />
and stability <strong>of</strong> each spirometer was determined from these<br />
data. AU but five <strong>of</strong> 42 spirometers accurately measured a<br />
3 L calibrating syringe to within ±3 percent. Dynamic<br />
waveform testing consisted <strong>of</strong> introducing 24 standard<br />
waveforms into the spirometer from a computer-controlled<br />
air pump. The values <strong>of</strong>FVC, FEy1, and FEF2.5-75% were<br />
compared to the actual values for each waveform to<br />
determine a performance rating. Only 35 (56.5 percent) <strong>of</strong><br />
the spirometers performed acceptably when measuring the<br />
T he need for accuracy in measuring spirometry<br />
parameters has been widely recognized and ac-<br />
cepted. -I The American College <strong>of</strong><strong>Chest</strong> Physicians,<br />
the Association for the Advancement <strong>of</strong> Medical<br />
Instrumentation,5 and American Thoracic Society#{176}’#{176}<br />
have all published recommendations for spirometer<br />
performance. Earlier studies <strong>of</strong> spirometer accuracy<br />
have found several performance problems. FitzGerald<br />
and co-workers’ found that all seven “electronic”<br />
spirometers they tested in 1973 were incapable <strong>of</strong><br />
For editorial comment see page 258<br />
measuring FVC and FEy1 accurately or reproducibly<br />
when compared with a water-seal spirometer. Gardner<br />
et al tested 12 volume-based and seven flow-based<br />
spirometers. Eight (67 percent) <strong>of</strong> the volume-based<br />
devices performed acceptably, while all seven <strong>of</strong> the<br />
flow-based devices had performance difficulties. We-<br />
ver et al,6 in a clinical test, found that ony two <strong>of</strong> five<br />
spirometers were acceptable.<br />
With the proliferation <strong>of</strong> computerized spirometry<br />
systems, it is now important to test the volume or flow<br />
transducer as a system with the computer, rather than<br />
*Fmm the Departments <strong>of</strong> Medical Informatics and Medicine,<br />
Pulmonary Division, School <strong>of</strong> Medicine, University <strong>of</strong> Utah, Salt<br />
Lake City.<br />
<strong>Evaluation</strong> results and listing <strong>of</strong> brand names does not constitute<br />
endorsement or approval by the University <strong>of</strong> Utah, the authors,<br />
or the American College <strong>of</strong><strong>Chest</strong> Physicians.<br />
Manuscript received May 8; revision accepted June 22.<br />
Reprint requests: Dr. Gardner, LDS Hospital, Salt Lake City, Utah<br />
84143<br />
24 standard waveforms. Nine (14.5 percent) were marginal<br />
and 18 (29.0 percent) were unacceptable. Fifty-nine (95<br />
percent) <strong>of</strong>the 62 spirometers were computerized. S<strong>of</strong>tware<br />
errors were found in 25 percent <strong>of</strong>the computerized systems<br />
evaluated. Although using a 3 L syringe for quality control<br />
purposes is essential, simple testing <strong>of</strong> spirometers with a<br />
3 L calibrating syringe for validation purposes was madequate<br />
to assess spirometer perftirmance when compared to<br />
dynamic waveform testing. Dynamic waveform testing is<br />
essential to accurately measure and validate acceptability<br />
<strong>of</strong> spirometer system performance. (<strong>Chest</strong> 1990; 97:288-97)<br />
[-ACCPAmerican College <strong>of</strong> <strong>Chest</strong> Physicians; AAMI Association<br />
for the Advancement <strong>of</strong> Medical Instrumentation;<br />
ATS American Thonacic Society<br />
testing only parts <strong>of</strong> the system as some authors have<br />
chosen.” A volume or flow transducer may be inher-<br />
ently accurate and precise, but may be attached to a<br />
computer with an inadequate sampling rate, made-<br />
quate flow or volume resolution, or inadequate call-<br />
bration or computation ri’#{176}<br />
Our principal objective was to determine whether<br />
contemporary spirometers were able to meet perform-<br />
ance criteria when measuring a set <strong>of</strong> 24 standard<br />
spirometry waveforms.5’7”0 To accomplish this objec-<br />
tive, we developed a computer-controlled, stepper<br />
motor-driven air pump. The pump was then used to<br />
evaluate 62 contemporary spirometers.<br />
In addition, we wanted to determine whether<br />
testing spirometer performance with a calibrated<br />
syringe alone was adequate. Daily quality control<br />
checks done with a 3 L syringe can show when a<br />
change in accuracy <strong>of</strong> a particular instrument has<br />
occurred . However, these checks are performed under<br />
the basic assumption that the spirometer is inherently<br />
capable <strong>of</strong> proper operation. Therefore, an additional<br />
objective was to determine whether the testing with a<br />
3 L syringe alone was adequate to differentiate spirom-<br />
eters that performed correctly from those that did<br />
not. The need for daily quality control still exists; it is<br />
required for maintaining proper laboratory quality<br />
control and operations.<br />
288 <strong>Performance</strong> <strong>Evaluation</strong> <strong>of</strong> <strong>Contemporary</strong> Spsrometers (Nelson et a!)<br />
Downloaded From: http://journal.publications.chestnet.org/ on 07/13/2013<br />
M<br />
All testing was performed with ambient air at about 21#{176}C, relative<br />
humidity 30 percent and 647 mm Hg barometric pressure. Using
OHIO 822<br />
ROLLING SEAL<br />
SPIROMETER<br />
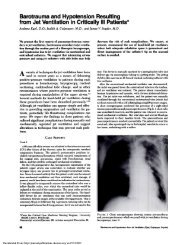
FI;uRF: 1 Photograph <strong>of</strong>coluputer-c()ntrolled air I)LIIO1P. The stepper iootor is cOIlII(’cte(l 1)) a 1 thread it’r<br />
inch latll sci#{149}ev alIt1 feflIl shaft to on Ohio 822 horizontal rolling st-al spironoeter.<br />
aIfll)ielot air allowed testing the spiroInett’rs SIII(ler l)est-case CoIl-<br />
ditiosis, oiid elinii,iated pote’Iltial Illicertainties relatcd to the oct,,al<br />
te’fIl1)eratLlrt- ltI(l hunliditv <strong>of</strong> gusts (lvliere(l to the flov or olIIIne<br />
sensors. The sI)irS1ot’t(-rs Ise(l a ariet <strong>of</strong> 1)atiellt corlIIectu)us ith<br />
varying (lead-S1)aCe voltiiiot’s. Tl’ oritble voltiiiies aIl(1 COIIIICCtiOIIS<br />
%VOLII(l ln’e int,odi,ct’d 0I)1)re(lictal)k’ gas-ccliIlg effects. ‘I’he ability<br />
<strong>of</strong> svstens to deal with BTPS C()II(liti<strong>of</strong>ls, 1 soslrie <strong>of</strong> error that is<br />
greater thati 10 1erct’Ilt, was itot test#{128}’(l.<br />
(alibrated syringe testing t’xainiin’cl the actiraoc liit’ait; aIlCI<br />
stal)ilitv over tilOc. For each <strong>of</strong> these tests, the 3 L calibrating<br />
syringe was emptied into each spirometer ten times. Accuracy <strong>of</strong><br />
the spironieters was determined by manually injecting the volunoc<br />
from the 3 L calibrating syringe “fast” and “slow” as reconhoownde(l<br />
13%’the American Tluracic Societ’ and the lnternlollntain Tliracic<br />
Societs’’2 The fast flow test was coslclllcte(l l)\ elliptyilig the 3 L<br />
syringe in less thato one secon(I with o I)eak Hon <strong>of</strong> at least 6 IJs<br />
(ten repetitions). The slow flow test emptied the syringe over at<br />
least a six-second perit1, not exceeding 0.5 Us (tell repetitions).<br />
Linearity ssas measured in spirosneters with volume scissors (eg,<br />
hellosvs) l)\ eniptving the syringe at t’sv() (liflerent starting vo1uiies<br />
in the spirooneter; approximately 1 L, then approximately 4 L.<br />
Linearity for flow seissrs s’as perfrnle(l l)% comparing the voliinw<br />
ineasured (luring fast and slow syringe injections. Stability sas<br />
measured I)\ repeating the accuracy tests after the device had been<br />
in operation for at least eight hours.<br />
Dynamic waveform testing was performed using a co)mI)uter-<br />
controlled air pump to inject 24 standard waveh)rlus into the<br />
spirometer l)eing tested. ‘‘ The AAMI and the ATS recommend<br />
perfornance testing for validation <strong>of</strong>spirolneter caI)al)ilit\ Earlier<br />
spirometry testing used 16 waveforms, 12 expo)nelltial, lIl(l four<br />
patient waeforins. ‘ The 24 standard waveforms allow for snore<br />
comprehensive testing <strong>of</strong> spirometers.7 Testing start- and end-<strong>of</strong>-<br />
test algorithons is also best (lone with actual patient waveforms.<br />
A co)Inpo,ter-controlle(I air 1”1P constructed with sn IBNI<br />
PC-c’cnpatible coml)tlter connected to a ConlpoItslotor 106-178<br />
stepper motor (Fig 1). The stepper motor prodtlce(l rOtatn)flal<br />
displacement ill discrete steps iii respnse to electrical pulses. The<br />
motor svas capable <strong>of</strong> resolving one revolutn)n into 25,(XX) discrete<br />
steps. The motor was then connected to a nl()(lifie(l Ohio 822<br />
spirneter with i lo friction. low hysteresis ball-scrcw assenhi)ly.<br />
The ‘svavefirm silnulator (Ielivcrc(l voliuno’ in iIlcreul(’IIts <strong>of</strong> 0.06e<br />
ml for each polse gelicrated i the co,optiter. Tloe i,uiiiiiio,,n flos<br />
tilt’ 1)510111) could (ieli\er svas 0.(X)49 1./s. tist’ tiocoictical InaXinulni<br />
Downloaded From: http://journal.publications.chestnet.org/ on 07/13/2013<br />
\vats 159 L/s, altin)ugh 16 1Js scas tile I)ractical tper ii,nit. NLLXiIIILII33<br />
Hos’ VL5 lilllit(’(l i)\ the s<strong>of</strong>tsvare routines re(I,ire(i to gra(iually<br />
dccCleldte the IllOtOl to Pre’s’(’Ilt stalling aI)(l i)\ the liinitt’d solllnle<br />
(lisl)la(eIIIeIIt <strong>of</strong> tue (lrv-rolling seal spironlett-r. The c()Inputer-<br />
controlled air 1)111131) \L5 (lesigne(l to have an accuracy <strong>of</strong> ± 1 I)crteI,t<br />
for F’V(, FE\71 a,id FEF2575C/o. I I SIIbse(1ucnt Vali(latioll <strong>of</strong> the<br />
air 1)111131) showed less thall 0.5 percellt ariaoinlit Figure 2 is a<br />
flow-voluult’ 1)lot<strong>of</strong>standard waseforln 1 overlai(i 1 1 times illustrat-<br />
ing tiot’ excelleit repro(loIcii)ilitv <strong>of</strong> tiu’ air )01IIlp.<br />
rioC values iieasured liv spirometrrs for FVC, FEV and FEF25-<br />
75% for cach <strong>of</strong> the 24 waveforms were assessed. The 1979 ATS<br />
sPir1etrY recommendations for FVC and FEV, accuracy allow<br />
errors <strong>of</strong> ± 5() ml tip to 1 667 ml, then ± 3.0 PerceSlt <strong>of</strong> tile known<br />
altIe. For FEF25-75%, accuracy liIllits ere ± 2()0 sol/s up to 4,()()0<br />
1131/5, tileIl ± 5.0 percesit <strong>of</strong> the ksoown ‘aisle. ‘l() all() for the<br />
Vaflai)ility intr()dt1ced b the coniptter-controlled Munp, we cx-<br />
C’)<br />
0<br />
-J<br />
IL.<br />
14 0<br />
1? .0<br />
1’..<br />
40<br />
0.0 00<br />
10 2.0 30 40 ‘30 60 70<br />
VOLUME (L)<br />
F’I( Uhf: 2. Flov-voiuiiie Plot <strong>of</strong> 1 1 iteratu)ns <strong>of</strong> the out1)lIt from (lot<br />
colnpo,ter-controli(-d air j)tIIl() illustrating (lu itcurac’ and repro-<br />
(llICil)ilitt <strong>of</strong> the air 1)111011). hit’ inset waveforn, shows tiot’ fiuoal liter<br />
<strong>of</strong> the F\( CX()all(l(’(l 4 thoies. Note e’xtrt’noe’lv repro(hlcii)lt’ results<br />
(‘vt-Il with tin’ eXpan(lt’(l scale.<br />
CHEST I 97 I 2 I FEBRUARY, 1990 289
Spirometer NamelModel Type Version<br />
Computer Size Source<br />
AEC Spirocomp<br />
Biotnne MultiSpiro PC<br />
Brentwood Spiroscan 2000<br />
CDX 101<br />
CDX 110<br />
Chesebrough-Ponds Respiradyne<br />
Cybermedic CM5<br />
Cybermedic CM31O<br />
Cybermedic Moose<br />
Fukuda Sangyo ST200<br />
Gould Telemetry MR1<br />
Gould 21E<br />
Gould 2180<br />
Gould Spiroscreen<br />
Infomed IFU<br />
Infomed MWS 6000<br />
Kinetex Windmill<br />
KL Engineering Pneumoscan<br />
LDSH Ohio 822 Telemetry<br />
Med Equip Design Autospiro<br />
Medical Graphics 1070<br />
MedScience 3200 AT<br />
NIOSH<br />
Omnitek w/Ohio 822<br />
PK Morgan Pocket Respirometer<br />
PK Morgan SPIROFLOW 12<br />
PK Morgan TFC<br />
Pneumedics Dataloop<br />
Pneumedics Spiroloop<br />
Puritan-Bennett VS400<br />
Riko AS500<br />
S&M Inst w/Infomed<br />
S&M Inst w/Jaeger Screenmate<br />
S&M Inst w/Mijnhardt Vicatest 3<br />
S&M Inst w/Ohio 822<br />
S&M Inst w/WE Collins Svy III<br />
SensorMedics Horizon 2<br />
Sherwood Medical Respiradyne II<br />
Spirometrics SM! 3<br />
Spirotech 5500<br />
Tenet wfPK Morgan Spir<strong>of</strong>low<br />
VacuMed UCI 500<br />
Vertek VR5000<br />
Vitalograph Alpha<br />
Vitalograph Compact<br />
Vitalograph PFr II<br />
WE Collins DS 520<br />
WE Collins DS 560<br />
WE Collins DS-Plus<br />
WE Collins Eagle!! w/pneumotach<br />
WE Collins Eaglell w/Survey<br />
WE Collins MLA 3000<br />
WE Collins 13.5L Respirometer<br />
Spirometer 1<br />
Spirometer 2<br />
Spirometer 3<br />
Spirometer 4<br />
Spirometer 5<br />
Spirometer 6<br />
Spirometer 7<br />
Spirometer 8<br />
Spirometer 9<br />
C<br />
C<br />
F<br />
C<br />
C<br />
R<br />
F<br />
B<br />
F<br />
F<br />
M<br />
1. 1X<br />
1.21<br />
N/A<br />
industrial<br />
2.1X<br />
5-7905<br />
2.16<br />
2.16<br />
2.19<br />
N/A<br />
N/A<br />
MP<br />
PPC<br />
MP<br />
other<br />
MP<br />
MP<br />
IBM<br />
IBM<br />
IBM<br />
MP<br />
other<br />
H 5.0 IBM<br />
H 4.1C APPLE<br />
V N/A M<br />
M 1ASX MP<br />
D 2-25-86-T IBM<br />
H 2-25-86-T IBM<br />
V 9-3-85 IBM<br />
D 9-3-85 IBM<br />
W 9-3-85 IBM<br />
D 2.05 TI<br />
R N/A MP<br />
V 2.1 MP<br />
D 3C.7 IBM<br />
D N/A other<br />
D 1.OD PPC<br />
F N/A MP<br />
0 N/A MP<br />
F PP5 MP<br />
B 39.070 MP<br />
W 3.83 APPLE<br />
W 2.86 IBM<br />
W 2.86 IBM<br />
F 2.86 MP<br />
W 2.86 MP<br />
W 6.84 APPLE<br />
W N/A other<br />
F<br />
B<br />
B<br />
290 <strong>Performance</strong> <strong>Evaluation</strong> <strong>of</strong> <strong>Contemporary</strong> Spirorneters (Ne!son at a!)<br />
Downloaded From: http://journal.publications.chestnet.org/ on 07/13/2013<br />
Table 1-ldentficaUon <strong>of</strong><strong>Spirometers</strong> Tested<br />
V<br />
M<br />
S<br />
D<br />
D<br />
T<br />
T<br />
D<br />
S<br />
H<br />
B<br />
D<br />
D<br />
T<br />
D<br />
D<br />
0<br />
V<br />
V<br />
V<br />
V<br />
H<br />
S<strong>of</strong>tware<br />
POS-W010205<br />
POS-F030301<br />
G3<br />
R3.40F<br />
R4.041<br />
N/A<br />
N/A<br />
N/A<br />
N/A<br />
1070.3<br />
3200-2-3-A<br />
Version 2<br />
1.3<br />
N/A<br />
N/A<br />
N/A<br />
other<br />
other<br />
MP<br />
MP<br />
CTNGEN<br />
MP<br />
MP<br />
other<br />
MP<br />
CTNGEN<br />
PC AT<br />
other<br />
IBM<br />
MP<br />
IBM<br />
other<br />
MP<br />
MP<br />
MP<br />
M<br />
M<br />
MP<br />
MP<br />
MP<br />
MP<br />
p<br />
p<br />
p<br />
p<br />
p<br />
h<br />
m<br />
m<br />
m<br />
p<br />
m<br />
m<br />
m<br />
p<br />
m<br />
m<br />
h<br />
p<br />
m<br />
p<br />
m<br />
1<br />
1<br />
m<br />
h<br />
1<br />
1<br />
m<br />
m<br />
p<br />
p<br />
m<br />
m<br />
m<br />
m<br />
m<br />
m<br />
p<br />
p<br />
m<br />
1<br />
p<br />
p<br />
p<br />
p<br />
p<br />
m<br />
m<br />
m<br />
p<br />
m<br />
m<br />
1<br />
p<br />
p<br />
p<br />
p<br />
p<br />
p<br />
p<br />
m<br />
m<br />
3<br />
2<br />
1#<br />
1$#<br />
1$#<br />
2<br />
1$#<br />
1$#<br />
1$#<br />
1#<br />
1#<br />
3#<br />
2<br />
3<br />
1$#<br />
1$<br />
3$<br />
1<br />
3<br />
3$<br />
3<br />
1$<br />
1$<br />
3<br />
1$<br />
1$<br />
1$<br />
1$<br />
1$<br />
1$#<br />
I<br />
1<br />
3<br />
1$<br />
1$<br />
1$<br />
3<br />
3<br />
1$#<br />
1$#<br />
3<br />
3<br />
1$#<br />
1$#<br />
1$#<br />
1$#<br />
1$#<br />
1#<br />
1#<br />
1#<br />
(see next page for footnotes)
Type B Bellows spirometer<br />
C Ceramic element pneumotachometer<br />
D Dry rolling seal spirometer (Horizontal)<br />
F Fleisch-type pneumotachometer<br />
H Screen (Hans Rudolph-type) pneumotachometer<br />
M Mass flowmeter / Hot-wire anemometer<br />
0 Other flow-based spirometer<br />
R Nonwoven resistive element pneumotachometer<br />
S “Swirl meter” pneumotachometer<br />
T Turbine pneumotachometer / Rotameter<br />
V (Vertical) Dry rolling seal<br />
W Water seal spirometer<br />
S<strong>of</strong>tware Version<br />
Version identifier <strong>of</strong> the last version, if more than one tested<br />
Computer<br />
Size<br />
Source<br />
M<br />
APPLE<br />
CTNGEN<br />
IBM<br />
MP<br />
OTHER<br />
PC AT<br />
PPC<br />
TI<br />
Manual<br />
Apple II series<br />
Convergent Technologies N-Gen<br />
IBM Personal Computer, PC/XT, or compatible<br />
Microprocessor based (e.g. Z80, 6502)<br />
Other micro-, mini-, and mainframe computers<br />
IBM Personal Computer Model AT<br />
IBM Portable Personal Computer or compatible<br />
Texas Instruments Pr<strong>of</strong>essional Computer<br />
h Handheld<br />
1 Large, generally not able to move<br />
m Movable, able to move on a small cart<br />
p Portable, able to be hand carried<br />
1 Manufacturer or S<strong>of</strong>tware Company<br />
2 Distributor<br />
3 User<br />
Paid/Observed<br />
$ Indicates testing paid for<br />
# Observed testing<br />
Many model names are trademarks <strong>of</strong> the company listed.<br />
panded the acceptable range for FVC and FEY, to 3.5 percent <strong>of</strong><br />
the known value ( ± 70 ml for volumes less than 2,000 ml). The<br />
acceptable range for FEF25-75% was increased to 5.5 percent <strong>of</strong><br />
the known value or ± 250 mI/s for flows less than 4,545 mI/s. The<br />
ATS Standardization <strong>of</strong> Spirometry- 1987 Updatebo subsequently<br />
adopted these expanded limits for future testing <strong>of</strong>spirometers with<br />
waveform simulators. Since most <strong>of</strong> the testing was performed<br />
BEFORE the 1987 ATS Spirometry standardization update was<br />
published,’#{176} and since some <strong>of</strong> the testing was done as early as<br />
August 1985, some <strong>of</strong> the manufacturers had not updated their<br />
designs-most <strong>of</strong>which were based on the 1979 ATS criteria.3<br />
Each waveform was injected into the spirometer at least once. If<br />
a value was outside the acceptable limit, the waveform in question<br />
was injected multiple additional times to assess whether the<br />
difference was a random occurrence or an inability <strong>of</strong>the spirometry<br />
system to correctly measure the particular waveform. If only the<br />
first measured parameter was outside the acceptable limits, the<br />
parameter was judged acceptable.<br />
For the three manual systems tested, waveforms were handmeasured<br />
by two technicians and rechecked if the volumes meas-<br />
ured by the technicians for FVC and FEV, did not agree to within<br />
± 20 ml or ± 1 percent <strong>of</strong> reading to eliminate human measurement<br />
errors. The FEF25-75% had to agree within ± 50 mI/s or ± 2<br />
percent <strong>of</strong>reading. Only four <strong>of</strong>216 hand-measured values required<br />
rechecking. The results <strong>of</strong> the manual systems were then judged<br />
using the same criteria as the computerized systems.<br />
No spirometer readings were excluded from either the calibrated<br />
syringe or dynamic waveform performance testing unless a technical<br />
error was identified. Technical errors included such problems as<br />
Downloaded From: http://journal.publications.chestnet.org/ on 07/13/2013<br />
not having connections properly attached or inadvertently initiating<br />
a spirometer’s sampling routine after waveform injection had begun.<br />
<strong>Spirometers</strong> that measured FVC,FEV1, and FEF25-75% for each<br />
<strong>of</strong>the 24 waveforms produced a total <strong>of</strong>72 results. Ifthe spirometer<br />
measured 68 or more parameters correctly, it was judged acceptsble.<br />
Three grades for classifying spirometer performance were<br />
used:<br />
Acceptable = 4 or fewer total errors<br />
Marginal=5 to 8 total errors<br />
Unacceptable 9 or more total errors<br />
<strong>Spirometers</strong> were obtained by sending a letter to 83 spirometer<br />
vendors in August 1985 explaining the test procedure and requesting<br />
spirometers for evaluation. Vendors that did not respond to the<br />
initial solicitation were contacted by telephone and follow up letters<br />
advising them <strong>of</strong> our intent to evaluate their spirometer. Vendors<br />
were invited to pay for the testing if they desired to remain<br />
anonymous or wanted testing results from their device prior to<br />
publication. Vendors were also given an opportunity to observe the<br />
testing for an additional fee. Some vendors chose not to pay for the<br />
testing but voluitarily sent spirometers for testing. Other spirom-<br />
eters were obtained from users or distributors. All spirometers,<br />
including those obtained from users rather than vendors, were<br />
calibrated and checked for proper operation prior to evaluation. All<br />
devices were tested with the same protocol. Manufacturers who<br />
paid for testing and sent a device that failed were given prompt<br />
feedback to assist them in correcting the problems. All manufacturers<br />
were given the opportunity to review their results and have<br />
their spirometer retested. Because several manufacturers chose to<br />
have their spirometers retested, the results reported here are from<br />
the most recent testing <strong>of</strong> each spirometer.<br />
RESULTS<br />
Sixty two spirometers were obtained from 37 sources<br />
comprising spirometers from the United States,<br />
United Kingdom, Germany, Holland, and Japan. At<br />
least one spirometer from each <strong>of</strong> the major United<br />
States vendors was tested. Thirty-three (53 percent)<br />
<strong>of</strong> the spirometers were volume-based, and 29 (47<br />
percent) were flow-based. Fifty-nine (95 percent) were<br />
computerized.<br />
Table 1 alphabetically lists the 62 spirometers tested<br />
and the source. The type <strong>of</strong> spirometer, s<strong>of</strong>tware<br />
version, type <strong>of</strong> computer, and size <strong>of</strong> the spirometer<br />
are listed in Table 1. The results listed in the accom-<br />
panying tables apply ONLY to the spirometer model<br />
and s<strong>of</strong>tware version listed in Table 1 . Other models<br />
or s<strong>of</strong>tware versions may yield different results.<br />
Table 2 shows the results <strong>of</strong> the calibrated syringe<br />
testing. Forty-two (68 percent) <strong>of</strong> the 62 systems were<br />
evaluated using the calibrated syringe. For a variety<br />
<strong>of</strong> reasons, three manual and 18 automated systems<br />
were not tested with the calibrated syringe. The<br />
accuracy <strong>of</strong> the spirometers at fast and slow injection<br />
rates is reported. For calibrated syringe testing, the<br />
mean absolute value <strong>of</strong> the accuracy errors (absolute<br />
value <strong>of</strong> [syringe volume - measured volume]) <strong>of</strong> the<br />
remaining devices was 38.4 ml (SD 30.7) for “fast<br />
flows” and 36.0 ml (SD 28.6) for “slow flows.” The<br />
Kinetix Windmill was not included in the absolute<br />
value results because <strong>of</strong> the large errors associated<br />
with this device. Five (12 percent) <strong>of</strong> the 42 devices<br />
CHEST I 97 I 2 I FEBRUARY, 1990 291
(No. 1, 14, 19, 45, 58) had volume errors greater than<br />
the ATS recommended ± 3 percent. All five <strong>of</strong> these<br />
devices were also found not to have acceptable dynamic<br />
waveform results. However, 19 spirometers had<br />
acceptable volume errors with the 3 L syringe but had<br />
unacceptable (12) or marginal (7) dynamic waveform<br />
results. Thirty-four spirometers were tested for stabil-<br />
AEC Spirocomp<br />
Spirometer<br />
Biotrine MultiSpiro PC<br />
CDX 110<br />
Chesebrough-Ponds Respiradyne<br />
Cybermedic CM5<br />
Cybermedic CM31O<br />
Cybermedic Moose<br />
Fukuda Sangyo ST200<br />
Gould 21E<br />
Gould 2180<br />
Gould Spiroscreen<br />
Infomed IFU<br />
Kinetix Windmill<br />
KL Engineering Pneumoscan<br />
LDSH Ohio 822 telemetry<br />
Medical Graphics 1070<br />
MedScience 3200 AT<br />
Omnitek w/Ohio 822<br />
PK Morgan Pocket Respirometer<br />
PK Morgan TTC<br />
Pneumedics Spiroloop<br />
Riko AS500<br />
S&M Inst w/lnfomed<br />
S&M Inst w/Jaeger Screenmate<br />
S&M Inst w/Ohio 822<br />
S&M Inst w/WEC Survey III<br />
SensorMedics Horizon 2<br />
Spirotech 5500<br />
Tenet w/PK Morgan Spir<strong>of</strong>low<br />
VacuMed UCI 500<br />
Vertek VB5000<br />
Vitalograph Compact<br />
Vitalograph PVr II<br />
WE Collins DS 520<br />
WE Collins DS-Plus<br />
-55 112U 93<br />
Mean difference between actual volume and measured volume for 10 calibrated syringe injections<br />
Syringe emptying time less than 1 sec-See methods<br />
Syringe emptying time <strong>of</strong>more than 6 sec-See methods<br />
Change in mean volume (ml) over at least 8 hour period<br />
For volume-based systems, volume linearity is the mean difference in volume between low (1 L) and high volumes (4 L) at start<br />
<strong>of</strong> test (ml); for flow-based systems, the difference in volume between fast and slow emptying rates (ml).<br />
U Unacceptable result (>3% error) with 3 L syringe<br />
*Excluded from absolute average and standard deviation values, error >2SD<br />
Models missing from this table were not tested using a calibrated syringe (see text).<br />
ity. The absolute value <strong>of</strong> the average change in the<br />
measurement <strong>of</strong> the 3 L syringe volume over eight<br />
hours was 37.9 ml (SD 28.2). The AEC Spirocomp<br />
had a stability error greater than 3 percent <strong>of</strong> the<br />
syringe volume. This device was also found to be<br />
unacceptable during dynamic waveform testing.<br />
The final column in Table 2 shows the largest change<br />
Table 2-Accuracy, Stability and linearity <strong>of</strong><strong>Spirometers</strong> Thsted Using 3 L Calibrated Syringe<br />
-<br />
Accuracy (ml)<br />
-<br />
Model Fast Slow Stability, ml Vol Linear, ml<br />
WE Collins Eagle!! w/pneumotach<br />
WE Collins MLA 3000<br />
Spirometer 2<br />
Spirometer 3<br />
Spirometer 7<br />
Spirometer 8<br />
Spirometer 9<br />
Accuracy<br />
Fast<br />
Slow<br />
Stability<br />
Vol Linear<br />
-39<br />
-51<br />
. -12<br />
-27<br />
-87<br />
-60<br />
55<br />
86<br />
-97U<br />
-21<br />
3185U<br />
-50<br />
-81<br />
-11<br />
-16<br />
-21<br />
-7<br />
-72<br />
-31<br />
28<br />
10<br />
61<br />
89<br />
13<br />
0<br />
8<br />
0<br />
47<br />
-94U<br />
-1<br />
-3<br />
-52<br />
-4<br />
-34<br />
-36<br />
-20<br />
99U<br />
39<br />
17<br />
39<br />
292 <strong>Performance</strong> <strong>Evaluation</strong> 01 <strong>Contemporary</strong> <strong>Spirometers</strong> (Nelson eta!)<br />
Downloaded From: http://journal.publications.chestnet.org/ on 07/13/2013<br />
-16<br />
-51<br />
65<br />
-8<br />
-40<br />
-17<br />
-69<br />
44<br />
8<br />
- 126U<br />
-27<br />
-14845U<br />
-38<br />
11<br />
10<br />
6<br />
-67<br />
-26<br />
-10<br />
-13<br />
65<br />
23<br />
-79<br />
-27<br />
-48<br />
-38<br />
-43<br />
-10<br />
-55<br />
-36<br />
47<br />
11<br />
31<br />
-2<br />
6<br />
16<br />
29<br />
-67<br />
-21<br />
22<br />
-88<br />
-21<br />
-18<br />
18<br />
38<br />
84<br />
57<br />
16<br />
58<br />
72<br />
47<br />
54<br />
11<br />
40<br />
89<br />
47<br />
40<br />
16<br />
18<br />
3<br />
11<br />
8<br />
-22<br />
79<br />
-38<br />
34<br />
21<br />
9<br />
31<br />
82<br />
-14<br />
3<br />
8<br />
167<br />
23<br />
116<br />
81<br />
106<br />
26<br />
41<br />
119<br />
79<br />
104<br />
46<br />
163<br />
1802*<br />
17<br />
93<br />
10<br />
34<br />
98<br />
128<br />
34<br />
39<br />
34<br />
105<br />
18<br />
76<br />
61<br />
100<br />
42<br />
6<br />
188<br />
78<br />
30<br />
89<br />
23<br />
32<br />
114<br />
9<br />
85<br />
170<br />
106<br />
21<br />
13
Table 3-&#{231}formance <strong>Evaluation</strong><br />
FVC FEy, FEF2S-75% Total Perf<br />
Spirometer Model No. No. No. No. Bating MilYr<br />
AEC Spirocomp 8D 1 10 19 U 1/86<br />
Biotrine MultiSpiro PC 0 OB 0 0 A 1L/85<br />
Brentwood Spiroscan 2000 0 0 0 0 A 10/88<br />
CDX1OI 3D 1 1 5 M 2/86<br />
CDX11O 2D OV 0 2 A 1186<br />
Chesebrough-Fbnds Respiradyne (1) ff1’ 1V 5 12 U 12/85<br />
Cybermedic CM5 OF 1 0 1 A 12/85<br />
Cybermedic CM31O iF 3 0 4 A 12/85<br />
Cybermedic Moose OF 1 0 1 A 12/85<br />
Fukuda Sangyo ST200 7D 2 5 14 U Sf86<br />
CouldMRl 2D 3 7 12 U 2/86<br />
Gould2lE 0 OV 0 0 A 3/86<br />
Gould2lflO 0 1V 2 3 A 3/86<br />
GouldSpiroscreen(2) 4 IV 1 6 M 3/86<br />
InfomedlFU 2T 3B 0 5 M 2/86<br />
Infomed MWS 6000 2T OB 0 2 A 3/86<br />
Kinetix Windmill 23 23 X 46 U 2/86<br />
KL Engineering Pneumoscan 12N 5 X 17 U 2/86<br />
LDSH Ohio 822 telemetry (3) 0 OB 0 0 A 7/85<br />
Med Equip Design Autospiro (4) 17 20 1 38 U 6/86<br />
Medical Graphics 1070 0 OB 0 0 A 12/85<br />
MedScience3200AT 0 OB 0 0 A 0/85<br />
NIOSH(5) 0 0 0 0 A 5(87<br />
Omnitek w/Ohio 822 (6) 0 1 0 1 A 1/86<br />
PK Morgan Pocket Respirometer (7) 17 13 X 30 U 1/86<br />
PK Morgan SPIROFLOW 12 0 0 0 0 A 8/88<br />
PK Morgan TTC 4 OB 3 7 M<br />
Pneumedics Dataloop 0 2 2 4 A 1/87<br />
Pneumedics Spiroloop 11 lB 8 20 U 1/86<br />
Puritan-Bennett VS400 2 2 3 7 M 4/86<br />
RikoAS500(8) 0 0 2 2 A 12/85<br />
S&Mlnstw/Infomed 0 4 2 6 M 10/85<br />
S&M Inst wfJaeger Screenmate 6 0 2 8 M 3/86<br />
S&M Inst w/Mijnhardt 0 1 0 1 A 3/87<br />
S&Mlnstw/Ohio822 0 0 0 0 A 9/85<br />
S&M Inst w/WE Collins Survey 3 0 0 1 1 A 9/85<br />
SensorMedics Horizon 2 0 OV 0 0 A 8/85<br />
Sherwood Medical Respiradyne II 0 3 0 3 A 7/88<br />
SpirometncsSMl3 0 0 1 1 A 1/87<br />
SpirotechS500 0 0 0 0 A 10/85<br />
Tenet wfPK Morgan Spir<strong>of</strong>low 0 7 0 7 M 3/86<br />
VacuMedUCI500 0 1 2 3 A 3/86<br />
VertekVRS000 0 11 X 11 U 1/86<br />
Vitalograph Alpha 0 0 0 0 A 5/88<br />
Vitalograph Compact 3 1E 4 8 M 3/86<br />
Vitalograph PVf II 0 1 2 3 A 1/86<br />
WECollinsDS5ZO 1 OB 9 10 U 4/86<br />
WE Collins DS 560 0 0 1 1 A 4/86<br />
WE Collins DS-Plus 0 OV 0 0 A<br />
WE Collins Eaglell w/pneumotach 6N 0 6 12 AQ<br />
WE Collins Eaglell w/Survey 0 1 0 1 A 9/85<br />
WE Collins MLA 3000 0 lB 0 1 A 3/86<br />
WE Collins Respirometer 13.5L 0 2 0 2 A 4/86<br />
Spirometer 1 15 18 4 37 U<br />
Spirometer 2 13 10 3 26 U<br />
Spirometer 3 6 1V 8 15 U<br />
Spirometer4 13 8 5 26 U<br />
Spirometer5 3 8 7 18 U<br />
Spirometer6 7D 0 4 11 U<br />
Spirometer 7 21 14B 12 47 U<br />
Spirometer8 1 lB 1 3 A 2/86<br />
Spirometer 9 0 lB 2 3 A 2/86<br />
Downloaded From: http://journal.publications.chestnet.org/ on 07/13/2013<br />
Test<br />
Date<br />
(see next page for footnotes)<br />
CHEST I 97 I 2 I FEBRUARY, 1990 293
Notes:<br />
A Acceptable performance<br />
B Performs back-extrapolation, but does not indicate extrapolated volumes >10%<br />
D Has greater than average instability, should be rezeroed more frequently than once a day<br />
E Waveforms with large extrapolated volumes were marked unacceptable, values could not be saved or printed<br />
F Meets FVC accuracy recommendation only in the manual end-<strong>of</strong>-test mode<br />
M Marginal performance<br />
N Not accurate due to noise from simulator<br />
Q Qualified acceptable based on tests other than FVC<br />
R Chart recorder should be running before starting FVC<br />
T Terminates data collection at 10 seconds<br />
U Unacceptable performance<br />
V Either displays extrapolated volume or % for all tests, or warns <strong>of</strong>extrapolated volumes greater than 5% <strong>of</strong> FVC<br />
X Not measured<br />
Date Period during which final version <strong>of</strong> s<strong>of</strong>tware was tested<br />
(1) New version now manufactured by Sherwood Medical see Sherwood Medical Respirodyne II.<br />
(2) Also sold by Quinton and <strong>Chest</strong> (Japan)<br />
(3) LDSH = LDS Hospital (See Reference 16)<br />
(4) NIOSH = National Institutes <strong>of</strong>Occupational Safety and Health-a specially designed computerized spirometer system.<br />
(5) Manufactured by <strong>Chest</strong> (Japan)<br />
(6) Now manufactured by Zao Medical Systems<br />
(7) Manufactured by Micro Medical Instruments (UK)<br />
(8) Also sold by Minata (Japan)<br />
The results listed apply ONLY to the spirometer model and s<strong>of</strong>tware version lLsted in Table 1, other nwdets or s<strong>of</strong>tware versions may yield<br />
different result& The ability to measure extrapolated volume was NOT used to rate spimmeters. <strong>Evaluation</strong> results and lLsting <strong>of</strong> brand names<br />
does not constitute endorsement or approval by the University <strong>of</strong> Utah, the authors, or the American College <strong>of</strong><strong>Chest</strong> Physician&<br />
in the volume linearity test for each spirometer. The<br />
absolute value <strong>of</strong>the average difference over the tested<br />
range <strong>of</strong> flow or volume was 71 ml (SD 49. 1). Sixteen<br />
spirometers (38 percent) had differences greater than<br />
3 percent <strong>of</strong> the syringe volume. Five <strong>of</strong> these 16<br />
performed acceptably on the waveform evaluation.<br />
The results for dynamic waveform testing are shown<br />
in Table 3. Dynamic testing showed 35 (56.5 percent)<br />
spirometers acceptably measured the 24 standard<br />
waveforms. Nine (14.5 percent) were marginal and 18<br />
(29.0 percent) were unacceptable. Note that 15 spirometers<br />
measured the three spirometric parameters<br />
on all 24 waveforms without any errors. All 62 spirom-<br />
eters tested were capable <strong>of</strong>measuring FVC and FEy,,<br />
and all but four spirometers measured FEF25-75%.<br />
Because <strong>of</strong>high frequency noise that may have been<br />
generated by the waveform simulator, the WE Collins<br />
Eagle and the KL Engineering Pneumoscan, both<br />
flow-based devices, were unable to consistently determine<br />
the end-<strong>of</strong>-test for FVC. The WE Collins Eagle<br />
was given a qualified acceptable rating because it had<br />
no FEy, errors and the six FVC noise induced errors<br />
were the likely cause <strong>of</strong> the six FEF25-75% errors.<br />
These two spirometers did not appear to have adequate<br />
data smoothing functions, which are not addressed in<br />
the performance recommendations. However, good<br />
design practice usually filters out unwanted high<br />
frequency noise. In addition, the mechanical charac-<br />
teristics <strong>of</strong> rotameters <strong>of</strong> “stall before start and spin<br />
after stop” are ti’5 The pump created less<br />
than 1 ml bursts at low flows which could have caused<br />
an overestimation <strong>of</strong> the volume accumulated by<br />
rotameters. Two rotameter devices (No. 19 and 20),<br />
which each had more than 17 errors each with the<br />
dynamic waveforms, also failed the 3 L syringe test so<br />
their flaws were not due to test pump problems. The<br />
P.K. Morgan Pocket Respirometer had 30 errors and<br />
did poorly with the 3 L syringe testing.<br />
The Chesebrough-Ponds Respiradyne terminated<br />
data collection at eight seconds, and the two Infomed<br />
systems at ten seconds, which was not long enough to<br />
accurately measure the FVC <strong>of</strong> all 24 standard wave-<br />
294 <strong>Performance</strong> <strong>Evaluation</strong> <strong>of</strong> <strong>Contemporary</strong> <strong>Spirometers</strong> (Nelson a! a!)<br />
Downloaded From: http://journal.publications.chestnet.org/ on 07/13/2013<br />
forms.<br />
Eleven <strong>of</strong> the 59 automated systems (20 percent)<br />
either displayed the actual extrapolated volume or<br />
marked tests as unacceptable when extrapolated volume<br />
exceeded 5 percent. Twenty-seven (49 percent)<br />
identffied extrapolated volumes which exceeded 10<br />
percent. Seventeen (31 percent) did not provide any<br />
warning about large extrapolated volumes. Recently,<br />
the ATS has suggested that the extrapolated volumes<br />
not exceed 5 percent <strong>of</strong> the FVC.’#{176}Ability to aecu-<br />
rately measure extrapolated volume was not used to<br />
rate the spirometers.<br />
Fifty-four spirometers (93 percent) measured<br />
FEF25-75%. Several spirometers had errors in<br />
FEF25-75% most likely because <strong>of</strong>an insufficient data<br />
sampling rate.’#{176}-’’8 The FVC and FEy1 do not appear<br />
to be as sensitive to slow data sampling rates. Since<br />
FEF25-75% depends on accurate time and volume<br />
samples at two points, it is more easily affected by<br />
slow sample rates, typically
Table 4-Number <strong>of</strong>Errors by Waveform and Parameter<br />
For 46 <strong>of</strong>the <strong>Spirometers</strong> Tested<br />
Waveform FVC FEVI FEF25-75% Total<br />
1 0 1 1 2<br />
2 0 1 5 6<br />
3 3 1 0 4<br />
4 1 2 1 4<br />
5 3 3 4 10<br />
6 4 5 7 16<br />
7 0 13 0 13<br />
8 5 5 4 14<br />
9 1 1 4 6<br />
10 3 3 2 8<br />
11 3 0 0 3<br />
12 4 1 5 10<br />
13 0 4 3 7<br />
14 2 3 2 7<br />
15 0 2 8 10<br />
16 1 5 1 7<br />
17 10 1 2 13<br />
18 0 0 0 0<br />
19 11 1 5 17<br />
20 2 1 0 3<br />
21 0 1 10 11<br />
22 6 1 4 11<br />
23 6 2 0 8<br />
24 2 0 0 2<br />
Total 67 57 68 192<br />
*Several <strong>of</strong> the spirometers were not included because they had<br />
such a large number <strong>of</strong> errors.<br />
some spirometers had such a large number <strong>of</strong> errors.<br />
Note that only one waveform (No. 18) had no errors<br />
for the three parameters measured. Also <strong>of</strong> interest is<br />
the fact that the errors were almost uniformly spread<br />
over the three parameters-67 for FVC, 57 for FEy1,<br />
and 68 for FEF25-75%.<br />
Fifty-seven automated spirometry systems (95 per-<br />
cent) measured peak flow (FEFmax). Volume-based<br />
spirometers that require manual calculations do not<br />
provide an accurate method <strong>of</strong> measuring instantane-<br />
otis flow;’7-’8 consequently, it was not measured in the<br />
manual devices. Peak flow is dependent on numerous<br />
factors that were not readily determinable, including<br />
the natural frequency <strong>of</strong> the system, data sampling<br />
rate, and filtering algorithms. Therefore, peak flow<br />
Type Total<br />
was not used in the qualification criteria.<br />
Table 5 shows performance by spirometer type. All<br />
bellows spirometers performed acceptably. The only<br />
water-seal spirometer found unacceptable used s<strong>of</strong>t-<br />
ware written in 1978 (WE. Collins DS520). In addi-<br />
tion, at least 50 percent <strong>of</strong> the following spirometer<br />
types performed acceptably: horizontal dry rolling<br />
seal, Fleisch pneumotach, and ceramic pneumotachs.<br />
All turbine flowmeters performed 19<br />
The calibrated syringe and dynamic waveform test-<br />
ing results were examined to determine whether<br />
calibrated syringe testing alone was adequate to dif-<br />
ferentiate acceptable from unacceptable spirometer<br />
performance with dynamic waveform testing. None <strong>of</strong><br />
the spirometers which failed the calibrated syringe<br />
testing passed the dynamic waveform testing. How-<br />
ever, testing with the 3 L syringe alone did not<br />
differentiate between all acceptable and unacceptable<br />
spirometers except for spirometers that exhibited<br />
gross errors.<br />
DISCusSIoN<br />
The performance criteria used were based on the<br />
ATS recommendations3 and earlier testing and stan-<br />
dardization criteria.4-5-7 The major changes from the<br />
earlier methods were additional waveforms, more<br />
sophisticated end <strong>of</strong> test criteria, and a relaxation <strong>of</strong><br />
the limits <strong>of</strong> acceptability, which were all based on<br />
studies published since the 1979 ATS recommenda-<br />
tions.5’7<br />
Table 5-Pe,’formance by Spirometer Type<br />
An important addition to the earlier ATS recom-<br />
mendations was the allowance <strong>of</strong> a 5 percent random<br />
error rate. The authors felt that the 5 percent rate was<br />
necessary due to the complex interactions <strong>of</strong> the<br />
computer-controlled air pump and spirometry system.<br />
Much <strong>of</strong> the testing predated the acceptance and<br />
publication <strong>of</strong> the 1987 ATS spirometry standardiza-<br />
tion update.b0 Even though the waveforms recom-<br />
mended for testing spirometers were published in<br />
1982, most manufacturers had not tested their spi-<br />
rometers with the new waveforms.<br />
Compared to earlier testing studies, there was an<br />
overall improvement in spirometer performance. 1.4.6<br />
Acceptable<br />
(%)<br />
Marginal<br />
(%)<br />
Unacceptable<br />
Bellows 5 5 (100) 0 (0) 0 (0)<br />
Water seal 7 6 (86) 0 (0) 1 (14)<br />
Dry rolling seal (horizontal) 13 9 (69) 4 (31) 0 (0)<br />
Ceramic pneumotachometer 4 2 (50) 1 (25) 1 (25)<br />
Fleisch pneumotachometer 8 4 (50) 1 (13) 3 (38)<br />
Miscellaneous flowmeters 9 4 (44) 1 (11) 4 (44)<br />
Hans Rudolph (screen) pneumotach 5 2 (40) 1 (20) 2 (40)<br />
Vertical-Dry rolling seal 8 3 (38) 1 (12) 4 (50)<br />
Turbine flowmeter 3 0 (0) 0 (0) 3 (100)<br />
Total 62 35 (56.5) 9 (14.5) 18 (29.0)<br />
Downloaded From: http://journal.publications.chestnet.org/ on 07/13/2013<br />
(%)<br />
CHEST I 97 I 2 1 FEBRUARY, 1990 295
The results shown here are probably indicative <strong>of</strong> the<br />
“best-case” attainable when a device is properly used<br />
and maintained by well-trained personnel. Histori-<br />
cally, flow-based spirometers have been less accurate<br />
than volume-based 1,4.6 The present study<br />
shows 12 <strong>of</strong> 29 flow-based spirometers (41 percent)<br />
met the criteria for acceptable performance. Twenty-<br />
four <strong>of</strong> the 34 volume-based spirometers (71 percent)<br />
performed acceptably. While flow-based spirometers<br />
have improved, as a group they did not perform as<br />
well as the volume-based devices.<br />
The flow-based spirometers found to be unaccept-<br />
able were all intended to be used as portable screening<br />
units. By contrast, all <strong>of</strong> the laboratory-based flow<br />
systems were found acceptable. Several recent authors<br />
have implied that cheap spirometers are “good<br />
enough” for bedside patient evaluation, regardless <strong>of</strong><br />
their accuracy. Indeed, one paper shows numer-<br />
ous errors in FVC greater than 30 percent, then<br />
pronounces the spirometer being evaluated “a useful<br />
tool.” The present study shows that accurate flow-<br />
based spirometers can be manufactured inexpensively.<br />
Although using a 3 L syringe for quality control<br />
purposes is essential, simple testing <strong>of</strong> spirometers<br />
with a 3 L calibrating syringe for validation purposes<br />
was found to be an inadequate method <strong>of</strong> assessing<br />
spirometer performance when compared to dynamic<br />
waveform testing. Dynamic waveform testing is essen-<br />
tial to accurately measure and validate acceptability<br />
<strong>of</strong> spirometer system performance. We make this<br />
statement because we found spirometers that did not<br />
measure the 3 L syringe appropriately did not measure<br />
dynamic waveforms correctly either. Once a spirometer<br />
and its associated algorithths have been validated<br />
to be correct, quality control testing with a 3 L syringe<br />
will be able to monitor for calibration errors that arise<br />
due to aging, blocked sensors, leaks, etc. Testing with<br />
a calibrated syringe, however, cannot be used to<br />
determine whether the measurements other than total<br />
volume are accurate, since the syringe cannot recreate<br />
a test waveform reproducibly.<br />
S<strong>of</strong>tware problems, or “bugs:’ were found in 15 (25<br />
percent) <strong>of</strong>the 59 computerized systems. For example,<br />
some spirometers required a calibration syringe with<br />
exactly 3.000 L volume, and could not adapt to volumes<br />
such as the 3.021 L used in our testing. While 21 ml<br />
is a small volume, the error budget is only ± 90 ml<br />
and a 21 ml error is 23 percent <strong>of</strong> the error budget.<br />
One spirometer had an inadequate sample rate, caus-<br />
ing FEFma, to be overestimated by more than 200<br />
percent. The s<strong>of</strong>tware used by the Vitalograph Com-<br />
pact was a European version, not intended for distri-<br />
bution in the United States and used a method for<br />
determining start- and end-<strong>of</strong>-test different from the<br />
ATS recommendations. The results therefore may not<br />
be indicative <strong>of</strong> the performance <strong>of</strong> the device cur-<br />
rently being marketed in the United States with the<br />
same name.<br />
The authors believe that most <strong>of</strong> the nine spirome-<br />
ters with marginal performance could be brought to<br />
an acceptable level <strong>of</strong> performance with more careful<br />
s<strong>of</strong>tware design and testing. The potential to correct<br />
these problems was evident by the number <strong>of</strong> devices<br />
that met performance criteria after vendors were<br />
allowed to make changes in s<strong>of</strong>tware and resubmit<br />
their device for testing.<br />
Other important properties <strong>of</strong> spirometers which<br />
could be <strong>of</strong> importance which were not exhaustively<br />
tested included the following: (1) Air leaks-we made<br />
certain there were none when the testing was done.<br />
Air leaks can cause major errors in the clinical<br />
situation. (2) BTPS correction factors -Our testing<br />
was done with ambient room air. BTPS correction<br />
factors can cause errors <strong>of</strong> more than 10 percent and<br />
are complex to study because <strong>of</strong>varying tubing lengths<br />
before the flow or volume transducers and because <strong>of</strong><br />
ambient temperature effects.23 (3) Backpressure<br />
caused by the resistance <strong>of</strong> the flow or volume<br />
transducer-we tested about ten different types <strong>of</strong><br />
devices and found for waveform No. 2 that the peak<br />
pressure was about 1 cm H2O/L/s, well below the ATS<br />
recommendation <strong>of</strong> 1.5 cm H2O/LIs. (4) Effect <strong>of</strong><br />
manufacturing variability-We cannot be sure how<br />
well a different spirometer <strong>of</strong> the same model from<br />
the same manufacturer will perform because we tested<br />
only one instrument for each model. (5) <strong>Performance</strong><br />
over time - several <strong>of</strong> the devices tested had been in<br />
field use, but we did not test most devices after they<br />
had been in long term use. None <strong>of</strong> the spirometers<br />
was tested over time while in clinical use.<br />
In conclusion, we found that only 35 <strong>of</strong> 62 (56.5<br />
percent) spirometers performed acceptably. With such<br />
a high failure rate, spirometer purchasers should be<br />
certain that the spirometers they acquire meet ATS<br />
recommendations as validated by independent labo-<br />
ratories. We observed s<strong>of</strong>tware problems in 25 percent<br />
<strong>of</strong> the spirometers. These problems were fixed before<br />
final testing. These s<strong>of</strong>tware problems included large,<br />
complex spirometry systems as well as inexpensive<br />
handheld units. We also found that validating the<br />
accuracy <strong>of</strong> a spirometer with a calibrated 3 L syringe<br />
alone was not sufficient to demonstrate how well a<br />
spirometer would perform with dynamic patient wave-<br />
296 <strong>Performance</strong> <strong>Evaluation</strong> <strong>of</strong> <strong>Contemporary</strong> <strong>Spirometers</strong> (Nelson eta!)<br />
Downloaded From: http://journal.publications.chestnet.org/ on 07/13/2013<br />
forms.<br />
Substantial time has passed since the initial testing<br />
was completed. It is likely that changes have been<br />
made in basic equipment and computer systems. Test<br />
results may, therefore, not apply to current devices.<br />
<strong>Spirometers</strong> should meet the 1987 ATS recommenda-<br />
tions which are set as a lower limit <strong>of</strong> acceptable<br />
performance and not as an upper limit or design<br />
criteria.
ACKNOWLEDGMENTS: We thank the spirometer manufacturers,<br />
vendors and users who participated in our testing. Also we thank<br />
Steven L. Berlin for technical assistance in doing some <strong>of</strong> the more<br />
recent testing. Device 28 was provided to us by the Harvard School<br />
<strong>of</strong> Public Health and is being used for the Acid Aerosol Health<br />
Effects in North American Children Study.” We thank them for<br />
making the equipment available.<br />
REFERENCES<br />
1 FitzGerald MX, Smith AA, Gaensler EA. <strong>Evaluation</strong> <strong>of</strong> “elec-<br />
tronic” spirometers. N EngI J Med 1973; 289:1283-86<br />
2 Morgan WKC, Chairman. Committee recommendations: The<br />
assessment <strong>of</strong>ventilatory capacity: Statement <strong>of</strong>the committees<br />
on environmental health and respiratory physiology. <strong>Chest</strong> 1975;<br />
67:95-97<br />
3 Gardner RM, Chairman. ATS Statement-Snowbird workshop<br />
on standardization <strong>of</strong> spirometry. Am Rev Respir Dis 1979;<br />
119:831-38<br />
4 Gardner RM, Hankinson JL, West BJ. Evaluating commercially<br />
available spirometers. Am Rev Respir Dis 1980; 121:73-82<br />
5 Association for the Advancement <strong>of</strong> Medical Instrumentation.<br />
Standards for spirometers (Draft). AAMI, Arlington, VA, 1980<br />
6 Wever AMJ, Britton MG, Hughes DTD, van der Plas KH,<br />
Wever-Hess J. Clinical evaluation <strong>of</strong> five spirometers. Eur J<br />
Respir Dis 1981; 62:127-37<br />
7 Hankinson JL, Gardner RM . Standard waveforms for spirometer<br />
testing. Am Rev Respir Dis 1982; 126:362-64<br />
8 Sobol BJ. Spirometry and forced flow studies. In: Chusid EL.<br />
The selective and comprehensive testing <strong>of</strong> adult pulmonary<br />
function. Mount Kisco, NY: Futura Publishing, 1983<br />
9 Enright PL, Hyatt RE. Office spirometry. Philadelphia: Lea &<br />
Febiger, 1987<br />
10 Gardner RM, Hankinson JL, Clausen JL, Crapo RO, Johnson<br />
RL Jr. Epler GR. ATS Statement on Standardization <strong>of</strong> Spirometry-<br />
1987 Update. Am Rev Respir Dis 1987; 136:1285-98<br />
Downloaded From: http://journal.publications.chestnet.org/ on 07/13/2013<br />
11 Glindmeyer HW, Harwood C. A compact computer printer for<br />
quality control spirometric data collection. J Occup Med 1982;<br />
24:1003-07<br />
12 Morris All, Kanner RE, Crapo RO, Gardner RM. Clinical<br />
pulmonary function testing. 2nd ed. Salt Lake City, UT:<br />
Intermountain Thoracic Society, 1984<br />
13 Nelson SB, Gardner RM . Computer-controlled spirometry wave<br />
form simulator. Respir Care 1986; 31:964<br />
14 Nelson SB. Commercially available spirometers: a performance<br />
evaluation. MS Thesis, University <strong>of</strong> Utah, Salt Lake City, 1987<br />
15 Yeh MP, Adams TD, Gardner RM, Yanowitz FG. Turbine<br />
flowmeter vs Fleisch pneumotachometer: A comparative study<br />
for exercise testing. J Appi Physiol 1987; 63: 1289-95<br />
16 Ostler DV, Gardner RM, Crapo RO. A computer system for<br />
analysis and transmission <strong>of</strong>spirometry waveforms using volume<br />
sampling. Comptit Biomed Res 1984; 17:229-40<br />
17 Gardner RM, Crapo RO, Billings RG, Shigeoka JW, Hankinson<br />
JL. Spirometry: what paper speed? <strong>Chest</strong> 1983; 84:161-65<br />
18 Nelson SB, Gardner RM, Crapo RO, Jensen RL. Variability <strong>of</strong><br />
instantaneous flow measurements in spirometers. Am Rev Respir<br />
Dis 1987; 135:68<br />
19 Yeh MP, Adams TD, Gardner RM, Yanowitz FG. Rotameter<br />
flowmeter: its implications to exercise testing. J Appl Physiol<br />
1987; 63:1289-95<br />
20 Gs,nawardena KA, Houston K, Smith AP <strong>Evaluation</strong> <strong>of</strong> the<br />
turbine pocket spirometer. Thorax 1987; 42:689-93<br />
21 Zimnicki GL, Kline JL, MacDonell RJ. <strong>Evaluation</strong> <strong>of</strong> the<br />
Respiradyne pulmonary function monitor. Respir Care 1987;<br />
32:261-67<br />
22 Hess D, Chieppor PJ, Johnson K. An evahiation <strong>of</strong> the Respiradyne<br />
II spirometer. Respir Care 1987; 32:1123-30<br />
23 Hankinson JL, Viola JO. Dynamic BTPS correction factors for<br />
spirometric data. J Appl Physiol: Respir Environ Exercise<br />
Physiol 1983; 44:1353-60<br />
CHEST I 97 I 2 I FEBRUARY, 1990 297