Urology & Kidney Disease News Fall 2009 - Cleveland Clinic
Urology & Kidney Disease News Fall 2009 - Cleveland Clinic
Urology & Kidney Disease News Fall 2009 - Cleveland Clinic
Create successful ePaper yourself
Turn your PDF publications into a flip-book with our unique Google optimized e-Paper software.
32 <strong>Urology</strong> & <strong>Kidney</strong> <strong>Disease</strong> <strong>News</strong><br />
Robotics and Laparoscopy<br />
Laparoscopic Surgery Without Visible Scars:<br />
Experience with the First 100 Cases<br />
Jihad Kaouk, MD, Robert Stein, MD, Courtenay Moore, MD,<br />
and Raymond Rackley, MD<br />
In the past 2 years, the surgical community has witnessed<br />
an exciting foray into the burgeoning field of single-port<br />
laparoscopic or laparoendoscopic single site (LESS) surgery.<br />
Developed as an extension of standard laparoscopy that<br />
requires 3 to 6 small incisions, LESS seeks to minimize<br />
patient discomfort, shorten convalescence, and improve<br />
cosmesis by placing all instruments through a readily concealed<br />
2cm incision mostly within the umbilicus. Initial<br />
series have been published that extol the safety, aesthetics,<br />
and superior pain profile of the single-port approach. However,<br />
questions remain regarding the comparative benefit of<br />
LESS, its applicability, its potentially lengthy learning curve,<br />
and technical limitations of existing instrumentation.<br />
We present our initial experience with 100 patients who underwent<br />
LESS urologic surgery from September 2007 to February<br />
<strong>2009</strong>. Specifically, 74 patients underwent LESS renal<br />
surgery (cryoablation, 8; partial nephrectomy, 15; metastectomy,<br />
1; renal biopsy, 1; simple nephrectomy, 7; radical<br />
nephrectomy, 6; cyst decortication, 2; nephroureterectomy,<br />
7; donor nephrectomy, 19; and dismembered pyeloplasty,<br />
8) and 26 patients underwent LESS pelvic surgery (varicocelectomy,<br />
3; radical prostatectomy, 6; radical cystectomy,<br />
3; sacral colpopexy, 13; and ureteral reimplant, 1). Mean<br />
patient age was 54 years.<br />
<br />
<br />
Mean operative time was 199 minutes. Estimated blood<br />
loss was 136 mL. No intraoperative complications occurred.<br />
Six patients required conversion to standard laparoscopy.<br />
Mean length of hospitalization was 3 days. Mean Visual<br />
Analog Pain Scale score at discharge was 1.5/10. At a mean<br />
follow-up of 11 months, 9 Clavien Grade II (transfusion, 7;<br />
urinary tract infection, 1; deep vein thrombosis, 1) and 2<br />
Clavien Grade IIIb (recto-urethral fistula, 1; angioembolization,<br />
1) surgical complications occurred.<br />
Based on our initial experience that represents one of the<br />
largest experiences in this technique worldwide, LESS urologic<br />
surgery is safe, offers improved patient cosmesis and<br />
decreased pain, and can be performed with a modicum of<br />
laparoscopic skills. Its superiority compared to traditional<br />
laparoscopy is currently speculative. As such, a prospective,<br />
randomized trial is under way to better define its role.<br />
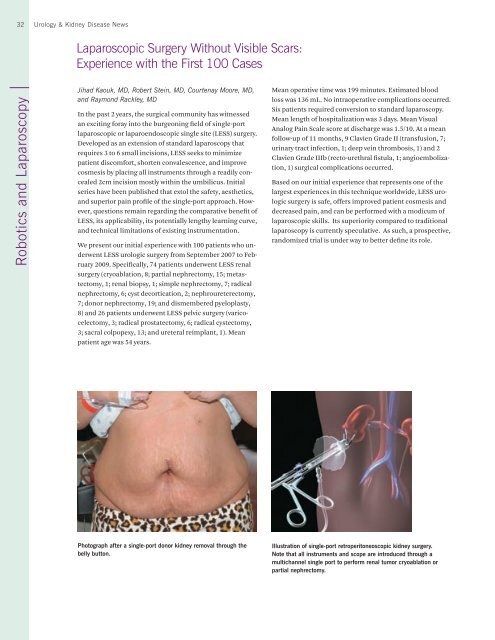
Illustration of single-port retroperitoneoscopic kidney surgery.<br />
Note that all instruments and scope are introduced through a<br />
<br />
partial nephrectomy.