Intraocular Photodisruption With Picosecond and Nanosecond Laser
Intraocular Photodisruption With Picosecond and Nanosecond Laser
Intraocular Photodisruption With Picosecond and Nanosecond Laser
Create successful ePaper yourself
Turn your PDF publications into a flip-book with our unique Google optimized e-Paper software.
Tissue Effects of <strong>Picosecond</strong> <strong>and</strong> <strong>Nanosecond</strong> <strong>Photodisruption</strong> 3041<br />
800jinr<br />
200|j,nr<br />
Ax<br />
400|anr<br />
600[iri<br />
RPE<br />
location of<br />
laser focus<br />
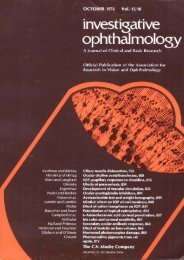
FIGURE 10. Macrophotograph of laser effects within the retina caused by ps pulses with a<br />
pulse energy of 200 n]. Ax is the distance between the laser focus in the vitreous <strong>and</strong> the<br />
retinal vessels as adjusted in the cenLer of each line of laser exposures. At the sides of each<br />
line, the laser focus was located within the retina or at the pigment epithelium. Focusing<br />
directly onto a vessel always caused a hemorrhage. The arrow indicates a vessel showing no<br />
macroscopic damage when the laser pulses had been focused on the pigment epithelium, that<br />
is, at a level about-300 fim below the vessel.<br />
by the bubble expansion <strong>and</strong> partly by the jet formation<br />
during bubble collapse, which is described elsewhere.<br />
714 Although the extent of tissue disruption by<br />
cavitation varies from case to case <strong>and</strong> decreases when<br />
the pulse energy is reduced, it is apparently the largest<br />
obstacle to a spatial confinement of the effects of intraocular<br />
photodisruption.<br />
Potential Applications of <strong>Picosecond</strong> Pulses<br />
<strong>Picosecond</strong> laser pulses can, in principle, be applied<br />
for all indications for which nanosecond pulses are<br />
presently used, whereby they offer the advantage of a<br />
reduced damage range. When very fine tissue effects<br />
are intended or when the application site is very close<br />
to sensitive ocular structures, such as the corneal endothelium<br />
or the retina, picosecond pulses are likely to<br />
be the only means to achieve the surgical aim. Possible<br />
new applications of this kind are corneal intrastromal<br />
refractive surgery, cataract fragmentation, <strong>and</strong> vitreous<br />
surgery close to the retina. Other uses could be<br />
trabeculopuncture for treatment of glaucoma <strong>and</strong>, as<br />
Figure 5 shows, the selective removal of a cell layer on<br />
a tissue surface, for example, polishing a lens capsule<br />
after cataract surgery.<br />
Intrastromal refractive surgery. Several authors have<br />
put forward the idea that refractive changes of the<br />
cornea may be achieved by removal of an intrastromal<br />
tissue layer through plasma-mediated evaporation.<br />
1115 " 17 They have expressed the hope that the corneal<br />
curvature can be changed without damaging the<br />
corneal epithelium, Bowman's membrane, or the endothelium,<br />
<strong>and</strong> that thereby the haze <strong>and</strong> regression<br />
arising during the healing process of the cornea can be<br />
diminished. This aim cannot be accomplished using<br />
conventional photodisruptors delivering nanosecond<br />
laser pulses because their tissue effects are too<br />
coarse. 715 If, as an alternative, the ps laser is used for