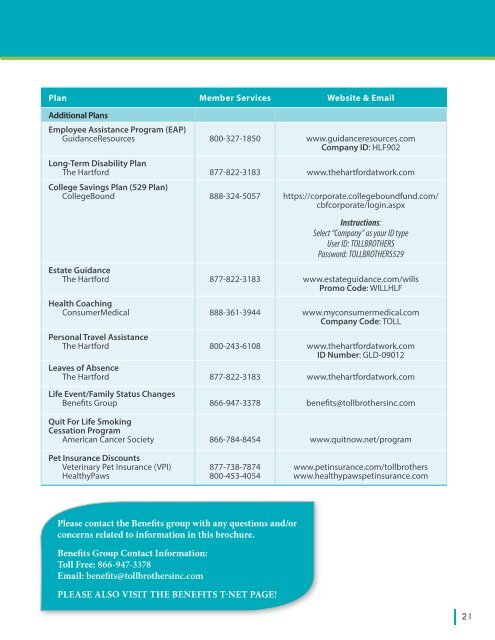
Plan Member Services Website & EmailAdditional Plans<strong>Employee</strong> Assistance Program (EAP)GuidanceResources 800-327-1850 www.guidanceresources.comCompany ID: HLF902Long-Term Disability PlanThe Hartford 877-822-3183 www.thehartfordatwork.comCollege Savings Plan (529 Plan)CollegeBound 888-324-5057 https://corporate.collegeboundfund.com/cbfcorporate/login.aspxInstructions:Select “Company” as your ID typeUser ID: TOLLBROTHERSPassword: TOLLBROTHERS529Estate GuidanceThe Hartford 877-822-3183 www.estateguidance.com/willsPromo Code: WILLHLFHealth CoachingConsumerMedical 888-361-3944 www.myconsumermedical.comCompany Code: TOLLPersonal Travel AssistanceThe Hartford 800-243-6108 www.thehartfordatwork.comID Number: GLD-09012Leaves of AbsenceThe Hartford 877-822-3183 www.thehartfordatwork.comLife Event/Family Status Changes<strong>Benefits</strong> Group 866-947-3378 benefits@tollbrothersinc.comQuit For Life SmokingCessation ProgramAmerican Cancer Society 866-784-8454 www.quitnow.net/programPet Insurance DiscountsVeterinary Pet Insurance (VPI)HealthyPaws877-738-7874800-453-4054www.petinsurance.com/tollbrotherswww.healthypawspetinsurance.comPlease contact the <strong>Benefits</strong> group with any questions and/orconcerns related to information in this brochure.<strong>Benefits</strong> Group Contact Information:Toll Free: 866-947-3378Email: benefits@tollbrothersinc.comPLEASE ALSO VISIT THE BENEFITS T-NET PAGE!21
IMPORTANT LEGAL NOTICES22SUMMARY HEALTH INFORMATIONAs an employee, the health benefits available to you representa significant component of your total rewards package. Theyalso provide important protection for you and your family inthe case of illness or injury. Toll Brothers offers a number ofhealth coverage options. Choosing a health coverage option isimportant and to help you make an informed decision choice,Toll Brothers makes available a Summary of <strong>Benefits</strong> and Coverage(SBC). The SBC summarizes important information aboutany health coverage option in a standard format.NOTICE OF SPECIAL ENROLLMENT RIGHTSIf you are declining enrollment for yourself or yourdependents (including your spouse) because of other healthinsurance coverage, you may in the future be able to enrollyourself or your dependents in this plan, provided that yourequest enrollment within 60 days after your othercoverage ends.In addition, if you have a new dependent as a result ofmarriage, birth, adoption, or placement for adoption, youmay be able to enroll yourself and your dependents, providedthat you request enrollment within 60 days after themarriage, birth, adoption, or placement for adoption.CONTINUATION OF COVERAGE RIGHTSYour group health plan may contain certain options tocontinuing your and/or your dependents health benefitsfollowing termination of coverage. These continuationoptions may include federal COBRA rights, conversion rights,and/or state mandated continuation rights.Additionally, your group life insurance certificates or bookletsmay also include and describe certain continuation optionsthat may be available to you.Please examine your options carefully before decliningthis coverage. You should be aware that companies sellingindividual health insurance typically require a review of yourmedical history that could result in a higher premium or youcould be denied coverage entirely.NOTICE REGARDING THE NEWBORNS’ ACTGroup health plans and health insurance issuers generallymay not, under Federal Law, restrict benefits for anyhospital length of stay in connection with childbirth for themother or newborn child to less than 48 hours following avaginal delivery, or less than 96 hours following a cesareansection. However, Federal Law generally does not prohibitthe mother’s or newborn’s attending provider, afterconsulting with the mother, from discharging the mother orher newborn earlier than 48 hours (or 96 hours as applicable).In any case, plans and issuers may not, under Federal Law,require that a provider obtain authorization from the Planor the insurance issuer for prescribing a length of stay not inexcess of 48 hours (or 96 hours).NOTICE OF WOMEN’S HEALTH AND CANCERRIGHTS ACT (WHCRA)Our medical plan, as required by the Women’s Health andCancer Rights Act of 1998, provides benefits for mastectomy-related services including all states of reconstructionand surgery to achieve symmetry between the breasts,prostheses, and complications resulting from a mastectomy,including lymphedema.If you have had or are going to have a mastectomy, you maybe entitled to certain benefits under the Women’s Health andCancer Rights Act of 1998 (WHCRA). For individuals receivingmastectomy-related benefits, coverage will be provided in amanner determined in consultation with the attendingphysician and the patient, for■■All stages of reconstruction of the breast on which themastectomy was performed,■■Surgery and reconstruction of the other breast toproduce a symmetrical appearance,■■Prostheses, and■■Treatment of physical complications of the mastectomy,including lymphedema.These benefits will be provided subject to the samedeductibles and coinsurance applicable to other medicaland surgical benefits provided under this plan. Pleasereview the plan option you elected to determine theactual deductible and coinsurance provisions.HIPAA SPECIAL ENROLLMENT NOTICEOur records show that you are eligible to participate in theToll Brothers Health Plan. (To actually participate, you mustcomplete an enrollment form and pay part of thepremium through payroll deduction). A federal law calledHIPAA requires that we notify you about an importantprovision in the plan – your right to enroll in the plan underits “special enrollment provision”. If you acquire a new dependent,or if you decline coverage under this plan for yourselfor an eligible dependent while other coverage is in effect andlater lose that other coverage for certain qualifying reasons.Loss of Other Coverage (Excluding Medicaid or a StateChildren’s Health Insurance Program). If you decline enrollmentfor yourself or for an eligible dependent (includingyour spouse) while other health insurance or group healthplan coverage is in effect, you may be able to enroll yourselfand your dependents in this plan if you or your dependentslose eligibility for that other coverage (or if the employerstops contributing toward your or your dependents’ other




![GBS DLL booklet 2016_V5_EDITS[2]](https://img.yumpu.com/54825056/1/190x245/gbs-dll-booklet-2016-v5-edits2.jpg?quality=85)



