Indications for the use of the Amplatzer vascular ... - ConsultiMedici.it
Indications for the use of the Amplatzer vascular ... - ConsultiMedici.it
Indications for the use of the Amplatzer vascular ... - ConsultiMedici.it
Create successful ePaper yourself
Turn your PDF publications into a flip-book with our unique Google optimized e-Paper software.
710 Radiol med (2008) 113:707–718<br />
a<br />
b<br />
c<br />
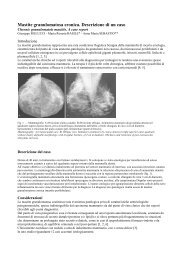
Fig. 2a-c Aortoiliac aneurysm. a Preprocedural computed tomography (CT) angiography (volume-rendered<br />
reconstruction): aortoiliac aneurysm involving <strong>the</strong> origin <strong>of</strong> both internal iliac<br />
arteries and small aneurysm <strong>of</strong> <strong>the</strong> left internal iliac artery. b Angiography per<strong>for</strong>med after deployment<br />
<strong>of</strong> a customised bifurcated stent-graft w<strong>it</strong>h a branch preserving <strong>the</strong> patency <strong>of</strong> <strong>the</strong><br />
right internal iliac artery (black arrow); aneurysm <strong>of</strong> <strong>the</strong> left internal iliac artery is excluded<br />
w<strong>it</strong>h endo<strong>vascular</strong> ligation w<strong>it</strong>h <strong>Amplatzer</strong> <strong>vascular</strong> plug (AVP) in <strong>the</strong> feeding artery (black<br />
asterisk) and coils in <strong>the</strong> draining tract (wh<strong>it</strong>e arrow). c CT angiography per<strong>for</strong>med 6 months<br />
after <strong>the</strong> procedure (maximum intens<strong>it</strong>y projection reconstruction): complete exclusion <strong>of</strong> <strong>the</strong><br />
aneurysm, patency <strong>of</strong> <strong>the</strong> stent-graft branch <strong>of</strong> <strong>the</strong> right internal iliac artery (black arrow) and<br />
exclusion <strong>of</strong> <strong>the</strong> left internal iliac artery aneurysm w<strong>it</strong>h AVP (asterisk) and coils (wh<strong>it</strong>e arrow).<br />
Fig. 2a-c Aneurisma aorto-iliaco. a Angio-TC pre-procedura (ricostruzione VR): aneurisma<br />
aorto-iliaco con coinvolgimento dell’emergenza delle arterie ipogastriche e piccolo aneurisma<br />
dell’arteria ipogastrica sinistra. b Angiografia espletata dopo posizionamento di endoprotesi<br />
bi<strong>for</strong>cata “custom-made” con braccietto protesico che preserva la pervietà dell’arteria ipogastrica<br />
destra (freccia nera); l’aneurisma dell’arteria ipogastrica sinistra è stato escluso<br />
mediante “legatura endovascolare” con VPA a monte (asterisco nero) e spirali metalliche a<br />
valle (freccia bianca). c Follow-up con angio-TC esegu<strong>it</strong>a 6 mesi dopo la procedura (ricostruzione<br />
MIP): completa esclusione dell’aneurisma con pervietà dell’arteria ipogastrica destra<br />
dove è riconoscibile braccietto protesico (freccia nera); esclusione anche dell’aneurisma<br />
dell’arteria ipogastrica sinistra con VPA (asterisco) e spirali metaliche (freccia bianca).<br />
<strong>it</strong>s typical plug shape. The AVP is 7 mm or 8 mm long, and<br />
<strong>it</strong>s elongation is inversely proportional to <strong>the</strong> vessel diameter.<br />
In vessels w<strong>it</strong>h a diameter less than 50% that <strong>of</strong> <strong>the</strong> cylinder,<br />
<strong>the</strong> device can reach more than 1 cm in length.<br />
In 10/12 cases, we <strong>use</strong>d percutaneous transfemoral access,<br />
whereas in 2/12 cases, requiring occlusion <strong>of</strong> <strong>the</strong> subclavian<br />
artery, percutaneous access was transhumeral. The<br />
target vessel was first ca<strong>the</strong>terised selectively w<strong>it</strong>h an appropriately<br />
shaped 5-Fr ca<strong>the</strong>ter (Cordis) and 0.035”<br />
guidewire (Glidewire, Terumo, Tokyo, Japan) (Fig. 3a-c).<br />
Then, w<strong>it</strong>h <strong>the</strong> aid <strong>of</strong> a 0.035” stiff guidewire (Amplatz,<br />
Boston Scientific, Ratingen, Germany), we advanced <strong>the</strong><br />
guiding ca<strong>the</strong>ter (Envoy, Cordis, Miami, FI, USA). In two<br />
cases <strong>of</strong> aortoiliac aneurysm, <strong>the</strong> internal iliac artery was<br />
ca<strong>the</strong>terised w<strong>it</strong>h <strong>the</strong> crossover technique, whereas in <strong>the</strong> remaining<br />
cases, <strong>the</strong> ostium <strong>of</strong> <strong>the</strong> internal iliac artery was<br />
ca<strong>the</strong>terised through an ipsilateral access owing to more<br />
favourable anatomy. Once <strong>the</strong> guiding ca<strong>the</strong>ter was close to<br />
dalla elastic<strong>it</strong>à del N<strong>it</strong>inol che permette l’espansione sino al<br />
raggiungimento del calibro vaso; successivamente il dispos<strong>it</strong>ivo<br />
si allunga conferendo la caratteristica morfologia “a<br />
tappo”. Il VAP è lungo 7 o 8 mm e l’allungamento è inversamente<br />
proporzionale al calibro del vaso; con vasi di calibro<br />
inferiore al 50% si può allungare più di 1 cm.<br />
In 10/12 casi l’approccio percutaneo è stato effettuato<br />
per via trans-femorale; in 2/12 casi, per l’occlusione<br />
dell’arteria succlavia, è stato utilizzato l’approccio transomerale.<br />
Il vaso da occludere è stato dapprima cateterizzato<br />
selettivamente mediante catetere da 5 F (Cordis, Miami,<br />
USA) di morfologia appropriata e guida 0,035” (Glidewire,<br />
Terumo, Tokyo, Giappone) (Fig. 3a-c); successivamente<br />
con l’ausilio di guida rigida 0,035” (Amplatz, Boston Scientific,<br />
Ratingen, Germania) viene avanzato il catetere guida<br />
(Envoy, Cordis, Miami, Fl, USA); in 2 casi di aneurisma<br />
aorto-iliaco, l’arteria ipogastrica è stata cateterizzata con<br />
tecnica “cross-over”, mentre nei rimanenti casi l’ostio