An overview of sexually transmitted diseases. Part III ... - Dermatology
An overview of sexually transmitted diseases. Part III ... - Dermatology
An overview of sexually transmitted diseases. Part III ... - Dermatology
You also want an ePaper? Increase the reach of your titles
YUMPU automatically turns print PDFs into web optimized ePapers that Google loves.
J AM ACAD DERMATOL<br />
VOLUME 43, NUMBER 3<br />
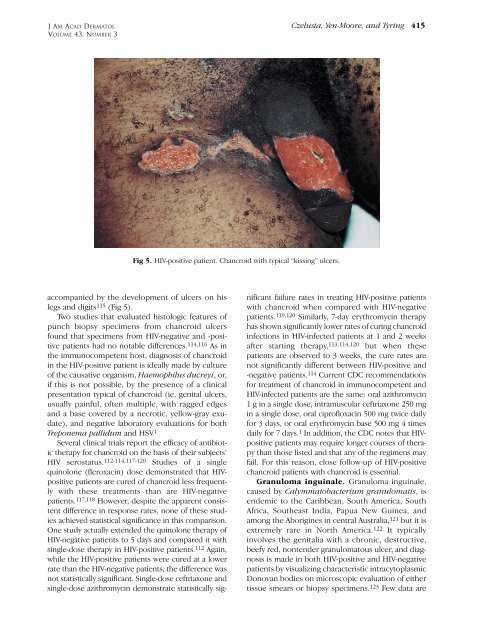
Fig 5. HIV-positive patient. Chancroid with typical “kissing” ulcers.<br />
accompanied by the development <strong>of</strong> ulcers on his<br />
legs and digits 115 (Fig 5).<br />
Two studies that evaluated histologic features <strong>of</strong><br />
punch biopsy specimens from chancroid ulcers<br />
found that specimens from HIV-negative and -positive<br />
patients had no notable differences. 114,116 As in<br />
the immunocompetent host, diagnosis <strong>of</strong> chancroid<br />
in the HIV-positive patient is ideally made by culture<br />
<strong>of</strong> the causative organism, Haemophilus ducreyi, or,<br />
if this is not possible, by the presence <strong>of</strong> a clinical<br />
presentation typical <strong>of</strong> chancroid (ie, genital ulcers,<br />
usually painful, <strong>of</strong>ten multiple, with ragged edges<br />
and a base covered by a necrotic, yellow-gray exudate),<br />
and negative laboratory evaluations for both<br />
Treponema pallidum and HSV. 1<br />
Several clinical trials report the efficacy <strong>of</strong> antibiotic<br />
therapy for chancroid on the basis <strong>of</strong> their subjects’<br />
HIV serostatus. 112-114,117-120 Studies <strong>of</strong> a single<br />
quinolone (fleroxacin) dose demonstrated that HIVpositive<br />
patients are cured <strong>of</strong> chancroid less frequently<br />
with these treatments than are HIV-negative<br />
patients. 117,118 However, despite the apparent consistent<br />
difference in response rates, none <strong>of</strong> these studies<br />
achieved statistical significance in this comparison.<br />
One study actually extended the quinolone therapy <strong>of</strong><br />
HIV-negative patients to 5 days and compared it with<br />
single-dose therapy in HIV-positive patients. 112 Again,<br />
while the HIV-positive patients were cured at a lower<br />
rate than the HIV-negative patients, the difference was<br />
not statistically significant. Single-dose ceftriaxone and<br />
single-dose azithromycin demonstrate statistically sig-<br />
Czelusta, Yen-Moore, and Tyring 415<br />
nificant failure rates in treating HIV-positive patients<br />
with chancroid when compared with HIV-negative<br />
patients. 119,120 Similarly, 7-day erythromycin therapy<br />
has shown significantly lower rates <strong>of</strong> curing chancroid<br />
infections in HIV-infected patients at 1 and 2 weeks<br />
after starting therapy, 113,114,120 but when these<br />
patients are observed to 3 weeks, the cure rates are<br />
not significantly different between HIV-positive and<br />
-negative patients. 114 Current CDC recommendations<br />
for treatment <strong>of</strong> chancroid in immunocompetent and<br />
HIV-infected patients are the same: oral azithromycin<br />
1 g in a single dose, intramuscular ceftriaxone 250 mg<br />
in a single dose, oral cipr<strong>of</strong>loxacin 500 mg twice daily<br />
for 3 days, or oral erythromycin base 500 mg 4 times<br />
daily for 7 days. 1 In addition, the CDC notes that HIVpositive<br />
patients may require longer courses <strong>of</strong> therapy<br />
than those listed and that any <strong>of</strong> the regimens may<br />
fail. For this reason, close follow-up <strong>of</strong> HIV-positive<br />
chancroid patients with chancroid is essential.<br />
Granuloma inguinale. Granuloma inguinale,<br />
caused by Calymmatobacterium granulomatis, is<br />
endemic to the Caribbean, South America, South<br />
Africa, Southeast India, Papua New Guinea, and<br />
among the Aborigines in central Australia, 121 but it is<br />
extremely rare in North America. 122 It typically<br />
involves the genitalia with a chronic, destructive,<br />
beefy red, nontender granulomatous ulcer, and diagnosis<br />
is made in both HIV-positive and HIV-negative<br />
patients by visualizing characteristic intracytoplasmic<br />
Donovan bodies on microscopic evaluation <strong>of</strong> either<br />
tissue smears or biopsy specimens. 123 Few data are