A guide to lower surgery for trans men - Gender Identity Research ...
A guide to lower surgery for trans men - Gender Identity Research ...
A guide to lower surgery for trans men - Gender Identity Research ...
You also want an ePaper? Increase the reach of your titles
YUMPU automatically turns print PDFs into web optimized ePapers that Google loves.
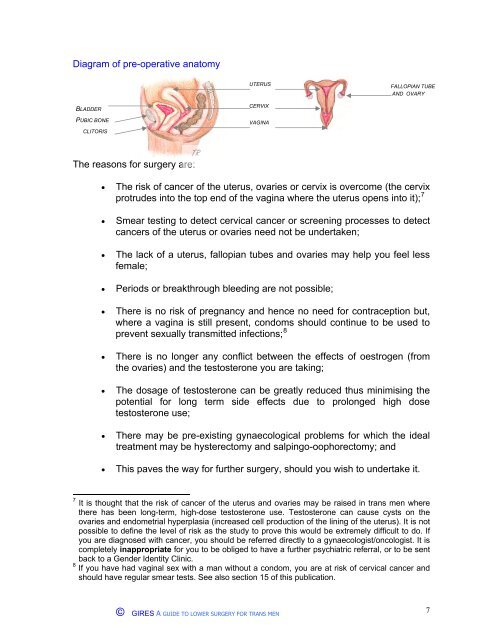
Diagram of pre-operative ana<strong>to</strong>my<br />
BLADDER<br />
PUBIC BONE<br />
CLITORIS<br />
TR<br />
The reasons <strong>for</strong> <strong>surgery</strong> are:<br />
UTERUS<br />
CERVIX<br />
VAGINA<br />
The risk of cancer of the uterus, ovaries or cervix is overcome (the cervix<br />
protrudes in<strong>to</strong> the <strong>to</strong>p end of the vagina where the uterus opens in<strong>to</strong> it); 7<br />
Smear testing <strong>to</strong> detect cervical cancer or screening processes <strong>to</strong> detect<br />
cancers of the uterus or ovaries need not be undertaken;<br />
The lack of a uterus, fallopian tubes and ovaries may help you feel less<br />
female;<br />
Periods or breakthrough bleeding are not possible;<br />
FALLOPIAN TUBE<br />
AND OVARY<br />
There is no risk of pregnancy and hence no need <strong>for</strong> contraception but,<br />
where a vagina is still present, condoms should continue <strong>to</strong> be used <strong>to</strong><br />
prevent sexually <strong>trans</strong>mitted infections; 8<br />
There is no longer any conflict between the effects of oestrogen (from<br />
the ovaries) and the tes<strong>to</strong>sterone you are taking;<br />
The dosage of tes<strong>to</strong>sterone can be greatly reduced thus minimising the<br />
potential <strong>for</strong> long term side effects due <strong>to</strong> prolonged high dose<br />
tes<strong>to</strong>sterone use;<br />
There may be pre-existing gynaecological problems <strong>for</strong> which the ideal<br />
treat<strong>men</strong>t may be hysterec<strong>to</strong>my and salpingo-oophorec<strong>to</strong>my; and<br />
This paves the way <strong>for</strong> further <strong>surgery</strong>, should you wish <strong>to</strong> undertake it.<br />
7 It is thought that the risk of cancer of the uterus and ovaries may be raised in <strong>trans</strong> <strong>men</strong> where<br />
there has been long-term, high-dose tes<strong>to</strong>sterone use. Tes<strong>to</strong>sterone can cause cysts on the<br />
ovaries and endometrial hyperplasia (increased cell production of the lining of the uterus). It is not<br />
possible <strong>to</strong> define the level of risk as the study <strong>to</strong> prove this would be extremely difficult <strong>to</strong> do. If<br />
you are diagnosed with cancer, you should be referred directly <strong>to</strong> a gynaecologist/oncologist. It is<br />
completely inappropriate <strong>for</strong> you <strong>to</strong> be obliged <strong>to</strong> have a further psychiatric referral, or <strong>to</strong> be sent<br />
back <strong>to</strong> a <strong>Gender</strong> <strong>Identity</strong> Clinic.<br />
8 If you have had vaginal sex with a man without a condom, you are at risk of cervical cancer and<br />
should have regular smear tests. See also section 15 of this publication.<br />
© GIRES A GUIDE TO LOWER SURGERY FOR TRANS MEN<br />
7