Active IQ Level 3 Diploma in Exercise Referral (sample manual)
For more information, please visit http://www.activeiq.co.uk/qualifications/level-3/active-iq-level-3-diploma-in-exercise-referral
For more information, please visit http://www.activeiq.co.uk/qualifications/level-3/active-iq-level-3-diploma-in-exercise-referral
Create successful ePaper yourself
Turn your PDF publications into a flip-book with our unique Google optimized e-Paper software.
Manual<br />
<strong>Level</strong> 3 <strong>Diploma</strong> <strong>in</strong><br />
<strong>Exercise</strong> <strong>Referral</strong> –<br />
All Units<br />
Version A<strong>IQ</strong>005179
Section 1: The heart and circulatory system and its relation to exercise and health<br />
The valves of the heart<br />
In order to function effectively as a pump, the heart needs<br />
to direct blood through the atria, ventricles and then the<br />
arteries of the body. The heart prevents unwanted backflow<br />
of blood <strong>in</strong>to the chambers us<strong>in</strong>g a number of valves.<br />
These valves open and close <strong>in</strong> response to changes <strong>in</strong><br />
pressure as the heart contracts and relaxes. The structure<br />
of the valves means that they only allow blood to flow<br />
<strong>in</strong> one direction by shutt<strong>in</strong>g once blood has been pushed<br />
through them. This is fundamental to effective circulation;<br />
any back-flow through the heart will compromise the<br />
efficiency of each heartbeat, which is likely to affect<br />
exercise performance and health.<br />
The ma<strong>in</strong> valves of the heart are the atrioventricular (AV)<br />
valves and the semilunar (SL) valves. The AV valves are<br />
located between the atria and the ventricles and prevent<br />
the back-flow of blood from the ventricles <strong>in</strong>to the atria.<br />
As the ventricles contract, pressure rises and forces the AV<br />
valves to snap shut, allow<strong>in</strong>g blood to be directed through<br />
the arteries leav<strong>in</strong>g the heart (pulmonary artery and aorta).<br />
SOMETHING EXTRA<br />
As the AV valves snap<br />
shut, they are anchored<br />
<strong>in</strong> place by tendonlike<br />
chords (chordae<br />
tend<strong>in</strong>eae) which prevent<br />
the valve flaps from be<strong>in</strong>g<br />
pushed too far <strong>in</strong>to the<br />
atria.<br />
The SL valves are located at<br />
the base of the arteries leav<strong>in</strong>g<br />
the heart (aorta and pulmonary<br />
artery). After each contraction,<br />
there is a relative drop <strong>in</strong><br />
pressure with<strong>in</strong> the ventricles<br />
as they relax. At this po<strong>in</strong>t, the<br />
blood with<strong>in</strong> the pulmonary<br />
artery and aorta could potentially<br />
flow back <strong>in</strong>to the ventricles. To<br />
prevent this, both sets of arteries<br />
have SL valves positioned at the<br />
po<strong>in</strong>t where they emerge from the ventricles. As the blood<br />
moves back towards the ventricles, the SL valves snap<br />
shut so blood cannot re-enter.<br />
It is the sequential shutt<strong>in</strong>g of the valves dur<strong>in</strong>g the cardiac<br />
cycle that causes the dist<strong>in</strong>ct ‘lub-dub’ noises associated<br />
with the heartbeat.<br />
Superior<br />
vena<br />
cava<br />
Right<br />
pulmonary<br />
ve<strong>in</strong>s<br />
Right<br />
atrium<br />
Right<br />
ventricle<br />
Inferior<br />
vena cava<br />
Atrioventricular (AV)<br />
valves<br />
Aorta<br />
Pulmonary<br />
artery<br />
Figure 1.2 The heart<br />
Figure 1.3 The valves of<br />
the heart<br />
Left<br />
pulmonary<br />
ve<strong>in</strong>s<br />
Left<br />
atrium<br />
Left<br />
ventricle<br />
Semilunar<br />
(SL) valves<br />
MEMORY JOGGER – HEART CIRCULATION<br />
The heart is stimulated to contract by a complex series of <strong>in</strong>tegrated systems. The heart’s pacemaker –<br />
the s<strong>in</strong>oatrial (SA) node – <strong>in</strong>itiates the cardiac muscle contraction. The SA node is located <strong>in</strong> the wall of<br />
the right atrium. The myocardium (heart muscle) is stimulated to contract about 72 times per m<strong>in</strong>ute<br />
by the SA node as part of the autonomic nervous system.<br />
6 | Copyright © 2017 <strong>Active</strong> <strong>IQ</strong> Ltd. Not for resale
Section 1: The heart and circulatory system and its relation to exercise and health<br />
Risks of high blood pressure<br />
It is normal for blood pressure to temporarily <strong>in</strong>crease dur<strong>in</strong>g exertion or when feel<strong>in</strong>g anxious or stressed.<br />
Hypertension (high blood pressure) is the term used to describe blood pressure that is consistently higher<br />
than the healthy level when at rest. A high SBP provides an <strong>in</strong>dication of the stra<strong>in</strong> on the blood vessels when<br />
the heart is attempt<strong>in</strong>g to pump out blood. If the DBP is high, it <strong>in</strong>dicates that the blood vessels have little<br />
chance to relax between heartbeats. Consequently, measur<strong>in</strong>g blood pressure provides an <strong>in</strong>dication of the<br />
health of the vascular system and an overall gauge of a person’s health.<br />
ACTIVITY<br />
The term ‘white coat hypertension’ may be used if you have high blood pressure read<strong>in</strong>gs<br />
(i.e. read<strong>in</strong>gs that are consistently 140/90mmHg or above) only when you are <strong>in</strong> a medical<br />
sett<strong>in</strong>g. Why do you th<strong>in</strong>k blood pressure read<strong>in</strong>gs might be higher <strong>in</strong> a medical environment?<br />
SOMETHING EXTRA<br />
There are currently<br />
about 12 million<br />
people <strong>in</strong> the UK who<br />
have hypertension<br />
(blood pressure<br />
≥140/90mmHg), and<br />
more than half of those<br />
are over the age of<br />
60. Around 5.7 million<br />
people have undiagnosed<br />
hypertension.<br />
(UK Blood Pressure<br />
Association, 2012)<br />
Hypertension <strong>in</strong>creases the risk of ischaemic heart disease and cerebrovascular<br />
disease – two of the three biggest killers <strong>in</strong> the developed world. Ischaemic heart<br />
disease covers a variety of heart conditions <strong>in</strong>clud<strong>in</strong>g valve disease and more<br />
acute problems such as myocardial <strong>in</strong>farction (heart attack). Cerebrovascular<br />
disease <strong>in</strong>cludes acute problems such as haemorrhagic and ischaemic strokes<br />
and chronically degenerative conditions like vascular dementia and Alzheimer’s<br />
disease. Hypertension also places stress on the small vessels to the ret<strong>in</strong>a, which<br />
can cause bl<strong>in</strong>dness, as well as the small vessels of the kidneys, which can lead<br />
to renal failure.<br />
The average rest<strong>in</strong>g blood pressure is def<strong>in</strong>ed by the American College of Sports<br />
Medic<strong>in</strong>e (2014) as 120/80 mmHg. A blood pressure of 140/90 mmHg is<br />
considered to be high. Individuals with measures above 140/90 mmHg are<br />
encouraged to see their doctor before commenc<strong>in</strong>g physical activity programmes.<br />
Read<strong>in</strong>gs above 180 systolic and 110 diastolic are a contra<strong>in</strong>dication for exercise.<br />
People with low blood pressure read<strong>in</strong>gs may also require medical referral (see<br />
table 1.1).<br />
MAKE A NOTE<br />
CATEGORY SYSTOLIC (mmHg) DIASTOLIC (mmHg)<br />
Low < 100 < 60<br />
Optimal < 120 < 80<br />
Normal < 130 < 85<br />
High normal - Pre-hypertension 130-139 85-89<br />
Stage 1 Hypertension 140-159 90-99<br />
Stage 2 Hypertension 160-179 100-109<br />
Stage 3 Hypertension > 180 > 110<br />
Table 1.1 Blood pressure classifications (ACSM, 2014)<br />
An ischaemic stroke is the most common form of stroke and is often caused by a thrombosis (an obstruction of a blood vessel lead<strong>in</strong>g to<br />
the bra<strong>in</strong> by a localised blood clot) or an embolism (an obstruction due to an embolus – a detached blood clot – from elsewhere <strong>in</strong> the<br />
body).<br />
An haemorrhagic stroke is an <strong>in</strong>tracranial haemorrhage (bleed) and can be l<strong>in</strong>ked to an aneurysm (a localised, blood-filled, balloon-like<br />
bulge <strong>in</strong> the wall of a weakened blood vessel). As the aneurysm <strong>in</strong>creases <strong>in</strong> size, the risk of it ruptur<strong>in</strong>g <strong>in</strong>creases.<br />
10 | Copyright © 2017 <strong>Active</strong> <strong>IQ</strong> Ltd. Not for resale
Section 1: The heart and circulatory system and its relation to exercise and health<br />
Short-term effects of exercise on blood pressure<br />
A short-term effect of exercise is a l<strong>in</strong>ear <strong>in</strong>crease <strong>in</strong> systolic blood pressure (SBP)<br />
with <strong>in</strong>creas<strong>in</strong>g levels of exertion. In contrast, diastolic blood pressure (DBP) may<br />
decrease slightly dur<strong>in</strong>g exertion due to vasodilation, or it will rema<strong>in</strong> unchanged.<br />
Individuals with hypertension may experience a rise <strong>in</strong> DBP as a result of an<br />
impaired vasodilatory response.<br />
Heavy weight tra<strong>in</strong><strong>in</strong>g and isometric exercise will significantly <strong>in</strong>crease both<br />
systolic and diastolic blood pressure. It is important for an <strong>in</strong>dividual not to hold<br />
their breath when perform<strong>in</strong>g these exercises to avoid the Valsalva effect. This<br />
effect is created by the Valsalva manoeuvre, which <strong>in</strong>volves hold<strong>in</strong>g the breath<br />
while stra<strong>in</strong><strong>in</strong>g or a forced exhalation aga<strong>in</strong>st a closed airway (glottis). This action<br />
<strong>in</strong>creases pressure with<strong>in</strong> the thoracic cavity and thereby impedes venous return<br />
of blood to the heart. Dur<strong>in</strong>g the manoeuvre, the mouth and nose are closed while<br />
the air is ‘pushed’ aga<strong>in</strong>st the closed airway without breath<strong>in</strong>g out. It’s similar to<br />
the pressure created when pass<strong>in</strong>g a bowel movement. The Valsalva effect can<br />
drastically <strong>in</strong>crease blood pressure and heighten the risk of a cardiovascular event<br />
such as a heart attack or stroke.<br />
Long-term effects of exercise on blood pressure<br />
Aerobic exercise us<strong>in</strong>g large muscle groups <strong>in</strong> rhythmical activity is very useful for reduc<strong>in</strong>g blood pressure<br />
over time. Durst<strong>in</strong>e and Moore (2003) state that endurance tra<strong>in</strong><strong>in</strong>g can elicit an average decrease of 10<br />
mmHg <strong>in</strong> both systolic and diastolic blood pressure <strong>in</strong> mild and moderate hypertensives.<br />
Anatomy and physiology for exercise and health<br />
With the exception of circuit weight tra<strong>in</strong><strong>in</strong>g, chronic strength or resistive tra<strong>in</strong><strong>in</strong>g has not consistently been<br />
shown to lower rest<strong>in</strong>g blood pressure. Resistance tra<strong>in</strong><strong>in</strong>g can have many benefits for hypertensives, but it<br />
is not recommended as a means of decreas<strong>in</strong>g blood pressure on its own.<br />
<strong>Exercise</strong> and blood pressure considerations<br />
Short-term <strong>in</strong>creases <strong>in</strong> blood pressure result naturally from physical activity. These <strong>in</strong>creases can be<br />
exaggerated by the Valsalva effect, which causes rapid short-term rises <strong>in</strong> blood pressure. Consequently, blood<br />
pressure can be elevated to dangerously high levels dur<strong>in</strong>g exercise <strong>in</strong> people with pre-exist<strong>in</strong>g hypertension.<br />
Increased risk of stroke<br />
dur<strong>in</strong>g and immediately<br />
after exercise.<br />
<strong>Exercise</strong> is therefore<br />
associated with<br />
a number of<br />
cardiovascular risks<br />
<strong>in</strong>clud<strong>in</strong>g:<br />
Increased risk of heart<br />
attack (myocardial<br />
<strong>in</strong>farction) dur<strong>in</strong>g and<br />
immediately after<br />
exercise.<br />
TRAINER TIP<br />
To avoid excessive<br />
<strong>in</strong>creases <strong>in</strong> blood<br />
pressure while<br />
resistance tra<strong>in</strong><strong>in</strong>g (as<br />
a consequence of the<br />
Valsalva effect), <strong>in</strong>hale<br />
as you’re br<strong>in</strong>g<strong>in</strong>g the<br />
resistance back to its<br />
rest<strong>in</strong>g position and<br />
exhale as you’re work<strong>in</strong>g<br />
hardest aga<strong>in</strong>st the<br />
resistance.<br />
For certa<strong>in</strong> clients, the risks associated with exercise need to be weighed up aga<strong>in</strong>st the benefits before they<br />
engage <strong>in</strong> any physical activity – especially if it’s high-<strong>in</strong>tensity. Physical activity can carry risks for people<br />
with high blood pressure, but for most people, the benefits far outweigh the dangers.<br />
Copyright © 2017 <strong>Active</strong> <strong>IQ</strong> Ltd. Not for resale | 11
Section 3: Postural and core stability<br />
Section 3: Postural and core stability<br />
One of the most pervasive trends <strong>in</strong> the health and fitness <strong>in</strong>dustry<br />
has been the cont<strong>in</strong>ual emphasis on tra<strong>in</strong><strong>in</strong>g the core of the body.<br />
The core is considered to be the trunk of the body, the part left over<br />
when the arms and legs are discounted.<br />
The core is often misconstrued as be<strong>in</strong>g only the abdom<strong>in</strong>als and<br />
lower back; the abdom<strong>in</strong>als have probably been focused on too much<br />
<strong>in</strong> many tra<strong>in</strong><strong>in</strong>g programmes around the country. In this section, we<br />
will be look<strong>in</strong>g <strong>in</strong>to the different muscles and ligaments that help<br />
to stabilise the sp<strong>in</strong>e and support movement around the core. It’s<br />
important to appreciate the problems that can result when the core<br />
musculature doesn’t function as it should. Then, to f<strong>in</strong>ish, we will<br />
look <strong>in</strong>to a few aspects of flexibility that can help to restore good<br />
movement and function around the body.<br />
MAKE A NOTE<br />
Core stability can be def<strong>in</strong>ed as:<br />
‘The ability of your trunk<br />
to support the effort and<br />
forces from your arms<br />
and legs, so that muscles<br />
and jo<strong>in</strong>ts can perform <strong>in</strong><br />
their safest, strongest and<br />
most effective positions.’<br />
The stabilis<strong>in</strong>g ligaments and muscles of the sp<strong>in</strong>e<br />
(Elph<strong>in</strong>stone and Pook, 1998)<br />
The sp<strong>in</strong>e is supported by ligaments and muscle tissue that help it to move with<strong>in</strong> set parameters.<br />
The ligaments of the sp<strong>in</strong>e<br />
The ligaments provide a certa<strong>in</strong> amount of passive support and<br />
prevent unwanted movement of the sp<strong>in</strong>e. There are four ma<strong>in</strong><br />
ligaments runn<strong>in</strong>g up and down the length of the sp<strong>in</strong>e:<br />
ANTERIOR<br />
LONGITUDINAL<br />
LIGAMENT:<br />
This connects each vertebral body together<br />
and runs anteriorly along the front of the<br />
sp<strong>in</strong>e prevent<strong>in</strong>g excess extension of the<br />
sp<strong>in</strong>e.<br />
Anterior<br />
longitud<strong>in</strong>al<br />
ligament<br />
Anatomy and physiology for exercise and health<br />
POSTERIOR<br />
LONGITUDINAL<br />
LIGAMENT:<br />
INTERSPINOUS<br />
LIGAMENTS:<br />
INTERTRANSVERSE<br />
LIGAMENTS:<br />
This runs along the back of the sp<strong>in</strong>e,<br />
underneath the sp<strong>in</strong>ous processes, and is<br />
also connected to the vertebral bodies of<br />
each segment. It prevents excess flexion of<br />
the sp<strong>in</strong>e.<br />
These connect each sp<strong>in</strong>ous process to the<br />
one immediately above or below and, together<br />
with the posterior longitud<strong>in</strong>al ligament,<br />
prevent excess flexion of the sp<strong>in</strong>e.<br />
These connect each transverse process to<br />
the one immediately above or below. These<br />
ligaments run on both the left and right side of<br />
the sp<strong>in</strong>e and prevent excess lateral flexion.<br />
Posterior<br />
longitud<strong>in</strong>al<br />
ligament<br />
Intersp<strong>in</strong>ous<br />
ligament<br />
Suprasp<strong>in</strong>ous<br />
ligament<br />
Intertransverse<br />
ligament<br />
Figure 3.1 The ligaments of the sp<strong>in</strong>e<br />
These passive structures are much weaker than muscles and can only withstand a small force (4-5 lbs)<br />
before buckl<strong>in</strong>g (Panjabi et al., 1989), which demonstrates that the muscular system is primarily responsible<br />
for ma<strong>in</strong>ta<strong>in</strong><strong>in</strong>g core stability and posture.<br />
Copyright © 2017 <strong>Active</strong> <strong>IQ</strong> Ltd. Not for resale | 33
Section 3: Postural and core stability<br />
An active stretch is one where a position is held with no assistance other than us<strong>in</strong>g the strength of the<br />
agonist muscles. An example would be dorsiflex<strong>in</strong>g the ankle and hold<strong>in</strong>g it <strong>in</strong> that position. The tension of<br />
the agonists <strong>in</strong> an active stretch helps to relax the muscles be<strong>in</strong>g stretched (the antagonists) by reciprocal<br />
<strong>in</strong>hibition. <strong>Active</strong> stretch<strong>in</strong>g <strong>in</strong>creases active flexibility and strengthens the agonistic muscles. <strong>Active</strong> stretches<br />
are usually quite difficult to hold and ma<strong>in</strong>ta<strong>in</strong> for more than ten seconds.<br />
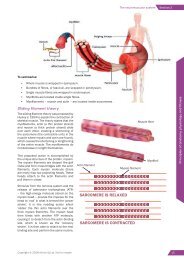
Dynamic stretch<strong>in</strong>g<br />
Dynamic stretch<strong>in</strong>g, as the name implies, <strong>in</strong>volves movement. It tends to be<br />
used as part of a warm-up and should be based around the exercise that will<br />
follow it. The movements used should be performed under control (avoid<strong>in</strong>g<br />
ballistic type movements), progress from mid to end range and start slowly,<br />
<strong>in</strong>creas<strong>in</strong>g <strong>in</strong> speed to promote blood flow and elasticity of the tissues. If<br />
movements are not controlled <strong>in</strong> speed and range, there is a potential to tear<br />
tissues.<br />
Dynamic stretch<strong>in</strong>g helps to reduce the risk of <strong>in</strong>jury by warm<strong>in</strong>g the muscle<br />
tissues and mobilis<strong>in</strong>g jo<strong>in</strong>ts us<strong>in</strong>g the types of movement that are about to<br />
follow <strong>in</strong> the exercise programme. Care should be taken not to use unnecessary<br />
explosive movements that could stra<strong>in</strong> tissues before they are ready.<br />
Proprioceptive neuromuscular facilitation (PNF)<br />
PNF is a way of tak<strong>in</strong>g advantage of the underly<strong>in</strong>g neuromuscular feedback loops <strong>in</strong>herent <strong>in</strong> muscle tissue.<br />
The most commonly used form of PNF is based on the contract–relax pr<strong>in</strong>ciple, where a contraction of a<br />
target muscle stimulates a subsequent relaxation of that muscle (the <strong>in</strong>verse stretch reflex).<br />
Anatomy and physiology for exercise and health<br />
Dur<strong>in</strong>g PNF, a muscle group is passively stretched then contracted isometrically (typically for 7-15 seconds)<br />
aga<strong>in</strong>st resistance while <strong>in</strong> the stretched position. After two to three seconds, the muscle is then passively<br />
stretched aga<strong>in</strong> through the result<strong>in</strong>g <strong>in</strong>creased range of motion. PNF stretch<strong>in</strong>g usually employs the use of<br />
a partner to provide resistance aga<strong>in</strong>st the isometric contraction and then later to passively take the jo<strong>in</strong>t<br />
through its <strong>in</strong>creased range of motion. PNF may be performed without a partner, although it is usually more<br />
effective with assistance.<br />
PNF should only be applied to thoroughly warm muscles and by an experienced practitioner.<br />
Copyright © 2017 <strong>Active</strong> <strong>IQ</strong> Ltd. Not for resale | 39
Section 2: ditibe riorection porunt, simo offic to m<strong>in</strong>Ipsam<br />
Section 3: Understand<strong>in</strong>g the healthcare systems <strong>in</strong> the UK<br />
fugia aut latiuntio. Fici ommos eatiandest qui doluptium<br />
The structure of the healthcare systems<br />
As a consequence of the Health and Social Care Act (2012) the responsibility to deliver Public Health<br />
moved from the NHS back to the Local Authorities (from where it had orig<strong>in</strong>ated) on 1st April 2013. This<br />
brought about changes to the structure of healthcare and also changes to how fund<strong>in</strong>g is distributed; GPs<br />
will hold the majority of the NHS budget, with other allocations go<strong>in</strong>g to the Cl<strong>in</strong>ical Commission<strong>in</strong>g Groups<br />
(CCGs) and Public Health <strong>in</strong> the Local Authorities.<br />
Figure 3 illustrates the structure of the healthcare system (2013). Clients and communities are at the centre<br />
or ‘heart’ of the new model, with layers of other services and bodies, <strong>in</strong>form<strong>in</strong>g the care they receive.<br />
• People & Communities (the service users) are at the centre (heart) of the model.<br />
• Local health and care services are the <strong>in</strong>ner layer; and <strong>in</strong>clude services that may be visited on a daily<br />
basis, e.g. pharmacies, GP surgeries, hospitals, opticians.<br />
• Health and Wellbe<strong>in</strong>g boards (H&WB) oversee all local services. They conta<strong>in</strong> representatives from the<br />
local services to work together to improve the health of the local community that they serve.<br />
• Local authorities and Cl<strong>in</strong>ical Commission<strong>in</strong>g Groups (CCGs), form the next layer of the system, their<br />
role is to ensure services meet community health needs.<br />
• National organisations <strong>in</strong>clud<strong>in</strong>g Public Health England and NHS Commission<strong>in</strong>g boards.<br />
• Regulation and safeguard<strong>in</strong>g organisations, e.g. Care Quality Commission (CQC) and various<br />
authorities.<br />
• Department of Health, Parliament and Government departments form the outer layer.<br />
Figure 3 The structure of the healthcare system (2013)<br />
Source: http://www.nhs.uk/NHSEngland/thenhs/about/Pages/nhsstructure.aspx<br />
Copyright © 2017 <strong>Active</strong> <strong>IQ</strong> Ltd. Not for resale | 79
The use of risk stratification tools<br />
In the UK most exercise referral schemes have developed their own risk stratification tools and protocols for<br />
work<strong>in</strong>g with specific <strong>in</strong>dividuals and groups. In most <strong>in</strong>stances these tools have been developed by work<strong>in</strong>g<br />
collaboratively with local medical practitioners (GPs, physiotherapists etc). To date there has been no s<strong>in</strong>gle<br />
model used and this has raised concerns <strong>in</strong> recent years because it was believed that a standardised approach<br />
should be adopted across schemes; for both safety standards and monitor<strong>in</strong>g and evaluation purposes.<br />
Some of the current risk stratification models are <strong>in</strong>troduced next.<br />
PAR-Q and PARmedX<br />
The screen<strong>in</strong>g tools used by many schemes are the Physical Activity Read<strong>in</strong>ess Questionnaire (PAR-Q) and the<br />
Physical Activity Read<strong>in</strong>ess Medical Exam<strong>in</strong>ation (PARmed-X); the latter consists of a physical activity specific<br />
checklist, developed for physicians to use with clients who have had positive responses (answered ‘yes’) to<br />
the PAR-Q. The <strong>in</strong>formation collected from these tools will usually be listed on a transfer of <strong>in</strong>formation record.<br />
Both questionnaires are designed by the Canadian Society for <strong>Exercise</strong> Physiology (2002). (NB: These<br />
documents are under review).<br />
The risk stratification pyramid<br />
The risk stratification pyramid (figure 8) presented <strong>in</strong> the National Quality Assurance Framework for <strong>Exercise</strong><br />
<strong>Referral</strong> report (NQAF, 2001) provided one of the earliest UK models for risk stratification. The model used<br />
guidance from the ACSM and identified four levels of client, with apparently healthy populations at the bottom<br />
of a pyramid, followed by low-risk populations, moderate-risk populations and high-risk populations. At each<br />
stage of the pyramid the qualifications that an <strong>in</strong>structor needed prior to work<strong>in</strong>g with these groups were stated<br />
(based on the qualifications available at that time) and the type of exercise environment/activity sett<strong>in</strong>g was<br />
also listed.<br />
HIGH RISK<br />
Cl<strong>in</strong>ical exercise<br />
Specialist sessions<br />
Moderate/Medium risk<br />
Advanced Instructor (2)<br />
<strong>Referral</strong> scheme<br />
Low risk<br />
Advanced Instructor (1)<br />
<strong>Referral</strong> scheme<br />
Apparently healthy<br />
<strong>Level</strong> 2 <strong>in</strong>structor<br />
General exercise programmes<br />
Figure 8 Risk Stratification Pyramid<br />
Logic model for risk stratification<br />
The logic model for risk stratification (ACSM, 2010) suggests that the health and medical history of the person<br />
should be reviewed to check for the presence of:<br />
• Known CVD conditions (diagnosis).<br />
• Signs and symptoms to <strong>in</strong>dicate the presence of cardiovascular disease, pulmonary disease and/or<br />
metabolic disease.<br />
• CVD risk factors.<br />
This model has been perhaps the most commonly used model by most exercise referral <strong>in</strong>structors (see figure<br />
9). Individuals who present with more than two signs and symptoms (as per PAR-Q) are signposted to a GP<br />
prior to participation and may then be referred for a more specialist programme, depend<strong>in</strong>g on other factors<br />
(current activity levels and overall health status).<br />
Copyright © 2017 <strong>Active</strong> <strong>IQ</strong> Ltd. Not for resale | 113