Supplementum 163 - Swiss Medical Weekly
Supplementum 163 - Swiss Medical Weekly
Supplementum 163 - Swiss Medical Weekly
You also want an ePaper? Increase the reach of your titles
YUMPU automatically turns print PDFs into web optimized ePapers that Google loves.
29 S SWISS MED WKLY 2008;138(Suppl <strong>163</strong>) · www.smw.ch<br />
Poster Session 2 - SSP / SGP<br />
eosinophilia was noted. All patients were active smokers and<br />
developed a blood eosinophilia with a latency of 4 to 6 days.<br />
In 2 cases elevated IgE-levels were measured.<br />
Conclusion: Though pulmonary side-effects seem to be rather<br />
uncommon, the possibility of chloroquine-induced pneumonitis<br />
should be considered if a suggestive clinical course exists following<br />
exposure to this substance.<br />
P138<br />
Sleep related breathing disorders in patients with pulmonary<br />
hypertension<br />
S. Ulrich, M. Fischler, R. Speich, K. Bloch.<br />
University Hospital of Zurich (Zurich, CH)<br />
Background: Cheyne-Stokes respiration and central sleep apnea<br />
(CSRA/CSA) are common in patients with left heart failure. We<br />
investigated the hypothesis that sleep disordered breathing is also<br />
prevalent in patients with right ventricular dysfunction due to<br />
pulmonary hypertension.<br />
Methods: We studied 38 outpatients (mean ± SD age 59 ± 16 years,<br />
11 males) with pulmonary arterial hypertension (n = 23) or<br />
thromboembolic pulmonary hypertension (n = 15). NYHA class was<br />
2-4, the 6 minute walk distance was 481 ± 120 m. In-laboratory<br />
polysomnography (n = 22) and ambulatory cardio-respiratory sleep<br />
studies (n = 38) including pulse oximetry were performed. Quality of<br />
life and sleepiness by Epworth score were assessed.<br />
Results: The apnea/hypopnea index was 14±14 events/h with 10 ± 9<br />
central and 3 ± 10 obstructive events/h. Seventeen patients (45%)<br />
had 010 apnea/hypopnea events/h. Comparison of 13 patients with<br />
010 CSR/CSA events/h with 21 patients with 10/h, Epworth score >8) were randomized to autoCPAP or<br />
fixedCPAP therapy at the 90.%-ile of mask pressure during a 2–4<br />
weeks autoCPAP adaptation period. At baseline and at 3 months we<br />
assessed sleepiness, quality of life, AHI, and 24h blood pressure.<br />
Equivalence of CPAP modes was evaluated by computing 95%<br />
confidence intervals of differences in treatment effects.<br />
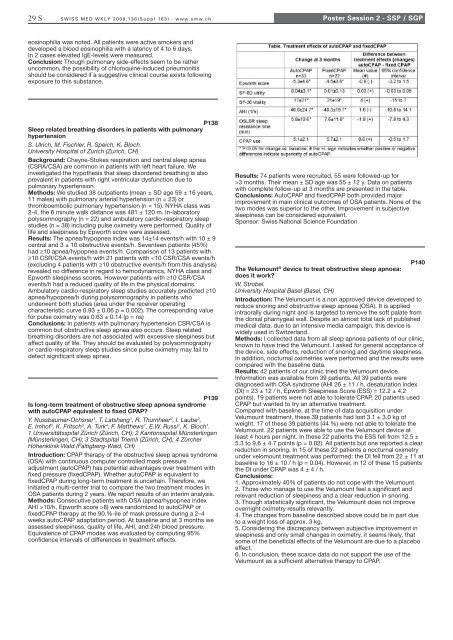
Results: 74 patients were recruited, 55 were followed-up for<br />
>3 months. Their mean ± SD age was 55 ± 12 y. Data on patients<br />
with complete follow-up at 3 months are presented in the table.<br />
Conclusions: AutoCPAP and fixedCPAP both provided major<br />
improvement in main clinical outcomes of OSA patients. None of the<br />
two modes was superior to the other. Improvement in subjective<br />
sleepiness can be considered equivalent.<br />
Sponsor: <strong>Swiss</strong> National Science Foundation<br />
P140<br />
The Velumount ® device to treat obstructive sleep apnoea:<br />
does it work?<br />
W. Strobel.<br />
University Hospital Basel (Basel, CH)<br />
Introduction: The Velumount is a non approved device developed to<br />
reduce snoring and obstructive sleep apnoea (OSA). It is applied<br />
intraorally during night and is targeted to remove the soft palate from<br />
the dorsal pharnygeal wall. Despite an almost total lack of published<br />
medical data, due to an intensive media campaign, this device is<br />
widely used in Switzerland.<br />
Methods: I collected data from all sleep apnoea patients of our clinic,<br />
known to have tried the Velumount. I asked for general acceptance of<br />
the device, side effects, reduction of snoring and daytime sleepiness.<br />
In addition, nocturnal oximetries were performed and the results were<br />
compared with the baseline data.<br />
Results: 42 patients of our clinic tried the Velumount device.<br />
Information was available from 39 patients. All 39 patients were<br />
diagnosed with OSA syndrome (AHI 26 ± 11 / h, desaturation index<br />
(DI) = 23 ± 12 / h, Epworth Sleepiness Score (ESS) = 12.2 ± 4.2<br />
points). 19 patients were not able to tolerate CPAP, 20 patients used<br />
CPAP but wanted to try an alternative treatment.<br />
Compared with baseline, at the time of data acquisition under<br />
Velumount treatment, these 39 patients had lost 3.1 ± 3.0 kg of<br />
weight. 17 of these 39 patients (44 %) were not able to tolerate the<br />
Velumount. 22 patients were able to use the Velumount device at<br />
least 4 hours per night. In these 22 patients the ESS fell from 12.5 ±<br />
5.3 to 9.6 ± 4.7 points (p = 0.02). All patients but one reported a clear<br />
reduction in snoring. In 15 of these 22 patients a nocturnal oximetry<br />
under velomount treatment was performed: the DI fell from 22 ± 11 at<br />
baseline to 16 ± 10 / h (p = 0.04). However, in 12 of these 15 patients<br />
the DI under CPAP was 4 ± 4 / h.<br />
Conclusions:<br />
1. Approximately 40% of patients do not cope with the Velumount.<br />
2. Those who manage to use the Velumount feel a significant and<br />
relevant reduction of sleepiness and a clear reduction in snoring.<br />
3. Though statistically significant, the Velumount does not improve<br />
overnight oximetry results relevantly.<br />
4. The changes from baseline described above could be in part due<br />
to a weight loss of approx. 3 kg.<br />
5. Considering the discrepancy between subjective improvement in<br />
sleepiness and only small changes in oximetry, it seems likely, that<br />
some of the beneficial effects of the Velumount are due to a placebo<br />
effect.<br />
6. In conclusion, these scarce data do not support the use of the<br />
Velumount as a sufficient alternative therapy to CPAP.