Overview of Electronic Secondary Claims (COB)
Overview of Electronic Secondary Claims (COB)
Overview of Electronic Secondary Claims (COB)
Create successful ePaper yourself
Turn your PDF publications into a flip-book with our unique Google optimized e-Paper software.
<strong>Electronic</strong> <strong>Secondary</strong> <strong>Claims</strong> (<strong>COB</strong>) <strong>Overview</strong>-NextGen® PM<br />
<strong>Overview</strong> <strong>of</strong> <strong>Electronic</strong> <strong>Secondary</strong> <strong>Claims</strong> (<strong>COB</strong>)<br />
General Information<br />
This guide is designed to assist users in the set up and process <strong>of</strong> creating HIPAA ASC X12N 837<br />
<strong>Electronic</strong> <strong>Secondary</strong> <strong>Claims</strong> (<strong>COB</strong>) when primary payments have been posted manually by utilizing the<br />
<strong>COB</strong> window in Payment Posting.<br />
Payments posted when the NextGen® system loads 835/ERA file transactions via the ERA Posting<br />
Process automatically imports information required for generating electronic secondary claims. This<br />
eliminates the need to utilize the <strong>COB</strong> window in Payment Posting.<br />
Once the original set up <strong>of</strong> the <strong>COB</strong> process is complete, there is minimal effort required to set up<br />
additional payers.<br />
Getting Started<br />
First, verify if your EDI trading partner accepts electronic secondary claims by reviewing their payer listing<br />
located on their website or contacting them directly. Since Medicare claims are no longer accepted on<br />
paper without a waiver on file, electronic Medicare secondary claims are typically available. Consult with<br />
the trading partner on the process for uploading these secondary electronic claim files from the<br />
NextGen® system to their system.<br />
To manage the secondary claim files, a naming convention and filing system for these files should be<br />
determined. For example, a directory could be created called: <strong>Claims</strong> Folder>Medicare><strong>COB</strong> Files. It is<br />
important to place the directory for the downloaded files in a location that can be accessed by all the<br />
appropriate users who create and submit claim files.<br />
NEXTGEN® Healthcare, Inc. EPM<strong>Claims</strong><br />
© Copyright 2010 All Rights Reserved Confidential and Proprietary DO NOT COPY<br />
V5.6SP1 Sept2010 Page 1 <strong>of</strong> 29
<strong>Electronic</strong> <strong>Secondary</strong> <strong>Claims</strong> (<strong>COB</strong>) <strong>Overview</strong>-NextGen® PM<br />
<strong>Electronic</strong> <strong>Secondary</strong> <strong>Claims</strong> (<strong>COB</strong>) Set-Up<br />
Libraries<br />
Libraries>Reason Codes<br />
Reason Code Libraries provide the ability to configure business rules which can be used to automate<br />
electronic transaction posting.<br />
The HIPAA X12 Standard Reason Codes Library (File Maintenance > Libraries > Reason Codes) is<br />
preloaded in the NextGen® application and contains industry Standard Reason Codes. Only HIPAA X12<br />
Standard Reason Codes are permitted for electronic secondary claims.<br />
Libraries> Reason Codes> Reason Code Priority<br />
Reason Code Priority has two main purposes:<br />
1. To determine the order reason codes will display in the transaction posting screen & <strong>COB</strong> window<br />
during payment posting<br />
2. To determine which business rules take priority when multiple reason codes are used on one line<br />
item.<br />
For example, if one code indicates a transaction status <strong>of</strong> “Appeal” and the other code allows the<br />
remaining balance to be moved to the next responsible payer, the system will process the reason codes<br />
according to which reason code appears first in the priority list.<br />
Select a Reason Code Library. Right-click and select Reason Code Priority. To move a code to the top<br />
or to the bottom <strong>of</strong> the list, highlight the code and select the blue “up” or “down” double-arrows. Use the<br />
blue “up” and “down” single-arrow to move a code ine by line.<br />
NEXTGEN® Healthcare, Inc. EPM<strong>Claims</strong><br />
© Copyright 2010 All Rights Reserved Confidential and Proprietary DO NOT COPY<br />
V5.6SP1 Sept2010 Page 2 <strong>of</strong> 29
<strong>Electronic</strong> <strong>Secondary</strong> <strong>Claims</strong> (<strong>COB</strong>) <strong>Overview</strong>-NextGen® PM<br />
Best Practice: Move commonly used HIPAA reason codes to the top to easily select during manual<br />
payment posting. The four most commonly used HIPAA codes include:<br />
CO45: Charges exceed your contract<br />
PR1: Deductible Amount<br />
PR2: Coinsurance Amount<br />
PR3: Co-payment Amount<br />
If your organization has additional reason codes commonly used, feel free to prioritize them accordingly.<br />
For additional information regarding Reason code functionality, enroll in the ERA eLearning courses as<br />
well as reference the <strong>Electronic</strong> Remittance Advice <strong>Overview</strong> available for download from the NextGen<br />
Knowledge exchange.<br />
NEXTGEN® Healthcare, Inc. EPM<strong>Claims</strong><br />
© Copyright 2010 All Rights Reserved Confidential and Proprietary DO NOT COPY<br />
V5.6SP1 Sept2010 Page 3 <strong>of</strong> 29
<strong>COB</strong> Rsn Code<br />
<strong>Electronic</strong> <strong>Secondary</strong> <strong>Claims</strong> (<strong>COB</strong>) <strong>Overview</strong>-NextGen® PM<br />
Some payers use proprietary reason codes; however, electronic secondary claims require HIPAA X12<br />
reason codes. <strong>COB</strong> Rsn Code replaces the proprietary reason code with a HIPAA X12 reason codes.<br />
This can be used instead <strong>of</strong> or in conjunction with the default <strong>COB</strong> reason code in payer maintenance.<br />
In the example below, the user selected DED as the reason code while in the transaction posting screen<br />
but the PR1 populated in the Coordination <strong>of</strong> Benefits Information window.<br />
The electronic secondary claim will be created using the PR1 reason code and not DED.<br />
NEXTGEN® Healthcare, Inc. EPM<strong>Claims</strong><br />
© Copyright 2010 All Rights Reserved Confidential and Proprietary DO NOT COPY<br />
V5.6SP1 Sept2010 Page 4 <strong>of</strong> 29
Submitter Pr<strong>of</strong>ile<br />
<strong>Electronic</strong> <strong>Secondary</strong> <strong>Claims</strong> (<strong>COB</strong>) <strong>Overview</strong>-NextGen® PM<br />
Default MSP (Medicare <strong>Secondary</strong> Payer) Type Code<br />
MSP Reason code (referred to interchangeably as MSP Type Code, insurance type code or the MSP<br />
Reason) identifies the type <strong>of</strong> other insurance specific to the beneficiary‟s MSP status. For claims billed<br />
electronically, the code is submitted in loop 2000B SBR05 segment <strong>of</strong> the 837P ANSI X12 4010 format.<br />
This code may be setup to automatically default if enabled by a Submitter Pr<strong>of</strong>ile setting.<br />
*NOTE: This setting pertains only to 837P/1500 MSP claims<br />
In File Maintenance, after opening the Submitter Pr<strong>of</strong>ile Library, click the Exception Options tab, scroll<br />
down to Subscriber Information (2000B Loop SBR Segments) - Override Insurance type code on<br />
Medicare <strong>Secondary</strong>/Tertiary <strong>Claims</strong>. Under the Setting column click the down arrow for a list <strong>of</strong> MSP<br />
type codes.<br />
Best Practice-Select “12 - Working Aged Beneficiary”. This type code is most likely to match what<br />
Medicare has on record.<br />
NEXTGEN® Healthcare, Inc. EPM<strong>Claims</strong><br />
© Copyright 2010 All Rights Reserved Confidential and Proprietary DO NOT COPY<br />
V5.6SP1 Sept2010 Page 5 <strong>of</strong> 29
Exceptions to Default MSP Reason Code<br />
<strong>Electronic</strong> <strong>Secondary</strong> <strong>Claims</strong> (<strong>COB</strong>) <strong>Overview</strong>-NextGen® PM<br />
When the patient‟s MSP type code is different from the default setting in the Submitter Pr<strong>of</strong>ile you may<br />
assign the appropriate one in the MSP Reason Code field in the encounter Insurance Maintenance<br />
window.<br />
Select the “Detail – 2” tab. On “MSP Reason Code” click the down arrow for a listing <strong>of</strong> acceptable MSP<br />
values and select the appropriate one for this patient.<br />
NEXTGEN® Healthcare, Inc. EPM<strong>Claims</strong><br />
© Copyright 2010 All Rights Reserved Confidential and Proprietary DO NOT COPY<br />
V5.6SP1 Sept2010 Page 6 <strong>of</strong> 29
Payer Master File<br />
<strong>Electronic</strong> <strong>Secondary</strong> <strong>Claims</strong> (<strong>COB</strong>) <strong>Overview</strong>-NextGen® PM<br />
Master Files > System > Payer Master File > Practice Tab><strong>Claims</strong> Sub-Tab<br />
First set the <strong>Secondary</strong> Media Type field to “<strong>Electronic</strong>” on the Practice Tab‟s <strong>Claims</strong> sub tab<br />
Verify „When Primary, force <strong>Secondary</strong> claims to Paper‟ is unchecked.<br />
If you also process UB (837I) secondary claims, repeat the setup on the UB <strong>Claims</strong> tab.<br />
NEXTGEN® Healthcare, Inc. EPM<strong>Claims</strong><br />
© Copyright 2010 All Rights Reserved Confidential and Proprietary DO NOT COPY<br />
V5.6SP1 Sept2010 Page 7 <strong>of</strong> 29
<strong>Electronic</strong> <strong>Secondary</strong> <strong>Claims</strong> (<strong>COB</strong>) <strong>Overview</strong>-NextGen® PM<br />
Master Files >System Tab >System Tab ><strong>COB</strong> <strong>Electronic</strong> <strong>Claims</strong><br />
The <strong>COB</strong> <strong>Electronic</strong> <strong>Claims</strong> sub-tab <strong>of</strong>fers several options. These options should only be enabled on<br />
NextGen® advisement. As a System tab option, all payers across the enterprise will be affected.<br />
Populate 2400 CN1 contractual adjustment segment<br />
o Select this option to add a service line CN1 segment (2400). This amount is also referred<br />
to as the OTAF (obligated to accept in full) amount. If this option is enabled and a service<br />
line contractual adjustment exists (CAS*CO), then the allowed amount is added as the<br />
2400 CN1 amount. The presence <strong>of</strong> the CAS*CO segment causes the CN1 segment to<br />
create mimicking the allowed/approved amount in AMT*AAE<br />
Medicare payers should have this enabled<br />
Enable <strong>COB</strong> Window information popup in payment entry<br />
o Select this option so when this payer is secondary, the Coordination <strong>of</strong> Benefits<br />
Information window automatically displays when the user tabs out <strong>of</strong> the Reason field for<br />
the last transaction detail row<br />
Populate 2320 AMT*F2 patient responsibility amount segment (4010 only)<br />
o Select this option to add a claim level AMT*F2 segment. If this option is enabled and a<br />
service line patient responsible adjustment exists (CAS*PR), the patient responsibility<br />
amount will be added in 2320 AMT*F2. The presence <strong>of</strong> the CAS*PR segment causes<br />
the AMT*F2 segment to create<br />
Populate claim-level adjudication date in 2330B DTP*573<br />
o Update description to say 2330B DTP*573<br />
Suppress other payer detail line 2430 loop<br />
o No change. Functions the same way in 5010<br />
Populate 2320 SBR04 with primary MSP payer ID or name<br />
o Selection this option to add the primary payer‟s MSP payer ID or name into 2320 SBR04<br />
NEXTGEN® Healthcare, Inc. EPM<strong>Claims</strong><br />
© Copyright 2010 All Rights Reserved Confidential and Proprietary DO NOT COPY<br />
V5.6SP1 Sept2010 Page 8 <strong>of</strong> 29
<strong>Electronic</strong> <strong>Secondary</strong> <strong>Claims</strong> (<strong>COB</strong>) <strong>Overview</strong>-NextGen® PM<br />
Master Files >System Tab >System Tab ><strong>COB</strong> <strong>Electronic</strong> <strong>Claims</strong> (cont’d)<br />
Populate 2320 claim level approved/allowed amounts (4010 only)<br />
o Select this option to add claim level (2320) AMT segments if the comparable segment<br />
exists at the service line level. This option will be sensitive to file format (pr<strong>of</strong>essional or<br />
institutional) and only inserts segments appropriate to the file type<br />
Pr<strong>of</strong>essional file added segments:<br />
2320 AMT*AAE (sum <strong>of</strong> all 2400 AMT*AAE segments)<br />
2320 AMT*B6 (sum <strong>of</strong> all 2400 AMT*AAE segments)<br />
2320 AMT*F2 (sum <strong>of</strong> all 2430 CAS*PR segments)<br />
Institutional file added segments:<br />
2320 AMT*F2 (sum <strong>of</strong> all 2430 CAS*PR segments)<br />
Populate 2320 CAS claim level adjustment amount (4010 only)<br />
o Select this option to add claim level (2300) CAS segments if the comparable segment<br />
exists at the service line level. These segments are the same for the different file formats<br />
(pr<strong>of</strong>essional or institutional). Only one claim-level CAS segment is allowed per individual<br />
group code. The two most common segments are listed below:<br />
2320 CAS*CO sums all service line level CAS*CO segments and adds one claim<br />
level segment with that total. Only one instance <strong>of</strong> a claim level CAS*CO is<br />
allowed. If multiple CAS*CO segments exist at the service line level with different<br />
reason codes, they are all combined in one claim level CAS*CO with the reason<br />
codes repeating in fields 02, 05, 08, 11, 14, and 17. The corresponding amounts<br />
are placed in fields 03, 06, 09, 12, 15, and 18<br />
2320 CAS*PR sums all service line level CAS*PR segments and adds one claim<br />
level segment with that total. Only one instance <strong>of</strong> a claim level CAS*PR is<br />
allowed. Multiple service line PR adjustments are handled as described above for<br />
the CAS segment<br />
NEXTGEN® Healthcare, Inc. EPM<strong>Claims</strong><br />
© Copyright 2010 All Rights Reserved Confidential and Proprietary DO NOT COPY<br />
V5.6SP1 Sept2010 Page 9 <strong>of</strong> 29
Practice Preferences<br />
<strong>Electronic</strong> <strong>Secondary</strong> <strong>Claims</strong> (<strong>COB</strong>) <strong>Overview</strong>-NextGen® PM<br />
Master Files > Practices > Preferences > Transactions<br />
Attaching Default Reason Code Library<br />
If a Reason Code Library is not selected on the Payer Master, the payment posting process (manual or<br />
ERA) will use the Default Reason Code Library selected in NextGen® File Maintenance (Master Files ><br />
Practices > Preferences > Transactions) Default Reason Code Library.<br />
Warn on <strong>COB</strong> Imbalance<br />
When closing the <strong>COB</strong> info entry form, a balance check will be done on the <strong>COB</strong> information. The user<br />
will get the following warning if there is an imbalance (Master Files > Practices > Preferences ><br />
Transactions) Warn on <strong>COB</strong> Imbalance.<br />
NEXTGEN® Healthcare, Inc. EPM<strong>Claims</strong><br />
© Copyright 2010 All Rights Reserved Confidential and Proprietary DO NOT COPY<br />
V5.6SP1 Sept2010 Page 10 <strong>of</strong> 29
Free Text Line Item Reason Codes<br />
<strong>Electronic</strong> <strong>Secondary</strong> <strong>Claims</strong> (<strong>COB</strong>) <strong>Overview</strong>-NextGen® PM<br />
To free text reason codes on the transaction line during payment posting, select the option in Practices<br />
master file in NextGen® File Maintenance (Master Files > Practices > Preferences > Transactions) Free<br />
text line item reason codes.<br />
In the Reasons field, enter the reason code; using a comma to separate if there is more than one:<br />
When tabbing out <strong>of</strong> the reason code field, it will pull in the code and description from the reason code.<br />
NEXTGEN® Healthcare, Inc. EPM<strong>Claims</strong><br />
© Copyright 2010 All Rights Reserved Confidential and Proprietary DO NOT COPY<br />
V5.6SP1 Sept2010 Page 11 <strong>of</strong> 29
<strong>COB</strong> Process Flow<br />
<strong>Electronic</strong> <strong>Secondary</strong> <strong>Claims</strong> (<strong>COB</strong>) <strong>Overview</strong>-NextGen® PM<br />
Payment posting begins with the creation <strong>of</strong> a posting batch. This document will describe the pertinent<br />
information required for creating a balanced <strong>COB</strong> claim under the assumption the user is pr<strong>of</strong>icient in<br />
manual transaction posting within the NextGen® application.<br />
Adjudication Date- Batch Header Default<br />
The adjudication date is the date the primary payer paid the claim. The adjudication date is an EDI<br />
requirement for all electronic secondary claims.<br />
Batch Maintenance Header<br />
If you are posting multiple checks in a single batch where the adjudication dates are different, leave<br />
Adjudication Date blank.<br />
NEXTGEN® Healthcare, Inc. EPM<strong>Claims</strong><br />
© Copyright 2010 All Rights Reserved Confidential and Proprietary DO NOT COPY<br />
V5.6SP1 Sept2010 Page 12 <strong>of</strong> 29
Allowed Amount- Payment Entry<br />
<strong>Electronic</strong> <strong>Secondary</strong> <strong>Claims</strong> (<strong>COB</strong>) <strong>Overview</strong>-NextGen® PM<br />
The Allowed Amount is required for the secondary electronic claim to balance. If an allowed amount is<br />
not listed on your EOB, enter the maximum amount <strong>of</strong> the billed charge the primary payer deemed<br />
payable by the plan for covered services or supply rendered.<br />
When there are no “PR” adjustments to post, enter the charge amount as the allowed amount on the<br />
payment transaction line so it defaults to the <strong>COB</strong> window. This typically happens when a denial is<br />
received. Post the $0.00 payment transaction and enter the value <strong>of</strong> the “Billed Amount” in the “Allowed<br />
Amt” field in order to meet the balancing requirement with the “Allowed Amount” formula.<br />
NEXTGEN® Healthcare, Inc. EPM<strong>Claims</strong><br />
© Copyright 2010 All Rights Reserved Confidential and Proprietary DO NOT COPY<br />
V5.6SP1 Sept2010 Page 13 <strong>of</strong> 29
Transaction Posting<br />
<strong>Electronic</strong> <strong>Secondary</strong> <strong>Claims</strong> (<strong>COB</strong>) <strong>Overview</strong>-NextGen® PM<br />
Once you have entered all the transaction information for every detail row, click on the <strong>COB</strong> button to<br />
access the Coordination <strong>of</strong> Benefits Information window. CPT4 codes, billed (charge amt), paid, allowed<br />
and reason codes will default. With the exception <strong>of</strong> the Allowed, these values are read-only and must<br />
be entered or corrected on the actual transaction detail row.<br />
Enter the corresponding adjustment amount for each reason code.<br />
NEXTGEN® Healthcare, Inc. EPM<strong>Claims</strong><br />
© Copyright 2010 All Rights Reserved Confidential and Proprietary DO NOT COPY<br />
V5.6SP1 Sept2010 Page 14 <strong>of</strong> 29
Balancing <strong>COB</strong> Window<br />
<strong>Electronic</strong> <strong>Secondary</strong> <strong>Claims</strong> (<strong>COB</strong>) <strong>Overview</strong>-NextGen® PM<br />
Certain elements <strong>of</strong> the electronic file are required to balance. There are two balancing formulas<br />
associated with the <strong>COB</strong> window:<br />
1. Paid Amount + Sum <strong>of</strong> all Adjustments (including PR‟s) = Billed Amount (charge amount)<br />
2. Paid Amount + Sum <strong>of</strong> all Patient Responsibility (PR‟s) amounts = Allowed Amount<br />
If the allowed amount is empty, update each payment row for the <strong>COB</strong> claim to balance.<br />
If "Warn on <strong>COB</strong> imbalance” is checked in Practice Preferences, the system will display a message if the<br />
balancing calculations are incorrect:<br />
NEXTGEN® Healthcare, Inc. EPM<strong>Claims</strong><br />
© Copyright 2010 All Rights Reserved Confidential and Proprietary DO NOT COPY<br />
V5.6SP1 Sept2010 Page 15 <strong>of</strong> 29
<strong>Electronic</strong> <strong>Secondary</strong> <strong>Claims</strong> (<strong>COB</strong>) <strong>Overview</strong>-NextGen® PM<br />
Adding Reason Code Lines to the <strong>COB</strong> Window<br />
To do so, click on the<br />
CPT code row so it is<br />
highlighted.<br />
Then right click and<br />
select New.<br />
May also click on the<br />
Norton button and select<br />
New.<br />
Once you select New, another bracket will appear on the left and the reason code field will open with the<br />
drop down. Select the appropriate patient responsible (PR) reason code and tab over to enter the<br />
corresponding Rsn Amount.<br />
NEXTGEN® Healthcare, Inc. EPM<strong>Claims</strong><br />
© Copyright 2010 All Rights Reserved Confidential and Proprietary DO NOT COPY<br />
V5.6SP1 Sept2010 Page 16 <strong>of</strong> 29
Continue that same process<br />
for each CPT code row until<br />
all rows have a reason code<br />
and amount.<br />
<strong>Electronic</strong> <strong>Secondary</strong> <strong>Claims</strong> (<strong>COB</strong>) <strong>Overview</strong>-NextGen® PM<br />
If the primary insurance pays the entire charge row and no balance is left, then no reason codes<br />
and amounts are required.<br />
Once all the reason code information, their corresponding amounts and an adjudication date are<br />
entered, click OK to save that information.<br />
Screen shot here for updating Allowed amt?<br />
NEXTGEN® Healthcare, Inc. EPM<strong>Claims</strong><br />
© Copyright 2010 All Rights Reserved Confidential and Proprietary DO NOT COPY<br />
V5.6SP1 Sept2010 Page 17 <strong>of</strong> 29
<strong>Electronic</strong> <strong>Secondary</strong> <strong>Claims</strong> (<strong>COB</strong>) <strong>Overview</strong>-NextGen® PM<br />
When the <strong>COB</strong> window closes, you are back on the Payment Entry screen. Click<br />
Recalc and then Save to save your transaction and the <strong>COB</strong> information.<br />
NEXTGEN® Healthcare, Inc. EPM<strong>Claims</strong><br />
© Copyright 2010 All Rights Reserved Confidential and Proprietary DO NOT COPY<br />
V5.6SP1 Sept2010 Page 18 <strong>of</strong> 29
Editing Batch and <strong>COB</strong> Window<br />
As long as the batch is not posted, you<br />
may still access the <strong>COB</strong> window for<br />
any particular transaction. To do so,<br />
open the Batch Posting window and<br />
select your batch. Right click to display<br />
the menu and select Ledger.<br />
<strong>Electronic</strong> <strong>Secondary</strong> <strong>Claims</strong> (<strong>COB</strong>) <strong>Overview</strong>-NextGen® PM<br />
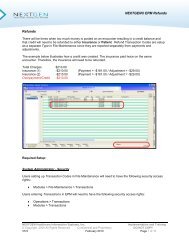
The Transaction Ledger will display listing all payments and transaction<br />
in that batch along with the associated encounter number (Source<br />
column). You may double-click on either the payment or adjustment to<br />
re-access the Payment entry screen.<br />
NEXTGEN® Healthcare, Inc. EPM<strong>Claims</strong><br />
© Copyright 2010 All Rights Reserved Confidential and Proprietary DO NOT COPY<br />
V5.6SP1 Sept2010 Page 19 <strong>of</strong> 29
<strong>Electronic</strong> <strong>Secondary</strong> <strong>Claims</strong> (<strong>COB</strong>) <strong>Overview</strong>-NextGen® PM<br />
Once back on the Payment Entry, click the <strong>COB</strong> button to bring up the <strong>COB</strong> Information window where<br />
the reason code, amount and adjudication date fields are available to edit.<br />
Another way to access the <strong>COB</strong> information from Payment Entry screen is to double click on the green<br />
checkmark in the <strong>COB</strong> column.<br />
After the batch is posted, you must view or edit <strong>COB</strong> information from each individual encounter. On the<br />
Patient Chart, select Transactions side tab, highlight a transaction and right click to select Transaction<br />
Detail.<br />
NEXTGEN® Healthcare, Inc. EPM<strong>Claims</strong><br />
© Copyright 2010 All Rights Reserved Confidential and Proprietary DO NOT COPY<br />
V5.6SP1 Sept2010 Page 20 <strong>of</strong> 29
<strong>Electronic</strong> <strong>Secondary</strong> <strong>Claims</strong> (<strong>COB</strong>) <strong>Overview</strong>-NextGen® PM<br />
The Payment Entry window will indicate the transaction is posted. In order to change the allowed<br />
amount, reason codes, amounts or adjudication date, simply open the <strong>COB</strong> window.<br />
Note: Changing this information after an initial claim is transmitted will result in different <strong>COB</strong> information<br />
in the resubmitted claim.<br />
NEXTGEN® Healthcare, Inc. EPM<strong>Claims</strong><br />
© Copyright 2010 All Rights Reserved Confidential and Proprietary DO NOT COPY<br />
V5.6SP1 Sept2010 Page 21 <strong>of</strong> 29
<strong>Electronic</strong> <strong>Secondary</strong> <strong>Claims</strong> (<strong>COB</strong>) <strong>Overview</strong>-NextGen® PM<br />
When filing Medicare <strong>Secondary</strong> Payer (MSP) 837I/UB claims electronically specific codes are required.<br />
E.g. Condition Codes, Value Codes, Occurrence Codes. Enter these codes with their respective amounts<br />
on the Encounter>UB tab while posting the primary payment. The <strong>COB</strong> window does not<br />
Medicare has indicated overpayments occurring when a provider does not correctly indicate on the claim<br />
if there is a contractual arrangement between the provider and the primary payer.<br />
To do this, the provider must report either a Condition Code 77 or Value Code 44 and the expected<br />
amount.<br />
Shown Above: Encounter>UB>Value Codes<br />
NEXTGEN® Healthcare, Inc. EPM<strong>Claims</strong><br />
© Copyright 2010 All Rights Reserved Confidential and Proprietary DO NOT COPY<br />
V5.6SP1 Sept2010 Page 22 <strong>of</strong> 29
<strong>Electronic</strong> <strong>Secondary</strong> <strong>Claims</strong> (<strong>COB</strong>) <strong>Overview</strong>-NextGen® PM<br />
Shown below: Encounter>UB>Condition Codes or Value Codes<br />
This information is then sent in Loop 2300 HI BE segment. Since MSP billing requirements are<br />
dependent upon many variables, be sure to research the MSP guidelines available at<br />
www.ngsmedicare.com or www.cms.gov to identify your particular service requirements. Only then you<br />
will know amounts to calculate, which codes to use and when they are required.<br />
NEXTGEN® Healthcare, Inc. EPM<strong>Claims</strong><br />
© Copyright 2010 All Rights Reserved Confidential and Proprietary DO NOT COPY<br />
V5.6SP1 Sept2010 Page 23 <strong>of</strong> 29
<strong>Electronic</strong> <strong>Secondary</strong> <strong>Claims</strong> (<strong>COB</strong>) <strong>Overview</strong>-NextGen® PM<br />
Transaction Posting with Encounter Rate Billing<br />
Primary payers, such as Medicare, which are setup to split-bill an encounter rate on a UB claim to<br />
Medicare Part A with an alternate payer for carve-out services on a 1500 claim to Medicare Part B, may<br />
present some challenges with secondary claims.<br />
<strong>Secondary</strong> payers receiving fee-for-service on a 1500 claim will generally want to see the payments and<br />
adjustments from the primary payer documented on the secondary claim<br />
Additional documentation titled “EPM Encounter Rate Billing and <strong>Secondary</strong> <strong>Claims</strong>” has been<br />
created to guide you through the following:<br />
Process <strong>of</strong> posting transactions from a primary encounter rate payer creating a balanced<br />
electronic secondary claim for a fee-for-service secondary payer<br />
Process <strong>of</strong> posting transactions from a primary payment from Medicare Part B to the carve-out<br />
services to create a balanced secondary claim<br />
When to use the NextGen® Portal<br />
This information is available in the NextGen® Knowledge Exchange.<br />
NEXTGEN® Healthcare, Inc. EPM<strong>Claims</strong><br />
© Copyright 2010 All Rights Reserved Confidential and Proprietary DO NOT COPY<br />
V5.6SP1 Sept2010 Page 24 <strong>of</strong> 29
<strong>Electronic</strong> <strong>Secondary</strong> <strong>Claims</strong> (<strong>COB</strong>) <strong>Overview</strong>-NextGen® PM<br />
Claim Edits & Billing - Reviewing Claim Production Status Report<br />
To prevent unbalanced secondary claims from creating, several claim edits are available:<br />
254: <strong>COB</strong> edit: Paid amount and patient responsible amounts do not equal allowed amount<br />
255: <strong>COB</strong> edit: All payments and adjustments do not equal billed amount<br />
256: Value code 39a <strong>of</strong> required for secondary institutional claim<br />
o Only for client‟s sending 837I<br />
261: <strong>Electronic</strong> <strong>COB</strong> claim requires adjudication date<br />
As with all claim edits, in order to prevent an encounter from producing a claim when the edit is fired, set<br />
the edit severity to „Required‟.<br />
If you set the claim edit severity to „Warning‟, you may correct the encounter and rebill before generating<br />
the next <strong>Secondary</strong> EDI file. Be sure to delete the previous claim generated. Otherwise two claims will<br />
be generated, one balanced and other unbalanced.<br />
<strong>COB</strong> edits will only fire if a Payer‟s <strong>Secondary</strong> Media Type is set to “Paper” and only when you are billing<br />
encounters.<br />
NEXTGEN® Healthcare, Inc. EPM<strong>Claims</strong><br />
© Copyright 2010 All Rights Reserved Confidential and Proprietary DO NOT COPY<br />
V5.6SP1 Sept2010 Page 25 <strong>of</strong> 29
Generating <strong>Secondary</strong> EDI Files<br />
<strong>Electronic</strong> <strong>Secondary</strong> <strong>Claims</strong> (<strong>COB</strong>) <strong>Overview</strong>-NextGen® PM<br />
Primary claims can still be generated without affecting secondary claims. When ready to generate secondary<br />
claims, access the EDI File icon, click on the “Advanced” tab. Deselect the “Primary” and “Tertiary” options to<br />
produce secondary claims in an EDI file separately.<br />
BBP (Background Business Processer)<br />
Uncheck Primary and Tertiary field to<br />
generate a <strong>Secondary</strong> file separately.<br />
Don‟t forget your star employee “Billy Bob Processer” (BBP). BBP is dependent upon your instructions<br />
and guidance on assignments. When considering queuing up Batch Billing and EDI files in the same run:<br />
Make sure your BBP is set up only to include “Primary” claims and not secondary‟s too, since it<br />
requires monitoring <strong>of</strong> the Claim Production Status report for any out <strong>of</strong> balance <strong>COB</strong> claims that<br />
may be edited.<br />
Generating secondary claim files should be done manually until version 5.5.28.28 where the edits<br />
are included in the Claim Edit Library.<br />
Remember; treat BBP as you would any other employee. Check in and verify work is completed correctly<br />
and in the time you specified on a consistent basis. If BBP jobs fail, verify the instructions you‟ve given<br />
match what BBP is performing.<br />
NEXTGEN® Healthcare, Inc. EPM<strong>Claims</strong><br />
© Copyright 2010 All Rights Reserved Confidential and Proprietary DO NOT COPY<br />
V5.6SP1 Sept2010 Page 26 <strong>of</strong> 29
NextGen® Portal<br />
<strong>Electronic</strong> <strong>Secondary</strong> <strong>Claims</strong> (<strong>COB</strong>) <strong>Overview</strong>-NextGen® PM<br />
<strong>COB</strong> functionality not currently supported may require editing secondary claims outside <strong>of</strong> the NextGen®<br />
application. Some clearinghouses allow you to edit secondary electronic claims with the correct<br />
information. Otherwise, as a workaround, NextGen® <strong>of</strong>fers a free product called the NextGen® Portal.<br />
Instances requiring secondary claims to be edited outside <strong>of</strong> the NextGen® application:<br />
DT Reviewed-Not Scheduled/Problem 12370-837I UB <strong>Secondary</strong> Billing<br />
Missing <strong>COB</strong> Total Submitted Charges-2320 AMT*T3 segment<br />
DT#55372/Problem 9386-Scheduled 5.6SP2-Encounter Rate Billing & <strong>Electronic</strong> <strong>Secondary</strong><br />
Encounter Rate Primary (837I/UB) and <strong>Secondary</strong> (837P/1500)<br />
Primary FFS (837P/1500) and Encounter Rate <strong>Secondary</strong> (837I/UB)<br />
Training for the NextGen® Portal is a non-billable service <strong>of</strong>fered as a separate one hour WebEx<br />
designed for an organization‟s Core Group or Super Users. Working knowledge <strong>of</strong> payment processing,<br />
including the use <strong>of</strong> the <strong>COB</strong> window is a prerequisite to Portal training.<br />
Log a support ticket specifically requesting <strong>COB</strong> Portal training and your ticket will be routed to an EDI<br />
Systems Analyst for scheduling.<br />
NEXTGEN® Healthcare, Inc. EPM<strong>Claims</strong><br />
© Copyright 2010 All Rights Reserved Confidential and Proprietary DO NOT COPY<br />
V5.6SP1 Sept2010 Page 27 <strong>of</strong> 29
<strong>Electronic</strong> <strong>Secondary</strong> <strong>Claims</strong> (<strong>COB</strong>) <strong>Overview</strong>-NextGen® PM<br />
Appendix A- Troubleshooting MSP (Medicare <strong>Secondary</strong> Payer) Rejections<br />
o CO16-This claim lacks additional information to adjudicate this claim<br />
MSP reason code submitted does not match what Medicare has on file due to an<br />
incorrect MSP code submission<br />
Update the valid MSP code in Patient Insurance Maintenance>Details 2 tab<br />
for each encounter effected and rebill<br />
o OTAF (Obligated to Accept in Full) record is missing<br />
Medicare denial for missing record<br />
Verify Payer Master>System><strong>Electronic</strong> <strong>Claims</strong>> <strong>Electronic</strong><br />
<strong>Secondary</strong>>Check box “Populate 2400 CN1 contractual adjustments”<br />
This should be checked for any Medicare type pay<br />
Appendix B-Defects and Enhancements<br />
DT#47641/Problem6809-Fixed 5.6-Multiple transactions being applied which creates additional<br />
transaction display pages. (i.e. Page 1 <strong>of</strong> 3): Whenever more than one type <strong>of</strong> transaction<br />
(payment) is applied to the same line item at different intervals, each <strong>COB</strong> window entry is added<br />
together incorrectly. Examples where multiple transactions can be applied:<br />
o Split Primary Claim Payments<br />
o Payment comes in and only applies to specified line items (not all) and is posted.<br />
Another payment is received (possibly same day) applied to other line item(s)<br />
o Denied <strong>Claims</strong><br />
o Zero payment applied first. <strong>Claims</strong> appeal results in payment<br />
DT#44501/Problem 7248/Fixed 5.6- “Allowed” amount field within the <strong>COB</strong> window is not<br />
editable. If not entered during transaction posting or populated incorrectly by a contract loaded<br />
DT#42957Problem 4762-TBD-Encounter>Ins maintenance>Ability to make the MSP reason code<br />
a required field<br />
DT#45649/Problem/Fixed 5.6- Claim Bundling <strong>of</strong> like CPT codes-Utilizing “Do Not Sum Units for<br />
CPT 4 Code” settings in Practice preferences, Payers, or SIM<br />
DT#55372/Problem 9386-Scheduled 5.6SP2-Encounter Rate Billing & <strong>Electronic</strong> Secondaries<br />
1. Encounter Rate Primary (837I/UB) and <strong>Secondary</strong> (837P/1500)<br />
2. Primary FFS (837P/1500) and Encounter Rate <strong>Secondary</strong> (837I/UB)<br />
DT#46804/Problem 3043–Scheduled 5.6SP2-<strong>COB</strong>: Need an edit and/or warning message for<br />
missing adjudication date<br />
DT#45648/Problem 8238-TBD-Change <strong>COB</strong> Logic popup to only POP up when secondary<br />
insurance is attached and secondary insurance is set to paper.<br />
NEXTGEN® Healthcare, Inc. EPM<strong>Claims</strong><br />
© Copyright 2010 All Rights Reserved Confidential and Proprietary DO NOT COPY<br />
V5.6SP1 Sept2010 Page 28 <strong>of</strong> 29
<strong>Electronic</strong> <strong>Secondary</strong> <strong>Claims</strong> (<strong>COB</strong>) <strong>Overview</strong>-NextGen® PM<br />
Appendix C- Handling Specialized Transactions (PQRI)<br />
PQRI- Physicians Quality Reporting Initiatives<br />
Must post as a $0.00 charge in order for the <strong>COB</strong> functionality to work as designed. When<br />
applying primary payment received, enter an allowed amount <strong>of</strong> 0.00 on the corresponding PQRI<br />
transaction and enter appropriately for any other billable charges involved.<br />
Within the <strong>COB</strong> window, do not add any reason codes and/or reason values associated to the PQRI rowonly<br />
to other chargeable line items with balances.<br />
Access Balance Control and check “R” for re-bill alongside the corresponding Ins2 Amt column <strong>of</strong> the<br />
PQRI SIM row so it will be included along with any other qualifying charge transactions(s) within the<br />
secondary electronic file.<br />
NEXTGEN® Healthcare, Inc. EPM<strong>Claims</strong><br />
© Copyright 2010 All Rights Reserved Confidential and Proprietary DO NOT COPY<br />
V5.6SP1 Sept2010 Page 29 <strong>of</strong> 29