Total hip replacement - College of Occupational Therapists
Total hip replacement - College of Occupational Therapists
Total hip replacement - College of Occupational Therapists
You also want an ePaper? Increase the reach of your titles
YUMPU automatically turns print PDFs into web optimized ePapers that Google loves.
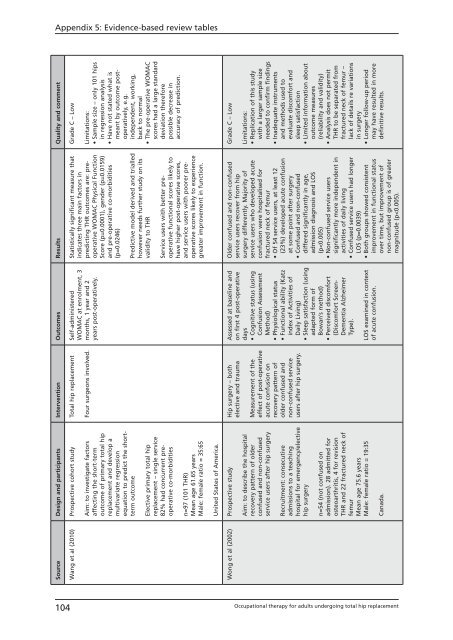
Appendix 5: Evidence- based review tables<br />
Source Design and participants Intervention Outcomes Results Quality and comment<br />
Wang et al (2010) Prospective cohort study<br />
Aim: to investigate factors<br />
affecting the short-term<br />
outcome <strong>of</strong> primary total <strong>hip</strong><br />
<strong>replacement</strong> and develop a<br />
multivariate regression<br />
equation to predict the shortterm<br />
outcome<br />
Elective primary total <strong>hip</strong><br />
<strong>replacement</strong> – single service<br />
82% had concurrent preoperative<br />
co- morbidities<br />
n=97 (101 THR)<br />
Mean age 61.65 years<br />
Male: female ratio = 35:65<br />
<strong>Total</strong> <strong>hip</strong> <strong>replacement</strong><br />
Four surgeons involved.<br />
Self-administered<br />
WOMAC at enrolment, 3<br />
months, 1 year and 2<br />
years post- operatively.<br />
Statistically significant measure that<br />
indicates three main factors in<br />
predicting THR outcomes are: preoperative<br />
WOMAC Physical Function<br />
Score (p=0.0001), gender (p=0.0159)<br />
and pre- operative co- morbidities<br />
(p=0.0246)<br />
Predictive model derived and trialled<br />
however needs further study on its<br />
validity to THR<br />
Service users with better preoperative<br />
functional scores likely to<br />
have higher post- operative scores,<br />
and service users with poorer preoperative<br />
scores likely to experience<br />
greater improvement in function.<br />
Grade C – Low<br />
Limitations:<br />
• Sample size – only 101 <strong>hip</strong>s<br />
in regression analysis<br />
• Have not stated what is<br />
meant by outcome postoperatively,<br />
e.g.<br />
independent, working,<br />
back to normal<br />
• The pre- operative WOMAC<br />
scores had a large standard<br />
deviation therefore<br />
possible decrease in<br />
accuracy <strong>of</strong> prediction.<br />
United States <strong>of</strong> America.<br />
Wong et al (2002) Prospective study<br />
Aim: to describe the hospital<br />
recovery pattern <strong>of</strong> older<br />
confused and non- confused<br />
service users after <strong>hip</strong> surgery<br />
Recruitment: consecutive<br />
admissions to a teaching<br />
hospital for emergency/elective<br />
<strong>hip</strong> surgery<br />
n=54 (not confused on<br />
admission). 28 admitted for<br />
osteoarthritis, 4 for revision<br />
THR and 22 fractured neck <strong>of</strong><br />
femur<br />
Mean age 75.6 years<br />
Male: female ratio = 19:35<br />
Canada.<br />
Hip surgery – both<br />
elective and trauma<br />
Measurement <strong>of</strong> the<br />
effect <strong>of</strong> post- operative<br />
acute confusion on<br />
recovery pattern <strong>of</strong><br />
older confused and<br />
non- confused service<br />
users after <strong>hip</strong> surgery.<br />
Assessed at baseline and<br />
on first 4 post- operative<br />
days<br />
• Cognitive status (using<br />
Confusion Assessment<br />
Method)<br />
• Physiological status<br />
• Functional ability (Katz<br />
index <strong>of</strong> Activities <strong>of</strong><br />
Daily Living)<br />
• Sleep satisfaction (using<br />
adapted form <strong>of</strong><br />
Bowan’s method)<br />
• Perceived discomfort<br />
(Discomfort Screen-<br />
Dementia Alzheimer<br />
Type).<br />
LOS examined in context<br />
<strong>of</strong> acute confusion.<br />
Older confused and non- confused<br />
service users recover from <strong>hip</strong><br />
surgery differently. Majority <strong>of</strong><br />
service users who developed acute<br />
confusion were hospitalised for<br />
fractured neck <strong>of</strong> femur<br />
• Of 54 service users, at least 12<br />
(23%) developed acute confusion<br />
at some point after surgery<br />
• Confused and non- confused<br />
differed significantly in age,<br />
admission diagnosis and LOS<br />
(p