Download the PDF
Download the PDF
Download the PDF
Create successful ePaper yourself
Turn your PDF publications into a flip-book with our unique Google optimized e-Paper software.
CET CONTINUING<br />
EDUCATION<br />
& TRAINING<br />
1 FREE CET POINT<br />
Approved for: Optometrists 4<br />
Dispensing Opticians 4<br />
OT CET content supports Optometry Giving Sight<br />
Retinoscopy in infancy:<br />
cycloplegic versus non-cycloplegic<br />
C-18551 O/D<br />
Fabrizio Bonci, Dip. Optom (ITA), MCOptom<br />
Luigi Lupelli, Dip. Optom (ITA), FAILAC, FIACLE, FBCLA<br />
The assessment of refractive status in very young children is often not conducted<br />
in <strong>the</strong> same manner as for adult patients. In particular, <strong>the</strong> child’s age, <strong>the</strong>ir cooperation<br />
and dynamic refractive status will be key factors which influence <strong>the</strong><br />
accuracy of refraction. For this reason, it is often necessary to choose procedures<br />
which inhibit or minimise accommodative activity. This can be achieved by<br />
fogging with positive lenses or rousing <strong>the</strong> tonic (resting) accommodation<br />
(dry refraction), or with pharmacological agents (wet refraction). This review<br />
article compares <strong>the</strong> two approaches, focusing on <strong>the</strong> retinoscopy techniques.<br />
Dry retinoscopy<br />
Static retinoscopy<br />
The patient views a distance target (foursix<br />
metres) so that accommodation is<br />
presumed to be static and in a relaxed<br />
condition. The fixating eye (contralateral<br />
to <strong>the</strong> one being examined) should be<br />
adequately “fogged” with a positive lens<br />
(resulting in an “against” movement seen<br />
on <strong>the</strong> retinoscopy swipe). 1 For children,<br />
maintaining fixation at this distance<br />
can be difficult and new computerised<br />
test charts generally provide dynamic<br />
and more interesting targets to view<br />
than a standard spotlight (Figure 1)<br />
to help with this. It is also possible<br />
to download a number of videoclips,<br />
especially cartoons, with different<br />
animations. Practitioners should also<br />
consider not using a phoropter or trial<br />
frame when conducting retinoscopy<br />
on a very young child, as this can be<br />
intimidating for <strong>the</strong> child. It is preferable<br />
to use single trial lenses or a lens rack.<br />
Speed during retinoscopy is essential<br />
when performing this technique in<br />
young children, especially as <strong>the</strong>y<br />
maintain fixation only for very short<br />
periods of time. In cases of fluctuation of<br />
accommodation, <strong>the</strong> practitioner should<br />
follow <strong>the</strong> “with” movement, ignoring <strong>the</strong><br />
occasional “against” movements seen.<br />
Figure 1<br />
Examples of exciting targets presented by computerized test charts during retinoscopy. Different face<br />
expressions allow to <strong>the</strong> practitioner to talk to <strong>the</strong> child to maintain attention on <strong>the</strong> target (Courtesy of<br />
Thomson Software Solutions, UK).<br />
For <strong>the</strong> latest CET visit www.optometry.co.uk/cet<br />
Having trouble signing in to take an exam?<br />
View CET FAQ Go to www.optometry.co.uk<br />
Yeotikar et al. 2 evaluated <strong>the</strong> difference<br />
in refractive error in non-strabismic<br />
children between <strong>the</strong> ages of seven years<br />
and 16 years, using static retinoscopy<br />
under two conditions – first by fogging<br />
<strong>the</strong> contralateral eye with a positive<br />
lens and second with cycloplegia using<br />
cyclopentolate 1%. The study found<br />
that <strong>the</strong> average difference in refractive<br />
error between <strong>the</strong>se two conditions<br />
was only 0.29DS more hypermetropic<br />
with cyclopentolate, highlighting <strong>the</strong><br />
accurate results that can be obtained<br />
when <strong>the</strong>re is adequate accommodative<br />
control during static retinoscopy.<br />
Fur<strong>the</strong>rmore, Chan and Edward3 suggested a calculation which can be<br />
used to match <strong>the</strong> dry retinoscopy<br />
result to that which would be obtained<br />
using cyclopentolate 1%, in children<br />
between 3.5 to five years of age. The<br />
astigmatic component is kept <strong>the</strong> same<br />
whilst <strong>the</strong> spherical component found<br />
in both meridians is multiplied by 1.45<br />
and a value of 0.39D is added. However,<br />
this depends on an accurate static<br />
retinoscopy result having been obtained.<br />
Mohindra retinoscopy<br />
The Mohindra technique, also known<br />
as near retinoscopy or near monocular<br />
retinoscopy, carries <strong>the</strong> main advantage<br />
of being child-friendly and requiring less<br />
co-operation from <strong>the</strong> child. 4 In this case,<br />
<strong>the</strong> stimulus is <strong>the</strong> dimmed light source<br />
of <strong>the</strong> retinoscope in a darkened room.<br />
The darkness of <strong>the</strong> room will facilitate<br />
<strong>the</strong> child to keep <strong>the</strong>ir attention on <strong>the</strong><br />
retinoscope’s light. The retinoscope<br />
is held at a distance of 50cm (errors in<br />
distance are not clinically relevant),<br />
with hand-held trial lenses used to find<br />
<strong>the</strong> neutral point. The accommodation<br />
activity during <strong>the</strong> examination is small<br />
and <strong>the</strong> same in both eyes. It is important<br />
during <strong>the</strong> examination to keep <strong>the</strong> light<br />
of <strong>the</strong> retinoscope on <strong>the</strong> child’s pupil<br />
49<br />
06/04/12 CET
50<br />
06/04/12 CET<br />
CET CONTINUING<br />
EDUCATION<br />
& TRAINING<br />
1 FREE CET POINT<br />
Approved for: Optometrists 4 Dispensing Opticians 4<br />
(to see <strong>the</strong> retinal reflex) for only a short<br />
period of time so as not to stimulate<br />
accommodation; subsequently <strong>the</strong><br />
optometrist’s attention should be focused<br />
on <strong>the</strong> pupil, watching for maximum<br />
dilation (indicating no accommodation). 5<br />
The procedure should be carried out<br />
with one eye occluded, preferably by <strong>the</strong><br />
parent, while <strong>the</strong> o<strong>the</strong>r eye is evaluated.<br />
However, Wesson et al. 6 confirmed that<br />
<strong>the</strong>re is no substantial difference in <strong>the</strong><br />
result if binocular fixation is allowed<br />
(Figure 2); indeed this can be useful if <strong>the</strong><br />
infant is resistant and becomes agitated<br />
with occlusion. Several people advocate<br />
neutralisation of <strong>the</strong> two principal<br />
meridians of <strong>the</strong> eye separately, using<br />
loose spherical trial lenses. However,<br />
Saunders and Westall7 confirmed that<br />
<strong>the</strong> accuracy of <strong>the</strong> technique can<br />
be improved using a combination of<br />
spherical and cylindrical lenses instead.<br />
Once <strong>the</strong> retinoscopy result is obtained, <strong>the</strong><br />
refractive error was originally calculated<br />
by adding -1.25DS to <strong>the</strong> gross finding. 8,9<br />
Saunders and Westall7 have reported<br />
that <strong>the</strong> accuracy can be improved if<br />
-0.75DS is added instead, for children<br />
aged between 0-2 years, and -1.00DS<br />
added for those children over two years<br />
of age. They also affirmed that <strong>the</strong> result<br />
achieved by <strong>the</strong> Mohindra procedure in<br />
children between six months and four<br />
years of age is similar to wet retinoscopy<br />
(using cyclopentolate 1% – see later),<br />
with a difference of only 0.50DS. O<strong>the</strong>rs<br />
have reported similar results, 10 and<br />
certainly no differences greater than<br />
1.00DS, 11 whilst similar results were<br />
also obtained for children with Down’s<br />
syndrome12 and even in adults. 13<br />
The Mohindra technique is useful for<br />
practitioners in Europe who are not<br />
permitted to used cycloplegic agents, 14<br />
whilst <strong>the</strong>re are benefits for conducting<br />
frequent follow-up assessments without<br />
repeated use of cycloplegic agents. 15<br />
One must remember, however, that <strong>the</strong><br />
OT CET content supports Optometry Giving Sight<br />
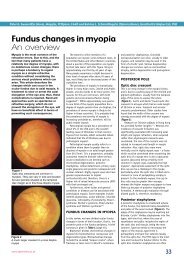
Figure 2<br />
Mohindra retinoscopy. Hand-held trial lenses are<br />
placed in front of both eyes whilst <strong>the</strong> child fixates<br />
<strong>the</strong> retinoscope light. The procedure should be run<br />
in darkened room (<strong>the</strong> high level of room light in<br />
this image was for photographic purposes only).<br />
accuracy of results will naturally depend<br />
on <strong>the</strong> practitioner’s experience. 16<br />
Cycloplegic agents<br />
Control of accommodation in children<br />
of pre-school age is more commonly<br />
achieved by pharmacological means,<br />
using cycloplegic agents such as<br />
cyclopentolate and tropicamide; atropine<br />
can only be used by <strong>the</strong>rapeutically<br />
qualified practitioners. All of <strong>the</strong>se drugs<br />
are muscarinic receptor blockers, thus<br />
<strong>the</strong>y work by blocking <strong>the</strong> muscarinic<br />
receptors in <strong>the</strong> ciliary body, which<br />
in turn prevents accommodation.<br />
A mydriatic effect is concurrently<br />
achieved by inhibiting muscarinic<br />
stimulation of <strong>the</strong> iris sphincter muscle.<br />
An ideal cycloplegic would have no<br />
ocular and systemic adverse effects.<br />
Also, it should produce a rapid onset of<br />
cycloplegia, blocking accommodation<br />
completely for an adequate period<br />
of time, before swiftly restoring<br />
accommodative ability. 17 Several<br />
studies have reported both ocular<br />
and systemic side effects (especially<br />
using atropine) in those children who<br />
have had a cycloplegic refraction,<br />
in addition to expected mydriasis<br />
and cycloplegia, as detailed later. 18<br />
Drug selection and instillation<br />
Cycloplegia is an invasive technique<br />
Having trouble signing in to take an exam?<br />
View CET FAQ Go to www.optometry.co.uk<br />
which can be uncomfortable, or even<br />
distressing, for <strong>the</strong> child. This is notably<br />
so because <strong>the</strong> acidic pH of <strong>the</strong> cycloplegic<br />
agent leads to stinging on instillation.<br />
Some practitioners advocate <strong>the</strong> use of a<br />
local anaes<strong>the</strong>tic prior to instillation of<br />
<strong>the</strong> cycloplegic agent; proxymetacaine<br />
0.5% is <strong>the</strong> drug of choice as it stings less<br />
than o<strong>the</strong>r topical anaes<strong>the</strong>tics. However,<br />
this is not always recommended due to<br />
<strong>the</strong> risks associated with an anaes<strong>the</strong>tised<br />
cornea. To facilitate <strong>the</strong> application<br />
of cycloplegics, cyclopentolate has<br />
been instilled in spray form onto <strong>the</strong><br />
eyelashes and <strong>the</strong> closed upper lid. 19<br />
Practitioners should also be conscious<br />
of <strong>the</strong>ir instillation technique, since<br />
different degrees of cycloplegia between<br />
<strong>the</strong> eyes can occur, especially if <strong>the</strong><br />
child does not keep <strong>the</strong>ir eyes open wide<br />
enough and/or if <strong>the</strong>re is significant postinstillation<br />
tearing (which is very likely).<br />
As such, practitioners can opt to instil<br />
<strong>the</strong> higher concentration of cycloplegic<br />
agent and/or instil fur<strong>the</strong>r drops if<br />
regular review (eg, periodic measurement<br />
of <strong>the</strong> amplitude of accommodation)<br />
reveals differing levels of cycloplegia.<br />
Differences in <strong>the</strong> main cycloplegic<br />
agents are summarised in Table 1. The<br />
optometrist should select an appropriate<br />
agent considering factors such as <strong>the</strong><br />
patient’s age and whe<strong>the</strong>r <strong>the</strong>y have<br />
dark, or light coloured, irides. Adequate<br />
cycloplegic effect could be achieved<br />
with tropicamide in a teenage patient<br />
suspected of having latent hypermetropia,<br />
for example, whereas cyclopentolate<br />
is likely to be required for an infant<br />
suspected of having an accommodative<br />
esotropia. Those with light coloured<br />
irides may exhibit an increased response<br />
to drugs as compared with darkly<br />
pigmented irides, and <strong>the</strong>refore a lower<br />
concentration/dose ought to be selected.<br />
Overdose of cycloplegic agent has to<br />
be avoided in children with Down’s<br />
syndrome or those affected by cerebral<br />
Find out when CET points will be uploaded to Vantage at www.optometry.co.uk/cet/vantage-dates
palsy, trisomy 13 and 18, and o<strong>the</strong>r<br />
central nervous system (CNS) disorders.<br />
This is because toxicity increases in<br />
<strong>the</strong>se people, especially children, which<br />
causes stimulation of <strong>the</strong> medulla<br />
and <strong>the</strong> cerebral centres, leading to<br />
hallucinogenic effects similar to those<br />
caused by LSD drugs. 20,21 These reactions<br />
generally occur within 20-30 minutes<br />
after administration. 22 Tropicamide<br />
1% should be considered in <strong>the</strong>se<br />
children as opposed to cyclopentolate.<br />
Cyclopentolate<br />
Cyclopentolate 0.5% or 1.0% is<br />
commonly used by practitioners as<br />
<strong>the</strong> cycloplegic agent of choice for<br />
paediatric examinations. The cycloplegia<br />
achieved is not too deep, as compared<br />
with atropine, but it is quicker in<br />
onset, often achieved after 30 minutes<br />
from its administration. Recovery of<br />
accommodation is typically between six-<br />
12 hours after instillation whilst mydriasis<br />
resolves by 24 hours after instillation.<br />
Although full cycloplegia is achieved<br />
with atropine, <strong>the</strong> cycloplegic refractive<br />
results obtained with cyclopentolate<br />
are comparable in “normals”, 23 high<br />
hypermetropic children24,25 and also<br />
those children with strabismus. 26,27<br />
For children under <strong>the</strong> age of three<br />
months, it is advised that two drops of<br />
cyclopentolate 0.5% are used as opposed<br />
to 1%. 28 This is becasue drug absorption<br />
through <strong>the</strong> conjunctival epi<strong>the</strong>lium and<br />
skin is more rapid in infants compared<br />
to adults, 29,30 due to immature metabolic<br />
enzyme systems in neonates and young<br />
children, which may prolong <strong>the</strong> effects<br />
of <strong>the</strong> drug. 31,32 The main side effects<br />
of cyclopentolate include incoherent<br />
speech, hallucinations and disorientation,<br />
psychosis and visual disturbances. 33,34<br />
Tropicamide<br />
This is an anti-muscarinic drug with<br />
short-lasting effect on <strong>the</strong> pupil<br />
(mydriasis) and on accommodation<br />
(cycloplegia) at <strong>the</strong> 1% concentration.<br />
Although tropicamide is mostly used for<br />
mydriasis, to examine <strong>the</strong> optical media<br />
and <strong>the</strong> ocular fundus, several studies<br />
have suggested that this drug can be used<br />
for a cycloplegic effect. 35 In particular,<br />
it is a cycloplegic agent that can at least<br />
detect latent hypermetropia, for example<br />
in school children, teenagers and those<br />
in <strong>the</strong>ir early 20s, with o<strong>the</strong>rwise normal<br />
refractive status and/or with moderate<br />
hypermetropia, 36 as well as for children<br />
during <strong>the</strong> post-natal period. 37 In adult<br />
patients undergoing refractive surgery, a<br />
study showed no significant difference<br />
in cycloplegic refraction between<br />
tropicamide 1% and cyclopentolate<br />
1%. 38 In <strong>the</strong> same patients, however,<br />
<strong>the</strong> study showed that cyclopentolate<br />
was more effective than tropicamide<br />
in reducing accommodative amplitude<br />
in adult myopes (near-point testing).<br />
Atropine sulphate<br />
This is a natural alkaloid extracted<br />
from <strong>the</strong> deadly nightshade (Atropa<br />
belladonna) plant. Its administration<br />
is justified in children of pre-verbal<br />
age or when o<strong>the</strong>r cycloplegic agents<br />
fail to produce a satisfactory level of<br />
cycloplegia. Atropine is administrated<br />
three times a day during <strong>the</strong> three days<br />
before <strong>the</strong> eye examination. Associated<br />
mydriasis decreases in two weeks after<br />
For <strong>the</strong> latest CET visit www.optometry.co.uk/cet<br />
Mydriasis Cycloplegia<br />
Agent Concentration Max effect Recovery<br />
time<br />
Max<br />
effect<br />
Recovery<br />
time<br />
Atropine 0.5-3.0% 1-2 hours 7-12 days 60-180 min 6-12 days<br />
Cyclopentolate 0.5-2.0% 30-60 min. 1 days 25-75 min 6-12 hours<br />
Tropicamide 0.5-1.0% 20-40 min 6 hours 20-35 min 4-6 hours<br />
Homatropine 2.0-5.0% 40-60 min. 1-3 days 30-60 min 1-3 days<br />
Scopolamine 0.25% 20-30 min 3-7 days 30-60 min 3-7 days<br />
Table 1<br />
Cycloplegic and mydriatic effects amongst <strong>the</strong> main cycloplegic drugs used in optometric practice<br />
<strong>the</strong> refractive examination. This drug is an<br />
antagonist of <strong>the</strong> muscarinic acetylcholine<br />
receptors, thus it dampens mediation of<br />
<strong>the</strong> parasympa<strong>the</strong>tic nervous system. As<br />
a result, systemic absorption of atropine<br />
can lead to difficulties with swallowing<br />
food (opposed effects of <strong>the</strong> vagus nerve),<br />
inhibition of <strong>the</strong> salivary glands leading<br />
to a dry mouth, and reduction of sweating.<br />
Atropine can also increase firing of <strong>the</strong><br />
sino-atrial node (SA) and conduction<br />
through <strong>the</strong> atrio-ventricular node (AV)<br />
of <strong>the</strong> heart, leading to tachycardia. It<br />
also decreases bronchial secretions,<br />
which can make breathing difficult.<br />
O<strong>the</strong>r side effects that have been reported<br />
include dizziness, nausea and sensation<br />
of being unbalanced and allergic<br />
reactions of <strong>the</strong> eyelids and conjunctiva.<br />
Atropine is able to pass through <strong>the</strong><br />
blood-cerebral-barrier and alter <strong>the</strong> state<br />
of consciousness of <strong>the</strong> child. Therefore,<br />
in order to minimise <strong>the</strong> systemic<br />
absorption of atropine, <strong>the</strong> practitioner<br />
can gently press <strong>the</strong> punctum of both eyes<br />
and keep <strong>the</strong> patient’s head tilted back.<br />
A recent study39 compared <strong>the</strong><br />
cycloplegic efficacy of homatropine<br />
2% and atropine 1% in children<br />
between <strong>the</strong> ages of four and 10 years by<br />
retinoscopy and automated refraction.<br />
As expected, <strong>the</strong> study reported that<br />
homatropine produced a significantly<br />
lesser cycloplegic effect than atropine,<br />
51<br />
06/04/12 CET
52<br />
06/04/12 CET<br />
CET CONTINUING<br />
EDUCATION<br />
& TRAINING<br />
1 FREE CET POINT<br />
Approved for: Optometrists 4 Dispensing Opticians 4<br />
with residual accommodation being<br />
greater (1.80±0.40D with atropine<br />
vs. 3.10±0.50D with homatropine;<br />
p
those with risk factors for binocular<br />
vision anomalies <strong>the</strong> refraction should<br />
be performed under cycloplegia.<br />
Tropicamide seems to be as effective<br />
as cyclopentolate for measurement of<br />
refractive error in most non-strabismic<br />
infants, particularly at <strong>the</strong> 1%<br />
concentration, so it should be considered<br />
more often in paediatric eye care in<br />
order to reduce <strong>the</strong> possibility of adverse<br />
Module questions Course code: C-18551 O/D<br />
PLEASE NOTE There is only one correct answer. All CET is now FREE. Enter online. Please complete online by midnight on May 4, 2012 – You will be unable to submit<br />
exams after this date. Answers to <strong>the</strong> module will be published on www.optometry.co.uk/cet/exam-archive. CET points for <strong>the</strong>se exams will be uploaded to Vantage<br />
on May 14, 2012. Find out when CET points will be uploaded to Vantage at www.optometry.co.uk/cet/vantage-dates<br />
1. Which of <strong>the</strong> following statements is TRUE?<br />
a) Atropine produces cycloplegia within 2-3 hours and recovery of<br />
accommodation in 2 days<br />
b) Cyclopentolate produces cycloplegia within 30 minutes and<br />
recovery of accommodation in 12 hours<br />
c) Homatropine produces cycloplegia in 20-30 minutes and recovery of<br />
accommodation in 24 hours<br />
d) All of <strong>the</strong> above<br />
2. Which pharmacological agent should be considered in a child<br />
with Down’s Syndrome?<br />
a) Atropine<br />
b) Homatropine<br />
c) Cyclpentolate<br />
d) Tropicamide<br />
3. When should Mohindra’s retinoscopy technique be<br />
performed?<br />
a) In all children<br />
b) Only in children aged 7-10 years<br />
c) Only in young children with moderate astigmatism<br />
d) In pre-verbal children<br />
reactions. Where <strong>the</strong>re is suspicion of a<br />
binocular vision anomaly, cyclopentolate<br />
should be <strong>the</strong> agent of choice.<br />
About <strong>the</strong> authors<br />
Fabrizio Bonci is an optometrist and<br />
clinical research fellow at <strong>the</strong> division<br />
of clinical neuroscience and mental<br />
health, Imperial College, London, and<br />
<strong>the</strong> Faculty of Medicine, Charing Cross<br />
4. How should Mohindra’s retinoscopy technique be performed?<br />
a) In darkness, fixation being on <strong>the</strong> retinoscope light, using hand held lenses<br />
b) In room lighting, fixation being on a high contrast target at <strong>the</strong> retinoscope mirror<br />
c) In darkness, fixation being on a spotlight at 6 metres, using hand held lenses<br />
d) In room light, fixation being on a high contrast target at 6 metres, under<br />
cycloplegia<br />
5. Which of <strong>the</strong> following statements regarding cycloplegic refraction is<br />
TRUE?<br />
a) It should be considered in children with high hypermetropia or strabismus<br />
b) It should be considered in every child at every sight test<br />
c) Atropine is <strong>the</strong> cycloplegic of choice for a 5-year-old child<br />
d) Objective automated refraction should be used for prescribing decisions<br />
6. Which of <strong>the</strong> following is NOT a side effect of cyclopentolate?<br />
a) Incoherent speech<br />
b) Hallucinations<br />
c) Mydriasis<br />
d) Conjunctival hyperaemia<br />
For <strong>the</strong> latest CET visit www.optometry.co.uk/cet<br />
Hospital, London. Luigi Lupelli is an<br />
optometrist, professor in contact lenses<br />
at <strong>the</strong> Faculty of Science, Department<br />
of Physics, (Optics and Optometry)<br />
at <strong>the</strong> University of Roma Tre, Italy.<br />
References<br />
See www.optometry.co.uk/<br />
clinical. Click on <strong>the</strong> article title and<br />
<strong>the</strong>n on ‘references’ to download.<br />
53<br />
06/04/12 CET