here - Australian College of Veterinary Scientists
here - Australian College of Veterinary Scientists
here - Australian College of Veterinary Scientists
You also want an ePaper? Increase the reach of your titles
YUMPU automatically turns print PDFs into web optimized ePapers that Google loves.
<strong>Australian</strong> <strong>College</strong> <strong>of</strong> <strong>Veterinary</strong><br />
<strong>Scientists</strong> Dermatology Chapter<br />
Science Week Proceedings 2005<br />
Equine Dermatology<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 1
2<br />
ACVSc Dermatology Chapter<br />
This is the third Science Week meeting <strong>of</strong> our Dermatology Chapter and<br />
we are looking forward to an exciting two days <strong>of</strong> equine dermatology.<br />
We are very pleased to welcome our key-note speakers Dr Janet<br />
Littlewood and Dr Reg Pascoe as well as <strong>Australian</strong> and European<br />
dermatologists, dermatology residents and pathologists who have all<br />
combined to create a fabulous program for dermatologists as well as<br />
equine clinicians for Science Week 2005.<br />
This continues to be an important time for veterinary dermatology in<br />
Australia. The Dermatology Chapter aims promote excellence in<br />
dermatology <strong>of</strong> all animal species. The objectives <strong>of</strong> the Chapter include<br />
advancing the science and art <strong>of</strong> veterinary science as it relates to<br />
dermatology and in particular to further the pr<strong>of</strong>essional education and<br />
training <strong>of</strong> veterinarians with a special interest in dermatology.<br />
For further information on joining the Dermatology Chapter, please<br />
contact Mandy Burrows on a.burrows@murdoch.edu.au.<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005
<strong>Australian</strong> <strong>College</strong> <strong>of</strong> <strong>Veterinary</strong> <strong>Scientists</strong> Dermatology Chapter<br />
Science Week Proceedings 2005<br />
Friday 1st July 2005 : Equine dermatology: Program<br />
8.20 Introduction: Equine allergic skin disease<br />
Mandy Burrows<br />
8.30 Equine atopic skin disease<br />
Janet Littlewood<br />
9.10 Intradermal testing in horses: the <strong>Australian</strong> perspective<br />
Tina Baxter<br />
10.00 Morning tea<br />
10.30 Intradermal testing in horses: the UK perspective<br />
Janet Littlewood<br />
11.10 Equine Rhodes grass contact allergy<br />
Ken Mason<br />
11.30 Immunotherapy for equine atopy<br />
Janet Littlewood<br />
12.30 Lunch<br />
1.30 Diagnostic approach to the horse with urticaria<br />
Reg Pascoe<br />
2.30 Urticaria case studies<br />
Greg Burton<br />
3.00 Afternoon tea<br />
3.30 Management <strong>of</strong> the atopic horse<br />
Janet Littlewood<br />
4.30 Dermatology AGM<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 3
4<br />
<strong>Australian</strong> <strong>College</strong> <strong>of</strong> <strong>Veterinary</strong> <strong>Scientists</strong> Dermatology Chapter<br />
Science Week Proceedings 2005<br />
Saturday 2nd July 2005 : Equine Dermatology (cont)<br />
8.20 Introduction: Equine dermatology<br />
Mandy Burrows<br />
8.30 The approach to the horse with pastern dermatoses<br />
Janet Littlewood<br />
9.20 A review <strong>of</strong> equine sarcoidosis<br />
Sonya Bettenay<br />
10.00 Morning tea<br />
10.30 The equine sarcoid: a review<br />
Reg Pascoe<br />
11.50 Histopathologic features <strong>of</strong> equine sarcoid<br />
Jenny Charles<br />
12.30 Lunch<br />
1.30 How I treat: equine bacterial folliculitis<br />
Sonya Bettenay<br />
1.50 How I treat: equine insect hypersensitivity<br />
Mandy Burrows<br />
2.10 How I treat: equine pemphigus foliaceus<br />
Ralf Mueller<br />
2.30 How I treat: equine phycomycoses<br />
Reg Pascoe<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005
3.00 Afternoon tea<br />
3.30 How I treat: equine dermatophytosis<br />
Greg Burton<br />
3.50 How I treat: equine chorioptes<br />
Janet Littlewood<br />
4.10 How I treat: equine vasculitis<br />
Linda Vogelnest<br />
4.30 CLOSE<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 5
Dr Tina Baxter<br />
6<br />
About the speakers:<br />
Graduated from University <strong>of</strong> Sydney in 1999<br />
- Worked in busy small animal practice after graduating<br />
- Did distance education course in Derm with Ralf and Sonya in 2003<br />
- Virbac created position for Resident in Derm at Sydney Uni through<br />
generous grant<br />
- Started this residency in 2004<br />
- Passed membership exams in Small Animal Med in 2004<br />
- Derm interests - any equine dermatology - research project into allergen<br />
concentration determination in horses.<br />
Dr Sonya Bettenay BVSc (Hons) MACVSc (Feline Medicine) FACVSc<br />
(Dermatology)<br />
Graduated from Melbourne University, worked in private small animal practice,<br />
industry and teaching Vet Nurses and Equine courses during the first 8 years <strong>of</strong><br />
graduation and then began a residency with Dr Ken Mason. Coinciding with this,<br />
founded the Animal Skin & Allergy Clinic in Melbourne, with satellite clinics in 4<br />
States until we obtained enough dermatologists to cover Adelaide, Canberra and<br />
Sydney. With her husband, Ralf Mueller, built the first purpose built private<br />
dermatology clinic in Australia. She is currently employed at Colorado State<br />
University and runs the dermatopathology service <strong>of</strong> the CSU Diagnostic Lab.<br />
Dr Mandy Burrows BVMS MACVSc (Canine Medicine) FACVSc<br />
(Dermatology)<br />
Graduated from Murdoch University in 1985. Completed a pathology and small<br />
animal residency at Murdoch University and Membership in Canine Medicine in<br />
1991. Commenced a dermatology residency in 1992 with Ken Mason and gained her<br />
Fellowship in <strong>Veterinary</strong> Dermatology in 1998. Mandy currently runs a dermatology<br />
referral practice at Murdoch University <strong>Veterinary</strong> Hospital and teaches dermatology<br />
and immunology to undergraduate and postgraduate veterinary students and has a<br />
strong interest in continuing veterinary education for veterinary practitioners and<br />
nurses.<br />
Dr Greg Burton<br />
Graduated University <strong>of</strong> Queensland (Hons 1st) 1983<br />
Small animal general practice 1983-1993<br />
Member ACVSc (small animal surgery) 1993<br />
Fellow ACVSc (dermatology) 1997<br />
Currently in referral dermatology practice Melbourne <strong>Veterinary</strong> Referral Centre and<br />
University <strong>of</strong> Melbourne <strong>Veterinary</strong> Teaching Hospital, Melbourne<br />
Principal Fellow (Associate Pr<strong>of</strong>essor), Dept <strong>of</strong> <strong>Veterinary</strong> Science, University <strong>of</strong><br />
Melbourne 3010<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005
Dr Jennifer A. Charles BVSc MVS Dip ACVP<br />
Jenny Charles graduated from The University <strong>of</strong> Sydney in 1985. She completed an<br />
internship, residency and Master <strong>of</strong> <strong>Veterinary</strong> Studies in anatomic pathology at The<br />
University <strong>of</strong> Melbourne and then pursued advanced studies in anatomic pathology<br />
at the Ontario <strong>Veterinary</strong> <strong>College</strong>, Guelph, Canada. In 1993, she became a<br />
Diplomate <strong>of</strong> the American <strong>College</strong> <strong>of</strong> <strong>Veterinary</strong> Pathologists. From 1993 to 1999,<br />
she was employed as a specialist veterinary pathologist at the Sydney Laboratory <strong>of</strong><br />
<strong>Veterinary</strong> Pathology Services Pty Ltd (now IDEXX Pty Ltd). In 1999, she was<br />
appointed Senior Lecturer in <strong>Veterinary</strong> Pathology at The University <strong>of</strong> Melbourne.<br />
Jenny’s particular interests lie in haematology, endocrinology, hepatobiliary and<br />
pancreatic pathology and dermatopathology.<br />
Dr Janet Littlewood MA PhD BVSc (Hons) DVR DVD MRCVS RCVS<br />
Recognised Specialist in <strong>Veterinary</strong> Dermatology<br />
Janet graduated with Honours from the University <strong>of</strong> Bristol, longer ago than she<br />
cares to remember! As a new graduate she spent a year as Intern at the University <strong>of</strong><br />
Pennsylvania, she spent some time in general practice before being appointed<br />
Assistant Physician at the University <strong>of</strong> Cambridge. After this training in small<br />
animal medicine, she studied for her PhD in aspects <strong>of</strong> comparative haemostasis, but<br />
then returned to clinical medicine and to focus on dermatology. She established the<br />
Dermatology Unit at the Animal Health Trust, Newmarket, w<strong>here</strong> she developed her<br />
interest in equine dermatology, in addition to the small animal clinical work, training<br />
residents and supervising a research student working on canine atopy. She holds the<br />
RCVS Diploma and has Recognised Specialist status in <strong>Veterinary</strong> Dermatology and<br />
has been examiner for both Certificate and Diploma examinations. She has written<br />
chapters for and edited a number <strong>of</strong> textbooks as well as contributing to peer<br />
reviewed journals. She is involved in postgraduate continuing education and has<br />
spoken at many national and international conferences and is renowned for her<br />
enthusiasm for her subject. Since 2001 Janet has been working in private referral<br />
practice in East Anglia, <strong>of</strong>fering a service for companion animals, including horses.<br />
As well as running her business, Janet is mum to two sons, is overseeing major house<br />
renovations, and still tries to find time to sing with the Cambridge Philharmonic<br />
Society and is learning to play the viola.<br />
Dr Ken Mason BSc BVSc MVSc MACVSc (Feline Medicine) FACVSc<br />
(<strong>Veterinary</strong> Dermatology)<br />
Clinical veterinarian, animal dermatologist and by marriage a cat person.<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 7
Dr. med. vet. Ralf S Mueller<br />
Graduated in Munich/Germany in 1985, completed his thesis in 1987, and worked in<br />
several large and small animal practices before completing a residency in veterinary<br />
dermatology at the University <strong>of</strong> California/Davis in 1992. He is a Diplomate <strong>of</strong> the<br />
American <strong>College</strong> <strong>of</strong> <strong>Veterinary</strong> Dermatology and a Fellow <strong>of</strong> the <strong>Australian</strong> <strong>College</strong><br />
<strong>of</strong> <strong>Veterinary</strong> Science. In 1992 he moved to Melbourne/Australia to work with his<br />
partner and wife Dr. Sonya Bettenay. Together, they created the first, purpose-built<br />
specialist practice not linked to a general practice in Australia. They established the<br />
Distance Education Program in <strong>Veterinary</strong> Dermatology <strong>of</strong> the Postgraduate<br />
Foundation in <strong>Veterinary</strong> Science <strong>of</strong> the University <strong>of</strong> Sydney. During that time, Dr.<br />
Mueller was concurrently consulting and teaching at the <strong>Veterinary</strong> Teaching<br />
Hospital/University <strong>of</strong> Sydney. In 1999, he became Assistant Pr<strong>of</strong>essor in <strong>Veterinary</strong><br />
Dermatology at the <strong>College</strong> <strong>of</strong> <strong>Veterinary</strong> Medicine and Biomedical<br />
Sciences/Colorado State University, w<strong>here</strong> he is involved in teaching, consulting and<br />
veterinary dermatology research. He has published over 100 studies, articles, book<br />
chapters and books in the German, English, Spanish and French literature in<br />
Australia, Europe and America and given over 200 seminars, lectures and talks in<br />
Australia, Europe, United States, New Zealand and Canada. Dr. Mueller has two<br />
children, Anya and Florian and when he is not working, he takes his family skiing,<br />
rock-climbing or hiking.<br />
Dr Reg Pascoe AM, BVSc. DVSc. FRCVS. FACVSc.<br />
Graduated from the University <strong>of</strong> Queensland in 1951. Commenced general large<br />
animal practice in Oakey and in 1969 established a large animal hospital,<br />
predominantly for horses. Is a registered specialist in Equine Surgery and has a<br />
special interest in Dermatology, presenting his first paper on skin diseases in<br />
1971.Author and co author on four equine Dermatology books and over 60<br />
refereed scientific published articles<br />
Biography: University <strong>of</strong> Queensland BVSc 1951, MVSc. 1967 , DVSc. 1984;<br />
Adjunct Pr<strong>of</strong>essor <strong>Veterinary</strong> Science 1998; FRCVS 1973, FACVSc 1975. Began<br />
private general rural practice in Oakey 1952; equine practice covering reproduction,<br />
surgery and dermatology from 1966; Specialist in Equine Surgery since 1988.<br />
Published over 60 referred articles, author <strong>of</strong> Equine Dermatoses (3 editions),<br />
Colour Atlas <strong>of</strong> Skin Diseases <strong>of</strong> Horses, and Vade Mecum II - Diseases <strong>of</strong><br />
Horses.Co-author Colour Atlas <strong>of</strong> Equine Diseases and Handbook <strong>of</strong> Equine<br />
Dermatology.<br />
Dr Linda Vogelnest<br />
Graduated from Sydney University 1984. Worked in small animal practice in<br />
Australia and locuming in UK for 4 years. Full-time head <strong>of</strong> small animal unit at<br />
Sydney University <strong>Veterinary</strong> Centre Camden for 2 years, then part-time registrar in<br />
small animals for 8 years. Achieved Membership <strong>of</strong> <strong>Australian</strong> <strong>College</strong> <strong>of</strong> <strong>Veterinary</strong><br />
8<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005
<strong>Scientists</strong> in Feline Medicine in 1997. Completed Dermatology Alternative Residency<br />
Program, supervised by Ralf Mueller, Ken Mason, Sonya Bettenay, Greg Burton,<br />
from 1997-2001; 3 years based in Sydney, one year in Melbourne. Achieved<br />
Fellowship <strong>of</strong> <strong>Australian</strong> <strong>College</strong> <strong>of</strong> <strong>Veterinary</strong> <strong>Scientists</strong> in <strong>Veterinary</strong> Dermatology<br />
in 2003. Currently employed as Specialist <strong>Veterinary</strong> Dermatology at University <strong>of</strong><br />
Sydney (Camden campus 3 days, Sydney campus 1 day per week) seeing small, large<br />
and exotic animal referrals.<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 9
Introduction:<br />
10<br />
Equine Atopic Dermatitis<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005<br />
Janet Littlewood<br />
Atopic dermatitis is defined as a genetically programmed disease mediated by<br />
reaginic-antibodies (type I hypersensitivity) in which the patient becomes sensitised<br />
to environmental allergens that are innocuous for non-atopic animals. Classically the<br />
diseases is associated with IgE allergen-specific antibodies, but in some species<br />
evidence supports a role for allergen-specific IgG. The importance <strong>of</strong> other<br />
components <strong>of</strong> the immune system are now known to be important in the aetiology<br />
<strong>of</strong> the disease process.<br />
In humans and dogs t<strong>here</strong> is good evidence that the disease is genetically<br />
programmed and t<strong>here</strong> are reports <strong>of</strong> familial incidence and breed predispositions in<br />
the horse that suggest genetic involvement. It is well recognised that insect bite<br />
hypersensitivity (IBH, Culicoides hypersensitivity) has a strong familial tendency, and<br />
t<strong>here</strong> are reports <strong>of</strong> familial occurrence <strong>of</strong> equine atopy suggesting a genetic<br />
predisposition (Rees 2001). Factors such as susceptibility to sensitisation during early<br />
life and the influence <strong>of</strong> the presence <strong>of</strong> parasitic infestation, viral infections,<br />
vaccination and environmental pollutants are <strong>of</strong> unknown significance in the horse.<br />
Genetically-predisposed individuals mount allergen-specific IgE (and possibly IgG)<br />
antibody responses to environmental (and possibly ingested) antigens. Equine IgE<br />
was isolated and characterised by Suter and colleagues in the early 1980's, with even<br />
earlier documentation <strong>of</strong> skin-sensitising antibodies. IgE binds to mast cells in the<br />
skin (and elsew<strong>here</strong>) via the high-affinity IgE receptor. Cross-linking <strong>of</strong> mast cellbound<br />
IgE by specific allergens, causes degranulation and release <strong>of</strong> preformed<br />
mediators, giving rise to the classical erythematous wheal reaction, and synthesis <strong>of</strong><br />
new mediators resulting in the recruitment <strong>of</strong> inflammatory cells to the area.<br />
However, the lesions that develop in atopic humans and dogs at the site <strong>of</strong> patch<br />
tests more closely mimic those found in the naturally occurring clinical disease.<br />
Atopic individuals show increased numbers <strong>of</strong> both dermal and epidermal<br />
Langerhans cells, as well as increased numbers <strong>of</strong> other inflammatory cells.<br />
Epidermal Langerhans cells have been shown to bear allergen-specific IgE molecules<br />
in atopic humans and dogs, further supporting that percutaneous absorption <strong>of</strong><br />
allergens is important in the aetiology <strong>of</strong> the natural disease, probably aided by<br />
epidermal barrier function defects.
IgE-bearing cells have been demonstrated in the epidermis and dermis <strong>of</strong> lesional<br />
skin from horses with IBH, together with increased numbers <strong>of</strong> mast cells, the<br />
majority <strong>of</strong> which were tryptase-positive (van der Haegen et al 2001) and also<br />
bearing IgE protein. No chymase-positive cells were found, similar to bovine skin,<br />
but in contrast to human and canine skin w<strong>here</strong> mast cells are both chymase and<br />
tryptase-positive. IgE-mRNA and IgE-protein positive cells were found in the<br />
dermis – likely B-lymphocytes and plasma cells – but also IgE-protein positive,<br />
mRNA negative cells in both the dermis and the epidermis, which are likely to be<br />
dendritic cells, including Langerhans cells. By comparison with samples from healthy<br />
horses and horses with an infectious skin disease, this study was the first to provide<br />
evidence demonstrating the role <strong>of</strong> IgE in the skin <strong>of</strong> allergic horses.<br />
Epidermal Langerhans cells bearing IgE are thought to capture percutaneously<br />
absorbed allergen, process and present to allergen-specific T-lymphocytes. In atopic<br />
humans t<strong>here</strong> is subsequent preferential expansion <strong>of</strong> T-helper cells <strong>of</strong> the Th2subset,<br />
which release cytokines such as interleukin (IL)-4, with resultant stimulation<br />
<strong>of</strong> IgE production by B-cells. The cytokine pr<strong>of</strong>ile <strong>of</strong> the increased number <strong>of</strong> Tlymphocytes<br />
demonstrated in the skin <strong>of</strong> allergic horses has yet to be elucidated.<br />
The horse, in comparison to humans and dogs, shows a prominent late-phase<br />
component 4-6 hours after intradermal challenge. As well as IgE-cross-linking<br />
resulting in histamine release from mast cells, liberation <strong>of</strong> histamine from equine<br />
basophils has also been demonstrated. Increased concentrations <strong>of</strong> a numbers <strong>of</strong><br />
inflammatory mediators has been documented during inflammatory reactions in the<br />
horse, including eicosanoids, lysosomal enzymes, proteases, IL-1, leukotriene (LT)B 4,<br />
prostaglandin (PG) E 2, histamine, serotonin, superoxides and tumour necrosis factor<br />
(TNF).<br />
In allergic skin disease in the horse the eosinophil is particularly important, together<br />
with histamine, LTB 4 and platelet aggregating factor (PAF). Histamine injected<br />
intradermally results in the ingress <strong>of</strong> numerous eosinophils and results in marked<br />
oedema. Injection <strong>of</strong> LTB 4 and PAF also stimulates migration <strong>of</strong> eosinophils and<br />
oedema, the number <strong>of</strong> eosinophils being proportional to the oedema. Foster and<br />
colleagues at the Royal <strong>Veterinary</strong> <strong>College</strong>, London, studied cutaneous inflammation<br />
in horses and demonstrated the importance <strong>of</strong> PAF and LTB 4 in horses with sweet<br />
itch (IBH). PAF and LTB 4 induction <strong>of</strong> migration <strong>of</strong> eosinophils and neutrophils in<br />
horses with allergic skin disease. PAF was shown to mimic antigen-induced<br />
inflammatory responses and receptor antagonists to inhibit the responses.<br />
Eosinophils are reported as the predominant inflammatory cells in skin biopsies<br />
taken from atopic horses, as well as those with IBH. Eosinophils contain a range <strong>of</strong><br />
cytotoxic proteins and produce several potent inflammatory mediators and are<br />
pivotal in the inflammatory process triggered by hypersensitivity reactions in the<br />
horse.<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 11
Clinical features:<br />
Whilst summer seasonal recurrent dermatitis has been long-recognised in the horse<br />
and the aetiopathological role <strong>of</strong> hypersensitivity responses to the bites <strong>of</strong> insects,<br />
particularly Culicoides species was elucidated as long ago as the early 1970's, the<br />
concept <strong>of</strong> equine atopy was later in becoming recognised, being featured in<br />
textbooks by the end <strong>of</strong> the 1980's. Although now universally recognised, the<br />
prevalence <strong>of</strong> equine atopic dermatitis is not known. Scott and Miller (2003) report<br />
atopy as the seventh most common equine dermatosis diagnosed at the Cornell<br />
University Clinic, accounting for 3.89% <strong>of</strong> all skin conditions, but some or all <strong>of</strong> an<br />
additional 2.11% with a final diagnosis <strong>of</strong> idiopathic pruritus and 2.44% with<br />
idiopathic urticaria might also be considered as atopic – giving a possible total <strong>of</strong><br />
8.44% <strong>of</strong> horses with skin disease.<br />
Clinical signs most commonly begin in young horses, 1.5-6 years <strong>of</strong> age. T<strong>here</strong> is no<br />
sex predilection, but some reports suggest breed predisposition, but t<strong>here</strong> is not<br />
usually any comparison to a reference population to validate the observation(s).<br />
Signs may be seasonal or non-seasonal, depending upon the allergens involved, and<br />
may initially be seasonal and progressing to be perennial in nature. The major clinical<br />
signs in equine atopic dermatitis are pruritus and/or urticaria. Early in the course <strong>of</strong><br />
the disease affected horses may present with pruritus without obvious<br />
dermatological lesions. Rubbing, biting, stamping, tail-flicking and, occasionally, head<br />
-shaking may be reported. Subsequent self-inflicted damage resulting in the presence<br />
<strong>of</strong> excoriations, partial to complete alopecia, lichenification, thickening and folding<br />
<strong>of</strong> the skin, hyperpigmentation and secondary bacterial infections. Affected areas<br />
included the head, ears, neck, trunk, and legs; in some cases t<strong>here</strong> is also involvement<br />
<strong>of</strong> the regions classically affected in IBH – the dorsolateral neck, mane, dorsal<br />
midline lumbar area and tail base. Urticaria is also a common reaction pattern in<br />
atopic horses, sometimes seen in conjunction with pruritus, but in some cases being<br />
non-pruritic. Some atopic horses present with tufted papules or nodules, which may<br />
become crusted and alopecic. Biopsy <strong>of</strong> these lesions reveals the presence <strong>of</strong><br />
eosinophilic folliculitis (sterile) and/or eosinophilic granulomata.<br />
Horses with atopic dermatitis are only rarely reported to show signs <strong>of</strong> concurrent<br />
allergic conjunctivitis, rhinitis and chronic obstructive pulmonary disease (COPD).<br />
Whilst t<strong>here</strong> is evidence that COPD is an atopic disease (genetically driven,<br />
hypersensitivity response to environmental allergens causing clinical disease), reports<br />
<strong>of</strong> concurrent atopic dermatitis and COPD are rare.<br />
In a series <strong>of</strong> 24 horses referred to the author whilst at the Animal Health Trust,<br />
Newmarket, for investigation <strong>of</strong> clinical signs suggestive <strong>of</strong> an allergic aetiology, but<br />
not consistent with classical summer seasonal recurrent dermatitis due to insect-bite<br />
hypersensitivity, the history and presenting signs were analysed (Littlewood et al<br />
1998). Seven <strong>of</strong> the horses were thoroughbreds (TB) and a further eight were TBcrosses,<br />
with five Welsh cob, unspecified cobs or cob-crosses, one Arab, one Arabcross,<br />
one Belgian warmblood and one pony. Age at diagnosis ranged from 2-30<br />
12<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005
years, median age 6.5 years, with age <strong>of</strong> onset <strong>of</strong> disease 1-27 years (median 5.5 years)<br />
and duration <strong>of</strong> clinical signs at time <strong>of</strong> referral ranging from 2 months to >5years.<br />
Fourteen <strong>of</strong> the horses presented with pruritus and six with pruritus and urticaria.<br />
Four horses had recurrent or chronic urticaria without obvious pruritus, including<br />
one with angio-oedema. The degree <strong>of</strong> pruritus was considered to be severe in six<br />
animals, and was particularly severe in case 3 (see figure 1) resulting in self inflicted<br />
damage and requiring the use <strong>of</strong> a nosebag to prevent biting. In most cases the<br />
clinical signs were restricted to the trunk, with tail rubbing also present in seven,<br />
mane involvement in two and facial irritation noted occasionally. Papules or<br />
“bumps” were reported or found on dermatological examination in six cases. Two<br />
horses had histories <strong>of</strong> intercurrent respiratory problems thought to be <strong>of</strong> allergic<br />
aetiology on the basis <strong>of</strong> previous investigations (endoscopy and cytological<br />
examination <strong>of</strong> tracheo-bronchial washes). In 12 horses the clinical signs were<br />
perennial, with exacerbation in the summer noted in two and winter exacerbation in<br />
two others. Four animals showed a seasonal pattern to their skin problem, one <strong>of</strong><br />
which was restricted to spring, two to the winter and the fourth to the summer. This<br />
latter horse was only stabled in the summer and turned out all winter. In eight<br />
animals the duration <strong>of</strong> clinical signs was not long enough to determine if the<br />
problem was going to be perennial, but in six the signs began in autumn or winter<br />
and two started with symptoms in late summer or autumn. All animals were stabled<br />
for at least 50% <strong>of</strong> the day, with 15 horses being stabled full time at the time <strong>of</strong><br />
maximal clinical signs.<br />
Diagnosis:<br />
A large number <strong>of</strong> differential diagnoses may need to be considered, depending on<br />
the history and distribution <strong>of</strong> clinical signs, but would include:<br />
insect hypersensitivity<br />
ectoparasites (lice, chorioptic mange, psoroptic mange, trombiculidiasis,<br />
poultry mites)<br />
oxyuriasis<br />
forage/storage mites<br />
helminth infestations (oxyuriasis, strongyloidosis, Pelodera cutaneous larval<br />
migrans)<br />
contact dermatitis<br />
adverse cutaneous food reaction<br />
drug reactions<br />
systemic diseases causing pruritus (rare cases <strong>of</strong> lymphoma, hepatic and renal<br />
neoplasia)<br />
As in the dog and cat, the diagnosis <strong>of</strong> atopic dermatitis is reached after ruling out all<br />
other possible differentials and the diagnosis is essentially a clinical diagnosis.<br />
Laboratory investigations such as routine haematological and biochemical pr<strong>of</strong>iles<br />
are rarely contributory to reaching a diagnosis in atopic horses, but may be indicated<br />
to investigate possible systemic disease in cases with suggestive clinical signs. Skin<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 13
iopsies may <strong>of</strong>fer supportive evidence, the typical histopathological features being<br />
superficial to deep, perivascular to interstitial dermatitis with eosinophils being the<br />
predominant inflammatory cell. The epidermis is <strong>of</strong>ten hyperplastic. Spongiosis and<br />
dermal oedema may be seen. Eosinophilic mural folliculitis and eosinophilic<br />
granulomata may occasionally be present as focal changes. These changes are not<br />
pathognomonic for equine atopy and may be present in other hypersensitivity<br />
disorders such as IBH.<br />
Once a clinical diagnosis is reached, specific allergy testing may be employed to<br />
identify allergens that may be implicated in the individual patient so that avoidance<br />
strategies or immunotherapy can be formulated.<br />
Specific allergy testing:<br />
Classically identification <strong>of</strong> implicated allergens in allergic patients has employed<br />
intradermal testing. Studies documenting optimal testing procedures for the horse<br />
are limited and comparisons between different commercial sources <strong>of</strong> allergens are<br />
difficult, since it has been shown the bioactivity <strong>of</strong> products may vary form 10- to<br />
1000- fold, with no relationship between bioactivity and declared concentrations.<br />
T<strong>here</strong> is little published about threshold concentrations <strong>of</strong> various allergens for the<br />
horse, to try and avoid false-positive, irritant reactions in non-allergic horses. T<strong>here</strong><br />
are problems <strong>of</strong> standardisation <strong>of</strong> allergen extracts in terms <strong>of</strong> the source, raw<br />
material, extraction methods, identification <strong>of</strong> substances, standardisation <strong>of</strong><br />
concentration <strong>of</strong> ingredients, stabilisation and potency. Selection <strong>of</strong> allergens for<br />
testing should take account <strong>of</strong> the experience <strong>of</strong> colleagues in the human and<br />
veterinary field, preferably those working in the same region. Use <strong>of</strong> allergen mixes is<br />
not advised, in case <strong>of</strong> false-negative reactions in horses allergic to only one or two<br />
<strong>of</strong> the mix – although the presence <strong>of</strong> common allergens within certain groups <strong>of</strong><br />
allergens, particularly tree pollens and grass pollens, may make this <strong>of</strong> less concern.<br />
Moulds and weed pollens show less antigenic similarity and thus testing with<br />
individual allergens is <strong>of</strong> more importance in these groups.<br />
False positive skin test reactions have been reported by a number <strong>of</strong> investigators.<br />
Fadok (1986) tested 39 normal horses and documented false positive reactions,<br />
mostly to insects, with more reactions in horses over 6 years <strong>of</strong> age; no false positive<br />
reactions were found with pollens or mould extracts. Evans et al (1992) reported<br />
false positives in a study <strong>of</strong> horses with COPD and urticaria, which were thought to<br />
be possibly subclinical cases. Interestingly, intradermal tests performed on specificpathogen<br />
(parasite) free ponies gave no positive reactions (Foil 1992).<br />
Rosenkrantz et al (1998) studied 28 horses with IBH and atopic disease and ten<br />
normal horses. Three <strong>of</strong> the ten had no reactions, but seven showed positive<br />
reactions, three including delayed reactions, against 1-9 antigens. Insect reactions<br />
were commonly found in these normal horses (deer fly, horse fly, house fly, black<br />
fly, mosquito, flea) and also weeds (yellow dock, Russian thistle, firebush). Other<br />
allergens that have been suggested to be possible irritants in horses include grain mill<br />
14<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005
dusts, grain smuts, moulds, danders and mites and so positive reactions must be<br />
interpreted with caution.<br />
More recent studies <strong>of</strong> intradermal testing in horses with atopic dermatitis or<br />
recurrent urticaria, compared to non-atopic horses, revealed significantly greater<br />
mean numbers <strong>of</strong> positive reactions in horses with skin disease, at 30minutes<br />
(immediate) and late-immediate and delayed time points, and to significantly higher<br />
numbers <strong>of</strong> allergens in each group <strong>of</strong> allergens (Lorch et al 2001, Jose-Cunilleras et<br />
al 2001). The authors emphasise that the presence <strong>of</strong> positive reactions to individual<br />
allergens is not diagnostic <strong>of</strong> hypersensitivity, but patterns <strong>of</strong> reactivity are helpful in<br />
management <strong>of</strong> cases when used together compatible history and evidence <strong>of</strong><br />
exposure.<br />
Selection <strong>of</strong> strict criteria for interpretation <strong>of</strong> positive versus negative results has<br />
been shown to reduce the number <strong>of</strong> false positive or irrelevant results and improve<br />
the sensitivity and predictive value <strong>of</strong> intradermal testing (Jose-Cunilleras et al 2001).<br />
Wheal reactions should be scored on the basis <strong>of</strong> diameter and turgidity <strong>of</strong> the<br />
reaction, in comparison to the controls. However, t<strong>here</strong> is no consensus on the<br />
criteria for scoring: a scale <strong>of</strong> 0-5+ is commonly cited, w<strong>here</strong> 0 is the size <strong>of</strong> the<br />
negative control, 5+ is the maximal response, 4+ is the size <strong>of</strong> the histamine control<br />
and 2+ is the mean <strong>of</strong> the difference between the positive and negative controls.<br />
Whilst 2+ reactions and greater have been considered positive by many authors,<br />
using a cut-<strong>of</strong>f <strong>of</strong> 3+ and greater reactions is recommended.<br />
In summary, a “positive” skin test reaction may indicate clinically relevant<br />
hypersensitivity, subclinical hypersensitivity or an irritant, false-positive reaction.<br />
Normal horses <strong>of</strong>ten show positive reactions, particularly to insect extracts, and<br />
show increasing numbers <strong>of</strong> positive reactions with age. Nonetheless, in horses with<br />
compatible clinical signs, intradermal testing is extremely useful in case management.<br />
Serological testing to identify the presence <strong>of</strong> circulating, antigen-specific IgE has<br />
received much attention in human and canine atopic disease, with fewer publications<br />
in feline and equine allergic skin disease. A number <strong>of</strong> problems exist with these in<br />
vitro tests, including the fact that IgE titres in dogs do not correlate with clinical<br />
disease. Heterogeneity <strong>of</strong> IgE is thought to exist, with some types being associated<br />
with clinical disease (IgE+) and others not (IgE-). Alternatively the defect may be<br />
at target tissue level rather than in circulating IgE concentrations. Studies at the<br />
Animal Health Trust with various reagents employed in canine in vitro tests, and<br />
published studies, have shown marked variation in test results with different<br />
reagents. Samples sent to different commercial companies have shown poor<br />
reproducibility <strong>of</strong> results. Normal dogs and dogs with any kind <strong>of</strong> skin disease may<br />
show positive reactions and publications have shown poor to moderate correlation<br />
with intradermal testing in dogs and cats. Some <strong>of</strong> these findings may be explained<br />
by poor specificity – particularly with polyclonal anti-IgE, but also with some<br />
monoclonal, reagents cross-reacting with other classes <strong>of</strong> immunoglobulin; low<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 15
affinity <strong>of</strong> binding with monoclonal reagents may also be a problem. Species<br />
specificity <strong>of</strong> reagents is also <strong>of</strong> vital importance.<br />
The most recent technology employs a recombinant peptide <strong>of</strong> the alpha chain <strong>of</strong><br />
the high-affinity Fc epsilon receptor for detection <strong>of</strong> IgE (Allercept reagent), and has<br />
vastly improved specificity. Studies <strong>of</strong> more than 250 atopic dogs comparing<br />
intradermal testing with Greer allergens and Allercept serological test results showed<br />
good correlation for dogs with housedust mite sensitivity, although intradermal<br />
testing was more sensitive; insufficient data were available to analyse other allergens<br />
(Foster et al, 2003).<br />
In the horse various commercial tests are available, but t<strong>here</strong> is little published<br />
evidence concerning the validation and reliability <strong>of</strong> such tests. A test using the<br />
FcR1 -based assay for horses is now available and t<strong>here</strong> is some published data<br />
comparing this and other in vitro tests with intradermal tests (Lorch et al 2001).<br />
Seventeen horses with recurrent urticaria and/or atopic dermatitis, 16 with COPD<br />
and 22 non-atopic horses were studied with a panel <strong>of</strong> 73 intradermal antigens and 3<br />
serological tests. The test using the FcR1 -based assay had the overall highest kappa<br />
statistic positive predictive and negative predictive values, but overall agreement with<br />
the intradermal test was only fair. The highest kappa statistic was for horses with<br />
atopic dermatitis. The kappa statistics for the radioallergosorbent test (RAST) and a<br />
polyclonal-base ELISA agreed only slightly with that <strong>of</strong> the intradermal test. The<br />
authors concluded that none <strong>of</strong> the three serum tests reliably detected allergen<br />
hypersensitivity, compared to the intradermal test, although the FcR1 -based assay<br />
performed significantly better than the other two tests, but the low sensitivity <strong>of</strong> all 3<br />
assays indicated the need for more sensitive tests.<br />
Antisera have been raised against equine epsilon chain peptides, derived from the<br />
nucleotide sequence <strong>of</strong> equine IgE and one reagent was found to be useful in the<br />
detection <strong>of</strong> equine IgE in clinically allergic animals and also as a research tool<br />
(Kaline et al 2003).<br />
Whilst the serological tests <strong>of</strong>fer the clinician the attraction <strong>of</strong> an easily performed<br />
test, the shortcomings <strong>of</strong> the currently available tests are considered by Scott and<br />
Miller (2003) “to be <strong>of</strong> no diagnostic or therapeutic benefit and to be a waste <strong>of</strong><br />
money”<br />
16<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005
References:<br />
Evans AG, Paradis MR, & O'Callaghan M. (1992) Intradermal testing <strong>of</strong> horses with<br />
chronic obstructive pulmonary disease and urticaria. American Journal <strong>of</strong> <strong>Veterinary</strong><br />
Research53, 203<br />
Fadok V (1986) Equine pruritus: results <strong>of</strong> intradermal skin testing. Proceedings <strong>of</strong> the<br />
Annual Meeting <strong>of</strong> the American Academy and <strong>College</strong> <strong>of</strong> <strong>Veterinary</strong> Dermatology New<br />
Orleans, p6<br />
Foil C (1992) Therapy <strong>of</strong> equine pruritus. Proceedings <strong>of</strong> the 2 nd World Congress <strong>of</strong><br />
<strong>Veterinary</strong> Dermatology, Montreal, Canada p434<br />
Foster AP, Littlewood JD, Webb P, Wood JLN, Rogers K & Shaw SE. (2003)<br />
Comparison <strong>of</strong> intradermal and serum testing for allergen-specific IgE using a<br />
FcR1 -based assay in atopic dogs in the UK. <strong>Veterinary</strong> Immunology &<br />
Immunopathology 92, 51-60<br />
Jose-Cunilleras E, Kohn CW, Hillier A, Saville WJ & Lorch G. (2001) Intradermal<br />
testing in health horses and horses wih chronic obstructive pulmonary disease,<br />
recurrent urticaria, or allergic dermatitis.Journal <strong>of</strong> the American <strong>Veterinary</strong> Medical<br />
Association 219, 1115-21<br />
Kalina WV, Pettigrew HD & Gershwin LJ (2003) IgE ELISA using antisera derived<br />
from epsilon chain antigenic peptides detects allergen-specific IgE in allergic horses.<br />
<strong>Veterinary</strong> Immunology & Immunopathology 92, 134-47.<br />
Littlewood JD, Paterson S, & Shaw SC. (1998) Atopy-like skin disease in the horse.<br />
Advances in <strong>Veterinary</strong> Dermatology 3, p563<br />
Lorch G, Hiller A, Kwochka KW, Saville WA & LeRoy BE (2001) Results <strong>of</strong><br />
intradermal tests in horses without atopy and with atopic dermatitis or recurrent<br />
urticaria. American Journal <strong>of</strong> <strong>Veterinary</strong> Research 62, 1051-9<br />
Rees CA (2001) Response to immunotherapy in six related horses with urticaria<br />
secondary to atopy. Journal <strong>of</strong> the American <strong>Veterinary</strong> Medical Association 218, 753-5<br />
Rosenkrantz WS, Griffin CE, Esch RE & Mullens BA (1998) Responses in horses to<br />
intradermal challenge <strong>of</strong> insects and environmental allergens with specific<br />
immunotherapy. Advances in <strong>Veterinary</strong> Dermatology 3, 191-200<br />
Scott DW & Miller WH (2003) Skin immune system and allergic skin diseases. In<br />
Equine Dermatology, Elsevier Science pp395-474.<br />
Van der Haegen A, Griot-Wenk M, Welle M, Busatro A, von Tscharner C,<br />
Zurbriggen A & Marti E (2001) Immunoglobulin-E-bearing cells in skin biopsies <strong>of</strong><br />
horses with insect bite hypersensitivity. Equine <strong>Veterinary</strong> journal 33, 699-706<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 17
18<br />
Intradermal Testing (IDT) in Horses:<br />
The <strong>Australian</strong> Perspective<br />
Applications <strong>of</strong> IDT in Australia<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005<br />
Tina Baxter<br />
Intradermal testing (IDT) is probably an underutilized diagnostic tool in Australia.<br />
The incidence <strong>of</strong> atopy in <strong>Australian</strong> horses has not been documented. ‘Skin disease’<br />
or ‘itch’ is a common presentation - approximately 20% <strong>of</strong> horse owners surveyed<br />
recently in Queensland reported their horses had a ‘skin problem’ (28) - and the<br />
majority <strong>of</strong> these had clinical presentations that were consistent with insect bite<br />
hypersensitivity. As the exact trigger <strong>of</strong> the skin disease was not identified in these<br />
cases, t<strong>here</strong> may be a poor clinical distinction between insect related hypersensitivity<br />
and atopic dermatitis.<br />
More importantly, intradermal testing has applications in diseases other than atopic<br />
dermatitis, both <strong>here</strong> and overseas, and the following notes are equally relevant in<br />
performing the test for horses with insect bite hypersensitivity (including Queensland<br />
itch), recurrent urticaria, head shaking, chronic obstructive pulmonary disease and<br />
other airway diseases (reactive airway disease) w<strong>here</strong> an allergic basis is suspected<br />
(7,12, 14, 16, 25). While Type I hypersensitivity is not the only contributing factor in<br />
these diseases, information gained from intradermal testing in these cases can only be<br />
<strong>of</strong> benefit. In a survey <strong>of</strong> aged horses, an estimate <strong>of</strong> 22% <strong>of</strong> horses had respiratory<br />
disease and the majority <strong>of</strong> these are thought to have an allergic pathogenesis (28).<br />
Possible reasons for the relative paucity <strong>of</strong> equine cases undergoing intradermal<br />
allergy testing include:<br />
The test requires time, skill and experience to perform, such that it is usually<br />
performed only by specialists in dermatology<br />
Much <strong>of</strong> the information and experience in IDT available to specialists in<br />
dermatology is based on small animals. Clinic facilities and personal<br />
preference <strong>of</strong> the dermatologist may preclude the handling <strong>of</strong> horses<br />
The allergens used in the test have a limited shelf life, so regular tests need to<br />
be performed to make the purchase <strong>of</strong> the allergens worthwhile and ensure<br />
the cost <strong>of</strong> the test to the individual owner remains reasonable<br />
Referral requires effort on the owners part to travel (in some cases significant<br />
distances from country regions <strong>of</strong> Australia) to the nearest major centre<br />
Costs and time to the owner: the average cost to the owner for IDT and<br />
consultation are around$500 to $650; costs <strong>of</strong> travel and time are additional
Comparatively simple, cheap and effective treatments are <strong>of</strong>fered by the<br />
general veterinarian. Glucocorticoids, environmental management (such as<br />
stabling, rugging, topical insecticides), antibiotics and antihistamines are<br />
<strong>of</strong>ten prescribed, with many patients achieving acceptable control <strong>of</strong> their<br />
clinical signs with this management.<br />
Additional treatment options made available by results <strong>of</strong> IDT may be<br />
perceived to be more complex and expensive; allergen specific<br />
immunotherapy (ASIT) is an onerous task for many owners despite it’s<br />
benefits; and avoidance <strong>of</strong> allergens is usually impractical or impossible.<br />
Lack <strong>of</strong> awareness by horse owners that allergy testing is available and <strong>of</strong>fers<br />
a beneficial alternative or adjunct to other standard treatments<br />
Often cases are referred as a last resort and poorer results are attained than<br />
had the case been referred early in the course <strong>of</strong> disease<br />
Education <strong>of</strong> both horse owners and veterinarians <strong>of</strong> the availability <strong>of</strong> IDT, and its<br />
means to improved management <strong>of</strong> many affected patients, is essential to improve the<br />
utilization <strong>of</strong> intradermal allergy testing as a diagnostic tool.<br />
Availablility <strong>of</strong> IDT in Australia<br />
T<strong>here</strong> are only four centres in Australia at which equine intradermal testing is<br />
performed in Australia:<br />
Sydney<br />
Melbourne<br />
Perth<br />
Brisbane<br />
Following are the summarized details <strong>of</strong> the testing procedure, which for the most<br />
part, are similar across the different centres.<br />
Allergen Purchase<br />
For all four centres, allergen extracts are purchased through Dermcare Vet (Pty Ltd)<br />
who import the extracts from Greer Laboratories (Lenoir NC, USA).<br />
Allergen Selection<br />
Each centre has selected a range <strong>of</strong> allergens based on regional knowledge <strong>of</strong> relevant<br />
plants and insects, but is somewhat limited by the allergens available from the<br />
manufacturer. Allergen selection can be refined through various sources <strong>of</strong><br />
information:<br />
Physicians in human allergy (and allergen testing panels from the same<br />
geographical region)<br />
National pollen charts; available from government agricultural organizations<br />
Local agronomists and botanists<br />
Entemologists may assist in insect species selection<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 19
The allergens used for equine skin testing tend to be the same that is used for small<br />
animal testing, and <strong>of</strong>ten allergen selection has occurred with small animals in mind.<br />
Additional horse-specific allergens such as Culicoides are also included for the equine<br />
tests. W<strong>here</strong> horses are housed in the same metropolitan area, it is assumed that<br />
exposure to similar allergens as small animals will occur. However, modifications to<br />
the allergen selection may be necessary for horses from more distant country areas.<br />
It is not apparent whether particular allergens are relevant in horses, as their lifestyle<br />
may prevent significant exposure to various substances; such as insects (cockroach),<br />
House-dust mites and pollens from fodder materials brought into the area rather than<br />
grown in the area. Testing with epithelia (from other animals and humans) is not<br />
possible in Australia due to quarantine regulation against the importation <strong>of</strong> such<br />
allergens, so the significance <strong>of</strong> these is unknown in the <strong>Australian</strong> context. In one<br />
study in affected horses, positive intradermal test reactions to epithelia were seen in a<br />
significant number <strong>of</strong> clinically affected horses (54.2% to human dander!)(2).<br />
Allergen mixes are available, but testing with these is not recommended (1), as the<br />
concentration <strong>of</strong> the individual allergens in the mix becomes too dilute for detection.<br />
Variation in species <strong>of</strong> insect and pollen allergens may also be important. The<br />
Culicoides extract available through Greer laboratories is derived from Culicoides<br />
nebiculosis. In Australia, Culicoides brevitarsis is considered to be the only relevant species<br />
<strong>of</strong> Culicoides (at least in NSW, according to entomologists at the Elizabeth Macarthur<br />
Agricultural Institute - pers comm.). Information from Greer suggests that crossreactivity<br />
across most species <strong>of</strong> Culicoides can be expected, but the reality <strong>of</strong> this<br />
assumption is not known.<br />
20<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005
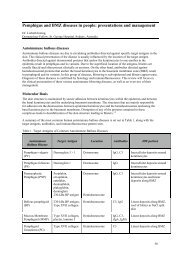
TABLE 1: CURRENT ALLERGENS SELECTED FOR INTRADERMAL<br />
TESTING BY VARIOUS CENTRES IN AUSTRALIA<br />
Melbourne Sydney Brisbane Perth<br />
Grass Pollens<br />
Bent <br />
Brome <br />
Canary (Phalaris) <br />
Cocksfoot <br />
Couch <br />
Couch, English <br />
Fescue <br />
Johnson grass <br />
Kentucky Bluegrass <br />
Maize <br />
Oat <br />
Orchard <br />
Paspalum <br />
Perennial Rye <br />
Prairie Grass <br />
Sweet Vernal <br />
Timothy <br />
Wheat, Cultivated <br />
Yorkshire Fog<br />
Weed Pollens<br />
<br />
Chenopodium mix <br />
Cocklebur <br />
Daisy <br />
Dandelion <br />
Dog Fennel) <br />
Fat Hen <br />
Lucerne (Alfalfa) <br />
Mexican Tea <br />
Mugwort <br />
Mustard <br />
Nettle <br />
Perennial Ragweed <br />
Plantain <br />
Ragweed, short <br />
Ragweed, Western <br />
Red Sorrel <br />
Rough Pigweed <br />
Sunflower <br />
Tobacco Leaf <br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 21
Tumbleweed <br />
Yellow<br />
Dock/Curled Dock<br />
Tree Pollens<br />
<br />
Alder <br />
Ash (Oregon) <br />
Birch (Birch mix) <br />
Birch, grey <br />
Casuarina <br />
Cypress <br />
Elm, cedar <br />
Elm, Chinese <br />
Eucalyptus <br />
Juniper <br />
Liquid Amber <br />
Maple <br />
Melaleuca <br />
Oak <br />
Oak, black <br />
Oak, red <br />
Oak, white <br />
Olive <br />
Palm <br />
Peppercorn (Pepper<br />
Tree)<br />
<br />
Pine (Pine mix) <br />
Pine, White <br />
Pine, yellow<br />
(Ponderosa)<br />
<br />
Plane Tree<br />
(Sycamore)<br />
<br />
Poplar <br />
Privet <br />
Wattle (Acacia spp) <br />
Willow, Arroyo <br />
Willow, black<br />
Moulds<br />
<br />
Alternaria <br />
Aspergillus <br />
Cladosporium <br />
Curvufaria <br />
Penicillium<br />
Insects<br />
<br />
Ant, Black <br />
22<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005
AmericanCockroach <br />
Cockroach mix <br />
Culicoides <br />
Deer Fly <br />
Flea <br />
Horse Fly <br />
House Fly <br />
Mosquito <br />
Moth<br />
Dust Mites<br />
<br />
D.farinae <br />
D.pteronyssinus<br />
Storage Mites<br />
<br />
Acarus siro (flour) <br />
Blomia tropicalis (grain) <br />
Lepidoglyphus destructor<br />
<br />
(fodder)<br />
Tyrophagus putrescentiae<br />
(cheese)<br />
<br />
Miscellaneous<br />
Carpet Grass Dialysate <br />
Carpet Grass <br />
Casuarina 1:40 <br />
Casuarina Dialysate 1:40 <br />
Grain Mill Dust Mix <br />
House Dust <br />
Kapok <br />
Kikuyu Dialysate <br />
Kikuyu Grass <br />
Kochia <br />
Malassezia <br />
Mixed feathers <br />
QLD Blue Couch 1:40 <br />
QLD Blue Couch Dialysate<br />
1:40<br />
Allergen Dilution<br />
Red Clover <br />
Concentrations <strong>of</strong> allergens used for skin testing in horses in Australia have been<br />
based on those used for small animals, which were loosely derived from human<br />
studies and modified according to reactions in normal dogs in early work (10). In<br />
Australia, most allergens (grass, tree and weed pollens, moulds and insects) from<br />
Greer are tested at a concentration <strong>of</strong> 1000pnu (Protein Nitrogen Units), with some<br />
minor exceptions (15, 16). Dust mite and various other allergens are provided in<br />
weight per volume measurements (w/v), and the standard testing concentration for<br />
these is 1:10 000 which is roughly equivalent to 1000pnu.<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 23
‘False positive’ results in equine intradermal tests are thought to be common (see<br />
further details under Interpretation <strong>of</strong> Results). To some extent, this may be a function <strong>of</strong><br />
using extracts that are too concentrated and thus induce an ‘irritant’ reaction w<strong>here</strong><br />
true allergy is not present.<br />
Extensive work into determination <strong>of</strong> allergen threshold concentrations for<br />
intradermal testing in horses has not been undertaken. A recent study into insect<br />
allergens suggests that concentrations lower than 1000pnu may be more appropriate<br />
for horses (9), and <strong>of</strong>fers some foundation for possible false positive reactions seen<br />
previously. The recommended testing concentration varied with the allergen, but for<br />
some allergens (particularly in the fly group) the concentration that evoked a positive<br />
response in 25% <strong>of</strong> normal horses was 250pnu/mL or less.<br />
Data is still being evaluated for a study the author has undertaken to determine<br />
pollen, insect, dust mite, mould and storage mite allergen threshold concentrations in<br />
normal horses. The aim <strong>of</strong> the study was to determine the concentration at which<br />
90% <strong>of</strong> normal horses would score (subjectively) less than 2 on the scale <strong>of</strong> 0 to 4<br />
commonly used by clinicians. The preliminary results suggest the following:<br />
24<br />
Many <strong>of</strong> the pollen concentrations may need to be increased (ie more<br />
concentrated)<br />
Results <strong>of</strong> the insect panel testing support the findings <strong>of</strong> Morris and<br />
Lindborg (9) that most concentrations need to be decreased from 1000pnu<br />
Dust mite concentrations may need to be dramatically decreased (ie more<br />
dilute)<br />
Mould concentrations may currently be somewhat too dilute<br />
The appropriate testing concentration <strong>of</strong> Culicoides appears to be around 1:10<br />
000 w/v, although the manufacturer recommends substantially more dilute<br />
concentrations than this (1:25 000 and 1:50 000)<br />
Storage mites commonly evoke strong delayed reactions, but in light <strong>of</strong> the<br />
immediate reading, higher concentrations than 1:10 000 may be more<br />
suitable<br />
It is apparent that the determination <strong>of</strong> threshold allergen concentrations is complex<br />
and t<strong>here</strong> are many possible variables. It seems unlikely that a single testing<br />
concentration will be possible across the allergens for horses. The completed study<br />
will also assess any variations in relation to season and skin reactivity in normal<br />
horses. It is hoped that this data will greatly increase the reliability and accuracy <strong>of</strong><br />
intradermal testing in horses.<br />
Solutions for skin testing should be made up fresh every 4 weeks, and stored in the<br />
refrigerator (and not allowing them to freeze repetitively) to maintain appropriate<br />
potency (16).<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005
Patient Preparation<br />
Drug Withdrawal<br />
Guidelines for drug withdrawal times in horses prior to skin testing are not based on<br />
scientific data, rather, they have been extrapolated from knowledge in small animals<br />
and with some degree <strong>of</strong> estimate. Recommended withdrawal times are as follows (1,<br />
16):<br />
Two to three weeks for inhaled, oral and topical corticosteroids (longer if<br />
oral corticosteroids have been given for extended periods)<br />
Eight weeks for injectable (‘depo’) corticosteroids<br />
Ten days for antihistamines<br />
Timing <strong>of</strong> skin testing<br />
T<strong>here</strong> is conflicting evidence as to whether intradermal test reactivity declines with<br />
allergen season (17), but clinical experience tends to suggest that it does. Supposing<br />
that IgE remains ad<strong>here</strong>nt to mast cells in skin for a limited period (say 30 days), it<br />
appears sensible to test animals within 6 to 8 weeks <strong>of</strong> the end <strong>of</strong> their allergy season<br />
(1). Falsely negative results are commonly seen in seasonally allergic dogs tested out<br />
<strong>of</strong> their allergy season (18); it would be reasonable to suppose a similar situation exists<br />
in horses. Repeating the skin test during a different season may thus yield different<br />
results.<br />
Intradermal Testing Procedure<br />
1. Restraint for testing<br />
Sedation is recommended for skin testing all but the quietest horses, as a quicker and<br />
smoother injection process will ultimately mean less stress and better results to the<br />
animal. Several sedatives have been suggested for horse skin testing, again based on<br />
knowledge <strong>of</strong> drug interference in small animals. The Alpha 2 agonists are commonly<br />
used, registered sedatives in horses (19) that do not apparently interfere with skin<br />
testing in small animals (18). The author finds the sedation through Detomodine<br />
(Dormosedan; Pfizer) at a dose rate <strong>of</strong> 0.01 to 0.02 mg/kg IV (depending on the<br />
horses nature) both effective and suitable for skin testing. Reversal <strong>of</strong> sedation,<br />
although possible, is not generally carried out.<br />
The length <strong>of</strong> sedation achieved with this protocol is around 30 to 45 minutes, with a<br />
gradual increase in awareness from about 10 minutes into the sedation.<br />
Some horses, despite sedation, remain very reactive to the injection process and will<br />
toss their heads at every injection. A standard nose twitch is recommended for these<br />
horses. We have found that increasing the sedation for these horses appears to make<br />
no difference to this head tossing response; and w<strong>here</strong> the test was repeated, applying<br />
the twitch and no sedation <strong>of</strong>fered a similar level <strong>of</strong> restraint compared with the<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 25
twitch and sedation previously. Caution should be given that not all horses tolerate a<br />
nose twitch well and common sense should prevail!<br />
2. Site Preparation<br />
The preferred site for skin testing is the lateral cervical neck above the jugular furrow,<br />
between the jaw and the shoulder. For a standard 80-injection skin test kit, an area<br />
around the size <strong>of</strong> an A4 sheet <strong>of</strong> paper is clipped with number 40 blades against the<br />
direction <strong>of</strong> hair growth.<br />
W<strong>here</strong> the skin is excessively dirty, gently cleaning with swabs moistened in plain<br />
water should provide a clean working surface.<br />
The author uses a template made <strong>of</strong> stiff plastic to ensure even spacing <strong>of</strong> the<br />
injection site ‘dots’. For 80 injections: 4 rows <strong>of</strong> 10 holes (about 2cm apart) were<br />
created in the template, and a waterpro<strong>of</strong> white ‘paint-pen’ is used to mark the<br />
injection sites. Given that almost all horses have dark skin (even with a pale coat<br />
colour), a dark felt-tipped pen can be completely invisible, particularly when the skin<br />
test site is examined 24 hours after injection.<br />
3. Injection process<br />
Injections are administered intradermally above and below the injection markers. Using<br />
a 30-gauge needle and a 1ml syringe, approximately 0.05 to 0.1ml <strong>of</strong> solution is<br />
injected. The quantity injected appears to be based on personal preference <strong>of</strong> the<br />
clinician; provided the quantity is consistent for every injection in the test, t<strong>here</strong> will<br />
be a relative correlation in the size <strong>of</strong> positive reactions.<br />
The first two and last two injections <strong>of</strong> every test should be the negative and positive<br />
controls <strong>of</strong> saline (or preferably allergen diluent) and histamine (1:100 000)<br />
respectively. The allergens are numbered at the base <strong>of</strong> the syringe plunger and<br />
injected in sequential numerical order.<br />
Some question remains as to whether needles need to be changed if the kit is to be<br />
used again for a different animal. This was discussed with equine veterinarians in<br />
Sydney who concluded it would be prudent to change needles between horses (and<br />
certainly between species <strong>of</strong> animals). Blood borne diseases that may be relevant in<br />
horses include: Equine morbillivirus (the zoonotic potential <strong>of</strong> this disease should<br />
also be observed), Equine infectious anaemia and viral arteritis. Even if the risk <strong>of</strong><br />
these diseases is relatively low, the practitioners were keenly aware that veterinarians<br />
must be seen to be doing the ‘right thing’ in the eyes <strong>of</strong> their clients.<br />
4. Reading the injection sites<br />
It has been recommended that reactions be evaluated at 15 to 30 minutes after<br />
injection, and if possible at 45mins, 4 to 6 hours and at 24 to 48 hours (16). This may<br />
or may not be practical or relevant.<br />
26<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005
Each injection site is visually examined and gently palpated for changes in size,<br />
erythema and turgidity. Reactions are scaled subjectively as with small animals with a<br />
score <strong>of</strong> 0 (no increase in wheal size, using the negative control as a reference) to 4<br />
(large increase in wheal size, using the positive control as a reference), with 2 and 3<br />
reactions being somew<strong>here</strong> in between. Reactions greater than 2/4 are considered to<br />
be positive (16). Some clinicians elect to also measure the wheal diameter to provide a<br />
more objective assessment <strong>of</strong> reactivity.<br />
Interpretation <strong>of</strong> Results<br />
What are we expecting to occur in an allergic individual? At a cellular level, relevant<br />
allergens will theoretically bind and bridge reaginic IgE antibodies on the surface <strong>of</strong><br />
mast cells and result in mast cell degranulation resulting in wheal and flare reactions<br />
(16).<br />
It has been suggested that positive intradermal reactions be interpreted with caution<br />
in horses (1). Various studies have proposed that irritant reactions may be responsible<br />
for false positive results and allergen concentration in the test kit may need to be<br />
adjusted in horses as compared with small animals. In particular, allergens reported to<br />
evoke strong reactions in horses include Lucerne, grain mill dust, grain smuts,<br />
cottonseed, fireweed, yellowdock, Russian thistle, deer fly, Rhizopus spp., Candida<br />
albicans, black fly, horse fly, and black ant (1, 2, 5, 6, 7, 8).<br />
Several studies comparing reactions in normal horses and horses with a variety <strong>of</strong><br />
allergic skin and respiratory diseases have concluded that normal horses will have one<br />
or more positive reactions, but that ‘allergic’ horses will have a significantly greater<br />
number <strong>of</strong> positive reactions; although the significance <strong>of</strong> reactions to individual<br />
allergens has been hard to interpret (1, 7, 8, 11, 12, 13, 14).<br />
Possible causes <strong>of</strong> false positive and false negative results are summarized in a table 2,<br />
extracted from Equine Dermatology by Scott and Miller (1).<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 27
Table 2: Reasons for False Negative and False Positive Reactions in<br />
Intradermal Test Reactions<br />
Reasons for False Negative Reactions Reasons for False Positive Reactions<br />
Subcutaneous injections<br />
Too little allergen<br />
Testing with mixes<br />
Outdated allergens<br />
Allergens too dilute<br />
Too small volume <strong>of</strong> allergen<br />
injected<br />
Drug interference (Glucocorticoids,<br />
antihistamines, tranquilisers,<br />
progestational compounds, any<br />
drugs that lower blood pressure<br />
significantly)<br />
Anergy (testing during peak <strong>of</strong><br />
hypersensitivity reaction)<br />
In<strong>here</strong>nt host factors (estrus,<br />
pregnancy, severe stress – systemic<br />
disease, fright, struggling)<br />
Off-season testing (1-2m after<br />
clinical signs have disappeared)<br />
Histamine ‘hyporeactivity’<br />
28<br />
Irritant test allergens<br />
Allergen too concentrated<br />
Contaminated test allergens (bacteria,<br />
fungi)<br />
Skin-sensitising antibody only (prior<br />
clinical or present subclinical<br />
sensitivity – these reactions would be<br />
more appropriately termed clinically<br />
insignificant)<br />
Poor technique (trauma in needle<br />
placement, blunt needles, too large a<br />
volume injected, air injected)<br />
‘Irritable’ skin (large reactions seen to<br />
all injected substances, including<br />
saline control)<br />
Dermatographism<br />
Ectoparasitism (cross reactions with<br />
house dust mite extracts)<br />
Mitogenic allergen<br />
As further information about skin testing in horses comes to light, more accurate or<br />
reliable skin test results and useful assumptions about the results can be expected. At<br />
this stage, intradermal testing is still just one <strong>of</strong> the diagnostic modalities in the workup<br />
<strong>of</strong> allergy cases and the importance <strong>of</strong> other details in the case such as clinical<br />
signs, history, season <strong>of</strong> testing and other test results should not be overlooked.<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005
References<br />
1. Scott DW, Miller WH: Skin Immune System and Allergic Skin Disorders. In:<br />
Equine Dermatology. Saunders, Missouri, 2003<br />
2. Littlewood JD, Paterson S, Shaw SC. Atopy-Like Skin Disease in the Horse.<br />
In: Kwochka KW et al (eds). Advances in <strong>Veterinary</strong> Dermatology III.<br />
Butterworth-Heinemann, Boston, 1998 p 563<br />
3. Barbet JL et al: Diseases <strong>of</strong> the skin. In: Colahan PT et al (Eds). Equine<br />
Medicine and Surgery IV, Vol II. American <strong>Veterinary</strong> Publications, Inc,<br />
Goleta 1991, p 1569<br />
4. Byars DT: Allergic skin diseases in the horse. Vet Clin N Am Large Anim<br />
Pract 6: 87, 1984<br />
5. Rosenkrantz WS, Frank LA: Therapy <strong>of</strong> equine prusitus. In Ihrke RJ, et al<br />
(eds). Advances in <strong>Veterinary</strong> Dermatology II. Pergamon Press, Oxford, 1993,<br />
p433<br />
6. Fadok VA: Overview <strong>of</strong> Equine pruritus. Vet Clin N Am Equine Pract 11:1,<br />
1995<br />
7. Jose-Cunilleras E, Kohn CW, Hillier A, Saville WJA, Lorch, G: Intradermal<br />
testing in healthy horses and horses with chronic obstructive pulmonary<br />
disease, recurrent urticaria, or allergic dermatitis. J Am Vet Med Assoc<br />
219:1115, 2001<br />
8. Rosenkrantz WS et al: Responses in horses to intradermal challenge <strong>of</strong> insects<br />
and environmental allergens with specific immunotherapy. In: Kwochka KW,<br />
et al (Eds). Advances in <strong>Veterinary</strong> Dermatology III. Butterworth-Heinemann,<br />
Boston, 1998, p 200<br />
9. Morris DO, Lindborg, S: Determination <strong>of</strong> ‘irritant’ threshold concentrations<br />
for intradermal testing with allergenic extracts in normal horses. <strong>Veterinary</strong><br />
Dermatology 14:31-36, 2003<br />
10. Willemse A, Van Den Brom WE: Evaluation <strong>of</strong> the intradermal allergy test in<br />
normal dogs. Research in <strong>Veterinary</strong> Science 32:57-61, 1982<br />
11. Fadok VA: Update on equine allergies. Vet Allergy Clin Immunology 5:68,<br />
1997<br />
12. Evans AG et al: Intradermal Testing <strong>of</strong> horses with chronic obstructive<br />
pulmonary disease and recurrent urticaria. Am J Vet Res 53:203, 1992<br />
13. Delger JM: Intradermal testing and immunotherapy in horses. Vet Med 92:635,<br />
1997<br />
14. Halliwell REW: The role <strong>of</strong> allergy in chronic pulmonary diseases <strong>of</strong> horses. J<br />
Am Vet Med Assoc 174:277, 1979<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 29
15. Hensel P, Austel M, Medleau L, Zhao Y, Vidtashankar A: Determination <strong>of</strong><br />
threshold concentrations <strong>of</strong> allergens and evaluation <strong>of</strong> two different histamine<br />
concentrations in canine intradermal testing. Vet Derm 15: 304-308, 2004<br />
16. Rosenkrantz W: Allergy Testing in Horses. Proceedings <strong>of</strong> the 5 th World<br />
Congress in <strong>Veterinary</strong> Dermatology, p244, 2004<br />
17. Nuttall T: Controversies in allergy testing. Proceedings <strong>of</strong> the 5 th World<br />
Congress in <strong>Veterinary</strong> Dermatology, p 367, 2004<br />
18. Scott, Miller, Griffin: Small Animal Dermatology, 6 th Edition. Eds: Muller and<br />
Kirk. WB Saunders, Pennsylvania 2001<br />
19. Freeman SL, England GC: Investigation <strong>of</strong> romifidine and detomodine for the<br />
clinical sedation <strong>of</strong> horses. The <strong>Veterinary</strong> Record 147: 507-511, 2000<br />
20. Fadok VA, Mullowney PC: Dermatologic diseases <strong>of</strong> horses, part 1. Parasitic<br />
dermatoses <strong>of</strong> the horse. Compend Cont Educ 5:S615, 1983<br />
21. Littlewood JD: Diagnostic procedures in equine skin disease. Equine Vet Educ<br />
9:174, 1997<br />
22. Mullowney PC: Dermatologic Diseases <strong>of</strong> horses part V: allergic, immunemediated<br />
and miscellaneous skin diseases. Compend continuing Educ 7:S217,<br />
1985<br />
23. Pascoe RR: The nature and treatment <strong>of</strong> skin conditions observed in horses in<br />
Queensland. Aust vet J 49:35, 1973<br />
24. Eder C, et al. Influence <strong>of</strong> environmental and genetic factors on allergenspecific<br />
immunoglobulin-E levels in sera from Lipizzan horses. Equine Vet J<br />
33:714 2001<br />
25. Quinn PJ, Baker KP, Morrow AN. Sweet itch: Responses <strong>of</strong> clinically normal<br />
and affected horses to intradermal challenge with extracts <strong>of</strong> biting insects.<br />
Equine Vet J 15:266-272 1983<br />
26. Kolm-Stark G, Wagner R: IDST in Icelandic horses in Austria. Equine Vet J<br />
34: 405, 2002<br />
27. Sloet van Oldruitenborgh-Oisterbann MM et al: Intradermal allergy testing in<br />
normal horses. In: Kwochka KW et al (eds). Advances in <strong>Veterinary</strong><br />
Dermatology III. Butterworth-Heinemann, Boston, 1998 p 564<br />
28. Personal communication with Cathy McGowan from the University <strong>of</strong><br />
Queensland<br />
30<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005
Intradermal Testing (IDT) in Horses:<br />
The UK Perspective<br />
Janet Littlewood<br />
Horses with a history <strong>of</strong> recurrent pruritus and /or urticaria represent the largest<br />
proportion <strong>of</strong> equine dermatology referral cases in the author's practice. Referred<br />
cases usually have a history <strong>of</strong> recurrent problems <strong>of</strong> at least 2 months duration.<br />
Ideally an elimination diet is undertaken before referral – although the almost<br />
complete absence <strong>of</strong> well-defined cases <strong>of</strong> adverse cutaneous food reaction in horses<br />
makes it a rare diagnosis, and so this is not considered essential, either prior to or<br />
after referral, although it is advised. Clients are <strong>of</strong>ten reluctant to limit their horses to<br />
strict, narrow elimination diets, particularly if they want to continue to work the<br />
horse. History and clinical examination are undertaken to rule out other possible<br />
causes <strong>of</strong> urticaria and pruritus, and if the signs are consistent with hypersensitivity,<br />
intradermal testing is undertaken. The author requests that horses be <strong>of</strong>f<br />
antihistamines for a minimum <strong>of</strong> 2 weeks and have received no steroids for a month<br />
(ideally), although withdrawal <strong>of</strong> low dose alternate day steroids may not need to be<br />
for this period. Food additives, particularly aloe vera extract, should also be<br />
withdrawn – this advice is given on the basis <strong>of</strong> negative intradermal test results<br />
being obtained in a horse currently receiving aloe vera, with positive results obtained<br />
at retesting 3 weeks after withdrawal.<br />
Horses are sedated for intradermal testing, with detomidine hydrochloride (0.06-<br />
0.12mg/kg) and butorphanol 0.075-0.15mg/kg) intravenously. An area on the lateral<br />
aspect <strong>of</strong> the shoulder is clipped with a number 40 blade and injection sites marked<br />
with a permanent marker pen at 2 cm intervals. Allergens for testing are obtained<br />
from Greer Laboratories Inc., North Carolina, USA with additional forage mites<br />
supplied by Artuvetrin Biologicals nv, Lelystad, Netherlands. In the past allergens<br />
have also been supplied by Stallervet, France. The selection <strong>of</strong> allergens used in<br />
intradermal testing in dogs in the UK was originally based on advice obtained from<br />
colleagues in human allergy medicine and using information from publications and<br />
texts. Over the years the author has changed and refined the test kit, in conjunction<br />
with colleagues and in the light <strong>of</strong> frequency <strong>of</strong> negative and positive reactions. In<br />
fact, apart from the Culicoides antigen, which is restricted for testing <strong>of</strong> horses, the<br />
author currently uses the same allergens in dogs and horses. Allergens supplied from<br />
Greer are stored in concentrated form and diluted to testing strength, w<strong>here</strong>as the<br />
European allergens are supplied at testing strength. The testing strengths used are<br />
selected on the basis <strong>of</strong> advice from the allergen companies and from published data.<br />
The restrictions on experimentation in the UK mean that very little work has been<br />
done on optimising <strong>of</strong> allergen concentrations, apart from work done on Culicoides<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 31
antigen concentration in the course <strong>of</strong> research projects conducted at the Royal<br />
<strong>Veterinary</strong> <strong>College</strong>, London. The author uses histamine at a concentration <strong>of</strong><br />
2.75μg/ml as the positive control and phenolised normal saline as the negative<br />
control and an injection volume <strong>of</strong> 0.05ml.<br />
The allergens used in a study <strong>of</strong> 24 horses referred with recurrent or chronic pruritus<br />
and/or urticaria, but not typical <strong>of</strong> Culicoides hypersensitivity (Littlewood et al 1998),<br />
are listed in the following tables:<br />
TABLE 1<br />
Allergens used for intradermal skin testing obtained from Greer and<br />
Artuvetrin<br />
Allergen Concentration Allergen Concentration<br />
Ctenocephalides spp 1:1,000 w/v Weed pollens<br />
Tyrophagus putresceantiae 10 PNU/ml Mugwort 1,000 PNU/ml<br />
Acarus siro 10 PNU/ml Wild brassica 1,000 PNU/ml<br />
Dermatophagoides farinae 1:2,000 w/v Jerusalem oak 1,000 PNU/ml<br />
D. pteronyssinus 1:2,000 w/v Lamb’s quarter 1,000 PNU/ml<br />
Housedust 250 PNU/ml Daisy 1,000 PNU/ml<br />
Human dander 10 µg/ml Plantain 1,000 PNU/ml<br />
Cat dander 1,000 PNU/ml Sheep’s sorrel 1,000 PNU/ml<br />
Sheep epithelia 500 PNU/ml Yellow dock 1,000 PNU/ml<br />
Mixed feathers 1,000 PNU/ml Dandelion 1,000 PNU/ml<br />
Kapok 1,000 PNU/ml Clover 1,000 PNU/ml<br />
Tree pollens Nettle 1,000 PNU/ml<br />
Birch 1,000 PNU/ml Moulds<br />
Alder 1,000 PNU/ml Alternaria alternata 1,000 PNU/ml<br />
Hazel 1,000 PNU/ml Aspergillus fumigatus 1,000 PNU/ml<br />
Beech 1,000 PNU/ml Botrytis cinerae 1,000 PNU/ml<br />
Ash 1,000 PNU/ml Cladosporium herbarum 1,000 PNU/ml<br />
Sycamore 1,000 PNU/ml Epicoccum purpurascens 1,000 PNU/ml<br />
Poplar 1,000 PNU/ml Fusarium moniliforme 1,000 PNU/ml<br />
Oak 1,000 PNU/ml Helminthosporium sativum 1,000 PNU/ml<br />
Willow 1,000 PNU/ml Penicillium notatum 1,000 PNU/ml<br />
Grass pollens Phoma betae 1,000 PNU/ml<br />
Meadow grass 1,000 PNU/ml Pullularia pullulans 1,000 PNU/ml<br />
Fescue 1,000 PNU/ml Rhodotorula rubra 1,000 PNU/ml<br />
Cocksfoot 1,000 PNU/ml Cereal smuts<br />
Bent-grass 1,000 PNU/ml Barley smut 1,000 PNU/ml<br />
Italian rye grass 1,000 PNU/ml Oat smut 1,000 PNU/ml<br />
Timothy 1,000 PNU/ml Wheat smut 1,000 PNU/ml<br />
Key: PNU = protein nitrogen units; w/v = weight/volume dilution<br />
32<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005
TABLE 2<br />
Additional allergens used in a limited number number <strong>of</strong> horses,<br />
obtained mainly from Stallervet<br />
Allergen Concentration Allergen Concentration<br />
Euroglyphus maynei 1/1.000 w/v Grass pollens<br />
Dog dander * 1,000 PNU/ml Sweet vernal grass 10 IRU/ml<br />
Tree pollens Yorkshire fog 1/1,000 w/v<br />
Horse chestnut 1/1,000 w/v Perennial rye grass 10 IRU/ml<br />
Elm 1/1,000 w/v Couch grass 1/1,000 w/v<br />
Elder 1/1,000 w/v Weed/flower pollens<br />
Privet 1/1,000 w/v Ragweed 10 IRU/ml<br />
Lime 1/1,000 w/v Golden rod 1/1,000 w/v<br />
Moulds Wall pellitory 1/1,000 w/v<br />
Micropolysporum faeni + 100 µg/ml<br />
Key: w/v = weight/volume dilution; PNU = protein nitrogen units; IRU = immunoreactive units;<br />
• * = Greer allergen; + = Artuvetrin allergen<br />
TABLE 3<br />
Insect extracts used for equine intradermal skin testing, from Greer<br />
Allergen Concentration<br />
Mosquito (Culicidae) 1,000 PNU/ml<br />
Blackfly (Simulidae) 1,000 PNU/ml<br />
Horsefly (Tabanidae) 1,000 PNU/ml<br />
Culicoides spp 1/1,000 w/v<br />
1/10,000 w/v<br />
1/100,000 w/v<br />
Key: PNU = protein nitrogen units; w/v = weight volume dilution<br />
Horses were examined continuously for 30 minutes and the size <strong>of</strong> the positive and<br />
negative control wheals measured and recorded. Any wheals equal to or greater than<br />
the mean <strong>of</strong> the size <strong>of</strong> the control wheals were considered positive and diameters in<br />
millimetres recorded. Horses were examined again 4-6 hours later and note made <strong>of</strong><br />
any positive reactions (criteria as before, using the histamine diameter at the 30minute<br />
time point). These reactions were considered immediate positive reactions.<br />
The owner or groom examined the test site 24-36 hours later and the presence <strong>of</strong><br />
delayed reactions recorded and reported.<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 33
The incidence <strong>of</strong> positive results in the series <strong>of</strong> cases was as follows:<br />
Allergen Positive<br />
reactions<br />
34<br />
Allergen Positive<br />
reactions<br />
Ctenocephalides spp 7/24 (2) Weed pollens<br />
Tyrophagus putresceantiae 13/23 (2) Mugwort 5/24 (1)<br />
Acarus siro 9/22 (2) Wild brassica 5/24 (1)<br />
Dermatophagoides farinae 18/24 (4) Jerusalem oak 4/21<br />
D. pteronyssinus 19/24 (3) Lamb’s quarter 3/24<br />
Housedust 17/21 (2) Daisy 8/24<br />
Human dander 13/24 (2) Plantain 3/24<br />
Cat dander 3/24 (1) Sheep’s sorrel 2/24 (1)<br />
Sheep epithelia 8/24 Yellow dock 4 (1)<br />
Mixed feathers 9/24 (2) Dandelion 4/24 (2)<br />
Kapok 2/21 (1) Clover 8/21<br />
Tree pollens Nettle 6/24<br />
Birch 2/24 (1) Moulds<br />
Alder 2/24 (1) Alternaria alternata 2/24 (1)<br />
Hazel 3/24 (1) Aspergillus fumigatus 3/23 (1)<br />
Beech 3/24 (1) Botrytis cinerae 4/20 (1)<br />
Ash 2/24 (1) Cladosporium herbarum 5/23 (1)<br />
Sycamore 2/21 (1) Epicoccum purpurascens 5/20<br />
Poplar 5/24 (1) Fusarium moniliforme 4/20<br />
Oak 3/24 (1) Helminthosporium sativum 3/20<br />
Willow 3/24 Penicillium notatum 2/23<br />
Grass pollens Phoma betae 3/20<br />
Meadow grass 2/24 Pullularia pullulans 4/19 (1)<br />
Fescue 2/24 Rhodotorula rubra 2/20 (2)<br />
Cocksfoot 3/24 (1) Cereal smuts<br />
Bent-grass 2/24 (1) Barley smut 10/24 (2)<br />
Italian rye grass 4/21 (1) Oat smut 10/24 (2)<br />
Timothy 2/24 (1) Wheat smut 8/23 (2)<br />
Allergen Positive Allergen Positive<br />
reactions<br />
reactions<br />
Euroglyphus maynei 1/3 Grass pollens<br />
Dog dander * 2/3 Sweet vernal grass 0/3<br />
Tree pollens Yorkshire fog 0/3<br />
Horse chestnut 0/3 Perennial rye grass 0/3<br />
Elm 1/3 Couch grass 1/3<br />
Elder 1/3 Weed/flower pollens<br />
Privet 1/3 Ragweed 0/3<br />
Lime 1/3 Golden rod 0/3<br />
Moulds Wall pellitory 0/3<br />
Micropolysporum faeni+ 1/2<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005
Allergen Positive reactions<br />
Mosquito (Culicidae) 2/11<br />
Blackfly (Simulidae) 3/11<br />
Horsefly (Tabanidae) 2/11<br />
Culicoides spp 6/13<br />
10-fold dilution 6/13 (1)<br />
100-fold dilution 4/13<br />
Delayed reactions in parentheses and underlined<br />
All horses showed at least two immediate positive reactions; in some cases reactions<br />
were not evident until the 4-hour time point. Twelve horses showed delayed<br />
(>24hour) reactions, not necessarily preceded by immediate or late-immediate<br />
reactions. Two horses reacted to all allergens tested; in both cases the negative<br />
control did not produce a wheal reaction, nor did application <strong>of</strong> mechanical pressure,<br />
ruling out dermatographism as the cause <strong>of</strong> the multiple reactions. Reactions to mite<br />
extracts were common; only 2 horses (8.3%) showed no reactions to any mite<br />
species. Dust mite reactions were seen in 20/24 (83.3%); 58.3% reacted to both dust<br />
and forage mites, 25% to dust mites alone. Two horses reacted to forage mites but<br />
not dust mites. Housedust reactions were also common, occurring in 81% <strong>of</strong> cases.<br />
Reactions to epithelial extracts were also frequent; 54.2% reacted to human dander,<br />
33.3% to sheep and 12.5% to cats; in all <strong>of</strong> the latter cases t<strong>here</strong> were yard cats that<br />
had access to the stables and tack rooms and <strong>of</strong>ten slept on rugs or in the stables.<br />
Feather reactions were also quite common (37.5%), including two delayed reactions;<br />
two cases improved dramatically following removal <strong>of</strong> birds nests and preventing<br />
further access <strong>of</strong> birds, with complete resolution <strong>of</strong> skin disease without any other<br />
interventions.<br />
The majority <strong>of</strong> cases showed reactions to pollens; 10/24 (41.7%) did not. Weed<br />
pollen reactions were the most common - seen in 13 horses (54.2%), with nine<br />
(37.5%) having reactions to tree pollens and five (20.8%) to grasses. In a number <strong>of</strong><br />
cases the history suggested that exposure to grass and weed pollens in meadow hay<br />
were relevant. A few positive reactions to each <strong>of</strong> the moulds were noted. A<br />
considerable number <strong>of</strong> cases showed reactions to cereal smuts – 41.7% to barley<br />
smut, 41.7% to oat smut and 34.8% to wheat smut.<br />
Six horses developed immediate and delayed reactions to biting insects, particularly<br />
Culicoides. Horses with reactions to mosquito, blackfly and horsefly extracts were also<br />
positive to Culicoides. All <strong>of</strong> these cases had a history <strong>of</strong> clinical signs consistent with<br />
“sweet itch”, but all showed additional symptoms that were not typical <strong>of</strong> summer<br />
recurrent seasonal hypersensitivity. Together with two further cases that had<br />
consistent history and clinical signs but were not tested with insect extracts, these<br />
horses were considered to be suffering from both atopic dermatitis and insect bite<br />
hypersensitivity (33.3% <strong>of</strong> cases).<br />
Reference:<br />
Littlewood JD, Paterson S, & Shaw SC. (1998) Atopy-like skin disease in the horse. Advances<br />
in <strong>Veterinary</strong> Dermatology 3, p563<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 35
36<br />
Contact Atopy in Five Horses on the<br />
Same Property<br />
History and Presentation<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005<br />
Ken Mason<br />
Five <strong>of</strong> 20 horses on a single property had developed a pruritic dermatitis over<br />
several years. The affected horses were approximately 10 to 15 years old having been<br />
obtained as adults. The five were a grey Arab cross gelding, a bay thoroughbred<br />
gelding a grey Dartmoor cross pony mare and a mare and a gelding Percherons.<br />
The history indicated that the skin problem started in summer and progressed<br />
through till autumn then settled in winter to spring.<br />
Examination results<br />
All horses were in good condition and seemed well systemically. The clinical signs<br />
were <strong>of</strong> a very itchy dermatitis on the limbs and face only and seemed to show a<br />
water line effect below which primary lesions were erythema and macular papular<br />
eruptions and secondary lesions <strong>of</strong> self trauma causing exudative and bleeding<br />
abrasions and alopecia.<br />
Test results<br />
Intradermal skin testing with a panel <strong>of</strong> environmental allergens including typical<br />
insects found around horses on the grey Arab cross gelding revealed several grass<br />
and insect positive reactions. Scratch testing with parts <strong>of</strong> plants collected from the<br />
paddocks in which the horses grazed revealed positive immediate reactions to the<br />
pasture grasses kikuyu (Pennisetum clandestinum)and couch (Cynodon spp.) and billy goat<br />
weed (Ageratum houstonianum) but no reaction to sow grass (Paspalum conjugatum bergius)<br />
and broad leaf paspalum (Paspalum dilatum). Isolation <strong>of</strong> the horses into dirt floored<br />
yards( with no plants) adjacent to the grazing paddocks resulted in all skin signs<br />
disappearing. Returning the horses to the grazing paddocks caused return <strong>of</strong> the skin<br />
lesions.<br />
Discussion<br />
The grey Arab horse tested and reactive on test to kikuyu, couch and billy goat weed<br />
had lesions that corresponded to the height <strong>of</strong> these plants touching the limbs and<br />
face when the horse was feeding. One throughbreed not allergy tested had lesions
much higher and corresponded to the much taller sow grass. The owner reported<br />
that the horse refused to pass through patched <strong>of</strong> this grass when it was "seeding"<br />
and if forced to would stomp its feet and chew at the limbs w<strong>here</strong> the grass had<br />
touched the skin. Washing the limbs down and isolating the horse <strong>of</strong>f the paddock<br />
with this grass and broad leaf paspalum resulted in signs resolving.<br />
Thus it would seem that these horses had contact allergy to these pasture plants and<br />
that the other insect reactions and pollens to which it was positive on intradermal<br />
skin test were not related to the skin lesions, as the horses would have still been<br />
exposed to these environmental allergens while yarded adjacent to the grazing<br />
paddocks. The paddock plants suspected to be the cause due to positive allergy<br />
tested with a crude saline extract were only allergic when pollen and seed heads were<br />
developed in summer and autumn.<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 37
38<br />
Immunotherapy for Equine Atopic<br />
Dermatitis<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005<br />
Janet Littlewood<br />
Allergen-specific immunotherapy (ASIT) is widely used in small animal dermatology<br />
in the management <strong>of</strong> atopic dermatitis and in some countries for atopic humans.<br />
ASIT is indicated in in animals in which avoidance <strong>of</strong> allergens is not possible or is<br />
ineffective, w<strong>here</strong> signs are pesent for more than 4-6 months <strong>of</strong> the year, and drugs<br />
for symptomatic control are ineffective, or required at excessively high doses, or are<br />
contraindicated (Scott & Miller 2003). Since the author has had very few cases that<br />
fall into the above category, she has only limited personal experience with<br />
immunotherapy in the horse and this presentation will draw on published<br />
information.<br />
The mechanisms <strong>of</strong> action <strong>of</strong> immunotherapy are complex and the details <strong>of</strong> their<br />
action still poorly characterised. Various hypotheses put forward historically include<br />
humoral desensitisation (reduced IgE production), immunisation (blocking IgG<br />
antibodies), cellular desensitisation (reduced reactivity <strong>of</strong> mast cells and basophils,<br />
induction <strong>of</strong> tolerance (generation <strong>of</strong> allergen-specific suppressor cells) and<br />
combinations <strong>of</strong> the above. However, in patients with good clinical responses to<br />
immunotherapy vaccine, t<strong>here</strong> may be no decrease and even increases in IgE<br />
concentrations. Increased numbers <strong>of</strong> CD25+ T-suppressor lymphocytes has been<br />
shown to correlate with a favourable response, indicating that the major beneficial<br />
effect is cellular rather than humoral.<br />
T<strong>here</strong> is a scarcity <strong>of</strong> published studies demonstrating the efficacy <strong>of</strong> ASIT in horses<br />
in prospective, randomised, controlled trials, although a number <strong>of</strong> publications<br />
report the clinical benefits in retrospective case studies. Overall success rates that are<br />
reported are remarkably similar to those reported for ASIT in dogs and cats, with<br />
60-71% <strong>of</strong> cases having a good to excellent response, when therapy is based on<br />
intradermal testing. Most published reports have used aqueous allergens, with a<br />
variety <strong>of</strong> protocols used. Although t<strong>here</strong> are some theoretical objections raised to<br />
the use <strong>of</strong> alum-precipitated vaccines (potential to further stimulate Th 2 type <strong>of</strong><br />
response and enhanced IgE production) experience with small animals would<br />
suggest that these are not clinically relevant, with the only randomised, blinded,<br />
placebo-controlled trial <strong>of</strong> ASIT in atopic dogs using an alum-precipitated vaccine,
and this and other uncontrolled trials using alum-precipitated vaccine having very<br />
similar rates <strong>of</strong> success compared with aqueous vaccines (~60-70% <strong>of</strong> cases showing<br />
good to excellent/greater than 50% improvement).<br />
T<strong>here</strong> is controversy regarding the benefits <strong>of</strong> ASIT using insect extracts. A<br />
randomised, double-blinded, placebo-controlled clinical trial <strong>of</strong> ASIT for Culicoides<br />
hypersensitive horses involving 14 horses over a 6-month period demonstrated no<br />
difference between verum and placebo treated groups (Barbet 1990). However, a<br />
later Canadian open study conducted over 1-2 years with a crude Culicoides extract<br />
injected into 10 horses severely affected by disease resulted in a reduction <strong>of</strong> clinical<br />
signs in 9/10 (90%) in the first year. Of the eight horses treated during the second<br />
year, three were free <strong>of</strong> clinical signs at the end <strong>of</strong> the year(37.5%), three showed<br />
much less severe signs(37.5%), and two (25%) showed moderate reduction in clinical<br />
signs (Anderson et al 1996).<br />
In a retrospective study <strong>of</strong> 43 horses with allergic skin disease, <strong>of</strong> which 33 had been<br />
on immunotherapy for a minimum <strong>of</strong> 4 months the following data were reported<br />
(Rosenkrantz 1992): 10 horses showed pruritus only, 14 were urticarial and 9 had<br />
pruritus and urticaria. Good-to-excellent responses to ASIT were reported in 60% <strong>of</strong><br />
the pruritic horses, 71% <strong>of</strong> the urticaria cases and 66% <strong>of</strong> the horses with both<br />
urticaria and pruritus. Another study (Fadok 1996) showed that in horses that were<br />
purely atopic 5/7 (71.4%) were greater than 50% improved and 7/13 (53.8%)<br />
atopic and insect-allergic horses were greater than 50% improved, w<strong>here</strong>as 3 <strong>of</strong> 4<br />
(75%) insect-only allergic horses had no response to immunotherapy.<br />
A subsequent study <strong>of</strong> symptomatic horses with positive intradermal responses to<br />
insect and environmental allergens evaluated the efficacy <strong>of</strong> insect hyposensitisation<br />
compared to insect and environmental hyposensitisation in a double-blinded,<br />
placebo-controlled study (Rosenkrantz et al 1998). Clinical scores were ascribed for<br />
pruritus, excoriations, scale-crust and alopecia) ranging from 1-10 for affected<br />
regions <strong>of</strong> the body and mean scores ascribed. Cases were re-evaluated after 3<br />
months and those that had received placebo were allowed to receive verum<br />
treatment, and subsequently horses in the insect-only treatment group were<br />
permitted to convert to insect + environmental ASIT. Analysis <strong>of</strong> clinical scores<br />
after the initial 3 months treatment showed no statistically significant difference<br />
between the placebo and verum treated groups with either formulation <strong>of</strong><br />
immunotherapy. However, when the pre-treatment and post-treatment scores for<br />
individual horses were analysed, t<strong>here</strong> was a significant difference in verum treated<br />
animals compared to the placebo groups. Similarly, when the placebo groups were<br />
changed to verum treatments, statistically significant changes in scores were<br />
achieved. T<strong>here</strong> was no significance in changing from insect only to insect +<br />
environmental ASIT. Minor reactions characterised by swelling at the injection site<br />
was observed in six <strong>of</strong> 27 horses receiving ASIT, but all reactions subsided in 24-72<br />
hours.<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 39
Recommendations:<br />
Allergens should be selected on the basis <strong>of</strong> positive intradermal test responses,<br />
incorporating all those that appear to be relevant in view <strong>of</strong> the history and<br />
environmental exposure. In multiply allergic horses, more detailed information may<br />
be needed regarding likely presence <strong>of</strong> allergens in that individual's environment, the<br />
allergens know to be important in that geographical region, and the duration <strong>of</strong> the<br />
presence <strong>of</strong> the allergen. Cross-reactivity within groups <strong>of</strong> allergens may be utilised<br />
in making selections; cross-reactivity is likely in plants <strong>of</strong> the same genus and family.<br />
In general grasses are the most cross-reactive and weeds less so. Mould and<br />
arthropod allergens contain proteases that may have adverse effects on other<br />
allergens when used in combination, which may or may not affect the success <strong>of</strong><br />
hyposensitisation.<br />
Beneficial effects may be seen as early as 2-3 months into treatment, but may take as<br />
long as a year to achieve benefit. Intervals between maintenance injections can be<br />
tailored to the individual, according to the reappearance <strong>of</strong> clinical signs, varying<br />
between weekly to monthly. Frequency <strong>of</strong> injections may very at different times <strong>of</strong><br />
the year. In general, lifelong administration <strong>of</strong> vaccine is required. Adverse reactions<br />
are uncommon and usually mild. Reactions may include intensification <strong>of</strong> clinical<br />
signs for a few hours to a few days after injection, local injection site reactions<br />
(swelling +/- pain) and urticaria. Serious, anaphylactic reactions are extremely rare.<br />
Reactions are treated symptomatically. Exacerbation <strong>of</strong> clinical signs is an indication<br />
to reduce to dose <strong>of</strong> vaccine. Severely affected horses may need additional<br />
glucocorticoid therapy to control their symptoms, but low-dose alternate day<br />
prednisolone can be used in conjunction with ASIT, just as in small animal patients,<br />
and immunotherapy still be successful at controlling the disease, with lower doses <strong>of</strong><br />
steroids than were required before or even subsequent withdrawal <strong>of</strong> steroids.<br />
References:<br />
Anderson GS, Belton P, Jahren E, Lange H & Kleider N (1996) Immunotherapy<br />
trial for horses in British Columbia with Culicoides (Diptera: Ceratopogonidae)<br />
hypersensitivity. Journal <strong>of</strong> Medical Entomology 33, 458-66<br />
Barbet JL, Bevier D & Greiner EC. (1990) Specific immunotherapy in the treatment<br />
<strong>of</strong> Culicoides hypersensitive horses: a double blind study. Equine <strong>Veterinary</strong> Journal 22,<br />
232-5<br />
Fadok VA (1996) Hyposensitisation <strong>of</strong> Equids with allergic skin/pulmonary disease.<br />
Proceedings <strong>of</strong> the Annual Meeting <strong>of</strong> the American Academy and <strong>College</strong> <strong>of</strong> <strong>Veterinary</strong><br />
Dermatology , Las Vegas, Nevada p47<br />
Rees CA (2001) Response to immunotherapy in six related horses with urticaria<br />
secondary to atopy. Journal <strong>of</strong> the American <strong>Veterinary</strong> Medical Association 218, 753-5<br />
Rosenkrantz WS (1992) Therapy <strong>of</strong> equine pruritus. Proceedings <strong>of</strong> the 2 nd World Congress<br />
<strong>of</strong> <strong>Veterinary</strong> Dermatology Montreal, Canada p 435<br />
40<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005
Introduction<br />
Diagnostic Approach to Urticaria<br />
Reg Pascoe<br />
Horses show the greatest incidence <strong>of</strong> urticaria <strong>of</strong> all the species <strong>of</strong> domestic animals.<br />
Urticaria is a specific skin lesion rather than a specific disease entity. It has many<br />
different aetiologies and pathogenesis (Logas & Barbet 1999). Generally, it is discussed<br />
as a single entity even though its clinical manifestations vary from a minor transitory<br />
nature to major systemic life endangering problems.<br />
Aetiology / Pathophysiology<br />
The pathogenesis <strong>of</strong> equine urticaria is not well understood. Urticaria has been<br />
associated with immunological and nonimmunological mechanisms leading to the<br />
release <strong>of</strong> various mediators by mast cells. In a study by Rufnacht et al (2004) skin<br />
biopsies <strong>of</strong> 32 horses with a history <strong>of</strong> urticaria were stained with toluidine blue, a<br />
double-labelling method for chymase and tryptase, plus immunohistochemistry for<br />
immunoglobulin IgE. These horses were compared with horses with pemphigus<br />
foliaceus, insect bite hypersensitivity and control horses with healthy skin. Neither<br />
formalin fixation time nor biopsy site influenced the staining methods.No chymasepositive<br />
cells were found. In all groups <strong>of</strong> horses, cells staining with toluidine blue and<br />
for tryptase and IgE were found in the epidermis and hair follicle papilla and<br />
significantly more positively staining cells were observed in the subepidermal dermis<br />
compared with the deep dermis. Horses with urticaria had significantly more IgEbearing<br />
cells in the subepidermal dermis than control horses. However, horses with<br />
urticaria had significantly fewer toluidine-blue-stained mast cells in both subepidermal<br />
and deep dermis compared with the insect bite hypersensitivity and pemphigus<br />
foliaceus groups.<br />
This study supports IgE-mediated reactions play a role in the pathogenesis <strong>of</strong> urticaria.<br />
The use <strong>of</strong> intradermal testing (IDT) <strong>of</strong> urticaria and atopy also can be equivocal as<br />
Evans et al (1992) had found that positive results were also obtained from horses not<br />
showing signs <strong>of</strong> atopy. Further studies (Lorch et al 2001) have assisted in the<br />
elucidation <strong>of</strong> more <strong>of</strong> the quandary associated with IDT<br />
Many causes <strong>of</strong> urticaria have been suggested. (Scott & Miller 2003)<br />
1. Degranulation <strong>of</strong> mast cells and basophils is presumed to be the basic<br />
pathogenesis. Liberation <strong>of</strong> chemical mediators, which cause increased vascular<br />
permeability leads to wheal formation.<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 41
42<br />
2. Immunological: hypersensitivity w<strong>here</strong> antigen/allergen probably reaches the<br />
skin via the systemic route rather than by local contact. The antigen reaches the<br />
systemic circulation mechanisms involved include type 1 and 111<br />
hypersensivity reactions<br />
• Injection (drugs such as some antibiotics, BTZ, Ivermectin, Moxidexin,<br />
pethidine, Vit B complex, flunixen, iron dextran and many others)<br />
• Ingestion (chemical, feeds pasture plants)<br />
• Inhalation (pollen, dust, chemicals, moulds)<br />
• Vaccines (strangles, botulism, salmonella, tetanus etc)<br />
• Transfusion reactions<br />
• Biting insects (biting flies, mosquitoes, blackflies,bees, wasps, spiders etc)<br />
• Infections (bacterial, fungal, viral parasites such as onchocerciasis, habronemiasis,)<br />
• Vasculitis (streps, purpura haemorrhagica)<br />
3. Allergic urticaria:<br />
• Atopy<br />
• Drug related<br />
• Food allergy<br />
• Inhaled antigens, pollens, moulds<br />
• Contact allergy (very rare); must be carefully distinguished from allergic contact<br />
dermatitis.<br />
4. Physical urticaria, non-immunological pathogenesis.<br />
• Dermatographism: wheal developing from blunt scratch on skin<br />
• Cold urticaria, heat and light<br />
• Exercise induced urticaria<br />
Clinical Presentation<br />
T<strong>here</strong> is no breed, age or sex predilection. Onset can be peracute to acute with signs<br />
developing within minutes up to a few hours and usually resolve in 24-48 hours<br />
occasional signs can last up to 6-8 weeks. Or in the instance <strong>of</strong> recurrent urticaria it<br />
may be chronic or persistent if present for more than 8 weeks<br />
Lesions<br />
An oedematous lesion <strong>of</strong> the skin or mucous membrane is called a wheal, which is a<br />
flat topped papule/nodule with steep walled sides which pits on pressure. Some have<br />
slightly depressed centres.<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005
Wheals vary in size and shape and quite arbitrarily may be divided into:<br />
1. Conventional: 2-3mm up to 3-5mm.<br />
2. Papular: multiple small uniform 3-6mm diameter wheals i.e. insect bites.<br />
3. Giant: either single or coalesced multiple wheals up to 20-30cm diameter.<br />
4. Annular: donut like lesions.<br />
The lesion may present differently depending on the location <strong>of</strong> the oedema i.e.<br />
whether it is in the upper layers <strong>of</strong> the dermis or subcutaneous and may be pruritic or<br />
non pruritic.<br />
1. "Oozing urticaria" - w<strong>here</strong> dermal oedema is severe, oozing <strong>of</strong> serum from<br />
the skin surface may occur. Care should be taken to distinguish this from an<br />
erosive/ulcerative process or a pyoderma. NB lesion must still pit on pressure.<br />
2. Gyrate urticaria - has been referred to as the dermal form <strong>of</strong> erythema<br />
multiforme but it should be stressed that this syndrome is not related to 'true'<br />
erythema multiforme which is primarily an epidermal disease (lesions DO NOT<br />
pit on pressure). Drug reactions appear to be the most common cause <strong>of</strong> this<br />
form <strong>of</strong> urticaria.<br />
3. Angiooedema (Angioneurotic oedema) - a subcutaneous form <strong>of</strong> urticaria<br />
which tends to be more diffuse due to lack <strong>of</strong> restraint to spread in the sub<br />
cutis. Usually involves the head and extremities and is more indicative <strong>of</strong> a<br />
systemic and serious disease than urticaria.<br />
Diagnosis<br />
Because <strong>of</strong> the numerous potential causes <strong>of</strong> urticaria a definitive diagnosis may only be<br />
reached after extensive clinical and diagnostic investigation which can be time<br />
consuming, expensive and <strong>of</strong>ten unrewarding. Horse owners usually are reluctant to<br />
undertake the costly task <strong>of</strong> endeavouring to obtain an accurate diagnosis.<br />
Initially, diagnosis is mostly based on clinical signs (mostly cutaneous reaction patterns)<br />
and a careful history <strong>of</strong> the case. (Scott & Miller 2003)<br />
History is important:<br />
- Is it the first attack?<br />
- If not, how many and are they seasonal?<br />
- Site <strong>of</strong> lesions- is it a point <strong>of</strong> contact with gear?<br />
- Use <strong>of</strong> any drugs, frequency and reaction at time <strong>of</strong> use, drenches,<br />
medicated sprays, ointments, shampoos, ultrasound gel. Etc<br />
- Pasture plants<br />
Specific activities-exercise only induced<br />
Being worked, (confirm by 30 min exercise producing urticaria) out<br />
in paddock for pick <strong>of</strong> grass<br />
- Food allergy can only be traced by elimination diets and then<br />
challenge with suspected feed ( very time consuming with NO short<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 43
44<br />
cuts)<br />
- Heat: over rugging to cause higher than normal body heat and poor<br />
loss <strong>of</strong> retained heat e.g. Show horses over rugged to induce hair<br />
changes<br />
- Cold: ‘Cold' urticaria: use ice cube - oedema in 15 minutes<br />
- Pressure induced-dermatographism by coarse instrument: scratch,<br />
wheals appear in
References<br />
Evans AG, Paradis MR & O’Callaghan M (1992) Intradermal testing <strong>of</strong> horses with<br />
chronic obstructive pulmonary disease and recurrent urticaria.<br />
American Journal <strong>of</strong> <strong>Veterinary</strong> Research 53: 203–8.<br />
Logas DB & Barbet JL (1999) Inflammatory, infectious and immune disease. In:<br />
Colahan PT, Merritt AM, Moore JN eds. Equine Medicine and Surgery. St. Louis,<br />
MO: Mosby Year Book 1999, 1868–73.<br />
Lorch G, Hillier A, Kwochka KW. Saville WA & Le Roy BE (2001) Results <strong>of</strong><br />
intradermal tests in horses without atopy and horses with atopic dermatitis or<br />
recurrent urticaria. American Journal <strong>of</strong> <strong>Veterinary</strong> Research; 62: 1051–9.<br />
Rüfenacht S, Marti E, Von Tscharner C, Doherr MG, Forster U, Welle M & Roosje<br />
PJ (2005) Immunoglobulin E-bearing cells and mast cells in skin biopsies <strong>of</strong> horses<br />
with urticaria <strong>Veterinary</strong> Dermatology 16, 94–101<br />
Scott DW & Miller WH (2003) Equine Dermatology Elsevier Science (USA)<br />
Philadelphia PA .USA<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 45
Erythema multiforme<br />
Rare, acute, self-limiting, urticarial, maculopapular or vesico-bullous dermatosis. Other<br />
triggering influences such as drugs, infections (especially Herpes virus), and tumours -<br />
especially lymphoreticular neoplasms. Many cases are classified as idiopathic.<br />
Aetiology / Pathophysiology<br />
Can be considered a type <strong>of</strong> allergic response, being very similar to graft versus host<br />
reaction.<br />
Clinical presentation<br />
Lesions tend to have a symmetrical distribution. Asymptomatic cutaneous eruptions.<br />
Characteristic 'donut like' skin urticarial lesions develop rapidly from initial urticaria and<br />
plaques. Occasionally involves mucous membranes <strong>of</strong> mouth. Persist from days to<br />
weeks. No scaling, crusting or alopecia in many horses. These plaques do not pit on<br />
pressure<br />
Differential diagnosis<br />
Urticaria, amyloidosis, mastocytoma, lymphosarcoma, fixed drug reaction, toxic<br />
epidermal necrolysis.<br />
Diagnosis<br />
Skin biopsy.<br />
Management<br />
Runs benign course over 2-3 months. Recurrence reported in some cases.<br />
Prognosis<br />
Guarded to poor for permanent recovery.<br />
46<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005
Introduction:<br />
Equine Chronic Urticaria<br />
Greg Burton<br />
Urticaria (hives) are relatively common in horses. Chronic urticaria is an ill-defined<br />
syndrome in the horse w<strong>here</strong>by transient urticarial eruptions occur in a recurrent<br />
fashion over a period <strong>of</strong> greater than 6 to 8 weeks. Chronic urticaria in people is<br />
more clearly defined as urticarial eruptions that occur at least twice weekly for greater<br />
than 6 weeks.<br />
Pathogenesis:<br />
The pathogenesis is poorly understood. Both immunological and nonimmunological<br />
mechanisms are considered likely. The major effector cell is likely to<br />
be the mast cell however basophils, mononuclear cells, platelets and endothelial cells<br />
may also play a role. Increased IgE bearing cells have been identified in skin<br />
biopsies <strong>of</strong> horses with urticaria.<br />
Potential triggers<br />
- type 1 and type III hypersensitivity reactions (atopy, adverse food<br />
reactions, contact reactions, arthropod bites, parasites)<br />
- physical triggers (sunlight, pressure, heat, cold and exercise)<br />
- psychological stress<br />
- drugs (ivermectin, various antibiotics, NSAIDs)<br />
- idiopathy<br />
Clinical features:<br />
T<strong>here</strong> is no reported age, breed or sex predisposition in horses with urticaria.<br />
Urticarial lesions appear suddenly, are <strong>of</strong>ten generalised and somewhat symmetrical,<br />
are associated with variable pruritus and usually not associated with oozing <strong>of</strong> serum<br />
or haemorrhage. They are variable sized from a few millimetres to several<br />
centimetres with sharply demarcated edges and flat tops. The lesions are not painful,<br />
have normal body temperature and pit on pressure. They are effervescent and<br />
resolve within 24 hours. A clinical classification exists and may have some<br />
aetiological significance.<br />
I. Conventional urticaria: papules and wheals <strong>of</strong> 2-5mm diameter<br />
II. Papular urticaria: uniform 3-6mm papules and <strong>of</strong>ten associated with<br />
insect bites, especially mosquitoes<br />
III. Giant urticaria: up to 40cm diameter<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 47
48<br />
IV. Exudative urticaria: associated with serum oozing and matting <strong>of</strong> the<br />
hair and hair loss.<br />
V. Gyrate urticaria: bizarre serpiginous and arciform shapes and <strong>of</strong>ten<br />
associated with drug reactions.<br />
Differential diagnoses:<br />
- folliculitides<br />
- vasculitis<br />
- erythema multiforme<br />
- cutaneous infiltrates (amyloidosis, neoplasia)<br />
-<br />
Diagnosis:<br />
History<br />
- record <strong>of</strong> client observations (seasonality, drug exposure, feeds, housing,<br />
environment, association with exercise)<br />
- Duration <strong>of</strong> the lesions<br />
- Location <strong>of</strong> the lesions (contact sites?)<br />
- Grooming protocol<br />
- Parasite control<br />
A thorough history should allow you to rule in/out drugs, parasitism, infections and<br />
give clues as to the likelihood <strong>of</strong> physical urticaria.<br />
Diagnostic tests<br />
Treatment:<br />
- Permanent marking pen to assess persistence <strong>of</strong> individual lesions<br />
- Histopathology for lesions that persist greater than 24 hours (infiltrative<br />
urticaria, vasculitis)<br />
- Assess for dermatographism (blunt pressure applied and observe for<br />
wheal formation)<br />
- Local application <strong>of</strong> heat (water > 44 o C) or cold (ice cube)<br />
- Exercise challenge<br />
- IDT (intradermal skin testing for airborne allergens)<br />
- Hymenoptera testing<br />
- Novel protein hypoallergenic diet 6 to 8 weeks<br />
- Avoidance <strong>of</strong> triggers if identified<br />
- Trigger “desensitisation”<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005
Acute treatment<br />
- Epinephrine 1:1000, 5 to 10 mls/450kg IM (given acutely)<br />
- Prednisolone 2mg/kg (given acutely)<br />
Chronic treatment<br />
Conclusion:<br />
- ASIT (allergen specific immunotherapy)<br />
- Antihistamines (hydroxyzine 400-500mg bid +/-cyproheptadine 20mg<br />
bid)<br />
Most common cause, once drugs are ruled out, is atopic dermatitis. Further<br />
elucidation <strong>of</strong> ideal concentration <strong>of</strong> allergens for IDT in the horse would lead to<br />
greater utilisation <strong>of</strong> IDT as a diagnostic step and ASIT as a therapeutic option for<br />
chronic urticaria in the horse.<br />
.<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 49
50<br />
Management <strong>of</strong> the Atopic Horse<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005<br />
Janet Littlewood<br />
Once a diagnosis <strong>of</strong> atopic dermatitis has been made in any companion animal, the<br />
various therapeutic options available need to be considered and discussed with the<br />
client. As with any hypersensitivity condition, allergen avoidance is the ideal solution,<br />
but this may not be achievable, depending on the trigger factors implicated. Other<br />
therapeutic approaches include hyposensitisation (immunotherapy), other<br />
immunomodulatory approaches and symptomatic ant-inflammatory and anti-pruritic<br />
treatments.<br />
Allergen avoidance:<br />
For horses with clinical disease related to indoor allergens, maintaining the horse at<br />
pasture all the year round is the ideal solution. However, for horses with pollen<br />
allergies and insect bite hypersensitivity, keeping the horse stabled for the majority <strong>of</strong><br />
the time is more appropriate. Treatment <strong>of</strong> horses with insect bite hypersensitivity<br />
will be covered in a later presentation and will not be addressed further in this<br />
presentation. Those patients with both indoor and outdoor allergens implicated in<br />
their disease process are the most challenging in terms <strong>of</strong> allergen avoidance.<br />
Nonetheless, it is possible with management modification to reduce allergen<br />
exposure in the indoor environment, which, in the author's experience, can be very<br />
effective in controlling the disease in many patients.<br />
Management measures that are recommended include housing the horse in a stable<br />
with its own air space, but with good ventilation, not underneath or next to a<br />
hay/grain l<strong>of</strong>t or store, removal <strong>of</strong> birds nests, removal <strong>of</strong> all loose bedding,<br />
vacuuming and pressure cleaning <strong>of</strong> the stable interior on a regular basis. Rubber<br />
matting is the ideal flooring, with no loose bedding at all, since even “low allergen”,<br />
dust-free beddings may provide a suitable micro-environment for dust and storage<br />
mite species. This flooring is well tolerated by even the largest horses, although<br />
owners tend to anthropomorphise about the comfort <strong>of</strong> their horse!<br />
Feeding <strong>of</strong> low allergen foods may also be helpful – such as vacuum-packed wilted<br />
grass products, or blow-dried (dust-free) ley-grown hay, and cubed rather than loose<br />
grain concentrate foods.<br />
For horses with reactions to dust mite species that show lesions on the skin under<br />
rugs, presumably due to mites living in the rugs/horse duvets, the author has had
anecdotal success with use <strong>of</strong> human dust mite-pro<strong>of</strong> bedding covers, for example<br />
using a dust mite-pro<strong>of</strong> mattress cover or duvet cover next to the horse's skin,<br />
underneath the other rugs. This has been beneficial in cases that persisted with<br />
lesions in spite <strong>of</strong> regular laundering <strong>of</strong> rugs.<br />
Immunotherapy:<br />
Immunotherapy is indicated for horses that are not adequately controlled by allergen<br />
avoidance measures and for those that have pollen reactions, unless they are to<br />
plants with a very narrow pollination season, w<strong>here</strong> symptomatic treatment may be<br />
more appropriate. Allergen selection for formulation <strong>of</strong> vaccine requires making<br />
judgements about which positive intradermal reactions are clinically significant and<br />
whether or not to include insect extracts in a vaccine. The author's practice is to<br />
recommend allergen avoidance measures in the first instance – both environmental<br />
and insect control – and to consider immunotherapy in those patients w<strong>here</strong> t<strong>here</strong> is<br />
still significant ongoing clinical disease.<br />
Immunomodulatory approaches other than allergen-specific are under active<br />
development, utilising naturally occurring, bacterial-derived, immunomodulators to<br />
down-regulate T-helper 2 and optimise T-helper 1 mechanisms. Extracts under<br />
investigation contain immunomodulators that occur in the bacterial cell wall,<br />
bacterial heat-shock proteins that share homology with mammalian mitochondrialderived<br />
stress proteins and bacterial sugars related to innate immunity and to the<br />
bacteriomimetic sugars presented on the surfaces <strong>of</strong> rapidly replicating mammalian<br />
cells, such as those <strong>of</strong> neoplasms and inflammatory responses.<br />
T<strong>here</strong> is in the UK a clinical trial underway, under a VMD test certificate, <strong>of</strong> a<br />
bacterial-derived product in horses with a clinical diagnosis <strong>of</strong><br />
Culicoides hypersensitivity. Two hundred susceptible horses are recruited to the trial,<br />
which is running over this year and into next year, with both open and randomised<br />
elements to the trial. No data will be available until later this year, but in a small<br />
placebo-controlled pilot trial the product has been demonstrated to statistically<br />
significantly reduce the severity <strong>of</strong> disease. Future results are awaited with interest.<br />
Glucocorticoids:<br />
Severely affected horses, particularly those with marked pruritus and those with<br />
chronic changes related to insect bite hypersensitivity, may well need systemic steroid<br />
therapy. T<strong>here</strong> are <strong>of</strong>ten concerns about the risks <strong>of</strong> steroid therapy in horses, but at<br />
the anti-inflammatory dose rates required for allergic patients the risks are<br />
considered very low, unless t<strong>here</strong> is a history <strong>of</strong> laminitis.<br />
Prednisolone is the author's drug <strong>of</strong> choice, given orally at an initial dose rate <strong>of</strong> 0.5-<br />
1mg/kg/day. Daily therapy used continued until the clinical signs are controlled,<br />
usually within 1-2 weeks, then reduced to alternate day therapy, with gradual tapering<br />
<strong>of</strong> the dose to the lowest possible maintenance dose as long as is needed. This<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 51
usually ends up in the range <strong>of</strong> 0.2-0.5mg/kg every other day. The author has had no<br />
problems dropping from the initial once daily dose to the same dose on alternate<br />
days for atopic horses (in contrast to patients with immune mediated disease). Some<br />
clinicians prefer to use an initial parenteral dose <strong>of</strong> dexamethasone – 0.02-0.1mg/kg;<br />
oral dexamethasone can be administered t<strong>here</strong>after, in the dose range <strong>of</strong> 0.01-<br />
0.02mg/kg every 2-3 days.<br />
In addition to laminitis, the other side effect concerns would be potentiation <strong>of</strong><br />
existing infections or increased susceptibility to infection, particularly opportunistic<br />
respiratory infections. At the doses required for management <strong>of</strong> most allergic horses,<br />
this does not present a big problem in the experience <strong>of</strong> the author.<br />
Antihistamines:<br />
Drugs that block the cellular receptors for histamine may be utilised in allergic<br />
horses. In the UK t<strong>here</strong> are no veterinary licensed antihistamines, but human<br />
products are used <strong>of</strong>f-label. The drug used most commonly by equine practitioners is<br />
hydroxyzine hydrochloride; doses <strong>of</strong> 0.5 -1.5mg/kg every 8-12 hours are suggested<br />
in the literature. Others that may be used in the horse are chlorpheniramine<br />
0.25mg/kg every 12 hours and diphenhydramine 0.75-1mg/kg every 12 hours.<br />
Doxepin hydrochloride is a tricyclic antidepressant with H1-receptor blocking<br />
effects and has been reported to be useful in some pruritic horses at dose rates <strong>of</strong><br />
0.5-0.75mg/kg every 12 hours.<br />
Antihistamines may be more effective for cases <strong>of</strong> urticaria than pruritus. Although<br />
the systemic side effects <strong>of</strong> antihistamines may be <strong>of</strong> less concern than for steroids,<br />
sedation and personality changes may occur and these drugs are not permitted in<br />
horses competing under certain regulatory authorities. Recommended withdrawal<br />
times should be checked with the relevant bodies for competition horses.<br />
Essential Fatty Acid supplementation:<br />
Administration <strong>of</strong> essential fatty acids (EFAs) has received a lot <strong>of</strong> attention in the<br />
field <strong>of</strong> small animal dermatology with many publications endorsing the benefits <strong>of</strong><br />
various combinations <strong>of</strong> omega 3 and omega 6 fatty acids at various dose rates in the<br />
management <strong>of</strong> allergy in both cats and dogs. These products may modify the<br />
arachidonic acid inflammatory cascade, diverting pathways away from the<br />
production <strong>of</strong> pro-inflammatory eicosanoids (prostaglandins, thromboxanes,<br />
leukotrienes) and leading to production <strong>of</strong> less inflammatory or inhibitory mediators<br />
such as PGE1. LTB5, PG-2 series, TxA3 and hydroxyeicosapentanoic acid (HEPE).<br />
EFAs also have been shown to optimise skin barrier function in dogs and have been<br />
shown to have an additive effect with antihistamines and a significant steroid-sparing<br />
effect in atopic dogs.<br />
T<strong>here</strong> are a small number <strong>of</strong> publications concerning the use <strong>of</strong> EFAs in horses. An<br />
open study <strong>of</strong> 14 horses with insect bite hypersensitivity that were given 20g daily <strong>of</strong><br />
52<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005
an 80:20 mixture <strong>of</strong> evening primrose oil and cold water marine fish oil for a<br />
minimum <strong>of</strong> 3 months gave promising results, with 4 horses better and 5 horses<br />
much better than at the beginning <strong>of</strong> the study and 4 horses no better. However, the<br />
double-blind placebo controlled trial subsequently conducted failed to demonstrate<br />
any significant reduction in disease in the treated group (Craig et al 1997). Similar<br />
results were obtained in a double-blinded cross-over study with omega-3 fatty acid<br />
supplementation (Friberg and Logas 1999). However, a more recent study <strong>of</strong><br />
flaxseed supplementation in horses with Culicoides hypersensitivity reported reduced<br />
skin test reactivity, concurrent with a significant decrease in the hair content <strong>of</strong> longchain<br />
fatty acids (O'Neill et al 2002).<br />
In spite <strong>of</strong> the lack <strong>of</strong> supportive controlled data in horses, many clinicians feel that<br />
EFA supplementation is beneficial in some horses. The product DVM Derm Caps<br />
100s given at doses <strong>of</strong> 1capsule per 50-100kg bodyweight is reported to be well<br />
tolerated and effective in some horses.<br />
Botanical extracts:<br />
The use <strong>of</strong> plant and herb extracts in the management <strong>of</strong> canine atopic dermatitis<br />
has received attention over recent years, with the development <strong>of</strong> a product<br />
containing three plant extracts, derived from tradition Chinese remedies for human<br />
atopic eczema (Phytopica). Whilst the author is unaware <strong>of</strong> any published data <strong>of</strong><br />
trials <strong>of</strong> plant extracts in the management <strong>of</strong> allergic horses, t<strong>here</strong> is anecdotal<br />
evidence <strong>of</strong> the benefits <strong>of</strong> oral administration <strong>of</strong> aloe vera liquid extract - doses <strong>of</strong><br />
150ml per horse per day suggested.<br />
Topical therapies:<br />
Regular bathing <strong>of</strong> atopic and insect-bite hypersensitive horses can be very helpful in<br />
alleviating and ameliorating clinical signs. Products which may be useful include<br />
colloidal oatmeal shampoos, either alone or in combination with other “soothing”<br />
products such as aloe vera extract. Moisturisers can also be helpful. For localised<br />
lesions witch hazel sprays and aloe vera gel extracts can be beneficial. In cases with<br />
secondary infection and/or secondary seborrhoea, t<strong>here</strong> are products with antiseptic<br />
properties (chlorhexidine, chloroxylenol, ethyl lactate, benzoyl peroxide) and<br />
keratoplastic properties (salicylic acid, tars, benzoyl peroxide) that may be<br />
appropriately utilised.<br />
Author's experience:<br />
The outcome in the series <strong>of</strong> 24 cases discussed previously (Littlewood et al 1998)<br />
serves to illustrate the author's personal experience in the management <strong>of</strong> equine<br />
atopic dermatitis. Advice was given regarding changes to management and feeding<br />
practices in an attempt to avoid or limit exposure to implicated allergens, with<br />
additional advise regarding insect avoidance w<strong>here</strong> appropriate. W<strong>here</strong> management<br />
changes were insufficient to secure resolution or adequate improvement in clinical<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 53
signs antihistamines (hydroxyzine hydrochloride at an initial dose <strong>of</strong> 300 mg twice<br />
daily) were given by mouth or oral prednisolone at a dose rate <strong>of</strong> 1 mg/kg initially<br />
daily, reducing to alternate day therapy.<br />
Follow-up information was obtained for all except one case. Two horses died shortly<br />
after referral before any response to management alterations could be assessed.<br />
Progress reports were obtained initially one and three months after referral and<br />
subsequently at various intervals for up to four years. All cases improved<br />
considerably after management alterations that were recommended on the basis <strong>of</strong><br />
the history and positive skin test reactions had been implemented. Drug therapy was<br />
necessary in only six cases. In four cases oral antihistamines were employed<br />
intermittently when the pruritus or urticaria were severe, <strong>of</strong>ten coincident with<br />
pollination times. A fifth was treated with antihistamines initially, but therapy was no<br />
longer required after a major change <strong>of</strong> management. Low dose steroid therapy was<br />
given to the sixth case initially, due to the severity <strong>of</strong> the urticaria and angioedema.<br />
Major management changes were not possible and this horse required ongoing<br />
intermittent administration <strong>of</strong> antihistamines because <strong>of</strong> recurrent urticaria, although<br />
he remained asymptomatic most <strong>of</strong> the time. The respiratory problem in this case<br />
has also persisted and worsened.<br />
The author has used immunotherapy in only a handful <strong>of</strong> cases, w<strong>here</strong> it has been<br />
felt to be <strong>of</strong> benefit, but the results <strong>of</strong> management modification are usually<br />
sufficient to control the problem sufficiently that clients rarely request<br />
immunotherapy.<br />
References:<br />
Craig JM et al (1997) A double-blind placebo-controlled trial <strong>of</strong> an evening primrose<br />
and fish oil combination versus hydrogenated coconut oil in the management <strong>of</strong><br />
recurrent seasonal pruritus in horses. <strong>Veterinary</strong> Dermatology 8, 177<br />
Fiberg CA & Logas D. (1999) Treatment <strong>of</strong> Culicoides hypersensitive horses with<br />
high-dose N-3 fatty acids: a double-blinded crossover study. <strong>Veterinary</strong> Dermatology 10,<br />
117.<br />
Littlewood JD, Paterson S, & Shaw SC. (1998) Atopy-like skin disease in the horse.<br />
Advances in <strong>Veterinary</strong> Dermatology 3, p563<br />
O'Neill W, McKee S & Clarke AF (2002) Flaxseed (Linum usitatissimum)<br />
supplementation associated with reduced skin test lesional area in horses with<br />
Culicoides hypersensitivity. Canadian Journal <strong>of</strong> <strong>Veterinary</strong> Research 66, 272-7<br />
54<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005
Clinical approach to the horse with<br />
pastern dermatoses<br />
Janet Littlewood<br />
Crusting and scaling lesions affecting the skin <strong>of</strong> the distal limb <strong>of</strong> horses presents a<br />
diagnostic and therapeutic challenge to the equine practitioner and dermatologist<br />
alike. The use <strong>of</strong> various colloquial descriptive terms such as “greasy heel”,<br />
“scratches” and “mud fever”, which horse owners frequently view as a definitive<br />
diagnosis, further serves to confuse the issue. At best, these terms should be viewed<br />
as describing a clinical syndrome, for which t<strong>here</strong> are a number <strong>of</strong> underlying<br />
aetiologies. Whilst empirical remedies may be effective in managing such cases, a<br />
significant number fail to respond to such therapies and can cause frustration to<br />
client and clinician alike, as well as being a significant welfare problem to the patient<br />
in some instances. The efforts <strong>of</strong> the attending clinician should be directed towards<br />
identifying underlying predisposing factors and pathogens and implementing specific<br />
therapy to eliminate the problem. Appropriate samples taken at the outset will<br />
minimise the risk <strong>of</strong> a chronic, recurrent skin problem whose features may be<br />
changed by the intervening therapy, making it harder to reach a definitive diagnosis<br />
later. The client is more likely to be impressed by attempts to make a proper<br />
diagnosis at the outset, so that correct treatment can be initiated and, hopefully,<br />
resolution achieved sooner.<br />
T<strong>here</strong> are a number <strong>of</strong> factors that may predispose to grease heel syndrome,<br />
including genetic factors such as presence <strong>of</strong> feathers in heavy breeds and nonpigmented<br />
skin; environmental factors such as moisture, prevailing climate and<br />
management practices; and iatrogenic factors including tack items and topical<br />
preparations, which are frequently utilised by horse owners. Primary causes <strong>of</strong> grease<br />
heel syndrome include physical and chemical irritants and infectious agents such as<br />
mites and dermatophytes. The extremities may be affected by extreme cold<br />
(frostbite) and ultraviolet light exposure may result in photodermatoses in nonpigmented<br />
limbs. Bacterial infection is common in grease heel syndrome, but<br />
whether this represents a true primary pyoderma or, as in the dog, a secondary<br />
phenomenon, is not clear. Progressive pathology with fibrosis is a particular problem<br />
<strong>of</strong> diseases <strong>of</strong> the distal equine limb and chronic lesions may be characterised by<br />
irreversible changes.<br />
The differential diagnosis for crusted papules, <strong>of</strong>ten with “paintbrush” tufting or<br />
matting <strong>of</strong> hair, includes dermatophilosis, dermatophytosis and staphylococcal<br />
(pastern) folliculitis. Cytological preparations are invaluable and are <strong>of</strong>ten diagnostic<br />
in acute, exudative lesions, with causal organisms identifiable in impression smears<br />
<strong>of</strong> underside <strong>of</strong> scabs or crusts. Bacterial and/or fungal culture are helpful in<br />
identifying actual species involved, although it should be noted that Dermatophilus<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 55
congolensis is not easy to isolate, particularly from older, longstanding lesions.<br />
However, typical organisms may be seen in wet preparations made from crusts after<br />
rehydration and maceration on slides, prior to staining. Dermatophilosis is <strong>of</strong>ten a<br />
problem <strong>of</strong> a number <strong>of</strong> horses in a yard and may be endemic, with increased<br />
numbers <strong>of</strong> affected animals noted in the winter months. The spores are persistent<br />
in the environment and careful attention to management practices is an important<br />
part <strong>of</strong> control measures. Ideally an area should be set aside for topical treatment <strong>of</strong><br />
affected animals and crusts carefully disposed <strong>of</strong> and the area disinfected. Systemic<br />
antibiotic therapy is usually effective in cases not responding to topical antibacterial<br />
agents, but should be continued beyond clinical cure.<br />
Dermatophytosis can be caused by a number <strong>of</strong> fungal organisms. Identification <strong>of</strong><br />
the causal agent may be helpful in identifying the original source (other horses, cattle,<br />
cats, sylvatic species, geophilic). T<strong>here</strong> is also a zoonotic risk to be considered. Scalp<br />
brushes provide a useful tool for sampling animals for culture, equivalent to the<br />
Mackenzie toothbrush technique employed in small animals. Management <strong>of</strong> this<br />
condition is covered later.<br />
Pastern folliculitis may be a primary pyoderma, but mixed growth <strong>of</strong> organisms is<br />
frequently obtained on swabs. Tissue samples obtained by biopsy may well be a<br />
better material for culture and provide a truer picture <strong>of</strong> the major pathogen<br />
involved. However, cytological examination <strong>of</strong>ten provides sufficient information to<br />
initiate antibacterial therapy. Management <strong>of</strong> bacterial folliculitis is the subject <strong>of</strong> a<br />
later presentation.<br />
Chorioptic mange is the major parasitic cause <strong>of</strong> skin lesions <strong>of</strong> the distal limb. The<br />
parasite exhibits a preference for heavy breeds <strong>of</strong> horse. An epidemiological study<br />
conducted by the author has shown that the presence <strong>of</strong> feathers is not a<br />
prerequisite, but the actual nature <strong>of</strong> the nutritional or other factors provided by<br />
such horses is unknown. Management <strong>of</strong> this condition is covered later.<br />
Harvest mite larvae (“chiggers”) can parasitise the lower limbs <strong>of</strong> horses grazed on<br />
pastures inhabited by the free-living adult mites or ridden through infested woods or<br />
trails. The larval stage requires a blood meal and any convenient mammal may be<br />
bitten. The larva is only attached for 48-72 hours, but in some horses lesions <strong>of</strong><br />
pruritus, crusting, erythema and scaling may persist beyond detachment <strong>of</strong> the<br />
parasite, suggesting a hypersensitivity component to the lesions. Fipronil has been<br />
demonstrated to be effective in the management <strong>of</strong> trombiculidiasis in dogs, and<br />
would be appropriate for the condition in equine patients too, as an <strong>of</strong>f-label use.<br />
Photosensitivity may affect the distal limbs <strong>of</strong> horses with white socks. The cause<br />
may be due to ingestion <strong>of</strong> primary photosensitising agents, such as hypericin in<br />
Hypericum spp. <strong>of</strong> plants (St John’s Wort). Photocontact dermatitis may occur. In the<br />
case <strong>of</strong> primary photocontact or systemic photosensitisation, one would expect<br />
several <strong>of</strong> a group <strong>of</strong> horses to be affected, although photoallergic reactions may<br />
occur, which would be limited to sensitised individuals. Often it is difficult to<br />
56<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005
identify plants in a pasture that might be implicated. It has been observed that some<br />
pastures rich in clover may be associated with cases <strong>of</strong> photodermatitis in some<br />
seasons, possibly associated with high rainfall and lush growth, but the exact nature<br />
<strong>of</strong> the agent remains obscure. Secondary, hepatogenous, photosensitisation occurs<br />
when pre-existing liver damage results in failure to metabolise chlorophyll effectively<br />
and presence <strong>of</strong> photoactive phylloerythrin in the circulation. The commonest cause<br />
<strong>of</strong> chronic liver damage in such cases is poisoning resulting from ingestion <strong>of</strong> Seneccio<br />
spp (ragwort), but mycotoxins have also been implicated. The prognosis for cases<br />
with underlying liver pathology is poor, but cases <strong>of</strong> primary photodermatitis<br />
respond to removal from the source <strong>of</strong> photoactive agent and ultraviolet light<br />
exposure and appropriate symptomatic therapy <strong>of</strong> lesions.<br />
A condition characterised histologically by vasculitis, which appears to be<br />
photoactivated, has been described. The nature <strong>of</strong> the underlying aetiology remains<br />
to be elucidated, but such cases usually respond well to glucocorticoid therapy and<br />
protection from further ultraviolet light exposure. This entity may well underlie some<br />
<strong>of</strong> the cases <strong>of</strong> so-called “canon keratosis” described in the literature. It is clear that<br />
this syndrome is not due to urine splashing in intact stallions (“stud crud”) since it<br />
occurs in females too. As ever, t<strong>here</strong> are some cases <strong>of</strong> crusting lesions <strong>of</strong> the distal<br />
limbs that defy attempts to make a definitive diagnosis and are termed idiopathic.<br />
Lesions <strong>of</strong> the coronary band present a distinct range <strong>of</strong> differential diagnoses. The<br />
use <strong>of</strong> various and sundry topical ho<strong>of</strong> products may be associated with irritant or<br />
allergic reactions <strong>of</strong> the coronary band. Dermatophytosis may be restricted to this<br />
region. Congenital dystrophies are described. Acquired lesions <strong>of</strong> the coronary band<br />
can be seen in pemphigus foliaceus, which in the older horse is not infrequently<br />
confined to the coronary bands. Lesions may also affect the ergots and chestnuts<br />
and the oral mucosa may be involved. The prognosis for complete cure <strong>of</strong> such cases<br />
is poor, but most cases appear to respond to immunosuppressive therapy with<br />
glucocorticoids and long-term remissions can be achieved, with return to useful<br />
work.<br />
Chronic selenosis due to ingestion <strong>of</strong> plants with high selenium content, or<br />
accidental misformulation <strong>of</strong> concentrate feeds results in a coronitis and abnormal<br />
ho<strong>of</strong> growth. Loss <strong>of</strong> mane and tail hair are other features, together with weight loss<br />
and unthriftiness. Prognosis is dependent upon the severity <strong>of</strong> lesions, with the ho<strong>of</strong><br />
deformity and pain seen in some cases necessitating euthanasia.<br />
Coronary band lesions with a histological appearance similar to that seen in<br />
hepatocutaneous syndrome have been encountered in horses with severe liver<br />
pathology. The coronary band is frequently involved in the rare condition <strong>of</strong><br />
exfoliative eosinophilic dermatitis and stomatitis/enteritis syndrome, which carries a<br />
grave prognosis.<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 57
In many cases <strong>of</strong> coronary band disease a definitive diagnosis can be made on<br />
histological examination <strong>of</strong> biopsy material. The optimum method for procuring<br />
tissue is by the shave biopsy technique, w<strong>here</strong>by a tangential incision is made over<br />
the curve <strong>of</strong> the bulbs <strong>of</strong> the heel, under regional nerve block and sedation, if<br />
necessary. Haemostasis is achieved by application <strong>of</strong> a dressing and pressure<br />
bandage. Healing is usually uneventful, without any adverse effect on ho<strong>of</strong> wall<br />
growth.<br />
58<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005
Equine sarcoidosis<br />
Sonya Bettenay<br />
These notes include findings from cases in a multi-centred study collated by Dr Christine Loewenstein, Dr<br />
Sonya Bettenay and Dr Ralf Mueller,with co-investigators Dr Janet Littlewood, Dr Wayne Rosenkrantz,<br />
Dr Claudia von Tscharner, Dr Fernando Ramiro-Ibanez and Dr Sherry Myers<br />
.<br />
Equine sarcoidosis (generalized or systemic granulomatous disease) is a rarely<br />
reported disease characterized clinically by multifocal to generalized exfoliative<br />
dermatitis and histologically by prominent multinucleated giant cell granulomas (also<br />
occur in up to 50% cases in other organ systems). Equine sarcoidosis has been<br />
named after the human sarcoidosis syndrome, so named because <strong>of</strong> these<br />
characteristic “naked” granulomas. It should not be confused with the far more<br />
common “equine sarcoid”, which is a fibroblastic tumorous lesion with various<br />
clinical presentations.<br />
Only few reports about equine sarcoidosis are published. Since the first published<br />
case (Anderson and others 1983) t<strong>here</strong> have been only 6 reports with a total <strong>of</strong> 10<br />
cases (Duell and others 1997, Heath and others 1990, Peters and others 2003, Rose<br />
and others 1996, Sellers and others 2001, Woods and others 1992) and several<br />
general review articles (Mullowney 1985, Scott 1988, Scott 1991, Scott 1992,<br />
Stannard 1987, von Tscharner and others 2000). All <strong>of</strong> the reported cases showed<br />
signs <strong>of</strong> general disease such as apathy, fever, weight loss or lymphadenopathy.<br />
Four <strong>of</strong> the horses died or were euthanized and underwent post mortem<br />
examination. They had involvement <strong>of</strong> internal organs including brain, lung, heart,<br />
lymph nodes, liver, kidney, pancreas, thyroid and adrenal glands (Anderson and<br />
others 1983, Peters and others 2003, Sellers and others 2001, Woods and others<br />
1992). Eight horses showed dermatologic symptoms such as scaling, crusting,<br />
alopecia and nodules (Duell and others 1997, Heath and others 1990, Rose and<br />
others 1996, Sellers and others 2001, Woods and others 1992). 50% <strong>of</strong> 8 horses<br />
recently presented (Spiegel 2005) were said to have pulmonary involvement.<br />
These findings are in contrast to the human disease w<strong>here</strong> skin lesions are present in<br />
only 16 to 36% <strong>of</strong> the cases (Braverman 1998). Pulmonary lesions, however are<br />
most common and seen with 90% <strong>of</strong> the patients (Braverman 2003). Human<br />
sarcoidosis is a multisystemic disease characterised by sarcoidal granulomas.<br />
Sarcoidal granulomas may also be associated with foreign bodies. They are discrete,<br />
round to oval and composed <strong>of</strong> epithelioid histiocytes and multinucleated giant cells<br />
with very occasional lymphocytes. This is in contrast to typical granulomas which are<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 59
surrounded by a sparse rim <strong>of</strong> lymphocytes. Thus, the granulomas are referred to as<br />
"naked" in appearance (Weedon 2002). In horses, the sparsity <strong>of</strong> lymphocytes is a<br />
common feature <strong>of</strong> dermal granulomas and is not emphasized by a special<br />
nomenclature.<br />
In a recent retrospective study we asked pathologists and dermatologists world wide<br />
to contribute cases. Clinical inclusion criteria were the presence <strong>of</strong> a generalised or<br />
multifocal, scaling, crusting dermatitis with or without systemic signs and with no<br />
evidence <strong>of</strong> a concurrent infectious agent. Histopathologic inclusion criteria were<br />
defined as diffuse granulomatous inflammation with an infiltrate dominated by<br />
macrophages and multinucleated giant cells, and negative fungal stains and/or<br />
cultures. Seven horses were included in this study based on dermatologic and<br />
histopathologic inclusion criteria.<br />
Equine sarcoidosis is a rarely reported disease (Sellers and others 2001, Stannard<br />
1987) and although dermatologists and dermatopathologists from around the world<br />
were contacted, only 7 cases were obtained which satisfied our inclusion criteria.<br />
Age <strong>of</strong> onset ranged from 7 months to 17 years with a mean age <strong>of</strong> 8 years. This is<br />
consistent with previously published data, indicating a predisposition for middleaged<br />
horses (mean age <strong>of</strong> 9 years in 10 horses reported). In 5/7 cases the breed was<br />
specified (Quarter horse, Irish hunter and Selle francaise). Comparing to previously<br />
reported breeds (Anderson and others 1983, Duell and others 1997, Heath and<br />
others 1990, Peters and others 2003, Rose and others 1996, Sellers and others 2001,<br />
Woods and others 1992) (1 crossbred, 3 thoroughbred, 1 quarterhorse, 1 hunter, 1<br />
welsh pony cross, 1 Warmblood, 1 miniature pony, 1 standardbred), Quarter horses<br />
seem to be overrepresented in our study, but due to the various sources <strong>of</strong> patients,<br />
statistical significance could not be verified.<br />
Previous reported cases included 3 females and 7 males (Anderson and others 1983,<br />
Duell and others 1997, Heath and others 1990, Peters and others 2003, Rose and<br />
others 1996, Sellers and others 2001, Woods and others 1992). In our study males<br />
were overrepresented (6/7), indicating an emphasis <strong>of</strong> the male gender. However,<br />
the number <strong>of</strong> cases is too small to conclude gender predisposition.<br />
Onset <strong>of</strong> the disease in our study was generally rapid ranging from weeks to a few<br />
months. Only one case exhibited clinical signs for longer than 6 months which is in<br />
accordance to previous reports w<strong>here</strong> one case with sudden worsening <strong>of</strong> the<br />
condition after 1 year was described (Heath and others 1990). In human sarcoidosis,<br />
either an abrupt onset over weeks or an insidious development over months is<br />
possible (Braverman 1998).<br />
Scaling, crusting, alopecia and papules in various combinations were the<br />
predominant lesions. This confirms previous reports (Duell and others 1997, Heath<br />
and others 1990, Rose and others 1996, Scott 1988, Sellers and others 2001, von<br />
Tscharner and others 2000, Woods and others 1992). Cutaneous nodules were<br />
60<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005
described as a possible feature <strong>of</strong> the disease (Scott and others 2003, Stannard 1987)<br />
and were found in one horse (Woods and others 1992). Nodules were identified in<br />
one horse in this study but were presumed to be injection reactions rather than part<br />
<strong>of</strong> the disease. This is in contrast to human medicine, w<strong>here</strong> prevalent lesions are<br />
papules, nodules, plaques, subcutaneous tumours and scaly erythema (Braverman<br />
2003). Edema at various body sites (lips, eye lids, distal limbs, ventral abdomen and<br />
prepuce) was reported previously (Anderson and others 1983, Heath and others<br />
1990, Peters and others 2003, Woods and others 1992) and was noted in one <strong>of</strong> our<br />
horses. Erosions and ulcers described in an earlier report (Sellers and others 2001)<br />
were seen in 2 horses in our study. In human sarcoidosis, violaceous plaques are<br />
commonly observed lesions. In some <strong>of</strong> these, large telangiectatic vessels are present<br />
on the surface. Inflammatory changes involving these vessels may be the<br />
pathomechanism responsible for the development <strong>of</strong> edema, erosions and ulcerative<br />
lesions in horses. Depigmentation on the lips and eyelid margins was described<br />
previously (Heath and others 1990). In one <strong>of</strong> our horses, depigmentation was<br />
observed at the prepuce. Loss <strong>of</strong> skin pigmentation is an uncommon manifestation<br />
in human sarcoidosis, reported to occur exclusively in black patients and may be<br />
related to decreased melanization <strong>of</strong> the overlying epidermal cells (Braverman 2003).<br />
In the literature only one report gives information about the localisation <strong>of</strong> the initial<br />
skin lesions manifesting as a swelling around the lips (Anderson and others 1983).<br />
One author describes the disease onset on the face or limb (Scott 1988, Scott and<br />
others 2003). This could not be confirmed by the findings <strong>of</strong> our study, as all horses<br />
exhibited initial lesions over the trunk and/or shoulder.<br />
Equine sarcoidosis is reportedly characterized clinically by multifocal to generalized<br />
exfoliative dermatitis with internal organ involvement and a poor to guarded<br />
prognosis (Anderson and others 1983, Peters and others 2003, Scott and others<br />
2003, Sellers and others 2001, von Tscharner and others 2000, Woods and others<br />
1992). Granulomatous lesions have been reported in lymph nodes, lungs, heart, liver,<br />
spleen, kidneys, gastrointestinal tract, adrenal and thyroid glands and brain. Affected<br />
horses typically develop a wasting syndrome and signs <strong>of</strong> other organ involvement<br />
such as dyspnoea, gastrointestinal or central nervous signs or lameness (Anderson<br />
and others 1983, Heath and others 1990, Peters and others 2003, Rose and others<br />
1996, Sellers and others 2001, Woods and others 1992). In this study, only one horse<br />
exhibited clinical signs <strong>of</strong> systemic disease such as intermittent fever, prescapular<br />
lymphadenopathy, depression, poor body condition, and nasal discharge. However,<br />
no internal tissue specimens were taken to further investigate internal organ<br />
involvement. As the horse actually responded clinically to glucocorticoid therapy, an<br />
infectious origin seems unlikely, but confirmation <strong>of</strong> granulomatous changes in<br />
organs other than the skin was not made.<br />
The low incidence <strong>of</strong> systemic signs seen in horses included in this study could have<br />
been influenced by our inclusion criteria. We contacted dermatologists rather than<br />
internists with the request for participation, which may have led to a bias for horses<br />
with predominant skin disease rather than horses affected with severe systemic<br />
disease evaluated by internists rather than dermatologists and the search criterion in<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 61
the pathology labs was for granulomatous skin. Recently, a group <strong>of</strong> 7 horses were<br />
investigated which had primary pulmonary disease and no reported concurrent<br />
dermatologic symptoms (Pusterla and others 2003). All <strong>of</strong> these horses showed<br />
granulomatous lesions in the lungs, which formed the inclusion criterion for the<br />
report. Cutaneous signs may not have been present, not mentioned specifically or<br />
overlooked due to the gravity <strong>of</strong> the systemic disease. T<strong>here</strong> may be significant<br />
similarity between human and equine sarcoidosis and the disease may present with a<br />
spectrum <strong>of</strong> clinical signs. Dermatologic lesions may be on one end <strong>of</strong> the spectrum<br />
and pulmonary lesions on the other.<br />
Sarcoidosis is a rare disease in equine medicine and the pathogenesis is unclear. In<br />
human medicine, histopathologic findings <strong>of</strong> sarcoidosis resemble those seen in<br />
tuberculosis. Furthermore, tuberculosis shows an increased incidence in patients<br />
with sarcoidosis. As long as 35 years ago, a role for atypical mycobacteria was<br />
presented (Mankiewicz 1964). By using molecular biologic methods, DNA from M.<br />
tuberculosis and an unidentified nontuberculous mycobacterium was identified in<br />
tissue sections and bronchial washings <strong>of</strong> some patients with sarcoidosis (Fidler and<br />
others 1993). Multiple species <strong>of</strong> mycobacteria were detected by polymerase chain<br />
reaction (PCR) predominantly from samples <strong>of</strong> the lymph nodes and pulmonary<br />
tissue (Li and others 1999). These findings support a potential role <strong>of</strong> mycobacteria<br />
in the pathogenesis <strong>of</strong> sarcoidosis in some human patients. However it must not be<br />
thought to be the exclusive infectious agent as recent studies in Japan and Europe<br />
suggest that Propionibacterium spp. may also be involved in the aetiology <strong>of</strong> sarcoidosis<br />
(Eishi and others 2002). Infectious agents could not be detected in horses by culture,<br />
electron microscopy, animal inoculation, direct immun<strong>of</strong>luorescence or<br />
immunoperoxidase testing (Heath and others 1990, Scott 1991, Stannard 1987, von<br />
Tscharner and others 2000). In three previously reported cases positive titers to<br />
Borrelia burgdorferi were shown (Rose and others 1996). In a recent report, paraffinembedded<br />
skin specimens from 8 horses with sarcoidosis were evaluated with special<br />
stains and PCR assays for Mycobacteria spp., Borrelia burgdorferi, Coccidioides immitis,<br />
Cryptococcus ne<strong>of</strong>ormans and Corynebacterium pseudotuberculosis to no avail (Spiegel and<br />
others 2005). T<strong>here</strong> are anecdotal reports about improvement <strong>of</strong> the condition in<br />
horses which were moved from one state to another (personal communication Tony<br />
Stannard). It was hypothesized that the beneficial effect <strong>of</strong> relocation was due to<br />
differences in environmental concentrations <strong>of</strong> mould spores which may play a role<br />
in the pathogenesis <strong>of</strong> the disease. None <strong>of</strong> the horses included in this study had a<br />
correspondent history.<br />
In humans, massive immunosuppressive doses <strong>of</strong> glucocorticoids are the treatment<br />
<strong>of</strong> choice for sarcoidosis with significant systemic involvement (Braverman 2003).<br />
Cutaneous lesions generally respond to therapy for systemic involvement, but <strong>of</strong>ten<br />
recur when the dosage is lowered or discontinued. Patients without systemic<br />
involvement are typically not treated with glucocorticoids. T<strong>here</strong> are anecdotal<br />
reports <strong>of</strong> success with chloroquine (Zic and others 1991), hydroxychloroquine<br />
(Jones and others 1990), methotrexate (Lower and others 1995), minocycline<br />
(Bachelez and others 2001), thalidomide (Calderon and others 1997, English and<br />
62<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005
others 2001), isotretinoin(Waldinger and others 1983), allopurinol (Pollock 1991),<br />
levamisol (Veien 1986) and tranilast (Yamada and others 1995), but controlled<br />
studies are lacking. Many <strong>of</strong> these agents have immunomodulating properties.<br />
Treatment with penicillin, sulfonamid/trimethoprim and doxycyclin was without<br />
beneficial effect. All but one horse responded to administration <strong>of</strong><br />
prednisolone/prednisone, typically at 1.0 to 1.5 mg/kg -1 q24h for 1 to 6 weeks<br />
followed by a gradual dose reduction. Alternative therapy to glucocorticoids (as<br />
advocated in human cutaneous disease) has not been evaluated in horses. Five <strong>of</strong> the<br />
seven horses were still alive one year after diagnosis; one was still alive 8 months<br />
after diagnosis and then lost to follow up. In two horses, prednisolone led to<br />
complete remission, but clinical signs initially recurred after cessation <strong>of</strong> therapy.<br />
These two horses went into remission again with reintroduction <strong>of</strong> treatment.<br />
Overall, 4/ 6 known horses are still alive 1 to 8 years after diagnosis without any<br />
treatment. This seems to indicate a fair to good prognosis for horses with cutaneous<br />
sarcoidosis. Based on previous reports, concurrent systemic signs indicate a guarded<br />
prognosis. However, the only horse in our study with systemic signs responded to<br />
glucocorticoid administration. None <strong>of</strong> the horses in our study died within one year.<br />
In previously reported cases, deterioration was rapid and occurred within a few<br />
weeks. We may indeed have a skewed sample selection, but it just may be possible<br />
that early presentation and treatment with glucocorticoids prevented generalisation<br />
<strong>of</strong> the disease in our cases.<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 63
References<br />
1. Anderson, C.A. and Divers, T.J. (1983) Systemic granulomatous<br />
inflammation in a horse grazing hairy vetch. Journal <strong>of</strong> the American<br />
<strong>Veterinary</strong> Medical Association 183, 569-570<br />
2. Bachelez, H., Senet, P., Cadranel, J., Kaoukhov, A. & Dubertret, L. (2001)<br />
The use <strong>of</strong> tetracyclines for the treatment <strong>of</strong> sarcoidosis. Archives <strong>of</strong><br />
Dermatology 137, 69-73<br />
3. Braverman, I.M. (1998) Skin Signs <strong>of</strong> Systemic Disease. 3rd edn.<br />
Philadelphia, W.B. Saunders. pp 373-376<br />
4. Braverman, I.M. (2003) Sarcoidosis. In Fitzpatrick´s Dermatology in General<br />
Medicine. 6th edn. Eds I.M. Freedberg, A.Z. Eisen, K. Wolff, K.F. Austen,<br />
L.A. Goldsmith and S.I. Katz. NewYork, McGraw-Hill. pp 1777-1783<br />
5. Calderon, P., Anzilotti, M. & Phelps, R. (1997) Thalidomide in dermatology.<br />
New indication for an old drug. Journal <strong>of</strong> the American Academy <strong>of</strong><br />
Dermatology 36, 881-887<br />
6. Duell, U., Wernitz, U., Onderka, J. & Andres, F. (1997) Sarkoidose - eine<br />
seltene Autoimmunerkrankung bei einem Pferd. Praktischer Tierarzt 78, 486-<br />
490<br />
7. Eishi, Y., Suga, M., Ishige, I., Kobayashi, D., Yamada, T., Takemura, T.,<br />
Takizawa, T., Koike, M., Kudoh, S., Costabel, U., Guzman, J., Rizzato, G.,<br />
Gambacorta, M., du Bois, R.M., Nicholson, A.G., Sharma, O.P. & Ando, M.<br />
(2002) Quantitative analysis <strong>of</strong> mycobacterial and propionibacterial DNA in<br />
lymph nodes <strong>of</strong> Japanese and European patients with sarcoidosis. Journal <strong>of</strong><br />
Clinical Microbiology 40, 198-204<br />
8. English, J.C., Patel, P.J. & Greer, K.E. (2001) Sarcoidosis. Journal <strong>of</strong> the<br />
American Academy <strong>of</strong> Dermatology 44, 725-743<br />
9. Fidler, H.M., Rook, G.A., Johnson, N.M. & McFadden, J. (1993)<br />
Mycobacterium tuberculosis DNA in tissue affected by sarcoidosis. British<br />
Medical Journal 306, 546-549<br />
10. Heath, S.E., Bell, R.J., Clark, E.G. & Haines, D.M. (1990) Idiopathic<br />
granulomatous disease involving the skin in a horse. Journal <strong>of</strong> the American<br />
<strong>Veterinary</strong> Medical Association 197, 1033-1036<br />
11. Jones, E. and Callen, J.P. (1990) Hydroxychloroquine is effective therapy for<br />
control <strong>of</strong> cutaneous sarcoidal granulomas. Journal <strong>of</strong> the American<br />
Academy <strong>of</strong> Dermatology 23, 487-489<br />
64<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005
12. LeGall, F., Loeuillet, L., Delaval, P., Thoreux, P.H., Desrues, B. & Ramee,<br />
M.P. (1996) Necrotizing sarcoid granulomatosiswith and without<br />
extrapulmonary involvement. Pathology Research and Practice 192, 306-313<br />
13. Li, N., Bajoghli, A., Kubba, A. & Bhawan, J. (1999) Identification <strong>of</strong><br />
mycobacterial DNA in cutaneous lesions <strong>of</strong> sarcoidosis. Journal <strong>of</strong><br />
Cutaneous Pathology 26, 271-278<br />
14. Lower, E.E. and Baughman, R.P. (1995) Prolonged use <strong>of</strong> methotrexate for<br />
sarcoidosis. Archives for Internal Medicine 155, 846-851<br />
15. Mankiewicz, E. (1964) The relationship <strong>of</strong> sarcoidosis to anonymous<br />
bacteria. Acta Medica Scandinavica Supplement 425, 68-73<br />
16. Mullowney, P.C. (1985) Dermatologic diseases <strong>of</strong> horses Part V: Allergic,<br />
immune-mediated and miscellaneous skin diseases. Compendium <strong>of</strong><br />
Continuing Education for the practicing Veterinarian 7, 217-228<br />
17. Panciera, R.J., Mosier, D.A. & Ritchey, J.W. (1992) Hairy vetch (Vicia villosa<br />
Roth) poisoning in cattle: update and experimental induction <strong>of</strong> disease.<br />
Journal <strong>of</strong> <strong>Veterinary</strong> Diagnostic Investigation 4, 318-325<br />
18. Peters, M., Graf, G. & Pohlenz, J. (2003) Idiopathic systemic granulomatous<br />
disease with encephalitis in a horse. Journal <strong>of</strong> <strong>Veterinary</strong> Medicine, series A-<br />
Physiology Pathology Clinical Medicine 50, 108-112<br />
19. Pollock, J.L. (1991) Sarcoidosis responding to allopurinol. Archives <strong>of</strong><br />
Dermatology 127, 1034-1040<br />
20. Pusterla, N., Wilson, W.D. & Magdesian, K.G. (2003) Investigation <strong>of</strong> the<br />
etiology and immunologic characterization <strong>of</strong> "idiopathic granulomatous<br />
pneumonia" in seven horses admitted to the VMTH from 1975-2001.<br />
http://www.vetmed.ucdavis.edu/ResServ.html<br />
21. Rose, J.F., Littlewood, J.D., Smith, K. & Shearer, D. (1996) A series <strong>of</strong> four<br />
cases <strong>of</strong> generalized granulomatous disease in the horse. In Advances in<br />
<strong>Veterinary</strong> Dermatology III. Eds K.W. Kwochka, T. Willemse and C. von<br />
Tscharner. Boston, Butterworth-Heinemann. pp 562-563<br />
22. Scott, D.W. (1988) Immunologic diseases. In Large Animal Dermatology.<br />
Philadelphia, W.B. Saunders. pp 326-328<br />
23. Scott, D.W. (1991) Unusual immune-mediated skin diseases in the horse.<br />
Equine Practice 13, 10-15<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 65
24. Scott, D.W. (1992) Diagnostic des dermatoses inflammatoires équines<br />
:analyse de la modalité de réaction histopathologique:étude personelle<br />
portant sur 315 cas. Point Vétérinaire 24, 245-248<br />
25. Scott, D.W. and Miller, W.H. (2003) Miscellaneous skin diseases. In Equine<br />
Dermatology. New York, Elsevier Health. pp 675-680<br />
26. Sellers, R.S., Toribio, R.E. & Blomme, E.A. (2001) Idiopathic systemic<br />
granulomatous disease and macrophage expression <strong>of</strong> PTHrP in a miniature<br />
pony. Journal <strong>of</strong> Comparative Pathology 125, 214-218<br />
27. Spiegel, I.B., White S.D. et al. (2005) Retrospective study <strong>of</strong> cutaneous<br />
equine sarcoidosis and potential underlying infectious etiologies. 20th<br />
Proceedings <strong>of</strong> North American <strong>Veterinary</strong> Dermatology Forum, 166.<br />
28. Stannard, A.A. (1987) Generalized granulomatous disease. In Current<br />
Therapy in Equine Medicine. 2nd edn. Eds N.E. Robinson. Philadelphia,<br />
W.B. Saunders. pp 645-646<br />
29. Strickland-Marmol, L.B., Fessler, R.G. & Rojiani, A.M. (2000) Necrotizing<br />
sarcoid granulomatosis mimicking an intracranial neoplasm:<br />
clinicopathologic features and review <strong>of</strong> the literature. Modern Patholology<br />
13, 909-913<br />
30. Veien, N.K. (1986) Cutaneous sarcoidosis: prognosis and treatment. Clinical<br />
Dermatology 75-87<br />
31. von Tscharner, C., Kunkle, G. & Yager, J. (2000) Stannard´s illustrated<br />
equine dermatology notes. <strong>Veterinary</strong> Dermatology 11, 161-223<br />
32. Waldinger, T.P., Ellis, C.N., Quint, K. & Voorhees, J.J. (1983) Treatment <strong>of</strong><br />
cutaneous sarcoidosis with isotretinoin. Archives <strong>of</strong> Dermatology 119, 1003-<br />
1005<br />
33. Weedon, D. (2002) Skin Pathology. 2nd edn. London, Churchill Livingstone.<br />
pp 194-195<br />
34. Woods, L.W., Johnson, B., Hietala, S.K., Galey, F.D. & Gillen, D. (1992)<br />
Systemic granulomatous disease in a horse grazing pasture containing vetch<br />
(Vicia sp.). Journal <strong>of</strong> <strong>Veterinary</strong> Diagnostic Investigation 4, 356-360<br />
35. Yamada, H., Ide, A., Sugiura, M. & Tajima, S. (1995) Treatment <strong>of</strong> cutaneous<br />
sarcoidosis with tranilast. Journal <strong>of</strong> Dermatology 22, 149-152<br />
36. Zic, J.A., Horowitz, D.H., Arzurbiaga, C. & King, L.E.J. (1991) Treatment <strong>of</strong><br />
cutaneous sarcoidosis with chloroquine. Archives <strong>of</strong> Dermatology 127, 1034-<br />
1040<br />
66<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005
Introduction<br />
The equine sarcoid: an update<br />
Reg Pascoe<br />
A locally aggressive fibroblastic tumour which is probably the most common<br />
cutaneous tumour found in horses. Prevalent in horses aged between 1-6<br />
years.(Torrentegui & Reid 1994: Pascoe & Knottenbelt 1999) The lesions are<br />
frequently not life threatening but they can severely limit the use <strong>of</strong> the horse and<br />
reduce its sale prospects, however euthanasia is not uncommon due to the<br />
prolonged nature <strong>of</strong> treatment, likelihood <strong>of</strong> recrudescence <strong>of</strong> the problem and cost<br />
The role <strong>of</strong> a virus, in particular Bovine papillomavirus (BPV), in its cause and<br />
transmission is still uncertain Population and family studies have shown an<br />
association between sarcoid susceptibility and MHC class II alleles (Lazary et al.,<br />
1985, 1994)<br />
Some research indicated t<strong>here</strong> were no mutations <strong>of</strong> the somatic tumour suppressor<br />
p53 gene in either horses or donkeys associated with the development <strong>of</strong> sarcoids<br />
More recently somatic p53 gene mutations have been found to be associated with<br />
the development <strong>of</strong> some sarcoid tumours in donkeys (Nasir et al 1999). BPV-DNA<br />
was detected in 88% and 91% <strong>of</strong> the successful swabs and scrapings from sarcoids<br />
respectively. The overall diagnostic sensitivity <strong>of</strong> the technique was significantly<br />
lower compared to the clinical diagnosis <strong>of</strong> sarcoids and is unsuitable for occult<br />
sarcoids. However, the detection <strong>of</strong> BPV-DNA in all samples obtained from<br />
sarcoids with an ulcerated surface opens new perspectives for the detection <strong>of</strong><br />
sarcoid involvement in wounds or recurrence after sarcoid removal.(Martens et al<br />
2001)<br />
In a further study BPV DNA was detected in essentially all sarcoids examined<br />
(96/98) it was also detected in normal skin samples from the horses with sarcoids<br />
suggesting the possibility <strong>of</strong> a latent viral phase. Viral latency may be one explanation<br />
<strong>of</strong> the high rate <strong>of</strong> recurrence following surgical removal. All tissues from healthy<br />
horses with non sarcoid neoplasms or papilloma were negative to BVP DNA ( Carr<br />
et al 2001)<br />
Lesions occur in locations which are prone to injury and some have a history <strong>of</strong><br />
previous skin wounds. T<strong>here</strong> is also strong presumptive evidence that sarcoids can<br />
be transmitted by biting and domestic flies which feed on sarcoid tissue and then<br />
browse on other horses with open sores, wounds or tumours. The introduction <strong>of</strong> a<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 67
horse with fibroblastic sarcoids can result in the appearance <strong>of</strong> sarcoids in other<br />
previously uninfected horses on the farm within 6-8 months.<br />
The distribution <strong>of</strong> lesions varies with type <strong>of</strong> sarcoid and geographical location. The<br />
para-genital region is most frequently and the limbs least affected in the UK. In<br />
Queensland (Australia) the majority <strong>of</strong> lesions occur on the head, neck and limbs<br />
and very rarely in the para-genital region (Pascoe & Summers (1981). A recent study<br />
<strong>of</strong> sarcoid cases in the UK showed single and small numbers <strong>of</strong> sarcoids (2-8<br />
sarcoids per horse) were uncommon, w<strong>here</strong>as 10 to several thousand are more<br />
common. The majority <strong>of</strong> lesions seen in UK horses are occult or verrucous, with at<br />
least six major types described (Knottenbelt et al 1995)<br />
The distribution <strong>of</strong> the six types show great variation with a preponderance <strong>of</strong><br />
fibroblastic tumours occurring in the para-genital area; in Australia almost all leg<br />
sarcoids are a fibroblastic type. Sarcoids have a high capacity to invade the dermis<br />
and subcutis. True metastatic dissemination does not appear to occur. Sarcoids can<br />
occur in fresh healing wounds in previously normal horses, or re-occur at the same<br />
site following apparent complete surgical removal.<br />
Six clinical entities:<br />
1.Verrucous (warty) type<br />
Definition<br />
These tend to be slow-growing and not very aggressive until injured in some fashion,<br />
e.g. biopsy, rubbing. poor surgical removal<br />
Clinical presentation<br />
Wart-like growth on and above skin, may be sessile or pedunculated.<br />
Slow growing. Trauma to surface may convert them to a fibroblastic reaction.<br />
(Pascoe 1990)<br />
Differential diagnosis<br />
Papillomatosis, chronic blistering, hyperkeratosis (chronic sweet itch), equine<br />
sarcoidosis (chronic granulomatous disease) squamous cell carcinoma.<br />
Diagnosis<br />
Biopsy: preferably total wide excision followed by cryotherapy<br />
2.Fibroblastic type<br />
Definition<br />
A more aggressive tumour, particularly when located on the lower limbs and<br />
coronet.<br />
68<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005
Clinical Presentation<br />
Small fibrous nodule in skin. Erosion or injury leads to excessive granulation tissue<br />
growth. Lateral progression by local invasion. Metastasise rarely if at all.<br />
difficulty lies in the determination <strong>of</strong> normal and infected granulation tissue<br />
regrowth after tumour removal<br />
Differential diagnosis<br />
Exuberant granulation tissue, habronemiasis, neur<strong>of</strong>ibroma / neur<strong>of</strong>ibrosarcoma,<br />
botryomycosis, fibrosarcoma, squamous cell carcinoma, pythiosis, sweat gland<br />
tumour.<br />
Diagnosis<br />
Biopsy should include normal skin as well as tumour.<br />
3.Mixed Verrucous and Fibroblastic type<br />
Definition<br />
Progressively more aggressive as changes from verrucous to fibroblastic type.<br />
Clinical Presentation<br />
Probably a progressive state from a verrucous type. Contains both verrucous and<br />
fibroblastic elements<br />
Differential diagnosis<br />
The presence <strong>of</strong> more than one form <strong>of</strong> sarcoid is almost self-diagnostic.<br />
4.Occult type<br />
Definition<br />
Hairless areas which contain one or more small cutaneous nodules.<br />
Clinical presentation<br />
Loss <strong>of</strong> hair. Often roughly circular. Very slow growing until injured. Presence <strong>of</strong><br />
one or more hard shot-like nodules in the skin from 2-5mm diam. Nodules may<br />
progress to warty verrucous growth or if injured, develop into fibroblastic lesions.<br />
Commonly around mouth, eyes, neck and body<br />
Differential diagnosis<br />
Dermatophytosis (ringworm), blisters, burns.<br />
Diagnosis Clinical picture. Remember biopsy may convert lesion into active<br />
fibroblastic sarcoid.<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 69
5.Nodular type<br />
Definition<br />
Occurs as subcutaneous nodules and when these erode the overlying skin, they<br />
become more aggressive fibroblastic type tumours<br />
Clinical Presentation<br />
Subcutaneous spherical nodules usually under normal skin(5-20mm). Most<br />
frequently found in the groin or eyelid area Skin may become thin over larger<br />
nodules. W<strong>here</strong> ulceration occurs, lesion quickly develops into fibroblastic sarcoids.<br />
Differential diagnosis<br />
Fibroma, neur<strong>of</strong>ibroma, equine eosinophilic granuloma, melanoma, collagen<br />
necrosis (axilla - rare), dermoid cysts.<br />
Diagnosis<br />
Biopsy: total excision if possible with wide margins<br />
6.Malevolent type (Knottenbelt DC, et al 1995))<br />
Definition<br />
A recent variation <strong>of</strong> sarcoids showing increased malignancy with a suggestion <strong>of</strong><br />
metastasis adjacent to the initial site.<br />
Clinical Presentation<br />
Invasive sarcoid. Infiltration <strong>of</strong> lymphatics. Multiple tumours locally to metastatic<br />
sarcoid in other lymph nodes. May follow surgical interference to sarcoids in jaw and<br />
elbow region. Cords <strong>of</strong> tumour extend in lymphatics.<br />
Differential diagnosis<br />
Squamous cell carcinoma, subcutaneous mycosis, lymphangitis, glanders, enzootic<br />
lymphangitis, cutaneous histoplasmosis.<br />
Diagnosis<br />
Clinical change to original sarcoid. Invasiveness <strong>of</strong> regrowth.<br />
Reaffirmation <strong>of</strong> diagnosis <strong>of</strong> sarcoid from new invasive tissue.<br />
General management consideration<br />
Due to the uncertain outcome in 100% <strong>of</strong> cases, the horse owner should be very<br />
aware <strong>of</strong> the seriousness <strong>of</strong> the problems which can arise from this disease.<br />
Treatment should involve a full discussion <strong>of</strong> treatment options, on the likelihood <strong>of</strong><br />
successful treatment, and at worst, the likelihood <strong>of</strong> prolonged or repeated treatment<br />
which, while the condition is contained, may not fully resolve it.<br />
70<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005
Assessment should be made on the following grounds:<br />
1. The value <strong>of</strong> the animal - actual or sentimental.<br />
2. Previous treatment and history, i.e. likelihood <strong>of</strong> chronic granulation tissue<br />
from old wire cuts or refractory granulation.<br />
3. The cost <strong>of</strong> each avenue <strong>of</strong> treatment and the likelihood <strong>of</strong> a successful<br />
outcome to that type <strong>of</strong> treatment, i.e. repeated single local medication may<br />
eventually be much more expensive than surgical removal, radiation therapy<br />
or cryosurgery.<br />
4. If at all possible, the results <strong>of</strong> biopsy should be known before the final<br />
prognosis is given.<br />
5. Likelihood <strong>of</strong> further spread <strong>of</strong> the condition if treatment is:<br />
(i) not undertaken<br />
(ii) delayed<br />
(iii) not correct.<br />
6. The possibility <strong>of</strong> a contagious nature <strong>of</strong> the sarcoid and the further<br />
transmission to other horses in the group.<br />
Overview <strong>of</strong> modalities for treatment <strong>of</strong> sarcoids<br />
1. Ligatures<br />
Elastrator rings, lycra or even heavy elastic bands can be used. Application<br />
can easily be made, even on fractious horses, using a twitch or tranquillizer.<br />
This works best on single sarcoids w<strong>here</strong> loose skin on body or neck is<br />
available to allow proper placement <strong>of</strong> ligature.<br />
2. Local medication<br />
Moderately successful on single small sarcoids:<br />
- use <strong>of</strong> podophyllin 50% applied daily for > 30 days.<br />
- 10% arsenic trioxide in aqueous solution for 5 days. Causes heavy<br />
scab formation which may be difficult to remove.<br />
- 5-fluorouracil applied under a bandage.(Roberts 1970)<br />
3. Vaccination or stimulation <strong>of</strong> immune system<br />
Bovine wart vaccine has been used and found to be valueless.<br />
Pox vaccines used into the actual sarcoid lesion were also unsuccessful.<br />
Autogenous vaccines have been manufactured but results have not been<br />
good: recovery in under 25% <strong>of</strong> animals treated (Wheat 1964, Page & Tiffany<br />
1967). In 1977 the use <strong>of</strong> BCG vaccine was reported. Lesions were injected<br />
with BCG vaccine, 1ml at 7-10 day intervals, and a good response claimed for<br />
this type <strong>of</strong> treatment (Wyman et al 1977). A similiar type treatment was made<br />
using a non-living wall preparation from BCG vaccine which was injected at<br />
intervals <strong>of</strong> 2-4 weeks. Anaphylaxis had been reported following the use <strong>of</strong><br />
the living BCG vaccine due to proteins produced from the metabolized<br />
vaccine bacteria causing the production <strong>of</strong> antibody which react when further<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 71
72<br />
treatment is given.<br />
This danger was overcome by the use <strong>of</strong> a BCG cell wall vaccine preparation<br />
which was as effective as the living BCG vaccine but does not have the<br />
adverse side effects <strong>of</strong> producing anaphylaxis (Hepler & Leuker 1980).The<br />
reported use <strong>of</strong> such a vaccine (CSL Equoid Australia) for the intradermal<br />
treatment <strong>of</strong> sarcoid gave favourable results with 1-2 injections 14-21 days<br />
apart in 80% <strong>of</strong> the cases treated.(Vaneslow et al 1988). Production problems<br />
with this vaccine led to its permanent withdrawal from the market in 1993.<br />
4. Surgical treatment<br />
Surgical excision– removal <strong>of</strong> sarcoid, under local or general anaesthetic, plus<br />
at least 15-20mm ring <strong>of</strong> normal. Disadvantages: 50% may return and as<br />
wound heals may spread to other areas on the horse; removal <strong>of</strong> large areas<br />
<strong>of</strong> normal skin precludes closure and slowshealing time; inability to remove<br />
this quantity <strong>of</strong> skin from leg lesions increases risk <strong>of</strong> return<br />
CO2 Laser Complete ablasion for small Sarcoids id very successful large<br />
tumours can be less well ablated and may reoccur<br />
5. Electrocautery<br />
W<strong>here</strong> single small masses are involved ordinary cautery is satisfactory but reoccurrence<br />
can be expected. With large electrocautery units, both cutting and<br />
fulguration are available and should be used: remove tumour by cutting<br />
current then treat area, particularly the skin edges, with fulguration to<br />
desiccate tissue.<br />
6. Cryosurgery<br />
Useful for Sarcoids. Complications are under or over treatment; injury to<br />
surrounding blood vessels, nerves, bone and tendon. The success <strong>of</strong><br />
cryotherapy depends on correct technique.(Fretz & Barbour 1987)<br />
Cryonecrosis therapy - The success or otherwise <strong>of</strong> cryotherapy rests in<br />
proper observation <strong>of</strong> correct technique. The following summary assists in<br />
understanding the modality and its side effects.<br />
Cryosurgery summary<br />
(i)Select adequate 'heat' sink (best is liquid N2)<br />
(ii)Freeze tissues rapidly to below -20C<br />
(iii)Allow slow thaw to +36C<br />
(iv)Repeat cycle 2-3 times<br />
(v)Restrict circulation to area using tourniquet<br />
(vi)Protect surrounding tissue with Polystyrene<br />
(vii)Hair follicles are destroyed by double cycle<br />
(viii)Vitiligo occurs with a single freeze thaw cycle; scars with double cycle<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005
(ix)Bone becomes devitalized if included in freeze/thaw cycles; regeneration<br />
may take 2 years<br />
(x)Deep infiltrative tumours are seldom satisfactorily treated by cryosurgery<br />
(xi)Eliminate bulk by surgical trimming before freezing<br />
Technique summary<br />
(i)use <strong>of</strong> thermocouple<br />
(ii)use <strong>of</strong> 2 cycle freeze and thaw<br />
(iii)freeze adequately<br />
(iv)protect normal tissue if using liquid spray<br />
(v)assess patient's temperament and use the correct restraint<br />
(vi)give Tetanus antitoxin or Toxoid booster<br />
(vii)give full explanation <strong>of</strong> the process and after-care to the owner<br />
(viii)do not fail to tell the owner about white hair formation<br />
7. Radiation therapy<br />
Can either be a large distant irradiating source (Teletherapy) which restricts<br />
the use to a limited number <strong>of</strong> large facilities; or (Brachytherapy) treatment<br />
with implants or isotopes to the tumour which is more practical for equine<br />
treatments.(Blackwood & Dobson 1994, Theon 1998, Knottenbelt & Kelly<br />
2000, Henson & Dobson 2004)<br />
Squamous cell carcinoma, sarcoids, s<strong>of</strong>t tissue sarcomas (fibrosarcoma,<br />
haemangiosarcoma and neur<strong>of</strong>ibromas), cutaneous lymphomas and<br />
melanoma are suitable for successful treatment.<br />
Advantages<br />
less disfigurement, better therapeutic success<br />
and as a follow-up to failed surgery, cryosurgery or immunotherapy.<br />
Best results come with debulking surgery under general anaesthesia<br />
previous debulking leads to residual activity <strong>of</strong> dividing tumour cells which<br />
are most susceptible to radiation and to lowered isotope cost due to smaller<br />
treatment area.<br />
Disadvantages-<br />
requires the presence <strong>of</strong> a specialist radiologist or radiophysicist<br />
special secure areas for use <strong>of</strong> hospitalised horses<br />
training <strong>of</strong> personnel to use care around treated horses<br />
increased costs due to isotopes, general anaesthetic<br />
and longer hospitalization in specialized accommodation<br />
Isotopes<br />
Strontium 90 and Radon 222 (Fraunfelder et al 1982a,b), Iodine 128, Caesium<br />
137 and Gold 198 (Wyn Jones 1979,1983) and Iridium 192 (Turrel et al 1985)<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 73
74<br />
In practical terms, those commonly used are iridium 192 and gold 198 which<br />
are both gamma emitters.<br />
Strontium 90, a beta particle emitter has a limited penetration <strong>of</strong> 3mm, so it's<br />
use is restricted to those tumours following very careful debulking or to cleanup<br />
surface cells in conjunction with implants. When applied to the target area<br />
following post surgical ablation <strong>of</strong> the tumour, Strontium 90 in an applicator<br />
has been successfully used for some sarcoids and ocular squamous cell<br />
carcinoma<br />
8. Photodynamic Therapy<br />
The therapeutic potential <strong>of</strong> the photodynamic compound, hypericin, in the<br />
treatment <strong>of</strong> equine sarcoids has been evaluated.In vitro cytotoxicity on three<br />
equine cell lines to phototoxic effect was comparable to that on different<br />
highly sensitive human cell lines and significantly influenced by the energy<br />
density used although independent <strong>of</strong> the cell type.<br />
In vivo anti tumoural action <strong>of</strong> photodynamic therapy using hypericin was<br />
used experimentally on three equine sarcoids in a donkey. With either a 0.3%<br />
hypericin solution in polyethylene glycol (PEG400)/H2O L/L. or a 0.3%<br />
hypericin solution in DMSO/H2O L/L was used.<br />
Intratumoural injections were performed every 5days under short acting GA.<br />
Mean dosage <strong>of</strong> hypericine was 0.7mg/cm3 tumoural tissue. Tumours were<br />
illuminated over 30 min each day with a light delivery by a KL 1500 cold light<br />
source at 1 cm distance from the surface (results in an energy density <strong>of</strong> 72<br />
J/cm2.) . However, this is only for a total <strong>of</strong> 25 days.<br />
81% reduction in tumour volume was obtained at the end <strong>of</strong> therapy and 2<br />
months later, a 90% reduction was observed. Further experimental work<br />
should be performed, but these results suggest that photodynamic therapy<br />
using hypericin has a potential for the non-invasive treatment <strong>of</strong> equine<br />
sarcoids. (Martens 2000)<br />
9. Radio frequency hyperthermia<br />
This modality has been used in equine sarcoid and squamous cell carcinoma<br />
and is most successful in small tumours Reports <strong>of</strong> treatments indicate repeat<br />
treatments are common and the method is not gained wide acceptance<br />
10. Chemotherapy<br />
Many and varied compounds <strong>of</strong> inorganic tissue poisons such as arsenic,<br />
mercury and antimony, and their combinations have been used to treat<br />
sarcoids. More recently podophyllin, methotrexate, 5-fluorouracil, cisplatin<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005
and mitomycin C have been used. All require some form <strong>of</strong> repeat treatment<br />
medication, many on a daily basis for as long as 30 days. Our results are<br />
similar to those <strong>of</strong> the Liverpool <strong>Veterinary</strong> School, UK using AW-3-LUDES<br />
a 80% recovery rate with emphasis on initial treatment success as being a<br />
peculiarity <strong>of</strong> the drug combination ( Knottenbelt & Walker 1994). Repeat<br />
treatment and treatment <strong>of</strong> previously treated unresolved lesions is likely to<br />
be less successful but still more likely than other compounds and treatments<br />
commonly used.<br />
Persistence and client compliance are important for the likelihood <strong>of</strong> higher<br />
success rates.<br />
11. Electro chemotherapy<br />
Enhances the effectiveness <strong>of</strong> chemotherapeutic agents all treatments were<br />
given under short General anaesthesia. An intra tumoral drug Cisplatin in oil<br />
is injected into the lesion. After 5mins two electrodes are placed over the<br />
tumour using a conductive paste and short, intensive electrical pulses (8<br />
pulses 0.1ms at 1-Hz frequency with 1.3 kV voltages) are applied to increase<br />
the permeability <strong>of</strong> the tumour cell membrane to achieve higher cell<br />
concentrates <strong>of</strong> the injected drug.<br />
It works most satisfactorily on small tumours( 10cm tumours were found to be best<br />
treated after de bulking and given multiple electro treatments simply by<br />
overlapping and shifting the electrodes. Eradication so far has been<br />
successful in all treated horses in under four treatments (Tamzali et al.2003)<br />
Prognosis<br />
Varies from good to poor depending on the site, number and type <strong>of</strong> lesions, and<br />
their response to initial treatment.Good client understanding is important for final<br />
resolution<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 75
References<br />
Blackwood L & Dobson JM (1994) - Radiotherapy in the horse; Equine vet Educ<br />
6(2) 95-99<br />
Carr AE, Theon AP, Madewell BR,Griffey SM, & Hitchcock ME (2001) Bovine<br />
Papillomavirus DNA in neoplastic and non neoplastic tissues obtained from horses<br />
with and without sarcoids in the western United States Am J Vet Res 62:741-744<br />
Fretz PB & Barber SM (1987) - Prospective analysis <strong>of</strong> cryosurgery as the sole<br />
treatment for equine sarcoids; Vet Clin Nth Am 10:847<br />
Frauenfelder HC Blevins WE & Page EH (1982a) Strontium 90 for the treatment <strong>of</strong><br />
periocular squamous cell carcinoma in the horse J Am,vet med Assn 180:307-09<br />
Frauenfelder HC Blevins WE & Page EH (1982b) 222rn for the treatment <strong>of</strong><br />
periocular squamous cell carcinoma in the horse J Am,vet med Assn 180:310-312<br />
Henson FMD.& Dobson JM. (2004) Use <strong>of</strong> radiation therapy in the treatment <strong>of</strong> equine<br />
neoplasia Equine vet Educ 15 (6) 315-318<br />
Hepler DI and Lueker DC (1980) - Letter to the Editor, J Am vet med Ass 176:390<br />
Knottenbelt DC. & Kelly DF. (2000) The diagnosis and treatment <strong>of</strong> periorbital<br />
sarcoid in the horse :445 cases from 1974-1999 Vet Ophthal.3, 169-191<br />
Knottenbelt DC & Walker JA (1994) - Topical treatment <strong>of</strong> the equine sarcoid.<br />
Equine vet Educ 6(2) 72-75<br />
Knottenbelt DC, Edwards S & Daniel E (1995) - diagnosis and treatment <strong>of</strong> the<br />
equine sarcoid; In Practice 17(3):123-129<br />
Lazary S, Gerber H, Glatt,PA & Straub R. (1985).Equine leucocyte antigens in<br />
sarcoid affected horses. Equine <strong>Veterinary</strong> Journal 17, 283–6.<br />
Lazary S, Marti E, Salai G, Gaillard C, & Gerber H.(1994). Studies on the frequency<br />
and associations <strong>of</strong> equine leucocyte antigens in sarcoid and summer dermatitis.<br />
Animal Genetics 25, 75–80.<br />
Martens A, De Moor A,& Ducatelle P (2001) PCR Detection <strong>of</strong> Bovine Papilloma<br />
Virus DNA in Superficial Swabs and Scrapings from Equine Sarcoids The<br />
<strong>Veterinary</strong> Journal 161, 280–286<br />
Martens A,. DeMoor A,. Waelkens E. Merlevede W &. De Witte P (2000) InVitro<br />
and In Vivo Evaluation <strong>of</strong> Hypericin for Photodynamic Therapy <strong>of</strong> Equine Sarcoids<br />
The <strong>Veterinary</strong> Journal 159, 77–84<br />
Murphy JM, Severin GA, Lavach JD, Hepler DI and Lueker DC (1979) -<br />
Immunotherapy in ocular equine sarcoid; J Am vet med Ass 174:269<br />
Nasir L , McFarlane ST, & J. Reid SW (1999) Mutational Status <strong>of</strong> the Tumour<br />
Suppressor Gene (P53) in Donkey Sarcoid Tumours The <strong>Veterinary</strong> Journal 157,<br />
99–101<br />
76<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005
Owen LN & Barnett KC (1983) - Treatment <strong>of</strong> equine Squamous Cell Carcinoma <strong>of</strong><br />
the conjunctiva using a Strontium 90 applicator: Equine vet J Supp 2 125-126<br />
Page EH & Tiffany LW (1967) - Use <strong>of</strong> autogenous equine fibrosarcoma vaccine;J<br />
Am vet med Ass 150:177<br />
Pascoe RR (1990) A Colour Atlas <strong>of</strong> Equine Dermatology Wolfe Publishing Ltd<br />
London UK<br />
Pascoe RR& Knottenbelt DC (1999) Manual <strong>of</strong> Equine Dermatology WB Saunders<br />
London UK<br />
Pascoe RR & Summers PM (1981) - A survey <strong>of</strong> Neoplastic and Non-neoplastic<br />
tumours <strong>of</strong> horses in South-east Queensland; Equine Vet J 13(4):235-239<br />
Ragland WL, McLaughlin CA. & Spencer, G. R. (1970). Equine Sarcoid. Equine<br />
<strong>Veterinary</strong> Journal 2, 2–11.<br />
Roberts D (1970) - Experimental treatment <strong>of</strong> equine sarcoid; Vet Med sm anim<br />
Clin 65:67-73<br />
Scott DW & Miller WH (2003) Equine Dermatology Elsevier Science (USA)<br />
Philadelphia PA USA<br />
Tamzali Y, Teissie J & Rols (2003) - First horse Sarcoid treatment by<br />
Electrochemotherapy Preliminary experimental results AAEP Proc 49 : 381-384<br />
Theon A.(1998) Radiation therapy in the horse Vet Clin. N Am. Equine Prac.14 673-<br />
688<br />
Torrontegui BO & Reid SWJ (1994) - Clinical and pathological epidemiology <strong>of</strong> the<br />
equine sarcoid in a referral population; Equine vet Educ 6(2) 85-88<br />
Turrel JM, Stover SM & Guorgyfalvy J (1985) - Iridium-192 interstitial brachytherapy<br />
<strong>of</strong> equine sarcoid: Vet Radiol 26:20-24<br />
Vaneslow BA, Abetz I and Jackson ARB (1988) - BCG emulsion immunotherapy <strong>of</strong><br />
equine sarcoid; Equine vet J (1988) - 20(6)444-447<br />
Wheat JD (1964) - Therapy for equine sarcoids; Mod vet Prac 45:62<br />
Wyman et al (1977) Immunotherapy <strong>of</strong> equine sarcoid: a report <strong>of</strong> 2 cases J Am Vet<br />
Assoc 171 :449<br />
Wyn-Jones G (1983) - Treatment <strong>of</strong> equine cutaneous neoplasia by radiotherapy<br />
using iridium 192 linear sources; Equine vet J 15:361-365<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 77
Introduction<br />
78<br />
Histopathological review <strong>of</strong><br />
equine sarcoids<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005<br />
Jenny Charles<br />
The sarcoid is the most common skin tumour <strong>of</strong> horses, donkeys and mules and is a<br />
locally invasive fibroblastic neoplasm which lacks metastatic potential. Individual<br />
animals may have multiple tumours, either synchronously or sequentially. Although<br />
spontaneous regression <strong>of</strong> equine sarcoids after a protracted growth period has been<br />
reported, it is a rare occurrence and most lesions require surgical excision,<br />
cryosurgery, immunotherapy, radiation brachytherapy or other intervention. Local<br />
recurrence <strong>of</strong> sarcoids is common and is expected <strong>of</strong> incompletely excised lesions.<br />
T<strong>here</strong> is considerable evidence implicating papillomaviruses (closely related to<br />
bovine papillomaviruses types 1 and 2) in the aetiopathogenesis <strong>of</strong> equine sarcoids.<br />
Gross appearance<br />
Most sarcoids are grossly characterised by firm dermal thickening by cream-white<br />
tissue with thickening, roughening and hyperkeratosis <strong>of</strong> the skin surface. The<br />
tumour may be sessile, domed or pedunculated and well demarcated or poorly<br />
circumscribed. The surface <strong>of</strong> protruberant sarcoids is commonly ulcerated. The<br />
gross appearance <strong>of</strong> many sarcoids may closely mimic that <strong>of</strong> exuberant granulation<br />
tissue and, in ulcerated tumours, granulation tissue may coexist with neoplastic tissue<br />
and contribute to lesion growth.<br />
Various classification schemes have been proposed by equine clinicians based upon<br />
the gross appearance <strong>of</strong> sarcoids. These schemes are essentially for descriptive<br />
purposes. The gross appearance <strong>of</strong> sarcoids may alter over time, both as part <strong>of</strong><br />
neoplastic progression and in response to lesion abrasion, ulceration or iatrogenic<br />
trauma. The anatomic location <strong>of</strong> a sarcoid may also influence its gross appearance.<br />
Six variants have been described: occult, verrucous, fibroblastic, nodular, mixed and<br />
malevolent.<br />
Occult sarcoids emerge as one or a few, well-defined, annular areas <strong>of</strong> hair loss<br />
with variable scaling or crusting. These lesions, which may closely resemble those <strong>of</strong><br />
dermatophytosis or focal frictional injury, may gradually expand or remain static for<br />
months or years before ultimately evolving into firm dermal or subcutaneous<br />
nodules or relatively sessile, hyperkeratotic verrucous lesions. Abrasion or surgical<br />
biopsy <strong>of</strong> occult sarcoids may provoke vigorous fibroblastic proliferation and<br />
emergence <strong>of</strong> a more aggressive fibroblastic variant. Occult sarcoids may occur at
any anatomic location but commonly arise on the medial thigh, prepuce, neck and<br />
face.<br />
Verrucous (warty) sarcoids are usually less circumscribed than occult sarcoids and<br />
protrude as palpable masses due to an increased dermal neoplastic component.<br />
They may be sessile or pedunculated. The degree <strong>of</strong> overlying hyperkeratosis and<br />
scaling is variable but t<strong>here</strong> is <strong>of</strong>ten a partially or totally alopecic, dry, cauliflower-like<br />
surface. This variant is also relatively slow-growing but a more aggressive<br />
fibroblastic type may emerge following trauma. Verrucous sarcoids need to be<br />
distinguished from squamous papillomas induced by equine papillomavirus and from<br />
chronic frictional irritation. Verrucous sarcoids are most commonly located in the<br />
axillary and inguinal areas.<br />
Fibroblastic sarcoids involve both the dermis and subcutis, with the extent <strong>of</strong> deep<br />
dermal and subcutaneous infiltration <strong>of</strong>ten being underestimated on clinical<br />
examination. This variant typically manifests as a protruberant, firm to fleshy,<br />
ulcerated mass which closely resembles exuberant granulation tissue. It is wellvascularised<br />
and prone to bleed when minimally traumatised. Most sarcoids arising<br />
on the brisket or limbs are <strong>of</strong> fibroblastic appearance. Fibroblastic sarcoids may<br />
enlarge rapidly over weeks to months and then stabilise and persist for years.<br />
Differential diagnoses for such lesions include, in addition to proud flesh, squamous<br />
cell carcinoma, botryomycosis, habronemiasis, phycomycosis, fibrosarcoma and<br />
peripheral nerve sheath tumour.<br />
Nodular sarcoids usually involve only the subcutis as one or multiple, spherical,<br />
mobile nodules usually covered by intact skin <strong>of</strong> normal appearance. Intradermal<br />
nodular sarcoids may occasionally be seen and the overlying skin may appear thin<br />
and shiny. Sarcoids involving the palpebral margins are typically nodular and this<br />
variant is also commonly found on the medial thigh, prepuce and inguinal area.<br />
Nodular sarcoids, being well demarcated, are amenable to surgical excision but<br />
incomplete excision (or traumatic ulceration <strong>of</strong> the overlying skin) may encourage<br />
emergence <strong>of</strong> a more aggressive fibroblastic variant. Nodular sarcoids may grossly<br />
resemble nodular necrobiosis (equine eosinophilic collagenolytic granuloma) and<br />
other mesenchymal tumours such as melanoma, fibroma or peripheral nerve sheath<br />
tumour.<br />
Mixed sarcoids present with a combination <strong>of</strong> the gross characteristics <strong>of</strong> two or<br />
more <strong>of</strong> the verrucous, fibroblastic and nodular forms and may represent a<br />
transitional phase as a more rapidly growing and locally aggressive neoplasm emerges<br />
from a previously stable focus. Mixed sarcoids are most commonly found in the<br />
axillary and inguinal areas and on the face.<br />
Malevolent sarcoids are rare, highly invasive variants which infiltrate along<br />
lymphatics to produce nodular cording and multiple ulcerated fibroblastic nodules.<br />
The neoplastic tissue may extend along lymphatics to involve regional lymph nodes.<br />
Most malevolent sarcoids have been observed following intereference with a<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 79
fibroblastic variant, particularly on the elbow or jaw. Differential diagnoses for such<br />
lesions include various forms <strong>of</strong> chronic infectious lymphangitis/lymphadenitis (e.g.<br />
glanders, epizootic lymphangitis and cutaneous histoplasmosis) and metastasising<br />
carcinomas.<br />
Why biopsy?<br />
Histopathology usually permits confirmation <strong>of</strong> a clinical diagnosis <strong>of</strong> equine sarcoid<br />
and elimination <strong>of</strong> the considerable list <strong>of</strong> differential diagnoses. However, nonexcisional<br />
biopsy may provoke transition <strong>of</strong> a quiescent sarcoid into a rapidly<br />
growing aggressive one. For this reason, many equine practitioners are loath to<br />
interfere, particularly with large or poorly demarcated lesions or when a suitable<br />
method <strong>of</strong> treatment is unlikely to be available once the diagnosis is confirmed.<br />
Diagnostic histological features <strong>of</strong> equine sarcoids<br />
Histologically, most sarcoids are characterised by dermal fibroblastic proliferation<br />
and intimately associated, pseudoepitheliomatous hyperplasia <strong>of</strong> the epidermis.<br />
T<strong>here</strong> is usually some degree <strong>of</strong> hyperkeratosis and t<strong>here</strong> may be mild parakeratosis.<br />
Long, narrow, anastomosing rete pegs <strong>of</strong> hyperplastic and at least focally acanthotic<br />
epidermis extend into the proliferating spindle cell component in the dermis.<br />
The infiltrative and poorly demarcated dermal component is usually <strong>of</strong> moderately<br />
high cell density, with the superficial portion tending to be more cellular than the<br />
deep part. The dermal fibroblasts are slender to plump fusiform cells with poorly<br />
defined cytoplasmic boundaries. The nuclei may be slender and elongate or enlarged<br />
and <strong>of</strong> irregular shape. Mitotic figures are usually infrequent (0-1 per high power<br />
field) but may be more numerous (up to 2-3 per high power field) in superficial than<br />
in deep areas <strong>of</strong> sarcoids and adjacent to areas <strong>of</strong> ulceration. Mitoses and<br />
fibroblastic nuclear pleomorphism, anisokaryosis and nucleolar enlargement may be<br />
observed in rapidly growing or recurrent sarcoids; cellular anaplasia is, however, rare.<br />
The fibroblasts are typically arrayed in tight whorls, interweaving bundles, haphazard<br />
tangles and occasionally herringbone and basket weave patterns, with a small to<br />
moderate amount <strong>of</strong> intercellular collagen. In recently developed sarcoids, the<br />
volume <strong>of</strong> intercellular collagen may be minimal. In chronic lesions, the collagen<br />
content increases and the dense fibres may appear hyalinised. Plump dermal<br />
fibroblasts usually directly abut the epidermis and, in a high percentage <strong>of</strong> sarcoids,<br />
are characteristically oriented perpendicular to the epidermal basement membrane in<br />
a picket-fence arrangement. Hair follicles enveloped by fibroblasts may undergo<br />
cystic dilation.<br />
Histological variants<br />
Prominent hyperplasia <strong>of</strong> the epidermis with formation <strong>of</strong> long rete pegs is not<br />
invariably present in sarcoids. It is usually observed in verrucous and mixed forms<br />
and at the margins <strong>of</strong> ulcerated areas in fibroblastic sarcoids. In occult sarcoids, the<br />
80<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005
epidermis may be histologically normal, minimally hyperplastic or atrophic;<br />
hyperkeratosis, if present, is <strong>of</strong>ten mild. Epidermal thinning is a common finding in<br />
nodular sarcoids but the epidermis may be normal if the fibroblastic component is<br />
confined to the subcutis or involves the dermis but does not directly underrun the<br />
epidermis.<br />
All sarcoids are characterised by an increased density <strong>of</strong> fibroblasts but occult<br />
sarcoids are usually less cellular than other forms. Some occult sarcoids are<br />
characterised by only a subtle increase in the density <strong>of</strong> fibroblasts in the superficial<br />
to mid dermis and a localised reduction in the number <strong>of</strong> adnexal structures. The<br />
fibroblasts are frequently not in typical whorling patterns or oriented as<br />
subepidermal picket-fences in occult tumours. Picket-fence alignment is also<br />
commonly absent in nodular sarcoids.<br />
In some sarcoid variants, hyperplasia <strong>of</strong> the epidermis is more pronounced than the<br />
dermal fibroblastic proliferation. These variants may histologically mimic a<br />
squamous papilloma.<br />
Non-diagnostic biopsies<br />
Excisional biopsies are more likely to be diagnostic than are punch biopsies,<br />
particularly if the excisional biopsies are histologically sectioned perpendicular to the<br />
skin surface to reveal the epidermal component <strong>of</strong> the lesion and the epidermaldermal<br />
interface. If punch biopsies are taken, it is important to avoid ulcerated or<br />
superficially inflamed areas in which diagnostic features may be obliterated or<br />
obscured.<br />
The typical epidermal component <strong>of</strong> sarcoids may not be demonstrable in ulcerated<br />
lesions. In the absence <strong>of</strong> a hyperplastic epidermis, the dermal component <strong>of</strong> the<br />
sarcoid may be misdiagnosed as granulation tissue, a fibroma, a fibrosarcoma or a<br />
peripheral nerve sheath tumour. Superficial dermal fibroblast proliferation may also<br />
be obliterated by ulceration or obscured by granulation tissue in traumatised lesions.<br />
Differential diagnoses<br />
Sarcoids are usually readily distinguished from squamous papillomas histologically by<br />
virtue <strong>of</strong> their dermal fibroblastic component.<br />
Granulation tissue may be present within ulcerated sarcoids and is characterised by<br />
orderly proliferation <strong>of</strong> both fibroblasts and endothelial cells, with the new capillaries<br />
aligned in parallel and at right angles to the fibroblasts and new collagen fibres. A<br />
maturation face may be apparent in older granulating lesions, with collagen <strong>of</strong> low<br />
cellularity in deeper areas and ongoing fibrovascular proliferation superficially.<br />
Fibromas can be distinguished from sarcoids by being expansively growing, well<br />
circumscribed nodules which compress adjacent structures. They are mainly<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 81
composed <strong>of</strong> collagen with only small numbers <strong>of</strong> fibroblasts/fibrocytes <strong>of</strong> normal<br />
morphology and only rarely are mitotic figures visible. Histological differentiation <strong>of</strong><br />
sarcoids and fibrosarcomas may be more problematical; however, anaplasia <strong>of</strong><br />
fibroblasts is rarely observed in sarcoids and perpendicular alignment <strong>of</strong> fibroblasts<br />
beneath the epidermis is not expected in fibrosarcomas or other mesenchymal<br />
neoplasms. Histological detection <strong>of</strong> close association <strong>of</strong> a spindle cell tumour with<br />
a peripheral nerve or its sheath may be useful in identifying peripheral nerve sheath<br />
tumours.<br />
Alternative diagnostic methods<br />
With the advent <strong>of</strong> polymerase chain reaction (PCR) technology, t<strong>here</strong> is the<br />
potential for rapid diagnosis <strong>of</strong> equine sarcoids by identification <strong>of</strong> bovine<br />
papillomaviral DNA in swabs or scrapings <strong>of</strong> the surface <strong>of</strong> suspected lesions. In<br />
one study <strong>of</strong> 92 sarcoids, the overall sensitivity <strong>of</strong> this test was 88% for swabs and<br />
91% for scrapings, with all sarcoids having partially or completely ulcerated surfaces<br />
being correctly identified. The swab technique was found to be unsuitable for occult<br />
sarcoids due to low sensitivity.<br />
PCR amplification <strong>of</strong> bovine papillomaviral sequences can also be performed on<br />
formalin-fixed, paraffin-embedded tissues to confirm a diagnosis <strong>of</strong> equine sarcoid<br />
when histopathological examination <strong>of</strong> biopsy material is inconclusive.<br />
82<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005
References<br />
D.C. Knottenbelt, S. Edwards and E. Daniel. Diagnosis and treatment <strong>of</strong> the equine<br />
sarcoid. In Practice 1995; 17: 123-129.<br />
D.C. Knottenbelt and R.R. Pascoe. Colour Atlas <strong>of</strong> Diseases and Disorders <strong>of</strong> the Horse.<br />
Wolfe Publishing, Barcelona, 1994: pp. 275-279.<br />
A. Martens, A. De Moor, J. Demeulemeester and R. Ducatelle. Histopathological<br />
characteristics <strong>of</strong> five clinical types <strong>of</strong> equine sarcoid. Res. Vet. Sci. 2000; 69:295-300.<br />
A. Martens, A. De Moor and R. Ducatelle. PCR detection <strong>of</strong> bovine papilloma virus<br />
DNA in superficial swabs and scrapings from equine sarcoids. Vet. J. 2001; 161:280-<br />
286.<br />
E. Marti, S. Lazary, D.F. Antczak and H. Gerber (eds.). Report <strong>of</strong> the first<br />
international workshop on equine sarcoid. Equine vet. J. 1993; 25:397-407.<br />
R.R. Pascoe and D.C. Knottenbelt. Manual <strong>of</strong> Equine Dermatology. W.B. Saunders<br />
Company Ltd., London, 1999: pp. 244-248.<br />
J.N. Tarwid, P.B. Fretz and Clark, E.G. Equine sarcoids: a study with emphasis on<br />
pathologic diagnosis. Comp. Contin. Educ. 1985; 7:S293-300.<br />
I.F. Williams, A. Heaton and K.G. McCullagh. Connective tissue composition <strong>of</strong><br />
the equine sarcoid. Equine vet. J. 1982; 14:305-310.<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 83
84<br />
How I treat: equine bacterial<br />
folliculitis<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005<br />
Sonya Bettenay<br />
The diagnosis <strong>of</strong> bacterial folliculitis in the horse will be made typically based on the<br />
clinical lesions, frequently with supportive cytology and bacterial culture. Less<br />
frequently a biopsy will be performed.<br />
Clinical presentation:<br />
Varies depending on the underlying predisposing cause. It occurs frequently<br />
secondary to trauma and maceration, less commonly to an underlying disease and is<br />
most commonly seen in spring and summer. Bacterial folliculitis is also a frequent<br />
complicating factor <strong>of</strong> Dermatophytosis. Lesions are <strong>of</strong>ten painful which can have<br />
interesting consequences when the affected area is in the saddle and/or tack area.<br />
Indeed the pain (or rather the horses response to it!) is <strong>of</strong>ten the driving reason for<br />
the consultation and need for therapy.<br />
The most common initial lesions include papules, pustules, crusted papules and<br />
larger crusts. These may not be observed until t<strong>here</strong> are actual fissures and/or ulcers<br />
with larger crusts. However they may be detected early in animals which are<br />
groomed daily. Urticaria with small follicular papules is a common early<br />
presentation <strong>of</strong> some horses, which can be confused as an uncomplicated allergy.<br />
These early cases will frequently respond to symptomatic steroid therapy, only to<br />
relapse again once the anti-inflammatory component <strong>of</strong> the treatment has stopped.<br />
They may also show a slightly more prolonged clinical response to a topical<br />
combined antibiotic-steroid agent…. But have a higher relapse rate as these topicals<br />
do not always reach the deeper affected areas <strong>of</strong> the follicle.<br />
Medication Choices:<br />
Bacterial folliculitis in the horse is most frequently caused by coagulase-positive<br />
staphylococci. This is a “deep” pyoderma, which will typically not self resolve and<br />
so antibacterial therapy is an essential part <strong>of</strong> any treatment regime. Clipping and<br />
cleaning, topical antibacterial agents and systemic antibiotics are frequently all<br />
utilised and even then the lesions may take quit some time (weeks to months) to<br />
resolve. Superficial pyodermas can, at least initially, be treated empirically. If<br />
appropriate therapy does not resolve the condition, a culture and sensitivity is
indicated. Each sample for culture and sensitivity should be accompanied by<br />
cytologic examination and culture results interpreted in light <strong>of</strong> the cytology, as<br />
growth <strong>of</strong> different microorganisms does not indicate necessarily that they are<br />
present in significant numbers in vivo.<br />
A bacterial culture and sensitivity is almost always indicated when treating horses<br />
with a deep pyoderma, however whether the owners will elect to pursue this without<br />
an initial empirical trial therapy is another question. T<strong>here</strong>fore we frequently make a<br />
“best guess” when using systemic antibiotics. Whilst Streptococcus equi or<br />
Corynebacterium pseudotuberculosis are the most common organisms found in abscesses,<br />
Streptococci and coagulase-positive staphylococci and are most commonly seen with<br />
folliculitis.<br />
Local geographic use <strong>of</strong> antimicrobials does lead to a geographic variation in<br />
resistance (and sensitivity) rates, so that extrapolating a report from Colorado to<br />
Queensland or even Sydney to Brisbane is not necessarily useful and may even be<br />
counterproductive. Similarly a horse stabled in (for example) a busy racing stable,<br />
with multiple animals and a frequently changing population which is intensively<br />
husbandried in Melbourne, may have quite a different bacterial population than one<br />
in the Dandenongs which is not stabled, lives alone, retired in a paddock with a few<br />
sheep. They may both have a coagulase-positive staphylococcus, but the resistance<br />
patterns may have more to do with husbandry and immediate environment, than<br />
with significant geography.<br />
The intensity <strong>of</strong> investigation and treatment will, as always in veterinary medicine, be<br />
to a large part determined by the owner finances, expectations and abilities to<br />
undertake recommended treatment regimes.<br />
1. Shampoo therapy. Shampoo therapy can provide effective medical and<br />
cosmetic management <strong>of</strong> dermatoses. However, shampooing the whole<br />
body <strong>of</strong> a horse is a major undertaking and thus shampoo therapy is most<br />
commonly used for localized skin disease. Fungal and bacterial<br />
infections, allergies as well as mane and tail seborrheas are the most<br />
common indication for shampoo therapy in equine practice. T<strong>here</strong> are<br />
few adverse effects associated with shampoo therapy, although they are<br />
recognized. However, shampoo therapy is a symptomatic treatment, and<br />
rarely "cures"a dermatosis. Chlorhexidine (frequency q 1-14 days) is<br />
useful in horses as it is not inactivated by organic matter and tends to be<br />
not irritating or drying. Benzoyl peroxide (frequency q 7-14 days) is a far<br />
more potent antibacterial agent. Degreasing (and thus drying),<br />
keratolytic. In horses with dry or normal skin, a moisturizer must be used<br />
after the shampoo! It may be irritating, particularly in concentrations<br />
over 3%. Iod<strong>of</strong>ors (frequency q 7-14 days) are typically used by every<br />
horse owner as the first step prior to calling the vet, they are antifungal,<br />
antibacterial, viricidal and sporicidal. They may also be helpful in<br />
decreasing environmental contamination with fungi.<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 85
86<br />
2. Topical antibacterials: are not listed <strong>here</strong>, almost every veterinarian will<br />
have their own “favourite”. The combination <strong>of</strong> antibiotic with a low<br />
penetration steroid is frequently a helpful treatment modality. The<br />
inflammatory response can be exuberant in horses and can actually<br />
complicate the resolution <strong>of</strong> the foliculitis. It can also play a particularly<br />
helpful role in those horses which have allergies as an underlying<br />
predisposing cause.<br />
3. Macrolids such as erythromycin and lincomycin may cause severe<br />
diarrhea due to their effects on bacterial flora in the large colon.<br />
Tetracyclines also should be used with caution.<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005
Proper dosage and proper duration are important for the success <strong>of</strong> antibacterial<br />
therapy. Although many bacterial infections in the horse respond to short courses <strong>of</strong><br />
antibiotics, longer courses may be needed in particular if the folliculitis has extended<br />
to a furunculosis. The likelihood <strong>of</strong> this occurrence increases with the duration <strong>of</strong><br />
the (untreated) disease and also with the pathogenicity <strong>of</strong> the causative agent(s). For<br />
example it is more likely to occur early in a dermatophyte associated folliculitis than<br />
an allergic, non-traumatised one.<br />
Selected antibiotics in equine dermatology:<br />
Drug<br />
Formulation Indications<br />
Adverse effects Dose<br />
Penicillin G 300,000 Infections with most gram-positive and Hypersensitivity 20,000-40,000IU/kg (10 ml/70-<br />
IU/ml for gram-negative cocci (not penicillinase- reactions 150 kg bodyweight) IM q 12h<br />
injection producing strains), Clostridium sp.,<br />
Fusobacterium and Actinomyces.<br />
Penicillin V 500-mg Infections with Actinomyces, most Gastrointestinal 40-60 mg/kg (10 tablets/100kg<br />
tablets spirochetes and Gram-positive and signs with oral bodyweight) q 8 h<br />
Gram–negative cocci, which do not administration,<br />
produce penicillinase.<br />
hypersensitivity<br />
reactions<br />
Trimethoprim/ 800mg Infections with Gram-positive bacteria Transient 20-30 mg/kg (1 tablet/30-50 kg<br />
sulfadiazine<br />
trimethoprim (streptococci, staphylococci). Many pruritus, bodyweight) q 12-24 h; 15-20<br />
/ 160mg Gram-negative organisms <strong>of</strong> the family diarrhea, mg/kg (10 ml/250-350 kg<br />
sulfadiazine, Enterobacteriaceae are also susceptible hypersensitivities bodyweight) IV q 12-24 h<br />
48% sterile (but not Pseudomonas aeruginosa). ,blood dyscrasias<br />
Chlor-amphenicol<br />
injection<br />
1000mg Infections with most gram-positive and Bone marrow 50 mg/kg q 8 h (10 tablets/200<br />
tablets, 100 gram-negative cocci, Clostridium sp., toxicity<br />
kg bodyweight)<br />
mg/ml<br />
sodium<br />
succinate<br />
as Fusobacterium and Nocardia.<br />
powder<br />
injection<br />
for<br />
Cephalexin 1000-mg Infections with streptococci, Vomiting and 20-30 mg/kg q 8 h<br />
tablets staphylococci,Actinobacillus,<br />
diarrhea; very<br />
Corynebacteria (except C. equi)<br />
rarely<br />
excitability,<br />
tachypnea or<br />
Enr<strong>of</strong>loxacin 136-mg<br />
blood dyscrasias<br />
Cartilage 2.5-5 mg/kg q 24 h<br />
tablets<br />
erosions<br />
growing foals<br />
in<br />
Taken from, with permission, Equine Dermatology Made Easy,<br />
Teton New Media, author Dr Ralf Mueller.<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 87
Treatment Regime:<br />
This varies with a number <strong>of</strong> factors, some <strong>of</strong> which will be more important than<br />
others in different individuals:<br />
1. Site<br />
88<br />
1. Site<br />
2. Affect on the horse<br />
3. Affect to the owner (is it a show horse?)<br />
4. Response (or lack <strong>of</strong>) to previous therapy<br />
5. Extent (area) and severity (depth) <strong>of</strong> the lesions<br />
6. Owners ability to treat / manage<br />
7. Environmental conditions<br />
8. Monies available for therapy<br />
I associate various sites with various possible underlying causes and as such, the<br />
treatment regime will include a treatment modality aimed at the presumed, or<br />
diagnosed underlying cause, as well as addressing the folliculitis.<br />
Tack areas: such as underneath bridle cheek straps, girths, saddles, cruppers. These<br />
areas have a naturally thicker skin than many other areas and so frequently the<br />
folliculitis +/- associated furunculosis will require a longer course <strong>of</strong> systemic<br />
antibiotics. I do not expect these infections to heal well without systemic antibiotics<br />
and also without rest from the presence <strong>of</strong> the overlying tack. Completely spelling a<br />
horse for the 3 to 4 weeks the folliculitis may require to resolve can be catastrophic<br />
from the point <strong>of</strong> view <strong>of</strong> a working horse (owner), however I expect that any<br />
external trauma to these areas during that time will extend the recovery period.<br />
Lambskin pads, utilising different tack, frequent surface washes may all help to<br />
minimise this trauma IF the horse must be worked.<br />
Pastern: frequently associated with environmental maceration, which needs to be<br />
corrected before one can honestly expect a recovery. However t<strong>here</strong> are the other<br />
implicated factors such as UV-light and a contact hypersensitivity (whether that is<br />
mediated through a UV-sensitisation is still discussed). The lower leg swelling<br />
associated with a lymphadenopathy in “Draught horses” can also be associated<br />
initially with a pastern folliculitis.<br />
These are <strong>of</strong>ten deep, fissured and associated with a furunculosis which requires<br />
both topical and systemic therapy for the bacterial component.<br />
Generalised: may be associated with underlying stress or allergy factors, which will<br />
ned to be addressed concurrently. Due to the large body area affected, these will<br />
also require a systemic course, but typically respond fast.<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005
2. Affect on the horse and 3. Affect to the owner<br />
The degree with which the dermatitis is interfering with work, the cosmetic<br />
appearance and the simple well being <strong>of</strong> the horse will all be factors which affect just<br />
how intensive the chosen treatment will be. These lesions are frequently painful and<br />
may turn a placid creature into a demon. If the horse is a work or show horse and<br />
the lesions are in the tack area, then the consequences are even more dramatic<br />
Owners will be affected emotionally, by the change in personality <strong>of</strong> their beloved<br />
pet, and by the potential inability <strong>of</strong> their horse to fulfil its “job”.<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 89
90<br />
How I treat: equine insect bite<br />
hypersensitivity<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005<br />
Mandy Burrows<br />
Insect bite hypersensitivity is the most common allergic skin disease <strong>of</strong> the horse. It<br />
has a worldwide distribution.<br />
Cause and Pathogenesis<br />
This disorder represents type I (immediate and late phase) and type IV (delayed)<br />
hypersensitivity to antigens (presumably salivary) from numerous Culicoides (gnats)<br />
and Simulium (black flies) species, Stomoxys calcitrans (stable fly) and possibly<br />
Haematobia irritans (horn fly). Some horses have hypersensitivities to multiple insects.<br />
Culicoides gnats (biting midges, sandflies) are the most important cause <strong>of</strong> equine<br />
insect hypersensitivity. Results <strong>of</strong> gnat collection techniques, intradermal testing with<br />
gnat antigens and passive cutaneous anaphylaxis trials have incriminated numerous<br />
Culicoides species in various parts <strong>of</strong> the world. C.brevitarus (C.robertsi) appears to be<br />
most important in Australia. In general Culicoides gnats are most active when the<br />
ambient temperature is above 28C, when humidity is high and when t<strong>here</strong> is no<br />
breeze. Culicoides gnats breed in standing water and generally fly short distances.<br />
Clinical evidence strongly suggests that this disorder has familial and genetic<br />
predispositions. Intradermal injections <strong>of</strong> Culicoides (and occasionally Simulium,<br />
Stomoxys and Haematobia) extracts produce immediate (30 mins) and delayed (24 to 48<br />
hours) reactions in over 80% and about 50% respectively <strong>of</strong> affected horses. Some<br />
affected horses also develop late phase immediate (4 to 6 hours) reactions. Affected<br />
horses typically react to all Culicoides spp injected suggesting shared common<br />
allergens. Most horses react to two or more genera <strong>of</strong> insects.<br />
Clinical features<br />
No age or sex predilection; most horses first develop clinical signs at 3 to 4 years and<br />
the condition typically worsens with age. Coat colour is not a risk factor. It may be<br />
seen in any breed but certain breeds are reported to be at increased risk; Icelandic,<br />
German Shire, Welsh ponies, Arabians, Connemaras, and quarter horses. Clinical<br />
signs are distinctly seasonal (spring through to autumn) but in warmer subtropical to<br />
tropical climates the disease can be non seasonal with seasonal (summer)<br />
exacerbations. Clinical signs are <strong>of</strong>ten worse near dawn and dusk as this is the<br />
favourite feeding time for many Culicoides species.
Affected horses usually scratch and chew themselves and rub against environmental<br />
objects (stalls, fences, doorways, posts, trees etc) Reflex nibbling movements can<br />
<strong>of</strong>ten be elicited by manipulation <strong>of</strong> the skin <strong>of</strong> the mane. Horses usually show one<br />
<strong>of</strong> three patterns <strong>of</strong> skin disease i.e dorsal, ventral or some combination t<strong>here</strong><strong>of</strong> and<br />
these differences in lesion distribution probably reflect the different preferential<br />
feeding sites <strong>of</strong> the various insect species.<br />
Dorsal insect hypersensitivity is characterised by pruritus with or without crusted<br />
papules, usually beginning at the mane, rump and base <strong>of</strong> tail. The condition then<br />
extends to involve the face, pinna, neck, shoulder and dorsal thorax. Self trauma and<br />
chronicity lead to excoriations, variable hypotrichosis and alopecia, lichenification<br />
and pigmentary disturbances especially melanoderma and melanotrichia.<br />
Ventral insect hypersensitivity is characterised by pruritus with or without crusted<br />
papules, beginning on the ventral thorax and abdomen, axillae and groin. The legs<br />
and intermandibular space are <strong>of</strong>ten involved. Secondary changes may occur as<br />
above. Horses with insect bite hypersensitivity rarely have involvement <strong>of</strong> the flanks.<br />
In addition, horses with insect hypersensitivity uncommonly develop urticaria and<br />
when they do it is typically papular.<br />
Secondary bacterial folliculitis is not uncommon. Affected horses may suffer<br />
behavioural changes (anxious, nervous, restless, aggressive) and be unfit for riding,<br />
showing or working. Some horses will lose weight due to the constant irritation.<br />
Some horses have concurrent atopic disease or adverse food reactions which can<br />
greatly complicate the diagnostic work-up and therapeutic management.<br />
Diagnosis<br />
The differential diagnosis will vary according to the distribution <strong>of</strong> lesions. The<br />
definitive diagnosis is based on history, physical examination, ruling out other<br />
conditions and response to insect control.<br />
Intradermal testing with insect extracts, especially Culicoides is usually positive with<br />
insect hypersensitivity. Reactions may be present at 30 minutes (immediate), 4-6 hrs<br />
(late phase) and 24-48hrs (delayed) or combinations <strong>of</strong> these. Normal horses can<br />
have positive reactions and the prevalence <strong>of</strong> positive reactions in normal horses<br />
increases with increasing age.<br />
Antibodies against Culicoides and Stomoxys have been detected in the serum <strong>of</strong><br />
affected horses by ELISA. Other investigators have found no difference in ELISA<br />
scores using Culicoides extract between normal horses and horses with insect<br />
hypersensitivity. The diagnostic value <strong>of</strong> ELISA results is presently undocumented.<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 91
The typical histologic appearance <strong>of</strong> insect hypersensitivity is a superficial and deep<br />
perivascular to interstitial eosinophilic dermatitis with focal areas <strong>of</strong> infiltrative to<br />
necrotising eosinophilic mural folliculitis and focal eosinophilic granulomas. These<br />
changes are not pathognomonic for insect hypersensitivity and may be seen with<br />
adverse food reactions and atopic dermatitis<br />
Treatment<br />
The management <strong>of</strong> insect hypersensitivity involves insect control and the use <strong>of</strong><br />
topical and systemic antipruritic agents. Treatment <strong>of</strong> unrugged, grazing horses<br />
is difficult and frustrating. Secondary bacterial infections must be recognized and<br />
treated.<br />
Insect control<br />
92<br />
• Stable horses between 4pm and 8am<br />
• Cover horses with rugs and hoods<br />
• Use fine mesh screens in stables<br />
• Spray housing and screens with residual insecticides<br />
• Install floor or overhead fans in stables<br />
• Time operated spray mist insecticide systems are useful but expensive<br />
• Drain lakes, marshes, swamps, irrigation channels<br />
Fly repellents and insecticides<br />
• 4% permethrin (Permoxin ® Dermcare Vet Pty Ltd); use a 0.1% solution as<br />
a spray or rinse daily for 7 days then once a week<br />
• 0.2% fenvalerate (Sumifly Buffalo Fly Insecticide ® Fort Dodge); use 0.1%<br />
solution and apply 800ml to 1L on dorsal midline and body every 7 days<br />
• 0.15% pyrethrin, piperonly butoxide, N-octyl bicycloheptene dicarboxamide,<br />
di-N-propylisocinchromeronate, citronella (Musca-Ban Insecticidal spray ®<br />
Country Lfe Animal Health) spray/wipe-on<br />
• 0.2% pyrethrin, piperonyl butoxide, N-octyl bicycloheptene dicarboxamide,<br />
di-N-propylisocinchromeronate, diethyltoluamide, (N-Dem spray Insecticidal<br />
Lotion and Spray ® Joseph Lyddy)<br />
• 0.2% pyrethrin, diethyltoluamide, N-octyl bicycloheptene dicarboxamide, di-<br />
N-propylisocinchromeronate, benzalkonium chloride (Fly-Repella cream ®<br />
Troy Laboratories)<br />
• Commercial bath oils diluted with equal parts <strong>of</strong> water has been reported<br />
anecdotally as a useful leave on repellent<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005
• Cattle ear tags impregnated with pyrethroids braided into manes and tails and<br />
attached to halters<br />
• Maintaining a continuous film <strong>of</strong> liquid film <strong>of</strong> mineral oil on paraffin is<br />
reportedly useful to prevent Culicoides gnats from crawling down the hairs to<br />
the skin<br />
Antipruritic therapy<br />
Topical<br />
• Cold water<br />
• Colloidal oatmeal shampoo Episoothe ® Virbac or Aloveen ® Dermcare-<br />
Vet Pty Ltd<br />
• 0.2% benzyl benzoate Ectosol ® Troy Laboratories<br />
Systemic<br />
Antihistamines have limited effect<br />
• Chlorpheniramine 0.25 to 0.5mg/kg q 12 hours PO<br />
• Doxepin 0.5 to 0.75mg/kg q 12 hours PO<br />
• Amitryptilline 1mg/kg q 12 hrs PO<br />
Corticosteroids<br />
• Methyl prednisolone acetate 200mg IM<br />
• Triamcinolone acetonide 0.02 to 0.04 mg/kg IM<br />
• Prednisolone 2 mg/kg PO q 24 hrs induction dosage for 5 days reducing to<br />
1mg/kg q 24 hrs for 5 days reducing to 1mg/kg q 48 hrs<br />
• Dexamethasone 0.2mg/kg PO q 24hrs induction dosage for 5 days<br />
reducing to 0.1mg/kg q 24 hrs for 5 days reducing to 0.05 to 0.1mg/kg q 72<br />
hrs<br />
Fatty acids<br />
• Linseed oil<br />
• Flaxseed oil<br />
• Commercial fatty acid supplements<br />
Immunotherapy<br />
• The usefulness <strong>of</strong> allergen specific immunotherapy (ASIT) in equine insect<br />
hypersensitivity is unclear. Early attempts to use immunotherapy were<br />
reported to be unsuccessful. A few horses that had positive reactions to only<br />
mosquito or black fly extracts appear to respond well.<br />
• A small study was conducted using 14 horses in a double-blinded, placebocontrolled<br />
fashion using an aqueous whole body extract <strong>of</strong> C.variipenis. T<strong>here</strong><br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 93
94<br />
was no difference in response to the Culicoides extract compared to placebo<br />
but the study only lasted 6 months.<br />
• Another small open study using 10 horses used a whole body C.variipenis<br />
extract in adjuvant (mycobacterial cell wall fraction). Injections were<br />
administered subcutaneously every 6 to 10 days for first year then every<br />
month for the second year. After two years 8/10 horses had moderate to<br />
complete control <strong>of</strong> pruritus. This protocol should be repeated in a doubleblinded,<br />
placebo controlled fashion in a larger number <strong>of</strong> horses.<br />
Control<br />
• Affected animals should not to be used for breeding due to the <strong>here</strong>ditary<br />
nature <strong>of</strong> insect hypersensitivity<br />
References<br />
Anderson GS et al: Immunotherapy trial for horses in British Columbia with<br />
Culicoides hypersensitivity. J Med Entomol 33: 458, 1996<br />
Barbet JL et al Specific immunotherapy <strong>of</strong> Culicoides hypersensitive horses: a double<br />
blind study. Equine Vet J 22:232, 1990<br />
Brostrom H et al Allergic dermatitis (sweet itch) <strong>of</strong> Icelandic horses in Sweden: an<br />
epidemiological study. Equine Vet J 19:229, 1987<br />
Fadok VA: Culicoides hypersensitivity. In:Robinson NE (ed). Current Therapy in<br />
Equine Medicine II. WB Saunders Co. Philadelphia, PA, 1987, p 624<br />
Fadok VA, Greiner EC: Equine insect hypersensitivity: skin test and biopsy results<br />
correlated with clinical data. Equine Vet J 22: 236, 1990<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005
How I treat: equine<br />
pemphigus foliaceus<br />
Ralf Mueller<br />
Pemphigus foliaceus (PF) is an autoimmune disease, directed against desmosomes in<br />
the stratified squamous epithelium, leading to the loss <strong>of</strong> intracellular cohesion,<br />
acantholysis and blister formation within the epidermis (Halliwell 1979, Laing and<br />
others 1992, Scott and Miller 2003). It is the most common equine autoimmune<br />
skin disease (Scott and others 1987, Von Tscharner and others 2000). The first<br />
clinical article <strong>of</strong> pemphigus foliaceus in the horse was published by Barnick and<br />
Gutzeit in 1891. In 1981, the first histopathologic and immunopathologic<br />
documentation <strong>of</strong> equine PF in a horse was reported (Johnson and others 1981).<br />
The reported age in recent publications varied from 2 months (Laing and others<br />
1992) to 25.5 years (Zabel and others 2005). Most authors do not report breed, sex<br />
predilection or seasonality (Scott and others 1983, Pascal and others 1995, Von<br />
Tscharner and others 2000, Zabel and others 2005). Appaloosas were over<br />
represented in one study (Scott 1989).<br />
A retrospective study <strong>of</strong> 20 cases <strong>of</strong> equine pemphigus foliaceus reported an<br />
increased prevalence <strong>of</strong> disease between September and February (Vandanebeele and<br />
others 2004). Another recent retrospective study was not able to duplicate these<br />
findings (Zabel and others 2005). Scott (1989) and White (1992) reported a<br />
deterioration <strong>of</strong> disease in warm, humid, and sunny weather. Two horses (13%) in a<br />
recent case series showed evidence <strong>of</strong> seasonal disease deterioration. One <strong>of</strong> these<br />
horses, a Warmblood, did not show clinical signs during winter and deteriorated<br />
every summer when it was brought on a high altitude pasture. After the horse was<br />
kept in the valley permanently, no more clinical signs were noted (Zabel and others,<br />
2005). Environmental factors such as increased exposure to ultraviolet light may<br />
have been involved in the pathogenesis. The second horse was a research pony,<br />
which showed worsening <strong>of</strong> clinical signs in summer and also related to stress<br />
(anaesthesia, handling). Pemphigus foliaceus may be triggered by various factors<br />
such as stress, drug administration, systemic disease or Culicoides hypersensitivity<br />
(White 1992, Von Tscharner and others 2000), and the disease may wax and wane<br />
(Fadok 1995). Von Tscharner and others (2000) describe <strong>here</strong>ditary as well as<br />
infectious or environmental factors predisposing horses to pemphigus foliaceus, as<br />
the disease has been noted in unrelated horses living in the same area. The head and<br />
lower extremities have been reported as commonly affected sites (Von Tscharner<br />
and others 2000, Scott and Miller 2003). In a report <strong>of</strong> 8 horses with pemphigus<br />
foliaceus, a site predilection for the ventrum was found (Scott 1983). The disease<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 95
frequently generalizes within 1-3 months (Von Tscharner and others 2000, Scott and<br />
Miller 2003). The coronary band may show changes and may be the only affected<br />
site (Fadok 1995, Von Tscharner and others 2000). Other targets might be the<br />
prepuce or the mammary glands (Johnson 1997, Scott and Miller 2003). Pitting<br />
oedema <strong>of</strong> the lower extremities and the ventral abdomen is seen in over 50% <strong>of</strong> the<br />
cases (Manning 1983, Scott 1989, White 1992) and might be the only initial sign <strong>of</strong><br />
disease (Scott and Manning 1983, Schulte and others 1989, Von Tscharner and<br />
others 2000, Scott and Miller 2003). Urticaria can occur weeks before classical<br />
lesions such as pustules and/or crusts are seen (Von Tscharner and others 2000).<br />
Some authors state that horses may occasionally be pruritic, but more <strong>of</strong>ten are<br />
painful (Von Tscharner and others 2000, Scott and Miller 2003), others mention<br />
pruritus in 50% <strong>of</strong> the horses (Zabel and others 2005).<br />
The primary lesions in PF are vesicles, bullae and pustules. These lesions are very<br />
fragile and short-lived. Most <strong>of</strong>ten patients present with secondary lesions such as<br />
erosions, epidermal collarettes, crusts, alopecia, and scaling (Von Tscharner and<br />
others 2000, Scott and Miller 2003). Systemic signs like fever, depression, anorexia,<br />
lethargy and weight loss (Scott 1989, White 1992, Manning 1983), and nonregenerative<br />
anaemia, neutrophilia, hypoalbuminia, elevated alkaline phosphatase,<br />
elevated fibrinogen and hyperglobunemia may occur (George 1984, Edmond 1986,<br />
Day and others 1986, Scott and others 1987).<br />
Tests useful in the diagnosis <strong>of</strong> equine pemphigus foliaceus include direct smears,<br />
skin biopsies and immun<strong>of</strong>luorescence or immunohistochemical testing (Scott and<br />
Miller 2003). Cytology from crusted areas or intact pustules may show large<br />
numbers <strong>of</strong> neutrophils and acantholytic cells and is reported to be a useful test in<br />
the diagnosis <strong>of</strong> equine pemphigus foliaceus. Multiple biopsies from intact pustules<br />
or crusts are needed to confirm the diagnosis (Von Tscharner and others 2000).<br />
Primary dermatohistopathologic findings include subcorneal and/or intraepidermal<br />
pustules, associated with marked acantholysis (Scott 1989, Yaeger and Scott 1993,<br />
Von Tscharner and others 2000). In the absence <strong>of</strong> pustules, large numbers <strong>of</strong><br />
acantholytic cells and neutrophils found in the crusts are <strong>of</strong>ten the only diagnostic<br />
finding. As acantholysis may also be seen in dermatophytosis, special stains and<br />
fungal cultures are recommended (Scott and Miller 2003). Histopathology is<br />
reported to be far more reliable than immunopathologic testing in the diagnosis <strong>of</strong><br />
equine pemphigus foliaceus. (Scott and others 1984, Day and Penhale 1986, Griffith<br />
1987, Scott and Miller 2003).<br />
The prognosis for equine pemphigus foliaceus patients depends on age <strong>of</strong> onset.<br />
Younger horses (< 1 year) seem to have a better prognosis, the disease tends to be<br />
less severe, responds better to treatment and may spontaneously regress or not<br />
require further medication once in remission (Laing and others 1992, Von Tscharner<br />
and others 2000, Scott and Miller 2003). However, mature horses (> 5 years) have a<br />
less favourable prognosis and most require aggressive treatment (Von Tscharner and<br />
others 2000). Spontaneous remission is rare, but has been reported (White 1992,<br />
Amory and others 1997, Von Tscharner and others 2000, Scott and Miller 2003).<br />
96<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005
Treatment <strong>of</strong> pemphigus foliaceus in the horse requires immunosuppressive therapy.<br />
Due to financial reasons, the most commonly used drugs are glucocorticoids (Scott<br />
and Miller 2003, von Tscharner and others 2000). If prednisone is used and not<br />
effective, prednisolone or dexamethasone may be used successfully. The reason for<br />
this may be poor absorption, failure <strong>of</strong> hepatic conversion, possibly rapid secretion<br />
or a combination <strong>of</strong> these factors. Prednisone or prednisolone is given at 1-2<br />
mg/kg/day, the dexamethasone dose is 0.05-0.1 mg/kg/day. Treatment is altered to<br />
every other day once patients are in remission and doses may be reduced further<br />
depending on the individual situation. Long term remission after complete cessation<br />
<strong>of</strong> therapy has been reported and seems to be more common in young horses. The<br />
most feared adverse effect seen with glucocorticoids is laminitis. Corticosteroids<br />
may alter the flood flow in the ho<strong>of</strong> causing hypoxia in the lamina. They may also<br />
have a direct effect on epidermal cell metabolism. If unacceptable adverse effects<br />
are noted or if the response to glucocorticod treatment is unsatisfactory,<br />
azathioprine or gold salts may be used. Azathioprine has been used for the<br />
treatment <strong>of</strong> immune-mediated skin disease in the horse at a dose <strong>of</strong> 1 mg/kg/day<br />
(Scott and Miller 2003). It is associated with bone marrow suppression and<br />
occasional acute liver toxicity in dogs and humans, however, this has not been noted<br />
in the horses treated so far. The reason for this lack <strong>of</strong> adverse effects may be the<br />
low number <strong>of</strong> horses treated, poor oral absorption or a more rapid metabolisation<br />
<strong>of</strong> the drug in horses. Chrysotherapy is another option for the treatment <strong>of</strong> equine<br />
pemphigus foliaceus at a dose <strong>of</strong> 1 mg/kg IM weekly (Vandenabeele and others<br />
2004). However, aurothioglucose is currently not available in many countries. Dogs<br />
frequently develop secondary infections with immunosuppressive therapy. This is<br />
not seen <strong>of</strong>ten in horses.<br />
The prognosis <strong>of</strong> equine foliaceus should be given as guarded at first presentation.<br />
However, in some horses (particularly those with disease onset at young age) therapy<br />
can be discontinued without recurrence after it resulted in clinical remission, thus we<br />
always attempt treatment. In patients with financial constraints, glucocortocoids are<br />
used exclusively for therapy, but azathioprine or aurothioglucose may be used as<br />
steroid-sparing agents in horses with unacceptable treatment results or adverse<br />
effects, if owners are willing to accept the higher financial burden.<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 97
References<br />
AMORY, H., BECO, L., DESMECHT, D., JAQUINET, E., VANDENPUT, S.,<br />
LOMBA, F., (1996) Pemphigus foliace dans l’espece equine: Synthese at description<br />
de 2 cas. Annales de Medecine Veterinaire 141, 139- 148<br />
BARNICK, W. & GUTZEIT, R., (1891) Ein Fall von acutem Pemphigus beim<br />
Pferde. Zeitschrift Veterinär Kunde 3, 241-244<br />
DAY, M.J., PENHALE, W.J., (1986) Immunodiagnostics <strong>of</strong> autoimmune skin<br />
disease in the dog, cat and horse. <strong>Australian</strong> <strong>Veterinary</strong> Journal 63 (3), 65-68<br />
EDMOND, R.J., FREVERT, C., (1986) Pemphigus foliaceus in a horse. Modern<br />
<strong>Veterinary</strong> Practice 67, 527-530<br />
FADOK, V.A., (1995) An overview <strong>of</strong> equine dermatoses characterized by scaling<br />
and crusting. <strong>Veterinary</strong> Clinics <strong>of</strong> North America: Equine Practice11, 43-51<br />
GEORGE, L.W., WHITE S.L., (1984) Autoimmune Disease in Large Animals.<br />
<strong>Veterinary</strong> Clinics <strong>of</strong> North America: Large Animal Practice 6, 79- 86<br />
GRIFFITH, G., (1987) Pemphigus foliaceus in a Welsh Pony. Compendium on<br />
Continuing Education for the Practicing Veterinarian 9, 347-353<br />
HALLIWELL R.E., (1979) Skin disease associated with autoimmunity. <strong>Veterinary</strong><br />
Clinics <strong>of</strong> Northern America: Small Animal Practice 9, 57-71<br />
JOHNSON, M.E., SCOTT, D.W., MANNING, T.O., SMITH, C.A., LEWIS, R.M.,<br />
(1981) Pemphigus Foliaceus in the Horse. Equine Practice 3, 40-45<br />
LAING, J.A., ROTHWELL, T.L.W., PENHALE, W.J., (1992) Pemphigus foliaceus<br />
in a 2month-old foal. Equine <strong>Veterinary</strong> Journal 24 (6) 490-491<br />
MANNING, T.O., (1983) Pemphigus foliaceus. In: Current Therapy in equine<br />
medicine Ed Robinson NE. Philadelphia, WB Saunders Co. pp. 541-542<br />
PASCAL, A., SHIEBERT, J. IHRKE, PJ., (March 23 to 26, 1995) Seasonality and<br />
environmental risk factors for pemphigus foliaceus in animals. A retrospective study<br />
<strong>of</strong> 83 cases presented to the veterinary medical teaching hospital, University <strong>of</strong><br />
California Davis from 1976 to 1994. Proceedings <strong>of</strong> the 11 th Annual Meeting <strong>of</strong> the<br />
American Academy <strong>of</strong> <strong>Veterinary</strong> Dermatology/American <strong>College</strong> <strong>of</strong> <strong>Veterinary</strong><br />
Dermatology, Santa Fe, New Mexico, USA pp. 24-25<br />
SCOTT, D.W., (1989) Autoimmune Skin Diseases in the Horse. Equine Practice 11,<br />
20-32<br />
SCOTT, D.W. & Miller, W.H. (2003) Immune mediated Disorders. In: Equine<br />
Dermatology. Eds WB Saunders Co. Philadelphia. pp. 475- 547<br />
SCOTT, D.W., WALTON, D.K., SMITH, C.A., LEWIS, R.M., (1984) Pitfalls in<br />
immun<strong>of</strong>luorecscence testing in Dermatology. III. Pemphigus-like antibodies in the<br />
horse and direct immun<strong>of</strong>luorescence testing in equine dermatophilosis, Cornell<br />
Veterinarian 74, 305- 311<br />
98<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005
SCOTT, D.W., WALON, D.K., SLATER, M.R., SMITH, C.A. and LEWIS, R.M.<br />
(1987) Immune mediated dermatosis in domestic animals: ten years after.<br />
Compendium on Continuing Education for the Practicing Veterinarian 9, 424-435<br />
VANDENABEELE, S.I.J., WHITE, S.D., AFFOLTER, V.K., IHRKE, P.J. (2004)<br />
Pemphigus foliaceus in Horses: A retrospective study <strong>of</strong> 20 cases. <strong>Veterinary</strong><br />
Dermatology 15, 381-388<br />
VON TSCHARNER, C., KUNKLE G., YAGER, J., (2000) Stannard’s illustrated<br />
equine dermatology notes. <strong>Veterinary</strong> Dermatology 11, 172- 175<br />
WHITE, S.L., (1992) Bullous Autoimmune skin disease: diagnostics, therapy<br />
prognosis. Proceedings American Association for Equine Practice 28, 507<br />
YAEGER, J.A., SCOTT, D.W., (1993) The skin and appendages. In: Pathology <strong>of</strong><br />
Domestic Animals IV. Vol I. Ed Jubb, K.V.F. New York, Academic Press. p. 531<br />
ZABEL, S., MUELLER, R.S., FIESELER, K.V., BETTENAY, S.V.,<br />
LITTLEWOOD, J.D., WAGNER, R. Pemphigus foliaceus in the horse and pony –<br />
a retrospective study <strong>of</strong> 15 cases. <strong>Veterinary</strong> Record, in press.<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 99
Introduction<br />
100<br />
How I treat: equine phycomycosis<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005<br />
Reg Pascoe<br />
Chronic, subcutaneous, fungal, ulcerative, granulomatous, subtropical and tropical<br />
skin disease caused by Pythium insidiosum. Affects horses <strong>of</strong> all breeds, ages and sexes.<br />
Most cases occur in summer and autumn Other names include Bursatee, Florida<br />
horse leech, Swamp cancer.(Bridges & Emmons 1961, Blackford 1984 Scott & Miller<br />
2003)<br />
Aetiology / Pathophysiology<br />
Caused by Pythium spp., free-living aquatic organisms which are not true fungi. Horses<br />
become infected by standing for long periods in stagnant water with rotting organic<br />
material and high ambient temperatures. 30º C to 40º C favour infection. Damaged<br />
skin assists the entry <strong>of</strong> the organisms into the horse’s skin<br />
Clinical Presentation<br />
T<strong>here</strong> is no age, sex or breed predeliction. Pruritus occurs early in the infection with<br />
biting and kicking at affected area with subsequent ulceration <strong>of</strong> skin or wound<br />
Most lesions occur on legs and lower abdomen and chest. Lesions are usually single<br />
and unilateral but occasionally are multiple. Body lesions are <strong>of</strong>ten roughly circular<br />
with a sticky, serosanguineous, stringy discharge which either mats hairs or hangs<br />
from body wall in thick mucopurulent strands. Numerous irregular, gritty,coral like<br />
bodies (kunkers) occur within the necrotic sinuses found in the lesion. These are<br />
composed <strong>of</strong> fungal hyphae and tissue debris. Involvement <strong>of</strong> joint and tendons with<br />
sinus formation is a serious complication. Bone involvement is seldom seen in<br />
lesions less than four weeks old. Chronically affected horses may show invasion <strong>of</strong><br />
underlying bone commonest areas are the cannon bones sesamoids and phalanges<br />
Lymphadenopathy occurs in chronic cases<br />
Differential diagnosis<br />
Sarcoid, habronema infestation in wounds, neoplasms (especially sarcoids and<br />
squamous cell carcinomas), Mycetoma, Botryomycosis, excess granulation tissue,<br />
foreign body granulomas and other Zygomycetes.
Diagnosis<br />
History <strong>of</strong> access <strong>of</strong> horses to water-logged pasture or lagoon creeks, or inescapable<br />
rain flooded paddocks.<br />
Clinical signs <strong>of</strong> pruritus with serosanguineous stringy discharge is almost<br />
pathognomonic.<br />
Biopsy early lesions; send fresh sample for culture and culture immediately on<br />
selective media such as Campy blood agar or on Sabouraud's dextrose agar (if being<br />
transported for over 1 to 3 days, samples are better transported on ice packs and<br />
cultured on non-selective blood agar) (Grooters et al 2002).<br />
Histopathology<br />
Cytological examination <strong>of</strong> aspirates and direct smears shows granulomatous and<br />
pyogranulomatous inflammation with possible eosinophils. Fungal elements are<br />
<strong>of</strong>ten found in foci <strong>of</strong> necrotic material (kunkers) , Such findings are not definitive<br />
due to the similarity to the hyphae <strong>of</strong> Basidiobolus haptosporus and Conidiobolus coronatus<br />
Management<br />
T<strong>here</strong> are no reported cases <strong>of</strong> spontaneous remission with pythiosis.<br />
Surgical excision <strong>of</strong> the tumour is the most common and successful method,<br />
particularly in the more chronic cases. As the surgery can be both extensive and time<br />
consuming, general anaesthesia is usually preferred (Bridges & Emmons 1961,<br />
Bridges 1972, Restrepo et al 1980).<br />
Surgery on leg lesions is considerably aided if tourniquets are used above the surgical<br />
area. Careful dissection over tendon and joint locations is important and in some<br />
cases, close application <strong>of</strong> tumour to joint capsule and tendon sheath makes the<br />
surgical approach extremely difficult. Due to the extensive nature <strong>of</strong> the draining<br />
holes and sinus, the skin edges <strong>of</strong>ten cannot be closed.<br />
Strong iodine is packed into the surgical area and pressure bandages are applied to<br />
the lesion. These are left in situ for 2-3 days, and once granulation has commenced,<br />
the wound can be left unbandaged. Local application <strong>of</strong> strong iodine (10%) may<br />
have some beneficial effect. Repeat surgery is more usual than not when the lesions<br />
occur around tendons and joints.<br />
Intravenous medication with sodium iodide, 1g/15kg b.w. twice at weekly intervals<br />
(Pascoe 1973) is a useful adjunct to surgery, and also aids in the reduction <strong>of</strong> some<br />
abdominal growths <strong>of</strong> excessive size. Amphotericin B was used both systemically<br />
and topically (McMullan et al 1977). Intravenous treatment was well tolerated at an<br />
average daily dose starting at 0.38 mg/kg and increasing to as high as 1.47 mg/kg.<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 101
They concluded that ideal treatment would be early surgical removal <strong>of</strong> the lesion,<br />
followed by daily intravenous and topical administration <strong>of</strong> Amphotericin B, with<br />
periodical extirpation <strong>of</strong> small necrotic tracts as necessary. Cost and a fairly high risk<br />
<strong>of</strong> nephrotoxicity due to Amphotericin B may be a deterring factor and more<br />
recently some strains <strong>of</strong> Pythium have shown resistance to amphotericin B (Eaton<br />
1993).More recent information has cast serious doubt on the efficacy <strong>of</strong> parentral<br />
Amphoteracin B and parentral treatment is now questionable<br />
Local treatment:<br />
After surgical removal <strong>of</strong> the tumour, Amphotericin B (50g Amphotericin B in 10ml<br />
sterile water) + 10ml DMSO in gauze was applied and bandaged in place. Treatment<br />
is continued daily for at least 1 week.<br />
More recently a severe case involving bone lesions in a mare was treated by surgery<br />
followed by daily packing with Ketaconazole, Rifampin, DMSO and 2N HCI applied<br />
to the wound cavity under bandages pre-coated with 10% Povidone-iodine ointment<br />
to stop leaking <strong>of</strong> the initial dressing. Immunotherapy was used as an adjunct to<br />
treatment in this case (Eaton 1993).<br />
Originally the production <strong>of</strong> a phenolised vaccine manufactured by the<br />
department <strong>of</strong> Tropical <strong>Veterinary</strong> Science, Townsville, showed indications <strong>of</strong><br />
success in the treatment <strong>of</strong> early lesions. Results <strong>of</strong> vaccination compare favourably<br />
with surgery and when used in conjunction with surgery, has given very good results.<br />
This is given in 2ml doses weekly for 2-6 weeks. Lesions show some regressions in<br />
7-10 days after the first injection, but reaction at the injection site can be moderate to<br />
severe. Indications <strong>of</strong> successful treatment are reduction <strong>of</strong> pruritus, drying <strong>of</strong><br />
exudate, expulsion <strong>of</strong> 'kunkers', fibrosis <strong>of</strong> granuloma and eventually, complete<br />
epithelialization (Miller 1981).<br />
Recently two types <strong>of</strong> vaccines were produced (Newton & Ross 1993), one being<br />
that originally developed in 1981 by Miller who produced a vaccine prepared with<br />
killed sonicated whole-cell hypha antigen <strong>of</strong> P. insidiosum.<br />
A second vaccine prepared by precipitation <strong>of</strong> soluble antigen from Pythium growth<br />
medium showed a similar cure rate with less side effects at the injection site and<br />
reportedly has a longer shelf life (Mendoza et al 1992). Successful treatment depends<br />
on a number <strong>of</strong> factors such as the age <strong>of</strong> the horse, general physical condition,<br />
previous treatment, age/size/site <strong>of</strong> the lesion and whether t<strong>here</strong> is bony<br />
involvement. Young fresh lesions <strong>of</strong> 2 weeks duration responded very well to<br />
immunotherapy alone, but if present for more than 2 months, t<strong>here</strong> was a poor<br />
response to this treatment (Mendoza et al 1992).<br />
Horses with infection in the bone have mostly died, even though they have some<br />
clinical improvement with surgery and post-operative medical treatment (Alfaro &<br />
Mendoza 1990).<br />
102<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005
These vaccines are not manufactured commercially at this time, but may be available<br />
on request from select diagnostic laboratories<br />
Prognosis<br />
Good for body wall lesions. Guarded for lesions involving joints and tendon.<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 103
Basidiobolus haptosporus<br />
Introduction<br />
A member <strong>of</strong> Zygomycetes, a soil saprophyte, causing lesions on chest, abdomen, head<br />
and neck. A similar disease to Pythiosis with several important clinical differences.<br />
Aetiology/Pathophysiology<br />
Characteristically this disease occurs in a much drier environment than Pythium,<br />
usually in dusty conditions. Lives in the soil. Injury allows entry to horse’s body.<br />
Single lesions are common<br />
Clinical Presentation<br />
As for Pythiosis but growths are more shallow, are confined to neck and abdomen<br />
with no isolations on legs. Kunkers are small to non-existent. Pruritus is moderate to<br />
severe<br />
Differential diagnosis<br />
Pythiosis, mycetoma exuberant granulation tissue, habronema infestation, neoplasms,<br />
fibroblastic sarcoids.<br />
Diagnosis<br />
As for Pythiosis infection. Occurs in drier conditions and organisms probably live in<br />
soil. "Kunkers" are smaller and few in number. Fungal hyphae found in foci <strong>of</strong><br />
necrosis.<br />
Biopsy: culture punch samples direct into Sabouraud’s dextrose agar.<br />
Management<br />
Surgery is curative if all affected tissue is removed. Sodium iodide 1g/15kg b.w.<br />
given intravenously twice weekly as a 3.5% solution in normal Sodium chloride<br />
solution. No vaccine is available.<br />
Prognosis<br />
Guarded to good.<br />
104<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005
References<br />
Alfaro AA & Mendoza L (1990) - Four cases <strong>of</strong> equine bone lesions caused by<br />
Pythium insidiosum; Equine vet J 22(4):295-297<br />
Blackford J (1984) - Superficial and deep mycosis in horses; Vet Clinics Nth Am<br />
LargeAnimal Practice 6:1<br />
Bridges CH & Emmons CW (1961) - A Phycomycosis <strong>of</strong> Horses caused by<br />
Hypomyces destruens; J Am vet med Ass 138:579<br />
Eaton SA (1993) - Osseous involvement by Pythium insidiosum. Compend Contin<br />
Educ Pract 15(3) 485-488<br />
Grooters AM et al (2002) Evaluation <strong>of</strong> microbial culture techniques for the<br />
isolation <strong>of</strong> Pythium insidiosum from equine tissues: J Vet Diag Invest 14 288<br />
McMullan WC, Joyce JR, Henselka DV & Heitmann JM (1977) - Amphotericin B<br />
for the treatment <strong>of</strong> localised subcutaneous Phycomycosis in the horse: J Am vet<br />
med Ass 170:1293<br />
Mendoza L, Villalobos J, Calleja CE et al (1992) - Evaluation <strong>of</strong> two vaccines for the<br />
treatment <strong>of</strong> Pythium insidiosum in horses; Mycopathologia 119:89-95<br />
Miller RI (1981) - Treatment <strong>of</strong> equine Phycomycosis by immunotherapy and<br />
surgery Aust vet J 57:377-382<br />
Newton JC& Ross PS (1993) Equine pythiosis: an overview<strong>of</strong> immunotherapy<br />
Comp Cont Educ Prac Vet 15:491<br />
Pascoe RR (1973) The nature and treatment <strong>of</strong> skin conditions observed in horses in<br />
Queensland Aust vet J 49:35-40<br />
Scott DW & Miller WH (2003) Equine Dermatology Elsevier Science (USA)<br />
Philadelphia PA . USA<br />
Restrepo LF, Morales LF, Robledo M, Restrepo A, Tenica C & Correa de I (1973) -<br />
Antioquia Medica 23:13-25, cited by RI Miller (1980) Treatment <strong>of</strong> Equine<br />
Phycomycosis by Immunotherapy and Surgery; Aust vet J 57:377-382<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 105
106<br />
How I treat: equine dermatophytosis<br />
Introduction:<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005<br />
Greg Burton<br />
Dermatophytes are a group <strong>of</strong> septate fungi that invade keratinised tissues (skin, hair<br />
and nails). The infectious stage is the arthroconidia (arthrospores). Arthrospores are<br />
released from hyphal fragmentation and have been reported to remain viable in<br />
environs for up to 12 months. Dermatophytic fungi <strong>of</strong> the genera Microsporum and<br />
Trichophyton have been isolated from equine cases <strong>of</strong> dermatophytosis including,<br />
M. canis, M. equinum, M. gypseum, * T. equinum, T. equinum var autotrophicum,<br />
T. verrucosum and T. metagrophytes var. mentagrophytes. A number <strong>of</strong> other<br />
species are also isolated in rare cases.<br />
* T. equinum is the most commonly isolated dermatophyte in horses<br />
Pathogenesis:<br />
Clinical lesions seen in dermatophytosis will vary depending on the virulence <strong>of</strong> the<br />
dermatophyte and the immunological response <strong>of</strong> the host. Young horses (< 2 years)<br />
and immunocompromised horses may have increased susceptibility. Infection occurs<br />
via direct or indirect contact with arthrospores in epithelial debris. Arthrospores<br />
ad<strong>here</strong> to keratinised tissue and germinate within 6 hours. Trauma to the skin (tack<br />
rub, arthropods, scratching) and warmth and wetting <strong>of</strong> the skin (sweating,<br />
macroclimate) can facilitate germination. Race tracks and horse studs provide<br />
grouped, working horses that combined with the right climatic conditions can create<br />
an ideal situation for rapid spread <strong>of</strong> dermatophytes.<br />
The incubation period post inoculation has been reported as 7 to 42 days.<br />
Dermatophytes produce keratinases to assist penetration into the hair cuticle and<br />
grow downward in the follicle until they reach the keratogenous zone. Active keratin<br />
production (growing hairs) is needed to maintain the infection within the follicle.<br />
Large numbers <strong>of</strong> arthrospores are produced and spread to neighboring follicles.<br />
Centrifugal growth gives the characteristic annular appearance to the lesion.<br />
Experimentally T. equinum infections will continue to enlarge for 3 to 10 weeks and<br />
heal within 5 to 14 weeks.<br />
As with any infectious disease the host’s response to the pathogen plays a major role<br />
in determining the clinical lesions. Inflammatory changes in the skin may be induced
y a variety <strong>of</strong> fungal metabolites. T equinum produces urease, gelatinase, protease,<br />
hemolysins, keratinases and lipases. Trichophyton spp<br />
have been shown to produce proteolytic enzymes capable <strong>of</strong> inducing acantholysis.<br />
As well as pro-inflammatory metabolites T. mentagrophytes produces mannans that<br />
may inhibit T cell responses and reduce epidermal turnover (exfoliation being an<br />
innate defence mechanism <strong>of</strong> the skin to surface microbes). Concurrent bacterial<br />
infection is sometimes seen in dermatophytosis and dermatophytes may liberate<br />
penicillin-like substances that result in the formation <strong>of</strong> penicillin resistant bacteria<br />
from affected skin.<br />
T<strong>here</strong> seems to be a lack <strong>of</strong> specific immunological studies in the equine however<br />
based on other species it would appear that spontaneous resolution is associated<br />
with the development <strong>of</strong> cell mediated immunity (IFNγ and IL2). T<strong>here</strong> does not<br />
appear to be any correlation with antibody titres. Recovered horses from T equinum<br />
and M. gypseum infections are reported to be resistant to re-infection with<br />
dermatophytes <strong>of</strong> the same species.<br />
Clinical features:<br />
Dermatophytosis is a follicular infection so the common clinical symptom is <strong>of</strong><br />
folliculitis. This may include hive like follicular tufts, annular, peripherally expanding<br />
areas <strong>of</strong> alopecia with variable scaling or crusting, classical ring lesion with peripheral<br />
papules, coalescing areas forming serpiginous patterns <strong>of</strong> alopecia, exudative lesions<br />
on the caudal fetlocks “grease heal” and rarely subcutaneous and dermal nodules<br />
(dermatophytic pseudomycetoma). Pruritus is minimal or absent unless complicated<br />
by ectoparasites and pain is uncommon unless complicated by Staphylococcal<br />
folliculitis.<br />
Lesions in dermatophytosis are most commonly seen on the face, neck, dorsolateral<br />
thorax and the girth area. It has been reported that dermatophytosis affecting the<br />
girth is most likely to be T equinum (fomite transmission) and that M. gypseum is most<br />
commonly isolated from face, neck, legs and rump (geophylic fungus spread via<br />
arthropods). T verrucosum is reported to have a thicker, grayish crust. Due to clinical<br />
overlap, lesion type and location should not be relied on to identify species <strong>of</strong><br />
dermatophyte involved.<br />
Zoonotic factors:<br />
T equinum, T. verrucosum and M. canis all have zoonotic potential<br />
Differential diagnoses:<br />
Other folliculitides<br />
- Staphylococcal folliculitis<br />
- Dermatophilosis<br />
- Pemphigus foliaceous<br />
- Eosinophilic folliculitis<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 107
Dermatophytic pseudomycetoma requires differentiation from other infectious and<br />
inflammatory granulomas and neoplasia.<br />
Diagnosis:<br />
History<br />
- Affected in-contact animals or people<br />
- Duration and progression <strong>of</strong> the lesion<br />
Diagnostic tests<br />
- Wood’s lamp <strong>of</strong> limited value in the horse<br />
- Trichogram to identify hyphae and arthrospores, sensitivity <strong>of</strong> 54 to 64%<br />
- Acetate tape looking for hyphae<br />
- Pustule cytology (acantholytic form)<br />
- Culture, standard dermatophyte test media <strong>of</strong> limited use (specific culture<br />
requirements needed for some species)<br />
- Histopathology and PAS stains<br />
Treatment:<br />
Spontaneous remission usually occurs in healthy horses within 12 weeks. Treatments<br />
are aimed at shortening the duration <strong>of</strong> the lesions in the infected horse, reducing<br />
the discomfort associated with the inflammation and restriction <strong>of</strong> transmission to<br />
other animals.<br />
Step 1.<br />
108<br />
- Isolation <strong>of</strong> infected horses<br />
- Identify and control concurrent health, environmental and nutritional<br />
issues<br />
- Reduce work load on horse<br />
Step 2.<br />
- Topical antifungals<br />
- Systemic antifungal therapy?<br />
- Antibiotic therapy?<br />
Step 3.<br />
- Environmental decontamination<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005
Authors recommendations:<br />
1. Both Imaverol ® (0.2% enilconazole rinse) and Malaseb ® (2% chlorhexidine<br />
2% miconazole, Dermcare Vet) appear effective at reducing the duration <strong>of</strong><br />
disease. I am happy to use either and recommend weekly to twice weekly whole<br />
body treatments<br />
2. I also recommend the use <strong>of</strong> Lamisil ® ointment (terbinafine) to individual<br />
lesions w<strong>here</strong> practical twice daily<br />
3. I do not recommend the use <strong>of</strong> systemic antifungals in horses with<br />
dermatophytosis<br />
4. I find concurrent bacterial folliculitis uncommon with the exception <strong>of</strong> disease<br />
involving the lower limbs. This generally responds to Trimidine powder 15 to<br />
30mg/kg bid for 3 to 4 weeks.<br />
5. I have no personal experience with dermatophytic pseudomycetoma but the<br />
literature suggests these lesions are usually singular and surgery is curative.<br />
Environmental decontamination:<br />
1. Washable surfaces, tack, blankets grooming equipment should be treated with<br />
0.2% enilconazole twice at 10 day intervals.<br />
2. Tack, grooming equipment should not be shared with other horses.<br />
3. Straw, bedding materials that are not treatable should be destroyed.<br />
Prophylaxis<br />
1. Recovered animals are unlikely to be infected again.<br />
2. Attenuated live and inactivated T. equinum vaccines have been used in Europe<br />
and the USA respectively. Vaccines were administered intramuscularly on two<br />
occasions, 14 days apart. Both vaccines were effective at preventing or reducing<br />
the severity <strong>of</strong> disease with both experimental and naturally occurring challenges.<br />
Points for discussion.<br />
1. IDEXX laboratories report zero equine dermatophyte cultures in the last 18<br />
months. Is identifying the species important?<br />
2. Topically applied porphyrins followed by UVA therapy has been shown to be<br />
effective in human dermatophytosis. This may support the anecdotal reports that<br />
equine dermatophytosis resolves more rapidly in sunny conditions.<br />
3. Trichophyton spp antigens have been demonstrated to cause IgE mediated<br />
reactions in humans with asthma and clinical severity <strong>of</strong> asthma has been<br />
reduced with antifungal therapy. Any role for antifungal therapy in COPD in<br />
horses?<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 109
How I treat: equine chorioptic mange<br />
110<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005<br />
Janet Littlewood<br />
Equine chorioptic mange is caused by the surface-living mange mite Chorioptes bovis<br />
var equi. Mites are principally found on the lower limbs <strong>of</strong> horses with feat<strong>here</strong>d<br />
lower limbs, causing variable irritation and erythema, alopecia, exudation and<br />
crusting, although some infested animals may show only seborrhoea. Although leg<br />
mange is the usual clinical manifestation, infestation <strong>of</strong> the body may also occur.<br />
Clinical signs and mite numbers are higher in winter months, with mites thriving in<br />
groups <strong>of</strong> stabled horses and also surviving for prolonged periods <strong>of</strong>f the host, in the<br />
presence <strong>of</strong> epidermal debris, and dark, humid and cool conditions.<br />
T<strong>here</strong> are no licensed products for this disease in the United Kingdom, necessitating<br />
the use <strong>of</strong> drugs <strong>of</strong>f label, according to the “cascade” guidance on prescribing. T<strong>here</strong><br />
are a number <strong>of</strong> options open to the clinician, with varying amounts <strong>of</strong> evidence in<br />
support <strong>of</strong> each.<br />
Flumethrin is licensed for bovine chorioptic mange in Eire and mainland Europe<br />
and is available as a sheep scab and tick product in the UK; the 6% solution can be<br />
diluted 1:900 and applied at a dose rate <strong>of</strong> 30ml/kg, repeated in 14 days.<br />
Doramectin, eprinomectin and moxidectin have claims for bovine chorioptic mange<br />
in the USA. However, clinicians in the USA <strong>of</strong>ten use ivermectin at 0.3mg/kg per os<br />
weekly on 4 occasions.<br />
A published clinical trial with oral ivermectin paste given orally at the dose <strong>of</strong><br />
0.1mg/kg per os daily for 7-10 days or 0.2mg/kg twice at 2 week intervals,<br />
eliminated mites in 74% <strong>of</strong> treated horses, with only occasional mites in the<br />
remaining animals, w<strong>here</strong>as large numbers <strong>of</strong> mites remained in the control group<br />
(Littlewood et al 1995).<br />
Topical 2% lime sulfur washes are also used in the US, weekly for up to 6<br />
applications. A pilot study using 1% selenium sulphide shampoo was effective in<br />
treating 7 infested horses. Whole body washes were given on three occasions at 5<br />
day intervals; the hair was clipped from the limbs <strong>of</strong> two <strong>of</strong> the horses (Curtis 1998).<br />
The author has previously shown that chlorhexidine bathing had no curative effect<br />
in infested horses, although it assisted in controlling secondary bacterial infection.<br />
On the basis that fipronil is effective for a similar disease in dogs, cheyletiellosis, as<br />
well as for harvest mite infestation, 0.25% fipronil spray was used to treat a case <strong>of</strong>
chorioptic mange by the author (Littlewood 2000). A single application was<br />
successful in securing parasitic cure and resolution <strong>of</strong> all clinical signs. Subsequent to<br />
this a blinded, randomised, controlled clinical trial was undertaken in a group <strong>of</strong><br />
army horses with an endemic problem <strong>of</strong> leg mange. The lower limbs <strong>of</strong> infested<br />
horses were sprayed with either 0.25% fipronil spray or isopropyl alcohol vehicle, at<br />
a dose rate <strong>of</strong> 500ml per horse. Parasitological cure was achieved in all the horses in<br />
the verum group, but in none <strong>of</strong> the horses in the placebo group, after only a single<br />
application. (Littlewood 2001). Epidemiological work undertaken alongside this<br />
study revealed that horses may be subclinically affected. On the basis <strong>of</strong> this work<br />
the author's current recommendation is that all horses in contact with diseased<br />
patients, in addition to the clinically affected animals, should be treated and the<br />
environment should be thoroughly cleaned.<br />
In addition to the above options, many UK equine clinicians are using injections <strong>of</strong><br />
moxidectin, with anecdotal success and no reactions that have been reported to the<br />
author, and it is likely that a controlled trial may be undertaken in the near future.<br />
References:<br />
Curtis C F (1999) Pilot study to investigate the efficacy <strong>of</strong> a 1% selenium sulphide<br />
shampoo in the treatment <strong>of</strong> equine chorioptic mange. <strong>Veterinary</strong> Record 144, 674-675<br />
Littlewood J D (2000) Chorioptic mange; successful treatment with fipronil. Equine<br />
<strong>Veterinary</strong> Education 12, 144-146<br />
Littlewood J D (2001) Equine chorioptic mange: an epidemiological study and<br />
controlled clinical trial. RCVS Diploma Dissertation<br />
Littlewood JD, Rose JF & Paterson S (1995) Oral ivermectin paste for the treatment<br />
<strong>of</strong> chorioptic mange in horses. <strong>Veterinary</strong> Record 137, 661-663<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 111
Introduction<br />
112<br />
How I treat: equine vasculitis<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005<br />
Linda Vogelnest<br />
Vasculitis is an uncommon disease in the horse that most frequently affects the skin,<br />
however may affect multiple body organs. Cutaneous vasculitis can occur in a variety<br />
<strong>of</strong> clinical forms and is characterised by lesions <strong>of</strong> purpura, urticarial wheals, or<br />
necrosis and ulceration. Similarly to cutaneous vasculitis in other animals and<br />
humans, disease aetiology and pathogenesis are complex and incompletely<br />
understood. A diverse range <strong>of</strong> triggering primary aetiological events underlies this<br />
disease in humans, including inflammatory, autoimmune and malignant diseases,<br />
although ~50% cases remain idiopathic. In the horse, clearly identified aetiological<br />
agents include bacterial infections (Streptococcus equi or zooepidemicus [“strangles”],<br />
Salmonella spp., and Corynebacterium pseudotuberculosis); and viral infections (equine<br />
influenza and equine viral arteritis). Drugs (eg phenylbutazone, vaccines), immunemediated<br />
colitis, cholangiohepatitis, omphalitis in foals, photo-activation, and<br />
neoplasia have also been implicated in disease aetiology, however many cases <strong>of</strong><br />
equine cutaneous vasculitis remain idiopathic.<br />
Disease Pathogenesis<br />
Both immunological and non-immunological mechanisms have been implicated in<br />
disease pathogenesis; however immune-complex deposition and damage to small<br />
vessels, most <strong>of</strong>ten postcapillary venules, is reportedly the most common mechanism<br />
in humans and <strong>of</strong> proposed importance in animals. A complex series <strong>of</strong> events<br />
leading to disease may include initial antigenic stimulation, local immune complex<br />
deposition & inflammatory-mediator release (TNF-α, IFN-γ, IL-1, IL-4, IL-8),<br />
complement activation, increased local endothelial cell adhesion molecule expression<br />
(LFA-1, ICAM-1, E-selectin, P-selectin), coagulation (enhanced by plasminogen<br />
activator inhibior-1 [PAI-1]), and immunological response to initial inflammation (eg<br />
dermal dendritic cells, LH cells and T cells) further enhancing inflammation.<br />
Disruption to blood flow in affected vessels may result from inflammatory cell attack<br />
<strong>of</strong> vessel walls (which may be neutrophilic, lymphocytic or rarely eosinophilic or<br />
granulomatous, classically resulting in leukocytoclastic changes), inflammatory<br />
mediator damage to endothelial cells (producing primarily hyalinisation), or<br />
thrombogenic or hypercoagulable states (w<strong>here</strong> thrombosis predominates).
Clinical Disease<br />
The clinical result <strong>of</strong> disruption to blood supply from cutaneous vasculitis is lesions<br />
that range in severity from wheals, papules, purpura, erythema and oedema if acute;<br />
to alopecia and scarring if mild and chronic; to areas <strong>of</strong> well-demarcated necrosis,<br />
ulceration and crusting if severe. Lesions occur most commonly on the distal limbs,<br />
pinnae, lips and periocular areas. Diascopy confirms purpura as erythemic lesions<br />
that will not blanch. Signs <strong>of</strong> systemic illness, including pyrexia, lethargy, decreased<br />
appetite and weight loss may accompany cutaneous lesions. Forms <strong>of</strong> cutaneous<br />
vasculitis recognised in horses include:<br />
1. Purpura Haemorrhagica - is reported as the most common form <strong>of</strong><br />
cutaneous vasculitis in the horse. It is an acute disease characterised by extensive<br />
oedematous swelling <strong>of</strong> the distal limbs, ventral abdomen, and sometimes face and<br />
muzzle, and typically concurrent signs <strong>of</strong> systemic illness. Incidence is low and<br />
sporadic, with most affected horses greater than 2 years <strong>of</strong> age, and no apparent<br />
breed or sex predispositions. This syndrome may occur within 2-4 weeks <strong>of</strong> a<br />
respiratory infection (Streptococcus equi or zooepidemicus), or other potential triggering<br />
factors or disease. Urticaria may occur initially, and progress to oedema that is<br />
usually well-demarcated, painful, symmetrical, and involving all four limbs. Severely<br />
affected areas may have surface serum exudation and progress to necrosis and<br />
ulceration. Petechiae and ecchymoses may be present on mucous membranes. Most<br />
affected horses have obvious signs <strong>of</strong> depression and are reluctant to move,<br />
anorexic, tachycardic, tachypnoeic, and <strong>of</strong>ten pyrexic. T<strong>here</strong> is a wide variation in<br />
severity and clinical course.<br />
2. Subacute Pastern Vasculitis – is proposed to be a relatively common<br />
although poorly characterised entity in the horse. Lesions primarily occur on nonpigmented<br />
lower limbs, and may be more prevalent in animals on pasture. Sunlight<br />
exposure and photactivation are proposed aetiological factors in some cases,<br />
however appear uninvolved in others. Early lesions include erythema and<br />
oedematous swelling, which progress to serum exudation, necrosis, crusting and<br />
ulceration. Pain on palpation is <strong>of</strong>ten present, and pruritus absent. Chronic lesions<br />
may be alopecic, scaling, lichenified, and proliferative.<br />
Diagnosis<br />
Definitive diagnosis <strong>of</strong> cutaneous vasculitis requires consistent history, clinical<br />
lesions, and histopathological changes. In acute disease varying degrees <strong>of</strong> specific<br />
vessel wall changes may be identified, including disproportionately more leukocytes<br />
within vessel walls than surrounding perivascular areas, leukocytoclasis within or<br />
adjacent to walls, fibrinoid necrosis, and vessel thrombosis. Less specific supportive<br />
changes include intense oedema, red cell extravasation, and endothelial cell swelling.<br />
T<strong>here</strong> may be evidence <strong>of</strong> cutaneous infarction if severe, and follicular atrophy<br />
(“faded follicles”) with chronic disease. Clear histological support for a diagnosis <strong>of</strong><br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 113
cutaneous vasculitis can be difficult to obtain, and similarly to other dynamic disease<br />
processes, multiple and repeat biopsies may be needed to confirm a diagnosis.<br />
Treatment<br />
Aggressive treatment for cutaneous vasculitis is indicated in severe disease to prevent<br />
extensive ulceration and limit tissue damage and scarring. Glucocorticoids are the<br />
cornerstone <strong>of</strong> therapy for severe cutaneous vasculitis in humans, with prednisolone<br />
considered the most reliable medication for reducing lesions and halting progression<br />
<strong>of</strong> disease. Similarly, prednisolone is widely used for treatment <strong>of</strong> equine cutaneous<br />
vasculitis, with oral doses <strong>of</strong> 2-4mg/kg once daily reported successful. In more<br />
recalcitrant cases, dexamethasone 0.2-0.4mg/kg once daily may be more effective at<br />
inducing response. Daily induction doses should be continued until the disease is in<br />
clinical remission and then gradually reduced, with alternate day dosing commenced<br />
as soon as possible. With severe or slowly responsive cases, reduction in dose by<br />
25% <strong>of</strong> the 48-hour dose per 10-14 days has been recommended to help limit<br />
relapse. Such high-dose glucocorticoid therapy should ideally be instituted<br />
concurrently with a management plan to minimise the risk <strong>of</strong> laminitis, as<br />
glucocorticoids, in particular triamcinolone or dexamethasone have been linked to an<br />
increased risk <strong>of</strong> this debilitating disease. Low energy diets, weight control, and<br />
regular gentle exercise are strongly recommended. In the acute stages <strong>of</strong> cutaneous<br />
vasculitis supportive care including hydrotherapy, walking and good skin hygiene can<br />
also be helpful.<br />
The clinical course <strong>of</strong> cutaneous vasculitis in any patient is difficult to predict, with<br />
some cases resolving completely within a few weeks, and others becoming chronic<br />
or recurrent. It is important to search thoroughly for underlying aetiological factors,<br />
especially in severe, chronic or recurrent cases, and treat promptly w<strong>here</strong>ver possible.<br />
Minimising factors likely to exacerbate vasculitis, such as excessive stress, heat or<br />
cold exposure is also proposed <strong>of</strong> help with human disease. The use <strong>of</strong> alternative<br />
immunomodulating drugs to glucocorticoids for equine cutaneous vasculitis appears<br />
unreported, however a range <strong>of</strong> other drugs have been used in human disease. For<br />
treatment <strong>of</strong> severe, chronic, or poorly responsive cutaneous vasculitis in humans,<br />
azathioprine, cyclophosphamide, methotrexate, or mycophenolate m<strong>of</strong>etil have been<br />
recommended. Little or no information is available on the use <strong>of</strong> these drugs in the<br />
horse, however expense likely limits their use regardless. For subacute and chronic<br />
disease in humans, drugs including colchicine, dapsone, sulphasalazine, and<br />
antimalarial agents can be effective alternatives or additions to prednisolone.<br />
Colchicine and dapsone primarily inhibit neutrophil chemotaxis and activation, so<br />
are theoretically most likely to be effective in neutrophilic vasculitis. Dapsone or<br />
sulphasalazine are reported to be effective steroid-sparing options in some forms <strong>of</strong><br />
canine cutaneous vasculitis. The author has used Dapsone in one horse with initial<br />
urticaria progressing to purpura haemorrhagica syndrome, at a dose <strong>of</strong> 1mg/kg twice<br />
daily for over 4 weeks concurrently with prednisolone. T<strong>here</strong> was apparent poor<br />
response, with continued rapid relapse on attempts to lower prednisolone dosage. In<br />
cutaneous vasculitis in humans caused primarily by thrombosis some further<br />
114<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005
treatment options have been used. Pentoxifylline, that modifies plasticity <strong>of</strong> red<br />
blood cells allowing easier passage through narrowed vessel lumina, along with a<br />
myriad <strong>of</strong> inhibitory effects on cytokines, leukocytes and endothelial cells, is an<br />
apparently safe and well-tolerated option with efficacy in both human and canine<br />
disease, although a lag phase <strong>of</strong> weeks to months to see beneficial effects is apparent<br />
in humans. Low-dose aspirin, anabolic steroids, anticoagulants, and<br />
niacinamide/tetracycline combinations have also been used.<br />
In summary, for acute cutaneous vasculitis in the horse, rapid treatment with<br />
prednisolone at immunosuppressive doses is currently the recommended treatment<br />
option. A search for underlying aetiological factors is vital, and a concurrent<br />
management plan to minimise risks <strong>of</strong> laminitis prudent, along with general<br />
supportive and wound care to help limit the debilitation <strong>of</strong> severe disease. For<br />
recalcitrant or recurrent cases with poor response or glucocorticoid side-effects,<br />
alternative options remain speculative, with little information available on efficacy or<br />
safety. More potent glucocorticoids such as dexamethasone or triamcinolone may be<br />
used to help induce remission in severe cases. Dapsone has been used in a steroidsparing<br />
role in at least one horse without evidence <strong>of</strong> benefit at the doses and<br />
duration chosen, but also without apparent adverse effects, and it may be used as a<br />
treatment option for poorly responsive or subacute disease. Screening for adverse<br />
haematopoietic or liver effects, which have been reported in humans with the use <strong>of</strong><br />
this drug, may be indicated. Pentoxifylline has been used safely in the horse, and<br />
could similarly be considered for poorly responsive or subacute disease, especially if<br />
t<strong>here</strong> is histological evidence <strong>of</strong> vessel thrombosis in the face <strong>of</strong> minimal<br />
inflammation. Gold salts are another option to consider for recalcitrant disease and<br />
have been used effectively and safely in horses with pemphigus foliaceus and some<br />
other immune-mediated diseases, although their use in equine vasculitis appears<br />
unreported, and they are not a recognised treatment option for cutaneous vasculitis<br />
in humans.<br />
References<br />
Equine Dermatology. Scott DW. WB Saunders, St. Louis, Mo. 2003: 522-546.<br />
Cutaneous Vasculitis Update. Gibson LE. Dermatologic Clinics 2001:19;4:603-615.<br />
Purpura haemorrhagica in 53 horses. Pusterla N, Watson JL, Affolter VK et al.<br />
<strong>Veterinary</strong> Record 2003. 153: 4, 118-121.<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 115
116<br />
Notes<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005
Notes<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005 117
118<br />
Notes<br />
ACVSC Proceedings Dermatology Chapter Science Week 2005