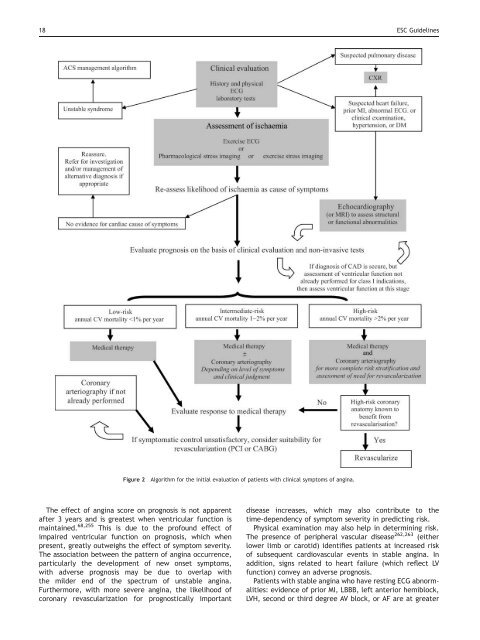
18 ESC <str<strong>on</strong>g>Guidelines</str<strong>on</strong>g>Figure 2Algorithm for <strong>the</strong> initial evaluati<strong>on</strong> <strong>of</strong> patients with clinical symptoms <strong>of</strong> angina.The effect <strong>of</strong> angina score <strong>on</strong> prognosis is not apparentafter 3 years and is greatest when ventricular functi<strong>on</strong> ismaintained. 68,255 This is due to <strong>the</strong> pr<strong>of</strong>ound effect <strong>of</strong>impaired ventricular functi<strong>on</strong> <strong>on</strong> prognosis, which whenpresent, greatly outweighs <strong>the</strong> effect <strong>of</strong> symptom severity.The associati<strong>on</strong> between <strong>the</strong> pattern <strong>of</strong> angina occurrence,particularly <strong>the</strong> development <strong>of</strong> new <strong>on</strong>set symptoms,with adverse prognosis may be due to overlap with<strong>the</strong> milder end <strong>of</strong> <strong>the</strong> spectrum <strong>of</strong> unstable angina.Fur<strong>the</strong>rmore, with more severe angina, <strong>the</strong> likelihood <strong>of</strong>cor<strong>on</strong>ary revascularizati<strong>on</strong> for prognostically importantdisease increases, which may also c<strong>on</strong>tribute to <strong>the</strong>time-dependency <strong>of</strong> symptom severity in predicting risk.Physical examinati<strong>on</strong> may also help in determining risk.The presence <strong>of</strong> peripheral vascular disease 262,263 (ei<strong>the</strong>rlower limb or carotid) identifies patients at increased risk<strong>of</strong> subsequent cardiovascular events in stable angina. Inadditi<strong>on</strong>, signs related to heart failure (which reflect LVfuncti<strong>on</strong>) c<strong>on</strong>vey an adverse prognosis.Patients with stable angina who have resting ECG abnormalities:evidence <strong>of</strong> prior MI, LBBB, left anterior hemiblock,LVH, sec<strong>on</strong>d or third degree AV block, or AF are at greater
ESC <str<strong>on</strong>g>Guidelines</str<strong>on</strong>g> 19Figure 3 Prognostic angina score. The pattern <strong>of</strong> angina occurrence can be used to predict prognosis. 80risk <strong>of</strong> future cardiovascular events than those with a normalECG. 45,264–267 It is possible that in an unselected populati<strong>on</strong>with stable angina <strong>the</strong> baseline risk is lower than in many <strong>of</strong><strong>the</strong> studies quoted accepting that many <strong>of</strong> <strong>the</strong>se studieshave been c<strong>on</strong>ducted in patients referred for fur<strong>the</strong>r angiographicevaluati<strong>on</strong>.Recommendati<strong>on</strong>s for risk stratificati<strong>on</strong> by clinical evaluati<strong>on</strong>,including ECG and laboratory tests in stable anginaClass I(1) Detailed clinical history and physical examinati<strong>on</strong>including BMI and/or waist circumference in allpatients, also including a full descripti<strong>on</strong> <strong>of</strong> symptoms,quantificati<strong>on</strong> <strong>of</strong> functi<strong>on</strong>al impairment, past medicalhistory, and cardiovascular risk pr<strong>of</strong>ile (level <strong>of</strong>evidence B)(2) Resting ECG in all patients (level <strong>of</strong> evidence B)Risk stratificati<strong>on</strong> using stress testingStress testing can take <strong>the</strong> form <strong>of</strong> exercise or pharmacologicalstress with or without imaging. Prognostic informati<strong>on</strong>obtained from stress testing relates not just to detecti<strong>on</strong><strong>of</strong> ischaemia as a simple binary resp<strong>on</strong>se, but also <strong>the</strong>ischaemic threshold, <strong>the</strong> extent and severity <strong>of</strong> ischaemia(for imaging techniques), and functi<strong>on</strong>al capacity (for exercisetesting). Stress testing al<strong>on</strong>e is insufficient to assess risk<strong>of</strong> future events. In additi<strong>on</strong> to <strong>the</strong> limitati<strong>on</strong>s <strong>of</strong> <strong>the</strong> differenttechniques in <strong>the</strong> detecti<strong>on</strong> <strong>of</strong> myocardial ischaemia,however small, it must also be recognized that ischaemiaper se is not <strong>the</strong> <strong>on</strong>ly factor which influences <strong>the</strong> likelihood<strong>of</strong> acute events. Several lines <strong>of</strong> evidence have shown that<strong>the</strong> majority <strong>of</strong> vulnerable plaques appear angiographicallyinsignificant before <strong>the</strong>ir rupture, and may not impinge <strong>on</strong>cor<strong>on</strong>ary flow to reveal characteristic changes during exerciseECG or stress imaging. This may explain <strong>the</strong> occasi<strong>on</strong>alacute cor<strong>on</strong>ary event that occurs shortly after a negativestress test result. Risk stratificati<strong>on</strong> with <strong>the</strong> exercise testshould be a part <strong>of</strong> a process that includes readily accessibledata from clinical examinati<strong>on</strong> and should not take place inisolati<strong>on</strong>. Thus <strong>the</strong> stress test is performed to provideadditi<strong>on</strong>al informati<strong>on</strong> regarding <strong>the</strong> patient’s risk status.Symptomatic patients with suspected or known CAD shouldundergo stress testing to assess <strong>the</strong> risk <strong>of</strong> future cardiacevents unless cardiac ca<strong>the</strong>terizati<strong>on</strong> is urgently indicated.However, no randomized trials <strong>of</strong> stress testing have beenpublished, and <strong>the</strong>refore <strong>the</strong> evidence base c<strong>on</strong>sists <strong>of</strong>observati<strong>on</strong>al studies <strong>on</strong>ly. The choice <strong>of</strong> initial stress testshould be based <strong>on</strong> <strong>the</strong> patient’s resting ECG, physicalability to perform exercise, local expertise, and availabletechnologies.Exercise ECG. The exercise ECG has been extensively validatedas an important tool in risk stratificati<strong>on</strong> in symptomaticpatients with known or suspected cor<strong>on</strong>ary disease.The prognosis <strong>of</strong> patients with a normal ECG and a low clinicalrisk for severe CAD is excellent. In <strong>on</strong>e study in which 37%<strong>of</strong> outpatients referred for n<strong>on</strong>-invasive testing met <strong>the</strong>criteria for low risk 261 fewer than 1% had LM stem arterydisease or died within 3 years. Lower-cost opti<strong>on</strong>s such astreadmill testing should <strong>the</strong>refore be used, whenever possible,for initial risk stratificati<strong>on</strong>, and <strong>on</strong>ly those withabnormal results should be referred to arteriography.The prognostic exercise testing markers include exercisecapacity, blood pressure resp<strong>on</strong>se, and exercise-inducedischaemia (clinical and ECG). Maximum exercise capacityis a c<strong>on</strong>sistent prognostic marker, this measure is at leastpartly influenced by <strong>the</strong> extent <strong>of</strong> rest ventricular dysfuncti<strong>on</strong>and <strong>the</strong> amount <strong>of</strong> fur<strong>the</strong>r LV dysfuncti<strong>on</strong> induced byexercise. 139,268 However, exercise capacity is also affectedby age, general physical c<strong>on</strong>diti<strong>on</strong>, comorbidites, andpsychological state. Exercise capacity may be measured bymaximum exercise durati<strong>on</strong>, maximum MET level achieved,maximum workload achieved in Watts, maximum heart rate,and double (rate–pressure) product. The specific variableused to measure exercise capacity is less important than<strong>the</strong> inclusi<strong>on</strong> <strong>of</strong> this marker in <strong>the</strong> assessment. In patientswith known CAD and normal, or mildly impaired LV functi<strong>on</strong>,5-year survival is higher in patients with a better exercisetolerance. 123,139,152,269,270O<strong>the</strong>r prognostic exercise testing markers are related toexercise-induced ischaemia and markers include changesin ST-segment (depressi<strong>on</strong> or elevati<strong>on</strong>), and exerciseinducedangina. McNeer et al. 270 dem<strong>on</strong>strated that anearly positive exercise test (ST-depressi<strong>on</strong> .1 mm in <strong>the</strong>first two stages <strong>of</strong> <strong>the</strong> Bruce protocol) identified a high-riskpopulati<strong>on</strong>, whereas patients who could exercise into stageIV were at low risk regardless <strong>of</strong> <strong>the</strong> ST resp<strong>on</strong>se. ST-segmentelevati<strong>on</strong> is observed most frequently in patients with ahistory <strong>of</strong> MI; in patients without infarcti<strong>on</strong>, ST-elevati<strong>on</strong>during exercise has been associated with severe transmuralmyocardial ischaemia.In <strong>the</strong> CASS Registry, 12% <strong>of</strong> medically treated patientswere identified as high risk <strong>on</strong> <strong>the</strong> basis <strong>of</strong> 0.1 mV <strong>of</strong>exercise-induced ST-segment depressi<strong>on</strong> and inability tocomplete stage I <strong>of</strong> <strong>the</strong> Bruce protocol. These patients hadan average mortality rate <strong>of</strong> 5% per year. Patients whocould exercise to at least stage III <strong>of</strong> <strong>the</strong> Bruce protocolwithout ST changes (34%) c<strong>on</strong>stituted <strong>the</strong> low-risk group(estimated annual mortality, less than 1%). 123Several studies have attempted to incorporate multipleexercise variables into a prognostic score. The clinicalvalue <strong>of</strong> stress testing is improved c<strong>on</strong>siderably by