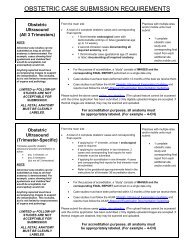
American Institute of Ultrasound in Medicine <strong>Proceedings</strong> J Ultrasound Med 32(suppl):S1–S134, 2013cesarean delivery. The primary outcome was risk of cesarean delivery inlabor. Groups were compared using Fisher exact and χ 2 tests with significancedefined as P < .05.Results—A total of 216 patients met inclusion criteria. At 22 to24 weeks, the mean CL was 35 mm (range, 4–60 mm); at 28 to 32 weeks,the mean CL was 29 mm (range, 3–54 mm). CL at 22 to 24 weeks was notsignificantly associated with the risk of cesarean delivery. However, CL at28 to 32 weeks was significantly associated with the risk of cesarean delivery(Table 1). A CL ≥50 mm (95th percentile) had sensitivity of 20%,specificity of 99%, a positive predictive value of 71.4%, and a negativepredictive value of 90.4% for cesarean delivery in labor (P < .001).Conclusions—CL at 28 to 32 weeks is significantly associatedwith the likelihood of cesarean delivery in labor; however, CL at 22 to 24weeks did not correlate with the risk of cesarean delivery. A longer CL inthe early third trimester may represent underdevelopment of the uterus,leading to a higher risk of cesarean delivery in labor. The lack of an associationat 22 to 24 weeks suggests that the normal cervical ripening processis one that occurs after the second trimester.Table 1. Risk of Cesarean Delivery in Labor by CL Quartile at 28 to 32 Weeks’GestationQuartile Cesarean Delivery, % (n) Vaginal Delivery, % (n)1st (3–23 mm) 5.6 (3/54) 94.4 (51/54)2nd (24–29 mm) 10.9 (6/55) 89.1 (49/55)3rd (30–36 mm) 9.1 (5/55) 90.9 (50.55)4th (37–54 mm) 21.2 (11/52) 78.8 (41/52)P
American Institute of Ultrasound in Medicine <strong>Proceedings</strong> J Ultrasound Med 32(suppl):S1–S134, 20131537208 Midtrimester Transabdominal Ultrasound for Detection ofPlacenta PreviaHayley Quant,* Alexander Friedman, Eileen Wang, SamuelParry, Nadav Schwartz Maternal and Child Health ResearchProgram, Obstetrics and Gynecology, University of PennsylvaniaPerelman School of Medicine, Philadelphia, PennsylvaniaUSAObjectives—Transvaginal ultrasound (TVUS) is the gold standardfor diagnosing placenta previa. Transabdominal ultrasound (TAUS)is often used as a screening test given the cost and invasiveness of TVUS.We sought to determine the ability of TAUS to diagnose previa.Methods—TAUS was performed prior to TVUS for allanatomic surveys at 18 to 23 6/7 weeks. Sonographers prospectivelyrecorded the distance from the leading placental edge (if visible) to the internalos on both TA and TV scans. The primary outcome was a TV placentaldistance of 0 cm (complete previa). Secondary outcomes includedTV distances of ≤1, ≤2, and ≤2.5 cm. ROC curves were generated usingall cases with TA placental distance of ≤5cm. The TA placental distancecutoffs at 100% and 90% sensitivity were identified for each outcome andthen applied to the entire cohort to determine the sensitivity, specificity,positive predictive value (PPV), and negative predictive value (NPV) ofTAUS for detecting previa.Results—A total of 1214 patients underwent both TAUS andTVUS; 415 (34.2%) had a TA distance ≤5cm from placenta to os. Theprevalence, optimal TA cutoffs by outcome and, test characteristics arepresented Table 1. A TA measurement of ≤4.2 cm detected 93.3% of completeprevias by TVUS with an NPV of 99.8% and a screen-positive rate(SPR) of 25%. A TA cutoff of 2.8 cm lowered the SPR to 11.4%, thoughthe sensitivity decreased to 86.7% and the NPV to 88.6%.Conclusions—Despite a high NPV, the lack of a cutoff to excludeplacenta previa makes TAUS an inadequate screen. Universal TVUSwould improve midtrimester detection and allow for appropriate followup.Since most suspected previas resolve, further investigation is neededto assess whether TVUS can decrease morbidity later in gestation.Table 1TVTA PlacentalPlacental Distance SPR, Sensitivity, Specificity, PPV, NPV,Distance Cutoff, cm % % % % %0 (complete previa) 4.2 25.0 93.3 76.7 9.2 99.8n = 30 (2.5%) 2.8 11.4 86.7 90.5 18.7 88.6≤1 cm 4.2 25.0 93.3 77.6 13.8 99.7n = 45 (3.7%) 3.1 13.5 84.4 89.2 23.2 99.3≤2 cm 4.9 32.9 89.0 72.2 22.3 98.7n = 100 (8.2%) 3.9 21.0 81.0 84.4 31.8 98.0≤2.5 cm 5.0 34.2 82.9 72.5 29.2 96.9n = 146 (12.0%) 4.2 25.0 76.7 82.0 36.8 96.31539742 Outcome of Pregnancies With a Low-Lying Placenta DiagnosedBetween 16 and 24 Weeks’ GestationHoward Heller, 1 Katherine Mullen, 1 * Robert Gordon, 1Rosemary Reiss, 2 Carol Benson 1 1 Radiology, 2 Obstetrics andGynecology, Brigham and Women’s Hospital, Boston,Massachusetts USAObjectives—To determine how often a low-lying placenta diagnosedbetween 16 and 24 weeks resolves prior to delivery.Methods—We assessed all cases of a low-lying placenta, definedas a placenta ending within 2 cm of the internal cervical os, diagnosedby sonography between 16 and 24 weeks’ gestation from July 1,2007, to September 4, 2011. We reviewed medical records to determine thegestational age when a low-lying placenta was diagnosed, the gestationalage at which the placenta was no longer low lying or previa, and, for thosewhose placentas never cleared sonographically, how many went on to cesareansection for placenta previa.Results—A total of 1416 pregnancies were diagnosed with alow-lying placenta between 16 and 24 weeks’ gestation. Of these, 174were lost to follow-up. Of the remaining 1242 pregnancies, 1220 (98.2%)resolved to no previa prior to delivery. The mean age at resolution was26.0 weeks. The age at resolution was similar in those diagnosed prior to20 weeks’ gestation to those diagnosed after 20 weeks. Approximately77% of placentas that eventually cleared did so before 29 weeks. Twentytwopatients had persistent placenta previa by sonography at or near term,all of which were confirmed at cesarean section.Conclusions—A low-lying placenta diagnosed between 16 and24 weeks rarely (1.8% of the time) persists as placenta previa to term, necessitatingcesarean section. Most cases resolve during the early thirdtrimester. Thus, we suggest that reevaluation of the placental location insuch cases be performed at approximately 28 to 30 weeks, not earlier.In addition, patients diagnosed with a low-lying placenta in the secondtrimester can be reassured that the likelihood of persistent placenta previaat the time of delivery is small.1533371 Association Between Transvaginal UltrasonographicCervical Characteristics and Preterm Delivery After aHistory-Indicated CerclageEmily Miller,* Susan Gerber Maternal-Fetal Medicine,Northwestern University, Chicago, Illinois USAObjectives—To assess the relationship between the transvaginalultrasonographic characteristics of the cervix in the mid trimester andthe risk of delivery prior to 34 weeks in women with a history-indicatedcerclage.Methods—A retrospective case-control study of subjects witha singleton gestation and a history-indicated cerclage placed in the firsttrimester. Transvaginal ultrasound images of the cervix at the time of theanatomic survey in the second trimester were reviewed, and measurementsof cervical length (CL) proximal and distal to the cervical suture as wellas the presence or absence of funneling were recorded. χ 2 tests and logisticregression analysis were performed to evaluate the association betweenthese cervical variables and preterm birth prior to 34 weeks.Results—One hundred three subjects met inclusion criteria.Sixteen (15.5%) delivered prior to 34 weeks’ gestation. CL proximal to thesuture was lower in women who delivered prior to 34 weeks (1.6 vs 2.5cm; P = .005), whereas distal CL was similar (1.5 vs 1.7 cm; P = .18). Thefrequency of cervical funneling was higher in women who delivered priorto 34 weeks (57% vs 9%; P < .001). In multivariable regression, only thepresence of a cervical funnel remained significantly associated with an increasedrisk of preterm delivery before 34 weeks (Table 1).Conclusions—Cervical funneling is strongly associated withan increased risk of delivery before 34 weeks in women with a history-indicatedcerclage. Midtrimester transvaginal cervical imaging can be usedto augment risk assessment this patient population.Table 1. Odds Ratios for Birth Prior to 34 Weeks According to UltrasonographicCervical AppearanceOR 95% CI aOR 95% CIProximal CL 0.48 0.27–0.82 0.88 0.41–1.85Distal CL 0.46 0.14–1.45 0.64 0.19–2.21Cervical funnel present 13.5 3.74–48.74 9.96 1.62–61.03aOR indicates adjusted odds ratio; CI, confidence interval; and OR, odds ratio.S26