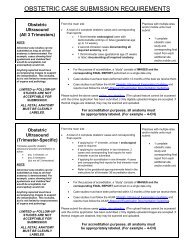
American Institute of Ultrasound in Medicine <strong>Proceedings</strong> J Ultrasound Med 32(suppl):S1–S134, 2013were diagnosed at the early second-trimester anatomy scan. No cases ofONTD were diagnosed after 18 weeks’ gestation, and no cases of ONTDwere missed by our unit (sensitivity, 100%).Conclusions—Ultrasound for a fetal anatomic survey duringthe first and early second trimesters detected 100% of ONTDs in our population,with the majority identified in the first trimester. MSAFP was notuseful as a screening tool for ONTDs in the setting of this ultrasoundscreening protocol. Given the sensitivity of first- and early secondtrimesterultrasound in detecting ONTDs, physicians may choose not tooffer MSAFP for this indication.1541097 Novel Insights Into Early Embryonic Demise via 3-Dimensional Surface-Rendered Imaging in 107 CasesDavid Hartge, Andreas Schroer, Jan Weichert* Division ofPrenatal Medicine, University of Schleswig-Holstein, Luebeck,Schleswig-Holstein, GermanyObjectives—Modern sonographic imaging techniques such as3D volumetry will be evaluated for 107 cases of pregnant women withmissed abortions in the first trimester. Special emphasis is put on the impactof additional information and improved visualization of embryonicand fetal anomalies due to application of newest imaging tools, eg, HDLive. Additionally, parental acceptance of a more realistic display of theembryo/fetus in missed abortion is analyzed.Methods—Between September 2009 and September 2012, 109pregnancies with a missed abortion during the first trimester were includedin this survey. Using a transvaginal approach, all studies were carried outwith high-resolution 5–9- and 6–12-MHz probes. Postrendering processingof actual and stored volume sets included application of HD Live technology.2D evaluation was also conducted during the same examination.Results—Two of 109 cases with a missed abortion were excludedfrom our study. In 1 case, the parents refused to participate in thesurvey. In another case, the 3D volume acquisition was not completed successfully.One hundred seven cases were included in the final evaluation.The mean gestational age was 70.4 days (range, 44–110 days). Meancrown-rump length (CRL) was 17.3 mm (2.9–49.9 mm). The differencebetween estimated gestational age and sonographic age at evaluation formissed abortion was 14.4 days (0–40 days). Sufficient sonographic evaluationwas possible in 91 of 107 cases (85.0%). Additional information via3D volume acquisition such as craniofacial deformities, clefts, neural tubedefects, abdominal wall defects, and sirenomelia could be documented in11 of 107 cases (10.3%), which were not detected by conventional 2D imaging.In 1 of 107 cases, the parents disapproved of the 3D visualizationdue to the more realistic presentation.Conclusions—3D ultrasound in cases of missed abortions canprovide additional information regarding the presence of structural anomaliesand may further give hints regarding the timing of embryonic/fetaldemise in early pregnancy. Based on our data, sufficient informationalvalue is regularly obtained in cases having a CRL >5 mm. In counselingparents, 3D ultrasound is a useful tool and is generally well accepted.1536871 Prenatal Sonographic Predictors of Surgery-TreatedUreteropelvic Junction Obstruction: Which Is the BestPredictor?Hadar Mudrik-Zohar, 1 * Israel Meizner, 1,2 Zvi Bar-Sever, 1,3David Ben-Meir, 1,4 Miriam Davidovits 1,5 1 Sackler Faculty ofMedicine, Tel Aviv University, Tel-Aviv, Israel; 2 GynecologicUltrasound Unit, Rabin Medical Center, Beilinson Campus,Petah Tikva, Israel; 3 Nuclear Medicine Institute, 4 PediatricUrology Unit, 5 Institute of Pediatric Nephrology, SchneiderChildren’s Medical Center, Petah Tikva, IsraelObjectives—Prenatally detected hydronephrosis (HN) with noevidence of ureter dilatation or bladder anomalies might suggest ureteropelvicjunction obstruction (UPJO), which requires postnatal pyeloplasty.Yet, in the majority of fetuses, the HN is transient and conservativelytreated. Our study aimed to identify prenatal sonographic predictors ofsurgery-treated UPJO and their cutoff values.Methods—This case-control study compared the sonographicprenatal findings of HN-diagnosed fetuses that underwentpyeloplasty after birth and HN-diagnosed fetuses that needed conservativemanagement only, all treated in Schneider Children’s MedicalCenter. We retrospectively evaluated 39 cases of patients who underwentpyeloplasty due to UPJO between 2001 and 2012 and 30 cases ofpatients that were diagnosed prenatally with HN and treated conservativelybetween 2005 and 2012. Prenatal sonographic data for both patientgroups were taken from the Gynecologic Ultrasound unit at RabinMedical Center. The main sonographic measures we tested were (1)anterior-posterior diameter (APD) of the affected kidney, (2) parenchymalthickness (PT), (3) calyces dilatation, and (4) renal length. A fewpatients had records of only some of the measures.Results—The prenatal APD dilatation of the surgery-treatedUPJO group (mean, 22.9 mm; SD, 8.7 mm) was higher than the controlgroup (mean, 14.3 mm; SD, 5.9 mm; P < .001). Furthermore, the PT in thesurgery-treated UPJO group (mean, 5.9 mm; SD, 2.8 mm) was lower thanthe control group (mean, 8.1 mm; SD, 2.6 mm; P = .009). Logistic regressionreveled that APD was the main parameter significantly associatedwith surgery-treated UPJO cases (receiver operating characteristic plotwas 0.79). A possible threshold of 14 mm APD may be used as a cutoffvalue of the surgery-treated UPJO group with sensitivity of 77% and specificityof 69%.Conclusions—APD dilatation was the strongest predictor ofsurgery-treated UPJO. PT and renal length also significantly discriminatethe two groups and correlate with APD, only with lower predictive power.Our findings expand the clinical knowledge in the field of prenatal consultationby highlighting a threshold of APD, which predicts the need forsurgery in prenatally detected HN cases.1540842 Prenatal Diagnosis and Neonatal Outcomes in NonimmuneHydrops: A Comparison of 2 Decades at an Academic CenterPadmalatha Gurram, 1 * Peter Benn, 2 Naveed Hussain, 3 ChristineCrawford, 1 Kisti Fuller, 1 Ann Marie Prabulos, 1 WinstonCampbell 1 1 Obstetrics and Gynecology, 2 Genetics and DevelopmentalBiology, 3 Pediatrics, University of Connecticut,Farmington, Connecticut USAObjectives—To evaluate the differences in the maternal characteristics,prenatal ultrasound (US) diagnosis and outcomes of nonimmunehydrops (NIH) delivered between 1990 and 2010.Methods—We performed a retrospective review of NIH casesdiagnosed antenatally and delivered at our institution. The cases were dividedinto 2 groups: 1990 to 1999 and 2000 to 2010. Stillbirths and multiplegestations were excluded. Gestational age (GA) at diagnosis, prenatalUS findings, GA at delivery, mode of delivery, birth weight (BW), postnataldiagnosis, length of neonatal intensive care unit (NICU) stay, survival>28 days, and mortality were compared.Results—In the 20-year period, there were 19 live-born casesof NIH (11 cases in the 1990 group vs 8 in the 2000 group). The meanGA at diagnosis was 2 weeks earlier in the 2000 group (Table 1). Asciteswas the most common US feature in both groups, followed by pleural effusion.Amniocentesis was done in 50% of cases in the 2000 group vs37.5% in 1990. The GA at delivery was similar in both groups, and BWwas lower in the 1990 group (Table 1). In the 1990 group, 10 of 11 caseswere delivered by cesarean delivery vs 8 of 8 in 2000. The etiologieswere cardiac (27%), idiopathic (27%), genetic (18%), and infectious(9%) in 1990 vs idiopathic (50%), genetic (25%), and cardiac (12.5%)in 2000. The average length of the NICU stay for cases that were dischargedhome alive in the 1990 group (4 of 11) was 28.5 days and in the2000 group (3 of 8) was 70 days. In the 2000 group, 3 of 8 cases weretransferred to other facilities compared to 1 of 11 cases in the 1990 groupS55
American Institute of Ultrasound in Medicine <strong>Proceedings</strong> J Ultrasound Med 32(suppl):S1–S134, 2013for further care. There were 6 of 11 deaths in the 1990 group vs 2 of 8deaths in 2000.Conclusions—The outcome of NIH cases improved in the laterdecade. The commonest etiology continues to be idiopathic.Table 1. Prenatal and Neonatal Characteristics1990–1999 (n = 11) 2000–2010 (n = 8)Mean GA at diagnosis, wk 31 29Ascites on US, % 63 75GA at delivery, wk 31 31BW, g 2018 2560Idiopathic etiology, % 27 50Survival >28 d, % 46 75Mortality, % 54 251528272 Qualitative Performance of Fetal Magnetic ResonanceImaging Compared to Ultrasound in Cases of MultipleFetal AnomaliesChristina Herrera,* Amber Samuel, Sherelle Laifer-Narin,Lynn Simpson, Russell Miller Obstetrics and Gynecology,Columbia University Medical Center, New York, New York USAObjectives—Pregnancies complicated by multiple fetal anomaliesare a common indication for fetal magnetic resonance imaging (MRI)as an adjunct to diagnostic ultrasound (US). This study investigated the diagnosticperformance of fetal MRI when compared to US alone for the accuratecharacterization of fetuses with multiple anomalies.Methods—In a retrospective review from 2003 to 2011 at a singletertiary care center, potential cases were identified if MRI was performedfollowing sonographic concern for multiple fetal anomalies.Inclusion required documented neonatal outcomes or postmortem assessments.Interstudy reliability between MRI and US was assessed by calculatingκ. Diagnostic accuracy of adjunct MRI compared to US alonewas assessed using qualitative statistics.Results—A total of 121 MRIs were performed due to antenatalsonographic concern for multiple fetal anomalies, of which 60 casespossessed documented neonatal or pathologic outcomes. The κ for MRIcompared with US was 0.28. The correct diagnosis was secured in 47%of cases by US and 50% of cases by MRI (Table 1). Nearly all inaccuratesonographic diagnoses were due to additional postnatal findings (48%).While MRI was most commonly inaccurate due to additional postnatalfindings (27%), discrepant postnatal findings (3%), discrepant and additionalpostnatal findings (13%), and false-positive imaging findings (5%)also contributed significantly to study inaccuracies.Conclusions—Agreement is poor between MRI and US for thecharacterization of fetuses with multiple anomalies. For either imagingmodality, complete and accurate diagnosis of fetal anomalies occurs inapproximately half of cases, with the majority of inaccuracies due to incompleteantenatal characterizations.Table 1US, n (%) MRI, n (%)Accurate diagnosis 28 (47) 30 (50)Additional anomalies discovered postnatally 29 (48) 16 (27)Discrepant findings between imaging and 2 (3) 2 (3)postnatal assessmentDiscrepant and additional anomalies 0 8 (13)False-positive imaging findings 1 (2) 3 (5)Study inconclusive 0 1 (2)S56