Overview of Electronic Secondary Claims (COB)
Overview of Electronic Secondary Claims (COB)
Overview of Electronic Secondary Claims (COB)
Create successful ePaper yourself
Turn your PDF publications into a flip-book with our unique Google optimized e-Paper software.
<strong>Electronic</strong> <strong>Secondary</strong> <strong>Claims</strong> (<strong>COB</strong>) <strong>Overview</strong>-NextGen® PM<br />
Claim Edits & Billing - Reviewing Claim Production Status Report<br />
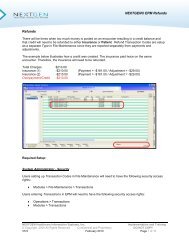
To prevent unbalanced secondary claims from creating, several claim edits are available:<br />
254: <strong>COB</strong> edit: Paid amount and patient responsible amounts do not equal allowed amount<br />
255: <strong>COB</strong> edit: All payments and adjustments do not equal billed amount<br />
256: Value code 39a <strong>of</strong> required for secondary institutional claim<br />
o Only for client‟s sending 837I<br />
261: <strong>Electronic</strong> <strong>COB</strong> claim requires adjudication date<br />
As with all claim edits, in order to prevent an encounter from producing a claim when the edit is fired, set<br />
the edit severity to „Required‟.<br />
If you set the claim edit severity to „Warning‟, you may correct the encounter and rebill before generating<br />
the next <strong>Secondary</strong> EDI file. Be sure to delete the previous claim generated. Otherwise two claims will<br />
be generated, one balanced and other unbalanced.<br />
<strong>COB</strong> edits will only fire if a Payer‟s <strong>Secondary</strong> Media Type is set to “Paper” and only when you are billing<br />
encounters.<br />
NEXTGEN® Healthcare, Inc. EPM<strong>Claims</strong><br />
© Copyright 2010 All Rights Reserved Confidential and Proprietary DO NOT COPY<br />
V5.6SP1 Sept2010 Page 25 <strong>of</strong> 29