Chapter 96
Create successful ePaper yourself
Turn your PDF publications into a flip-book with our unique Google optimized e-Paper software.
1650 PART 5 ■ Anesthetic, Surgical, and Interventional Procedures: Considerations<br />
congenitally-acquired disease may be asymptomatic, patients with<br />
acquired disease may be symptomatic from a respiratory perspective,<br />
owning to the acute change in diaphragmatic function.<br />
The diagnosis, regardless of etiology, can be assessed with<br />
diagnostic imaging tests, including ultrasound and fluoroscopy of<br />
the diaphragm, looking for paradoxical motion of the diaphragm.<br />
In the event that the diagnosis continues to be unclear, an upper<br />
gastrointestinal series can be obtained. Once a diagnosis is<br />
secured, the option of surgical repair is generally considered for all<br />
patients who are symptomatic and those patients who are<br />
asymptomatic but also have a markedly elevated hemidiaphragm<br />
that is compressing the ipsilateral lung. The surgical procedure<br />
involves plication of involved diaphragm; infrequently, a<br />
redundant portion of the diaphragm will have to be excised. The<br />
approach can be via abdominal or thoracic approach and can be<br />
via an open or thoracoscopic/laparoscopic technique. The latter<br />
technique has been slowly gaining favor among surgeons. A<br />
number of case reports and small case series have been published<br />
that advocate for the use of the laparoscopic/thoracoscopic<br />
techniques. 48 A study by Sato et al. noted that all of the cases were<br />
successfully completed with the thoracoscopic technique and there<br />
were no recurrences in long term follow-up.<br />
ANOMALIES OF THE<br />
LUNG AND AIRWAY<br />
Anomalies of the lung and airway are an area of pediatric surgery<br />
that is undergoing changes with respect to optimal treatment and<br />
management. Some authors have suggested that not all of these<br />
lesions need to be surgically excised and some can be safely<br />
monitored. 49 Aziz et al. have suggested that asymptomatic<br />
congenital cystic adenomatoid malformations can be observed.<br />
Other authors, such as Azizkhan et al., have suggested that all of<br />
these asymptomatic lesions be surgically excised. 50 This remains a<br />
very controversial area and there remains considerable disagreement<br />
on this topic. This section will focus on the current<br />
treatment options for these largely congenital anomalies and will<br />
mention areas of controversy where it alters clinical management;<br />
included in this section is a discussion of spontaneous pneumothorax,<br />
which may be congenital or acquired in origin.<br />
Congenital Pulmonary<br />
Airway Malformation<br />
These lesions are referred to as congenital cystic adenomatoid<br />
malformations (CCAMs) or more recently as congenital<br />
pulmonary airway malformations (CPAMs). They can be<br />
macrocystic, macrocytic, or solid masses which may involve all or<br />
a portion of the lobe of the lung; they communicate with the<br />
airway and usually do not have anomalous blood vessels. There<br />
are a number of histologic subtypes, which embryologically<br />
contain no cartilage and arise from the excessive proliferation of<br />
bronchial structures without alveoli. 51 These lesions are now<br />
diagnosed in three clinical settings: (1) on antenatal ultrasound<br />
examination, (2) when the child presents with symptoms related<br />
to respiratory distress or pulmonary infection (pneumonia and/<br />
or intrapulmonary abscess), or (3) when the lung anomaly is<br />
discovered incidentally on diagnostic chest imaging. The<br />
former examinations have demonstrated that these lesions can<br />
have dramatically distinct clinical courses, including complete<br />
resolution of the lesion before birth, little change in the size of the<br />
lesion, progressive enlargement of the lesion, and in utero demise<br />
related to compression of the heart with impairment of central<br />
venous return, ultimately leading to hydrops.<br />
The primary preoperative indications for surgical resection<br />
of these lesions are: (1) respiratory distress from direct compression<br />
of adjacent intrathoracic structures, (2) prevention of<br />
pulmonary infection (or recurrent pulmonary infection), and (3)<br />
prevention of possible pulmonary malignancy. The latter<br />
indication is one of the most controversial, because it is unclear<br />
whether these malignancies have arisen from a benign congenital<br />
lung lesion or whether the diagnosis of the benign congenital lung<br />
lesion has been in error and the lesion is, in fact, a malignancy.<br />
These lesions are optimally assessed with CT scan imaging,<br />
although ultrasound can be used for lesions that are fluid-filled or<br />
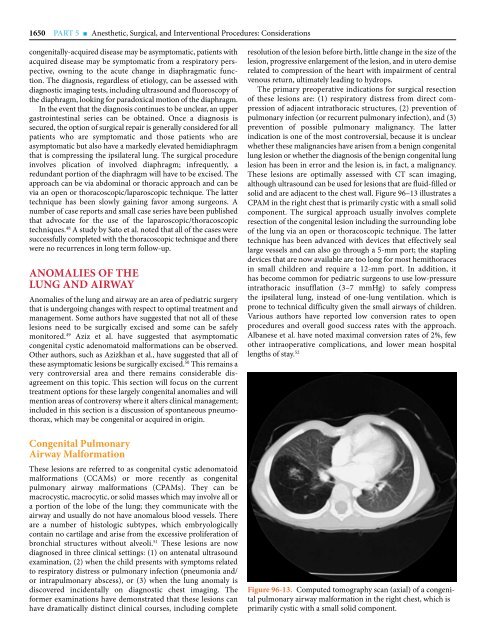
solid and are adjacent to the chest wall. Figure <strong>96</strong>–13 illustrates a<br />
CPAM in the right chest that is primarily cystic with a small solid<br />
component. The surgical approach usually involves complete<br />
resection of the congenital lesion including the surrounding lobe<br />
of the lung via an open or thoracoscopic technique. The latter<br />
technique has been advanced with devices that effectively seal<br />
large vessels and can also go through a 5-mm port; the stapling<br />
devices that are now available are too long for most hemithoraces<br />
in small children and require a 12-mm port. In addition, it<br />
has become common for pediatric surgeons to use low-pressure<br />
intrathoracic insufflation (3–7 mmHg) to safely compress<br />
the ipsilateral lung, instead of one-lung ventilation. which is<br />
prone to technical difficulty given the small airways of children.<br />
Various authors have reported low conversion rates to open<br />
procedures and overall good success rates with the approach.<br />
Albanese et al. have noted maximal conversion rates of 2%, few<br />
other intraoperative complications, and lower mean hospital<br />
lengths of stay. 52<br />
Figure <strong>96</strong>-13. Computed tomography scan (axial) of a congenital<br />
pulmonary airway malformation in the right chest, which is<br />
primarily cystic with a small solid component.