Chapter 96
You also want an ePaper? Increase the reach of your titles
YUMPU automatically turns print PDFs into web optimized ePapers that Google loves.
1648 PART 5 ■ Anesthetic, Surgical, and Interventional Procedures: Considerations<br />
can accommodate the repair, which includes closure of the<br />
sternal defect, repair of the diaphragmatic hernia, and closure of<br />
the omphalocele. 30<br />
Pectus Excavatum<br />
Pectus excavatum accounts for approximately 90% of chest wall<br />
defects, with an incidence of 1 in 300 live births. The etiology is<br />
possibly related to the overgrowth of cartilage in the adjacent ribs,<br />
displacing the sternum posteriorly. Clinically, it presents more<br />
commonly in boys at a ratio of 3:1, becoming more progressive in<br />
posterior displacement as the child enters puberty. It is associated<br />
with Marfan’s syndrome (2% of cases), diaphragmatic abnormalities<br />
(2% of cases) and congenital heart disease (1.5%). 31<br />
Patients may present asymptomatically or may have complaints of<br />
chest pain, palpitations, and asthma-like symptoms. There<br />
continues to be considerable debate about the clinical impact of<br />
this defect upon cardiovascular and pulmonary function.<br />
Intuitively, the compression of the heart and the lungs by the<br />
sternum should result in dysfunction. Lower lung volumes and<br />
decreased cardiac output have been recorded in patients with<br />
severe defects during exercise; 32–33 improvements in function have<br />
been demonstrated in patients postoperatively. Indications for<br />
surgical repair are more commonly psychological, related to issues<br />
around poor self-image, and less commonly related to issues of<br />
physiologic compromise of clinically relevant cardiopulmonary<br />
dysfunction; the latter may be important for a patient with a severe<br />
defect who also happens to be a competitive athlete.<br />
The occasional child with a concurrent diagnosis of Marfan’s<br />
syndrome or congenital heart disease should be considered for<br />
repair of the chest wall defect before open heart surgery to avert<br />
the issues of compression of the cardiac structures. The surgical<br />
options are essentially two: the Ravitch procedure (an open<br />
surgical approach) and the Nuss procedure (a minimally invasive<br />
approach). The former technique has been used for more than 50<br />
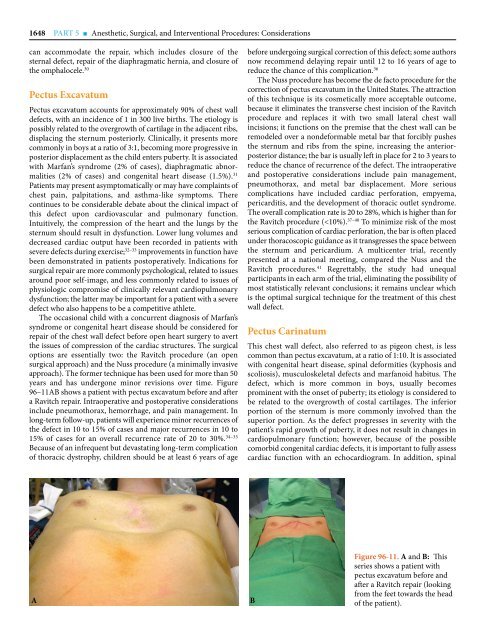
years and has undergone minor revisions over time. Figure<br />
<strong>96</strong>–11AB shows a patient with pectus excavatum before and after<br />
a Ravitch repair. Intraoperative and postoperative considerations<br />
include pneumothorax, hemorrhage, and pain management. In<br />
long-term follow-up, patients will experience minor recurrences of<br />
the defect in 10 to 15% of cases and major recurrences in 10 to<br />
15% of cases for an overall recurrence rate of 20 to 30%. 34–35<br />
Because of an infrequent but devastating long-term complication<br />
of thoracic dystrophy, children should be at least 6 years of age<br />
before undergoing surgical correction of this defect; some authors<br />
now recommend delaying repair until 12 to 16 years of age to<br />
reduce the chance of this complication. 36<br />
The Nuss procedure has become the de facto procedure for the<br />
correction of pectus excavatum in the United States. The attraction<br />
of this technique is its cosmetically more acceptable outcome,<br />
because it eliminates the transverse chest incision of the Ravitch<br />
procedure and replaces it with two small lateral chest wall<br />
incisions; it functions on the premise that the chest wall can be<br />
remodeled over a nondeformable metal bar that forcibly pushes<br />
the sternum and ribs from the spine, increasing the anteriorposterior<br />
distance; the bar is usually left in place for 2 to 3 years to<br />
reduce the chance of recurrence of the defect. The intraoperative<br />
and postoperative considerations include pain management,<br />
pneumothorax, and metal bar displacement. More serious<br />
complications have included cardiac perforation, empyema,<br />
pericarditis, and the development of thoracic outlet syndrome.<br />
The overall complication rate is 20 to 28%, which is higher than for<br />
the Ravitch procedure (