EUROHEALTH
Eurohealth-volume22-number2-2016
Eurohealth-volume22-number2-2016
You also want an ePaper? Increase the reach of your titles
YUMPU automatically turns print PDFs into web optimized ePapers that Google loves.
26<br />
Moving towards universal health coverage<br />
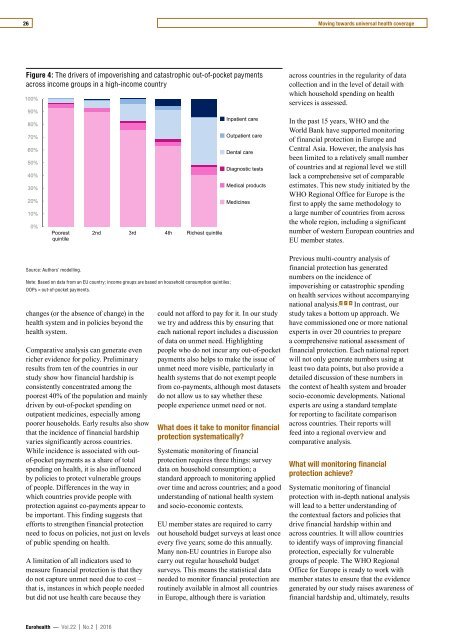
Figure 4: The drivers of impoverishing and catastrophic out-of-pocket payments<br />
across income groups in a high-income country<br />
100%<br />
90%<br />
80%<br />
70%<br />
60%<br />
50%<br />
40%<br />
30%<br />
20%<br />
10%<br />
0%<br />
Poorest<br />
quintile<br />
Source: Authors’ modelling.<br />
Note: Based on data from an EU country; income groups are based on household consumption quintiles;<br />
OOPs = out-of-pocket payments.<br />
changes (or the absence of change) in the<br />
health system and in policies beyond the<br />
health system.<br />
Comparative analysis can generate even<br />
richer evidence for policy. Preliminary<br />
results from ten of the countries in our<br />
study show how financial hardship is<br />
consistently concentrated among the<br />
poorest 40% of the population and mainly<br />
driven by out-of-pocket spending on<br />
outpatient medicines, especially among<br />
poorer households. Early results also show<br />
that the incidence of financial hardship<br />
varies significantly across countries.<br />
While incidence is associated with outof-pocket<br />
payments as a share of total<br />
spending on health, it is also influenced<br />
by policies to protect vulnerable groups<br />
of people. Differences in the way in<br />
which countries provide people with<br />
protection against co-payments appear to<br />
be important. This finding suggests that<br />
efforts to strengthen financial protection<br />
need to focus on policies, not just on levels<br />
of public spending on health.<br />
A limitation of all indicators used to<br />
measure financial protection is that they<br />
do not capture unmet need due to cost –<br />
that is, instances in which people needed<br />
but did not use health care because they<br />
2nd 3rd 4th Richest quintile<br />
Inpatient care<br />
Outpatient care<br />
Dental care<br />
Diagnostic tests<br />
Medical products<br />
Medicines<br />
could not afford to pay for it. In our study<br />
we try and address this by ensuring that<br />
each national report includes a discussion<br />
of data on unmet need. Highlighting<br />
people who do not incur any out-of-pocket<br />
payments also helps to make the issue of<br />
unmet need more visible, particularly in<br />
health systems that do not exempt people<br />
from co-payments, although most datasets<br />
do not allow us to say whether these<br />
people experience unmet need or not.<br />
What does it take to monitor financial<br />
protection systematically?<br />
Systematic monitoring of financial<br />
protection requires three things: survey<br />
data on household consumption; a<br />
standard approach to monitoring applied<br />
over time and across countries; and a good<br />
understanding of national health system<br />
and socio-economic contexts.<br />
EU member states are required to carry<br />
out household budget surveys at least once<br />
every five years; some do this annually.<br />
Many non-EU countries in Europe also<br />
carry out regular household budget<br />
surveys. This means the statistical data<br />
needed to monitor financial protection are<br />
routinely available in almost all countries<br />
in Europe, although there is variation<br />
across countries in the regularity of data<br />
collection and in the level of detail with<br />
which household spending on health<br />
services is assessed.<br />
In the past 15 years, WHO and the<br />
World Bank have supported monitoring<br />
of financial protection in Europe and<br />
Central Asia. However, the analysis has<br />
been limited to a relatively small number<br />
of countries and at regional level we still<br />
lack a comprehensive set of comparable<br />
estimates. This new study initiated by the<br />
WHO Regional Office for Europe is the<br />
first to apply the same methodology to<br />
a large number of countries from across<br />
the whole region, including a significant<br />
number of western European countries and<br />
EU member states.<br />
Previous multi-country analysis of<br />
financial protection has generated<br />
numbers on the incidence of<br />
impoverishing or catastrophic spending<br />
on health services without accompanying<br />
national analysis. 2 7 8 In contrast, our<br />
study takes a bottom up approach. We<br />
have commissioned one or more national<br />
experts in over 20 countries to prepare<br />
a comprehensive national assessment of<br />
financial protection. Each national report<br />
will not only generate numbers using at<br />
least two data points, but also provide a<br />
detailed discussion of these numbers in<br />
the context of health system and broader<br />
socio-economic developments. National<br />
experts are using a standard template<br />
for reporting to facilitate comparison<br />
across countries. Their reports will<br />
feed into a regional overview and<br />
comparative analysis.<br />
What will monitoring financial<br />
protection achieve?<br />
Systematic monitoring of financial<br />
protection with in-depth national analysis<br />
will lead to a better understanding of<br />
the contextual factors and policies that<br />
drive financial hardship within and<br />
across countries. It will allow countries<br />
to identify ways of improving financial<br />
protection, especially for vulnerable<br />
groups of people. The WHO Regional<br />
Office for Europe is ready to work with<br />
member states to ensure that the evidence<br />
generated by our study raises awareness of<br />
financial hardship and, ultimately, results<br />
Eurohealth — Vol.22 | No.2 | 2016