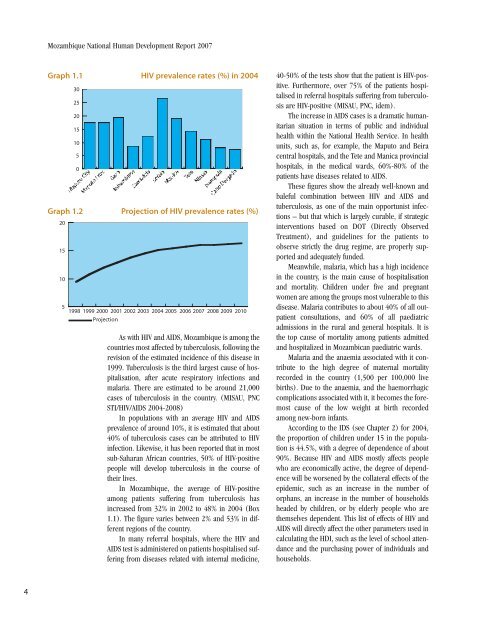
Mozambique National <strong>Human</strong> <strong>Development</strong> Report 2007Graph 1.1 HIV prevalence rates (%) in 2004201510302520151050Graph 1.2 Projection of HIV prevalence rates (%)51998 1999 2000 2001 2002 2003 2004 2005 2006 2007 2008 2009 2010ProjectionAs with HIV and AIDS, Mozambique is among thecountries most affected by tuberculosis, following therevision of the estimated incidence of this disease in1999. Tuberculosis is the third largest cause of hospitalisation,after acute respiratory infections andmalaria. There are estimated to be around 21,000cases of tuberculosis in the country. (MISAU, PNCSTI/HIV/AIDS 2004-2008)In populations with an average HIV and AIDSprevalence of around 10%, it is estimated that about40% of tuberculosis cases can be attributed to HIVinfection. Likewise, it has been reported that in mostsub-Saharan African countries, 50% of HIV-positivepeople will develop tuberculosis in the course oftheir lives.In Mozambique, the average of HIV-positiveamong patients suffering from tuberculosis hasincreased from 32% in 2002 to 48% in 2004 (Box1.1). The figure varies between 2% and 53% in differentregions of the country.In many referral hospitals, where the HIV andAIDS test is administered on patients hospitalised sufferingfrom diseases related with internal medicine,40-50% of the tests show that the patient is HIV-positive.Furthermore, over 75% of the patients hospitalisedin referral hospitals suffering from tuberculosisare HIV-positive (MISAU, PNC, idem).The increase in AIDS cases is a dramatic humanitariansituation in terms of public and individualhealth within the National Health Service. In healthunits, such as, for example, the Maputo and Beiracentral hospitals, and the Tete and Manica provincialhospitals, in the medical wards, 60%-80% of thepatients have diseases related to AIDS.These figures show the already well-known andbaleful combination between HIV and AIDS andtuberculosis, as one of the main opportunist infections– but that which is largely curable, if strategicinterventions based on DOT (Directly ObservedTreatment), and guidelines for the patients toobserve strictly the drug regime, are properly supportedand adequately funded.Meanwhile, malaria, which has a high incidencein the country, is the main cause of hospitalisationand mortality. Children under five and pregnantwomen are among the groups most vulnerable to thisdisease. Malaria contributes to about 40% of all outpatientconsultations, and 60% of all paediatricadmissions in the rural and general hospitals. It isthe top cause of mortality among patients admittedand hospitalized in Mozambican paediatric wards.Malaria and the anaemia associated with it contributeto the high degree of maternal mortalityrecorded in the country (1,500 per 100,000 livebirths). Due to the anaemia, and the haemorrhagiccomplications associated with it, it becomes the foremostcause of the low weight at birth recordedamong new-born infants.According to the IDS (see Chapter 2) for 2004,the proportion of children under 15 in the populationis 44.5%, with a degree of dependence of about90%. Because HIV and AIDS mostly affects peoplewho are economically active, the degree of dependencewill be worsened by the collateral effects of theepidemic, such as an increase in the number oforphans, an increase in the number of householdsheaded by children, or by elderly people who arethemselves dependent. This list of effects of HIV andAIDS will directly affect the other parameters used incalculating the HDI, such as the level of school attendanceand the purchasing power of individuals andhouseholds.4
<strong>Human</strong> <strong>Development</strong>, HIV and AIDS in MozambiqueBox 1.1Tuberculosis (TB) remains one of the most seriousglobal threats to public health. In March 2006Tuberculosis was declared a national emergency inMozambique. Mozambique is among the 22 countriesin the world most affected by TB (the HBC), withan estimated 91,000 cases in 2006 and an incidenceof 460 per 100,000 inhabitants in 2004.The incidence of TB has been growing rapidly inthe last 10 years, due, above all, to its association withHIV. In 1998, HIV prevalence among adult tuberculosispatients (aged 15-49) was 32% (that is, one out ofevery three tuberculosis patients was HIV-positive).In 2004, the HIV prevalence among adult tuberculosispatients was 48% (that is, one out of everytwo tuberculosis patients). Due to this association,and because tuberculosis is the opportunist diseasemost associated with AIDS, mortality among tuberculosispatients has been increasing. The most dramaticsituations are in Manica, Sofala and Gaza.Tuberculosis is not distributed equally across thecountry. The association of tuberculosis with HIV isvery serious in the central provinces, particularly inManica and Sofala, followed by Gaza, MaputoProvince and Maputo City.For example, data from studies held in the centralcity of Beira in 2003 and 2004 show that almost3,200 new cases of TB were recorded per year, whichis an incidence of 566 per 100,000 people.The patho-physiological link between TB andHIV is extremely deadly, since co-infection with HIVsignificantly increases the possibility of activatinglatent TB or a greater risk of re-infection, due to thelow immunity. Furthermore, the immunological stimuluscaused by TB can also increase the HIV viral load,the rate of progression of HIV and lead to higher mortality.It is this link between HIV and TB which has led tothe appearance of the terms “co-epidemic” or “doubleepidemic” to describe the lethal marriagebetween the two illnesses in the same patient.Due to the great number of patients living withTB and HIV, the World Health Organisation (WHO)has, since 2000, recommended and encouraged thestrengthening of an integrated approach betweenthe programmes controlling the two epidemics insub-Saharan Africa.HIV and Tuberculosis: Double epidemicThis integrated approach could facilitate, to agreat extent, the rapid and efficient diagnosis of dualHIV-TB infection, and provide beneficial interventionssuch as chemoprophylaxis with cotrimoxazol,reducing mortality among patients with dual HIV-TBinfection, and leading to a effective coordination oftuberculosis treatment and the concomitant administrationof anti-retrovirals.The National Tuberculosis Control Programme, setup in 1977, has used supervised treatment since 1984.Later, when WHO re-established the GlobalTuberculosis Programme in 1991, Mozambique contributedwith its experience to the world launch of thestrategy of the Directly Observed Treatment ShortCourse (DOTS). Under the current conditions of coverageby the national health network, the number ofcases detected is still well below the recommendedlevel. DOTS now covers about 40% of the population.The targets set by the WHO’s Global TuberculosisProgramme stipulate detection of 70% of the infectiouscases (that is, the pulmonary ones, since it is thesethat spread the disease) and the cure of 85% of them.The data presented by the National TuberculosisControl Programme (PNCTL) for 2005, indicate a detectionrate of 48% and a cure rate of 80%.The coordinated efforts of the sector, includingwith foreign partners, seeks to extend the coverageof the TB Programme to identifying 70% of cases,with a success rate of at least 85%, by 2010.The treatment of tuberculosis is the only way ofreducing the sources of infection in a community.Thus detecting and treating these cases is the priorityfor any tuberculosis programme in the world. Onecase of infectious (pulmonary) tuberculosis can infect10 to 20 people per year.Tuberculosis is curable and in Mozambique itstreatment is free of charge, as is Cotrimoxazol forchemoprophylaxy for tuberculosis patients withAIDS.Between 1995 and 2004, about 22 millionpatients were treated by the DOTS strategy acrossthe world. Internationally, 183 (of 192) countrieswere implementing the DOTS strategy in late 2004.The Millennium <strong>Development</strong> Goals include targetsfor containing the prevalence of and deathsfrom TB by 2015.5